Abstract
Background:
More than 70 million couples suffer from infertility worldwide. The aim of this study was to evaluate the fertility outcomes after laparoscopic fimbrioplasty and neosalpingostomy in female infertility.
Methods:
Laparoscopic distal tuboplasty was carried out for 402 cases at the Gynecological Endoscopic Surgery and Human Reproductive Teaching Hospital in Yaoundé-Cameroon in Central Africa from December 2002 to December 2007. Laparoscopic fimbrioplasty and neosalpingostomy were done using bipolar electrocoagulation and conventional endoscopic instruments. Log-rank test was used to compare cumulative rate curves of intrauterine pregnancy with respect to the tubal stages. P<0.05 was considered statistically significant.
Results:
The mean age of the patients was 31.6±5.45 years. Secondary infertility was the most frequent type of infertility (70.14%). The laparoscopic tubal surgery done consisted of fimbrioplasty in 185(46%) cases and neosalpingostomy in 217 (54%) cases. Of 260 women followed up after tuboplasty, there were overall 74 (28.48%) pregnancies; 68(26.1%) intrauterine pregnancies and 6(2.3%) ectopic pregnancies. Pregnancy rates were significantly associated to the tubal stage (63% in stage 1, 15% in stage 3 and 00% in stage 4; p<0.001) and the adnexal adhesion scores (73.91% in the absence of adnexal adhesions and 8.8% in the case of a severe adnexal adhesion score). Of the 68 intrauterine pregnancies, there were 60(88%) live births and 8(12%) spontaneous abortions.
Conclusion:
It is believed that laparoscopic fimbrioplasty and neosalpingostomy should be the preferred choice when faced with tubal distal occlusion in a context of female infertility. This implies that training in endoscopic surgery should be regarded as an important issue in developing countries.
Keywords: Adnexal adhesion, Fimbrioplasty, Infertility, Laparoscopy, Neosalpingostomy, Tubal stage
Introduction
The clinical definition of infertility used by the World Health Organization (WHO) is “a disease of the reproductive system defined by the failure to achieve a clinical pregnancy after 12 months or more of regular unprotected sexual intercourse” (1). One of the most important and underappreciated reproductive health problems in developing countries is the high rate of infertility and childlessness (2, 3). The inability to procreate is frequently considered a personal tragedy and a curse for the couple, impacting on the entire family and even the local community (4–6). Although good documentation of the prevalence of infertility is lacking, it is generally believed that more than 70 million couples suffer from infertility worldwide (7).
Fallopian tube abnormalities account for up to 40% of female subfertility and are most often caused by infections (8). The post-infectious inflammation induces damage of the mucosa and the tube wall, with a flattening of mucosal folds, a deciliation and fibrosis of the wall (9).
In Africa, over 85% of women had an infertility diagnosis attributable to an infection compared with 33% of women worldwide (10).
Surgical techniques for tubal infertility have been tried and have success rates of around 50%, but depend on the severity of damage, associated abnormalities, technique of surgery (open versus microsurgery versus laparoscopic) and training of the surgeon (11, 12). Laparoscopic surgery is an important tool in the diagnosis and treatment of infertility (10, 13).
In the previous study carried out in 1997 at the yaoundé General Hospital, Cameroon on 194 patients, the overall pregnancy rate after laparoscopic distal tuboplasty was 27,3% (14).
The aim of this study was to evaluate the fertility outcome of laparoscopic fimbrioplasty and neosalpingostomy in female infertility from 402 cases at the Gynecological Endoscopic Surgery and Human Reproductive Teaching Hospital in Yaoundé - Cameroon in Central Africa.
