Abstract
Purpose
To identify mutations in COL2A1 and COL11A1 genes and to examine the genotype-phenotype correlation in a cohort of Chinese patients with Stickler syndrome.
Methods
A total of 16 Chinese probands with Stickler syndrome were recruited, including nine with a family history of an autosomal dominant pattern and seven sporadic cases. All patients underwent full ocular and systemic examinations. Sanger sequencing was used to analyze all coding and adjacent regions of the COL2A1 and COL11A1 genes. Multiplex ligation-dependent probe amplification was performed to detect the gross indels of COL2A1 and COL11A1. Bioinformatics analysis was performed to evaluate the pathogenicity of the variants.
Results
Five mutations in COL2A1 were identified in six of 16 probands, including three novel (c.85C>T, c.3356delG, c.3401delG) mutations and two known mutations (c.1693C>T, c.2710C>T). Of the five mutations, three were truncated mutations, and the other two were missense mutations. Putative pathogenic mutations of the COL11A1 gene were absent in this cohort of patients. Gross indels were not found in COL2A1 or COL11A1 in any of the probands. High myopia was the most frequent initial ocular phenotype of Stickler syndrome. In this study, 12 Chinese probands lacked obvious systemic phenotypes.
Conclusions
In this study, three novel and two known mutations in the COL2A1 gene were identified in six of 16 Chinese patients with Stickler syndrome. This is the first study in a cohort of Chinese patients with Stickler syndrome, and the results expand the mutation spectrum of the COL2A1 gene. Analysis of the genotype-phenotype correlation showed that the early onset of high myopia with vitreous abnormalities may serve as a key indicator of Stickler syndrome, while the existence of mandibular protrusion in pediatric patients may be an efficient indicator for the absence of mutations in COL2A1 and COL11A1.
Introduction
Stickler syndrome (OMIM 108300, 604841, 184840) is a common hereditary connective tissue disorder of fibrillar collagen. Collagen alterations in patients with Stickler syndrome contribute to bilateral ophthalmological symptoms, as well as systemic effects, such as a distinctive facial appearance (orofacial features), hearing loss, and joint problems [1]. Typical ophthalmological findings of this disease include congenital high myopia, abnormal vitreous, glaucoma, cataracts, and retinal detachment. The phenotype of Stickler syndrome is complicated and develops over a lifetime. According to previous reports, approximately 55–73% of Caucasian patients with a clinical diagnosis of Stickler syndrome previously suffered retinal detachment [2-4]. Retinal detachment can lead to a high incidence of blindness and severely decreases the patient’s quality of life. Prophylactic retinopexy, such as cryotherapy, significantly reduces the risk of retinal detachment and blindness from Stickler syndrome [3,5,6]. Therefore, an early clinical diagnosis is important for improving prognosis. Nevertheless, the heterogeneous clinical phenotype may present a challenge, particularly for patients with only ocular phenotypes.
The estimated prevalence rate of Stickler syndrome is 1 in every 10,000 newborns [7]. According to the locus heterogeneity and differences in the vitreous phenotype, Stickler syndrome is primarily classified into six subtypes. Types 1 and 2 are caused by mutations in the COL2A1 (OMIM 120140) and COL11A1 (OMIM 120280) genes, respectively. It is estimated that these two genes are responsible for more than 95% of the mutations in patients with Stickler syndrome (HGMD, last updated in March 2015).
Advances in sequencing technologies may allow for more efficient diagnosis of disease by combining analyses of phenotypes and gene mutations. COL2A1 and COL11A1 are common candidate genes for Stickler syndrome, and both are related to the form of Stickler syndrome with an obvious ocular phenotype. Thus, by evaluating these two genes, patients may obtain an early diagnosis, and early prophylactic measurements may be obtained.
