Abstract
Background:
Physical disability is common though not inevitable in older age and has direct bearing on a person’s ability to perform activities essential for self-care and independent living. Air pollution appears to increase the risk of several chronic diseases that contribute to the progression of disability.
Objective:
We evaluated long-term exposure to traffic-related air pollution (TRAP) in relation to progression in physical disability.
Methods:
We conducted our investigation within the Chicago Health and Aging Project. We measured participants’ exposures to TRAP using two surrogates: residential proximity to major roads (1993 onwards) and ambient concentrations of oxides of nitrogen (NOX; 1999 onwards), predicted via a geographic information systems-based spatiotemporal smoothing model (cross-validation R2 = 0.87) that incorporated community-based monitoring and resolved intraurban exposure gradients at a spatial scale of tens of meters. Participants’ lower-extremity physical ability was assessed every 3 years (1993–2012) via tandem stand, chair stand, and timed walking speed.
Results:
In multivariable-adjusted analyses (n = 5,708), higher long-term NOX exposure was associated with significantly faster progression in disability. Compared with the 5-year decline in physical ability score among participants in the lowest quartile of NOX exposure, decline among those in the highest exposure quartile was 1.14 units greater (95% confidence interval [CI]: –1.86, –0.42), equivalent to 3 additional years of decline among those in the lowest exposure quartile. The association was linear across the continuum of NOX exposure: per 10-ppb increment in exposure, the 5-year decline in physical ability score was 0.87 unit greater (95% CI: –1.35, –0.39). Proximity to a major road was not associated with disability progression (n = 9,994).
Conclusions:
These data join a growing body of evidence suggesting that TRAP exposures may accelerate aging-related declines in health.
Citation:
Weuve J, Kaufman JD, Szpiro AA, Curl C, Puett RC, Beck T, Evans DA, Mendes de Leon CF. 2016. Exposure to traffic-related air pollution in relation to progression in physical disability among older adults. Environ Health Perspect 124:1000–1008; http://dx.doi.org/10.1289/ehp.1510089
Introduction
Aging-related physical disability has become a critical health concern because of its high associated health care costs and because of the rapidly growing number of older Americans (Administration on Aging 2009; Federal Interagency Forum on Aging-Related Statistics 2010). Disability represents the combined impact of common, often comorbid chronic diseases and subclinical pathologic processes on a person’s ability to perform tasks and activities that are essential for self-care and independent living. Regarded as a key indicator of overall health in older adulthood (Manton et al. 1997; Pope and Tarlov 1991), disability becomes increasingly prevalent with advancing age, from ~10% among 65- to 74-year-olds in the United States to > 50% of those > 85 years old (Manton et al. 2006; Seeman et al. 2010). Disability is the primary reason for the requirement of long-term care (Kemper 1992; McKinlay et al. 1995) and accounted for $350 billion in Medicare costs in 2009 (Manton et al. 2007). Therefore, reducing the number of disability-affected years during late life is of interest because disability threatens an individual’s independence and increases both health care utilization and the burden on informal caregivers (Fries 2003).
Exposure to air pollution—particularly long-term exposure—appears to have multiple adverse health effects, including increased risks for cardiovascular and respiratory disease [Brook et al. 2010; Brunekreef et al. 2009; Committee on the Medical Effects of Air Pollutants 2006; Health Effects Institute (HEI) 2010; Pope and Dockery 2006], stroke (Brook et al. 2010; Pope and Dockery 2006; Wellenius et al. 2012b), age-related cognitive decline (Tonne et al. 2014; Weuve et al. 2012a), rheumatoid arthritis (Hart et al. 2009), and diabetes (Andersen et al. 2012; Brook et al. 2010; Chen et al. 2013; Coogan et al. 2012; Krämer et al. 2010; Pearson et al. 2010). High exposures also appear to be associated with pathophysiologic processes that contribute to these conditions (e.g., hypertension, systemic inflammation) (Brook et al. 2010; HEI 2010; Pope and Dockery 2006; Wellenius et al. 2013). Some of these health effects may be more pronounced in older adults (Fischer et al. 2003; Goldberg et al. 2000; Medina-Ramón and Schwartz 2008) in part because of the interplay between exposures and chronic disease processes (Anderson et al. 1990; Annesi-Maesano et al. 2003; Segal et al. 2002). Given that physical disability is a common functional consequence of these subclinical processes and chronic disease conditions (CDC 2009; Black and Rush 2002), it is likely that exposure to air pollution also influences physical disability at advanced ages.
We studied the relationship between long-term exposure to air pollution and the progression of physical disability in older age by combining data from participants in the Chicago Health and Aging Project (CHAP) and exposure estimates derived using a model developed for the Multi-Ethnic Study of Atherosclerosis and Air Pollution (MESA Air) Study. Our work focused on traffic-related air pollution (TRAP), a major source of exposures to toxic pollutants in urban settings that include but are not limited to nitrogen oxides, carbon monoxide, ozone, and ultrafine suspended particles (Adar and Kaufman 2007; HEI 2010). We hypothesized that physical disability would progress faster among those with greater long-term exposure to TRAP. An increasing number of people live in urban areas (United Nations, Department of Economic and Social Affairs, Population Division 2014), where TRAP is highly concentrated but is not uniformly distributed (Jerrett et al. 2005), providing impetus for determining whether TRAP exposure influences the disabling process and for studying this question in intra-urban settings.
Methods
Study Population
We conducted our investigation within CHAP, a longitudinal study of residents of a geographically defined area on the south side of Chicago, IL, who were aged 65 and older (Bienias et al. 2003; Evans et al. 2003). From 1993 to 1996, an original cohort of 6,157 participants was recruited into CHAP (79% of all eligible persons, established by community census); 4,644 newly age-eligible participants were recruited in successive cohorts. Until 2003, participants were drawn from three contiguous neighborhoods. Starting in 2003, participants were also recruited from an adjoining neighborhood. Altogether, the study area is approximately 15 mi2 (39 km2) with participants living throughout. All participants underwent triennial in-home assessments during which they completed questionnaires and underwent evaluation of their cognitive and physical function (see “Assessment of Physical Disability”); 85% of all survivors, on average, completed follow-up visits after their baseline evaluations.
Assessment of Exposure to Traffic-Related Air Pollution
We estimated participants’ exposures to TRAP using two surrogates: residential proximity to major roads and outdoor concentrations of nitrogen oxides (NOX) at each participant’s residential location, as predicted by the spatiotemporal model described below. Participants’ exposure measurements were assessed specific to the time periods during which they resided in those locations. These measurements depended on participants’ residential locations and the periods during which they resided in those locations. All available residential locations were geocoded in ArcGIS 9.3 [Environmental Systems Research Institute (ESRI), Inc.] using the Tele Atlas® Dynamap® 2000 v.16.1 road network (Boston, MA). Geocodes were calculated using side offsets of 30 ft. Automated geocoding was used for all addresses with an 80% or greater match on both spelling sensitivity and match score. Addresses that could not be automatically matched with at least 80% accuracy were matched manually. Nearly all of the locations (98%) were sufficiently complete and correct to allow geocoding to an exact location.
Exposure to ambient NOX. Our primary measure of exposure was local outdoor concentrations of NOx which serve as tracers of TRAP. For each CHAP residential location and for each 2-week interval between 1999 and 2011 (e.g., 1–14 January 1999; 15–28 January 1999; etc.), we generated predicted outdoor, ambient-source NOx concentration using spatiotemporal modeling optimized via maximum likelihood methods that were developed by MESA Air investigators (Keller et al. 2015; Sampson et al. 2011). These investigators developed a geographic information systems-based model for Chicago (Gill et al. 2011) that incorporated hundreds of variables including geographic features, roadway information, and data from a community-monitoring campaign. They calculated a suite of geographic covariates for all MESA residential locations in Chicago. These covariates included distances to a variety of features (nearest airport, railroad, rail yard, city center, major roadway, roadway intersection, port, air pollution emission source, and truck route), information about the local geography within buffers of various sizes (sum of roadway lengths; sum of truck route roadway lengths; counts of intersections; percentages of residential, commercial, and industrial land use; percentage of impervious surface cover; percentage of vegetative land cover; population density; and total air pollution emissions). Additional geographically based covariates included absolute and relative elevation, urban topography (to identify features such as “street canyons”), traffic dispersion model outputs (i.e., CALINE), and a variety of census data. The model also incorporated data from a community-monitoring campaign and included a long-term spatial mean, temporal trends with spatially varying coefficients, and a spatiotemporal residual. The mean structure was derived from the large set of geographic covariates that was reduced using partial least squares regression. Temporal trends were estimated from observed time series, and spatial smoothing methods were used to borrow strength between observations. The resulting model had a 10-fold cross-validation R 2 of 0.87 (described in detail by Keller et al. 2015). The model was finely resolved both temporally (with predictions specific to 2-week intervals) and spatially (on the order of tens of meters), allowing it to predict temporally varying intraurban exposure gradients. Figure 1 shows average predicted NOX concentrations from 1999 to 2011 in the CHAP study area, which was fully contained by the MESA Air modeling area.
