Abstract
Incidence rates of acute coronary heart disease (ACHD; including myocardial infarction and angina pectoris), stroke, and heart failure (HF) were studied for their age, disability, and comorbidity patterns in the U.S. elderly population using the National Long Term Care Survey (NLTCS) data linked to Medicare records for 1991–2005. Incidence rates increased with age with a decrease in the oldest old (stroke and HF) or were stable at all ages (ACHD). For all diseases, incidence rates were lower among institutionalized individuals and higher in individuals with higher comorbidity indices. The results could be used for understanding currently debated effects of biomedical research, screening, and therapeutic innovations on changes in disease incidence with advancing age as well as for projecting future Medicare costs.
Keywords: Medicare data, incidence rates, circulatory diseases, age pattern, disability, comorbidity, elderly
Introduction
Heart disease and stroke have been the leading causes of death and major causes of disability (including long-term severe disability) in the United States for about 80 years, resulting in substantial health care expenditures: for example, in 2007 a projected cost was about $151.6 billion for coronary heart disease and $62.7 billion––for stroke (Greenlund, Giles, & Keenan, 2006; Rosamond et al., 2007). Mortality rates of heart disease and stroke steadily declined during past decades; however, they are still ranked as number 1 and number 3 causes of mortality in the United States, being responsible for about 36% of total deaths in populations of 65 years and older (cancer keeps the second position; Centers for Disease Control and Prevention/ National Center for Health Statistics [CDC/NCHS], 2006; Xu, Kochanek, Murphy, & Tejada-Vera, 2010). Mortality rates of heart and cerebrovascular diseases increase with age: being 518.9 and 101.1 per 100,000 at age 65–74. At ages 85+, they become 4,778.4 and 1,141.8 per 100,000, respectively (National Center for Health Statistics [NCHS], 2009). To better address the health demands in the elderly and to reduce economic burdens on society, it is important to understand the key factors driving the onset and progression of aging-related chronic diseases such as heart disease and stroke. However, identification of circulatory disease age patterns with sufficient precision requires large population-based data sets that are costly to collect. This is a reason why studies on age patterns of diseases in the United States along with investigations of factors affecting them are not common in the elderly population. Among aging-associated diseases, cancer incidences are better studied at a national level in the United States, predominantly using data from the SEER registry (Altekruse et al., 2009). Age patterns of incidence of cardio- and cerebrovascular (Arnold et al., 2005) diseases were recently studied in the Cardiovascular Health Study (CHS); however, the results of this study cannot be considered as nationally representative.
Description of the Problem
Incidence rates can be calculated using data from the national registers or from the surveys representing the U.S. population. In the latter case, special procedures are needed to generalize survey results to the national level. One way to do that is to use a weight function (possibly time-dependent) assigned to each individual in the sample—for example, “weighted” sums (means) over individuals in the sample give quantities at the national level. One national survey with such a design is the 1982–2005 National Long-Term Care Survey (NLTCS), which focuses on the U.S. elderly (65+) population. Since the NLTCS is linked with the Medicare records and with the Vital Statistics files, this is a unique data set with continuous recording of health services, age of death, and detailed reassessment of health status performed by survey every 5 years (except for the first two waves in 1982 and 1984). Several analyses of the NLTCS data have provided consistent results on functional disability, active life expectancy, and chronic disease incidence and prevalence in the U.S. elderly (Akushevich, Kulminski, Akushevich, & Manton, 2006; Akushevich & Yashin, 2008; Kulminski et al., 2006; Manton, Corder, & Stallard, 1997; Manton & Gu, 2001; Manton, Gu, & Lamb, 2006; Manton, Stallard, & Corder, 1998; Stallard, 2006), proving that this data set could be a valuable source of information on health status in the elderly. To get a more comprehensive data set allowing for dealing with more detailed information on disease onset and outcome as well as comorbidity and other important health-related issues, the NLTCS data set was linked to the Medicare Service Use (MSU) files providing detailed information about diagnoses and dates of medical service use allowing for estimates of the date of disease onset.
Purpose
The primary goal of this study was to estimate the patterns of age-adjusted and age-, disability-, and comorbidity-specific incidence rates of circulatory diseases in the U.S. elderly population (including the oldest elderly) using the NLTCS data linked to the MSU files (NLTCS-M). The NLTCS-M data is a good candidate for this analysis because (i) the results are representative at the national level, (ii) the spectrum of old ages available for age-pattern analysis is wider than in many other data sets, and (iii) information on disability and comorbidity can be included in the analysis, which is very important for studies among elderly. Thus, the circulatory disease incidence estimates for advanced ages presented here could be valuable for both understanding age-specific risks of circulatory diseases in the U.S population which could provide an insight into the mechanisms of age-related diseases, and for projections of the health trends and forecasting the future Medicare expenditures associated with circulatory diseases in the U.S. elderly population.
Data and Methods
NLTCS and Medicare files of Service Use
The NLTCS data include 1982, 1984, 1989, 1994, 1999, and 2004/2005 waves and contain longitudinal and cross-sectional information on a nationally representative sample of over 49,258 U.S. elderly aged 65+ years, with 17,000–20,000 age-eligible survivors in each of the six waves (Manton et al., 2006). The universe of interest for NLTCS is the population of Medicare enrollees aged 65 and older in the United States. Geographically, NLTCS is interested in people living within the United States, including Alaska and Hawaii. To reduce the cost of the survey, the NLTCS samples were clustered in 173 primary sampling units (PSUs) that consisted of individual counties and groups of adjoining counties.
The NLTCS provides hundreds of variables measured at each wave including demographic factors, residence type, income, assets, height, weight, alcohol and cigarette use, exercise, 28 major medical conditions, disability (7 activities of daily living [ADLs] and 9 instrumental activities of daily living [IADLs]) measured as the inability to perform respective ADLs/IADLs without help for 90 or more days, 7 functional limitation items (Nagi, 1976), subjective health status, and cognition. The response rate in all NLTCS waves is high (95%).
The NLTCS individuals are linked to Medicare claims data for 1991–2005 to allow for tracking of mortality, health histories, and health maintenance organization (HMO) enrollment/disenrollment. Medicare records are available for each institutional (inpatient, outpatient, skilled nursing facility, hospice, or home health agency) and noninstitutional (Carrier–Physician–Supplier and durable medical equipment providers) claim types. The percentage of coverage by Medicare is high: in January 2001, 95.85% had both Part A and B coverage, 3.46% of sample persons had Part A only, and 0.69% had Part B only. Continuous medical records in Medicare data allow us to reconstruct the individual histories of medical service use and, therefore, investigate disease incidence in the cohort design style.