Several surveys of the nosological characteristics of Stickler syndrome have evaluated mutations in the COL2A1 and COL11A1 genes. These studies revealed the genotype-phenotype correlation of Caucasian patients with Stickler syndrome for types 1 and 2 [4,8-10]. Hoornaert reported that compared to mutation-negative patients, patients with a COL2A1 mutation had more frequent phenotypes of vitreous anomalies and retinal detachment. In addition, more than 90% of COL2A1 mutations are predicted to result in nonsense-mediated decay [4]. However, Liberfarb suggested that it may be difficult to predict the prevalence of certain clinical features for various inter- and intrafamilies based on the genotype [9]. Moreover, although Rose established new diagnostic criteria with high sensitivity and specificity for Stickler syndrome [10], few research studies have involved Chinese patients with Stickler syndrome with an initial diagnosis of an ocular phenotype. In this study, the COL2A1 and COL11A1 genes were analyzed in 16 Chinese probands with Stickler syndrome who presented with an initial ocular phenotype. The purpose of this study was to identify the spectrum of candidate genes and the genotype-phenotype correlation in Chinese patients with Stickler syndrome.
Methods
Patients
Sixteen unrelated Chinese patients with Stickler syndrome were recruited from the Pediatric and Genetic Clinic of Zhongshan Ophthalmic Center between 2007 and 2015. Before venous blood and clinical data were collected, written informed consent conforming to the tenets of the Declaration of Helsinki was obtained from the participants or their guardians. Studies were performed with approval from the Institutional Review Board of the Zhongshan Ophthalmic Center. Patients were diagnosed mainly according to the criteria of Stickler syndrome used by Snead and Yates [11]. The ocular phenotype was diagnosed if the following criteria were present: (1) a vitreous anomaly, (2) myopia with onset before the age of 6 years, and (3) rhegmatogenous retinal detachment or paravascular pigmented lattice degeneration. In addition, at least two of the following features had to be present: (4) hypermobility with an abnormal Beighton score, (5) sensorineural hearing defect, and (6) midfacial dysplasia. A full ophthalmic examination was performed, including a best-corrected visual acuity assessment, slit-lamp biomicroscopy, fundus photography, B-ultrasound scan, retinoscopy with cycloplegia, and the IOL Master. Systemic examination included an audiogram, a musculoskeletal examination with skeletal X-rays of the long bones, and Beighton scoring. For children who were too young to finish the audiogram, the brainstem auditory evoked potential was tested.
Mutation screening
Genomic DNA was extracted from leukocytes obtained from peripheral blood samples, as previously described [12]. After lysis of the whole blood, genomic DNA was extracted from leukocytes of the peripheral venous blood with phenol-chloroform extraction and ethanol precipitation. The COL2A1 gene (NM_001844.4) was evaluated first. If the COL2A1 gene was negative, then the COL11A1 gene (NM_080629.2) was evaluated. The primer pairs were designed using primer3 [13]; see Appendix 1 for all primers used for amplification and sequencing. The products from individual exons were sequenced using the ABI BigDye Terminator cycle sequencing kit v3.1 and an ABI 3100 Genetic Analyzer (Applied Biosystems, Foster City, CA). Then, consensus sequences were used to identify variations in the sequencing results with a sequencing program (Lasergene SeqMan II; DNASTAR, Madison, WI). Repeated sequencing was performed for every variant to confirm the result. Frequencies of variants were determined from the 1000 Genomes database and exome variant server (EVS), removing minor allele frequency (MAF) values that were greater than 0.0002. The frequency was based on the incidence of Stickler syndrome (1/10,000) and the fraction of heterozygotes in Hardy–Weinberg equilibrium. Any variation detected in the patients was further evaluated by sequencing 96 healthy individuals as a control. The PolyPhen-2 [14] and SIFT [15] online tools were used to predict the pathogenicity of missense mutations on the encoding regions. The pathogenicity of splice-site changes in the introns and synonymous variants in the exons were predicted using the Splice Site Prediction program with Neural Network (BDGP) [16]. Segregation analyses of mutations were performed for the available family members.
Multiplex ligation-dependent probe amplification
Multiplex ligation-dependent probe amplification (MLPA) assays were designed by MRC-Holland (Amsterdam, the Netherlands). There are a total of 28 COL2A1 exon-specific probes and 57 COL11A1 exon-specific probes (see Appendix 2 or the WebForm manufacturer’s website for detailed exon specific probes in each kit). The MLPA kits and cDNA reference sequences were NM_001844.4 for COL2A1 and NM_080629.2 for COL11A1. MLPA was performed according to the manufacturer’s protocol (WebForm). Analysis of the results was conducted with the GeneMarker software (Soft Genetics, State College, PA). All three MLPA probe sets were used to initially screen for duplications or deletions in COL2A1 and COL11A1 of the probands.
