Abstract
Purpose
The aim of this study was to investigate the clinical features and extraintestinal manifestations (EIMs) of Crohn disease (CD) in Korean pediatric patients.
Methods
The medical records of 73 children diagnosed with CD were retrospectively reviewed. Data regarding baseline demographic and clinical characteristics, including CD phenotype at diagnosis based on the Montreal classification, and clinical features and course of EIMs were investigated.
Results
Fifty-two (71.2%) of the patients were males. The mean age of the patients was 12.5 years. The mean follow-up period was 3.4 years. The disease location was ileal in 3 (4.1%) of the patients, colonic in 13 (17.8%), ileocolonic in 56 (76.7%). The clinical behavior was inflammatory in 62 (84.9%) of the patients, stricturing in 8 (11.0%), and penetrating in 3 (4.1%). Perianal abscesses or fistulas were found in 37 (50.7%) of the patients. EIMs observed during the study period were anal skin tag in 25 patients (34.2%), hypertransaminasemia in 20 (27.4%), peripheral arthritis in 2 (2.7%), erythema nodosum in 2 (2.7%), vulvitis in 1 (1.4%), uveitis in 1 (1.4%), and pulmonary thromboembolism in 1 (1.4%).
Conclusion
Perianal diseases and manifestations were present in more than half of Korean pediatric CD patients at diagnosis. Inspection of the anus should be mandatory in Korean children with suspicious CD, as perianal fistulas, abscesses, and anal skin tags may be the first clue to the diagnosis of CD.
Keywords: Crohn disease, Extraintestinal, Children
INTRODUCTION
The incidence of inflammatory bowel disease (IBD) in pediatric and adolescent patients has increased. It is estimated that 15% to 25% of patients experience the onset of symptoms before 20 years of age [1]. In particular, reports have shown an increasing incidence of pediatric Crohn disease (CD) in the last decades [2,3]. The epidemiologic and clinical characteristics of CD seem to differ among ethnic groups, but data on the clinical course of pediatric CD are scarce.
Patients with CD frequently manifest a spectrum of clinical symptoms and signs due to a combination of intestinal and extraintestinal lesions. The pathogenesis of extraintestinal manifestations (EIMs) with CD is poorly understood. An immune mechanism has been suspected because of some of the lesions that accompany CD, such as those involving the skin, joints, eye, mouth, and hepatobiliary tract [4]. The EIMs of CD have been reported to involve almost every organ system. Sometimes it can be difficult to differentiate true EIMs from secondary extraintestinal complications. Some EIMs may not correlate with disease activity but in general EIMs tend to follow the clinical course of IBD [5]. The incidence of the EIMs of IBD in previous studies has ranged from 21-41%, depending on the patient population and criteria used [6]. EIMs were more common in CD than ulcerative colitis (UC) and the clinical spectrum of EIMs varied from mild transitory to very severe lesions [6].
Although about 25% of Crohn patients are diagnosed as children and adolescents, and their clinical features differ from those of adults [7], only a few Korean studies involving a small number of patients have been published to date [8,9,10]. Data on the differences between the EIMs of IBD in children and adults are also lacking. Understanding the prevalence and clinical course of the EIMs in children with CD is necessary to provide guidelines for the appropriate management of CD.
Therefore we aimed to investigate the clinical features and EIMs of CD in Korean pediatric patients.
MATERIALS AND METHODS
The medical records of 73 children diagnosed with CD between July 1995 and June 2011 at Pusan National University Hospital and Pusan National University Children's Hospital were reviewed retrospectively. We evaluated the baseline demographic and clinical characteristics including sex, age, follow-up duration, CD phenotype at diagnosis, clinical features and course of EIMs, and the drugs used for treatment.
The diagnosis of CD was based on the clinical features in combination with endoscopic and radiologic findings, and in most cases it was supplemented by results from histologic examinations. CD phenotype at diagnosis was assessed using the Montreal Classification [11]. The CD location and the disease behavior were determined at the time of diagnosis. The EIMs were determined at diagnosis and during follow-up.
Arthritis was defined as pain, swelling, redness, and warmth in one or more joints. Erythema nodosum was diagnosed when tender, red nodules, mainly on the extensor surface of the legs, were observed. The skin lesions were diagnosed by dermatologists. Patients with suspicious iritis or painful uveitis underwent ocular examinations by ophthalmologists. Hepatobiliary involvement was suspected when abnormal liver biochemistry results had been detected. For the diagnosis of pulmonary thromboembolism (TE) in one patient, a ventilation-perfusion scan and angiography were performed.
