Abstract
The endothelial lining of the vasculature is exposed to a large variety of biochemical and hemodynamic stimuli with different gradients throughout the vascular network. Adequate adaptation requires endothelial cells to be highly plastic, which is reflected by the remarkable heterogeneity of endothelial cells in tissues and organs. Hemodynamic forces such as fluid shear stress and cyclic strain are strong modulators of the endothelial phenotype and function. Although endothelial plasticity is essential during development and adult physiology, proatherogenic stimuli can induce adverse plasticity which contributes to disease. Endothelial-to-mesenchymal transition (EndMT), the hallmark of endothelial plasticity, was long thought to be restricted to embryonic development but has emerged as a pathologic process in a plethora of diseases. In this perspective we argue how shear stress and cyclic strain can modulate EndMT and discuss how this is reflected in atherosclerosis and pulmonary arterial hypertension.
1. Introduction
Mechanical forces, laminar shear stress (LSS), and cyclic strain (CS) are two major and well-established regulators of vascular development and adaptation (reviewed in [1–3]). Vasculogenesis, which marks the onset of embryonic vascularization, is driven by hypoxia and initiated by the differentiation of endothelial cells from mesodermal angioblasts [4]. Herein, hypoxia inducible factor 1 alpha (HIF1α) induces the expression of vascular endothelial growth factor (VEGFa) which results in endothelial differentiation and proliferation. The endothelial cells derived from the blood islands form a vascular network known as the primitive capillary plexus [5]. This plexus is highly uniform without a clear vascular hierarchy.
With the interconnection of the vascular plexus and major vessels a functional loop is formed and, as the heart begins to beat, the physical flow of fluid is introduced [6]. Arteriogenesis ensues the remodeling of the vessels to accommodate the physical forces associated with the increased pressures and flow. The pulsatile nature of the blood flow generated by the beating heart produces a complex interplay between two distinct mechanical forces, namely, fluid shear stress (FSS), the frictional force exerted by the flow of blood, and cyclic strain (CS), which results from the distensibility of the vessel wall caused by pulsations and increased hydrostatic pressures. Adaptation to these forces, known as angioadaptation, results in a hierarchical vascular tree composed of arteries, arterioles, capillaries, venules, and veins [7].
In the adult vasculature, hemodynamic forces play a major role in the maintenance of vessel homeostasis [8]. The most important intimation for a role of hemodynamic forces in vascular homeostasis is found in the focal nature of most vascular diseases. For example, despite the fact that most risk factors for atherosclerosis development and progression are present at the systemic level, this inflammatory arterial disease preferentially develops in regions which are characterized by disturbed hemodynamic flow, typically encountered at the outer walls of vascular bifurcations and at the inner wall of vascular curvatures [9, 10]. Indeed, disturbances of fluid shear stress levels encountered at these locations are predictors of plaque location [11], associate with the increased mass transport of low-density lipoproteins (LDL) which build up the plaques [12], and are major determinants of plaque transition from stable plaques to high-risk unstable plaques and plaque rupture [13].
In recent years, it has become apparent that the endothelium plays a pivotal role in the development and progression of cardiovascular diseases [14–16]. The endothelial lining of the vasculature is exposed to a large variety of stimuli which require the endothelium to be highly plastic [17], as is reflected by the remarkable heterogeneity of endothelial cells in tissues and organs. Although this endothelial plasticity is essential during homeostasis, during disease, pathological stimuli might induce adverse plasticity which can contribute to disease. Herein, endothelial-mesenchymal transition (EndMT) and its contribution to neointima formation [18–21] is a perfect example.
In this perspective, we focus on how hemodynamic forces, that is, shear stress and cyclic strain, are sensed by the endothelium, how these forces modulate EndMT, and how this is reflected in vascular disease.
2. Endothelial-to-Mesenchymal Transition: The Hallmark of Endothelial Plasticity
Endothelial-to-mesenchymal transition (EndMT) was originally described as an embryonic phenomenon involved in cardiac valve formation [22]. EndMT has mainly been studied in vitro, where it is characterized by the loss of cell-cell adhesions and changes in cell polarity, resulting in a spindle-shaped morphology. Endothelial cell markers such as VE-Cadherin and PECAM-1 are repressed, whilst the expression of mesenchymal cell markers such as α-smooth muscle actin (α-SMA) and calponin is enhanced [23–26]. Functionally, endothelial cells acquire myofibroblast-like characteristics with contractile function, enhanced migratory phenotype, and increased extracellular matrix production [24]. In EndMT, endothelial functions, such as antithrombogenicity and angiogenic sprouting capacity, are lost [23, 24].
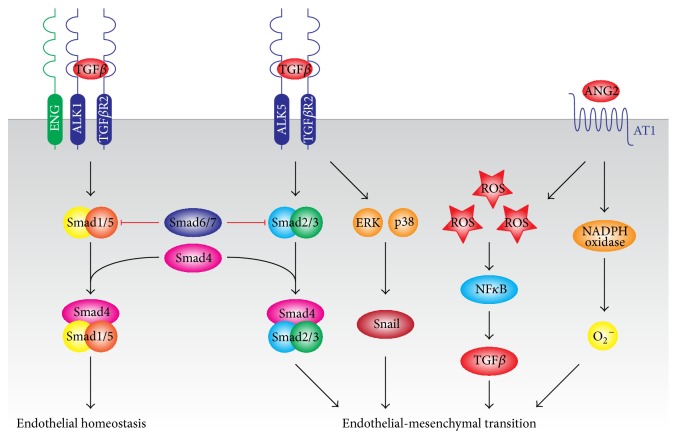
Through extensive studies on EndMT in vitro, we have gained in-depth knowledge of the signaling cascades that regulate EndMT (Figure 1). Many signaling pathways are involved in the induction and progression of EndMT, wherein the transforming growth factor β (TGFβ)/bone morphogenetic protein (BMP) superfamily plays a pivotal role.
Figure 1.
Mechanisms of endothelial-mesenchymal transition. EndMT is induced by TGFβ-dependent and TGFβ-independent mechanisms. Canonically, TGFβ-induced activation of SMAD2/3 induces the expression of mesenchymal genes and repression of endothelial genes. Noncanonically, TGFβ-induced activation of Erk1/2 and p38 MAPK activate the transcription factor Snail which induces mesenchymal differentiation and inhibits VE-Cadherin expression. Inflammatory signals and increased ROS production facilitate EndMT by increasing endogenous TGFβ expression, in an NFκB-dependent manner, creating a feed forward signaling mechanism. AT1 receptor can induce EndMT through activation of NADPH oxidase, resulting in increased ROS production and reduction of eNOS expression and activity.
In endothelial cells, canonical TGFβ signaling occurs through the type II TGFβ receptor (TGFβR2) which activates the type I TGFβ receptor Activin-like kinase (ALK) 5, activating receptor-regulated Smad2/3, and leads to inhibition of cell proliferation and induction of EndMT [27–30]. In contrast, TGFβ and bone morphogenetic proteins (BMP) can also bind the BMP type I receptor, ALK1, which activates receptor-regulated Smad1/5/8 and induces proliferation and inhibits EndMT [27–29]. The common-mediator Smad4 interacts with the receptor-regulated Smads and is required for signaling. The inhibitory Smads 6 and 7 block activation of the receptor-regulated Smads and thus inhibit TGFβ signaling. The balance between ALK1 and ALK5 signaling pathways is partially regulated by an accessory type III TGFβ receptor called endoglin, which stimulates ALK1-induced Smad1/5/8 responses and thus indirectly inhibits ALK5 signaling [29].
Besides canonical TGFβ signaling, TGFβ can induce EndMT noncanonically through the activation of the ERK1/2 and p38 MAPK signaling pathways and the downstream induction of the mesenchymal transcription factor Snail [31, 32] (Figure 1). Furthermore, Notch is known to promote TGFβ-induced EndMT shifting the balance between different ALK1 and ALK5 signaling pathways in favor of ALK5 [33, 34].
Other signaling mechanisms can also induce EndMT, albeit often indirectly involving TGFβ signaling. Proinflammatory molecules, such as IL1β and TNFα, synergize with TGFβ in the induction of EndMT [35–37]. Besides, IL1β and TNFα induce the expression of Snail and Slug, two pivotal transcription factors in EndMT [38–40]. Reactive oxygen species (ROS) are potential stimulators of EndMT (Figure 1) by inducing endogenous TGFβ expression and activating latent TGFβ [41]. TGFβ also stimulates ROS production, resulting in a positive feedback loop [41]. Besides, ROS activates NFκB signaling which acts in synergy with TGFβ in induction of EndMT [36, 42].
The AT1 receptor (angiotensin II receptor type I), a member of the G-protein coupled receptor family, mediates EndMT of human aortic endothelial cells in vitro [43] as well as in cardiac endothelial cells in vivo [44, 45]. Angiotensin II-induced EndMT can be mediated both by release of cytokines such as TGFβ or through changes in the redox status of EC by the activation of NADPH oxidase system [45] which leads to higher superoxide production, NFκB activation [42], and lower NO bioavailability through uncoupling eNOS [46, 47] (Figure 1).
In summary, TGFβ signaling plays a dominant role as inducer of EndMT directly via both canonical and noncanonical signaling pathways. In recent years, it has become evident that EndMT is not restricted to embryogenesis but can also occur in adult life, where it contributes to organ and muscle fibrogenesis [48–52], cancer [53], and atherosclerosis [18–20]. In the following section, we argue how hemodynamic forces can modulate EndMT and how these mechanisms are reflected by vascular disease.
3. Hemodynamic Forces as Modulators of EndMT
3.1. Go with the Flow: Laminar Shear Stress Is a Hemodynamic Force Transduced by the Endothelium
Hemodynamic forces play a pivotal function in the maintenance of the vascular integrity. It is well established that high uniform laminar shear stress (LSS) has atheroprotective effects [54], which is evidenced by the occurrence of endothelial dysfunction [55], aneurysms [56], and atherosclerosis [57–59] at sites where LSS is reduced or worse, absent or disturbed.
A variety of signaling cascades are involved in endothelial mechanotransduction of LSS; however, identifying which pathways are primary or secondary to LSS sensing remains elusive as the initial mechanosensory complexes are not completely identified.
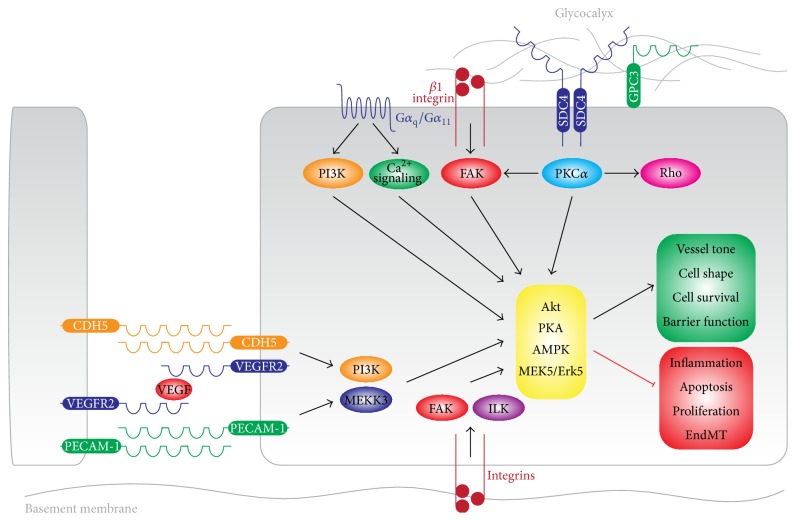
Endothelial cells sense LSS through a number of mechanisms including the endothelial glycocalyx [60–62], growth factor receptors [63, 64], cell-cell adhesion molecules [65, 66], integrins [67], and G-protein-coupled receptors [68–70] (Figure 2). The endothelium is covered by a slimy layer of plasma proteins and glycoproteins, known as the glycocalyx, which is an organized hydrated mesh of negatively charged membranous macromolecules, proteoglycans, and glycosaminoglycans [71]. The proteoglycan core proteins are the membrane-bound glypican and the transmembrane syndecans. Syndecans directly associate with the cytoskeleton [72] and may thus directly transmit mechanical stresses to the nucleus or remote mechanotransducers [73, 74] (Figure 2). Indeed, disruption of the endothelial glycocalyx either genetically or by pharmacological inhibitors of glycocalyx producing enzymes renders the endothelium shear insensitive [60–62]. Although insights into glycocalyx signaling remain elusive, syndecans and glypicans are known to associate with the β1 integrins and mediate the activity of focal adhesion kinase (FAK) through protein kinase C-alpha (PKCα) [61, 62, 67, 73], resulting in the activation of Akt, Rho, and the endothelial nitric oxide synthase (eNOS). Combined, glycocalyx signaling enhances endothelial survival and maintenance of the endothelial barrier (Figure 2).
