Abstract
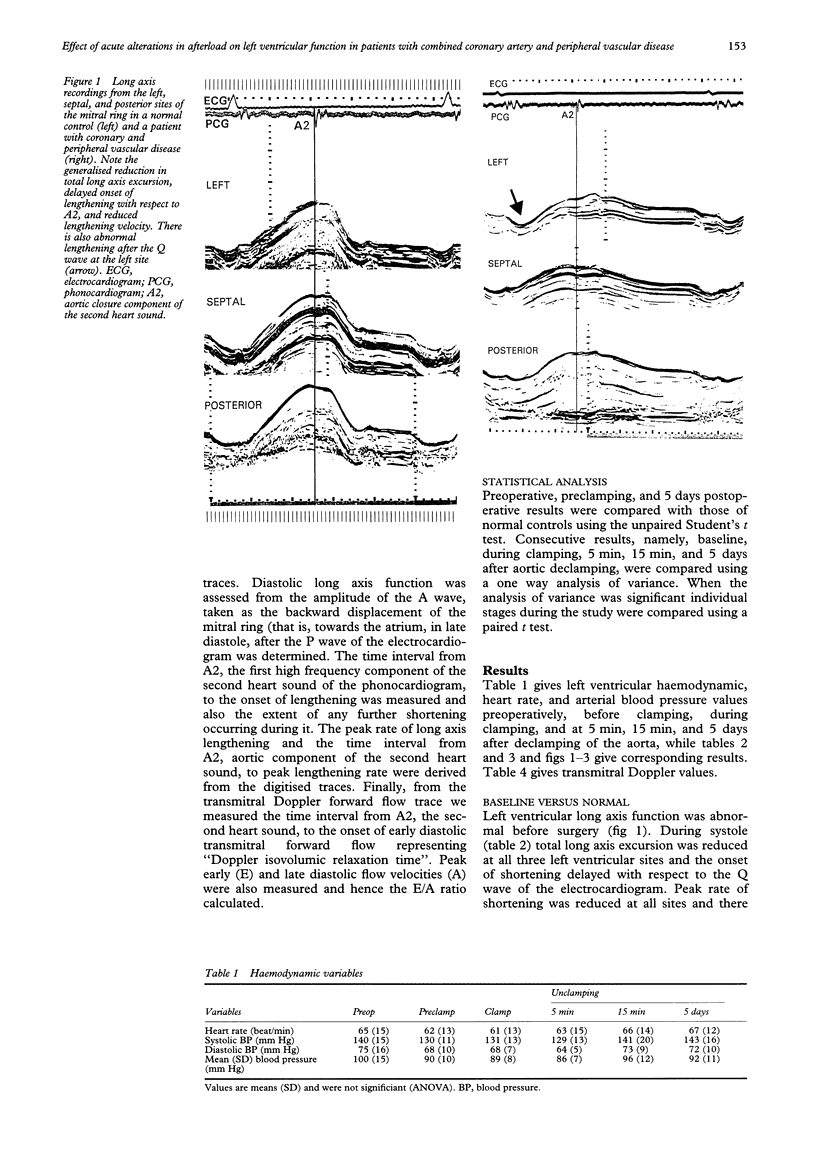
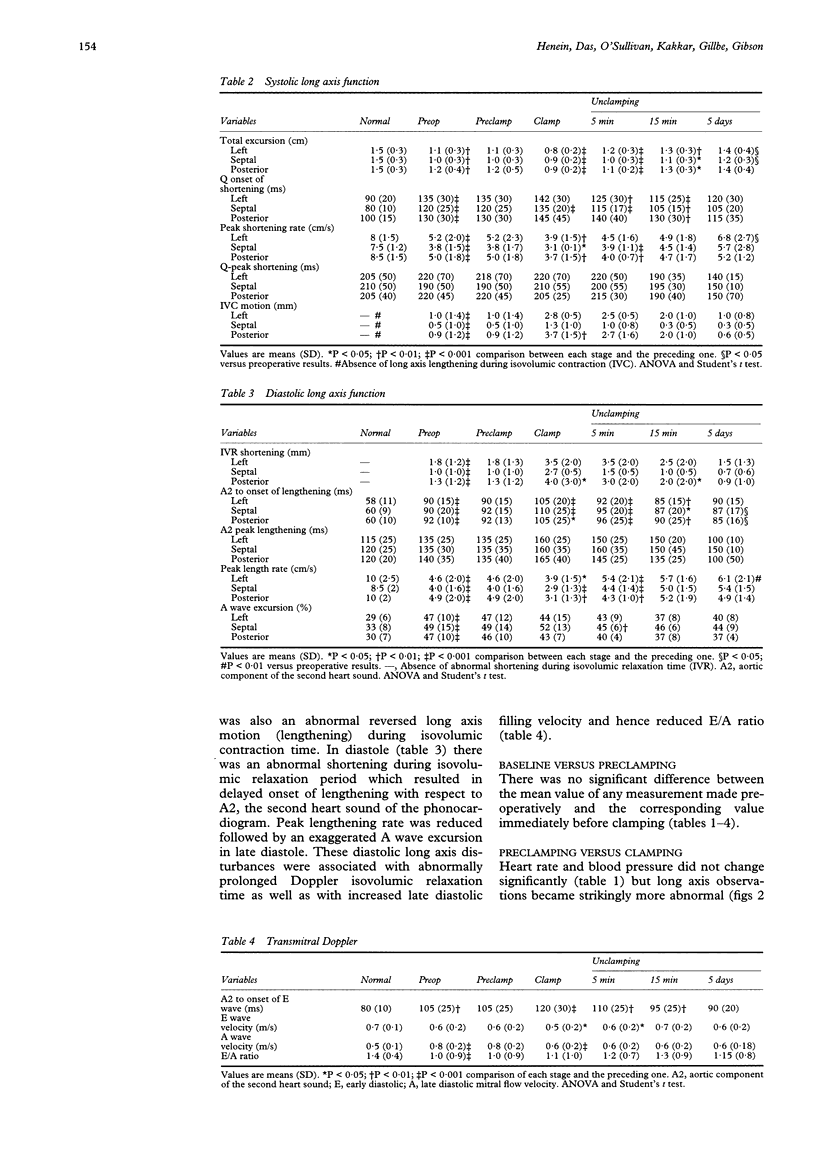
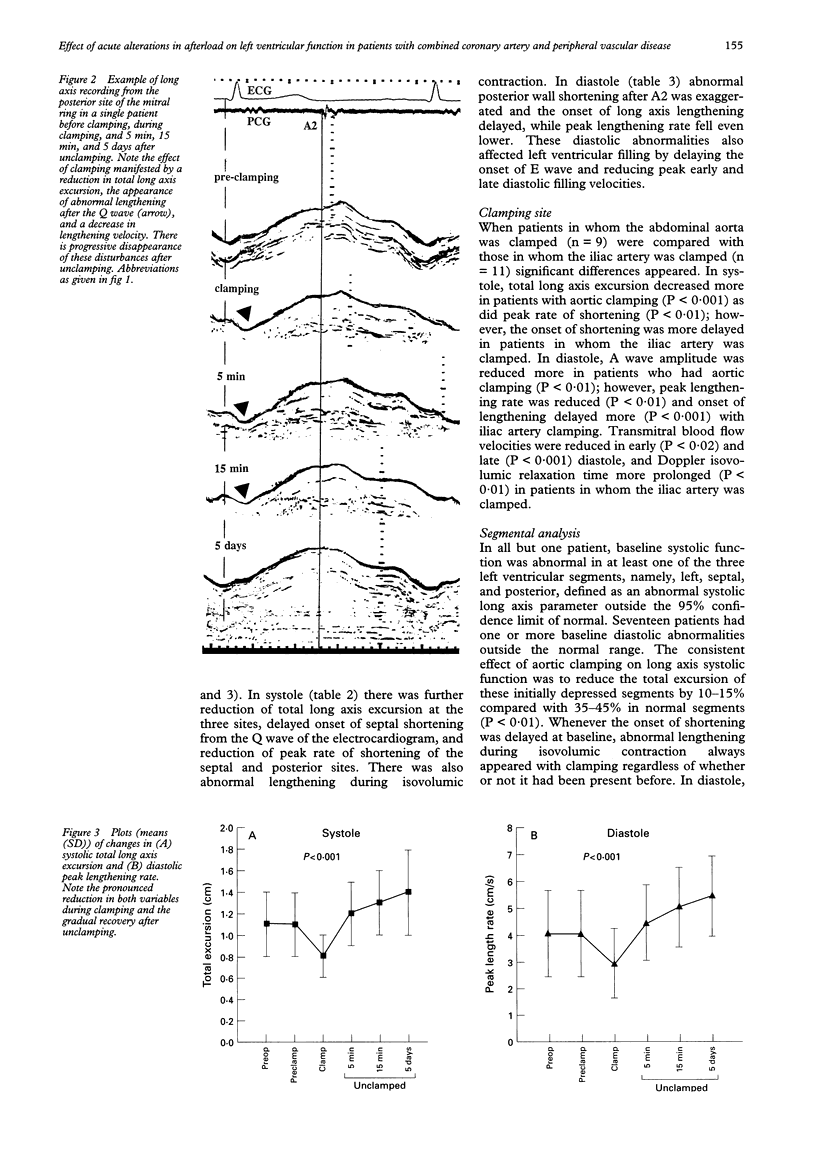
OBJECTIVE: To assess the effect of acute alterations in afterload by aortoiliac clamping, during peripheral vascular surgery, on left ventricular function. DESIGN: Prospective examination of the left ventricular long axis and transmitral Doppler flow preoperatively and intraoperatively; before aortic clamping, during clamping and 5 min, 15 min, and 5 days after unclamping. SETTING: A tertiary referral centre for cardiac and vascular disease equipped with invasive and non-invasive facilities. PATIENTS: 20 patients (11 men; mean (SD) age 61 (8) years) with significant aortoiliac disease and documented coronary artery disease and 21 normal controls of similar age. RESULTS: Preoperatively: long axis function was abnormal compared with that in normal controls. In systole total long axis excursion and peak shortening rate were reduced, onset of shortening delayed, and there was pre-ejection lengthening (P < 0.001). In diastole there was abnormal