Abstract
Individuals undertaking a weight loss effort have a choice among proven dietary approaches. Factors contributing to choice of either a low-fat/low-calorie diet or a low-carbohydrate diet, two of the most studied and popular dietary approaches, are unknown. The current study used data from participants randomized to the ‘choice’ arm of a trial examining whether being able to choose a diet regimen yields higher weight loss than being randomly assigned to a diet. At study entry, participants attended a group session during which they were provided tailored feedback indicating which diet was most consistent with their food preferences using the Geiselman Food Preference Questionnaire (FPQ), information about both diets, and example meals for each diet. One week later, they indicated which diet they chose to follow during the 48-week study, with the option of switching diets after 12 weeks. Of 105 choice arm participants, 44 (42%) chose the low-fat/low-calorie diet and 61 (58%) chose the low-carbohydrate diet. In bivariate analyses, diet choice was not associated with age, race, sex, education, BMI, or diabetes (all p > 0.05). Low-carbohydrate diet choice was associated with baseline higher percent fat intake (p = 0.007), lower percent carbohydrate intake (p = 0.02), and food preferences consistent with a low-carbohydrate diet according to FPQ (p < 0.0001). In a multivariable logistic regression model, only FPQ diet preference was associated with diet choice (p = 0.001). Reported reasons for diet choice were generally similar for those choosing either diet; however, concerns about negative health effects of the unselected diet was rated as more influential among participants selecting the low-fat diet. Only three low-carbohydrate and two low-fat diet participants switched diets at 12 weeks. Results suggest that when provided a choice between two popular weight loss dietary approaches, an individual's selection is likely influenced by baseline dietary intake pattern, and especially by his or her dietary preferences. Research is needed to determine if congruency between food preferences and dietary approach is associated with weight loss.
Keywords: Diet, Fat-restricted, Diet, Carbohydrate-restricted, Choice behavior
Low-fat/low-calorie diets prescribed as part of behavioral weight loss interventions have produced clinically significant weight loss in several large clinical trials (Knowler et al., 2002; The Look AHEAD Research Group, 2010). Accordingly, a low-fat/low-calorie diet has been the mainstay of guidelines from public health organizations for the past several decades (Marantz, Bird, & Alderman, 2008). More recent clinical trials of low-carbohydrate diets have supported the effectiveness of this dietary approach as well (Foster et al., 2003; Gardner et al., 2007; Samaha et al., 2003; Shai et al., 2008). Thus, multiple effective dietary approaches are available for weight loss, leading some experts to suggest that individuals beginning weight loss programs should be provided a choice between empirically supported dietary approaches, consistent with patient-centered care (Sacks et al., 2009; Shai et al., 2008).
Little is currently known about how individuals choose between different dietary approaches to weight loss. The existing literature on food choice may provide insights into how choice among diets is made. Early food choice research suggested that food selection is influenced by factors such as taste, health, social status, and cost (Lewin, 1943). Food choice is also thought to reflect the influence of social factors (e.g., opinions or habits of household members), food availability, and convenience (Furst, Connors, Bisogni, Sobal, & Falk, 1996; Sobal, Bisogni, & Jastran, 2014). However, the existing literature has not addressed selection of a dietary approach at the onset of a weight loss effort, which differs from making specific food choices in several important ways. When starting a weight loss effort, individuals are selecting a diet with the understanding that they will be striving to adhere to that diet for a prolonged period of time (versus making a food selection for only one meal). Diet selection that is intended to be for a prolonged period of time may evoke more careful, deliberate consideration and take into account more factors than one-time food selection, which may be subject to greater automaticity (Sobal et al., 2014). Additionally, when selecting a diet to follow, individuals are selecting with a particular goal (i.e., weight loss) as an identified priority. Thus, selection of a diet at the onset of a weight loss attempt differs considerably from individual food or meal choices, and may have different determinants.
In the context of selecting a dietary approach during a weight loss attempt, it has been suggested that individuals would select the diet that is most closely aligned or congruent with their food preferences (Borradaile et al., 2011), a prediction suggested by the broader literature on food choice (Furst et al., 1996; Lewin, 1943; Sobal et al., 2014). However, a dietary approach might be selected on the basis of being incongruent with food preferences, as a diet that restricts preferred foods could be viewed as beneficial to weight loss. Further, the congruency between food preferences and diet selection could differ depending on the foods preferred. Americans are generally familiar and accepting of the low-fat diet because of marketing attempts and public health messages. In contrast, many people have negative perceptions of the low-carbohydrate diet. For example, only one-third believe that a low-carbohydrate diet is a healthy way to lose weight (Rutten, Yaroch, Colón-Ramos, & Atienza, 2008). Thus, individuals may be less likely to select a diet that is congruent with their food preferences when their food preferences are consistent with a low-carbohydrate diet.
Diet selection at onset of a weight loss attempt may also be related to habitual food intake patterns. Individuals who tend to consume greater dietary fat, for example, may select a diet that is consistent with that pattern (i.e., a low-carbohydrate diet) out of habit. Another influential factor in diet selection may be presence of type 2 diabetes. Adults with diabetes often receive counseling to monitor their carbohydrate intake, which may make a low-carbohydrate diet appear more beneficial to them. Finally, dietary choice may also be associated with demographic factors given that sex, race, and age are related to dietary behaviors and preferences (Drewnowski, Kurth, Holden-Wiltse, & Saari, 1992; Monsivais, Rehm, & Drewnowski, 2013; Sijtsma et al., 2012; Wyant & Meiselman, 1984; Yang, Buys, Judd, Gower, & Locher, 2013).
Examining individuals’ self-reported reasons for diet selection could provide a better understanding of the process of diet selection. Factors that patients may report as influencing dietary choice include perceptions of diets’ costs, effects on appetite, acceptability in the social/household environment, effectiveness for weight loss or risk reduction, and safety. We are unaware of studies that have asked patients to rate the importance of these and other factors in selecting between low-fat and low-carbohydrate diets.
