Abstract
Objective. Tenofovir disoproxil fumarate (TDF) is associated with proximal tubular dysfunction (tubulopathy) when used in the treatment of human immunodeficiency virus (HIV) infection. We evaluated whether TDF causes tubulopathy when used as HIV preexposure prophylaxis (PrEP) and whether tubulopathy predicts clinically relevant decline (≥25%) in the estimated glomerular filtration rate (eGFR).
Methods. A subgroup analysis of the Partners PrEP Study, a randomized, placebo-controlled trial of daily oral TDF, alone or with emtricitabine (FTC), in HIV-uninfected African men and women (Clinicaltrials.gov NCT00557245). Tubulopathy was assessed in concurrently obtained urine and serum samples at the 24-month or last on-treatment visit, predefined as ≥2 of the following: tubular proteinuria, euglycemic glycosuria, increased urinary phosphate, and uric acid excretion.
Results. Of 1549 persons studied (776 receiving FTC-TDF, 773 receiving placebo), 64% were male, and the median age was 37 years. Over a median 24 months of study-drug exposure, the frequency of tubulopathy was 1.7% for FTC-TDF versus 1.3% for placebo (odds ratio, 1.30; 95% confidence interval, .52–3.33; P = .68); Tubulopathy occurred in 2 of 52 persons (3.8%) with versus 3 of 208 (1.4%) without ≥25% eGFR decline (adjusted odds ratio, 1.39; .10–14.0; P > .99).
Conclusions. Daily oral FTC-TDF PrEP was not significantly associated with tubulopathy over the course of 24 months, nor did tubulopathy predict clinically relevant eGFR decline.
Keywords: PrEP, TDF toxicity, proximal tubular dysfunction, TDF nephrotoxicity
(See the editorial commentary by Krakower and Mayer on pages 983–5.)
Preexposure prophylaxis (PrEP) with tenofovir disoproxil fumarate (TDF), alone or in combination with emtricitabine (FTC), protects against human immunodeficiency virus (HIV) acquisition in diverse at-risk populations [1–4]. Although TDF is well tolerated, proximal tubular dysfunction has been observed more frequently in HIV-infected persons using TDF-containing antiretroviral regimens than in those using non–TDF-containing regimens [5–10]. Clinically significant proximal tubular dysfunction, or Fanconi syndrome, is a rare but serious complication characterized by low molecular-weight proteinuria, euglycemic glycosuria, hypophosphatemia, phosphaturia, metabolic acidosis, and hypouricemia. In clinical trials [1–3, 11–13], TDF-based PrEP was not associated with overt kidney toxicity as assessed by serum creatinine, but early proximal tubular injury can occur without severe decline in the glomerular filtration rate (GFR) [5].
To our knowledge, no study has assessed the effect of TDF-based PrEP on proximal tubular function in HIV-uninfected women. An optional substudy of the preexposure prophylaxis initiative (iPrEx) Study previously demonstrated a low rate of proximal tubulopathy in HIV-uninfected men assigned to TDF-based PrEP; however, a substantial number of participants randomized to FTC-TDF were not adherent to PrEP, as measured by plasma tenofovir concentrations in the primary study [14]. In a randomized placebo-controlled comparison, we investigated whether daily FTC-TDF PrEP causes proximal tubular dysfunction among HIV-uninfected men and women with high adherence to PrEP and whether tubular dysfunction predicts a subsequent clinically relevant decline in estimated GFR (eGFR).
METHODS
Study Population
This is a subgroup analysis of the Partners PrEP Study, a large randomized, placebo-controlled trial of daily oral TDF and FTC-TDF PrEP (Clinicaltrials.gov NCT00557245) [1]. The study enrolled 4747 heterosexual HIV-serodiscordant couples at 9 sites in Kenya and Uganda between July 2008 and November 2010. Eligible HIV-uninfected participants were ≥18 years of age, did not have active hepatitis B infection, and had Cockcroft-Gault creatinine clearance (CrCl) ≥60 mL/min). HIV-uninfected partners were randomly assigned in a 1:1:1 ratio to one of 3 study treatment groups: TDF (300 mg/d), FTC-TDF (300–200 mg/d), or matching placebo, and were followed up monthly for ≤36 months. Serum and urine samples were collected and archived at baseline and month 3, and then annually to assess proximal tubular function. In July 2011, the independent data and safety monitoring board (DSMB) recommended that the placebo arm be discontinued owing to definitive demonstration of PrEP efficacy. The study protocol was approved by the University of Washington Human Subjects Review Committee and ethics review committees at collaborating institutions. All participants provided written informed consent.
Approach for the Current Analysis
We used 2 complementary analyses to answer 2 related questions: (1) a subgroup cohort analysis of HIV-uninfected men and women randomly assigned to FTC-TDF versus placebo to determine whether FTC-TDF PrEP causes proximal tubular dysfunction, as the primary aim, and (2) a nested case-control analysis of persons receiving TDF or FTC-TDF to investigate whether proximal tubular dysfunction predicts subsequent clinically relevant eGFR decline (≥25%), as the secondary aim.
