Highlights
-
•
Angiosarcomas are rare malignant vascular tumors of the breast.
-
•
They frequently are associated with previous breast radiotherapy.
-
•
Total mastectomy without axillary lymphadenectomy appears to be the only treatment.
-
•
Chemotherapy and radiotherapy have not proven any benefit in terms of survival.
Keywords: Primary angiosarcoma, Breast cancer, Young woman, Mastectomy, Diffusion-weighted magnetic resonance imaging (MR-DWI), Radiotherapy
Abstract
Introduction
Angiosarcomas of the breast are a rare subtype of sarcomas that frequently are diagnosed after radiation therapy for primary breast cancer. Primary angiosarcomas are rare entities accounting 0.05% of all malignant breast neoplasm.
Presentation of Case
We report a case of primary angiosarcoma of the breast in a 25 years woman, with no previous radiotherapy, treated with a total mastectomy followed by radio-chemotherapy.
Discussion
Total mastectomy appears to be the only treatment known that has proven to benefit these patients. Adjuvant treatment has not proven value up until today. The 5-year disease free survival for grade 1 tumors can be as high as 76%, and up to 15% for grade 3.
Conclusion
Due to the rarity of these tumors there is no standard therapies approach.
1. Introduction
Primary breast angiosarcomas are rare malignant vascular neoplasias that originate from the breast parenchyma and occasionally affect the skin. Globally, angiosarcoma represents less than 0.05% of all breast cancers [1].
Breast angiosarcomas usually affect women in the thirties or forties. Clinically they appear as a painless, irregular breast mass [2] that occasionally grow fast [3].
Secondary malignancy usually occurs in elderly women with a history of radiotherapy for breast cancer with an incidence rate from 0.04% to 0.15% [4].
The best treatment for breast angiosarcomas is a simple mastectomy. Axillary lymphadenectomy is not needed, due to the fact that angiosarcomas tend to metastasize by vascular spread [1].
2. Case report
A 25 year-old Caucasian woman presents a bulky breast mass involving entire right breast. The patient referred having a 2 cm sized lump two years earlier in a right breast. Several breasts ultrasound were informed as benign findings. In the last 6 months she felt a quick growth of the mass, but did not consult any doctor until it reached 14 cm in its size. She had no history of breast trauma and no breast cancer in her family.
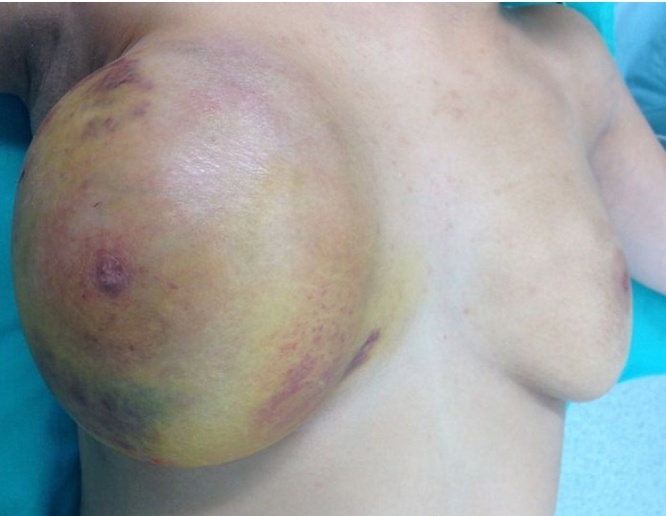
On physical exam we found a bulky and irregular breast mass of approximately 14 cm causing important breast asymmetry (Fig. 1), and skin devitalization secondary to the distension reaching the inframammary groove. No suspicious lymphadenopathies were palpated at the diagnosis.
Fig. 1.
Right breast’s mass that causes great asymmetry with ulceration and trophic skin changes.
The diffusion-weighted magnetic resonance imaging (MR-DWI) revealed a 14 × 13 × 10.5 cm mass with solid and hypervascularized components with significant enhancement, type 3-curve and high apparent diffusion coefficient (ADC) (1,85–3,17 × 10–3 mm2/s). Areas with intratumoral bleeding were also identified.
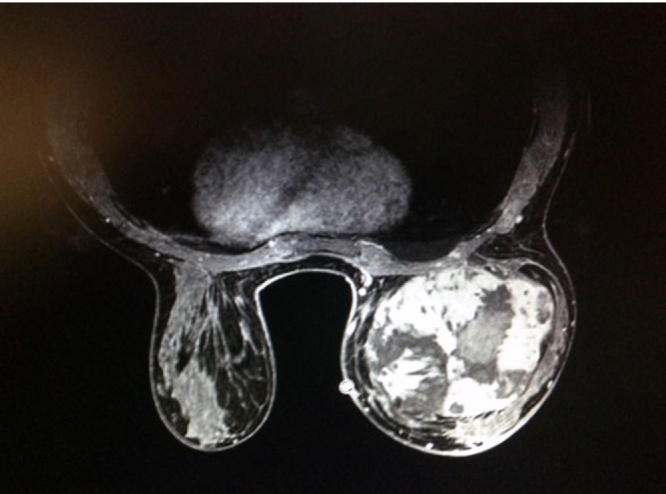
The right breast was completely occupied by the tumor, leaving a small amount of residual breast tissue surrounded by a pseudocapsule caused by tumor effect (Fig. 2). A diagnostic core needle biopsy was performed. The final histology was read as a grade 1 angiosarcoma of the breast. Metastatic work-up was negative by PET-Scan.