Figure 1.
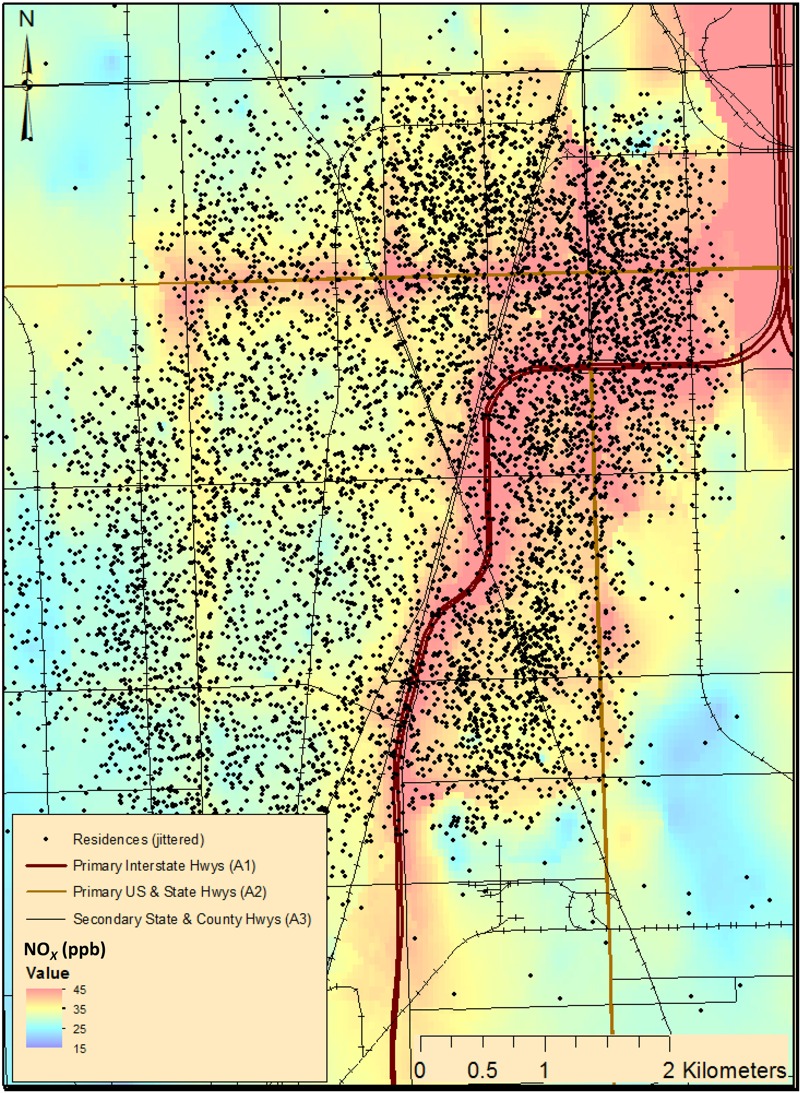
Average concentrations of oxides of nitrogen (NOX), in parts per billion, major roadways in the Chicago Health and Aging Project (CHAP) study area (1999–2011), and participants’ residential locations. Residential locations have been moved slightly (jittered) to protect participants’ confidentiality.
The location-specific 2-week NOx concentrations formed the building blocks for estimating a given CHAP participant’s long-term NOx exposure over a specific interval, as described in “Statistical Analyses.” [Although the MESA Air Study developed Chicago-based models for other ambient pollutants, including fine and coarse particulate matter (PM) (Keller et al. 2015; Zhang et al. 2014), the estimated concentrations did not vary sufficiently within the CHAP area or were unavailable for CHAP participants at the time of the present study.]
Distance to major roads. We conducted secondary analyses using residential distance to major roads. Although predicted NOX concentration is a more refined measure of TRAP exposure, the sample with road proximity estimates included 75% more participants. For each residential location, we estimated distances to different classes of road: census feature classes A1 (interstate expressways), A2 (generally state highways), and A3 (some state highways and county roads), as well as truck routes, which are a major source of exposure to diesel particles.
Assessment of Physical Disability
Every 3 years, participants underwent performance-based assessments of their basic lower-extremity functions. The Short Physical Performance Battery (SPPB) measures the participant’s balance, lower-extremity strength, and gait. It entails three progressively more difficult standing tests [standing with feet side by side, a semi-tandem stand (one foot adjacent to but a half foot in front of the other), and then a full tandem stand (one foot immediately in front of the other)], each for up to 10 sec; five repeated chair stands (rising from chair to standing position); and a timed walking test over an 8-ft course (gait speed). The SPPB has been used in a variety of epidemiologic studies of aging and has well-established reliability and validity (Freiberger et al. 2012; Guralnik et al. 1994, 2000; Mendes de Leon et al. 2002, 2005; Ostir et al. 2007). We divided scores on each of the three component tests into quintiles of performance (using cutoffs from baseline measurements), establishing an additional category for those who were unable to complete the test. Thus, scores ranged from 0 (inability to complete the test) to 5, which we summed across the three tests for a summary measure of physical function (range, 0–15). Higher scores indicated a higher level of physical ability.
Statistical Analyses
Measures of exposure. Our analyses targeted measures that reflected long-term TRAP exposure that occurred prospectively with respect to disability status.
To estimate each participant’s long-term exposure to NOX, we averaged the predicted NOX concentrations at each of her/his residential locations over the 5-year period preceding the first eligible physical performance assessment. Because the NOX model began in 1999 and both enrollment in CHAP and follow-up assessments were ongoing, we identified the first physical performance assessment and the NOX averaging period to use for these analyses following an iterative process. First, we designated a date that would be an initial placeholder for starting the NOX averaging. 1 January 1999 was the working start date for participants who were previously enrolled in CHAP or who enrolled by 1 January 2001 (2 years later), corresponding to the assumption that most noninstitutionalized participants did not move between 3-year study cycles. For the remaining participants, we used responses to a question posed in the third field cycle (2000–2002) that asked how many years they had lived in their current residential location, subtracting the number of years reported from their enrollment dates. The resulting date became the working start date, unless it fell before 1 January 1999, in which case, the latter was designated as the working start date. The working start date for all others (those who enrolled after 1 January 2001 and who did not respond to the questionnaire) was their enrollment date minus 2 years. As warranted, the 5-year NOX average accounted for multiple locations and time residing at those locations.
From each participant’s working start date, we identified the first physical performance assessment that occurred 5 or more years later. Data from this and all subsequent assessments were used in our analyses. We then recalibrated each participant’s NOX averaging period, designating the period as the 5 years before this physical performance assessment. For nearly all of these participants (94%), NOX exposure averaging began in 1999. We excluded participants who moved to a nursing home within 5 years following their averaging start date. We analyzed this measure in relation to concurrent and subsequently assessed physical performance (through 2012), analyses that included 10,911 observations from 5,708 participants.
We categorized distances to each road type as ≥ 200 m, 100–199 m, 50–99 m, and < 50 m (Karner et al. 2010); we also generated a composite measure equal to the minimum of the distances to truck routes and class A1 and A2 roads. We analyzed baseline roadway proximity (1993–2000) in relation to concurrent and to subsequently assessed physical performance (1993–2012). These analyses included 23,434 observations from 9,994 participants.
Association of TRAP exposure with physical disability. We evaluated the relationship of TRAP exposure with physical disability and disability progression by fitting multivariable-adjusted generalized estimating equation (GEE) regression models, with identity links (Zeger and Liang 1986), of repeated physical performance score. We fitted separate models for each measure of exposure, beginning with categories of the measure (for long-term NOX exposure, quartiles) and progressing to continuous measures as we established linearity in the association between exposure and physical performance. The GEE approach accounted for the correlation of within-individual repeated physical performance scores over the cycles.
