Abstract
Purpose
The sperm membrane undergoes extensive surface remodeling as it matures in the epididymis. During this process, the sperm is encapsulated in an extensive glycocalyx layer, which provides the membrane with its characteristic negative electrostatic charge. In this study, we develop a method of microelectrophoresis and standardize the protocol to isolate sperm with high negative membrane charge.
Methods
Under an electric field, the percentage of positively charged sperm (PCS), negatively charged sperm (NCS), and neutrally charged sperm was determined for each ejaculate prior to and following density gradient centrifugation (DGC), and evaluated for sperm DNA damage, and histone retention. Subsequently, PCS, NCS, and neutrally charged sperm were selected using an ICSI needle and directly analyzed for DNA damage.
Results
When raw semen was analyzed using microelectrophoresis, 94 % were NCS. In contrast, DGC completely or partially stripped the negative membrane charge from sperm resulting PCS and neutrally charged sperm, while the charged sperm populations are increased with an increase in electrophoretic current. Following DGC, high sperm DNA damage and abnormal histone retention were inversely correlated with percentage NCS and directly correlated with percentage PCS. NCS exhibited significantly lower DNA damage when compared with control (P < 0.05) and PCS (P < 0.05). When the charged sperm population was corrected for neutrally charged sperm, sperm DNA damage was strongly associated with NCS at a lower electrophoretic current.
Conclusion
The results suggest that selection of NCS at lower current may be an important biomarker to select healthy sperm for assisted reproductive treatment.
Keywords: Membrane glycocalyx, Micro-electrophoresis, Sperm membrane charge, Sperm DNA damage, Sperm selection
Introduction
Mature mammalian sperm generally carry a net negative surface charge [1], and migrate toward the anode during electrophoresis [2]. One of the most interesting observations about this negative potential is that the charge is not a fixed property of the sperm, but rather is a dynamic characteristic that is acquired by the sperm during its development [3]. Bedford [4] first reported that the net negative charge is acquired during the maturation of the sperm within the epididymis, and it is now recognized that sperm undergo a number of modifications during transit through the male and female reproductive tracts [5, 6]. Some of these modifications occur directly to the membrane, a unique property of sperm that is distinct from somatic cells. Modifications to the sperm membrane have been reported during maturation in the epididymis, and during capacitation and acrosome reaction in the female reproductive tract [7–9]. Broader changes in membrane configuration during sperm maturation are important for various cellular interactions, such as cell-to-cell recognition, and sperm-egg interaction during fertilization [10, 11]. The negative charge on the sperm surface also prevents the sperm from aggregation, non-specific binding to the female reproductive tract, and storage [12].
The phenomenon of sperm maturation is viewed primarily as nuclear protein exchange [13], nuclear compaction [14], and membrane or surface modifications [9, 15, 16]. One of the most important modifications to the sperm membrane is the accumulation and encapsulation of glycocalyx over the sperm surface [9, 17]. In mammalian species, CD52, a bipolar glycopeptide of epididymal origin, forms a major component of the sperm glycocalyx [12]. CD52 is a highly sialated glycosylphosphatidylinositol-anchored protein that is acquired during epididymal transit and is located on the sperm plasma membrane [9, 18]. During sperm maturation, the lipid-anchored CD52 antigen is transferred to the sperm membrane [9, 19]. The highly glycosylated sialic acid residues form a 20–60 nm thick negative covering around the sperm, providing a negative charge of −16 to −20 mV [20, 21].
It is thought that the presence of high concentrations of sialic acid residue on the sperm membrane reflects normal spermatogenesis and sperm maturation. Such sperm have higher net negative charge when compared with abnormal and immature sperm [18]. Selection of mature sperm based on differences in sperm membrane charge has been employed by two methods, the Zeta test [22, 23] and electrophoretic sperm separation [24, 25]. Sperm with high negative membrane charge have been shown to be morphologically normal, contain high protamine content [26] and have low levels of DNA damage [24, 26–29]. Charge-separated sperm have been successfully used for assisted reproductive treatment [25, 30] and resulted in a successful pregnancy following multiple ART failures using conventional sperm selection methods [30, 31].
It is well known that sperm selection is an essential part of all assisted conception procedures. Currently, selection for ART mainly relies on selecting motile and morphologically normal sperm. Despite the global use of these conventional sperm selection approaches, it has become evident that sperm selection based on motility and morphology alone inefficiently identifies the most suitable sperm for fertilization [32]. Recently, several molecular features of the sperm such as hyaluronic acid binding, annexin V labeling, ultrastructure at high magnification, membrane charge, and zeta potential have been associated with sperm function and are considered as potentially important markers for selection [22, 24, 25, 33, 34]. Inclusion of these molecular markers along with the conventional method of sperm selection has shown potential promise to improve ART outcomes [35–38].
Elzectrophoretically isolated sperm have been demonstrated to have low DNA damage [24, 29] and suggested to be a more promising sperm selection method for assisted reproductive treatment [30]. Recently, we showed that selection of negatively charged sperm through microelectrophoresis has the potential to isolate sperm relatively free of DNA damage, and that in IVF cycles not utilizing microelectrophoresis for sperm selection, the percentage of negatively charged sperm was positively associated with fertilization rate and blastocyst development and inversely associated with embryo arrest [39]. In addition, we observed that implantation rate and clinical pregnancies rate were higher in patient groups with increased negatively charged sperm [39]. The aim of this study is to optimize the microelectrophoresis sperm selection method to isolate good quality sperm with high negative charge.
Materials and methods
Study population and semen analysis
Seventy-one infertile men undergoing infertility diagnosis were included in the study. The Institutional Review Board governed by the University of Utah approved this study. This study was conducted at the Andrology and IVF laboratories of the University of Utah between January 2013 and April 2014. Sperm samples for research were obtained after each couple gave written consent. Semen samples were collected from infertile men after 2–5 days of recommended abstinence. After liquefaction, routine semen analyses were performed according to WHO guidelines [40].
Sperm used for microelectrophoresis
Raw semen and sperm prepared by density gradient centrifugation (DGC) were used for microelectrophoresis. Semen was processed using a two-step discontinuous DGC (90–35 %; Irvine Scientific, California, United States). Two milliliters of semen was layered on 1.5 mL (90 %) and 1.5 mL (35 %) layers and centrifuged at 400 g for 15 min. The sperm collected after DGC were adjusted to a concentration of 20 million/mL using Quinn’s sperm washing media (CooperSurgical, CT, USA). Approximately, 10–15 μl of raw semen and DGC-prepared sperm was used for inoculation in the microelectrophoresis.
Microelectrophoresis instrumentation
The microelectrophoresis instrument consists of three parts [39]: (1) the power supply, consisting of a basic power-pack unit that can control and supply 0–300 V and 0–300 mA of electricity, (2) the reusable connecting electrodes are used to connect the electrophoresis unit to the power supply, and (3) the disposable sterile electrophoresis unit consists of (a) electrophoresis chamber, (b) egg injection chambers, and (c) bubble restriction chambers (Fig. 1).
