Abstract
Omental and mesenteric lipomas are very rare benign lesions of mature adipose tissue. They are well-defined, noninvasive, and encapsulated masses that can be discovered in asymptomatic patients or may cause variable nonspecific symptoms depending on their size and location. The omental and mesenteric lipoma has confusing features in ultrasound; however, computed tomography and magnetic resonance imaging can well characterize and demarcate these lesions. Though few cases of mesenteric and omental lipomas have been reported in the literature, but because of its large size and childhood presentation, the case we present, can be one of the largest childhood omental and mesenteric lipomas ever reported. A 6-year-old girl presented with slowly progressing abdominal distension and repeated dull abdominal pain for last 4 years. Abdominal and pelvic computed tomography examination revealed a huge mesenteric and omental lipoma that was resected surgically without any complications.
Keywords: Lipoma, Mesenteric and omental mass, Pediatric abdominal mass, Abdominal distension
Case report
A six-year-old girl presented with slowly progressing abdominal distension and repeated dull abdominal pain for last 4 years. No history of vomiting, diarrhea, constipation, or urinary tract symptoms were present.
Abdominal ultrasound examination revealed a large, heterogeneous, relatively echogenic mass lesion occupying almost entire abdominal cavity. The outlines of the lesion were not well recognizable on ultrasound. Apart from displacement of the major abdominal viscera to periphery of the abdominal cavity, no gross abnormality was detected in the intra-abdominal organs.
The patient subsequently underwent the abdominal and the pelvic computed tomography (CT) examination with 128-slice Siemens scanner.
CT images revealed a huge, well-defined, low density, fat attenuation, nonenhancing, intraperitoneal, mass lesion occupying majority of the abdominal cavity. This large mass lesion was extending from just beneath the right dome of diaphragm down to level of symphysis pubis. Multiple fibrous septations and few specks of calcifications were seen within this essentially fatty lesion. No major abdominal vessels were traversing the lesion. There was no evidence of inflammatory reaction or infiltration of surrounding structures or tissues (Fig. 1A).
Fig. 1.
(A) Contrast-enhanced right parasagittal CT section through the abdomen and pelvis shows a huge, well-defined, low density, nonenhancing, intraperitoneal, mass lesion extending from the diaphragm down to pelvis. Note the fibrous septa and a calcified focus (arrow). No evidence of inflammatory reaction or infiltration of surrounding structures. (B) Contrast-enhanced axial CT section through the abdomen and pelvis: The well demarcated, low attenuating mass lesion is compressing the bowel loops rather than infiltrating them (arrows). No extension to the retroperitoneal spaces. The retroperitoneal structures and the bowel loops are displaced posterolateraly (arrows). No evidence of any obstructive compression on gastrointestinal or urinary tract organs.
This well demarcated huge mass lesion was compressing the bowel loops rather than infiltrating them; however, no extension of the mass lesion was seen to the retroperitoneal spaces.
There was no sign of entering of any part of this fatty lesion into the spaces between the liver and right kidney or spleen and left kidney. This finding excluded the possibility of peritoneal lipomatosis.
The retroperitoneal structures and the bowel loops were displaced posterolateraly toward the abdominal walls. There was no evidence of any obstructive compression on gastrointestinal or urinary tract organs (Fig. 1B).
This mass lesion measured 28 × 24 × 10 cm3 in maximum craniocaudal, transverse, and anterioposterior dimensions, respectively.
The patient underwent open abdominal surgery under general anesthesia and a huge, encapsulated mass was discovered adherent to the stomach, transverse colon, intestinal mesentery, and posterior abdominal wall. The mass was not separable from both the omentum and the mesentery.
As the mass lesion was neither originating form nor infiltrating the important abdominal viscera and blood vessels, so this huge; 4 kilograms mass lesion was easily resected without major bleeding or postoperative complications.
Macroscopically it was a large, tan and gray color glistening surfaced, encapsulated, moderately firm mass. The cut sections of the mass showed homogenous yellowish tan soft surfaces (Fig. 2).
Fig. 2.
Macroscopic view from the cut of the large 4 kilograms tan and gray color glistening surfaced encapsulated moderately firm mass. The cut sections show homogenous yellowish tan soft surfaces.
