Abstract
Introduction
High telomerase activity has been detected in the majority of malignant neoplasms including lung cancer. The purpose of the study was to attempt to use telomerase activity as a prognostic factor in patients with non-small cell lung cancer (NSCLC).
Material and methods
Telomerase activity was analyzed in 47 tissue specimens taken from patients with NSCLC. The control group consisted of 30 specimens of non-cancerous lung parenchyma. Telomerase activity was measured by means of the telomeric repeat amplification protocol (TRAP).
Results
Telomerase activity in the neoplastic tissue was significantly higher than in the lung parenchyma that was free from neoplastic infiltration. There was no significant association between telomerase activity and age, gender, tobacco smoking, histological type of the tumor, or staging (pTNM). No association was found between the level of telomerase activity in NSCLC specimens and the two-year survival rate of patients (p = 0.326). A higher level of telomerase activity in poorly differentiated tumors (G3) as compared to moderately differentiated tumors (G2) was detected (p = 0.008). A positive association was identified between telomerase activity in pulmonary parenchyma free from tumor infiltration and the presence of leukocyte infiltration (p = 0.0001).
Conclusions
No association was found between the level of telomerase activity in NSCLC specimens and the two-year survival rate of patients. The study has revealed a positive association between telomerase activity and the grade of differentiation (G) in NSCLC.
Keywords: telomerase, TRAP, lung cancer, survival rate
Abstract
Wstęp
Wysoka aktywność telomerazy jest stwierdzana w większości nowotworów złośliwych, w tym również w raku płuca. Celem pracy była próba oceny aktywności telomerazy jako czynnika prognostycznego u pacjentów z niedrobnokomórkowym rakiem płuca (non-small cell lung cancer – NSCLC).
Materiał i metody
Aktywność telomerazy oznaczono w tkankach guza pochodzących od 47 pacjentów z potwierdzonym w badaniu histopatologicznym NSCLC. Grupę kontrolną stanowiło 30 fragmentów tkanki płucnej wolnej od nacieku nowotworowego. Do oznaczenia aktywności telomerazy wykorzystano metodę amplifikacji powtórzeń telomerowych (telomeric repeat amplification protocol – TRAP).
Wyniki
Aktywność telomerazy w tkance nowotworowej była znamiennie wyższa od aktywności w tkance wolnej od nacieku nowotworowego. Nie wykazano zależności pomiędzy aktywnością telomerazy a wiekiem, płcią, paleniem tytoniu, typem histologicznym nowotworu oraz stopniem zaawansowania klinicznego (pTNM). Wykazano, że aktywność telomerazy w guzach nisko zróżnicowanych (G3) jest istotnie wyższa niż w przypadku guzów o większym stopniu zróżnicowania (G2) (p = 0,008). Nie wykazano znamiennej zależności pomiędzy aktywnością telomerazy a 2-letnim czasem przeżycia pacjentów z NSCLC (p = 0,326). Ponadto wykazano pozytywną korelację pomiędzy aktywnością telomerazy w tkance płucnej bez zmian nowotworowych a obecnością nacieku leukocytarnego (p = 0,0001).
Wnioski
Autorzy nie wykazali zależności pomiędzy aktywnością telomerazy a 2-letniem czasem przeżycia pacjentów z NSCLC. Dowiedziono także, że istnieje pozytywna korelacja pomiędzy aktywnością telomerazy a stopniem zróżnicowania nowotworu (G) w przypadku NSCLC.
Introduction
Almost 99% of gene mutations leading to the development of lung cancer are somatic mutations. These mutations can occur in oncogenes as well as suppressor genes that control the cell cycle and are responsible for telomerase activity [1].
Telomeres are nucleoproteins that play an essential role in the stable maintenance of the eukaryotic chromosome and protect it from exonucleases that may damage the coding sequences of the DNA. They cap the ends of linear chromosomes, thereby preventing end-to-end fusion and other mutations that are normally lethal to the cell. In most eukaryotes, telomeric DNA consists of repeated sequences. In humans, this is a sequence of 6 nucleotides, TTAGGG, repeated for approx. 15 kb, observed since the moment of birth. This sequence shortens throughout the life of an organism. In certain chronic illnesses, this process proceeds very rapidly [2].