All models included terms for age at the baseline physical performance assessment (continuous); sex; race (African American, white); years of education (continuous); household income (three categories and missing); baseline smoking status (current, former, never); time, in years, since the baseline physical performance assessment (continuous); and the cross-products of time with age, sex, race, education, income (distance to road only), and the air pollution exposure variable. Our principal interest was in the estimated parameter corresponding to the time-exposure cross-product, directly interpreted as the difference in the annual rate of change in the physical performance score across levels of exposure. For reporting, we converted the parameter estimate into the difference in score change over a 5-year period. The results remained unchanged with further adjustment for other factors (e.g., alcohol consumption) and cross-products of other covariates with time (data not shown). Because baseline disability and health status was likely to be a result of TRAP exposure rather than a cause of it, we did not adjust our analyses for these factors. Tests for linear trends across categories of exposure were conducted using a single term taking on the median values of each category. We tested subgroup differences in the association of exposure with decline in physical performance using three-way cross-products of the exposure measure, time, and group indicator.
Accounting for differential attrition. Attrition, particularly from mortality, is common in longitudinal studies of older adults, and participants bearing greater physical disability have an increased likelihood of being lost to follow-up (Chatfield et al. 2005; Matthews et al. 2006). If the risk factor of interest also influences attrition, the resulting differential attrition can bias estimates of the causal association between that factor and progression in disability (Hernán et al. 2004; Weuve et al. 2012b). To explore the relationship of air pollution exposure and physical performance to attrition in our data, we fitted pooled logistic regression models of continuation (the inverse of attrition) from study cycle to study cycle, following a procedure that we previously adopted and refined (Tchetgen Tchetgen et al. 2012; Weuve et al. 2012b). We fitted separate models for each of the distance to roadway and NOX measures and included a variety of time-invariant (e.g., baseline age, sex, race, education) and time-varying terms (e.g., cognitive function score, diabetes), along with the exposure of interest and a time-varying term for physical performance (i.e., score at most recent visit). Notably, these continuation models can include variables that may be plausible intermediates on the causal pathway between air pollution exposure and disability. By contrast, it would not be appropriate to include these plausible intermediate variables in models estimating the total effect of air pollution exposure on disability progression.
Of the CHAP participants in our analyses of NOX exposure, 24% died and 12% dropped out at some point after their index physical disability assessment. The risk of attrition increased with higher long-term NOX exposure [hazard ratio (HR) per 10 ppb increment, 1.14; 95% confidence interval (CI): 0.99, 1.31] and lower previous physical performance score [HR per standard deviation (sd) in score, 0.79; 95% CI: 0.74, 0.85]. (Roadway proximity was not associated with attrition.) Therefore, for analyses of NOX exposure, we used inverse probability-of-continuation-weighted regression to correct, at least in part, the possible bias introduced by the attrition related to this exposure and outcome (Cole et al. 2005; Hernán et al. 2000; Tchetgen Tchetgen et al. 2012; Weuve et al. 2012b). For each observation in our GEE model of NOX exposure and physical performance, we computed stabilized weights, as previously described (Weuve et al. 2012b), as the inverse of the predicted probability of continuation multiplied by the predicted probability of continuation from a model containing only the time-invariant variables of the GEE model.
Sensitivity analyses. We performed several analyses to assess the robustness of our findings. For NOX, these included restricting analyses to participants who did not move over the course of the exposure averaging period; exploring the potential influence of very small or large continuation weights on the results by using weights truncated at the 0.5th and 99.5th percentiles of the weight distribution; and repeating analyses using NOX averages computed over 1, 2, 3, and 4 years. Averaging exposures over the 5 years before disability more accurately characterizes the historic long-term exposures hypothesized to affect the course of physical disability than does averaging over shorter time periods. However, this approach limits the amount of disability data included in the analyses: the number of observations and participants included in these alternative analyses ranged from 12,097 observations from 6,041 participants (4-year NOX average) to 16,479 observations from 7,291 participants (1-year NOX average).
Sensitivity analyses applied to distance to road included exploring the alternative A3 road proximity categories ≥ 500 m, 251–499 m, 101–250 m, and ≤ 100 m (Karner et al. 2010; Wellenius et al. 2012a); analyzing the composite variable, in which we classified participants as living “near a major road” if their residence was < 100 m from an A1 or A2 road, < 100 m from a truck route, or < 50 m from an A3 road; and restricting analyses to the subgroup of participants who were in the analyses of 5-year NOX exposure.
Sensitivity analyses of both TRAP measures included differences in association by baseline smoking status, race, and adjustment for a composite measure of area-based socioeconomic status (SES) (see Supplemental Material, “Computation of area-level socioeconomic status”).
All CHAP participants provided their written informed consent to engage in the CHAP protocols. This study was approved by the Institutional Review Boards of Rush University Medical Center and the University of Washington.
Results
Exposure to NOX
Long-term exposure to NOX, as indicated by predicted concentrations averaged over 5 years, ranged from 20.7 to 56.0 ppb, with a mean of 39.7 ppb (standard deviation, 5.8 ppb). NOX exposure was markedly higher, on average, among participants who were African American (versus white), and who had less formal education and lower household incomes (Table 1). Participants living in areas with higher NOX concentrations were also less likely to rate their health as excellent.
Table 1.
Participant characteristics,a by quartile of long-term exposure to oxides of nitrogen.
| Characteristic | Overallc n = 5,708 | Quartile of long-termb NOX exposure | p-Value | |||
|---|---|---|---|---|---|---|
| Lowest (20.7–36.2 ppb) n = 1,431 | Second (36.3–39.6 ppb) n = 1,435 | Third (39.7–43.7 ppb) n = 1,423 | Highest (43.8–56.0 ppb) n = 1,419 | |||
| Age, years (mean ± SD) | 75.9 ± 7.1 | 76.8 ± 8.0 | 76.2 ± 7.2 | 75.4 ± 6.8 | 75.2 ± 6.3 | < 0.0001 |
| Male, % | 2,071 (36) | 36 | 39 | 34 | 37 | 0.05 |
| Race, % | < 0.0001 | |||||
| African American | 3,668 (64) | 35 | 41 | 83 | 98 | |
| White | 2,040 (36) | 65 | 59 | 17 | 2 | |
| Education, years (mean ± SD) | 12.8 ± 3.2 | 14.0 ± 3.4 | 13.1 ± 3.1 | 12.1 ± 3.1 | 11.9 ± 3.3 | < 0.0001 |
| Household income, %d | < 0.0001 | |||||
| < 15,000 USD | 1,149 (20) | 13 | 15 | 26 | 27 | |
| 15,000–29,999 USD | 2,129 (37) | 26 | 33 | 43 | 48 | |
