Abstract
Background
Diabetic neuropathic foot ulcers are a risk factor for lower leg amputation. Many experts recommend offloading with fibreglass total contact casting, removable cast walkers, and irremovable cast walkers as a way to treat these ulcers.
Methods
We completed a health technology assessment, which included an evaluation of clinical benefits and harms, value for money, and patient preferences for offloading devices. We performed a systematic literature search on August 17, 2016, to identify randomized controlled trials that compared fibreglass total contact casting, removable cast walkers, and irremovable cast walkers with other treatments (offloading or non-offloading) in patients with diabetic neuropathic foot ulcers. We developed a decision-analytic model to assess the cost-effectiveness of fibreglass total contact casting, removable cast walkers, and irremovable cast walkers, and we conducted a 5-year budget impact analysis. Finally, we interviewed people with diabetes who had lived experience with foot ulcers, asking them about the different offloading devices and the factors that influenced their treatment choices.
Results
We identified 13 randomized controlled trials. The evidence suggests that total contact casting, removable cast walkers, and irremovable cast walkers are beneficial in the treatment of neuropathic, noninfected foot ulcers in patients with diabetes but without severe peripheral arterial disease. Compared to removable cast walkers, ulcer healing was improved with total contact casting (moderate quality evidence; risk difference 0.17 [95% confidence interval 0.00–0.33]) and irremovable cast walkers (low quality evidence; risk difference 0.21 [95% confidence interval 0.01–0.40]). We found no difference in ulcer healing between total contact casting and irremovable cast walkers (low quality evidence; risk difference 0.02 [95% confidence interval −0.11–0.14]). The economic analysis showed that total contact casting and irremovable cast walkers were less expensive and led to more health outcome gains (e.g., ulcers healed and quality-adjusted life-years) than removable cast walkers. Irremovable cast walkers were as effective as total contact casting and were associated with lower costs. The 5-year budget impact of funding total contact casting, removable cast walkers, and irremovable cast walkers (device costs only at 100% access) would be $17 to $20 million per year. The patients we interviewed felt that wound healing was improved with total contact casting than with removable cast walkers, but that removable cast walkers were more convenient and came with a lower cost burden. They reported no experience or familiarity with irremovable cast walkers.
Conclusions
Ulcer healing improved with total contact casting, irremovable cast walkers, and removable cast walkers, but total contact casting and irremovable cast walkers had higher rates of ulcer healing than removable cast walkers. Increased access to offloading devices could result in cost savings for the health system because of fewer amputations. Patients with diabetic foot ulcers reported a preference for total contact casting over removable cast walkers, largely because they perceived wound healing to be improved with total contact casting. However, cost, comfort, and convenience are concerns for patients.
OBJECTIVE
This health technology assessment looked at the clinical benefits and harms, cost-effectiveness, cost utility, and patient experiences of fibreglass total contact casting, removable cast walkers, and irremovable cast walkers in patients with diabetic neuropathic foot ulcers to determine whether they should be publicly funded.
BACKGROUND
Health Condition
Diabetes can lead to nerve damage (diabetic neuropathy), causing muscle weakness or wasting and loss of pain and protective sensation.1 Loss of pain and feeling in the foot, combined with increased pressure from shoes, trauma, or foot deformity,1 all contribute to the development of foot ulcers.1,2
Foot ulcers can cause substantial morbidity (disease) and put people at risk for amputation of the foot or leg.3 Foot ulcers can also become infected, which impairs healing1,4 and further increases the risk of amputation.1
Clinical Need and Target Population
In Ontario in 2015, the estimated prevalence of diabetes was 1.5 million (10.2%).5 People with diabetes have a 15% to 25% lifetime risk of developing a foot ulcer,3,6,7 and estimates indicate that 2% to 3% of people with diabetes experience a foot ulcer in a given year.7
Compared with the general population, rates of diabetes are higher among people with First Nations,8 South Asian, Asian, African, or Hispanic heritage.5 Because of this, the prevalence of diabetes-related ulcers in these populations is also higher.9
Current Treatment Options
Treatment of diabetic neuropathic foot ulcers involves debridement (removing dead or diseased tissue), pressure offloading,10,11 infection control, and maintaining adequate circulation.4
Health Technology Under Review
Offloading (redistributing) pressure from high-pressure areas on the foot is a basic aspect of neuropathic foot ulcer care.12 Offloading interventions include wheelchairs or crutches and bed rest, but these options limit a person's mobility.13 Therapeutic shoes, felted foam, removable cast walkers, and total contact casting allow people to get around more easily.10,13 Many types of therapeutic shoes are available, including half-shoes, healing sandals, custom-made shoes, and depth-inlay shoes.14 However, these shoes have different characteristics and may differ in their ability to offload pressure.14
Total Contact Casting
Total contact casting can be prepared using different types of materials such as plaster or fibreglass.14 The cast is usually prepared using casting tape that is moulded to maintain contact with the sole of the foot and lower leg.14 The cast supports the foot and lower leg and redistributes pressure over the entire plantar surface (sole of the foot) to reduce pressure over the ulcer area.11,15,16 Casts may also help reduce or control swelling15,17 and protect the foot from infection.10 Because the cast is moulded to the patient's lower leg and foot, it may also be useful when premade cast walkers do not fit properly.16
Total contact casts cannot be removed by the patient, so they do not allow for daily inspection of the ulcer.18 For this reason, they are not recommended for patients with severe peripheral arterial disease15; untreated osteomyelitis or soft-tissue infections11; ulcers on the opposite foot; or poor balance (because of a risk of falls).2,12 Health Quality Ontario's Quality Standards on Diabetic Foot Ulcers will provide additional information about the recommended use of total contact casting.19 Total contact casts may affect daily activities, interfering with sleeping, bathing, and driving.14 Casts must be applied by a qualified health care professional2: they can irritate the skin and lead to more ulcers if they are not applied appropriately.12,14 They should be changed weekly,3 and they are time-consuming to apply and remove.4 The fact that total contact casts cannot be removed by the patient enforces treatment adherence, which may lead to improved outcomes.14
Note: Throughout the report, whenever we mention total contact casting, we are referring to fibreglass total contact casting unless specified otherwise.
Removable and Irremovable Cast Walkers
Removable cast walkers keep the ankle at a 90-degree angle, reducing pressure on the forefoot.4 They can be removed by the patient, allowing for frequent ulcer inspection and dressing changes.14 For this reason, they can be used for infected ulcers.14 Removable cast walkers also allow the patient to bathe and sleep more comfortably.10 However, the fact that they can be easily removed affects patient adherence and may have a negative effect on ulcer healing.14
Removable cast walkers can be made irremovable by securing them in place with a cohesive bandage, plaster, or fibreglass.14 Irremovable cast walkers enforce treatment adherence, because patients cannot take them off.14
Removable and irremovable cast walkers are not recommended in patients with poor balance or severe peripheral arterial disease.20 They are not custom-made, so they may not fit all patients, including those with very short legs, wide feet, or severe deformities.16
Regulatory Information
Cast walkers and the fibreglass tape used to prepare total contact casting and irremovable cast walkers are considered class I devices and do not require medical device licensing from Health Canada.
Ontario Context
In Ontario, patients pay for cast walkers. Patients pay out of pocket for the materials used to prepare the total contact cast, but application of the cast is publicly funded. Access to total contact casting may be limited by the need for qualified personnel to apply the cast. Geographic isolation may also be a concern, because patients need to make frequent clinic visits to have total contact casts or irremovable cast walkers replaced or reapplied.
CLINICAL EVIDENCE
Research Question
What are the clinical benefits and harms of total contact casting, removable cast walkers, and irremovable cast walkers compared with other offloading devices (including each other) and non-offloading treatments in patients with diabetic neuropathic foot ulcers?
Methods
Research questions were developed by Health Quality Ontario in consultation with patients, health care providers, clinical experts, and other health system stakeholders.
Literature Search
We performed a literature search on August 17, 2016, to retrieve studies published from inception to the search date. We used the Ovid interface to search the following databases: MEDLINE, Embase, Cochrane Central Register of Controlled Trials, Cochrane Database of Systematic Reviews, Health Technology Assessment, National Health Service Economic Evaluation Database (NHSEED), and Database of Abstracts of Reviews of Effects (DARE); we also used the EBSCOhost interface to search the Cumulative Index to Nursing & Allied Health Literature (CINAHL).
Search strategies were developed by medical librarians using controlled vocabulary (i.e., Medical Subject Headings) and relevant keywords. Search filters for randomized controlled trials, systematic reviews, meta-analyses, and health technology assessments were applied to the search strategies. The final search strategy was peer-reviewed using the PRESS Checklist.21 Database auto-alerts were created in MEDLINE, Embase, and CINAHL and monitored for the duration of the health technology assessment (HTA) review.
We performed targeted grey literature searching of HTA agency sites and clinical trial registries. We also reviewed reference lists of included studies for any additional studies not identified through the systematic search. See Appendix 1 for literature search strategies, including all search terms.
Literature Screening
A single reviewer reviewed the abstracts and, for those studies meeting the eligibility criteria, we obtained full-text articles. We also examined reference lists for any additional relevant studies not identified through the search.
Types of Participants
The population of interest included patients with type 1 or 2 diabetes who had neuropathic infected or noninfected foot ulcers.
Types of Interventions
The interventions evaluated were:
Fibreglass total contact casting
Removable cast walkers
Irremovable cast walkers
We included the following comparators:
The interventions listed above, compared to each other
Other offloading devices, such as total contact casting prepared using materials other than fibreglass, therapeutic shoes, custom braces, or ankle and foot orthoses
Non-offloading ulcer treatments (e.g., ulcer dressings)
Types of Outcomes Measures
Treatment discontinuations and reasons for discontinuation
Ulcer healing
Time to ulcer healing
Patient adherence to treatment, as measured by level of activity
Quality of life and patient satisfaction
Complications
Inclusion Criteria
English-language full-text publications in patients with diabetic, neuropathic, plantar ulcers (infected or noninfected)
Randomized controlled trials (RCTs) evaluating at least one of the interventions of interest
Studies with a mixed population, if at least 90% of the patients matched the population of interest
Studies in which less than 90% of the patients matched the population of interest but reported results separately for the population of interest
Exclusion Criteria
Nonrandomized controlled trials and noncomparative studies
Studies evaluating total contact casting prepared with materials other than fibreglass, unless fibreglass total contact casting was used as a comparator
Editorials, case reports, and commentaries
Data Extraction
We extracted relevant data on study characteristics and risk-of-bias items, and PICOT (population, intervention, comparison, outcome, time). We used a data form to collect information about:
Source (i.e., citation information, contact details, study type)
Methods (i.e., study design, study duration and years, participant allocation, allocation sequence concealment, blinding, reporting of missing data, reporting of outcomes, and whether or not the study compared two or more groups)
Outcomes (i.e., outcomes measured, number of participants for each outcome, number of participants missing for each outcome, outcome definition and source of information, unit of measurement, standard deviations or 95% confidence intervals [CIs], and time points at which outcome was assessed)
Baseline characteristics of the patients included in the studies, including those based on the PROGRESS-Plus categories (place of residence, race/ethnicity, occupation, gender, religion, education, socioeconomic status, social capital)22
We contacted authors of the studies to provide clarification when needed.
Statistical Analysis
For dichotomous variables, we presented the number and percentage of participants who experienced the outcome, the risk ratio, the risk difference, and 95% CIs. We reported the results of intention-to-treat analyses. We expressed results for continuous outcomes as mean difference and standard deviation (SD). For time to ulcer healing, we reported the results of Kaplan-Meier analyses.23
Quantitative syntheses of the individual studies were performed when appropriate and in the absence of substantial heterogeneity using Review Manager v. 5.3 (Copenhagen: The Nordic Cochrane Centre, The Cochrane Collaboration, 2014).24 Statistical heterogeneity was assessed using the I2 statistic.25 Graphical display of the forest plots was also examined. A P-value <0.05 was considered significant for the overall effect estimate.
Subgroup analyses were undertaken according to population subgroups such as ethnicity, comorbidities (diabetes control), adherence, ulcer characteristics, and any PROGRESS-Plus categories22 if the information was available.
Quality of Evidence
The level of quality of the body of evidence for each outcome was evaluated according to the Grading of Recommendations Assessment Development and Evaluation (GRADE) Handbook.26 We started with the assumption that randomized controlled trials are high quality, whereas observational studies are low quality. We then rated the studies based on the following considerations: risk of bias, inconsistency, indirectness, imprecision, publication bias, magnitude of effect, dose-response gradient, and any residual confounding factors. The overall quality was determined to be high, moderate, low, or very low using a step-wise, structural methodology. The quality level determination reflects our certainty about the evidence.
The quality of the randomized controlled trials was assessed according to the Cochrane Collaboration criteria for evaluating risk of bias (Appendix 2).27
Expert Consultation
Between August 2016 and January 2017, we sought expert consultation on the use of total contact casting, removable cast walkers, and irremovable cast walkers to treat diabetic neuropathic foot ulcers. Members of the consultation included physicians, nurses, and chiropodists who manage diabetic foot ulcers. The role of the expert advisors was to contextualize the evidence and provide advice on the use of the interventions being evaluated.
Results
Literature Search
The search yielded 329 citations published before August 17, 2016. After removing duplicates, we reviewed titles and abstracts to identify potentially relevant articles. We obtained the full texts of these articles for further assessment. Thirteen RCTs met the inclusion criteria.16,28–39 The results of one study were reported in two separate publications.38,40 We hand-searched the reference lists of the included studies, along with health technology websites and other sources, to identify additional relevant studies, but none were identified.
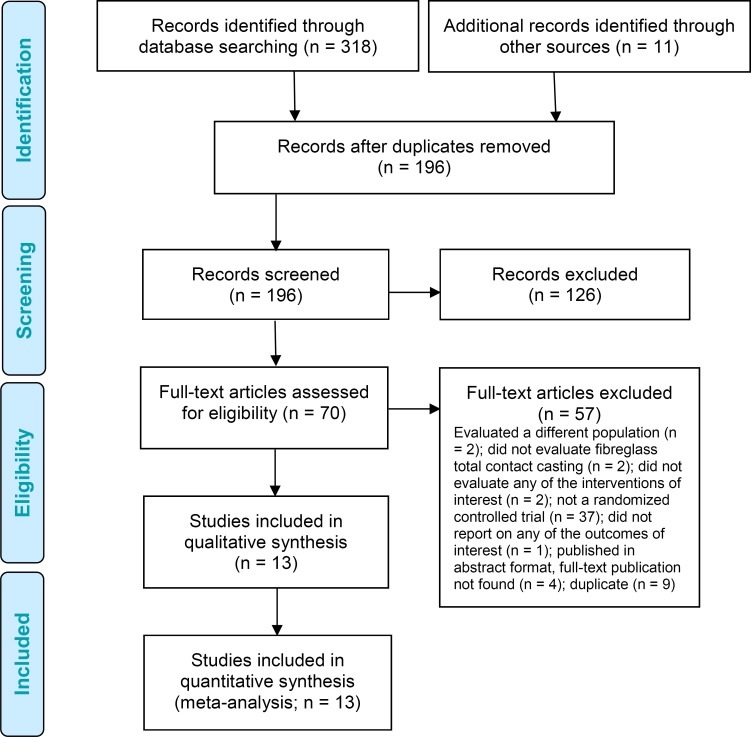
Figure 1 presents the flow diagram for the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA).
Figure 1: PRISMA Flow Diagram.
Abbreviation: PRISMA, Preferred Reporting Items for Systematic Reviews and Meta-analyses.
Source: Adapted from Moher et al.41
Design and Characteristics of the Included Studies
The 13 RCTs yielded a total of 19 treatment comparisons.16,28–39 Total contact casting was compared with irremovable cast walkers in three studies,28,29,36 with removable cast walkers in six studies,16,28,32–34,38 and with therapeutic shoes in five studies.16,31,35,38,39 Irremovable cast walkers were compared with removable cast walkers in three studies.28,30,37 Removable cast walkers were compared with therapeutic shoes in two studies.16,38
No studies compared irremovable cast walkers with therapeutic shoes. No studies compared any of the interventions with custom braces, ankle and foot orthoses, or non-offloading ulcer treatments.
The studies were conducted in the United States16,30,33,36–39 and Europe.28,29,31,32,34,35
In all studies that evaluated total contact casting (except for two in which the information was not provided35,36) the cast was prepared by wrapping fibreglass tape around the patient's lower leg and foot. Some used a mix of plaster (inner layer) and fibreglass.33,38,39 In five of the studies that used only fibreglass, casting tapes of two different rigidities were used.28,29,31,32,34 One study reported that patients were given crutches or a cane to aid with balance, if needed.35
The studies that evaluated removable and/or irremovable cast walkers used different walker brands. Irremovable cast walkers were prepared by wrapping a cohesive bandage30,36,37 or straps28,29 around a removable cast walker. The studies used different types of therapeutic shoes as comparators, such as healing sandals,16,39 half-shoes,38 custom-made temporary shoes,35 and therapeutic shoes with a rocker-bottom sole.31
Sample sizes were small, with 11 to 30 patients per study group. The duration of follow-up was 3 months in most studies, 4 months in one study,35 and 1 month in another,31 or until ulcer closure, whichever came first.
The studies evaluated the percentage of ulcers healed, time to healing, and discontinuations. Three studies also assessed patient adherence to treatment by measuring the daily level of activity with a pedometer or an activity sensor.16,30,38 Five studies assessed patient quality of life and/or satisfaction with treatment using the visual analogue scale or the Short-Form 36 questionnaire.16,28,29,31,40 Treatment complications were among the outcomes defined a priori in some studies.28,29,31,35,36,39 One study prospectively assessed the occurrence of ulcer infection, but no other treatment complications.16 The other studies reported some treatment complications without prespecifying complications as a study outcome.30,32–34,37,38
Appendix 3 provides more detailed information about study design and characteristics.
Definitions and Patient Characteristics in the Included Studies
Most study participants were men (56% to 91%).16,28–31,33–39 Two studies reported patients' ethnicity. One reported that 34% of participants were white, 59% were Hispanic, and 5% were African-American.16 The other reported that 12% were white, 61% were Hispanic, and 34% were black.36
The studies generally included patients with diabetes who had noninfected neuropathic plantar ulcers. They generally excluded patients with peripheral arterial disease, although some included patients with mild to moderate peripheral arterial disease.16,30–32,35,37 The definitions of peripheral neuropathy and peripheral arterial disease used in the studies are presented in Appendix 4.