Thus, the purpose of the current study was to describe the choice process as well as the factors associations with and self-reported reasons for choice of either a low-fat/low-calorie diet or a low-carbohydrate diet at initiation of a behavioral weight loss program. These data are from a trial comparing participants randomized to either a no choice arm or a choice arm. If randomized to the no choice arm, participants were further randomized to either a low-fat/low-calorie or low-carbohydrate diet. If randomized to the choice arm, participants chose between a low-fat/low-calorie or a low-carbohydrate diet. Presented herein are the results of the diet choice process for participants in the diet choice arm. Analyses of the primary outcome of weight change are ongoing and will be presented separately.
Based upon the aforementioned literature, we hypothesized that selection of the low-carbohydrate diet would be associated with: (1) preference for foods consistent with low carbohydrate diet (i.e., high in fat or protein content and low in carbohydrate content), (2) habitual patterns of food intake consistent with a low-carbohydrate diet, (3) presence of type 2 diabetes, and (4) past experience with a low-carbohydrate diet. We also tested the hypothesis that participants with food preferences consistent with a low-fat diet would be more likely to select a diet congruent with their preferences than those with preferences consistent with a low-carbohydrate diet. Additionally, we explored associations between diet choice and demographics, BMI, and other health behaviors (e.g., tobacco use, physical activity) and reported on patients’ self-reported reasons for selecting their diet. The current study is the first to present the outcomes of choosing between a low-fat and low-carbohydrate diet during a weight loss attempt, to describe the correlates of that choice, and to provide descriptive data on patients’ perspectives on reasons for their diet selection.
Subjects and methods
Participants
Study participants were recruited from the Durham Veterans Affairs (VA) Medical Center between June 2011 and June 2012 through flyers, brochures, and advertisements. VA health care personnel were informed of the study and encouraged to refer patients to the study through the VA's electronic referral option. Additionally, a search of electronic health records for patients meeting study criteria was conducted, with potentially eligible patients contacted via a recruitment letter with a telephone number to contact if they were interested. Sample size was determined based on power analyses conducted for the parent trial.
Patients were eligible for the study if they had BMI ≥30 kg/m2, were in stable health, desired to lose weight, agreed to attend regular visits per study protocol, had access to a telephone and reliable transportation, and had a VA provider. Exclusion criteria included age over 75; pregnancy, breastfeeding or lacking birth control; certain chronic or unstable medical conditions (e.g. kidney or liver disease; daily insulin use; severely high blood pressure, cholesterol or hemoglobin A1c); dementia; psychiatric illness; substance abuse; or presence of a pacemaker or defibrillator. Other exclusion criteria were concurrent enrollment in a conflicting study, use of weight loss therapy in the previous month, or previous enrollment in a weight loss research study using the low-fat/low-calorie or low-carbohydrate diet. Eligibility was determined during screening telephone calls and at an in-person screening visit, during which participants also completed the Geiselman Food Preference Questionnaire (FPQ).
Procedures
Randomization
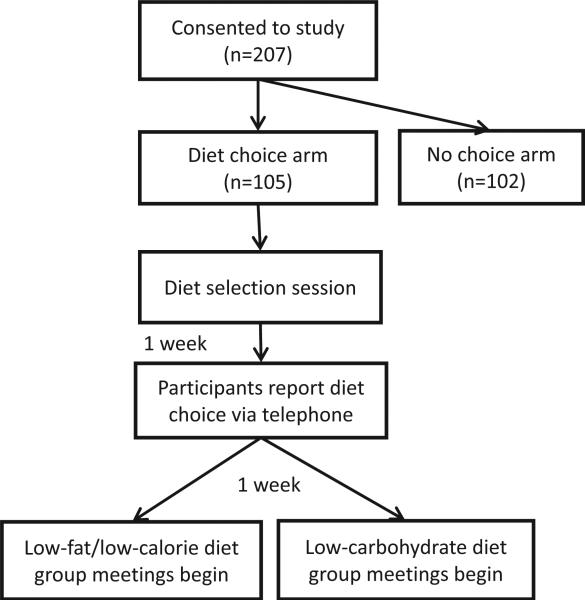
Details of the study procedures and intervention have been reported (Yancy et al., 2013). All study procedures were approved by the Durham VA Institutional Review Board and Research and Development Committee and all participants provided written informed consent. After the screening visit, participants were randomized to the no choice arm or the diet choice arm (Fig. 1). Following randomization, participants in the diet choice arm attended a group session focused on providing information to guide diet selection.
Fig. 1.
Study procedures.
Diet choice counseling
The diet choice counseling session was led by the study dietitian and study physician/principal investigator. At this session, participants were informed of their randomization assignment, provided with an overview of the study schedule, and guided through the diet choice process. The diet choice process consisted of several components. First, participants received FPQ results in print form indicating which diet was most consistent with their reported food preferences and how this result was generated from their FPQ responses. Both in print and verbally, participants were advised that it was their choice as to how to use this information for their diet selection – they could select the diet congruent with their FPQ results, select the diet incongruent with their results, or select without regard to their results. Next, a hand-out describing the two diets was provided and reviewed by the dietitian. The diet descriptions included specific information about the restrictions involved in each diet with regard to total calories and each macronutrient. An example meal for each diet was described in the handout and discussed. Participants were informed that both diets have been extensively researched and proven safe and effective. Factors other than food preference that might influence diet choice were mentioned as additional factors to consider (e.g., input from family/friends/medical providers). Participants were informed that they would be provided the option to switch diets 12 weeks into the intervention for any reason such as if dissatisfied with or intolerant of their initial diet. They were encouraged to ask questions during the counseling session, but were asked to refrain from stating opinions about the diets and from discussing diet choice with other group participants so as to avoid influencing one another. Instructions were given to review handouts provided and to think about their diet choice over the upcoming week. They were encouraged to consult with family, friends or health care providers if desired.
One week following the diet choice counseling session, participants were contacted via telephone by the study dietitian to answer questions and solicit diet choice. The dietitian then administered a questionnaire to assess reasons for their diet choice and scheduled their first group weight loss session for the following week.