Two of the six waves, namely cohorts of 1994 and 1999, are used in the analysis. These specific waves were chosen primarily because the high-quality Medicare follow-up data are available only starting from 1991, and also because the complete 5-year follow-up after the NLTCS interview for later than 1991 is accessible only for these two waves. The cohort of 1994 year consists of longitudinal portion (i.e., 13,631 persons eligible for 1989 survey), 5,000 newly selected individuals aged 65+, and supplementary selected sample of 540 persons aged 95+. The cohort of 1999 year includes 13,775 individuals from the longitudinal portion, 5,500 newly selected individuals of age 65+, and 600 individuals from the supplement of age 95+. Excluding the nonrespondents, 34,077 individuals were followed up between 1994 and 2004.
Individuals from these two cohorts (i.e., cohorts formed in 1994 and 1999 years) are followed up during 5 years from the date of interview. The following variables collected for all individuals in 1994 and 1999 cohorts are used in analysis: (i) sex, (ii) age at interview, (iii) disability index (with outcomes nondisabled, IADL only, 1–2 ADLs, 3–4 ADLs, 5–6 ADLs, Institutionalized) measured at the date of interview, that is, at the beginning of the follow-up, (iv) Charlson comorbidity index according to the specifications described in (Charlson, Pompei, Ales, & Mackenzie, 1987; Quan et al., 2005; this index has been validated for ischemic heart disease, ischemic stroke, as well as studied in Medicare part B claims data (see DHoore, Bouckaert, & Tilquin, 1996; Goldstein, Samsa, Matchar, & Horner, 2004; Klabunde, Potosky, Legler, & Warren, 2000) measured at the date of interview using Medicare records during a year prior to the date of interview, (v) the set of individual Medicare records covering the entire follow-up period used for date at onset identification, (vi) fraction of months additionally covered by HMO during the follow-up period, and (vii) the sample weight provided by the U.S. Census Bureau.
Each interviewed person in the NLTCS received a screener wave-specific weight. This weight is calculated by the U.S. Census Bureau using a multistage procedure in which the final screener weight is the product of four factors: (i) screener base weight, (ii) screener non-interview adjustment factor, (iii) first-stage (ratio estimate) factor, and (iv) second-stage (ratio estimate) factor. The screener base weight is the inverse of the probability of selection of an individual in a sample. These weights are the same for all individuals in the 1982 survey and different for subsequent surveys because of variety of sample components (longitudinal parts, newcomers, healthy supplements, etc.). The screener non-interview adjustment factor in a cell h is calculated as, , where Ih and NIh denote the weighted number of interviews and non-interviews in hth cell, respectively. The cells are defined by the age groups (65–74, 75–79, 80–84, and 85+), the reason for Medicare entitlement (for the first age group only) and the PSUs. Special cell collapsing procedures are applied wherever necessary. The first-stage ratio estimate factors adjust for differences between the characteristics of the NLTCS sample and respective population within PSUs. The cells for the first-stage factors are based on the regions (North, North-Central, South, and West), age groups (65–74, 75–79, 80–84, and 85+), and residential status (Standard Metropolitan Statistical Area or not). The second-stage factors represent the ratio adjustments to correct for the difference between weighted sample counts of persons and independent estimates of the total number of persons, within certain defined cells. The independent estimates or “population controls” were projections based on the Census population counts. The second-stage factor cells are based on age groups (65–69, 70–74, 75–79, 80–84, and 85+), race (Black or non-Black), and sex. Thus, the individual weights are defined such that weighted sums of characteristics of sample individuals produce the national cross-sectional estimates of persons aged 65 (Manton & Gu, 2001).
Date of Onset Definitions
To calculate the age-specific disease incidence rates, one needs to know the date of disease onset. The MSU files provide dates of claims for medical service, which are accompanied by the corresponding ICD-9-CM codes (the International Classification of Diseases, Ninth Revision, Clinical Modification). Therefore, it is reasonable to assume that an individual might experience an onset of a disease during the period of observation if there are one or several records with the ICD-9-CM code corresponding to this disease on institutional claim/claims. Actually, Medicare data do not contain information on whether the appearance of an ICD-9-CM code is a “true” disease onset or just a visit to treat a disease with its onset possibly first registered outside (before) the observation period. Therefore, the date of onset can be identified using information collected in the Medicare Claims files with specific assumptions, which outline the specific calculation algorithm. Note, the date of onset of a certain chronic disease is a quantity which is not defined as precisely as mortality. Besides, different strategies can be used in clinical practice for different diseases. Thus, there is certain arbitrariness in defining the date of onset, which can be used for constructing a unified definition of date of onset appropriate for population studies. The scheme used in this article has resulted from the review of the approaches used in several published studies for different diseases (Nattinger, Laud, Bajorunaite, Sparapani, & Freeman, 2004, 2006; Sloan, Brown, Carlisle, Ostermann, & Lee, 2003). The unified scheme offered for defining the date of onset is useful for comparative analyses of effects of different diseases on medical cost and is also appropriate for prediction purposes.
The ages at onsets of the circulatory diseases were reconstructed from the MSU data using the following scheme. First, the individual medical histories of the applicable disease were reconstructed from Medicare files combining all records with their respective ICD-9 codes. The following ICD-9 codes were used for the considered cases of diseases of the circulatory system: (i) ischemic heart disease (referred in the manuscript as ACHD (acute coronary heart disease), as referred in Luepker et al., 2003), including acute myocardial infarction (MI; 410), other acute and subacute forms of ischemic heart disease (411), and angina pectoris (AP; 413); (ii) cerebrovascular diseases including intracerebral hemorrhage (431), occlusion and stenosis of precerebral arteries with cerebral infarction (433.x1), occlusion of cerebral arteries with cerebral infarction (434.x1), and acute but ill-defined cerebrovascular disease (436); and (iii) heart failure (HF; 428). Then individuals with the history of the considered disease before the date of interview in 1994 or in 1999 were excluded from the cohort studies for the onset of this disease. The detailed individual records in Medicare files are available from 1991, so we have a sufficient time period to reject prevalence cases. The numbers of individuals in the pooled cohort without prevalent cases for each disease are shown in Table 1. All individual trajectories were reviewed by empirical methods (e.g., stratification) resulting in the base algorithm (Algorithm A) for identification of the date of onset. In Algorithm A, a date of a Medicare record (referred to as “this record” below in this subsection) is identified with the date of onset of applicable disease if both of the conditions mentioned below are met:
Table 1.