Telomerase is a reverse transcriptase which elongates the telomeres, thereby stabilizing their structure and protecting the end of the chromosome during mitosis. The cells in which it operates become basically immortal and capable of dividing indefinitely. Human telomerase consists of a catalytic protein subunit, an RNA-dependent DNA polymerase referred to as human telomerase reverse transcriptase (hTERT), and one molecule of human template RNA (hTR). It is the hTR that constitutes the template for building telomere sequences. Under normal conditions, telomerase activity in humans occurs in quickly dividing cells such as gametes, fibroblasts, marrow stem cells, or activated T cells and B cells [1].
Despite the fact that telomerase activity is detected in 85-90% of cancer cells, it does not directly contribute to their emergence [3]. Instead, the moment of its activation is of decisive importance here. If telomerase activation occurs after the interaction of an oncogene or other mechanisms of carcinogenesis (when the first tumor cell has already been created), the tumorigenic process will take place. The cells will become immortal and capable of dividing indefinitely. However, the telomerase can also suppress tumorigenicity. If inactive, it reduces the number of cell divisions and, thereby, the possibility of occurrence of a critical number of mutations. If activated in healthy cells, the telomerase stabilizes the genome by elongating the telomeres.
Cancer cells have shorter telomeres than healthy cells; therefore, they need stable high telomerase activity [3]. In 89% of cases, in the preinvasive stage of bladder cancer, head and neck cancer, colon cancer, esophageal cancer, and oral cavity cancer, telomeres were proven to be very short. The initial stages of epithelial carcinogenesis are characterized by shortening of telomeres, which thereby lose their protective capabilities [4].
The purpose of the study was to determine the impact of the telomerase activity level on prognosis in patients with non-small cell lung cancer (NSCLC).
Material and methods
The study covered a group of 47 NSCLC patients in various stages of disease progression, treated with surgery in the Department of Thoracic Surgery of the Specialist Hospital of Lung Diseases and Tuberculosis in Bystra Śląska in 2009-2010.
The study was approved by the Bioethics Commission of the Medical University of Silesia (approval no. KNW/0022/KB1/119/I/09).
The cohort of patients covered by the study included 12 females and 35 males aged 49 to 75 (median age: 62).
The material for the study was constituted by specimens of neoplastic tissue obtained during surgery, and the control group was formed by specimens of parenchyma collected from the lungs deemed free from tumor infiltration at least 5 cm from the edge of the tumor. The collected tissue specimens were frozen at a temperature of –70°C and then transported to the molecular research lab of the Department of Medical and Molecular Biology in Zabrze for analysis.
The assessment of the histological specimens was conducted in the Pathomorphology Lab of the Beskid Oncology Center in Bielsko-Biała. All the histological specimens were independently verified by two pathomorphologists. The histological type of the tumor was determined in the microscopic examination. In addition, the clinical and pathological staging of the tumor (pTNM) and the grade of differentiation (G) were determined. Furthermore, the absence of tumor infiltration in the parenchyma of the lung that was deemed healthy, from which the specimens were obtained for examination, was each time confirmed with histopathological examination.
After being secured, the tissues were used as material for the preparation of 10-15 µm thick slices using a freezing microtome. Next, approx. 50 slices were transferred to sterile reaction tubes containing 200 µl of lysis reagent, pre-cooled on ice, comprising the TeloTAGGG Telomerase PCR ELISA PLUS (cat. no. 12 013 789 001, Roche, USA) set. The slices were subjected to mechanical homogenization until a uniform mixture was obtained. After a 30-minute incubation on ice, the lysate was centrifuged (for 20 minutes, at 16 000 x g, at a temperature of 2-8°C), and the supernatant was carefully transferred to a new reaction tube. To obtain valid quantitative analysis of the telomerase products, each sample should have the same protein content. With this in mind, the total level of protein in the supernatant was determined using the Lowry protein assay. The remaining part of the solution was mixed with the same volume of liquid nitrogen and stored at –80°C until further tests.
