Abstract
Many studies have been conducted in health-care settings with regards to complementary and alternative medicine (CAM) use among patients. However, information regarding CAM use among patients in the emergency department (ED) is scarce. The aim of this article was to conduct a systematic review of published studies with regards to CAM use among the ED patients. A literature search of published studies from inception to September 2015 was conducted using PubMed, Scopus, and manual search of the reference list. 18 studies that met the inclusion criteria were reviewed. The prevalence rate of CAM use among ED patients across the studies ranged of 1.4-68.1%. Herbal therapy was the sub-modality of CAM most commonly used and frequently implicated in CAM-related ED visits. Higher education, age, female gender, religious affiliation, and chronic diseases were the most frequent factors associated with CAM use among the ED patients. Over 80% of the ED physicians did not ask the patients about the CAM therapy. Similarly, 80% of the ED patients were ready to disclose CAM therapy to the ED physician. The prevalence rate of CAM use among patients at ED is high and is growing with the current increasing popularity, and it has been a reason for some of the ED visits. There is a need for the health-care professionals to receive training and always ask patients about CAM therapy to enable them provide appropriate medical care and prevent CAM-related adverse events.
Keywords: Alternative medicine, complementary medicine, emergency department, prevalence, traditional medicine
INTRODUCTION
The World Health Organization has reported the use of complementary and alternative medicine (CAM) therapy for disease prevention and maintenance of well-being to be increasing worldwide in the recent years [1]. The prevalence rate of CAM use among the general population in developed countries such as the US is 42%, Canada 50%, and France 75% [2]. Similarly, in developing countries, CAM utilization is becoming increasingly popular. Up to 90% population of Asian and African countries relied on CAM for primary health purposes [2]. The prevalence rate of CAM utilization among the general population in the developing countries such as Uganda is 60%, India 70%, and Ethiopia 90% [2]. In China, CAM accounts for around 40% of all health care delivered [3]. Furthermore, the global market sales of CAM increased from over US$ 700 million, in 1999, to over US$ 1,000 million, in 2001 [1]. In Australia, CAM use was responsible for an estimated national expenditure of $A2.3 billion in 2000 [4].
The reason for the current increased popularity may be related to the perceived CAM as a holistic approach to life, self-empowerment, “safer” low cost, greater accessibility, variety of practices, and philosophical beliefs [5]. Even though, CAM use has made significant contributions in the healthcare management [3], the recent growth in the prevalence rate of CAM use among patients have raised concerns about the toxicity and the potential herbal-drug, herbal-disease, and herbal-herbal interactions [6,7]. However, some of the therapeutic potentials of some herbs have been established in vitro [8].
Extensive research on CAM utilization has been focused on patients receiving medical care at clinical settings. Clinical settings such as hospitals are the interface between CAM users and conventional therapies. Previous studies of ED patients have identified a higher prevalence rate of CAM usage among ED patients compared to the general population [9-12]. This is because, the ED comprises of many categories of patients with chronic underlying diseases such as diabetes mellitus, cardiovascular system disorder, central nervous system disorder, asthma, and cancer that were associated with utilization of CAM therapy [13,14]. Second, some of the ED visits due to toxicities or adverse events resulting from the use of CAM or non-adherence to conventional medication in preference to CAM therapy [15,16]. The ED physicians, on the other hand, do not always inquire about the use of CAM from patients, leading to wrong diagnosis and consequent deterioration of disease condition [17,18]. In spite of the high prevalence rate of CAM use among ED patients, only a few studies were conducted on CAM use among patients seeking care at the ED [19]. Furthermore, there is a paucity of systematic reviews on the studies on CAM use among ED patients.
The purpose of this systematic review is, therefore, to review published original articles regarding the prevalence of CAM use, CAM-related toxicities, and factors associated with CAM use among patients seeking care at ED.
LITERATURE SEARCH
The literature search and study selection were performed based on PRISMA for systematic review protocol [20]. An online search of literature from inception to September 2015 regarding the prevalence of CAM use among patients at ED was conducted in PubMed and Scopus using Medical Subject Heading (MeSH) and title abstract (tiab) terms. The keywords searched (including all MeSH, headings, subheadings, and tiab terms); “Complementary medicine” OR “alternative medicine” OR “traditional medicine” AND “prevalence” AND “emergency department (ED).” Only original research articles published in the English language were considered. Relevant articles were also identified from the reference list of the studies selected from PubMed and Scopus.