| ≥ 30,000 USD | 2,310 (40) | 59 | 50 | 29 | 24 | |
| Missing | 120 (2) | 3 | 2 | 2 | 1 | |
| Self-rated health, %d | < 0.0001 | |||||
| Excellent | 1,201 (21) | 28 | 23 | 18 | 15 | |
| Good | 2,828 (50) | 50 | 51 | 48 | 50 | |
| Fair | 1,400 (25) | 19 | 21 | 29 | 29 | |
| Poor | 275 (5) | 4 | 5 | 6 | 5 | |
| Global cognitive score, standard units (mean ± SD) | 0.3 ± 0.8 | 0.4 ± 0.7 | 0.4 ± 0.7 | 0.2 ± 0.8 | 0.2 ± 0.8 | < 0.0001 |
| Social network score, median (iqr)e | 6 (7) | 6 (8) | 6 (7) | 6 (6) | 6 (6) | < 0.0001 |
| Walks > 3 hr per week, % | 1,030 (18) | 19 | 20 | 16 | 17 | 0.01 |
| Smoking status, %d | 0.004 | |||||
| Never | 2,673 (47) | 48 | 46 | 47 | 46 | |
| Former | 2,460 (43) | 44 | 45 | 41 | 42 | |
| Current | 575 (10) | 8 | 9 | 12 | 11 | |
| Alcohol intake, %d | < 0.0001 | |||||
| None | 3,693 (65) | 56 | 60 | 70 | 72 | |
| Moderate | 1,698 (30) | 36 | 33 | 26 | 24 | |
| Heavy | 315 (6) | 8 | 7 | 4 | 4 | |
| Systolic blood pressure, mmHg (mean ± SDe) | 135 ± 20 | 134 ± 21 | 135 ± 19 | 136 ± 19 | 136 ± 19 | 0.2 |
| Diastolic blood pressure, mmHg (mean ± SDe) | 77 ± 11 | 78 ± 12 | 76 ± 11 | 78 ± 11 | 77 ± 11 | 0.005 |
| Self-reported history of disease | ||||||
| Hypertension, % | 3,905 (68) | 65 | 62 | 73 | 73 | < 0.0001 |
| Cardiovascular disease, % | 818 (14) | 14 | 15 | 15 | 14 | 0.6 |
| Stroke, % | 648 (11) | 9 | 11 | 13 | 12 | 0.007 |
| Cancer, % | 1,308 (23) | 28 | 23 | 22 | 19 | < 0.0001 |
| Minimum distance to Class A3 road, %d | < 0.0001 | |||||
| ≤ 50 m | 640 (11) | 5 | 8 | 15 | 16 | |
| 50 m–99 m | 601 (11) | 7 | 10 | 14 | 12 | |
| 100 m–199 m | 1,372 (24) | 24 | 26 | 24 | 22 | |
| ≥ 200 m | 2,095 (54) | 64 | 56 | 47 | 49 | |
| Near busy roadf, % | 1,018 (18) | 8 | 11 | 20 | 33 | < 0.0001 |
| Moved over the course of follow-up, % | 252 (4) | 5 | 5 | 4 | 3 | 0.01 |
| Physical performance score (mean ± SD) | 9.5 ± 4.1 | 9.8 ± 4.1 | 10.0 ± 4.1 | 9.1 ± 4.1 | 9.0 ± 4.0 | |
| Abbreviations: iqr, interquartile range; NOX, oxides of nitrogen; SD, standard deviation; USD, U.S. dollars. aUnless specified, all characteristics reflect baseline values, that is, the values at the first assessment used in analyses of 5-year average NOX exposure. bPredicted exposures averaged over 5 years. cWhere percentages are listed in the “Overall” column, counts are also provided [n (%)]. dSome columns do not sum to 100% because of rounding. eData on self-rated health, social network score, walking, alcohol intake, blood pressure, and self-reported history of the four chronic conditions were missing for a small percentage of participants (< 2%). Values shown reflect non-missing responses. Data on these characteristics were not used in the association models. fNear busy road: < 100 m from A1, A2, or truck route, or < 50 m from A3. | ||||||
Unless otherwise specified, all NOX results presented below are from weighted analyses. In unadjusted analyses, irrespective of weighting, higher long-term NOX exposure was associated with worse physical performance at baseline (Table 1; see Figure S1 left). However, this pattern was reversed with multivariable adjustment. For example, baseline physical performance scores were, on average, 0.26 unit higher per 10-ppb increment in NOX exposure (95% CI: 0.06, 0.45). Nonetheless, the higher baseline scores associated with NOX exposure were eclipsed over time by the faster rate of decline in performance among those with higher exposures (see Figure S2). Specifically, decline in physical performance was significantly more rapid among participants exposed to higher long-term concentrations of NOX (p trend = 0.002; Table 2; see Figure S2). Compared with participants in the lowest exposure quartile, performance among participants in the highest exposure quartile declined by 1.14 units (95% CI: –1.86, –0.42) more per 5-year interval. With NOX exposure modeled as a continuous variable, a 10-ppb increment in exposure corresponded to a 0.87-unit excess decline in performance (95% CI: –1.35, –0.39). Placing the magnitude of these estimates in context, those in the highest NOX quartile declined in performance over a 5-year interval to the same degree that those in the lowest quartile declined over an 8-year interval. Likewise, comparing participants 10 ppb apart in exposure, the 5-year decline in physical performance in the more highly exposed individuals was equivalent to the expected 7-year decline in the less-exposed individuals.
Table 2.
Adjusteda differences [and 95% confidence interval (CI)] in 5-year change in physical performance by exposure to traffic-related air pollution.
| Exposure measure | Difference in 5-year change in physical performance score (95% CI) | |
|---|---|---|
| Long-term exposure to oxides of nitrogen (NOX)b (n = 5,708) | ||
| Quartile of long-term NOX exposure | ||
| Lowest (20.7–36.2 ppb) | 0.00 | Reference |
| 2nd (36.3–39.6 ppb) | –0.49 | (–1.06, 0.08) |
| 3rd (39.7–43.7 ppb) | –0.52 | (–1.13, 0.10) |
| Highest (43.8–56.0 ppb) | –1.14 | (–1.86, –0.42) |
| ptrendc = 0.002 | ||
| Per 10-ppb increment in long-term NOX exposure | –0.87 | (–1.35, –0.39) |
| Residential distance to road (n = 9,994) | ||
| Minimum distance to nearest truck route or A1 or A2 road | ||
| ≥ 200 m | 0.00 | Reference |
| 100–199 m | 0.20 | (0.02, 0.38) |
| 50–99 m | –0.02 | (–0.28, 0.23) |
| < 50 m | –0.17 | (–0.62, 0.28) |
| ptrendc = 0.2 | ||
| Distance to nearest A3 road | ||
| ≥ 200 m | 0.00 | Reference |
| 100–199 m | –0.24 | (–0.38, –0.10) |
| 50–99 m | –0.12 | (–0.32, 0.08) |
| < 50 m | –0.04 | (–0.25, 0.16) |
| ptrendc = 0.02 | ||
| NOX, oxides of nitrogen aAdjusted for age, sex, race, education, income, and smoking status. bPredicted exposures averaged over 5 years. cTrend p-values computed from models containing a term that took on the median values of each category. | ||
Sensitivity analyses. Results were smaller in magnitude when we truncated the analytical weights (Figure 2; see Table S1). Unweighted results were smaller still but remained statistically significant. From analyses in which we averaged NOX exposures over 4 years and in which the earliest disability assessment included was in 2003, the results were consistent with the results from analyses of 5-year average NOX exposures. Estimated associations using shorter averaging intervals were discernibly smaller in magnitude and, with respect to 2- and 1-year exposure averages, were not statistically significant. Results among participants who did not move and results adjusted for the composite measure of area-level SES were similar to those from the primary analyses. The results did not vary substantially by race or by smoking status (Figure 2).
Figure 2.
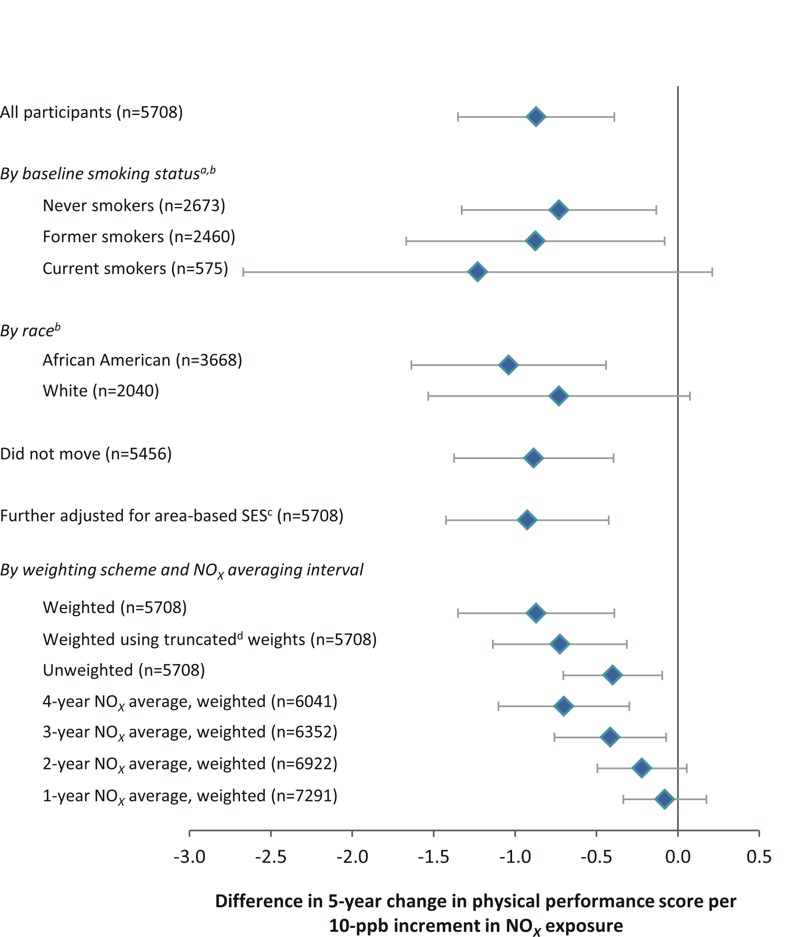
Adjusted difference in 5-year change in physical performance score per 10-ppb increment in long-term exposure to oxides of nitrogen (NOX): subgroup and sensitivity analyses. Estimates are adjusted for age, sex, race (as appropriate), education, income, and smoking status. Predicted exposures are averaged over 5 years, unless another interval is specified. aSmoking status for each participant is defined at the time of the first physical performance assessment used in the analyses of long-term NOX exposure. bInteraction p-values for differences in the NOX-performance change association by smoking and race are 0.7 and 0.5, respectively. cArea-based socioeconomic status (SES) refers to the composite area-based measure of SES. dTruncated weights refer to analyses with extreme weights truncated to the lowest 0.5 percentile and highest 99.5 percentile.
