Abstract
Pediatric obesity is a worldwide health epidemic affecting both developed and developing countries. Mexico ranks second to the United States in rates of pediatric obesity. Obesity among youth has immediate and long-term consequences on physical and psychosocial development, including cardiovascular, respiratory, and health-related quality of life. Eventual amelioration of this epidemic will require change at the level of the family and community, along with policy initiatives to support healthier eating and activity habits. Evidence-based interventions for overweight/obese youth include family-based lifestyle programs that incorporate attention to diet quantity and quality, physical activity, sedentary behavior, and behavioral strategies to support change. While much of this research has been conducted in the United States, several recent studies suggest the efficacy of similar approaches for youth in Mexico.
Keywords: adolescents, behavioral intervention, diet, pediatric obesity, physical activity
INTRODUCTION
Pediatric obesity is a global problem that affects low-, middle-, and high-income countries. Both the United States and Mexico are among countries with the highest prevalence. Given the short- and long-term health and economic consequences of pediatric obesity, interventions are needed in both countries that affect change at all levels of society. This paper reviews the intervention literature at both the clinical and community levels in an effort to highlight strategies that show promise in countries of varying levels of development.
PREVALENCE
Pediatric obesity is widely recognized as a significant public health concern in the United States and internationally. Obesity has been identified as the most common physical health problem among youth and the leading cause of preventable deaths.1 For youth in the United States, weight status is categorized using age- and sex-specific percentiles for body mass index (BMI, kg/m2), with BMI percentiles greater than or equal to the 85th and 95th, respectively, indicating overweight and obesity.2 Prevalence trends over the past several years indicate that the rates of overweight/obesity have stabilized, although data from the most recent National Health and Nutrition Examination Survey indicate that the prevalence of obesity remains high. Among children and adolescents age 2–19 years, 31% of youth are overweight and 17% are obese.1 Notably, there is a substantial health disparity in obesity prevalence, with obesity disproportionately affecting racial and ethnic minority youth.
Similar trends in rates of overweight and obesity have been observed in Mexico. The prevalence of overweight and obesity was examined in a sample of 12- to 18-year-olds from Mexico City using age- and sex-specific international BMI cut-off points, as described by the International Obesity Task Force. Approximately 37% of the sample met criteria for overweight or obesity.3 As in the United States, recent data suggest there may be a stabilization in the prevalence of overweight and obesity among Mexican children.4
COMORBIDITY
Overweight and obesity in childhood may result in a wide range of negative physical health problems, as well as psychosocial concerns. Compared to children and adolescents of healthy weight, overweight youth are at increased risk for deleterious physical health outcomes such as orthopedic complications, type 2 diabetes, asthma, and sleep apnea.5–7 Moreover, pediatric obesity is associated with risk factors for cardiovascular disease including hypertension and atherosclerosis.7,8 Among Mexican adolescents, those who were obese had 3.2 times the odds of having hypertension relative to healthy weight teens (odds ratio [OR], 3.2; 95% confidence interval [CI]: 2.4–4.1). 3 The health effects of childhood obesity can also lead to future disease risk. Pediatric obesity has been linked to obesity in adulthood,9,10 with preadolescents’ weight status shown to be a stronger predictor of adult overweight than parent weight.10
Pediatric obesity is also associated with a number of negative psychosocial concerns, including impairments in health-related quality of life, decreased self-worth, higher body dissatisfaction, and more weight-related teasing by peers and family members.11,12 Findings regarding psychological distress vary based on whether data are drawn from a community or a clinical sample. In clinical samples, obese youth demonstrate higher rates of psychiatric disorders, such as mood and anxiety disorders, compared to healthy-weight peers13 whereas findings among non-treatment-seeking samples are inconclusive.14,15
SOCIOECOLOGICAL MODEL OF PEDIATRIC OBESITY