STUDY SELECTION CRITERIA
Studies were selected for inclusion in the current review based on the following criteria: (i) Studies conducted on CAM use among patients seeking medical care at ED. (ii) Studies on the knowledge, attitude, and perception of CAM use among physicians and patients in the ED. The exclusion criteria included (i) studies of CAM use among patients in other study settings (ii) Studies of CAM use among non-hospitalized patients.
OVERVIEW
The online search of literature generated 543 articles. A total of 18 studies that met the inclusion criteria were reviewed. The PRISMA flow in Figure 1 demonstrated the study flow selection. The key findings from these studies are summarized in Table 1.
Figure 1.
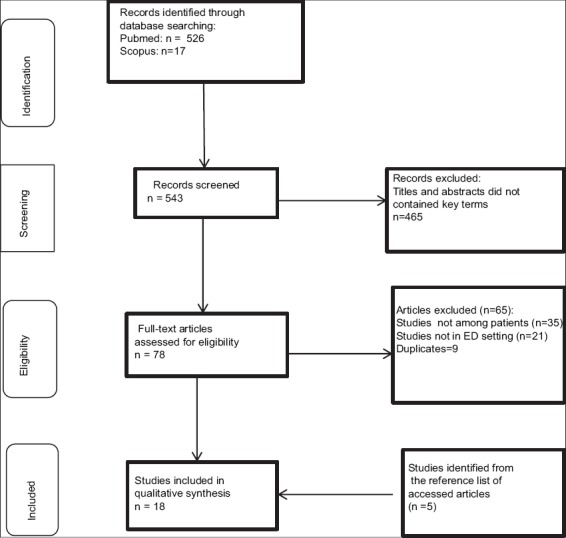
PRISMA flow of the study flow selection
Table 1.
Summary of the key findings
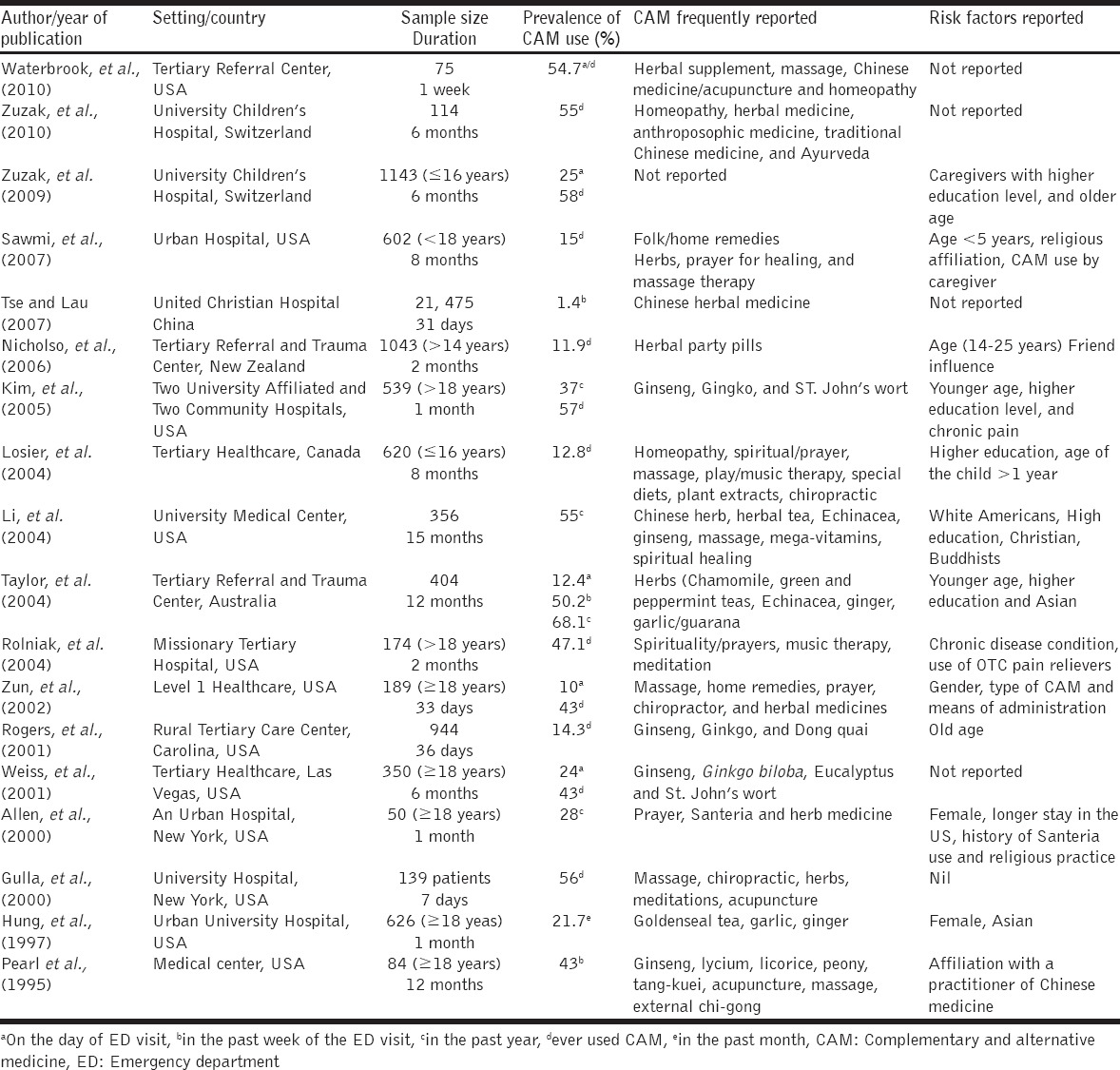
The publications were based on studies conducted in six countries, with the majority of the studies from the United States of America (U.S) (12/18), Switzerland (2/18), Canada (1/18), New Zealand (1/18) China (1/18), and Australia (1/18). There were no published articles from the developing countries. 