Distance to Road
Residential distances to road types were distributed most extensively across categories of A3 road (see Table S2): approximately half of the participants lived < 200 m from the nearest A3 road, and 9% overall lived < 50 m away. Participants who lived closer to major roads, including A3 roads, were more likely to be African American (e.g., 73% of those < 50 m from an A3 road were African American, compared with 61% of those living ≥ 200 m from an A3 road) and of lower socioeconomic status, indicated by fewer years of education and lower household income (see Table S3).
Compared with ≥ 200 m to A3 road, shorter distance was associated with significantly worse physical performance at baseline in both unadjusted (see Table S3) and multivariable-adjusted analyses (see Figure S3; p trend = 0.004). With proximity to A3 roadway < 200 m, performance declined more rapidly over time (Table 2), but these findings were small in magnitude. Moreover, although the linear trend p-value was 0.02, those living at 100- to 199-m distances declined an excess 0.24 unit (95% CI: –0.38, –0.10) more in performance over 5 years than those living at ≥ 200 m distances, whereas those living at < 50 m distances declined at nearly the same rate as those living at ≥ 200 m distances. Minimum distance to truck route/A1 road/A2 road was not consistently associated with baseline physical performance (results not shown) or longitudinal deterioration in performance (Table 2).
Sensitivity analyses. The results were similar under the alternative scheme for classifying distance to A3 road, with closer proximity associated with significantly worse physical performance at baseline (see Figure S3; p trend = 0.01). However, proximity to A3 road, using these alternative categories, was not associated with longitudinal decline in performance (see Table S1). As of enrollment, 16% of participants lived “near a busy road” (see Table S2). This status was not associated with baseline physical performance (results not shown) or with longitudinal decline in performance (see Table S1).
Restricting analyses to the 5,708 participants who were in the analyses of 5-year NOX exposure, we analyzed residential distance to A3 road at the time at which their 5-year NOX averaging began (1999 for most). Compared with the primary analyses, these analyses revealed a less-consistent association of distance to A3 roadway with baseline physical disability, but a clearer gradient in disability progression was observed with closer proximity to A3 road (p trend = 0.05; see Table S1). These results are consistent with the findings on NOX exposure in the same population.
The results did not vary significantly by smoking status or race (results not shown). Further adjustment for area-based SES modestly attenuated the association of distance to A3 roadway with baseline physical performance (results not shown).
Discussion
In this large study of urban-dwelling older adults, physical disability progressed more rapidly among those with higher long-term exposure to ambient NOX, a measure of exposure to TRAP. Comorbid conditions are extremely common among older adults, and studies of air pollution and single-system endpoints, such as cardiovascular and respiratory disease, may overlook the aggregate effects of air pollution exposure on multiple organ systems in this population. Evidence supporting such a relationship could motivate the use of exposure-reduction policies to reduce the burden of physical disability on the population, particularly among African Americans, who, on average, experience higher air pollutant exposures than do whites (Lopez 2002). Our study assessed physical disabilities that predict an individual’s subsequent independence. In contrast to performance-based assessments of physical disability, activities-of-daily-living (ADL) disability entails self-reported difficulty in performing specific tasks. Factors other than physical disability, such as depressive symptoms and cognitive status, can influence ADL reporting. Moreover, performance-based assessments can detect lower-extremity deficits even in persons without an ADL disability (den Ouden et al. 2011). This subclinical detection capacity is relevant to characterizing the full range of air pollution’s effects on the health of older adults: persons with chronic health conditions that are associated with air pollution exposure [e.g., lung and heart disease (Eisner et al. 2008; Khan et al. 2013)] perform substantially worse on these tests than those without such chronic conditions, and comorbidities worsen performance further (see, for example, Cesari et al. 2006). However, to a more subtle but nevertheless detectable extent, performance is also worse among persons who are free of clinical disease but who have indications of subclinical pathologies, such as inflammation or atherosclerosis (Brinkley et al. 2009; den Ouden et al. 2014).
Our study is, to our knowledge, the first to prospectively evaluate the relationship between long-term exposure to air pollution and progression in physical disability. Previous epidemiologic studies of air pollution exposure and disability were cross-sectional, evaluated acute effects of short-term exposures, used single self-reported measures of disability and exposures measured at the level of the community, or did not focus on older adults. In cross-sectional data from adults representative of the U.S. population in 1976–1981, higher exposure to ambient fine PM, estimated at the metropolitan level, was associated with more restricted activity days among adults 18–65 years of age (Ostro 1987). Similar findings emerged from a time series study of adults (mean age, 43 years) in Toronto, Canada, from 1994 to 1999, when overall pollutant exposures were much lower than in the period studied in the Ostro (1987) study: higher levels of short-term exposure to fine PM and carbon monoxide were both associated with increased disability days (Stieb et al. 2002). The only previous study among older adults was set in China, where high community-level ambient air pollution was associated with having at least one ADL disability 7 years after the period during which the exposure was assessed (Zeng et al. 2010).
Our study introduces several critical strengths to advance the field, notably: we provide individual-level estimates of long-term exposure and performance-based assessments of the trajectory of physical disability, and we account for possible bias from selective attrition. However, several limitations merit attention. First, as necessitated by research on the health effects of exposure to long-term air pollution, our study follows an observational design, making it susceptible to bias from confounding. Confounding by socioeconomic disadvantage is a particular concern because indicators such as education and income track inversely with exposure. The CHAP population is well characterized in this regard, and we took several approaches to adjust for socioeconomic disadvantage, including the use of cross-product terms between several socioeconomic indices and time. In sensitivity analyses, further adjustment for area-based socioeconomic disadvantage did not attenuate the association of NOX exposure with decline in physical performance (Figure 2). Finally, compared with unadjusted and unweighted results, weighted multivariable-adjusted results actually indicated a more deleterious association of long-term NOX exposure with this outcome (see Figure S1).
Second, the exposure measurements were based on participants’ residential locations and thus were limited by the assumption that participants spent most of their time at home, although this assumption may be reasonable for older individuals (Spalt et al. 2015). Personal air monitoring devices are impractical for long-term exposures in large epidemiologic studies. By contrast, GIS-based spatiotemporal models offer the ability to estimate individual exposures for thousands of participants, customized to time period. The MESA Air NOX exposure model, developed specifically for Chicago, accounts for small-scale variations in exposure from traffic and nontraffic sources, allowing us to distinguish among different exposure levels over space and time within the study area (Cohen et al. 2009; Keller et al. 2015; Sampson et al. 2011). We took several steps toward making the NOX measures optimal reflections of the long-term exposures that might influence disability. We first averaged predicted exposures over the 5 years before the disability assessment, offering gains in precision and accuracy beyond the use of exposure measures averaged over shorter periods or periods encompassing disability follow-up. Next, to avoid reverse causation bias, we excluded participants living in nursing homes. In such cases, estimated exposures could result from, rather than lead to, disability.
Third, the use of inverse probability-of-continuation weights addressed selection bias in the estimates of change in physical performance, but it had no bearing on bias from differential selection into the study and by extension, no bearing on estimates of baseline differences in physical performance. Assuming that selection into the study fell under the same influences as continuation in the study, estimated associations of TRAP exposure with baseline physical performance would be biased upward (even in the presence of no relationship), possibly explaining the observation of better baseline function with higher NOX exposure.