Some studies included only patients with forefoot ulcers,16,28,29,34,37 and some included patients with midfoot (13% to 27%)30,33,35,36,39 and heel ulcers30,36,39 (5%36 and 7.5%39 in the studies that provided this information).
The ulcers evaluated in the studies were classified as grade 1 or 2 according to the University of Texas Wound Grading System (Appendix 4). Five studies included mostly grade 1 ulcers (superficial wound not involving tendon, capsule, or bone): 100% in three studies34,37,38 and 70% to 75% in two studies.28,39 The remaining studies included grade 1 and 2 ulcers (wound penetrating to tendon or capsule), except for three that did not provide this information.30–32
The mean ulcer area at baseline varied between 1 and 4 cm2 in most studies. In one study that compared irremovable and removable cast walkers, the mean (SD) ulcer areas at baseline were 6.5 (8.5) and 10.1 (12.0) cm2, respectively,30 but ulcer classification and duration were not reported.
Ulcer healing was defined as complete re-epithelialization of the ulcerated area. Patients who discontinued treatment were considered unhealed (Appendix 4).
In most studies, information was not available on ulcer duration before study enrolment, ulcer history, or prior amputation. None of the studies provided information on ulcer treatment prior to enrolment.
Additional patient baseline characteristics are presented in Appendix 5.
Methodological Quality of the Included Studies
Complete results of the methodology checklist for included studies are presented in Appendix 2.
It was not possible to blind the patients or the treating physician to the treatment assignment, although some studies did attempt to blind the outcome assessor to the treatment group. Nevertheless, we did not consider lack of blinding to confer a high risk of bias for the main outcomes of ulcer healing and time to ulcer healing. There were very few losses to follow-up in the studies identified. The sample sizes were small; as a result, despite adequate randomization, differences in baseline characteristics between study groups could not be ruled out.
Overall, the risk of bias was low in the studies identified, especially for ulcer healing.
Intention-to-treat analysis was used for ulcer healing; patients whose ulcer did not heal and patients who discontinued treatment or were lost to follow-up were considered to be unhealed.
Results for Total Contact Casting Versus Irremovable Cast Walkers
Three studies compared total contact casting with irremovable cast walkers.28,29,36
Treatment Discontinuation
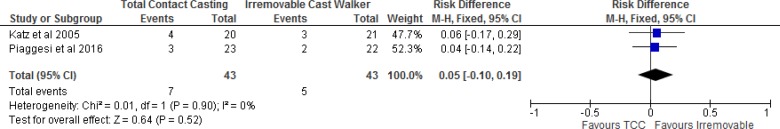
One study reported no treatment discontinuations.29 In the other two, treatment discontinuations occurred in 13% and 20% of the total contact casting group and 9% and 14% of the irremovable cast walker group.28,36 Treatment discontinuations resulted from voluntary withdrawal and losses to follow-up (Table 1). We found no statistically significant difference in treatment discontinuations between groups based on the results of the two studies (Figure 2).
Table 1:
Total Contact Casting Versus Irremovable Cast Walkers
| Author, Year N (TCC/ICW) Follow-up | Treatment Discontinuation, n (%) | Ulcer Healing, n (%) | Mean Time to Ulcer Healing, d (SD) |
|---|---|---|---|
| Piaggesi et al, 201628 45 (23/22) 3 months |
Overall TCC: 3 (13.0) ICW: 2 (9.1) Voluntary withdrawal TCC: 3 (13.0) ICW: 1 (4.5) Lost to follow-up TCC: 0 ICW: 1 (4.5) |
TCC: 19 (82.6) ICW: 18 (81.8) |
TCC: 37.0 (21.6) ICW: 39.6 (12.2) Kaplan-Meier curve showed no statistically significant difference between groups |
| Piaggesi et al, 200729 40 (20/20) 3 months |
No treatment discontinuation reported | TCC: 19 (95.0) ICW: 17 (85.0) P = .21 |
TCC: 45.5 (30.8) ICW: 46.9 (23.8) P = .87 Kaplan-Meier curve showed no statistically significant difference between groups |
| Katz et al, 200536 41 (20/21) 3 months |
Overall TCC: 4 (20.0) ICW: 3 (14.3) Lost to follow-up TCC: 4 (20.0) ICW: 2 (9.5) Osteomyelitis (before starting treatment) TCC: 0 ICW: 1 (4.8) |
TCC: NA (74.0) ICW: NA (80.0) P = .65 |
Median (IQR) TCC: 35 (21–49) ICW: 28 (21–49) P = .65 |
Abbreviations: ICW, irremovable cast walker; IQR, interquartile range; NA, not available; SD, standard deviation; TCC, total contact casting.
Figure 2: Total Contact Casting Versus Irremovable Cast Walkers, Treatment Discontinuations.
Abbreviations: CI, confidence interval; M-H, Mantel-Haenszel; TCC, total contact casting.
Ulcer Healing
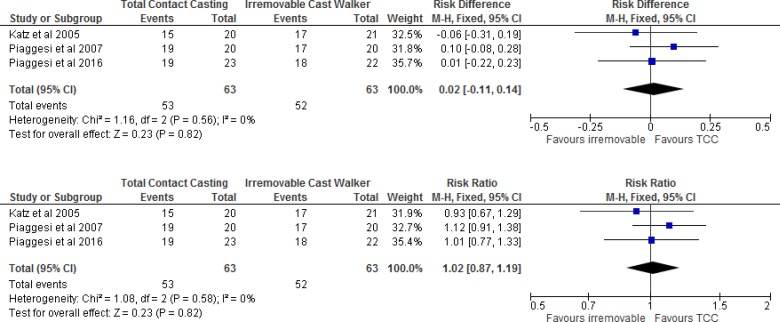
At 3 months' follow-up, the percentage of patients with a healed ulcer was between 74% and 95% for total contact casting, and between 80% and 85% for irremovable cast walkers (Table 1). We found no statistically significant difference between the two groups when we combined the results of the studies (Figure 3).
Figure 3: Total Contact Casting Versus Irremovable Cast Walkers, Percentage of Healed Ulcersa.
Abbreviations: CI, confidence interval; M-H, Mantel-Haenszel; TCC, total contact casting.
aKatz et al provided the percentage of healed ulcers, but not the exact number of patients who had a healed ulcer. We calculated the number of patients with a healed ulcer based on the total number of patients in each treatment group and the percentage of healed ulcers in each group.
Time to Ulcer Healing
Based on survival (Kaplan-Meier) analyses from two studies, we found no statistically significant difference in time to healing between the two groups over 3 months of follow-up (Table 1).28,29
Patient Satisfaction
One study reported that patients treated with irremovable cast walkers had a higher level of satisfaction (visual analogue scale; mean [SD] 8.45 [1.79] for irremovable cast walkers and 6.85 [2.39] for total contact casting; P < .05).29 However, another study found no difference between the two groups (figures not provided).28
Complications
In one study, 6 patients (30%) in the total contact casting group and 5 (25%) in the irremovable cast walker group experienced complications, none of which resulted in treatment discontinuation (Table 2).29 In another,36 13 patients (65%) in the total contact casting group and eight patients (38%) in the irremovable cast walker group reported complications that were considered to be potential side effects of treatment (some patients had more than one complication). In the third study, 7 patients in the total contact casting group (30%) and two patients (9%) in the irremovable cast walker group reported complications, none of them serious or leading to discontinuation.28 However, differences in the proportion of complications between the two groups were difficult to interpret owing to the small number of events reported.
Table 2:
Total Contact Casting Versus Irremovable Cast Walkers, Complications
| Author, Year N (TCC/ICW) | Complication, n (%) | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Skin Maceration | Ulcer Infection | New Ulcer | Amputation | Broken Cast | Fall | Abrasion | Trauma | Other | |
| Piaggesi et al, 201628 45 (23/22) |
TCC: 0 ICW: 1 (4.5) |
Not reported | Not reported | Not reported |
Broken cast TCC: 3 (13.0) ICW: 0 |
Not reported | TCC: 4 (17.4) ICW: 0 |
Accidental minor trauma in contralateral foot TCC: 0 ICW: 1 (4.5) |
Not reported |
| Piaggesi et al, 200729 40 (20/20) |
TCC: 4 (20.0) ICW: 2 (10.0) |
TCC: 1 (5.0) ICW: 1 (5.0) Did not lead to discontinuation |
TCC: 0 ICW: 0 |
Not reported |
Partial cast rupture TCC: 1 (5.0) ICW: 0 |
Not reported | Not reported | Not reported |
Transient paresthesia TCC: 0 ICW: 1 (5.0) Superficial hematoma of the calf due to accidental trauma TCC: 0 ICW: 1 (5.0) |
| Katz et al, 200536 41 (20/21) |
TCC: 7 (35.0) ICW: 6 (28.6) P = .49 |
Not reported |
Second ulcer ICW: 1 (5.0) P = .53 Kissing ulcer TCC: 1 (5.0) ICW: 0 P = .33 |
Toe TCC: 1 (5.0; kissing ulcer) ICW: 1 (5.0; nonadherence) P = .97 |
Broken cast TCC: 3 (15.0) TCC: 1 (5.0) P = .29 |
TCC: 0 ICW: 1 (5.0) P = .35 |
TCC: 2 (10.0) ICW: 0 P = .15 |
Not reported |
Edema TCC: 2 (10.0) ICW: 1 (5.0) ICW: 0 P = .33 |
Abbreviations: ICW, irremovable cast walker; TCC, total contact casting.
Quality of Evidence
Table 3 provides the GRADE evidence profile for total contact casting versus irremovable cast walkers.
Table 3:
GRADE Evidence Profile for Total Contact Casting Versus Irremovable Cast Walkers
| Number of Studies (Design) | Risk of Bias | Inconsistency | Indirectness | Imprecision | Publication Bias | Upgrade Considerations | Quality |
|---|---|---|---|---|---|---|---|
| Percentage of Patients with a Healed Ulcer | |||||||
| 3 (RCTs)28,29,36 | No serious limitations | No serious limitations | No serious limitations | Very serious limitations (−2)a | Undetected | None | ⊕⊕ Low |
| Time to Healing (Kaplan-Meier Analysis) | |||||||
| 2 (RCTs)28,29 | No serious limitations | No serious limitations | No serious limitations | Very serious limitations (−2)b | Undetected | None | ⊕⊕ Low |
| Patient Satisfaction With Treatment | |||||||
| 2 (RCTs)28,29 | No serious limitations | Serious limitations (−1)c | No serious limitations | Serious limitations (−1)d | Undetected | None | ⊕⊕ Low |
| Complications | |||||||
| 3 (RCTs)28,29,36 | No serious limitations | No serious limitations | No serious limitations | Very serious limitations (−2)e | Undetected | None | ⊕⊕ Low |
Abbreviations: GRADE, Grading of Recommendations Assessment, Development, and Evaluation; RCT, randomized controlled trial.
Very low statistical power to detect a statistically significant difference between groups.
No statistically significant difference between the two groups in the studies identified.
Study results were inconsistent.
Some of the studies did not find a statistically significant difference between the study groups.
Very few events reported in the studies, leading to very low statistical power to detect a difference between groups.
Results for Total Contact Casting Versus Removable Cast Walkers
Six studies compared total contact casting with removable cast walkers.16,28,32–34,38
Treatment Discontinuation
There was a large variation across studies in the percentage of patients who discontinued treatment. Treatment discontinuations occurred in 8% to 24% of patients in the total contact casting group and 0% to 44% of patients in the removable cast walker group. Reasons for discontinuation included complications, voluntary withdrawal, and nonadherence (Table 4). When we pooled the results, we found no statistically significant difference between groups (Figure 4).
Table 4:
Total Contact Casting Versus Removable Cast Walkers
| Author, Year N (TCC/RCW) Follow-up | Treatment Discontinuation, n (%) | Ulcer Healing, n (%) | Mean Time to Ulcer Healing, d (SD) |
|---|---|---|---|
| Piaggesi et al, 201628 43 (23/20) 3 months |
Overall TCC: 3 (13.0) RCW: 0 Voluntary withdrawal TCC: 3 (13.0) RCW: 0 |
TCC: 19 (82.6) RCW: 16 (80.0) |
TCC: 37.0 (21.6) RCW: 43.2 (15.1) Kaplan-Meier curve showed no statistically significant difference between groups |
| Lavery et al, 201516 50 (23/27) 3 months |
Overall TCC: 5 (21.7) RCW: 12 (44.4) Complications TCC: 1 (4.3; infection) RCW: 5 (18.5; infection 4, device-related ulcer 1) Voluntary withdrawal TCC: 4 (17.4) RCW: 4 (14.8) Nonadherence TCC: 0 RCW: 3 (11.1) |
TCC: 16 (69.6) RCW: 6 (22.2) Statistically significant (P-value not provided) |
TCC: 37.8 (20.3) RCW: 46.9 (30.1) P = .22 |
| Gutekunst et al, 201133 23 (11/12) >3 months |
Not reported | TCC: 9 (81.8) RCW: 5 (41.7) P < .05 |
TCC: 95 (61) RCW: 94 (64) Not statistically significant |
| Faglia et al, 201034 48 (25/23) 3 months |
Overall TCC: 2 (8.0) RCW: 1 (4.3) Complications TCC: 1 (4.0; ulcer on contralateral foot) RCW: 1 (4.3; ulcer infection requiring antibiotic therapy and more frequent clinic visits) Voluntary withdrawal TCC: 1 (4.0) RCW: 0 |
TCC: 17 (68.0) RCW: 16 (69.6) |
TCC: 35.3 (3.1) RCW 39.7 (4.2) P = .71 Kaplan-Meier curve showed no difference between groups P = .79 |
| Caravaggi et al, 200732 60 (30/30) 3 months |
Overall TCC: 6 (20.0) RCW: 7 (23.3) Complications TCC: 5 (16.7) RCW: 6 (20.0) Nonadherence TCC: 1 (3.3) RCW: 1 (3.3) |
TCC: 24 (80.0) RCW: 23 (76.7) Not statistically significant |
TCC: 48 (NA) RCW: 71 (NA) Statistically significant (P-value not provided) Kaplan-Meier curve showed a faster heating rate with TCC vs. RCW P < .005 |
| Armstrong et al, 200138 50 (25/25) 3 months |
Overall TCC: 6 (24.0) RCW: 5 (20.0) Discomfort TCC: 4 (16.0) RCW: 3 (12.0) Lost to follow-up TCC: 2 (8.0) RCW: 2 (8.0) |
TCC: 17 (68.0) RCW: 13 (52.0) |
TCC: 33.5 (24.3) RCW: 50.4 (26.0) P = .07 Kaplan-Meier curve showed a faster heating rate with TCC vs. RCW P = .033 |
Abbreviations: NA, not available; RCW, removable cast walker; TCC, total contact casting.
Figure 4: Total Contact Casting Versus Removable Cast Walkers, Treatment Discontinuations.
Abbreviations: CI, confidence interval; M-H, Mantel-Haenszel; TCC, total contact casting.
Sources: Armstrong et al,38Caravaggi et al,32Faglia et al,34Lavery et al,16and Piaggesi et al.28
Ulcer Healing
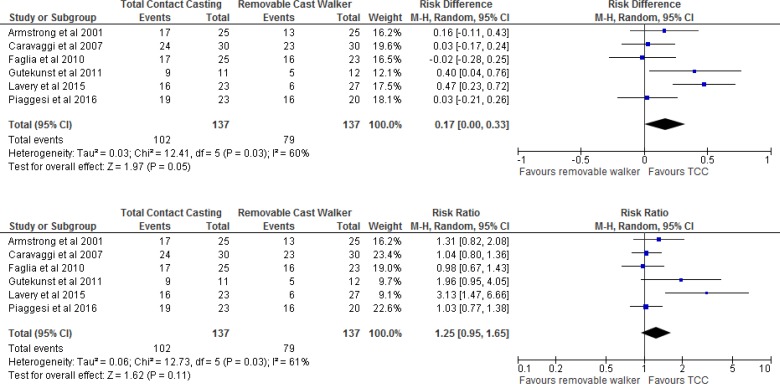
At 3 months of follow-up, the percentage of patients with a healed ulcer varied between 68% and 83% with total contact casting, and between 22% and 80% with removable cast walkers. Pooling the results yielded an absolute increase of 17% (risk difference 0.17 [95% confidence interval 0.00–0.33]) in the percentage of healed ulcers with total contact casting compared with removable cast walkers (Figure 5).
Figure 5: Total Contact Casting Versus Removable Cast Walkers, Percentage of Healed Ulcers.
Abbreviations: CI, confidence interval; M-H, Mantel-Haenszel; TCC, total contact casting.
Sources: Armstrong et al,38Caravaggi et al,32Faglia et al,34Gutekunst et al,33Lavery et al,16and Piaggesi et al.28
The level of heterogeneity we found (I2 = 61%) may be partially explained by the different rates of discontinuation across the studies. According to Lavery et al,16 the large proportion of treatment discontinuations with removable cast walkers affects treatment success and may explain the large variation among studies in the percentage of ulcers healed. This suggestion was corroborated by other authors' comments that poor adherence to the removable cast walker may affect its healing ability and its inferior results compared to total contact casting.33,34 Piaggesi et al28 acknowledged that the lack of difference they found in ulcer healing between the two groups was in contrast to what other studies had demonstrated. They believed that this finding may have been due in part to high patient adherence with the removable cast walker in their study, possibly because it included weekly reinforcement of the importance of adherence.28
The small sample sizes may also explain the heterogeneity we found. Although these studies were randomized, we could not rule out the possibility that differences in baseline characteristics may still have been present because of the small sample sizes, and this could explain the differences in point estimates across studies.
Time to Ulcer Healing
Among four studies that evaluated time to ulcer healing using survival (Kaplan-Meier) analysis, two found no statistically significant difference between the groups,28,34 and two showed statistically significantly faster healing with total contact casting than with removable cast walkers (Table 4).32,38
Adherence to Treatment and Daily Activity
Two studies assessed treatment adherence by measuring the level of daily activity.16,38 The difference between total contact casting and removable cast walkers was not statistically significant, with a mean (SD) daily number of steps of 1,447 (1,310) versus 1,404 (1,234) in one study,16 and 600 (320) versus 768 (563)38 in the other.