14 of the reviewed studies were conducted at tertiary hospitals while the remaining four were performed in secondary and primary health-care hospitals. Hence, the urgent need for more studies in other countries of the world, to have a comprehensive knowledge of CAM use among patients seeking care at ED. Having a wider knowledge of CAM will help conventional healthcare providers at all level of healthcare system to be aware and familiar with different modalities of CAM used as well as the adverse events related to the CAM use presented by the patients at the ED. These will eventually prevent CAM-related hospitalization and complication of an underlying illness.
DEFINITIONS OF CAM USED IN THE STUDIES REVIEWED
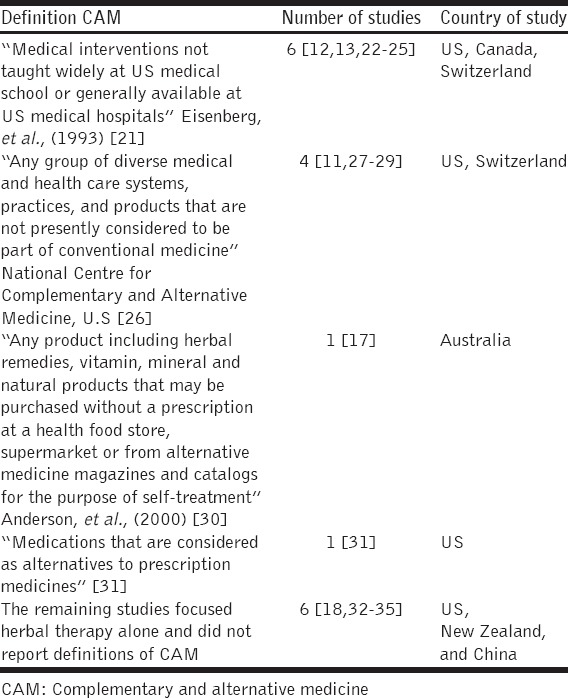
Different definitions of CAM have been reported among the studies. The variations may be because CAMs involved wide varieties of practices and beliefs that may be peculiar to a particular population. Moreover, the variation in the definition of CAM may have affected the estimation of the prevalence rates, generalization, and comparison of the findings in the studies reviewed. Therefore, standardization of the definition, terminology, and classification of CAM for comparison and generalization of the findings may not be possible [Table 2].
Table 2.
