Highlights
-
•
Pseudoaneurysm of pancreaticoduodenal and gastric artery are rare complications of acute pancreatitis.
-
•
Arterial pseudoaneurysms have 90% of mortality if not recognized and treated during pancreatitis.
-
•
Presented an unusual case of arterial pseudoaneurysm complicating acute pancreatitis because it appeared in an early phase, during the acute process, and it had an uncommon arterial localization.
-
•
Presented an unusual case of arterial pseudoaneurysm complicating acute pancreatitis.
-
•
It appeared in an early phase, during the acute process, and it had an uncommon arterial localization.
Keywords: Pseudoaneurysm &minus, Acute necrotizing pancreatitis &minus, Complications &minus, Therapeutic embolization
Abstract
Introduction
Arterial pseudoaneurysm is a rare and life-threatening complication of pancreatitis, seen more often in chronic than in acute pancreatitis. It involves mostly the splenic artery, while only in 10% of the case it appears in pancreaticoduodenal and gastric artery. This case report described an asymptomatic pseudoaneurysm of the posterior superior pancreaticoduodenal artery and of the right gastric artery, which occurred after 13 days from the episode of acute pancreatitis and, then it was treated with vascular angioembolization.
Presentation of case
A 71 year-old female was admitted to the Emergency Surgery Department for severe acute pancreatitis. After 13 days from the onset, pseudoaneurysms were detected with a control contrast-enhanced computed tomography and they were localized in a branch of the right gastric artery and in a branch of the posterior superior pancreaticoduodenal artery. The patient underwent angiography and the pseudoaneurysms were treated with platinum coil embolization, without complications or further bleeding.
Discussion
This is an unusual case because of the low incidence of arterial pseudoaneurysm as acute pancreatitis complication (1.3–10%), and the uncommon localization in the pancreaticoduodenal arteries.
Conclusion
It is important to be aware of pancreatitis-related arterial pseudoaneurysms, as they have a mortality of 90% if not recognized and treated, not only in chronic but also in acute pancreatitis, and to work out a scheduled follow-up with abdominal computed tomography or pancreatic contrast-enhanced ultrasound in order to control and prevent late onset complications.
1. Background
Severe acute pancreatitis (SAP) is associated with a high rate of complications and significant mortality, as high as 8%–39% [1]. Although the major causes of death are secondary infection of pancreatic necrotic tissue and, subsequently multiple organ failure [2], peripancreatic arterial pseudoaneurysm (AP) is still a rare but life-threatening complication, seen most often in patients with chronic pancreatitis [3]. AP is due to wall erosion of vessels crossing the inflammation area, and its rupture can led to haemorrhagic complications, which require immediate intervention [4], [5]. AP involves the splenic artery in up to 50% of cases [6], and usually appears after weeks to months from an episode of acute pancreatitis [7], [8], [9]. Contrast-enhanced computed tomography (CECT) is the gold standard to detect such kind of complications, and its use is recommended not only in the initial phase of SAP but also and mainly in the late phase [10]. Because of the low incidence of AP as acute pancreatitis complication (1.3-10%), the high rate of mortality due to its rupture (40–90%), and the uncommon localization in the pancreaticoduodenal arteries (10%) [6], the authors decide to report the case of an asymptomatic pseudoaneurysm of the posterior superior pancreaticoduodenal artery and of the right gastric artery, which occurred after 13 days from the episode of acute pancreatitis and then, it was treated with vascular angioembolization.
2. Case presentation
2.1. Presenting concerns
A 71 year-old female came to the Emergency Room of Sant’ Anna University Hospital of Ferrara (Italy), complaining abdominal pain spread to all quadrants, with nausea and vomiting, and anuria from one day.
2.2. Clinical findings
Personal history was characterized by obesity (Body Mass Index of 33.3 kg/cm2), diabetes, arterial hypertension, chronic renal failure, severe osteoporosis, hypothyroidism, previous appendectomy and ovariectomy for a mature cystic ovarian teratoma. No history of alcohol abuse was reported. At admission, the laboratory results (neutrophilic leukocytosis: 41.51 × 10^3/μl total white blood cells with 37.07 × 10^3/μl neutrophil; amylases: 251 U/L; lipases: 816 U/L; C-reactive protein: 34.1 mg/dl; procalcitonine: 10.93 ng/ml) and the CECT (Fig. 1) reveled an acute severe pancreatitis, which involved the whole pancreatic gland and presented peripancreatic, perihepatic and perisplenic free fluid, with a modified CT severity index [11] of 8 (range 0–10). Moreover, the CECT showed cholelithiasis and partial thrombosis of the splenic vein until its confluence with the superior mesenteric vein. So she was admitted to the Department of Emergency Surgery, a medical therapy was established and the patients was strictly observed, without alteration of vital signs. At day five, a control CECT showed a stability of the radiological imaging, with a contemporary improvement of laboratory tests and clinical conditions.