Quality of Life and Patient Satisfaction
Armstrong et al40 showed that the change in physical and mental health scores before and after treatment (measured using the Short-Form 36-item health survey) did not differ between the two groups.
Among two studies that evaluated patient satisfaction using a visual analogue scale, one found no statistically significant difference between the two groups,16 and the other reported statistically significantly higher patient satisfaction with removable cast walkers.28
Complications
Five studies reported complications with total contact casting or removable cast walkers (Table 5).16,28,32,34,38 Differences in the proportion of complications between the two groups were difficult to interpret owing to the small sample sizes and the small number of events.
Table 5:
Total Contact Casting Versus Removable Cast Walkers, Complications
| Author, Year N (TCC/RCW) | Complication, n (%) | ||||||
|---|---|---|---|---|---|---|---|
| Skin Maceration | Ulcer Infection | New Ulcer | Cast Rupture | Fall | Hitching | Abrasion | |
| Piaggesi et al, 201628 43 (23/20) |
Not reported |
Fungal intertrigo TCC: 0 RCW: 1 (5.0) |
Not reported |
Broken cast TCC: 3 (13.0) RCW: 0 |
Not reported | Not reported |
Traumatic abrasion TCC: 3 (13.0) RCW: 0 |
| Lavery et al, 201516 50 (23/27) |
Not reported |
Infection leading to treatment discontinuation TCC: 1 (4.3) RCW: 4 (14.8) |
Iatrogenic ulcers TCC: 0 RCW: 1 (3.7) |
Not reported | Not reported | Not reported | Not reported |
| Faglia et al, 201034 48 (25/23) |
TCC: 0 RCW: 1 (4.3) |
Infection leading to treatment discontinuation TCC: 0 RCW: 1 (4.3) |
Ulcer on the contralateral foot TCC: 1 (4.0) RCW: 0 |
Stirrup rupture (replaced without removing cast) TCC: 1 (4.0) RCW: 0 |
Not reported | TCC: 1 (4.0; resolved after removal of the German cotton) RCW: 0 after removal of the German cotton |
Not reported |
| Caravaggi et al, 200732 60 (30/30) |
Not reported |
Serious infection requiring discontinuation, antibiotics, and surgical debridement TCC: 5 (17.2) RCW: 6 (20.7) Not significant |
Not reported | Not reported | Not reported | Not reported | Not reported |
| Armstrong et al, 200138 50 (25/25) |
Not reported | Not reported |
Device-related ulcerations TCC: 0 RCW: 0 |
Not reported | TCC: 0 RCW: 0 |
Not reported | Not reported |
Abbreviations: RCW, removable cast walker; TCC, total contact casting.
Quality of Evidence
Table 6 provides the GRADE evidence profile for total contact casting versus removable cast walkers.
Table 6:
GRADE Evidence Profile for Total Contact Casting Versus Removable Cast Walkers
| Number of Studies (Design) | Risk of Bias | Inconsistency | Indirectness | Imprecision | Publication Bias | Upgrade Considerations | Quality |
|---|---|---|---|---|---|---|---|
| Percentage of Patients with a Healed Ulcer | |||||||
| 6 (RCTs)16,28,32–34,38 | No serious limitations | Serious limitations (−1)a | No serious limitations | No serious limitationsb | Undetected | None | ⊕⊕⊕ Moderate |
| Time to Healing (Kaplan-Meier Analysis) | |||||||
| 4 (RCTs)28,32,34,38 | No serious limitations | Serious limitations (−1)a | No serious limitations | Serious limitations (−1)c | Undetected | None | ⊕⊕ Low |
| Patient Satisfaction With Treatment | |||||||
| 2 (RCTs)16,28 | No serious limitations | Serious limitations (−1)a | No serious limitations | Serious limitations (−1)d | Undetected | None | ⊕⊕ Low |
| Quality of Life | |||||||
| 1 (RCT)40 | No serious limitations | Could not be evaluated | No serious limitations | Very serious limitations (−2)e | Undetected | None | ⊕⊕ Low |
| Complications | |||||||
| 5 (RCTs)16,28,32,34,38 | Serious limitations (−1)f | No serious limitations | No serious limitations | Very serious limitations (−2)g | Undetected | None | ⊕ Very Low |
Abbreviations: GRADE, Grading of Recommendations Assessment, Development, and Evaluation; RCT, randomized controlled trial.
The results were inconsistent across studies.
The lower limit of the confidence interval included the null; however, we did not determine that this warranted further downgrading the evidence, because it was already downgraded for inconsistency (which may have been the cause of the imprecision). Furthermore, the optimal information size was achieved when the studies were combined.
Some studies found a statistically significant difference in time to healing between the two groups, but other studies did not.
Some studies did not find a statistically significant difference between groups.
No statistically significant difference between groups. Only one small study (21 patients/study group) assessed the outcome.
Treatment complications were not defined as an outcome a priori in the studies included in this analysis.
Very few events were reported in the studies, leading to very low statistical power to detect a difference between groups.
Results for Total Contact Casting Versus Therapeutic Shoes
Five studies compared total contact casting with therapeutic shoes.16,31,35,38,39 The length of follow-up was 1 month in one study31 and 3 to 4 months in the others. Different types of shoes were used in the comparator group, including healing sandals,16,39 custom-made shoes,35 half-shoes,38 and therapeutic shoes.31
Treatment Discontinuation
Based on the results of four studies, 5% to 24% of patients in the total contact casting group and 0 to 13% of patients in the therapeutic shoes group discontinued treatment16,35,38 (unclear in one study39). One study did not report on treatment discontinuations.31 Reasons for discontinuations included complications, voluntary withdrawal, and losses to follow-up (Table 5). When we pooled the results of the studies, treatment discontinuations occurred more frequently with total contact casting than with therapeutic shoes (Figure 6).
Figure 6: Total Contact Casting Versus Therapeutic Shoes, Treatment Discontinuations.
Abbreviations: CI, confidence interval; M-H, Mantel-Haenszel; TCC, total contact casting.
Sources: Armstrong et al,38 Lavery et al,16 Mueller et al,39 and Van de Weg et al.35
Ulcer Healing
One study provided results for only 1 month of follow-up. The percentage of patients with a healed ulcer were 50% with total contact casting and 21% with therapeutic shoes.31
Three studies reported ulcer healing in 68% to 90% of patients in the total contact casting group and 32% to 56% in the therapeutic shoes group after 3 to 4 months of follow-up.16,38,39 In contrast, Van de Weg et al35 reported ulcer healing of 26% in the total contact casting group and 30% in the therapeutic shoes group. It is not clear why the findings of this study were different from those of the other three.
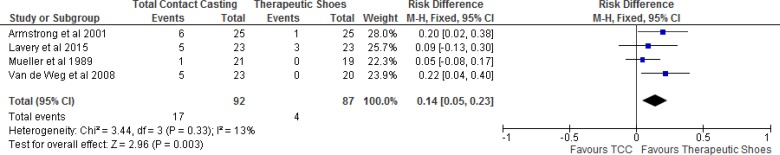
Our meta-analysis showed a statistically significant improvement in ulcer healing with total contact casting compared with therapeutic shoes within 1 to 4 months of follow-up (Figure 7).
Figure 7: Total Contact Casting Versus Therapeutic Shoes, Percentage of Healed Ulcers.
Abbreviations: CI, confidence interval; M-H, Mantel-Haenszel; TCC, total contact casting.
Sources: Armstrong et al,38 Caravaggi et al,31 Lavery et al,16 Mueller et al,39 and Van de Weg et al.35
The studies used different types of therapeutic shoes, which may have contributed to the heterogeneity we observed. Moreover, although these studies were randomized, we could not rule out the possibility that differences in baseline characteristics may have been present in some studies given the small sample sizes; this could also have explained part of the heterogeneity.
Time to Ulcer Healing
One study evaluated the time to ulcer healing using survival analysis and found a statistically significantly shorter healing time with total contact casting than with a half-shoe (Table 7).38
Table 7:
Total Contact Casting Versus Therapeutic Shoes
| Author, Year N (TCC/Shoes) Follow-up | Treatment Discontinuations, n (%) | Ulcer Healing, n (%) | Mean Time to Ulcer Healing, d (SD) |
|---|---|---|---|
| Lavery et al, 201516 46 (23/23) 3 months |
Overall TCC: 5 (21.7) Shoes: 3 (13.0) Complications TCC: 1 (4.3) Shoes: 3 (13.0) Voluntary withdrawal TCC: 4 (17.4) Shoes: 0 |
TCC: 16 (69.6) Shoes: 10 (43.5) Not statistically significant |
TCC: 37.8 (20.3) Shoes: 62.3 (24.5) P < .001 |
| Van de Weg et al, 200835 43 (23/20) 4 months |
TCC: 5 (21.7; 3 before starting treatment) Shoes: 0 Reasons for discontinuation: lost to follow-up 2 (8.7); death 1 (4.3); amputation 1 (4.3); crossover 1 (4.3) Unclear if death or amputation occurred before or after start of treatment |
TCC: 6 (26.1) Shoes: 6 (30.0) |
TCC: 59 (39) Shoes: 90 (12) P = .11 |
| Armstrong et al, 200138 50 (25/25) 3 months |
Overall TCC: 6 (24.0) Shoes: 1 (4.0) Discomfort TCC: 4 (16.0) Shoes: 0 Instability TCC: 0 Shoes: 1 (4.0) Lost to follow-up TCC: 2 (8.0) Shoes: 0 |
TCC: 17 (68.0) Shoes: 14 (56.0) P = .03 |
TCC: 33.5 (24.3) Shoes: 61.0 (23.4) P = .005 Kaplan-Meier curve showed a faster healing rate with TCC vs. half-shoe P = .012 |
| Caravaggi et al, 200031 50 (26/24) 30 days |
Not reported | TCC: 13 (50.0) Shoes: 5 (20.8) P = .032 |
Not reported |
| Mueller et al, 198939 40 (21/19) Duration of follow-up unclear |
Overall TCC: 1 (4.8; voluntary withdrawal) Shoes: unclear |
TCC: 19 (90.5) Shoes: 6 (31.6) P < .05 |
TCC: 42 (29) Shoes: 65 (29) |
Abbreviations: Shoes, therapeutic shoes; SD, standard deviation; TCC, total contact casting.
Adherence to Treatment and Daily Activity
Two studies assessed treatment adherence as measured by level of daily activity.16,38 The mean (SD) number of daily steps was lower with total contact casting than with therapeutic shoes in both studies: 1,447 (1,310) versus 4,022 (4,652), P = .014; and 600 (320) versus 1,462 (1,452), P = .04.16,38
Quality of Life and Patient Acceptance
The study by Armstrong et al40 showed that changes in physical and mental health scores before and after treatment as measured by the Short-Form 36-item health survey did not differ between the two groups.
Caravaggi et al31 measured patient acceptance of treatment at the end of 1-month follow-up with a visual analogue scale (1–100). They observed no statistically significant difference between the total contact casting group (mean 88.3, SD 17.3) and the therapeutic shoes group (mean 91.2, SD 9.9). Similarly, Lavery et al16 found no statistically significant difference in patient satisfaction between the groups.
Complications
Five studies reported complications with total contact casting or therapeutic shoes (Table 8).16,31,35,38,39 Differences in the proportion of complications between the two groups were difficult to interpret because of the small sample sizes and low number of events.
Table 8:
Total Contact Casting Versus Therapeutic Shoes, Complications
| Author, Year N (TCC/Shoes) | Complication, n (%) | |||||
|---|---|---|---|---|---|---|
| Skin Abrasion | Ulcer Infection | Amputation | New Ulcer | Fall | Edema | |
| Lavery et al, 201516 46 (23/23) |
Not reported | TCC: 1 (4.3) Shoes: 3 (13.0) |
Not reported | TCC: 0 Shoes: 0 |
Not reported | Not reported |
| Van de Weg et al, 200835 43 (23/20) |
Minor abrasion TCC: 0 Shoes: 2 (10.0) |
Not reported | Unclear | Not reported | Not reported | Not reported |
| Armstrong et al, 200138 50 (25/25) |
Not reported | Not reported | Not reported |
Device-related ulcerations TCC: 0 Shoes: 0 |
TCC: 0 Shoes: 0 |
Not reported |
| Caravaggi et al, 200031 50 (26/24) |
0 | Not reported | Not reported | 0 | Not reported | 0 |
| Mueller et al, 198939 40 (21/19) |
TCC: 0 Shoes: not reported |
Serious infection requiring admission to hospital TCC: 0 Shoes: 5 (26.3) P < .05 Fungal infection TCC: 3 (14.3) Shoes: 0 Did not lead to discontinuation |
Forefoot amputation due to serious infection TCC: 0 Shoes: 2 (10.5) |
Not reported | Not reported | Not reported |
Abbreviations: Shoes, therapeutic shoes; TCC, total contact casting.
Van de Weg et al35 reported five complications believed to be associated with total contact casting that led to treatment discontinuation, but they did not specify the types of complications. The study also reported one death and one amputation in the total contact casting group; however, based on the information provided by the authors, we could not determine whether these complications were associated with the treatment.35 Moreover, given that three patients were assigned to total contact casting but did not receive treatment, we could not tell whether these events occurred before or after the treatment started. We attempted to contact the authors of the study for clarification, but we received no response.
Quality of Evidence
Table 9 provides the GRADE evidence profile for total contact casting versus therapeutic shoes.
Table 9:
GRADE Evidence Profile for Total Contact Casting Versus Therapeutic Shoes
| Number of Studies (Design) | Risk of Bias | Inconsistency | Indirectness | Imprecision | Publication Bias | Upgrade Considerations | Quality |
|---|---|---|---|---|---|---|---|
| Percentage of Patients with a Healed Ulcer | |||||||
| 5 (RCTs)16,31,35,38,39 | No serious limitations | No serious limitations | Serious limitations (−1)a | No serious limitations | Undetected | None | ⊕⊕⊕ Moderate |
| Time to Healing (Kaplan-Meier Analysis) | |||||||
| 1 (RCT)38 | No serious limitations | Could not be evaluated | Serious limitations (−1)a | No serious limitations | Undetected | None | ⊕⊕⊕ Moderate |
| Patient Satisfaction With Treatment | |||||||
| 2 (RCTs)16,31 | No serious limitations | No serious limitations | Serious limitations (−1)a | Serious limitations (−1)b | Undetected | None | ⊕⊕ Low |
| Quality of Life | |||||||
| 1 (RCT)40 | No serious limitations | Could not be evaluated | Serious limitations (−1)a | Very serious limitations (−2)c | Undetected | None | ⊕ Very Low |
| Complications | |||||||
| 5 (RCTs)16,31,35,38,39 | No serious limitations | No serious limitations | Serious limitations (−1)a | Very serious limitations (−2)d | Undetected | None | ⊕ Very Low |
Abbreviations: GRADE, Grading of Recommendations Assessment, Development, and Evaluation; RCT, randomized controlled trial.
Different types of therapeutic shoes were used in the studies; the results with one type of shoe may not be applicable to other types.
Some of the studies did not find a statistically significant difference between study groups.
No statistically significant difference between groups. Only one small study (21 patients/study group) assessed the outcome.
Very few events reported in the studies, leading to very low statistical power to detect a difference between groups.
Results for Irremovable Cast Walkers Versus Removable Cast Walkers
Three studies compared irremovable cast walkers with removable cast walkers.28,30,37
Treatment Discontinuations
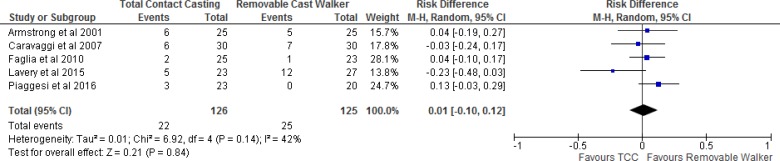
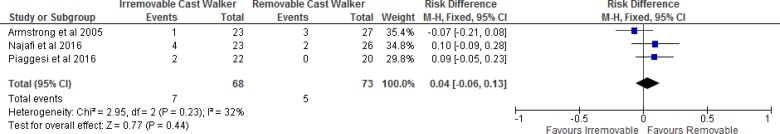
Treatment discontinuations varied between 4% and 17% in the irremovable cast walker group and 0% and 11% in the removable cast walker group.28,30,37 Reasons for discontinuation included discomfort, voluntary withdrawal, and losses to follow-up. Additional information is presented in Table 10. When we pooled the results of the studies, we found no statistically significant difference between groups (Figure 8).
Table 10:
Irremovable Cast Walkers Versus Removable Cast Walkers
| Author, Year N (ICW/RCW) Follow-up | Treatment Discontinuation, n (%) | Ulcer Healing, n (%) | Mean Time to Ulcer Healing, d (SD) |
|---|---|---|---|
| Najafi et al, 201630 49 (23/26a) 3 months |
Overall ICW: 4 (17.4) RCW: 2 (7.7) Infection ICW: 2 (8.7) RCW: 0 Surgical closure of the wound ICW: 1 (4.3) RCW: 1 (3.8) Lost to follow-up ICW: 1 (4.3) RCW: 1 (3.8) |
ICW: 16 (69.6) RCW: 10 (38.5) |
Not provided |
| Piaggesi et al, 201628 42 (22/20) 3 months |
Overall ICW: 2 (9.1) RCW: 0 Voluntary withdrawal ICW: 1 (4.5) RCW: 0 Lost to follow-up ICW: 1 (4.5) RCW: 0 |
ICW: 18 (81.8) RCW: 16 (80.0) |
ICW: 39.6 (12.2) RCW: 43.2 (15.1) Kaplan-Meier curve showed no statistically significant difference between groups |
| Armstrong et al, 200537 50 (23/27) 3 months |
Overall ICW: 1 (4.3) RCW: 3 (11.1) Discomfort/weight of device ICW: 1 (4.3) RCW: 1 (3.7) Lost to follow-up ICW: 0 RCW: 2 (7.4) |
ICW: 19 (82.6) RCW: 14 (51.9) P = .02 |
ICW: 41.6 (18.7) RCW: 58 (15.2) P = .02 Kaplan-Meier curve showed a shorter time to healing with irremovable vs. removable cast walkers P = .003 |
Abbreviations: ICW, irremovable cast walker; RCW, removable cast walker; SD, standard deviation.