Definition of CAM adopted
PREVALENCE RATE OF CAM USE AMONG ED PATIENTS
Due to the different definitions, practice, and prevalence rate of CAM use reported in the studies reviewed, general statement and comparison may not be possible. The prevalence rate of CAM use ranges from a low as 1.4% to as high as 68.1%. The studies reviewed reported different categories of prevalence rate of CAM use among patients at ED: (i) Prevalence rate of current CAM use, (ii) prevalence rate of CAM use in the past week, (iii) prevalence rate of CAM use in the past month, (iv) prevalence rate of CAM use in the past year, and (vi) prevalence rate of CAM use in the lifetime [Table 1]. Moreover, three studies reported a prevalence rate of 17%, 24%, and 25% of current CAM use for the management of the chief presenting complaints at the ED [22,24,27]. With regards to a prevalence rate of CAM use among gender, females were found to have higher proportions of CAM use among the studies reviewed, accounting for up to 68% of CAM users [17,11,13,22,24,28,33].
The previous study on CAM use among patients in other clinical settings have shown that the inclusion of prayer for healing (PFH) as a sub-modality of CAM has been attributed with inflation of prevalence rate of CAM use among the patients [36]. In the current review, the lower prevalence rate of CAM use reported by the studies that included PFH indicated that there was no overestimation in the prevalence rate [23,28]. This may be linked to the differences in religious belief of the study population and definitions of CAM adopted by the different studies.
SOURCE OF INFORMATION OF CAM THERAPY
Most of the CAM users learned about its use from family and friends, media, internet, physician, pharmacist, self-medication, and CAM practitioner. People are now more aware of CAM therapy because of the increased widespread information on the internet, media, the advent of online shopping and faster information dissemination through social networking among family and friends.
FREQUENTLY REPORTED CAM THERAPIES
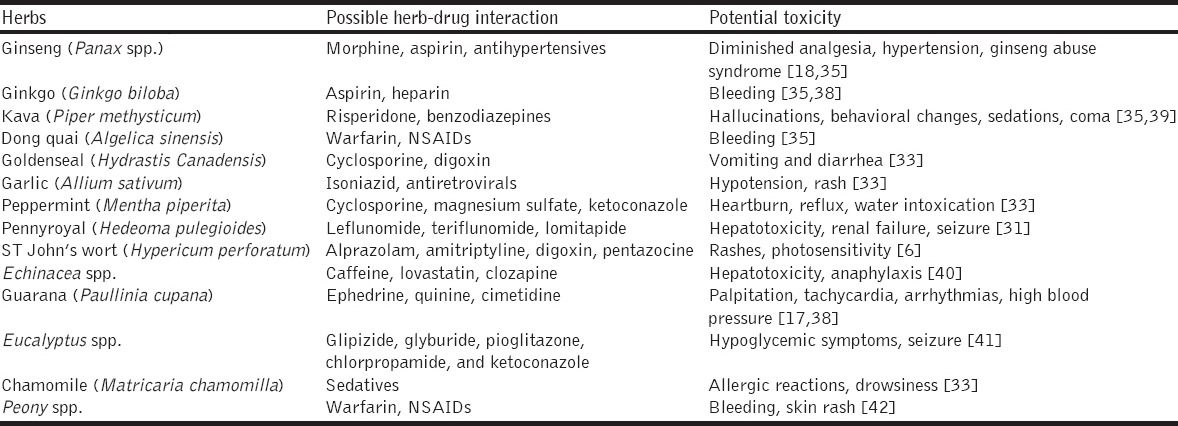
Table 1 demonstrates the frequently used CAM across the studies. Herbal therapy was the frequently used CAM reported among the patients seeking medical care at ED. However, the majority of the herbal therapy reported in the reviewed studies also has the potentials to interact with conventional drugs leading to adverse events (Table 3 demonstrates the possible interactions and toxicities related to herbal medication use reported in the studies reviewed). Similarly, the most commonly used CAMs among children (≤18 years) were herbs, homeopathy, folk remedies, PFH, Ayurveda, traditional Chinese medicine, and anthroposophic medicine. The parents normally utilized the CAM on their children for wellness and management of infection [25,29]. Moreover, some of the CAM-users were using CAMs particularly to manage the symptoms associated with the presenting complaints at the ED, whereas, some were using it for wellness and other health conditions. With regards to the change in the pattern of CAM use among patients from the studies reviewed, there was no change in the pattern of CAM utilization among the CAM users from 1995 to 2010.
Table 3.
