Abstract
Purpose
The purpose of this study is to determine the relationship between target clarity and the magnitude of accommodative lag using the metric accommodative gain (AG).
Methods
Monocular accommodative responses were measured with Grand Seiko autorefraction using both proximal and minus lens techniques in 139 subjects 5–35 years old. Subjects viewed a 1.5mm letter at 13 discrete distances (range = 40 – 3.33cm) for the proximal technique and fixed at 33cm through minus lenses of increasing power for the lens technique. Subjects were instructed to keep the target clear and report when it blurred. The AG was calculated (accommodative response / accommodative demand) for the four greatest consecutive demands perceived clear (termed conditions 1–4) and the first demand perceived blurry (termed condition 5).
Results
Multivariate planned contrast, including age as a predictor, revealed mean AG was significantly larger when the target was clear (range = 0.71 to 0.77 for conditions 1–4 across techniques) versus blurry (0.59 and 0.68 for condition 5 across techniques) (p<0.001 for proximal and p<0.036 for lens). Age was only a contributing factor for the proximal technique with youngest subjects having the largest decrease in AG when the target changed from clear to blurry (p=0.017).
Conclusions
These data suggest that across age and technique, the AG is relatively constant when the target is perceived clear, but drops below ~70%, on average, once the target is perceived as blurry for subjects ranging from 5 to 35 years of age. The AG may be a useful metric to compare accommodative responses across a range of demands and to identify accommodative responses which may not be sufficient to perceive a clear target.
Keywords: accommodation, accommodative lag, accommodative response, accommodative accuracy, blur, accommodative gain
Accommodative response is often described in terms of accuracy relative to accommodative demand, with a typical response being less than the demand and termed an accommodative lag. Clinical and laboratory-based studies have both established that as accommodative demand increases, accommodative lag increases as well.1–4 This has been observed in both children and adults2, 3, 5, 6 and when using methodology that increases the demand through changes in physical stimulus position,2, 3, 6 or through introduction of negative lenses before the viewing eye.2–4
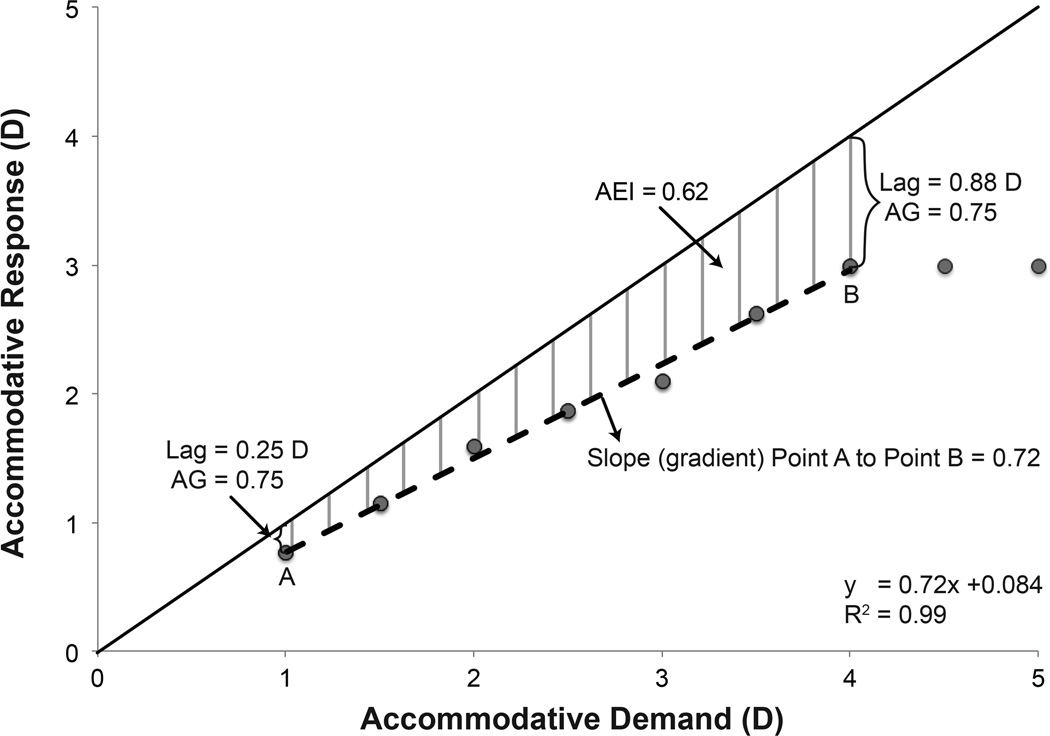
Accommodative accuracy can be quantified using a variety of techniques (Figure 1). When a response is measured for a single demand, accommodative accuracy can be represented as the magnitude of the accommodative lag (accommodative demand–accommodative response), or as an accommodative gain (AG) (ratio of the accommodative response/accommodative demand). When multiple demands are tested, the accommodative lag or gain can be calculated for each response, or the responses can be plotted graphically to create an accommodative stimulus response curve (ASRC), which is typically sigmoidal in shape, having two non-linear portions at the ends of the curve connected by a linear portion.7 Accommodative accuracy can be described by the components of the equation of a regression line fit to the linear portion of the ASRC: slope, y-intercept, and correlation. These components can then be used to calculate the accommodative error index (area between the linear portion of the ASRC and the unity line).8 The slope of the linear regression has also been utilized in isolation to compare accommodative performance across individuals; however, this metric does not fully capture the accuracy of the response since it does not account for the offset of the response from the unity line.
Figure 1.
Theoretical accommodative stimulus response curve representing possible ways to describe the accommodative response over multiple accommodative demands using accommodative lag, accommodative gain (AG), slope (gradient) of the linear portion of the response, and the accommodative error index (AEI).
Clinicians typically measure the magnitude of the accommodative lag for one given demand, the patient’s habitual near working distance,9 and compare the finding to a fixed cut-off (+0.75 diopters(D))10 derived from normative data. Two issues worth evaluating regarding this strategy is that the same cut-off is applied to all individuals regardless of working distance and secondly, the relationship between the magnitude of accommodative lag and blurred near vision has not been previously established. Regarding the use of habitual working distances, a non-presbyopic adult may perform a near task at 40cm (demand = 2.5D), whereas a child may perform a near task at 20cm (demand = 5D). Because the accommodative lag increases with demand, the use of various working distances makes it difficult to compare accommodative accuracy in terms of dioptric magnitude across individuals. Conversely, if accommodative accuracy of individuals of differing ages is compared for the same demand, these individuals will be functioning in a different portion of their ASRC due to differences in accommodative amplitude with age, resulting in greater accommodative lags at higher demands. Regarding the magnitude of lag associated with blur, as observed by Morgan (1944), one would expect accommodative lag to increase when the target is perceived blurred.11 Previous studies have looked at the accommodative response at various demands,1–4,6,8 yet there has not been a study that has investigated the simultaneous subjective response regarding target clarity and the magnitude of the accommodative lag for a given demand in a large sample of subjects ranging from childhood into adulthood. Therefore we determined that making comparisons of AG for multiple demands that are referenced to a common point in the ASRC (the first blur point) would allow comparison of different demands across subjects within common portions of the ASRC without necessitating a fit to the data.
The purpose of this study was to determine whether the AG differed significantly at demands when the target was perceived as clear versus when it first became blurry. Secondly, we sought to determine whether the AG differed with age from preschool to adulthood in non-presbyopic subjects across different accommodative demands for clear versus blurry stimuli. Lastly, we sought to determine whether the AG differed when accommodation was stimulated by moving the target closer versus stimulating accommodation with minus lenses.
METHODS
Study Subjects
Subjects were recruited from the University of Houston College of Optometry staff, student, and patient populations and their family members. The study followed the tenets of the declaration of Helsinki and was approved by the University’s institutional review board for the protection of human subjects. All subjects over age 18 provided informed consent. Subjects younger than 18 provided assent and their parents provided written parental permission.
