Abstract
Inguinal hernia repair is the most common surgery done by both young and experienced surgeons. The hernia in the inguinal region usually contains the omentum and small intestine but rarely can contain unusual contents like the appendix, ovary with fallopian tubes, urinary bladder, sigmoid colon, and cecum. The aim of this study is to present our experience of uncommon contents in the inguinal hernia sac and their surgical management. A retrospective study of 330 patients who underwent inguinal hernia repair was carried out over a period of 3 years from January 2008 to December 2011. Only five patients presented with unusual contents in the inguinal hernia sac; an incidence of 1.5 %. Two of them had vermiform appendix, with acute appendicitis (Amyand’s hernia) noted in one of them. The patient with acute appendicitis underwent appendicectomy with herniorrhaphy, while in the other, hernioplasty with mesh was done as the patient was with normal appendix. In one case, the urinary bladder was the content of the inguinal hernia sac and there were two cases with the ovary and fallopian tubes as its content. In all these cases, contents were replaced back and hernia repair was done. Unusual contents of the hernial sac may create a surgical dilemma (whether to save or sacrifice the organ) during hernia repair even to an experienced surgeon.
Keywords: Inguinal hernia, Amyand’s hernia, Appendix, Ovary
Introduction
Inguinal hernia repair is the most frequent surgery done by a surgeon. The hernia in the inguinal region frequently contains the omentum and small intestine. However, the presence of unusual organs in the inguinal hernial sac could create a tricky situation for the operating surgeon [1, 2]. The often-encountered unusual contents are the appendix, ovary, fallopian tubes, urinary bladder, Meckel’s diverticulum, and sigmoid colon [1, 2]. The reported incidence of such cases is mostly in the form of case reports; so, we carried out a 3-year retrospective study in our institution to determine the incidence of unusual hernial sac contents. We present here the surgical dilemma faced by the surgeon while operating on five inguinal hernia cases with unusual contents in its sac.
Material and Methods
A retrospective study of all operated cases of inguinal hernia during the period between January 2008 and December 2011 was carried out in a rural medical college. A total of 330 cases of inguinal hernia were operated on during this period. Information of clinical presentation, contents of sac including the presence of unusual organs in the sac, operative details, and complications were reviewed.
Operative Technique
Appendicectomy was carried out in one case due to an inflamed appendix and herniorrhaphy was done. In the rest, unusual organs were saved and reduced back into the peritoneal cavity and hernioplasty was carried out. In the remaining 225 cases, routine hernia surgical procedures were carried out.
Results
A total of 330 patients with inguinal hernias were operated on. Age ranged between 8 months and 70 years. Only 2 patients were female and 228 were males. Two hundred thirty-five patients presented with indirect inguinal hernia and 95 patients were suffering from direct inguinal hernia. Two hundred seventy patients had the small bowel as contents of the sac and the remaining 55 had the omentum as sac content. Only five cases (1.5 %) had unusual sac contents: two cases with the appendix, two cases with the ovary and fallopian tubes, and one case with the urinary bladder. One hundred five patients presented with obstruction and none with strangulation. Details about age group, male to female ratio, types of hernia, and postoperative complications are shown in Table 1. Only 2 % patients had superficial wound infection and recurrence. Follow-up period was 4 months to 3 years.
Table 1.