Potential adverse effects/interactions associated with the commonly reported herbal medicines
FREQUENTLY REPORTED CONDITIONS/DISEASES FOR USING CAM
The frequently reported conditions for which the patients reported using CAM included: Cold and flu, infections, pains, chronic diseases such as arthritis, hypertension, and diabetes, wellness, to aid digestion, sleep, energy, ecstasy, fever, abdominal pain, and respiratory disorder.
FACTORS ASSOCIATED WITH CAM USE AMONG ED PATIENTS
Table 1 indicated several factors associated with CAM use among patients at ED. Four of the studies reviewed did not report factors associated with CAM use. Knowing the factors may help the conventional health-care professionals in further assessing the patients with the related factors, to prevent adverse events related to CAM use.
ED VISITS-RELATED TO CAM TOXICITIES
Herbal therapy has been the most frequently implicated CAM in the ED visit-related to toxicities and allergy from CAM use. From the studies reviewed, some of the chief presenting complaints at the ED were adverse effects related to an overdose and allergic reaction to herbal medications. A study conducted in Australia [17] reported an ED visit-related to poisoning with Jimsom weed (Datura stramonium) and an unidentified Chinese herbal medicine. The patients presented at the ED with thrombocytopenia and acute anticholinergic symptoms. The second study in New Zealand also reported an ED visit due to toxicities related to “herbal party pill” made from pepper plant (Piper nigrum) [34]. The CAM users took the herbal pill for the purpose of getting high, ecstasy, and energy. The patients presented at the ED with extreme alertness, agitation, palpitation, dizziness, and pruritus. In the other study in Hong Kong, China, 7.6% of the CAM users were presented at the ED with CAM-related toxicities, including dermatitis and systemic allergic reaction from topical and oral use of Chinese herbal medicines, respectively [37].
Some of the herbs reported in the studies reviewed also have the potentials to cause adverse effects and interaction with conventional medicines. Some of the adverse effects, include palpitations, anxiety, tremor, nausea, vomiting, anticholinergic symptoms, and bleeding, were attributed to the use of guarana, ginseng, jimson weed, and gingko [17]. The physicians, nurses, and the pharmacists at the ED should be better informed and be familiar with the modalities of CAMs, to enable them to recognize the sign and symptoms of the CAM-related toxicities, and provide appropriated diagnosis and medical care. Table 3 demonstrates the frequently reported herbs by the ED patients and the related potential interactions/adverse effects.
DISCLOSURE OF CAM USE BY ED PATIENTS
9 studies have indicated that up to 70% of the ED patients do not inform their physician that they are using CAM therapies, 80% said they are willing to disclose to their ED physician the CAM they are using. Moreover, 82% claimed that the ED physicians do not ask them about CAM use. This is likely because some of the ED physicians may not have adequate knowledge and training of CAM therapy. The study on knowledge and usage of CAM among ED physicians shows that 46% of the ED physicians learned about CAM therapy from friends or family rather than medical school or other physicians. This finding also further buttresses this point [11]. Another study among pediatricians has indicated that most of the pediatricians did not ask about CAM use in children. This had led to many complications such as herbal-drug interactions [29]. The ED physician and other conventional healthcare providers should actively inquire about the use of CAM therapy in patients, to enable them provide appropriate care and prevent adverse events related to CAM use. Moreover, CAM should be included in the training of all health-care professionals, to have adequate knowledge of CAM therapies and CAM-related toxicities.
Limitations and Future Directions
All the studies reviewed were cross-sectional surveys that are associated with biases such as:
A sampling of subjects: Most of the studies employed convenience sampling. Thus, the subjects may not be a true representation of the population
Non-response rates: The non-response rate of the respondents in the studies reviewed was up to 28%, and the majority of the studies did not mention the measures they took in avoiding the non-response bias. This may have affected the estimation of the prevalence rate in the studies
Recall bias: Inaccuracy and inability to recall information by respondents during the data collection using questionnaire, may also affect the accuracy of the findings.
Based on the findings from the articles reviewed, there is a need for: (i) more studies, especially in developing countries, and other healthcare settings such as secondary and primary hospitals, to better understand the CAM use among patients. (ii) Further studies on the knowledge, attitude, and perception of ED physicians to CAM therapy. (iii) Studies solely on CAM-related ED visit and evaluation of CAM use in studies of drug-related ED visits.
The findings of the studies reviewed have implications for ED physicians:
ED visit may be related to CAM use as such inquiring the patient about CAM therapy will prevent misdiagnosis and wrong medication at the ED.
