Abstract
Background
An outbreak of food poisoning involving 121 persons of a military establishment was investigated.
Methods
On investigation, a total of 94 persons became ill, with an attack rate of 77.7%. The symptoms included nausea, vomiting, abdominal pain, diarrhoea, weakness and fever. The mean incubation period was 2.3 hours while the median was 1.7 hours. Retrospective cohort study incriminated raita as the food item responsible for the outbreak, with a risk ratio of 21.35. Left over food was not available for laboratory analysis. There were no deaths and all affected persons recovered within 24 hours.
Result
Coagulase positive staphylococci were cultured from the vomitus and stool samples of cases. Nasal and fingernail swabs collected from food handlers also showed staphylococcal growth. The most likely cause of contamination of raita with the enterotoxin could be the staphylococci which had colonised the bodies of food handlers.
Conclusion
The aggravating factor was the storage of raita at room temperature before its consumption, which provided ideal conditions for enterotoxin formation.
Key Words: Food poisoning, Staphylococci, Food handlers
Introduction
Foodborne transmission of pathogenic and toxigenic microorganisms has been a recognised hazard for decades [1]. The food may be contaminated with infectious or toxigenic microorganisms if it is not processed and stored properly [2]. Among the pathogenic microorganisms commonly encountered in food poisoning outbreaks, enterotoxigenic staphylococci have been isolated commonly, with the United States alone reporting 1,85,000 cases annually [3]. Mori et al [4], found that 22% of food handlers were carriers of enterotoxigenic staphylococci.
The Armed Forces constitute a high risk group for food poisoning because of community kitchen practice. An outbreak of food poisoning in the catering establishment of an army unit in a large cantonment was investigated with the purpose of characterising the outbreak in terms of time, place and person besides identifying the source of illness, isolating the pathogen responsible and recommending measures for future prevention.
A total of 121 people were dining in the catering establishment, out of which 94 suffered from food poisoning on 02 Feb 2007. These 94 persons reported to the hospital soon after having lunch, with complaints of nausea, vomiting, abdominal pain and loose motions. The index case reported within 30 minutes after having lunch.
All persons had taken lunch that had been prepared from a single cookhouse. The lunch consisted of chapati, dal, rice, vegetable consisting of potato and brinjal, raita and kheer. Of those affected, 37 were seriously ill and had to be admitted. No deaths were reported and all cases were discharged on the next day by 1100 hours.
Material and Methods
A retrospective cohort study was undertaken among all persons who had taken lunch from the same catering establishment on 02 Feb 2007, regardless of presence or absence of symptoms. Historical data pertaining to the outbreak was collected using an epidemiological case sheet containing items for personal information, time at which lunch was taken, food items eaten, presenting symptoms, time of onset of symptoms, medical care provided and time required for recovery.
Assessment of the clinico-epidemiological profile of the symptomatic persons led to the incrimination of lunch as the meal responsible for this outbreak. A case for the outbreak was therefore defined as any person who had consumed lunch from the implicated cookhouse and had experienced vomiting or diarrhoea or both within 12 hours of eating lunch. Diarrhoea was defined as three or more loose stools within a 24 hour period. Incubation period was assessed. Attack rate and risk ratio (RR) with 95% confidence interval (95% CI) were calculated for each item to assess the association between consumption of individual food items and subsequent illness.
An environmental survey was undertaken to investigate into the course of food processing, food preparation and storage of the prepared food pending consumption. The left over food of the incriminated meal had been disposed off by the mess staff. To determine the possible source of contamination, samples of vomitus and stools of the cases were subjected to bacteriological culture. Nasal, throat and fingernail swabs were taken from the food handlers. Swabs were also taken from the refrigerator, floor and shelves of the cookhouse. A sample of the water used in cooking the lunch was available and was sent for bacteriological examination. Water samples from the adjacent cookhouse were also analysed. Data processing and analysis was done using EPI-Info.