The Numbers of Individuals Followed-up for Onsets of Circulatory Diseases and the Total Numbers of Registered Onsets.
| Individuals in two waves | Individuals without HMO | Individuals without HMO and without prevalent cases | The number of onsets | |
|---|---|---|---|---|
| ACHD | 34,077 | 27,607 | 25,568 | 2,394 |
| MI | 34,077 | 27,607 | 26,785 | 1,991 |
| AP | 34,077 | 27,607 | 26,634 | 761 |
| Stroke | 34,077 | 27,607 | 26,408 | 2,768 |
| HF | 34,077 | 27,607 | 25,921 | 3,046 |
Note. ACHD = acute coronary heart disease; MI = myocardial infarction; AP = angina pectoris; HF = heart failure.
This record is the earliest record with respective ICD code as a primary diagnosis in one of four Medicare sources (inpatient care, outpatient care, physician services, and skilled nursing facilities). This choice is in accordance with the general practice of reconstruction of the date at onset from Medicare data (Nattinger et al. 2004; Nattinger et al. 2006).
In addition to this record, there is another record with its respective ICD code as the primary diagnosis from one of the four Medicare sources listed in (i) which appeared with a date different from the date of this record and not later than 0.3 years after this record. Death occurred during this period (i.e., 0.3 years after this record) is also considered as the second record.
The first condition allows for identifying the first occurrence of disease code, and the second condition is required for confirmation of disease presence. In acute conditions (e.g., ACHD, MI, AP), the requirement of confirmation by occurrence of another record is superfluous because of the definition of acute conditions and because of high mortality after these conditions. Therefore, we define also the Algorithm B, in which only the first condition is valid. Compared with MI, AP cannot be viewed as only acute condition, this is why it could be often registered not only as primary disease and second record is required for disease confirmation. Being heterogeneous by these characteristics, the ACHD group is analyzed both entirely and separately for MI and AP.
This algorithm was used to study recovery after stroke (Yashin et al., 2010), medical cost trajectories before and after age-related disease onsets (Akushevich et al., 2011b), wide spectrum of geriatric diseases incidence using two Medicare-based data sets (Akushevich et al., 2012), and the role of behavior factors in cancer risk (Akushevich et al., 2011a).
Estimates for U.S. Elderly Population
Age patterns of incidence rates are assessed by stratifying the sample into relevant age categories. For age-adjusted rates, 1-year interval age groups were chosen for ages 66–94, and longer intervals were used for grouping in advanced ages: 95–96, 97–99, and 100+ years. Slightly different grouping was used for evaluation of age-specific rates: 66–67, 68–70, 71–73, 74–76, 77–81, 82–85, 86–89, 90–94, 95–99, and 100+ years old. Empirical age-specific rates (λa) are calculated as a ratio of weighted numbers of cases to weighted person-years at risk: λa = na / Pa; where na = Σn wn, Pa = Σi wi, and wi is the individual weight; n runs over all disease onsets detected in the age group, and i runs over all individuals at risk in the age group. The effects of study design also influence the calculation of standard error (SE) and confidence intervals of rate estimates. The generalized variance function (Lohr, 2009) is used for calculation of approximate SE: , where b is the factor correcting the estimate of SE on the study design. The SE calculated with this factor provides the estimate of the approximate SE at the national level. The factors provided by the NLTCS data providers are different for noninstitutional (b= 1,545) and institutionalized (b= 1,079) persons and equal for both cohorts of 1994 and 1999.
Age-adjusted rates (or directly standardized incidence rates) are averages of age-specific rates. For population aged 66+, they are calculated as . Age-specific rates λa and population counts Pa are defined above through weighted sums; therefore, the age-adjusted λ rates are both standardized and weighted towards the U.S. population age distribution. Comorbidity- and disability-specific patterns are calculated using the same equations for stratified populations. The standard error for the age-adjusted rate is estimated assuming that the numbers of events observed in each age group are independent or/and have Poisson distributions (Breslow & Day, 1987). The hypothesis about the difference of age-adjusted rates is tested by comparing the difference between age-adjusted estimates of two compared rates (i.e., for 1994 and for 1999) with SE for this difference evaluated as the square root of the sum of their standard errors squared. Formally t-test is applied for which the approximate t-statistics is calculated as a ratio of the rate difference and its SE. Since the estimates of rates were obtained based on the large number of cases, respective t-distribution with large degrees of freedom is well approximated by the normal distribution. In this case | t | <2 approximately corresponds to p value < .05.
Results
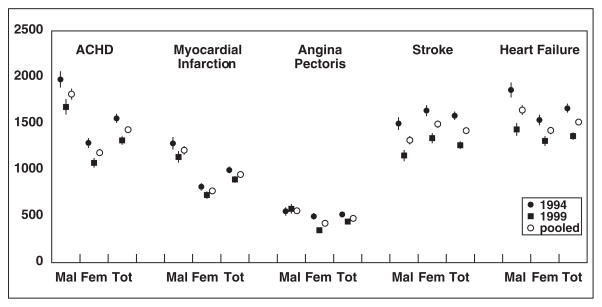
The age-adjusted incidence rates of diseases of the circulatory system are presented in Figure 1 for cohorts of 1994, 1999, and both cohorts pooled for males/females and for total population. For males, the ACHD (which included MI and AP) had a leading position, while for females stroke had the highest rates among analyzed diseases for cohorts of 1994, 1999, and for both cohorts pooled. Males of all cohorts had higher rates of ACHD and MI than females, and females had higher rates of stroke than males. Higher rates of HF in males were observed for 1994 cohort and in pooled analysis. For AP, higher rates in males were detected for 1999 cohort and pooled cohort. Because the weights used provided the estimates at the national level, the results (both for age-adjusted rates and SEs) appear to be valid for the U.S. elderly population.
Figure 1.
Age-adjusted incidence rates per 100,000 of circulatory diseases with standard errors.
The results on gender disparities and time trends in the age-adjusted incidence rates are shown in Table 2. There was a significant 5-year decline for incidences of ACHD, stroke, and HF.