Intervention and Adherence Assessment
For the cohort analysis, the intervention was a comparison of the frequency of proximal tubular dysfunction between persons who were randomized to FTC-TDF versus placebo. FTC-TDF was chosen because it is the drug approved by the US Food and Drug Administration for PrEP, and we assumed that potential safety signals would be equally or potentially more prevalent in persons receiving a dual coformulation than in those receiving a single agent. The nested case-control analysis included persons in the TDF or FTC-TDF arms to capture all cases of severe eGFR decline (≥25%) with TDF exposure observed in the Partners PrEP Study cohort. Adherence to study medication was assessed by pill counts of returned bottles at each monthly visit, and blood samples to determine tenofovir level were collected in a random sample of participants at months 1 and 3 and then biannually. Plasma tenofovir concentrations were previously determined in archived plasma samples using ultraperformance liquid chromatography-mass spectrometry assay methods, with detectable plasma tenofovir concentration defined as >0.31 ng/mL, consistent with other PrEP trials [3, 12].
Participant Selection
Prospective Cohort Analysis
Eligible persons were HIV-uninfected men and women randomized to FTC-TDF and placebo arms in the Partners PrEP Study ≥24 months before 10 July 2011, when the placebo arm was discontinued by the DSMB. Our goal was to maintain randomized group assignment in the selected cohort while maximizing the duration of drug exposure in the selected cohort to reflect the cumulative nature of TDF toxicity. The primary selection criterion for inclusion in the cohort analysis was the possibility to have ≥24 months of study follow-up by 10 July 2011 when the study placebo arm was suspended by the DSMB. This selection criterion is based on a baseline variable, “date of enrollment into the study,” and thus preserves the randomized group assignment in the selected subgroup. All eligible persons with concurrently collected urine and serum samples were included. We selected archived serum and urine samples from a single on-treatment visit, either the 24-month visit or, for those who did not achieve this 24 visit, the last on-treatment visit. Samples collected after HIV seroconversion were not included.
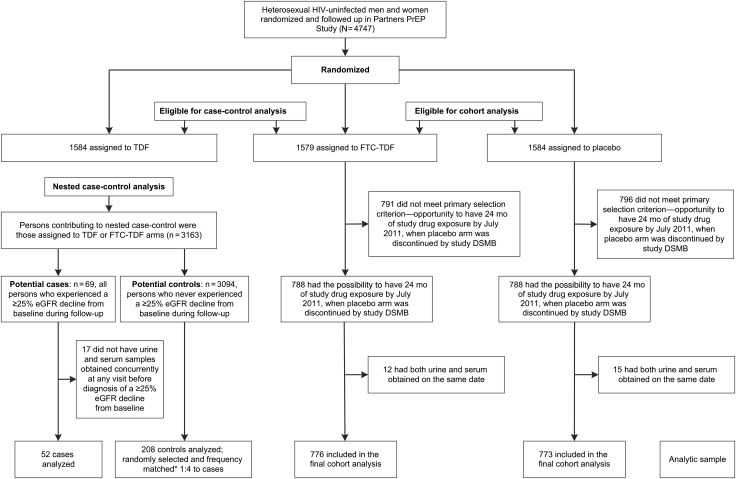
Nested Case-Control Analysis (Figure 1)
Figure 1.
Study flow diagram. We used 2 complementary designs to answer 2 related questions; (1) a cohort analysis to determine whether emtricitabine (FTC)–tenofovir disoproxil fumarate (TDF) preexposure prophylaxis (PrEP) causes proximal tubulopathy, and (2) a nested case-control analysis of participants receiving either FTC-TDF or TDF PrEP to investigate whether proximal tubulopathy predicts a subsequent ≥25% estimated glomerular filtration rate (eGFR) decline from baseline. The cohort analysis considered persons randomized to FTC-TDF and placebo in the Partners PrEP Study. The primary selection criterion for inclusion in the cohort analysis was the possibility to have the 24-month visit by 10 July 2011, when the study placebo arm was suspended by the data and safety monitoring board (DSMB); this criterion is based on a baseline variable “date of enrollment into the study” and thus preserves the randomized group assignment. Persons selected into the cohort approach (n = 1549) tended to be female and older, with lower creatinine clearance and elevated blood pressure at baseline—characteristics indicating a high propensity for kidney toxicity—compared with those not selected (n = 1614). The nested case-control analysis considered persons assigned to active PrEP arms (FTC-TDF or TDF) who experienced a ≥25% eGFR decline (case patients). Controls were persons receiving active PrEP who never experienced a ≥25% decline in eGFR and who were frequency matched to case patients by study arm (either TDF or FTC-TDF) and duration of drug exposure. Abbreviation: HIV, human immunodeficiency virus.
Clinically relevant eGFR decline was defined as a confirmed ≥25% decline from baseline, an established criterion for the diagnosis of acute kidney injury and a marker of increased morbidity and mortality [15–18]. As reported elsewhere [19], 69 persons in the 2 active PrEP arms experienced ≥25% eGFR decline from baseline, confirmed by repeated testing (case diagnosis): 37 in the FTC-TDF and 32 in the TDF arm. All case patients in the active PrEP arms with concurrent urine and serum samples at any visit before the case diagnosis visit were selected; for case patients with samples available at >1 visit, the most proximal visit sample was selected. Controls were participants randomized to TDF and FTC-TDF who never experienced ≥25% eGFR decline and who had concurrently collected urine and serum samples. For each selected case patient, 4 controls were randomly selected and were frequency matched to case patients by assigned treatment group (TDF or FTC-TDF) and duration of drug exposure.