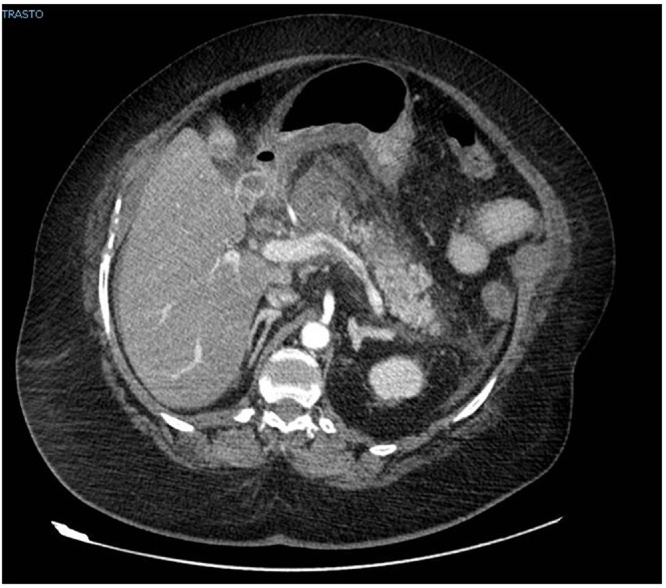
Fig. 1.
The first CECT scan revealed a severe acute pancreatitis. Any images related to a right gastric artery pseudoaneurysm were present.
2.3. Diagnostic focus and assessment
After 13 days from admission, patient’s clinical conditions were improving and she was completely asymptomatic; by the way, another control CECT was planned before transferring the patient to a medical ward. It revealed an organized fluid collection of 11 × 6.5 cm in the body of the pancreas and the appearance of a 7 mm pseudoaneurysm of the right gastric artery inside the collection (Fig. 2 a-b). Selective angiography of celiac trunk and of superior mesenteric artery showed a pseudoaneurysm localized not only in a branch of the right gastric artery, but also in a branch of the posterior superior pancreaticoduodenal artery (Fig. 3).
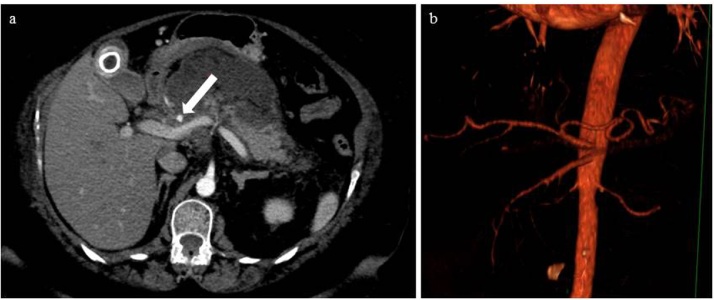
Fig. 2.
a Control CECT after 13 days from acute pancreatitis onset revealed the presence of a 7 mm pseudoaneurysm of the right gastric artery (arrow). b 3D reconstruction of Aorta and its principal branches (celiac trunk and superior mesenteric artery).
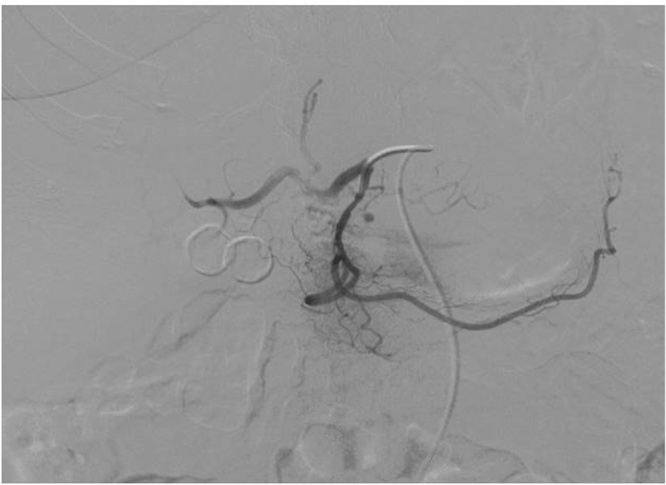
Fig. 3.
