Abstract
Human studies of brain stimulation have demonstrated modulatory effects on the perception of pain. However, whether the primary somatosensory cortical activity is associated with antinociceptive responses remains unknown. Therefore, we examined the antinociceptive effects of neuronal activity evoked by optogenetic stimulation of primary somatosensory cortex. Optogenetic transgenic mice were subjected to continuous or pulse-train optogenetic stimulation of the primary somatosensory cortex at frequencies of 15, 30, and 40 Hz, during a tail clip test. Reaction time was measured using a digital high-speed video camera. Pulse-train optogenetic stimulation of primary somatosensory cortex showed a delayed pain response with respect to a tail clip, whereas no significant change in reaction time was observed with continuous stimulation. In response to the pulse-train stimulation, video monitoring and local field potential recording revealed associated paw movement and sensorimotor rhythms, respectively. Our results show that optogenetic stimulation of primary somatosensory cortex at beta and gamma frequencies blocks transmission of pain signals in tail clip test.
Keywords: optogenetic stimulation, tail clip test, sensorimotor rhythms, primary somatosensory cortex, pain perception
INTRODUCTION
Since the first demonstration of cortical stimulation for pain control [1], cortical stimulation techniques have been used to treat intractable pain and satisfactory pain relief has been reported by patients [2,3,4,5]. Repetitive transcranial magnetic stimulation (rTMS) and transcranial direct current stimulation (tDCS) were later introduced as safer and inexpensive methods of neuromodulation. Recently published reviews have summarized the analgesic efficacy of rTMS [6] and tDCS [7]. High frequency (>5 Hz) rTMS has shown level A (definite) evidence of analgesic efficacy, when applied to the primary motor cortex (M1) with 90% intensity of individual resting motor threshold. Anodal tDCS to M1 also produced pain relief when applied to M1 for several days [8]. Although the mechanism of action remains to be clarified, these rTMS and tDCS studies suggest that cortical stimulation may be a promising therapeutic method of pain relief in patients. Interestingly, the most efficient region for pain control was reported to be M1 not the primary somatosensory cortex (S1), although the pain signal is transmitted from the thalamus to M1 via S1. The role of S1 in pain perception during the cortical modulation is still in question. In this study, we have investigated the neuromodulation effect on pain in response to the tail clip test while applying pulsetrain or continuous optogenetic stimulation to S1. The frequencies of pulse-train stimulation were selected to be 15, 30 and 40 Hz to evoke beta (15~30 Hz) or gamma (40 Hz) band oscillations. Beta band oscillations occur coherently in the mammalian somatosensory-motor system, and associated in somatosensory processing as well as muscle activity [9]. Gamma band oscillations are reported to be related to the subjective perception of pain [10].
MATERIALS AND METHODS
Animals and preparation
Adult C57BL/6 Thy1-ChR2-YFP transgenic mice (Jackson Laboratory stock # 7612, Bar Harbor, ME, USA) with age of 12~17 weeks (body weight, 20~30 g) were given food and water ad libitum. This study was carried out in accordance with the recommendations of Institutional Animal Care and Use Committee in Korea Institute of Science and Technology, following Act 1992 of the Korea Lab Animal Care Regulations and associated guidelines. The protocol was approved by the Institutional Animal Care and Use Committee (approval number: 2014-026). In total, 4 mice were used for behavior test for 7 different days. The number of tail clip test did not exceed more than 15 times. All efforts were made to minimize the number of animals used as well as animal pain and suffering.