The extent to which our results might generalize to other settings is unclear. For example, the study population comprises African American and white older residents of a large city in the midwestern United States. Coexposures and other factors that may influence susceptibility to TRAP’s effects on disability may be present (or lacking) in other populations. Moreover, outdoor NO2 concentrations and NOX emissions have been falling steadily in the United States [U.S. Environmental Protection Agency (EPA) 2013]. Nonetheless, associations of air pollutant exposures with other health outcomes, such as cardiopulmonary mortality, have been remarkably robust across space and time, and some evidence hints at the lack of an effect threshold for certain outcomes [e.g., stroke (Stafoggia et al. 2014; Wellenius et al. 2012b), lung cancer mortality (Pope et al. 2011), and total mortality (Correia et al. 2013)] or an exposure–response association that is steeper at lower levels of exposure for other outcomes [e.g., cardiovascular mortality (Pope et al. 2011)]. Moreover, ambient pollutant concentrations in some regions of the world far exceed those in the CHAP study area, and effect modification notwithstanding, our results may be pertinent to populations in those areas.
Finally, unlike long-term NOX exposure, road proximity was not consistently associated with progression in physical disability. Distance to road has been associated with several adverse health outcomes, notably incident cardiovascular disease and mortality (Adar and Kaufman 2007), but other studies that have detected associations between ambient pollutant concentrations and health outcomes have not detected comparable associations for residential distance to road [e.g., (Brunekreef et al. 2009)]. In the context of CHAP, data from thousands more participants and several more years of follow-up were available for the analysis of road proximity than for NOX exposure, but it is possible that any increase in statistical power offered by the road proximity measures was offset by their coarseness. For example, unlike NOX estimates, these measures do not account for traffic counts or differentiate between exposures emanating from a single road and exposures from two or more nearby roads. In addition to being conducted in different populations that were born approximately a decade apart, the primary analyses of distance to road and those of NOX exposure entailed exposures assessed in different periods (as early as 1993 vs. 1999–2004 for most) and outcome data beginning at different time points (as early as 1993 vs. 2004). When we restricted the analysis of A3 roadway proximity to the 5,708 participants and 10,911 observations from the NOX analyses, progressively closer proximity was associated with significantly worse progression in disability (see Table S1), consistent with the corresponding NOX association and supporting the possibility that the populations used in the primary analyses and/or their corresponding measurements may have differed in substantial ways.
Conclusion
In conclusion, higher long-term exposure to ambient NOX was associated with a greater decline in physical function among older adults living in Chicago, Illinois. This association was detected in a population with TRAP exposures consistent with current levels in some areas of the United States and in many areas worldwide. Therefore, if our findings are confirmed by other studies, air pollution reduction may be a means for reducing the population burden of physical disability and dependence.
Supplemental Material
Acknowledgments
The authors are grateful to G. Dombrowski, A. Gassett, A. Ho, L. Piepmeier, and B. Yu for their expert contributions to the preparation and transfer of the exposure data.
Footnotes
This study was supported by the National Institute for Environmental Health Sciences of the National Institutes of Health (NIEHS/NIH) under awards R21ES020404 (J.W.), K24ES013195 (J.D.K.), and R01ES020871 (A.A.S.); the National Institute on Aging of the NIH (NIA/NIH) under award AG011101 (D.A.E.); and the U.S. Environmental Protection Agency (EPA) under award RD-83479601-0 (A.A.S.) and STAR research assistance agreement RD-831697 (MESA Air; J.D.K.).
The content, findings, and conclusions of this report are solely the responsibility of the authors and do not necessarily represent the official views of the NIH or the U.S. EPA.
J.W. serves as a consultant to the Alzheimer’s Association, Biogen, Inc. and the AlzRisk Project (http://www.alzrisk.org), which receives funding from Fidelity Biosciences and from the Alzheimer’s Drug Discovery Foundation. The work entails interpretation of published dementia epidemiology studies.
The authors declare they have no actual or potential competing financial interests.
References
- Adar SD, Kaufman JD. Cardiovascular disease and air pollutants: evaluating and improving epidemiological data implicating traffic exposure. Inhal Toxicol. 2007;19(suppl 1):135–149. doi: 10.1080/08958370701496012. [DOI] [PubMed] [Google Scholar]
- Administration on Aging. Washington, DC: U.S. Department of Health and Human Services; 2009. A Profile of Older Americans: 2009. Available: http://www.aoa.gov/Aging_Statistics/Profile/2009/docs/2009profile_508.pdf [accessed 15 September 2014] [Google Scholar]
- Andersen ZJ, Raaschou-Nielsen O, Ketzel M, Jensen SS, Hvidberg M, Loft S, et al. Diabetes incidence and long-term exposure to air pollution: a cohort study. Diabetes Care. 2012;35(1):92–98. doi: 10.2337/dc11-1155. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Anderson PJ, Wilson JD, Hiller FC. Respiratory tract deposition of ultrafine particles in subjects with obstructive or restrictive lung disease. Chest. 1990;97(5):1115–1120. doi: 10.1378/chest.97.5.1115. [DOI] [PubMed] [Google Scholar]
- Annesi-Maesano I, Agabiti N, Pistelli R, Couilliot MF, Forastiere F. Subpopulations at increased risk of adverse health outcomes from air pollution. Eur Respir J Suppl. 2003;40:57s–63s. doi: 10.1183/09031936.03.00402103. [DOI] [PubMed] [Google Scholar]
- Bienias JL, Beckett LA, Bennett DA, Wilson RS, Evans DA. Design of the Chicago Health and Aging Project (CHAP). J Alzheimers Dis. 2003;5(5):349–355. doi: 10.3233/jad-2003-5501. [DOI] [PubMed] [Google Scholar]
- Black SA, Rush RD. Cognitive and functional decline in adults aged 75 and older. J Am Geriatr Soc. 2002;50(12):1978–1986. doi: 10.1046/j.1532-5415.2002.50609.x. [DOI] [PubMed] [Google Scholar]
- Brinkley TE, Leng X, Miller ME, Kitzman DW, Pahor M, Berry MJ, et al. Chronic inflammation is associated with low physical function in older adults across multiple comorbidities. J Gerontol A Biol Sci Med Sci. 2009;64(4):455–461. doi: 10.1093/gerona/gln038. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Brook RD, Rajagopalan S, Pope CA, III, Brook JR, Bhatnagar A, Diez-Roux AV, et al. Particulate matter air pollution and cardiovascular disease: an update to the scientific statement from the American Heart Association. Circulation. 2010;121(21):2331–2378. doi: 10.1161/CIR.0b013e3181dbece1. [DOI] [PubMed] [Google Scholar]
- Brunekreef B, Beelen R, Hoek G, Schouten L, Bausch-Goldbohm S, Fischer P, et al. Effects of long-term exposure to traffic-related air pollution on respiratory and cardiovascular mortality in the Netherlands: the NLCS-AIR study. Res Rep Health Eff Inst. 2009;139:5–71. [PubMed] [Google Scholar]
- CDC (Centers for Disease Control and Prevention) Prevalence and most common causes of disability among adults—United States, 2005. MMWR Morb Mortal Wkly Rep. 2009;58(16):421–426. [PubMed] [Google Scholar]
- Cesari M, Onder G, Russo A, Zamboni V, Barillaro C, Ferrucci L, et al. Comorbidity and physical function: results from the aging and longevity study in the Sirente geographic area (ilSIRENTE study). Gerontology. 2006;52(1):24–32. doi: 10.1159/000089822. [DOI] [PubMed] [Google Scholar]
- Chatfield MD, Brayne CE, Matthews FE. A systematic literature review of attrition between waves in longitudinal studies in the elderly shows a consistent pattern of dropout between differing studies. J Clin Epidemiol. 2005;58(1):13–19. doi: 10.1016/j.jclinepi.2004.05.006. [DOI] [PubMed] [Google Scholar]
