Abstract
Chilblain, also known as pernio, is an abnormal inflammatory response to cold, moist environmental conditions. Persistent or atypical lesions should prompt investigation to exclude underlying systemic illness. We describe a case of acute myeloid leukaemia that presented with chilblain-like leukaemia cutis.
Background
Chilblain, also known as pernio, manifests with tender violaceous to blue macules, papules and plaques across acral sites.1 Most cases are attributed to exposure to cold, moist environmental conditions. Persistent or atypical lesions can be a clue to lupus erythaematosus, sarcoidosis and haematological neoplasms. Chilblain-like eruptions have rarely been described in patients with myeloid leukaemias. We describe a case of chilblain-like leukaemia cutis (LC). Our patient had been initially diagnosed with idiopathic chilblain. The aim of this report is to spread awareness of chilblain-like LC. Physicians should be alert for atypical chilblain as a clue to an underlying systemic illness.
Case presentation
A 75-year-old woman presented in January with recent onset of erythaematous swelling of the nose, toes and fingers. She had recently visited another clinic and carried a diagnosis of idiopathic chilblain. Review of systems revealed a 4-month history of fatigue, joint pain, palpitations and difficulty thinking clearly. The patient denied fevers, chills, shortness of breath and photosensitive rash. Physical examination disclosed mildly tender, non-blanching dusky red to violaceous plaques across the nasal tip (figure 1A), toes and dorsal fingers (figure 1B). There were generalised petechiae and the right preauricular and cervical lymph nodes were enlarged. Liver and spleen were easily palpitated with inspiration. Delayed answering of questions and trouble initiating conversation were noted.
Figure 1.
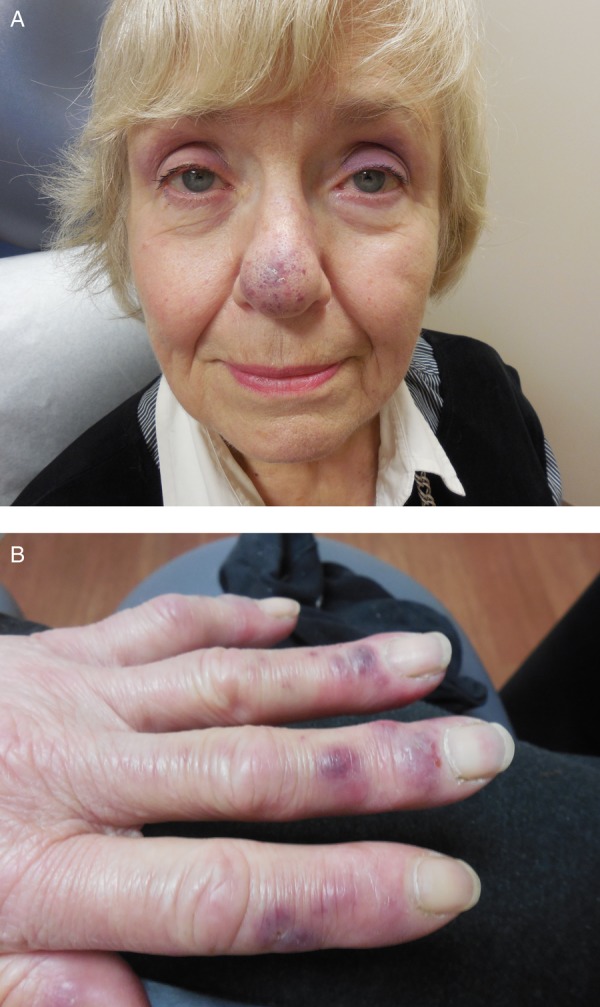
(A) Blue–purple discolouration and swelling of the patient's nose. (B) Violaceous papules across the patient's dorsal fingers.
Investigations
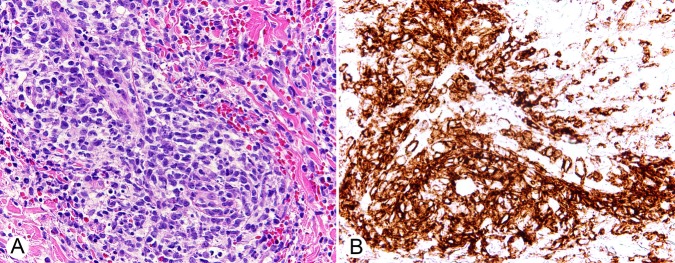
A punch biopsy was obtained from the finger. It revealed a dense, superficial and deep haemorrhagic perivascular infiltrate. The infiltrate was comprised of mononuclear cells with enlarged nuclei, finely dispersed chromatin and conspicuous nucleoli, (figure 2). The cells of interest expressed CD4, CD43, CD68 and lysozyme. Peripheral blood testing disclosed leucocytosis with a white cell count of 30 000/µL (reference range 3500–10 000/µL) with 89% blasts and Auer rods.
Figure 2.
(A) Biopsy demonstrates a dense perivascular infiltrate of immature mononuclear cells (H&E, ×400). (B) The mononuclear cells express CD43 (immunohistochemistry, ×400).