Surgery
All surgical procedures were performed under anesthetized state with the injection of ketamine/xylazine cocktail (120/6 mg/kg, i.p. injection). After fixing the mouse head in a stereotaxic apparatus (David Kopf Instruments, Model 902, Tujunga, CA, USA), the eyes were covered with Vaseline to keep the eyes from drying up. The midline of scalp was incised to expose the skull and a drop of 2% lidocaine was used around the incision to reduce any pain. After wiping and cleaning the skull, the skull was leveled using bregma and lambda positions. Holes were made on the forelimb S1 region (−0.38 mm AP, 2.25 mm ML from the bregma) and cerebellum (5.7 mm AP, ±1.7 mm ML from the bregma) using a dental drill (bur size 0.5 mm; MARATHON-3, Saeyang Microtech, Korea). A custom-made fiber optic cannula (FT200EMT, Thorlabs, Newton, New Jersey, USA; LC 1.25mm OD Multimode Ceramic Zirconia Ferrules, Precision Fiber Products, Milpitas, CA, USA) was attached to a Teflon-coated tungsten wire electrode (0.045″ in coated outer diameter, A-M systems, Sequim, WA, USA) and implanted into the forelimb S1 region for stimulation (1.5 mm DV from the bregma). Two micro screws (chrome plated stainless steel, 1 mm in diameter, Asia Bolt, Seoul, Korea) were implanted above the cerebellum and used as the reference and ground. The optrode and electrodes were fixed onto the skull by dental cement. After surgical procedures, the mouse was allowed to recover in an individual cage for at least a week. All the target coordinates of the electrodes followed the mouse brain atlas of Paxinos and Franklin [11].
Tail clip test
Acute pain was induced by a tail clip test according to a modification of Haffner's method [8,9]. While the mouse was put in the custom-made acrylic cylinder (20 cm in diameter), an alligator clip exerting a force of 2.5 N was manually applied to the tail approximately at 1.5 cm from the tail base to induce pain. The force was measured by attaching a flexible force sensor to the tail (FSR-400, Interlink Electronics, CA, USA). The mouse quickly responded to this nociceptive stimulus by biting the clip or licking the tail near the clipped position. The moment that the mouse first touched the clip or the tail was defined as the moment of reaction. Since the reaction time varied depending on the clipping position, the clipping position was adjusted for each mouse to give a mean reaction time of 1 sec for 5 test trials in prior. The time between tail clip stimulation onset and the moment of reaction was measured by slowmotion video recording using a high-speed camera (video sampling rate at 1000 frame/sec; Phantom Flex4K, AMTEK, Wayne, NJ, USA). When mouse became exhausted after experiencing a series of pain stimulation, it did not respond to the stimulation or did respond with a longer delay. If the mouse did not respond to the stimulation within 10 sec in three successive trials, the day's stimulation session was stopped and those trials with reaction time longer than 10 sec were rejected. To minimize adaptation for pain and prevent any tissue damage, clipping position was slightly changed in each trial. Inter-trial interval was kept longer than 10 min to give resting time enough for recovery and no more than 15 trials were performed in a day.
Optogenetic stimulation during tail clip test
Optogenetic stimulation was generated using a blue light LED (473 nm, Doric Lenses, Quebec, Quebec, Canada) delivered through a patch cable with core diameter of 200 µm (Doric Lenses, Quebec, Quebec, Canada). The light intensity was 3~4 mV/mm2 and the light intensity threshold was determined as the minimal intensity to induce the forepaw tremor in each mouse (individual thresholds in Supplementary). The stimulation paradigm is depicted in Fig. 1. Continuous or pulse-train stimulations were applied approximately 0.25 sec after the tail clip. The stimulation epochs were 2 sec in duration, and with a pulse width of 10 msec for pulse-train stimulation. For pulse-train stimulation, 15, 30, and 40 Hz frequencies were applied to evoke beta or gamma band oscillations in the somatosensory cortex. Different stimulation durations (1, 2, and 3 sec) were tested only at 15 Hz. Per stimulation type, 1 to 3 trials were applied to each animal per day, and in total, 10 to 19 trials per stimulation type were applied to each mouse. The intertest interval was 10 min. We acquired the local field potential (LFP) of S1 by SynAmps2 amplifier (Compumedics, Abbotsford, Victoria, Australia).