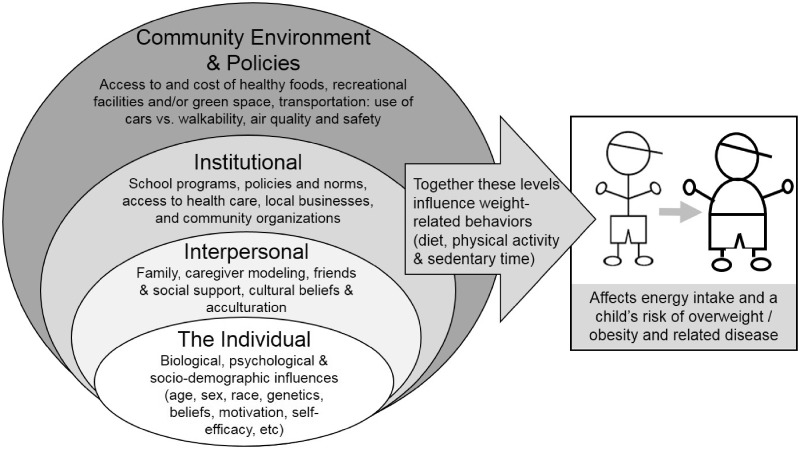
Pediatric obesity is conceptualized as a multifactorial condition that is impacted by individual genetic and behavioral factors, family characteristics, and broader community and societal characteristics (see Figure 1).16 Given that genetics have changed minimally over time, considerable attention has been paid to lifestyle factors, such as changes in diet, increased time in sedentary behavior, and decreased opportunity for physical activity, as important contributors to the obesity epidemic. Nationally representative data from 2013 indicate that over 40% of teens spend more than 3 hours per day playing video games or using computers for non-school-related activities, 32.5% watch television for over 3 hours per day, and the majority (52.7%) do not meet current physical activity recommendations.17 Further, dietary quality has simultaneously declined, with the majority of youth failing to meet recommendations for fruits and vegetables and fat intake.17,18 In a recent examination of dietary intake patterns among Mexican youth, researchers found that very few of them meet dietary recommendations. Specifically, 57.9% consumed fewer than 3 servings of fruit and 54.4% consumed fewer than 2 servings of vegetables per day. Instead, the majority of total calories came from high-fat dairy, refined carbohydrates, and sugar-sweetened beverages.19
Figure 1.
Socioecological model of obesity risk. Abbreviations: CVD, cardiovascular disease; SES, socioeconomic status. Adapted from Gordon-Larsen P (2004).16
LIFESTYLE INTERVENTIONS FOR PEDIATRIC WEIGHT CONTROL
There is considerable evidence to support the efficacy of comprehensive lifestyle interventions for decreasing weight status among overweight and obese youth. Comprehensive programs typically include nutrition recommendations, a physical activity prescription, and behavioral modification. Recommendations regarding diet focus on improving diet quality through targeted behaviors such as decreasing sugar-sweetened beverage intake and increasing consumption of fruits, vegetables, and whole grains, with many programs also including specific calorie targets. Activity prescription includes advising children to obtain 60 minutes of moderate-to-vigorous physical activity daily, typically in briefer (i.e., 10-min) bouts, and to reduce sedentary behavior (i.e., “screen time”) to less than 2 hours per day. These recommendations are supported by the use of behavioral strategies, including self-monitoring of diet and physical activity, goal setting, and reinforcement of positive changes in diet and activity.2 Behavioral interventions for obesity are typically delivered in outpatient settings, most commonly in a group setting. While there are few studies directly comparing group and individual treatments, the group modality is more cost-effective.20
Studies with school-age children support superior short- and long-term outcomes for family-based programs that include a high level of parental involvement.21 Several studies support the fact that treatments involving only parents are as effective, or more effective, than those that include the parent and child,22,23 and more efficacious compared to those that target the child alone.24 The parent-only treatment model is grounded in a systems approach in which the child’s weight is conceptualized as being related to the health behaviors of the entire family. There are potential added benefits to including only parents in a weight control intervention, including greater cost-effectiveness and ease of dissemination.25
Although comprehensive behavioral weight control interventions (i.e., dietary and physical activity prescription combined with behavioral treatment) are effective with school-age children,26,27 relatively fewer interventions have targeted adolescents,28 with inconsistent results.29,30 Likewise, while involving parents in weight control programs for children is clearly superior, the findings with adolescents are inconsistent. In 1 recent study, adolescents were randomly assigned to an enhanced treatment condition that included standard behavioral weight control combined with targeted parent-adolescent communication and parental modeling of healthy behaviors or a standard behavioral intervention with minimal parental involvement.31 Contrary to expectation, the results revealed a trend for adolescents randomized to the condition with minimal parent involvement to demonstrate greater decrease in BMI than those who received the enhanced condition. One potential explanation for this finding is that parental modeling of healthy eating and activity behaviors, considered to be a key factor in supporting weight loss in children, is less salient for adolescents.32
