Abstract
Hyperbaric oxygen is an adjunctive treatment for promoting wound healing and reducing infection. We present an unusual case of wound tissue necrosis occurring after external dacryocystorhinostomy (ExtDCR) that was subsequently treated with hyperbaric oxygen (HBO) and advancement flaps with good outcome. HBO improves vascularization of ischemic tissues after ExtDCR for greater success after reconstructive surgery.
Keywords: External dacryocystorhinostomy, Tissue necrosis, Hyperbaric oxygen therapy, Treatment
Introduction
Tissue necrosis at an infected external dacryocystorhinostomy (ExtDCR) incision site is a rare complication that is challenging to surgically reconstruct due to tissue avascularity. One method to address tissue avascularity is hyperoxygenation. Good outcomes have been reported after hyperbaric oxygen (HBO) treatment of carbon monoxide poisoning, compromised grafts and flaps, radiation injury to soft tissue and bone, clostridial myonecrosis, necrotizing infections, refractory osteomyelitis, compromised cutaneous ulcers, thermal burns, and peripheral ischemia.1, 2, 3, 4
HBO has been proposed for ophthalmic conditions such as central retinal artery occlusion, radiation optic neuropathy, acute post-radiation scleral necrosis, orbital implant vascularization and compromised periorbital soft tissue grafts.5, 6, 7
This report describes the use of HBO as an excellent adjuvant treatment for a case of tissue necrosis post-ExtDCR that was unresponsive to conventional therapy.
Case report
A 70-year-old female with systemic hypertension presented with tearing in the left eye. The patient was diagnosed with obstruction of the common canaliculus. An ExtDCR was performed using the Dupuy-Dutemps technique. Briefly, a U-flap was constructed between the lacrimal sac and nasal mucosa and bicanalicular stents were placed. Intraoperatively, there was severe bleeding from the orbicularis muscle, angularis vein and nasal mucosa which was controlled with extensive bipolar cauterization. At the end of the surgery, nasal packing was performed with 5 cc of physiologic saline combined with 5 cc diluted adrenaline in the left nostril for 24 h. Postoperative surgical wound site care included application of neomycin, bacitracin and dexamethasone ointment (Maxitrol, Alcon Inc., Fort Worth, Tx, USA) 4 times a day over 10 days and erythromycin ointment (Erythromycin, Alcon Inc., Fort Worth, Tx, USA) for 2 weeks. Systemic antibiotics were not prescribed preoperatively or postoperatively. Four days after surgery, the patient complained of pain and discharge at the wound site. On examination, there was breakdown of the skin in the left medial canthal region of the wound, which progressed to full thickness necrosis by 3 weeks postoperatively. There was extensive discharge from the wound, dehiscence of the incision site, an area of necrotic black tissue that measured 12 × 18 cm over the entire thickness of the surgical wound. Bone exposure occurred over a small portion of the osteotomy and there was loss of mucosal coverage over the anterior ethmoidal cells (Fig. 1A and B). The remainder of the ophthalmic examination was unremarkable. The patient was afebrile. The patient was started on intravenous antibiotics (gentamicin 100 mg (Hospira, Inc., Lake Forest, Il 60045, USA) every 8 h and cefazoline 1gr (Glaxosmithkline Research Triangle Park, NC 27709) every 8 h) and application of erythromycin ointment (Erythromycin, Alcon Inc., Fort Worth, Tx, USA) over the wound.
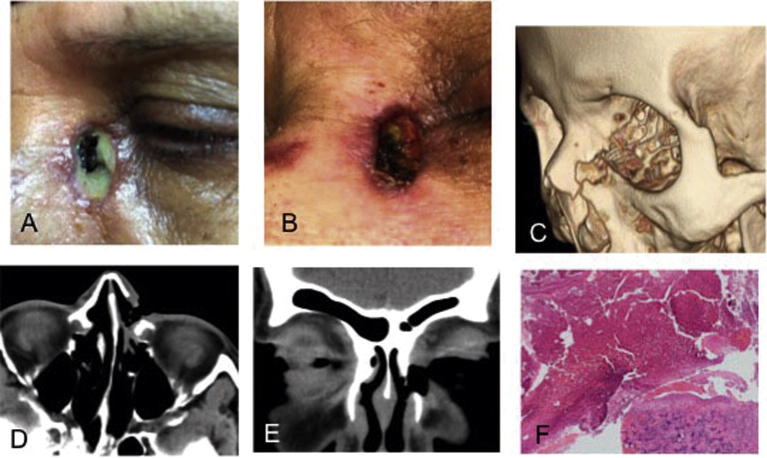
Fig. 1.
