Abstract
Objective
Despite progress to reduce the burden of tobacco, disparities in tobacco-related morbidity and mortality remain. This research examines trends in lung cancer incidence rates by race and by gender within race during 2001–2010 in Oklahoma.
Methods
Incident cases of lung cancer were obtained from the Oklahoma State Department of Health public use database. Cases were linked to the Indian Health Service database to reduce misclassification of American Indian race. Annual percent change (APC) was estimated by race and by gender within race to describe rates over time. Rates were considered to increase or decrease if the p-value for trend was <0.05.
Results
Average lung cancer incidence rates were highest among American Indians (105.52 per 100,000) and lowest among whites (78.64 per 100,000). Lung cancer incidence rates declined among the overall white (APC:−2.17%; p=0.001) and African American (APC:−2.95%; p=0.003) populations, as well as white (APC:−3.02%; p<.001) and African American males (APC:−3.39%; p=0.007). Rates increased among American Indian females (APC: 2.20%; p=0.03).
Conclusion
Analysis of lung cancer incidence data reveals an inequality in tobacco-related morbidity among American Indians, especially American Indian females. This research suggests a need for more evidence-based tobacco control interventions within the American Indian population.
Keywords: lung cancer, disparities, race, gender, tobacco, cigarette smoking, epidemiology
INTRODUCTION
Evidence-based strategies in tobacco control such as cessation services including state quitlines, tobacco excise taxes, smoke-free laws, and media counter-advertising have, in large part, contributed to reductions in cigarette smoking over the past few decades. Despite substantial declines, cigarette smoking is responsible for more than 480,000 deaths each year in the US alone.1 Moreover, disparities in cigarette smoking prevalences, and tobacco-related morbidity and mortality remain, rendering public health’s attention.
Lung cancer, a sentinel health consequence of cigarette smoking, is the second most commonly diagnosed cancer in the US and varies by gender and race.1 Due to the well-established causal relationship between cigarette smoking and lung cancer, lung cancer is often monitored to understand the impact of tobacco control and prevention efforts and to identify disparate populations. Recently, the Centers for Disease Control and Prevention (CDC) examined trends in lung cancer incidence among US men and women from 2005 to 2009.2 The CDC report identified statistically significant declines in lung cancer incidence and a narrowing of the gender gap in lung cancer incidence,2 a reflection of male cigarette smoking prevalences becoming increasingly more similar to that of females in recent decades.
Although lung cancer incidence is decreasing overall, and becoming increasingly more similar across gender, less is known about recent patterns in lung cancer by race or ethnicity. Race and ethnic analyses of US lung cancer incidence during 1996–2005 indicated statistically significant declines within men in all subgroups examined and mostly stable trends within women in all subgroups examined.3 This research illustrates the impact of anti-tobacco efforts and the necessity for more tailored interventions among women. Despite the meaningful findings, the research is somewhat dated and limited since the authors did not examine trends in lung cancer incidence among American Indians, a population with historically high prevalences of cigarette smoking.4,5 Due to the high percentage of American Indians in the state of Oklahoma (9.0%), nearly 8 times that of the US (1.2%),6 Oklahoma serves as an ideal study population for better understanding trends in lung cancer by race, including American Indians. Therefore, the purpose of this research was to examine trends in lung cancer incidence rates by race and by gender within race for the most recent 10-year period (2001–2010) in Oklahoma.
METHODS
Data on Oklahoma’s incident cases of lung, including bronchus, cancer (2001–2010) were obtained from the Oklahoma Central Cancer Registry via the Oklahoma State Department of Health OK2SHARE public use database.7 Invasive lung and bronchus cancer cases were identified by the third edition of the International Classification of Diseases for Oncology (ICD-O) codes C340-C349, excluding the following histologies: mesothelioma, Kaposi sarcoma and hematopoietic diseases (M-9050-9055, 9140, 9590-9989).8 Cases were linked to the Indian Health Service (IHS) database to reduce misclassification of American Indian race. 9–11 Denominators for the incidence rates, populations at risk, were bridged-race population estimates of the July 1 resident population prepared by the Census Bureau in collaboration with the National Center for Health Statistics and obtained from the CDC WONDER online database.12 Incidence rates were calculated per 100,000 population and age-adjusted to the 2000 US standard population using the direct method of standardization. Annual percent change (APC) was estimated by least-squares linear regression on a log-linear scale to describe trends in lung cancer incidence rates over time. Rates were considered to increase or decrease if the p-value for trend was <0.05. APCs were calculated by race (white, African American, and American Indian) and by gender within race (white males, white females, African American males, African American females, American Indian males, and American Indian females). Race is inclusive of both Hispanic and non-Hispanic origin, as recommended by the Surveillance, Epidemiology, and End Results Program.13 Male to female lung cancer incident rate ratios were calculated to estimate gender-related disparity gaps in lung cancer incident rates. All analyses were conducted in 2014.