The subjects in this study represent a subset from a larger study of accommodative amplitude12 in 3 to 64 year old subjects, using both a proximal technique and a minus lens technique. For inclusion in the present analysis, subjects had to be age 5 to 35 (inclusive), wearing refractive correction (if needed), and have given a subjective report of the accommodative demand for which the target (letter) became blurry during both measurement techniques. Subjects were excluded from participation if they had a history of eye or head injuries, intraocular surgery, strabismus, ocular pathology, or were taking medications known to alter accommodation. Subjects were also excluded if their presenting best-corrected distance visual acuity was worse than 20/25 on an age appropriate chart (Snellen for older subjects and Lea symbols13 for younger subjects) presented on an M&S SmartSystem (M&S Technologies, Inc. Niles, IL).
Subjects wore habitual correction (contact lenses, spectacles, or unaided) for all study measures and had a right eye spherical equivalent refractive error range spanning −11.00 to +2.00 DS. Subjects (n=139) were categorized by refractive error into 4 groups based on spherical power of the right eye: hyperopia (≥+1.00DS, n=9), emmetropia (−0.75 to +1.00DS with <1D of cylinder, n=65), myopia (≤−0.75DS, n=61), and astigmatism (spherical power no greater than ±0.50DS with ≥−1.00D cylinder, n=4). Distance over-refraction was performed with the Grand Seiko WAM-5500® open-field autorefractor (RyuSyo Industrial Co., Ltd. Hiroshima, Japan) set to measure the corneal plane to ensure subjects did not manifest large amounts of uncorrected refractive error (group mean±sd spherical equivalent over-refraction = 0.11±0.43D, range = −0.95 to +1.06D).
Monocular accommodative responses were measured objectively with the Grand Seiko as accommodative demand was increased using two different techniques performed in random order (proximal & lens). The Grand Seiko is capable of measuring refractive error up to −22D, which is beyond the level of anticipated accommodative responses.
Proximal Technique
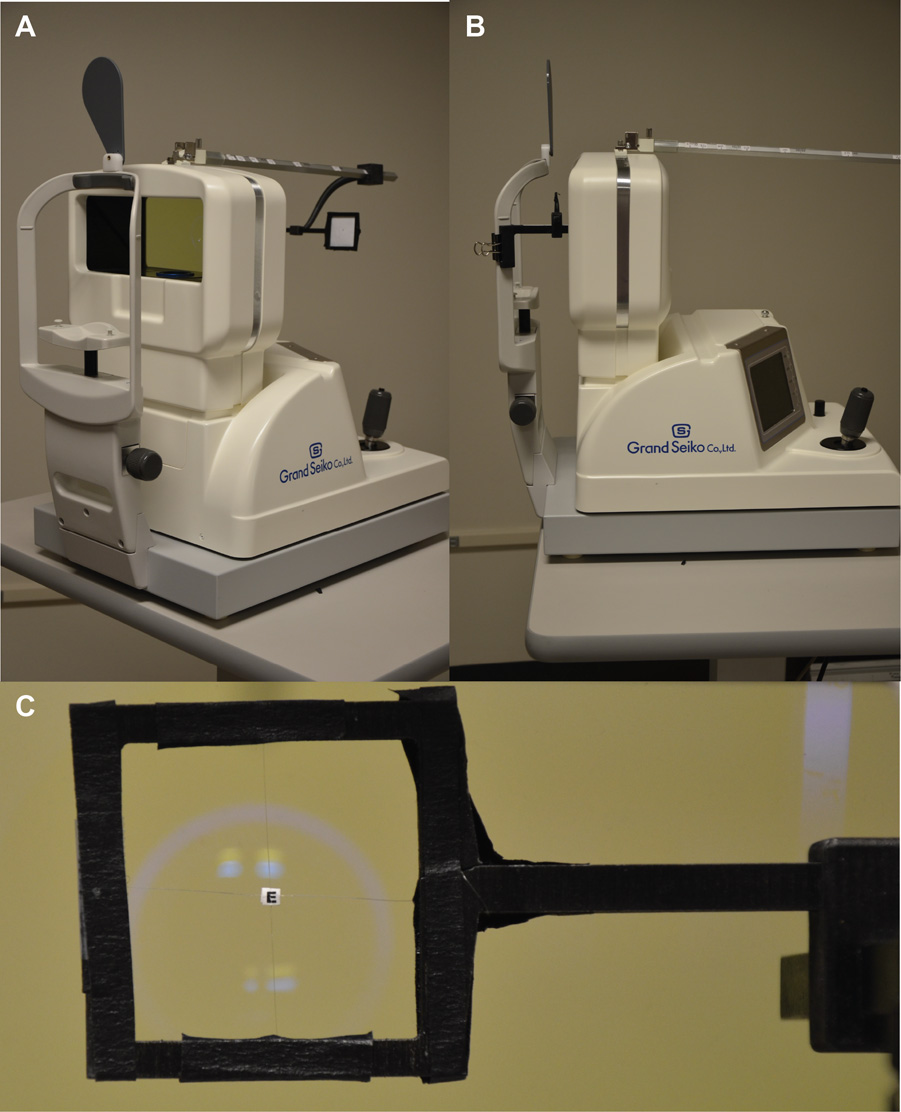
Each subject’s left eye was patched while viewing a 1.5mm letter “E” with their right eye. Accommodation was measured at fixed demands of 2.5, 3, 4, 5, 6, 7, 8, 10.5, 12, 15, 20, 25, and 30D. The target was suspended from the near point rod of the instrument (Figure 2a) at 40cm (2.5D) and then moved closer to the subject to eight discrete positions up to 9.5cm (10.5D), at which point the beam splitter prevented the target from being presented any closer along the near rod. The 1.5mm letter was then suspended by clear threads attached to the edges of an empty aperture and placed on the patient side of the beam splitter along a custom mount attached to the forehead rest (Figure 2b), allowing the target to be presented at five additional positions between 8 (12.5D) and 3.33cm (30.3D) without obstructing the measurement light of the autorefractor (Figure 2c). A book light was used to illuminate the target to ensure high contrast of the letter within the housing of the autorefractor. The average luminance of the target was 47.2(±0.84) cd/m2 when viewed on the investigator side of the housing and 83.2(±1.3) cd/m2 on the patient side of the housing. For all demands tested, subjects were asked to keep the target clear and to report when the target became slightly blurry, at which point the investigator asked the subject if the target remained blurry, or if they could make it clear. A given demand was classified as blurry once a subject confirmed that the target remained blurry. For young subjects, the word fuzzy was used in addition to blur to aid in patient comprehension. The young subjects are a subset from a previously published study of both subjective and objective accommodative amplitude,12 which reported excellent repeatability of subjective accommodative amplitude measures in the young children.
Figure 2.
Custom target mounts for proximal accommodative testing. (A) Target positioned on the investigator side of the beam splitter for demands from 2.5 to 10.5 D. (B) Target positioned on the subject side of the beam splitter for demands from 12.5 to 30 D. (C) Subject view of the printed letter Target for demands from 12 to 30 D. A color version of this figure is available online at www.optvissci.com. Reproduced with permission from Anderson HA, Stuebing KK. Subjective versus objective accommodative amplitude: preschool to presbyopia. Optom Vis Sci 2014;91:1290-301. ©The American Academy of Optometry 2014.
Lens Technique
Subjects wore a trial frame with left eye occluded and viewed the target at 33cm (3D demand). For subjects with spectacles, the sphero-cylindrical correction was placed in the trial frame in front of the viewing eye using an approximate vertex distance of 13mm. The subject first viewed the target in their habitual correction. Accommodative demand was increased in −1D steps by adding the appropriate powered lenses to the trial frame. If the subject had a habitual spectacle correction, the power of the demand was added to the spectacle lens power and placed in the trial frame to create the appropriate accommodative demand.