Progress of an infection and tissue necrosis following external dacryocystorhinostomy (DCR) on the left side. A. Twenty-one days post-ExtDCR the incision opened, with necrotic margins and secretion. B. Three days post-intravenous antibiotics, necrotic tissue is present at the bottom of the open wound. C. Computerized tomography scan in 3D-CT reconstructions (surface-shaded display showing the left bone defect post-ExtDCR opened in the surgical area). D–E Axial and coronal CT scans. F. Microphotograph showing large areas of necrosis and polymorphonuclear leukocytes infiltration. Mucosal epithelium and foreign body material consistent with surgical material (Hematoxylin and eosin; 4X original magnification).
Computed tomography (CT) scans showed an air filled cavity with bone dehiscence at the anatomical location of the wound into the adjacent area of the nasal cavity (Fig. 1C–E). The antineutrophil cytoplasmic antibodies (ANCA) test and routine laboratory work was normal.
The patient underwent endoscope assisted debridement of devitalized tissue, removal of the bicanalicular stent and drainage of the medial canthal abscess. Tissue specimens obtained during debridement contained necrotic tissue with signs of inflammation (Fig. 1F).
The culture was positive for Serratia marcescens sensitive to amikacin, ciprofloxacin, meropenem, trimethoprim/sulfametoxazole and Corynebacterium sensitive to erythromycin. The patient was prescribed Clindamycin Hydrochloride (Clindamycin capsules, Pfizer Inc., Greenstone LLC, US) 300 mg every 6 h to reduce chances of a secondary anaerobic infection and Ciprofloxacin hydrochloride tablets (Cipro, Bayer HealthCare Pharmaceuticals Inc., Wayne, NJ, US) 500 mg twice daily. Daily dressing was performed and the volume of discharge diminished as dressings with erythromycin ointment were applied to the osteotomy site.
On the 11th postoperative day, ExtDCR hyperbaric oxygen therapy (HBO) was added to the treatment regimen. The Oxyvet VM2000 hyperbaric chamber (Oxytec Inc., Waukesha, WI, USA) was used for 20 sessions over 10 consecutive days to improve vascularization of the affected area. Limited debridement of the necrotic area was performed during dressing changes (Fig. 2A and B). Once there was mucosal coverage of the bone, the patient underwent a round ear cartilage graft to occlude the previous bony surgical ostium associated with a skin muscle malar advancement and a V-Y forehead flap (Fig. 2C). Two weeks after postoperative repair, sutures were removed and antibiotics were stopped. At the most recent follow-up, 3 months after the repair, the wound had fully healed with no signs of bone infection on magnetic resonance imaging (Fig. 2D).
Fig. 2.
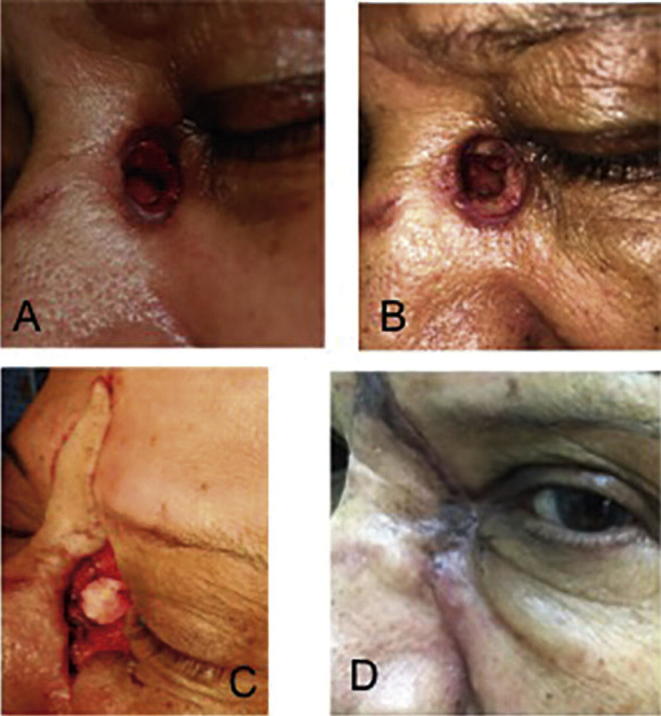
A. Day 7 post-intravenous antibiotics and post-debridement, shows a palid-colored nasal mucosa and necrotic margins of the wound. B. Day 10 post hyperbaric oxygen shows the wound margins recovering the red color. C. Reconstructive surgery was performed using round ear cartilage graft to occlude the previous bone surgical ostium, associated with a skin muscle malar advancement and a V-Y forehead flap. D. Three months post-surgical repair, the wound was closed and healed.
