Highlights
-
•
Basal cell carcinoma (BCC) is the most common malignancy of the sun-exposed area. About 80–85% occur on the head and neck [2] (Lorenzini et al., 2005). It occur rarely in the other area.
-
•
On the other hand, Pilonidal sinus (PNS) is a common benign disease that accounts for almost 15% of anal suppurations.
-
•
We report a case of BCC presented with signs and symptoms of PNS.
Keywords: Superficial mass, Abscesses, Palisades, Case report
Abstract
Introduction
Pilonidal sinus is a common benign disease that accounts for almost 15% of anal suppurations while basal cell carcinoma is the most common malignancy of the sun-exposed area occurring mainly on the head and neck. We report a case of basal cell carcinoma presented with signs and symptoms of PNS. A 40-year-old male presented with swelling of the lower back for 2 years. On examination, there was a round, mobile, soft 4 × 2.5 cm mass on the sacrococcygeal area. Ultrasound showed subcutaneous cystic lesion. Clinical diagnosis of PNS was done and excisional biopsy was performed under local anesthesia. The result of the histopathological examination was suggestive for basal cell carcinoma.
Conclusion
Basal cell carcinoma should not be forgotten in differential diagnosis of superficial mass and abscesses.
1. Introduction
Pilonidal sinus (PNS) is a common benign disease that accounts for almost 15% of anal suppurations. It is a sinus that contains hairs and occurs mainly in the sacrococcygeal region. Its diagnosis is rarely difficult on clinical bases [1]. On the other hand; basal cell carcinoma (BCC) is the most common malignancy of the sun-exposed area. About 80–85% occur on the head and neck [2]. BCC of the other area rarely mentioned in literature like nail, palm, vulva and nipple. Both condition best diagnosed by histopathological examination [2], [3], [4], [5]. We report a case of BCC presented with signs and symptoms of PNS. The work has been reported in line with the SCARE criteria [6].
1.1. Patient information
A 40-year-old Kurdish driver man presented with swelling of the lower back for 2 years associated with occasional pain and increasing in size.
1.2. Clinical findings
On examination, there was a round, mobile, soft mass on the sacrococcygeal area (intergluteal region) just right to the midline. It was 4 × 2.5 cm in size with slight tenderness.
1.3. Diagnostic assessment
Hematological tests were normal. Ultrasound showed subcutaneous cystic lesion with 41 × 26 × 1.4 cm in size, just distal to terminal part of the coccyx containing hetergenous fluid content.
1.4. Therapeutic intervention
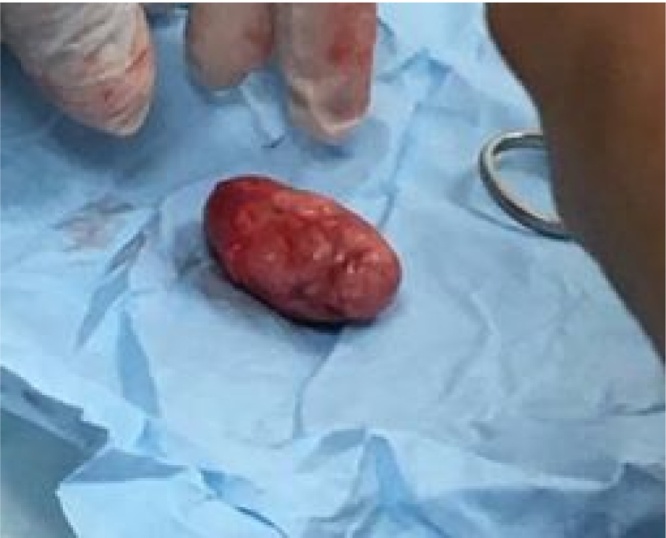
Clinical diagnosis of PNS was done and excisional biopsy was performed under general anesthesia. Fig. 1 shows the gross appearance of the specimen. The result of the histopathological examination showed focal erosion of the epidermis overlying multiple clusters of polygonal basaloid cells with dark hyperchromatic ovoid uniform nuclei extending from epidermis into superficial dermis, displaying peripheral nuclear palisades and artefactual separation stromal cleft (Fig. 2, Fig. 3). The picture was suggestive for BCC.
Fig. 1.
The specimen after resection.
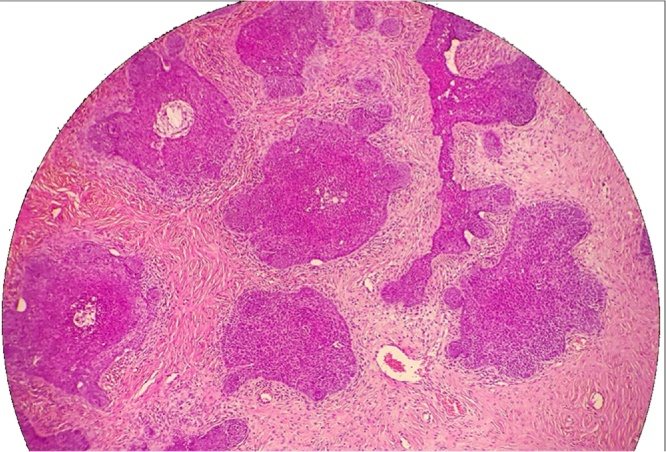
Fig. 2.
