Abstract
Purpose
This study aimed at comparing the diagnostic accuracy of ultrasonography (US) and magnetic resonance imaging (MRI) for the detection of joint effusion of the knee.
Methods
For this retrospective study, approbation by the institutional review board was not required, and written informed consent from the patients was waived. One hundred and fifty-eight patients (83 men and 75 women; median age 41.2 years; age range 13–81 years) who underwent US and MRI of the knee were included in the study. The sensitivity and specificity of US with respect to MRI in the evaluation of the effusion of the knee and in each recess were compared.
Results
In evaluating joint effusion of the knee, compared with MRI, US correctly identified 78 of 96 patients with joint effusion, showing a sensitivity of 81.3 % and a specificity of 100 %, with a positive predictive value (PPV) of 100 % and a negative predictive value (NPV) of 77.5 % (p value = 0.001). Various results were obtained comparing ultrasound with MRI, regarding the various recesses.
Conclusion
US showed high specificity and sensitivity in diagnosing knee joint effusion and could be used in patients who cannot undergo MRI.
Electronic supplementary material
The online version of this article (doi:10.1007/s40477-015-0180-3) contains supplementary material, which is available to authorized users.
Keywords: Ultrasound, Magnetic resonance imaging, Knee, Knee effusion
Riassunto
Scopo
Confrontare l’accuratezza diagnostica dell’ecografia (US) e la risonanza magnetica (MRI) per il rilevamento di versamento articolare del ginocchio.
Metodi
Per questo studio retrospettivo, non e’ stata necessaria formale approvazione da parte del Comitato Etico, ed e’ stato derogato il consenso informato scritto. Centocinquanta pazienti (83 uomini e 75 donne; età media: 41,2 anni; range di età: 13–81 anni) sottoposti a US e MRI del ginocchio sono stati inclusi nello studio. E’ stata valutata la sensibilità e la specificità dell’ US rispetto allan MRI nella valutazione del versamento del ginocchio e in ciascun recesso.
Risultati
Nella valutazione versamento articolare del ginocchio, rispetto alla MRI, l’ US ha identificato correttamente 78 su 96 pazienti con versamento articolare, mostrando una sensibilità del 81,3 % e una specificità del 100 %, con un valore predittivo positivo (PPV) del 100 % e un valore predittivo negativo (VPN) del 77,5 % (p value = 0.001). Risultati differenti sono stati ottenuti confrontando l’US con la MRI per quanto riguarda i vari recessi.
Conclusione
l’US ha mostrato elevata specificità e sensibilità nella diagnosi del ginocchio versamento articolare e potrebbe essere utilizzato in pazienti che non possono essere sottoposti a MRI.
Electronic supplementary material
The online version of this article (doi:10.1007/s40477-015-0180-3) contains supplementary material, which is available to authorized users.
Introduction
The synovial membrane plays an important role in the dynamics of the knee joint and in its pathology. The synovium is composed of thin connective tissue and is responsible for the secretion of synovial fluid, which lubricates and nourishes the joint and the removal of intra-articular debris. The synovial space of the knee consists of several interconnected structures [1, 2]. The anterior compartment contains the suprapatellar pouch (Fig. 1) (movie 1, 2). The superior and inferior intra-hoffatic recesses are contained within the Hoffa’s fat pad (Fig. 2) (movie 1). The synovium is displaced posterior to the infrapatellar fat pad of Hoffa, below the patella [3]. The central portion of the synovial membrane covers the anterior aspects of the cruciate ligaments, and it is reflected posteriorly onto the adjoining fibrous capsule (Fig. 3). A small synovial pouch, the popliteal recess, is present between the posterior aspect of the lateral meniscus and popliteus tendon (Fig. 4) (movie 4) [4, 5]. Along the medial and lateral aspects of the capsule, the synovial membrane extends inferiorly to the meniscal attachments, creating the perimeniscal recesses above and below the meniscal margins (Figs. 5, 6) (movie 4) [4, 5]. Posteriorly, there are three recesses—two deep, lateral and medial, and one in the midline, behind the posterior cruciate ligament (Fig. 7). The popliteal (Baker’s) cysts may be considered an articular recess (Figs. 8, 9) (movie 4) [6]. The knee joint communicates with the proximal tibiofibular joint in approximately 10 % of adults. Therefore, in patients with knee effusion, this may be present also in the tibiofibular joint (Fig. 10) (movie 4) [4, 5].