Methods
This was a cross sectional descriptive retrospective study based on a review of medical records of patients operated by laparoscopy at the Gynecological Endoscopic Surgery and Human Reproductive Teaching Hospital in Yaoundé, Cameroon in Central Africa, from December 2002 to December 2007. Laparoscopic fimbrioplasty and neosalpingostomy were done using bipolar electrocoagulation and conventional endoscopic instruments. An adhesiolysis was performed first, when necessary. Tubal patency was then assessed by hydrotubation through a canula introduced into the uterine cavity. For fimbrioplasty, an atraumatic endoscopic forceps is inserted into the tubal ostium not completely closed, then the spacing of the jaws is often sufficient to separate the fringes of the flag. If not, the section will be done by scissors. Then, the eversion of the fringes is performed by light touching by bipolar electrocoagulation. For neosalpingostomy, the ampullary portion of the fallopian tube is distended by injecting blue intrauterine. Ostium is identified and opened by an atraumatic endoscopic forceps. Then, the flag is completely opened by 3 or 4 incisions with endoscopic scissors. Finally, the eversion is performed by light touching by bipolar electrocoagulation. Our study population included 402 patients who underwent laparoscopic distal tuboplasty for infertility during the study period. The variables studied were, the socio-demographic and clinical characteristics of the patients, the type of tuboplasty performed, and the pregnancy rate: intrauterine pregnancy (IUP) or ectopic pregnancy (EP) after tuboplasty. The patients lost to follow up were excluded at the analysis of the outcome of tuboplasty because they came very often from other regions of the country and returned there at the exit of the hospital after tuboplasty. The patients were divided into four tubal stages according to the French preoperative classification and into four groups according to the American fertility society classification of adnexal adhesion score (15, 16).
Data was entered and analyzed using SPSS and Microsoft Excel software. The overall pregnancy rate (IUP and EP) was calculated taking into consideration only patients followed up during the study period and participants lost to follow up were excluded. The cumulative pregnancy rate was also calculated. We used the chi-square test and the Student test to compare the different variables and the log-rank test to compare cumulative rate curves of intrauterine pregnancy with respect to the tubal stages. A p-value<0.05 was considered statistically significant.
Results
During the study period, 650 cases of laparoscopy were done for infertility at the Gynecological Endoscopic Surgery and Human Reproductive Teaching Hospital in Yaoundé. Of these, 402 patients who had distal tuboplasty were included in this study.
Characteristics of the study population:
The age of the patients in this study was between 19 and 44 years. The mean age of the patients was 31.6±5.45 years. Table 1 shows the characteristics of the study population. The patients aged less than 35 years represented 67.8% of our sample. Secondary infertility was the most frequent type of infertility (70.14%) and the mean duration of infertility was 8.29±5.9 years. A little more than half (53.73%) of the patients in this study had a positive Chlamydia trachomatis serology. Adnexal adhesions were present in 335 (83.3%) patients. The moderate and severe adnexal adhesion scores were found in about half (50.7%) of the patients. About half (49%) of the patients presented with severe tubal damage (stage 3 and 4 with respect to the French classification).
