The Food and Drug Administration (FDA) has not approved any injectable glucocorticoid product for epidural administration, but epidural injection of glucocorticoids is commonly used to manage radicular neck and back pain.1 Severe and sometimes fatal neurological events have occurred immediately after epidural injection of glucocorticoids. Indeed, 90 events were reported to the FDA Adverse Event Reporting System (FAERS) between 1997 and 2014.2
In the December 10, 2015 issue of the New England Journal of Medicine, Racoosin et al,2 from the FDA, found that all the catastrophic neurological events (brain and spinal cord infarctions resulting in permanent disability or death) reported to the FAERS were associated with injection of a glucocorticoid suspension, with only a few cases, involving temporary symptoms, reported with glucocorticoid solutions. However, the authors found that suspension formulations still accounted for more than 80% of the commercially available corticosteroid products used for epidural injections in 2013, according to Medicare and IMS health data, despite the increasing use of solutions.
Potential causes of neurological complications after spinal injections of a suspension of particulate steroids include intrathecal injection, epidural hematoma, direct spinal cord injury and cord infarction due to an arterial spasm or vascular obliteration after inadvertent intra-arterial injection.2 However, the almost immediate onset of neurological deficit, as well as the MR findings performed in patients who underwent this complication, are very suggestive of spinal cord ischaemia following interruption of arterial blood supply.3–6 Brain or spinal cord ischaemia resulting from particulate steroid injection into the vertebral artery has also been demonstrated in an animal study.7 Occlusion of distal intramedullary arteries by steroid particles via an unexpected intra-arterial injection has been incriminated as the mechanism leading to cord infarction in severe neurological deficit occurring after foraminal steroid injections at the cervical spine.8 It has been suggested that the tendency of steroid particles to coalesce and the size of their final aggregates, which differ among the different types of particulate steroids, may influence the risk of arterial embolisation.9
To explore the mechanisms by which steroids provoke the cord infarction, we used intravital microscopy of mouse cremaster muscles to investigate the in vivo effects of an intra-arterial injection of four different particulate steroids, namely methylprednisolone acetate, triamcinolone acetonide, prednisolone acetate and cortivazol and one corticosteroid solution, namely dexamethasone sodium phosphate, on microvascular perfusion10. Intra-arterial administration of 20 µL of pure prednisolone acetate or triamcinolone acetonide suspension completely stopped blood flow in all arterioles and venules, which decreased the functional capillary density to zero (see online supplementary material). Methylprednisolone acetate sharply decreased perfusion as well, although some blood flow was maintained in a few areas of the arteriolar and venular network. In contrast, intra-arterial administration of the cortivazol suspension or dexamethasone sodium phosphate solution did not change microvascular blood flow.10 The formation of macroaggregates of particulate steroids, which has been suggested to lead to vascular obliteration,9 was not observed in our animal experiments. An arterial spasm was not observed as well. Our results disclosed another mechanism for microvascular occlusion. We found that an unexpected aggregation of red blood cells (RBCs), occurring immediately after injection of the particulate steroids into the blood stream, was responsible for the obstruction of arterioles.10 As well, the particulate steroids could directly interact with RBCs without mediation by white cells or plasma proteins. Scanning electron microscopy provided some insight into the mechanism of RBC agglutination, showing RBCs with a deformed shape and their transformation into spiculated cells with prednisolone acetate, triamcinolone acetonide and methylprednisolone acetate administration (figure 1). More than 28% of the RBCs changed into spiculated cells with these three corticosteroid suspensions.10
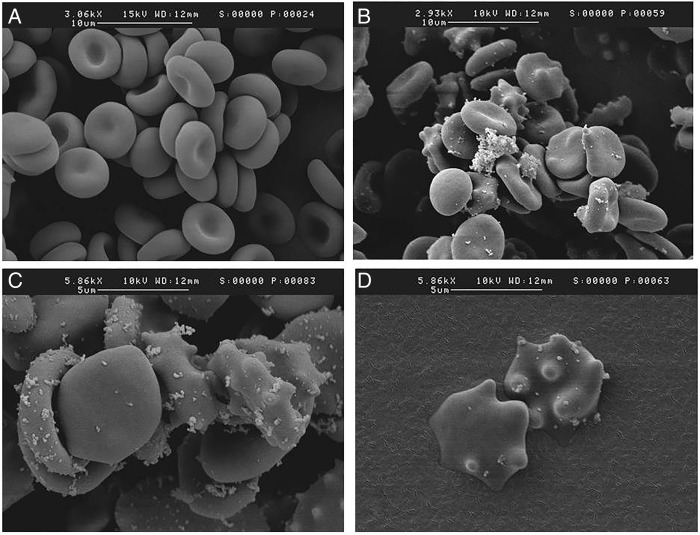
Figure 1.