Results
Molecular findings
The COL2A1 gene screen identified five potential pathogenic variants in six of 16 Stickler syndrome families. Of these five mutations, three were novel (c.85C>T, c.3356delG, c.3401delG), and two were previously reported (c.1693C>T, c.2710C>T) [5,17,18]. Both missense mutations were arginine to cysteine mutations in the X position of the Gly-X-Y triplet. Putative pathogenic mutations were absent in the COL2A1 gene in the remaining ten probands. The mutation results for the COL2A1 gene are summarized in Table 1.
Table 1. Mutations in COL2A1 identified in the probands with Stickler syndrome.
| Family ID | Exon | Mutation | Amino acid change | Inheritance patterns | MAF (%) in 1000G/ EVS | Reported |
|---|---|---|---|---|---|---|
| QT1527 |
1 |
c.85C>T |
p.(Gln29*) |
SC |
NA/NA |
No |
| QT851 |
48 |
c.3356delG |
p.(Gly1119Glufs*11) |
AD |
NA/NA |
No |
| QT1589 |
48 |
c.3401delG |
p.(Gly1134Alafs*93) |
AD |
NA/NA |
No |
| QT1016
/QT1791 |
26 |
c.1693C>T |
p.(Arg565Cys) |
AD |
NA/NA |
Richards et al. 2000 [5] |
| HM470 | 41 | c.2710C>T | p.(Arg904Cys) | SC | NA/NA | Ballo et al. 1998 [17]; Nagendran et al. 2012 [18] |
Note: AD=autosomal dominant; SC=sporadic case; NA=these variants were absent from the 1000 Genome and the Exome Variant Server database.
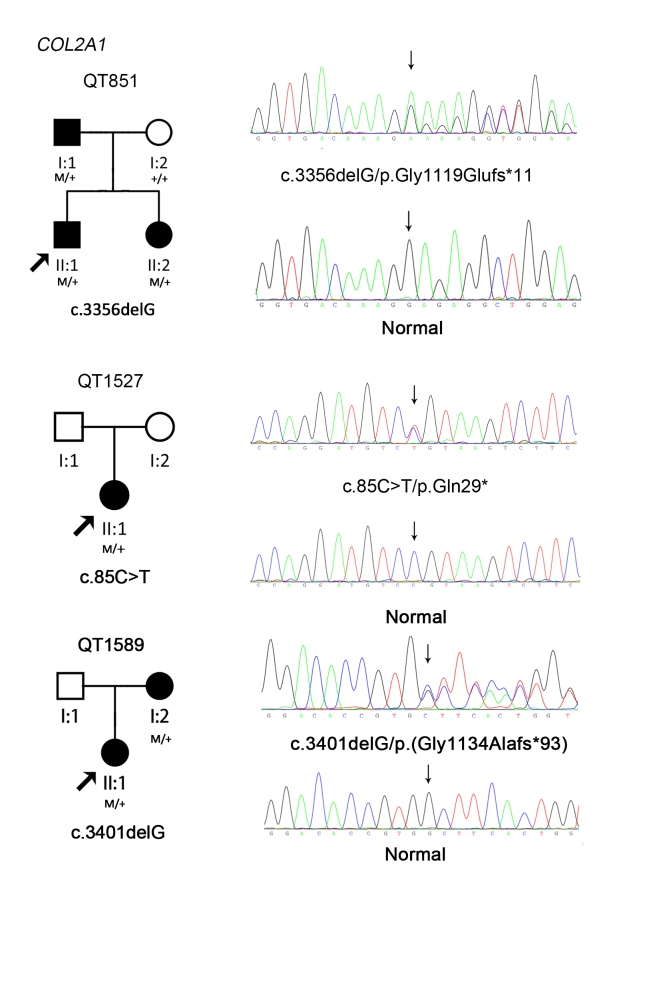
All three novel variants were premature termination codon mutations, which were considered most likely pathogenic [19]. These mutations were absent in the 1000 Genomes, EVS cohort, and 96 healthy individuals. Putative pathogenic variants were not detected in the COL11A1 gene. None of the gross indels in COL2A1 or COL11A1 was found in the 16 probands using MLPA. The sequence maps, pedigrees, and cosegregation analyses of the three families with novel mutations of COL2A1 are shown in Figure 1.
Figure 1.