Details of age group, types of hernia, sac contents, surgical procedures, and postoperative complications
| Total patients | 330 |
| Age group | 8 months to 70 years |
| Males | 228 |
| Females | 2 |
| No. of indirect inguinal hernia | 235 |
| No. of direct inguinal hernia | 95 |
| Nonobstructed | 225 |
| Obstructed | 105 |
| Strangulation | Nil |
| Surgical | Procedure hernioplasty/herniorrhaphy/hernioplasty |
| Intraoperative findings | Only five hernial sacs were with unusual contents (1.5 %) |
| Contents in sac | |
| Bowel loops | 270 |
| Omentum | 55 |
| Appendix | 2 |
| Ovary and fallopian tubes | 2 |
| Urinary bladder | 1 |
| Postoperative complications | |
| Wound infection (superficial) | 6 cases (2 %) |
| Recurrence of hernia | 6 cases (2 %) |
| Follow-up period | 3 years to 4 months |
Details of Unusual Cases
Cases with Appendix in Sac
First Case
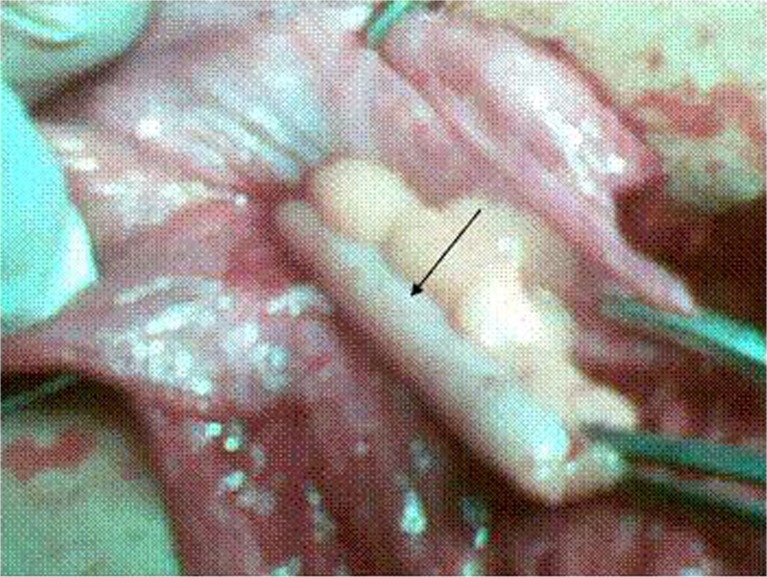
A 55-year-old male presented with pain in the right groin due to inguinoscrotal swelling for the last 3 days. Swelling was there for the last 9 months. The patient was diagnosed as a case of obstructed hernia. All laboratory data were within normal limits, except total leukocyte count which was higher than normal. The patient was operated on as an emergency case. An inflamed appendix was found as the content of the indirect hernia sac (Fig. 1). The distal end of the appendix was adherent to the wall of the sac. Appendectomy was performed and herniorrhaphy was done with Bassini’s method. The postoperative period was uneventful, and he was discharged on the fifth day. He was followed up at our outpatient department (OPD) for the removal of stitches. Histopathology of the removed appendix revealed acute appendicitis.
Fig. 1.
Inflamed appendix in the hernial sac
Second Case
A 35-year-old male presented with inguinoscrotal swelling for the last 6 months and was diagnosed as a case of indirect inguinal hernia. All blood investigations were within the normal range. The patient was operated on through conventional oblique incision. To our great surprise, the appendix was the content of the hernial sac and it was not inflamed (Fig. 2). The surgeon was in a dilemma on what to do with the normal-looking appendix as there are varied opinions—whether to sacrifice or save the normal-looking appendix. We decided to replace the appendix in the abdomen and herniorrhaphy was done with Prolene mesh. The postoperative period was uneventful, and the patient was discharged on the fifth day. He was followed up at the OPD for removal of the sutures.
Fig. 2.
Normal appendix in the hernial sac
Third Case with Ovary as Content
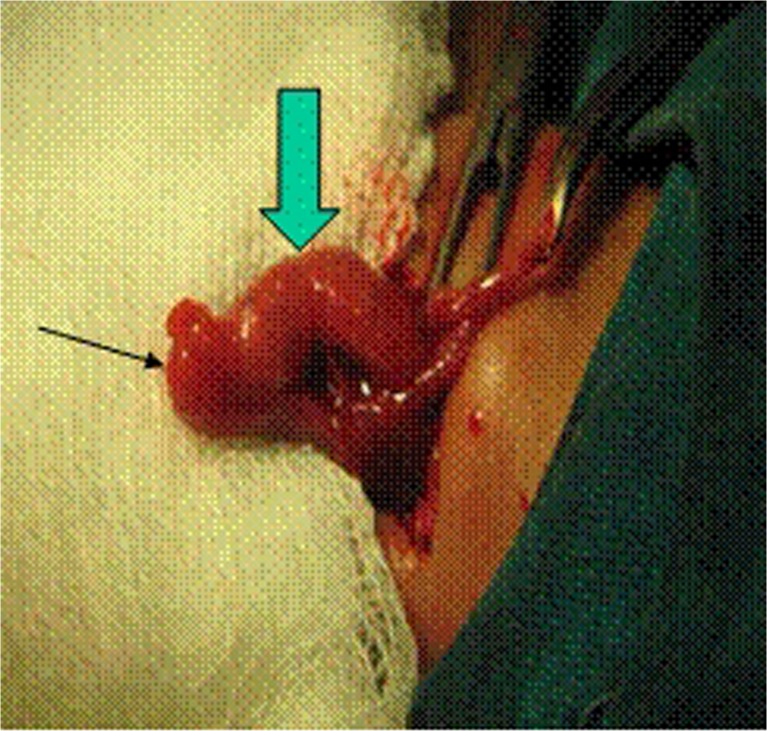
An 8-month-old girl was admitted to the emergency ward with acute left groin swelling that increased in size with the crying of the child. The swelling was there since birth. On examination, there was a 2 × 1.5-cm firm, irreducible, and tender swelling in the left inguinal region. The rest of the abdomen was normal, leading to a diagnosis of irreducible left inguinal hernia. Ultrasound of the left groin demonstrated a 2.5 × 2.0 × 2.0-cm solid oval structure. Overall features suggested the presence of the ovary with fallopian tubes. Emergency surgery was done. The hernia sac consisted of the congested ovary along with congested and swollen fallopian tubes (Fig. 3). The operating surgeon was in a dilemma whether to save or remove this edematous and congested swollen ovary with edematous fallopian tubes. But in spite of the edema and congestion, the ovary appeared viable, and therefore, we decided to reduce it back into the abdomen. Hernia repair was done, and the postoperative period was uneventful (Fig. 4).