Fig. 1.
Photograph of microelectrophoresis instrument on the stage of ICSI inverted microscope
Microelectrophoresis sperm separation
The basic methodology for microelectrophoresis is essentially the same as ICSI sperm selection procedure. The microelectrophoresis apparatus was set-up on the ICSI stage of an inverted microscope and sperm were viewed at 200× magnification and picked up with a beveled, glass ICSI pipette connected to a CellTram Vario manual microinjector (Eppendorf). Two milliliters of electrophoresis buffer (10 mM Tris, 20 mM NaOH, pH: 7.8) were added to the electrophoresis chamber. Approximately 10–15 μl sperm were added to the electrophoretic buffer and allowed to settle for 2 min. Electrophoresis was performed by applying current between 6–14 mA (increased from low to high) and a variable 30–100 V. Sperm was collected during electrophoresis (as soon as the electrophoresis was initiated and not after electrophoresis was completed). During electrophoresis, the sperm were viewed through the ICSI inverted microscope. The charge of the sperm was observed by visualizing the direction of sperm movement under the influence of current (PCS move toward cathode and NCS move toward the anode). Similarly charged sperm (PCS, NCS, or neutral) were collected into the ICSI pipette and placed on a marked glass slide for further analysis. The process was repeated until 50 PCS, NCS, and neutrally charged sperm were collected for each sample. In patients where the number of charged sperm was low, sperm were identified within the electrophoretic chamber at different microscopic field of view by moving the ICSI stage. The sperm were separated at low current first (6 mA) to ensure the isolation of sperm with a high negative charge. The current was gradually increased to facilitate the movement of sperm in the electrophoretic field. During electrophoresis, sperm were assessed for their morphology, and sperm with normal morphology and negatively charge were selected using the ICSI pipette. Subsequently, negatively charged sperm were selected at low current (6, 8, and 10 mA) and compared with PCS and controls for DNA damage. Fifty charged sperm were collected within 3–5 min of electrophoretic exposure. The electrophoretic duration varied between patient samples and according to the availability of charged sperm. The ratio of charged sperm in the native semen and prepared sperm were examined with 200–400× magnification: 200 sperm were evaluated per sample based on their movement in the electric field and classified into PCS, NCS, and neutrally charged sperm. The results were expressed in percent (Table 1).
Table 1.
Comparison of charged sperm population before and after density gradient centrifugation (DGC) at different electrophoretic current (mA) settings (n = 75)
| Current (mA) | Sperm charge | Difference ± SE | P value | Change in sperm charge after DGC (%) | ||
|---|---|---|---|---|---|---|
| ↓ | ↑ | No change | ||||
| 6 | Negative | 41.60 ± 3.95 | <0.001 | 89 | 10 | 1 |
| Neutral | −22.96 ± 5.06 | <0.001 | 27 | 72 | 1 | |
| Positive | −18.32 ± 3.24 | <0.001 | 7 | 69 | 24 | |
| 8 | Negative | 49.15 ± 3.94 | <0.001 | 90 | 7 | 3 |
| Neutral | −23.86 ± 4.49 | <0.001 | 22 | 73 | 5 | |
| Positive | −25.51 ± 3.52 | <0.001 | 5 | 74 | 21 | |
| 10 | Negative | 53.34 ± 4.09 | <0.001 | 89 | 10 | 1 |
| Neutral | −15.59 ± 3.46 | <0.001 | 20 | 73 | 7 | |
| Positive | −36.59 ± 3.56 | <0.001 | 4 | 84 | 12 | |
| 12 | Negative | 52.84 ± 3.98 | <0.001 | 89 | 8 | 3 |
| Neutral | −6.03 ± 1.86 | <0.002 | 20 | 57 | 23 | |
| Positive | −46.49 ± 3.88 | <0.001 | 4 | 85 | 11 | |
| 14 | Negative | 52.35 ± 3.98 | <0.001 | 86 | 3 | 11 |
| Neutral | −1.09 ± 0.87 | =0.039 | 8 | 17 | 75 | |
| Positive | −51.07 ± 3.94 | <0.001 | 3 | 86 | 11 | |
Comparison between native semen and DGC sperm was performed using a Wilcoxon signed-rank test
Aniline blue staining
Histone retention was assessed using the aniline blue staining method. Raw semen was smeared on a glass slide, air-dried, and fixed for 10 min with 4 % glutaraldehyde in phosphate-buffered saline. Staining was performed for 5 min using a 5 % aniline blue solution that was diluted in 4 % acetic acid (approximately pH 3.5). Subsequently, slides were carefully rinsed with tap water, air-dried, and analyzed using a bright-field microscope. Overall, 200 sperm were analyzed per slide. Sperm were classified into three categories; as high, moderate, and low histone content as previously described [41].
TUNEL assay
Measurement of sperm DNA damage was performed using the TUNEL assay as previously described by our group [42]. TUNEL assay was performed using the Fluorescein in situ Cell Death Detection kit, in accordance with the manufacturer’s guidelines (Roche Diagnostics GmbH, Mannheim, Germany). Fifty sperm per charge type (PCS, NCS, and neutral) were evaluated.
Statistical analysis
Data were analyzed using SPSS version 22.0 for Windows (SPSS Inc., Chicago, IL). Data are presented as mean ± SE. Pearson’s correlation coefficient was used to correlate sperm DNA damage and histone retention with the percentage of negatively (NCS) and positively (PCS) charged sperm at different electrophoretic currents (6, 8, 10, 12, and 14 mA). To identify the effect of PCS and NCS population on the test parameters, a correction for neutrally charged sperm was performed. A percentage was drawn across PCS and NCS following elimination of the neutrally charged population at each electrophoretic current setting. R2 values were determined by quadratic or linear line fit method and regression models, before and after correction for neutrally charged sperm. Duncan’s test of multiple variants was used to compare the percentage of charged sperm (NCS, PCS, and neutral) at each electrophoretic current. Wilcoxon signed-rank test was used to compare the proportion of charged sperm in the raw semen with DGC-prepared sperm. A paired sample t test was used to compare sperm DNA damage between the charged groups and DGC-control.
Results
Comparison of sperm charge distribution between raw semen and DGC-prepared sperm
In the native semen, an average of 89.0 ± 1.0 % of the sperm displayed a negative charge. The percentage of charged sperm varied between individuals. Under the electric field, some sperm did not move toward cathode or anode; such sperm were considered neutral or with very low +/− charge [39]. By increasing the current during electrophoresis it was possible to move the low charged sperm toward the cathode or anode. An electric field between 6 and 14 mA was found to be optimal for electrophoretically moving the sperm using microelectrophoresis. At 14 mA, 1.41 ± 0.7 % of the sperm were immobile (neutrally charged) in the electric field (Table 1).