RESULTS
Characteristics of patients with CD
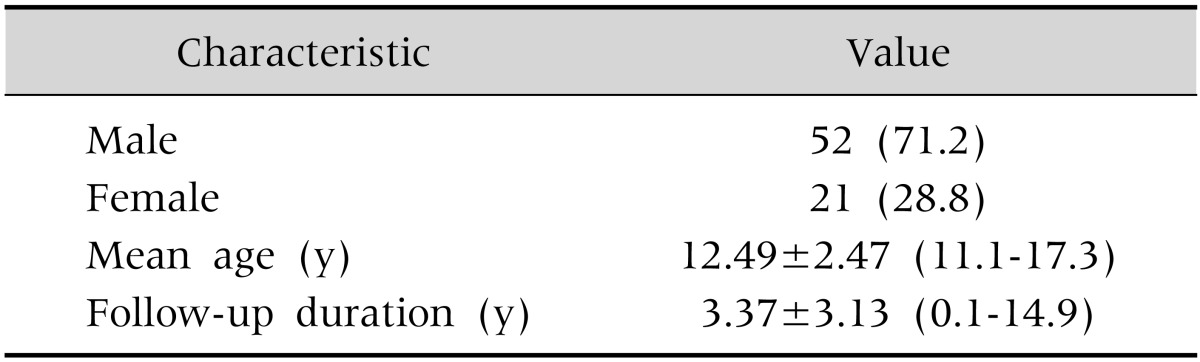
Among the 73 study patients, 52 (71.2%) of the patients were male and the male/female ratio was 2.5:1. The mean age at diagnosis was 12.49±2.47 (range, 11.1-17.3) years. The duration of follow-up after diagnosis was 3.37±3.13 (range, 0.1-14.9) years (Table 1).
Table 1. Baseline Characteristics of Patients with Crohn Disease (n=73).
Values are presented as number (%) or mean±standard deviation (range).
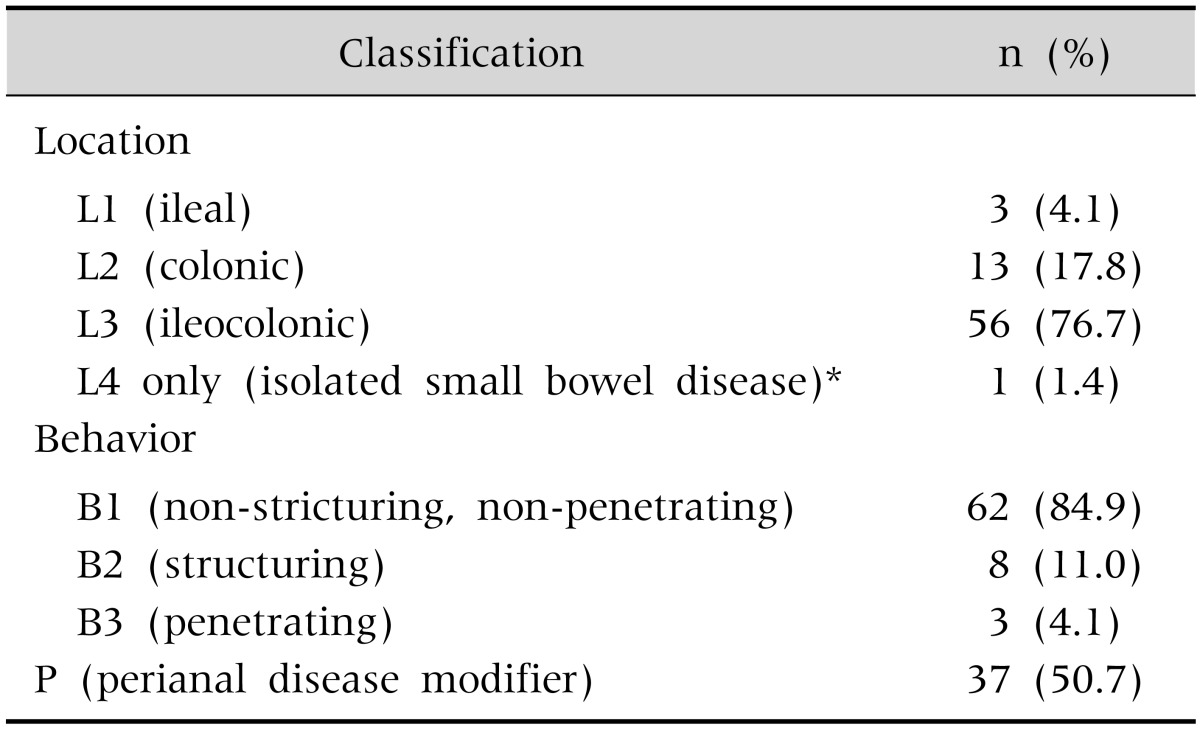
At diagnosis, 56 patients (76.7%) had ileocolonic disease, 13 (17.8%) had isolated colonic disease, and 3 (4.1%) had ileal disease. There was one case of isolated upper disease confirmed by capsule endoscopy (Table 2). With respect to the behavior of the disease, non-stricturing, non-penetrating type was present in 62 patients (84.9%), stricturing in 8 (11.0%), and penetrating in 3 (4.1%). Perianal abscesses or fistulas were found in 37 patients (50.7%) (Table 2).