The obtained supernatant was used for determining the telomerase activity with the PCR ELISA PLUS protocol (www.roche-applied-science.com). During the first stage, telomerase activity was measured by means of a Telomeric Repeat Amplification Protocol (TRAP) assay using a pair of specific primers: P1 and P2; the former primer was labeled with biotin. In this reaction, telomerase adds 6-nucleotide TTAGGG telomeric repeats to the 3’-end of the biotin labeled P1-TS-primer. Next, the elongation products were amplified by PCR using primers P1-TS and anchor primer P2. The PCR products derived from the telomerase-mediated elongation products contained telomerase-specific 6-nucleotide increments. During the second stage, the PCR products were denatured and hybridized separately to digoxigenin-labeled detection probes specific for the telomeric repeats. The resulting products were immobilized via the biotin label to a streptavidin-coated microplate. Immobilized amplicons were then detected with an antibody against digoxigenin that is conjugated to horseradish peroxidase. In the final stage of the ELISA reaction, 3,3’,5,5’-tetramethylbenzidine (TMB) was added and transformed into a stained product under the influence of horseradish peroxidase. The staining reaction was halted by acidifying the environment, i.e. adding 5% sulfuric acid. After approx. 30 minutes, the color intensity of the solution was analyzed with a spectrophotometer at a wavelength of 450 nm and compared with a control test. Telomerase activity was given in Relative Telomerase Activity (RTA) units.
Statistica v.10 software (Statsoft Inc. 2011) was used for statistical analysis. The data concerning the frequency of occurrence were presented in the form of absolute values and percentages. The results of ordinal variables and interval variables were presented in the form of 95% confidence intervals, medians, minimums and maximums, and in the form of average values and standard deviations. For continuous variables, Pearson's χ2 test was used for the analysis of correlations. Student's t-test was used for the comparison of dichotomous variables with normal distribution. The Mann-Whitney U test was used for variables with non-normal distributions. The Kaplan-Meier estimator was used for the estimation of survival, and the χ2 test was used for the comparison of survival curves. Values of p < 0.05 were accepted as statistically significant.
Results
The analysis encompassed 47 NSCLC tumor specimens and 30 specimens of pulmonary parenchyma deemed free from tumor infiltration. Telomerase activity was detected in 45 out of 47 (95.7%) NSCLC tumor specimens and in 20 out of 30 (66.7%) specimens free from tumor infiltration.
The average telomerase activity in the neoplastic tissue samples obtained intraoperatively from 45 patients was 971.1 RTA units; it was significantly higher than telomerase activity in the healthy pulmonary parenchyma: 51.46 RTA units (p < 0.0001).
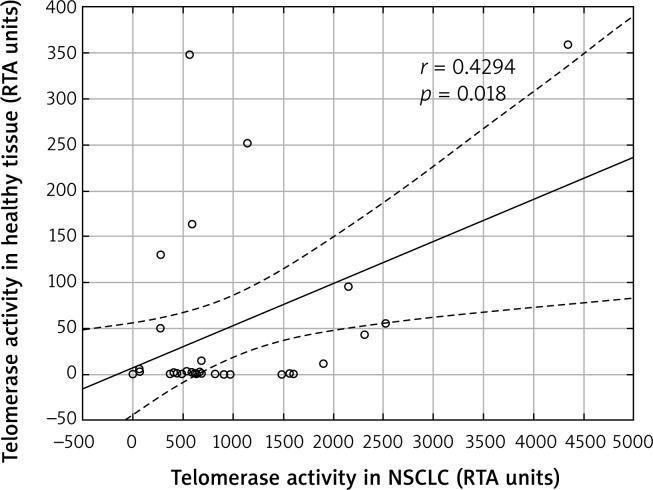
In addition, a positive association was found between increased telomerase activity in the tumor and the increased telomerase activity in the parenchyma of the lung that was deemed healthy (p = 0.018; r = 0.4294) (Fig. 1).