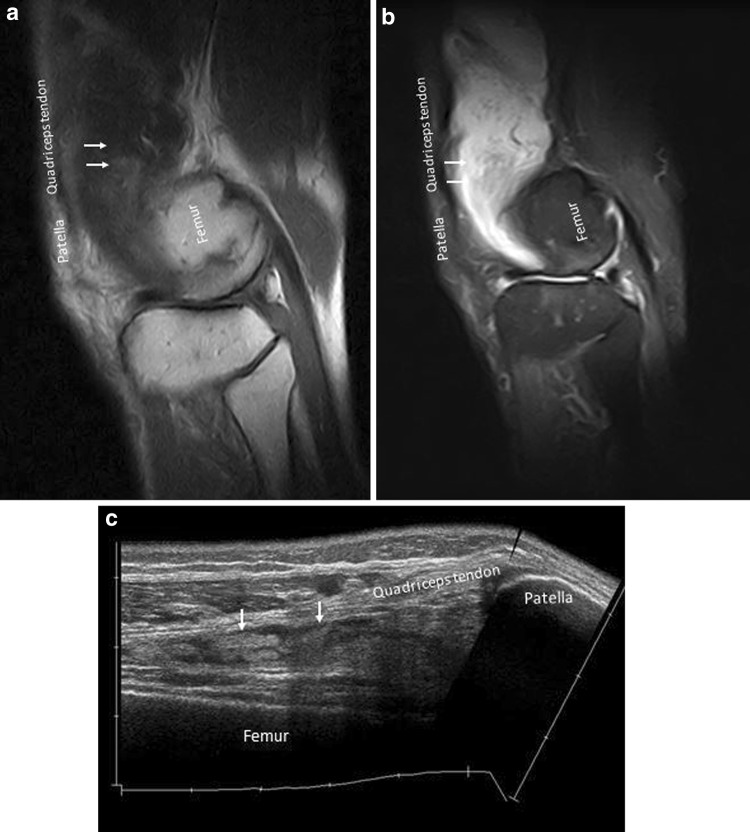
Fig. 1.
Suprapatellar pouch. Sagittal proton density fat suppressed image (a) and sonography (b) show fluid in the suprapatellar pouch (arrows) located between the quadriceps tendon and the femur
Fig. 2.
Infra-hoffatic recesses. Sagittal proton density fat suppressed image (a, b) and sonography (c) show within Hoffa’s fat pad, a vertically oriented superior supra-hoffatic recess (a) (arrow) and an horizontally oriented inferior infra-hoffatic (b, c) (arrow) recess
Fig. 3.

Central portion of the synovia. Sagittal proton density fat suppressed image shows the central portion of the synovial membrane (arrows) covering the anterior aspects of the anterior cruciate ligament (Ant cr lig)
Fig. 4.
Popliteal recess. Coronal proton density fat suppressed image (a) and sonography (b) shows a small pouch (arrow) between the posterior aspect of the lateral meniscus and popliteus tendon
Fig. 5.
Lateral perimeniscal recesses. Coronal proton density fat suppressed image (a) and sonography (b) show recesses above (arrow) and below (double arrow) the meniscal margin
Fig. 6.
Medial perimeniscal recesses. Coronal proton density fat suppressed image (a) and sonography (b) show recesses above (arrow) and below (double arrow) the meniscal margin
Fig. 7.

Posterior recesses. Axial T2W image showing fluid in the sub-gastrocnemius recesses, deep to the medial (double arrow), lateral (arrow) gastrocnemius tendons and to the posterior cruciate ligament (black arrow)
Fig. 8.

Gastrocnemius–semimembranosus bursa (popliteal or Baker’s cyst). Axial T2W image (a) and sonography images (b) show gastrocnemius–semimembranosus bursa (popliteal or Baker’s cysts) located posteriorly between the tendon of the semimembranosus (Semim ten) and the medial head of the gastrocnemius
Fig. 9.
Rupture of a popliteal cyst. Coronal proton density fat suppressed image (a) and sonography (b) show cyst rupture with synovial fluid surrounding the adjacent soft tissues, extending inferiorly from the cyst along the medial head of gastrocnemius
Fig. 10.