Subjects were asked to keep the target clear and report when it became and remained blurry (fuzzy). To determine the necessary maximum demand, the investigator monitored both the subject’s report of first sustained blur, as well as the accommodative response obtained with the Grand Seiko. When subjects accommodated accurately through the lenses, the Grand Seiko measured minus refraction values. Once subjects began to approach their maximum accommodative ability, refraction measures tended toward zero, ultimately becoming hyperopic when the maximum accommodative ability was exceeded. At this point, testing with the minus lens technique would cease, provided the first sustained blur response had been obtained. The maximum lens value used for any subject was −13D.
Data Exclusion
The Grand Seiko outputs spherical and cylindrical components of refractive error. Any measure containing >2D cylinder was excluded from analysis as it was likely due to poor subject fixation based on findings that the increase in astigmatism resulting from accommodation is <2D,15–17 and that the subjects in this experiment had low baseline amounts of uncorrected astigmatism in their habitual correction (mean −0.48±0.25D, range 0.00 to −1.27D).
Calculation of Accommodative Responses
Prior to data analysis, the first five measures of refractive error containing <2D cylinder were converted to spherical equivalent (1/2 cylindrical power + spherical power) and then averaged. Lens effectivity formulas were used to adjust both the refractive error measurements and the calculated accommodative demands for the effectivity of lenses placed in front of the measured/viewing eye.19 All of the demand and response values were referenced to the corneal plane using a 13mm vertex distance.
Calculation of the Accommodative Gain
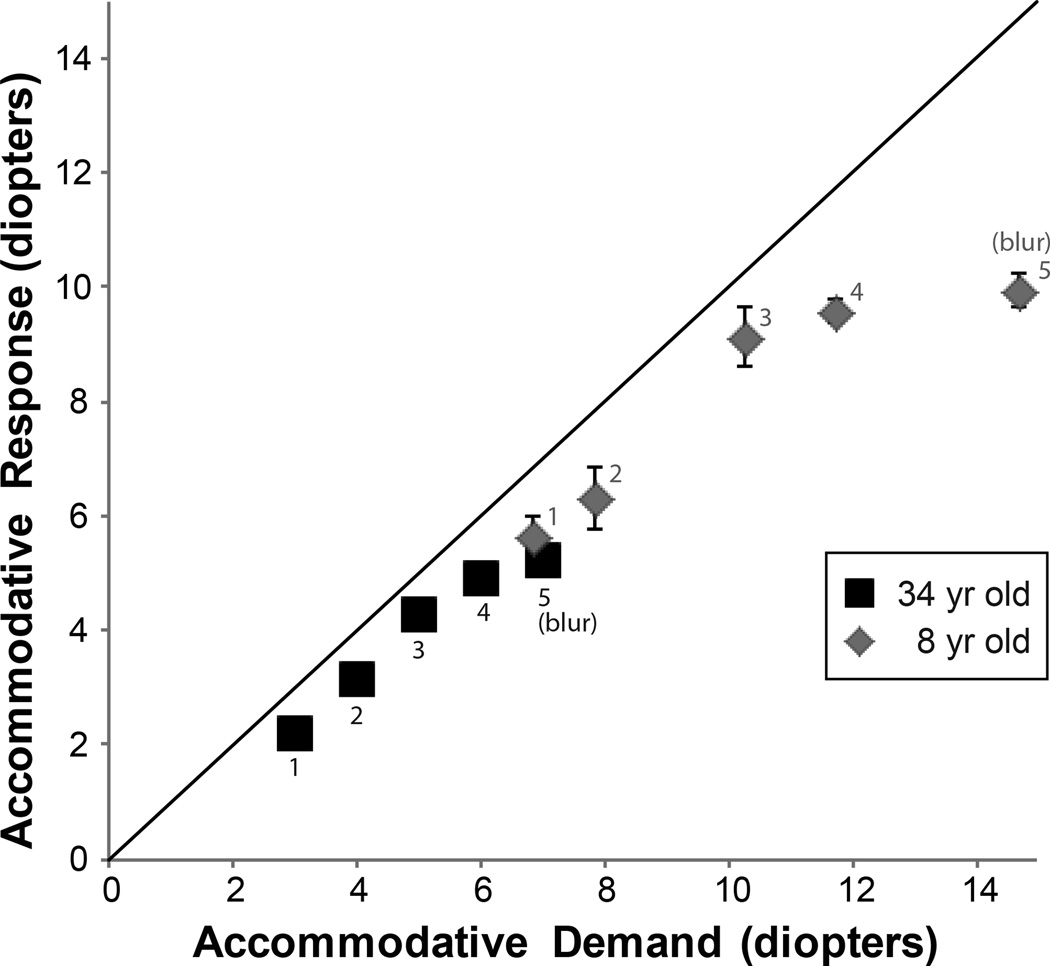
Subjects experienced blur at different accommodative demands due to both differences in age5 and their individual accommodative ability (Figure 3). The AG was calculated to represent the proportion of the demand met by the response of each subject for each demand. For example, if the accommodative demand was 10D and the measured accommodative response was 7.5D, the AG would be 0.75 (AG = 7.5D/10D). In effect, this ratio indicates the percentage of the demand met by the response.
Figure 3.
Representative accommodative responses (mean ± standard deviation) for an 8 year-old (diamonds) and a 34 year-old (squares) subject tested with the proximal technique. Numbers indicate the termed conditions for analysis with 1–4 representing a clear target perception and condition 5 representing a blurry target perception.
Data Analysis
The AG was calculated for the last four consecutive demands that each subject reported the target was clear (termed Conditions 1–4, with 1 being the lowest demand) and for the first demand the subject reported sustained blur of the target (Condition 5) (Figure 3). Thus, different demands were compared across subjects with a common reference point of blur dictating the upper demand. The AGs were analyzed using a mixed model approach to repeated measures to compare the AG across condition numbers, technique and subject age. Data analysis was performed using SAS version 9.3.19
RESULTS
One hundred and thirty-two subjects met inclusion criteria for the proximal technique (excluded subjects were 23 to 34 years) and 130 subjects met inclusion criteria for the lens technique (excluded subjects were 11 years and 32 to 35 years), leaving 126 subjects for comparison between both techniques. As described in the methods, the stimulus demands for Conditions 1–5 differed across subjects (Tables 1 & 2) as one would expect due to age-related changes in accommodative amplitude.
Table 1.
Proximal technique divided into age bins (5 years/bin). The mean and standard deviation for the accommodative response, accommodative demand and the accommodative (AG) are listed for each condition. AG was calculated by dividing the accommodative response by the accommodative demand for each individual.