In the native semen (Fig. 2a), there was an increase in the percentage of NCS (R2 = 0.999; P < 0.001) and PCS (R2 = 0.998; P < 0.001) with an increase in current. In contrast, the percentage of neutrally charged sperm decreased with increase in current (R2 = −0.999; P < 0.001). A similar trend was also observed in the NCS (R2 = 0.998; P < 0.001), PCS (R2 = 0.983; P < 0.001), and neutral (R2 = −0.993; P < 0.001) charged sperm population after DGC (Fig. 2b). After DGC, there was a decrease in the percentage of NCS and an increase in the percentage of positive and neutrally charged sperm (Table 1). As native semen samples contained a significantly higher percentage of negatively charged sperm than DGC samples, it is likely that the process of sperm preparation by DGC removes the charged particles adhered to the surface of the sperm membrane. The charge of the sperm was not associated to any of the sperm parameters (Table 2).
Fig. 2.
a The percentage of negative, positive, and neutrally charged sperm in the native semen at various electrophoretic current (mA) settings (n = 58). b The percentage of negative, positive, and neutrally charged sperm after density gradient centrifugation at various electrophoretic current (mA) settings (n = 58)
Table 2.
Demographics of patients included in the study (n = 71)
| Test parameters | Mean ± SE | Range | Correlation with NCS R 2 (P value) | Correlation with PCS R 2 (P value) |
|---|---|---|---|---|
| Semen volume (mL) | 3.72 ± 0.22 | 1.2 to 11.0 | 0.202 (0.143) | −0.217 (0.114) |
| Sperm count (million) | 85.07 ± 9.10 | 2.8 to 376.0 | −0.203 (0.142) | 0.197 (0.154) |
| Total sperm count (million) | 261.21 ± 28.13 | 9.5 to 923.0 | −0.136 (0.326) | 0.111 (0.423) |
| Total progressive motile count (%) | 124.32 ± 22.97 | 1.7 to 374.3 | 0.025 (0.915) | −0.153 (0.508) |
| Progressive motility (%) | 46.29 ± 3.56 | 9 to 71 | 0.061 (0.793) | −0.160 (0.489) |
| Non-motile sperm count (%) | 3.55 ± 0.94 | 0 to 14 | 0.287 (0.219) | −0.204 (0.388) |
| Total motility (million) | 57.46 ± 4.77 | 19.0 to 129.0 | 0.205 (0.372) | −0.246 (0.282) |
| Vitality (%) | 56.62 ± 3.59 | 20 to 86 | 0.013 (0.954) | −0.054 (0.817) |
| Hypoosmolarity (%) | 61.15 ± 2.73 | 29 to 80 | −0.137 (0.541) | −0.075 (0.592) |
| Normal head (%) | 27.85 ± 1.61 | 4 to 60 | 0.085 (0.541) | −0.075 (0.592) |
| Large head (%) | 0.87 ± 0.14 | 0 to 4 | −0.076 (0.581) | 0.082 (0.552) |
| Small head (%) | 1.33 ± 0.21 | 0 to 6 | 0.126 (0.259) | −0.077 (0.906) |
| Tapered head (%) | 33.67 ± 2.15 | 0 to 68 | 0.059 (0.666) | 0.016 (0.906) |
| Immature sperm (%) | 12.65 ± 1.46 | 0 to 59 | −0.073 (0.601) | 0.028 (0.842) |
| Normal tail (%) | 71.57 ± 1.52 | 23 to 88 | −0.088 (0.526) | 0.082 (0.554) |
| Amorphous cell content (million) | 0.14 ± 0.10 | 0 to 2 | 0.060 (0.797) | −0.028 (0.903) |
| Neutrophils (million) | 0.05 ± 0.04 | 0 to 1 | 0.144 (0.532) | −0.129 (0.578) |
| Male age (years) | 34.72 ± 0.79 | 24 to 51 | −0.210 (0.117) | 0.246 (0.065) |
Pearson’s correlation was used to associate the sperm charge (at 14 mA) with sperm parameters. P value <0.05 is considered statistically significant
Correlation between nucleoprotein maturation and sperm charge
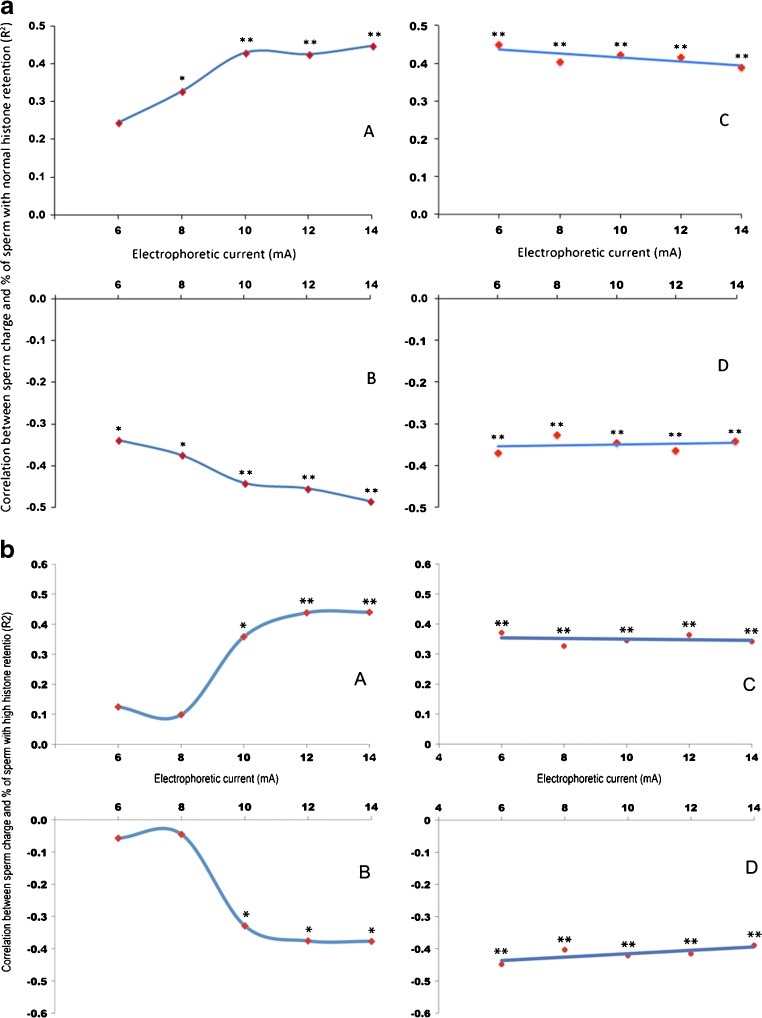
We previously showed that the percentage of sperm with abnormally high histone retention was inversely associated with NCS and positively associated with PCS [39]. Here we show that the percentage of sperm with normal histone retention was positively associated with NCS and inversely associated with PCS at each electrophoretic current setting, and the relationship grew stronger with increasing current (Fig. 3a). However, when we excluded neutrally charged sperm, the relationship was identical at all electrophoretic current settings (Fig. 3b). Similarly, a regression model showed that the percentage of sperm with normal histone retention was positively associated with NCS (R2 = 0.531, P < 0.001) and negatively associated with PCS (R2 = −0.473, P = 0.008).