Based on personal communication with the author.
Figure 8: Irremovable Cast Walkers Versus Removable Cast Walkers, Treatment Discontinuations.
Abbreviations: CI, confidence interval; M-H, Mantel-Haenszel.
Sources: Armstrong et al,37 Najafi et al,30 and Piaggesi et al.28
Ulcer Healing
At 3 months' follow-up, the percentage of patients with a healed ulcer ranged from 70% to 83% with the irremovable cast walkers, and 39% to 80% with the removable cast walkers.
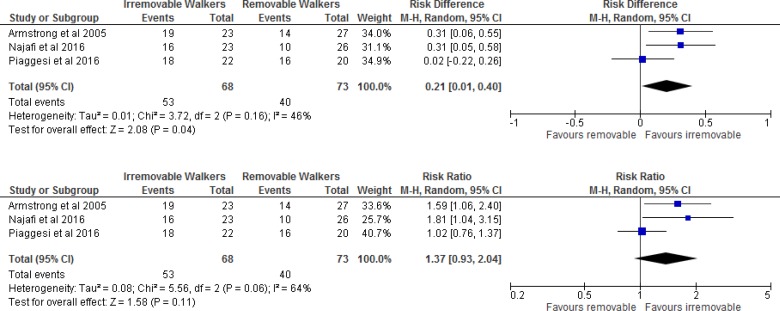
Pooling the results of the studies yielded an absolute increase of 21% (risk difference 0.21 [95% confidence interval: 0.01–0.40]) in the percentage of patients with a healed ulcer with the irremovable cast walkers (Figure 9).
Figure 9: Irremovable Cast Walkers Versus Removable Cast Walkers, Percentage of Healed Ulcers.
Abbreviations: CI, confidence interval; M-H, Mantel-Haenszel.
Sources: Armstrong et al,37 Najafi et al,30 and Piaggesi et al.28
The meta-analysis showed some inconsistency in the study results, however. Two studies showed a significant increase in ulcer healing with the irremovable cast walker,30,37 but one study showed no significant difference between the two groups.28 The authors of the latter study acknowledged that the lack of difference was in contrast to what other studies had demonstrated (i.e., better healing rates with irremovable cast walkers).28 They believed that their finding may have been partly due to high patient adherence with the removable cast walker, possibly because weekly reinforcement of the importance of treatment adherence was part of the study.28 Najafi et al30 corroborated this point, noting that low treatment adherence may have partially explained the low percentage of ulcer healing they observed with removable cast walkers.
Time to Ulcer Healing
Armstrong et al37 reported shorter healing time with the irremovable cast walkers than with the removable cast walkers, but Piaggesi et al28 found no statistically significant difference between the two groups (Table 10).
Adherence to Treatment and Daily Activity
Najafi et al30 evaluated activity patterns in the two study groups. At baseline, patterns were similar between the two groups, but from week 4 onward, patients in the removable cast walker group had a 50% longer walking period (P = .049), 56% longer unbroken walking episodes (P = .048), and a 43% longer average daily standing period (P = .03) than patients in the irremovable cast walker group. As noted above, the authors believed that the increased activity patterns seen with the removable cast walkers may have indicated low adherence to treatment, and that may have partially explained the differences in ulcer healing between the groups.
The authors also noted that the patients in the irremovable cast walker group spent almost twice as much time lying on their side as patients in the removable cast walker group, possibly due to limitations caused by the irremovable cast walker during sleep.30
Patient Satisfaction
In the study by Piaggesi et al,28 patients in the removable cast walker group reported higher satisfaction with treatment than those assigned to irremovable devices (total contact casting or irremovable cast walkers, P < .05). However, we could not determine whether the difference between removable cast walkers and the irremovable cast walkers alone was statistically significant.
Complications
Three studies reported complications in at least one of the study groups.28,30,37 Differences in the proportion of complications between the two groups were difficult to interpret because of the small number of events reported (Table 11).
Table 11:
Irremovable Cast Walkers Versus Removable Cast Walkers, Complications
| Author, Year N (ICW/RCW) | Complication, n (%) | |||
|---|---|---|---|---|
| Skin Maceration | Ulcer Infection | Trauma | Fall | |
| Najafi et al, 201630 49 (23/26) |
None reported | ICW: 2 (8.7) RCW: 0 |
Not reported | Not reported |
| Piaggesi et al, 201628 42 (22/20) |
ICW: 1 (4.5) RCW: 0 |
Fungal intertrigo ICW: 0 RCW: 1 (5) |
Accidental minor trauma in the contralateral foot ICW: 1 (4.5) RCW: 0 |
Not reported |
| Armstrong et al, 200537 50 (23/27) |
ICW: 15 (65.2) RCW: 9 (33.3) |
Antibiotics to treat soft-tissue infection (no device-related infections reported) ICW: 6 (26.1) RCW: 10 (37.0) |
Not reported | ICW: 0 RCW: 0 |
Abbreviations: ICW, irremovable cast walker; RCW, removable cast walker.
Najafi et al30 did not assess treatment complications as part of the outcomes defined a priori, but did report complications if they led to treatment discontinuation. The study by Piaggesi et al28 was designed to collect information on treatment complications, but the authors reported that no patient in any of the groups experienced severe complications; nonsevere complications (none leading to treatment discontinuation) are presented in Table 11.28
Quality of Evidence
Table 12 provides the GRADE evidence profile for irremovable cast walkers versus removable cast walkers.
Table 12:
GRADE Evidence Profile for Irremovable Cast Walkers Versus Removable Cast Walkers
| Number of Studies (Design) | Risk of Bias | Inconsistency | Indirectness | Imprecision | Publication Bias | Upgrade Considerations | Quality |
|---|---|---|---|---|---|---|---|
| Percentage of Patients with a Healed Ulcer | |||||||
| 3 (RCTs)28,30,37 | Serious limitations (−1)a | Serious limitations (−1)b | No serious limitations | No serious limitations | Undetected | None | ⊕⊕ Low |
| Time to Healing (Kaplan-Meier Analysis) | |||||||
| 2 (RCTs)28,37 | No serious limitations | Serious limitations (−1)b | No serious limitations | Serious limitations (−1)c | Undetected | None | ⊕⊕ Low |
| Patient Satisfaction With Treatment | |||||||
| 1 (RCT)37 | No serious limitations | Could not be evaluated | No serious limitations | Very serious limitations (−2)d | Undetected | None | ⊕⊕ Low |
| Complications | |||||||
| 3 (RCTs)28,30,37 | Serious limitations (−1)e | No serious limitations | No serious limitations | Very serious limitations (−2)f | Undetected | None | ⊕ Very Low |
Abbreviations: GRADE, Grading of Recommendations Assessment, Development, and Evaluation; RCT, randomized controlled trial.
In two of the studies included there was some indication of possible differences in baseline characteristics between the groups (ulcer area30 and glycated hemoglobin.37).
The results were inconsistent across studies.
One study showed a statistically significant difference in time to healing between the groups, and the other study did not.
The study did not provide separate information on irremovable vs. removable cast walker groups (i.e., the authors reported on the comparison of removable cast walkers and irremovable devices [total contact casting + irremovable cast walkers]. Additionally, only one small study (n = 22 and 20 in each study group) assessed the outcome.
Treatment complications were not defined as an outcome a priori in the studies included in this analysis.
Very few events were reported in the studies, leading to very low statistical power to detect a difference between groups.
Results for Removable Cast Walkers Versus Therapeutic Shoes
Two studies compared removable cast walkers with therapeutic shoes.16,38
Treatment Discontinuation
Treatment discontinuations were observed in 20% and 44% of the patients in the removable cast walker group and 4% and 13% of the patients in the therapeutic shoes group.16,38 Reasons for discontinuation included discomfort, voluntary withdrawal, and loss to follow-up (Table 13). When we pooled the results of the two studies, we found more treatment discontinuations with removable cast walkers than with therapeutic shoes (Figure 10).
Table 13:
Removable Cast Walkers Versus Therapeutic Shoes
| Author, Year N (RCW/Shoes) Follow-up | Treatment Discontinuation, n (%) | Ulcer Healing, n (%) | Mean Time to Ulcer Healing, d (SD) |
|---|---|---|---|
| Lavery et al, 201516 50 (27/23) 3 months |
Overall RCW: 12 (44.4) Shoes: 3 (13.0) Infection RCW: 4 (14.8) Shoes: 3 (13.0) Voluntary withdrawal RCW: 4 (14.8) Shoes: 0 Device-related wounds RCW: 1 (3.7) Shoes: 0 Nonadherence RCW: 3 (11.1) Shoes: 0 |
RCW: 6 (22.2) Shoes: 10 (43.5) |
RCW: 46.9 (30.1) Shoes: 62.3 (24.5) |
| Armstrong et al, 200138 50 (25/25) 3 months |
Overall RCW: 5 (20.0) Shoes: 1 (4.0) Discomfort RCW: 3 (12.0) Shoes: 0 Instability RCW: 0 Shoes: 1 (4.0) Lost to follow-up RCW: 2 (8.0) Shoes: 0 |
RCW: 13 (52.0) Shoes: 14 (56.0) |
RCW: 50.4 (7.2) Shoes: 61.0 (23.4) Kaplan-Meier curve shown, but difference between the two groups not reported No apparent difference between the groups based on visual inspection |
Abbreviations: RCW, removable cast walker; SD, standard deviation; Shoes, therapeutic shoes.
Figure 10: Removable Cast Walkers Versus Therapeutic Shoes, Treatment Discontinuations.
Abbreviations: CI, confidence interval; M-H, Mantel-Haenszel.
Ulcer Healing
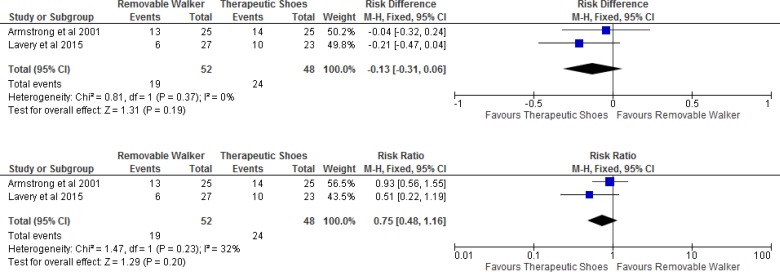
At 3 months of follow-up, the percentage of patients with a healed ulcer in each study was 22% and 52% with removable cast walkers, and 44% and 56% with therapeutic shoes (Table 13).
We found no statistically significant difference in ulcer healing between the two groups (Figure 11).
Figure 11: Removable Cast Walkers Versus Therapeutic Shoes, Percentage of Healed Ulcers.
Abbreviations: CI, confidence interval; M-H, Mantel-Haenszel.
Time to Ulcer Healing
Based on the survival curve provided in the study by Armstrong et al,40 it was not clear whether there was a difference in time to healing between removable cast walkers and therapeutic shoes (Table 13).
Adherence to Treatment and Daily Activity
Both studies assessed treatment adherence as measured by the level of daily activity. In the study by Lavery et al,16 the mean (SD) number of daily steps was lower with removable cast walkers than with therapeutic shoes (1,404 [1,234] vs. 4,022 [4,652], P = .007). The study by Armstrong et al38 did not find a difference between the two groups (768 [563] vs. 1,462 [1,452], P = .15).
Quality of Life and Patient Satisfaction
Armstrong et al40 found that changes in physical health and mental health scores before and after treatment, as measured with the Short-Form 36-item health survey, did not differ between groups.
Lavery et al16 found no statistically significant difference in satisfaction with treatment between patients treated with removable cast walkers or therapeutic shoes.
Complications
Treatment complications reported in the two studies are shown in Table 14. Differences in the proportion of complications between the two groups were difficult to interpret owing to the small sample sizes and low number of events.
Table 14:
Removable Cast Walkers Versus Therapeutic Shoes, Complications
| Author, Year N (RCW/Shoes) | Complication, n (%) | ||
|---|---|---|---|
| Ulcer Infection | New Ulcer | Fall | |
| Lavery et al, 201516 50 (27/23) |
RCW: 4 (14.8) Shoes: 3 (13.0) |
RCW: 1 (3.7) Shoes: 0 |
Not reported |
| Armstrong et al, 200138 50 (25/25) |
Not reported | 0 (device-related) | 0 |
Abbreviations: RCW, removable cast walker; Shoes, therapeutic shoes.
Quality of Evidence
Table 15 provides the GRADE evidence profile for removable cast walkers versus therapeutic shoes.
Table 15:
GRADE Evidence Profile for Removable Cast Walkers Versus Therapeutic Shoes
| Number of Studies (Design) | Risk of Bias | Inconsistency | Indirectness | Imprecision | Publication Bias | Upgrade Considerations | Quality |
|---|---|---|---|---|---|---|---|
| Percentage of Patients with a Healed Ulcer | |||||||
| 2 (RCTs)16,38 | No serious limitations | No serious limitations | Serious limitations (−1)a | Very serious limitations (−2)b | Undetected | None | ⊕ Very Low |
| Time to Healing (Kaplan-Meier Analysis) | |||||||
| 1 (RCT)38 | No serious limitations | Could not be evaluated | Serious limitations (−1)a | Very serious limitations (−2)c | Undetected | None | ⊕ Very Low |
| Patient Satisfaction With Treatment | |||||||
| 1 (RCTs)16 | No serious limitations | Could not be evaluated | Serious limitations (−1)a | Very serious limitations (−2)d | Undetected | None | ⊕ Very Low |
| Quality of Life | |||||||
| 1 (RCT)40 | No serious limitations | Could not be evaluated | Serious limitations (−1)a | Very serious limitations (−2)e | Undetected | None | ⊕ Very Low |
| Complications | |||||||
| 2 (RCTs)16,38 | Serious limitations (−1)f | No serious limitations | Serious limitations (−1)a | Very serious limitations (−2)g | Undetected | None | ⊕ Very Low |
Abbreviations: GRADE, Grading of Recommendations Assessment, Development, and Evaluation; RCT, randomized controlled trial.
Different types of therapeutic shoes were used in the studies; the results for one type of shoe may not be applicable to other types.
Very low statistical power to detect a difference between groups.
No statistically significant difference between the two groups in the studies identified. The statistical power to detect a difference in healing rates among the studies was very low.
No statistically significant difference between the two groups. Only one small study (n = 27 and 23 in each group) assessed the outcome.
No statistically significant difference between the groups. Only one small study (21 patients/study group) assessed the outcome.
Treatment complications were not defined as an outcome a priori in the studies included in this analysis.
Very few events were reported in the studies, leading to very low statistical power to detect a difference between groups.
Discussion
The evidence suggests that total contact casting, removable cast walkers, and irremovable cast walkers are beneficial in the treatment of neuropathic, noninfected foot ulcers in patients with diabetes but without severe peripheral arterial disease. The results of the studies showed that ulcer healing occurred in 68% to 95% of patients treated with total contact casting, 22% to 80% of patients treated with removable cast walkers, and 70% to 85% of patients treated with irremovable cast walkers, all within 3 to 4 months of follow-up. Based on the results of our meta-analyses both total contact casting and irremovable cast walkers healed more ulcers than removable cast walkers.
Treatment discontinuation occurred with all devices, mostly because of voluntary withdrawal, lack of adherence, or complications (8% to 24% with total contact casting; 4% to 17% with irremovable cast walkers; and 0% to 44% with removable cast walkers). According to the clinical experts we consulted, patients who discontinue treatment may require an alternative offloading device until their ulcer is healed.
Several study authors noted that treatment success was affected by adherence and acceptance, factors that may partially explain the differences we found in ulcer healing across studies.
Cast walkers (removable or irremovable) do not fit all patients properly; patients with short legs, wide feet, or severe foot deformities would benefit from total contact casting instead, because it is moulded to the patient's foot and lower leg.16 On the other hand, total contact casting must be applied by a qualified technician to avoid injuries. Geographical isolation may hinder the use of irremovable devices because of potential difficulties in returning for frequent clinic visits to remove and reapply the device. In these circumstances, removable devices may be a better option (expert opinion).
Convenience is also a factor: irremovable devices (total contact casting and irremovable cast walkers) affect daily activities such as bathing and sleeping more than removable cast walkers. However, ease of removal by the patient affects treatment adherence and ulcer healing. These factors should be taken into account when choosing an offloading device.
Strengths and Limitations
The included studies had small sample sizes, so we could not draw conclusions for some of the outcomes evaluated (time to healing and treatment complications), and the study results may not be generalizable to clinical practice. We were also unable to make associations between ulcer healing and factors such as ulcer characteristics, glycemic control, sex, ethnicity, or any other PROGRESS-Plus categories.
None of the studies identified compared fibreglass total contact casting with total contact casting made from other materials. Therefore we cannot determine if the outcomes of total contact casts made from material other than fibreglass would be different than those reported for fibreglass total contact casts in this report.
Most patients included in the studies presented with noninfected superficial ulcers (most grade 1A, some grade 2A, University of Texas Classification System).42 It is not clear whether patients with Grade 3 ulcers (penetrating to bone or joint) or infected ulcers would experience outcomes similar to those seen in the included studies.
Study follow-up was relatively short (3 to 4 months), so we could not assess the course of progression for patients whose ulcers did not heal within the study time frame or for patients who discontinued treatment. None of the studies provided follow-up information after ulcer closure.
Conclusions
The evidence suggests that fibreglass total contact casting and cast walkers (removable or irremovable) may be beneficial for treating neuropathic noninfected diabetic foot ulcers. The results of the treatment comparisons are summarized in Table 16.