Figure 2.
Endothelial shear stress sensing. Endothelial cells sense LSS through a number of mechanisms. Shear stress sensing through the endothelial glycocalyx is mediated by the syndecans and glypicans, which activate PKC signaling. Luminal β1-integrins also anchor to the endothelial glycocalyx and activate focal adhesion kinase (FAK). The G-protein-coupled receptors of Gα q/Gα 11 sense shear stress and activate downstream PI3K and Ca2+ signaling. The junctional mechanosensory complex consisting of PECAM-1, VEGFR2, and VE-Cadherin mediates PI3K and MAPK (MEKK3) signaling. Signaling through these mechanosensors culminates in activation of Akt, PKA, AMPK, and MEK5/Erk5 which collectively maintain the endothelial phenotype.
The protein complex consisting of PECAM-1, VEGFR2, and VE-Cadherin is a junctional mechanosensory complex that transduces hemodynamic forces into biochemical responses [75]. In this mechanosensory complex, VE-Cadherin functions as an initial adaptor which initiates the formation of the signaling complex, whereas PECAM-1 can directly transduce mechanical forces to the cytoskeleton [65]. VEGFR2, in association with VEGFa, initiates bidirectional activation of PI3K and MEKK3 which cause the downstream activation of Akt and MEK5/Erk5 signaling (Figure 2). Collectively, signaling through this junctional complex results in the activation of a number of transcription factors [63, 64] described below and loss of any one of its components ameliorates the endothelial response to LSS [2].
Additionally, the membrane bound G-protein-coupled receptors of type Gα q/Gα 11 transmit mechanical forces in part through the activation of PI3K and intracellular calcium signaling [76–78]. Activation of Gα q/Gα 11 proteins results in the activation of Akt and increased activation of eNOS (Figure 2).
Thus, the endothelium is highly sensitive to laminar shear stress and endothelial mechanosensing and transduction is achieved through a variety of cell-matrix and cell-cell receptor complexes. Endothelial mechanotransduction by these protein complexes culminates in the activation of the Akt, PKA, AMPK, and MEK5/Erk5 signaling cascades that ensure the maintenance of endothelial homeostasis and inhibit EndMT (Figure 2).
3.2. The Atheroprotective Effects of Laminar Shear Stress and the Inhibition of EndMT
It is well established that the extracellular signal-related kinase (Erk) 5, also known as MAPK7 and big-mitogen kinase-1 (BMK-1), has atheroprotective effects [54, 79, 80]. Erk5 is the only mitogen-activated protein kinase (MAPK) which is continuously activated by uniform LSS in vitro [18, 81] and several lines of evidence suggest that Erk5 transmits its atheroprotective effects through the activation of the transcription factors of the Krüppel-like factor (KLF) family [18, 82–84].
First, Krüppel-like factor 2 (KLF2) is an important shear stress-activated transcription factor, which exerts anti-inflammatory effects through inhibition of nuclear factor kappa B (NFκB) activation [85] and anticoagulant effects by induction of thrombomodulin and repression of tissue factor and plasminogen activator inhibitor (PAI-1) [86]. Besides, KLF2 regulates antioxidative signaling [87], induces quiescence [88], and inhibits VEGFa-induced angiogenesis, barrier disruption, and cell proliferation [89].
Second, KLF2 inhibits the phosphorylation and nuclear translocation of Smad2 through induction of inhibitory Smad7 [90]. Moreover, KLF2 also suppresses the activator protein 1 (AP-1), an important cofactor for TGFβ-dependent transcription [90]. Thus, KLF2 might directly inhibit EndMT by suppressing TGFβ signaling.
The expression of KLF4, a close family member of KLF2, is similarly induced upon exposure to LSS [91, 92]. Significant conservation exists between KLF2 and KLF4 [82, 93]. In fact, almost 60% of MEK5 regulated genes are coregulated by KLF2 and KLF4 [93]. Similar to KLF2, KLF4 exerts anti-inflammatory effects through suppression of NFκB activity [94]. KLF4-specific targets include forkhead box O1 (FOXO1) and vascular endothelial growth factor (VEGF) [93], both of which are known to inhibit TGFβ signaling [48, 95].
Third, KLF4 plays an important role in cell-cycle regulation and differentiation. KLF4 increases the expression of several inhibitors of proliferation, while genes that promote proliferation are repressed [88, 96, 97]. As such, KLF4 might partially be responsible for the quiescence observed in endothelial cells exposed to high levels of uniform LSS.
Fourth, KLF4 is known to suppress mesenchymal differentiation through several mechanisms. KLF4 inhibits myocardin expression, a potent coactivator of serum response factor (SRF) [98, 99], and prevents SRF/myocardin from associating with mesenchymal gene promoters [100]. KLF4 can also directly bind the TGFβ control element (TCE) in the promoter of mesenchymal genes, preventing transcription [101]. Furthermore, KLF4 interacts with Smad3, inhibiting its binding to Smad binding elements (SBE) and preventing transcription of mesenchymal genes [102]. Interestingly, KLF4 is also known to transcriptionally regulate VE-Cadherin [103]. Thus KLF4 might inhibit EndMT via multiple mechanisms.
Last, KLF2 and KLF4 can inhibit EndMT through the inhibition of ROS formation by eNOS-induced stimulation of superoxide dismutase (SOD), scavenging of ROS through NO production [104, 105], and facilitation of mitochondrial biogenesis [106].
In addition to the atheroprotective effects mediated by the KLFs, LSS induces the expression of inhibitor of DNA binding/inhibitor of differentiation proteins 1–3 (Id1–3) [107]. These dominant-negative regulators of basic helix-loop-helix DNA-binding transcriptional regulators play a role in lineage commitment, cell cycle control, and cell differentiation [108]. Id2 and Id3 repress Smad2-mediated gene transcription [109] and ectopic expression of Id2 and Id3 inhibits EMT [110]. Besides, Id3 is downregulated during EndMT [24] and Id1 has been shown to promote survival of endothelial cells and preserve the integrity of lung microvascular endothelial cells [111].
In summary, LSS plays a major role in endothelial homeostasis, wherein mechanical stimuli are transduced into biochemical signals which culminate in the expression of the KLF transcription factors. KLF2 and KLF4 govern endothelial thrombogenicity, inflammatory phenotype, permeability, proliferation, and redox state through a variety of mechanisms. In addition, the KLF transcription factors inhibit mesenchymal gene expression. Hence, the LSS-induced expression of the KLF transcription factors is pivotal in the inhibition of EndMT.
3.3. Disturbed Shear Stress: Inducer or Permitter of EndMT?
In contrast to the beneficial effects of LSS, oscillatory or nonuniform shear stress, further referred to as disturbed shear stress (DSS), has opposing effects on endothelial homeostasis; that is, DSS causes EC dysfunction. DSS is known to induce endothelial inflammatory activation [112–114]. DSS reduces the endothelial antithrombogenicity and increases the formation of reactive oxygen species (ROS), which further adds to the inflammatory activation and profibrotic signaling. During arteriogenesis, the screw-like curvatures of the collaterals convert LSS to DSS, which stimulates endothelial proliferation and MCP-1 activation, resulting in the recruitment of monocytes that are essential for remodeling of the vascular structure [115]. These mechanisms are reiterated during vascular pathology. Areas exposed to DSS are characterized by a high influx of leukocytes, which generates a microenvironment with excessive ROS production, high levels of TGFβ, and inflammatory mediators such as IL1β, which all favor EndMT [36].
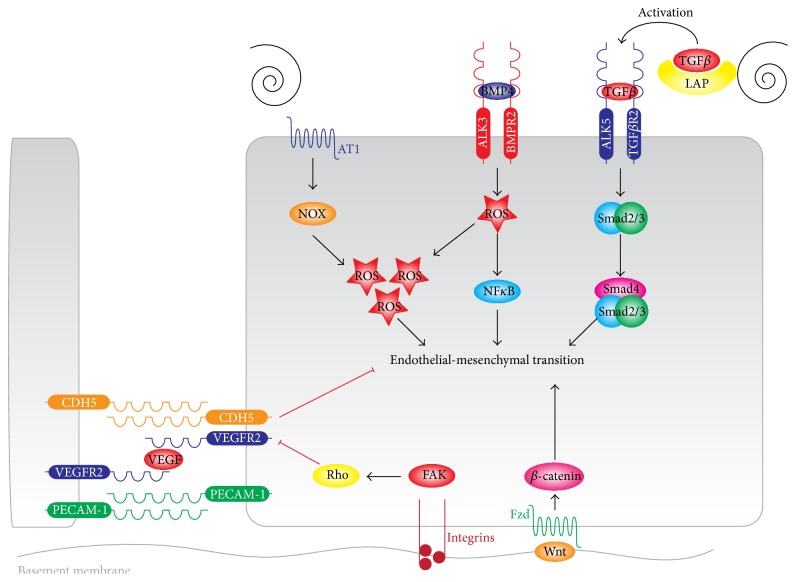
DSS induces ROS formation through several mechanisms. DSS leads to increased nicotinamide adenine dinucleotide phosphate (NADPH) oxidase (NOX) activity (Figure 4) which results in ROS production [116]. NADPH oxidase activity can induce xanthine oxidoreductase (XO), an important source of ROS [117]. Next, expression of NOX4, a subunit of vascular NADPH oxidase, is increased in response to DSS resulting in increased LDL oxidation [118]. Adding to this, intracellular glutathione, a powerful antioxidant, is greatly decreased by DSS [119].
Figure 4.
Disturbed shear stress and high cyclic strain signaling in endothelial-mesenchymal transition. Disturbed shear stress induces EndMT through several mechanisms. Disturbed shear stress activates latent TGFβ by liberating it from LAP, after which TGFβ can induce Smad2/3 signaling. Disturbed shear stress induces the expression of BMP4 which causes ROS formation and the activity of NFκB. Lastly, disturbed shear stress induces NOX and XO activity resulting in the generation of ROS. All these signaling intermediates culminate in EndMT. Increased cyclic strain (>10%) induces the FAK-dependent activation of Rho-kinases. Rho activity causes the translocation of VE-Cadherin from the cell membrane into cytoplasmic vesicles and causes a reduction in endothelial cell-cell contacts. Cyclic strain-dependent Wnt-β-catenin activity induces EndMT in part by the induction of Snail and Slug and the further activation of Rho activity.
DSS can also induce EndMT through direct activation of TGFβ signaling (Figure 4). BMP4 is a potent inducer of EndMT [48], expression of which is inhibited by LSS [120]. In contrast, exposure to DSS induces BMP4 [121] expression in endothelial cells and contributes to ROS production and NFκB activation [122]. Additionally, DSS induces TGFβ expression and activation in an NFκB-dependent manner [123].
