Abstract
Background
Obturator hernia is a rare condition associated with a high morbidity and mortality. It is an uncommon cause of bowel obstruction most commonly described in elderly females with comorbidity. Surgical intervention is often delayed as a result of subtle presenting signs. Coexisting ipsilateral femoral hernia is an even rarer condition represented by non-exhaustive series in the literature.
Case presentation
We report a case of a healthy 36 years old lady, nulliparous, with abdominal pain and swelling in the right groin. Preoperative CT showed only a right groin hernia, that was found to be femoral at operative intervention. She recovered and was discharged from hospital but represented with further symptoms of obstruction 9 days later. Diagnostic laparoscopy demonstrated a ipsilateral obturator hernia with associated bowel infarct. The bowel was resected and the defect was repaired.
Discussion and Conclusions
Obturator hernia presents subtly with medial thigh pain and no lump. They are notorious for difficulty to diagnosis. We describe the first case of coexisting ipsilateral femoral and obturator hernias in a young nulliparous woman with bowel obstruction. Appropriate intraoperative exploration should always be considered.
Keywords: Obturator hernia, Inguinal hernia, Femoral hernia, Small bowel obstruction
Introduction
Obturator hernia is a rare condition observed most commonly in the elderly, emaciated or multiparous women. It is often referred to as “ the little old lady’s hernia” (1). It is a rare cause of bowel obstruction (0.2–1.6% of all cases of mechanical obstruction of small bowel) but often presents with no specific signs or symptoms. Some classically described signs, though not always present, include obturator neuralgia, the Howship-Romberg sign and the Hannington-Kiff sign. It has an incidence of 0.05–1.4% compared with other abdominal hernias and the most common clinical presentation is intestinal obstruction (90%). The mortality rate can be as high as 70% when associated with acutely strangulated bowel, likely due to the difficulty in diagnosis and delay in surgical treatment (2). In addition, coexisting ipsilateral non-reducible femoral hernia is an even more rare condition represented by non-exhaustive series in the literature, especially in a young woman. This is the first reported case to our knowledge of coexisting obturator and femoral hernias in a young nulliparous women without any significant risk factors. A single report of coexisting hernias has been described in an elderly patient.
Case presentation
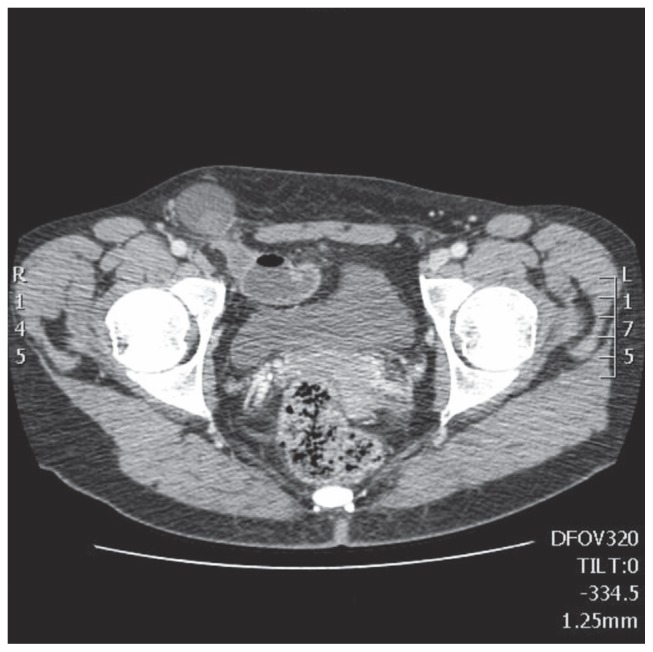
We report a case of a 36-year-old lady who was admitted under our care with abdominal pain and not reducible swelling in the right groin. A pelvic ultrasound scan was performed that showed only a non-specified 3 x 3 cm lump and some free fluid. A CT scan was recommended for further evaluation. The CT imaging was suggestive of a right inguinal hernia containing a loop of obstructed small bowel (Fig. 1).
Figure 1.
The CT imaging suggestive of a right inguinal hernia containing a loop of obstructed small bowel.
The patient was taken to theatre and exploration of the right groin was performed under local anaesthetic and sedation. Intraoperatively a right femoral hernia was identified containing viable small bowel. The bowel was reduced and the hernia was repaired with a polypropelene mesh plug.
Post-operatively she recovered well and was discharged the following day.