Table 16:
Treatment Comparisons—Summary
| Comparison | Risk Difference, % Ulcer Healing (95% CI) | GRADE |
|---|---|---|
| Total contact casting vs. irremovable cast walkers | 0.02 (−0.11 to 0.14) | Low |
| Total contact casting vs. removable cast walkers | 0.17 (0–0.33) | Moderate |
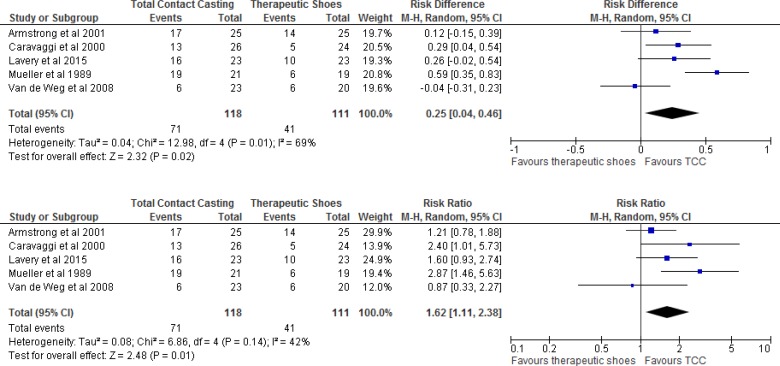
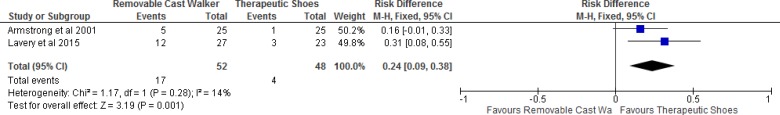
| Total contact casting vs. therapeutic shoes | 0.25 (0.04–0.46) | Moderate |
| Irremovable cast walkers vs. removable cast walkers | 0.21 (0.01–0.40) | Low |
| Removable cast walkers vs. therapeutic shoes | −0.13 (−0.31 to 0.06) | Very low |
| Irremovable cast walkers vs. therapeutic shoes | No studies identified |
Abbreviations: CI, confidence interval; GRADE, Grading of Recommendations Assessment, Development, and Evaluation.
The studies showed a relatively high frequency of treatment discontinuation with all treatments evaluated. Patients who discontinue one type of treatment may need to continue treatment with an alternative offloading device until the ulcer is healed. Each treatment evaluated has different characteristics and may not be appropriate for all patients.
ECONOMIC EVIDENCE
Research Question
What is the cost-effectiveness of fibreglass total contact casting, removable cast walkers, and irremovable cast walkers for patients with noninfected diabetic neuropathic foot ulcers?
Methods
Literature Search
We performed an economic literature search on August 18, 2016, for studies published from inception to the search date. To retrieve relevant studies, the search was developed using the clinical search strategy with an economic filter applied. Database auto-alerts were created in MEDLINE, Embase, and CINAHL and monitored for the duration of the HTA review.
We performed targeted grey literature searching of HTA agency sites and clinical trial registries. Finally, we reviewed reference lists of included economic literature for any additional relevant studies not identified through the systematic search. See Clinical Evidence, Literature Search, above, for further details on methods used, and Appendix 1 for literature search strategies, including all search terms.
Literature Screening
A single reviewer reviewed titles and abstracts, and, for those studies meeting the inclusion/exclusion criteria, we obtained full-text articles.
Types of Studies
We looked at economic evaluations that reported incremental cost-effectiveness ratios (ICERs; e.g., cost per quality-adjusted life-year [QALY]/life-year gained or cost per event avoided) and cost studies.
We did not include narrative reviews, letters/editorials, abstracts, posters, or unpublished studies.
Types of Participants
We looked at studies in patients with noninfected diabetic neuropathic foot ulcers.
Types of Interventions
We looked at studies that reported on fibreglass total contact casting, removable cast walkers, and irremovable cast walkers.
Types of Outcomes Measures
Outcomes of interest were full economic evaluations: cost-utility analyses, cost-effectiveness analyses, or cost-benefit analyses.
Data Extraction
We extracted relevant data on the following:
Source (i.e., name, location, year)
Population and comparator
Interventions
Outcomes (i.e., health outcomes, costs, and incremental cost-effectiveness ratios)
Study Applicability
We determined the usefulness of each identified study for decision-making by applying a modified applicability checklist for economic evaluations that was originally developed by the National Institute for Health and Care Excellence (NICE) in the United Kingdom. The original checklist is used to inform development of clinical guidelines by NICE. We retained questions from the NICE checklist related to study applicability and modified the wording of the questions to remove references to guidelines and make it Ontario-specific. A summary of the number of studies judged to be directly applicable, partially applicable, or not applicable to the research question is presented.
Results
Literature Search
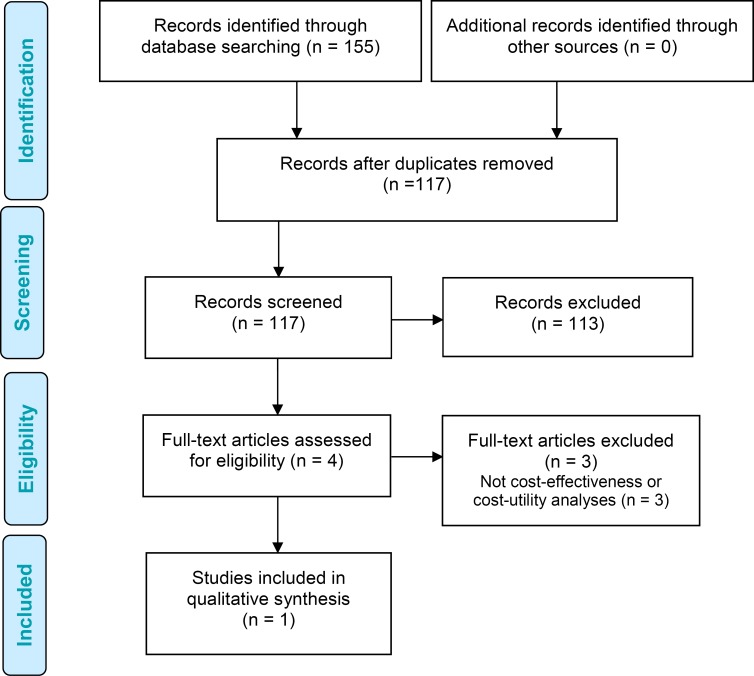
The database search yielded 117 citations published before August 18, 2016 (with duplicates removed). We excluded a total of 113 articles based on information in the title and abstract. We then obtained the full texts of four potentially relevant articles for further assessment. Figure 12 presents the flow diagram for the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA).
Figure 12: PRISMA Flow Diagram.
Abbreviation: PRISMA, Preferred Reporting Items for Systematic Reviews and Meta-analyses.
Source: Adapted from Moher et al.41
One study met the inclusion criteria.43 We hand-searched the reference lists of the included study to identify other relevant studies, but no additional citations were identified.
Review of Included Economic Studies
Craig et al.43 conducted two decision-tree models to compare the cost consequences of soft-heel casting and orthotic footwear in patients with diabetes who were at high risk of ulceration (preventative pathway) or who had a foot ulcer (curative pathway). The analysis was undertaken from the perspective of the National Health Service (NHS) Borders in the United Kingdom.
In the preventative pathway model, the clinical endpoints were new ulcers or no new ulcers. In the curative pathway model, the clinical endpoints were healed ulcers, improved ulcers, amputation, or death. The authors obtained data from an audit of patient outcomes associated with casting at NHS Borders for inpatients, and from a 3-year study of patients treated in a multidisciplinary foot care clinic for outpatients.
The authors combined their findings with other published data and expert opinion. They modelled the benefits of preventative and curative casting compared with standard practice, and they estimated the costs of healed and unhealed ulcers based on the treatment pathways adopted. Data from the economic models suggested that soft-heel casting could reduce the net costs of managing ulcers in these patients by approximately 10% because of increased rates of healing: about £500 per inpatient and £425 per outpatient with an ulcer (curative cohort); and £205 per patient at high risk for an ulcer (preventative cohort). The authors concluded that preventative and curative soft-heel casting could lead to cost savings in the management of patients with diabetes.
Table 17:
Results of Economic Literature Review—Summary
| Name, Year, Location | Study Design and Perspective | Populations | Interventions | Results | |
|---|---|---|---|---|---|
| Health Outcomes | Costs | ||||
| Craig et al, 2013,43 United Kingdom |
|
|
|
Preventative pathway
|
|
Abbreviations: NHS, National Health Service.
Applicability of Included Studies
The results of the methodology checklist for economic evaluations applied to the included articles are presented in Appendix 6. The included study was partially applicable to the research question, but it was not relevant for the Ontario setting.
Conclusions
The included study found net cost savings from using soft-heel casting to treat diabetic foot ulcers. However, it was neither a cost-effectiveness nor a cost-utility study, and it did not investigate total contact casting, removable cast walkers, or irremovable cast walkers to treat diabetic foot ulcers from a Canadian perspective.
PRIMARY ECONOMIC EVALUATION
The published economic evaluation identified in the literature addressed the interventions of interest, but it was neither a cost-effective nor a cost-utility study, and it did not take a Canadian perspective. Owing to these limitations, we conducted a primary economic evaluation.
Research Questions
What is the cost-effectiveness of fibreglass total contact casting, removable cast walkers, and irremovable cast walkers in treating patients with noninfected diabetic neuropathic foot ulcers in the context of the Ontario Ministry of Health and Long-Term Care?
What is the cost utility of fibreglass total contact casting, removable cast walkers, and irremovable cast walkers in treating patients with noninfected diabetic neuropathic foot ulcers in the context of the Ontario Ministry of Health and Long-Term Care?
Methods
The information presented in this report follows the reporting standards set out by the Consolidated Health Economic Evaluation Reporting Standards Statement.44
Type of Analysis
We conducted cost-effectiveness and cost-utility analyses to measure the costs and benefits of adopting total contact casting, removable cast walkers, and irremovable cast walkers, compared with each other and with therapeutic shoes.
Target Population
The study population was men and women aged 18 or older who present with a diabetic neuropathic foot ulcer.
Perspective
We conducted this analysis from the perspective of the Ontario Ministry of Health and Long-Term Care.
Interventions
We evaluated fibreglass total contact casting, removable cast walkers, and irremovable cast walkers, compared with each other and with therapeutic shoes (e.g., specially made footwear, over-the-counter footwear, and orthopedic sandals).
Discounting and Time Horizon
The time horizon for the cost-effectiveness analysis was 3 months, based on the follow-up time in the identified randomized controlled trials (RCTs).16,28,29,32–36,38,39
The time horizon for the cost-utility analysis was 6 months after the first use of total contact casting, a removable cast walker, an irremovable cast walker, or therapeutic shoes. To capture the long-term treatment effects of an offloading device, the ideal time horizon would be longer than this. However, the RCTs followed patients for only a short period (12 weeks), so information was unavailable on patients who were lost to follow-up, patients who did not heal from using an offloading device, patients who had a recurrence of the ulcer, patients who experienced delayed healing (i.e., after 12 weeks), or patients who developed a new ulcer. For this reason, a model with a time horizon longer than 6 months would have required many assumptions, and results would have been uncertain.
Because the time horizon was less than 1 year, we did not apply discounting.
Model Structure
For the cost-utility analysis, we developed a decision-analytic model (Figure 13a) to capture short-term costs and effects associated with the treatment of diabetic foot ulcer using total contact casting, removable cast walkers, irremovable cast walkers, or therapeutic shoes. In this model, a patient with a diabetic foot ulcer would receive treatment with one of the four offloading devices. Following the assigned treatment, an ulcer would be healed or unhealed. If the ulcer was healed, the patient would enter a maintenance phase, not needing active treatment but continuing to use orthotics to prevent ulcer recurrence for the rest of the model (expert opinion). We assumed that there would be no new ulcer or recurrence of an old ulcer once an ulcer had healed. If the ulcer was not healed, the patient would remain “unhealed” in the model and continue treatment or undergo amputation.
Figure 13a: Decision-Analytic Model.
Clinical evidence from RCTs was limited, so we proposed three scenarios to describe the treatment pathways after unsuccessful primary treatment of a diabetic foot ulcer (Figure 13b).
Figure 13b: Scenario Model.
aSwitch from total contact casting to removable cast walker; from irremovable cast walker to removable cast walker; from removable cast walker to total contact casting; from therapeutic shoes to removable cast walker (expert consultation).
Base-case scenario, a combination of primary and secondary treatments: If a patient had an unhealed ulcer at 3 months and did not undergo amputation, we assumed that they had a 50% chance of continuing with the primary treatment and a 50% chance of switching to a secondary treatment (a new offloading device). We applied device and treatment costs from the secondary treatment until the end of the model, and patients were considered unhealed. Choices of secondary treatment depended on the primary treatment, and were confirmed by expert consultation. If a patient underwent amputation as a result of an unhealed ulcer, they were considered amputated
Scenario 1, all patients switched to a secondary treatment: If a patient had an unhealed ulcer and did not undergo amputation, they would switch to a secondary treatment (a new offloading device). We applied costs from the secondary treatment until the end of the model, and patients were considered unhealed. Choices of secondary treatment depended on the primary treatment, and were confirmed by expert consultation. If a patient underwent amputation as a result of an unhealed ulcer, they were considered amputated
Scenario 2, all patients continued on the primary treatment: If a patient had an unhealed ulcer and did not undergo amputation, they would continue on the primary treatment until the end of the model and be considered unhealed. If the patient underwent amputation as a result of an unhealed ulcer, they would be considered amputated
We defined ulcer healing as complete re-epithelialization, without signs of exudate, as in the clinical evidence review. Also for consistency with the clinical evidence review, we considered patients who discontinued treatment to be unhealed (definition in Appendix 4). Because of the short time horizon, we did not consider death from a diabetic foot ulcer in the model.
Clinical Outcome and Utility Parameters
We used a number of different input parameters to populate the model:
Probability of ulcer healing
Time to ulcer healing
Complications
Health utilities
Tables 18 and 19 describe the model inputs.
Table 18:
Clinical Outcome Parameters Used in the Economic Model
| Variable | Outcome (Base Case) | Range | Referencea |
|---|---|---|---|
| Total Contact Casting | |||
| Probability of ulcer healing | 0.741 | 0.677–0.915 | Meta-analysis16,28,29,32–36,38,39 |
| Time to healing, weeks | 5.097 | 3.823–6.371 | Meta-analysis16,28,29,33–35,38,39 |
| Probability of amputation from an unhealed ulcer | 0.0092 | 0.0065–0.0153 | CDA45 |
| Removable Cast Walkers | |||
| Risk ratio of ulcer healing (total contact casting vs. removable cast walkers) | 1.25 | 0.95–1.65 | Meta-analysis32–34,38 |
| Probability of ulcer healing | 0.593 | 0.449–0.779 | Calculation |
| Mean difference in time to healing (total contact casting vs. removable cast walkers), weeks | –1.013 | –1.816 to −0.209 | Meta-analysis32–34,38 |
| Time to healing, weeks | 6.11 | 5.31–6.12 | Calculation |
| Probability of amputation from an unhealed ulcer | 0.0145 | 0.0102–0.0240 | CDA45 |
| Irremovable Cast Walkers | |||
| Risk ratio of ulcer healing (total contact casting vs. irremovable cast walkers) | 1.02 | 0.87–1.19 | Meta-analysis28,29,36 |
| Probability of ulcer healing | 0.726 | 0.623–0.852 | Calculation |
| Mean difference in time to healing (total contact casting vs. irremovable cast walkers), weeks | –0.329 | –1.59 to 0.939 | Meta-analysis28,29,36 |
| Time to healing, weeks | 5.425 | 4.164–6.687 | Calculation |
| Probability of amputation from an unhealed ulcer | 0.0097 | 0.0068–0.0161 | CDA45 |
| Therapeutic Shoes | |||
| Risk ratio of ulcer healing (total contact casting vs. therapeutic shoes) | 1.62 | 1.11–2.38 | Meta-analysis16,32,38,39 |
| Probability of ulcer healing | 0.457 | 0.311–0.667 | Calculation |
| Mean difference in time to healing (total contact casting vs. therapeutic shoes), weeks | –3.73 | –5.25 to −2.22 | Meta-analysis16,32,38,39 |
| Time to healing, weeks | 8.83 | 7.32–10.34 | Calculation |
| Probability of amputation from an unhealed ulcer | 0.0193 | 0.0136–0.0320 | CDA45 |
Table 19:
Utility Parameters Used in the Economic Model
| Health State | Utility (Base Case) | Range | Reference |
|---|---|---|---|
| Unhealed ulcer | 0.44 | 0.37–0.51 | Ragnarson Tennvall et al, 200046 |
| Healed ulcer, no amputation | 0.60 | 0.57–0.63 | Ragnarson Tennvall et al, 200046 |
| Amputation | 0.51a | 0.47–0.55 | Ragnarson Tennvall et al, 200046 |
Utility of amputation = proportion of patients with a diabetic foot ulcer who experienced a minor amputation × utility of minor amputation + proportion of diabetic foot ulcer patients who experienced a major amputation × utility of major amputation.
Probability of Ulcer Healing
We used an intention-to-treat analysis to calculate the percentage of ulcers healed. For this reason, we considered patients whose ulcers did not heal, patients who discontinued treatment, and patients who were lost to follow-up all to be unhealed (see the clinical evidence review for more details). Six studies compared total contact casting with removable cast walkers.16,28,32–34,38 Three studies compared total contact casting with irremovable cast walkers.28,29,36 Four studies compared total contact casting with therapeutic shoes.16,35,38,39
To calculate the probability of ulcer healing for each of the treatments, we first calculated the probability for total contact casting using a random-effects model. We then calculated the probability for the other devices by dividing the probability for total contact casting by the risk ratios of ulcer healing for total contact casting versus the other devices (Table 18). We took the risk ratios for each comparison from the clinical evidence review. We calculated the probability of ulcer healing by total contact casting over those of other offloading devices, because data on ulcer healing were available in the clinical evidence review that compared total contact casting with the other devices.
Time to Ulcer Healing
We estimated the time to ulcer healing for patients who were healed during the model period. Several studies reported time to ulcer healing for total contact casting versus the other offloading devices.16,28,29,32–34,36,38,39 We calculated time to ulcer healing for total contact casting because of data availability. First, we conducted a meta-analysis of time to ulcer healing for total contact casting using a random-effects model. We took the mean difference in time to ulcer healing for total contact casting versus removable cast walkers, irremovable cast walkers, and therapeutic shoes from the clinical evidence review. Based on the time to ulcer healing for total contact casting and the mean difference compared with removable cast walkers, irremovable cast walkers, and therapeutic shoes, we calculated the time to ulcer healing for the other offloading devices (Table 18).