The sequence maps, pedigrees, and cosegregation analyses of three families with novel mutations in COL2A1.
Clinical status
Detailed family histories and clinical data were analyzed for a total of 16 probands (four female patients and 12 male patients) with Stickler syndrome. Nine patients had family histories of autosomal dominance, and seven were sporadic cases. A total of 15 patients presented at the ophthalmic department with an initial phenotype of myopia. Five patients had developed unilateral or bilateral retinal detachment. The ages of initial diagnosis of Stickler syndrome ranged from 3 to 53 years. Monocular or binocular rhegmatogenous retinal detachment developed in 31.3% of the patients (5/16) at a median age of 11.3 years (ranging from 1.5 to 28 years old). The early onset of moderate or high myopia (<–4.00 D) was found in 93.8% of patients (15/16) before the age of 6 years old. A total of 37.5% of patients (6/16) developed cataracts before their third decade, and two developed cataracts after retinal detachment. The clinical phenotypes of the patients with observed mutations are summarized in Appendix 3. The clinical phenotypes of other probands without any mutations in COL2A1 or COL11A1 are summarized in Appendix 4.
One of the three novel mutations was a nonsense mutation, c.85C>T (p.Gln29*), in proband QT1527, and the other two novel mutations were small deletions in exon 48, c.3356delG (p.Gly1119Glufs*11) in proband QT851 and c.3401delG (p.Gly1134Alafs*93) in proband QT1589, and all three variants resulted in truncation. QT1527 was a sporadic case; this female patient had severe myopia (−13.75 D/−17.50 D) and experienced retinal detachment of the right eye at the age of 28 years. Fundus examination detected perivascular retinal degeneration that developed into a horseshoe hole. She had prominent eyes, a low nasal bridge, and micrognathia. No other systemic phenotypes were detected. QT851 was a young male patient who developed retinal detachment in both eyes before 1.5 years of age. After vitrectomy, he suffered severe cataract in both eyes, and it was difficult to observe his vitreous anomaly. His Beighton scale score was 1/1, and no arthropathy or hearing loss was detected. His father also had a history of bilateral retinal detachments, and his sister had high myopia (−5.00 D/−6.00 D) at the age of 4.5 years. All patients in the QT851 family had flat faces with micrognathia. QT1589 showed moderate myopia at age 6; this female patient showed vitreous membranous anomalies. She had no complaints about pain in joints, although the X-ray examination showed epiphyseal dysplasia of both wrists. Joint hypermobility was also present. Her Beighton scale score was 7/7. Her midfacial dysplasia was obvious, and her mother also had bilateral retinal detachments. There was no evidence of midline clefting in all patients with detected COL2A1 mutations.
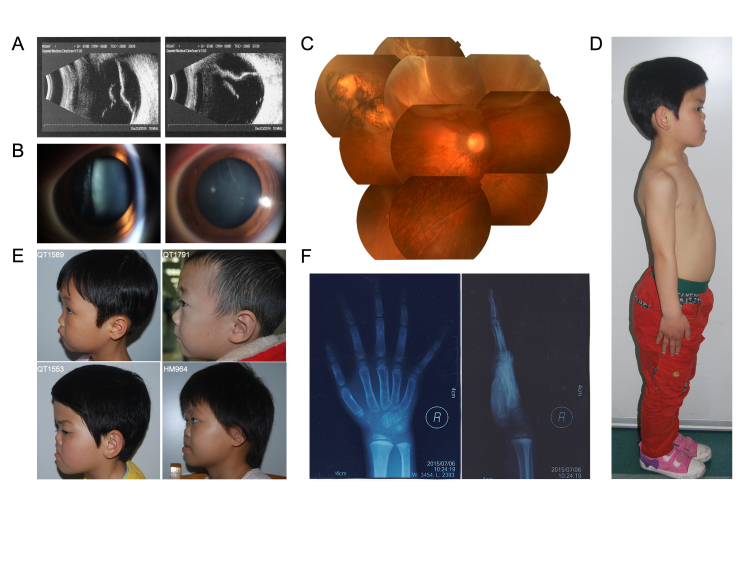
With the exception of midfacial dysplasia, only four probands had systemic phenotypes. X-rays revealed that QT1589 and HM964 had epiphyseal dysplasia in both wrists. QT1211 had had mixed hearing loss since childhood. QT1553 was a sporadic case and upon a general physical checkup was found to have a pigeon chest and a protuberant abdomen without tenderness. In the four probands with obvious systemic phenotypes, the COL2A1 mutation was detected only in QT1589. Although all pediatric patients had the facial phenotype of prominent eyes and low nasal bridges, and QT851, QT1791, and QT1589 (who had detected mutations in COL2A1) all had micrognathia, whereas no mutations in COL2A1 or COL11A1 were detected in QT1553 and HM964 who were hypognathous. Both groups corresponded to the diagnosis standards of Stickler syndrome. The typical phenotypes observed in the patients are shown in Figure 2.