Proximal tibiofibular synovial “cyst”. Coronal (a) and sagittal (b) proton density fat suppressed images and sonography (c) show a cystic lesion extending from the proximal tibiofibular joint (arrow)
The first manifestation of synovial disease is joint effusion. Knee effusion may be the result of trauma, overuse or systemic disease. Overuse syndromes, ligamentous, osseous and meniscal injuries are the most common causes of effusion. Arthritis, infections, crystal deposition, pigmented villonodular synovitis, osteochondromatosis and tumors are other possible causes of effusion (Figs. 11, 12) [7–12]. A thorough medical history, systematic physical examination, appropriate use of diagnostic imaging and arthrocentesis, are essential to establish the correct diagnosis and treatment [2].
Fig. 11.
Pigmented villonodular synovitis. Sagittal T1W (a), sagittal proton density fat suppressed image (b) and sonography (c) show diffuse multifocal synovial depositions in the suprapatellar pouch, hypointense due to the paramagnetic effect of hemosiderin
Fig. 12.
Synovial chondromatosis. Sagittal proton density fat suppressed image (a, b) and sonography (c) show loose bodies in the suprapatellar pouch (a) and in the infra-hoffatic recess (b, c)
While the role of radiography, computed tomography and magnetic resonance imaging are widely described in the medical literature, the role of ultrasonography in the evaluation of the knee joint is poorly understood [2, 4, 5]. We have reviewed ultrasound examinations of the knee of patients who also underwent MRI and have compared the diagnostic accuracy for evaluating knee joint effusion using MRI as a gold standard.
Materials and methods
Inclusion criteria
Institutional review board approval was not required because of the retrospective nature of the study, and the information obtained was recorded by the investigator in such a manner that subjects could not be identified, directly or through identifiers linked to the subjects. Written informed consent from patients was waived. One hundred and fifty-eight patients (83 men and 75 women; mean age 41.2 years; age range 13–81 years) who underwent an ultrasound examination of the knee from May 2013 to May 2014 and an MRI of the knee during the following two weeks (range 1–15 days; mean 8 days) were eligible for the study.
Ultrasonography
Sonography was performed using a linear multi-frequency probe on an ACUSONS 2000 (Siemens, Erlangen, Germany), a Philips IU22 (Philips Medical System, The Netherlands), a GE LOGIC E9 (GE Healthcare, USA), a Toshiba Aplio 500 system (Toshiba Corporation, Japan), or a Philips Epic 7 (Philips Medical System, The Netherlands).
The patients were placed in the supine position with the knee in extension to evaluate the suprapatellar pouch, inferior infrahoffatic recesses, perimeniscal recesses and the popliteus tendon recess. They were also placed prone to evaluate the popliteal fossa and proximal tibiofibular joint. Particularly, the examination of the suprapatellar pouch was performed using an extended knee avoiding quadriceps muscle contraction and avoiding excessive probe compression to prevent effusion migration (movie 2). This could also guarantee that MRI and ultrasound examination were performed with patients in the same position. Imaging of the contralateral knee, as well as dynamic examination, was not performed. The total examination time was approximately 10 min.
Magnetic resonance imaging
MR imaging of the knee was performed using a 1.5-T unit (Siemens Symphony, Erlangen, Germany) and a 0.25-T unit (Esaote; E-scan, Genova, Italy). Image acquisition includes sagittal T1-weighted and either short tau inversion recovery (STIR), proton density (PD) or gradient echo sequences (GRE) in orthogonal planes depending on the machine used.
Data analysis
Images were reviewed by a radiologist (F.D.) with more than 20 years of experience in musculoskeletal ultrasound and magnetic resonance imaging. The results of ultrasound with respect to MRI in the evaluation of knee effusion and in each recess were compared. The presence of pain, chondropathy, cruciate ligament lesions, meniscal pathology and bone edema were considered.
Descriptive statistics were produced for the demographic, clinical and laboratory characteristics of cases. The mean and standard deviation (SD) are presented for normally distributed variables, the median and interquartile range (IQR) for non-normally distributed variables and the number and percentages for categorical variables. Groups were compared with parametric or nonparametric tests, according to data distribution, for continuous variables, and with Pearson’s χ2 test (Fisher exact test where appropriate) for categorical variables.