Fig. 3.
a Correlations between sperm charge and normal histone retention (n = 67) at various electrophoretic current (mA) settings (A and B), and following correction for neutrally charged sperm (C and D). Negatively charged sperm (A and C), and positively charged sperm (B and D). Each point represents the correlation between sperm charge and histone retention at each respective current setting. Correlation coefficient was determined by quadratic or linear line fit model. The line represents the trend in correlations across the different currents. *P < 0.05, **P < 0.01. b Correlations between sperm charge and high histone retention (n = 67) at various electrophoretic current (mA) settings (A and B), and following correction for neutrally charged sperm (C and D). Positively charged sperm (A and C), and negatively charged sperm (B and D). Each point represents the correlation between sperm charge and histone retention at each respective current setting. Correlation coefficient was determined by quadratic or linear line fit model. The line represents the trend in correlations across the different currents. *P < 0.05, **P < 0.01
Correlation between sperm DNA damage and sperm charge
We previously showed that sperm DNA damage measured by TUNEL assay was negatively associated with %NCS, and positively correlated with %PCS [39]. In the current study, we found that as current is increased, this correlation becomes stronger (Fig. 4a). The presence of neutrally charged sperm at lower voltage (6, 8, and 10 mA) reduced the correlation coefficient in both NCS and PCS. When we exclude the neutrally charged sperm, we observed a significant correlation between the NCS and PCS with DNA damage at lower electrophoretic settings (Fig. 4b). There were no differences in the level of sperm DNA damage when sperm were picked at lower electrophoretic current settings (Fig. 5); however, at all current settings NCS showed significantly lower DNA damage, when compared with PCS and their corresponding DGC-control. The results were confirmed using a regression model, where the percentage of sperm with DNA damage was inversely associated with NCS before (R2 = −0.346, P = 0.002) and after (R2 = −0.228, P = 0.049) correction for neutrally charged sperm.
Fig. 4.
a Correlations between sperm charge and sperm DNA damage at various electrophoretic current (mA) settings (n = 71). Negatively charged sperm (A), and positively charged sperm (B). Each point represents the correlation between sperm charge and sperm DNA damage at each respective current setting. Correlation coefficient was determined by quadratic or linear line fit model. The line represents the trend in correlations across the different currents. *P < 0.05, **P < 0.01. b Correlations between sperm charge and sperm DNA damage at various electrophoretic current (mA) settings (n = 71), following correction for neutrally charged sperm. Negatively charged sperm (A), and positively charged sperm (B). Each point represents the correlation between sperm charge and sperm DNA damage at each respective current setting. Correlation coefficient was determined by quadratic or linear line fit model. The line represents the trend in correlations across the different currents. *P < 0.05, **P < 0.01
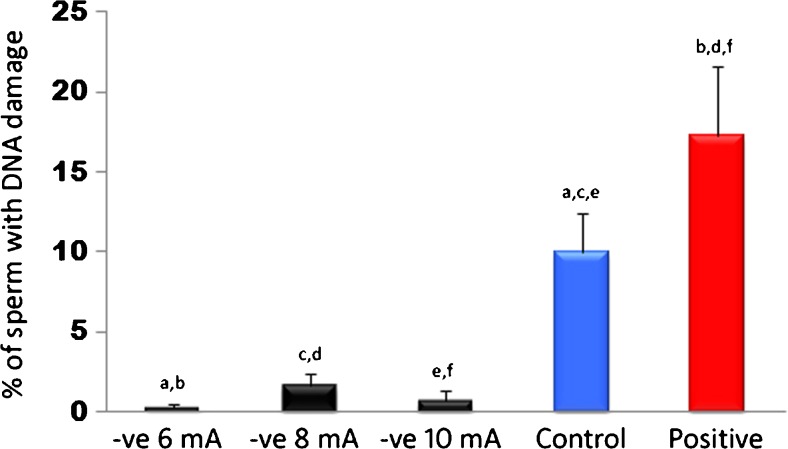
Fig. 5.
Percentage of sperm with DNA damage, when sperm were picked based on their charge using an ICSI pipette (n = 18). Negative charged sperm (−ve) was picked at three electrophoretic current settings (6, 8, and 10 mA). Columns with identical superscripts were statistically significant (P < 0.05). Comparison between the charged groups and control were performed using a paired sample t test
Discussion
Sperm maturation in the epididymis involves changes to the plasma membrane in the form of alterations in lipid and protein composition, modifications of surface proteins, and increased total negative charge of the extracellular surface. In this study, we aimed to optimize conditions in which sperm membrane charge may be use as a biomarker to identify a healthy sperm for ART. In the ejaculated semen, we observed that the vast majority of sperm had acquired a negative membrane charge. However, after the process of density gradient centrifugation, a partial or complete removal of the negative surface charge occurs, leading to an increased proportion of positively charged sperm. Here, we associate sperm charge with histone retention and sperm DNA damage at different electrophoretic current settings and optimize microelectrophoretic sperm selection method to most efficiently isolate healthy sperm suitable for ART.
Sperm must traverse the epididymis to acquire motility and fertility potential [43]. In mammalian species, approximately 125 epididymal epithelial cell secretions have been identified in the form of proteins and glycoproteins [44, 45]. Accumulation of these components on the sperm membrane provides the sperm its characteristic negative charge [3, 4]. Here, we observed that about 60 % of the sperm in the ejaculate possess negative membrane charge when observed under a low electrophoretic current setting of 6 mA. However, when the current is increased to 14 mA, 89 % of the sperm show electrophoretic mobility toward the anode. A gradual increase in the population of NCS was observed as current was increased. These findings suggest that not all sperm in the ejaculate have identical membrane charge. We also observed that less than 10 % of the sperm in the ejaculate carry a positive charge, which can be identified by the movement of these sperm toward the cathode. Our results support the notion that sperm membrane charge is a variable factor, which may depend on the accumulation of negatively charged glycoproteins to the sperm membrane.