- Chen H, Burnett RT, Kwong JC, Villeneuve PJ, Goldberg MS, Brook RD, et al. 2013. Risk of incident diabetes in relation to long-term exposure to fine particulate matter in Ontario, Canada. Environ Health Perspect 121 804 810, doi: 10.1289/ehp.1205958 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cohen MA, Adar SD, Allen RW, Avol E, Curl CL, Gould T, et al. Approach to estimating participant pollutant exposures in the Multi-Ethnic Study of Atherosclerosis and Air Pollution (MESA Air). Environ Sci Technol. 2009;43(13):4687–4693. doi: 10.1021/es8030837. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cole SR, Hernán MA, Margolick JB, Cohen MH, Robins JM. Marginal structural models for estimating the effect of highly active antiretroviral therapy initiation on CD4 cell count. Am J Epidemiol. 2005;162(5):471–478. doi: 10.1093/aje/kwi216. [DOI] [PubMed] [Google Scholar]
- Committee on the Medical Effects of Air Pollutants. London: Public Health England; 2006. Cardiovascular Disease and Air Pollution. Available: https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/304668/COMEAP_cardiovascular_disease_and_air_pollution.pdf [accessed 15 September 2014] [Google Scholar]
- Coogan PF, White LF, Jerrett M, Brook RD, Su JG, Seto E, et al. Air pollution and incidence of hypertension and diabetes mellitus in black women living in Los Angeles. Circulation. 2012;125(6):767–772. doi: 10.1161/CIRCULATIONAHA.111.052753. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Correia AW, Pope CA, III, Dockery DW, Wang Y, Ezzati M, Dominici F. Effect of air pollution control on life expectancy in the United States: an analysis of 545 U.S. counties for the period from 2000 to 2007. Epidemiology. 2013;24(1):23–31. doi: 10.1097/EDE.0b013e3182770237. [DOI] [PMC free article] [PubMed] [Google Scholar]
- den Ouden ME, Schuurmans MJ, Arts IE, van der Schouw YT. Physical performance characteristics related to disability in older persons: a systematic review. Maturitas. 2011;69(3):208–219. doi: 10.1016/j.maturitas.2011.04.008. [DOI] [PubMed] [Google Scholar]
- den Ouden ME, Schuurmans MJ, Mueller-Schotte S, Bots ML, van der Schouw Y. Do subclinical vascular abnormalities precede impaired physical ability and ADL disability? Exp Gerontol. 2014;58:1–7. doi: 10.1016/j.exger.2014.06.002. [DOI] [PubMed] [Google Scholar]
- Eisner MD, Blanc PD, Yelin EH, Sidney S, Katz PP, Ackerson L, et al. COPD as a systemic disease: impact on physical functional limitations. Am J Med. 2008;121(9):789–796. doi: 10.1016/j.amjmed.2008.04.030. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Evans DA, Bennett DA, Wilson RS, Bienias JL, Morris MC, Scherr PA, et al. Incidence of Alzheimer disease in a biracial urban community: relation to apolipoprotein E allele status. Arch Neurol. 2003;60(2):185–189. doi: 10.1001/archneur.60.2.185. [DOI] [PubMed] [Google Scholar]
- Federal Interagency Forum on Aging-Related Statistics. Washington, DC: U.S. Government Printing Office; 2010. Older Americans 2010: Key Indicators of Well-Being. Available: http://www.agingstats.gov/main_site/data/2010_Documents/docs/OA_2010.pdf [accessed 15 September 2014] [Google Scholar]
- Fischer P, Hoek G, Brunekreef B, Verhoeff A, van Wijnen J. Air pollution and mortality in The Netherlands: are the elderly more at risk? Eur Respir J Suppl. 2003;40:34s–38s. doi: 10.1183/09031936.03.00402503. [DOI] [PubMed] [Google Scholar]
- Freiberger E, de Vreede P, Schoene D, Rydwik E, Mueller V, Frändin K, et al. Performance-based physical function in older community-dwelling persons: a systematic review of instruments. Age Ageing. 2012;41(6):712–721. doi: 10.1093/ageing/afs099. [DOI] [PubMed] [Google Scholar]
- Fries JF. Measuring and monitoring success in compressing morbidity. Ann Intern Med. 2003;139(5 pt 2):455–459. doi: 10.7326/0003-4819-139-5_part_2-200309021-00015. [DOI] [PubMed] [Google Scholar]
- Gill EA, Curl CL, Adar SD, Allen RW, Auchincloss AH, O’Neill MS, et al. Air pollution and cardiovascular disease in the Multi-Ethnic Study of Atherosclerosis. Prog Cardiovasc Dis. 2011;53(5):353–360. doi: 10.1016/j.pcad.2011.02.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Goldberg MS, Bailar JC, III, Burnett RT, Brook JR, Tamblyn R, Bonvalot Y, et al. Identifying subgroups of the general population that may be susceptible to short-term increases in particulate air pollution: a time-series study in Montreal, Quebec. Res Rep Health Eff Inst. 2000;97:7–113; discussion 115–120. [PubMed] [Google Scholar]
- Guralnik JM, Ferrucci L, Pieper CF, Leveille SG, Markides KS, Ostir GV, et al. Lower extremity function and subsequent disability: consistency across studies, predictive models, and value of gait speed alone compared with the short physical performance battery. J Gerontol A Biol Sci Med Sci. 2000;55(4):M221–M231. doi: 10.1093/gerona/55.4.m221. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Guralnik JM, Simonsick EM, Ferrucci L, Glynn RJ, Berkman LF, Blazer DG, et al. A short physical performance battery assessing lower extremity function: association with self-reported disability and prediction of mortality and nursing home admission. J Gerontol. 1994;49(2):M85–M94. doi: 10.1093/geronj/49.2.m85. [DOI] [PubMed] [Google Scholar]
- Hart JE, Laden F, Puett RC, Costenbader KH, Karlson EW. 2009. Exposure to traffic pollution and increased risk of rheumatoid arthritis. Environ Health Perspect 117 1065 1069, doi: 10.1289/ehp.0800503 [DOI] [PMC free article] [PubMed] [Google Scholar]
- HEI (Health Effects Institute) Boston, MA: Health Effects Institute; 2010. Traffic-Related Air Pollution: A Critical Review of the Literature on Emissions, Exposure, and Health Effects. Special Report 17. HEI Panel on the Health Effects of Traffic-Related Air Pollution. [Google Scholar]
- Hernán MA, Brumback B, Robins JM. Marginal structural models to estimate the causal effect of zidovudine on the survival of HIV-positive men. Epidemiology. 2000;11(5):561–570. doi: 10.1097/00001648-200009000-00012. [DOI] [PubMed] [Google Scholar]
- Hernán MA, Hernández-Díaz S, Robins JM. A structural approach to selection bias. Epidemiology. 2004;15(5):615–625. doi: 10.1097/01.ede.0000135174.63482.43. [DOI] [PubMed] [Google Scholar]
- Jerrett M, Arain A, Kanaroglou P, Beckerman B, Potoglou D, Sahsuvaroglu T, et al. A review and evaluation of intraurban air pollution exposure models. J Expo Anal Environ Epidemiol. 2005;15(2):185–204. doi: 10.1038/sj.jea.7500388. [DOI] [PubMed] [Google Scholar]
- Karner AA, Eisinger DS, Niemeier DA. Near-roadway air quality: synthesizing the findings from real-world data. Environ Sci Technol. 2010;44(14):5334–5344. doi: 10.1021/es100008x. [DOI] [PubMed] [Google Scholar]
- Keller JP, Olives C, Kim SY, Sheppard L, Sampson PD, Szpiro AA, et al. 2015. A unified spatiotemporal modeling approach for predicting concentrations of multiple air pollutants in the Multi-Ethnic Study of Atherosclerosis and Air Pollution. Environ Health Perspect 123 301 309, doi: 10.1289/ehp.1408145 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kemper P. The use of formal and informal home care by the disabled elderly. Health Serv Res. 1992;27(4):421–451. [PMC free article] [PubMed] [Google Scholar]
- Khan H, Kalogeropoulos AP, Georgiopoulou VV, Newman AB, Harris TB, Rodondi N, et al. Frailty and risk for heart failure in older adults: the health, aging, and body composition study. Am Heart J. 2013;166(5):887–894. doi: 10.1016/j.ahj.2013.07.032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Krämer U, Herder C, Sugiri D, Strassburger K, Schikowski T, Ranft U, et al. 2010. Traffic-related air pollution and incident type 2 diabetes: results from the SALIA cohort study. Environ Health Perspect 118 1273 1279, doi: 10.1289/ehp.0901689 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lopez R. Segregation and black/white differences in exposure to air toxics in 1990. Environ Health Perspect. 2002;110(suppl 2):289–295. doi: 10.1289/ehp.02110s2289. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Manton KG, Corder L, Stallard E. Chronic disability trends in elderly United States populations: 1982–1994. Proc Natl Acad Sci USA. 1997;94(6):2593–2598. doi: 10.1073/pnas.94.6.2593. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Manton KG, Gu X, Lamb VL. Change in chronic disability from 1982 to 2004/2005 as measured by long-term changes in function and health in the U.S. elderly population. Proc Natl Acad Sci USA. 2006;103(48):18374–18379. doi: 10.1073/pnas.0608483103. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Manton KG, Lamb VL, Gu X. Medicare cost effects of recent U.S. disability trends in the elderly: future implications. J Aging Health. 2007;19(3):359–381. doi: 10.1177/0898264307300186. [DOI] [PubMed] [Google Scholar]