Selective angiography of celiac trunk and of superior mesenteric artery showed a pseudoaneurysm localized in a branch of the right gastric artery and in a branch of the posterior superior pancreaticoduodenal artery.
2.4. Therapeutic focus and assessment
The pseudoaneurysms were angioembolized successfully with platinum coils MRI-compatible, without any complications (Fig. 4).
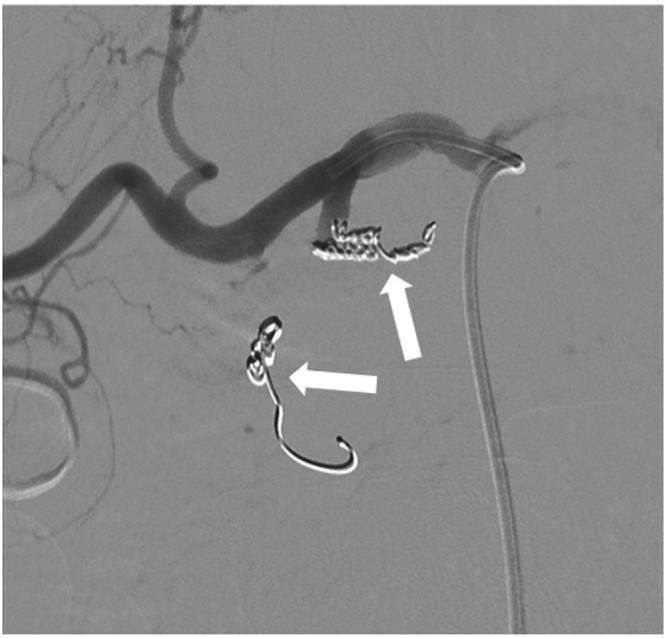
Fig. 4.
Selective angiography of celiac trunk after pseudoaneurysm coil embolization.
2.5. Follow-up and outcomes
After 6 days from the procedure, the patient was transferred to a medical ward to continue observation and medical therapy. After ten days from pseudoaneurysms angioembolization, a CECT showed the good outcomes of the radiological interventive procedure and an improvement of the pancreatic gland inflammation process with the persistent of the organized fluid collection of 10 × 6.5 cm in the pancreatic body. The patient was discharged after 30 days of hospital stay, a CECT for pseudocysts monitoring was planned after 3 months and it did not present any new pseudoaneurysm formation but, on the other side, it confirmed the presence of the enlarging pancreatic body pseudocysts (12 cm). At four months follow-up, the patient was in good clinical conditions and the Gastroenterology Unit charged her for planning an endoscopic ultrasound-guided drainage of pancreatic pseudocysts.
3. Discussion
Vascular complications, associated with pancreatitis, include hemorrhage due to vascular erosion, pseudoaneurysm and venous thrombosis [12]. AP is rare but potentially lethal disease and it can appear in different clinical conditions, even though it is mostly associated with pancreatitis and pancreatobiliary surgery [13]. AP usually does not occur immediately after an episode of pancreatitis and typically presents itself with bleeding or abdominal pain [14]. Other presenting symptoms might be melena and hypotension due to ongoing bleeding in the gastrointestinal tract, the peritoneum cavity or the retroperitoneum, while on the other hand, AP might be also asymptomatic [15]. In this case, AP was detected after 13 days from acute pancreatitis onset, which was earlier in comparison to literature, where some authors reported pseudoaneurysms occurring 3 to 5 weeks after SAP [7], others from 2 months to 8 years (mean, 2.3 years) [8] and, finally, Bretagne et al. reported a presentation even from 1 to 9 years after SAP (mean, 4 years) [9]. Moreover, AP was occasionally detected with a control CECT and it was completely asymptomatic. Regarding this, guidelines did not define a precise timing for repeating CECT when monitoring an acute pancreatitis [16], but it is recommended to perform CECT at beginning of the late phase of disease to identify patients at increased risk for an adverse outcome [17]. In fact, CECT had nearly 100% of sensitivity in recognizing pseudoaneurysms, even though the tiny one still might only be seen on angiography [6]. In agreement to this, in this case the CECT detected only a pseudoaneurysm of a branch of the right gastric artery and the following angiography showed a further pseudoaneurysm of a branch of the posterior superior pancreaticoduodenal artery. Angiography had the advantage of permitting to treat the pseudoaneurysm with coil embolization, which is the gold standard management for that kind of vessels disease, in hemodynamically stable patients [13], [18]. A particularity of this case was the AP localization in right gastric artery and pancreaticoduodenal artery branches: in literature, the most affected vessel is the splenic artery (up to 50%), followed by gastroduodenal artery (up to 20%) and, finally, pancreaticoduodenal artery (up to 10%), with minor involvement of superior mesenteric and proper hepatic arteries [6], [12]. Although the early phase of SAP is the most critical because of the risk of persistent multi-organ failure onset, the late phase might be marked by life-threatening complications, such as the vascular ones [12], [19]. Therefore, it is important to be aware of pancreatitis-related arterial pseudoaneurysms, as they have a mortality of 90% if not recognized and treated, not only in chronic but also in acute pancreatitis, and to work out a scheduled follow-up with abdominal CECT or pancreatic contrast-enhanced ultrasound [20] in order to control and prevent late onset complications.