It is well documented that some epididymal proteins are weakly associated with the sperm membrane [46, 47], whereas others are anchored to the membrane by glycosylphosphatidylinositol sub-units [12, 48]. Modifications in membrane configuration could disrupt the association between epididymal proteins and the sperm membrane. During cryopreservation (reviewed by Leahy and Gadella [48],) and early capacitation [49], modification and redistribution of molecules to the sperm membrane could also cause the loss of the epididymal proteins from the sperm surface [50, 51], resulting in the loss of electro negativity. For the first time, we showed that the process of DGC appears to physically wash off the negative charge from the sperm, a beneficial effect for charge-based sperm selection. Interestingly, not all sperm in the ejaculate loose their negative charge. Although the process of DGC should have identical effect on all sperm, presumably the cells with a higher starting negative charge retain some of their negative charge, while the cells with low negative charge completely loose their charge to become PCS. This effect increases our ability to identify the sperm that display the highest negative charge, and thus the sperm that generally display the lowest DNA damage. This concept is supported by the observation that sperm with high negative membrane charge could be electrophoretically moved at low current (6 mA), while the immovable (neutrally charged) sperm could be moved toward the cathode or anode by increasing the electrophoretic current (Fig. 2a, b). Our observations here are in accordance with the published literature [12, 46–48] suggesting that the epididymal proteins adhered to the sperm surface are removable.
The correlation between sperm charge (NCS and PCS) and DNA damage increased with an increase in electrophoretic current (Fig. 3a). The stronger correlation at higher electrophoretic current is because at these settings the proportion of neutrally charged sperm is low and the majority of the sperm show electrophoretic mobility. As current is increased, the neutrally charged sperm population attained electrophoretic mobility and were able to move toward the cathode or anode. To establish the actual correlation between the PCS and NCS with DNA damage, we corrected the sperm population for neutral charge at each electrophoretic current setting. By eliminating the neutrally charged population, we found that the correlation between sperm charge and DNA damage was stronger at lower electrophoretic current settings. A sperm becomes positively charged when it completely loses the negatively charged glycoproteins anchored/adhered on its membrane. It is well known that apoptosis is a mechanism to eliminate dysfunctional cells [52]. During apoptosis in sperm, the integrity of the membrane is lost due to the translocation of phosphatidylserine [53], during which the phosphatidylserine is shifted from the interior to the exterior of the plasma membrane [54, 55]. In addition, apoptosis results in DNA fragmentation and degradation of cytoskeletal and nuclear proteins (reviewed by Elmore [56],), and affects fluidity of the plasma membrane [57]. The externalization of phosphatidylserine and loss of membrane fluidity may also facilitate the loss of epididymal glycoproteins anchored to the membrane, thereby causing a loss in negative charge. In accordance with this hypothesis, our results showed that NCS are relatively free of DNA damage when compared to PCS.
During spermatogenesis, sperm chromatin undergoes structural modifications to result in a highly condensed state [58] by the replacement of nucleo-histones by protamines [59, 60]. Here we observe that normal histone packaging increases with an increase in NCS, and conversely, the proportion of sperm with abnormal histone increases with an increase in PCS. When analyzed at different electrophoretic current settings, the correlation between abnormal histone retention and PCS grew stronger with an increase in electrophoretic current. However, this effect was comparable in all current settings, when corrected for neutrally charged sperm. Multiple studies have reported an association between sperm chromatin compaction and abnormal sperm head morphology [61–63] and acrosome abnormalities [64]. Although the compaction of the nuclear chromatin and DNA integrity are two interdependent parameters [65, 66], some studies have reported an association between them [67, 68]. We hypothesize the loss of negative charge from the plasma membrane may be associated via an apoptosis-mediated pathway. It is evident that sperm with protamine deficiency and increased histone retention negatively affects fertilization and embryo development (reviewed by Oliva [13],); in light of our results, selection of NCS may be effective in identifying sperm with normal chromatin status, potentially improving ART outcomes.
Sperm membrane charge has been exploited by two other methods of sperm selection, Zeta test [22, 23] and electrophoretic sperm separation [24, 25]. Use of NCS selected by Zeta method resulted in an improvement in fertilization, implantation, and pregnancy rates [31, 36], suggesting that selection of sperm with a high negative charge could aid in the isolation of mature and healthy sperm for ART.
In humans, binding of the epididymal secretions to the sperm membrane is functionally important for zona binding [69], oocyte fusion [70], and fertilization [71]. Defects in the uptake of epididymal secretions onto the sperm membrane have been reported in patients with abnormal sperm parameters [72]. In this study, we used the negatively charged epididymal glycoproteins as a biomarker to identify healthy sperm. The electrophoretic buffer used here is hypotonic, which may induce osmotic stress to sperm. We performed electrophoresis by substituting Quinn’s sperm media for electrophoresis buffer and likewise observed electrophoretic mobility of the sperm. In Quinn’s media, the electrophoretic mobility of the sperm was reduced, presumably due to the lower ionic concentration. We also observed that the sperm motility is altered before and after five minutes of electrophoresis. Further studies are required to optimize the electrophoresis buffer and to evaluate the safety of the sperm selected using microelectrophoresis. Our findings in this study show that selection of highly negatively charged sperm is now possible through microelectrophoresis, which is an extremely versatile, quick, easy to use method that does not require complex instruments. Selection of sperm with a high negative charge may serve as a non-invasive biomarker for selecting non-apoptotic sperm; however, this proof-of-principle has yet to be confirmed in the context of ART.
Acknowledgments
This project was supported by research grants from EMD Serono, Rockland, Massachusetts, and the Howard and Georgeanna Jones Foundation for Reproductive Medicine, Norfolk, Virginia. The authors wish to thank the UCRM IVF unit and laboratory staff for their commitment and support to this project, for preparing tissue samples, and for helping to collect data on ART outcomes.
Footnotes
Capsule This study is aimed to standardize the microelectrophoresis protocol to isolate sperm with high negative membrane charge. The results from this study suggest that selection of negatively charged sperm at lower current may serve as an important biomarker to select healthy sperm for assisted reproductive treatment.