Fig. 3.
Edematous bulky ovary with congested fallopian tubes
Fig. 4.
Hernia of the canal of Nuck up to the labia
Fourth Case with Ovary and Fallopian Tube
A 3-year-old girl was admitted to the ward with a history of right groin swelling that increased in size with the crying of the child since birth. On examination, there was a 2.5 × 1.5-cm firm reducible swelling in the right inguinal region (Fig. 5). The rest of the abdomen was normal, leading to a diagnosis of reducible right inguinal hernia. Ultrasound of right groin demonstrated a 3 × 2.5 × 2.0-cm solid oval structure. Overall features suggested the presence of the right ovary with fallopian tube. Surgery was done as a routine case of inguinal hernia. We were able to reduce the ovary. Hernia repair was done, and the postoperative period was uneventful.
Fig. 5.
Urinary bladder as the contents of the right direct inguinal hernial sac
Fifth Case with Urinary Bladder as Content
A 24-year-old male presented with an inguinal swelling for the last 6 months and was diagnosed as a case of inguinal hernia as swelling was reducible with positive cough impulse. All blood investigations were normal. The patient was operated on through standard inguinal incision. There was direct inguinal hernia with the urinary bladder as its content (Fig. 5). The bladder was gently separated from the spermatic cord and was replaced back. The bladder was catheterized to look for hematuria in the postoperative period. If there is injury to the bladder, there is always hematuria in the postoperative period. Bladder drainage also heals minor bladder perforation during surgery. So, it was a dilemma whether to catheterize or not because catheterization will infect a virgin urethra. Herniorrhaphy was done with Prolene mesh. The postoperative period was uneventful.
Discussion
Inguinal hernia repair is a regularly done surgical procedure which may sometimes astonish the surgeon with its peculiar contents [1, 2]. This may create problems in management due to its unexpected constituent. Inguinal hernias are mostly diagnosed with history and clinical examination. Ultrasonography (USG), computed tomography scan, magnetic resonance imaging, or color Doppler is never carried out in the preoperative period, but if done, these investigations are very useful to confirm the presence of unusual organs as well as their vascularity in case of strangulated hernias.
The presence of a normal vermiform appendix in an inguinal hernia sac is uncommon, with a reported incidence of 0.6 to 1 % of inguinal hernias [3, 4]. It has generally been associated with large indirect inguinoscrotal hernias, but occasionally, direct hernias may also contain them [1, 3]. Acute appendicitis within an inguinal hernia accounts for 0.1 % of all cases [1]. More common in males and are invariably on the right side and exceptionally on the left side due to situs inversus [5].
The pathophysiology is unfamiliar. When the appendix enters the sac, it becomes susceptible to trauma due to external force or due to contraction of the abdominal muscles. Thus, the compressed appendix can get injured and inflamed [6, 7]. Mobile cecum may be a predisposing factor for developing Amyand’s hernia [8].The most common presentation is irreducible painful hernia (83 %). Most common differential diagnoses are strangulated hernia and incarcerated omentum [9].
If the appendix is inflamed, then appendicectomy is mandatory and hernial repair should be performed with Bassini or Shouldice technique, without making use of synthetic meshes because the mesh may get infected [10]. In huge hernia, even with appendicitis, hernioplasty can be done with antibiotics. Laparoscopic reduction of Amyand’s hernia has been described in the literature.
Whether to remove or leave behind a noninflamed appendix is confusing. The patient’s age, size of the appendix, life expectancy, and lifelong risk of developing acute appendicitis influence the surgeon’s decision of performing appendicectomy. If one plans to do appendicectomy for a normal appendix, then there are chances of infection to an otherwise clean surgery and surgical handling to reach the base of the appendix may also weaken the muscles and thus increases the possibility of recurrence; so, it is ideal to replace the normal-looking appendix and do hernioplasty.
