Introduction
Orf, also known as ecthyma contagiosum, contagious pustular dermatitis, infectious pustular dermatosis, ovine pustular dermatitis, and sore mouth, is a viral zoonotic disease resulting from the direct or indirect contact of damaged skin with infected animals. The virus is endemic in sheep and goats worldwide and manifests as an acute contagious skin condition that can cause substantial morbidity.1 The causative microorganism is the orf virus, an epitheliotropic DNA virus from the Parapoxvirus group.2 In humans, after a brief incubation period of 3 to 7 days, an orf lesion appears as a pruritic erythematous macule and then rises to form a papule.1 Lesions become nodular and vesicular and progress to a weeping target lesion that ulcerates and forms a dry crust. Here we describe a case of orf disease in a patient with scleroderma.
Case report
A 70-year-old woman presented to our clinic 2 weeks after traumatic injury in the kitchen with a knife to the dorsum of her left hand after cutting lamb. One week after injury, a rapidly expanding asymptomatic erythematous and bullous plaque developed, which failed to respond to flucloxacillin and betadine.
Dermatologic examination found a desquamating erythematous bullous plaque on the dorsum of her left hand, 30 mm in diameter extending to the bases of the index and middle fingers (Fig 1). Her general practitioner diagnosed scleroderma at the age of 50 when she presented with symmetrical skin thickening of her hands; she also reported numbness of her fingers with associated color change lasting minutes. The condition was often triggered by emotional stress and cold weather, and her general practitioner then diagnosed Raynaud's syndrome secondary to scleroderma. She never experienced systemic organ involvement. The patient was on a calcium channel blocker, diltiazem, and a statin.
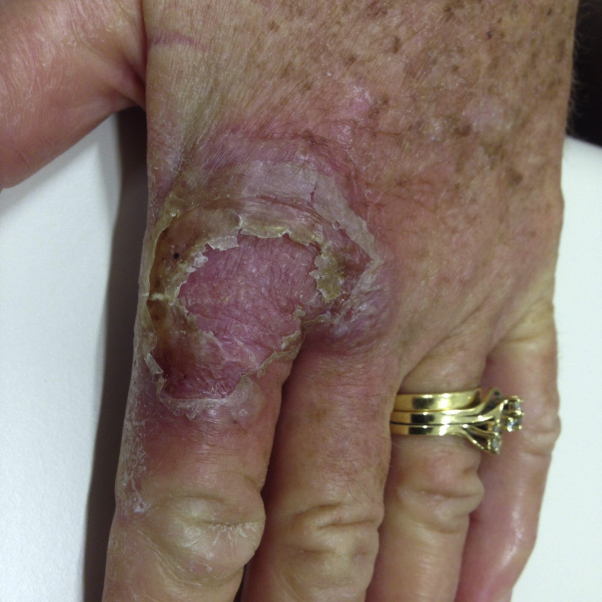
Fig 1.
Ecthyma contagiosum. Presentation 2 weeks after initial traumatic injury to hand. Desquamating erythematous bullous plaque on the dorsum of left hand, extending to the bases of the index and middle fingers. A classic location of orf on the index finger.
The patient did not have constitutional symptoms. She suffered from itching, redness, and swelling of her hand, however, had no subjective complaints.
Clinical impression was that of an infective process, likely orf from cutting and contamination with lamb. Other differential diagnoses included a deep fungal or atypical mycobacterial infection contracted subsequently from contamination in the garden. Upon assessment of her skin, there was slight thickening and hardening of her hands.
Biopsies of the blister for microbiology (fungi, atypical, nocardia) and for histology were performed (Fig 2). Microscopic findings of the skin biopsy showed atypical dermal squamous proliferation consistent with pseudoepitheliomatous hyperplasia. Swabs of the lesion were taken and were negative for bacterial, mycobacterial, and deep fungal infections. Four weeks later the patient presented again for follow-up, and on clinical examination her lesion had improved dramatically (Fig 3).
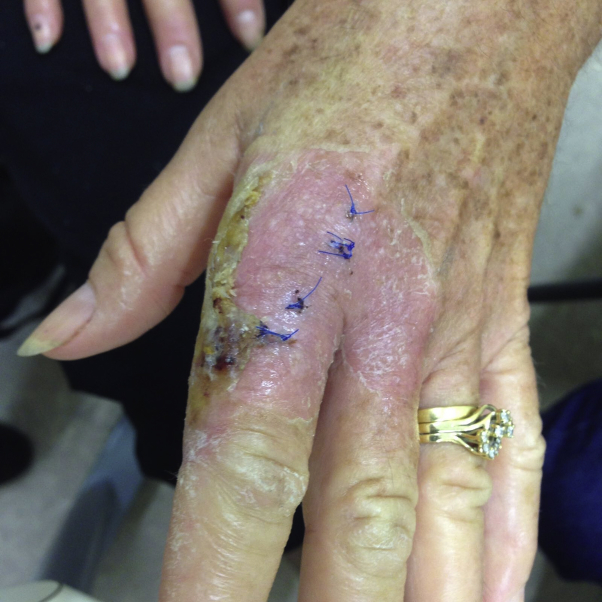
Fig 2.