Figure 2.
Typical clinical phenotypes of Chinese patients with Stickler syndrome. A: Vitreous opacities and retinal detachment in QT1547. B: Membrane vitreous abnormalities in QT1547. C: Rhegmatogenous retinal detachment and paravascular pigmented lattice degeneration in QT1547. D: The pigeon chest and protuberant abdomen of QT1553. E: The micrognathia of QT1589 and QT1791 compared to the mandibular protrusion of QT1553 and HM964. F: Bone retardation in the wrist of QT1589.
Discussion
In this study, we detected five COL2A1 mutations in six of 16 Chinese probands with Stickler syndrome, including three novel and two known mutations. All three novel mutations were premature termination codons. The two known variants were heterozygous missense mutations that involved arginine changed to cysteine in the X position of the Gly-X-Y triple helix.
The stop and frameshift mutations leading to nonsense-mediated decay are typical and common mutation types reported in type 1 Stickler syndrome [4]. The mutation of arginine to cysteine in the X position of Gly-X-Y is significant in patients with initial ocular phenotypes. Our findings differ from previous reports in which the most common missense mutation in the helix was the glycine substitution in Gly-X-Y repeating motifs of COL2A1 in Caucasians [20]. According to the Human Gene Mutation Database, 81.8% (193/236) of missense mutations of COL2A1 are substitutions of glycine (HGMD, last updated in March 2015). Glycine substitutions in Gly-X-Y repeating motifs can lead to more serious systemic phenotypes, such as chondrodysplasias and spondyloepiphyseal dysplasia in Caucasian and Chinese individuals [8,21-23]. For patients with truncations and other types of missense mutations, the systemic phenotype may be mild. In this study, three of the six patients with mutations of COL2A1 had missense mutations of arginine changed to cysteine. Nevertheless, due to the small sample size of the study, the importance of arginine changed to cysteine in Chinese patients with Stickler syndrome initially diagnosed in the ophthalmic department must be qualified pending further larger-scale studies.
According to a previous study, nearly three quarters of patients with Stickler syndrome have significant refractive error [24]. In this study, the ratio was much higher in the patients who came to the ophthalmic department. The early onset of moderate or high myopia (<–4.00 D) was found in 93.8% of patients (15/16). All eight children diagnosed under the age of 6 years had an initial symptom of myopia; of these patients, 87.5% (7/8) had bilateral severe myopia greater than −10.00 D (six patients), and QT851 had secondary bilateral retinal detachment. In comparison to the serious ocular anomalies, the systemic phenotypes were relatively mild. All children had a typical flat face with prominent eyes and a low nasal bridge. Only QT1553 had an obvious pigeon chest. QT1589 and HM964 had epiphyseal dysplasia and precocious osteoarthrosis in both wrists based on X-ray without complaints. None of the children had hearing loss. According to Sun’s study, 14 Chinese patients with mutations of COL2A1 or COL11A1 were detected with exome sequencing in 298 probands with an initial diagnosis of early-onset high myopia [25]. Several patients with Stickler syndrome had a missed diagnosis under the outstanding phenotype of myopia. Diagnosis in young children is more difficult because the phenotype evolves over the lifetime, particularly in sporadic cases. Early-onset high myopia with vitreous abnormalities may be a key indicator of Stickler syndrome, particularly for those worse than −10.00 D. The early diagnosis of Stickler syndrome is essential for its specific management, such as prophylactic cryotherapy, to protect the eyes from retinal detachment [3,5,6]. Gene detection is also useful as an auxiliary diagnosis, particularly for high-myopia children with a family history.