Fig. 1. Schematic design for the experiment. Optogenetic stimulation of S1 was applied to the animal right after clipping the tail. The reaction time measured with respect to the clipping time was referred as T and the reaction time from the light stimulation cessation was referred as τ.
Behavior analysis
As in Fig. 1, the reaction time (T) was defined as the latency from tail clipping to bit the clip or lick on the tail. To quantitate the delay caused by optical stimulation, we also defined the time to reaction from stimulation cessation (τ). Data with the same type of stimulation were collected from all the mice and used for the analysis. The paw movement was quantified by tracking the paw trajectory recorded with a high-speed camera. The trajectory of paw was captured by a motion capture algorithm, and then the general path was subtracted to get the trembling trajectory in one dimension.
Statistical test
Kruskal-Wallis ANOVA and post-hoc Mann-Whitney U test with Bonferroni correction was performed to compare reaction times. Significance was set at p<0.05. T-test was used for the linearity of slop. Firstly, t-value was calculated according to t=(r √(n-2))/√(1-r2), where n is the degree of freedom and r is the Pearson correlation coefficient. Then, the p-value was obtained from the t-distribution. All of analysis and statistics procedure were calculated by Matlab (Mathworks, Natick, MA, USA).
RESULTS
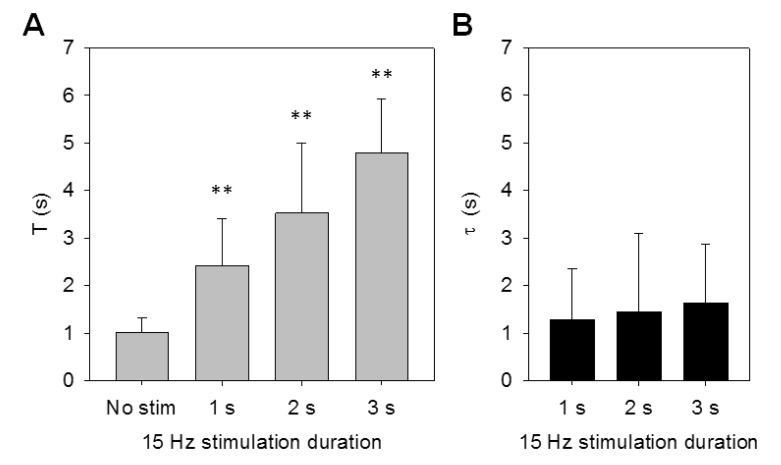
As shown in Fig. 2A, the pulse-train stimulation to forelimb S1 significantly increased T compared to no-stimulation condition (Kruskal-Wallis ANOVA, p<0.001; post-hoc Mann-Whitney U test, p<0.001 for all pulse-train stimulation compared to no-stimulation), while T for continuous-stimulation group was not significantly different (post-hoc Mann-Whitney U test, p>0.05). None of the mice showed a response to pain during pulse-train stimulation, and the τ for pulse-train stimulation at 15, 30 and 40 Hz was not statistically different from the T of the no-stimulation condition (Kruskal-Wallis ANOVA, p=0.68) as shown in Fig. 2B. In the case of the continuous stimulation, all the mice showed the pain response during the stimulation period so τ was not defined. Simultaneously recorded LFPs and paw movement showed phase-locked oscillatory responses to pulse-train stimulation (Fig. 3B~D). On the other hand, continuous stimulation induced transient effects in LFP and paw movements (Fig. 3A), implicating that cortical oscillations generated by repetitive stimulation of S1 are associated with the hindered transmission of nociceptive signals from the tail clipping. With respect to different stimulation duration, T showed an incremental increase exhibiting a positive correlation (R2=0.68; p=0.18 for linearity test, Fig. 4A). However, τ for different stimulation duration was not significantly different from the T of no-stimulation condition (Kruskal-Wallis ANOVA, p=0.20) as shown in Fig. 4B, indicating that the simulation length itself does not elongate or shorten the reaction time after the stimulation cessation.