Differential diagnosis
Our differential diagnosis included idiopathic chilblain, autoimmune chilblain, lymphoma and chilblain-like LC. The weather at the time of presentation was unseasonably warm. Combined with the findings on review of systems, this excluded idiopathic chilblain. Autoimmune chilblain was excluded by absence of a photosensitive rash and the finding of atypical cells on skin biopsy. Immunophenotyping of the atypical cells in the skin biopsy combined with the abundant circulating blast cells in the peripheral blood allowed us to make the diagnosis of chilblain-like LC and exclude lymphoma.
Treatment
The patient was treated for acute myelomonocytic leukaemia using systemic idarubicin and cytarabine.
Outcome and follow-up
The patient's cutaneous lesions resolved completely following treatment of her leukaemia. She continues to follow-up with oncology and has reported neither new skin lesions nor leukaemia relapse 1 year following her diagnosis.
Discussion
Cutaneous manifestations of leukaemia are classified as specific or non-specific, depending on whether a leukaemic or a reactive infiltrate is found on biopsy of lesional skin.2 Non-specific lesions are more common and include petechiae, purpura, ecchymosis, vasculitis, neutrophilic dermatoses and opportunistic infections. Many non-specific manifestations of leukaemia are secondary to underlying cytopaenias and adverse drug reactions. LC is a specific manifestation of leukaemia. It is most commonly seen in acute myeloid leukaemia and manifests as papules, nodules, tumours and plaques that vary in colour from yellow, brown and red to violaceous.
Whether chilblain-like eruptions in patients with underlying haematological disorders represent specific (neoplastic) skin changes or non-specific leukaemoid reactions is debateable. Most previous reports from the literature have been from patients with myelomonocytic myelodysplasia and have been classified as leukaemoids.3 4 Our case meets criteria for LC because leukaemic cells were demonstrated in the lesion by histopathology. Chilblain-like eruptions in acute leukaemia are rare. To the best of our knowledge, there is a single previous case report of chilblain-like LC in a patient presenting in the blast crisis of chronic myelogenous leukaemia.5
It is unknown whether chilblain-like LC begins as a leukaemic infiltrate de novo or whether the leukaemic infiltrate secondarily involves a pre-existent non-specific chilblain-like eruption. LC has a predilection for damaged or inflamed skin and has been described at the sites of scars and prior dermatoses. Our patient had a high concentration of circulating blast cells in her peripheral blood at the time of biopsy and it is not surprising they were recognisable in routine sections of clinically inflamed skin. This suggests to us that malignant cells in chilblain-like LC may reflect the propensity of circulating leukaemia cells to infiltrate damaged skin rather than representing a specific lesion of LC, per se.
In sum, patients with chilblain-like lesions and a positive review of systems or an atypical presentation should be evaluated for underlying systemic illness. Complete blood count to exclude haematological dyscrasias, cryoglobulin and cold agglutinin, and cryofibrinogen assays to rule out cold-sensitive dysproteinaemia, serum protein electrophoresis for monoclonal gammopathy, antinuclear antibody testing to preclude chilblain lupus erythaematosus and biopsy, may be necessary depending on the clinical presentation.
Learning points.
Patients with atypical chilblains should be evaluated for systemic illness.
Atypical chilblains may be a clue to lupus erythaematosus, dysproteinaemia, sarcoidosis and haematological neoplasms.
Chilblain-like leukaemia cutis is associated with myelodysplasia and myeloid leukaemias.
Biopsy can be diagnostic of chilblain-like leukaemia cutis.
Footnotes
Competing interests: None declared.
Patient consent: Obtained.
Provenance and peer review: Not commissioned; externally peer reviewed.
References
- 1.Cappel JA, Wetter DA. Clinical characteristics, etiologic associations, laboratory findings, treatment, and proposal of diagnostic criteria of pernio (chilblains) in a series of 104 patients at Mayo Clinic, 2000 to 2011. Mayo Clin Proc 2014;89:207–15. 10.1016/j.mayocp.2013.09.020 [DOI] [PubMed] [Google Scholar]
- 2.Wagner G, Fenchel K, Back W et al. Leukemia cutis—epidemiology, clinical presentation, and differential diagnosis. J Dtsch Dermatol Ges 2012;10:27–36. 10.1111/j.1610-0387.2011.07842.x [DOI] [PubMed] [Google Scholar]
- 3.Kelly JW, Dowling JP. Pernio: a possible association with chronic myelomonocytic leukemia. Arch Dermatol 1985;121:1048–52. 10.1001/archderm.1985.01660080102025 [DOI] [PubMed] [Google Scholar]
- 4.Affleck AG, Ravenscroft JC, Leach IH. Chilblain-like leukemia cutis. Pediatr Dermatol 2007;24:38–41. 10.1111/j.1525-1470.2007.00330.x [DOI] [PubMed] [Google Scholar]
- 5.Yazawa H, Saga K, Omori F et al. The chilblain-like eruption as a diagnostic clue to the blast crisis of chronic myelocytic leukemia. J Am Acad Dermatol 2004;50(2 Suppl):S42–4. 10.1016/S0190 [DOI] [PubMed] [Google Scholar]