4. Conclusions
This was an unusual case of arterial pseudoaneurysm complicating acute pancreatitis because it appeared in an early phase, during the acute process, and it had an uncommon arterial localization. Data from the present case suggest being aware of SAP vascular complications, which might be treated with arterial angioembolization, if promptly recognized.
Competing interests
The authors declare that they have no competing interests.
Author contribution
SO design the study, LM and DA acquire data and draft the article, LC and RS revise it critically for important intellectual content, GV and SO final approved version to be submitted.
Informed consent
Written informed consent was obtained from the patient for publication of this Case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Funding for your research
The authors declare that there is not sources of funding for their research.
Ethical approval
No Ethical Approval has been given.
Consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal on request.
Guarantor
Giorgio Vasquez and Savino Occhionorelli are the guarantors.
Contributor Information
Savino Occhionorelli, Email: savino.occhionorelli@unife.it.
Lucia Morganti, Email: mrglcu@unife.it.
Lorenzo Cappellari, Email: l.cappellari@ospfe.it.
Rocco Stano, Email: r.stano@ospfe.it.
Dario Andreotti, Email: ndrdra@unife.it.
Giorgio Vasquez, Email: vsg@unife.it.
References
- 1.Banks P.A., Freeman M.L. Practice guidelines in acute pancreatitis. Am. J. Gastroenterol. 2006;101(10):2379–2400. doi: 10.1111/j.1572-0241.2006.00856.x. [DOI] [PubMed] [Google Scholar]
- 2.Mole D.J., Olabi B., Robinson V., Garden O.J., Parks R.W. Incidence of individual organ dysfunction in fatal acute pancreatitis: analysis of 1024 death records. HPB (Oxford) 2009;11(2):166–170. doi: 10.1111/j.1477-2574.2009.00038.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Von Flue M., Kocher T., Herzog U., Looser C., Schuppisser J.P. Hemorrhage from pseudocysts caused by pseudoaneurysms in chronic pancreatitis: diagnosis and management. Helv. Chir. Acta. 1993;59(5–6):785–789. [PubMed] [Google Scholar]
- 4.Hagiwara A., Miyauchi H., Shimazaki S. Predictors of vascular and gastrointestinal complications in severe acute pancreatitis. Pancreatology. 2008;8(2):211–218. doi: 10.1159/000128558. [DOI] [PubMed] [Google Scholar]
- 5.Kirby J.M., Vora P., Midia M., Rawlinson J. Vascular complications of pancreatitis: imaging and intervention. Cardiovasc. Intervent. Radiol. 2008;31(5):957–970. doi: 10.1007/s00270-007-9138-y. [DOI] [PubMed] [Google Scholar]
- 6.Verde F., Fishman E.K., Johnson P.T. Arterial pseudoaneurysms complicating pancreatitis: literature review. J. Comput. Assist. Tomogr. 2015;39(1):7–12. doi: 10.1097/RCT.0000000000000153. [DOI] [PubMed] [Google Scholar]
- 7.Dörffel T., Wruck T., Rückert R.I., Romaniuk P., Dörffel Q., Wermke W. Vascular complications in acute pancreatitis assessed by color duplex ultrasonography. Pancreas. 2000;21(2):126–133. doi: 10.1097/00006676-200008000-00004. [DOI] [PubMed] [Google Scholar]
- 8.Balthazar E.J. Complications of acute pancreatitis: clinical and CT evaluation. Radiol. Clin. North Am. 2002;40(6):1211–1227. doi: 10.1016/s0033-8389(02)00043-x. [DOI] [PubMed] [Google Scholar]