Table 2. Montreal Classification of Patients with Crohn Disease (n=73).
*Crohn disease was diagnosed with wireless capsule endoscopy.
Treatment of patients with CD
Systemic corticosteroids were administered to all patients (100.0%) for remission induction. Oral 5-aminosalicylic acids (5-ASA) only or 5-ASA plus azathioprine was used for maintenance therapy in 43 (58.9%) and 30 (41.1%) patients, respectively. A total of 17 patients (23.3%) failed remission induction or maintenance and were successfully treated with infliximab.
EIMs of patients with CD
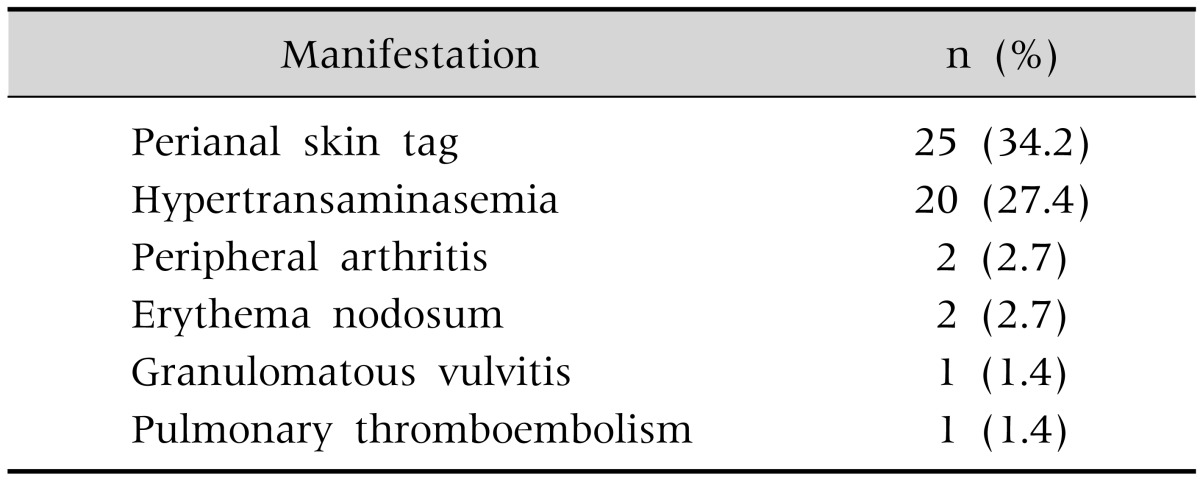
The EIMs of the patients with CD included anal skin tags in 25 patients (34.2%), hypertransaminasemia in 20 (27.4%), peripheral arthritis in 2 (2.7%), erythema nodosum in 2 (2.7%), vulvitis in 1 (1.4%), uveitis in 1 (1.4%), and pulmonary TE in 1 (1.4%) (Table 3).
Table 3. Extraintestinal Manifestations of Patients with Crohn Disease (n=73).
Anal skin tags developed in 25 patients (34.2%) (19 male, 6 female). The location of the disease was the small bowel and colon in 15 (60.0%) patients, isolated colon in 8 (32.0%), and isolated small bowel in 2 patients (8.0%).