RESULTS
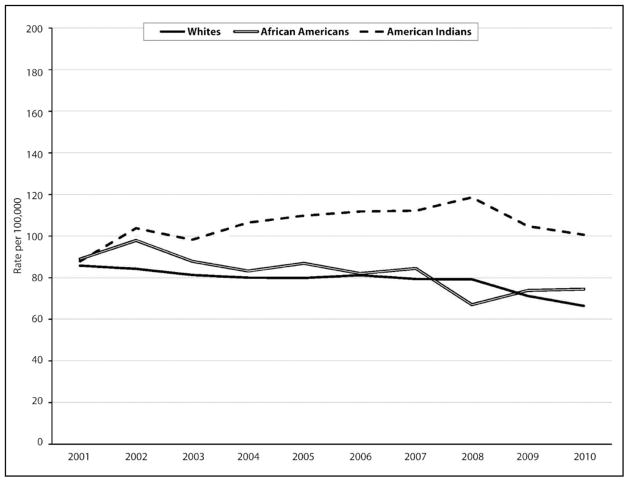
During 2001–2010, a total of 31,076 incident cases of lung cancer were reported among residents of Oklahoma. More cases of incident lung cancer were reported among whites (n=26,747) than both African Americans (n=1,630) and American Indians (2,410). During the same time period, average lung cancer incidence rates were higher among American Indians (105.52 per 100,000) than whites (78.64 per 100,000) and African Americans (82.10 per 100,000) (Table 1). Among whites and African Americans, rates of incident lung cancer were lower in 2010 compared to 2001; whereas, among American Indians rates were lowest in 2001 (Figure 1).
Table 1.
Age-adjusted rates of lung cancer incidence per 100,000 population by race and by gender within race, Oklahoma 2001–2010
| 2001 | 2002 | 2003 | 2004 | 2005 | 2006 | 2007 | 2008 | 2009 | 2010 | Avg. | |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Whites | |||||||||||
| Overall | 85.8 | 84.3 | 81.3 | 80.0 | 79.9 | 81.2 | 79.3 | 79.2 | 71.2 | 66.4 | 78.6 |
| Male | 115.0 | 110.1 | 107.0 | 100.5 | 101.7 | 99.3 | 103.4 | 96.1 | 90.0 | 80.9 | 99.9 |
| Female | 64.5 | 65.1 | 62.5 | 64.6 | 63.3 | 68.1 | 61.2 | 66.3 | 56.4 | 55.1 | 62.6 |
| African Americans | |||||||||||
| Overall | 89.0 | 97.9 | 87.9 | 83.3 | 86.9 | 82.0 | 84.4 | 67.1 | 73.9 | 74.5 | 82.1 |
| Male | 129.5 | 141.7 | 114.8 | 125.1 | 125.9 | 118.3 | 117.7 | 95.9 | 92.1 | 109.3 | 116.1 |
| Female | 60.9 | 66.9 | 69.3 | 53.7 | 59.4 | 54.4 | 59.6 | 45.3 | 59.4 | 51.3 | 57.7 |
| American Indians | |||||||||||
| Overall | 87.9 | 103.7 | 98.2 | 106.5 | 109.7 | 111.8 | 112.1 | 118.6 | 104.8 | 100.6 | 105.5 |
| Male | 103.5 | 130.0 | 129.0 | 140.4 | 124.5 | 134.6 | 148.6 | 150.1 | 116.2 | 117.8 | 130.0 |
| Female | 76.4 | 84.2 | 75.8 | 82.8 | 98.1 | 94.3 | 86.4 | 96.7 | 95.3 | 89.4 | 88.2 |
Abbreviation: Avg, 2001–2010 Average
Figure 1.