Dietary intervention and option to switch diets
Group weight loss sessions were held every 2 weeks for the first 24 weeks of the study. Over the subsequent 24 weeks of the study, participants met monthly and had interposed individual monthly telephone calls from the dietitian focused on goal setting. Groups contained 12–15 choice arm participants on the same diet. All sessions were led by a registered dietitian with experience delivering both low-fat/low-calorie diets and low-carbohydrate diets.
The low-carbohydrate diet prescribed an initial carbohydrate intake of 20 g or less per day without calorie restriction. Carbohydrate intake could be increased gradually as participants’ weight loss goals were approached or if cravings threatened adherence. The low-fat/low-calorie diet prescribed total fat intake of less than 30% of daily intake, saturated fat intake of less than 10%, and cholesterol intake of less than 300 mg per day throughout the study. Low-fat/low-calorie participants were given a caloric goal of 500 kcals less than their estimated maintenance energy requirement. Caloric restriction could be further reduced or increased for individuals based on their progress towards their weight loss goals.
At week 12, ‘choice arm’ participants met individually with study personnel to report their progress and indicate whether they would like to switch to the other diet. Participants who chose to switch diets participated in an individual counseling session to obtain information on the new diet and thereafter attended a choice arm group session for that diet.
Measures
Background and clinical measurements
Participants self-reported age, sex, race, and highest education completed. Participants were asked if they had used any tobacco products in the past week (yes or no) and whether they had received a diagnosis of diabetes (yes or no). Body weight was measured at baseline by trained research assistants on a standardized digital scale (Tanita) with participants wearing light clothes and shoes removed.
Food preferences
The Geiselman Food Preference Questionnaire (FPQ) was used to obtain hedonic ratings of foods with specific macronutrient contents and to calculate macronutrient preferences (Geiselman et al., 1998). The FPQ was developed as a 2 (Fat: High Fat and Low Fat) × 3 (Other Macronutrient: High Complex Carbohydrate, High Simple Sugar, and High Protein) design, yielding the following six cells indicative of food type preference: high fat/high complex carbohydrate, high fat/high sugar, high fat/high protein, low-fat/high complex carbohydrate, low-fat/high sugar, and low-fat/high protein. Twelve foods are included in each of the six cells of the FPQ, for a total of 72 foods, which are listed in random order. The FPQ asks participants to rate how much they like each of the 72 foods on a 9-point Likert-type scale (1 = dislike extremely; 5 = neutral, neither like nor dislike; 9 = like extremely). Foods listed on the FPQ vary significantly and systematically in macronutrient content. Each food item in each of the three high-fat cells has ≥45% fat (expressed as percentage of the total kilocalories in a given food), and each food in each of the three low-fat cells has <20% fat. Other macronutrient criteria for the FPQ are: high complex carbohydrate (≥30% complex carbohydrate); high sugar (≥30% sugar); and high protein (≥13% protein, although most items were 20–35% protein). The foods rated are common sources of macronutrients in the typical U.S. diet and/or are among the favorite foods of specific populations, including obese men and obese women, and Whites and African-Americans (Drewnowski, 1997). Example foods include pudding, pot roast, French fries, ice cream, and various preparations of eggs. The FPQ has demonstrated test–retest reliability, with test–retest reliability of individual cells ranging from 0.83 to 0.96. Validity is supported by correlations with food intake measured in a laboratory setting and with self-reported dietary intake (Geiselman et al., 1998).
In this study, FPQ cell scores were used to categorize participants as having food preferences consistent with a low-fat diet or with a low-carbohydrate diet. Participants who scored highest in either the low-fat/high protein or high fat/high protein category were classified as having food preferences consistent with a low-carbohydrate diet, whereas participants who scored highest in low-fat/high sugar or low fat/high complex carbohydrate were classified as having food preferences consistent with a low-fat diet preference. Participants who scored highest in the high fat/high sugar or high fat/high complex carbohydrate cells were assigned according to their next highest cell score.
Habitual dietary intake
Habitual dietary intake was measured with the Block Brief 2000 Food Frequency Questionnaire (FFQ) (Hartman et al., 1996). Participants were provided images demonstrating food portion sizes and instructed to indicate which foods they had eaten in the previous 3 months and the corresponding portion. We examined the FFQ variables total calorie, percent fat, percent carbohydrate, and percent protein as these macronutrients are relevant to the two diets.
Physical activity
The long version International Physical Activity Questionnaire (IPAQ) was used to measure physical activity over the previous 7 days. The IPAQ has been validated against accelerometer and is associated with physical fitness (Craig et al., 2003; Fogelholm et al., 2006). Minutes per week of moderate intensity physical activity were examined.
Quality of life
Weight-related quality of life was measured with the Impact of Weight on Quality of Life (IWQOL) total scale score, which comprises physical function, self-esteem, sexual life, public distress, and work scores (Kolotkin, Crosby, Kosloski, & Williams, 2001a). This measure has correlated significantly with BMI and changes in BMI (Kolotkin, Crosby, Williams, Hartley, & Nicol, 2001b) and has good internal consistency (Kolotkin, Head, Hamilton, & Tse, 1995) and test–retest reliability (Kolotkin & Crosby, 2002).
Weight loss history
Weight loss history was determined by asking participants if they had ever attempted to lose weight in the past. If they answered affirmatively, they were then asked to endorse previously used weight loss approaches from a list developed for this study.
Reasons for diet selection
Participants were asked to rate on a 4-point scale (1 = not at all, 2 = only a little, 3 = some, 4 = very much) how influential 19 factors were in their diet choice. Participants were then asked to name which factor was most influential. Participants who switched diets at 12 weeks were asked to select the single most important factors influencing choice to switch diets from a provided list of 11 reasons. Participants had the option of selecting “other.” These lists were developed by the study investigators based on their clinical experience and the existing literature related to perceptions of different dietary approaches.