Table 1.
Characteristics of the study population
| Variables | Patients; (N=402) | |
|---|---|---|
| n | (%) | |
| Age (years) | ||
| 15–24 | 40 | (09.95) |
| 25–34 | 236 | (58.70) |
| 35–45 | 126 | (31.3) |
| Type of infertility | ||
| Primary | 120 | (29.85) |
| Secondary | 282 | (70.14) |
| Positive chlamydia serology | 216 | (53.73) |
| History of voluntary abortion | 160 | (39.80) |
| Mean infertility duration (years) | 08.29±5.9 | |
The occurrence of pregnancy after laparoscopic fimbrioplasty and neosalpingostomy:
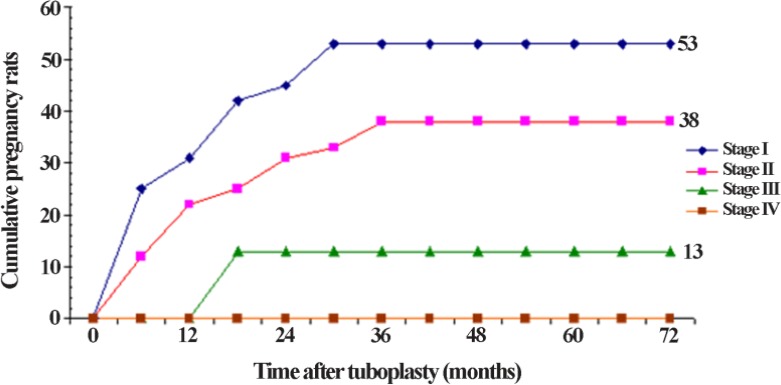
The laparoscopic tubal surgery done included fimbrioplasty in 185(46%) cases and neosalpingostomy in 217 (54%) cases. Complete or partial adhesiolysis was done in patients presenting with adnexal adhesions (83.03%). Table 2 shows the pregnancy rate after laparoscopic tuboplasty. Of the 260 women followed up after tuboplasty, 74(28.48%) got pregnant with 68(26.1%) intra uterine and 6(2.3%) extra uterine pregnancies. The adnexal adhesion score and tubal stage are two factors which influence the occurrence of pregnancy after tuboplasty. The absence of adnexal adhesions was associated with the highest pregnancy rates (73.91%) while the lowest pregnancy rates (8.8%) was seen in the group of women who had a severe adnexal adhesion score. Also, pregnancy rates were significantly associated to the tubal stage: 63% in stage 1, 15% in stage 3 and 00% in stage 4; p<0.001. The cumulative intrauterine pregnancy rate was higher in tubal stage 1 than in tubal stage 2 but this difference was not statistically significant (log-rank c2: 2.4; p=0.1). On the other hand, the cumulative intrauterine pregnancy rate was higher in tubal stage 1 than in tubal stage 3 and this difference was statistically significant (log-rank c2:=0.02; p< 0.001), figure 1. Of the 68 intrauterine pregnancies, there were 60(88%) deliveries and 8(12%) spontaneous abortions.
Table 2.
Pregnancies after tuboplasty with respect to the patients’ characteristics
| Characteristics | Number of patients | Overall pregnancy | IUP | EP | P-value |
|---|---|---|---|---|---|
| n (%) | n (%) | n (%) | |||
| Type of infertility | |||||
| Primary | 86 | 24 (27.9%) | -- | -- | 0.300 |
| Secondary | 174 | 50 (28.7%) | -- | -- | |
| Type of tuboplasty | |||||
| Fimbrioplasty | 120 | 40 (33) | 40 (33) | 0 (0) | 0.107 |
| Neosalpingostomy | 140 | 34 (24) | 28 (20) | 6 (4) | |
| Adnexal adhesion score | |||||
| Absent | 46 | 34 (73.91) | 32 (68%) | 2 (6%) | 0.000 * |
| Mild | 78 | 22 (28.20) | 20 (25.5%) | 2 (2.5%) | |
| Moderated | 68 | 12 (17.64) | 12 (17%) | 0 | |
| Severe | 68 | 6 (8.82) | 4 (6%) | 2 (3%) | |
| Tubal stage | |||||
| 1 | 82 | 52 (63.41) | 52 (63.4%) | 0 | 0.000 * |
| 2 | 32 | 18 (56.25) | 16 (50%) | 2 (6.2%) | |
| 3 | 26 | 4 (15.38) | 2 (7.7%) | 2 (7.7%) | |
| 4 | 120 | 0 | 0 | 0 | |
IUP: Intra Uterine Pregnancy; EP: Ectopic Pregnancy,
p<0.001
Figure 1.
Cumulative intra uterine pregnancy rate with respect to tubal stage
(Curves tubal stage 1 and 2: log-rank c2: 2, 4; p=0.1)
(Curves tubal stage 1 and 3: log-rank c2: 9; p=0.02)
Discussion
Pathologies of the fallopian tubes are responsible for about 20 to 30% of female infertility in the world (17). In the literature, several techniques have been used in the treatment of tubal disease. This goes from observation to laparotomy, gaseous insufflation, hydrotubation, microsurgery and more recently laparoscopic surgery (18).
The outcome of surgical treatment of distal tubal lesions has considerably improved (18–20). Several studies reveal that the global pregnancy rates after laparoscopic tuboplasty vary between 20 to 40% (21–25).