An alternative strategy for engaging adolescents in weight control interventions is enhancing the role of peers. A series of studies suggest that adolescent weight control interventions that focus on enhancing peer support in the group demonstrate positive outcomes. In the first study, adolescents were randomized to group-based behavioral weight control combined with 1 of 2 exercise programs (supervised aerobic vs a peer-enhanced activity based on Outward Bound). Adolescents in both groups demonstrated significant weight loss over time, averaging a 4.5 kg loss.33 In a larger trial comparing the same 2 treatment conditions, findings again indicated significant decreases in measures of weight status (i.e., z-BMI, waist circumference) at the end of intervention, and these were maintained at 12-month follow-up for both treatment conditions.34 Furthermore, decreases in percent overweight were maintained at 24-month follow-up.35 Of note, adolescents randomized to behavioral treatment combined with exercise sessions did as well as those assigned to the more complex peer-enhanced intervention with regard to decrease in weight status, as well as improved self-concept. Consequently, it appears that the process of adolescents engaging in physical activity within a group setting is beneficial in and of itself.
The aforementioned studies were all conducted within the United States. A recent review includes interventions to address pediatric obesity conducted within Mexico.36 The authors identified 6 studies that explicitly targeted a decrease in BMI or other measure of weight status. The interventions tended to incorporate components similar to those reviewed above, including some type of dietary prescription and attention to physical activity, and some included parental involvement. However, only 1 of the interventions, a 12-month, clinic-based randomized controlled trial, was rated as having both good design suitability and execution.37 This randomized controlled trial, consisted of 12 weekly 2-hour group sessions hosted by a registered dietitian followed by monthly visits, and concurrent monthly consultation with a physician. Although study attrition was high, results are promising in that there was a significant difference in BMI in the intervention group as compared to the control group (−2.2 kg/m2; 95% CI, −3.4, −1.0)38. As noted by the authors of the review, more research is warranted to identify intervention components that show the most promise in decreasing BMI in this population. Given the important role of the family in Mexican culture and findings from studies conducted in the United States showing the importance of parental involvement, a focus on involving parents and other caregivers may be particularly relevant.23,39
In addition to leading to decreases in weight status, lifestyle interventions have been associated with improvements in cardiometabolic outcomes.40,41 Children between the ages of 8 and 16 years with BMIs at the 95th percentile or higher were randomly assigned to either standard clinical management or the Bright Bodies program, which included twice weekly meetings for 6 months, followed by meetings every other week for an additional 6 months. The program included a comprehensive approach, incorporating on-site exercise sessions, behavioral modification, and nutrition prescription. The dietary recommendations focused on consumption of moderate portions of low-fat, nutrient-dense foods, and did not include a calorie target. Significant decreases in BMI, total cholesterol, and improvements in fasting insulin and homeostasis model assessment of insulin resistance (HOMA-IR) were observed in participants in the Bright Bodies program at 6 and 12 months.40 At 24 months, total cholesterol and low-density lipoprotein cholesterol were significantly lower in the Bright Bodies condition, and improvements in fasting insulin and HOMA-IR were maintained.41 A recent study similarly demonstrated improvements in cardiorespiratory fitness (VO2 peak) and decreases in low-density lipoprotein and fasting glucose among successful participants in a behavioral weight control program.42
TRANSLATION TO COMMUNITY SETTINGS