Microscopic sections showed tumor composed of large nodules and a sheet of mature adipocytes without atypia that were separated by thin fibrous bands. The findings were negative for malignancy (Fig. 3).
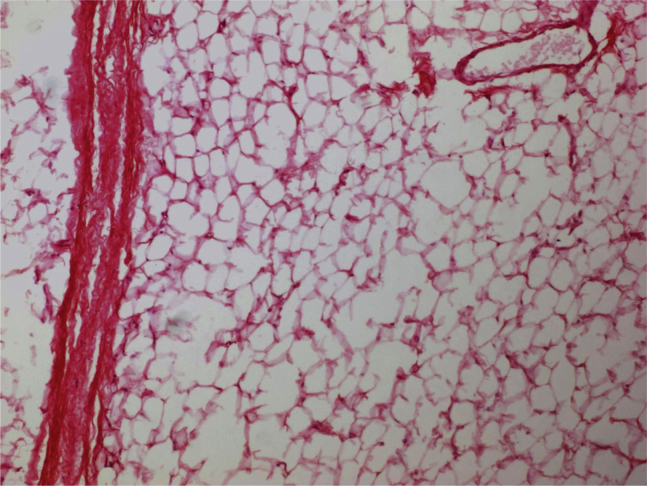
Fig. 3.
Microscopic section of the mass lesion shows tumor composed of large nodules and sheet of mature adipocytes without atypia, separated by thin fibrous bands. Negative for malignancy.
Keeping in view the clinical, radiological, surgical, and histological findings; a rare childhood giant omental and mesenteric lipoma was diagnosed.
Discussion
Lipomas are benign, well-defined, noninvasive, and encapsulated tumor of mature adipose tissue [1]. These common benign lesions can arise in any part of the body [2], but mesenteric and omental lipomas are rare entities [3], [4].
A literature review performed by Cha, Jae Myung et al at 2007 showed that less than 30 cases of mesenteric lipomas were reported with only 7 cases in children. He presented a lipoma of 19 × 10 × 5.1 cm3 in a 29-year-old man and argued that this was one of the largest lipomas reported in literature [3]. The case presented here; can exactly be one of the largest childhood omental and mesenteric lipomas reported.
Mesenteric lipomas are slow-growing, mobile, soft, masses that does not infiltrate the surrounding organs [5], [6].
Abdominal cavity lipomas may be discovered as asymptomatic masses or they may cause variable nonspecific symptoms. These symptoms include progressive abdominal distention, [7] anorexia, abdominal pain, constipation, weight loss, and sensation of abdominal fullness [3]. Cases of intestinal volvulus caused by mesenteric lipoma are also reported [8].
When the omental and mesenteric lipomas are large enough, they can be palpated as soft to firm masses in physical examination [9].
Imaging features
Ultrasound can detect abdominal lipomas as homogenous echogenic masses; however, they may present a confusing picture from homogenous to heterogeneous echo pattern [3]. If not so large, abdominal lipomas can be misdiagnosed as normal mesenteric fat [3].
Thin fibrous septations [7] and calcification may be present in up to 11% of cases [10].
CT and magnetic resonance imaging can well depict these fatty tumors [9].
CT shows the typical fat tissue attenuation valves [11] from (−80 to −120 HU) [12], [13]. CT can also determine the omental or mesenteric origin of the tumor and depicts the precise anatomic features [14].
Magnetic resonance imaging, owing the high capability of tissue characterization, can nicely differentiate the lesion from adjacent structures and depict precise anatomic demarcations.
Lipoma will demonstrate homogeneous signal intensity identical to fat in all pulse sequences. The thin fibrous septa will show low signal intensity on T1- and T2-weighted images [12].
Because of lack of published reports, the long-term behavior of these lesions is not well known in children [15]; therefore, a long-term follow-up is advised [7].
Footnotes
Competing Interests: The authors have declared that no competing interests exist.