Some CAM therapies, herbal medicine, in particular, has the potentials to interact with the conventional treatments leading to adverse events.
Adverse effects of some CAM therapies may mimic the clinical manifestations of many diseases leading to wrong diagnosis and complication of diseases.
Three categories of CAM users may be found at the ED: Patients currently using CAM while on the ED visit (on the day of the visit), those using CAM for the management of the presenting complaints at the ED and those using CAM in the past week, month, or year.
The conventional health care providers should, therefore, be aware and familiar with CAM therapy the patient is using while on the ED visit.
CONCLUSION
There is growing prevalence rate of CAM use among ED patients. Herbal therapy was the sub-modality of CAM most commonly used by ED patients and was responsible for some of the ED visits. Moreover, the majority of the patients were not asked by the ED physicians regarding the CAM use, and most of the ED physicians seem to lack the knowledge of CAM therapy. Therefore, physicians and other health-care professionals at the ED should be better informed about CAM therapies, to improve patient safety.
Footnotes
Source of Support: Nil
Conflict of Interest: None declared.
REFERENCES
- 1.National Policy on Traditional Medicine and Regulation of Herbal Medicines. Report of a WHO Global Survey. World Health Organization. 2005. [Last accessed on 2015 Sep 02]. Available from: http://www.apps.who.int/medicinedocs/pdf/s7916e/s7916e.pdf .
- 2.WHO. Traditional Medicine Strategy; 2002-2005. [Last accessed on 2015 Sep 20]. Available from: http://www.wpro.who.int/health_technology/book_who_traditional_medicine_strategy_2002_2005.pdf .
- 3.Division TC, editor. Ministry of Health Malaysia. A Handbook of Traditional and Complementary Medicine Programme in Malaysia. Kuala Lumpur: Traditional and Complementary Medicine Division; 2011. [Last accessed on 2015 Oct 02]. pp. 1–5. Available from: http://www.tcm.moh.gov.my/v4/pdf/handbook.pdf . [Google Scholar]
- 4.MacLennan AH, Wilson DH, Taylor AW. The escalating cost and prevalence of alternative medicine. Prev Med. 2002;35:166–73. doi: 10.1006/pmed.2002.1057. [DOI] [PubMed] [Google Scholar]
- 5.WHO Global Atlas of Traditional, Complementary and Alternative Medicine. World Health Organization. 2005. [Last accessed on 2015 Oct 05]. Available from: http://www.apps.who.int/iris/handle/10665/43108 .
- 6.Moss TM. Herbal medicine in the emergency department: A primer for toxicities and treatment. J Emerg Nurs. 1998;24:509–13. doi: 10.1016/s0099-1767(98)70037-6. [DOI] [PubMed] [Google Scholar]
- 7.Tulunay M, Aypak C, Yikilkan H, Gorpelioglu S. Herbal medicine use among patients with chronic diseases. J Intercult Ethnopharmacol. 2015;4:217–20. doi: 10.5455/jice.20150623090040. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Ogur R, Istanbulluoglu H, Korkmaz A, Barla A, Tekbas OF, Oztas E. Report: Investigation of anti-cancer effects of cherry in vitro. Pak J Pharm Sci. 2014;27:587–92. [PubMed] [Google Scholar]
- 9.Tindle HA, Davis RB, Phillips RS, Eisenberg DM. Trends in use of complementary and alternative medicine by US adults 1997-2002. Altern Ther Health Med. 2005;11:42–9. [PubMed] [Google Scholar]
- 10.Eisenberg DM, Davis RB, Ettner SL, Appel S, Wilkey S, Van Rompay M, et al. Trends in alternative medicine use in the United States, 1990-1997: Results of a follow-up national survey. JAMA. 1998;280:1569–75. doi: 10.1001/jama.280.18.1569. [DOI] [PubMed] [Google Scholar]
- 11.Waterbrook AL, Southall JC, Strout TD, Baumann MR. The knowledge and usage of complementary and alternative medicine by emergency department patients and physicians. J Emerg Med. 2010;39:569–75. doi: 10.1016/j.jemermed.2008.01.007. [DOI] [PubMed] [Google Scholar]