As documented above, comprehensive lifestyle interventions are effective in decreasing obesity and improving cardiometabolic outcomes in youth. However, these programs are commonly delivered in academic or hospital settings and are available to a relatively small percentage of the population affected by obesity. In 2010, the US Preventive Services Task Force made a Grade B recommendation for clinicians to screen children between the ages of 6 and 17 years for obesity and refer identified youth to comprehensive programs.43 The inherent challenge with such a recommendation is that there are very few such programs to which primary care physicians are able to refer. JOIN involved collaboration among a large health insurer, United HealthGroup, Y-USA, and the YMCA of Greater Providence (RI) to deliver a pediatric weight control program through area YMCAs.44 A total of 155 youth ranging in age from 6 to 17 years, the majority of whom (92%) were above the 95th percentile BMI, participated in the program across 8 different YMCA locations. Participants under the age of 13 years demonstrated a 4.3% decrease in percent overweight at the end of 6 months, while adolescents (≥13 years) showed a more modest loss (−1.0%).44 Of note, facilitators, who were YMCA staff, were found to be highly adherent to delivering the intervention content, highlighting that lay facilitators can be effectively trained to deliver comprehensive behavioral weight control programs.45
Another community-based intervention that has been widely disseminated is the Mind, Exercise, Nutrition, Do it (MEND) program.46 Consistent with the comprehensive programs described above, the MEND program includes nutrition guidance (e.g., healthy meal preparation, advice for healthy eating), attention to behavioral strategies such as stimulus control, self-monitoring, and reinforcement, and supervised exercise sessions for children. In an initial test of the program, obese children in the United Kingdom were randomly assigned to receive either the MEND program or a waitlist control. Following 6 months, children randomized to the MEND program showed significant decreases in BMI z-score and waist circumference, as well as improvements in cardiovascular health, compared to controls. Moreover, reductions in BMI z-score were maintained at 12 months. A twice weekly, 10-week (2 times/wk) program was subsequently disseminated on a large scale across multiple community venues across England. Data from more than 9000 children between the ages of 7 and 13 years enrolled in MEND indicate that the program was effective in decreasing BMI and zBMI, as well as in enhancing self-concept.47 Based on the success of the program in the United Kingdom, MEND is being included as a secondary prevention approach as part of a comprehensive community-based plan to decrease pediatric obesity among a primarily Latino population in the cities of Austin and Houston, Texas.48
CONCLUSION
Comprehensive behavioral interventions have demonstrated efficacy in improving weight status in children and adolescents. Recent research suggests similar outcomes for interventions conducted in Mexico. Studies with school-age children provide strong support for programs that include parents in interventions with their children or that are targeted to parents alone. Parents play a critical role in modeling healthy eating and activity habits and in providing access to healthy foods and opportunities for physical activity. Parental modeling of healthy eating habits has predicted both child and parent decrease in percent overweight over an extended follow-up period.49 Similarly, change in a parent’s BMI has been related to change in their children’s z-BMI during both active treatment and long-term follow-up.50 Thus, interventions with youth should emphasize the role of parents as recipients of information and as models of healthy behavior for their children.
Lifestyle interventions for youth who already struggle with excess weight occur within the context of broader societal influences, which may serve to support or hinder their efficacy. In the case of Mexico, the government has adopted a comprehensive set of initiatives that are aimed at preventing and controlling obesity and diabetes. One component of this program is implementation of policies to support healthier eating. Specifically, the Mexican government implemented a tax on sugar-sweetened beverages, as well as on energy-dense foods. In addition, regulations were implemented to ban the advertising of unhealthy foods during prime TV viewing hours for children.4 In the context of community-based interventions, such as MEND, which make local environments more supportive of healthy lifestyle behaviors, regulatory initiatives are expected to help with prevention of obesity in youth. Accordingly, to promote the adoption of healthier eating and physical activity habits among children and adolescents who are overweight or obese, both community-based interventions and policy change are needed.