Fig. 1.
Correlation between telomerase activity in non-small cell lung cancer (NSCLC) tumor specimens and in pulmonary parenchyma free from tumor infiltration
It was also demonstrated that telomerase activity in poorly differentiated (high grade) NSCLC (G3) was significantly higher than in moderately differentiated (intermediate grade) tumors (G2) (p = 0.008) (Table I).
Tab. I.
Telomerase activity in non-small cell lung cancer (NSCLC) tumor specimens depending on various clinical and pathological factors
| Clinical and pathological factors | N [%] | Average telomerase activity | P | |
|---|---|---|---|---|
| Gender | F | 12 (25.5) | 964.98 | 0.818 |
| M | 35 (74.5) | 895.40 | ||
| Tobacco smoking | Yes | 33 (70.2) | 1038.08 | 0.140 |
| No | 14 (29.8) | 618.73 | ||
| Type of histological pattern | Squamous cell carcinoma | 33 (70.2) | 951.82 | 0.652 |
| Adenocarcinoma | 14 (29.8) | 822.06 | ||
| Grading | G2 | 18 (38.3) | 488.94 | 0.008 |
| G3 | 29 (61.7) | 1176.48 | ||
| Angioinva-sion | Yes | 27 (57.5) | 917.14 | 0.972 |
| No | 20 (42.5) | 907.80 | ||
| pTNM | I | 14 (29.8) | 938.21 | 0.901 |
| II-III | 33 (70.2) | 902.54 | ||
| T: Primary tumor | T1 | 11 (23.4) | 677.51 | 0.320 |
| T2-T3 | 36 (76.6) | 985.52 | ||
| N: Lymph nodes | N0 | 21 (44.7) | 1087.31 | 0.231 |
| N1-N2 | 26 (55.3) | 772.52 | ||
| Infiltration of the pulmona-ry pleura | Yes | 20 (42.5) | 818.24 | 0.534 |
| No | 27 (57.5) | 983.48 | ||
On the other hand, no significant difference in telomerase activity was observed between the various stages of the tumor (pTNM), types of the histopathological pattern, sizes of the tumor, degrees of involvement of nearby (regional) lymph nodes, presence of infiltration in the pleura of the lung, detection of angioinvasion in histopathological examination, and patient gender. Moreover, it was also determined that there was no statistically significant correlation between the intensity of tobacco smoking and the level of telomerase activity in the tumor (r = –0.0186; p = 0.922) or in the parenchyma of the lung free from neoplastic infiltration (r = –0.1754; p = 0.354).
Telomerase activity in the resected pulmonary parenchyma that was free from tumor infiltration but in which leukocyte infiltration was detected amounted to 116.97; it was significantly higher than in the parenchyma without such infiltration: 1.37 (p = 0.0001).
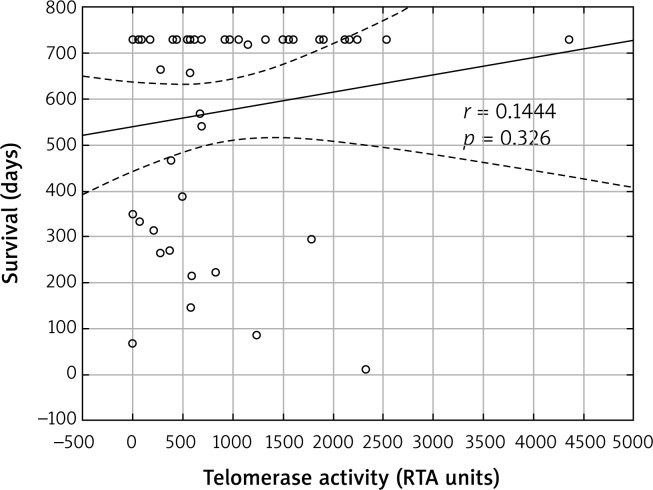
Overall, the two-year survival rate among the 47 patients treated with surgery was 59.6%. During the two-year observation period, 19 (40.4%) patients died as a result of disease progression. No statistically significant differences in the telomerase activity of the resected NSCLC samples were found between the deceased patients and the survivors (p = 0.178). In addition, no significant correlation was found between telomerase activity in the NSCLC tumors and the two-year survival rate (r = 0.1444, p = 0.326) (Fig. 2).