Cohen’s kappa coefficient was used to assess concordance between MRI and US at each anatomical site. Moreover, the sensitivity, specificity and positive and negative predictive values for US (with MRI as gold-standard) were calculated. Two-tailed tests were used throughout. The p value significance cut-off was 0.05.
To consider the panel data structure (two radiological techniques per each site, multiple sites per knee, and sometimes two knees involved per patient), multilevel mixed logistic regression models were fitted to assess the association between effusion and specific sites (sites were fixed effects, patients, knees, and radiological technique were random effects).
Results
The results are reported in Tables 1 and 2.
Table 1.
Diagnostic performance of US compared with MRI in evaluating knee joint effusion
| NO | MRI (%) | Sonography (%) | |
|---|---|---|---|
| Effusion | 62 | 96 (60.76) | 78 (81.25) |
| Suprapatellar pouch | 77 | 81 (51.27) | 54 (66.67) |
| Anterior aspects of the cruciate ligaments | 89 | 69 (43.67) | 0 |
| Lateral inferior perimeniscal recess | 108 | 50 (31.65) | 48 (96.00) |
| Lateral superior perimeniscal recess | 114 | 44 (27.85) | 42 (95.45) |
| Popliteus recess | 119 | 39 (24.68) | 38 (97.44) |
| Medial posterior recess | 134 | 24 (15.19) | 0 |
| Lateral posterior recess | 138 | 20 (12.66) | 0 |
| Inferior infra-hoffatic recess | 138 | 20 (12.66) | 14 (70.00) |
| Baker’s cyst | 140 | 18 (11.39) | 16 (88.89) |
| Superior intra-hoffatic recess | 146 | 12 (7.59) | 1 (8.33) |
| Medial superior perimeniscal recess | 146 | 12 (7.59) | 5 (41.67) |
| Medial inferior perimeniscal recess | 147 | 11 (6.96) | 4 (36.36) |
| Behind the posterior cruciate ligament recess | 152 | 6 (3.8) | 0 |
| Proximal tibiofibular joint | 152 | 6 (3.8) | 5 (83.33) |
Table 2.
US compared with MRI in evaluating knee joint effusion: statistical analysis for synovial recesses
| kappa | Sensitivity (95 % CI) | Specificity (95 % CI) | Positive predictive value (95 % CI) | Negative predictive value (95 % CI) | |
|---|---|---|---|---|---|
| Suprapatellar pouch | 0.66 | 54/81 66.7 (55.3–76.8) |
77/77 100 (95.3–100) |
54/54 100 (93.4–100) |
77/104 74 (64.5–82.1) |
| Superior intra-hoffatic recess | 0.14 | 1/12 8.33 (0.2–38.5) |
146/146 100 (97.5–100) |
1/1 100 (2.5–100) |
146/157 93 (87.8–96.5) |
| Inferior infra-hoffatic recess | 0.80 | 14/20 70 (45.7–88.1) |
138/138 100 (97.4–100) |
14/14 100 (76.8–100) |
138/144 95.8 (91.2–98.5) |
| Anterior aspects of the cruciate ligaments | 0 | – | – | – | – |
| Lateral superior perimeniscal recess | 0.96 | 42/44 95.5 (84.5–99.4) |
114/114 100 (96.8–100) |
42/42 100 (91.6–100) |
114/116 98.3 (93.9–99.8) |
| Lateral inferior perimeniscal recess | 0.97 | 48/50 96 (86.3–99.5) |
108/108 100 (96.6–100) |
48/48 100 (92.6–100) |
108/110 98.2 (93.6–99.8) |
| Medial superior perimeniscal recess | 0.56 | 5/12 41.7 (15.2–72.3) |
146/146 100 (97.5–100) |
5/5 100 (47.8–100) |
146/153 95.4 (90.8–98.1) |
| Medial inferior perimeniscal recess | 0.51 | 4/11 36.4 (10.9–69.2) |
147/147 100 (97.5–100) |
4/4 100 (39.8–100) |
147/154 95.5 (90.9–98.2) |
| Lateral posterior recess | 0 | – | – | – | – |
| Medial posterior recess | 0 | – | – | – | – |
| Recess behind the posterior cruciate ligament | 0 | – | – | – | – |
| Popliteal recess | 0.98 | 38/39 97.4 (86.5–99.9) |
119/119 100 (96.9–100) |
38/38 100 (90.7–100) |
119/120 99.2 (95.4–100) |
| Baker’s cyst | 0.93 | 16/18 88.9 (65.3–98.6) |
140/140 100 (97.4–100) |
16/16 100 (79.4–100) |
140/142 98.6 (95–99.8) |
| Proximal tibiofibular joint | 0.90 | 5/6 83.3 (35.9–99.6) |
152/152 100 (97.6–100) |
5/5 100 (47.8–100) |
152/153 99.3 (96.4–100) |
In summary, in evaluating knee joint effusion, US, compared with MRI, correctly identified 78 of 96 patients with joint effusion, showing a sensitivity of 81.3 % and a specificity of 100 %, with a positive predictive value (PPV) of 100 % and a negative predictive value (NPV) of 77.5 % (with a p value less than 0.001) (with CI 95 %).