References
- 1.Veres I. Negative electrical charge of the surface of bull sperm. Mikroskopie. 1968;23:166–9. [PubMed] [Google Scholar]
- 2.Nevo AC, Michaeli I, Schindler H. Electrophoretic properties of bull and of rabbit spermatozoa. Exp Cell Res. 1961;23:69–83. doi: 10.1016/0014-4827(61)90064-7. [DOI] [PubMed] [Google Scholar]
- 3.Yanagimachi R, Noda YD, Fujimoto M, Nicolson GL. The distribution of negative surface charges on mammalian spermatozoa. Am J Anat. 1972;135:497–520. doi: 10.1002/aja.1001350405. [DOI] [PubMed] [Google Scholar]
- 4.Bedford JM. Changes in the electrophoretic properties of rabbit spermatozoa during passage through the epididymis. Nature. 1963;200:1178–80. doi: 10.1038/2001178a0. [DOI] [PubMed] [Google Scholar]
- 5.Bostwick EF, Bentley MD, Hunter AG, Hammer R. Identification of surface glycoprotein on porcine spermatozoa and its alteration during epididymal maturation. Biol Reprod. 1980;23:161–5. doi: 10.1095/biolreprod23.1.161. [DOI] [PubMed] [Google Scholar]
- 6.Olson GE, Danzo BJ. Surface changes in the rat spermatozoa during epididymal transit. Biol Reprod. 1981;24:431–6. doi: 10.1095/biolreprod24.2.431. [DOI] [PubMed] [Google Scholar]
- 7.Lassalle B, Testart J. Human zona pellucida recognition associated with removal of sialic acid from human sperm surface. J Reprod Fertil. 1994;101:703–11. doi: 10.1530/jrf.0.1010703. [DOI] [PubMed] [Google Scholar]
- 8.Deng X, Czymmek K, Deleon M. Biochemical maturation of spam1 (PH-20) during epididymal transit of mouse sperm involves modifications of N-linked oligosaccharides. Mol Reprod Dev. 1999;52:196–206. doi: 10.1002/(SICI)1098-2795(199902)52:2<196::AID-MRD11>3.0.CO;2-A. [DOI] [PubMed] [Google Scholar]
- 9.Ainsworth CJ, Nixon B, Aitken RJ. The electrophoretic separation of spermatozoa: an analysis of genotype, surface carbohydrate composition and potential for capacitation. Int J Androl. 2011;34:422–34. doi: 10.1111/j.1365-2605.2011.01164.x. [DOI] [PubMed] [Google Scholar]
- 10.Bedford JM. Sperm capacitation and fertilization in mammals. Biol Reprod. 1970;2:128–58. doi: 10.1095/biolreprod2.Supplement_2.128. [DOI] [PubMed] [Google Scholar]
- 11.Bedford JM, Nicander L. Ultrastructural changes in the acrosome and sperm membranes during maturation of spermatozoa in the testis and epididymis of the rabbit and monkey. J Anat. 1971;108:527–43. [PMC free article] [PubMed] [Google Scholar]
- 12.Kirchhoff C, Schroter S. New insights into the origin, structure and role of CD52: a major component of the mammalian sperm glycocalyx. Cells Tissues Organs. 2001;168:93–104. doi: 10.1159/000016810. [DOI] [PubMed] [Google Scholar]
- 13.Oliva R. Protamines and male infertility. Hum Reprod Update. 2006;12:417–35. doi: 10.1093/humupd/dml009. [DOI] [PubMed] [Google Scholar]
- 14.Golan R, Shochat L, Weissenberg R, Soffer Y, Marcus Z, Oschry Y, et al. Evaluation of chromatin condensation in human spermatozoa: a flow cytometric assay using Acridine Orange staining. Mol Hum Reprod. 1977;3:47–54. doi: 10.1093/molehr/3.1.47. [DOI] [PubMed] [Google Scholar]
- 15.Turner TT. On the epididymis and its role in the development of the fertile ejaculate. J Androl. 1995;16:292–8. [PubMed] [Google Scholar]
- 16.Cooper TG. Interactions between epididymal secretions and spermatozoa. J Reprod Fertil. 1998;53:119–36. [PubMed] [Google Scholar]
- 17.Schroter S, Osterhoff C, McArdle W, Ivell R. The glycocalyx of the sperm surface. Hum Reprod Update. 1999;5:302–13. doi: 10.1093/humupd/5.4.302. [DOI] [PubMed] [Google Scholar]
- 18.Giuliani V, Pandolfi C, Santucci R, Pelliccione F, Macerola B, Focarelli R, et al. Expression of gp20, a human sperm antigen of epididymal origin, is reduced in spermatozoa from subfertile men. Mol Reprod Dev. 2004;69:235–40. doi: 10.1002/mrd.20166. [DOI] [PubMed] [Google Scholar]
- 19.Schroter S, Derr P, Conradt HS, Nimtz M, Hale G, Kirchhoff C. Male-specific modification of human CD52. J Biol Chem. 1999;274:29862–73. doi: 10.1074/jbc.274.42.29862. [DOI] [PubMed] [Google Scholar]
- 20.Ishijima SA, Okuno M, Mohri H. Zeta potential of human X- and Y-bearing sperm. Int J Androl. 1991;14:340–7. doi: 10.1111/j.1365-2605.1991.tb01102.x. [DOI] [PubMed] [Google Scholar]
- 21.Yudin AI, Generao SE, Tollner TL, Treece CA, Overstreet JW, Cherr GN. Beta-defensin 126 on the cell surface protects sperm from immunorecognition and binding of anti-sperm antibodies. Bio Reprod. 2005;73:1243–52. doi: 10.1095/biolreprod.105.042432. [DOI] [PubMed] [Google Scholar]
- 22.Chan PJ, Jacobson JD, Corselli JU, Patton WC. A simple zeta method for sperm selection based on membrane charge. Fertil Steril. 2006;85:481–6. doi: 10.1016/j.fertnstert.2005.07.1302. [DOI] [PubMed] [Google Scholar]
- 23.Kam TL, Jacobson JD, Patton WC, Corselli JU, Chan PJ. Retention of membrane charge attributes by cryopreserved-thawed sperm and zeta selection. J Assist Reprod Genet. 2007;24:429–34. doi: 10.1007/s10815-007-9158-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Ainsworth C, Nixon B, Aitken RJ. Development of a novel electrophoretic system for the isolation of human spermatozoa. Hum Reprod. 2005;20:2261–70. doi: 10.1093/humrep/dei024. [DOI] [PubMed] [Google Scholar]
- 25.Ainsworth C, Nixon B, Jansen RP, Aitken RJ. First recorded pregnancy and normal birth after ICSI using electrophoretically isolated spermatozoa. Hum Reprod. 2007;22:197–200. doi: 10.1093/humrep/del351. [DOI] [PubMed] [Google Scholar]
- 26.Razavi SH, Nasr-Esfahani MH, Deemeh MR, Shayesteh M, Tavalaee M. Evaluation of zeta and HA-binding methods for selection of spermatozoa with normal morphology, protamine content and DNA integrity. Andrologia. 2010;42:13–9. doi: 10.1111/j.1439-0272.2009.00948.x. [DOI] [PubMed] [Google Scholar]
- 27.Deemeh MR, Nasr-Esfahani MH, Razavi S, Nazem H, Moghadam MS, Tavalaee M. The comparison of HA binding and Zeta methods efficiency in selection of sperm with normal morphology and intact chromatin. J Isfahan Med School. 2009;27:46–56. [Google Scholar]
- 28.Khajavi NA, Razavi S, Mardani M, Tavalaee M, Deemeh MR, Nasr-Esfahani MH. Can Zeta sperm selection method, recover sperm with higher DNA integrity compare to density gradient centrifugation? Iranian J Reprod Med. 2009;7:73–7. [Google Scholar]