Fig. 2.
Correlation between telomerase activity in non-small cell lung cancer (NSCLC) tumor specimens and the two-year survival rate of the patients
Discussion
Several biological properties of lung cancers are analyzed from the standpoint of their usefulness for prognostication in lung cancer patients. In various cancers, telomerase activity was also described as an indicator of the tumor pathologic stage and poor patient prognosis. Although routine tests are already conducted in NSCLC patients, checking for various gene mutations in both neoplastic tissues and tissues deemed “healthy”, analysis of telomerase activity is still uncommon.
Our measurements of telomerase activity in pulmonary parenchyma were confirmed by the results obtained by Metzger [5] and Albanell [6], who found higher telomerase activity in neoplastic lung specimens than in parenchyma samples from lungs that were deemed healthy. Other studies have shown high telomerase activity and hTERT expression in 75.8-93% of tumors [7, 8]. In turn, Shibuya analyzed material collected by means of fine needle biopsy during fluorescence bronchoscopy. He compared telomerase activity and hTERT mRNA expression in normal bronchial epithelium, cases of squamous metaplasia and dysplasia, and squamous cell carcinoma of the lung. The lowest telomerase activity and hTERT expression was observed in normal bronchial epithelium, higher in cases of squamous metaplasia and dysplasia, and the highest in carcinomas [9]. In our study we obtained similar results.
In research conducted on lung tumor cell lines, high telomerase activity is observed in all histopathological types of the tumor. The level of telomerase activity in lung tumor cell lines is significantly higher than the level of telomerase activity observed in neoplastic tissues resected during lung parenchyma excision surgery [10]. This difference is most likely attributable to the fact that neoplastic tissue is not homogeneous, and its composition is not limited to cancer cells of one particular line. Neoplastic tissue often includes cancer-associated fibroblasts, lymphocyte infiltration, non-cancerous mesenchymal cells, hyperplastic pneumocytes, or necrotic foci [11]. Therefore, varying levels of telomerase activity in NSCLC tumor specimens may be attributed to different proportions of cancerous and non-cancerous cells. No telomerase activity was found in two tumor specimens that were analyzed in the present study. In both cases, the histopathological examination identified 90% tumor necrosis, which seems to confirm the foregoing observations. In his publication, Yashima also mentions absence of telomerase activity in the resected necrotic lesions of a squamous cell carcinoma and in a carcinoid tumor, with only small quantities of tumor cells identified [12]. On the other hand, it should be emphasized that telomerase activity was observed in bronchial epithelial cells obtained from bronchoalveolar lavage fluid (BALF) of lung cancer patients – even if no tumor was confirmed in those cells by histopathological examination. Xinarinios and Dikmen found high telomerase activity in 70% and 72.7%, respectively of BALF specimens [13, 14].
A number of authors did not find any telomerase activity in pulmonary parenchyma free from neoplastic lesions [6–8, 10, 15, 16]. Others, however, detected telomerase activity in the remaining part of pulmonary parenchyma that was considered free from tumor infiltration based on macroscopic examination. They believe that these “false positive” results can be attributed to activated leukocytes infiltrating the parenchyma or to cigarette smoke-mutated cells constituting an intermediate link of the neoplastic process [11, 13, 14, 17, 18]. In our research, high telomerase activity was found in 66.7% of pulmonary parenchyma samples that were deemed healthy based on macroscopic examination. We also found significantly higher levels of telomerase activity in the pulmonary parenchyma free from tumor infiltration when leukocyte infiltration was present. Therefore, the results confirm the suggestions by other authors in that regard [13, 14]. High telomerase activity was also determined by Pasrija in his study on bronchial epithelial cells found in the sputum of sarcoidosis patients [18]. By and large, researchers agree that there is a positive association between high telomerase activity and the presence of an active inflammatory process and significant leukocyte infiltration [13, 14].