Statistical methods
Bivariate analyses were used to examine the association of demographics, health factors, clinical measures, nutrient intake, FPQ dietary preference, weight-related quality of life, and previous weight loss attempt with diet choice; independent samples t-tests were used for continuous factors (e.g. age) and chi-squared tests, or their corresponding exact tests for small sample sizes, for categorical factors (e.g. tobacco use). Among those who reported a previous weight loss attempt, chi-squared tests were conducted to examine associations with each type of past weight loss attempt and diet choice. We then estimated a multivariable model to predict diet choice using as predictors all variables that were significant in bivariate analyses (with the exception of previous weight loss approaches, as it was only conducted on the subset of participants who endorsed previous weight loss attempts). This model was estimated in order to determine if variables that were significantly related to choice in bivariate analyses were associated with choice independently of other factors. Age and sex were controlled for in these analyses, given their known associations with numerous weight and diet related variables. We compared participants choosing the low fat diet with those choosing the low carbohydrate diet on the Reasons for Diet Selection measure using Mantel–Haenszel chi-square tests for the ordinal ratings. A p-value of less than 0.05 was required to reject the null hypothesis. Analyses were conducted using SAS (version 9.2, SAS Institute Inc).
Results
Our study sample included 105 participants randomized to the diet choice arm (see Table 1 for sample characteristics). The low-fat/low-calorie diet was chosen by 44 participants (42%) and the low-carbohydrate diet by 61 participants (58%).
Table 1.
Characteristics of participants randomized to the choice arm of the parent randomized trial.
| Characteristic | N = 105 |
|---|---|
| Age (years), mean(SD) | 54 (11) |
| Women, no. (%) | 28 (27%) |
| Race, no. (%) | |
| White | 54 (51%) |
| African–American | 45 (43%) |
| Other/refused | 6 (6%) |
| Weight (kg), mean (SD) | 109 (21) |
| BMI(kg/m2), mean (SD) | 36.0 (6.4) |
| College degree, no. (%) | 34 (32%) |
| Tobacco use, no. (%) | 13 (12%) |
| Diabetes, no. (%) | 23 (22%) |
| Prior weight loss attempt, no. (%) | 86 (82%) |
In bivariate analyses, higher percentage of fat intake and lower percent of carbohydrate intake at baseline were associated with choosing the low-carbohydrate diet (Table 2). Based on their FPQ results, 77 participants had food preferences aligned with a low-carbohydrate diet, and 28 had preferences aligned with a low-fat diet. Of those with a low-carbohydrate food preference, 70% choose a diet congruent with their preference. Of those with a low-fat food preference, 75% choose a diet congruent with their preference. Thus, FPQ-derived dietary preferences were significantly associated with ultimate diet choice, and the likelihood of selecting a diet congruent with dietary preferences did not differ between those with low-carbohydrate food preferences and those with low-fat food preferences.
Table 2.
Bivariate analyses of baseline participant characteristics with diet choice outcome.
| Characteristic | Diet choice |
p Value | |
|---|---|---|---|
| Low-carbohydrate (n = 61) | Low-fat/low-calorie (n = 44) | ||
| Demographics | |||
| Age (years), mean (SD) | 55 (12) | 53 (11) | 0.37 |
| Sex, no. (%) | |||
| Women | 15 (54%) | 13 (46%) | 0.57 |
| Men | 46 (60%) | 31 (40%) | |
| Race, no. (%) | |||
| White | 30 (56%) | 24 (44%) | 0.42 |
| African-American | 29 (64%) | 16 (36%) | |
| Other/refused | 2 (33%) | 4 (67%) | |
| College degree, no. (%) | |||
| Yes | 19 (56%) | 15 (44%) | 0.75 |
| No | 42 (59%) | 29 (41%) | |
| Clinical characteristics | |||
| Tobacco use, no. (%) | |||
| Yes | 11 (85%) | 2 (15%) | 0.07 |
| No | 50 (54%) | 42 (46%) | |
| Diabetes, no. (%) | |||
| Yes | 17 (74%) | 6 (26%) | 0.08 |
| No | 44 (54%) | 38 (46%) | |
| Weight (kg) | 111 (18) | 106 (25) | 0.21 |
| BMI(kg/m2) | 36.4 (5.5) | 35.6 (7.4) | 0.53 |
| Nutrient intake, mean (SD) | |||
| Energy, kcal/d | 2010 (1156) | 1631 (736) | 0.06 |
| Carbohydrates, % | 41.6 (7.4) | 45.4 (8.6) | 0.02 |
| Total fat, % | 42.2 (5.9) | 38.7 (7.5) | 0.007 |
| Protein, % | 16.4 (2.6) | 16.5 (3.5) | 0.84 |
| IPAQ moderate-intensity physical activity (min/week), mean (SD)a | 465 (449) | 374 (416) | 0.30 |
| Prior weight loss attempts | |||
| Yes | 51 (59%) | 35 (41%) | 0.59 |
| No | 10 (53%) | 9 (47%) | |
| FPQ diet preference, no.o (%)b | |||
| Low-carbohydrate | 54 (70%) | 23 (30%) | <0.001 |
| Low-fat | 7 (25%) | 21 (75%) | |
| IWQOL-Lite total score, mean (SD)c | 71.7 (18.6) | 71.4 (21.0) | 0.95 |
3 participants had missing baseline on the IPAQ. IPAQ, International Physical Activity Questionnaire.
FPQ Food Preference Questionnaire.
IWQOL-Lite, Impact of Weight on Quality of Life-Lite questionnaire.
The multivariable logistic regression included age and sex and the following variables that were associated with diet choice in bivariate analyses: percent carbohydrate intake, percent fat intake, and FPQ-derived dietary preference. Of these, only FPQ-derived diet preference was significantly associated with dietary choice (Table 3); the odds of choosing the low-carbohydrate diet were 5.8 times higher for a low-carbohydrate preference per FPQ compared with a low-fat diet preference per FPQ.
Table 3.