References
- 1.Sirikci A., Bayram M., Kervancioglu R., Sarica K. Abdominopelvic lipomatosis in a child with indefinite physical findings. Pediatr Radiol. 2000;30(7):480. doi: 10.1007/s002470000253. [DOI] [PubMed] [Google Scholar]
- 2.Rhydholm A., Berg N.O. Size, site and clinical incidence of lipoma. Acta Orthop Scand. 1983;54:929–934. doi: 10.3109/17453678308992936. [DOI] [PubMed] [Google Scholar]
- 3.Cha J.M., Lee J.I., Joo K.R., Choe J.W., Jung S.W., Shin H.P. Giant mesenteric lipoma as an unusual cause of abdominal pain: a case report and a review of the literature. J Korean Med Sci. 2009;24(2):333–336. doi: 10.3346/jkms.2009.24.2.333. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Chaudhary V., Narula M.K., Anand R., Gupta I., Kaur G., Kalra K. Giant omental lipoma in a child. Iran J Radiol. 2011;8(3):167–169. doi: 10.5812/kmp.iranjradiol.17351065.3150. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Prando A., Wallace S., Marins J.L., Pereira R.M., de Oliveira E.R., Alvarenga M. Sonographic features of benign intraperitoneal lipomatous tumor in children: report of 4 cases. Pediatr Radiol. 1990;20:571–574. doi: 10.1007/BF02129056. [DOI] [PubMed] [Google Scholar]
- 6.Ilhan H., Tokar B., Isiksoy S., Koku N., Pasaoglu O. Giant mesenteric lipoma. J Pediatr Surg. 1999;34:639–640. doi: 10.1016/s0022-3468(99)90094-5. [DOI] [PubMed] [Google Scholar]
- 7.Mohammed A.M., Yakubu A.A. Giant retroperitoneal lipoma in an infant. J Surg Tech Case Rep. 2010;2(1):33–34. doi: 10.4103/2006-8808.63722. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Sheen A.J., Drake I., George P.P. A small bowel volvulus caused by a mesenteric lipoma: report of a case. Surg Today. 2003;33:617–619. doi: 10.1007/s00595-003-2533-3. [DOI] [PubMed] [Google Scholar]
- 9.Srinivasan K.G., Gaikwad A., Ritesh K., Ushanandini K.P. Giant omental and mesenteric lipoma in an infant. Afr J Paediatr Surg. 2009;6(1):68. doi: 10.4103/0189-6725.48585. [DOI] [PubMed] [Google Scholar]
- 10.Murphey M.D., Carroll J.F., Flemming D.J., Pope T.L., Gannon F.H., Kransdorf M.J. From the archives of the AFIP: benign musculoskeletal lipomatous lesions. Radiographics. 2004;24(5):1433–1466. doi: 10.1148/rg.245045120. [DOI] [PubMed] [Google Scholar]
- 11.Brazilai M., Biterman A. Two sonographic presentations of giant retroperitoneal lipomas. J Diagn Med Sonogr. 1997;13:140–142. [Google Scholar]
- 12.Pereira J.M., Sirlin C.B., Pinto P.S., Casola G. CT and MR imaging of extrahepatic fatty masses of the abdomen and pelvis: techniques, diagnosis, differential diagnosis, and pitfalls. Radiographics. 2005;25:69–85. doi: 10.1148/rg.251045074. [DOI] [PubMed] [Google Scholar]
- 13.Méndez-Uriburu L., Ahualli J., Méndez-Uriburu J., Méndez-Uriburu M., Fajre L., Méndez-Uriburu F. CT appearances of intraabdominal and intrapelvic fatty lesions. Am J Roentgenol. 2004;183(4):933–943. doi: 10.2214/ajr.183.4.1830933. [DOI] [PubMed] [Google Scholar]
- 14.Ishida H., Ishida J. Primary tumours of the greater omentum. Eur Radiol. 1998;8:1598–1601. doi: 10.1007/s003300050594. [DOI] [PubMed] [Google Scholar]
- 15.Weitzner S., Blumenthal I.B., Moynihan P.C. Retroperitoneal lipoma in children. J Pediatr Surg. 1979;14:88–90. doi: 10.1016/s0022-3468(79)80585-0. [DOI] [PubMed] [Google Scholar]