Measurement and Definitions of Proximal Tubular Dysfunction
Serum assays for tubular function included creatinine, phosphorus, glucose, and uric acid, and urine assays included creatinine, phosphorus, glucose, uric acid, albumin, and total protein. Proximal tubulopathy was predefined as the occurrence of ≥2 of the following markers of proximal tubular dysfunction at the same time point: tubular proteinuria, defined as proteinuria of >200 mg/g with a urine albumin–total protein ratio <0.4; euglycemic glycosuria, defined as a positive urine glucose level (≥10 mg/dL) with a normal random serum glucose level (<126 mg/dL); increased urinary excretion of phosphorus, defined as a fractional tubular resorption of phosphorus <82%; and increased urinary excretion of uric acid, defined as fractional excretion of uric acid >15%. To characterize low-grade phosphate and glucose wasting, 2 cardinal features of Fanconi syndrome, we also computed the ratio of maximum rate of tubular phosphate reabsorption to the GFR (TmP/GFR) using the algorithm derived by Kenny and Glen [20–22], with values below 2.6 mg/dL (0.80 mmol/L) considered abnormal, and fractional resorption of glucose, with values <100% considered glucose wasting. In the nested case-control analysis, persons who experienced ≥25% eGFR decline were identified from our previous work on eGFR changes associated with TDF-based PrEP [19]. The eGFR was calculated from serum creatinine using the Chronic Kidney Disease Epidemiology Collaboration equation [23]. Testing for tubular parameters was performed by the Laboratory Medicine Research Testing Services of the University of Washington.
Statistical Analysis
For the cohort analysis, the primary outcome was proximal tubulopathy, predefined as the composite of ≥2 markers of proximal tubular dysfunction and compared between those assigned to FTC-TDF PrEP and those assigned to placebo. We tested for the difference in proportions using exact or asymptotic methods where appropriate. Additional analysis compared the frequency of the individual markers of proximal tubular dysfunction between FTC-TDF and placebo. In sensitivity analyses, we used more stringent definitions of abnormal values for phosphate resorption (fractional tubular resorption of phosphorus <95% with serum phosphate <2.6 mg/dL or TmP/GFR <0.80 mmol/L) and glucose resorption (fractional resorption of glucose <100%).
For the nested case-control analysis, the primary exposure of interest was proximal tubulopathy as defined in the cohort analysis, and case patients (who experienced ≥25% eGFR decline) were compared with controls using logistic regression. In addition to the primary composite variable defining proximal tubulopathy, we evaluated whether any of the individual markers of proximal tubular dysfunction separately predict a ≥25% eGFR decline. Each model was adjusted for sex, age, body mass index, baseline eGFR, and indicator for elevated systolic blood pressure. Analyses were conducted using SAS software, version 9.4 (SAS Institute).
RESULTS
General Characteristics
Of the 3163 HIV-uninfected participants randomized to the FTC-TDF and placebo groups in the Partners PrEP Study, 1576 were randomized ≥24 months before termination of the placebo arm and thus met the primary selection criterion; 1549 of those (98%) had concurrently obtained urine and serum samples and were included in the cohort analysis, 776 in the FTC-TDF and 773 in the placebo arm (Figure 1). Of these 1549, 64% were male, the median age was 37 years (range, 18–64 years), and baseline characteristics were comparable in the 2 treatment groups (Table 1). Overall, 1394 (90%) and 93 (6%)of them had tubular testing performed on their month 24 and 12 samples, respectively, with similar proportions across treatment groups.
Table 1.
Participant Enrollment Characteristics: Cohort Analysis
| Characteristics | FTC-TDF (n = 776) | Placebo (n = 773) | P Valuea |
|---|---|---|---|
| Male sex, % | 65 | 63 | .39 |
| Age, mean (SD), y | 37 (9) | 37 (9) | .93 |
| Age group, % | |||
| <35 y | 43 | 45 | |
| 35–44 y | 36 | 35 | |
| ≥45 y | 21 | 20 | |
| CrCl, mean (SD), mL/min | 107 (24) | 107 (25) | .75 |
| Serum creatinine, mean (SD), mg/dL | 0.79 (15) | 0.78 (15) | .29 |
| Serum bicarbonate, mean (SD), mEq/L | 24.4 (3) | 24.2 (2.9) | .02 |
| Serum phosphorus, mean (SD), mg/dL | 3.4 (0.7) | 3.4 (0.68) | .40 |
| Elevated blood pressure, % | |||
| Systolic (>140 mm Hg) | 3 | 5 | .29 |
| Diastolic (>90 mm Hg) | 3 | 4 | .50 |
| BMI category, (kg/m²), % | 22.2 (3.3) | 22.3 (3.7) | .30 |
| <18.5 | 9 | 7 | |
| 18.5–24.9 | 75 | 75 | |
| 25–29.9 | 13 | 14 | |
| ≥30 | 3 | 4 |
Abbreviations: BMI, body mass index; CrCl, creatinine clearance; FTC, emtricitabine; SD, standard deviation; TDF, tenofovir disoproxil fumarate.
a P values are from Mann–Whitney-Wilcoxon test for continuous outcomes and χ2 or Fisher exact tests for categorical variable where appropriate, testing the null hypothesis that the 2 distributions are identical.
In the nested case-control approach, 52 case patients with ≥25% eGFR decline from baseline in the active PrEP arms were frequency matched to 208 controls (ie, participants in the active PrEP arms who never experienced a ≥25% eGFR decline from baseline) in a 1:4 ratio; 17 case patients were excluded owing to absence of concurrently obtained urine and serum samples. Compared with controls, case patients were more likely to be female, to be older, and to have lower baseline CrCl values, but they were comparable on all other baseline characteristics (Table 2). The median follow-up duration at case diagnosis was 15 months. Overall, excluded case patients (n = 17) were comparable to included ones on baseline characteristics (data not shown).
