Introduction
Proton pump inhibitors (PPIs) are commonly used to treat acid-related disorders, but are associated with an increased risk of pneumonia and Clostridium difficile associated-diarrhea.1,2 Initiation of PPIs in hospitalized patients should therefore be limited to specific clinical situations, such as upper gastrointestinal bleeding or stress ulcer prophylaxis in the critically ill.3 Prior studies suggest significant overuse of PPIs in hospitalized patients exists,4–7 but these were published before the widespread implementation of local and national quality improvement efforts targeted at reducing PPI use in medical inpatients (e.g. Society of Hospital Medicine’s (SHM) “Choosing Wisely” list8). We aimed to determine the frequency of inappropriate use of PPIs in a contemporary cohort of hospitalized patients in a tertiary care academic medical center.
Methods
We conducted a retrospective cohort study of 297 patients admitted to a tertiary-care center hospitalist service comprised of teaching and non-teaching medical patients who were not critically ill, were admitted between 01/01/2012 and 3/31/12, and received a PPI during their hospital stay. Three internists used American College of Gastroenterology and the American Society for Gastrointestinal Endoscopy and prior studies to develop criteria to identify “appropriate” and “inappropriate” PPI use (Table 1).4–7 “Appropriate” indications included gastrointestinal (GI) bleeding, esophagitis, gastritis, gastroesophageal reflux (GERD), and continuation of home PPI (abrupt discontinuation can trigger reflux symptoms).9 We extracted the medical records of included patients, applying our prespecified criteria to determine whether use was appropriate. In patients in whom PPI was a continued home medication, we also extracted 2 years of data prior to the index date to determine if the medication was started during a prior hospital admission and, if so, whether this initiation was appropriate. We used descriptive statistics and chi-squared tests to compare patient characteristics and indications for PPI use.
Table 1.
Appropriate and inappropriate PPI uses
| Appropriate PPI use | Inappropriate PPI use |
|---|---|
| History of upper GI bleeding | No reason given |
| Endoscopic evidence of peptic ulcer disease | Unspecified GI prophylaxis |
| Esophagitis | Nonspecific abdominal pain |
| Gastritis and duodenitis | Heartburn (non-chronic) |
| Eradication of H.pylori | Acute pancreatitis |
| GERD | Anemia |
| Barrett’s esophagus | Heparin use for DVT prophylaxis |
| Continued on Home PPI* | Use of aspirin, NSAID, steroids or Coumadin (as a single agent) |
| Acute esophageal variceal bleeding | |
| NSAID used in patient >65 years-old | |
| High risk groups; combination of two or more of (aspirin, NSAID, clopidogrel or Coumadin) |
Results
Of 297 patients, mean age was 64.4 years, (SD 16.3), most were white (69%) and 56% were women (Table 2). PPI use was appropriate in 231 (78%, 95% CI 73.0% – 82.5%) patients. Of these, the majority, 172 (74%) patients, received a PPI because it was a continued home medication. Only 40 of the 172 patients had the medication started during a recent hospitalization and in half of these cases (20) the PPI use was appropriate.
Table 2.
Baseline Characteristics of Hospitalized Patients with Prescribed PPI
| Demographics | PPI Not Indicated (N = 66) | PPI Indicated (N = 231) | Total 297 |
|||||
|---|---|---|---|---|---|---|---|---|
| Age | Mean | SD | Mean | SD | Mean | SD | ||
| 62.5 | 16.2 | 64.9 | 16.3 | 64.4 | 16.3 | |||
| % | N | % | N | % | N | |||
| Sex | Female | 51.5% | 34 | 56.7% | 131 | 55.6% | 165 | |
| Male | 48.5% | 32 | 43.3% | 100 | 44.4% | 132 | ||
| Race | Asian | 0.0% | 0 | 0.9% | 2 | 0.7% | 2 | |
