Description
A 15-year-old, previously healthy teenager who had fatigue, shortness of breath, vomiting, chest discomfort, lower extremity oedema and inability to lay flat for 3 weeks prior to her initial presentation. She was warm, well perfused with alternating strong and weak central as well as peripheral pulses and laterally displaced cardiac impulse. Her monitoring showed visual evidence of ‘pulsus alternans’—alternating low and high amplitude waveforms on the arterial waveform and plethysmography (figure 1). Her echocardiography showed severely depressed left ventricular function with ejection fraction of 15%. In addition, sinus tachycardia and varying capnography waveform supported the diagnosis. She gradually worsened requiring intubation and mechanical ventilation. She was diagnosed with primary cardiomyopathy. She underwent the placement of ventricular assist device and now awaits heart transplant.
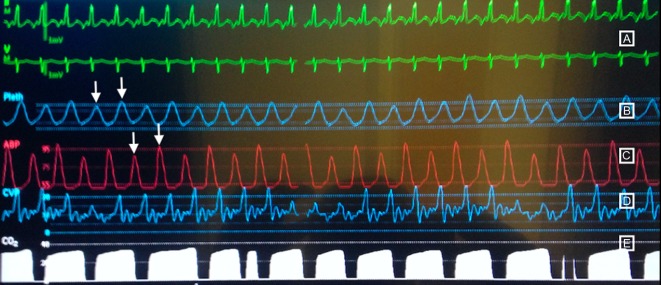
Figure 1.
Monitor showing (A) sinus tachycardia on telemetry. (B) Plethysmography showing alternating low and high amplitude waves as indicated by white arrows. (C) Arterial line waveform showing alternating low and high amplitude waves as indicated by white arrows. (D) Central venous pressure tracing. (E) Capnography showing varying waveform consistent with poor cardiac output.
One proposed mechanism is that the left ventricular failure leads to decreased stroke volume (weak beat—low amplitude wave) resulting in an increase in end-diastolic volume. The next cardiac cycle that increased end-diastolic volume causes increased stretch and contraction of the cardiac muscle by Frank-Starling mechanism resulting in increased stroke volume (strong pulse—high amplitude wave).1 Another proposed mechanism involved abnormal calcium handling by cardiac myocytes. It has been shown in mouse model that overexpression of major calcium storage protein (calsequestrin) in sarcoplasmic reticulum resulted in significant reduction in contractile forces and the development of pulsus alternans.2 3 It can be diagnosed by arterial palpation, sphygmomanometer, plethysmography and arterial waveforms.4 5 Pulsus alternans is a sign of grave disorder, and early recognition is important.
Learning points.
Pulsus alternans alternating low and high amplitude waveforms on the arterial waveform and plethysmography can be a sign of worsening heart failure.
It can be diagnosed by arterial palpation, sphygmomanometer, plethysmography and arterial waveforms.
Early recognition is important as it may affect the management decisions.
Footnotes
Contributors: VA, MLG and AB discussed planning, conducting, reporting, conception and design, acquisition of data or analysis and interpretation of data.
Competing interests: None declared.
Patient consent: Obtained.
Provenance and peer review: Not commissioned; externally peer reviewed.
References
- 1.Harris LC, Nghiem QX, Schreiber MH, et al. Severe pulsus alternans associated with primary myocardial disease in children. Observations on clinical features, hemodynamic findings. Mechanisms and prognosis. Circulation 1966;34:948–61. doi:10.1161/01.CIR.34.6.948 [DOI] [PubMed] [Google Scholar]
- 2.Kotsanas G, Holroyd SM, Young R, et al. Mechanisms contributing to pulsus alternans in pressure-overload cardiac hypertrophy. Am J Physiol 1996;271:H2490–H2500. [DOI] [PubMed] [Google Scholar]
- 3.Schmidt AG, Kadambi VJ, Ball N, et al. Cardiac-specific overexpression of calsequestrin results in left ventricular hypertrophy, depressed force-frequency relation and pulsus alternans in vivo. J Mol Cell Cardiol 2000;32:1735–44. doi:10.1006/jmcc.2000.1209 [DOI] [PubMed] [Google Scholar]
- 4.Saghaei M, Mortazavian M. Pulsus alternans during general anesthesia with halothane: effects of permissive hypercapnia. Anesthesiology 2000;93:91–4. [DOI] [PubMed] [Google Scholar]
- 5.Givertz MM, Colucci W, Braunwald E. Clinical aspects of heart failure: high-output heart failure; pulmonary edema : Braunwald E, Zipes DP, Libby P, Heart disease: a textbook of cardiovascular medicine. 6th edn Philadelphia, Pa: WB Saunders Co, 2001:534–61. [Google Scholar]