In this study, the global pregnancy rate after distal tuboplasty was 28.4% with 26.1% for the IUP and 2.3% for the EP. These rates of IUP and EP were comparable to those found by other authors; 33.3% and 6.9% for Canis et al. (22), 27.4% and 4.1% for Dubuisson et al. (23), 28.4% and 4% for Madelenat et al. (21) and 23.2% and 4.1% for Kasia et al. (14).
The pregnancy rate after neosalpingostomy is 10 to 33% and 20 to 60% after fimbrioplasty (14, 26, 27). Our results were within this range with a pregnancy rate after fimbrioplasty of 33% and 20% after neosalpingostomy.
As reported by several authors (14, 21–25), decreasing pregnancy rates were found in this study according to the tubal stage (stage 1: 63.41%; stage 2: 56.25%; stage 3: 15.38%; stage 4: 0%; p=0.000). The more damage of the tube was accompanied with the lesser the chances of having a pregnancy.
Tuboplasty is found as a risk factor for extrauterine pregnancy by several studies (29, 30). Therefore, the risk of EP after distal tuboplasty increases with worsening of tubal stage.
In accordance with a previous study done in Yaoundé (14), an increasing rate of EP was found after tuboplasty with respect to tubal stage (0% for stage 1; 6.2% for stage 2 and 7.7% for stage 3).
Adhesions involving the fallopian tube are considered as the causes of infertility. Several authors found an association between the degree of adnexal adhesions and the rate of occurrence of life births after adhesiolysis (19, 20, 31).
Adhesiolysis formerly was done by laparotomy with unsatisfactory results; the techniques of microsurgery and laparoscopic surgery have improved the results of adhesiolysis (19, 23). The pregnancy rates of 17% to 25.5% in the mild to moderate adnexal adhesion score and 6% in the severe adnexal adhesion score found in our study were comparable to those found in literature (19). The mean age of patients in our study was 31.2± 5.2 years which is close to that found by Kasia et al. in 1997 (14), Eyraud et al. (27), and Strandel et al. (32) who respectively reported mean ages of 31, 33 and 32 years. The mean duration of infertility of 8.29±5.9 years in this study was higher than that found by Strandell (32) and Eyraud (27) who reported, respectively, a mean infertility duration of 3.9 and 3.88 years. This discrepancy can be explained by the wide disparity that exists in the quality, availability, and delivery of infertility services between the developed and developing nations of the world (33).
One of the limits of this study was the high proportion of patients lost to follow up after tuboplasty which can be explained by the fact that the Gynecological Endoscopic Surgery and Human Reproductive Teaching Hospital in Yaoundé receives women from all regions of Cameroon for laparoscopic surgery for tuboperitoneal lesions. After surgery, some of these women returned to their respective regions for follow-up.
Conclusion
The results of this study revealed that the global pregnancy rate after laparoscopic fimbrioplasty and neosalpingostomy was 28.4% in our context and was comparable to 20–40% found in literature. The tubal stage and the adnexal adhesion score are two main factors influencing the occurrence of pregnancy after fimbrioplasty and neosalpingostomy. In our context where access to in vitro fertilization remains limited, it is believed that laparoscopic fimbrioplasty and neosalpingostomy should be the preferred choice when faced with tubal distal occlusion in a context of female infertility. This implies that training in endoscopic surgery should be regarded as an important issue in developing countries.
Footnotes
Conflict of Interest
The authors declare that there is no conflict of interest regarding the publication of this paper.