| Age (years) |
Condition 1 | Condition 2 | Condition 3 | Condition 4 | Condition 5 | Condition 6* | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| AG | AG | AG | AG | AG | AG | ||||||||
| 5–9 | Response | 5.09±1.24 | 0.77±0.09 | 5.94±1.38 | 0.77±0.07 | 7.01±1.63 | 0.75±0.11 | 7.98±1.76 | 0.71±0.15 | 7.15±2.07 | 0.53±0.17 | 6.93±2.01 | 0.41±0.14 |
| Demand | 6.69±1.76 | 7.78±2.34 | 9.51±3.19 | 11.82±4.1 | 13.85±3.6 | 17.47±4.82 | |||||||
| 10–14 | Response | 4.83±0.95 | 0.77±0.09 | 5.68±1.52 | 0.77±0.13 | 7.01±1.96 | 0.78±0.12 | 7.83±2.05 | 0.73±0.13 | 7.33±2.83 | 0.55±0.19 | 7.00±2.82 | 0.43±0.16 |
| Demand | 6.21±0.92 | 7.29±1.12 | 8.87±1.67 | 10.63±2.0 | 13.13±2.5 | 16.57±3.89 | |||||||
| 15–19 | Response | 3.76±0.74 | 0.74±0.11 | 4.67±0.72 | 0.77±0.11 | 5.57±0.90 | 0.78±0.09 | 5.99±1.25 | 0.72±0.1 | 6.8±1.46 | 0.64±0.14 | 6.18±1.67 | 0.5±0.15 |
| Demand | 5.07±0.80 | 6.07±0.80 | 7.17±1.10 | 8.30±1.33 | 10.66±1.7 | 12.46±2.4 | |||||||
| 20–24 | Response | 3.38±0.88 | 0.74±0.13 | 4.12±1.04 | 0.74±0.14 | 4.75±1 | 0.73±0.12 | 5.21±1.11 | 0.69±0.13 | 5.68±1.73 | 0.6±0.16 | 5.62±2.16 | 0.5±0.19 |
| Demand | 4.50±0.81 | 5.50±0.81 | 6.49±0.81 | 7.58±1.04 | 9.38±1.56 | 11.19±1.67 | |||||||
| 25–29 | Response | 3.19±1.08 | 0.74±0.17 | 4.08±0.91 | 0.78±0.10 | 4.73±0.96 | 0.76±0.10 | 5.20±1.04 | 0.72±0.11 | 5.43±1.06 | 0.61±0.09 | 4.9±1.64 | 0.46±0.15 |
| Demand | 4.24±0.85 | 5.21±0.91 | 6.21±0.91 | 7.21±0.91 | 8.92±1.61 | 10.62±1.68 | |||||||
| 30–35 | Response | 2.71±0.86 | 0.75±0.09 | 3.45±0.96 | 0.76±0.07 | 4.09±1.01 | 0.74±0.1 | 4.53±0.93 | 0.70±0.12 | 4.51±1.1 | 0.58±0.14 | 4.51±0.96 | 0.5±0.12 |
| Demand | 3.59±0.98 | 4.47±1.12 | 5.48±1.22 | 6.47±1.12 | 7.86±1.72 | 9.26±2.01 | |||||||
(* Note that Conditions 1–5 included subjects that had data for all Conditions from 1–5 (n = 132), whereas Condition 6 included fewer subjects since not all subjects had data for condition 6 (n = 131)).
Table 2.
Lens technique divided into age bins (5 years/bin). The mean and standard deviation for the accommodative response, accommodative demand and the accommodative gain (AG) are listed for each condition. AG was calculated by dividing the accommodative response by the accommodative demand for each individual.
| Age (years) |
Condition 1 | Condition 2 | Condition 3 | Condition 4 | Condition 5 | Condition 6* | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| AG | AG | AG | AG | AG | AG | ||||||||
| 5–9 | Response | 4.97±1.75 | 0.78±0.11 | 5.41±1.78 | 0.75±0.10 | 6.11±1.58 | 0.76±0.07 | 7.00±1.67 | 0.76±0.07 | 6.56±2.12 | 0.67±0.18 | 6.82±1.28 | 0.68±0.09 |
| Demand | 6.30±1.74 | 7.15±1.70 | 8.00±1.66 | 8.79±1.62 | 9.58±1.59 | 9.87±1.11 | |||||||
| 10–14 | Response | 4.72±1.51 | 0.76±0.08 | 5.32±1.51 | 0.75±0.07 | 6.01±1.52 | 0.76±0.10 | 6.5±1.45 | 0.75±0.09 | 6.60±1.33 | 0.69±0.07 | 6.60±1.66 | 0.64±0.12 |
| Demand | 6.14±1.70 | 6.99±1.66 | 7.82±1.62 | 8.63±1.58 | 9.43±1.55 | 10.1±1.54 | |||||||
| 15–19 | Response | 3.81±1.38 | 0.73±0.10 | 4.69±1.33 | 0.77±0.08 | 5.32±1.32 | 0.77±0.07 | 5.91±1.26 | 0.76±0.06 | 5.97±1.41 | 0.69±0.10 | 6.06±1.71 | 0.65±0.13 |
| Demand | 5.14±1.50 | 6.01±1.46 | 6.87±1.43 | 7.70±1.40 | 8.51±1.37 | 9.23±1.35 | |||||||
| 20–24 | Response | 3.82±1.59 | 0.74±0.13 | 4.56±1.38 | 0.77±0.08 | 5.19±1.39 | 0.76±0.08 | 5.66±1.33 | 0.74±0.07 | 5.87±1.31 | 0.69±0.08 | 5.72±1.45 | 0.62±0.012 |
| Demand | 4.97±1.40 | 5.84±1.37 | 6.70±1.34 | 7.53±1.32 | 8.34±1.29 | 9.15±1.27 | |||||||
| 25–29 | Response | 3.29±1.04 | 0.76±0.12 | 4.03±1.01 | 0.78±0.09 | 4.71±1.09 | 0.78±0.10 | 5.19±1.05 | 0.75±0.09 | 5.11±1.13 | 0.66±0.1 | 5.04±1.35 | 0.59±0.13 |
| Demand | 4.19±0.81 | 5.09±0.79 | 5.96±0.77 | 6.81±0.76 | 7.65±0.74 | 8.47±0.73 | |||||||
| 30–35 | Response | 3.01±1.04 | 0.76±0.09 | 3.77±1.04 | 0.78±0.11 | 4.38±0.84 | 0.77±0.06 | 4.86±0.76 | 0.74±0.06 | 4.88±0.75 | 0.66±0.07 | 4.79±0.56 | 0.59±0.05 |
| Demand | 3.91±0.99 | 4.81±0.96 | 5.68±0.94 | 6.54±0.92 | 7.38±0.90 | 7.38±0.90 | |||||||
(* Note that Conditions 1–5 included subjects that had data for all Conditions from 1–5 (n = 130), whereas Condition 6 included fewer subjects since not all subjects had data for Condition 6 (n = 125)).
A multivariate planned contrast was first performed to assess the initial hypothesis that AG is significantly higher when the target is perceived as clear (Conditions 1–4) versus blurry (Condition 5). Subject age was included as a predictive variable to identify whether age was related to the differences in AG between clear and blurry conditions. AG (mean±sd) decreased significantly by 21% for the proximal technique (0.75±0.12 to 0.59±0.16, [F (1,130)=52.59, p<0.001]) and 11% for the lens technique (0.76±0.09 to 0.68±0.11, [F (1,128)=4.62, p<0.036]) when the subject perceived the target as being clear (average Conditions 1–4) versus blurry (Condition 5) (Figure 4). Age was only a significant factor for the proximal technique (F (1,130)=5.90, p=0.017) as the younger subjects had a larger decrease in AG once they perceived the target as blurry (Figure 5).
Figure 4.
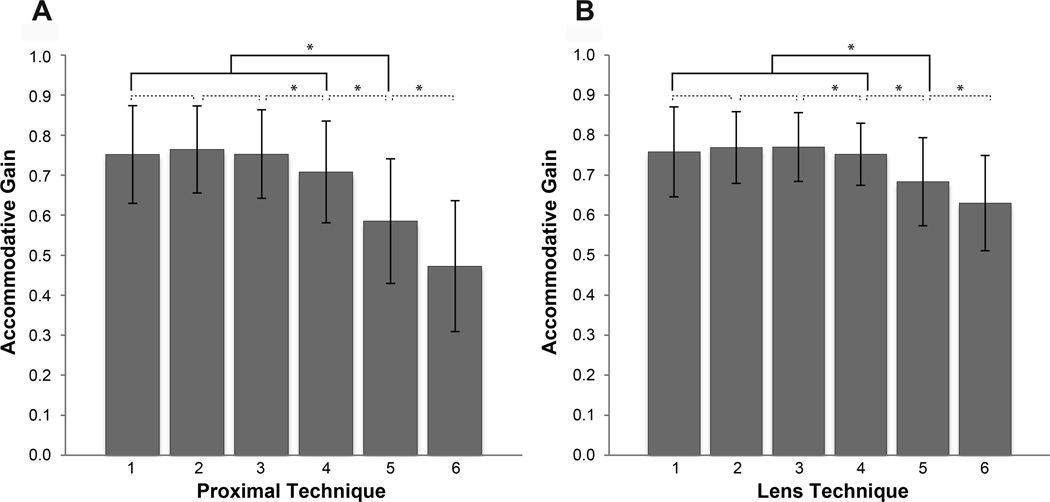
Accommodative gains (mean ± standard deviation) for each condition for both the proximal and minus lens techniques. The solid brackets represent the comparison of the mean of conditions 1–4 to condition 5 (Proximal technique: n = 132, Lens Technique: n = 130). The dashed lines represent the comparison of neighboring conditions (condition 1 to 2, 2 to 3, 3 to 4, 4 to 5 and 5 to 6; Proximal technique n = 131, Lens technique n = 125). The asterisks represent p < 0.05.