Table 2.
Participant Enrollment Characteristics: Nested Case-Control Analysis
| Characteristics | Case Patients (n = 52) | Controls (n = 208) | P Valuea |
|---|---|---|---|
| Male sex, % | 40 | 68 | <.01 |
| Age, median (range), y | 38 (19–58) | 34 (18–58) | .01 |
| Age group, % | |||
| <35 y | 35 | 55 | |
| 35–44 y | 44 | 33 | |
| ≥45 y | 21 | 12 | |
| CrCl, median (range), mL/min | 100 (60–162) | 111 (60–172) | <.01 |
| Serum creatinine, median (range), mg/dL | 0.70 (0.49–1.06) | 0.80 (0.40–1.24) | .02 |
| Serum bicarbonate, median (range), mEq/L | 24 (16–31) | 24 (16–34) | .79 |
| Serum phosphorus, median (range), mg/dL | 3.4 (2.3–4.8) | 3.4 (2.3–4.8) | .35 |
| Elevated blood pressure, % | |||
| Systolic (>140 mm Hg) | 2 | 3 | .59 |
| Diastolic (>90 mm Hg) | 2 | 3 | .70 |
| BMI, median (range) | 22.4 (16.6–31.8) | 22.2 (15.9–34.4) | .96 |
| BMI category, (kg/m²), % | |||
| <18.5 | 12 | 10 | |
| 18.5–24.9 | 69 | 72 | |
| 25–29.9 | 13 | 14 | |
| ≥30 | 6 | 4 | |
| Duration of follow-up, median (range), mo | |||
| At sample collection | 12 (3–24) | 12 (3–24) | >.99 |
| At case diagnosis | 15 (6–33) |
Abbreviations: BMI, body mass index; CrCl, creatinine clearance.
a P values from Mann–Whitney–Wilcoxon test for continuous outcomes and χ2 or Fisher exact testing for categorical variable where appropriate, testing the null hypothesis that the 2 distributions are identical.
Effect of FTC-TDF PrEP on Proximal Tubular Function
Proximal tubulopathy, defined as a composite of ≥2 markers of proximal tubular dysfunction as described in Methods, was rare in this study population (Table 3), occurring in 13 (1.7%) of the participants in the FTC-TDF group and 10 (1.3%) in the placebo group (odds ratio [OR], 1.30; 95% confidence interval [CI], 0.52–3.33; P = .68). Multivariate analysis with sex and baseline age, CrCl, indicator for elevated systolic blood pressure, and body mass index did not have substantial effect on the estimates (data not shown). Sensitivity analyses with conservative definitions for phosphate and glucose wasting yielded similar results, as did analysis excluding 68 participants with >4 consecutive weeks off study medication for any reason during the 24-month period. The distributions of individual biomarkers of phosphate and glucose resorption were similar in the 2 treatment groups; however, tubular proteinuria (57 participants [7.3%] vs 31 [4.0%]; P = .01) and increased urinary excretion of uric acid (27 [3.5%] vs 10 [1.3%]; P = .001) occurred more frequently in the FTC-TDF group than in the placebo group. Overall, drug exposure was high in this cohort; tenofovir was detectable in 787 of 1028 plasma samples (77%) available from a subset of 303 participants in the FTC-TDF group (median tenofovir plasma concentration, 67 ng/mL; interquartile range, 1.89–101.0; >40 ng/mL is indicative of daily dosing).
Table 3.
Frequency of Markers of Proximal Tubular Dysfunction in Cohort Analysis Comparing FTC-TDF to Placebo
| Outcome Definition | Participants, No. (%) |
OR (95% CI) | P Valuea | |
|---|---|---|---|---|
| FTC-TDF (n = 776) | Placebo (n = 773) | |||
| Primary analysis: ≥2 markers of proximal tubular dysfunction | ||||
| Fractional tubular resorption of phosphate <82%, urine glucose ≥10 mg/dL with serum glucose ≤126 mg/dL, urine total protein–urine creatinine >200 mg/g with urine albumin–total protein ratio <0.4, fractional excretion of uric acid >15% | 13 (1.7) | 10 (1.3) | 1.30 (.52–3.33) | .68 |
| Sensitivity analysis for composite outcome | ||||
| Fractional tubular resorption of phosphate <95% with serum phosphate <2.6 mg/dL; all other criteria as in primary analysis | 9 (1.2) | 8 (1.0) | 1.12 (.38–3.36) | >.99 |
| TmP/eGFR <0.8 mmol/L; all other criteria as in primary analysis | 15 (1.9) | 11 (1.4) | 1.36 (.58–3.31) | .56 |
| Fractional tubular resorption of phosphate <95% with serum phosphate <2.6 mg/dL, fractional resorption of glucose <100%; all other criteria as in primary analysis | 8 (1.0) | 5 (0.7) | 1.60 (.45–6.24) | .58 |
| Individual markers of proximal tubular dysfunction | ||||
| Phosphate handling | ||||
| Fractional tubular resorption of phosphate <82% | 20 (2.6) | 21 (2.7) | 0.95 (.51–1.76) | .86 |
| Fractional tubular resorption of phosphate <95% with serum phosphate <2.6 mg/dL | 14 (1.8) | 8 (1.0) | 1.76 (.73–4.21) | .21 |
| TmP/GFR <2.6 mg/dL | 34 (4.4) | 33 (4.3) | 1.03 (.63–1.68) | .91 |
| Glucose resorption | ||||
| Urine glucose ≥10 mg/dL with serum glucose ≤126 mg/dL | 84 (10.8) | 96 (12.4) | 0.86 (.63–1.17) | .32 |
| Fractional tubular resorption of glucose <100% | 10 (1.3) | 7 (0.9) | 1.43 (.54–3.77) | .63 |
| Proteinuria | ||||
| Tubular proteinuria: urine total protein–urine creatinine >200 mg/g with urine albumin– total protein ratio <0.4 | 57 (7.3) | 31 (4.0) | 1.90 (1.21–2.97) | <.01 |
| Urine total protein–urine creatinine >200 mg/g | 62 (8.0) | 34 (4.4) | 1.89 (1.23–2.90) | <.01 |
| Uric acid excretion | ||||
| Fractional excretion of uric acid >15% | 27 (3.5) | 10 (1.3) | 2.27 (1.32–5.72) | .001 |
Abbreviations: CI, confidence interval; FTC, emtricitabine; OR, odds ratio; TDF, tenofovir disoproxil fumarate; TmP/eGFR, ratio of maximum rate of tubular phosphate resorption to glomerular filtration rate.