Multivariable logistic regression of predictors and diet choice.a
| Variable | Odds Ratio (CI)b | p-value |
|---|---|---|
| Age (years) | 1.0 (1.0, 1.1) | 0.30 |
| Baseline carbohydrates, % | 1.0 (0.9, 1.1) | 0.97 |
| Baseline total fat, % | 1.1 (0.9, 1.2) | 0.39 |
| Sex | ||
| Women | 1.1 (0.4, 3.0) | 0.90 |
| Men | Reference | |
| FPQ diet preference | ||
| Low-carbohydrate | 5.8 (2.0, 16.9) | 0.001 |
| Low-fat | Reference |
1 = low-carbohydrate, 0 = low-fat/low-calorie; n = 105.
Comparing odds of choosing low-carbohydrate diet.
Among participants with a previous weight loss attempt, diet choice was associated with past use of a low-fat/high-carbohydrate diet: 35% of participants with past use of a low-fat/high-carbohydrate diet chose the low-carbohydrate diet in the current study, compared with 65% without past use of this diet (Table 4).
Table 4.
Bivariate analyses of methods of prior weight loss attempts by diet choice (n = 86).a
| Method | Diet choice |
p-Value | |
|---|---|---|---|
| Low-carbohydrate (n = 51) | Low-fat/low-calorie (n = 35) | ||
| Commercial/organized weight loss program (e.g., Weight Watchers, etc.) | |||
| Yes | 10 (59%) | 7 (41%) | 0.96 |
| No | 41 (59%) | 28 (41%) | |
| Prescription diet pills | |||
| Yes | 4 (50%) | 4 (50%) | 0.71 |
| No | 47 (60%) | 31 (40%) | |
| Non-prescription (over the counter) diet pills | |||
| Yes | 8 (47%) | 9 (53%) | 0.25 |
| No | 43 (62%) | 26 (38%) | |
| Exercise | |||
| Yes | 40 (59%) | 28 (41%) | 0.86 |
| No | 11 (61%) | 7 (39%) | |
| Calorie-restricted diet | |||
| Yes | 23 (53%) | 20 (47%) | 0.27 |
| No | 28 (65%) | 15 (35%) | |
| High protein/low-carbohydrate (for example, Atkins, South Beach, Zone) | |||
| Yes | 13 (65%) | 7 (35%) | 0.55 |
| No | 38 (58%) | 28 (42%) | |
| Low-fat/high carbohydrate diet | |||
| Yes | 6 (35%) | 11 (65%) | 0.02 |
| No | 45 (65%) | 24 (35%) | |
| Other do-it-yourself diet plan (for example, Slim fast) | |||
| Yes | 19 (63%) | 11 (37%) | 0.58 |
| No | 32 (57%) | 24 (43%) | |
Only participants who endorsed a previous weight loss attempt were included in analyses.
Participants’ self-reported ratings of factors influencing their diet choice are shown in Table 5. Factors rated particularly high in importance were food preferences and perceptions of the diet's positive effects on weight and health. Reasons rated lower in importance for dietary choice were food costs, food intolerances, and perceptions that the diet would harm health. Generally, ratings differed little between those selecting the low-carbohydrate diet and those selecting the low-fat diet. However, participants who selected the low-fat diet endorsed concern about the unselected diet harming their health as more influential in their diet choice than participants who selected the low-carbohydrate diet. When asked which reason was most influential, the most frequently endorsed reason was “food preferences prior to completing the FPQ” among participants who selected the low-fat/low-calorie diet (26%) and the low-carbohydrate diet (22%).
Table 5.
Mean (SD) ratings and percentage endorsing factors influencing initial diet choice (n = 101).a
| Low carbohydrate (n = 58) |
Low fat (n = 43) |
p-Valuec | |||
|---|---|---|---|---|---|
| Average rating | Endorsed (%)b | Average rating | Endorsed (%)b | ||
| Anticipated effects on health and weight | |||||
| How much the diet would improve your health. | 3.3 (1.0) | 79% | 3.5 (0.9) | 91% | 0.28 |
| How much the other diet would harm your health. | 1.2 (0.5) | 2% | 1.8 (1.2) | 24% | 0.004 |
| How well the diet would help you lose weight. | 3.6 (0.7) | 91% | 3.6 (0.5) | 98% | 0.85 |
| How well the diet has worked for you in the past. | 1.9 (1.2) | 34% | 2.3 (1.4) | 46% | 0.20 |
| Food preferences and diet knowledge | |||||
| Your food preferences before completing the Food Preference Questionnaire. | 3.2 (1.0) | 79% | 3.2 (0.9) | 81% | 0.77 |
| Your food preferences as shown by the Food Preference Questionnaire. | 3.0 (1.0) | 74% | 2.9 (1.0) | 71% | 0.52 |
| Descriptions of the two diets provided at the first group visit. | 3.2 (0.9) | 81% | 2.9 (1.1) | 71% | 0.24 |
| How well you understand the diet instructions. | 2.8 (1.1) | 68% | 3.0 (1.1) | 74% | 0.37 |
| Social factors | |||||
| Discussions with your spouse/significant other | 2.4 (1.3) | 53% | 2.6 (1.3) | 54% | 0.54 |
| Discussions with other family members, friends, or co-workers | 2.0 (1.2) | 36% | 1.6 (1.0) | 22% | 0.15 |
| Discussions with a health care worker (doctor, nurse, dentist, therapist, etc). | 2.0 (1.2) | 33% | 2.1 (1.3) | 40% | 0.57 |
| Consideration of who shops or cooks in your home. | 2.6 (1.2) | 58% | 2.5 (1.3) | 52% | 0.67 |
| Consideration of others who eat in your home. | 2.4 (1.3) | 52% | 2.2 (1.3) | 45% | 0.31 |
| Anticipated effects on appetite and adherence | |||||
| How full you would feel on the diet you chose. | 2.7 (1.2) | 58% | 2.8 (1.1) | 63% | 0.62 |
| How hungry you would be on the other diet. | 2.1 (1.1) | 35% | 2.2 (1.1) | 34% | 0.77 |
| How hard it would be to follow the other diet. | 2.3 (1.1) | 44% | 2.7 (1.2) | 53% | 0.15 |
| Other factors | |||||
| Food allergies or intolerances. | 1.3 (0.7) | 7% | 1.3 (0.7) | 11% | 0.83 |
| Cost of the food. | 1.8 (1.1) | 21% | 2.0 (1.1) | 31% | 0.45 |
Items were rated on a scale of 1 to 4 scale (1 = not at all, 2 = only a little, 3 = some, 4 = very much).