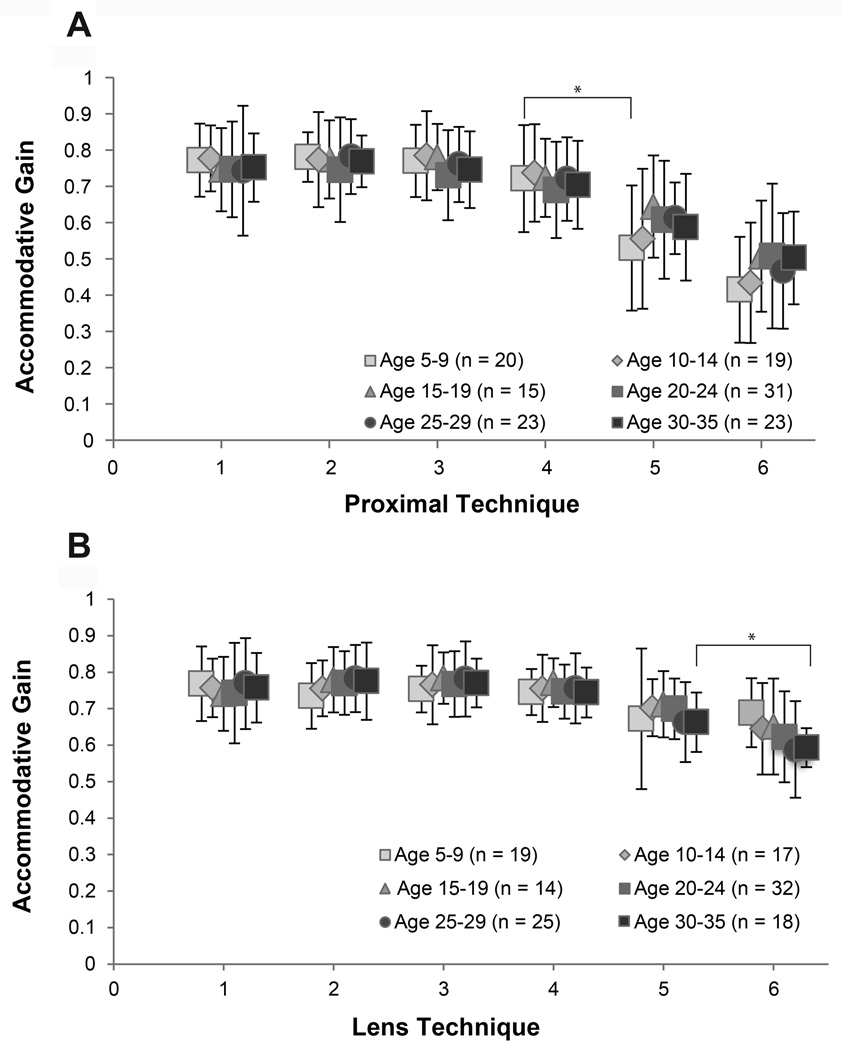
Figure 5.
Accommodative gains (mean ± standard deviation) grouped by age for both techniques (proximal & minus lens) to illustrate that the AG was similar across age with the exception that the AG decreased by a greater amount for the youngest age group when comparing conditions 4 and 5 for the proximal condition (asterisk represents p = 0.013) and the older age groups for the lens condition when comparing conditions 5 and 6 (asterisk represents p = 0.013). (Conditions 1–5 included subjects that had data for all Conditions from 1–5 (Proximal technique n = 132, Lens technique n = 130), whereas Condition 6 included fewer subjects since not all subjects had data for condition 6 (Proximal technique n = 131, Lens technique n = 125)).
These findings supported our hypothesis that AG is greater when the target is perceived as clear and led to a second hypothesis that AG is stable across clear demands, decreasing only once the target is perceived blurry (i.e. from Condition 4 to 5). We used a set of planned contrasts of adjacent conditions to test this new hypothesis. Since the classification of Condition 5 was based upon the subjective interpretation of each individual subject to recognize blur, we included the next consecutive greater accommodative demand following Condition 5 (termed Condition 6) to check for the reliability of the subject’s blur identification. Including Condition 6 required the exclusion of 1 additional subject from the proximal technique and 6 additional subjects from the lens technique since these subjects did not have measurements for the second blur demand.
The planned contrast tests compared the AG for neighboring conditions (Condition 1 to 2, 2 to 3, 3 to 4, 4 to 5 and 5 to 6), and included age as a predictive variable. For both the proximal and lens techniques, there were minimal, non-significant differences (<2% change) in the AG in the first three neighboring conditions (p>0.10) (Figure 4). Comparing Condition 3 to 4, there were statistically significant decreases in AG with the proximal technique (0.76±0.11 vs 0.71±0.13, p=0.001) and the lens technique (0.77±0.09 to 0.75±0.08, p=0.003). However, these changes were small (6% for proximal and 2% for lens) compared to the much larger decrease in AG when going from the last clear condition to the first blurred with the proximal (17% decrease; 0.71±0.13 to 0.59±0.16, p<0.001) and lens techniques (9% decrease; 0.75±0.08 to 0.69±0.11, p<0.001). Mean AG again decreased significantly by an additional 19% when comparing Condition 5 to 6 with the proximal technique (0.59±0.16 to 0.47±0.16, p<0.001) and an additional 8% with the lens technique (0.69±0.11 to 0.63±0.12, p<0.001), suggesting that Condition 5 likely captured the initial blur point.
Age was only a significant factor in the magnitude of AG change once the target was perceived blurred for the proximal technique (p=0.013), with younger subjects having a greater decrease in AG when comparing Condition 4 to 5 (Figure 5A). For the lens technique, age was not a factor until the target was already blurred (p=0.013) with older subjects having a greater decline in AG than the younger subjects when comparing Condition 5 to 6 (Figure 5B).
Given previously reported associations of myopic refractive error with increased accommodative lag,2, 3, 20, 21 exploratory analyses were performed to look for a relationship of refractive error to AG. For the myopic and emmetropic subjects, refractive error classification was added as a predictive variable to both of the analyses previously described. Subjects categorized as hyperopic or only having astigmatism were not included in the analysis since combined they made up only 9.4% (13/139) of the sample and thus statistical power was lacking.
When comparing the mean AG of Conditions 1–4 to Condition 5, myopic versus emmetropic refractive error was not a significant factor for either technique (proximal: n=121, F (3,118)=0.27, p=0.61; lens: n=119, F (3,116)<0.01, p=0.99) and the AG for Condition 5 was still significantly less than the average AG of Conditions 1–4 for both techniques (p<0.001). The previously observed significant age effect (greater decrease in AG for younger subjects at Condition 5) remained for the proximal technique for this subject subset (p=0.006) and there was still no significant effect of age for the lens technique (p=0.31).
Myopic versus emmetropic refractive error was also not a significant factor when comparing the AG for neighboring conditions for either technique (proximal: n=121, p≥0.07; lens: (n=119, p≥0.06). The previously observed significant age effect (greater decrease in AG for younger subjects when comparing Condition 4 to 5) remained for this subject subset (p=0.004), but age was not a significant factor for the lens technique (p=0.40).