Multiple clusters of polygonal basaloid cells.
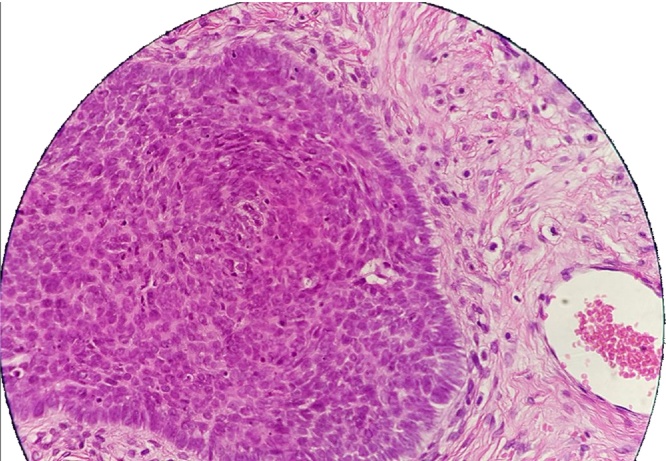
Fig. 3.
Polygonal basaloid cells with dark hyperchromatic ovoid uniform nuclei displaying peripheral nuclear palisades and artefactual separation stromal cleft.
1.5. Follow-up and outcomes
The patient was lost from follow up.
2. Discussion
BCC is 4 to 5 times more common than squamous cell carcinoma of the skin and it is reported to be continuosly increasing [7]. Most frequently arises on sun exposed area. However, it may occur in other covered regions of the body, including the axillae, inguinal region, and nipple [3]. In Japanese and black people, BCCs are mostly pigmented which resembling malignant melanoma [7]. Several histological types of BCC are recognized including: pilar (keratotic), primordial (solid or medullary), morphea-like (sclerosing or fibrotic), adenoid (adenoid cystic), superficial spreading, and pigmented (melanotic). Usually one type appears, but a mixture of two or more may co-exist [8]. The aetiology of BCC is not clear, but excessive exposure to ultraviolet radiation is implicated. Other etiological factors are old age, male gender, immunosuppressed patients, specific phenotype (freckling, blonde or red hair), environmental causes such as exposure to polycyclic aromatic amines and genetic syndromes [2], [9]. BCCs develop from the adnexal structures and basal layer of the epidermis. large nucleus to cytoplasm ratio, elongated ovoid nuclei, variable peripheral palisading with abnormal mitoses are the histological hallmarks of BCC [2]. BCC presents mainly with either one of three types; nodulo-ulcerative lesion, flat lesion or polypoid tumor with an intact surface [10]. Our case presented with mass like lesion with intact overlying skin. BCC rarely metastasize ranging from 0.0028 to 0.5% [4], [11]. Definitive diagnosis and treatment usually done by excisional biopsy with histopathological examination. Among perineal and genital BCC, vulva affected most commonly, accounting for about 1% of all BCCs which may present with bleeding, palpable vulvar mass, ulceration, irritation, pain, and pruritis [10]. Table 1 shows important reported cases of BCC occurred in perineal and genital areas.
Table 1.
Summary of important reported cases of BCC occurred in perineal and genital areas.
| References & Authors | No. of cases | Average Age(Year) | Site | presentation |
|---|---|---|---|---|
| 12/Roger | 45 | 76 | vulva | Mass, pruritis, ulcer |
| 11/Breen | 17 | 59 | Left labium majus (9 patients), Right labium majus (6 patients)* | Mass (2 patients), mass and pruritis (4 patients), sore (5) ulcer (3 patients) pruritis (2 patients)* |
| 13/Goldminz | 12 | 69 | penis | Nodule (7 patients)Scaly plaque(3), ulceration (2) |
| 8/Jimenez | 11 | 59 | labium majus (9 patients), posterior fourchette (2 patients), | Mass (6 patients), ulcer (2 patients), pruritis (2 patients), induration (1 patient) |
| 14/Piura | 8 | 70.5 | labium majus | Mass (4 patients), ulcer (4 patients) |
| 15/Ward | 5 | 69.8 | vulva(4 patient) right labium majum (1 patient) | Soreness (1 patient) mass (4 patients) |
| 16/Karim | 1 | 83 | anal verge | Ulcer |
| 17/Misago | 1 | 88 | 9 o'clock perianal region | Polypoid nodular lesion |
Although BCC is a rare disease in covered area of the body especially perineal and genital regions, it should not be forgotten in differential diagnosis of superficial mass and abscesses. Its main line of treatment is complete resection.