Those in favor of appendicectomy, however, feel that surgical handling will traumatize the appendix partially. So, it is better to deal with appendicectomy with outmost care taken to prevent contamination. As younger patients have a higher risk of developing acute appendicitis in later age, appendectomy may be considered, whereas in elderly individuals, the appendix may be left intact [1].
So, it is a surgical dilemma for the surgeon to decide whether to save or remove a normal-looking appendix which might have become traumatized while handling and may present as appendicitis in the postoperative period or we unnecessarily remove a normal appendix and open the gut and thus increase the chances of wound infection. We replaced the appendix in our second case as it was looking absolutely normal and also we were very gentle while handling the appendix to avoid perioperative trauma.
In female infants, bowel loops and the ovary are the most frequent contents of the inguinal hernial sac [1]. Inguinal hernia is more common in infants and children [11]. The reported incidence of its occurrence is 71 % in children under 5 years [12] and 30 % in adolescents or women in the reproductive age group [12] and 2.9 % exclusively in adults [1]. Embryogenic derangements are associated with this condition. The canal of Nuck is obliterated by the eighth week of fetal life. If it remains unobliterated, the ovary and the fallopian tubes may travel through the canal to form a congenital hernial sac. When the ovary and fallopian tubes form the contents of the inguinal hernia sac, they are often associated with anomalies in the development of the genital tract, such as vaginal atresia, bicornuate uterus, and renal anomalies [1, 2, 12, 13]. These patients are treated with reduction of the content, provided there is no ovarian or tubal abnormality, the blood supply is not impaired, and there is no evidence of salpingitis [1, 2]. Kapur et al. [14] suggested that, despite incarceration, the blood supply to the ovary is not usually impaired, and if the ovary is tender, this should be considered as an urgent surgical emergency. The operating surgeon is always in dilemma whether to save a congested and swollen adnexa because if he replaces an infected fallopian tube with a damaged ovary, there are chances of pelvic infection, or if we unnecessarily remove such adnexa, there is a chance of infertility in the future. In our case, we reduced the congested ovary and fallopian tubes as they appeared viable during surgery, and later on, it was confirmed with the help of USG after 4 weeks postoperatively.
The incidence of bladder herniation in patients with inguinal hernia has been estimated at 1 to 3 % by some authors and as high as 10 % by others [15]. Because of the proximity of the bladder to the inguinal and femoral canals, the degree of herniation will vary from a small to a massive protrusion. Mostly, it is asymptomatic and rarely is diagnosed preoperatively [16]. Bladder herniation is mostly associated with direct hernia [17] and rarely with indirect hernias [1, 17]. Mostly, urinary bladder herniations are right-sided (as in our case). When it is small, then it is asymptomatic. As the size of the hernia increases, it becomes symptomatic. Urinary symptoms like dysuria, polyuria, hematuria, nocturia, and reduction of hernia size after micturition were reported [18]. Rarely, it may present with abdominal pain [19]. It is common in males and in older age. Obesity is a predisposing risk factor [1]. When the urinary bladder is incarcerated in indirect inguinal hernia, then the incidence of bladder injury during surgery is quiet high (28.6 %). Postoperative hematuria is an alarming symptom to the surgeon as there is a possibility of bladder injury. So, the operating surgeon faces a dilemma whether to catheterize the patient or not. If catheterized unnecessarily, then there will be chances of catheter infection, and if there is no catheter, he may miss bladder injury. We catheterized our patient and there was no hematuria; so, the catheter was removed on the next day to minimize infection.
Conclusion
Unusual contents of inguinal hernia sac are rare, but surgeons still encounter such possibilities. Atypical contents may pose a surgical dilemma (whether to save or sacrifice the organ) even to an experienced surgeon. In the majority of such cases, the organ found in the hernia sac should be protected. One should be aware of this unusual presentation and its appropriate management to deliver better results.
Contributor Information
Sunder Goyal, Phone: +91-96-75139955, Email: goyal.sunder@yahoo.in.
Snigdha Goyal, Phone: +91-97-11578378, Email: drgoyal4@gmail.com.