Discussion
Tissue necrosis after ExtDCR is rare and the published cases are summarized in Table 1. In the current case, tissue necrosis was likely caused by excessive cauterization to halt intraoperative bleeding. Although excessive coagulation from cautery could be one cause, the energy alone may be enough to cause necrosis.8 Several factors may be involved in delayed wound healing including vasospasm, subcutaneous hematoma, prolonged pressure on wound margins during surgery and systemic diseases such as Wegener, diabetes, tuberculosis and leukemia. 9, 10, 11
Table 1.
Published cases of tissue necrosis post-dacryocystorhinostomy and the current case report.
| Author | Case | sx | Age/gender | Days after | Associated diseases | Size breakdown (cm) | Treatment | Culture |
|---|---|---|---|---|---|---|---|---|
| Present case, 2016 | 1 | Ext DCR | 71/F | 4 | Severe bleeding | 12x18 | AbIV+ hyperbaric oxygen+flap | Serratia marcescens + Corynebacterious |
| Jordan et al.11 | 1 | Ext DCR | 50/F | 15 | Wegener | – | Pedicle flap | – |
| 2 | 26/M | – | Wegener | – | Direct closure +Steroids | – | ||
| Alour & Montazeri9 | 1 | Ext DCR | 51/F | 3 | DiabetesIntense bleeding | 0.5–0.8 | Direct suture failed, Necrotic removal +flap | – |
| 2 | 38/M | 6 | Intense bleeding | – | Necrotic removal +flap | – | ||
| Yeniad et al.17 | 1 | EC DCR | 65/F | 3 | – | – | AbIV failedFlap failedAntifungal therapy + secondary healing | Aspergillus |
| Goel et al.18 | 1 | EC DCR | 60/F | 4 | Canalicular burn | – | Second healing granulation + AbIV | Gram positive cocci |
| McClintic et al.8 | 1 | EC DCR | 63/F | 6 | Turbinectomy+ Merocel | – | Secondary healing | – |
| 2 | 83/F | 30 | BCC excision medial canthusMMTC cotonoide | – | Flap failedSecondary healing | – | ||
| 3 | 63/F | 7 | Canalicular burn | – | Forehead flap failedAdvancement flap failedSecondary healing | – |
ExtDCR = External Dacryocystorhinostomy; ECDCR = Endocanalicular Dacryocystorhinostomy; M = Male; F = Female; AbIV = antibiotics endovenous; BCC = basocell carcinoma; MMTC = Mytomicin C.
Incision site necrosis is a possible post-surgical complication, especially in traumatic and infectious surgeries. However it is very rare in facial surgery due to the rich vascularization to this area. 9
The patient in the current case report underwent ExtDCR to treat an obstruction of the common canaliculus and had no history of infectious episodes prior to surgery. Opportunistic infections can occur after ExtDCR due to breakdown of the skin barrier with possibility of soft tissue infection in 4.6% (19/413) of cases.12 Infection can occur in 7.9% (12/152) of these cases where postoperative antibiotics are not used and in 1.6% (2/128) of cases that do receive postoperative antibiotics (P < 0.02).12
The initial therapy in the current case was systemic antibiotics and surgical debridement with stent removal. We elected to perform stent removal due to previous reports of intubation and postoperative infection.12, 13
Compared to previous reports of necrotic tissue post-DCR, this is the largest full thickness skin breakdown, with bone exposure and necrosis extending to the margins. The extent of breakdown led us to believe that healing by primary granulation was unlikely and advancement flaps would be unsuccessful. Hence we introduced HBO into the treatment regimen because metabolic processes such as wound healing require adequate oxygenation, which would normally be provided by unaffected tissue surrounding the wound.4 Another advantage of HBO is the antibiotic/antifungal effect.9, 14, 15, 16 After the HBO sessions, the patient underwent successful surgical repair with advancement flaps.
The main drawbacks of HBO include the lack of availability in some regions, additional costs of treatment and the possibility of adverse effects.4
Conclusion
Full thickness local tissue necrosis after ExtDCR is a rare complication. However HBO can be a useful adjuvant for cases of tissue necrosis after ExtDCR prior to performing advancement flaps. HBO can improve outcomes in similar cases.
Conflict of interest
The authors declared that there is no conflict of interest.
Footnotes
Peer review under responsibility of Saudi Ophthalmological Society, King Saud University.