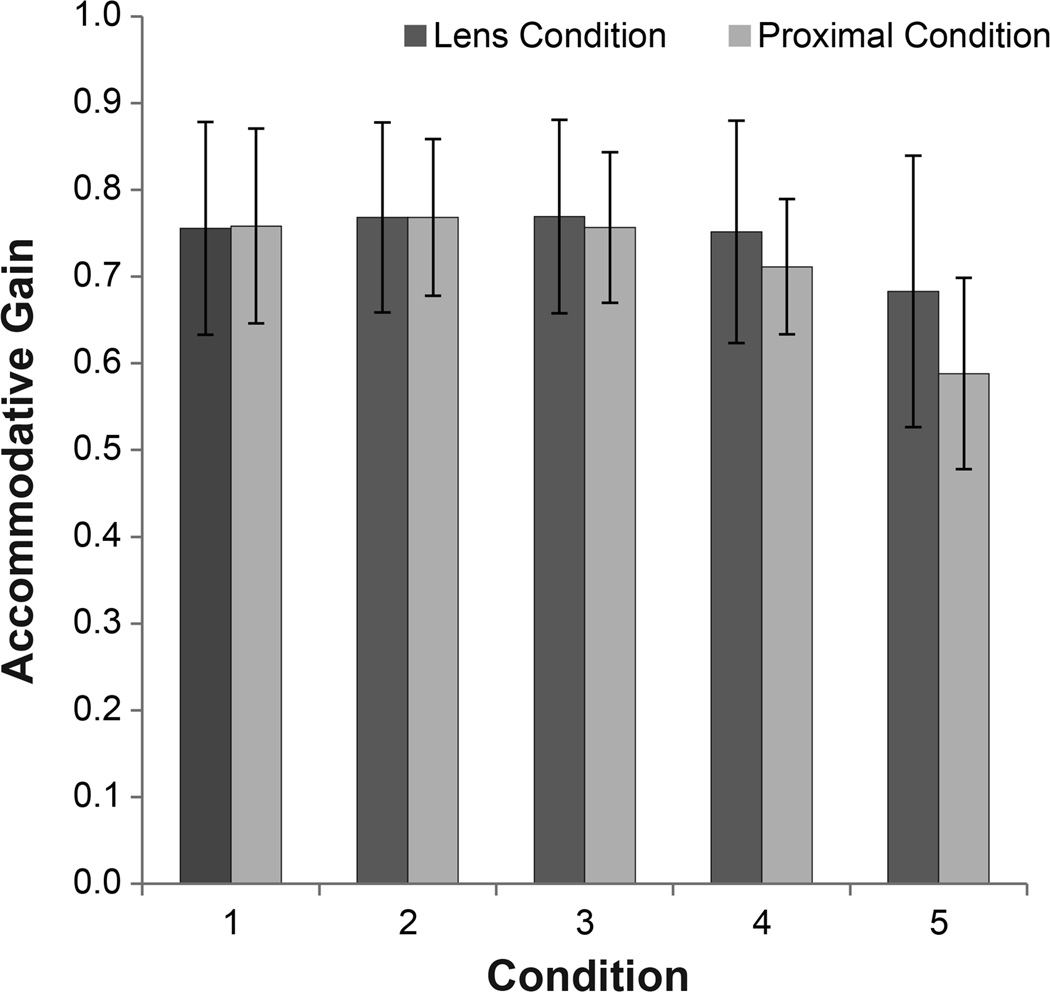
Finally, AG was compared between the two techniques to determine if AG varied with the technique used to increase demand (Figure 6). AGs were similar for both techniques when the subjects perceived the target as clear (Conditions 1–4). However, once the target was perceived blurry (Condition 5), the AG decreased 7.6% more for the proximal technique than the lens technique (F (1,125)=13.43, p=0.004).
Figure 6.
Comparison of the mean ± standard deviation accommodative gains for Conditions 1 through 5 between the proximal and lens techniques. The AGs for the two techniques were not found to be significantly different from one another for conditions 1 – 4 (p > 0.05). The AG for the proximal technique was significantly less than the AG for the lens technique for Condition 5, once the target was perceived as being blurry (asterisk represents p = 0.004).
DISCUSSION
This study demonstrates mean AG is consistent across a large range of accommodative demands and subject ages, as well as two methods for stimulating accommodation when the target is perceived clear by the subject and accommodative accuracy is compared within similar portions of each subject’s ASRC. Whereas previous studies have reported differences in the magnitude of the accommodative response and resultant accommodative lag from preschool to presbyopia when comparing performance at matched accommodative demands3, 4, 22, the analysis in the present study demonstrates that accommodative accuracy, expressed as gain, is consistent across ages when individual subject demands are grouped relative to the demand at which the subject perceives a first sustained blur. Our finding that AG is similar across Conditions 1–4 is consistent with Mordi and Ciuffreda (1998) and others that have shown stability of the linear portion of the ASRC in non-presbyopic adult subjects.7, 23–25 Our findings now add evidence that the linear portion of the ASRC is stable in younger children as well. Furthermore, there were no significant differences in AG between stimulus techniques for the clear conditions, despite the fact that one technique progressively magnified the retinal image size (proximal) while the other progressively minified the retinal image size (minus-lens).
Our finding that AG remained constant across stimulus demands until subjects perceived the target blurred suggests that a cut-off value for AG might be defined to predict target clarity (i.e. clear versus sustained blur). Using the 95% confidence intervals for Conditions 4 and 5 for each technique as a guide (Table 3), if subjects met ~70% of the accommodative demand, then they likely reported the target as clear. Once subjects perceived the target blurred, the 95% CI for the AG dropped to 0.70 and below. These results were consistent for both techniques, and across all ages tested (Figure 5). However, before a criterion can be clinically recommended, it must be determined whether the value is repeatable using clinical techniques under a variety of testing conditions, such as with different targets or levels of illumination, as well as presenting the demands in various orders. An additional consideration is how the cut-off may differ with monocular versus binocular viewing, which has previously been shown to impact accommodative lag.6, 26, 27 Our study was performed with monocular measurements and may not be generalizable to binocular testing. Lastly, our subjects had no known accommodative deficits. Future studies to compare the AG between symptomatic and asymptomatic patients may yield useful clinical guidelines.
Table 3.
Mean, standard deviation, and 95% confidence intervals (CI) of the accommodative gain (AG) for each condition for both the proximal and lens techniques.
| Condition 1 | Condition 2 | Condition 3 | Condition 4 | Condition 5 | Condition 6* | ||
|---|---|---|---|---|---|---|---|
| Proximal | Mean ± sd | 0.76±0.12 | 0.77±0.11 | 0.76±0.11 | 0.71±0.13 | 0.59±0.16 | 0.47±0.16 |
| 95% CI | 0.74, 0.78 | 0.75, 0.79 | 0.74, 0.78 | 0.69, 0.73 | 0.56, 0.62† | 0.45, 0.50† | |
| Lens | Mean ± sd | 0.76±0.11 | 0.77±0.09 | 0.77±0.09 | 0.75±0.08 | 0.68±0.11 | 0.63±0.12 |
| 95% CI | 0.74, 0.78 | 0.75, 0.79 | 0.76, 0.79 | 0.74, 0.77 | 0.67, 0.70† | 0.61, 0.65† | |
The bolded 95% CI values under Condition 5 (†) illustrate that when the AG falls below ~0.70, on average, individuals reported the target was blurred.
(* Note that Conditions 1–5 included subjects that had data for all Conditions from 1–5 (proximal n = 132, lens n = 130), whereas Condition 6 included fewer subjects since not all subjects had data for Condition 6 (proximal n = 131, lens n = 125)).