- 29.Aitken RJ, Hanson AR, Kuczera L. Electrophoretic sperm isolation: optimization of electrophoresis conditions and impact on oxidative stress. Hum Reprod. 2011;26:1955–64. doi: 10.1093/humrep/der162. [DOI] [PubMed] [Google Scholar]
- 30.Fleming SD, Ilad RS, Griffin AM, Wu Y, Ong KJ, Smith HC, et al. Prospective controlled trial of an electrophoretic method of sperm preparation for assisted reproduction: comparison with density gradient centrifugation. Hum Reprod. 2008;23:2646–51. doi: 10.1093/humrep/den330. [DOI] [PubMed] [Google Scholar]
- 31.Deemeh MR, Tavalaee M, Ahmadi SM, Kalantari SA, Nasab SVA, Najafi MH, et al. The first report of successfully pregnancy after ICSI with combined DGC/Zeta sperm selection procedure in a couple with eleven repeated fail IVF/ICSI cycles. Int J Fertil Steril. 2010;4:41–3. [Google Scholar]
- 32.Yetunde I, Vasiliki M. Effects of advanced selection methods on sperm quality and ART outcome. Minerva Ginecol. 2013;65:487–96. [PubMed] [Google Scholar]
- 33.Bartoov B, Berkovitz A, Eltes F, Kogosovsky A, Yagoda A, Lederman H, et al. Pregnancy rates are higher with intracytoplasmic morphologically selected sperm injection than with conventional intracytoplasmic injection. Fertil Steril. 2003;80:1413–9. doi: 10.1016/j.fertnstert.2003.05.016. [DOI] [PubMed] [Google Scholar]
- 34.Parmegiani L, Cognigni GE, Bernardi S, Troilo E, Ciampaglia W, Filicori M. “Physiologic ICSI”: hyaluronic acid (HA) favors selection of spermatozoa without DNA fragmentation and with normal nucleus, resulting in improvement of embryo quality. Fertil Steril. 2010;93:598–604. doi: 10.1016/j.fertnstert.2009.03.033. [DOI] [PubMed] [Google Scholar]
- 35.Nasr-Esfahani MH, Razavi S, Vahdati AA, Fathi F, Tavalaee M. Evaluation of sperm selection procedure based on hyaluronic acid binding ability on ICSI outcome. J Assist Reprod Genet. 2008;25:197–203. doi: 10.1007/s10815-008-9223-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Kheirollahi-Kouhestani M, Razavi S, Tavalaee M, Deemeh MR, Mardani M, Moshtaghian J, et al. Selection of sperm based on combined density gradient and Zeta method may improve ICSI outcome. Hum Reprod. 2009;24:2409–16. doi: 10.1093/humrep/dep088. [DOI] [PubMed] [Google Scholar]
- 37.Polak de Fried E, Denaday F. Single and twin ongoing pregnancies in two cases of previous ART failure after ICSI performed with sperm sorted using annexin V microbeads. Fertil Steril. 2010;94(351):e15–8. doi: 10.1016/j.fertnstert.2009.12.037. [DOI] [PubMed] [Google Scholar]
- 38.Wilding M, Coppola G, di Matteo L, Palagiano A, Fusco E, Dale B. Intracytoplasmic injection of morphologically selected spermatozoa (IMSI) improves outcome after assisted reproduction by deselecting physiologically poor quality spermatozoa. J Assist Reprod Genet. 2011;28:253–62. doi: 10.1007/s10815-010-9505-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Simon L, Murphy K, Aston KI, Emery BR, Hotaling JM, Carrell DT. Micro-electrophoresis: a non-invasive method of sperm selection based on membrane charge. Fertil Steril. 2015;103:361–6. doi: 10.1016/j.fertnstert.2014.10.047. [DOI] [PubMed] [Google Scholar]
- 40.World Health Organization . WHO laboratory manual for the examination of human semen and sperm-cervical mucus interaction. 4. Cambridge: Cambridge University Press; 1999. [Google Scholar]
- 41.Boitrelle F, Ferfouri F, Petit JM, Segretain D, Tourain C, Bergere M, et al. Large human sperm vacuoles observed in motile spermatozoa under high magnification: nuclear thumbprints linked to failure of chromatin condensation. Hum Reprod. 2011;26:1650–8. doi: 10.1093/humrep/der129. [DOI] [PubMed] [Google Scholar]
- 42.Chohan KR, Griffin JT, Lafromboise M, De Jonge CJ, Carrell DT. Comparison of chromatin assays for DNA fragmentation evaluation in human sperm. J Androl. 2006;27:53–9. doi: 10.2164/jandrol.05068. [DOI] [PubMed] [Google Scholar]
- 43.Cornwall GA, Lareyre JJ, Matusik RJ, Hinton BT, Orgebin-Crist MC. Gene expression and epididymal function. In: The epididymis: from molecules to clinical practice—a comprehensive survey of the efferent ducts, the epididymis and the vas deferens. Roubaire, B., Hinton, B.T., (Eds.) New York, 2002, pp. 575.
- 44.Syntin P, Dacheux X, Gatti JL, Okamura N, Dacheux JL. Characterization and identification of proteins secreted in the various regions of the adult boar epididymis. Bio Reprod. 1996;55:956–74. doi: 10.1095/biolreprod55.5.956. [DOI] [PubMed] [Google Scholar]
- 45.Yeung CH, Cooper TG, Wagenfeld A, Kirchhoff C, Kliesch S, Poser D, et al. Interaction of the human epididymal protein CD52 (HE5) with epididymal spermatozoa from men and cynomolgus monkey. Mol Reprod Develop. 1997;48:267–75. doi: 10.1002/(SICI)1098-2795(199710)48:2<267::AID-MRD15>3.0.CO;2-V. [DOI] [PubMed] [Google Scholar]
- 46.Howes EA, Hurst S, Laslop A, Jones R. Cellular distribution and molecular heterogeneity of MAC393 antigen (clusterin, beta-chain) on the surface membrane of bull spermatozoa. Mol Hum Reprod. 1998;4:673–81. doi: 10.1093/molehr/4.7.673. [DOI] [PubMed] [Google Scholar]
- 47.Kirchhoff C, Osterhoff C, Pera I, Schroter S. Function of human epididymal proteins in sperm maturation. Andrologia. 1998;30:225–32. doi: 10.1111/j.1439-0272.1998.tb01164.x. [DOI] [PubMed] [Google Scholar]
- 48.Leahy T, Gadella BM. Sperm surface changes and physiological consequences induced by sperm handling and storage. Reprod. 2011;142:759–78. doi: 10.1530/REP-11-0310. [DOI] [PubMed] [Google Scholar]
- 49.Gadella BM, Lopescardozo M, Vangolde LMG, Colenbrander B, Gadella TWJ. Glycolipid migration from the apical to the equatorial subdomains of the sperm head plasma membrane precedes the acrosome reaction—evidence for a primary capacitation event in boar spermatozoa. J Cell Sci. 1995;108:935–46. doi: 10.1242/jcs.108.3.935. [DOI] [PubMed] [Google Scholar]
- 50.Bedford JM, Chang MC. Removal of decapacitation factor from seminal plasma by high-speed centrifugation. Am J Physiol. 1962;202:179–87. doi: 10.1152/ajplegacy.1962.202.1.179. [DOI] [PubMed] [Google Scholar]
- 51.Yanagimachi R. Mammalian fertilization. Knobil E, Neill JD. (Eds.) In: The Physiology of Reproduction, 2nd edition, New York, 1994, pp. 189–317.