Age-adjusted rates of lung cancer incidence per 100,000 by race, Oklahoma 2001–2010. Source: Oklahoma State Department of Health OK2SHARE public use database and CDC WONDER online database
Within males, American Indians, followed by African Americans, have the highest average lung cancer incidence rate. Within females, American Indians, followed by whites, have the highest lung cancer incidence rate, on average. For all races, males have higher rates of incident lung cancer than females. The most apparent gender gap is among African Americans, with a rate ratio of the average (2001–2010) lung cancer incidence rate among males (116.08 per 100,000) to females (57.66 per 100,000) of 2.01, followed by whites and American Indians with rate ratios of 1.60 and 1.47, respectively.
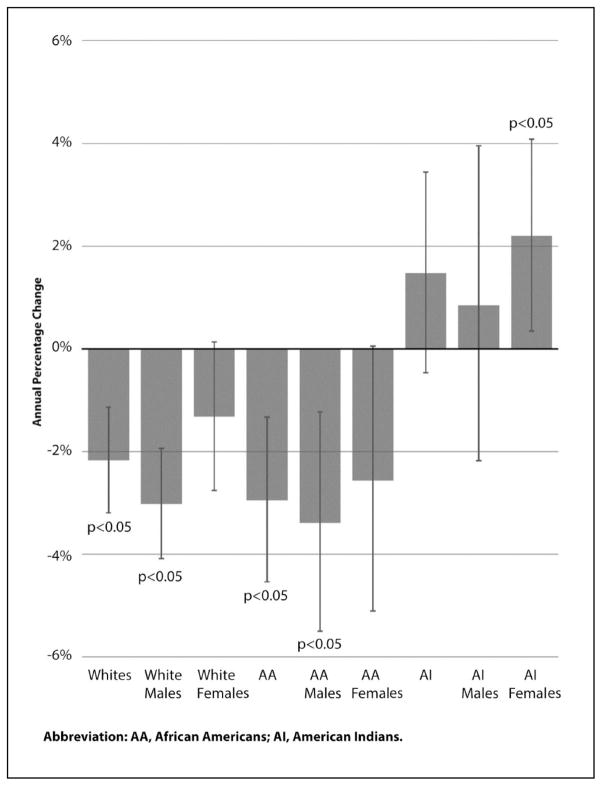
Declines in lung cancer incidence rates were observed among whites and African Americans, but not among American Indians, from 2001 through 2010 (Figure 2). During this time period, lung cancer incidence rates declined among whites with an annual percent change (APC) of −2.17% (95% Confidence Interval (CI): −3.19, −1.13; p=0.001) and among African Americans with an APC of −2.95% (CI: −4.54, −1.33; p=0.003). Lung cancer incidence rates was stable among American Indians (APC: 1.47%; CI: −0.46, 3.44; p=0.12).
Figure 2.
Annual percent change in lung cancer incidence rates by race and gender within race groups, Oklahoma 2001–2010. Source: Oklahoma State Department of Health OK2SHARE public use database and CDC WONDER online database.
Within males, declines in lung cancer incidence rates were observed among whites and African Americans with APCs of −3.02% (CI: −4.08, −1.94; p<.001) and −3.39% (CI: −5.50, −1.23; p=0.007), respectively. Within females, an increase of 2.20% (CI: 0.35, 4.08; p=0.03) per year was observed among American Indians. Stable trends were observed for American Indian males (APC: 0.84%; CI:−2.18, 3.96; p=0.12), white females (APC: −1.32; CI: −2.76, 0.14; p=0.07), and African American females (APC: −2.56%; CI: −5.10, 0.05; p=0.05).