Results
Of the 121 persons who reported eating lunch between 1230 hours to 1400 hours on 02 Feb 2007, 94 met the case definition for the outbreak, thus leading to an attack rate of
77.7%. The index case reported at 1305 hours on the same day. 67.0% of the cases had onset of illness within two hours after taking lunch. Almost 90% of the cases reported within the first three hours. 39.4% of the patients required hospitalisation. All cases were discharged within 22 hours of admission. No cases were reported after 02 Feb 2007. The sharp rise and fall of the epidemic curve confirms that the present outbreak was a point source outbreak (Fig. 1).
Fig. 1.
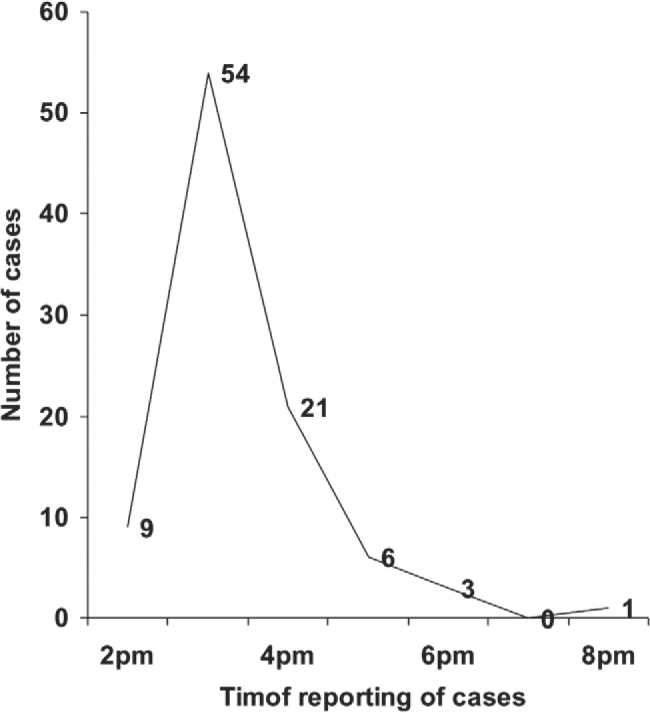
Epidemic curve
The main symptoms reported are discussed in Table 1. Highest risk of illness was associated with consumption of raita (Table 2). This association was statistically significant (RR 21.35, 95% CI 3.12-146.23).
Table 1.
Clinico-epidemiological profile of patients
| Clinico-epidemiologic features | Percentage of patients affected | Likely aetiologic agents (in order of priority) |
|---|---|---|
| Nausea | 97.9 |
|
| Vomiting | 91.5 |
|
| Abdominal pain | 81.9 |
|
| Diarrhoea | 61.7 |
|
| Fever | 6.7 |
|
| Mean incubation period | 2.3 hours | S aureus |
| Range of incubation | 30 minutes | S aureus |
| period | to 7 hours |
Table 2.
Risk of illness by food item consumed
| Food item | Ate food item |
Did not eat food item |
RR | 95% CI* | ||||
|---|---|---|---|---|---|---|---|---|
| Ill | Not Ill | % Ill | Ill | Not Ill | % Ill | |||
| Chapati | 47 | 51 | 43.5 | 6 | 7 | 46.2 | 1.04 | 0.56<RR<1.94 |
| Dal | 34 | 57 | 37.4 | 13 | 17 | 43.3 | 0.86 | 0.53<RR<1.40 |
| Rice | 43 | 41 | 51.2 | 14 | 23 | 37.8 | 1.35 | 0.85<RR<2.15 |
| Vegetable | 42 | 67 | 38.5 | 5 | 7 | 41.7 | 0.92 | 0.45<RR<1.88 |
| Raita | 78 | 17 | 82.1 | 1 | 25 | 3.9 | 21.35 | 3.12<RR<146.23 |
| Kheer | 32 | 56 | 36.4 | 18 | 15 | 54.5 | 0.67 | 0.44<RR<1.01 |
95% confidence interval
Since leftover food of the incriminated meal had not been preserved, samples of vomitus and stools of the cases were subjected to laboratory analysis, which showed colonies of coagulase positive Staphylococcus aureus (S aureus) after 24 hours incubation at 37°C. Samples were obtained from the nose and fingernails of the five food handlers (two cooks, two waiters and one masalchi) working in the cookhouse using sterile swabs. These showed growth of S aureus. Swabs taken from the refrigerator, floor and shelves of the cookhouse also showed presence of S aureus. Water samples collected from the affected cookhouse and the nearest unaffected cookhouse showed normal bacteriological counts (Table 3).