Complications
We defined amputation as a complication that happened as a consequence of an unhealed ulcer when using any offloading device. We derived the probability of amputation from the literature (Table 18).45
Health Utilities
We quantified health outcomes as QALYs. Ragnarson Tennvall et al46 collected health utility data from 457 people with diabetes who were treated for foot ulcers and assessed their health status using the EQ-5D quality-of-life questionnaire.46 Table 19 provides the utility values for patients who had an unhealed ulcer, a healed ulcer, and an amputation. We calculated the utility for amputation using the utilities for both minor and major amputations. We then adjusted these values to the respective proportions of patients with minor and major amputations.
Cost Parameters
All cost parameters included in our study originated from consultation with experts, from the Ontario Schedule of Benefits for Physician Services,47 and from previous publications.45,47,48 We obtained information about the following:
Offloading devices (i.e., raw materials, dressings, plasters, and devices)
Treatment (i.e., cost of initial treatment when a patient receives an offloading device until an ulcer is healed; cost of a second treatment for unhealed ulcers; and maintenance costs, including orthotics and monthly follow-up visits to a clinic)
Labour (i.e., salaries of physicians, cast technicians, or nurses)
Complications (amputation costs as a consequence of an unhealed ulcer)
Costs
We estimated the costs of healed and unhealed ulcers based on the treatment pathways for each offloading device. Table 20 shows the items and associated costs used in the economic model.
Table 20:
Costs Used in the Economic Model
| Variable | Value (Base Case) | Range | Reference |
|---|---|---|---|
| Total Contact Casting | |||
| Cost of cast | $90 | $80–$100 | Expert opinion |
| Removable Cast Walkers | |||
| Cost of removable cast walker | $150 | — | Expert opinion |
| Irremovable Cast Walkers | |||
| Cost of removable cast walker | $150 | — | Expert opinion |
| Cost of Coban wrap | $25 | $15–$30 | Expert opinion |
| Therapeutic Shoes | |||
| Cost of shoes | $100 | — | Expert opinion and assumption |
| Other Materials | |||
| Cost per dressing | $15 | — | Expert opinion |
| Professional Labour | |||
| Cost of putting on a cast | $10.25 | — | OHIP47 |
| Cost of taking off a cast | $24.10 | — | OHIP47 |
| Cost of seeing a new patient | $75 | — | Expert opinion |
| Cost of seeing a follow-up patient | $55 | — | Expert opinion |
| Cost per nursing visit | $65 | — | Expert opinion |
| Complications | |||
| Cost of amputation | $75,081 | $8,848–$100,000 | CDA45,48 and calculation |
Abbreviations: CDA, Canadian Diabetes Association; OHIP, Ontario Health Insurance Plan.
Resource Utilization
Resource utilization consisted of casts, the number of devices, and dressing changes for each offloading device per patient with a diabetic foot ulcer (Table 21).
Table 21:
Resource Utilization Used in the Economic Model
| Variable | Value (Base Case) | Range | Reference |
|---|---|---|---|
| Total Contact Casting | |||
| First cast | Within the first 3 days | — | Expert opinion |
| Subsequent casts | Every 7 days | 7–10 days | Expert opinion |
| Dressing change frequency | Every time a cast is replaced | — | Expert opinion |
| Removable Cast Walkers | |||
| First dressing | Within the first 3 days | — | Expert opinion |
| Subsequent dressings | Once a week | 1–3 times per week | Expert opinion |
| Number of devices per patient | 1 | 1–4 | Assumption |
| Dressing change frequency | 3 | — | Expert opinion |
| Irremovable Cast Walkers | |||
| First dressing | Within the first 3 days | — | Expert opinion |
| Subsequent dressings | Every 7 days | 7–10 days | Expert opinion |
| Number of devices per patient | 1 | 1–4 | Assumption |
| Dressing change frequency | 3 | — | Expert opinion |
| Therapeutic Shoes | |||
| First dressing | Within the first 3 days | — | Expert opinion |
| Subsequent dressings | Once a week | 1–3 times per week | Expert opinion |
| Number of devices per patient | 1 | 1–4 | Assumption |
| Dressing change frequency | 3 | — | Expert opinion |
Analysis
Cost-Effectiveness Analysis
The primary outcome of the base case analysis was incremental cost per healed ulcer in the treatment of diabetic foot ulcers. We determined this by comparing one offloading device with another. We calculated the average cost per patient to treat a diabetic foot ulcer and the number of healed ulcers per 1,000 patients for each offloading device. Because we were evaluating more than two treatment strategies, we conducted a full incremental cost-effectiveness analysis. We ranked offloading devices by treatment cost; the treatment with the lowest cost was ranked first.
The average treatment cost per patient with a diabetic foot ulcer consisted of the management costs for an ulcer, the management costs for a healed ulcer, and the management costs for complications. The treatment cost also included the cost of the offloading device (e.g., device, dressing, and bandages), the number of visits to a health care professional, and treatments for healed and unhealed ulcers, as well as the number of amputations.
The base case analysis provided the best estimates of the cost of managing a patient with a diabetic foot ulcer using total contact casting, removable cast walkers, irremovable cast walkers, and therapeutic shoes, but we wanted to address the uncertainty of the model inputs and clinical scenarios. Therefore, we assessed possible variabilities and uncertainties in the model using one-way sensitivity analyses.
Cost-Utility Analysis
The primary outcome of the base case analysis was the incremental cost per QALY gained comparing the four treatment modalities: total contact casting, removable cast walkers, and irremovable cast walkers, compared with one another and with therapeutic shoes. We calculated ICERs by dividing the difference between the expected costs by the difference between the expected QALYs of treatment for the two offloading devices being compared. We presented the ICERs in three scenarios that reflected different treatment options: the base case, in which 50% of diabetic foot ulcer patients with an unhealed ulcer remained on the primary treatment and 50% switched to a secondary treatment; scenario 1, in which all patients with an unhealed ulcer switched to a secondary treatment; and scenario 2, which all patients with an unhealed ulcer stayed on the primary treatment.
Because of the uncertainties and assumptions used in the model, we have presented the primary outcomes in the base case analysis via probabilistic sampling by running 10,000 simulations of the model parameters. We applied beta distributions to probabilities and utility parameters. We applied lognormal distributions to the risk ratios of the probability of ulcer healing, comparing total contact casting with removable cast walkers, irremovable cast walkers, and therapeutic shoes. We applied gamma distributions to cost parameters.
We assessed the variability and uncertainty of the model parameters by conducting one-way sensitivity analyses and varied the model variables over plausible ranges. Tables 18 to 20 show the impact this would have on the ICERs from each scenario.
Main Assumptions
We made a number of major assumptions in the cost-utility analysis:
Patients with a diabetic foot ulcer who were healed after the primary treatment would enter the maintenance phase and remain healed for the rest of the model cycle
Each patient with a diabetic foot ulcer experienced only one ulcer
There were no new ulcers, and there was no recurrence of an ulcer once it was healed
Only patients with a diabetic foot ulcer who were treated as outpatients were included
Generalizability
The findings of this economic analysis cannot be generalized to all patients with diabetic foot ulcers. They may, however, be used to guide decision-making about the specific patient populations in Ontario addressed in the studies evaluated by Health Quality Ontario.
Expert Consultation
Throughout the development of the model, we consulted clinicians who specialized in treating diabetic foot ulcers. The role of the expert advisors was to review the structure and inputs of the economic model to confirm that the information we used reasonably reflected the clinical setting. The statements, conclusions, and views expressed in this report do not necessarily represent the views of the consulted experts.
Results
Cost-Effectiveness Analysis
Base Case Analysis
Cost-effectiveness results for the base case analysis are presented in Table 22. We ranked the four offloading devices from lowest to highest by treatment cost per 1,000 patients with a diabetic foot ulcer. A gain of a healed ulcer with total contact casting would cost $17,923 more than with irremovable cast walkers. Removable cast walkers were dominated by total contact casting, because they were more expensive and less effective than total contact casting. Therapeutic shoes were also dominated by total contact casting for the same reasons.
Table 22:
Base Case Cost-Effectiveness Analysis
| Strategy | Cost Per Patient | Cost Per 1,000 Patients | Number of Healed Ulcers Per 1,000 Patients | Incremental Cost Per 1,000 Patientsa | Incremental Healed Ulcers Gained per 1,000 Patientsb | Sequential ICER |
|---|---|---|---|---|---|---|
| Irremovable cast walkers | $876.50 | $876,500 | 726 | — | — | Reference |
| Total contact casting | $1,136.92 | $1,136,920 | 741 | $260,420 | 15 | $17,923 |
| Removable cast walkers | $1,628.98 | $1,628,980 | 593 | $492,060 | –148 | Dominated |
| Therapeutic shoes | $1,933.75 | $1,933,750 | 457 | $796,830 | –284 | Dominated |
Abbreviation: ICER, incremental cost-effectiveness ratio.
Incremental cost = average cost (treatment A) – average cost (treatment B).
Incremental healed ulcers gained = total healed ulcers gained (treatment A) – total healed ulcers gained (treatment B).
Sensitivity Analysis
In the treatment of diabetic foot ulcers, removable cast walkers, and therapeutic shoes were both dominated by irremovable cast walkers and total contact casting. Interestingly, the experts we consulted indicated that irremovable cast walkers are not a common treatment choice. For this reason, we conducted one-way sensitivity analyses on the number of weekly clinic visits for a patient with a diabetic foot ulcer to explore the changes in cost-effectiveness when comparing total contact casting with irremovable cast walkers (Table 23). When weekly visits increased to 1.5 or 2 times per week, the average treatment cost was lower for total contact casting than for irremovable cast walkers, and total contact casting was associated with more healed ulcers. In the sensitivity analysis, total contact casting was a dominant strategy compared to irremovable cast walkers.
Table 23:
Sensitivity Analysis—Change of Irremovable Cast Walker Weekly Visits
| Irremovable Cast Walker Weekly Visits | Strategy | Cost per Patient | Incremental Cost per Patienta | Number of Healed Ulcers Per 1,000 Patients | Incremental Healed Ulcers Gained Per 1,000 Patientsb | ICER ($/Ulcer Healed) |
|---|---|---|---|---|---|---|
| 1c | Irremovable cast walkers | $876.50 | — | 726 | — | — |
| Total contact casting | $1,136.92 | $260.42 | 741 | 15 | $17,923 | |
| 1.5 | Irremovable cast walkers | $1,239.75 | — | 726 | — | Dominated |
| Total contact casting | $1,136.92 | –$102.82 | 741 | 15 | — | |
| 2 | Irremovable cast walkers | $1,603.00 | — | 726 | — | Dominated |
| Total contact casting | $1,136.92 | –$466.07 | 741 | 15 | — |
Abbreviation: ICER, incremental cost-effectiveness ratio.
Incremental cost = average cost (treatment A) – average cost (treatment B).
Incremental healed ulcers gained = total healed ulcers gained (treatment A) – total healed ulcers gained (treatment B).
Base case cost-effectiveness results.
Cost-Utility Analysis
Base Case Analysis
For the base case, in which there was a 50% chance a patient with an unhealed diabetic foot ulcer would stay on the primary treatment and a 50% chance they would switch to a secondary treatment, both therapeutic shoes and removable cast walkers were dominated by irremovable cast walkers and total contact casting (Table 24). When we compared total contact casting with irremovable cast walkers, we found that gaining a QALY with total contact casting would require an additional $198,928.
Table 24:
Base Case Cost-Utility Analysis
| Treatment Option | Strategy | Cost per Patient | Incremental Cost Per Patienta | QALYs | Incremental QALYs Gainedb | Sequential ICER ($/QALY) |
|---|---|---|---|---|---|---|
| Combining primary and secondary treatment | Irremovable cast walkers | $2,584 | — | 0.266 | — | Reference |
| Total contact casting | $2,982 | $398 | 0.268 | 0.002 | $198,928 | |
| Removable cast walkers | $3,999 | $1,017 | 0.257 | –0.011 | Dominated | |
| Therapeutic shoes | $4,990 | $2,008 | 0.245 | –0.023 | Dominated |
Abbreviations: ICER, incremental cost-effectiveness ratio; QALY, quality-adjusted life-year.
Incremental cost = average cost (treatment A) – average cost (treatment B).
Incremental QALYs gained = QALYs (treatment A) – QALYs (treatment B).
Scenario Analysis
The findings of the scenario analysis are presented in Table 25.
Table 25:
Scenario Analysis
| Scenario | Strategy | Cost Per Patient | Incremental Cost Per Patienta | QALYs | Incremental QALYs Gainedb | ICER ($/QALY) |
|---|---|---|---|---|---|---|
| Scenario 1: All switching | Irremovable cast walkers | $2,742 | — | 0.266 | — | Reference |
| Total contact casting | $3,021 | $279 | 0.268 | 0.002 | $176,807 | |
| Removable cast walkers | $3,980 | $959 | 0.257 | –0.011 | Dominated | |
| Therapeutic shoes | $5,036 | $2,015 | 0.245 | –0.023 | Dominated | |
| Scenario 2: No switching | Irremovable cast walkers | $2,431 | — | 0.266 | — | Reference |
| Total contact casting | $2,924 | $493 | 0.268 | 0.002 | $289,140 | |
| Removable cast walkers | $4,005 | $1,080 | 0.257 | –0.011 | Dominated | |
| Therapeutic shoes | $4,940 | $2,015 | 0.245 | –0.023 | Dominated |
Abbreviation: ICER, incremental cost-effectiveness ratio; QALY, quality-adjusted life-year.
Incremental cost = average cost (treatment A) – average cost (treatment B).
Incremental QALYs gained = QALYs (treatment A) – QALYs (treatment B).
For scenario 1, in which all patients with an unhealed diabetic foot ulcer would switch to a secondary treatment, therapeutic shoes and removable cast walkers were dominated by irremovable cast walkers and total contact casting. When we compared total contact casting with irremovable cast walkers, we found that gaining a QALY using total contact casting would require an additional $176,807.
For scenario 2, in which all patients would continue on their primary treatment if an ulcer was not healed, therapeutic shoes and removable cast walkers were dominated by irremovable cast walkers and total contact casting. When we compared total contact casting with irremovable cast walkers, we found that gaining a QALY using total contact casting would require an additional $289,140.
Sensitivity Analysis
One-Way Sensitivity Analysis
Figure 14 presents the results of the one-way sensitivity analysis for the base case (a 50% chance that a patient with an unhealed diabetic foot ulcer would remain on the primary treatment and a 50% chance they would switch to a secondary treatment). The model was most sensitive to time to healing for total contact casting, time to healing for irremovable cast walkers, healing probability for total contact casting, and the number of weekly visits and healing probability for irremovable cast walkers. When time to healing for total contact casting was reduced to 3.82 weeks, it was less costly and more effective (dominant) than irremovable cast walkers. Similarly, when time to healing for irremovable cast walkers was increased to 6.69 weeks, total contact casting was less costly and more effective (dominant). When the healing probability of total contact casting was increased to 84%, it dominated irremovable cast walkers. When the number of visits using irremovable cast walkers increased to three times per week, total contact casting also dominated.
Figure 14: One-Way Sensitivity Analysis, Base Case, Total Contact Casting Versus Irremovable Cast Walkersa.
Abbreviations: ICER, incremental cost-effectiveness ratio; QALY, quality-adjusted life-year; TCC, total contact casting.
aX-axis represents range of ICERs when base-case values are varied (ranges shown in parentheses). Vertical line represents the ICER for total contact casting ($198,928 per QALY gained). The variables that could cause TCC to dominate irremovable cast walkers are as follows: when time to healing for TCC decreases to 3.82 weeks; when time to healing for irremovable cast walkers increases to 6.69 weeks; when healing probability for TCC increases to 84%; when weekly visits for irremovable cast walkers increase to 3 times; or when healing probability for irremovable cast walkers decreases to 62%.
Figure 15 presents the results of the one-way sensitivity analysis for scenario 1 (all patients with an unhealed diabetic foot ulcer would switch to a secondary treatment). The model was most sensitive to time to healing for total contact casting, time to healing for irremovable cast walkers, the number of weekly visits using irremovable cast walkers, the healing probability for total contact casting, and the healing probability for irremovable cast walkers.
Figure 15: One-Way Sensitivity Analysis, Scenario 1, Total Contact Casting Versus Irremovable Cast Walkersa.
Abbreviations: ICER, incremental cost-effectiveness ratio; QALY, quality-adjusted life-year; TCC, total contact casting.
aX-axis represents range of ICERs when base-case values are varied (ranges shown in parentheses). Vertical line represents the ICER for total contact casting ($176,807 per QALY gained). The variables that could cause TCC to dominate irremovable cast walkers are as follows: when time to healing for TCC decreases to 3.82 weeks; when time to healing for irremovable cast walkers increases to 6.69 weeks; when weekly visits for irremovable cast walkers increases to 3 times; when healing probability for TCC increases to 84%; or when healing probability for irremovable cast walkers decreases to 62%.
Figure 16 presents the results of the one-way sensitivity analysis for scenario 2 (no switching of treatment for patients with unhealed diabetic foot ulcers). The model was most sensitive to time to healing for total contact casting, time to healing for irremovable cast walkers, healing probability for total contact casting, healing probability for irremovable cast walkers, and the number of weekly visits using irremovable cast walkers.
Figure 16: One-Way Sensitivity Analysis, Scenario 2, Total Contact Casting Versus Irremovable Cast Walkersa.
Abbreviations: ICER, incremental cost-effectiveness ratio; QALY, quality-adjusted life-year; TCC, total contact casting.
aX-axis represents range of ICERs when base-case values are varied (ranges shown in parentheses). Vertical line represents the ICER for total contact casting ($289,140 per QALY gained). The variables that could cause TCC to dominate irremovable cast walkers are as follows: when time to healing for TCC decreases to 3.82 weeks; when time to healing for irremovable cast walkers increases to 6.69 weeks; when healing probability for TCC increases to 84%; when healing probability for irremovable cast walkers decreases to 62%; or when weekly visits for irremovable cast walkers increases to 3 times.
Discussion
Resources for health care are scarce relative to needs or wants, and an economic evaluation is intended to inform the choices that decision-makers face in these circumstances. This study investigated resource allocations, cost-effectiveness, and cost utility for total contact casting, removable cast walkers, and irremovable cast walkers, compared with each other and with therapeutic shoes.