a P values from unadjusted χ2 or Fisher exact test, where appropriate, for the randomized comparison of participants assigned to FTC-TDF versus placebo. Multivariate analyses including sex, baseline age, eGFR, indicator for elevated systolic blood pressure, and body mass index yielded similar results.
Association of Proximal Tubular Dysfunction With Clinically Relevant Decline in eGFR
In the nested case-control analysis, proximal tubulopathy occurred in 2 of 52 case patients (3.8%) with ≥25% eGFR decline compared with 3 of 208 controls (1.4%) (adjusted OR, 1.39; 95% CI, .10–14.0; P > .99) (Table 4). Sensitivity analyses with more conservative definitions of proximal tubulopathy composite outcome yielded similar findings. Conversely, individual markers of proximal tubular dysfunction, as defined in Methods, seemed to be associated with elevated odds for ≥25% eGFR decline, but no significant differences were recorded (P > .05 for all assessed markers; Table 4). Overall, baseline covariates significantly associated with increased risk of ≥25% eGFR decline were female sex (adjusted OR, 3.03; 95% CI, 1.48 to –6.21; P = .002) and older age (adjusted OR for every 5-year age increase, 1.27; 1.04–1.57; P = .02). Tenofovir was detectable in 87 of 107 plasma samples (81%) available from a subset of 24 case patients (median tenofovir plasma concentration, 83 ng/mL; interquartile range, 12.7–98.7 ng/mL). Overall, we identified a single participant with concurrent proximal tubulopathy and ≥25% eGFR decline that clinically would be characterized as Fanconi syndrome, a 49-year-old man in the FTC-TDF arm enrolled with a CrCl of 107 mL/min (serum creatinine, 0.7 mg/dL), a serum phosphorus level of 4.8 mg/dL, trace dipstick proteinuria, and a long-standing history of unspecified dermatitis (case report provided in the online supplement).
Table 4.
Nested Case-control Analysis of Relationship Between eGFR Decline of ≥25% and Antecedent Proximal Tubular Dysfunctiona
| Exposure Definition | Case Patients, No. (%) (n = 52) | Controls, No. (%) (n = 208) | OR (95% CI) | P Value |
|---|---|---|---|---|
| Primary analysis: ≥2 markers of proximal tubular dysfunction | ||||
| Fractional tubular resorption of phosphate <82%, urine glucose ≥10 mg/dL with serum glucose ≤126 mg/dL, urine total protein–urine creatinine >200 mg/g with urine albumin–total protein ratio <0.4, fractional excretion of uric acid >15% | 2 (3.8) | 3 (1.4) | 1.39 (.10–14.0) | >.99 |
| Sensitivity analysis for composite outcome | ||||
| Fractional tubular resorption of phosphate <95% with serum phosphate <2.6 mg/dL; all other criteria as in primary analysis | 1 (1.9) | 5 (2.4) | 0.58 (.01–5.58) | >.99 |
| TmP/eGFR <0.8 mmol/L; all other criteria as in primary analysis | 1 (1.9) | 5 (2.4) | 0.58 (.01–5.58) | >.99 |
| Fractional tubular resorption of phosphate <95% with serum phosphate <2.6 mg/dL, fractional resorption of glucose <100%; all other criteria as in primary analysis | 1 (1.9) | 2 (1.0) | 1.55 (.02–32.26) | >.99 |
| Individual markers of proximal tubular dysfunction | ||||
| Phosphate handling | ||||
| Fractional tubular resorption of phosphate <82% | 4 (7.7) | 3 (1.4) | 5.24 (.74–42.10) | .11 |
| Fractional tubular resorption of phosphate <95% with serum phosphate <2.6 mg/dL | 3 (5.8) | 5 (2.4) | 2.65 (.39–14.43) | .36 |
| TmP/GFR <2.6 mg/dL | 4 (7.7) | 6 (2.9) | 2.64 (.53–11.70) | .27 |
| Glucose resorption | ||||
| Urine glucose ≥10 mg/dL with serum glucose ≤126 mg/dL | 8 (15.4) | 30 (14.4) | 1.11 (.40–2.82) | .97 |
| Fractional resorption of glucose <100% | 2 (3.8) | 2 (1.0) | 4.61 (.30–70) | .33 |
| Proteinuria | ||||
| Tubular proteinuria: urine total protein–urine creatinine >200 mg/g with urine albumin–total protein ratio <0.4 | 2 (3.8) | 13 (6.3) | 2.18 (.43–2201) | .53 |
| Urine total protein–urine creatinine >200 mg/g | 2 (3.8) | 14 (6.7) | 0.44 (.04–2.20) | .48 |
| Uric acid excretion | ||||
| Fractional excretion of uric acid >15% | 3 (5.8) | 3 (1.4) | 2.93 (.34–24.47) | .41 |
Abbreviations: CI, confidence interval; eGFR, estimated glomerular filtration rate; OR, odds ratio; TmP/eGFR, ratio of maximum rate of tubular phosphate resorption to glomerular filtration rate.