Endorsed (%) is the percentage of subjects who rated the item as a 3 or 4. Measures were not completed by 3 low-carbohydrate diet participants and 1 low-fat diet participant. Additionally, 10 items had missing responses in the low-carbohydrate diet group and 13 in the low-fat diet group (ranging from 1 to 8 participants missing per item).
p-values are for Mantel-Haenszel chi-square comparison of ratings between participants selecting low carbohydrate and low fat diet.
When provided the option to switch diets at 12 weeks, three participants who had originally chosen the low-carbohydrate diet and two who had originally chosen the low-fat diet (4.8% of total) decided to switch. Among the participants who switched from the low-carbohydrate diet, reasons selected as most influential were the desire to eat other foods (n = 1), “family/friends” (n = 1), and “other” (n = 1). Among those switching from the low-fat diet, the reasons selected were not losing sufficient weight (n = 1) and “other” (n = 1).
Discussion
This manuscript describes the results of providing participants a choice between a low-fat/low-calorie or low-carbohydrate diet upon initiation of a behavioral weight loss program. Increasingly, there is recognition that several dietary approaches to weight loss are safe and effective, and that individuals have a choice among these various dietary approaches. This is the first study to report on the frequency of choosing either a low-fat diet or low-carbohydrate diet, associations of diet selection, and participants’ perspective on reasons for selecting diet in the context of a weight loss attempt.
In the current study, the low-carbohydrate diet was selected with a slightly greater frequency (58%) than the low-fat diet (42%). We are aware of only two previous studies that have provided participants the choice between distinct diet options at the onset of a weight loss intervention (Burke et al., 2007). Burke and colleagues offered participants the choice between a low-fat diet and a lacto-ovo-vegetarian diet. In that study, 58% selected the low-fat diet and 42% selected the lacto-ovo-vegetarian diet. In another study, participants were given the choice of South Beach diet, Mediterranean diet, and a diet developed by the study center that was high protein, moderate carbohydrate, and low fat (Coles, Fletcher, Galbraith, & Clifton, 2014). The study center-developed diet was selected by 48% of participants, the Mediterranean diet by 37%, and the South Beach diet by 16%. Thus, in that study, the lowest carbohydrate diet (i.e., South Beach) was least commonly selected, which is inconsistent with our results. Another study asked individuals to rate their preference for a low-fat or low-carbohydrate diet prior to beginning a weight loss trial, although their stated preference had no bearing on their diet assignment, which was decided randomly (Borradaile et al., 2011). In that study, preference for a low-carbohydrate diet was reported by 58% of participants, which is consistent with our study results. Taken together, these results suggest that when participating in programs that prescribe only one diet, many individuals may be initiating a diet that is inconsistent with their preferences. Behavioral weight loss programs may appeal to a wider variety of individuals if they offer options for following empirically supported diet options, including the option to use diets that are not usually offered (i.e., diets other than low-fat diets).
It has been suggested that providing dietary choice may increase weight loss because participants will choose diets that align with their food preferences, which may result in greater adherence to the diet (Sacks et al., 2009; Samaha et al., 2003). The current study supports the first part of the assertion; that is, most participants chose a diet approach that was consistent with their food preferences as measured by a valid and reliable macronutrient preference questionnaire. Furthermore, when participants were asked to rank which factor most influenced their diet choice, food preferences was the most commonly cited factor. However, a substantial minority of individuals did not select a diet that is consistent with their preferences, at least according to the FPQ. The dietary choice feedback and counseling session that participants attended prior to choosing their diet discussed food preferences as a potential guiding factor for dietary selection, yet emphasized that they may wish to choose opposite their preference, or may choose without regard to their dietary preferences. It is currently unclear if individuals are more adherent to diets that are consistent with their food preferences; however, the observed tendency to select a diet congruent with food preferences underscores the importance of determining if weight loss is greater when there is congruency between food preferences and diet type. The study by Borradaile et al. (2011) found that receiving a preferred diet was associated with less weight loss than receiving a less preferred diet. Notably, however, participants in that study rated which diet approach they would prefer, not which foods they prefer. The results of the parent trial of the current study will provide important data on the influence of dietary choice and food preferences on weight loss.
We did not find support for our hypothesis that individuals would be more likely to select a diet incongruent with their food preference if they had a preference for low-carbohydrate foods. This may suggest that efforts to educate patients on both diet types were successful in dispelling misperceptions about, and increasing familiarity with, the low-carbohydrate diet. On the other hand, participants who selected the low-fat diet were more likely to cite concerns about the unselected diet harming their health as a reason for diet selection.
Demographic, clinical factors, and health behaviors were not generally associated with diet choice. This is consistent with the previously described study by Borradaile and colleagues in which no association was found between diet preference and sex, race, age, or BMI (Borradaile et al., 2011). In a study of a nationally representative sample, past use of a low-carbohydrate diet was associated with female sex, a college education, income higher than $50,000, and age range 50–64 (Rutten et al., 2008). However, that study included both participants who had and had not dieted. Therefore, it is unclear if the observed relationships were a result of these characteristics being associated with weight loss attempts more generally or low-carbohydrate diets specifically. Although demographics and clinical characteristics were not associated with diet choice in the current study, previous use of a low-fat diet was associated with choice of a low-fat diet, suggesting that familiarity with a weight loss diet may influence choice.