In the anterior aspect of the knee, ultrasound correctly identified 54 of 81 suprapatellar recess effusions, and 14 of 20 inferior intrahoffatic recess effusions (Figs. 1, 2). In the lateral aspect of the knee, ultrasound identified 38 of 39 patients with popliteal recess effusion, 42 of 44 patients with perimeniscal superior lateral recess effusion and 48 of 50 patients with perimeniscal inferior lateral recess effusion (Figs. 4, 5). In the medial aspect of the knee, 5 of 12 patients showed perimeniscal superior medial recess effusion on ultrasound, and 4 of 11 patients with perimeniscal inferior medial recess effusion (Fig. 6). In the posterior aspect, ultrasound correctly identified 16 of 18 Baker recess effusions and 5 of 6 patients with proximal tibioperoneal recess effusion (Figs. 8, 9, 10).
Patients with effusion significantly differed from those without effusion in terms of age, meniscal pathology (p = 0.007), cruciate ligament lesions, chondropathy and bone edema (p = 0.001). There was no correlation between effusion and gender (p = 0.207). Interestingly, no statistical correlation between effusion and pain was noted either (p = 0.688).
Discussion
In recent decades, magnetic resonance imaging has become the most important modality for the assessment of knee effusion, in both clinical and research environments. One of the major advantages of MRI is that it allows the manipulation of contrast to highlight different tissue types. Various MRI parameters, including tissue relaxation times, affect the contrast between fluid and tissues. A fat suppression technique may be used to increase the contrast.
On MRI, effusion shows low signal intensity on T1-weighted and high signal intensity on high contrast images; particular aspects, however, are present in various diseases such as hemarthrosis, lipohemarthrosis, villonodular synovitis, osteochondromatosis and Baker cyst tear (Fig. 13) [4, 5]. Hemarthrosis and lipohemarthrosis are commonly posttraumatic, but may result from various abnormalities, including pigmented villonodular synovitis, hemophilia, crystal deposition and tumors (Fig. 11). In acute hemarthrosis, a layering phenomenon may be observed separating the serum, above, from the sediment, below; in lipohemarthrosis, intra-articular fat appears as a floating band superficial to the serum (Fig. 13) [4, 5]. Synovial osteochondromatosis is characterized by synovial metaplasia with resultant intrasynovial cartilaginous and then calcified bodies [12]. MRI shows lobulated synovial membrane with or without intraarticular loose bodies (Fig. 12). Pigmented villonodular synovitis is characterized by the proliferation of synovial cells, resulting in a villonodular appearance, hyperplasia of lipid-laden or hemosiderin-laden macrophages and multinucleated giant cells (Fig. 11). MR imaging reveals synovial mass-like proliferations with lobular margins, with intermediate signal intensity on T1-weighted images and relatively low signal intensity on T2 weighted or high contrast sequences, particularly on gradient echo images, due to hemosiderin deposition from repeated hemorrhage (Fig. 11) [9]. In Baker cyst rupture, synovial fluid surrounds the adjacent soft tissues (Fig. 9).
Fig. 13.
Hemarthrosis. Sagittal proton density fat suppressed image (a) and sonography (b) show fluid–fluid levels (arrows) in the suprapatellar pouch in an acute hemarthrosis
Joint effusion on ultrasound is anechoic and is most commonly observed in the suprapatellar pouch, but fluid distribution is influenced by the size of effusion and the position of the knee (Fig. 1) [8]. Effusion can be overlooked in the suprahoffatic recess, posterolateral and posteromedial recess, anterior to ACL recess and posterior to PCL. Characteristic imaging findings, however, can be recognized with sonography in various diseases such as hemarthrosis (the presence of 2 layers), lipohemarthrosis (3 layers), osteochondromatosis (intraarticular loose bodies), villonodular synovitis (synovial mass-like proliferations with lobular margins) and Baker cyst rupture (synovial fluid surrounding the adjacent soft tissues) (Figs. 9, 11, 13).