Fig. 2. (A) The reaction time to tail clip, T in different stimulation conditions. (B) The time to reaction from the stimulation cessation, τ in different frequency stimulation. Whiskers indicate standard deviation. No statistical difference was found between T of no-stimulation and τ of pulse-train stimulation groups. The number of trials was 48 for No stim, 44 for Cont, 50 for 15 Hz, 48 for 30 Hz, and 47 for 40 Hz. *p<0.01, **p<0.001 in comparison to no-stim group.
Fig. 3. (A) LFP and paw movements during continuous stimulation. (B) LFP and paw movements during 15 Hz pulse-train stimulation. (C) LFP and paw movements during 30 Hz pulse-train stimulation. (D) LFP and paw movements during 40 Hz pulse-train stimulation. LFP was acquired from the optrode implanted in the forelimb S1.
Fig. 4. (A) The reaction time to tail clip, T in different stimulation duration. (B) The time to reaction from the stimulation cessation, τ in different stimulation duration. Whiskers indicate standard deviation. No statistical difference of τ was found between other groups. The number of trials was 48 for No stim, 55 for 1 s, 50 for 2 s, and 53 for 3 s.
DISCUSSION
By directly stimulating the S1 cortex, we showed that repetitive stimulation at beta and gamma frequencies blocked the pain perception. During pulse-train S1 stimulation, the mouse paw in the contralateral side of stimulation trembled along with the oscillatory response in S1 and no animals responded to tail clip during the stimulation period. No obvious delay in pain perception was observed with continuous stimulation of S1, indicating that a simple increase of S1 activation is not relevant to the delayed pain response. Differently from the phasic stimulation, continuous stimulation of S1 induced neither sustained oscillatory paw movement nor rhythmic oscillations in the cortex. This result partly supports the idea that the sensory perception might be interfered by motor response induced by the neuromodulation, which is evidenced by the stronger suppression of sensory perception with the stronger motor responses [12]. If the presence of motor response or the rhythmic activation of motor cortex indirectly induced by the S1 activation is the key factor affecting the pain perception, it is understandable that neuromodulation of S1 suppressed tactile perception by tDCS [13] and TMS [14], yet the suppression effect was stronger for the case of motor cortex stimulation [14].
One possible mechanism of the interference in pain perception is that the afferent signals from the paw movement induced by optogenetic stimulation might compete with the pain signals from the tail. Phasic activation of S1 in beta & gamma band frequency possibly generated resonant rhythmic oscillations in the sensorimotor area [15,16] and induced oscillatory paw movement, whereas continuous stimulation of S1 did not. On the other hand, the neuromodulation weaker than motor threshold was also proven effective to relieve pain [6], indicating that the competition between afferent sensory signals is not a single mechanism for the attenuating or blocking sensory perception. Another possibility is that the modulation of S1 and M1 might palliate the pain via cortico-incerto-thalamic pathway [17,18]. Zona incerta (ZI) receives inputs from diffusive cortical areas including M1 as well as S1 [19], and provides inhibition to postromedial (POm) nucleus of thalamus [20,21] which is crucial for nociceptive processing [22,23,24,25]. Abnormally enhanced activation of POm [26,27,28] and accompanying suppression of ZI [17] in central pain syndrome were rescued by motor cortex stimulation [29] or ZI stimulation [30]. Considering that the frequency range of action is about 10~30 Hz in ZI [31], sensorimotor rhythms generated by the phasic optogenetic stimulation might effectively trigger the incerto-thalamic circuit for pain control.
Putting aside the contribution of motor cortex, it has been known that tactile signals are transmitted to S1 via the ventroposterior nuclei of thalamus and are then passed to other cortical regions such as the M1 and secondary somatosensory cortex [32], as well as the centromedial thalamus and POm via corticothalamic projections [33]. Nicolelis and coworkers confirmed that oscillatory neuronal activity in the S1 spread to VPM, and became synchronized during tactile exploration [34]. In addition, Romo and coworkers have observed the frequency-locking rhythms in S1 and VPL produced by a 20 Hz tactile stimulation. Of interest to note is that they observed that the threshold for tactile discrimination was changed in both S1 [35] and VPL [36] depending on the strength of oscillations, suggesting altered signal transmission during sensorimotor rhythms. Taken together, repetitive S1 stimulation may cause the strong oscillations in cortico-thalamic circuits and block the timely transmission of peripheral pain signals.
