Summary
Burn scars still represent a challenge to the reconstructive surgeon. Their management requires a specific expertise and set up involving the possibility of long term rehabilitation and follow up. Cases encountered in humanitarian missions present additional issues. Often the local environment is not suitable for an appropriate treatment plan, requiring the case to be transferred to a foreign country for surgical care as part of an integrated international and multidisciplinary management. We present the case of a three year-old patient injured in a bomb explosion during the Arab Spring and suffering from severe scar contracture limiting thoracic and upper limb movement. After initial consultation at distance, transfer to our country was organized and an intensive surgical and rehabilitative program was carried out over three months. After five months, the patient returned to his home country where a supportive network had been set up for continued rehabilitation, ensuring follow up for over a year and ultimate success.
Keywords: burn, scar, plastic surgery, humanitarian mission
Abstract
Les cicatrices de brûlures représentent toujours un défi pour le chirurgien de reconstruction. Leur gestion nécessite une expertise spécifique et la possibilité de réhabilitation à long terme, y compris le suivi. Les cas rencontrés dans les missions humanitaires présentent des problèmes supplémentaires. Souvent l’environnement local n’est pas adapté pour un plan de traitement approprié, et donc il faut transféré le patient dans un pays étranger pour des soins chirurgicaux dans le cadre d’une gestion internationale et multidisciplinaire intégrée. Nous présentons le cas d’un patient de trois ans blessé à cause de l’explosion d’une bombe pendant le printemps arabe. Ce patient souffrait de contractures graves qui limitaient le mouvement du membre thoracique et supérieure. Après une consultation initiale à distance, il a été transferé à notre pays où il a subi un programme de chirurgie et de réadaptation intensive qui a duré trois mois. Après cinq mois, le patient est retourné à son pays d’origine où un réseau de soutien a été mis en place pour continuer la réhabilitation, assurer un suivi de plus d’un an et le succès final.
Introduction
Burn care has an important role in the history of plastic Surgery; requirements of burn and scar treatment have formed the basis of the development of most of the techniques that constitute plastic Surgery core knowledge. While deeper understanding of burns physiology helped greatly to reduce mortality and improve outcomes in the acute burn phase, scar revision and postoperative management are still a major challenge.1 The approach to pathologic scars remains a long and painful process, requiring great surgical experience and a well-defined preoperative assessment. in wealthy countries, there is usually a well organized and complete network of care for burn patients, encompassing patient support after healing, with the aim of minimizing the impact of scarring preventing complications, and treating any pathologic scars which occur. For a wide range of reasons, in developing countries the care of burn patients is less structured. Early exit of patients from the follow up process is thus an easier occurrence, leading to more frequent cases of patients who develop scarring complications in the mid and long term.2,3
Retracting scars and secondary deformations, which limit physical and social life, are still the main severe longterm complications after burns. inhibition of joints’ movement and disfiguring deformities limit patients’ every day life and relationships, with a particularly significant impact in children. The aim of surgical treatment and rehabilitation is to restore function, correct any deformities induced, improve morphological appearance and permit normal growth. This is carried out by involving the family in the rehabilitation projects and prolonging the follow up until growth is complete.4,5 When all these needs are to be met for patients encountered during humanitarian projects in countries where optimal treatment is not otherwise available, specific issues arise.
We present the case of a 3-year-old child suffering from severe burn scars of the chest and upper limbs, who received surgical treatment at our Clinic in a humanitarian project.