Hypertransaminasemia developed in 20 (27.4%) patients. The alanine aminotransferase (ALT) level was 116.4±86.1 IU/L (range, 40-346 IU/L). The duration of ALT elevation was 2.4±1.7 months (range, 10 days-6 months). Hepatitis developed at the time CD was diagnosed in one patient (5.0%), during the induction period in 11 patients (55.0%), and during the maintenance period in 8 (40.0%) patients. The hepatitis resolved in all of the patients without specific treatment.
One of the two patients with peripheral arthritis was a 14-year-old boy who had pain in both knees. The joint symptom developed during the maintenance therapy, and the patient developed hepatitis at the same time. The other patient was a 14-year-old girl who had right knee pain. Arthritis developed when she elected to stop medical treatment. The disease was located in the ileum and colon in both patients. The symptoms disappeared several months after they resumed medical treatment.
Erythema nodosum developed in two patients, an 11-year-old and 14-year-old boy, whose lesion sites were the colon only and the ileum and colon, respectively. The skin lesions developed before they were diagnosed with gastrointestinal CD and disappeared after they underwent treatment with corticosteroids.
Vulvitis developed in a 10-year-old girl and was her presenting symptom of CD. Crohn vulvitis was diagnosed by skin biopsy of the lesion. The location of the disease in this patient was the ileum. The skin lesion did not resolve during treatment of the disease.
Uveitis developed in a 14-year-old boy whose lesion site was the colon only, and the condition resolved 1 month after treatment.
A pulmonary TE developed in an 11-year-old boy whose presenting symptom was severe hematochezia probably due to the TE. The initial abdominal computed tomography (CT) revealed enlargement of the right ileocolic branch. Despite proper medical treatment, intermittent severe hematochezia continued. The patient eventually received right hemicolectomy and segmental resection of the ileum to control the bleeding. The patient developed repetitive hemoptysis 2 years later. The follow-up CT scan demonstrated dilatation of the main pulmonary artery and the right pulmonary artery, and obliteration of the pulmonary vein. Pulmonary hypertension was detected by cardiac angiography. The initial location of this patient was the ileum.
Most of the EIMs developed prior to the diagnosis of CD or during relapse of the intestinal lesions in our study. All of the EIMs, except the perianal skin tags, vulvitis and pulmonary TE, resolved during treatment of the intestinal disease of CD.
DISCUSSION
This is the first study in Korean pediatric CD patients to investigate the EIMs associated with CD. Despite the limitations related with the small number of patients included in this study, we were capable of finding that diseases or manifestations involving the anus or the perianal region occurred in more than half of Korean children with Crohn's disease at diagnosis.
In our study, the incidence of CD showed a male predominance (2.5:1), as was also reported in Korean pediatric (2.2:1)[10] and adult (2.2:1) [12] studies. Male predominance was also reported in Western pediatric studies [13-15]. However, recent large-scale studies in Western pediatric CD patients have shown a lower male predominance of a male-to-female sex ratio of 1.43-1.45:1 [3,16] compared to our study, suggesting a gender difference between Caucasian and Korean ethnicity in the pediatric population of CD. Further large-scale prospective studies are required in order to clarify this difference, considering the small-scale and retrospective design of our study. Meanwhile, the mean diagnosis age of patients in our study was similar to the results of other Korean and Western pediatric studies which ranged from 11.4 to 13.2 years [3,10,16].
Most of the patients with CD in our study had disease in both the small bowel and colon (76.7%). and non-stricturing and non-penetrating behavior (84.9%), results similar to other reports on Korean children [10] and adults [12]. Kim et al. [10] reported that 75% of children with CD presented with both small bowel and colonic involvement, and 85% of patients had inflammatory behavior. Ye et al. [12] reported that 67.3% of the adults with CD in their sample had disease in both the small bowel and colon. However, the number of patients with stricturing and penetrating behavior increased from 31.3% at the time of diagnosis to 50.7% at the final evaluation. This discrepancy between our study's and Ye et al.'s findings [12] may have resulted from the differences in the follow-up periods and the contraction of disease. The Western study of Müller et al. [3] reported that 58.7% of children with CD had ileocolonic disease and 84.4% had inflammatory behavior. Another recent European study reported that ileocolonic disease was seen at presentation in 53% of patients, and nonstricturing and nonpenetrating disease in 82% [16].