Our research showed significantly higher levels of telomerase activity in poorly differentiated (high grade) NSCLC tumors (G3) as compared to moderately differentiated (intermediate grade) tumors (G2). Similar observations were also made by other authors [7, 15, 16, 19, 20]. On the other hand, Albanell did not confirm the existence of a positive association between telomerase activity and the level of differentiation (grade). However, he documented a strong correlation between telomerase activity and higher Ki-67 proliferation index [6]. Kumaki observed a positive association between telomerase activity and the level of differentiation (grade), but the results were not statistically significant [8].
In literature, telomerase activity is occasionally mentioned as a prognostic indicator in various types of malignant tumors. High hTERT expression and high telomerase activity is detected in 90% of invasive mammary carcinomas [21]. Tatsumoto also noted that high telomerase activity in colorectal cancer patients amounted to poorer prognosis [22]. However, the results of stomach cancer research are not that unambiguous [23]. The reports of the prognostic utility of high telomerase activity in NSCLC are also questionable. Targowski has proven that high telomerase activity in TBAC aspirate increases the risk of death seven-fold. Surgically treated patients without high telomerase activity had a 28% greater chance of surviving one year. In addition, in patients not qualified for surgical treatment, whose tumors did not exhibit high telomerase activity, survival was significantly longer than in patients whose tumors had high telomerase activity (p = 0.048). According to Targowski, high telomerase activity is a prognostic marker independent of the clinical staging of the disease as well as age and gender of both patients treated with surgery and patients that are not qualified for surgical treatment [1]. Moreover, Taga proved that the survival time of patients with telomerase-positive tumors was significantly lower than that of patients whose tumors were telomerase-negative. However, the difference was not statistically significant when a survival analysis was made in patient groups with stage IA and IB [16]. Opposite conclusions were reached by Marchetti who analyzed telomerase activity as a prognostic indicator in stage I NSCLC. He found a statistically significant association between the 5-year survival rate of the patients and detection of telomerase activity. The survival time of patients whose tumors were positive for telomerase activity was significantly shorter than that of patients in whom no telomerase activity was detected [15]. Telomerase activity is also described as an independent prognostic indicator in a study by Li. High telomerase activity in pleural lavage fluid samples indicates poorer prognosis and more frequent occurrence of pleural micro-metastasis [24].
In the course of our research, we found no significant association between the telomerase activity in the tumors and the survival time of NSCLC patients. On the other hand, it should be noted that the 2-year survival rate of patients with both low telomerase activity (i.e. less than 200 RTA units) and high telomerase activity in the tumor (i.e. more than 600 RTA units) was 70%, while as few as 30% of patients survived two years if their telomerase activity was between 200 and 600 RTA units. However, the differences in the survival time of the patients in particular groups were not statistically significant. Given the limited number of patients, the results presented should be approached with caution. Nevertheless, they form a starting point for further analyses in this area. Similar observations were made by other authors. Albanell analyzed 99 primary NSCLC tumor specimens. He found that the patients whose tumors were positive for telomerase activity did not live significantly longer than the patients in whom no telomerase activity was detected [6]. In their research, Chen and Wang also did not find telomerase activity in the tumor to have any prognostic impact [17, 25]. In his work devoted to the role of telomerase and hTERT in NSCLC, Metzger proved that an increased hTERT expression (but not telomerase activity) was positively associated with poor prognosis in patients treated with surgery [5]. These results are consistent with the results obtained by Hara [7].
Conclusions
Our study has identified a positive association between telomerase activity in NSCLC and the grade of differentiation. Moreover, a positive association was found between the presence of leukocyte infiltration in benign pulmonary parenchyma and high telomerase activity.
Disclosure
Authors report no conflict of interest.