Compared to adults, characteristic facial phenotypes are more typical in children [9]. Interestingly, in this study, all children with a detected mutation in COL2A1 had micrognathia, while two children who had an absence of mutation in COL2A1 and COL11A1 showed a mandibular protrusion. The existence of mandibular protrusion in pediatric patients may be an efficient indicator of the absence of mutations in COL2A1 and COL11A1. However, the sample size was limited, and more studies in young Chinese patients are necessary to confirm this result.
In this study, the efficiency of mutation detection of COL2A1 (37.5%) was between the range of Liberfarb et al. (15.6%) and Hoornaert et al. (53.2%) and was limited compared to Richards et al. (96.5%) [4,8,9]. The main reason for this difference may be the lack of candidate gene selection based on the type of vitreous anomalies. In this study, all vitreous anomalies of patients were confirmed with a B-scan. However, due to a history of cataracts, vitrectomy or eyeball atrophy, and the noncooperation of children, it was difficult to clearly classify the type of vitreous anomaly in some patients. Second, the genetic screening of COL2A1 and COL11A1 was performed with Sanger sequencing and MLPA. Due to the limitations of the methodology used, large-scale genomic rearrangements could not be excluded. According to Richards et al. [26], deep intronic mutations that result in multiple transcripts can also be an important finding in type 1 and 2 disease. Moreover, mutations in COL2A1 and COL11A1 cannot be completely excluded in COL2A1- or COL11A1-negative patients. Third, the mild systemic phenotype made the classification of Stickler syndrome more difficult, and less obvious hearing loss, cleft palate, or arthropathy may lead to misdiagnosis. Thus, the accurate diagnosis of Stickler syndrome remains a challenge for ophthalmologists. In addition to these reasons, other candidate genes for Stickler syndrome may remain. To identify a new candidate gene, linkage analysis must be performed in families without detected mutations.
In summary, we analyzed the COL2A1 and COL11A1 genes in Chinese patients with Stickler syndrome and detected five different mutations, including three novel ones, which expand the spectrum of COL2A1 genes. This is the first study in a cohort of Chinese patients with Stickler syndrome, and COL2A1 is also the main candidate gene in Chinese individuals. We found that early-onset high myopia is an important phenotype in most patients with Stickler syndrome and that early diagnosis and prevention are overlooked in Chinese patients, particularly in children. The existence of mandibular protrusion in pediatric patients may be an efficient indicator of the absence of mutations in COL2A1 and COL11A1. However, there must be larger-scale studies to reveal the genotype-phenotype correlation of Asian patients with Stickler syndrome.
Acknowledgments
The authors are thankful to all patients and their family members for their participation in this study. This study was supported in part by the National Natural Science Foundation of China (81170847; to X. G).
Appendix 1. Primers used in Sanger sequencing.
To access the data, click or select the words “Appendix 1.”
Appendix 2. Exon specific probes in each kit of MLPA of COL2A1 and COL11A1.
To access the data, click or select the words “Appendix 2.”
Appendix 3. Clinical phenotypes in the six probands with COL2A1 mutation.
To access the data, click or select the words “Appendix 3.”
Appendix 4. Clinical phenotypes of the 10 patients without mutations in COL2A1 or COL11A1.
To access the data, click or select the words “Appendix 4.”