Scanning electron microscopy images of a mixture of human blood mixed with saline showing normal red blood cells (A) and human blood mixed with prednisolone acetate at different magnifications (B–D) showing spiculated red blood cells tending to interdigitate. (Images courtesy Massoud Mirshahi MD, PhD, UMR 965, Université Paris-Diderot, Paris, France).
rmdopen-2016-000320supp_video.mp4 (64.1MB, mp4)
We were not able to determine the exact mechanisms by which the particulate steroids induced an altered RBC shape. The role of drug concentration, osmolarity and viscosity remains to be studied. In addition, why some particulate steroids induce the altered RBC shape and finally vascular occlusion while cortivazol, another particulate steroid, does not, remains to be explained. Our results were obtained in an animal model of microvascularisation. However, the same direct effect of the steroids on human RBCs was also demonstrated in vitro.10
Other potential causes of vascular occlusion such as vascular obliteration due to particulate steroids aggregates or a vascular spasm were not specifically addressed in our work. Therefore, up to now, it is not possible to discriminate if there is only one or several mechanisms responsible for the neurological deficits in humans.
In 2014, the FDA issued a requirement that all injectable glucocorticoid product labels carry a warning stating that ‘serious neurological events, some resulting in death, have been reported with epidural injection of corticosteroids’ and that the ‘safety and effectiveness of epidural administration of corticosteroids have not been established and corticosteroids are not approved for this use’.1 However, the warning did not distinguish any difference in the risk associated with the various injection approaches (interlaminar, transforaminal and caudal), locations of spinal injections (cervical, thoracic, lumbar and sacral) or glucocorticoid formulations (solutions and suspensions), because ‘the data suggested that each approach, location, and formulation was associated with some risk of neurological injury’.2 An advisory committee meeting of the FDA, held in November 2014, decided not to modify the warning.2 This decision was taken despite all catastrophic events reported to the FAERS occurred after injection of a glucocorticoid suspension.2
In a recent review, MacMahon et al11 concluded that, in cervical, thoracic and high lumbar transforaminal epidural steroid injections, a growing consensus of the literature supports the exclusive use of non-particulate glucocorticoid to reduce the risk of embolic injury to the brain and spinal cord, but that both particulate and non-particulate glucocorticoid are acceptable choices in lower lumbosacral transforaminal epidural spine injection since serious neurological events are exceedingly rare at this level.
However, we believe that cord infarction is rarer at the lower lumbar level compared to upper levels just because the anatomical disposition of a metameric artery contributing to the cord vascularisation is only present in very few persons.12
From our results, we suggest that the particulate steroids responsible for blood-flow arrest in our experiments, namely methylprednisolone acetate, triamcinolone acetonide and prednisolone acetate, should no longer be used for foraminal injections at the cervical as well at the lumbar level and probably, as a precaution, for epidural injections as well.
In our clinical practice, we presently use the particulate steroid cortivazol, which does not provoke RBC agglutination,10 but which is not available for epidural injection in most other countries. However, more experience is needed to confirm the agent's innocuity, especially with foraminal administration.
In countries where cortivazol is not available, use of dexamethasone sodium phosphate solution for epidural injection, despite it is short action time, is the only available alternative to corticosteroid suspensions. Dexamethasone is widely used with intra-arterial administration and to our knowledge has never been associated with permanent neurological complications. Several studies that compared pain reduction with transforaminal injection of either dexamethasone sodium phosphate or steroid suspensions have found no evidence that dexamethasone is less effective than particulate steroids.13 However, there is no direct evidence that non-particulate steroids are superior to sham injections, and studies that show no difference between particulate and non-particulate steroids are underpowered.14 Therefore, further studies are needed to confirm the effectiveness of dexamethasone sodium phosphate with this method of administration.