DISCUSSION
This research documents trends in lung cancer incidence rates by race and by gender within race in the state of Oklahoma and reveals American Indians face an inequality in tobacco-related morbidity, as average lung cancer incidence rates during 2001 through 2010 are substantially higher among American Indians (105 per 100,000) than whites (79 per 100,000) or African Americans (82 per 100,000). Declines in lung cancer incidence rates of similar pace were observed for the overall white and African American populations, as well as white and African American males. In contrast, lung cancer incidence rates were stable among the American Indian population and even increased among American Indian females. Since the vast majority of lung cancer cases are attributed to cigarette smoking,1 changes in lung cancer incidence rates can be attributed to changes in exposure to cigarette smoking, after accounting for an estimated lag period between 5 and 20 years.14–16
Although the prevalence of US cigarette smoking has declined by almost half since the 1960s, several additional factors may explain the patterns of lung cancer in the present study. Traditionally, males have had much higher levels of cigarette smoking than females which have contributed to the male-female difference in lung cancer occurrence.17 In recent years the gender difference in smoking prevalences has increasingly narrowed due to quicker declines in smoking prevalences among men as compared to among women.17,18 For instance, from 2001 through 2010 current smoking declined −1.7% each year on average among males and −0.9% each year on average among females in the state of Oklahoma, resulting in a lower male to female ratio of smoking prevalence estimates in 2010 (1.13) when compared to 2001 (1.21).19 Subsequently, the gender gap in lung cancer is reported to be narrowing.2,20 When examining gaps in lung cancer incidence rate during 2001 through 2010 by gender, no noticeable change was observed among either African Americans or American Indians; whereas, the gender gap among whites reduced from 1.78 in 2001 to 1.47 in 2010. The present study confirms narrowing of the gender gap for whites, but not African Americans or American Indians, as lung cancer incidence rates are declining more quickly only among white males than white females.
Supporting previous literature,21 lung cancer occurrence is considerably higher among African American males than white males, but quite similar for African American females and white females. Higher smoking among African American males may explain the lung cancer difference between African American and white males.22 It is less clear why African American and whites females have comparable rates, as African American females tend to smoke the least.22 Previous studies have hypothesized menthol cigarettes, preferred by 69–76% of African Americans versus 20–23% of whites,23,24 may contribute to a higher lung cancer burden.21,25 However, current evidence, including a scientific evaluation by the US Food and Drug Administration, suggests no more risk for disease, including lung cancer, among smokers of menthol compared to non-menthol cigarettes.26–28 Public health should place priority on monitoring race-specific trends in lung cancer and testing new hypotheses to better understand the persistent lung cancer discrepancy between African Americans and whites.
The prevalence of smoking among both male and female American Indians has been persistently high, and shown to vary substantially by geography.29 For instance, the 1999–2005 average adult current smoking prevalence among American Indians varied by Indian Health Service (IHS) region from 19.6 to 43.6, and was higher for American Indians (35.8), regardless of IHS region, than that of non-Hispanic whites (22.6).29 Subsequently, lung cancer incidence rates vary up to 7-fold across IHS regions with the highest rates observed in the Northern and Southern Plains, which includes Oklahoma, and Alaska.30 In the present study, rates of incident lung cancer are highest among American Indians and not declining. Even worse, the female American Indian population shows an increase in the rate of incident lung cancer of more than 2% per year on average. These undesirable patterns among American Indians reflect sustained high levels of cigarette smoking, and illustrate an urgent need for more tailored evidence-based interventions among this at-risk population.
The results and their interpretations are subject to a few limitations. First, delays in cancer reporting may result in biased, underestimated, incidence rates. Second, results were not presented by Hispanic origin due to the small number of cases reported each year. Third, denominators for the incidence rates, populations at risk, were estimated by the US Census Bureau. If errors occurred in reporting of the population this could result in biased incidence rates. Also, populations at risk were not IHS linked, resulting in incidence rates that are likely underestimated for whites and overestimated for American Indians. Finally, results among American Indians may not be generalizable, as Oklahoma’s American Indian population may be fundamentally different from others. Strengths of this study include that it is the most recent analysis of lung cancer incidence data by race, including a sufficient number of American Indian cases, and the utilization of linked data to correct for some misclassification of race, resulting in improved accuracy of lung cancer incidence rates.
CONCLUSIONS
This research documents 10-year trends in lung cancer incidence rates in the state of Oklahoma and reveals persistent and growing disparities by race and by gender within race. American Indians face an inequality in tobacco-related morbidity, as lung cancer incidence rates during 2001 through 2010 are highest among American Indians and not declining, unlike patterns among whites and African Americans. Moreover, results demonstrate an increasing pattern of lung cancer among American Indian females and an urgent need for more tailored evidence-based interventions among this at-risk population.
Acknowledgments
This study was funded by the Oklahoma Tobacco Research Center.
Footnotes
The authors declare that there is no conflict of interests regarding the publication of this paper.