Conflicts of interest
There is no conflict to be declared.
Funding
None.
Ethical approval
Approval has been taken from bioscience center.
Author contribution
Abdulwahid M. Salih: Surgeon performed the operation and follow up. Fahmi H. Kakamad: writing the manuscript and follow up. Goran M rauf: Examining the specimen, follow up.
Informed consent
Informed consent was taken from the patient for publication.
References
- 1.Salih Abdulwahid M., Kakamad Fahmi H. Intermammary pilonidal sinus: a rare presentation. Int. J. Case Rep. Images. 2016;7(1):48–50. [Google Scholar]
- 2.Lorenzini M., Gatti S., Giannitrapani A. Giant basal cell carcinoma of the thoracic wall: a case report and review of the literature. Br. J. Plast. Surg. 2005;58:1007–1010. doi: 10.1016/j.bjps.2005.04.017. [DOI] [PubMed] [Google Scholar]
- 3.Martinelli Periungual basal cell carcinoma: case report and literature review. Dermatol. Surg. 2006;32:320–323. doi: 10.1111/j.1524-4725.2006.32062.x. [DOI] [PubMed] [Google Scholar]
- 4.Sworn Metastatic basal cell carcinoma; a case report. Br. J. Obstet. Gynaecol. 1979;86:332–334. doi: 10.1111/j.1471-0528.1979.tb11265.x. [DOI] [PubMed] [Google Scholar]
- 5.Takeno Basal cell carcinoma of the nipple in male patients with gastric cancer recurrence: report of a case. Breast Cancer. 2014;21(1):102–107. doi: 10.1007/s12282-010-0217-6. (Epub 2010 Aug 11) [DOI] [PubMed] [Google Scholar]
- 6.Agha R.A., Fowler A.J., Saetta A., Barai I., Rajmohan S., Orgill D.P., for the SCARE Group The SCARE Statement: consensus-based surgical case report guidelines. Int. J. Surg. 2016 doi: 10.1016/j.ijsu.2016.08.014. (article in press) [DOI] [PubMed] [Google Scholar]
- 7.Weedon D. 2nd ed. Churchill Livingstone; Philadelphia: 2002. Skin Pathology; pp. 765–772. [Google Scholar]
- 8.Jimenez Cutaneous basal cell carcinoma of vulva. Cancer. 1975;36 doi: 10.1002/1097-0142(197511)36:5<1860::aid-cncr2820360543>3.0.co;2-w. 186&1868. [DOI] [PubMed] [Google Scholar]
- 9.Rosai J. 9th edn. St. Louis; Mosby: 2004. Rosai and Ackerman’s Surgical Pathology; pp. 136–139. 132-133. [Google Scholar]
- 10.Koçak Basal cell carcinoma of the vulva: a case report. Eur. J. Med. Sci. 2015;2(1):26–29. [Google Scholar]
- 11.Breen Basal cell carcinoma of vulva. Obstet. Gynecol. 1975;45(2) [PubMed] [Google Scholar]
- 12.Roger Basal cell carcinoma of the vulva a clinicopathologic study of 45 cases. Int. J. Gynecol. Pathol. 1997;16(4) doi: 10.1097/00004347-199710000-00005. [DOI] [PubMed] [Google Scholar]
- 13.Goldminz Penile basal cell carcinoma: report of a case and review of the literature. J. Am. Acad. Dermatol. 1989;20(6) doi: 10.1016/s0190-9622(89)70139-0. [DOI] [PubMed] [Google Scholar]
- 14.Piura Basal cell carcinoma of the vulva. J. Surg. Oncol. 1999;70:172–176. doi: 10.1002/(sici)1096-9098(199903)70:3<172::aid-jso5>3.0.co;2-i. [DOI] [PubMed] [Google Scholar]
- 15.Ward Jeseph. Five cases of basal cell carcinoma of the vulva. J. Obstetr. Gynecol. 1956;1(1):697–705. doi: 10.1111/j.1471-0528.1956.tb05549.x. [DOI] [PubMed] [Google Scholar]
- 16.Karim Pedicled scrotal island skin flap in the treatment of anal basal cell carcinoma. Br. J. Plast. Surg. 2001:54. doi: 10.1054/bjps.2000.3488. [DOI] [PubMed] [Google Scholar]
- 17.Misago Polypoid basal cell carcinoma on the perianal region: a case report and review of the literature. J. Dermatol. 2004;31:51–55. doi: 10.1111/j.1346-8138.2004.tb00505.x. [DOI] [PubMed] [Google Scholar]