Taken together, high LSS can inhibit EndMT via multiple mechanisms, either directly or indirectly interfering with TGFβ signaling. DSS suppresses these protective mechanisms making endothelial cells more prone to microenvironmental cues which favor EndMT. Besides, DSS can induce EndMT directly through induction of BMP4 or via increased ROS production. Indeed, exposing aortic endothelial cells (which normally are exposed to LSS) to DSS by aortic banding efficiently induces EndMT in vivo in the absence of other stimuli [18]. Therefore, DSS acts both as a permitter and inducer of EndMT by either suppressing protective signaling or by directly inducing the transition process.
3.4. Cyclic Strain
Cyclic strain (CS) is defined as the repetitive mechanical deformation of the vessel during the cardiac cycle. Vascular CS can vary from 2 to 20% in vivo as a result of arterial wall expansion and contraction in response to pulsatile pressure changes [124]. CS plays an important role in the modulation of cell proliferation, migration, apoptosis, morphological changes, and alignment through the production of vasoactive substances such as nitric oxide (NO) [125], endothelin (ET-1), [126] and antioxidants [127, 128].
Physiologically, the level of CS is around 6–10% but this strongly varies throughout the vasculature. CS can increase with hypertension and artificial pulmonary ventilation (10% to 20%) and decrease with ageing due to vascular stiffening or acutely due to sepsis (2%–6%) [129]. CS levels up to 10% do not induce endothelial injury [130] but inhibit endothelial apoptosis through activation of PI3-kinase and Akt. In contrast, CS levels of over 15% induce apoptosis [131].
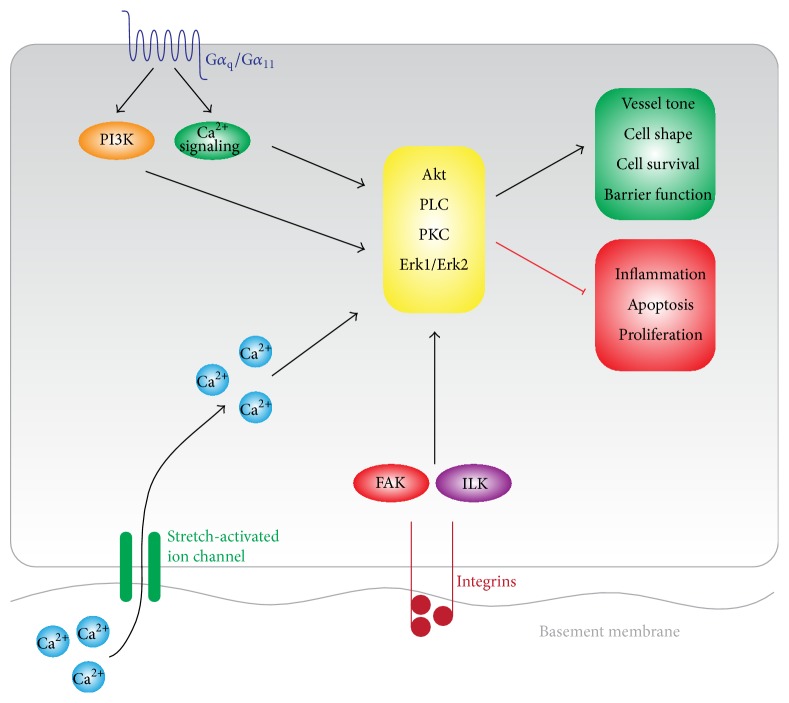
Endothelial cells sense CS through a number of mechanisms involving stretch-activated ion channels, integrins, and G-protein-coupled receptors. Stretch-activated ion channels play a pivotal role in CS sensing. Stretching of endothelial cells opens the ion channels allowing extracellular Ca2+ to enter the cell, thereby activating downstream phospholipase C (PLC) signaling [132] (Figure 3). Additionally, the cell-matrix adhesion families of integrins mediate CS signaling in endothelial cells by the activation of focal adhesion kinase (FAK) and integrin-linked kinase (ILK) complexes that result in the downstream activation of the small GTPase family Rho, PI3K, and Akt (Figure 3). Combined, these signals result in changes in endothelial morphology and the regulation of cell survival and cytokine production. However, to what extent CS induces these effects and the relation between the magnitude of CS and the endothelial integrin-mediated response remain elusive [133, 134]. The heterotrimeric Gα q/α 11 subunit of the G protein family is rapidly activated by CS and the intensity is related to the magnitude of the strain applied [135]. AT1 receptors bind and signal through all members of the G-protein family and are activated by mechanical forces in vitro and in vivo, independently of angiotensin II [136, 137].
Figure 3.
Endothelial cyclic strain sensing. Endothelial cells sense CS through a number of mechanisms. Stretch-sensitive ion channels undergo a conformational change during stretch which opens up the channel and induces Ca2+ flux from the extracellular space into the endothelial cell. Basal β1-integrins anchor to the endothelial basement membrane and activate focal adhesion kinase (FAK) and the integrin-linked kinases (ILK). The G-protein-coupled receptors of Gα q/Gα 11 sense CS and activate downstream PI3K and Ca2+ signaling. Signaling through these stretch sensors culminates in activation of Akt, PKC, PLC, and Erk1/2 which collectively maintain the endothelial phenotype.
Stimulation of the CS sensors causes downstream activation of small GTPases that are essential for the biochemical transduction of the mechanical stimulus. The most extensively characterized members are Rho, Rac, and Cdc42, which have distinct effects on actin cytoskeleton, cell adhesion, and cell motility [138]. Rho kinase induces assembly of stress fibers and focal adhesions and Rac plays an important role in junction formation and integrity of the endothelial barrier [139]. The activity of the Rho pathway determines the direction and extent of stretch-induced stress fiber orientation in endothelial cells. This demonstrates on one hand that physically stressing a cell determines Rho activity (in a linear fashion) and that Rho activation directly correlates with physical shape shifting of cells through cytoskeletal reorganization [140, 141]. Also, preconditioning of endothelial cells at 18% CS enhanced the effects of prothrombotic stimuli to induce permeability of the endothelial monolayer, while 5% CS prevents thrombin-induced disruptive response and accelerates barrier recovery [142]. Corroboratively, CS in the 10–20% range causes activation of Rho and a reduction of basal Rac activity (Figure 4). In contrast, 5% stretch maintains the balance between Rho and Rac activity [143, 144]. These studies suggest a major role for amplitude-dependent CS in regulation of the endothelial barrier.
3.5. Cyclic Strain Sets the Stage for EndMT
Enhanced CS (>10%) potentiates EndMT of valvular endothelial cells in a manner dependent on both strain magnitude and direction [145]. Modest CS (10%) induces EndMT via amplified TGFβ1 signaling, while high CS (20%) activates wnt/β-catenin signaling [145], a known inducer of EndMT in aortic endothelial cells [146, 147]. Both intensities decreased VEGFa signaling, a known inhibitor of EndMT [48]. Notably, mechanical stretch induces epithelial-to-mesenchymal transition (EMT) of renal tubular epithelial cells by induction of TGFβ1 mRNA expression and activation of latent TGFβ [146].
VE-Cadherin is a central component of endothelial adherens junctions. VE-Cadherin is a transmembrane glycoprotein that complexes via its cytoplasmic tail to β-catenin, which links VE-Cadherin to the cortical actin cytoskeleton [148]. The cellular localization of VE-Cadherin is dependent on the small GTPases Rho and Rac that when appropriately balanced stabilize VE-Cadherin at the cell membrane [149].
EndMT results in a loss of barrier function, that is, increased permeability, which correlates with loss of VE-Cadherin at the cell surface (Figure 4). In response to the increase of Rho activity by high levels of CS [141], VE-Cadherin is translocated from the membrane into the cytoplasm. The concomitant loss of complexed β-catenin and its nuclear translocation might therefore be a secondary mediator of EndMT. Indeed, Rho activity plays a pivotal role in TGFβ1-induced EMT through induction of cytoskeleton remodeling and activation of the smooth muscle actin (SMA) promoter [150] and β-catenin/Rho signaling efficiently induces EndMT [32, 147, 151, 152]. This implies that supraphysiological CS is a direct inducer of EndMT (Figure 4).
Vascular remodeling is accompanied by changes in extracellular matrix (ECM) turnover, which result from alterations in the balance of matrix deposition and its proteolytic degradation. Matrix metalloproteinases (MMPs) represent the main group of proteases involved in remodeling of ECM [153]. An imbalance between the activity of MMPs and their tissue inhibitors (TIMPs) contributes to adverse remodeling. MMP2 induces matrix degradation during vascular remodeling [154] and TGFβ2-induced EndMT is characterized by a marked increase in MMP2 [151]. Interestingly, biaxial CS induces endothelial MMP2 expression and regulates its secretion and activity [130, 155]. Additionally, in a model for intimal hyperplasia, stretched human saphenous vein grafts increased expression and activity of MMP2 throughout the vascular wall [156]. Taken together, cyclic strain induces MMP2 expression in endothelial cells thereby facilitating the migratory and proliferative phenotype acquired through EndMT.
Clearly, cyclic strain is not an ON/OFF switch of pathological vascular remodeling and EndMT, illustrated by the fact that endothelial cells react to CS in an amplitude-dependent manner. Stretching of endothelial cells may exert beneficial effects in physiological conditions (uniaxial, 5%–10%) but might induce advert effect during pathologies (strains <6% or >10%) such as hypertension. Reduced vascular distensibility is a common feature of vascular aging and is correlated with an increased risk of cardiovascular disease [157]. Loss of vessel wall compliance with age or increased CS during disease may blunt or aggravate the endothelial response to mechanical strain and induce EndMT. Whether and how this might contribute to pathophysiology remains to be determined.
3.6. Hemodynamic Forces Act in Concert
It should be emphasized that, for clarity reasons, LSS and CS were discussed as separate entities, yet they act in concert in vivo. For technical reasons, few studies have integrated both forces. However, fragmented evidence indicates that synchronicity between LSS and CS is important for vascular homeostasis, showing that asynchronicity between these hemodynamic forces induces a proatherogenic response through reduced expression of eNOS and cyclooxygenase-2 and increased expression of endothelin-1 and NFκB [158–160]. These findings illustrate the importance of studying both entities in combination.
4. Hemodynamic Forces, EndMT, and Vascular Disease
EndMT contributes to vascular pathologies such as cardiac fibrosis [44, 50, 161], atherosclerosis [18, 20, 79], vascular restenosis [162], and the remodeling observed with pulmonary arterial hypertension [26]. As stated previously, the focal nature of these diseases, despite their systemic or genetic risk factors, intimates a pivotal role for hemodynamic forces in modulating these pathologies.
In atherosclerosis, levels of activated Smad2 are elevated especially at areas exposed to DSS [163]. Also, endothelial BMP4 expression is elevated at the site of atheroma formation and in calcifed atherosclerotic plaques, characterized by DSS [164], where also increased levels of ROS production are found [165], which all favor EndMT induction and progression. Indeed, at these sites, EndMT contributes to intimal hyperplasia and atherosclerosis development [18, 20].
In patients with pulmonary arterial hypertension (PAH), elevations in pulmonary venous pressure or long-term increases in blood flow such as those produced by intracardiac shunts result in increased hemodynamic loads and cause structural changes of the pulmonary vasculature. The remodeling response is characterized by endothelial dysfunction, intimal hyperplasia, muscularization of small peripheral vessels, and wall thickening in proximal vessels [166]. The increased hemodynamic load results in increased CS and DSS originating from flow reversal in the pulmonary trunk due to the curved path of the blood flow and dilatation of the pulmonary artery [167]. Pulmonary artery endothelial cells from patients with PAH display a hyperproliferative, apoptosis-resistant phenotype [168] concomitant with EndMT [24]. Interestingly, expression of the Early growth response protein 1 (Egr-1) is elevated in experimental flow-associated PAH [169, 170] and in the vessels of PAH patients with media hypertrophy and neointimal lesions, including plexiform lesions [169]. Egr-1 induces the expression of Snail and Slug, two important mediators of EndMT [171–173], which argues for a definite role of EndMT in the pathogenesis of PAH, as was recently evidenced in human PAH and in experimental models for PAH [19, 174, 175].