Fig. 2.
Mass with intratumoral bleeding areas and solid areas with significant enhancement hypervascular with type 3 curve and apparent diffusion coefficient (ADC) tall (1.85–3.17 × 10–3 mm2/s), with a compression of pseudocapsule breast tissue residual.
A nipple sparing simple mastectomy was needed to remove the tumor. Nipple-areola skin biopsies were sent during the procedure for intraoperative pathological study to rule out skin infiltration. The final pathology report confirmed the diagnosis of breast angiosarcoma grade 1 with free surgical margins and no skin infiltration. Breast reconstruction was performed during the procedure, placing a retropectoral expander, which was replaced by a definitive implant after completed radiotherapy. The patient opted for oocyte cryopreservation prior chemotherapy. The case was discussed in the multidisciplinary Tumor Committee deciding subsequent adjuvant treatment with 4 cycles of chemotherapy with ifosfamide-Adriamycin, followed by 12 weeks of weekly taxol, and breast radiotherapy.
The patient is asymptomatic and free of disease 13 months after the diagnosis.
3. Discussion
Primary breast angiosarcoma is a rare tumor usually affecting women in their early forties. The majority of these tumors are diagnosed with a history of breast radiotherapy [5]. However they also appear without previous risky factors like the one described in this case.
The 5-year overall survival for grade 1 breast angiosarcomas is approximately 75% and 15% for grade 3 tumors [6].
Approximately 2% of the patients with breast angiosarcoma may present with diffuse increase breast volume and skin changes (bluish red coloration). To the date nearly all case reports, present no correlation between the size of the tumor and the survival rate [7].
Angiosarcoma is often initially misdiagnosed and preoperative diagnosis by biopsy can be difficult. The fine needle aspiration is controversial given the extensive vascularity of the tumor [6]. Large-core biopsies might facilitate the correct diagnosis as they provide a larger sample, but such a macro biopsy is often difficult to perform due to the vascular nature of these tumors.
MRI is the best imaging test for characterizing breast angiosarcomas, due to the fact that it allows a better assessment of the regional distribution and visualizes the vascular nature of the lesion, helping in the diagnosis. In our case we used diffusion MRI, allowing a better lesion characterization and more accurate assessment of local involvement, including skin and pectoral muscle invasion.
Primary angiosarcomas present on MR imaging as a heterogeneous masses with low signal intensity on T1W images and high signal on T2W images. High-grade tumors may demonstrate rapid enhancement with washout kinetics, but lower grade tumors usually demonstrate plateau or persistent enhancement kinetics. High-grade tumors can also demonstrate focal areas of high signal on T1-weighting images, reflecting hemorrhage or vascular lakes [8].
The best treatment of breast angiosarcoma is surgery, performing a free margin simple mastectomy as soon as possible.
We performed a sparing nipple mastectomy for the young age of the patient. The big question is that technique was associated a higher risk of local recurrence, even if the skin biopsy was negative. Literature shown that nipple sparing mastectomy can be safely performed for breast cancer treatment in carefully selected cases. In a study of Memorial Sloan-Kettering Cancer Center where analyze the nipple sparing mastectomy for breast cancer found that the 39 nipple-areola complexes (100%) were intact and there were no local or systemic recurrences in cases treated for cancer [9]. Although there is no experience described in literature related to breast angiosarcoma.
Axillary dissection is not indicated, as nodal involvement is rare. Skin ulceration or muscle involvement requires adjuvant chemotherapy and radiotherapy. No randomized studies on the role of radiation therapy after surgery for breast angiosarcoma have been published to the date and no systematic therapeutic approach has been described in the literature due to the rarity of this tumor [3].
Local recurrences can appear after surgery in approximately one third of the patients diagnosed with primary angiosarcoma, suggesting that surgery alone often leads to inadequate local tumor control. We perform adjuvant chemotherapy in our case, based on several studies that have compared chemotherapy regimens based on epirubicin and ifosfamide versus no treatment showing a significant improvement in disease-free survival in those patients treated with chemotherapy [10].
4. Conclusion
The importance of this case is to emphasize that primary breast angiosarcoma can develop in breasts with no previous history of radiation. Breast masses with heterogeneous hyperechogenicity on ultrasound exploration, along with distorted architecture should suggest the radiologist the diagnosis of breast angiosarcoma, diagnostic core needle biopsy should be performed in all cases regardless the age of the patient.