Participants’ self-reported reasons for choosing a diet can inform future efforts to guide selection among diets. Currently, it is unclear on what basis to guide individuals to select between diets because empirical studies have not identified characteristics that distinguish among individuals who are more successful on one diet than another. Once data to guide diet selection are available, efforts to guide patients based on this information should take into consideration those factors that patients report are important when selecting between diets, as described in this study. For example, most participants in our study rated “how well you understand the diet instructions,” as influential to their choice, indicating the need to carefully explain the diet to participants. Less important was the cost of foods, which may be relevant for a smaller subset of people.
An important feature of the informed choice process was allowing participants the option to switch diets at 12 weeks. Few participants opted to switch, suggesting that most participants were satisfied with their diet at that point in the intervention. However, participants may not have switched diets due to a desire to remain in their weight loss group, as they would have had to switch to a different group. In prior behavioral weight loss trials, people tend to continue experiencing weight loss at 12 weeks, with a plateau occurring between 16 and 24 weeks. Future studies may wish to examine the impact of choice when offered at a later or earlier time point than 12 weeks, or offering the option to switch diet at any time.
This study had several limitations. Participants were VA patients; generalization to other populations is uncertain. The greater proportion of participants selecting the low-carbohydrate diet may reflect that this diet option is not available in the weight loss program offered by the VA where participants were recruited. The diet choice counseling used in the current study attempted to present both diets accurately and in a positive light, but the relationships observed may not generalize to dietary choice using different diet choice counseling strategies.
The diet choice process was designed to mimic how this may occur in clinical practice and was based on principles of collaborative, informed-decision making. The diet choice process was conducted in a group format, which is consistent with how behavioral weight loss treatment is often delivered. The findings should provide guidance as weight management programs begin offering participants a choice between different dietary approaches. Allocation of resources for each diet can be guided by our findings that participants have similar likelihood of selecting a low-fat and low-carbohydrate diet, and that few participants’ switched diets. Further, the information provided to participants and the procedure used for helping participants to choose a diet can serve as a guide for clinicians who are offering these diet options in their clinics.
Conclusions
In conclusion, this was the first study to report the factors associated with choice between a low-fat/low-calorie and low-carbohydrate diet at the onset of a weight loss intervention. Weight loss programs (and their participants) may benefit from offering participants several empirically supported diet options and from considering patients’ reasons for diet selection when planning efforts to guide diet choice. Additional research on the effects of weight loss on congruency between food preferences and diet approach are warranted.
Footnotes
Acknowledgements: Funding for the trial was provided by the U.S. Department of Veterans Affairs (IIR 09-381). Funding for Megan McVay, Ph.D, was provided by fellowship grant T32 HS00079 from the Agency for Healthcare Research and Quality. The funder had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; nor preparation, review, or approval of the manuscript. The views expressed in this article are those of the authors and do not necessarily reflect the position or policy of the Department of Veterans Affairs, Duke University, Pennington Biomedical Research Center, Louisiana State University, or Virginia Commonwealth University. Paula Geiselman, Ph.D, has a financial relationship with the Geiselman Food Preference Questionnaire (FPQ), as she receives royalties from Pennington Biomedical Research Center for use of the FPQ. None of the other authors had any conflicts of interest to disclose. Sources of Support: This research was supported by VA HSR&D (IIR 09-381).
Clinical Trial Registry: NCT01152359.
References
- Borradaile KE, Halpern SD, Wyatt HR, Klein S, Hill JO, Bailer B, et al. Relationship between treatment preference and weight loss in the context of a randomized controlled trial. Obesity. 2011;20:1218–1222. doi: 10.1038/oby.2011.216. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Burke L, Warziski M, Styn M, Music E, Hudson A, Sereika S. A randomized clinical trial of a standard versus vegetarian diet for weight loss. The impact of treatment preference. International Journal of Obesity. 2007;32:166–176. doi: 10.1038/sj.ijo.0803706. [DOI] [PubMed] [Google Scholar]
- Coles LT, Fletcher EA, Galbraith CE, Clifton PM. Patient freedom to choose a weight loss diet in the treatment of overweight and obesity. A randomized dietary intervention in type 2 diabetes and pre-diabetes. The International Journal of Behavioral Nutrition and Physical Activity. 2014;11:64. doi: 10.1186/1479-5868-11-64. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Craig CL, Marshall AL, Sjöström M, Bauman AE, Booth ML, Ainsworth BE, et al. International physical activity questionnaire: 12-country reliability and validity. Medicine and Science in Sports and Exercise. 2003;35:1381–1395. doi: 10.1249/01.MSS.0000078924.61453.FB. [DOI] [PubMed] [Google Scholar]
- Drewnowski A. Taste preferences and food intake. Annual Review of Nutrition. 1997;17:237–253. doi: 10.1146/annurev.nutr.17.1.237. [DOI] [PubMed] [Google Scholar]
- Drewnowski A, Kurth C, Holden-Wiltse J, Saari J. Food preferences in human obesity. Carbohydrates versus fats. Appetite. 1992;18:207–221. doi: 10.1016/0195-6663(92)90198-f. [DOI] [PubMed] [Google Scholar]