Acknowledgments
The articles in this supplement were presented as part of the Tenth Nestlé Nutrition Conference on Research Perspectives for Prevention of Diabetes: Environment, Lifestyles, and Nutrition, held in México City on November 12 and 13, 2014. The conference was organized by the Nestlé Nutrition Fund of the Mexican Health Foundation and the National Institute of Medicine and Nutrition Salvador Zubirán. The supplement coordinators are Ernestina Polo-Oteyza, Mexican Health Foundation and Héctor Bourges-Rodríguez and Carlos Aguilar-Salinas, National Institute of Medicine and Nutrition Salvador Zubirán, México.
Funding. This work was supported, in part, by grant R34DK100981 from the National Institute of Diabetes and Digestive and Kidney Diseases (to E.J.). The conference and this supplement were funded by the Nestlé Nutrition Fund of the Mexican Foundation for Health.
Declaration of interest. The authors have no relevant interests to declare.
REFERENCES
- 1.Ogden CL, Carroll MD, Kit BK, et al. Prevalence of childhood and adult obesity in the United States, 2011-2012. JAMA. 2014;311:806–814. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Barlow S. Expert committee recommendations regarding the prevention, assessment and treatment of child and adolescent overweight and obesity: summary report. Pediatrics. 2007;120:S164–S192. [DOI] [PubMed] [Google Scholar]
- 3.Dyson PA, Anthony D, Fenton B, et al. High rates of child hypertension associated with obesity: a community survey in China, India and Mexico. Paediatr Int Child Health. 2014;34:43–49. [DOI] [PubMed] [Google Scholar]
- 4.Organisation for Economic Cooperation and Development. Obesity Update 2014. http://www.oecd.org/els/health-systems/Obesity-Update-2014.pdf. Published 2014. Accessed May 28, 2015.
- 5.Lazorick S, Peaker B, Perrin EM, et al. Prevention and treatment of childhood obesity: care received by a state medicaid population. Clin Pediatr (Phila). 2011;50:816–826. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Pulgaron ER. Childhood obesity: a review of increased risk for physical and psychological comorbidities. Clin Ther. 2013;35:A18–A32. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Daniels SR. Complications of obesity in children and adolescents. Int J Obes (Lond). 2009;33(Suppl 1):S60–S65. [DOI] [PubMed] [Google Scholar]
- 8.Farpour-Lambert NJ, Aggoun Y, Marchand LM, et al. Physical activity reduces systemic blood pressure and improves early markers of atherosclerosis in pre-pubertal obese children. J Am Coll Cardiol. 2009;54:2396–2406. [DOI] [PubMed] [Google Scholar]
- 9.Freedman DS, Khan LK, Serdula MK, et al. Racial differences in the tracking of childhood BMI to adulthood. Obesity Res. 2005;13:928–935. [DOI] [PubMed] [Google Scholar]
- 10.Magarey AM, Daniels LA, Boulton TJ, et al. Predicting obesity in early adulthood from childhood and parental obesity. Int J Obes Relat Metab Disord. 2003;27:505–513. [DOI] [PubMed] [Google Scholar]
- 11.Schwimmer JB, Burwinkle TM, Varni JW. Health-related quality of life of severely obese children and adolescents. JAMA. 2003;289:1813–1819. [DOI] [PubMed] [Google Scholar]
- 12.Wardle J, Cooke L. The impact of obesity on psychological well-being. Best Pract Res Clin Endocrinol Metab. 2005;19:421–440. [DOI] [PubMed] [Google Scholar]
- 13.Erermis S, Cetin N, Tamar M, et al. Is obesity a risk factor for psychopathology among adolescents? Pediatr Int. 2004;46:296–301. [DOI] [PubMed] [Google Scholar]
- 14.Crow S, Eisenberg ME, Story M, et al. Psychosocial and behavioral correlates of dieting among overweight and non-overweight adolescents. J Adolesc Health. 2006;38:569–574. [DOI] [PubMed] [Google Scholar]