Table 2.
Estimates of t-Statistics for Time Trend and Male/Female Differences in the Age-Adjusted Incidence Rates of Geriatric Diseases.
| Time trends
|
Male/female differences
|
|||||
|---|---|---|---|---|---|---|
| Males | Female | Total | 1994 | 1999 | Combined | |
| ACHD | −2.45 | −2.83 | −3.59 | 6.62 | 6.18 | 8.91 |
| MI | −1.59 | −1.52 | −2.02 | 5.93 | 5.58 | 8.04 |
| AP | 0.40 | −3.31 | −1.98 | 0.94 | 3.89 | 3.33 |
| Stroke | −3.73 | −3.64 | −5.18 | −1.51 | −2.30 | −2.81 |
| HF | −4.04 | −2.86 | −4.72 | 3.25 | 1.43 | 3.33 |
Note. Absolute value of t-statistics larger than 2 approximately correspond to significant differences with p < .05.
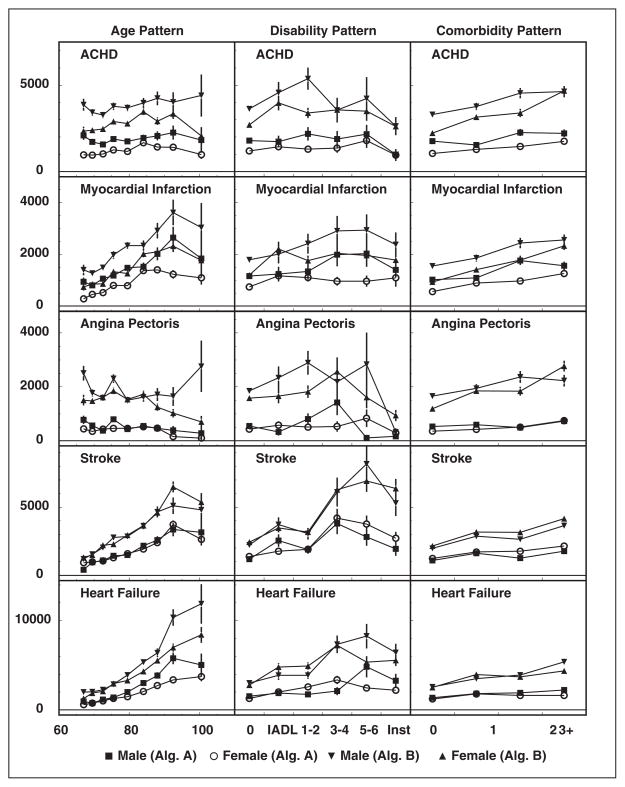
The age, disability, and comorbidity patterns were analyzed for all considered diseases (see Figure 2). All patterns were obtained using both strategies for disease onset identification (with or without the requirement for another record with primary diagnosis) implemented in Algorithms A and B. As it was discussed in the Date of Onset Definitions section, the latter approach can be more appropriate for acute diseases. As expected, the rates obtained using Algorithm A were significantly higher (Figure 2); however, no substantial changes in the shape of patterns of incidence rates were observed for all studied diseases while Algorithm A or B were used. The patterns presented in Figure 2 substantially differed for males and females: for ACHD and for HF, males had higher rates for all three patterns analyzed. The evaluated person-years for each age group were higher than 500 years (except the group of 95+ years old males with 434 years for HF), the numbers of individuals in each disability or comorbidity sex-specific groups were higher than 250. The incidence rates were increasing with age for MI, stroke, and HF. Rates of ACHD and AP had a tendency to be more stable for all ages. For MI, stroke (females), and HF (males), the changes of incidence age patterns were observed for advanced ages (e.g., 85+) compared to younger elderly (e.g., 65–85 years old): incidence rates decreased in the oldest old opposite to the trends observed at younger ages.
Figure 2.
Age (left columns), Disability (central columns), and comorbidity (right columns) patterns of the incidence rates (per 100,000) of geriatric diseases for males and females with error bars represented approximate SE. The aArguments are years (age), disability groups (nondisabled, IADL only, 1–2 ADLs, 3–4 ADLs, 5–6 ADLs, and institutionalized), and comorbidity group in the units of Charlson index (0, 1, 2, and 3 and more). The rates are calculated using Algorithms A and B.
For MI (males), stroke, and HF (males), the incidence rates were higher for individuals with severe disabilities. Interestingly, for all the considered diseases, institutionalized individuals have lower rates. Among individuals with higher comorbidity indices (i.e., Charlson index), the higher rates were observed for all the considered circulatory diseases.
Discussion
In this article, three types of the patterns of incidence of several circulatory diseases (such as ACHD, HF, and stroke) were analyzed: age-, disability-, and comorbidity-specific rates were calculated. At our knowledge, this kind of analysis was performed for the first time. While there are several studies characterizing age-patterns of incidence of aging-related diseases among elderly population (aNational Institutes of Health/National Heart, Lung and Blood Institute [NIH/NHLBI], 2006a), patterns of circulatory disease incidence among individuals with various disabilities and comorbidities were not studied at the national level. Data from the linked NLTCS-Medicare files made the analysis of various types of the patterns in the same population––such as U.S. older adults––possible. Below, we discuss why the results of this study could be treated as nationally representative for the U.S. elderly population and how the different algorithms of evaluation of disease onset influence incidence rates.
NLTCS/Medicare Information as a Source of Information about the Referent Values of Incidence Rates for the U.S. Elderly Population
An increasing number of elderly in the United States makes studies on the most prevalent aging-related diseases very important––it is essential to know how incidence rates of circulatory diseases change with age in males and females, what the disability prevalence and patterns for each disease are, and how common and how severe comorbidities in the U.S. elderly are. In this article, such estimates were obtained using the NLTCS-M data, which are capable of providing the estimates that may serve as referent values for different studies designed in the United States and abroad. We used several strategies of identifying the disease onset. One of the schemes is considered basic: it requires occurrence of repeated claims containing chosen ICD code as a prime diagnosis in basic Medicare sources. Such definition is in accordance with the practice of onset identification for many diseases (Nattinger et al., 2004; Nattinger et al., 2006; Sloan et al., 2003). We have described how NLTCS-M data set could be very useful for answering the spectrum of questions on elderly health in the United States from both medical and economical perspectives. These data are population based, minimizing selection bias with respect to geographic region, urban versus rural location, racial health disparities with a whole spectrum of race- and ethnic-specific populations, and socioeconomic characteristics. Each of these factors are important predictors of disease risk, progression, treatment availability, and response––actually this information is limited in databases from more restricted populations (Nattinger et al., 2004).