shortening during isovolumic relaxation, delaying the onset of long axis lengthening (P < 0.001). Peak lengthening rate was also reduced and A wave excursion increased (P < 0.001). Transmitral Doppler showed increased A wave velocity and reduced peak E/A diastolic flow velocities ratio (P < 0.001). Intraoperatively: preclamping results did not differ from those before operation. With clamping the extent of systolic and diastolic abnormalities promptly increased as to a lesser extent did those of transmitral flow velocity, although heart rate and blood pressure did not change significantly. Total long axis excursion and A wave amplitude were more reduced by aortic than iliac clamping, whereas the onset of lengthening was more delayed and the lengthening velocity more reduced with iliac clamping. Some 5 min after unclamping systolic long axis function had already returned towards normal; total excursion increased, as did the peak shortening rate, and the onset of shortening became less delayed (P < 0.001). In diastole the delayed onset of lengthening regressed, its lengthening velocity increased, and A wave excursion fell (P < 0.001). Early diastolic transmitral flow velocity also increased. This improvement in systolic and diastolic long axis function had progressed 15 min after unclamping but showed no further change at 5 days. At 5 days after operation, however, systolic and diastolic measurements had improved compared with those preoperatively. CONCLUSION: Resting left ventricular long axis function is abnormal in patients with combined coronary artery disease and peripheral vascular disease. It is unaffected by anaesthesia but deteriorates with aortic or iliac clamping, although blood pressure remains unchanged. It promptly improves with unclamping after successful peripheral arterial reconstruction. Thus, even in apparently stable coronary artery disease, resting subendocardial function is labile, showing pronounced alterations with changing after-load, even when arterial pressure itself does not change.
Full text
PDF




Selected References
These references are in PubMed. This may not be the complete list of references from this article.