- Matthews FE, Chatfield M, Brayne C, Medical Research Council Cognitive Function and Ageing Study 2006. An investigation of whether factors associated with short-term attrition change or persist over ten years: data from the Medical Research Council Cognitive Function and Ageing Study (MRC CFAS). BMC Public Health 6 185, doi: 10.1186/1471-2458-6-185 [DOI] [PMC free article] [PubMed] [Google Scholar]
- McKinlay JB, Crawford SL, Tennstedt SL. The everyday impacts of providing informal care to dependent elders and their consequences for the care recipients. J Aging Health. 1995;7(4):497–528. doi: 10.1177/089826439500700403. [DOI] [PubMed] [Google Scholar]
- Medina-Ramón M, Schwartz J. Who is more vulnerable to die from ozone air pollution? Epidemiology. 2008;19(5):672–679. doi: 10.1097/EDE.0b013e3181773476. [DOI] [PubMed] [Google Scholar]
- Mendes de Leon CF, Barnes LL, Bienias JL, Skarupski KA, Evans DA. Racial disparities in disability: recent evidence from self-reported and performance-based disability measures in a population-based study of older adults. J Gerontol B Psychol Sci Soc Sci. 2005;60(5):S263–S271. doi: 10.1093/geronb/60.5.s263. [DOI] [PubMed] [Google Scholar]
- Mendes de Leon CF, Guralnik JM, Bandeen-Roche K. Short-term change in physical function and disability: the Women’s Health and Aging Study. J Gerontol B Psychol Sci Soc Sci. 2002;57(6):S355–S365. doi: 10.1093/geronb/57.6.s355. [DOI] [PubMed] [Google Scholar]
- Ostir GV, Kuo YF, Berges IM, Markides KS, Ottenbacher KJ. Measures of lower body function and risk of mortality over 7 years of follow-up. Am J Epidemiol. 2007;166(5):599–605. doi: 10.1093/aje/kwm121. [DOI] [PubMed] [Google Scholar]
- Ostro BD. Air pollution and morbidity revisited: a specification test. J Environ Econ Manage. 1987;14:87–98. [Google Scholar]
- Pearson JF, Bachireddy C, Shyamprasad S, Goldfine AB, Brownstein JS. Association between fine particulate matter and diabetes prevalence in the U.S. Diabetes Care. 2010;33(10):2196–2201. doi: 10.2337/dc10-0698. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pope AM, Tarlov AR. Washington, DC: National Academy Press; 1991. Disability in America: Toward a National Agenda for Prevention. [Google Scholar]
- Pope CA, III, Burnett RT, Turner MC, Cohen A, Krewski D, Jerrett M, et al. 2011. Lung cancer and cardiovascular disease mortality associated with ambient air pollution and cigarette smoke: shape of the exposure-response relationships. Environ Health Perspect 119 1616 1621, doi: 10.1289/ehp.1103639 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pope CA, III, Dockery DW. Health effects of fine particulate air pollution: lines that connect. J Air Waste Manag Assoc. 2006;56(6):709–742. doi: 10.1080/10473289.2006.10464485. [DOI] [PubMed] [Google Scholar]
- Sampson PD, Szpiro AA, Sheppard L, Lindström J, Kaufman JD. Pragmatic estimation of a spatio-temporal air quality model with irregular monitoring data. Atmos Environ. 2011;45:6593–6606. [Google Scholar]
- Seeman TE, Merkin SS, Crimmins EM, Karlamangla AS. Disability trends among older Americans: National Health And Nutrition Examination Surveys, 1988–1994 and 1999–2004. Am J Public Health. 2010;100(1):100–107. doi: 10.2105/AJPH.2008.157388. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Segal RA, Martonen TB, Kim CS, Shearer M. Computer simulations of particle deposition in the lungs of chronic obstructive pulmonary disease patients. Inhal Toxicol. 2002;14(7):705–720. doi: 10.1080/08958370290084593. [DOI] [PubMed] [Google Scholar]
- Spalt EW, Curl CL, Allen RW, Cohen M, Adar SD, Stukovsky KH, et al 2015. Time-location patterns of a diverse population of older adults: the Multi-Ethnic Study of Atherosclerosis and Air Pollution (MESA Air). J Expo Sci Environ Epidemiol, doi: 10.1038/jes.2015.29 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Stafoggia M, Cesaroni G, Peters A, Andersen ZJ, Badaloni C, Beelen R, et al. 2014. Long-term exposure to ambient air pollution and incidence of cerebrovascular events: results from 11 European cohorts within the ESCAPE Project. Environ Health Perspect 122 919 925, doi: 10.1289/ehp.1307301 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Stieb DM, Smith-Doiron M, Brook JR, Burnett RT, Dann T, Mamedov A, et al. Air pollution and disability days in Toronto: results from the National Population Health Survey. Environ Res. 2002;89(3):210–219. doi: 10.1006/enrs.2002.4373. [DOI] [PubMed] [Google Scholar]
- Tchetgen Tchetgen EJ, Glymour MM, Weuve J, Robins J. Specifying the correlation structure in inverse-probability-weighting estimation for repeated measures. Epidemiology. 2012;23(4):644–646. doi: 10.1097/EDE.0b013e31825727b5. [DOI] [PubMed] [Google Scholar]
- Tonne C, Elbaz A, Beevers S, Singh-Manoux A. Traffic-related air pollution in relation to cognitive function in older adults. Epidemiology. 2014;25(5):674–681. doi: 10.1097/EDE.0000000000000144. [DOI] [PMC free article] [PubMed] [Google Scholar]
- U.S. EPA (U.S. Environmental Protection Agency) Air Trends: Nitrogen Dioxide. 2013 Available: http://www.epa.gov/airtrends/nitrogen.html [accessed 5 February 2015]
- United Nations, Department of Economic and Social Affairs, Population Division. World Urbanization Prospects: The 2014 Revision, Highlights (ST/ESA/SER.A/352). 2014 Available: http://esa.un.org/unpd/wup/Publications/Files/WUP2014-Highlights.pdf [accessed 17 April 2015]
- Wellenius GA, Boyle LD, Coull BA, Milberg WP, Gryparis A, Schwartz J, et al. Residential proximity to nearest major roadway and cognitive function in community-dwelling seniors: results from the MOBILIZE Boston Study. J Am Geriatr Soc. 2012a;60(11):2075–2080. doi: 10.1111/j.1532-5415.2012.04195.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wellenius GA, Boyle LD, Wilker EH, Sorond FA, Coull BA, Koutrakis P, et al. Ambient fine particulate matter alters cerebral hemodynamics in the elderly. Stroke. 2013;44(6):1532–1536. doi: 10.1161/STROKEAHA.111.000395. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wellenius GA, Burger MR, Coull BA, Schwartz J, Suh HH, Koutrakis P, et al. Ambient air pollution and the risk of acute ischemic stroke. Arch Intern Med. 2012b;172(3):229–234. doi: 10.1001/archinternmed.2011.732. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Weuve J, Puett RC, Schwartz J, Yanosky JD, Laden F, Grodstein F. Exposure to particulate air pollution and cognitive decline in older women. Arch Intern Med. 2012a;172(3):219–227. doi: 10.1001/archinternmed.2011.683. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Weuve J, Tchetgen Tchetgen EJ, Glymour MM, Beck TL, Aggarwal NT, Wilson RS, et al. Accounting for bias due to selective attrition: the example of smoking and cognitive decline. Epidemiology. 2012b;23(1):119–128. doi: 10.1097/EDE.0b013e318230e861. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zeger SL, Liang KY. Longitudinal data analysis for discrete and continuous outcomes. Biometrics. 1986;42(1):121–130. [PubMed] [Google Scholar]
- Zeng Y, Gu D, Purser J, Hoenig H, Christakis N. Associations of environmental factors with elderly health and mortality in China. Am J Public Health. 2010;100(2):298–305. doi: 10.2105/AJPH.2008.154971. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zhang K, Larson TV, Gassett A, Szpiro AA, Daviglus M, Burke GL, et al. 2014. Characterizing spatial patterns of airborne coarse particulate (PM10–2.5) mass and chemical components in three cities: the Multi-Ethnic Study of Atherosclerosis. Environ Health Perspect 122 823 830, doi: 10.1289/ehp.1307287 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.