- 12.Kim S, Hohrmann JL, Clark S, Munoz KN, Braun JE, Doshi A, et al. A multicenter study of complementary and alternative medicine usage among ED patients. Acad Emerg Med. 2005;12:377–80. doi: 10.1197/j.aem.2005.02.008. [DOI] [PubMed] [Google Scholar]
- 13.Rolniak S, Browning L, Macleod BA, Cockley P. Complementary and alternative medicine use among urban ED patients: Prevalence and patterns. J Emerg Nurs. 2004;30:318–24. doi: 10.1016/j.jen.2004.04.008. [DOI] [PubMed] [Google Scholar]
- 14.Metcalfe A, Williams J, McChesney J, Patten SB, Jetté N. Use of complementary and alternative medicine by those with a chronic disease and the general population - Results of a national population based survey. BMC Complement Altern Med. 2010;10:58. doi: 10.1186/1472-6882-10-58. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Jose VM, Bhalla A, Sharma N, Hota D, Sivaprasad S, Pandhi P. Study of association between use of complementary and alternative medicine and non-compliance with modern medicine in patients presenting to the emergency department. J Postgrad Med. 2007;53:96–101. doi: 10.4103/0022-3859.32208. [DOI] [PubMed] [Google Scholar]
- 16.Milton D. Using alternative and complementary therapies in the emergency setting. J Emerg Nurs. 1998;24:500–8. doi: 10.1016/s0099-1767(98)70036-4. [DOI] [PubMed] [Google Scholar]
- 17.Taylor DM, Walsham N, Taylor SE, Wong L. Use and toxicity of complementary and alternative medicines among emergency department patients. Emerg Med Australas. 2004;16:400–6. doi: 10.1111/j.1742-6723.2004.00644.x. [DOI] [PubMed] [Google Scholar]
- 18.Pearl WS, Leo P, Tsang WO. Use of Chinese therapies among Chinese patients seeking emergency department care. Ann Emerg Med. 1995;26:735–8. doi: 10.1016/s0196-0644(95)70046-3. [DOI] [PubMed] [Google Scholar]
- 19.Isbister GK, Adams J. Investigating the relationship between emergency departments and complementary and alternative medicine use in Australia. Emerg Med Australas. 2004;16:378–81. doi: 10.1111/j.1742-6723.2004.00639.x. [DOI] [PubMed] [Google Scholar]
- 20.Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Int J Surg. 2010;8:336–41. doi: 10.1016/j.ijsu.2010.02.007. [DOI] [PubMed] [Google Scholar]
- 21.Eisenberg DM, Kessler RC, Foster C, Norlock FE, Calkins DR, Delbanco TL. Unconventional medicine in the United States. Prevalence, costs, and patterns of use. N Engl J Med. 1993;328:246–52. doi: 10.1056/NEJM199301283280406. [DOI] [PubMed] [Google Scholar]
- 22.Li JZ, Quinn JV, McCulloch CE, Jacobs BP, Chan PV. Patterns of complementary and alternative medicine use in ED patients and its association with health care utilization. Am J Emerg Med. 2004;22:187–91. doi: 10.1016/j.ajem.2004.02.006. [DOI] [PubMed] [Google Scholar]
- 23.Losier A, Taylor B, Fernandez CV. Use of alternative therapies by patients presenting to a pediatric emergency department. J Emerg Med. 2005;28:267–71. doi: 10.1016/j.jemermed.2004.11.019. [DOI] [PubMed] [Google Scholar]
- 24.Allen R, Cushman LF, Morris S, Feldman J, Wade C, McMahon D, et al. Use of complementary and alternative medicine among Dominican emergency department patients. Am J Emerg Med. 2000;18:51–4. doi: 10.1016/s0735-6757(00)90048-2. [DOI] [PubMed] [Google Scholar]
- 25.Zuzak TJ, Zuzak-Siegrist I, Rist L, Staubli G, Simões-Wüst AP. Medicinal systems of complementary and alternative medicine: A cross-sectional survey at a pediatric emergency department. J Altern Complement Med. 2010;16:473–9. doi: 10.1089/acm.2009.0601. [DOI] [PubMed] [Google Scholar]
- 26.National Center for Complementary and Alternative Medicine. National Institute of Health. [Last accessed on 2015 Oct 23]. Available from: http://www.nccam.nih.gov/health/whatiscam .