References
- 1.US Department of Health, Human Services. The health consequences of smoking—50 years of progress: A report of the surgeon general. Atlanta, GA: US Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health; 2014. p. 17. [Google Scholar]
- 2.Centers for Disease Control and Prevention. Lung Cancer Incidence Trends Among Men and Women — United States, 2005–2009. MMWR. Morbidity and mortality weekly report. 2014;63(1):1–5. [PMC free article] [PubMed] [Google Scholar]
- 3.Jemal A, Simard EP, Dorell C, et al. Annual Report to the Nation on the Status of Cancer, 1975–2009, Featuring the Burden and Trends in Human Papillomavirus (HPV)–Associated Cancers and HPV Vaccination Coverage Levels. Journal of the National Cancer Institute. 2013 Feb 6;105(3):175–201. doi: 10.1093/jnci/djs491. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Eichner JE, Cravatt K, Beebe LA, et al. Tobacco use among American Indians in Oklahoma: an epidemiologic view. Public health reports (Washington, DC: 1974) 2005 Mar-Apr;120(2):192–199. doi: 10.1177/003335490512000214. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Cobb N, Espey D, King J. Health behaviors and risk factors among American Indians and Alaska Natives, 2000–2010. Am J Public Health. 2014 Jun;104(Suppl 3):S481–489. doi: 10.2105/AJPH.2014.301879. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.U.S. Census Bureau. Data derived from Population Estimates, Census of Population and Housing, Small Area Income and Poverty Estimates, State and County Housing Unit Estimates, County Business Patterns, Nonemployer Statistics, Economic Census, Survey of Business Owners, Building Permits, Consolidated Federal Funds Report. State and County QuickFacts. [Google Scholar]
- 7.Oklahoma State Department of Health (OSDH), Disease, Prevention, & Preparedness Service, Chronic Disease Service, Oklahoma Central Cancer Registry (OCCR) [Accessed September 10, 2014];on Oklahoma Statistics on Health Available for Everyone (OK2SHARE) 2010 http://www.health.ok.gov/ok2share.
- 8.Fritz AG. International classification of diseases for oncology: ICD-O. World Health Organization; 2000. [Google Scholar]
- 9.Wiggins CL, Espey DK, Wingo PA, et al. Cancer among American Indians and Alaska Natives in the United States, 1999–2004. Cancer. 2008 Sep 1;113(5 Suppl):1142–1152. doi: 10.1002/cncr.23734. [DOI] [PubMed] [Google Scholar]
- 10.Anderson RN, Copeland G, Hayes JM. Linkages to Improve Mortality Data for American Indians and Alaska Natives: A New Model for Death Reporting? American Journal of Public Health. 2014 Jun;104:S258–S262. doi: 10.2105/AJPH.2013.301647. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Espey DK, Jim MA, Richards TB, Begay C, Haverkamp D, Roberts D. Methods for improving the quality and completeness of mortality data for American Indians and Alaska Natives. Am J Public Health. 2014 Jun;104(Suppl 3):S286–294. doi: 10.2105/AJPH.2013.301716. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.United States Department of Health and Human Services (US DHHS), Centers for Disease Control and Prevention(CDC), National Center for Health Statistics (NCHS) Bridged-Race Population Estimates, United States July 1st resident population by state, county, age, sex, bridged-race, and Hispanic origin. Compiled from 1990–1999 bridged-race intercensal population estimates (released by NCHS on 7/26/2004); revised bridged-race 2000–2009 intercensal population estimates (released by NCHS on 10/26/2012); and bridged-race Vintage 2013 (2010–2013) postcensal population estimates (released by NCHS on 6/26/2014) [Accessed Sep 24, 2014]; Available on CDC WONDER Online Database. http://wonder.cdc.gov/bridged-race-v2013.html.