The rate of perianal abscesses or fistulas in our study was high (50.7%), and these findings were similar to those reported in other Korean pediatric (63.0%) [10] and adult (46.8%) [12] studies. However, Western studies by Müller et al. [3] and Palder et al. [17] reported perianal disease rates of 14.5% and 28.0% in children with CD, respectively. Another European study reported that perianal disease (presence of fistula and/or abscess) at diagnosis was seen in 9% of pediatric CD patients [16].
The proportion of patients with anal skin tags in our study was relatively higher compared to previous studies which ranged from 21% to 29% in CD patients [10,18]. Anal skin tags are one of the anorectal malformations of CD; they are flesh colored and waxy in appearance, painless, can be raised and firm, narrow or broad, and patients are more likely to develop multiple tags than isolated tags [18]. Taylor et al. [19] reported that granulomas were more frequently found in anal skin tags than in rectal biopsies (34.6% vs. 30.8%) of patients with CD. Studies on anal skin tags as a potential predictor of CD may be an interesting topic for investigation in the future.
Although there is limited data regarding the occurrence of EIM in pediatric IBD patients, it seems that one quarter to almost half of them experience at least 1 EIM at the time of diagnosis [20]. Veloso [6] reported that the inflammatory EIMs (peripheral arthritis, erythema nodosum, pyoderma gangrenosum, iritis/uveitis, and aphthous stomatitis) occurred at least once in 25.8% of pediatric and adult patients with IBD, and these manifestations were more common in CD than in UC. They were also more common in patients with colonic involvement than in patients with ileal disease. The cumulative probability of a second manifestation was about 70% after 10 years of follow-up [21].
The proportion of EIMs observed in our study was similar to this study in which a single EIM occurred in 60.5% of patients, whereas multiple manifestations occurred in 39.5%. Müller et al. [3], however, reported that 12.5% of children with CD had EIMs. This big discrepancy regarding the incidence of EIMs between these reports may have resulted from different inclusion criteria. The overall rate of EIM will vary based on which conditions are included as an EIM, as well as the period of follow-up. When EIMs are more broadly defined to include other systemic effects such as growth delay, nutritional deficiency, anemia, decreased bone mineral density, and fatigue, the rate of EIMs could approach 100% [20].
Elevations in transaminases were reported in up to 17% of the patients with IBD [22]. Primary sclerosing cholangitis and autoimmune hepatitis are important causes of elevated liver enzymes in these patients. Medications used to treat IBD such as sulfasalazine, thiopurine, and methotrexate can also have adverse effects on the liver [23]. There are conflicting opinions about etiology of transient hypertransaminasemia in pediatric CD patients undergoing their initial treatment with enteral nutrition [24,25]. In our study, modest and transient hypertransaminasemia developed in 27.4% of the patients.
Several studies have suggested that there is an increased risk of venous and arterial TE in adults with IBD. Sonoda et al. [26] reported that a venous TE was detected in 8 of 47 consecutive Japanese patients with active IBD (17.0%). Guerra Montero et al. [27] reported that 15 of 515 IBD patients (2.9%) had thromboembolic events, and they were more common in patients with extensive disease, colonic involvement, and other EIMs. Lazzerini et al. [28] reported that TE in children with IBD occurred most often during active disease (82.8%) and more frequently in UC. The sites of the TE were the cerebral vessels (54.3%), the vessels in the limbs (26.0%), the abdominal vessels (13.0%), and the vessels in the retina and lungs (6.7%). Nylund et al. [29] reported that hospitalized children and adolescents with IBD are at increased risk for TE. Conservative methods such as hydration, mobilization, and pneumatic devices should be considered to prevent TE in hospitalized children with IBD.
There are some limitations in this study. Since this is a single-center study, common EIMs of CD such as pyoderma gangrenosum, primary sclerosing cholangitis and psoriasis were not observed. The small number of patients and the short follow-up period may have resulted in observational bias. A further prospective population-based study in pediatric CD is needed to accurately estimate the incidence of EIMs and their natural course.
In conclusion, perianal diseases and manifestations occur in more than half of Korean pediatric CD patients, which may be the first clue in diagnosing CD. Therefore, inspection of the anus should be mandatory in Korean children with suspicious CD.
ACKNOWLEDGEMENTS
This work was supported by a 2-year research grant of Pusan National University.