Besides, certain patients with familial PAH have mutations of the bone morphogenetic protein (BMP) receptor type II (BMPR2) gene or Activin-like kinase 1 (ALK1) gene [176, 177]. Under normal conditions, these receptors can stimulate Smad1/5/8 signaling in endothelial cells which inhibits EndMT [27, 28, 178]. Hence, impaired BMPR2 or ALK1 signaling renders the pulmonary endothelial cells from these patients more prone to EndMT. BMPR2 deficient rats show spontaneous pulmonary vascular remodeling with enhanced expression of Twist-1, an inducer of EndMT [175]. Corroboratively, adenoviral BMPR2 gene delivery to the pulmonary vascular endothelium in experimental models of PAH reduces the vascular remodeling [179].
5. Conclusion
In conclusion, hemodynamic forces clearly modulate vascular homeostasis and endothelial plasticity. Exposure of endothelial cells to proper amplitudes of LSS and CS safeguard the endothelial integrity through a variety of signaling cascades. Deviations in these hemodynamic forces, both by ageing or pathology, results in adverse endothelial plasticity and culminates in EndMT. Current advances on endothelial mechanotransduction can provide us with many new insights into the regulation of endothelial plasticity.
Acknowledgments
The authors gratefully acknowledge support from the Groningen University Institute for Drug Development and Exploration (GUIDE; to Guido Krenning, Jan-Renier A. J. Moonen, and Martin C. Harmsen), the Netherlands Organization for Health Research and Development (#916.11.022 to Guido Krenning), the Netherlands Heart Foundation (#2013T116 to Jan-Renier A. J. Moonen), the Netherlands CardioVascular Research Initiative, the Dutch Heart Foundation, Dutch Federation of University Medical Centers, the Netherlands Organisation for Health Research and Development, the Royal Netherlands Academy of Sciences (CVON #2012-08, to Jan-Renier A. J. Moonen), the Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP-2013/17368-0, to José E. Krieger), the Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq-401749/2012-6, to José E. Krieger), and the Science Without Borders (Ciência sem fronteiras) program of the Brazilian Federal Government (to Valerio G. Barauna, Martin C. Harmsen, and José E. Krieger).
Conflict of Interests
The authors declare that there is no conflict of interests regarding the publication of this paper.
Authors' Contribution
Guido Krenning and Valerio G. Barauna contributed equally to this work.
References
- 1.García-Cardeña G., Gimbrone M. A., Jr. Biomechanical modulation of endothelial phenotype: implications for health and disease. In: Moncada S., Higgs A., editors. The Vascular Endothelium II. 176/II. Berlin, Germany: Springer; 2006. pp. 79–95. (Handbook of Experimental Pharmacology). [DOI] [PubMed] [Google Scholar]
- 2.Hahn C., Schwartz M. A. Mechanotransduction in vascular physiology and atherogenesis. Nature Reviews Molecular Cell Biology. 2009;10(1):53–62. doi: 10.1038/nrm2596. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Taber L. A. Biomechanics of cardiovascular development. Annual Review of Biomedical Engineering. 2001;3(1):1–25. doi: 10.1146/annurev.bioeng.3.1.1. [DOI] [PubMed] [Google Scholar]
- 4.Ferguson J. E., III, Kelley R. W., Patterson C. Mechanisms of endothelial differentiation in embryonic vasculogenesis. Arteriosclerosis, Thrombosis, and Vascular Biology. 2005;25(11):2246–2254. doi: 10.1161/01.ATV.0000183609.55154.44. [DOI] [PubMed] [Google Scholar]
- 5.Risau W., Flamme I. Vasculogenesis. Annual Review of Cell and Developmental Biology. 1995;11(1):73–91. doi: 10.1146/annurev.cb.11.110195.000445. [DOI] [PubMed] [Google Scholar]
- 6.Jones E. A. V., le Noble F., Eichmann A. What determines blood vessel structure? Genetic prespecification vs. Hemodynamics. Physiology. 2006;21(6):388–395. doi: 10.1152/physiol.00020.2006. [DOI] [PubMed] [Google Scholar]
- 7.Zakrzewicz A., Secomb T. W., Pries A. R. Angioadaptation: keeping the vascular system in shape. News in Physiological Sciences. 2002;17(5):197–201. doi: 10.1152/nips.01395.2001. [DOI] [PubMed] [Google Scholar]
- 8.Chien S. Mechanotransduction and endothelial cell homeostasis: the wisdom of the cell. American Journal of Physiology—Heart and Circulatory Physiology. 2007;292(3):H1209–H1224. doi: 10.1152/ajpheart.01047.2006. [DOI] [PubMed] [Google Scholar]
- 9.Friedman M. H., Bargeron C. B., Deters O. J., Hutchins G. M., Mark F. F. Correlation between wall shear and intimal thickness at a coronary artery branch. Atherosclerosis. 1987;68(1-2):27–33. doi: 10.1016/0021-9150(87)90090-6. [DOI] [PubMed] [Google Scholar]
- 10.Ku D. N., Giddens D. P., Zarins C. K., Glagov S. Pulsatile flow and atherosclerosis in the human carotid bifurcation. Positive correlation between plaque location and low oscillating shear stress. Arteriosclerosis. 1985;5(3):293–302. doi: 10.1161/01.atv.5.3.293. [DOI] [PubMed] [Google Scholar]
- 11.Antoniadis A. P., Giannopoulos A. A., Wentzel J. J., et al. Impact of local flow haemodynamics on atherosclerosis in coronary artery bifurcations. EuroIntervention. 2015;11(supplement):V18–V22. doi: 10.4244/eijv11sva4. [DOI] [PubMed] [Google Scholar]
- 12.Kim S., Giddens D. P. Mass transport of low density lipoprotein in reconstructed hemodynamic environments of human carotid arteries: the role of volume and solute flux through the endothelium. Journal of Biomechanical Engineering. 2015;137(4) doi: 10.1115/1.4028969.041007 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Koskinas K. C., Chatzizisisa Y. S., Baker A. B., Edelman E. R., Stone P. H., Feldman C. L. The role of low endothelial shear stress in the conversion of atherosclerotic lesions from stable to unstable plaque. Current Opinion in Cardiology. 2009;24(6):580–590. doi: 10.1097/HCO.0b013e328331630b. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Hirase T., Node K. Endothelial dysfunction as a cellular mechanism for vascular failure. American Journal of Physiology—Heart and Circulatory Physiology. 2012;302(3):H499–H505. doi: 10.1152/ajpheart.00325.2011. [DOI] [PubMed] [Google Scholar]
- 15.Mudau M., Genis A., Lochner A., Strijdom H. Endothelial dysfunction: the early predictor of atherosclerosis. Cardiovascular Journal of Africa. 2012;23(4):222–231. doi: 10.5830/cvja-2011-068. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Sena C. M., Pereira A. M., Seiça R. Endothelial dysfunction—a major mediator of diabetic vascular disease. Biochimica et Biophysica Acta (BBA)—Molecular Basis of Disease. 2013;1832(12):2216–2231. doi: 10.1016/j.bbadis.2013.08.006. [DOI] [PubMed] [Google Scholar]
- 17.Moonen J.-R. A. J., Harmsen M. C., Krenning G. Cellular plasticity: the good, the bad, and the ugly? Microenvironmental influences on progenitor cell therapy. Canadian Journal of Physiology and Pharmacology. 2012;90(3):275–285. doi: 10.1139/y11-107. [DOI] [PubMed] [Google Scholar]
- 18.Moonen J. A., Lee E. S., Schmidt M., et al. Endothelial-to-mesenchymal transition contributes to fibro-proliferative vascular disease and is modulated by fluid shear stress. Cardiovascular Research. 2015;108(3):377–386. doi: 10.1093/cvr/cvv175. [DOI] [PubMed] [Google Scholar]
- 19.Qiao L., Nishimura T., Shi L., et al. Endothelial fate mapping in mice with pulmonary hypertension. Circulation. 2014;129(6):692–703. doi: 10.1161/CIRCULATIONAHA.113.003734. [DOI] [PubMed] [Google Scholar]
- 20.Yao Y., Jumabay M., Ly A., Radparvar M., Cubberly M. R., Boström K. I. A role for the endothelium in vascular calcification. Circulation Research. 2013;113(5):495–504. doi: 10.1161/circresaha.113.301792. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Cooley B. C., Nevado J., Mellad J., Cooley B. C., et al. Tgf-β signaling mediates endothelial-to-mesenchymal transition (endmt) during vein graft remodeling. Science Translational Medicine. 2014;6(227) doi: 10.1126/scitranslmed.3006927.227ra34 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Markwald R. R., Fitzharris T. P., Manasek F. J. Structural development of endocardial cushions. American Journal of Anatomy. 1977;148(1):85–119. doi: 10.1002/aja.1001480108. [DOI] [PubMed] [Google Scholar]
- 23.Krenning G., Moonen J.-R. A. J., van Luyn M. J. A., Harmsen M. C. Vascular smooth muscle cells for use in vascular tissue engineering obtained by endothelial-to-mesenchymal transdifferentiation (EnMT) on collagen matrices. Biomaterials. 2008;29(27):3703–3711. doi: 10.1016/j.biomaterials.2008.05.034. [DOI] [PubMed] [Google Scholar]
- 24.Moonen J.-R. A. J., Krenning G., Brinker M. G. L., Koerts J. A., Van Luyn M. J. A., Harmsen M. C. Endothelial progenitor cells give rise to pro-angiogenic smooth muscle-like progeny. Cardiovascular Research. 2010;86(3):506–515. doi: 10.1093/cvr/cvq012. [DOI] [PubMed] [Google Scholar]
- 25.Frid M. G., Kale V. A., Stenmark K. R. Mature vascular endothelium can give rise to smooth muscle cells via endothelial-mesenchymal transdifferentiation: In vitro analysis. Circulation Research. 2002;90(11):1189–1196. doi: 10.1161/01.RES.0000021432.70309.28. [DOI] [PubMed] [Google Scholar]
- 26.Arciniegas E., Frid M. G., Douglas I. S., Stenmark K. R. Perspectives on endothelial-to-mesenchymal transition: potential contribution to vascular remodeling in chronic pulmonary hypertension. American Journal of Physiology—Lung Cellular and Molecular Physiology. 2007;293(1):L1–L8. doi: 10.1152/ajplung.00378.2006. [DOI] [PubMed] [Google Scholar]
- 27.Goumans M.-J., Valdimarsdottir G., Itoh S., et al. Activin receptor-like kinase (ALK)1 is an antagonistic mediator of lateral TGFβ/ALK5 signaling. Molecular Cell. 2003;12(4):817–828. doi: 10.1016/s1097-2765(03)00386-1. [DOI] [PubMed] [Google Scholar]
- 28.Goumans M.-J., Valdimarsdottir G., Itoh S., Rosendahl A., Sideras P., Ten Dijke P. Balancing the activation state of the endothelium via two distinct TGF-β type I receptors. The EMBO Journal. 2002;21(7):1743–1753. doi: 10.1093/emboj/21.7.1743. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Lebrin F., Goumans M.-J., Jonker L., et al. Endoglin promotes endothelial cell proliferation and TGF-β/ALK1 signal transduction. The EMBO Journal. 2004;23(20):4018–4028. doi: 10.1038/sj.emboj.7600386. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Díez M., Musri M. M., Ferrer E., Barberá J. A., Peinado V. I. Endothelial progenitor cells undergo an endothelial-to-mesenchymal transition-like process mediated by TGFβRI. Cardiovascular Research. 2010;88(3):502–511. doi: 10.1093/cvr/cvq236. [DOI] [PubMed] [Google Scholar]