In conclusion, our study strongly suggests that evoked sensorimotor rhythms block the external pain input, possibly via an insensitive state in thalamic neurons during entrained oscillation. This finding may potentially be applied in the clinical arena, to any patient with drug-resistant, chronic neuropathic pain.
ACKNOWLDGMENTS
This research was supported by the Korean Research Council of Fundamental Science & Technology (No. CRC-15-04-KIST). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
This study was carried out in accordance with the recommendations of Institutional Animal Care and Use Committee in Korea Institute of Science and Technology, following Act 1992 of the Korea Lab Animal Care Regulations and associated guidelines. The protocol was approved by the Institutional Animal Care and Use Committee (approval number: 2014-026).
SUPPLEMENTARY MATERIAL
Light intensity threshold and tail clippin trial information for individual mice
References
- 1.Tsubokawa T, Katayama Y, Yamamoto T, Hirayama T, Koyama S. Chronic motor cortex stimulation in patients with thalamic pain. J Neurosurg. 1993;78:393–401. doi: 10.3171/jns.1993.78.3.0393. [DOI] [PubMed] [Google Scholar]
- 2.Cruccu G, Aziz TZ, Garcia-Larrea L, Hansson P, Jensen TS, Lefaucheur JP, Simpson BA, Taylor RS. EFNS guidelines on neurostimulation therapy for neuropathic pain. Eur J Neurol. 2007;14:952–970. doi: 10.1111/j.1468-1331.2007.01916.x. [DOI] [PubMed] [Google Scholar]
- 3.Rokyta R, Fricová J. Neurostimulation methods in the treatment of chronic pain. Physiol Res. 2012;61(Suppl 2):S23–S31. doi: 10.33549/physiolres.932392. [DOI] [PubMed] [Google Scholar]
- 4.Antal A, Paulus W. Effects of transcranial theta-burst stimulation on acute pain perception. Restor Neurol Neurosci. 2010;28:477–484. doi: 10.3233/RNN-2010-0555. [DOI] [PubMed] [Google Scholar]
- 5.Lefaucheur JP, Ménard-Lefaucheur I, Goujon C, Keravel Y, Nguyen JP. Predictive value of rTMS in the identification of responders to epidural motor cortex stimulation therapy for pain. J Pain. 2011;12:1102–1111. doi: 10.1016/j.jpain.2011.05.004. [DOI] [PubMed] [Google Scholar]
- 6.Lefaucheur JP, André-Obadia N, Antal A, Ayache SS, Baeken C, Benninger DH, Cantello RM, Cincotta M, de Carvalho M, De Ridder D, Devanne H, Di Lazzaro V, Filipović SR, Hummel FC, Jääskeläinen SK, Kimiskidis VK, Koch G, Langguth B, Nyffeler T, Oliviero A, Padberg F, Poulet E, Rossi S, Rossini PM, Rothwell JC, Schönfeldt-Lecuona C, Siebner HR, Slotema CW, Stagg CJ, Valls-Sole J, Ziemann U, Paulus W, Garcia-Larrea L. Evidence-based guidelines on the therapeutic use of repetitive transcranial magnetic stimulation (rTMS) Clin Neurophysiol. 2014;125:2150–2206. doi: 10.1016/j.clinph.2014.05.021. [DOI] [PubMed] [Google Scholar]
- 7.Plow EB, Pascual-Leone A, Machado A. Brain stimulation in the treatment of chronic neuropathic and non-cancerous pain. J Pain. 2012;13:411–424. doi: 10.1016/j.jpain.2012.02.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Nitsche MA, Cohen LG, Wassermann EM, Priori A, Lang N, Antal A, Paulus W, Hummel F, Boggio PS, Fregni F, Pascual-Leone A. Transcranial direct current stimulation: State of the art 2008. Brain Stimul. 2008;1:206–223. doi: 10.1016/j.brs.2008.06.004. [DOI] [PubMed] [Google Scholar]