References
- 1.Goodhand J, Hedin CR, Croft NM, Lindsay JO. Adolescents with IBD: the importance of structured transition care. J Crohns Colitis. 2011;5:509–519. doi: 10.1016/j.crohns.2011.03.015. [DOI] [PubMed] [Google Scholar]
- 2.Benchimol EI, Fortinsky KJ, Gozdyra P, Van den Heuvel M, Van Limbergen J, Griffiths AM. Epidemiology of pediatric inflammatory bowel disease: a systematic review of international trends. Inflamm Bowel Dis. 2011;17:423–439. doi: 10.1002/ibd.21349. [DOI] [PubMed] [Google Scholar]
- 3.Müller KE, Lakatos PL, Arató A, Kovács JB, Várkonyi Á, Szűcs D, et al. Incidence, Paris classification, and follow-up in a nationwide incident cohort of pediatric patients with inflammatory bowel disease. J Pediatr Gastroenterol Nutr. 2013;57:576–582. doi: 10.1097/MPG.0b013e31829f7d8c. [DOI] [PubMed] [Google Scholar]
- 4.Veloso FT, Carvalho J, Magro F. Immune-related systemic manifestations of inflammatory bowel disease. A prospective study of 792 patients. J Clin Gastroenterol. 1996;23:29–34. doi: 10.1097/00004836-199607000-00009. [DOI] [PubMed] [Google Scholar]
- 5.Rothfuss KS, Stange EF, Herrlinger KR. Extraintestinal manifestations and complications in inflammatory bowel diseases. World J Gastroenterol. 2006;12:4819–4831. doi: 10.3748/wjg.v12.i30.4819. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Veloso FT. Extraintestinal manifestations of inflammatory bowel disease: do they influence treatment and outcome? World J Gastroenterol. 2011;17:2702–2707. doi: 10.3748/wjg.v17.i22.2702. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Mamula P, Markowitz JE, Baldassano RN. Inflammatory bowel disease in early childhood and adolescence: special considerations. Gastroenterol Clin North Am. 2003;32:967–995. doi: 10.1016/s0889-8553(03)00046-3. [DOI] [PubMed] [Google Scholar]
- 8.Seo JK, Yeon KM, Chi JG. Inflammatory bowel disease in children--clinical, endoscopic, radiologic and histopathologic investigation. J Korean Med Sci. 1992;7:221–235. doi: 10.3346/jkms.1992.7.3.221. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Lee NY, Park JH. Clinical features and course of Crohn disease in children. Korean J Gastrointest Endosc. 2007;34:193–199. [Google Scholar]
- 10.Kim BJ, Song SM, Kim KM, Lee YJ, Rhee KW, Jang JY, et al. Characteristics and trends in the incidence of inflammatory bowel disease in Korean children: a single-center experience. Dig Dis Sci. 2010;55:1989–1995. doi: 10.1007/s10620-009-0963-5. [DOI] [PubMed] [Google Scholar]
- 11.Silverberg MS, Satsangi J, Ahmad T, Arnott ID, Bernstein CN, Brant SR, et al. Toward an integrated clinical, molecular and serological classification of inflammatory bowel disease: report of a working party of the 2005 montreal world congress of gastroenterology. Can J Gastroenterol. 2005;19(Suppl A):5A–36A. doi: 10.1155/2005/269076. [DOI] [PubMed] [Google Scholar]
- 12.Ye BD, Yang SK, Cho YK, Park SH, Yang DH, Yoon SM, et al. Clinical features and long-term prognosis of Crohn's disease in Korea. Scand J Gastroenterol. 2010;45:1178–1185. doi: 10.3109/00365521.2010.497936. [DOI] [PubMed] [Google Scholar]
- 13.Spray C, Debelle GD, Murphy MS. Current diagnosis, management and morbidity in paediatric inflammatory bowel disease. Acta Paediatr. 2001;90:400–405. [PubMed] [Google Scholar]
- 14.Sawczenko A, Sandhu BK. Presenting features of inflammatory bowel disease in Great Britain and Ireland. Arch Dis Child. 2003;88:995–1000. doi: 10.1136/adc.88.11.995. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Kugathasan S, Judd RH, Hoffmann RG, Heikenen J, Telega G, Khan F, et al. Epidemiologic and clinical characteristics of children with newly diagnosed inflammatory bowel disease in Wisconsin: a statewide population-based study. J Pediatr. 2003;143:525–531. doi: 10.1067/s0022-3476(03)00444-x. [DOI] [PubMed] [Google Scholar]