In conclusion, MRI is the most accurate modality for the evaluation of joint effusion of the knee, allowing the evaluation of the presence of even minimal effusion and evaluation of all the synovial recess. Many synovial abnormalities have MR typical characteristics. Ultrasound has a lower sensitivity and specificity of MRI and does not perform equally well in evaluating all of the synovial recesses. Synovial abnormalities that have MR typical characteristics have also, generally, ultrasound typical characteristics. Ultrasound has high specificity in evaluating knee joint effusion and can be used as a valuable tool for the evaluation of joint effusion of the knee in patients who cannot undergo MRI.
Electronic supplementary material
Movie 1 In the anterior aspect of the knee, the suprapatellar pouch and inferior infra-hoffatic recess are evaluable with sonography. For the evaluation of the suprapatellar pouch, the quadriceps tendon is used as a landmark. Moving the transducer proximally to distally, deep to the quadriceps tendon and superficial to the femur, the suprapatellar pouch is highlighted. For the evaluation of the inferior infra-hoffatic recess, the patellar tendon is used as a landmark, deeply to the patellar tendon and fat pad of Hoffa, in touch with the tibia, the inferior infra-hoffatic recess is present (MP4 420 kb)
Movie 2 Examination of the suprapatellar pouch is performed with an extended knee, avoiding excessive probe compression, quadriceps muscle contraction and knee excessive flexion, to prevent effusion migration (MP4 661 kb)
Movie 3 In the lateral aspect of the knee, the popliteal recess and perimeniscal recesses could be evaluated with ultrasound. For the evaluation of the popliteal recess, the iliotibial tract is used as a landmark. Moving the transducer posteriorly and proximally, the popliteal recess is evaluated. Additionally, for the evaluation of the medial perimeniscal recesses, the iliotibial tract is used as a landmark. Deeply to the iliotibial tract, the perimeniscal recesses are present. In the medial aspect of the knee, medial perimeniscal recesses could be evaluated with ultrasound. The medial collateral ligament is used as a landmark. Deeply to the lateral collateral ligament, the perimeniscal recesses are present (MP4 632 kb)
Movie 4 In the posterior knee, synovial fluid can be detected in the Baker’s cyst and in the proximal tibiofibular joint. As a landmark for Baker’s cyst, the semimembranosus tendon and medial gastrocnemius muscle could be used. Once the medial gastrocnemius in the middle of the leg is identified moving the transducer proximal to the knee, the Baker’s cyst can be seen. The head of the fibula is the landmark for the evaluation of the proximal tibiofibular joint. From the head of the fibula, moving the transducer distally, effusion in the proximal tibiofibular joint is highlighted (MP4 386 kb)
Compliance with ethical standards
Conflict of interest
All authors declare that they have no conflict of interest.
Informed consent
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000 (5). All patients provided written informed consent to enroll in the study and to the inclusion in this article of information that could potentially lead to their identification.
Human and animal studies
The study was conducted in accordance with all institutional and national guidelines for the care and use of laboratory animals.