- 52.Norbury CJ, Hickson ID. Cellular responses to DNA damage. Annu Rev Pharmacol Toxicol. 2001;41:367–401. doi: 10.1146/annurev.pharmtox.41.1.367. [DOI] [PubMed] [Google Scholar]
- 53.Mourdjeva M, Kyurkchiev D, Mandinova A, Altankova I, Kehayov I, Kyurkchiev S. Dynamics of membrane translocation of phosphatidylserine during apoptosis detected by a monoclonal antibody. Apoptosis. 2005;10:209–17. doi: 10.1007/s10495-005-6076-5. [DOI] [PubMed] [Google Scholar]
- 54.Martin SJ, Reutelingsperger CP, McGahon AJ, Rader JA, van Schie RC, LaFace DM, et al. Early redistribution of plasma membrane phosphatidylserine is a general feature of apoptosis regardless of the initiating stimulus: inhibition by overexpression of Bcl-2 and Abl. J Exp Med. 1995;182:1545–56. doi: 10.1084/jem.182.5.1545. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Vermes I, Haanen C, Steffens-Nakken H, Reutelingsperger C. A novel assay for apoptosis. Flow cytometric detection of phosphatidylserine expression on early apoptotic cells using fluorescein labeled Annexin V. J Immunol Methods. 1995;184:39–51. doi: 10.1016/0022-1759(95)00072-I. [DOI] [PubMed] [Google Scholar]
- 56.Elmore S. Apoptosis: a review of programmed cell death. Toxicol Pathol. 2007;35:495–516. doi: 10.1080/01926230701320337. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Gibbons E, Pickett KR, Streeter MC, Warcup AO, Nelson J, Judd AM, et al. Molecular details of membrane fluidity changes during apoptosis and relationship to phospholipase A2 activity. Biochim Biophys Acta. 1828;2013:887–95. doi: 10.1016/j.bbamem.2012.08.024. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Roux C, Tripogney C, Joanne C, Bresson JL. Sperm chromatin packaging as an indicator of in-vitro fertilization rates. Gynecol Obstet Fertil. 2004;32:792–8. doi: 10.1016/S1297-9589(04)00199-7. [DOI] [PubMed] [Google Scholar]
- 59.Hou JW, Chen D, Jeyendran RS. Sperm nuclear maturity in spinal cord-injured men: evaluation by acidic aniline blue stain. Arch Phys Med Rehab. 1995;76:444–5. doi: 10.1016/S0003-9993(95)80574-5. [DOI] [PubMed] [Google Scholar]
- 60.Dadoune JP. Expression of mammalian spermatozoal nucleoproteins. Microscopy Res Tech. 2003;61:56–75. doi: 10.1002/jemt.10317. [DOI] [PubMed] [Google Scholar]
- 61.Dadoune JP, Mayaux MJ, Guihard-Moscato ML. Correlation between defects in chromatin condensation of human spermatozoa stained by aniline blue and semen characteristics. Andrologia. 1988;20:211–7. doi: 10.1111/j.1439-0272.1988.tb01058.x. [DOI] [PubMed] [Google Scholar]
- 62.Hofmann N, Hilscher B. Use of aniline blue to assess chromatin condensation inmorphologically normal spermatozoa in normal and infertile men. Hum Reprod. 1991;6:979–82. doi: 10.1093/oxfordjournals.humrep.a137472. [DOI] [PubMed] [Google Scholar]
- 63.Kim HS, Kang MJ, Kim SA, Oh SK, Kim H, Ku SY, et al. The utility of sperm DNA damage assay using toluidine blue and aniline blue staining in routine semen analysis. Clin Exp Reprod Med. 2013;40:23–8. doi: 10.5653/cerm.2013.40.1.23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Sellami A, Chakroun N, Zarrouk SB, Sellami H, Kebaili S, Rebai T, et al. Assessment of chromatin maturity in human spermatozoa: useful aniline blue assay for routine diagnosis of male infertility. Adv Urol. 2013;578631:8. doi: 10.1155/2013/578631. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.de Iuliis GN, Thomson LK, Mitchell LA, Finnie JM, Koppers AJ, Hedges A, et al. DNA damage in human spermatozoa is highly correlated with the efficiency of chromatin remodeling and the formation of 8-hydroxy-2′-deoxyguanosine, a marker of oxidative stress. Biol Reprod. 2009;81:517–24. doi: 10.1095/biolreprod.109.076836. [DOI] [PubMed] [Google Scholar]
- 66.Schulte RT, Ohl DA, Sigman M, Smith GD. Sperm DNA damage in male infertility: etiologies, assays, and outcomes. J Assist Reprod Genet. 2010;27:3–12. doi: 10.1007/s10815-009-9359-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Morel F, Mercier S, Roux C, Elmrini T, Clavequin MC, Bresson JL. Interindividual variations in the disomy frequencies of human spermatozoa and their correlation with nuclear maturity as evaluated aniline blue staining. Fertil Steril. 1998;69:1122–7. doi: 10.1016/S0015-0282(98)00058-2. [DOI] [PubMed] [Google Scholar]
- 68.Ovari L, Sati L, Stronk J, Borsos A, Ward DC, Huszar G. Double probing individual human spermatozoa: aniline blue staining for persistent histones and fluorescence in situ hybridization for aneuploidies. Fertil Steril. 2010;93:2255–61. doi: 10.1016/j.fertnstert.2009.05.033. [DOI] [PubMed] [Google Scholar]
- 69.Boue F, Blais J, Sullivan R. Surface localization of P34H, an epididymal protein, during maturation, capacitation, and acrosome reaction of human spermatozoa. Biol Reprod. 1996;54:1009–17. doi: 10.1095/biolreprod54.5.1009. [DOI] [PubMed] [Google Scholar]
- 70.Boue F, Duquenne C, Lassalle B, Lefèvre A, Finaz C. FLB1, a human protein of epididymal origin that is involved in the sperm-oocyte recognition process. Biol Reprod. 1995;52:267–8. doi: 10.1095/biolreprod52.2.267. [DOI] [PubMed] [Google Scholar]
- 71.Lefevre A, Ruis CM, Chokomian S, Duquenne C, Finaz C. Characterization and isolation of SOB2, a human sperm protein with a potential role in oocyte membrane binding. Mol Hum Reprod. 1997;3:507–16. doi: 10.1093/molehr/3.6.507. [DOI] [PubMed] [Google Scholar]
- 72.Yeung CH, Cooper TG, Schroter S, Kirchhoff C, Nieschlag E. Epididymal secretion of CD52 as measured in human seminal plasma by a fluorescence immunosaasy. Mol Hum Reprod. 1998;4:447–51. doi: 10.1093/molehr/4.5.447. [DOI] [PubMed] [Google Scholar]