Footnotes
Contributors: The paper has been written by J-DL and EV.
Competing interests: None declared.
Provenance and peer review: Not commissioned; externally peer reviewed.
Data sharing statement: No additional data are available.
References
- 1.Food and Drug Administration. FDA Drug Safety Communication: FDA requires label changes to warn of rare but serious neurologic problems after epidural corticosteroid injections for pain. 23 April 2014. http://www.fda.gov/Drugs/DrugSafety/ucm394280.htm
- 2.Racoosin JA, Seymour SM, Cascio L et al. . Serious neurologic events after epidural glucocorticoid injection—The FDA's Risk Assessment. N Engl J Med 2015;373:2299–301. 10.1056/NEJMp1511754 [DOI] [PubMed] [Google Scholar]
- 3.Houten JK, Errico TJ. Paraplegia after lumbosacral nerve root block: report of three cases. Spine J 2002;2:70–5. 10.1016/S1529-9430(01)00159-0 [DOI] [PubMed] [Google Scholar]
- 4.Huntoon MA, Martin DP. Paralysis after transforaminal epidural injection and previous spinal surgery. Reg Anesth Pain Med 2004;29:494–5. 10.1097/00115550-200409000-00016 [DOI] [PubMed] [Google Scholar]
- 5.Somayaji HS, Saifuddin A, Casey ATH et al. . Spinal cord infarction following therapeutic computed tomography-guided left L2 nerve root injection. Spine 2005;30:E106–8. 10.1097/01.brs.0000153400.67526.07 [DOI] [PubMed] [Google Scholar]
- 6.Yuh WT, Marsh EE III, Wang AK et al. . MR imaging of spinal cord and vertebral body infarction. Am J Neuroradiol 1992;3:145–54. [PMC free article] [PubMed] [Google Scholar]
- 7.Okubadejo GO, Talcott MR, Schmidt RE et al. . Perils of intravascular methylprednisolone injection into the vertebral artery: an animal study. J Bone Joint Surg Am 2008;90:1932–8. 10.2106/JBJS.G.01182 [DOI] [PubMed] [Google Scholar]
- 8.Tiso RL, Cutler T, Catania JA et al. . Adverse central nervous system sequelae after selective transforaminal block: the role of corticosteroids. Spine J 2004;4:468–74. 10.1016/j.spinee.2003.10.007 [DOI] [PubMed] [Google Scholar]
- 9.Derby R, Lee SH, Date ES et al. . Size and aggregation of corticosteroids used for epidural injections. Pain Med 2008;9: 227–34. 10.1111/j.1526-4637.2007.00341.x [DOI] [PubMed] [Google Scholar]
- 10.Laemmel E, Segal N, Mirshahi M et al. . Deleterious effects of intra-arterial administration of particulate steroids on microvascular perfusion in a mouse model. Radiology 2016;279:731–40. 10.1148/radiol.2015142746 [DOI] [PubMed] [Google Scholar]
- 11.MacMahon PJ, Huang AJ, Palmer WE. Spine injectables: what is the safest cocktail? AJR Am J Roentgenol 2016;24:1–8. 10.2214/AJR.16.16379 [DOI] [PubMed] [Google Scholar]
- 12.Wybier M, Gaudart S, Petrover D et al. . Paraplegia complicating selective steroid injections of the lumbar spine. Report of five cases and review of the literature. Eur Radiol 2010;20:181–9. 10.1007/s00330-009-1539-7 [DOI] [PubMed] [Google Scholar]
- 13.El-Yahchouchi C, Geske JR, Carter RE et al. . The noninferiority of the nonparticulate steroid dexamethasone vs the particulate steroids betamethasone and triamcinolone in lumbar transforaminal epidural steroid injections. Pain Med 2013;14:1650–7. 10.1111/pme.12214 [DOI] [PubMed] [Google Scholar]
- 14.Rathmell JP, Benzon HT, Dreyfuss P et al. . Safeguards to prevent neurologic complications after epidural steroid injections: consensus opinions from a multidisciplinary working group and national organizations. Anesthesiology 2015;122:974–84. 10.1097/ALN.0000000000000614 [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
rmdopen-2016-000320supp_video.mp4 (64.1MB, mp4)