Our exploratory analysis showed no difference in AG between subjects with emmetropia versus myopia for either stimulus technique. While some investigators have found significant differences in accommodative behaviors between these two refractive groups,2, 3, 20, 21 others have not.5, 26, 28, 29 One potential source of differences between studies may be whether study participants had active myopia progression at the time of participation.2 Our study was not designed to recruit subjects with specific refractive errors, and it is also unknown whether subjects with myopia were actively progressing at the time of the study. Thus it is unknown if the status of myopia progression may have impacted our findings.
For analysis of this study, subjects were excluded if they did not have data for all 5 conditions when comparing the average of Conditions 1–4 to Condition 5. Excluded subjects were those who perceived blur at such a low demand that four preceding clear demands were unavailable for analysis. Seven subjects (aged 23–34 years) were excluded from the proximal technique, an age distribution which is unlikely to cause a significant change in the age effect. Nine subjects, eight of whom were 30–35 years, were excluded from the lens technique due to missing Condition 1 data. This distribution could potentially affect age-related results, so the mean AGs for Conditions 2–5 for the lens technique were calculated with and without these excluded subjects to explore potential effects. Mean AGs for the 30–35 year age group when excluding subjects were 0.78, 0.77, 0.74 and 0.66 for Conditions 2 – 5,respectively, and 0.78, 0.75, 0.73 and 0.65 when including these subjects. Given the similar AGs, exclusion of these older subjects was unlikely to impact the finding that age was not a significant predictor of AG. For analysis of the change in AG for neighboring conditions (Conditions 1–6), the excluded subjects spanned large age ranges for both techniques (proximal: 5–34 years; lens: 8–35 years) and thus there was unlikely a systematic bias in the age effect from exclusion of these subjects.
With respect to study design, once the target reached the 8D proximal demand, the dioptric interval between each successive demand increased in size rather than remaining at 1D steps, with the largest increase being 5D between consecutive demands. While this does reflect large dioptric jumps, the differences are small in physical distance (a change from 25 to 30D is only a physical change from 4 to 3.3cm). Additionally, only 10% of all subjects had proximal demands ≥12D for Condition 5, therefore this likely had little impact on the group mean AG. However, it is possible that these larger dioptric jumps contributed to the greater decrease in AG observed during proximal testing from Condition 4 to 5, particularly for the young children, versus the lens technique for which the dioptric interval between demands was fixed at 1D (Figure 6).
The results of this study are not readily comparable to other studies measuring accommodative responses or accommodative lags for set stimulus demands. Anderson et al. (2009) demonstrated that accuracy of accommodation through minus lenses improved throughout childhood, yet in the current study we found no age effect until the target was blurry.4 However, the Anderson et al. (2009) study investigated change in accommodative lag by age over a fixed series of demands (from 3 to 6.52D), whereas the current study investigated AG at demands in the upper end of each individual subject’s ASRC, which had minimal overlap with the demands from the previously published study.
It has previously been demonstrated that blur may be defined as a range from noticeable30 to non-resolvable,31 which can be further confounded by each individual’s ability to adapt to and interpret blur.32 One possible limitation to this study is that we do not know what criterion subjects used when determining if the target was clear or blurry. If blur classification did affect our results, it would have caused some inter-subject variation in the categorization of the accommodative demands for Conditions 1–5 in our study. However, there was a significant decrease in AG between Conditions 4 and 5 and an even larger decrease for one more consecutive demand beyond Condition 5, suggesting we captured the first blur point for the majority of subjects.
Another possible limitation of the study is that pupil size was not measured during data collection. Pupil size is known to affect the subjective depth-of-focus30 and therefore could influence the subjects’ identification of the demand at which the first blur occurred. With the range of ages represented in this study, there were certainly differences in pupil sizes across subjects; however, there were no significant age effects of AG for the clear stimulus demands, suggesting no systematic effect of pupil size related to age. This study also included a large range of stimulus demands and one would predict small pupil sizes for the largest accommodative demands, especially during the proximal technique. Although stimuli up to 30D were presented, of the data included in this analysis, only 14 subjects viewed the target at the 15D demand and 4 at the 20D demand, all of which were children. Schaeffel et al. (1993) reported not being able to measure a consistent reduction in pupil size in children even for an accommodative demand of 10D when viewing monocularly and also reported no consistent reduction in pupil size until subjects were older than 35 years, which is outside the age range of our study,33 so there is prior evidence that we may not have had large changes in pupil size during testing.
The decision not to measure pupil size was due to substantial increases in testing time for both the capture and printing of measures with the Grand Seiko which might compromise the attention and cooperation of the youngest subjects. While we do not have pupil size measures, we do have certainty that pupil size was not less than 2.3mm since the Grand Seiko does not take measures for pupils below 2.3mm.34 Although we are unable to explore the impact of pupil size on AG, the results still characterize the trends in AG for a large age range of subjects with habitual pupils. The fact that pupil was not controlled across these subjects perhaps makes it even more interesting that the AG had such a robust association with target clarity. If pupil size were collected, it would have allowed exploration of the variability in AG as a function of pupil size, and potentially accounted for some of the variation in subject identification of the first blurred demand.
A final limitation is the possibility of obtaining erroneous measures of accommodative response. Care was taken to ensure the measurement reticule was centered in the pupil to avoid off-axis measures. Additionally, measurements with large amounts of astigmatism were excluded, as this could be an indicator of poor fixation. A previous study reported the introduction of lenses in front of the eye may lead to erroneous measures of over-refraction with the Grand Seiko in subjects with uncorrected refractive error.35 However, the errors in that study were smallest for emmetropes (±0.30), which is representative of the subjects in the present study given that they had minimal uncorrected refractive error.
CONCLUSIONS
AG is a useful metric to describe accommodative accuracy for any given accommodative demand. Our results suggest AG is significantly smaller once the target is perceived blurred in a large age range of subjects (pre-school to adulthood) across a variety of accommodative demands and independent of the technique used to stimulate accommodation (proximal vs. minus-lens). Our results also suggest that for non-presbyopic individuals, an AG of less than ~70% (equivalent to an accommodative lag >30% of the accommodative demand) may indicate that the patient is not experiencing adequate image clarity at the tested accommodative demand.
Acknowledgments
Supported by Fight for Sight Grant-In-Aid (HAA); NIH/NEI K23EY022357 (TLR); and P30 EY007551 – University of Houston College of Optometry Core Grant.
Contributor Information
Tawna L. Roberts, University of Houston, College of Optometry, Houston, Texas.
Heather A. Anderson, University of Houston, College of Optometry, Houston, Texas.
Karla K. Stuebing, University of Houston Department of Psychology/TIMES Institute, Houston, Texas.