Ecthyma contagiosum. Lesion after biopsy and 3 weeks after initial contamination to hand. Lesion self-resolving.
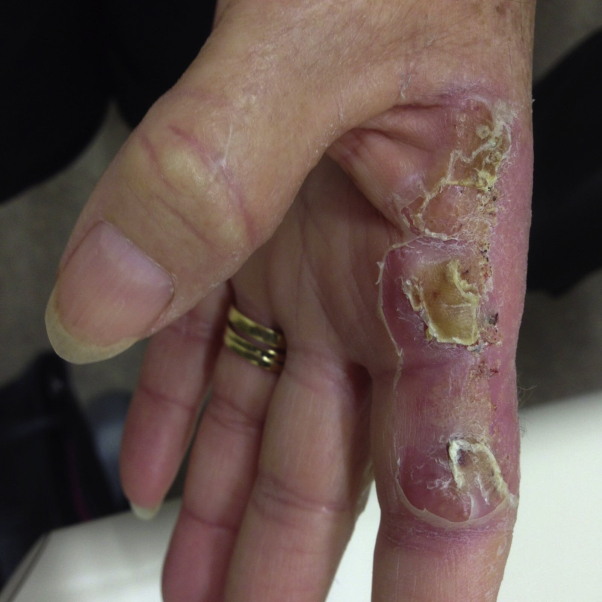
Fig 3.
Ecthyma contagiosum. Four weeks later and the desquamating lesion has healed dramatically.
Orf was diagnosed on the basis of her clinical history of contact with lamb and her lesion passing through a typical evolution of an orf lesion. The patient was not treated with any medication, and 5 days later her lesion had almost completely resolved.
Discussion
Orf (ecthyma contagiosum) is primarily a disease of sheep and goats. Humans are infected by coming in contact with infected animals or with a fomite carrying the virus.3 No human-to-human transmission of Parapoxvirus has been reported.4
Many infectious and inflammatory entities may be considered within the clinical differential of orf lesions. Differential diagnoses include pyoderma, herpetic whitlow, cowpox, pseudo cowpox (Milker nodule), cat-scratch disease, anthrax, tularemia, primary inoculation tuberculosis, atypical mycobacteria, syphilitic chancre, sporotrichosis, keratoacanthoma, and pyogenic granuloma.5 Diagnosis of orf virus requires an astute clinician who observes the characteristic lesion of orf occurring in the correct clinical setting. It most commonly affects people who handle sheep and goats occupationally, but it may infect people without a history of direct animal contact through fomite transmission.
Lesions of orf virus pass through a characteristic evolution and may present as inflamed macules/papules, papulovesicles, weeping nodules, verrucous papules, or eschars. After a brief incubation period of 3 to 5 days, lesions begin as erythematous macules and then rise to form papules, often with a target appearance (days 7–14). Lesions become nodular or vesicular and often ulcerate after 14 to 21 days—referred to as the acute stage. Lesions may be pruritic and are typically painless, although pain may result from secondary infection. In some cases, there may also be suppuration and scabbing.4 Complete healing can take up to 4 to 8 weeks.6
Within the poxvirus family, secondary immunologic reactions such as erythema multiforme (EM) are most frequently reported in association with orf.7 A review of the literature on human orf infection found some complications such as fever, lymphangitis, lymphadenopathy, giant or recurring lesions, and EM.8 Systemic symptoms are characteristically absent, but infection of an immunocompromised patient may present with fever, chills, sweats, lymphadenopathy, or a generalized varicelliform eruption of the skin and oral mucosa. Orf virus has also been associated with the development of autoimmune bullous disease, including a bullous pemphigoid-like eruption. The bullous pemphigoidlike lesions are characterized by a subepidermal blister associated with a mixed inflammatory infiltrate including neutrophils and eosinophils.
In the case of our patient, the evolution of her wound and the time it took to heal was consistent with the known development of cutaneous lesions of orf. Initially, it was thought that her known background of scleroderma would significantly delay her wound healing, as autoimmune diseases are a common cause of delayed wound healing. In patients with chronic wounds evaluated in specialized wound healing clinics, 20% to 23% have autoimmune etiologies for their wounds including scleroderma.9 For many of these challenging patients, a multidisciplinary approach with involvement of dermatology and rheumatology improves clinical outcome.