On the 9th post-operative day she represented to our hospital with signs of small bowel obstruction; including nausea, vomiting and absolute constipation. Observations showed BP 100/75 mmHg, HR 115/min, SpO2 96% on O2 therapy 2 l, T 37.2°. On examination her abdomen was distended and there was tenderness but no peritonism in the right iliac fossa. Blood tests showed a raised WCC (11.000), CRP (92 mg/L) and lactate (2.1 mmol/L). Naso-gastric tube was placed and 800mls of biliary fluid were drained. An abdominal X-ray showed dilated small bowel loops.
Our initial differential diagnosis was small bowel obstruction secondary to post-operative adhesions or recurrent hernia. Given the raised lactate and relative haemodynamic instability the decision was made to perform urgent diagnostic laparoscopy. Laparoscopy revealed an ipsilateral obstructed obturator hernia with associated small bowel infarction.
After conversion to a lower midline laparotomy the hernia was reduced. The infarcted loop of bowel was resected and a side to side stapled ileo-caecal anastomosis performed. The obturator defect was closed intra-abdominally using interrupted sutures. Mesh repair was not undertaken given the associated risk of mesh infection following bowel resection. The patient recovered well following the second operation and was discharged on the 4th post-operative day.
Discussion
Femoral and obturator hernias are both notorious for difficulty of diagnosis. Femoral hernia should be recognized as a painful non-reducible mass below and lateral to the pubic tubercle. This was suspected on clinical examination on the patient’s first admission however was confused by the CT scan that suggested an inguinal hernia.
Obturator hernia often present more subtly. The sac can irritate the obturator nerve manifesting as medial thigh pain, and often no hernia lump can be detected on clinical examination. A timely CT scan is often the only way to accurately diagnose an obturator hernia. Anatomically the femoral and obturator canals are closely associated which could make them difficult to distinguish on a scan if present concurrently and possibly appear more like a, typically larger, inguinal hernia. Coexisting ipsilateral femoral and obturator hernia should be taken in consideration in cases of intestinal obstruction with inguinal swelling.
Seppala et al. (3) published a case report in the British Medical Journal in 2015 describing the concurrence of right femoral and obturator ipsilateral hernia in a 91 years old lady. She presented to their emergency department with signs of small bowel obstruction but without groin pain or swelling. In this case a CT scan showed a hernia in the right groin area but the diagnosis was delayed. The hernias were repaired using a pre-peritoneal transinguinal approach and the obturator and femoral canals were covered with a Bard Polysoft patch.
The management of obturator hernias is always operative. Traditionally laparotomy has been the most common surgical approach, however, several studies have shown the feasibility of laparoscopic techniques for the management of incarcerated obturator hernia (4). A retrospective analysis of 80 patients at the same institute published in 2014 (5) compared the use of mesh repair to non-mesh repair in case of obturator hernia and concluded that mesh repair is preferable to prevent the recurrence, if no contraindications are present.
Conclusion
Our experience shows that concurrent femoral and obturator hernia in a young nulliparous woman is possible and this diagnosis should be considered in patients who present with small bowel obstruction and inguinal pain and swelling. Unfortunately examination of the groin does not always reveal the underlying diagnosis and performing a CT scan could lead to a time delay to definitive repair and a resultant increase in morbidity and mortality. If a CT scan is not performed, an appropriate intraoperative exploration, such as the pre-peritoneal approach described above, should be mandatory to exclude other complicated hernias.
Acknowledgements
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Footnotes
Conflicts of interest
The authors declare that there is no conflict of interest regarding the publication of this paper.
References
- 1.Durgakeri P, Strauss P, Jones B. Obturator hernia: the ‘little old lady’s hernia’. ANZ journal of surgery. 2014 doi: 10.1111/ans.12903. [DOI] [PubMed] [Google Scholar]
- 2.Petrie A, Tubbs RS, Matusz P, Shaffer K, Loukas M. Obturator hernia: anatomy, embryology, diagnosis, and treatment. Clinical anatomy. 2011;24(5):562–9. doi: 10.1002/ca.21097. [DOI] [PubMed] [Google Scholar]
- 3.Seppala TT, Tuuliranta M. Coexisting ipsilateral right femoral hernia and incarcerated obturator hernia. BMJ case reports. 2015;2015 doi: 10.1136/bcr-2014-208361. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Yokoyama T, Kobayashi A, Kikuchi T, Hayashi K, Miyagawa S. Transabdominal preperitoneal repair for obturator hernia. World journal of surgery. 2011;35(10):2323–7. doi: 10.1007/s00268-011-1211-7. [DOI] [PubMed] [Google Scholar]
- 5.Karasaki T, Nomura Y, Tanaka N. Long-term outcomes after obturator hernia repair: retrospective analysis of 80 operations at a single institution. Hernia: the journal of hernias and abdominal wall surgery. 2014;18(3):393–7. doi: 10.1007/s10029-013-1159-7. [DOI] [PubMed] [Google Scholar]