- 15.Tanofsky-Kraff M, Yanovski SZ, Wilfley DE, et al. Eating-disordered behaviors, body fat, and psychopathology in overweight and normal-weight children. J Consult Clin Psychol. 2004;72:53–61. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Gordon-Larsen P. Add health: the obesity and environment project. Presentation at NHLBI workshop: predictors of obesity, weight gain, diet and physical activity; August 2004 Bethesda, MD. [Google Scholar]
- 17.Kann L, Kinchen S, Shanklin SL, et al. Youth risk behavior surveillance–United States, 2013. MMWR Suppl. 2014;63(Suppl 4):1–168. [PubMed] [Google Scholar]
- 18.Sanchez A, Norman GJ, Sallis JF, et al. Patterns and correlates of physical activity and nutrition behaviors in adolescents. Am J Prev Med. 2007;32:124–130. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Perichart-Perera O, Balas-Nakash M, Rodríguez-Cano A, et al. Correlates of dietary energy sources with cardiovascular disease risk markers in Mexican school-age children. J Am Diet Assoc. 2010;110:253–260. [DOI] [PubMed] [Google Scholar]
- 20.Goldfield GS, Epstein LH, Kilanowski CK, et al. Cost-effectiveness of group and mixed family-based treatment for childhood obesity. Int J Obes Relat Metab Disord. 2001;25:1843–1849. [DOI] [PubMed] [Google Scholar]
- 21.Epstein LH, Valoski A, Wing RR, et al. Ten-year follow-up of behavioral, family-based treatment for obese children. JAMA. 1990;264:2519–2523. [PubMed] [Google Scholar]
- 22.Boutelle KN, Cafri G, Crow SJ. Parent-only treatment for childhood obesity: a randomized controlled trial. Obesity (Silver Spring). 2011;19:574–580. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Janicke DM, Sallinen BJ, Perri MG, et al. Comparison of parent-only vs family-based interventions for overweight children in underserved rural settings: outcomes from project STORY. Arch Pediatr Adolesc Med. 2008;162: 1119–1125. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Golan M, Crow S. Targeting parents exclusively in the treatment of childhood obesity: long-term results. Obes Res. 2004;12:357–361. [DOI] [PubMed] [Google Scholar]
- 25.Janicke DM. Treatment of pediatric obesity using a parent-only approach: a case example. Health Psychol. 2013;32:345–350. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Jelalian E, Saelens BE. Empirically supported treatments in pediatric psychology: Pediatric obesity. J Pediatr Psychol. 1999;24:223–248. [DOI] [PubMed] [Google Scholar]
- 27.Wilfley DE, Tibbs TL, Van Buren D, et al. Lifestyle interventions in the treatment of childhood overweight: A meta-analytic review of randomized controlled trials. Health Psychol. 2007;26:521–532. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Butryn ML, Wadden TA, Rukstalis MR, et al. Maintenance of weight loss in adolescents: current status and future directions. J Obes. 2010;2010:789280. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Jelalian E, Hart CN, Mehlenbeck RS, et al. Predictors of attrition and weight loss in an adolescent weight control program. Obesity. 2008;16:1318–1323. [DOI] [PubMed] [Google Scholar]
- 30.Oude Luttikhuis H, Baur L, Jansen H, et al. Interventions for treating obesity in children. Cochrane Database Syst Rev. 2009:CD001872. [DOI] [PubMed] [Google Scholar]
- 31.Jelalian E, Hadley W, Sato AF, et al. Adolescent weight control: an intervention targeting parent communication and modeling compared with minimal parental involvement. J Pediatr Psychol. 2015;40:203–213. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Wrotniak BH, Epstein LH, Paluch RA, et al. The relationship between parent and child self-reported adherence and weight loss. Obesity Res. 2005;13:1089–1096. [DOI] [PubMed] [Google Scholar]
- 33.Jelalian E, Mehlenbeck R, Lloyd-Richardson EE, et al. ‘Adventure therapy' combined with cognitive-behavioral treatment for overweight adolescents. Int J Obes 2006;30:31–39. [DOI] [PubMed] [Google Scholar]