Identified Properties of Incidence Rates
Patterns of majority of diseases are well described by the base algorithm. The most important features of the algorithm include occurrence of primary diagnosis in one of four Medicare sources (inpatient care, outpatient care, physician services, and skilled nursing facilities) and confirmation of the diagnoses in another record. Patterns of several diseases require certain corrections to the base algorithm to be adequately described. For example, only one record has to be required for ACHD. In addition, disability and comorbidity patterns of disease incidence were evaluated. Disability was measured using self-reported information, while comorbidity was estimated using Medicare records during the year before the date of interview and beginning of 5-year follow-up period. Because of using the special weight, the results appear to be valid at the national level. Properties of these patterns were briefly discussed in the Results section.
Two definitions of disease incidence and two respective computation algorithms were developed and applied to data. To check which of the definitions better corresponds to those used in other studies on incidence rate evaluation, the definitions were compared with diagnostic criteria typically used (reviewed in (NIH/NHLBI, 2006a)). We found that the base definition involving the requirement of quick confirmation of the original diagnosis better corresponds to widely used definitions for HF and stroke, while the algorithm without this requirement better corresponds for MI and AP. The diagnostic criteria of different heart studies reviewed in appendix of ref. (NIH/NHLBI, 2006a) do not allow us to unambiguously conclude that our choice exactly corresponds to those made in these studies. However, the difference between the results obtained in our study with Algorithms A and B (that could be, for example, due to the fraction of the patients with transitional circulatory attacks whose diagnoses were not confirmed by the second examination or who did not appear at the follow-up exams due to the improved health condition) was more prominent for stroke than for MI. It allows for speculations about more strict criteria required for MI diagnosis in all compared studies than for the stroke.
Several types of age patterns were observed in our study: monotonic increase with age (HF), the shape with a maximum (such as increasing with age with subsequent decrease after age 90––MI and stroke), and the shape with a tendency of decreasing with age (AP). ACHD pattern can be described as flat or a plateau. In spite of larger statistical uncertainty estimated for this age region, the occurrences of shapes with a maximum and, especially, with monotonic decline may be interpreted to contradict the hypothesis that risk of geriatric diseases correlates with accumulation of adverse health events (genetic mutations, deterioration of vascular system, immunosenescence, etc.). There are three basic concepts that are basically attracted to explain such shape of age patterns. Appearance of such effects can be attributed to the effect of selection (Vaupel et al., 1998), where frail individuals do not survive to advanced ages. The frailty models are popular in cancer modeling and were successfully applied to SEER data (Manton, Akushevich, & Kravchenko, 2009; Trussell & Richards, 1985; Yashin et al., 2009). Another explanation is related to possible under-registration of diagnoses at advanced ages—which, however, cannot be proved with available data (Enright, McClelland, Newman, Gottlieb, & Lebowitz, 1999; Solomon & Murphy, 2005). Other possible biologically motivated explanations are discussed in Ukraintseva and Yashin (2001): the authors suggested the existence of the mechanisms of possible contribution of individual aging to the shape of mortality curve by subdividing the individual age-associated changes into three components differed by the influence on morbidity and mortality (i.e., basal, ontogenetic, and time-dependent).
In our study, incidence rates of stroke (in males and females) and HF (in males) were higher in elderly with severe disabilities. There are very few studies analyzing incidences of circulatory diseases in populations with certain preexisting levels of functional disability––usually, disabilities are studied as consequences of these diseases rather than preexisting and/or accompanying conditions. Our results are in agreement with other observations that patients with severe disability had a higher chance to be hospitalized with several diseases, including stroke and congestive HF, during the year of follow-up (i.e., about 50–75% cases) than slightly disabled or individuals without disability (i.e., about 15–22% cases; Ferrucci, Guralnik, Pahor, Corti, & Havlik, 1997). Taking into account, that about 24–30% of elderly could recover from their ADL function or improve them within a couple of years as it has been demonstrated in several longitudinal studies (Gill, Robison, & Tinetti, 1997; Katz et al., 1983; Manton, Corder, & Stallard, 1993), it has been suggested that some factors (such as poor nutrition, over-medication, and other risk factors) may directly impede ADL recovery and thus patients who cannot increase their functional level could be at higher risk of developing certain aging-related diseases, for example, HF or stroke. Lower rates of diseases of the circulatory system observed in our study among institutionalized individuals could be explained, at least in part, by the fact that institutionalized patients get treatment which decreases risk of ACHD and stroke. Our findings that individuals with high comorbidity indices had the higher rates of all studied circulatory diseases are in agreement with observations from other studies (Fang & Alderman, 2001; Levy, Larson, Vasan, Kannel, & Ho, 1996; Wenger, 2003).
Comparison of the results obtained for cohorts formed in 1994 and 1999 showed 5-year declines in incidence rates for all studied circulatory diseases. The highest and lowest 5-year declines were detected for stroke (−20%) and MI (−10%), respectively. Comparison of cohort specific age-, disability-, and comorbidity-patterns (not shown) allows us to reveal that (i) the decline in the incidence rate was reached for ages 75–90 (for MI––for ages 95+), (ii) the decline was detected for nondisabled individuals for ACHD, for individuals with IADL only and 5–6 ADLs for HF and stroke, (iii) no decline (even increase for ACHD and HF) was detected for institutionalized individuals, and (iv) no noticeable dependence on comorbidity was found. From the perspectives of sex disparities (see Figure 1 and Table 2), the decline in incidence of HF was more prominent among male, and sex-specific patterns of the decline are comparable for other diseases. Further investigation of the time trend of circulatory diseases as well as other diseases whose incidence rate is capable of detection from Medicare data is required.