About 30% of sheep workers in the United Kingdom report having had an orf infection.10 Abattoir workers in New Zealand have an annual orf incidence of less than 4%,11 and human orf infections in North America are considered rare.12 It is therefore difficult in some instances to diagnose orf in areas where it is not commonly seen when there are other more common diseases causing similar lesions. For example, pseudocowpox or milker's nodule results from infection with the paravaccinia virus and has a virtually identical clinical presentation to orf. Hence, in places such as North America, polymerase chain reaction studies are done to confirm the diagnosis. However, in the case of our patient in Western Australia, the diagnosis was made clinically, as it was a classic case of orf with the typical evolution and history. It was therefore not necessary to perform polymerase chain reaction studies, as it is not a routine test done in Australia.
Orf is typically a self-limiting, single-organ system infection. For an immunocompetent patient with a limited number of skin lesions, supportive therapy with dressing changes and analgesia may be used. Of note, corticosteroid therapy, both intralesional and systemic, and irradiation or extensive surgical procedures, are not beneficial and should be avoided. The lesion must be kept clean and the wound cared for appropriately. Spontaneous resolution occurs in about 4 to 6 weeks. Recurrence may occur for those who are immunocompromised.
Conclusion
Taking a precise history, clinical appearance, and epidemiologic data are important for diagnosis, as prompt diagnosis is crucial to avoid inappropriate treatment. When present, the appearance of a single or multiple erythematous lesions often over the dorsum of the hand extending to the thumb and index finger, with a history of contact with lamb should alert the physician to the possibility of orf disease.
Footnotes
Funding sources: None.
Conflicts of interest: None declared.
References
- 1.Joseph R.H., Haddad F.A., Matthews A.L., Maroufi A., Monroe B., Reynolds M. Erythema multiforme after orf virus infection: a report of two cases and literature review. Epidemiol Infect. 2015;143(2):385–390. doi: 10.1017/S0950268814000879. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Turan E., Yesilova Y., Ucmak D. A case of orf (ecthyma contagiosum) with multiple lesions. J Pak Med Assoc. 2013;63(6):786–787. [PubMed] [Google Scholar]
- 3.Robinson A.J. Prevalence of contagious pustular dermatitis (orf) in six million lambs at slaughter: a three-year study. N Z Vet J. 1983;31(9):161–163. doi: 10.1080/00480169.1983.35008. [DOI] [PubMed] [Google Scholar]
- 4.Slattery W.R., Juckett M., Agger W.A., Radi C.A., Mitchell T., Striker R. Milkers' nodules complicated by erythema multiforme and graft-versus-host disease after allogeneic hematopoietic stem cell transplantation for multiple myeloma. Clin Infect Dis. 2005;40(7):e63–e66. doi: 10.1086/428619. [DOI] [PubMed] [Google Scholar]
- 5.Ozturk P., Sayar H., Karakas T., Akman Y. Erythema multiforme as a result of Orf disease. Acta Dermatovenerol Alp Pannonica Adriat. 2012;21(2):45–46. [PubMed] [Google Scholar]
- 6.Diven D.G. An overview of poxviruses. Journal of the American Academy of Dermatology. 2001;44(1):1–16. doi: 10.1067/mjd.2001.109302. [DOI] [PubMed] [Google Scholar]
- 7.Ilkit M., Durdu M., Karakas M. Cutaneous id reactions: a comprehensive review of clinical manifestations, epidemiology, etiology, and management. Critical Reviews in Microbiology. 2012;38(3):191–202. doi: 10.3109/1040841X.2011.645520. [DOI] [PubMed] [Google Scholar]
- 8.Alian S., Ahangarkani F., Arabsheybani S. A Case of Orf Disease Complicated with Erythema Multiforme and Bullous Pemphigoid-Like Eruptions. Case reports in infectious diseases. 2015;2015:105484. doi: 10.1155/2015/105484. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Shanmugam V.K. Vasculitic Diseases and Prothrombotic States Contributing to Delayed Healing In Chronic Wounds. Curr Dermatol Rep. 2016;5(4):270–277. doi: 10.1007/s13671-016-0157-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Buchan J. Characteristics of orf in a farming community in mid-Wales. BMJ. 1996;313(7051):203–204. doi: 10.1136/bmj.313.7051.203. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Robinson A.J., Petersen G.V. Orf virus infection of workers in the meat industry. N Z Med J. 1983;96(725):81–85. [PubMed] [Google Scholar]
- 12.Uzel M., Sasmaz S., Bakaris S. A viral infection of the hand commonly seen after the feast of sacrifice: human orf (orf of the hand) Epidemiol Infect. 2005;133(4):653–657. doi: 10.1017/s0950268805003778. [DOI] [PMC free article] [PubMed] [Google Scholar]