References
- 1.Stickler GB, Belau PG, Farrell FJ, Jones JD, Pugh DG, Steinberg AG, Ward LE. Hereditary Progressive Arthro-ophthalmopathy. Mayo Clin Proc. 1965;40:433–55. [PubMed] [Google Scholar]
- 2.Stickler GB, Hughes W, Houchin P. Clinical features of hereditary progressive arthro-ophthalmopathy (Stickler syndrome): a survey. Genet Med. 2001;3:192–6. doi: 10.1097/00125817-200105000-00008. [DOI] [PubMed] [Google Scholar]
- 3.Ang A, Poulson AV, Goodburn SF, Richards AJ, Scott JD, Snead MP. Retinal detachment and prophylaxis in type 1 Stickler syndrome. Ophthalmology. 2008;115:164–8. doi: 10.1016/j.ophtha.2007.03.059. [DOI] [PubMed] [Google Scholar]
- 4.Hoornaert KP, Vereecke I, Dewinter C, Rosenberg T, Beemer FA, Leroy JG, Bendix L, Bjorck E, Bonduelle M, Boute O, Cormier-Daire V, De Die-Smulders C, Dieux-Coeslier A, Dollfus H, Elting M, Green A, Guerci VI, Hennekam RC, Hilhorts-Hofstee Y, Holder M, Hoyng C, Jones KJ, Josifova D, Kaitila I, Kjaergaard S, Kroes YH, Lagerstedt K, Lees M, Lemerrer M, Magnani C, Marcelis C, Martorell L, Mathieu M, McEntagart M, Mendicino A, Morton J, Orazio G, Paquis V, Reish O, Simola KO, Smithson SF, Temple KI, Van Aken E, Van Bever Y, van den Ende J, Van Hagen JM, Zelante L, Zordania R, De Paepe A, Leroy BP, De Buyzere M, Coucke PJ, Mortier GR. Stickler syndrome caused by COL2A1 mutations: genotype-phenotype correlation in a series of 100 patients. Eur J Hum Genet. 2010;18:872–80. doi: 10.1038/ejhg.2010.23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Richards AJ, Baguley DM, Yates JR, Lane C, Nicol M, Harper PS, Scott JD, Snead MP. Variation in the vitreous phenotype of Stickler syndrome can be caused by different amino acid substitutions in the X position of the type II collagen Gly-X-Y triple helix. Am J Hum Genet. 2000;67:1083–94. doi: 10.1016/s0002-9297(07)62938-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Fincham GS, Pasea L, Carroll C, McNinch AM, Poulson AV, Richards AJ, Scott JD, Snead MP. Prevention of retinal detachment in Stickler syndrome: the Cambridge prophylactic cryotherapy protocol. Ophthalmology. 2014;121:1588–97. doi: 10.1016/j.ophtha.2014.02.022. [DOI] [PubMed] [Google Scholar]
- 7.Nowak CB. Genetics and hearing loss: a review of Stickler syndrome. J Commun Disord. 1998;31:437–53. doi: 10.1016/s0021-9924(98)00015-x. [DOI] [PubMed] [Google Scholar]
- 8.Richards AJ, McNinch A, Martin H, Oakhill K, Rai H, Waller S, Treacy B, Whittaker J, Meredith S, Poulson A, Snead MP. Stickler syndrome and the vitreous phenotype: mutations in COL2A1 and COL11A1. Hum Mutat. 2010;31:E1461–71. doi: 10.1002/humu.21257. [DOI] [PubMed] [Google Scholar]
- 9.Liberfarb RM, Levy HP, Rose PS, Wilkin DJ, Davis J, Balog JZ, Griffith AJ, Szymko-Bennett YM, Johnston JJ, Francomano CA, Tsilou E, Rubin BI. The Stickler syndrome: genotype/phenotype correlation in 10 families with Stickler syndrome resulting from seven mutations in the type II collagen gene locus COL2A1. Genet Med. 2003;5:21–7. doi: 10.1097/00125817-200301000-00004. [DOI] [PubMed] [Google Scholar]
- 10.Rose PS, Levy HP, Liberfarb RM, Davis J, Szymko-Bennett Y, Rubin BI, Tsilou E, Griffith AJ, Francomano CA. Stickler syndrome: clinical characteristics and diagnostic criteria. Am J Med Genet A. 2005;138A:199–207. doi: 10.1002/ajmg.a.30955. [DOI] [PubMed] [Google Scholar]
- 11.Snead MP, Yates JR. Clinical and Molecular genetics of Stickler syndrome. J Med Genet. 1999;36:353–9. [PMC free article] [PubMed] [Google Scholar]
- 12.Li L, Xiao X, Li S, Jia X, Wang P, Guo X, Jiao X, Zhang Q, Hejtmancik JF. Detection of variants in 15 genes in 87 unrelated Chinese patients with Leber congenital amaurosis. PLoS One. 2011;6:e19458. doi: 10.1371/journal.pone.0019458. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Rozen S, Skaletsky H. Primer3 on the WWW for general users and for biologist programmers. Methods Mol Biol. 2000;132:365–86. doi: 10.1385/1-59259-192-2:365. [DOI] [PubMed] [Google Scholar]