Importance of the Results for Heart Disease and Stroke
Heart disease and stroke account for more than 40% of all deaths among persons aged 65 to 74 years and almost 60% of those aged 85 years and older (Kissela et al., 2004; NIH/NHLBI, 1998; Williams, 2001). However, no nationally representative data are available on incidence, severity, or recurrence of acute coronary or stroke events in either the inpatient or out-patient settings, with the performance measures that are not consistent across databases (Goff et al., 2007). For heart disease and stroke, most of the readily available statistics in the United States are data sets with self-reported diseases and conditions, and results obtained from their analyses are predominantly on disease prevalence rather than on incidence events (NIH/NHLBI, 2005; NIH/NHLBI, 2006b; Thom et al., 2006). While most of the hospital-based surveillance programs are research projects rather than public health surveillance programs, the population-oriented surveys (such as those studying various risk factors prevalence) often have limited or no data on disease onset, detailed diagnosis, treatment, comorbidities, and so on. Therefore, the linked NLTCS-Medicare data equally representing both genders and various race/ethnic groups, and, specifically, having large enough number of incident cases of circulatory diseases could be very useful in estimating diseases incidence events in the U.S. elderly, together with associated medical costs, as well as comorbidities and disability (Feigin, Lawes, Bennett, & Anderson, 2003).
Limitations of the Study
The following points have to be kept in mind in interpreting the results of the study. Only primary diagnoses were taken into account. Secondary diagnoses can escape registration. The approximate statistical errors for age-specific and age-adjusted rates were obtained using a correction on sample design. Age-adjusted rates represent aggregated effects of different age groups with, maybe, different time trends (time trends of age-specific rates are discussed in Akushevich and Yashin [2008]). The rates obtained with alternative definitions of age at onset can differ and therefore, a detailed sensitivity analysis and the comparison of obtained rates to those obtained in other studies is a useful extension of this study which will be a subject of another investigation.
Conclusion
The performed analyses suggested that the national age-specific incidence patterns of circulatory diseases can be adequately evaluated from the Medicare Files of Service use. The NLTCS-M data set allows for bringing in additional information such as data allowing for analysis of comorbidity and disability patterns, data on use of medical procedures, data on case fatality assessment, specifically for ACHD and stroke, and so on. This information is extremely important for detailed analysis of health related effects in the U.S. elderly and cannot be obtained from the existing data sets. In addition, an advantage of the Medicare data is that they relate these age-specific incidence patterns to Medicare costs and, using NLTCS files, to disability prevalence. These results are timely and important as they may inform current scientific and policy debates about the effects of biomedical research and therapeutic innovations on disease incidence at increasingly advanced ages when effective therapeutic interventions are actively introduced in coming decades.
Acknowledgments
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by the National Institute on Aging grants R01AG027019, R01AG032319 and R01AG028259. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institute on Aging or the National Institutes of Health.
Biographies
Igor Akushevich is a senior research scientist at the Center for Population Health and Aging, Duke University. He received PhD in Theoretical and Mathematical Physics from the Byelorussian Academy of Sciences. He works in the area of biodemography of aging with special interest to studying geriatric-disease epidemiology from large-scale data.
Julia Kravchenko is a research scientist at the Duke Cancer Institute, Duke University. She received PhD in Medicine and Biochemistry from the Belorussian Medical Academy of Postgraduate Education. She works in the areas of cancer epidemiology, population-based disease risk studies, disease mechanisms modeling, clinical data analyses, and environmental/behavioral risks analyses.
Konstantin Arbeev is a senior research scientist at the Center for Population Health and Aging, Duke University. He received PhD in Mathematics and Physics from Ulyanovsk State University (Russia). His research interests include development of stochastic models for analyses of dynamic mechanisms of aging from longitudinal measurements of physiological indices.
Svetlana Ukraintseva is a senior research scientist at the Center for Population Health and Aging, Duke University, USA. She received her PhD in Genetic Epidemiology from the Moscow Institute for Medical Genetics, Russia. Her research interests include factors and mechanisms responsible for connection between aging, aging-related chronic diseases, and longevity.
Anatoli Yashin is a professor at the Center for Population Health and Aging, Duke University, USA. He received his PhD in Theoretical Cybernetics and DSc in Applied Statistics from the USSR Academy of Sciences. He studies mechanisms of aging-related changes in humans using advanced methods of statistical modeling.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
References
- Akushevich I, Kravchenko J, Ukraintseva S, Arbeev K, Yashin AI. Age patterns of geriatric disease incidences in the U.S. elderly population: Medicare-based analysis. Journal of American Geriatrics Society 2012. 2012;60:323–327. doi: 10.1111/j.1532-5415.2011.03786.x. Akushevich et al. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Akushevich I, Kulminski A, Akushevich L, Manton KG. TRENDS Working Paper Series. 2006. Age patterns of disease incidences in the U.S. elderly: Population-based analysis. [Google Scholar]
- Akushevich I, Kravchenko J, Akushevich L, Ukraintseva S, Arbeev K, Yashin AI. Cancer risk and behavioral factors, comorbidities, and functional status in the US elderly population. ISRN Oncology. 2011a;2011:415790. doi: 10.5402/2011/415790. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Akushevich I, Kravchenko J, Akushevich L, Ukraintseva S, Arbeev K, Yashin AI. Medical cost trajectories and onsets of cancer and noncancer diseases in US elderly population. Computational and Mathematical Methods. 2011b;2011:857892. doi: 10.1155/2011/857892. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Akushevich I, Yashin AI. Circulatory diseases and aging. In: Heggenhougen K, Quah S, editors. International encyclopedia of public health. Vol. 1. San Diego, CA: Academic Press; 2008. pp. 717–726. [Google Scholar]