- 13.Surveillance, Epidemiology, and End Results Program. Race Recode Changes For the 1973–2005 SEER Research Data (November 2007 Submission) and Later Releases. [Accessed Oct 20 2014]; http://seer.cancer.gov/seerstat/variables/seer/race_ethnicity/
- 14.Alberg AJ, Samet JM. EPidemiology of lung cancer*. CHEST Journal. 2003;123(1_suppl):21S–49S. doi: 10.1378/chest.123.1_suppl.21s. [DOI] [PubMed] [Google Scholar]
- 15.Toh C-K. Cancer Epidemiology. Springer; 2009. The changing epidemiology of lung cancer; pp. 397–411. [DOI] [PubMed] [Google Scholar]
- 16.Jemal A, Cokkinides VE, Shafey O, Thun MJ. Lung Cancer Trends in Young Adults: An Early Indicator of Progress in Tobacco Control (United States) Cancer Causes & Control. 2003;14(6):579–585. doi: 10.1023/a:1024891201329. [DOI] [PubMed] [Google Scholar]
- 17.Anderson CM, Burns DM, Dodd KW, Feuer EJ. Chapter 2: Birth-cohort-specific estimates of smoking behaviors for the U.S. population. Risk analysis: an official publication of the Society for Risk Analysis. 2012 Jul;32(Suppl 1):S14–24. doi: 10.1111/j.1539-6924.2011.01703.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Fiore MC, Novotny TE, Pierce JP, Hatziandreu EJ, Patel KM, Davis RM. Trends in cigarette smoking in the united states: The changing influence of gender and race. JAMA. 1989;261(1):49–55. [PubMed] [Google Scholar]
- 19.Beebe LA, Mushtaq N. Trends in cigarette smoking – Oklahoma BRFSS 2001–2010. Department of Biostatistics and Epidemiology, University of Oklahoma College of Public Health; 2011. [Google Scholar]
- 20.Thun MJ, Carter BD, Feskanich D, et al. 50-year trends in smoking-related mortality in the United States. The New England journal of medicine. 2013 Jan 24;368(4):351–364. doi: 10.1056/NEJMsa1211127. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Alberg AJ, Brock MV, Samet JM. Epidemiology of lung cancer: looking to the future. Journal of clinical oncology: official journal of the American Society of Clinical Oncology. 2005 May 10;23(14):3175–3185. doi: 10.1200/JCO.2005.10.462. [DOI] [PubMed] [Google Scholar]
- 22.American Lung Association. Epidemiology and Statistics Unit, Research and Scientific Affairs. American Lung Association; 2011. Trends in tobacco use. [Google Scholar]
- 23.Giovino GA, Sidney S, Gfroerer JC, et al. Epidemiology of menthol cigarette use. Nicotine & tobacco research: official journal of the Society for Research on Nicotine and Tobacco. 2004 Feb;6(Suppl 1):S67–81. doi: 10.1080/14622203710001649696. [DOI] [PubMed] [Google Scholar]
- 24.Stahre M, Okuyemi KS, Joseph AM, Fu SS. Racial/ethnic differences in menthol cigarette smoking, population quit ratios and utilization of evidence-based tobacco cessation treatments. Addiction (Abingdon, England) 2010 Dec;105(Suppl 1):75–83. doi: 10.1111/j.1360-0443.2010.03200.x. [DOI] [PubMed] [Google Scholar]
- 25.Clark PI, Gardiner PS, Djordjevic MV, Leischow SJ, Robinson RG. Menthol cigarettes: setting the research agenda. Nicotine and Tobacco Research. 2004;6:S5–S10. doi: 10.1080/14622200310001649441. [DOI] [PubMed] [Google Scholar]
- 26.Blot WJ, Cohen SS, Aldrich M, McLaughlin JK, Hargreaves MK, Signorello LB. Lung cancer risk among smokers of menthol cigarettes. Journal of the National Cancer Institute. 2011 May 18;103(10):810–816. doi: 10.1093/jnci/djr102. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Brooks DR, Palmer JR, Strom BL, Rosenberg L. Menthol cigarettes and risk of lung cancer. American journal of epidemiology. 2003 Oct 1;158(7):609–616. doi: 10.1093/aje/kwg182. discussion 617–620. [DOI] [PubMed] [Google Scholar]
- 28.US Food Drug Administration. Preliminary scientific evaluation of the possible public health effects of menthol versus nonmenthol cigarettes. Jul, 2013. [Google Scholar]
- 29.Espey DK, Wu X-C, Swan J, et al. Annual report to the nation on the status of cancer, 1975–2004, featuring cancer in American Indians and Alaska Natives. Cancer. 2007;110(10):2119–2152. doi: 10.1002/cncr.23044. [DOI] [PubMed] [Google Scholar]
- 30.Bliss A, Cobb N, Solomon T, et al. Lung cancer incidence among American Indians and Alaska Natives in the United States, 1999–2004. Cancer. 2008 Sep 1;113(5 Suppl):1168–1178. doi: 10.1002/cncr.23738. [DOI] [PMC free article] [PubMed] [Google Scholar]