- 9.Bretagne J.F., Heresbach D., Darnault P., Raoul J.L., Gosselin M., Carsin M., Gastard J. Pseudoaneurysms and bleeding pseudocysts in chronic pancreatitis: radiological findings and contribution to diagnosis in 8 cases. Gastrointest. Radiol. 1990;15(1):9–16. doi: 10.1007/BF01888725. [DOI] [PubMed] [Google Scholar]
- 10.Banks P.A., Bollen T.L., Dervenis C., Gooszen H.G., Johnson C.D., Sarr M.G. Acute Pancreatitis Classification Working Group: classification of acute pancreatitis-2012: revision of the Atlanta classification and definitions by international consensus. Gut. 2013;62(1):102–111. doi: 10.1136/gutjnl-2012-302779. [DOI] [PubMed] [Google Scholar]
- 11.Mortele K.J., Wiesner W., Intriere L., Shankar S., Zou K.H., Kalantari B.N. A modified CT severity index for evaluating acute pancreatitis: improved correlation with patient outcome. AJR Am. J. Roentgenol. 2004;183(5):1261–1265. doi: 10.2214/ajr.183.5.1831261. [DOI] [PubMed] [Google Scholar]
- 12.Mendelson R.M., Anderson J., Marshall M., Ramsay D. Vascular complications of pancreatitis. ANZ J. Surg. 2005;75(12):1073–1079. doi: 10.1111/j.1445-2197.2005.03607.x. [DOI] [PubMed] [Google Scholar]
- 13.Kalva S.P., Yeddula K., Wicky S., Fernandez del Castillo C., Warshaw A.L. Angiographic intervention in patients with a suspected visceral artery pseudoaneurysm complicating pancreatitis and pancreatic surgery. Arch. Surg. 2011;146(6):647–652. doi: 10.1001/archsurg.2011.11. [DOI] [PubMed] [Google Scholar]
- 14.Agrawal G.A., Johnson P.T., Fishman E.K. Splenic artery aneurysms and pseudoaneurysms: clinical distinctions and CT appearances. AJR Am. J. Roentgenol. 2007;188(4):992–999. doi: 10.2214/AJR.06.0794. [DOI] [PubMed] [Google Scholar]
- 15.Lermite E., Regenet N., Tuech J.J., Pessaux P., Meurette G., Bridoux V. Diagnosis and treatment of hemosuccus pancreaticus: development of endovascular management. Pancreas. 2007;34(2):229–232. doi: 10.1097/MPA.0b013e31802e0315. [DOI] [PubMed] [Google Scholar]
- 16.Besselink M., van Santvoort H., Freeman M., Gardner T., Mayerle J., Vege S.S. Working Group IAP/APA Acute Pancreatitis Guidelines. IAP/APA evidence-based guidelines for the management of acute pancreatitis. Pancreatology. 2013;13(4 Suppl. 2):e1–e15. doi: 10.1016/j.pan.2013.07.063. [DOI] [PubMed] [Google Scholar]
- 17.Brand M., Götz A., Zeman F., Behrens G., Leitzmann M., Brünnler T. Acute necrotizing pancreatitis: laboratory, clinical, and imaging findings as predictors of patient outcome. AJR Am. J. Roentgenol. 2014;202(6):1215–1231. doi: 10.2214/AJR.13.10936. [DOI] [PubMed] [Google Scholar]
- 18.Baiocchi G.L., Piardi T., Cuomo R., Battaglia G., Ronconi M., Coniglio A. Endovascular treatment for bleeding gastroduodenal pseudoaneurysm after acute pancreatitis. Ann. Ital. Chir. 2007;78(2):145–148. [PubMed] [Google Scholar]
- 19.Sharma P.K., Madan K., Garg P.K. Hemorrhage in acute pancreatitis: should gastrointestinal bleeding be considered an organ failure? Pancreas. 2008;36(2):141–145. doi: 10.1097/MPA.0b013e318158466e. [DOI] [PubMed] [Google Scholar]
- 20.Cai D.M., Parajuly S.S., Ling W.W., Li Y.Z., Luo Y. Diagnostic value of contrast enhanced ultrasound for splenic artery complications following acute pancreatitis. World J. Gastroenterol. 2014;20(4):1088–1094. doi: 10.3748/wjg.v20.i4.1088. [DOI] [PMC free article] [PubMed] [Google Scholar]