- 27.Zuzak TJ, Zuzak-Siegrist I, Simões-Wüst AP, Rist L, Staubli G. Use of complementary and alternative medicine by patients presenting to a paediatric emergency department. Eur J Pediatr. 2009;168:431–7. doi: 10.1007/s00431-008-0765-3. [DOI] [PubMed] [Google Scholar]
- 28.Zun LS, Gossman W, Lilienstein D, Downey L. Patients' self-treatment with alternative treatment before presenting to the ED. Am J Emerg Med. 2002;20:473–5. doi: 10.1053/ajem.2002.34963. [DOI] [PubMed] [Google Scholar]
- 29.Sawni-Sikand A, Schubiner H, Thomas RL. Use of complementary/alternative therapies among children in primary care pediatrics. Ambul Pediatr. 2002;2:99–103. doi: 10.1367/1539-4409(2002)002<0099:uocata>2.0.co;2. [DOI] [PubMed] [Google Scholar]
- 30.Anderson DL, Shane-McWhorter L, Crouch BI, Andersen SJ. Prevalence and patterns of alternative medication use in a university hospital outpatient clinic serving rheumatology and geriatric patients. Pharmacotherapy. 2000;20:958–66. doi: 10.1592/phco.20.11.958.35257. [DOI] [PubMed] [Google Scholar]
- 31.Weiss SJ, Takakuwa KM, Ernst AA. Use, understanding, and beliefs about complementary and alternative medicines among emergency department patients. Acad Emerg Med. 2001;8:41–7. doi: 10.1111/j.1553-2712.2001.tb00548.x. [DOI] [PubMed] [Google Scholar]
- 32.Gulla J, Singer AJ. Use of alternative therapies among emergency department patients. Ann Emerg Med. 2000;35:226–8. doi: 10.1016/s0196-0644(00)70072-2. [DOI] [PubMed] [Google Scholar]
- 33.Hung OL, Shih RD, Chiang WK, Nelson LS, Hoffman RS, Goldfrank LR. Herbal preparation use among urban emergency department patients. Acad Emerg Med. 1997;4:209–13. doi: 10.1111/j.1553-2712.1997.tb03743.x. [DOI] [PubMed] [Google Scholar]
- 34.Nicholson TC. Prevalence of use, epidemiology and toxicity of ‘herbal party pills’ among those presenting to the emergency department. Emerg Med Australas. 2006;18:180–4. doi: 10.1111/j.1742-6723.2006.00826.x. [DOI] [PubMed] [Google Scholar]
- 35.Rogers EA, Gough JE, Brewer KL. Are emergency department patients at risk for herb-drug interactions? Acad Emerg Med. 2001;8:932–4. doi: 10.1111/j.1553-2712.2001.tb01157.x. [DOI] [PubMed] [Google Scholar]
- 36.Chui PL, Abdullah KL, Wong LP, Taib NA. Prayer-for-health and complementary alternative medicine use among Malaysian breast cancer patients during chemotherapy. BMC Complement Altern Med. 2014;14:425. doi: 10.1186/1472-6882-14-425. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Tse M, Lau F. Traditional Chinese medicine use among emergency patients in Hong Kong. Hong Kong J Emerg Med. 2007;14:151–3. [Google Scholar]
- 38.Staines S. Herbal medicines: Adverse effects and drug-herb interactions. J Malta Coll Pharm Pract. 2011;17:38–42. [Google Scholar]
- 39.Almeida JC, Grimsley EW. Coma from the health food store: Interaction between kava and alprazolam. Ann Intern Med. 1996;125:940–1. doi: 10.7326/0003-4819-125-11-199612010-00023. [DOI] [PubMed] [Google Scholar]
- 40.Myers SP, Wohlmuth H. Echinacea-associated anaphylaxis. Med J Aust. 1998;168:583–4. doi: 10.5694/j.1326-5377.1998.tb139097.x. [DOI] [PubMed] [Google Scholar]
- 41.Burkhard PR, Burkhardt K, Haenggeli CA, Landis T. Plant-induced seizures: Reappearance of an old problem. J Neurol. 1999;246:667–70. doi: 10.1007/s004150050429. [DOI] [PubMed] [Google Scholar]
- 42.WebMD. Side Effects of Peony. 2015. [Last accessed on 2015 Oct 29]. Available from: http://www.webmd.com/vitamins-supplements/ingredientmono-32-peony.aspx?activeingredientid=32&activeingredientname=peony .