a Comparisons were adjusted for age, sex, and baseline eGFR. P values are from Fisher exact tests comparing the frequency of markers of proximal tubular dysfunction between case patients and controls. Case patients were persons receiving active preexposure prophylaxis (PrEP) who experienced a ≥25% decline in eGFR from baseline. Controls were persons receiving active PrEP without ≥25% decline in eGFR, frequency matched to case patients by study arm (tenofovir disoproxil fumarate alone or with emtricitabine) and duration of drug exposure.
DISCUSSION
In this placebo-controlled study of daily oral FTC-TDF PrEP, TDF was not significantly associated with subclinical proximal tubular dysfunction during up to 24 months of observation. These results did not change in sensitivity analyses with alternate definitions for tubulopathy. We observed a higher frequency of isolated tubular proteinuria and isolated hyperuricosuria in persons receiving FTC-TDF compared with placebo. Because total proteinuria and albuminuria have been associated with increased risk of adverse outcomes, further research is needed to determine the clinical significance of nonalbumin proteinuria. Our study has several strengths, including a prospective, randomized design with high adherence to PrEP [24, 25], a placebo comparison, and a large sample size of men and women across a broad range of ages, and thus it provides robust evidence assessing the effect of TDF-based PrEP on proximal tubular function in HIV-uninfected persons. The Partners PrEP study had the highest adherence to PrEP of any reported PrEP trial, with tenofovir detectable in 82% of a random samples of participants; in the current analysis, plasma tenofovir concentrations were indicative of consistent daily dosing in the majority of included participants. The current analysis is further enriched for drug exposure by including participants with 24 months of observation, making this cohort an important source of empirical evidence for TDF-related nephrotoxicity in HIV-uninfected persons [26].
An important concern for TDF use in healthy HIV-uninfected persons is the potential to cause kidney toxicity. Secondary safety analyses from the Partners PrEP and iPrEx trials showed that TDF-based PrEP is associated not with severe eGFR decline but rather with a very small and nonprogressive eGFR decline [14, 19]. However, the absence of severe GFR decline does not preclude tubular injury [5]. The present study demonstrates that proximal tubular dysfunction is rare among healthy HIV-uninfected men and women with high adherence to daily oral FTC-TDF PrEP. The US Centers for Disease Control and Prevention and the World Health Organization have issued guidelines recommending that PrEP be offered as a prevention option to persons at substantial risk for HIV acquisition [27, 28]; our findings are informative for evidence-based guidelines on renal monitoring during PrEP use.
As reported elsewhere [19], 69 (2%) of the participants receiving active PrEP in the Partners PrEP Study cohort had a ≥25% eGFR decline. Whether early TDF-related proximal tubular dysfunction can be used to identify a minority of patients at increased risk of TDF-related Fanconi syndrome or progressive GFR decline has not previously been studied to our knowledge. We found that a clinically relevant decline in eGFR (ie, ≥25% eGFR decline from baseline) was not significantly correlated with proximal tubular dysfunction, using either a composite definition or individual markers of proximal tubular dysfunction. These findings suggest that monitoring with routine urine markers of proximal tubulopathy will not be an efficient approach for predicting this rare but serious adverse renal event with PrEP. However, it is notable that the ORs for several individual markers of proximal tubulopathy were >2, suggesting the possibility that there is an association with eGFR decline but that proximal tubulopathy was not fully established at the earlier time point. Because it is unlikely that more definitive data will become available to address this possibility, it seems prudent to consider increased frequency of toxicity monitoring in persons with evidence of proximal tubulopathy based on serum or urine markers. We observed a single case of concurrent proximal tubulopathy and ≥25% eGFR decline that would be clinically characterized as Fanconi syndrome in a participant assigned to FTC-TDF PrEP in combination with potentially nephrotoxic comedications, reinforcing the importance of toxicity monitoring and further studies in individuals at increased risk of adverse events. Importantly, this adverse event was also identified during routine follow-up in the Partners PrEP Study, and the abnormalities resolved rapidly after drug discontinuation.
Our data complement the findings of an optional substudy of iPrEx, which demonstrated a very low rate of proximal tubulopathy in men predominantly enrolled in South America [14]. The current analysis expands on that study by including both men and women with high TDF exposure and by preserving the benefits of randomization.
This study has several limitations. First, it is possible that the criterion used for characterizing proximal tubular dysfunction may be less sensitive than proposed biomarkers, such as retinol binding protein and β2-microglobulin. However, these biomarkers are more costly, and data on their clinical usefulness in HIV-uninfected persons are limited. The tubular parameters used in this study are routinely available for clinical practice and have been used in prior studies. Second, tubular parameters were assessed at a single on-treatment visit without testing at baseline; thus, incident tubulopathy could not be accurately characterized. Importantly, because our approach preserved randomized assignment, the interpretation of the between-group comparison is unaffected. Third, the parent trial excluded persons with baseline CrCl <60 mL/min, confirmed dipstick proteinuria, or concomitant use of nephrotoxic medications; consequently, tubular function in those subpopulations could not be evaluated. In addition, the median age in our cohort was 36 years, and <10% of participants were aged ≥50 years. Fourth, against a very low background rate of proximal tubulopathy, we were able to detect only large increases in the risk of proximal tubulopathy. Finally, long-term PrEP effects beyond the study duration cannot be ascertained.