- 9.van Ede F, Maris E. Somatosensory demands modulate muscular beta oscillations, independent of motor demands. J Neurosci. 2013;33:10849–10857. doi: 10.1523/JNEUROSCI.5629-12.2013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Gross J, Schnitzler A, Timmermann L, Ploner M. Gamma oscillations in human primary somatosensory cortex reflect pain perception. PLoS Biol. 2007;5:e133. doi: 10.1371/journal.pbio.0050133. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Paxinos G, Franklin KB. The mouse brain in stereotaxic coordinates. 2nd ed. San Diego, CA: Elsevier Academic Press; 2004. [Google Scholar]
- 12.Cohen LG, Bandinelli S, Sato S, Kufta C, Hallett M. Attenuation in detection of somatosensory stimuli by transcranial magnetic stimulation. Electroencephalogr Clin Neurophysiol. 1991;81:366–376. doi: 10.1016/0168-5597(91)90026-t. [DOI] [PubMed] [Google Scholar]
- 13.Rogalewski A, Breitenstein C, Nitsche MA, Paulus W, Knecht S. Transcranial direct current stimulation disrupts tactile perception. Eur J Neurosci. 2004;20:313–316. doi: 10.1111/j.0953-816X.2004.03450.x. [DOI] [PubMed] [Google Scholar]
- 14.McKay DR, Ridding MC, Miles TS. Magnetic stimulation of motor and somatosensory cortices suppresses perception of ulnar nerve stimuli. Int J Psychophysiol. 2003;48:25–33. doi: 10.1016/s0167-8760(02)00159-9. [DOI] [PubMed] [Google Scholar]
- 15.Haegens S, Nácher V, Hernández A, Luna R, Jensen O, Romo R. Beta oscillations in the monkey sensorimotor network reflect somatosensory decision making. Proc Natl Acad Sci U S A. 2011;108:10708–10713. doi: 10.1073/pnas.1107297108. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Murthy VN, Fetz EE. Coherent 25- to 35-Hz oscillations in the sensorimotor cortex of awake behaving monkeys. Proc Natl Acad Sci U S A. 1992;89:5670–5674. doi: 10.1073/pnas.89.12.5670. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Masri R, Quiton RL, Lucas JM, Murray PD, Thompson SM, Keller A. Zona incerta: a role in central pain. J Neurophysiol. 2009;102:181–191. doi: 10.1152/jn.00152.2009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Lucas JM, Ji Y, Masri R. Motor cortex stimulation reduces hyperalgesia in an animal model of central pain. Pain. 2011;152:1398–1407. doi: 10.1016/j.pain.2011.02.025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Barthó P, Slézia A, Varga V, Bokor H, Pinault D, Buzsáki G, Acsády L. Cortical control of zona incerta. J Neurosci. 2007;27:1670–1681. doi: 10.1523/JNEUROSCI.3768-06.2007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Power BD, Kolmac CI, Mitrofanis J. Evidence for a large projection from the zona incerta to the dorsal thalamus. J Comp Neurol. 1999;404:554–565. [PubMed] [Google Scholar]
- 21.Barthó P, Freund TF, Acsády L. Selective GABAergic innervation of thalamic nuclei from zona incerta. Eur J Neurosci. 2002;16:999–1014. doi: 10.1046/j.1460-9568.2002.02157.x. [DOI] [PubMed] [Google Scholar]
- 22.Apkarian AV, Shi T. Squirrel monkey lateral thalamus. I. Somatic nociresponsive neurons and their relation to spinothalamic terminals. J Neurosci. 1994;14:6779–6795. doi: 10.1523/JNEUROSCI.14-11-06779.1994. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Casey KL. Unit analysis of nociceptive mechanisms in the thalamus of the awake squirrel monkey. J Neurophysiol. 1966;29:727–750. doi: 10.1152/jn.1966.29.4.727. [DOI] [PubMed] [Google Scholar]