References
- 1.Ernsting J. Hyperbaric oxygen therapy: physiological considerations. Proc R Soc Med. 1971;64(9):873. [PMC free article] [PubMed] [Google Scholar]
- 2.Hom D.B., Unger G.M., Pernell K.J., Manivel J.C. Improving surgical wound healing with basic fibroblast growth factor after radiation. Laryngoscope. 2005;115(3):412–422. doi: 10.1097/01.mlg.0000157852.01402.12. [DOI] [PubMed] [Google Scholar]
- 3.Tuk B., Tong M., Fijneman E.M., van Neck J.W. Hyperbaric oxygen therapy to treat diabetes impaired wound healing in rats. PLoS One. 2014;9(10):e108533. doi: 10.1371/journal.pone.0108533. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Plafki C., Peters P., Almeling M. Complications and side effects of hyperbaric oxygen therapy. Aviat Space Environ Med. 2000;71(2):119–124. [PubMed] [Google Scholar]
- 5.Ng J.D., Nunery W.R., Martin R.T. Effects of hyperbaric oxygen therapy on hydroxyapatite orbital implant vascularization in rabbits. Ophthal Plast Reconstr Surg. 2001;17(4):254–263. doi: 10.1097/00002341-200107000-00004. [DOI] [PubMed] [Google Scholar]
- 6.Zhou Y.Y., Liu W., Yang Y.J., Lu G.D. Use of hyperbaric oxygen on flaps and grafts in China: analysis of studies in the past 20 years. Undersea Hyperb Med. 2014;41(3):209–216. [PubMed] [Google Scholar]
- 7.Sula B., Ekinci C., Ucak H. Effects of hyperbaric oxygen therapy on rat facial skin. Hum Exp Toxicol. 2016;35(1):35–40. doi: 10.1177/0960327115575758. [DOI] [PubMed] [Google Scholar]
- 8.McClintic S.M., Yoon M.K., Bidar M. Tissue necrosis following diode laser-assisted transcanalicular dacryocystorhinostomy. Ophthal Plast Reconstr Surg. 2015;31(1):e18–e22. doi: 10.1097/IOP.0000000000000045. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Salour H., Montazerin N. Incision site tissue necrosis after dacryocystorhinostomy. Ophthal Plast Reconstr Surg. 1998;14(2):146–148. doi: 10.1097/00002341-199803000-00014. [DOI] [PubMed] [Google Scholar]
- 10.Pang C.Y., Chiu C., Zhong A., Xu N. Pharmacologic intervention of skin vasospasm and ischemic necrosis in pigs. J Cardiovasc Pharmacol. 1993;21(1):163–171. doi: 10.1097/00005344-199301000-00024. [DOI] [PubMed] [Google Scholar]
- 11.Jordan D.R., Miller D., Anderson R.L. Wound necrosis following dacryocystorhinostomy in patients with Wegener's granulomatosis. Ophthalmic Surg. 1987;18(11):800–803. [PubMed] [Google Scholar]
- 12.Walland M.J., Rose G.E. Factors affecting the success rate of open lacrimal surgery. Br J Ophthalmol. 1994;78(12):888–891. doi: 10.1136/bjo.78.12.888. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Walland M.J., Rose G.E. Soft tissue infections after open lacrimal surgery. Ophthalmology. 1994;101(3):608–611. doi: 10.1016/s0161-6420(13)31269-x. [DOI] [PubMed] [Google Scholar]
- 14.Ayan F., Sunamak O., Paksoy S.M. Fournier's gangrene: a retrospective clinical study on forty-one patients. ANZ J Surg. 2005;75(12):1055–1058. doi: 10.1111/j.1445-2197.2005.03609.x. [DOI] [PubMed] [Google Scholar]
- 15.Imbernon A., Agud J.L., Cuetara M.S. Successful therapy of progressive rhino-orbital mucormycosis caused by Rhizopus arrhizus with combined and sequential antifungal therapy, surgery and hyperbaric therapy. Med Mycol Case Rep. 2014;6:51–54. doi: 10.1016/j.mmcr.2014.09.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Colon-Acevedo B., Kumar J., Richard M.J., Woodward J.A. The role of adjunctive therapies in the management of invasive sino-orbital infection. Ophthal Plast Reconstr Surg. 2015;31(5):401–405. doi: 10.1097/IOP.0000000000000488. [DOI] [PubMed] [Google Scholar]
- 17.Yeniad B., Bilgin L.K., Cagatay A., Aslan I. A rare complication after transcanalicular dacryocystorhinostomy: tissue necrosis and nasal-cutaneous fistula. Ophthal Plast Reconstr Surg. 2011;27(5):e112–e113. doi: 10.1097/IOP.0b013e3181fc0611. [DOI] [PubMed] [Google Scholar]
- 18.Goel R., Garg S., Nagpal S. Naso-cutaneous fistula following transcanalicular laser dacrocystorhinostomy. Saudi J Ophthalmol. 2014;28(1):69–71. doi: 10.1016/j.sjopt.2013.11.006. [DOI] [PMC free article] [PubMed] [Google Scholar]