Table 3.
Results of laboratory investigations
| Sample collected | Number of Samples taken | Number of Positive samples | Remarks |
|---|---|---|---|
| Bacteriological examination of water in affected cookhouse | 02 | Nil | Normal coliform count |
| Bacteriological examination of water in adjacent cookhouse | 02 | Nil | Normal coliform count |
| Vomitus culture of cases | 12 | 11 | Coagulase positive S aureus growth |
| Stool RE of cases | 12 | 10 | 9 showed pus cells, 1 showed RBCs |
| Hanging drop preparation of stool | 12 | Nil | Negative for Vibrio |
| Stool culture of cases | 12 | 08 | Coagulase positive S aureus growth |
| Stool culture of food handlers | 05 | Nil | No growth observed |
| Nasal swab culture of food handlers | 05 | 01 | Coagulase positive S aureus in sample taken from first cook |
| Throat swab culture of food handlers | 05 | Nil | No microbial growth observed |
| Fingernail swab culture of food handlers | 05 | 02 | Coagulase positive S aureus in samples taken from masalchi and first waiter |
| Refrigerator swab culture | 02 | 02 | Coagulase positive S aureus in both samples |
| Kitchen floor swab culture | 02 | 02 | Coagulase positive S aureus in both samples |
| Kitchen shelf swab culture | 02 | 01 | Coagulase positive S aureus |
Discussion
Staphylococcal food poisoning, caused by enterotoxin-producing strains of S aureus, is one of the most common foodborne illnesses [4]. Although staphylococci are commonly found on environmental surfaces and in a wide variety of mammals and birds, humans are the primary source of staphylococcal food contamination [5]. Staphylococci are present in the nasal passage, throat, hair and skin of more than 50 percent healthy individuals and are abundant in cuts, pustules, and abscesses [6]. They thrive in protein-rich foods with a high salt content and thrive in the temperature range of 7° C to 48° C [7].
Foods that are frequently incriminated in staphylococcal food poisoning include salads, custards, milk and other dairy products [8]. In the present outbreak, the results of investigation revealed that raita was the food item responsible for occurrence of food poisoning. Persons who had consumed raita were 21 times more likely to become ill than those who did not consume raita.
Fig. 2.
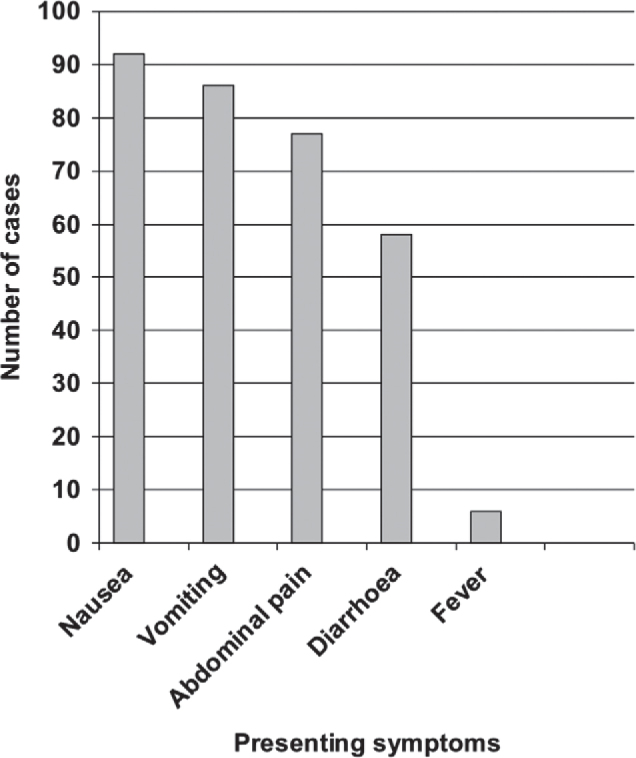
Distribution of cases according to symptoms.