- 24.Poggio GF, Mountcastle VB. A study of the functional contributions of the lemniscal and spinothalamic systems to somatic sensibility. Central nervous mechanisms in pain. Bull Johns Hopkins Hosp. 1960;106:266–316. [PubMed] [Google Scholar]
- 25.Zhang X, Giesler GJ., Jr Response characterstics of spinothalamic tract neurons that project to the posterior thalamus in rats. J Neurophysiol. 2005;93:2552–2564. doi: 10.1152/jn.01237.2004. [DOI] [PubMed] [Google Scholar]
- 26.Lee JI, Ohara S, Dougherty PM, Lenz FA. Pain and temperature encoding in the human thalamic somatic sensory nucleus (Ventral caudal): inhibition-related bursting evoked by somatic stimuli. J Neurophysiol. 2005;94:1676–1687. doi: 10.1152/jn.00343.2005. [DOI] [PubMed] [Google Scholar]
- 27.Vierck CJ, Jr, Greenspan JD, Ritz LA. Long-term changes in purposive and reflexive responses to nociceptive stimulation following anterolateral chordotomy. J Neurosci. 1990;10:2077–2095. doi: 10.1523/JNEUROSCI.10-07-02077.1990. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Weng HR, Lenz FA, Vierck C, Dougherty PM. Physiological changes in primate somatosensory thalamus induced by deafferentation are dependent on the spinal funiculi that are sectioned and time following injury. Neuroscience. 2003;116:1149–1160. doi: 10.1016/s0306-4522(02)00796-0. [DOI] [PubMed] [Google Scholar]
- 29.Cha M, Ji Y, Masri R. Motor cortex stimulation activates the incertothalamic pathway in an animal model of spinal cord injury. J Pain. 2013;14:260–269. doi: 10.1016/j.jpain.2012.11.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Petronilho A, Reis GM, Dias QM, Fais RS, Prado WA. Antinociceptive effect of stimulating the zona incerta with glutamate in rats. Pharmacol Biochem Behav. 2012;101:360–368. doi: 10.1016/j.pbb.2012.01.022. [DOI] [PubMed] [Google Scholar]
- 31.Trageser JC, Burke KA, Masri R, Li Y, Sellers L, Keller A. State-dependent gating of sensory inputs by zona incerta. J Neurophysiol. 2006;96:1456–1463. doi: 10.1152/jn.00423.2006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Patestas MA, Gartner LP. A textbook of neuroanatomy. Malden, MA: Blackwell Pub.; 2006. [Google Scholar]
- 33.Reichova I, Sherman SM. Somatosensory corticothalamic projections: distinguishing drivers from modulators. J Neurophysiol. 2004;92:2185–2197. doi: 10.1152/jn.00322.2004. [DOI] [PubMed] [Google Scholar]
- 34.Nicolelis MA, Baccala LA, Lin RC, Chapin JK. Sensorimotor encoding by synchronous neural ensemble activity at multiple levels of the somatosensory system. Science. 1995;268:1353–1358. doi: 10.1126/science.7761855. [DOI] [PubMed] [Google Scholar]
- 35.Haegens S, Vázquez Y, Zainos A, Alvarez M, Jensen O, Romo R. Thalamocortical rhythms during a vibrotactile detection task. Proc Natl Acad Sci U S A. 2014;111:E1797–E1805. doi: 10.1073/pnas.1405516111. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Vázquez Y, Salinas E, Romo R. Transformation of the neural code for tactile detection from thalamus to cortex. Proc Natl Acad Sci U S A. 2013;110:E2635–E2644. doi: 10.1073/pnas.1309728110. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Light intensity threshold and tail clippin trial information for individual mice