References
- Zegers-Hochschild F, Adamson GD, de Mouzon J, Ishihara O, Mansour R, Nygren K, et al. The International Committee for Monitoring Assisted Reproductive Technology (ICMART) and the World Health Organization (WHO) Revised Glossary on ART Terminology, 2009. Hum Reprod. 2009; 24 ( 11): 2683– 7. [DOI] [PubMed] [Google Scholar]
- Leke RJ, Oduma JA, Bassol-Mayagoitia S, Bacha AM, Grigor KM. Regional and geographical variations in infertility: effects of environmental, cultural, and socioeconomic factors. Environ Health Perspect. 1993; 101 Suppl 2 :73– 80. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bergstrom S. Reproductive failure as a health priority in the Third World: a review. East Afr Med J. 1992; 69 (4): 174– 80. [PubMed] [Google Scholar]
- Daar AS, Merali Z. Infertility and social suffering: the case of ART in developing countries. In: Vayena E , Rowe PJ , Griffin PD , editors. Current Practices and Controversies in Assisted Reproduction. Geneva, Switzerland: World Health Organization; 2002. 396 p. [Google Scholar]
- Dyer SJ, Abrahams N, Hoffman M, van der Spuy ZM. ‘Men leave me as I cannot have children’: women’s experiences with involuntary childlessness. Hum Reprod. 2002; 17 (6): 1663– 8. [DOI] [PubMed] [Google Scholar]
- Umezulike AC, Efetie ER. The psychological trauma of infertility in Nigeria. Int J Gynaecol Obstet. 2004; 84 (2): 178– 80. [DOI] [PubMed] [Google Scholar]
- Boivin J, Bunting L, Collins JA, Nygren KG. International estimates of infertility prevalence and treatment-seeking: potential need and demand for infertility medical care. Hum Reprod. 2007; 22 (6): 1506– 12. [DOI] [PubMed] [Google Scholar]
- Steinkeler JA, Woodfield CA, Lazarus E, Hillstrom MM. Female infertility: a systematic approach to radiologic imaging and diagnosis. Radiographics. 2009; 29 (5): 1353– 70. [DOI] [PubMed] [Google Scholar]
- Donnez J, Casanas-Roux F. Prognostic factors of fimbrial microsurgery. Fertil Steril. 1986; 46 (2): 200– 4. [DOI] [PubMed] [Google Scholar]
- Ombelet W, Cooke I, Dyer S, Serour G, Devroey P. Infertility and the provision of infertility medical services in developing countries. Hum Reprod Update. 2008; 14 (6): 605– 21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Fathalla MF, Sinding SW, Rosenfield A, Fathalla MM. Sexual and reproductive health for all: a call for action. Lancet. 2006; 368 (9552): 2095– 100. [DOI] [PubMed] [Google Scholar]
- Okonofua FE, Essen UI, Nimalaraj T. Hysterosal-pingography versus laparoscopy in tubal infertility: comparison based on findings at laparatomy. Int J Gynaecol Obstet. 1989; 28 (2): 143– 7. [DOI] [PubMed] [Google Scholar]
- Sharma S, Mittal S, Aggarwal P. Management of infertility in low resource countries. BJOG. 2009 . ; 116 Suppl 1 :77– 83. [DOI] [PubMed] [Google Scholar]
- Kasia JM, Raiga J, Doh AS, Biouele JM, Pouly JL, Kwiatkowski F, et al. Laparoscopic fimbrioplasty and neosalpingostomy. Experience of the Yaounde General Hospital, Cameroon (report of 194 cases). Eur J Obstet Gynecol Reprod Biol. 1997; 73 (1): 71– 7. [DOI] [PubMed] [Google Scholar]
- American Fertility Society. Classification of adnexal adhesions, distal tubal occlusions secondary to tubal ligation, tubal pregnancies, mullerian abnormalities and intra uterine adhesions. Fertil Steril. 1988; 49 (6): 944– 55. [DOI] [PubMed] [Google Scholar]