The cost-effectiveness analysis showed that treating diabetic foot ulcers with therapeutic shoes and removable cast walkers was more costly and less effective than using total contact casting or irremovable cast walkers. This left total contact casting and irremovable cast walkers as the two strategies for consideration. When we compared total contact casting with irremovable cast walkers, we found that gaining a healed ulcer with total contact casting would require an additional $17,923. One-way sensitivity analyses showed that these cost-effectiveness results were sensitive to the number of weekly clinic visits if patients used an irremovable cast walker. One of the strengths of this cost-effectiveness analysis was that the results were calculated based on data from RCTs, without assumptions, reflecting the clinical evidence.
The cost-utility analysis showed that total contact casting and irremovable cast walkers were less expensive and more effective than removable cast walkers and therapeutic shoes, and that irremovable cast walkers were as effective as total contact casting but at a lower cost. One-way sensitivity analyses showed that the time to healing for total contact casting, the time to healing for irremovable cast walkers, the healing probability of total contact casting and irremovable cast walkers, and the number of weekly visits for irremovable cast walkers had the most influence on ICER values.
In Ontario, clinicians regularly use removable cast walkers and total contact casting, and it is unclear how often irremovable cast walkers are used. The reasons for this are unclear, but may relate to clinician preference or feasibility.
Our findings were consistent with those of other studies in terms of treatment costs. Piaggesi and colleagues concluded that total contact casting was more expensive than irremovable cast walkers.29 This finding was verified in a more recent study by the same authors.28 In another study by Katz and colleagues, the authors also reported that total contact casting was more expensive than irremovable cast walkers.36
This analysis had several limitations. First, the care pathway has been simplified. The model followed patients for only 6 months. As a result, long-term effects such as death have not been captured. As well, we were unable to obtain information from RCTs about treatment pathways for patients with unhealed ulcers, or about outcomes for patients who were lost to follow-up, who had unhealed ulcers, or who had recurring or new ulcers. The 6-month duration of this model was reasonable for capturing the short-term treatment effects of offloading devices and did allow us to explore treatment options for unhealed ulcers.
The second limitation was the assumptions made about the treatment pathway. When a diabetic foot ulcer went unhealed from the primary treatment, the patient would continue to be treated. Because the treatment trajectories and sequence of offloading devices are not standardized, we chose to review different scenarios for switching treatment. We consulted with several experts about their opinions on treatment pathways. The information provided in our analysis represented feasible treatment options based on available data from RCTs and from expert opinion. Furthermore, we presented the cost-utility results as probabilistic rather than deterministic sampling to avoid uncertainties and assumptions.
Another limitation was related to other major assumptions in the cost-utility model. We assumed that there would be no recurrence of an old ulcer, that no new ulcer would form after a healed ulcer, and that each patient had only one ulcer treatment at a time. In addition, since the RCTs had small sample sizes, it was difficult to quantify the outcomes and complications among patients with diabetic foot ulcers. We included amputation as the only complication in the model. Data from more patients with longer follow-up would provide an opportunity to consolidate the results of our analysis. A Markov model may have been more suitable for monitoring patients over a long time. This type of model could have captured the long-term consequences of treatment, particularly in cases of unhealed ulcers. However, given the short-term nature of the available data on clinical outcomes from the various offloading devices, a Markov model in this study was not possible.
Conclusions
Therapeutic shoes and removable cast walkers were more costly and had fewer health outcome gains than irremovable cast walkers and total contact casting. From a health economic point of view, irremovable cast walkers were as effective as total contact casting for treating diabetic foot ulcers and were associated with fewer costs. Irremovable cast walkers should be the preferred option when they are acceptable to patients and clinicians. When they cannot be used, total contact casting may be a reasonable alternative. Removable cast walkers would be a preferred option for patients who are not eligible for or have not had success with total contact casting or irremovable cast walkers.
BUDGET IMPACT ANALYSIS
We conducted a budget impact analysis from the perspective of the Ontario Ministry of Health and Long-Term Care to determine the estimated cost burden of implementing total contact casting, irremovable cast walkers, and removable cast walkers over the next 5 years (2016–2020). All costs are reported in 2016 Canadian dollars.
Research Question
What is the budget impact of implementing fibreglass total contact casting, removable cast walkers, and irremovable cast walkers over the next 5 years from the perspective of the Ontario Ministry of Health and Long-Term Care?
Methods
Target Population
The target population was patients with diabetic neuropathic foot ulcers who were eligible for treatment with total contact casting, removable cast walkers, and irremovable cast walkers.
The prevalence of diabetes in Ontario was estimated at 10.20% in 2015 and predicted to increase to 11.9% by 2020.49 Assuming that the number of people diagnosed with diabetes would increase at a steady rate between 2015 and 2020, we estimated prevalence for the years 2016 to 2020 (Table 26).
Table 26:
Estimated Diabetes Prevalence in Ontario, 2016–2020
| 2016 | 2017 | 2018 | 2019 | 2020 | |
|---|---|---|---|---|---|
| Ontario population, na | 13,930,021 | 14,069,321 | 14,210,014 | 14,352,115 | 14,495,635 |
| Diabetes prevalence, % | 10.54 | 10.88 | 11.22 | 11.55 | 11.90 |
| People with diabetes, n | 1,468,224 | 1,530,561 | 1,593,815 | 1,657,999 | 1,723,122 |
| Diabetic foot ulcer prevalence, %b | 2.5 | 2.5 | 2.5 | 2.5 | 2.5 |
| Patients with diabetic foot ulcer, nb | 36,705 | 38,264 | 39,845 | 41,450 | 43,078 |
Data from Statistics Canada.50
Based on yearly probabilities of developing a diabetic foot ulcer among people with diabetes in Ontario.
Using the projected Ontario population and the estimated diabetes prevalence, we estimated the number of people with diabetes over the next 5 years (Table 26).49
Approximately 2% to 3% of patients with diabetes will develop a foot ulcer each year.49 We assumed that 2.5% of people with diabetes in Ontario would develop a diabetic foot ulcer and estimated the annual number of diabetic foot ulcer cases in Ontario, based on the diabetes prevalence estimates (Table 26).
Resource
Access to Offloading Devices
Based on information from a published in a report by the Canadian Diabetes Association, we estimated the annual usage of offloading devices for three possible scenarios of access to an offloading device: 50%, 75%, and 100% (Table 27).45
Table 27:
Estimated Annual Number of Patients With Diabetic Foot Ulcers and Access to an Offloading Device in Ontario, 2016–2020
| Access to An Offloading Devicea | 2016 | 2017 | 2018 | 2019 | 2020 |
|---|---|---|---|---|---|
| 50% | 18,353 | 19,132 | 19,923 | 20,725 | 21,539 |
| 75% | 27,529 | 28,698 | 29,884 | 31,087 | 32,309 |
| 100% | 36,706 | 38,264 | 39,845 | 41,450 | 43,078 |
Categorized by rates of access to an offloading device per annum among patients with diabetic foot ulcers in Ontario.
Source: Canadian Diabetes Association.45
Proportion of Use of the Different Offloading Devices
We estimated the proportion of patients with a diabetic foot ulcer who would use each of the offloading devices, based on information from a published report.15 According to the report, 40% of patients would use total contact casting, 30% would use removable cast walkers, and 30% would use other offloading devices (e.g., custom braces, ankle and foot orthoses, postoperative shoes) to treat a diabetic foot ulcer. We excluded other devices from the analysis. No data were available on the proportion of patients who would use an irremovable cast walker. Based on expert opinion, we estimated that 50% of patients who would use a removable cast walker might use an irremovable cast walker. We used these estimates in both the base case and the scenario analyses. The proportions of use of total contact casting, removable cast walkers, and irremovable cast walkers were 57%, 21.5%, and 21.5%, respectively.
Number of Amputations
The number of amputations among patients with diabetic foot ulcers depends on the proportion of patients who have access to offloading devices. The probability of amputation as a result of an unhealed ulcer has been estimated at 7.1%.45 We estimated the number of amputations among patients with diabetic foot ulcers who did or did not have access to an offloading device based on the access scenarios described in Table 27. The expected number of expected amputations is presented in Table 28.
Table 28:
Estimated Amputations Among Patients With Diabetic Foot Ulcers by Access to an Offloading Device in Ontario, 2016–2020
| 2016 | 2017 | 2018 | 2019 | 2020 | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Access to an Offloading Device | 50% | 75% | 100% | 50% | 75% | 100% | 50% | 75% | 100% | 50% | 75% | 100% | 50% | 75% | 100% |
| Amputations among patients without access to an offloading device | 1,303 | 652 | — | 1,358 | 679 | — | 1,415 | 707 | — | 1,471 | 736 | — | 1,529 | 765 | — |
| Amputations among patients with access to total contact casting | 96 | 145 | 193 | 101 | 151 | 201 | 105 | 157 | 209 | 109 | 163 | 218 | 113 | 170 | 226 |
| Amputations among patients with access to removable cast walkers | 57 | 85 | 114 | 59 | 89 | 119 | 62 | 93 | 123 | 64 | 96 | 128 | 67 | 100 | 133 |
| Amputations among patients with access to irremovable cast walkers | 38 | 57 | 76 | 40 | 60 | 80 | 41 | 62 | 83 | 43 | 65 | 86 | 45 | 67 | 90 |
| Total amputations | 1,495 | 939 | 383 | 1,558 | 979 | 399 | 1,622 | 1,019 | 416 | 1,688 | 1,060 | 433 | 1,754 | 1,102 | 450 |
| Change in amputations with 25% increase in access to an offloading device | — | −556 | −556 | — | −579 | −579 | — | −603 | −603 | — | −628 | −628 | — | −652 | −652 |
Canadian Costs
Costs included in the analysis were the cost of an offloading device, labour and professional costs, and the treatment costs of amputation (taken from the primary economic evaluation).
We calculated the 1-year cost as follows. We took the first 3-month treatment cost per patient from the cost-effectiveness analysis. To calculate the subsequent 9-month treatment cost per patient, we assumed that if a patient had a healed ulcer from the primary treatment, they would continue in a maintenance phase of 9 months, during which orthotics would be used. If an ulcer was unhealed from the primary treatment, the patient would continue with a secondary treatment. For simplicity, we assumed that therapeutic shoes would be the secondary treatment, regardless of the primary treatment. Since the probability of ulcer healing was approximately 50% for therapeutic shoes, 50% of patients with an unhealed ulcer would continue for 9 months with the secondary treatment. Therefore, we assumed that on average, a patient would receive 4.5 months of a secondary treatment.
We based the total 1-year treatment cost on the following formula:
Total cost per patient per year = Average cost per patient (first 3 months) + (1 – probability of ulcer healing of primary treatment) × average cost per patient (next 9 months) + probability of ulcer healing of primary treatment × average cost of maintenance (next 9 months)
Details of the cost components are provided in Table 29. The cost of offloading devices and Coban wrap are not publicly funded. The costs of physicians, nurses, and the dressing are publicly funded.
Table 29:
| Offloading Device | Resource Item | Cost |
|---|---|---|
| Fibreglass total contact casting | Device cost | $620 |
| Treatment cost | $1,763 | |
| Total cost | $2,383 | |
| Removable cast walkers | Device cost | $150 |
| Treatment cost | $3,107 | |
| Total cost | $3,257 | |
| Irremovable cast walkers | Device cost | $331 |
| Treatment cost | $1,817 | |
| Total cost | $2,148 |
Cost data were provided in consultation with experts.
Treatment costs included professional labour and dressings.
Analysis
We calculated the required budget for funding total contact casting, removable cast walkers, and irremovable cast walkers when access to an offloading device was 50%, 75%, and 100%. We also calculated the net budget impact when access was increased by 25% (50% to 75% and 75% to 100%) and by 100% (0% to 100%).
Base Case Analysis
In the base case analysis, we assumed all three offloading devices (total contact casting, removable cast walkers, and irremovable cast walkers) would be funded. We assumed that the proportion of use of total contact casting, removable cast walkers, and irremovable cast walkers would be 57%, 21.5%, and 21.5%, respectively, and that those proportions would remain the same for all three access scenarios.
Scenario Analysis
In the scenario analyses, we explored the possibility of each device being exclusively funded. We increased the proportional use to 100% for each device for the three scenarios of access.
Because irremovable cast walkers are not commonly used, we also explored the budget impact of funding total contact casting, removable cast walkers, and irremovable cast walkers by varying the proportional use of irremovable cast walkers.
Results
Base Case Analysis
The budget impact of adopting total contact casting, removable cast walkers, and irremovable cast walkers would range from $8.4 million to $20 million (device costs only) per year over the next 5 years, depending on level of access to offloading devices (Tables 30 to 32).
Table 30:
Budget Impact of Adopting Offloading Devices at 50% Access in Ontario, 2016–2020
| Year | Cost | Total Contact Casting | Removable Cast Walkers | Irremovable Cast Walkers | Total |
|---|---|---|---|---|---|
| 2016 | Device cost | $6,498,285 | $589,912 | $1,300,146 | $8,388,343 |
| Treatment cost | $18,495,619 | $12,218,435 | $7,148,435 | $37,862,489 | |
| Total cost | $24,993,904 | $12,808,347 | $8,448,581 | $46,250,832 | |
| 2017 | Device cost | $6,774,185 | $614,958 | $1,355,347 | $8,744,489 |
| Treatment cost | $19,280,892 | $12,218,435 | $7,451,938 | $38,951,266 | |
| Total cost | $26,055,077 | $12,833,393 | $8,807,285 | $47,695,755 | |
| 2018 | Device cost | $7,054,146 | $640,372 | $1,411,360 | $9,105,878 |
| Treatment cost | $20,077,726 | $13,263,595 | $7,759,909 | $41,101,230 | |
| Total cost | $27,131,872 | $13,903,967 | $9,171,269 | $50,207,108 | |
| 2019 | Device cost | $7,338,218 | $666,160 | $1,468,196 | $9,472,574 |
| Treatment cost | $20,886,260 | $13,797,723 | $8,072,402 | $42,756,385 | |
| Total cost | $28,224,478 | $14,463,883 | $9,540,598 | $52,228,959 | |
| 2020 | Device cost | $7,626,448 | $692,326 | $1,525,864 | $9,844,637 |
| Treatment cost | $21,706,630 | $14,339,669 | $8,389,470 | $44,435,769 | |
| Total cost | $29,333,078 | $15,031,995 | $9,915,334 | $54,280,406 |
Note: Numbers may appear inexact due to rounding.
Table 32:
Budget Impact of Adopting Offloading Devices at 100% Access in Ontario, 2016–2020
| Year | Cost | Total Contact Casting | Removable Cast Walkers | Irremovable Cast Walkers | Total |
|---|---|---|---|---|---|
| 2016 | Device cost | $12,996,571 | $1,179,823 | $2,600,292 | $16,776,686 |
| Treatment cost | $36,991,237 | $24,436,871 | $14,296,870 | $75,724,978 | |
| Total cost | $49,987,808 | $25,616,694 | $16,897,163 | $92,501,664 | |
| 2017 | Device cost | $13,548,370 | $1,229,915 | $2,710,694 | $17,488,978 |
| Treatment cost | $38,561,784 | $24,436,871 | $14,903,877 | $77,902,531 | |
| Total cost | $52,110,154 | $25,666,786 | $17,614,570 | $95,391,509 | |
| 2018 | Device cost | $14,108,292 | $1,280,745 | $2,822,720 | $18,211,756 |
| Treatment cost | $40,155,452 | $26,527,190 | $15,519,819 | $82,202,460 | |
| Total cost | $54,263,743 | $27,807,935 | $18,342,539 | $100,414,217 | |
| 2019 | Device cost | $14,676,435 | $1,332,320 | $2,936,392 | $18,945,148 |
| Treatment cost | $41,772,520 | $27,595,445 | $16,144,805 | $85,512,770 | |
| Total cost | $56,448,955 | $28,927,766 | $19,081,197 | $104,457,917 | |
| 2020 | Device cost | $15,252,896 | $1,384,651 | $3,051,727 | $19,689,275 |
| Treatment cost | $43,413,260 | $28,679,338 | $16,778,940 | $88,871,538 | |
| Total cost | $58,666,156 | $30,063,990 | $19,830,667 | $108,560,813 |
Note: Numbers may appear inexact due to rounding.
Table 31:
Budget Impact of Adopting Offloading Devices at 75% Access in Ontario, 2016–2020
| Year | Cost | Total Contact Casting | Removable Cast Walkers | Irremovable Cast Walkers | Total |
|---|---|---|---|---|---|
| 2016 | Device cost | $9,747,428 | $884,867 | $1,950,219 | $12,582,514 |
| Treatment cost | $27,743,428 | $18,327,653 | $10,722,653 | $56,793,733 | |
| Total cost | $37,490,856 | $19,212,520 | $12,672,872 | $69,376,248 | |
| 2017 | Device cost | $10,161,277 | $922,436 | $2,033,020 | $13,116,734 |
| Treatment cost | $28,921,338 | $18,327,653 | $11,177,907 | $58,426,898 | |
| Total cost | $39,082,615 | $19,250,089 | $13,210,928 | $71,543,632 | |
| 2018 | Device cost | $10,581,219 | $960,558 | $2,117,040 | $13,658,817 |
| Treatment cost | $30,116,589 | $19,895,392 | $11,639,864 | $61,651,845 | |
| Total cost | $40,697,807 | $20,855,951 | $13,756,904 | $75,310,662 | |
| 2019 | Device cost | $11,007,327 | $999,240 | $2,202,294 | $14,208,861 |
| Treatment cost | $31,329,390 | $20,696,584 | $12,108,604 | $64,134,577 | |
| Total cost | $42,336,716 | $21,695,824 | $14,310,897 | $78,343,438 | |
| 2020 | Device cost | $11,439,672 | $1,038,488 | $2,288,795 | $14,766,956 |
| Treatment cost | $32,559,945 | $21,509,504 | $12,584,205 | $66,653,654 | |
| Total cost | $43,999,617 | $22,547,992 | $14,873,000 | $81,420,609 |
When access to all three offloading devices increased by 25% (50% to 75%, and 75% to 100%) and 100% (0% to 100%), the net budget impact was a cost savings for the health care system (Table 33), because increased access to an offloading device would lead to fewer amputations.