References
- 1.Schweitzer ME, Falk A, Berthoty D, et al. Knee effusion: normal distribution of fluid. AJR. 1992;159:361–363. doi: 10.2214/ajr.159.2.1632356. [DOI] [PubMed] [Google Scholar]
- 2.Fenn S, Datir A, Saifuddin A. Synovial recesses of the knee: MR imaging review of anatomical and pathological features. Skeletal Radiol. 2009;38(4):317–328. doi: 10.1007/s00256-008-0570-0. [DOI] [PubMed] [Google Scholar]
- 3.Aydingöz U, Oguz B, Aydingöz O, et al. Recesses along the posterior margin of the infrapatellar (Hoffa’s) fat pad: prevalence and morphology on routine MR imaging of the knee. Eur Radiol. 2005;15(5):988–994. doi: 10.1007/s00330-004-2457-3. [DOI] [PubMed] [Google Scholar]
- 4.McCarthy CL, McNally EG. The MRI appearance of cystic lesions around the knee. Skelet Radiol. 2004;33(4):187–209. doi: 10.1007/s00256-003-0741-y. [DOI] [PubMed] [Google Scholar]
- 5.Marra MD, Crema MD, Chung M, et al. MRI features of cystic lesions around the knee. Knee. 2008;15(6):423–438. doi: 10.1016/j.knee.2008.04.009. [DOI] [PubMed] [Google Scholar]
- 6.Alessi S, Depaoli R, Canepari M, et al. Baker’s cyst in pediatric patients: ultrasonographic characteristics. J Ultrasound. 2012;15(1):76–81. doi: 10.1016/j.jus.2011.06.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Draghi F, Danesino GM, Coscia D, et al. Overload syndromes of the knee in adolescents: sonographic findings. J Ultrasound. 2008;11(4):151–157. doi: 10.1016/j.jus.2008.09.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Bonnefoy O, Diris B, Moinard M, et al. Acute knee trauma: role of ultrasound. Eur Radiol. 2006;16(11):2542–2548. doi: 10.1007/s00330-006-0319-x. [DOI] [PubMed] [Google Scholar]
- 9.Garner HW, Ortiguera CJ, Nakhleh RE. Pigmented villonodular synovitis. Radiographics. 2008;28(5):1519–1523. doi: 10.1148/rg.285075190. [DOI] [PubMed] [Google Scholar]
- 10.Murphey MD, Rhee JH, Lewis RB, et al. Pigmented villonodular synovitis: radiologic-pathologic correlation. Radiographics. 2008;28(5):1493–1518. doi: 10.1148/rg.285085134. [DOI] [PubMed] [Google Scholar]
- 11.Sosio D, Draghi F, Pietrobono L, et al. Unusual location of villonodular tenosynovitis. Three case reports and review of the literature. Radiol Med. 2000;100(5):378–379. [PubMed] [Google Scholar]
- 12.Amin MU, Qureshi PS, Ghaffar A, et al. Primary synovial osteochondromatosis of the suprapatellar pouch of knee Correlation of imaging features with surgical findings. J Radiol Case Rep. 2010;4(8):7–14. doi: 10.3941/jrcr.v4i8.504. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Movie 1 In the anterior aspect of the knee, the suprapatellar pouch and inferior infra-hoffatic recess are evaluable with sonography. For the evaluation of the suprapatellar pouch, the quadriceps tendon is used as a landmark. Moving the transducer proximally to distally, deep to the quadriceps tendon and superficial to the femur, the suprapatellar pouch is highlighted. For the evaluation of the inferior infra-hoffatic recess, the patellar tendon is used as a landmark, deeply to the patellar tendon and fat pad of Hoffa, in touch with the tibia, the inferior infra-hoffatic recess is present (MP4 420 kb)
Movie 2 Examination of the suprapatellar pouch is performed with an extended knee, avoiding excessive probe compression, quadriceps muscle contraction and knee excessive flexion, to prevent effusion migration (MP4 661 kb)
Movie 3 In the lateral aspect of the knee, the popliteal recess and perimeniscal recesses could be evaluated with ultrasound. For the evaluation of the popliteal recess, the iliotibial tract is used as a landmark. Moving the transducer posteriorly and proximally, the popliteal recess is evaluated. Additionally, for the evaluation of the medial perimeniscal recesses, the iliotibial tract is used as a landmark. Deeply to the iliotibial tract, the perimeniscal recesses are present. In the medial aspect of the knee, medial perimeniscal recesses could be evaluated with ultrasound. The medial collateral ligament is used as a landmark. Deeply to the lateral collateral ligament, the perimeniscal recesses are present (MP4 632 kb)
Movie 4 In the posterior knee, synovial fluid can be detected in the Baker’s cyst and in the proximal tibiofibular joint. As a landmark for Baker’s cyst, the semimembranosus tendon and medial gastrocnemius muscle could be used. Once the medial gastrocnemius in the middle of the leg is identified moving the transducer proximal to the knee, the Baker’s cyst can be seen. The head of the fibula is the landmark for the evaluation of the proximal tibiofibular joint. From the head of the fibula, moving the transducer distally, effusion in the proximal tibiofibular joint is highlighted (MP4 386 kb)