In conclusion, in this large placebo-controlled investigation, daily oral FTC-TDF PrEP was not associated with increased prevalence of proximal tubular dysfunction after up to 24 months of tenofovir use. The observation of a single case of overt Fanconi syndrome during active PrEP reinforces the importance of toxicity monitoring, particularly in individuals with risk factors for kidney injury, including concomitant nephrotoxic medications, older age, and comorbid risk factors for kidney disease. These findings support the safety of TDF-based PrEP for up to 24 months as a component of HIV prevention in healthy HIV-uninfected individuals.
Supplementary Data
Supplementary materials are available at http://jid.oxfordjournals.org. Consisting of data provided by the author to benefit the reader, the posted materials are not copyedited and are the sole responsibility of the author, so questions or comments should be addressed to the author.
Notes
Acknowledgments. We thank the study participants and the study team.
Partners PrEP Study Team. C. C. (principal investigator, protocol cochair), J. B. (medical director, protocol cochair), D. D. (protocol statistician), Robert W. Coombs, Lisa Frenkel, Craig W. Hendrix, Jairam R. Lingappa, and M. Juliana McElrath, University of Washington Coordinating Center and Central Laboratories, Seattle.
Study sites and site principal investigators. Eldoret, Kenya (Moi University, Indiana University): Kenneth H. Fife and Edwin Were; Kabwohe, Uganda (Kabwohe Clinical Research Center): Elioda Tumwesigye; Jinja, Uganda (Makerere University, University of Washington): Patrick Ndase and Elly Katabira; Kampala, Uganda (Makerere University): Elly Katabira and A. R.; Kisumu, Kenya (Kenya Medical Research Institute, University of California San Francisco): Elizabeth Bukusi and Craig R. Cohen; Mbale, Uganda (The AIDS Support Organization, CDC Uganda): Jonathan Wangisi, James D. Campbell, and J. T.; Nairobi, Kenya (University of Nairobi, University of Washington): J. K., Carey Farquhar, and Grace John-Stewart; Thika, Kenya (University of Nairobi, University of Washington): N. M.; and Tororo, Uganda (CDC Uganda, The AIDS Support Organization): James D. Campbell, J. T., and Jonathan Wangisi. Data management was provided by DF/Net Research (Seattle), and site laboratory oversight by Contract Laboratory Services of the Wits Health Consortium (University of the Witwatersrand, Johannesburg, South Africa).
Disclaimer. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health (NIH). The views expressed are those of the authors and do not necessarily represent the views of the Centers for Disease Control and Prevention.
Financial support. This work was supported by the Bill & Melinda Gates Foundation (grant OPP47674) and the US NIH (grants R01MH095507 and R01DK100272).
Potential conflicts of interest. J. B. and C. C. have received research grants related to tenofovir disoproxil fumarate (TDF) from US government agencies and the Bill & Melinda Gates Foundation. C. W.'s institution has received research grant funding related to TDF from the National Institutes of Health and Gilead Sciences. Study medication for the Partners PrEP Study was donated by Gilead Sciences. All other authors report no potential conflicts. All authors have submitted the ICMJE Form for Disclosure of Potential Conflicts of Interest. Conflicts that the editors consider relevant to the content of the manuscript have been disclosed.
Contributor Information
Collaborators: for the Partners PrEP Study Team, Connie Celum, Jared M. Baeten, Deborah Donnell, Robert W. Coombs, Lisa Frenkel, Craig W. Hendrix, Jairam R. Lingappa, M. Juliana McElrath, Eldoret Kenya, Kenneth H. Fife, Edwin Were, Elioda Tumwesigye, Patrick Ndase, Elly Katabira, Allan Ronald, Elizabeth Bukusi, Craig R. Cohen, Jonathan Wangisi, James D. Campbell, Jordan W. Tappero, James Kiarie, Carey Farquhar, Grace John-Stewart, Nelly R. Mugo, James D. Campbell, Jordan W. Tappero, and Jonathan Wangisi
References
- 1.Baeten JM, Donnell D, Ndase P et al. . Antiretroviral prophylaxis for HIV prevention in heterosexual men and women. N Engl J Med 2012; 367:399–410. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Choopanya K, Martin M, Suntharasamai P et al. . Antiretroviral prophylaxis for HIV infection in injecting drug users in Bangkok, Thailand (the Bangkok Tenofovir Study): a randomised, double-blind, placebo-controlled phase 3 trial. Lancet 2013; 381:2083–90. [DOI] [PubMed] [Google Scholar]
- 3.Grant RM, Lama JR, Anderson PL et al. . Preexposure chemoprophylaxis for HIV prevention in men who have sex with men. N Engl J Med 2010; 363:2587–99. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Thigpen MC, Kebaabetswe PM, Paxton LA et al. . Antiretroviral preexposure prophylaxis for heterosexual HIV transmission in Botswana. N Engl J Med 2012; 367:423–34. [DOI] [PubMed] [Google Scholar]
- 5.Labarga P, Barreiro P, Martin-Carbonero L et al. . Kidney tubular abnormalities in the absence of impaired glomerular function in HIV patients treated with tenofovir. AIDS 2009; 23:689–96. [DOI] [PubMed] [Google Scholar]