- Altekruse SF, Kosary CL, Krapcho M, Neyman N, Aminou R, Waldron W, Edwards BK, editors. SEER Cancer Statistics Review, 1975–2007. Vol. 2010. Bethesda, MD: National Cancer Institute; 2009. [Google Scholar]
- Arnold AM, Psaty BM, Kuller LH, Burke GL, Manolio TA, Fried LP, Kronmal RA. Incidence of cardiovascular disease in older Americans: The cardiovascular health study. Journal of the American Geriatrics Society. 2005;53:211–218. doi: 10.1111/j.1532-5415.2005.53105.x. [DOI] [PubMed] [Google Scholar]
- Breslow NE, Day NE. IARC Scientific Publications 82. International Agency for Research on Cancer; Lyon, France: 1987. Statistical methods in cancer research. Volume II—The design and analysis of cohort studies; pp. 1–406. [PubMed] [Google Scholar]
- Centers for Disease Control and Prevention/National Center for Health Statistics. Deaths, percent of total deaths, and death rates for the 15 leading causes of death in selected age groups, by race and sex: United States, 1999–2006. Vol. 2010. Atlanta, GA: Centers for Disease Control and Prevention; 2006. [Google Scholar]
- Charlson ME, Pompei P, Ales KL, Mackenzie CR. A new method of classifying prognostic co-morbidity in longitudinal-studies—Development and validation. Journal of Chronic Diseases. 1987;40:373–383. doi: 10.1016/0021-9681(87)90171-8. [DOI] [PubMed] [Google Scholar]
- DHoore W, Bouckaert A, Tilquin C. Practical considerations on the use of the Charlson comorbidity index with administrative data bases. Journal of Clinical Epidemiology. 1996;49:1429–1433. doi: 10.1016/s0895-4356(96)00271-5. [DOI] [PubMed] [Google Scholar]
- Enright PL, McClelland RL, Newman AB, Gottlieb DJ, Lebowitz MD. Underdiagnosis and undertreatment of asthma in the elderly. Chest. 1999;116:603–613. doi: 10.1378/chest.116.3.603. [DOI] [PubMed] [Google Scholar]
- Fang J, Alderman MH. Trend of stroke hospitalization, United States, 1988–1997. Stroke. 2001;32:2221–2225. doi: 10.1161/hs1001.096193. [DOI] [PubMed] [Google Scholar]
- Feigin VL, Lawes CMM, Bennett DA, Anderson CS. Stroke epidemiology: A review of population-based studies of incidence, prevalence, and case-fatality in the late 20th century. The Lancet Neurology. 2003;2:43–53. doi: 10.1016/s1474-4422(03)00266-7. [DOI] [PubMed] [Google Scholar]
- Ferrucci L, Guralnik JM, Pahor M, Corti MC, Havlik RJ. Hospital diagnoses, Medicare charges, and nursing home admissions in the year when older persons become severely disabled. Journal of the American Medical Association. 1997;277:728–734. [PubMed] [Google Scholar]
- Gill TM, Robison JT, Tinetti ME. Predictors of recovery in activities of daily living among disabled older persons living in the community. Journal of General Internal Medicine. 1997;12:757–762. doi: 10.1046/j.1525-1497.1997.07161.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Goff DC, Jr, Brass L, Braun LT, Croft JB, Flesch JD, Fowkes FGR, Jencks SF. Essential features of a surveillance system to support the prevention and management of heart disease and stroke: A scientific statement from the American Heart Association Councils on Epidemiology and Prevention, Stroke, and Cardiovascular Nursing and the Interdisciplinary Working Groups on Quality of Care and Outcomes Research and Atherosclerotic Peripheral Vascular Disease. Circulation. 2007;115:127–155. doi: 10.1161/CIRCULATIONAHA.106.179904. [DOI] [PubMed] [Google Scholar]
- Goldstein LB, Samsa GP, Matchar DB, Horner RD. Charlson index comorbidity adjustment for ischemic stroke outcome studies. Stroke. 2004;35:1941–1945. doi: 10.1161/01.STR.0000135225.80898.1c. [DOI] [PubMed] [Google Scholar]
- Greenlund K, Giles W, Keenan N. Heart disease and stroke mortality in the 20th century. In: Ward J, Warren C, editors. Silent victories: The history and practice of public health in twentieth century America. Oxford, England: Oxford University Press; 2006. [Google Scholar]
- Katz S, Branch LG, Branson MH, Papsidero JA, Beck JC, Greer DS. Active life expectancy. New England Journal of Medicine. 1983;309:1218–1224. doi: 10.1056/NEJM198311173092005. [DOI] [PubMed] [Google Scholar]
- Kissela B, Schneider A, Kleindorfer D, Khoury J, Miller R, Alwell K, Moomaw C. Stroke in a biracial population: The excess burden of stroke among blacks. Stroke. 2004;35:426–431. doi: 10.1161/01.STR.0000110982.74967.39. [DOI] [PubMed] [Google Scholar]
- Klabunde CN, Potosky AL, Legler JM, Warren JL. Development of a comorbidity index using physician claims data. Journal of Clinical Epidemiology. 2000;53:1258–1267. doi: 10.1016/s0895-4356(00)00256-0. [DOI] [PubMed] [Google Scholar]
- Kravchenko J, Akushevich I, Abernethy AP, Lyerly HK. Evaluating the Number of Stages in Development of Squamous Cell and Adenocarcinomas across Cancer Sites Using Human Population-Based Cancer Modeling. PLoS One. 2012;7(5):e37430. doi: 10.1371/journal.pone.0037430. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kulminski A, Yashin A, Ukraintseva S, Akushevich I, Arbeev K, Land K, Manton K. Accumulation of health disorders as a systemic measure of aging: Findings from the NLTCS data. Mechanisms of Ageing and Development. 2006;127:840–848. doi: 10.1016/j.mad.2006.08.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Levy D, Larson MG, Vasan RS, Kannel WB, Ho KKL. The progression from hypertension to congestive heart failure. Journal of the American Medical Association. 1996;275:1557–1562. [PubMed] [Google Scholar]
- Lohr SL. Sampling: Design and analysis. Brooks/Cole Cengage Learning; Boston, MA: 2009. [Google Scholar]
- Luepker RV, Apple FS, Christenson RH, Crow RS, Fortmann SP, Goff D, Tunstall-Pedoe H. Case definitions for acute coronary heart disease in epidemiology and clinical research studies—A statement from the AHA council on epidemiology and prevention; AHA Statistics Committee; World Heart Federation Council on epidemiology and prevention; the European Society of Cardiology working group on epidemiology and prevention; Centers for Disease Control and Prevention; and the National Heart, Lung, and Blood Institute. Circulation. 2003;108:2543–2549. doi: 10.1161/01.CIR.0000100560.46946.EA. [DOI] [PubMed] [Google Scholar]