- 16.de Bie CI, Paerregaard A, Kolacek S, Ruemmele FM, Koletzko S, Fell JM, et al. Disease phenotype at diagnosis in pediatric Crohn's disease: 5-year analyses of the EUROKIDS registry. Inflamm Bowel Dis. 2013;19:378–385. doi: 10.1002/ibd.23008. [DOI] [PubMed] [Google Scholar]
- 17.Palder SB, Shandling B, Bilik R, Griffiths AM, Sherman P. Perianal complications of pediatric Crohn's disease. J Pediatr Surg. 1991;26:513–515. doi: 10.1016/0022-3468(91)90694-o. [DOI] [PubMed] [Google Scholar]
- 18.Korelitz BI. Anal skin tags: an overlooked indicator of Crohn's disease. J Clin Gastroenterol. 2010;44:151–152. doi: 10.1097/MCG.0b013e3181c21d20. [DOI] [PubMed] [Google Scholar]
- 19.Taylor BA, Williams GT, Hughes LE, Rhodes J. The histology of anal skin tags in Crohn's disease: an aid to confirmation of the diagnosis. Int J Colorectal Dis. 1989;4:197–199. doi: 10.1007/BF01649703. [DOI] [PubMed] [Google Scholar]
- 20.Dotson JL, Hyams JS, Markowitz J, LeLeiko NS, Mack DR, Evans JS, et al. Extraintestinal manifestations of pediatric inflammatory bowel disease and their relation to disease type and severity. J Pediatr Gastroenterol Nutr. 2010;51:140–145. doi: 10.1097/MPG.0b013e3181ca4db4. [DOI] [PubMed] [Google Scholar]
- 21.Veloso FT, Ferreira JT, Barros L, Almeida S. Clinical outcome of Crohn's disease: analysis according to the vienna classification and clinical activity. Inflamm Bowel Dis. 2001;7:306–313. doi: 10.1097/00054725-200111000-00005. [DOI] [PubMed] [Google Scholar]
- 22.Seibold F, Weber P, Jenss H, Scheurlen M. Autoimmune hepatitis in inflammatory bowel disease: report of two unusual cases. Z Gastroenterol. 1997;35:29–32. [PubMed] [Google Scholar]
- 23.Uko V, Thangada S, Radhakrishnan K. Liver disorders in inflammatory bowel disease. Gastroenterol Res Pract. 2012;2012:642923. doi: 10.1155/2012/642923. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Schatorjé E, Hoekstra H. Transient hypertransaminasemia in paediatric patients with Crohn disease undergoing initial treatment with enteral nutrition. J Pediatr Gastroenterol Nutr. 2010;51:336–340. doi: 10.1097/MPG.0b013e3181d94f63. [DOI] [PubMed] [Google Scholar]
- 25.Lemberg DA, Leach ST, Day AS. Transient hypertransaminasemia in pediatric patients with Crohn disease. J Pediatr Gastroenterol Nutr. 2011;53:229. doi: 10.1097/MPG.0b013e31821c6497. [DOI] [PubMed] [Google Scholar]
- 26.Sonoda K, Ikeda S, Mizuta Y, Miyahara Y, Kohno S. Evaluation of venous thromboembolism and coagulation-fibrinolysis markers in Japanese patients with inflammatory bowel disease. J Gastroenterol. 2004;39:948–954. doi: 10.1007/s00535-004-1426-6. [DOI] [PubMed] [Google Scholar]
- 27.Guerra Montero LJ, Ingver A, Casañas A, Sosa C, Iade B. Clinical characteristics of patients with inflammatory bowel disease and thromboembolic events. Acta Gastroenterol Latinoam. 2010;40:134–141. [PubMed] [Google Scholar]
- 28.Lazzerini M, Bramuzzo M, Maschio M, Martelossi S, Ventura A. Thromboembolism in pediatric inflammatory bowel disease: systematic review. Inflamm Bowel Dis. 2011;17:2174–2183. doi: 10.1002/ibd.21563. [DOI] [PubMed] [Google Scholar]
- 29.Nylund CM, Goudie A, Garza JM, Crouch G, Denson LA. Venous thrombotic events in hospitalized children and adolescents with inflammatory bowel disease. J Pediatr Gastroenterol Nutr. 2013;56:485–491. doi: 10.1097/MPG.0b013e3182801e43. [DOI] [PubMed] [Google Scholar]