References
- 1.Targowski T. Rozprawa na stopień doktora habilitowanego nauk medycznych. Warszawa: 2006. Przydatność kliniczna oznaczeń aktywności telomerazy w materiale z transtorakalnej aspiracyjnej biopsji cienkoigłowej u chorych na niedrobnokomórkowego raka płuca. [Google Scholar]
- 2.Shay JW, Wright WE. Senescence and immortalization: role of telomeres and telomerase. Carcinogenesis. 2005;26:867–874. doi: 10.1093/carcin/bgh296. [DOI] [PubMed] [Google Scholar]
- 3.Kowalska A, Kowalik A. Telomer i telomeraza w onkogenezie. Współcz Onkol. 2006;10:485–496. [Google Scholar]
- 4.Artandi SE, DePinho RA. Telomeres and telomerase in cancer. Carcinogenesis. 2010;31:9–18. doi: 10.1093/carcin/bgp268. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Marchetti A, Bertacca G, Buttitta F, Chella A, Quattrocolo G, Angeletti CA, Bevilacqua G. Telomerase activity as a prognostic indicator in stage I non-small cell lung cancer. Clin Cancer Res. 1999;5:2077–2081. [PubMed] [Google Scholar]
- 6.Albanell J, Lonardo F, Rusch V, Engelhardt M, Langenfeld J, Han W, Klimstra D, Venkatraman E, Moore MA, Dmitrovsky E. High telomerase activity in primary lung cancers: association with increased cell proliferation rates and advanced pathologic stage. J Natl Inst. 2003;89:1609–1615. doi: 10.1093/jnci/89.21.1609. [DOI] [PubMed] [Google Scholar]
- 7.Hara H, Yamashita K, Shinada J, Yoshimura H, Kameya T. Clinicopathologic significance of telomerase activity and hTERT mRNA expression in non-small cell lung cancer. Lung Cancer. 2001;34:219–226. doi: 10.1016/s0169-5002(01)00244-6. [DOI] [PubMed] [Google Scholar]
- 8.Kumaki F, Kawai T, Hiroi S, Shinomiya N, Ozeki Y, Ferrans VJ, Torikata C. Telomerase activity and expression of human telomerase RNA component and human telomerase reverse transcriptase in lung carcinomas. Hum Pathol. 2001;32:188–195. doi: 10.1053/hupa.2001.21567. [DOI] [PubMed] [Google Scholar]
- 9.Shibuya K, Fujisawa T, Hoshino H, Baba M, Saitoh Y, Iizasa T, Sekine Y, Suzuki M, Hiroshima K, Ohwada H. Increased telomerase activity and elevated hTERT mRNA expression during multistage carcinogenesis of squamous cell carcinoma of the lung. Cancer. 2001;92:849–855. doi: 10.1002/1097-0142(20010815)92:4<849::aid-cncr1392>3.0.co;2-4. [DOI] [PubMed] [Google Scholar]
- 10.Lee JC, Jong HS, Yoo CG, Han SK, Shim YS, Kim YW. Telomerase activity in lung cancer cell lines and tissues. Lung Cancer. 1998;21:99–103. doi: 10.1016/s0169-5002(98)00034-8. [DOI] [PubMed] [Google Scholar]
- 11.Liu Y, Wu BQ, Zhong HH, Xu ML, Fang WG. Detection of telomerase activity in cultured cells and tumor tissue of lung carcinoma by modified telomeric repeat amplification protocol. Pathol Int. 2010;60:386–394. doi: 10.1111/j.1440-1827.2010.02529.x. [DOI] [PubMed] [Google Scholar]
- 12.Yashima K, Litzky LA, Kaiser L, Rogers T, Lam S, Wistuba II, Milchgrub S, Srivastava S, Piatyszek MA, Shay JW, Gazdar AF. Telomerase expression in respiratory epithelium during the multistage pathogenesis of lung carcinomas. Cancer Res. 1997;57:2373–2377. [PubMed] [Google Scholar]
- 13.Dikmen E, Kara M, Dikmen G, Cakmak H, Dogan P. Detection of telomerase activity in bronchial lavage as an adjunct to cytological diagnosis in lung cancer. Eur J Cardiothorac Surg. 2003;23:194–199. doi: 10.1016/s1010-7940(02)00741-8. [DOI] [PubMed] [Google Scholar]