References
- 1.Gurer A, Ozdogan M, Ozlem N, Yildirim A, Kula-coglu H, Aydin R. Uncommon content in groin hernia sac. Hernia. 2006;10:152–155. doi: 10.1007/s10029-005-0036-4. [DOI] [PubMed] [Google Scholar]
- 2.Ballas K, Kontoulis TH, Skouras CH, Triantafyl-lou A, Symeonidis N, Pavlidis TH, et al. Unusual findings in inguinal hernia surgery. Report of 6 rare cases. Hippokratia. 2009;13:169–171. [PMC free article] [PubMed] [Google Scholar]
- 3.D’Alia C, Lo Schiavo MG, Tonante A, Taranto F, Gagliano E, Bonanno L, et al. Amyand’s hernia: case report and review of the literature. Hernia. 2003;7:89–91. doi: 10.1007/s10029-002-0098-5. [DOI] [PubMed] [Google Scholar]
- 4.Thomas WEG, Vowles KDJ, Williamson RCN. Appendicitis in external herniae. Ann R Coll Surg Engl. 1982;64:121–122. [PMC free article] [PubMed] [Google Scholar]
- 5.Solecki R, Matyja A, Milanowski W. Amyand’s hernia: a report of 2 cases. Hernia. 2003;7:50–51. doi: 10.1007/s10029-002-0093-x. [DOI] [PubMed] [Google Scholar]
- 6.Abu-Dalu J, Ucra I. Incarcerated inguinal hernia with a perforated appendix and periappendicular abscess. Dis Colon Rectum. 1972;15:464–465. doi: 10.1007/BF02642658. [DOI] [PubMed] [Google Scholar]
- 7.Apostolidis S, Papadopoulos V, Michalopoulos A, Paramythiotis D, Harlaftis N (2005) Amyand’s hernia: a case report and review of literature. The Internet J Surgery 6(1)
- 8.Kwok CM, Su CH, Kwang WK, Chui YC. Amyand’s hernia—a case report and review of literature. Case Rep Gastroenterol. 2007;1:65–70. doi: 10.1159/000107472. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Ranganathan G, Kouchupapy R, Dias S. An approach to the management of Amyand’s hernia and presentation of an interesting case report. Hernia. 2011;15:79–82. doi: 10.1007/s10029-009-0609-8. [DOI] [PubMed] [Google Scholar]
- 10.Psarras K, Lalountas M, Baltatzis M, Pavlidis E, Tsitlakidis A, Symeonidis N, Ballas K, Pavlidis T, Sakantamis A. Amyand’s hernia—a vermiform appendix presenting in an inguinal hernia: a case series J Med Case Rep. 2011;5:463. doi: 10.1186/1752-1947-5-463. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Machado NO, Machado NN. Unusual contents of inguinal hernial sac. An approach to management. Surg Sci. 2011;2:322–325. doi: 10.4236/ss.2011.26068. [DOI] [Google Scholar]
- 12.van Heesewijk HP, Smith FW, Heitbrink MA, Kok FP. Herniation of an ovarian cyst through the inguinal canal: diagnosis with CT. Am J Roentgenol. 1990;154:202–203. doi: 10.2214/ajr.154.1.2104715. [DOI] [PubMed] [Google Scholar]
- 13.Mayer M, Templeton FG. Inguinal ectopia of the ovary and fallopian tube. Review of the literature and report of the case of an infant. Arch Surg. 1941;43:397–408. doi: 10.1001/archsurg.1941.01210150073005. [DOI] [Google Scholar]
- 14.Kapur P, Caty MG, Glick PH. Pediatric hernias and hydrocele. Pediatr Clin North Am. 1998;45:773–789. doi: 10.1016/S0031-3955(05)70044-4. [DOI] [PubMed] [Google Scholar]
- 15.Becker JA. A hernia of the urinary bladder. Radiology. 1965;84:270–273. doi: 10.1148/84.2.270. [DOI] [PubMed] [Google Scholar]
- 16.Oruc MT, Akbulut Z, Ozozan O, Coskun F. Urological findings in inguinal hernia: a case report and review of the literature. Hernia. 2004;8(1):76–79. doi: 10.1007/s10029-003-0157-6. [DOI] [PubMed] [Google Scholar]
- 17.Gomella LG, Spires SM, Burton JM, Ram MD, Flanigan RC. The surgical implications of herniation of the urinary bladder. Arch Surg. 1985;120(8):964–968. doi: 10.1001/archsurg.1985.01390320084018. [DOI] [PubMed] [Google Scholar]
- 18.Gurbulak EK, Gurbulak B, Sahin TT (2010) Amyand’s hernia combined direct inguinal hernia containing urinary bladder: report of a case. The Internet Journal of Surg 24(2)
- 19.Kuo W-Y, Lin T-Y, Lee W-J. Urinary bladder hernia: an unusual presentation of abdominal pain. Emerg Med J. 2010;27:489. doi: 10.1136/emj.2009.074195. [DOI] [PubMed] [Google Scholar]