- 6.Horberg M, Tang B, Towner W et al. . Impact of tenofovir on renal function in HIV-infected, antiretroviral-naive patients. J Acquir Immune Defic Syndr 2010; 53:62–9. [DOI] [PubMed] [Google Scholar]
- 7.Dauchy F-A, Lawson-Ayayi S, de La Faille R et al. . Increased risk of abnormal proximal renal tubular function with HIV infection and antiretroviral therapy. Kidney Int 2011; 80:302–9. [DOI] [PubMed] [Google Scholar]
- 8.Fux CA, Christen A, Zgraggen S, Mohaupt MG, Furrer H. Effect of tenofovir on renal glomerular and tubular function. AIDS 2007; 21:1483–5. [DOI] [PubMed] [Google Scholar]
- 9.Scherzer R, Estrella M, Li Y et al. . Association of tenofovir exposure with kidney disease risk in HIV infection. AIDS 2012; 26:867–75. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Laprise C, Baril J-G, Dufresne S, Trottier H. Association between tenofovir exposure and reduced kidney function in a cohort of HIV-positive patients: results from 10 years of follow-up. Clin Infect Dis 2013; 56:567–75. [DOI] [PubMed] [Google Scholar]
- 11.Marrazzo JM, Ramjee G, Richardson BA et al. . Tenofovir-based preexposure prophylaxis for HIV infection among African women. N Engl J Med 2015; 372:509–18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Van Damme L, Corneli A, Ahmed K et al. . Preexposure prophylaxis for HIV infection among African women. N Engl J Med 2012; 367:411–22. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Martin M, Vanichseni S, Suntharasamai P et al. . Renal function of participants in the Bangkok tenofovir study—Thailand, 2005–2012. Clin Infect Dis 2014; 59:716–24. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Solomon MM, Lama JR, Glidden DV et al. . Changes in renal function associated with oral emtricitabine/tenofovir disoproxil fumarate use for HIV pre-exposure prophylaxis. AIDS 2014; 28:851–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Bellomo R, Ronco C, Kellum JA, Mehta RL, Palevsky P. Acute renal failure - definition, outcome measures, animal models, fluid therapy and information technology needs: the Second International Consensus Conference of the Acute Dialysis Quality Initiative (ADQI) Group. Crit Care 2004; 8:R204–12. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Choi AI, Li Y, Parikh C, Volberding PA, Shlipak MG. Long-term clinical consequences of acute kidney injury in the HIV-infected. Kidney Int 2010; 78:478–85. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Coca SG, Singanamala S, Parikh CR. Chronic kidney disease after acute kidney injury: a systematic review and meta-analysis. Kidney Int 2012; 81:442–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Wyatt CM, Arons RR, Klotman PE, Klotman ME. Acute renal failure in hospitalized patients with HIV: risk factors and impact on in-hospital mortality. AIDS 2006; 20:561–5. [DOI] [PubMed] [Google Scholar]
- 19.Mugwanya KK, Wyatt C, Celum C et al. . Changes in glomerular kidney function among HIV-1–uninfected men and women receiving emtricitabine–tenofovir disoproxil fumarate preexposure prophylaxis: a randomized clinical trial. JAMA Intern Med 2015; 175:246–54. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Barth JH, Jones RG, Payne RB. Calculation of renal tubular reabsorption of phosphate: the algorithm performs better than the nomogram. Ann Clin Biochem 2000; 37(pt 1):79–81. [DOI] [PubMed] [Google Scholar]
- 21.Kenny AP, Glen AC. Tests of phosphate reabsorption. Lancet 1973; 2:158. [DOI] [PubMed] [Google Scholar]
- 22.Walton RJ, Bijvoet OL. Nomogram for derivation of renal threshold phosphate concentration. Lancet 1975; 2:309–10. [DOI] [PubMed] [Google Scholar]
- 23.Levey AS, Stevens LA, Schmid CH et al. . A new equation to estimate glomerular filtration rate. Ann Intern Med 2009; 150:604–12. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Donnell D, Baeten JM, Bumpus NN et al. . HIV protective efficacy and correlates of tenofovir blood concentrations in a clinical trial of PrEP for HIV prevention. J Acquir Immune Defic Syndr 2014; 66:340–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Haberer JE, Baeten JM, Campbell J et al. . Adherence to antiretroviral prophylaxis for HIV prevention: a substudy cohort within a clinical trial of serodiscordant couples in East Africa. PLoS Med 2013; 10:e1001511. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Rodríguez-Nóvoa S, Labarga P, D'Avolio A et al. . Impairment in kidney tubular function in patients receiving tenofovir is associated with higher tenofovir plasma concentrations. AIDS 2010; 24:1064–6. [DOI] [PubMed] [Google Scholar]
- 27.Centers for Disease Control and Prevention. Pre-exposure prophylaxis for the prevention of HIV infection in the United States: a clinical practice guideline—2014. http://www.cdc.gov/hiv/pdf/PrEPguidelines2014.pdf Accessed 27 September 2015.
- 28.World Health Organization. Guideline on when to start antiretroviral therapy and on pre-exposure prophylaxis for HIV, 2015. http://www.who.int/hiv/pub/guidelines/earlyrelease-arv/en/ Accessed 27 October 2015. [PubMed]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.