- Manton KG, Corder LS, Stallard E. Estimates of change in chronic disability and institutional incidence and prevalence rates in the united-states elderly population from the 1982, 1984, and 1989 National Long-Term-Care survey. Journals of Gerontology. 1993;48:S153–S166. doi: 10.1093/geronj/48.4.s153. [DOI] [PubMed] [Google Scholar]
- Manton KG, Corder L, Stallard E. Chronic disability trends in elderly United States populations: 1982–1994. Proceedings of the National Academy of Sciences of the United States of America. 1997;94:2593–2598. doi: 10.1073/pnas.94.6.2593. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Manton KG, Gu XL. Changes in the prevalence of chronic disability in the United States black and nonblack population above age 65 from 1982 to 1999. Proceedings of the National Academy of Sciences of the United States of America. 2001;98:6354–6359. doi: 10.1073/pnas.111152298. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Manton KG, Gu X, Lamb VL. Change in chronic disability from 1982 to 2004/2005 as measured by long-term changes in function and health in the US elderly population. Proceedings of the National Academy of Sciences of the United States of America. 2006;103:18374–18379. doi: 10.1073/pnas.0608483103. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Manton KG, Stallard E, Corder LS. The dynamics of dimensions of age-related disability 1982 to 1994 in the U.S. elderly population. Journals of Gerontology Series A, Biological Sciences and Medical Sciences. 1998;53:B59–B70. doi: 10.1093/gerona/53a.1.b59. [DOI] [PubMed] [Google Scholar]
- Nagi SZ. An epidemiology of disability among adults in the United States. Milbank Memorial Fund Quarterly Health and Society. 1976;54:439–467. [PubMed] [Google Scholar]
- Nattinger AB, Laud PW, Bajorunaite R, Sparapani RA, Freeman JL. An algorithm for the use of Medicare claims data to identify women with incident breast cancer. Health Services Research. 2004;39:1733–1749. doi: 10.1111/j.1475-6773.2004.00315.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nattinger AB, Laud PW, Bajorunaite R, Sparapani RA, Freeman JL. Clarification note to an algorithm for the use of medicare claims data to identify women with incident breast cancer (vol 39, pg 6, 2004) Health Services Research. 2006;41:302–302. doi: 10.1111/j.1475-6773.2004.00315.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- National Center for Health Statistics. Health, United States, 2008 with Chart-book. Hyattsville, MD: National Center for Health Statistics; 2009. [Google Scholar]
- National Institutes of Health, Public Health Service, National Heart, Lung and Blood Institute. Morbidity and mortality, 1998 Chartbook on cardiovascular, lung, and blood diseases. Bethesda, MD: Author; 1998. [Google Scholar]
- National Institutes of Health, Public Health Service, National Heart, Lung and Blood Institute. Morbidity and mortality: 2004 chart book on cardiovascular, lung, and blood diseases. Vol. 2010. Bethesda, MD: Author; 2005. [Google Scholar]
- National Institutes of Health, Public Health Service, National Heart, Lung and Blood Institute. Incidence and prevalence: 2006 chart book on cardiovascular and lung diseases. Vol. 2010. Bethesda, MD: Author; 2006a. [Google Scholar]
- National Institutes of Health, Public Health Service, National Heart, Lung and Blood Institute. Morbidity and mortality: 2006 chart book on cardiovascular, lung, and blood diseases. Vol. 2010. Bethesda, MD: Author; 2006b. [Google Scholar]
- Quan HD, Sundararajan V, Halfon P, Fong A, Burnand B, Luthi JC, Ghali WA. Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Medical Care. 2005;43:1130–1139. doi: 10.1097/01.mlr.0000182534.19832.83. [DOI] [PubMed] [Google Scholar]
- Rosamond W, Flegal K, Friday G, Furie K, Go A, Greenlund K, Hong Y. Heart disease and stroke statistics—2007 update: A report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation. 2007;115:e69–e171. doi: 10.1161/CIRCULATIONAHA.106.179918. [DOI] [PubMed] [Google Scholar]
- Sloan FA, Brown DS, Carlisle ES, Ostermann J, Lee PP. Estimates of incidence rates with longitudinal claims data. Archives of Ophthalmology. 2003;121:1462–1468. doi: 10.1001/archopht.121.10.1462. [DOI] [PubMed] [Google Scholar]
- Solomon PR, Murphy CA. Should we screen for Alzheimer’s disease? A review of the evidence for and against screening for Alzheimer’s disease in primary care practice. Geriatrics and Gerontology International. 2005;60:26–31. [PubMed] [Google Scholar]
- Stallard E. Demographic issues in longevity risk analysis. Journal of Risk and Insurance. 2006;73:575–609. [Google Scholar]
- Thom T, Haase N, Rosamond W, Howard VJ, Rumsfeld J, Manolio T, Kittner S. Heart disease and stroke statistics—2006 update: A report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation. 2006;113:85–151. doi: 10.1161/CIRCULATIONAHA.105.171600. [DOI] [PubMed] [Google Scholar]
- Trussell J, Richards T. Correcting for unmeasured heterogeneity in hazard models using the Heckman-Singer procedure. Sociological Methodology. 1985;15:242–276. [Google Scholar]
- Ukraintseva SV, Yashin AI. How individual age-associated changes may influence human morbidity and mortality patterns. Mechanisms of Ageing and Development. 2001;122:1447–1460. doi: 10.1016/s0047-6374(01)00277-9. [DOI] [PubMed] [Google Scholar]
- Vaupel JW, Carey JR, Christensen K, Johnson TE, Yashin AI, Holm NV, Liedo P. Biodemographic trajectories of longevity. Science. 1998;280:855–860. doi: 10.1126/science.280.5365.855. [DOI] [PubMed] [Google Scholar]
- Wenger NK. Coronary heart disease: The female heart is vulnerable. Progress in Cardiovascular Diseases. 2003;46:199–229. doi: 10.1016/j.pcad.2003.08.003. [DOI] [PubMed] [Google Scholar]
- Williams GR. Incidence and characteristics of total stroke in the United States. BMC Neurology. 2001;1:2. doi: 10.1186/1471-2377-1-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Xu J, Kochanek KD, Murphy SL, Tejada-Vera B. Deaths: Final data for 2010. National Vital Statistics Reports. 58:19. [PubMed] [Google Scholar]
- Yashin AI, Akushevich I, Arbeev K, Akushevich L, Kulminski A, Ukraintseva S. Studying health histories of cancer: A new model connecting cancer incidence and survival. Mathematical Biosciences. 2009;218:88–97. doi: 10.1016/j.mbs.2008.12.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Yashin A, Akushevich I, Ukraintseva S, Akushevich L, Arbeev K, Kulminski A. Trends in survival and recovery from stroke: Evidence from the National Long-Term Care Survey/Medicare Data. Stroke. 2010;41:563–565. doi: 10.1161/STROKEAHA.109.572339. [DOI] [PMC free article] [PubMed] [Google Scholar]