- 14.Xinarianos G, Scott FM, Liloglou T, Prime W, Turnbull L, Walshaw M, Field JK. Evaluation of telomerase activity in bronchial lavage as a potential diagnostic marker for malignant lung disease. Lung Cancer. 2000;28:37–42. doi: 10.1016/s0169-5002(99)00111-7. [DOI] [PubMed] [Google Scholar]
- 15.Marchetti A, Bertacca G, Buttitta F, Chella A, Quattrocolo G, Angeletti CA, Bevilacqua G. Telomerase activity as a prognostic indicator in stage I non-small cell lung cancer. Clin Cancer Res. 1999;5:2077–2081. [PubMed] [Google Scholar]
- 16.Taga S, Osaki T, Ohgami A, Imoto H, Yasumoto K. Prognostic impact of telomerase activity in non-small cell lung cancers. Ann Surg. 1999;230:715–720. doi: 10.1097/00000658-199911000-00015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Chen KY, Lee LN, Yu CJ, Lee YC, Kuo SH, Yang PC. Elevation of telomerase activity positively correlates to poor prognosis of patients with non-small cell lung cancer. Cancer Lett. 2006;240:148–156. doi: 10.1016/j.canlet.2005.09.005. [DOI] [PubMed] [Google Scholar]
- 18.Pasrija T, Srinivasan R, Behera D, Majumdar S. Telomerase activity in sputum and telomerase and its components in biopsies of advanced lung cancer. Eur J Cancer. 2007;43:1476–1482. doi: 10.1016/j.ejca.2007.04.003. [DOI] [PubMed] [Google Scholar]
- 19.Liu Y, Wu BQ, Zhong HH, Tian XX, Fang WG. Quantification of alternative splicing variants of human telomerase reverse transcriptase and correlations with telomerase activity in lung cancer. PLoS One. 2012;7:e38868. doi: 10.1371/journal.pone.0038868. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Hashim M, Sayed M, Samy N, Elshazly S. Prognostic significance of telomerase activity and some tumor markers in non-small cell lung cancer. Med Oncol. 2011;28:322–330. doi: 10.1007/s12032-010-9444-0. [DOI] [PubMed] [Google Scholar]
- 21.Chen CH, Chen RJ. Prevalence of telomerase activity in human cancer. J Formos Med Assoc. 2011;110:275–289. doi: 10.1016/S0929-6646(11)60043-0. [DOI] [PubMed] [Google Scholar]
- 22.Tatsumoto N, Hiyama E, Murakami Y, Imamura Y, Shay JW, Matsuura Y, Yokoyama T. High telomerase activity is an independent prognostic indicator of poor outcome in colorectal cancer. Clin Cancer Res. 2000;6:2696–2701. [PubMed] [Google Scholar]
- 23.He X, Qiao Q, Ge N, Ge, Nan J, Shen S, Wang Z, Yang Y, Bao G. Irradiation-induced telomerase activity and gastric cancer risk: a case-control analysis in a Chinese Han population. BMC Cancer. 2010;10:312. doi: 10.1186/1471-2407-10-312. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Li W, Ni Y, Tu Z, Wu S, Wu Z, Zheng S. Study of telomerase activity in pleural lavage fluid specimens in patients with non-small-cell lung cancer and its clinical significance. Eur J Cardiothorac Surg. 2009;36:460–464. doi: 10.1016/j.ejcts.2009.03.057. [DOI] [PubMed] [Google Scholar]
- 25.Wang J, Liu X, Jiang W, Liang L. Telomerase activity and expression of the telomerase catalytic subunit gene in NSCLC correlation with decreased apoptosis and clinical prognosis. Chin Med J (Engl) 2000;113:985–990. [PubMed] [Google Scholar]