Staphylococcal enterotoxins induce food poisoning when food contaminated with the enterotoxin produced by coagulase-positive staphylococci is consumed. Foods prepared by hand and stored at room temperature are frequently involved [9]. For staphylococcal food poisoning to occur, it is necessary that adequate time should have elapsed. Besides, optimum temperature must also be present for the bacteria to multiply and produce the enterotoxin [10]. Raita was prepared in the morning at 0800 hours by mixing curd with cucumber procured from the local market and stored in a steel container at room temperature until midday, when it was served. Hence, the most probable time of contamination could have been at the time of processing the curd, when manual handling could have probably contaminated the curd with the staphylococci that had colonised in the nose and body surface of the food handlers. Another possibility is that the vegetables used in making raita could have been contaminated by the staphylococci present in the immediate surroundings such as the refrigerator, the shelf or the steel container itself.
The main symptoms reported were nausea, vomiting, abdominal pain, diarrhoea, weakness and fever. The mean incubation period was 2.3 hours with a range of 30 minutes to 7 hours. Staphylococcus aureus has a short incubation period in the range of 1 to 6 hours because of the intradietetic toxin which is preformed in the contaminated food. Fever is rare in staphylococcal food poisoning as compared to salmonella food poisoning [11].
One nasal swab and two fingernail swabs of food handlers in the cookhouse showed staphylococcal growth. However, all five food handlers in the cookhouse were apparently healthy and showed no signs or symptoms of infection. Only one third of food handlers from whom staphylococci are isolated have symptoms consistent with an active staphylococcal infection [12]. Although food handlers are usually the main source of food contamination in food poisoning outbreaks, equipment and environmental surfaces can also be sources of contamination with S aureus [13], as was observed in the present outbreak in which coagulase positive S aureus was isolated from the refrigerator, floor and shelf of the cookhouse. Food handlers form an important link in the chain of any food poisoning outbreak. Hence they should be subjected to thorough clinical and laboratory evaluation to find out the probable source of infection.
Environmental factors that could have played an important role in bacterial proliferation and enterotoxin production are manual handling of curd by the mess staff and storage of the curd at room temperature for a long time without refrigeration.
All the cases recovered within 24 hours and there were no fatalities. Death from staphylococcal food poisoning is very rare, although such cases have occurred among the elderly, infants, and severely debilitated persons [14].
To reduce the incidence of staphylococcal food poisoning, potentially hazardous foods such as salads, milk and other dairy products must be prepared and served under hygienic conditions. Milk should be pasteurised or boiled and care should be taken to prevent subsequent contamination [15]. Manual handling should be restricted to a minimum and food handlers should wash their hands thoroughly before handling food, after handling garbage and after visiting the toilet. Food contact surfaces and equipment such as knives, slicers and peelers should be cleaned and sanitised. Food should be eaten promptly after cooking or refrigerated immediately at a temperature less than or equal to 5°C. Food stored under cold conditions should be re-heated to above 70°C before being served so that any staphylococci present will not be able to grow and produce the enterotoxin. Containers should be kept in all cookhouses to preserve samples of all food items prepared for a particular meal. The containers should be sealed by the duty staff and the food items preserved for 24 hours.