- Fogelholm M, Malmberg J, Suni J, Santtila M, Kyröläinen H, Mäntysaari M, et al. International physical activity questionnaire. Validity against fitness. Medicine and Science in Sports and Exercise. 2006;38:753–760. doi: 10.1249/01.mss.0000194075.16960.20. [DOI] [PubMed] [Google Scholar]
- Foster GD, Wyatt HR, Hill JO, McGuckin BG, Brill C, Mohammed BS, et al. A randomized trial of a low-carbohydrate diet for obesity. The New England Journal of Medicine. 2003;348:2082–2090. doi: 10.1056/NEJMoa022207. [DOI] [PubMed] [Google Scholar]
- Furst T, Connors M, Bisogni CA, Sobal J, Falk LW. Food choice. A conceptual model of the process. Appetite. 1996;26:247–265. doi: 10.1006/appe.1996.0019. [DOI] [PubMed] [Google Scholar]
- Gardner CD, Kiazand A, Alhassan S, Kim S, Stafford RS, Balise RR, et al. Comparison of the Atkins, Zone, Ornish, and LEARN diets for change in weight and related risk factors among overweight premenopausal women. JAMA: The Journal of the American Medical Association. 2007;297:969–977. doi: 10.1001/jama.297.9.969. [DOI] [PubMed] [Google Scholar]
- Geiselman P, Anderson A, Dowdy M, West D, Redmann S, Smith S. Reliability and validity of a macronutrient self-selection paradigm and a food preference questionnaire. Physiology and Behavior. 1998;63:919–928. doi: 10.1016/s0031-9384(97)00542-8. [DOI] [PubMed] [Google Scholar]
- Hartman AM, Block G, Chan W, Williams J, McAdams M, Banks WL, Jr., et al. Reproducibility of a self-administered diet history questionnaire administered three times over three different seasons. Nutrition and Cancer. 1996;25:305–315. doi: 10.1080/01635589609514454. [DOI] [PubMed] [Google Scholar]
- Knowler WC, Barrett-Connor E, Fowler SE, Hamman RF, Lachin JM, Walker EA, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. The New England Journal of Medicine. 2002;346:393–403. doi: 10.1056/NEJMoa012512. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kolotkin RL, Crosby RD. Psychometric evaluation of the impact of weight on quality of life-lite questionnaire (IWQOL-lite) in a community sample. Quality of Life Research: An International Journal of Quality of Life Aspects of Treatment, Care and Rehabilitation. 2002;11:157–171. doi: 10.1023/a:1015081805439. [DOI] [PubMed] [Google Scholar]
- Kolotkin RL, Crosby RD, Kosloski KD, Williams GR. Development of a brief measure to assess quality of life in obesity. Obesity Research. 2001a;9:102–111. doi: 10.1038/oby.2001.13. [DOI] [PubMed] [Google Scholar]
- Kolotkin RL, Crosby RD, Williams GR, Hartley GG, Nicol S. The relationship between health-related quality of life and weight loss. Obesity Research. 2001b;9:564–571. doi: 10.1038/oby.2001.73. [DOI] [PubMed] [Google Scholar]
- Kolotkin RL, Head S, Hamilton M, Tse CKJ. Assessing impact of weight on quality of life. Obesity Research. 1995;3:49–56. doi: 10.1002/j.1550-8528.1995.tb00120.x. [DOI] [PubMed] [Google Scholar]
- Lewin K. Forces behind food habits and methods of change. In The problem of changing food habits. National Academy of Sciences; Washington, DC: 1943. Bulletin 108. [Google Scholar]
- Marantz PR, Bird ED, Alderman MH. A call for higher standards of evidence for dietary guidelines. American Journal of Preventive Medicine. 2008;34:234–240. doi: 10.1016/j.amepre.2007.11.017. [DOI] [PubMed] [Google Scholar]
- Monsivais P, Rehm CD, Drewnowski A. The DASH diet and diet costs among ethnic and racial groups in the United States. JAMA Internal Medicine. 2013;173:1922–1924. doi: 10.1001/jamainternmed.2013.9479. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rutten LJF, Yaroch AL, Colón-Ramos U, Atienza AA. Awareness, use, and perceptions of low-carbohydrate diets. Preventing Chronic Disease. 2008;5:A130. [PMC free article] [PubMed] [Google Scholar]
- Sacks FM, Bray GA, Carey VJ, Smith SR, Ryan DH, Anton SD, et al. Comparison of weight-loss diets with different compositions of fat, protein, and carbohydrates. The New England Journal of Medicine. 2009;360:859–873. doi: 10.1056/NEJMoa0804748. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Samaha FF, Iqbal N, Seshadri P, Chicano KL, Daily DA, McGrory J, et al. A low-carbohydrate as compared with a low-fat diet in severe obesity. The New England Journal of Medicine. 2003;348:2074–2081. doi: 10.1056/NEJMoa022637. [DOI] [PubMed] [Google Scholar]
- Shai I, Schwarzfuchs D, Henkin Y, Shahar DR, Witkow S, Greenberg I, et al. Weight loss with a low-carbohydrate, Mediterranean, or low-fat diet. The New England Journal of Medicine. 2008;359:229–241. doi: 10.1056/NEJMoa0708681. [DOI] [PubMed] [Google Scholar]
- Sijtsma FP, Meyer KA, Steffen LM, Shikany JM, Van Horn L, Harnack L, et al. Longitudinal trends in diet and effects of sex, race, and education on dietary quality score change. The Coronary Artery Risk Development in Young Adults study. The American Journal of Clinical Nutrition. 2012;95:580–586. doi: 10.3945/ajcn.111.020719. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sobal J, Bisogni CA, Jastran M. Food choice is multifaceted, contextual, dynamic, multilevel, integrated, and diverse. Mind, Brain, and Education. 2014;8:6–12. [Google Scholar]
- The Look AHEAD Research Group Long-term effects of a lifestyle intervention on weight and cardiovascular risk factors in individuals with type 2 diabetes mellitus. Four-year results of the look AHEAD trial. Archives of Internal Medicine. 2010;170:1566–1575. doi: 10.1001/archinternmed.2010.334. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wyant K, Meiselman H. Sex and race differences in food preferences of military personnel. Journal of the American Dietetic Association. 1984;84:169–175. [PubMed] [Google Scholar]
- Yancy WS, Jr., Coffman CJ, Geiselman PJ, Kolotkin RL, Almirall D, Oddone EZ, et al. Considering patient diet preference to optimize weight loss. Design considerations of a randomized trial investigating the impact of choice. Contemporary Clinical Trials. 2013;35:106–116. doi: 10.1016/j.cct.2013.03.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Yang Y, Buys DR, Judd SE, Gower BA, Locher JL. Favorite foods of older adults living in the black belt region of the United States. Influences of ethnicity, gender, and education. Appetite. 2013;63:18–23. doi: 10.1016/j.appet.2012.12.007. [DOI] [PMC free article] [PubMed] [Google Scholar]