Case Report
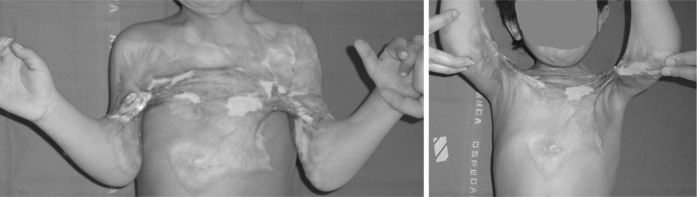
We were consulted on the case of a 3-year-old child who had sustained severe thermal burns in a bomb explosion during an uprising in the Arab Spring, two years prior. The patient was first evaluated in his home country by physicians on a humanitarian mission; preliminary surgical consultation was performed by means of photographs and the internet. Scar contractures originating on the anterior thorax and extending to the anterior axillary pillars, arms and volar aspect of the elbows lead to arm to thorax partial fusion with severe functional limitation of arm abduction to <45° and reduced forearm extension (Fig. 1). Major nipples’ dislocation to the axillae and minor retracting scars to the left side of the neck coexisted.
Fig. 1.
A case of a 3 year-old child suffering from severe retracting burn scars of the anterior chest and upper limbs (left) determining functional impairment of arms abduction (right).
A surgical plan was discussed and an intensive schedule was decided to allow effective treatment with recourse to safe techniques in the minimal timeframe possible. As healthy skin appeared insufficient to provide repair by mobilization after scar excision, the surgical approach was established around three principal stages:
Release of axillary and elbow retractions by scar excision and multiple Z-plasties.
Expansion of anterior thoracic skin.
Rotation of the expanded skin flaps to obtain satisfactory and stable axillary opening.
The patient was then transferred to our country accompanied by one parent. Anesthesiology reassessment was performed and the reconstructive plan began. in a first operation, extension of the joints was restored by multiple Z-plasties extended from the thorax to the elbows, with minimal scar excision (Fig. 2). The plasties flaps were insufficient to cover the entire surface in order to achieve full extension. prioritizing full closure at the axillae, bare areas remained between the flaps on the medial aspect of the arm. These were treated by implant of a collagen-GAG dermal regenerative template (Integra©, Integra Life- Sciences Inc., Plainsboro, NJ, USA) (Fig. 3) as an intermediate step before skin grafting, with the aim of improving functional and aesthetic quality of the grafts. The arms were stabilized at 90° by means of thermoplastic casts. At the same time, two tissue expanders (left 225 cm3, right 350 cm3) were implanted subcutaneously in the anterior thorax (Fig. 2), and retracting cervical scars were revised by multiple Z-plasties.
Fig. 2.

The retracting scars were released by multiple Z-plasties running from the chest to the elbows bilaterally. priority was given to full skin coverage of the anterior pillar of the axillae, leaving bare surfaces between the plasties flaps at the arms. These areas were initially covered with a dermal regenerative template. in the same operation, two skin expanders were implanted in the anterior chest.
Fig. 3.
Once full skin expansion was achieved (a), the two expanded skin flaps were raised (b) and rotated to provide functionally and aesthetically optimal repair of the axillary and chest regions (c).
Expansion was performed every third day under sedation, with 30 cc of saline until overfilling was reached (left 265 cm3, right 380 cm3) after three months. During one of these sessions, four weeks after the first operation, arm areas in which the collagen-GAG had matured were repaired with split-thickness skin grafts.
After 15 days of expansion stabilization (Fig. 3a), a second operation was performed in which axillary and anterior thorax scar excision was completed and the expanded skin flaps were rotated in its place (Figs. 3b and 3c) to achieve stable arm extension (Figs. 4-5). in this way, repositioning of the nipples was also achieved.
Fig. 4.

This approach allowed a quick restoration of almost complete upper limbs function, stable at 1 year follow up (a). To prevent recurrence, stabilize the benefits in the long term, and improve the functional outcomes, custom made elastic garments were provided (b).
Soon after surgery, the patient started an intensive rehabilitation program of active and passive movements (Fig. 4a). Customized elastic pressure garments were provided as part of the physical therapy (Fig. 4b).
The recovery of the upper limbs and neck range of motion was estimated at over 95%, with 90% neck rotation capacity, and almost full excursion of the upper limbs in abduction/adduction movements (Fig. 4a). Two months after surgery - five and a half months after starting treatment - the patient returned to his home country where physical therapy and follow up had been organized.