- 31.Medici D., Potenta S., Kalluri R. Transforming growth factor-β2 promotes Snail-mediated endothelial—mesenchymal transition through convergence of Smad-dependent and Smad-independent signalling. Biochemical Journal. 2011;437(3):515–520. doi: 10.1042/bj20101500. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Liebner S., Cattelino A., Gallini R., et al. β-catenin is required for endothelial-mesenchymal transformation during heart cushion development in the mouse. Journal of Cell Biology. 2004;166(3):359–367. doi: 10.1083/jcb.200403050. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Fu Y. X., Chang A., Chang L., et al. Differential regulation of transforming growth factor beta signaling pathways by notch in human endothelial cells. The Journal of Biological Chemistry. 2009;284(29):19452–19462. doi: 10.1074/jbc.m109.011833. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Timmerman L. A., Grego-Bessa J., Raya A., et al. Notch promotes epithelial-mesenchymal transition during cardiac development and oncogenic transformation. Genes & Development. 2004;18(1):99–115. doi: 10.1101/gad.276304. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Maleszewska M., Gjaltema R. A., Krenning G., Harmsen M. C. Enhancer of zeste homolog-2 (EZH2) methyltransferase regulates transgelin/smooth muscle-22 alpha expression in endothelial cells in response to interleukin-1 beta and transforming growth factor-beta 2. Cellular Signalling. 2015;27(8):1589–1596. doi: 10.1016/j.cellsig.2015.04.008. [DOI] [PubMed] [Google Scholar]
- 36.Maleszewska M., Moonen J.-R. A. J., Huijkman N., van de Sluis B., Krenning G., Harmsen M. C. IL-1β and TGFβ2 synergistically induce endothelial to mesenchymal transition in an NFκB-dependent manner. Immunobiology. 2013;218(4):443–454. doi: 10.1016/j.imbio.2012.05.026. [DOI] [PubMed] [Google Scholar]
- 37.Rieder F., Kessler S. P., West G. A., et al. Inflammation-induced endothelial-to-mesenchymal transition: a novel mechanism of intestinal fibrosis. American Journal of Pathology. 2011;179(5):2660–2673. doi: 10.1016/j.ajpath.2011.07.042. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Wu Y., Deng J., Rychahou P. G., Qiu S., Evers B. M., Zhou B. P. Stabilization of snail by NF-κB is required for inflammation-induced cell migration and invasion. Cancer Cell. 2009;15(5):416–428. doi: 10.1016/j.ccr.2009.03.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Storci G., Sansone P., Mari S., et al. TNFalpha up-regulates SLUG via the NF-kappaB/HIF1alpha axis, which imparts breast cancer cells with a stem cell-like phenotype. Journal of Cellular Physiology. 2010;225(3):682–691. doi: 10.1002/jcp.22264. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Mahler G. J., Farrar E. J., Butcher J. T. Inflammatory cytokines promote mesenchymal transformation in embryonic and adult valve endothelial cells. Arteriosclerosis, Thrombosis, and Vascular Biology. 2013;33(1):121–130. doi: 10.1161/ATVBAHA.112.300504. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Liu R.-M., Gaston Pravia K. A. Oxidative stress and glutathione in TGF-β-mediated fibrogenesis. Free Radical Biology and Medicine. 2010;48(1):1–15. doi: 10.1016/j.freeradbiomed.2009.09.026. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Gloire G., Legrand-Poels S., Piette J. NF-κB activation by reactive oxygen species: fifteen years later. Biochemical Pharmacology. 2006;72(11):1493–1505. doi: 10.1016/j.bcp.2006.04.011. [DOI] [PubMed] [Google Scholar]
- 43.Tang R., Li Q., Lv L., et al. Angiotensin II mediates the high-glucose-induced endothelial-to-mesenchymal transition in human aortic endothelial cells. Cardiovascular Diabetology. 2010;9, article 31 doi: 10.1186/1475-2840-9-31. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Tang R.-N., Lv L.-L., Zhang J.-D., et al. Effects of angiotensin II receptor blocker on myocardial endothelial-to-mesenchymal transition in diabetic rats. International Journal of Cardiology. 2013;162(2):92–99. doi: 10.1016/j.ijcard.2011.06.052. [DOI] [PubMed] [Google Scholar]
- 45.Murdoch C. E., Chaubey S., Zeng L., et al. Endothelial NADPH oxidase-2 promotes interstitial cardiac fibrosis and diastolic dysfunction through proinflammatory effects and endothelial-mesenchymal transition. Journal of the American College of Cardiology. 2014;63(24):2734–2741. doi: 10.1016/j.jacc.2014.02.572. [DOI] [PubMed] [Google Scholar]
- 46.de Cavanagh E. M. V., Inserra F., Ferder L. Angiotensin II blockade: a strategy to slow ageing by protecting mitochondria? Cardiovascular Research. 2011;89(1):31–40. doi: 10.1093/cvr/cvq285. [DOI] [PubMed] [Google Scholar]
- 47.Zhang Q., Malik P., Pandey D., et al. Paradoxical activation of endothelial nitric oxide synthase by NADPH oxidase. Arteriosclerosis, Thrombosis, and Vascular Biology. 2008;28(9):1627–1633. doi: 10.1161/atvbaha.108.168278. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Medici D., Shore E. M., Lounev V. Y., Kaplan F. S., Kalluri R., Olsen B. R. Conversion of vascular endothelial cells into multipotent stem-like cells. Nature Medicine. 2010;16(12):1400–1406. doi: 10.1038/nm.2252. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Zeisberg E. M., Potenta S. E., Sugimoto H., Zeisberg M., Kalluri R. Fibroblasts in kidney fibrosis emerge via endothelial-to-mesenchymal transition. Journal of the American Society of Nephrology. 2008;19(12):2282–2287. doi: 10.1681/ASN.2008050513. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Zeisberg E. M., Tarnavski O., Zeisberg M., et al. Endothelial-to-mesenchymal transition contributes to cardiac fibrosis. Nature Medicine. 2007;13(8):952–961. doi: 10.1038/nm1613. [DOI] [PubMed] [Google Scholar]
- 51.Zordan P., Rigamonti E., Freudenberg K., et al. Macrophages commit postnatal endothelium-derived progenitors to angiogenesis and restrict endothelial to mesenchymal transition during muscle regeneration. Cell Death & Disease. 2014;5, article e1031 doi: 10.1038/cddis.2013.558. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Pessina P., Kharraz Y., Jardí M., et al. Fibrogenic cell plasticity blunts tissue regeneration and aggravates muscular dystrophy. Stem Cell Reports. 2015;4(6):1046–1060. doi: 10.1016/j.stemcr.2015.04.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Zeisberg E. M., Potenta S., Xie L., Zeisberg M., Kalluri R. Discovery of endothelial to mesenchymal transition as a source for carcinoma-associated fibroblasts. Cancer Research. 2007;67(21):10123–10128. doi: 10.1158/0008-5472.CAN-07-3127. [DOI] [PubMed] [Google Scholar]
- 54.Traub O., Berk B. C. Laminar shear stress: mechanisms by which endothelial cells transduce an atheroprotective force. Arteriosclerosis, Thrombosis, and Vascular Biology. 1998;18(5):677–685. doi: 10.1161/01.atv.18.5.677. [DOI] [PubMed] [Google Scholar]
- 55.Deverse J. S., Sandhu A. S., Mendoza N., et al. Shear stress modulates VCAM-1 expression in response to TNF-α and dietary lipids via interferon regulatory factor-1 in cultured endothelium. American Journal of Physiology—Heart and Circulatory Physiology. 2013;305(8):H1149–H1157. doi: 10.1152/ajpheart.00311.2013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Kadasi L. M., Dent W. C., Malek A. M. Colocalization of thin-walled dome regions with low hemodynamic wall shear stress in unruptured cerebral aneurysms: clinical article. Journal of Neurosurgery. 2013;119(1):172–179. doi: 10.3171/2013.2.jns12968. [DOI] [PubMed] [Google Scholar]
- 57.Sunamura M., Ishibashi H., Karino T. Flow patterns and preferred sites of intimal thickening in bypass-grafted arteries. International Angiology. 2012;31(2):187–197. [PubMed] [Google Scholar]
- 58.Meirson T., Orion E., Di Mario C., et al. Flow patterns in externally stented saphenous vein grafts and development of intimal hyperplasia. The Journal of Thoracic and Cardiovascular Surgery. 2015;150(4):871–879. doi: 10.1016/j.jtcvs.2015.04.061. [DOI] [PubMed] [Google Scholar]
- 59.Katranas S. A., Kelekis A. L., Antoniadis A. P., et al. Differences in stress forces and geometry between left and right coronary artery: a pathophysiological aspect of atherosclerosis heterogeneity. The Hellenic Journal of Cardiology. 2015;56(3):217–223. [PubMed] [Google Scholar]
- 60.Potter D. R., van Teeffelen J., Vink H., van den Berg B. M. Perturbed mechanotransduction by endothelial surface glycocalyx modification greatly impairs the arteriogenic process. The American Journal of Physiology—Heart and Circulatory Physiology. 2015;309(4):H711–H717. doi: 10.1152/ajpheart.00257.2015. [DOI] [PubMed] [Google Scholar]
- 61.Ebong E. E., Lopez-Quintero S. V., Rizzo V., Spray D. C., Tarbell J. M. Shear-induced endothelial NOS activation and remodeling via heparan sulfate, glypican-1, and syndecan-1. Integrative Biology. 2014;6(3):338–347. doi: 10.1039/c3ib40199e. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Zeng Y., Waters M., Andrews A., et al. Fluid shear stress induces the clustering of heparan sulfate via mobility of glypican-1 in lipid rafts. American Journal of Physiology—Heart and Circulatory Physiology. 2013;305(6):H811–H820. doi: 10.1152/ajpheart.00764.2012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Coon B. G., Baeyens N., Han J., et al. Intramembrane binding of VE-cadherin to VEGFR2 and VEGFR3 assembles the endothelial mechanosensory complex. The Journal of Cell Biology. 2015;208(7):975–986. doi: 10.1083/jcb.201408103. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Baeyens N., Nicoli S., Coon B. G., et al. Vascular remodeling is governed by a VEGFR3-dependent fluid shear stress set point. eLife. 2015;4 doi: 10.7554/elife.04645. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Conway D. E., Breckenridge M. T., Hinde E., Gratton E., Chen C. S., Schwartz M. A. Fluid shear stress on endothelial cells modulates mechanical tension across VE-cadherin and PECAM-1. Current Biology. 2013;23(11):1024–1030. doi: 10.1016/j.cub.2013.04.049. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Slee J. B., Lowe-Krentz L. J. Actin realignment and cofilin regulation are essential for barrier integrity during shear stress. Journal of Cellular Biochemistry. 2013;114(4):782–795. doi: 10.1002/jcb.24416. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Yang B., Rizzo V. Shear stress activates eNOS at the endothelial apical surface through β1 containing integrins and caveolae. Cellular and Molecular Bioengineering. 2013;6(3):346–354. doi: 10.1007/s12195-013-0276-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Ramkhelawon B., Rivas D., Lehoux S. Shear stress activates extracellular signal-regulated kinase 1/2 via the angiotensin II type 1 receptor. The FASEB Journal. 2013;27(8):3008–3016. doi: 10.1096/fj.12-222299. [DOI] [PubMed] [Google Scholar]