REFERENCES
- 1.McClelland JF, Saunders KJ. Accommodative lag using dynamic retinoscopy: age norms for school-age children. Optom Vis Sci. 2004;81:929–933. [PubMed] [Google Scholar]
- 2.Abbott ML, Schmid KL, Strang NC. Differences in the accommodation stimulus response curves of adult myopes and emmetropes. Ophthalmic Physiol Opt. 1998;18:13–20. [PubMed] [Google Scholar]
- 3.Gwiazda J, Thorn F, Bauer J, Held R. Myopic children show insufficient accommodative response to blur. Invest Ophthalmol Vis Sci. 1993;34:690–694. [PubMed] [Google Scholar]
- 4.Anderson HA, Glasser A, Stuebing KK, Manny RE. Minus lens stimulated accommodative lag as a function of age. Optom Vis Sci. 2009;86:685–694. doi: 10.1097/OPX.0b013e3181a7294f. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Anderson HA, Hentz G, Glasser A, Stuebing KK, Manny RE. Minus-lens-stimulated accommodative amplitude decreases sigmoidally with age: a study of objectively measured accommodative amplitudes from age 3. Invest Ophthalmol Vis Sci. 2008;49:2919–2926. doi: 10.1167/iovs.07-1492. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Sreenivasan V, Aslakson E, Kornaus A, Thibos LN. Retinal image quality during accommodation in adult myopic eyes. Optom Vis Sci. 2013;90:1292–1303. doi: 10.1097/OPX.0000000000000068. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Mordi JA, Ciuffreda KJ. Static aspects of accommodation: age and presbyopia. Vision Res. 1998;38:1643–1653. doi: 10.1016/s0042-6989(97)00336-2. [DOI] [PubMed] [Google Scholar]
- 8.Chauhan K, Charman WN. Single figure indices for the steady-state accommodative response. Ophthalmic Physiol Opt. 1995;15:217–221. doi: 10.1016/0275-5408(95)90573-k. [DOI] [PubMed] [Google Scholar]
- 9.Scheiman M, Wick B. Clinical Management of Binocular Vision: Heterophoric, Accommodative, and Eye Movement Disorders. 3rd. Philadelphia: Lippincott Williams & Wilkins; 2008. [Google Scholar]
- 10.Rouse MW, Hutter RF, Shiftlett R. A normative study of the accommodative lag in elementary school children. Am J Optom Physiol Opt. 1984;61:693–697. doi: 10.1097/00006324-198411000-00008. [DOI] [PubMed] [Google Scholar]
- 11.Morgan WM. Accommodation and its relationship to convergence. Am J Optom Arch Am Acad Optom. 1944;21:183–195. [Google Scholar]
- 12.Anderson HA, Stuebing KK. Subjective versus objective accommodative amplitude: preschool to presbyopia. Optom Vis Sci. 2014;91:1290–1301. doi: 10.1097/OPX.0000000000000402. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Hyvärinen L, Näsänen R, Laurinen P. New visual acuity test for pre-school children. Acta Ophthalmol (Copenh) 1980;58:507–511. doi: 10.1111/j.1755-3768.1980.tb08291.x. [DOI] [PubMed] [Google Scholar]
- 14.Hofstetter HW. A comparison of Duane’s and Donder’s tables of the amplitude of accommodation. Am J Optom Arch Am Acad Optom. 1944;21:345–363. [Google Scholar]
- 15.Radhakrishnan H, Charman WN. Changes in astigmatism with accommodation. Ophthalmic Physiol Opt. 2007;27:275–280. doi: 10.1111/j.1475-1313.2007.00474.x. [DOI] [PubMed] [Google Scholar]
- 16.Mutti DO, Enlow NL, Mitchell GL. Accommodation and induced with-the-rule astigmatism in emmetropes. Optom Vis Sci. 2001;78:6–7. doi: 10.1097/00006324-200101010-00004. [DOI] [PubMed] [Google Scholar]
- 17.Harvey EM, Miller JM, Schwiegerling J. Utility of an open field Shack-Hartmann aberrometer for measurement of refractive error in infants and young children. J AAPOS. 2013;17:494–500. doi: 10.1016/j.jaapos.2013.05.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Mutti DO, Jones LA, Moeschberger ML, Zadnik K. AC/A ratio, age, refractive error in children. Invest Ophthalmol Vis Sci. 2000;41:2469–2478. [PubMed] [Google Scholar]
- 19.SAS Institute Inc. Base SAS® 9.3 Procedures Guide: Statistical Procedures. 2nd. Cary, NC: SAS Institute Inc; 2012. [Google Scholar]
- 20.McBrien NA, Millodot M. A biometric investigation of late onset myopic eyes. Acta Ophthalmol (Copenh) 1987;65:461–468. doi: 10.1111/j.1755-3768.1987.tb07024.x. [DOI] [PubMed] [Google Scholar]
- 21.Allen PM, O'Leary DJ. Accommodation functions: co-dependency and relationship to refractive error. Vision Res. 2006;46:491–505. doi: 10.1016/j.visres.2005.05.007. [DOI] [PubMed] [Google Scholar]
- 22.Chen AH, O'Leary DJ, Howell ER. Near visual function in young children. Part I: Near point of convergence. Part II: Amplitude of accommodation. Part III: Near heterophoria. Ophthalmic Physiol Opt. 2000;20:185–198. [PubMed] [Google Scholar]
- 23.Nakatsuka C, Hasebe S, Nonaka F, Ohtsuki H. Accommodative lag under habitual seeing conditions: comparison between adult myopes and emmetropes. Jpn J Ophthalmol. 2003;47:291–298. doi: 10.1016/s0021-5155(03)00013-3. [DOI] [PubMed] [Google Scholar]
- 24.Yeo AC, Kang KK, Tang W. Accommodative stimulus response curve of emmetropes and myopes. Ann Acad Med Singapore. 2006;35:868–874. [PubMed] [Google Scholar]
- 25.Ramsdale C, Charman WN. A longitudinal study of the changes in the static accommodation response. Ophthalmic Physiol Opt. 1989;9:255–263. doi: 10.1111/j.1475-1313.1989.tb00903.x. [DOI] [PubMed] [Google Scholar]
- 26.Seidel D, Gray LS, Heron G. The effect of monocular and binocular viewing on the accommodation response to real targets in emmetropia and myopia. Optom Vis Sci. 2005;82:279–285. doi: 10.1097/01.opx.0000159369.85285.21. [DOI] [PubMed] [Google Scholar]
- 27.Sreenivasan V, Irving EL, Bobier WR. Binocular adaptation to near addition lenses in emmetropic adults. Vision Res. 2008;48:1262–1269. doi: 10.1016/j.visres.2008.02.015. [DOI] [PubMed] [Google Scholar]
- 28.Davies LN, Wolffsohn JS, Gilmartin B. Cognition, ocular accommodation, and cardiovascular function in emmetropes and late-onset myopes. Invest Ophthalmol Vis Sci. 2005;46:1791–1796. doi: 10.1167/iovs.04-0986. [DOI] [PubMed] [Google Scholar]
- 29.Langaas T, Riddell PM, Svarverud E, Ystenaes AE, Langeggen I, Bruenech JR. Variability of the accommodation response in early onset myopia. Optom Vis Sci. 2008;85:37–48. doi: 10.1097/OPX.0b013e31815ed6e9. [DOI] [PubMed] [Google Scholar]
- 30.Atchison DA, Fisher SW, Pedersen CA, Ridall PG. Noticeable, troublesome and objectionable limits of blur. Vision Res. 2005;45:1967–1974. doi: 10.1016/j.visres.2005.01.022. [DOI] [PubMed] [Google Scholar]
- 31.Ciuffreda KJ, Selenow A, Wang B, Vasudevan B, Zikos G, Ali SR. "Bothersome blur": a functional unit of blur perception. Vision Res. 2006;46:895–901. doi: 10.1016/j.visres.2005.10.004. [DOI] [PubMed] [Google Scholar]
- 32.Artal P, Chen L, Fernandez EJ, Singer B, Manzanera S, Williams DR. Neural compensation for the eye's optical aberrations. J Vis. 2004;4:281–287. doi: 10.1167/4.4.4. [DOI] [PubMed] [Google Scholar]
- 33.Schaeffel F, Wilhelm H, Zrenner E. Inter-individual variability in the dynamics of natural accommodation in humans: relation to age and refractive errors. J Physiol (Lond) 1993;461:301–320. doi: 10.1113/jphysiol.1993.sp019515. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Davies LN, Mallen EA, Wolffsohn JS, Gilmartin B. Clinical evaluation of the Shin-Nippon NVision-K 5001/Grand Seiko WR-5100K autorefractor. Optom Vis Sci. 2003;80:320–324. doi: 10.1097/00006324-200304000-00011. [DOI] [PubMed] [Google Scholar]
- 35.Kimura S, Hasebe S, Ohtsuki H. Systematic measurement errors involved in over-refraction using an autorefractor (Grand-Seiko WV-500): is measurement of accommodative lag through spectacle lenses valid? Ophthalmic Physiol Opt. 2007;27:281–286. doi: 10.1111/j.1475-1313.2007.00466.x. [DOI] [PubMed] [Google Scholar]