| Black | 10.6% | 7 | 9.1% | 21 | 9.4% | 28 | ||
| Hispanic | 18.2% | 12 | 19.5% | 45 | 19.2% | 57 | ||
| Unknown | 0.0% | 0 | 2.2% | 5 | 1.7% | 5 | ||
| White | 71.2% | 47 | 68.4% | 158 | 69.0% | 205 | ||
| Insurance | Insured | 95.5% | 63 | 87.4% | 202 | 89.2% | 265 | |
| Uninsured | 0.0% | 0 | 0.9% | 2 | 0.7% | 2 | ||
| Unknown | 4.5% | 3 | 11.7% | 27 | 10.1% | 30 | ||
| Service | teaching | 25.8% | 17 | 32.9% | 76 | 31.3% | 93 | |
| nonteaching | 74.2% | 49 | 66.7% | 154 | 68.4% | 203 | ||
| Unknown | 0.0% | 0 | 0.4% | 1 | 0.3% | 1 | ||
| Chronic Disease | Cardiac Disease | 16.7% | 11 | 13.4% | 31 | 14.1% | 42 | |
| Pulmonary Disease | 16.7% | 11 | 14.7% | 34 | 15.2% | 45 | ||
| Gastrointestinal Disease | 13.6% | 9 | 19.5% | 45 | 18.2% | 54 | ||
| Hepatic Disease | 7.6% | 5 | 3.9% | 9 | 4.7% | 14 | ||
| stroke | 1.5% | 1 | 5.2% | 12 | 4.4% | 13 | ||
| sepsis | 12.1% | 8 | 13.0% | 30 | 12.8% | 38 | ||
| other | 33.3% | 22 | 29.4% | 68 | 30.3% | 90 | ||
| PPI Status | Continued Home PPI | 0.0% | 0 | 74.5% | 172 | 58.1% | 172 | |
| Started on PPI in Hospital | 100% | 65 | 25.5% | 59 | 41.9% | 124 | ||
|
| ||||||||
| Discharged on AST | Yes | 36.4% | 24 | 89.6% | 207 | 22.2% | 231 | |
| PPI | 87.5% | 21 | 96.6% | 200 | 95.7% | 221 | ||
| Brand | 52.4% | 11 | 59.5% | 119 | 58.8% | 130 | ||
| Generic | 47.6% | 10 | 40.5% | 81 | 41.2% | 91 | ||
| H2Blocker | 12.5% | 3 | 3.4% | 7 | 4.3% | 10 | ||
| Brand | 0.0% | 0 | 71.4% | 5 | 50.0% | 5 | ||
| Generic | 100.0% | 3 | 28.6% | 2 | 50.0% | 5 | ||
|
| ||||||||
| Medications | % | N | % | N | % | N | ||
| Aspirin | 36.4% | 24 | 43.7% | 101 | 42.1% | 125 | ||
| NSAID | 10.6% | 4 | 6.5% | 15 | 6.4% | 19 | ||
| Corticosteroids | 13.6% | 9 | 16.9% | 39 | 16.2% | 48 | ||
| Warfarin | 0.0% | 5 | 19.0% | 44 | 16.5% | 49 | ||
| Clopidogrel | 12.1% | 8 | 10.8% | 25 | 11.1% | 33 | ||
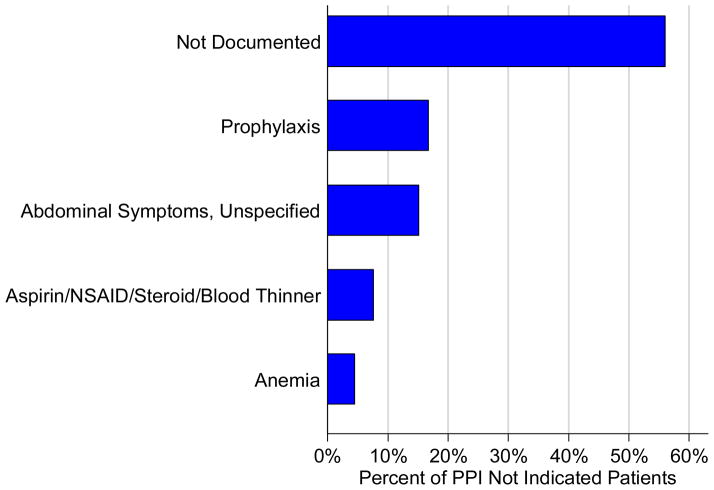
The second most common appropriate diagnosis was GERD (31%) followed by history of GI bleeding (19%) and treatment for esophagitis or gastritis (18%). Among the 66 patients receiving a PPI inappropriately, the majority of patients (56%) had no documented reason for PPI use and only 11 patients (17%) were receiving PPI for stress ulcer prophylaxis (Figure-1). Five patients (8%) were treated prophylactically because of steroid or anticoagulant use. We observed no differences in age, gender, race or reason for admission between the patients treated appropriately versus inappropriately.
Figure 1.
Reasons for inappropriate PPI prescription
Discussion
In a contemporary cohort, chronic PPI use prior to admission was the most common reason PPIs were prescribed in the hospital. About 20% of hospitalized patients were started on a PPI for an inappropriate indication, the majority of whom lacked documentation concerning the reason for use. Among patients treated inappropriately, 36% were discharged on acid suppressive therapy.
The prior literature has reported much higher percentages of unnecessary PPI use in hospitalized patients.4–7 Gupta et al., found that 70% of patients admitted to an internal medicine service received acid-suppressive therapy, 73% of whom were treated unnecessarily.5 Similarly, Nardino found that 65% of acid-suppressive therapy in hospitalized medical patients was not indicated.4 If we had excluded patients on home PPIs from our study cohort, we would have found a higher rate of inappropriate use due to a smaller overall patient population. However, we chose to include these patients because they represented the vast majority of hospitalist-prescribed PPIs. Notably, most of these prior prescriptions were not written during a recent hospital stay, indicating that the majority were initiated by outpatient physicians.