Conflicts of Interest
None identified
Intellectual Contribution of Authors
Study Concept : Maj MS Mustafa
Drafting & Manuscript Revision : Maj MS Mustafa, Lt Col S Jain
Statistical Analysis : Maj MS Mustafa
Study Supervision : Col VK Agrawal (Retd)
References
- 1.Foster EM. Historical overview of key issues in food safety. Emerg Infect Dis. 1997;3:417–435. doi: 10.3201/eid0304.970410. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Luiz SC, Ricardo SD, Valter RL, Maria JS. An outbreak of staphylococcal food poisoning in the municipality of Passos, Brazil. J Brazilian Archives of Biol and Technol. 2003;46:581–586. [Google Scholar]
- 3.Mead PS, Slutsker L, Dietz V. Food related illness and death in the United States. Emerg Infect Dis. 1999;5:607–625. doi: 10.3201/eid0505.990502. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Mori M, Kato E, Hamada S. Distribution of enterotoxigenic staphylococci in healthy food handlers and biological properties of isolates. Japan J Bacteriol. 1977;32:501–508. [PubMed] [Google Scholar]
- 5.Bergdoll MS. Staphylococcal food poisoning. In: Cliver DO, editor. Foodborne diseases. Academic Press; San Diego, California: 1990. pp. 85–106. [Google Scholar]
- 6.Adesium AA, Webb LA, Romain HT. Prevalence and characteristics of Staphylococcus aureus strains isolated from bulk and composite milk and cattle handlers. J Food Protec. 1998;61:629–632. doi: 10.4315/0362-028x-61.5.629. [DOI] [PubMed] [Google Scholar]
- 7.Centre for disease control and prevention: Outbreak of staphylococcal food poisoning associated with pre-cooked ham. MMWR. 1997;46:1189–1191. [PubMed] [Google Scholar]
- 8.Park K. Food poisoning. In: Park K, editor. Park's Textbook of Preventive and Social Medicine. 19th edition. M/s Banarsidas Bhanot; Jabalpur: 2007. pp. 198–199. [Google Scholar]
- 9.Min JR, Donald WS. Microbial risk assessment of styaphylococcal food poisoning in Korean kimbab. Int J Food Microbiol. 2007;116:332–338. doi: 10.1016/j.ijfoodmicro.2007.02.006. [DOI] [PubMed] [Google Scholar]
- 10.Armstrong GL, Hollingworth J, Morris JG. Bacterial foodborne disease. In: Evans AS, Brachman PS, editors. Bacterial infections in humans: Epidemiology and Control. 3rd ed. Kluwer Academic/Plenum Publishers; New York: 1998. pp. 109–138. [Google Scholar]
- 11.Panico MG, Primiano F, Nappi F. An outbreak of Salmonella enteritidis food poisoning from commercially produced cheese. Euro Surveill. 1999;4:47–48. doi: 10.2807/esm.04.04.00074-en. [DOI] [PubMed] [Google Scholar]
- 12.Holmberg SD, Blake PA. Staphylococcal food poisoning in the United States: new facts and old misconceptions. JAMA. 1984;251:487–489. [PubMed] [Google Scholar]
- 13.Yves LL, Florence B, Gautier M. Staphylococcus aureus and food poisoning. Genet Mol Res. 2003;2:63–76. [PubMed] [Google Scholar]
- 14.Noel AC, Mary TH, Andrew JL, Trudy MG, John RB. Outbreak of staphylococcal enterotoxin food poisoning. Communicable Diseases Intelligence. 2002;26:113–118. [PubMed] [Google Scholar]
- 15.Directorate General Armed Forced Medical Services . Manual of Health for the Armed Forces. Vol 1. New Delhi. 2003. Food poisoning; pp. 605–612. [Google Scholar]