Discussion
Severe burn scars are becoming a less frequent encounter in developed countries, where the combination of increased workplace safety, a diffused preventive attitude, and a high attention to aesthetic and functional outcomes made serious burns in both the adult and pediatric populations overall uncommon events. However, burns remain a major concern in less developed countries, where a culture of safety in the home and work setting is less diffuse. in other countries exceptional events, such as wars, further increase this risk. in particular, a high incidence of burns occurs in the pediatric age group.6 in underdeveloped countries, the network of care and follow up of burn sequelae is also less organized, with worse outcomes being more likely as a consequence. Such outcomes tend to be more severe in children, as retracting scars can not only limit an acquired function, but may also impair the development of entire body segments. This transforms a potentially difficult case into a more severe one. For this reason, a prompt and full resolution is even more important.
Although projects aimed at transferring health care knowledge and organization to developing countries are the current mainstream of humanitarian missions,7 as opposed to patient transfer, there is still a need to organize treatment of specific patients in more adequate settings. Such an example is the case of a child with severe functionally impairing scarring, requiring prompt action with minimal anesthesiology and surgery risks, and especially a proper follow up system that readily takes care of early post-surgery rehabilitation.
The organization of this approach poses some issues. The patient has to be moved to a different country, and needs to be accompanied by someone he knows, likely a parent, who will remain far from the rest of the family, and even out of work, for a prolonged time. For this reason, treatment time has to be minimized, compatibly with the surgical plan. legal matters and compensation issues should also be considered well in advance, as their resolution may significantly delay the process. Suitable lodging needs to be provided and interpreters must be available to allow adequate interaction with the patient and his family. in all these steps, close collaboration between multiple players, ranging from clinicians and hospital administration to local and international humanitarian organizations, to diplomatic authorities is fundamental.
An accurate pre-operative evaluation needs to be performed at distance, based on photographs and videos, so that a realistic reconstructive plan is devised that can begin as soon as the patient is on site. With internet and digitalization diffusion, most pre-operative studies (laboratory tests, ECG, X-rays, CT-scans) can be performed in the home country, limiting uncertainty, and even an anesthesiology pre-assessment can be performed, to be completed by the actual anesthesiology team once the patient is available. The plan should be discussed with the entire care team well ahead, and clinicians from the home country should be included in this process from the beginning to ensure the possibility of long-term management of the case before and after the acute treatment steps in the foreign country. At least one year of physiotherapy and physical rehabilitation is necessary to stabilize and maintain the surgical results, which is hardly feasible unless an effective care network is established for the specific patient in his home country.8
From a surgical point of view, in most cases, a multistep approach including operations, dressing changes, and postoperative follow up is required. However, to guarantee minimization of risks and treatment time, the surgical approach should be simplified, avoiding more complex alternative solutions. Any intermediate steps, such as expanders inflation, should be managed with the shortest interval possible.
A traditional multiple Z-plasties technique allows full release of joint retractions and provides an early acquisition of an acceptable range of motion.9 The adjunct use of dermal substitutes on remaining bare areas offers high functional and aesthetic results, superior to skin grafting alone, resulting in a more pliable and physiologic skin, and minimizing donor site morbidity.10,11 After a while, skin expansion provides versatile local flaps to stabilize the gained results and improve the aesthetic outcome. The filling of skin expanders normally occurs with a weekly cadence; however, if necessary, expansions can be performed with a reduced spacing, especially in the case of the more elastic and biologically active skin of a child.12,13
Conclusion
The management of severe burn scars remains complex and cases encountered as part of humanitarian missions present further specific challenges. Combined organizational efforts are required on multiple parts, especially if treatment of the case is moved to a different country. A multidisciplinary approach in which surgery is but a step, involving health professionals in the home country, guarantees success and long term results.