- 34.Jelalian E, Lloyd-Richardson EE, Mehlenbeck RS, et al. Behavioral weight control treatment with supervised exercise or peer-enhanced adventure for overweight adolescents. J Pediatr. 2010;157:923–928. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Lloyd-Richardson EE, Jelalian E, Sato AF, et al. Two-year follow-up of an adolescent behavioral weight control intervention. Pediatrics. 2012;130:e281–e288. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Eisenberg CM, Sánchez-Romero LM, Rivera-Dommarco JA, et al. Interventions to increase physical activity and healthy eating among overweight and obese children in Mexico. Salud Pública Méx. 2013;55:441–446. [DOI] [PubMed] [Google Scholar]
- 37.Diaz R, Esparza-Romero J, Moya-Camarena S, et al. Lifestyle intervention in primary care settings improves obesity parameters among Mexican youth. J Am Diet Assoc. 2010;110:285–290. [DOI] [PubMed] [Google Scholar]
- 38.Diaz RG, Esparza-Romero J, Moya-Camarena SY, et al. Lifestyle intervention in primary care settings improves obesity parameters among Mexican youth. J Am Diet Assoc. 2010;110:285–290. [DOI] [PubMed] [Google Scholar]
- 39.Boutelle KN, Cafri G, Crow SJ. Parent-only treatment for childhood obesity: a randomized controlled trial. Obesity. 2011;19:574–580. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Savoye M, Shaw M, Dziura J, et al. Effects of a weight management program on body composition and metabolic parameters in overweight children: a randomized controlled trial. JAMA. 2007;297:2697–2704. [DOI] [PubMed] [Google Scholar]
- 41.Savoye M, Nowicka P, Shaw M, et al. Long-term results of an obesity program in an ethnically diverse pediatric population. Pediatrics. 2011;127:402–410. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Browning MG, Bean MK, Wickham EP, et al. Cardiometabolic and fitness improvements in obese girls who either gained or lost weight during treatment. J Pediatr. 2015;166:1364–1369. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.United States Preventive Services Task Force. Screening for obesity in children and adolescents: US preventive services task force recommendation statement. Pediatrics. 2010;125:361–367. [DOI] [PubMed] [Google Scholar]
- 44.Foster GD, Sundal D, McDermott C, et al. Feasibility and preliminary outcomes of a scalable. Community-based treatment of childhood obesity. Pediatrics. 2012;130:652–659. [DOI] [PubMed] [Google Scholar]
- 45.Jelalian E, Foster GD, Sato AF, et al. Treatment adherence and facilitator characteristics in a community based pediatric weight control intervention. Int J Behav Nutr Phys Act. 2014;11:17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Sacher PM, Kolotourou M, Chadwick PM, et al. Randomized controlled trial of the MEND program: a family-based community intervention for childhood obesity. Obesity. 2010;18(Suppl 1):S62–S68. [DOI] [PubMed] [Google Scholar]
- 47.Fagg J, Cole TJ, Cummins S, et al. After the RCT: who comes to a family-based intervention for childhood overweight or obesity when it is implemented at scale in the community? J Epidemiol Community Health. 2015;69:142–148. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Hoelscher D, Blanck H, Ayala G. Childhood Obesity Research Demonstration (CORD) Project: implementing strategies across the community to help families with childhood obesity. https://sph.uth.edu/research/centers/dell/webinars/CORD-webinar_3-17-2015.pdf. Published 2015. Accessed May 28, 2015.
- 49.Wrotniak BH, Epstein LH, Paluch RA, et al. The relationship between parent and child self-reported adherence and weight loss. Obesity Res. 2005;13:1089–1096. [DOI] [PubMed] [Google Scholar]
- 50.Wrotniak BH, Epstein LH, Paluch RA, et al. Parent weight change as a predictor of child weight change in family-based behavioral obesity treatment. Arch Pediatr Adolesc Med. 2004;158:342–347. [DOI] [PubMed] [Google Scholar]