Our study is limited by its small sample size, single-center design, and inability to determine the indications for outpatient PPI use. Still, it has important implications. Prior work has suggested that focusing efforts on PPI “overuse” may be premature in the absence of valid risk prediction models defining the patient populations that most benefit from PPI therapy.10 Our work additionally suggests that hospital rates of inappropriate initiation may be relatively low, perhaps because hospitalist culture and practice have been affected by both local and national quality improvement efforts and by evidence dissemination.8 Quality improvement efforts focused on reducing inpatient PPI use are likely to reveal diminishing returns, as admitting hospitalists are unlikely to abruptly discontinue PPIs prescribed in the outpatient setting.9 Hospitalists should be encouraged to assess and document the need for PPIs during admission, hospitalization, and discharge processes. However, future efforts to reduce PPI overuse among hospitalized patients should predominately be focused on reducing inappropriate chronic PPI use in the outpatient setting.
Acknowledgments
The study was conducted with funding from the Department of Medicine at Baystate Medical Center. Dr. Lagu is supported by the National Heart, Lung, and Blood Institute of the National Institutes of Health under Award Number K01HL114745.
We would like to acknowledge Peter Lindenauer for his comments on an earlier draft of this manuscript.
Footnotes
The authors have no conflicts of interest.
Drs. Lagu and Albugeaey had full access to all of the data in the study. They take responsibility for the integrity of the data and the accuracy of the data analysis. Dr. Lagu, Albugeaey, and Seiler conceived of the study. Drs. Albugeaey and Al Faraj acquired the data. Dr. Lagu, Albugeaey, Al Faraj, Seiler, and Ms. Garb analyzed and interpreted the data. Drs. Albugeaey and Lagu drafted the manuscript. Dr. Lagu, Albugeaey, Al Faraj, Seiler, and Ms. Garb critically reviewed the manuscript for important intellectual content. Dr. Albugeaey is a recipient of a scholarship from the Ministry of Higher Education, Kingdom of Saudi Arabia.
References
- 1.Herzig SJ, Vaughn BP, Howell MD, Ngo LH, Marcantonio ER. Acid-suppressive medication use and the risk for nosocomial gastrointestinal tract bleeding. Arch Intern Med. 2011;171(11):991–997. doi: 10.1001/archinternmed.2011.14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Herzig SJ, Howell MD, Ngo LH, Marcantonio ER. Acid-suppressive medication use and the risk for hospital-acquired pneumonia. JAMA J Am Med Assoc. 2009;301(20):2120–2128. doi: 10.1001/jama.2009.722. [DOI] [PubMed] [Google Scholar]
- 3.Laine L, Jensen DM. Management of patients with ulcer bleeding. Am J Gastroenterol. 2012;107(3):345–360. doi: 10.1038/ajg.2011.480. quiz 361. [DOI] [PubMed] [Google Scholar]
- 4.Nardino RJ, Vender RJ, Herbert PN. Overuse of acid-suppressive therapy in hospitalized patients. Am J Gastroenterol. 2000;95(11):3118–3122. doi: 10.1111/j.1572-0241.2000.03259.x. [DOI] [PubMed] [Google Scholar]
- 5.Gupta R, Garg P, Kottoor R, et al. Overuse of acid suppression therapy in hospitalized patients. South Med J. 2010;103(3):207–211. doi: 10.1097/SMJ.0b013e3181ce0e7a. [DOI] [PubMed] [Google Scholar]
- 6.Reid M, Keniston A, Heller JC, Miller M, Medvedev S, Albert RK. Inappropriate prescribing of proton pump inhibitors in hospitalized patients. J Hosp Med Off Publ Soc Hosp Med. 2012;7(5):421–425. doi: 10.1002/jhm.1901. [DOI] [PubMed] [Google Scholar]
- 7.Craig DGN, Thimappa R, Anand V, Sebastian S. Inappropriate utilization of intravenous proton pump inhibitors in hospital practice--a prospective study of the extent of the problem and predictive factors. QJM Mon J Assoc Physicians. 2010;103(5):327–335. doi: 10.1093/qjmed/hcq019. [DOI] [PubMed] [Google Scholar]
- 8. [Accessed April 11, 2014];Choosing Wisely | Society of Hospital Medicine – Adult Hospital Medicine. Available at: http://www.choosingwisely.org/doctor-patient-lists/society-of-hospital-medicine-adult-hospital-medicine/
- 9.Thomson ABR, Sauve MD, Kassam N, Kamitakahara H. Safety of the long-term use of proton pump inhibitors. World J Gastroenterol WJG. 2010;16(19):2323–2330. doi: 10.3748/wjg.v16.i19.2323. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Herzig SJ, Rothberg MB. Prophylaxis rates for venous thromboembolism and gastrointestinal bleeding in general medical patients: too low or too high? BMJ. 2012;344(may18 1):e3248–e3248. doi: 10.1136/bmj.e3248. [DOI] [PubMed] [Google Scholar]