Acknowledgments
Acknowledgements. The authors would like to thank the members of the rotary Club padova Euganea, whose contribution in the form of Club Service granted treatment to the patient. The authors are also in debt to Ms. Emanuela Ometto for her essential personal and financial contribution and lawyer ilaria gobbato for the pro bono legal assistance and support.
Conflict of interest. None.
Funding. None.
References
- 1.Stiefel D, Schiestl C, Meuli M. Integra Artificial Skin for burn scar revision in adolescents and children. Burns. 2010;36:114–20. doi: 10.1016/j.burns.2009.02.023. [DOI] [PubMed] [Google Scholar]
- 2.Peck MD. Epidemiology of burns throughout the world. part i: Distribution and risk factors. Burns. 2011;37:1087–100. doi: 10.1016/j.burns.2011.06.005. [DOI] [PubMed] [Google Scholar]
- 3.Forjuoh SN. Burns in low- and middle-income countries: a review of available literature on descriptive epidemiology, risk factors, treatment, and prevention. Burns. 2006;32:529–37. doi: 10.1016/j.burns.2006.04.002. [DOI] [PubMed] [Google Scholar]
- 4.Poiret G, Guerreschi P, Maillet M, De Broucker V, Gottrand L, Pellerin P. Treatment of sequelae of burns in children. Ann Chir Plast Esthet. 2011;56:474–83. doi: 10.1016/j.anplas.2011.07.007. [DOI] [PubMed] [Google Scholar]
- 5.Germann G, Cedidi C, Hartmann B. Post-burn reconstruction during growth and development. Pediatr Surg Int. 1997;12:321–6. doi: 10.1007/BF01076930. [DOI] [PubMed] [Google Scholar]
- 6.Lancerotto L, Sferrazza R, Amabile A, Azzena B. Burn care in relation to burn epidemiology in Italy. Burns. 2011;37:835–41. doi: 10.1016/j.burns.2010.12.014. [DOI] [PubMed] [Google Scholar]
- 7.Hashmi M, Kamal R. Management of patients in a dedicated burns intensive care unit (BiCU) in a developing country. Burns. 2013;39:493–500. doi: 10.1016/j.burns.2012.07.027. [DOI] [PubMed] [Google Scholar]
- 8.Rochet JM, Hareb F. Burns and rehabilitation. Pathol Biol. 2002;50:137–49. doi: 10.1016/s0369-8114(01)00278-4. [DOI] [PubMed] [Google Scholar]
- 9.Hudson DA, Renshaw A. An algorithm for the release of burn contractures of the extremities. Burns. 2006;32:663–8. doi: 10.1016/j.burns.2006.02.009. [DOI] [PubMed] [Google Scholar]
- 10.Dantzer E, Braye FM. Reconstructive surgery using an artificial dermis (integra): results with 39 grafts. Br J Plast Surg. 2001;54:659–64. doi: 10.1054/bjps.2001.3684. [DOI] [PubMed] [Google Scholar]
- 11.Heit YI, Lancerotto L, Cortes R, Mesteri I, Ackermann M, Hollander R, et al. Early kinetics of integration of collagen-glycosaminoglycan regenerative scaffolds in a diabetic mouse model. Plast Reconstr Surg. 2013;132:767–76. doi: 10.1097/PRS.0b013e3182a3c091. [DOI] [PubMed] [Google Scholar]
- 12.Friedman RM, Ingram AE, Rohrich RJ, Byrd HS, Hodges PL, Burns AJ, et al. Risk factors for complications in pediatric tissue expansion. Plast Reconstr Surg. 1996;98:1242–6. doi: 10.1097/00006534-199612000-00019. [DOI] [PubMed] [Google Scholar]
- 13.Neumann CG. The expansion of an area of skin by progressive distention of a subcutaneous balloon; use of the method for securing skin for subtotal reconstruction of the ear. Plast Reconstr Surg. 1957;19:124–30. doi: 10.1097/00006534-195702000-00004. [DOI] [PubMed] [Google Scholar]