- Mage G, Pouly JL, de Joliniere JB, Chabrand S, Riouallon A, Bruhat MA. A preoperative classification to predict the intrauterine and ectopic pregnancy rates after distal tubal microsurgery. Fertil Steril. 1986; 46 (5): 807– 10. [DOI] [PubMed] [Google Scholar]
- De Cherney AH. Tubal disease: surgery and in vitro fertilization. In: Kase NG , Weingold AB , Gershenson DM , editors. Principles and Practice of Clinical Gynecology. London, England: Churchill Livingstone; 1990. p. 445– 57. [Google Scholar]
- El-Mowafi DM, Ngoh NN. Management of tubal obstructions. Surg Technol Int. 2005; 14: 199– 212. [PubMed] [Google Scholar]
- Berker B, Mahdavi A, Shahmohamady B, Nezhat C. Role of laparoscopic surgery in infertility. Middle East Fertil Soc J. 2005; 10 (2): 94– 104. [Google Scholar]
- Bruhat MA, Mage G, Pouly JL, Manhes H, Canis M, Wattiez A. [Adhesions in operatory laparoscopy]. Paris: Medsi/McGraw-Hill; ;1989. 215 p. French. [Google Scholar]
- Madelenat P, Filoux Y, Hazout A, Palmer R. [Laparoscopic treatment of stenoses and phimosis of the ampulla of the tube. A critical study of the results (author’s transl)]. J Gynecol Obstet Biol Reprod (Paris). 1979; 8 (5): 445– 50. French. [PubMed] [Google Scholar]
- Canis M, Mage G, Pouly JL, Manhes H, Wattiez A, Bruhat MA. Laparoscopic distal tuboplasty: report of 87 cases and a 4-year experience. Fertil Steril. 1991; 56 (4): 616– 21. [DOI] [PubMed] [Google Scholar]
- Dubuisson JB, Bouquet de Joliniere J, Aubriot FX, Darai E, Foulot H, Mandelbrot L. Terminal tuboplasties by laparoscopy: 65 consecutive cases. Fertil Steril. 1990; 54 (3): 401– 3. [DOI] [PubMed] [Google Scholar]
- Larue L, Sedbon E, Crequat J, Madelenat P. [Percelioscopic surgery of the distal fallopian tube in infertility]. J Gynecol Obstet Biol Reprod (Paris). 1990; 19 (3): 343– 7. French. [PubMed] [Google Scholar]
- Ahmad G, Watson AJ, Metwally M. Laparoscopy or laparotomy for distal tubal surgery? A meta-analysis. Hum Fertil (Camb). 2007; 10 (1): 43– 7. [DOI] [PubMed] [Google Scholar]
- Dlugi AM, Reddy S, Saleh WA, Mersol-Barg MS, Jacobsen G. Pregnancy rates after operative endoscopic treatment of total (neosalpingostomy) or near total (salpingostomy) distal tubal occlusion. Fertil Steril. 1994; 62 (5): 913– 20. [DOI] [PubMed] [Google Scholar]
- Eyraud B, Erny R, Vergnet F. [Distal tubal surgery using laparoscopy]. J Gynecol Obstet Biol Reprod (Paris). 1993; 22 (1): 9– 14. French. [PubMed] [Google Scholar]
- Audebert AJ, Pouly JL, Von Theobald P. Laparoscopic fimbrioplasty: an evaluation of 35 cases. Hum Reprod. 1998; 13 (6): 1496– 9. [DOI] [PubMed] [Google Scholar]
- Nordenskjold F, Ahlgren M. Risk factors in ectopic pregnancy. Results of a population-based case-control study. Acta Obstet Gynecol Scand. 1991; 70 (7–8): 575– 9. [DOI] [PubMed] [Google Scholar]
- Bouyer J, Coste J, Shojaei T, Pouly JL, Fernandez H, Gerbaud L, et al. Risk factors for ectopic pregnancy: a comprehensive analysis based on a large case-control, population-based study in France. Am J Epidemiol. 2003; 157 (3): 185– 94. [DOI] [PubMed] [Google Scholar]
- Gomel V. Salpingo-ovariolysis by laparoscopy in infertility. Fertil Steril. 1983; 40 (5): 607– 11. [PubMed] [Google Scholar]
- Strandell A, Bryman I, Janson PO, Thorburn J. Background factors and scoring systems in relation to pregnancy outcome after fertility surgery. Acta Obstet Gynecol Scand. 1995; 74 (4): 281– 7. [DOI] [PubMed] [Google Scholar]
- Nachtigall RD. International disparities in access to infertility services. Fertil Steril. 2006; 85 (4): 871– 5. [DOI] [PubMed] [Google Scholar]