- 69.Barauna V. G., Mantuan P. R., Magalhães F. C., Campos L. C. G., Krieger J. E. AT1 receptor blocker potentiates shear-stress induced nitric oxide production via modulation of eNOS phosphorylation of residues Thr495 and Ser1177 . Biochemical and Biophysical Research Communications. 2013;441(4):713–719. doi: 10.1016/j.bbrc.2013.10.108. [DOI] [PubMed] [Google Scholar]
- 70.Chachisvilis M., Zhang Y.-L., Frangos J. A. G protein-coupled receptors sense fluid shear stress in endothelial cells. Proceedings of the National Academy of Sciences of the United States of America. 2006;103(42):15463–15468. doi: 10.1073/pnas.0607224103. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Pries A. R., Secomb T. W., Gaehtgens P. The endothelial surface layer. Pflügers Archiv. 2000;440(5):653–666. doi: 10.1007/s004240000307. [DOI] [PubMed] [Google Scholar]
- 72.Thi M. M., Tarbell J. M., Weinbaum S., Spray D. C. The role of the glycocalyx in reorganization of the actin cytoskeleton under fluid shear stress: a ‘bumper-car’ model. Proceedings of the National Academy of Sciences of the United States of America. 2004;101(47):16483–16488. doi: 10.1073/pnas.0407474101. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Bass M. D., Humphries M. J. Cytoplasmic interactions of syndecan-4 orchestrate adhesion receptor and growth factor receptor signalling. Biochemical Journal. 2002;368(1):1–15. doi: 10.1042/bj20021228. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Simons M., Horowitz A. Syndecan-4-mediated signalling. Cellular Signalling. 2001;13(12):855–862. doi: 10.1016/S0898-6568(01)00190-5. [DOI] [PubMed] [Google Scholar]
- 75.Tzima E., Irani-Tehrani M., Kiosses W. B., et al. A mechanosensory complex that mediates the endothelial cell response to fluid shear stress. Nature. 2005;437(7057):426–431. doi: 10.1038/nature03952. [DOI] [PubMed] [Google Scholar]
- 76.Melchior B., Frangos J. A. Gα q/11-mediated intracellular calcium responses to retrograde flow in endothelial cells. American Journal of Physiology: Cell Physiology. 2012;303(4):C467–C473. doi: 10.1152/ajpcell.00117.2012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Busch R., Strohbach A., Pennewitz M., et al. Regulation of the endothelial apelin/APJ system by hemodynamic fluid flow. Cellular Signalling. 2015;27(7):1286–1296. doi: 10.1016/j.cellsig.2015.03.011. [DOI] [PubMed] [Google Scholar]
- 78.Wang S., Iring A., Strilic B., et al. P2Y2 and Gq/G11 control blood pressure by mediating endothelial mechanotransduction. The Journal of Clinical Investigation. 2015;125(8):3077–3086. doi: 10.1172/jci81067. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Le N.-T., Heo K.-S., Takei Y., et al. A crucial role for p90RSK-mediated reduction of ERK5 transcriptional activity in endothelial dysfunction and atherosclerosis. Circulation. 2013;127(4):486–499. doi: 10.1161/CIRCULATIONAHA.112.116988. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Le N.-T., Takei Y., Izawa-Ishizawa Y., et al. Identification of activators of erk5 transcriptional activity by high-throughput screening and the role of endothelial ERK5 in vasoprotective effects induced by statins and antimalarial agents. The Journal of Immunology. 2014;193(7):3803–3815. doi: 10.4049/jimmunol.1400571. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Yan C., Takahashi M., Okudat M., Lee J.-D., Berk B. C. Fluid shear stress stimulates big mitogen-activated protein kinase 1 (BMK1) activity in endothelial cells. Dependence on tyrosine kinases and intracellular calcium. Journal of Biological Chemistry. 1999;274(1):143–150. doi: 10.1074/jbc.274.1.143. [DOI] [PubMed] [Google Scholar]
- 82.Ohnesorge N., Viemann D., Schmidt N., et al. Erk5 activation elicits a vasoprotective endothelial phenotype via induction of Krüppel-like factor 4 (KLF4) The Journal of Biological Chemistry. 2010;285(34):26199–26210. doi: 10.1074/jbc.m110.103127. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Sathanoori R., Rosi F., Gu B. J., et al. Shear stress modulates endothelial KLF2 through activation of P2X4. Purinergic Signalling. 2015;11(1):139–153. doi: 10.1007/s11302-014-9442-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Parmar K. M., Larman H. B., Dai G., et al. Integration of flow-dependent endothelial phenotypes by kruppel-like factor 2. The Journal of Clinical Investigation. 2006;116(1):49–58. doi: 10.1172/jci24787. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.SenBanerjee S., Lin Z., Atkins G. B., et al. KLF2 is a novel transcriptional regulator of endothelial proinflammatory activation. Journal of Experimental Medicine. 2004;199(10):1305–1315. doi: 10.1084/jem.20031132. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86.Lin Z., Kumar A., SenBanerjee S., et al. Kruppel-like factor 2 (KLF2) regulates endothelial thrombotic function. Circulation research. 2005;96(5):e48–e57. doi: 10.1161/01.res.0000159707.05637.a1. [DOI] [PubMed] [Google Scholar]
- 87.Fledderus J. O., Boon R. A., Volger O. L., et al. KLF2 primes the antioxidant transcription factor Nrf2 for activation in endothelial cells. Arteriosclerosis, Thrombosis, and Vascular Biology. 2008;28(7):1339–1346. doi: 10.1161/ATVBAHA.108.165811. [DOI] [PubMed] [Google Scholar]
- 88.Dekker R. J., Boon R. A., Rondaij M. G., et al. KLF2 provokes a gene expression pattern that establishes functional quiescent differentiation of the endothelium. Blood. 2006;107(11):4354–4363. doi: 10.1182/blood-2005-08-3465. [DOI] [PubMed] [Google Scholar]
- 89.Bhattacharya R., Senbanerjee S., Lin Z., et al. Inhibition of vascular permeability factor/vascular endothelial growth factor-mediated angiogenesis by the kruppel-like factor KLF2. The Journal of Biological Chemistry. 2005;280(32):28848–28851. doi: 10.1074/jbc.c500200200. [DOI] [PubMed] [Google Scholar]
- 90.Boon R. A., Fledderus J. O., Volger O. L., et al. KLF2 suppresses TGF-β signaling in endothelium through induction of Smad7 and inhibition of AP-1. Arteriosclerosis, Thrombosis, and Vascular Biology. 2007;27(3):532–539. doi: 10.1161/01.atv.0000256466.65450.ce. [DOI] [PubMed] [Google Scholar]
- 91.Dekker R. J., van Soest S., Fontijn R. D., et al. Prolonged fluid shear stress induces a distinct set of endothelial cell genes, most specifically lung Krüppel-like factor (KLF2) Blood. 2002;100(5):1689–1698. doi: 10.1182/blood-2002-01-0046. [DOI] [PubMed] [Google Scholar]
- 92.McCormick S. M., Eskin S. G., McIntire L. V., et al. DNA microarray reveals changes in gene expression of shear stressed human umbilical vein endothelial cells. Proceedings of the National Academy of Sciences of the United States of America. 2001;98(16):8955–8960. doi: 10.1073/pnas.171259298. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93.Villarreal G., Jr., Zhang Y., Larman H. B., Gracia-Sancho J., Koo A., García-Cardeña G. Defining the regulation of KLF4 expression and its downstream transcriptional targets in vascular endothelial cells. Biochemical and Biophysical Research Communications. 2010;391(1):984–989. doi: 10.1016/j.bbrc.2009.12.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 94.Hamik A., Lin Z., Kumar A., et al. Kruppel-like factor 4 regulates endothelial inflammation. The Journal of Biological Chemistry. 2007;282(18):13769–13779. doi: 10.1074/jbc.m700078200. [DOI] [PubMed] [Google Scholar]
- 95.Jung Y.-A., Lee K.-M., Kim M.-K., et al. Forkhead transcription factor foxO1 inhibits insulin- and transforming growth factor-β-stimulated plasminogen activator inhibitor-1 expression. Biochemical and Biophysical Research Communications. 2009;386(4):757–761. doi: 10.1016/j.bbrc.2009.06.124. [DOI] [PubMed] [Google Scholar]
- 96.Ghaleb A. M., Nandan M. O., Chanchevalap S., Dalton W. B., Hisamuddin I. M., Yang V. W. Krüppel-like factors 4 and 5: the yin and yang regulators of cellular proliferation. Cell Research. 2005;15(2):92–96. doi: 10.1038/sj.cr.7290271. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 97.Maleszewska M., Vanchin B., Harmsen M. C., Krenning G. The decrease in histone methyltransferase EZH2 in response to fluid shear stress alters endothelial gene expression and promotes quiescence. Angiogenesis. 2016;19(1):9–24. doi: 10.1007/s10456-015-9485-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 98.Wang Z., Wang D.-Z., Pipes G. C. T., Olson E. N. Myocardin is a master regulator of smooth muscle gene expression. Proceedings of the National Academy of Sciences of the United States of America. 2003;100(12):7129–7134. doi: 10.1073/pnas.1232341100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.Li S., Wang D.-Z., Wang Z., Richardson J. A., Olson E. N. The serum response factor coactivator myocardin is required for vascular smooth muscle development. Proceedings of the National Academy of Sciences of the United States of America. 2003;100(16):9366–9370. doi: 10.1073/pnas.1233635100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Liu Y., Sinha S., McDonald O. G., Shang Y., Hoofnagle M. H., Owens G. K. Kruppel-like factor 4 abrogates myocardin-induced activation of smooth muscle gene expression. The Journal of Biological Chemistry. 2005;280(10):9719–9727. doi: 10.1074/jbc.m412862200. [DOI] [PubMed] [Google Scholar]
- 101.Adam P. J., Regan C. P., Hautmann M. B., Owens G. K. Positive- and negative-acting Kruppel-like transcription factors bind a transforming growth factor β control element required for expression of the smooth muscle cell differentiation marker SM22α in vivo. Journal of Biological Chemistry. 2000;275(48):37798–37806. doi: 10.1074/jbc.m006323200. [DOI] [PubMed] [Google Scholar]
- 102.Hu B., Wu Z., Liu T., Ullenbruch M. R., Jin H., Phan S. H. Gut-enriched Krüppel-like factor interaction with Smad3 inhibits myofibroblast differentiation. American Journal of Respiratory Cell and Molecular Biology. 2007;36(1):78–84. doi: 10.1165/rcmb.2006-0043OC. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 103.Cowan C. E., Kohler E. E., Dugan T. A., Mirza M. K., Malik A. B., Wary K. K. Krüppel-like factor-4 transcriptionally regulates VE-cadherin expression and endothelial barrier function. Circulation Research. 2010;107(8):959–966. doi: 10.1161/circresaha.110.219592. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 104.Sun D., Huang A., Yan E. H., et al. Reduced release of nitric oxide to shear stress in mesenteric arteries of aged rats. The American Journal of Physiology—Heart and Circulatory Physiology. 2004;286(6):H2249–H2256. doi: 10.1152/ajpheart.00854.2003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 105.Woodman C. R., Muller J. M., Rush J. W. E., Laughlin M. H., Price E. M. Flow regulation of ecNOS and Cu/Zn SOD mRNA expression in porcine coronary arterioles. American Journal of Physiology—Heart and Circulatory Physiology. 1999;276(3):H1058–H1063. doi: 10.1152/ajpheart.1999.276.3.H1058. [DOI] [PubMed] [Google Scholar]