- Bogren H. G., Mohiaddin R. H., Klipstein R. K., Firmin D. N., Underwood R. S., Rees S. R., Longmore D. B. The function of the aorta in ischemic heart disease: a magnetic resonance and angiographic study of aortic compliance and blood flow patterns. Am Heart J. 1989 Aug;118(2):234–247. doi: 10.1016/0002-8703(89)90181-6. [DOI] [PubMed] [Google Scholar]
- Brutsaert D. L., Housmans P. R., Goethals M. A. Dual control of relaxation. Its role in the ventricular function in the mammalian heart. Circ Res. 1980 Nov;47(5):637–652. doi: 10.1161/01.res.47.5.637. [DOI] [PubMed] [Google Scholar]
- Henein M. Y., Priestley K., Davarashvili T., Buller N., Gibson D. G. Early changes in left ventricular subendocardial function after successful coronary angioplasty. Br Heart J. 1993 Jun;69(6):501–506. doi: 10.1136/hrt.69.6.501. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hertzer N. R., Beven E. G., Young J. R., O'Hara P. J., Ruschhaupt W. F., 3rd, Graor R. A., Dewolfe V. G., Maljovec L. C. Coronary artery disease in peripheral vascular patients. A classification of 1000 coronary angiograms and results of surgical management. Ann Surg. 1984 Feb;199(2):223–233. doi: 10.1097/00000658-198402000-00016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jones C. J., Raposo L., Gibson D. G. Functional importance of the long axis dynamics of the human left ventricle. Br Heart J. 1990 Apr;63(4):215–220. doi: 10.1136/hrt.63.4.215. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kelly R. P., Tunin R., Kass D. A. Effect of reduced aortic compliance on cardiac efficiency and contractile function of in situ canine left ventricle. Circ Res. 1992 Sep;71(3):490–502. doi: 10.1161/01.res.71.3.490. [DOI] [PubMed] [Google Scholar]
- Leppo J., Plaja J., Gionet M., Tumolo J., Paraskos J. A., Cutler B. S. Noninvasive evaluation of cardiac risk before elective vascular surgery. J Am Coll Cardiol. 1987 Feb;9(2):269–276. doi: 10.1016/s0735-1097(87)80374-1. [DOI] [PubMed] [Google Scholar]
- Parker K. H., Jones C. J., Dawson J. R., Gibson D. G. What stops the flow of blood from the heart? Heart Vessels. 1988;4(4):241–245. doi: 10.1007/BF02058593. [DOI] [PubMed] [Google Scholar]
- Stefanadis C., Stratos C., Boudoulas H., Kourouklis C., Toutouzas P. Distensibility of the ascending aorta: comparison of invasive and non-invasive techniques in healthy men and in men with coronary artery disease. Eur Heart J. 1990 Nov;11(11):990–996. doi: 10.1093/oxfordjournals.eurheartj.a059639. [DOI] [PubMed] [Google Scholar]
- Upton M. T., Gibson D. G., Brown D. J. Echocardiographic assessment of abnormal left ventricular relaxation in man. Br Heart J. 1976 Oct;38(10):1001–1009. doi: 10.1136/hrt.38.10.1001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Urschel C. W., Covell J. W., Sonnenblick E. H., Ross J., Jr, Braunwald E. Effects of decreased aortic compliance on performance of the left ventricle. Am J Physiol. 1968 Feb;214(2):298–304. doi: 10.1152/ajplegacy.1968.214.2.298. [DOI] [PubMed] [Google Scholar]
- Van Den Bos G. C., Westerhof N., Elzinga G., Sipkema P. Reflection in the systemic arterial system: effects of aortic and carotid occlusion. Cardiovasc Res. 1976 Sep;10(5):565–573. doi: 10.1093/cvr/10.5.565. [DOI] [PubMed] [Google Scholar]
- Van Den Bos G. C., Westerhof N., Elzinga G., Sipkema P. Reflection in the systemic arterial system: effects of aortic and carotid occlusion. Cardiovasc Res. 1976 Sep;10(5):565–573. doi: 10.1093/cvr/10.5.565. [DOI] [PubMed] [Google Scholar]
- Watanabe H., Ohtsuka S., Kakihana M., Sugishita Y. Coronary circulation in dogs with an experimental decrease in aortic compliance. J Am Coll Cardiol. 1993 May;21(6):1497–1506. doi: 10.1016/0735-1097(93)90330-4. [DOI] [PubMed] [Google Scholar]
- Watanabe H., Ohtsuka S., Kakihana M., Sugishita Y. Coronary circulation in dogs with an experimental decrease in aortic compliance. J Am Coll Cardiol. 1993 May;21(6):1497–1506. doi: 10.1016/0735-1097(93)90330-4. [DOI] [PubMed] [Google Scholar]
- Watanabe H., Ohtsuka S., Kakihana M., Sugishita Y. Decreased aortic compliance aggravates subendocardial ischaemia in dogs with stenosed coronary artery. Cardiovasc Res. 1992 Dec;26(12):1212–1218. doi: 10.1093/cvr/26.12.1212. [DOI] [PubMed] [Google Scholar]