Breast angiosarcoma presents no standard therapeutic approach till the moment, due to the rarity of this tumor and its idiosyncrasies. Surgery with posterior adjuvant chemotherapy and/or radiotherapy remain as the main treatments to the moment [11].
Conflicts of interest
The authors declare no conflict of interest.
Funding
Nothing to declare.
Ethical approval
Local (Hospital Quiron) ethics committee has been given and patient’s permission.
Consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal on request.
Author contribution
Sara Iacoponi: study concept, data collection, writing the paper.
Jackie Calleja: review and correct the manuscript.
Gines Hernandez: review and correct the manuscript.
Ricardo Sainz: review and correct the manuscript.
Guarantor
Sara Iacoponi, Jackie Calleja, Gines Hernandez and Ricardo Sainz are guarantors.
References
- 1.Nacimiento A.F., Raut C.P., Fletcher C. Primary angiosarcoma of the breast clinicopathologic analysis of 49 cases, suggesting that grade is not prognostic. Am. J. Surg. Pathol. 2008;32:1896–1904. doi: 10.1097/PAS.0b013e318176dbc7. [DOI] [PubMed] [Google Scholar]
- 2.Adem C., Reynolds C., Ingle J.N., Nascimento A.G. Primary breast sarcoma: clinicopathologic series from the mayo clinic and review of the literature. Br. J. Cancer. 2004;91:237–241. doi: 10.1038/sj.bjc.6601920. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Scow J.S., Reynolds C.A., Degnim A.C., Petersen I.A., Jakub J.W., Boughey J.C. Primary and secondary angiosarcoma of the breast: the mayo clinic experience. J. Surg. Oncol. 2010;101(5):401–407. doi: 10.1002/jso.21497. [DOI] [PubMed] [Google Scholar]
- 4.Tahir M., Hendry P., Baird L. Radiation induced angiosarcoma as a sequela of radiotherapy for breast cancer following conservative surgery. Int. J. Surg. Oncol. 2006;3:1–4. doi: 10.1186/1477-7800-3-26. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Hung J., Hiniker S.M., Lucas D.R., Griffith K.A., McHugh J.B., Meirovits A., Thomas D.G., Chugh R., Herman J.M. Sporadic versus radiation−associated angiosarcoma: a comparative clinicopathologic and molecular analysis of 48 cases. Sarcoma. 2013;2013:798403. doi: 10.1155/2013/798403. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Rosen P.P., Kimmel M., Ernsberger D. Mammary angiosarcoma: the prognostic significance of tumour differentiation. Cancer. 1998;62(10):2145–2151. doi: 10.1002/1097-0142(19881115)62:10<2145::aid-cncr2820621014>3.0.co;2-o. [DOI] [PubMed] [Google Scholar]
- 7.Georgiannos S.N., Sheaff M. Angiosarcoma of the breast: a 30 year perspective with an optimistic outlook. Br. J. Plast. Surg. 2003;56(2):129–134. doi: 10.1016/s0007-1226(03)00025-0. [DOI] [PubMed] [Google Scholar]
- 8.O’Neill A.C., D’Arcy C., McDermott E., O’Doherty A., Quinnand C., McNally S. Magnetic resonance imaging appearances in primary and secondary angiosarcoma of the breast. J. Med. Imaging Radiat. Oncol. 2014;58(2):208–212. doi: 10.1111/1754-9485.12100. [DOI] [PubMed] [Google Scholar]
- 9.Garcia-Etienne C.A., Cody Iii H.S., 3rd, Disa J.J., Cordeiro P., Sacchini V. Nipple-sparing mastectomy: initial experience at the memorial sloan-kettering cancer center and a comprehensive review of literature. Breast J. 2009;15(4):440–449. doi: 10.1111/j.1524-4741.2009.00758.x. [DOI] [PubMed] [Google Scholar]
- 10.Frustaci S., Gherlinzoni F., De Paoli A., Bonetti M., Azzarelli A., Comandone A., Olmi P., Buonadonna A., Pignatti G., Barbieri E., Apice G., Zmerly H., Serraino D., Picci P. Adjuvant chemotherapy for adult soft tissue sarcomas of the extremities and girdles: results of the Italian randomized cooperative trial. J. Clin. Oncol. 2001;19(5):1238–1247. doi: 10.1200/JCO.2001.19.5.1238. [DOI] [PubMed] [Google Scholar]
- 11.Dickson M.A., D’Adamo D.R., Keohan M.L., D'Angelo S.P., Carvajal R.D., Gounder MM1, Maki R.G., Qin L.X., Lefkowitz R.A., McKennon O.R., Hirst C.M., Schwartz G.K., Tap W.D. Phase II trial of gemcitabine and docetaxel with bevacizumab in soft tissue sarcoma. Sarcoma. 2015;2015:532478. doi: 10.1155/2015/532478. [DOI] [PMC free article] [PubMed] [Google Scholar]