- 106.Kim B., Lee H., Kawata K., Park J.-Y. Exercise-mediated wall shear stress increases mitochondrial biogenesis in vascular endothelium. PLoS ONE. 2014;9(11) doi: 10.1371/journal.pone.0111409.e111409 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 107.Wasserman S. M., Mehraban F., Komuves L. G., et al. Gene expression profile of human endothelial cells exposed to sustained fluid shear stress. Physiological Genomics. 2003;12(1):13–23. doi: 10.1152/physiolgenomics.00102.2002. [DOI] [PubMed] [Google Scholar]
- 108.Norton J. D. Id helix-loop-helix proteins in cell growth, differentiation and tumorigenesis. Journal of Cell Science. 2000;113(22):3897–3905. doi: 10.1242/jcs.113.22.3897. [DOI] [PubMed] [Google Scholar]
- 109.Saika S., Ikeda K., Yamanaka O., et al. Adenoviral gene transfer of BMP-7, Id2, or Id3 suppresses injury-induced epithelial-to-mesenchymal transition of lens epithelium in mice. The American Journal of Physiology—Cell Physiology. 2006;290(1):C282–C289. doi: 10.1152/ajpcell.00306.2005. [DOI] [PubMed] [Google Scholar]
- 110.Kowanetz M., Valcourt U., Bergström R., Heldin C.-H., Moustakas A. Id2 and Id3 define the potency of cell proliferation and differentiation responses to transforming growth factor β and bone morphogenetic protein. Molecular and Cellular Biology. 2004;24(10):4241–4254. doi: 10.1128/mcb.24.10.4241-4254.2004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 111.Zhang H., Lawson W. E., Polosukhin V. V., et al. Inhibitor of differentiation 1 promotes endothelial survival in a bleomycin model of lung injury in mice. The American Journal of Pathology. 2007;171(4):1113–1126. doi: 10.2353/ajpath.2007.070226. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 112.Li R., Aslan A., Yan R., et al. Histone deacetylase inhibition and IκB kinase/nuclear factor-kappab blockade ameliorate microvascular proinflammatory responses associated with hemorrhagic shock/resuscitation in mice. Critical Care Medicine. 2015;43(12):e567–e580. doi: 10.1097/ccm.0000000000001203. [DOI] [PubMed] [Google Scholar]
- 113.Chappell D. C., Varner S. E., Nerem R. M., Medford R. M., Alexander R. W. Oscillatory shear stress stimulates adhesion molecule expression in cultured human endothelium. Circulation Research. 1998;82(5):532–539. doi: 10.1161/01.res.82.5.532. [DOI] [PubMed] [Google Scholar]
- 114.Hsiai T. K., Cho S. K., Wong P. K., et al. Monocyte recruitment to endothelial cells in response to oscillatory shear stress. The FASEB Journal. 2003;17(12):1648–1657. doi: 10.1096/fj.02-1064com. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 115.Bergmann C. E., Hoefer I. E., Meder B., et al. Arteriogenesis depends on circulating monocytes and macrophage accumulation and is severely depressed in op/op mice. Journal of Leukocyte Biology. 2006;80(1):59–65. doi: 10.1189/jlb.0206087. [DOI] [PubMed] [Google Scholar]
- 116.De Keulenaer G. W., Chappell D. C., Ishizaka N., Nerem R. M., Wayne Alexander R., Griendling K. K. Oscillatory and steady laminar shear stress differentially affect human endothelial redox state: role of a superoxide-producing NADH oxidase. Circulation Research. 1998;82(10):1094–1101. doi: 10.1161/01.res.82.10.1094. [DOI] [PubMed] [Google Scholar]
- 117.McNally J. S., Davis M. E., Giddens D. P., et al. Role of xanthine oxidoreductase and NAD(P)H oxidase in endothelial superoxide production in response to oscillatory shear stress. American Journal of Physiology—Heart and Circulatory Physiology. 2003;285(6):H2290–H2297. doi: 10.1152/ajpheart.00515.2003. [DOI] [PubMed] [Google Scholar]
- 118.Hwang J., Ing M. H., Salazar A., et al. Pulsatile versus oscillatory shear stress regulates nadph oxidase subunit expression: implication for native ldl oxidation. Circulation Research. 2003;93(12):1225–1232. doi: 10.1161/01.res.0000104087.29395.66. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 119.Takeshita S., Inoue N., Ueyama T., Kawashima S., Yokoyama M. Shear stress enhances glutathione peroxidase expression in endothelial cells. Biochemical and Biophysical Research Communications. 2000;273(1):66–71. doi: 10.1006/bbrc.2000.2898. [DOI] [PubMed] [Google Scholar]
- 120.Chen B. P., Li Y. S., Zhao Y., et al. DNA microarray analysis of gene expression in endothelial cells in response to 24-h shear stress. Physiological Genomics. 2001;7(1):55–63. doi: 10.1152/physiolgenomics.2001.7.1.55. [DOI] [PubMed] [Google Scholar]
- 121.Sorescu G. P., Sykes M., Weiss D., et al. Bone morphogenic protein 4 produced in endothelial cells by oscillatory shear stress stimulates an inflammatory response. Journal of Biological Chemistry. 2003;278(33):31128–31135. doi: 10.1074/jbc.m300703200. [DOI] [PubMed] [Google Scholar]
- 122.Sorescu G. P., Song H., Tressel S. L., et al. Bone morphogenic protein 4 produced in endothelial cells by oscillatory shear stress induces monocyte adhesion by stimulating reactive oxygen species production from a Nox1-based NADPH oxidase. Circulation Research. 2004;95(8):773–779. doi: 10.1161/01.RES.0000145728.22878.45. [DOI] [PubMed] [Google Scholar]
- 123.Mahler G. J., Frendl C. M., Cao Q., Butcher J. T. Effects of shear stress pattern and magnitude on mesenchymal transformation and invasion of aortic valve endothelial cells. Biotechnology and Bioengineering. 2014;111(11):2326–2337. doi: 10.1002/bit.25291. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 124.Dobrin P. B. Mechanical properties of arteries. Physiological Reviews. 1978;58(2):397–460. doi: 10.1152/physrev.1978.58.2.397. [DOI] [PubMed] [Google Scholar]
- 125.Takeda H., Komori K., Nishikimi N., Nimura Y., Sokabe M., Naruse K. Bi-phasic activation of eNOS in response to uni-axial cyclic stretch is mediated by differential mechanisms in BAECs. Life Sciences. 2006;79(3):233–239. doi: 10.1016/j.lfs.2005.12.051. [DOI] [PubMed] [Google Scholar]
- 126.Sung L. C., Chao H. H., Chen C. H., et al. Lycopene inhibits cyclic strain-induced endothelin-1 expression through the suppression of reactive oxygen species generation and induction of heme oxygenase-1 in human umbilical vein endothelial cells. Clinical and Experimental Pharmacology and Physiology. 2015;42(6):632–639. doi: 10.1111/1440-1681.12412. [DOI] [PubMed] [Google Scholar]
- 127.Liu X.-M., Peyton K. J., Durante W. Physiological cyclic strain promotes endothelial cell survival via the induction of heme oxygenase-1. American Journal of Physiology—Heart and Circulatory Physiology. 2013;304(12):H1634–H1643. doi: 10.1152/ajpheart.00872.2012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 128.Wagner A. H., Kautz O., Fricke K., et al. Upregulation of glutathione peroxidase offsets stretch-induced proatherogenic gene expression in human endothelial cells. Arteriosclerosis, Thrombosis, and Vascular Biology. 2009;29(11):1894–1901. doi: 10.1161/atvbaha.109.194738. [DOI] [PubMed] [Google Scholar]
- 129.Imura T., Yamamoto K., Kanamori K., Mikami T., Yasuda H. Non-invasive ultrasonic measurement of the elastic properties of the human abdominal aorta. Cardiovascular Research. 1986;20(3):208–214. doi: 10.1093/cvr/20.3.208. [DOI] [PubMed] [Google Scholar]
- 130.Von Offenberg Sweeney N., Cummins P. M., Cotter E. J., et al. Cyclic strain-mediated regulation of vascular endothelial cell migration and tube formation. Biochemical and Biophysical Research Communications. 2005;329(2):573–582. doi: 10.1016/j.bbrc.2005.02.013. [DOI] [PubMed] [Google Scholar]
- 131.Liu X.-M., Ensenat D., Wang H., Schafer A. I., Durante W. Physiologic cyclic stretch inhibits apoptosis in vascular endothelium. FEBS Letters. 2003;541(1–3):52–56. doi: 10.1016/s0014-5793(03)00285-0. [DOI] [PubMed] [Google Scholar]
- 132.Naruse K., Sokabe M. Involvement of stretch-activated ion channels in Ca2+ mobilization to mechanical stretch in endothelial cells. American Journal of Physiology—Cell Physiology. 1993;264(4):C1037–C1044. doi: 10.1152/ajpcell.1993.264.4.C1037. [DOI] [PubMed] [Google Scholar]
- 133.Sasamoto A., Nagino M., Kobayashi S., Naruse K., Nimura Y., Sokabe M. Mechanotransduction by integrin is essential for IL-6 secretion from endothelial cells in response to uniaxial continuous stretch. American Journal of Physiology: Cell Physiology. 2005;288(5):C1012–C1022. doi: 10.1152/ajpcell.00314.2004. [DOI] [PubMed] [Google Scholar]
- 134.Ngu H., Feng Y., Lu L., Oswald S. J., Longmore G. D., Yin F. C.-P. Effect of focal adhesion proteins on endothelial cell adhesion, motility and orientation response to cyclic strain. Annals of Biomedical Engineering. 2010;38(1):208–222. doi: 10.1007/s10439-009-9826-7. [DOI] [PubMed] [Google Scholar]
- 135.Clark C. B., McKnight N. L., Frangos J. A. Strain and strain rate activation of G proteins in human endothelial cells. Biochemical and Biophysical Research Communications. 2002;299(2):258–262. doi: 10.1016/s0006-291x(02)02628-1. [DOI] [PubMed] [Google Scholar]
- 136.Zou Y., Akazawa H., Qin Y., et al. Mechanical stress activates angiotensin II type 1 receptor without the involvement of angiotensin II. Nature Cell Biology. 2004;6(6):499–506. doi: 10.1038/ncb1137. [DOI] [PubMed] [Google Scholar]
- 137.Yasuda N., Miura S.-I., Akazawa H., et al. Conformational switch of angiotensin II type 1 receptor underlying mechanical stress-induced activation. EMBO Reports. 2008;9(2):179–186. doi: 10.1038/sj.embor.7401157. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 138.Bishop A. L., Hall A. Rho GTPases and their effector proteins. Biochemical Journal. 2000;348(2):241–255. doi: 10.1042/0264-6021:3480241. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 139.Beckers C. M. L., van Hinsbergh V. W. M., van Nieuw Amerongen G. P. Driving Rho GTPase activity in endothelial cells regulates barrier integrity. Thrombosis and Haemostasis. 2010;103(1):40–55. doi: 10.1160/th09-06-0403. [DOI] [PubMed] [Google Scholar]
- 140.Kaunas R., Nguyen P., Usami S., Chien S. Cooperative effects of Rho and mechanical stretch on stress fiber organization. Proceedings of the National Academy of Sciences of the United States of America. 2005;102(44):15895–15900. doi: 10.1073/pnas.0506041102. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 141.Greiner A. M., Biela S. A., Chen H., Spatz J. P., Kemkemer R. Temporal responses of human endothelial and smooth muscle cells exposed to uniaxial cyclic tensile strain. Experimental Biology and Medicine. 2015;240(10):1298–1309. doi: 10.1177/1535370215570191. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 142.Birukov K. G., Jacobson J. R., Flores A. A., et al. Magnitude-dependent regulation of pulmonary endothelial cell barrier function by cyclic stretch. American Journal of Physiology—Lung Cellular and Molecular Physiology. 2003;285(4):L785–L797. doi: 10.1152/ajplung.00336.2002. [DOI] [PubMed] [Google Scholar]