- 14.Adzhubei IA, Schmidt S, Peshkin L, Ramensky VE, Gerasimova A, Bork P, Kondrashov AS, Sunyaev SR. A method and server for predicting damaging missense mutations. Nat Methods. 2010;7:248–9. doi: 10.1038/nmeth0410-248. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Flanagan SE, Patch AM, Ellard S. Using SIFT and PolyPhen to predict loss-of-function and gain-of-function mutations. Genet Test Mol Biomarkers. 2010;14:533–7. doi: 10.1089/gtmb.2010.0036. [DOI] [PubMed] [Google Scholar]
- 16.Houdayer C, Dehainault C, Mattler C, Michaux D, Caux-Moncoutier V, Pages-Berhouet S, d’Enghien CD, Lauge A, Castera L, Gauthier-Villars M, Stoppa-Lyonnet D. Evaluation of in silico splice tools for decision-making in molecular diagnosis. Hum Mutat. 2008;29:975–82. doi: 10.1002/humu.20765. [DOI] [PubMed] [Google Scholar]
- 17.Ballo R, Beighton PH, Ramesar RS. Stickler-like syndrome due to a dominant negative mutation in the COL2A1 gene. Am J Med Genet. 1998;80:6–11. doi: 10.1002/(sici)1096-8628(19981102)80:1<6::aid-ajmg2>3.0.co;2-0. [DOI] [PubMed] [Google Scholar]
- 18.Nagendran S, Richards AJ, McNinch A, Sandford RN, Snead MP. Somatic mosaicism and the phenotypic expression of COL2A1 mutations. Am J Med Genet A. 2012;158A:1204–7. doi: 10.1002/ajmg.a.35303. [DOI] [PubMed] [Google Scholar]
- 19.Richards S, Aziz N, Bale S, Bick D, Das S, Gastier-Foster J, Grody WW, Hegde M, Lyon E, Spector E, Voelkerding K, Rehm HL. Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med. 2015;17:405–24. doi: 10.1038/gim.2015.30. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Kannu P, Bateman J, Savarirayan R. Clinical phenotypes associated with type II collagen mutations. J Paediatr Child Health. 2012;48:E38–43. doi: 10.1111/j.1440-1754.2010.01979.x. [DOI] [PubMed] [Google Scholar]
- 21.Richards AJ, Laidlaw M, Meredith SP, Shankar P, Poulson AV, Scott JD, Snead MP. Missense and silent mutations in COL2A1 result in Stickler syndrome but via different molecular mechanisms. Hum Mutat. 2007;28:639. doi: 10.1002/humu.9497. [DOI] [PubMed] [Google Scholar]
- 22.Zhang Z, He JW, Fu WZ, Zhang CQ, Zhang ZL. Identification of three novel mutations in the COL2A1 gene in four unrelated Chinese families with spondyloepiphyseal dysplasia congenita. Biochem Biophys Res Commun. 2011;413:504–8. doi: 10.1016/j.bbrc.2011.08.090. [DOI] [PubMed] [Google Scholar]
- 23.Cao LH, Wang L, Ji CY, Wang LB, Ma HW, Luo Y. Novel and recurrent COL2A1 mutations in Chinese patients with spondyloepiphyseal dysplasia. Genetics and molecular research. GMR. 2012;11:4130–7. doi: 10.4238/2012.September.27.1. [DOI] [PubMed] [Google Scholar]
- 24.Snead MP, McNinch AM, Poulson AV, Bearcroft P, Silverman B, Gomersall P, Parfect V, Richards AJ. Stickler syndrome, ocular-only variants and a key diagnostic role for the ophthalmologist. Eye (Lond) 2011;25:1389–400. doi: 10.1038/eye.2011.201. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Sun W, Huang L, Xu Y, Xiao X, Li S, Jia X, Gao B, Wang P, Guo X, Zhang Q. Exome Sequencing on 298 Probands With Early-Onset High Myopia: Approximately One-Fourth Show Potential Pathogenic Mutations in RetNet Genes. Invest Ophthalmol Vis Sci. 2015;56:8365–72. doi: 10.1167/iovs.15-17555. [DOI] [PubMed] [Google Scholar]
- 26.Richards AJ, McNinch A, Whittaker J, Treacy B, Oakhill K, Poulson A, Snead MP. Splicing analysis of unclassified variants in COL2A1 and COL11A1 identifies deep intronic pathogenic mutations. European journal of human genetics. Eur J Hum Genet. 2012;20:552–8. doi: 10.1038/ejhg.2011.223. [DOI] [PMC free article] [PubMed] [Google Scholar]