- 143.Birukova A. A., Chatchavalvanich S., Rios A., Kawkitinarong K., Garcia J. G. N., Birukov K. G. Differential regulation of pulmonary endothelial monolayer integrity by varying degrees of cyclic stretch. The American Journal of Pathology. 2006;168(5):1749–1761. doi: 10.2353/ajpath.2006.050431. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 144.Katsumi A., Milanini J., Kiosses W. B., et al. Effects of cell tension on the small GTPase Rac. The Journal of Cell Biology. 2002;158(1):153–164. doi: 10.1083/jcb.200201105. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 145.Balachandran K., Alford P. W., Wylie-Sears J., et al. Cyclic strain induces dual-mode endothelial-mesenchymal transformation of the cardiac valve. Proceedings of the National Academy of Sciences of the United States of America. 2011;108(50):19943–19948. doi: 10.1073/pnas.1106954108. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 146.Sato M., Muragaki Y., Saika S., Roberts A. B., Ooshima A. Targeted disruption of TGF-β1/Smad3 signaling protects against renal tubulointerstitial fibrosis induced by unilateral ureteral obstruction. Journal of Clinical Investigation. 2003;112(10):1486–1494. doi: 10.1172/jci200319270. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 147.Cheng S.-L., Shao J.-S., Behrmann A., Krchma K., Towler D. A. Dkk1 and msx2–wnt7b signaling reciprocally regulate the endothelial–mesenchymal transition in aortic endothelial cells. Arteriosclerosis, Thrombosis, and Vascular Biology. 2013;33(7):1679–1689. doi: 10.1161/atvbaha.113.300647. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 148.Vincent P. A., Xiao K., Buckley K. M., Kowalczyk A. P. VE-cadherin: adhesion at arm's length. American Journal of Physiology—Cell Physiology. 2004;286(5):C987–C997. doi: 10.1152/ajpcell.00522.2003. [DOI] [PubMed] [Google Scholar]
- 149.Rolfe B. E., Worth N. F., World C. J., Campbell J. H., Campbell G. R. Rho and vascular disease. Atherosclerosis. 2005;183(1):1–16. doi: 10.1016/j.atherosclerosis.2005.04.023. [DOI] [PubMed] [Google Scholar]
- 150.Masszi A., Di Ciano C., Sirokmány G., et al. Central role for Rho in TGF-β 1-induced α-smooth muscle actin expression during epithelial-mesenchymal transition. American Journal of Physiology—Renal Physiology. 2003;284(5):F911–F924. doi: 10.1152/ajprenal.00183.2002. [DOI] [PubMed] [Google Scholar]
- 151.Mihira H., Suzuki H. I., Akatsu Y., et al. TGF-β-induced mesenchymal transition of MS-1 endothelial cells requires Smad-dependent cooperative activation of Rho signals and MRTF-A. Journal of Biochemistry. 2012;151(2):145–156. doi: 10.1093/jb/mvr121. [DOI] [PubMed] [Google Scholar]
- 152.Wu M., Tang R.-N., Liu H., Ma K.-L., Lv L.-L., Liu B.-C. Nuclear translocation of β-catenin mediates the parathyroid hormone-induced endothelial-to-mesenchymal transition in human renal glomerular endothelial cells. Journal of Cellular Biochemistry. 2014;115(10):1692–1701. doi: 10.1002/jcb.24832. [DOI] [PubMed] [Google Scholar]
- 153.Woessner J. F., Jr. Matrix metalloproteinases and their inhibitors in connective tissue remodeling. The FASEB Journal. 1991;5(8):2145–2154. [PubMed] [Google Scholar]
- 154.Mark Jenkins G., Crow M. T., Bilato C., et al. Increased expression of membrane-type matrix metalloproteinase and preferential localization of matrix metalloproteinase-2 to the neointima of balloon-injured rat carotid arteries. Circulation. 1998;97(1):82–90. doi: 10.1161/01.CIR.97.1.82. [DOI] [PubMed] [Google Scholar]
- 155.Wang B.-W., Chang H., Lin S., Kuan P., Shyu K.-G. Induction of matrix metalloproteinases-14 and -2 by cyclical mechanical stretch is mediated by tumor necrosis factor-alpha in cultured human umbilical vein endothelial cells. Cardiovascular Research. 2003;59(2):460–469. doi: 10.1016/s0008-6363(03)00428-0. [DOI] [PubMed] [Google Scholar]
- 156.Meng X., Mavromatis K., Galis Z. S. Mechanical stretching of human saphenous vein grafts induces expression and activation of matrix-degrading enzymes associated with vascular tissue injury and repair. Experimental and Molecular Pathology. 1999;66(3):227–237. doi: 10.1006/exmp.1999.2260. [DOI] [PubMed] [Google Scholar]
- 157.Safar M. E. Arterial aging—hemodynamic changes and therapeutic options. Nature Reviews Cardiology. 2010;7(8):422–449. doi: 10.1038/nrcardio.2010.102. [DOI] [PubMed] [Google Scholar]
- 158.Dancu M. B., Berardi D. E., Vanden Heuvel J. P., Tarbell J. M. Asynchronous shear stress and circumferential strain reduces endothelial NO synthase and cyclooxygenase-2 but induces endothelin-1 gene expression in endothelial cells. Arteriosclerosis, Thrombosis, and Vascular Biology. 2004;24(11):2088–2094. doi: 10.1161/01.ATV.0000143855.85343.0e. [DOI] [PubMed] [Google Scholar]
- 159.Amaya R., Pierides A., Tarbell J. M., West J. The interaction between fluid wall shear stress and solid circumferential strain affects endothelial gene expression. PLoS ONE. 2015;10(7) doi: 10.1371/journal.pone.0129952.e0129952 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 160.Kohn J. C., Zhou D. W., Bordeleau F., et al. Cooperative effects of matrix stiffness and fluid shear stress on endothelial cell behavior. Biophysical Journal. 2015;108(3):471–478. doi: 10.1016/j.bpj.2014.12.023. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 161.Ma K. L., Liu J., Ni J., et al. Inflammatory stress exacerbates the progression of cardiac fibrosis in high-fat-fed apolipoprotein e knockout mice via endothelial-mesenchymal transition. International Journal of Medical Sciences. 2013;10(4):420–426. doi: 10.7150/ijms.5723. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 162.Beranek J. T. Vascular endothelium-derived cells containing smooth muscle actin are present in restenosis. Laboratory Investigation. 1995;72(6):p. 771. [PubMed] [Google Scholar]
- 163.Volger O. L., Fledderus J. O., Kisters N., et al. Distinctive expression of chemokines and transforming growth factor-β signaling in human arterial endothelium during atherosclerosis. The American Journal of Pathology. 2007;171(1):326–337. doi: 10.2353/ajpath.2007.061196. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 164.Dhore C. R., Cleutjens J. P. M., Lutgens E., et al. Differential expression of bone matrix regulatory proteins in human atherosclerotic plaques. Arteriosclerosis, Thrombosis, and Vascular Biology. 2001;21(12):1998–2003. doi: 10.1161/hq1201.100229. [DOI] [PubMed] [Google Scholar]
- 165.Kojda G., Harrison D. Interactions between NO and reactive oxygen species: pathophysiological importance in atherosclerosis, hypertension, diabetes and heart failure. Cardiovascular Research. 1999;43(3):562–571. doi: 10.1016/s0008-6363(99)00169-8. [DOI] [PubMed] [Google Scholar]
- 166.Rabinovitch M. Pathobiology of pulmonary hypertension. Annual Review of Pathology. 2007;2:369–399. doi: 10.1146/annurev.pathol.2.010506.092033. [DOI] [PubMed] [Google Scholar]
- 167.Okamoto M., Miyatake K., Kinoshita N., Sakakibara H., Nimura Y. Analysis of blood flow in pulmonary hypertension with the pulsed Doppler flowmeter combined with cross sectional echocardiography. British Heart Journal. 1984;51(4):407–415. doi: 10.1136/hrt.51.4.407. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 168.Masri F. A., Xu W., Comhair S. A. A., et al. Hyperproliferative apoptosis-resistant endothelial cells in idiopathic pulmonary arterial hypertension. American Journal of Physiology—Lung Cellular and Molecular Physiology. 2007;293(3):L548–L554. doi: 10.1152/ajplung.00428.2006. [DOI] [PubMed] [Google Scholar]
- 169.Dickinson M. G., Bartelds B., Molema G., et al. Egr-1 expression during neointimal development in flow-associated pulmonary hypertension. American Journal of Pathology. 2011;179(5):2199–2209. doi: 10.1016/j.ajpath.2011.07.030. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 170.Van Albada M. E., Bartelds B., Wijnberg H., et al. Gene expression profile in flow-associated pulmonary arterial hypertension with neointimal lesions. American Journal of Physiology—Lung Cellular and Molecular Physiology. 2010;298(4):L483–L491. doi: 10.1152/ajplung.00106.2009. [DOI] [PubMed] [Google Scholar]
- 171.Cheng J.-C., Chang H.-M., Leung P. C. K. Egr-1 mediates epidermal growth factor-induced downregulation of E-cadherin expression via Slug in human ovarian cancer cells. Oncogene. 2013;32(8):1041–1049. doi: 10.1038/onc.2012.127. [DOI] [PubMed] [Google Scholar]
- 172.Grotegut S., von Schweinitz D., Christofori G., Lehembre F. Hepatocyte growth factor induces cell scattering through MAPK/Egr-1-mediated upregulation of Snail. The EMBO Journal. 2006;25(15):3534–3545. doi: 10.1038/sj.emboj.7601213. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 173.Kokudo T., Suzuki Y., Yoshimatsu Y., Yamazaki T., Watabe T., Miyazono K. Snail is required for TGFβ-induced endothelial-mesenchymal transition of embryonic stem cell-derived endothelial cells. Journal of Cell Science. 2008;121(20):3317–3324. doi: 10.1242/jcs.028282. [DOI] [PubMed] [Google Scholar]
- 174.Good R. B., Gilbane A. J., Trinder S. L., et al. Endothelial to mesenchymal transition contributes to endothelial dysfunction in pulmonary arterial hypertension. The American Journal of Pathology. 2015;185(7):1850–1858. doi: 10.1016/j.ajpath.2015.03.019. [DOI] [PubMed] [Google Scholar]
- 175.Ranchoux B., Antigny F., Rucker-Martin C., et al. Endothelial-to-mesenchymal transition in pulmonary hypertension. Circulation. 2015;131(11):1006–1018. doi: 10.1161/circulationaha.114.008750. [DOI] [PubMed] [Google Scholar]
- 176.Harrison R. E., Berger R., Haworth S. G., et al. Transforming growth factor-beta receptor mutations and pulmonary arterial hypertension in childhood. Circulation. 2005;111(4):435–441. doi: 10.1161/01.cir.0000153798.78540.87. [DOI] [PubMed] [Google Scholar]
- 177.Lane K. B., Machado R. D., Pauciulo M. W., et al. Heterozygous germline mutations in BMPR2, encoding a TGF-β receptor, cause familial primary pulmonary hypertension. Nature Genetics. 2000;26(1):81–84. doi: 10.1038/79226. [DOI] [PubMed] [Google Scholar]
- 178.Kawabata M., Imamura T., Miyazono K. Signal transduction by bone morphogenetic proteins. Cytokine and Growth Factor Reviews. 1998;9(1):49–61. doi: 10.1016/s1359-6101(97)00036-1. [DOI] [PubMed] [Google Scholar]
- 179.Reynolds A. M., Holmes M. D., Danilov S. M., Reynolds P. N. Targeted gene delivery of BMPR2 attenuates pulmonary hypertension. European Respiratory Journal. 2012;39(2):329–343. doi: 10.1183/09031936.00187310. [DOI] [PubMed] [Google Scholar]