Table 33:
Net Budget Impact of Adopting Offloading Devices When Access Increased by 25% and 100% in Ontario, 2016–2020, Base Case Analysis
| Year | Cost | Change in Accessibility | ||
|---|---|---|---|---|
| 50% to 75% | 75% to 100% | 0% to 100% | ||
| 2016 | Device cost | $4,194,171 | $4,194,171 | $16,776,684 |
| Treatment cost | $18,931,244 | $18,931,244 | $75,724,976 | |
| Amputation costs | −$41,680,264 | −$41,680,264 | −$166,721,056 | |
| Total cost | −$18,554,848 | −$18,554,848 | −$74,219,392 | |
| 2017 | Device cost | $4,372,245 | $4,372,245 | $17,488,980 |
| Treatment cost | $19,475,633 | $19,475,633 | $77,902,532 | |
| Amputation costs | −$43,449,895 | −$43,449,895 | −$173,799,580 | |
| Total cost | −$19,602,017 | −$19,602,017 | −$78,408,068 | |
| 2018 | Device cost | 4,552,939 | $4,552,939 | $18,211,756 |
| Treatment cost | 20,550,615 | $20,550,615 | $82,202,460 | |
| Amputation costs | −$45,245,576 | −$45,245,576 | −$180,982,304 | |
| Total cost | −$20,142,022 | −$20,142,022 | −$80,568,088 | |
| 2019 | Device cost | $4,736,287 | $4,736,287 | $18,945,148 |
| Treatment cost | $21,378,192 | $21,378,192 | $85,512,768 | |
| Amputation costs | −$47,067,625 | −$47,067,625 | −$188,270,500 | |
| Total cost | −$20,953,145 | −$20,953,145 | −$83,812,580 | |
| 2020 | Device cost | $4,922,319 | $4,922,319 | $19,689,276 |
| Treatment cost | $22,217,885 | $22,217,885 | $88,871,540 | |
| Amputation costs | −$48,916,346 | −$48,916,346 | −$195,665,384 | |
| Total cost | −$21,776,142 | −$21,776,142 | −$87,104,568 | |
Note: Numbers may appear inexact due to rounding. Negative numbers mean cost savings.
Scenario Analysis
When access to each of total contact casting, removable cast walkers, and irremovable cast walkers increased by 25% (50% to 75% and 75% to 100%) and by 100% (0% to 100%), there were also cost savings to the health care system, because of fewer amputations with increased access to these three devices (Table 34). Further details are available in Appendix 7.
Table 34:
Net Budget Impact of Adopting Offloading Devices When Access to Offloading Devices Increased by 25% and 100% in Ontario, 2016–2020, Scenario Analysis
| Year | Cost | Change in Accessibility | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| 50% to 75% | 75% to 100% | 0% to 100% | ||||||||
| Total Contact Casting | Irremovable Cast Walkers | Removable Cast Walkers | Total Contact Casting | Irremovable Cast Walkers | Removable Cast Walkers | Total Contact Casting | Irremovable Cast Walkers | Removable Cast Walkers | ||
| 2016 | Device cost | $5,686,000 | $3,033,674 | $1,376,460 | $5,686,000 | $3,033,674 | $1,376,460 | $22,744,000 | $12,134,696 | $5,505,840 |
| Treatment cost | $16,183,666 | $16,679,682 | 28,509,682 | $16,183,666 | $16,679,682 | $28,509,682 | $64,734,664 | $66,718,728 | $114,038,728 | |
| Amputation cost | −$42,532,022 | −$42,177,123 | −38,912,051 | −$42,532,022 | −$42,177,123 | −$38,912,051 | −$170,128,088 | −$168,708,492 | −$155,648,204 | |
| Total cost | −$20,662,356 | −$22,463,766 | –9,025,909 | −$20,662,356 | −$22,463,766 | −$9,025,909 | −$82,649,424 | −$89,855,064 | −$36,103,636 | |
| 2017 | Device cost | $5,927,412 | $3,162,476 | $1,434,901 | $5,927,412 | $3,162,476 | $1,434,901 | $23,709,648 | $12,649,904 | $5,739,604 |
| Treatment cost | $16,870,781 | $17,387,856 | $29,720,126 | $16,870,781 | $17,387,856 | $29,720,126 | $67,483,124 | $69,551,424 | $118,880,504 | |
| Amputation cost | −$44,337,816 | −$43,967,849 | −$40,564,151 | −$44,337,816 | −$43,967,849 | −$40,564,151 | −$177,351,264 | −$175,871,396 | −$162,256,604 | |
| Total cost | −$21,539,623 | −$23,417,517 | −$9,409,124 | −$21,539,623 | −$23,417,517 | −$9,409,124 | −$86,158,492 | −$93,670,068 | −$37,636,496 | |
| 2018 | Device cost | $6,172,378 | $3,293,174 | −7,577,412 | $6,172,378 | $3,293,174 | $1,494,202 | $24,689,512 | $13,172,696 | $5,976,808 |
| Treatment cost | $17,568,010 | $18,106,455 | −52,873,665 | $17,568,010 | $18,106,455 | $30,948,388 | $70,272,040 | $72,425,820 | $123,793,552 | |
| Amputation cost | −$46,170,193 | −$24,385,307 | −53,559,960 | −$46,170,193 | −$45,784,936 | −$42,240,572 | −$184,680,772 | −$183,139,744 | −$168,962,288 | |
| Total cost | −$22,429,805 | −$24,385,307 | –9,797,981 | −$22,429,805 | −$24,385,307 | −$9,797,981 | −$89,719,220 | −$97,541,228 | −$39,191,924 | |
| 2019 | Device cost | $6,420,940 | $17,155,221 | −7,882,556 | $6,420,940 | $3,425,790 | $1,554,374 | $25,683,760 | $13,703,160 | $6,217,496 |
| Treatment cost | $18,275,477 | −$48,831,019 | −55,002,898 | $18,275,477 | $18,835,606 | $32,194,686 | $73,101,908 | $75,342,424 | $128,778,744 | |
| Amputation cost | −$48,029,476 | −$19,264,557 | −55,716,830 | −$48,029,476 | −$47,628,705 | −$43,941,608 | −$192,117,904 | −$190,514,820 | −$175,766,432 | |
| Total cost | −$23,333,058 | −$25,367,309 | –10,192,548 | −$23,333,058 | −$25,367,309 | −$10,192,548 | −$93,332,232 | −$101,469,236 | −$40,770,192 | |
| 2020 | Device cost | $6,673,142 | $17,829,043 | −8,192,166 | $6,673,142 | $3,560,348 | $1,615,426 | $26,692,568 | $14,241,392 | $6,461,704 |
| Treatment cost | $18,993,301 | −$50,749,002 | −57,163,300 | $18,993,301 | $19,575,430 | $33,459,228 | $75,973,204 | $78,301,720 | $133,836,912 | |
| Amputation cost | −$49,915,976 | −$20,021,230 | −57,905,274 | −$49,915,976 | −$49,499,464 | −$45,667,545 | −$199,663,904 | −$197,997,856 | −$182,670,180 | |
| Total cost | −$24,249,533 | −$26,363,685 | –10,592,890 | −$24,249,533 | −$26,363,685 | −$10,592,890 | −$96,998,132 | −$105,454,740 | −$42,371,560 | |
Note: Numbers may appear inexact due to rounding. Negative numbers mean cost savings.
Discussion
Implementing total contact casting, removable cast walkers, and irremovable cast walkers would require $17 million to $20 million per year between 2016 and 2020, assuming that access to these three offloading devices was 100% and that the annual probability of developing a diabetic foot ulcer was 2.5%. According to expert opinion, access to offloading devices would increase if these devices were publicly funded. Our analysis showed that increased access to offloading devices would likely result in cost savings to the health care system because of fewer amputations.
Experts indicated that in Ontario, clinicians regularly use removable cast walkers and total contact casting, but irremovable cast walkers are less common. The reasons for this are unclear, but may relate to clinician preference or feasibility. The increase in use of irremovable cast walkers would be directly correlated with the increase in diabetes prevalence, and with training of clinicians in the use of irremovable cast walkers to treat neuropathic diabetic foot ulcers (expert opinion).
The budget impact analysis included the up-front costs (device costs and the frequency of changing offloading devices) and the treatment costs (labour and professional costs). However, increased access to offloading devices led to potential cost savings because of the likelihood of fewer amputations as a result of using the devices.
Conclusions
If total contact casting, removable cast walkers, and irremovable cast walkers were publicly funded in patients with diabetic foot ulcers, the device costs would be $17 million to $20 million per year over the next 5 years (2016–2020) at 100% access. However, access to offloading devices could result in cost savings for the health care system if the potential savings from avoiding amputations are taken into account.
PATIENT, CAREGIVER, AND PUBLIC ENGAGEMENT
Objective
The objective of this analysis was to explore the underlying values, needs, impacts, and preferences of those who have lived experience with the treatment of diabetic foot ulcers. The treatment focus was total contact casting, removable cast walkers, and irremovable cast walkers.
Background
Public and patient engagement explores the lived experience of a person with a health condition, including the impact that the condition and its treatment has on the patient, the patient's family or other caregivers, and the patient's personal environment. Public and patient engagement increases awareness and builds appreciation for the needs, priorities, and preferences of the person at the centre of a treatment program. The insights gained through public and patient engagement provide an in-depth picture of lived experience, through an intimate look at the values that underpin the experience.
Lived experience is a unique source of evidence about the personal impact of a health condition and how that condition is managed, including what it is like to navigate the health care system with that condition and how technologies may or may not make a difference in people's lives. Information shared from lived experience can also identify gaps or limitations in published research (for example, outcome measures that do not reflect what is important to those with lived experience).51–53 Additionally, lived experience can provide information or perspectives on the ethical and social values implications of technologies and treatments. Because the needs, priorities, preferences, and values of those with lived experience in Ontario are not often adequately explored by published literature, Health Quality Ontario reaches out to and directly speaks with people who live with the health condition, including those who may have experience with the intervention in question.
The impact of diabetes—in particular diabetic foot ulcers—on patients and families was perceived at the outset of this project to have significant bearing on quality of life. To truly understand impact on quality of life, we spoke with patients who had diabetes and foot ulcers, and who had experience with offloading devices such as total contact casting, removable cast walkers, and irremovable cast walkers. Understanding and appreciating their day-to-day functioning and treatment experience, including with the offloading devices in question, helps to contextualize the potential value of the interventions from a lived experience perspective.
Methods
Engagement Plan
Engagement as a concept captures a range of efforts used to involve the public and patients in various domains and stages of health technology assessment decision-making.54 Rowe and Frewer outline three types of engagement: communication, consultation, and participation.55 Communication constitutes a one-way transfer of information from the sponsor to the individual, while participation involves the sponsor and individual collaborating through real-time dialogue. Consultation, on the other hand, refers to the sponsor seeking out and soliciting information (for example, experiential input) from the public, patients, and caregivers affected by the health technology or intervention in question.
The engagement plan for this health technology assessment was consultation.56 Within this typology, the engagement design focused on interviews to examine the lived experience of patients with diabetes who have foot ulcers, including those who have experience with total contact casting, removable cast walkers, and irremovable cast walkers.
The qualitative interview was selected as an appropriate methodology because it allowed Health Quality Ontario staff to deeply explore the meaning of central themes in the lived experience of the participants. The main task in interviewing is to understand the meaning of what participants say.57 Interviews are particularly useful for getting the story behind a participant's experiences, which was the objective of this portion of the study. The sensitive nature of exploring quality-of-life issues is another reason supporting the use of interviews for this project.
Recruitment of Participants
The recruitment strategy for this project pursued an approach called purposive sampling58–61 to actively recruit individuals with direct lived experience. Patient, Caregiver, and Public Engagement staff reached out to patients, caregivers, and families (including those with experience of the intervention in question) through a variety of partner organizations, including the Ontario Centres for Complex Diabetes Care, wound care advocacy and support groups, diabetes associations, and clinical wound care centres across the province. We asked interview participants to reach out to other patients with diabetes after they completed their interview.
Inclusion Criteria
We sought a broad range of participants, including those who had experience with diabetic foot ulcers and the offloading devices in question (total contact casting, removable cast walkers, and irremovable cast walkers). We wanted to speak with patients of various ages, assuming that different life commitments (work, family, etc.) would affect patients' choices in terms of treatment options and outcomes sought. Finally, we aimed to obtain broad geographic representation as a way of raising possible equity issues and different themes in treatment decision-making across the province.
Exclusion Criteria
We set no exclusion criteria.
Participants
Patient, Caregiver, and Public Engagement staff spoke to 16 patients with diabetic foot ulcers from across Ontario. We interviewed eight patients twice for further clarification and analysis related to the offloading devices. All patients were familiar with a variety of treatments for diabetic foot ulcers, including offloading devices and medical therapy options.
Approach
At the outset of the interview, Patient, Caregiver, and Public Engagement staff at Health Quality Ontario explained the purpose of the health technology assessment process (including the role of Health Quality Ontario and the Ontario Health Technology Advisory Committee), risks to participation, and protection of personal health information. These attributes were explained to participants orally and through a letter of information. Written or verbal consent was then obtained from participants prior to commencing the interview. The letter of information and consent form can be found in Appendix 8. Interviews were recorded and transcribed.
Questions focused on the impact of diabetic foot ulcers on patients', caregivers, and families' quality of life, experiences with other health interventions related to managing diabetic foot ulcers, experiences with total contact casting, removable cast walkers, and irremovable cast walkers, and any perceived benefits and limitations when comparing the different offloading devices. The interview guide is included in Appendix 8.
The interview was semi-structured, consisting of a series of open-ended questions. Interviews lasted approximately 10 to 30 minutes. Questions for the interview were based on a list developed by the Health Technology Assessment International Patient and Citizen Involvement Group to elicit lived experiences specific to the impact of a health technology or intervention.62
Data Extraction and Analysis
Patient, Caregiver, and Public Engagement staff at Health Quality Ontario selected a modified version of a grounded theory methodology to analyze transcripts of participant interviews, because it captures themes and allows for elements of the lived experience to be organized and compared across participants. The inductive nature of grounded theory follows an iterative process of eliciting, documenting, and analyzing responses while simultaneously collecting and analyzing data using a constant comparative approach.63,64 Through this approach, staff coded transcripts and compared themes using NVivo (QSR International, Doncaster, Victoria, Australia). NVivo enables the identification and interpretation of patterns in interview data about the meaning and implications of a lived condition from the patient's perspective of what is important in their daily lived experience with diabetic foot ulcers, before and after the intervention in question.
Results
Physical and Emotional Experience of Living With Diabetic Foot Ulcers
Patients frequently reported multiple health issues related to their diabetes, including recurring foot ulcers. Neuropathy of the lower legs, which could prevent patients from monitoring and caring for their own feet, was one of these. Given these comorbidities and the nature and location of foot ulcers in the patients interviewed, the effect of the ulcers on quality of life was moderate to severe. Patients consistently reported mobility challenges, and also spoke about their decreased ability to leave home and engage in activities outside of home. They also described reduced quality of life. Walking, visiting with friends, vacations, and driving were all affected by diabetic foot ulcers. For people who were employed, challenges arose with performing work duties, often requiring leaves of absence or modified work duties. These changes affected patients and their families.
“Until it really got bad, I wasn't doing much too differently, because I didn't know. After that, I was being told to stay off my feet as much as possible, and at that time I was working, so I had to take the time off to just stay off my feet.”
“Especially now that you can't walk, you're off work, you've got a family to raise and children, and now you can't work, and you're spiralling down into the abyss pretty quick.”
Following the first occurrence of a diabetic foot ulcer and dealing with its complexity and treatment, patients reported increased awareness of and vigilance about the status of their feet. They monitored small cuts or bruises closely and reported careful maintenance of the skin on several occasions. They also reported more appointments with physicians, chiropodists, and wound care clinics, as well as the tendency to get off their feet when swelling, redness, or calluses arose.
“I perform daily wound care, plus I wear custom orthotics, and I'm committed to daily application of moisturizers.”
This vigilance could constitute an emotional burden: participants regularly report constant stress and the fear of developing a foot ulcer. Family members also saw this emotional burden.
Patients and their family caregivers reported a clear understanding that a foot ulcer could have serious health consequences, such as amputation.
“Her life shrank to her house, essentially. And to her bed. She was spending a lot of time in bed sleeping, and they think she was overwhelmed, trying to deal with all of this and with the inevitable fear of this potential amputation looming over her head …”
“I live in constant fear that the other shoe will drop and the ulcer will return or occur elsewhere.”
“Having these things is incredibly terrifying for people. Most [people with diabetes] will not admit that they have a problem until it becomes evident to the family around them, and they're forced into care.”
Frustration with slow healing was a common sentiment among the patients interviewed. This frustration extended to ulcer recurrence: patients reported knowing that it could take up to 2 years for the skin to regain its full strength, and that the reopening of ulcers was a fairly common occurrence.
“It is frustrating at times; you think everything's healed up, but they say the integrity of the skin takes two full years to reach its strong point. Once it heals, then the 2-year period starts, but then if you open up a wound, then that stops and … then you've gotta start all over again.”
Patients reported that this emotional burden often required the support of family members. Those with family supports spoke of gratitude for their aid and acknowledged the physical and emotional difficulties they would have faced if not for family. Because of the physical limitations that diabetic foot ulcers can impose, families often helped get patients to and from treatment centres, and advocated for treatment options.
“Without my family, without my close friends, I don't know where I would have been. I don't think I would have been in my home. I wouldn't have been able to manage on my own those early months.”
Treatments for Diabetic Foot Ulcers
Patients reported familiarity with a wide variety of treatment options for diabetic foot ulcers, including dressings, bandages, silver nitrate, packing, and offloading devices (total contact casting, air casts, removable cast walkers, orthopedic shoes, ankle foot orthosis, Charcot restraint orthotic walker [CROW] boots, felt padding, wheelchairs, crutches, canes, and walkers). Patients reported encountering these treatment options at hospitals, wound care clinics, and chiropody clinics, as well as in home nursing visits through a community care access centre.
Preventing amputation was top-of-mind when patients chose offloading and wound care treatments. A number of patients had had experience with amputations, including single-toe, multiple-toe, foot, and below-the-knee. They made the physical and emotional effects of these amputations very clear.
“Got my confidence back and you know, I felt pretty low, I must admit. Not nice … you've had a member of your body attached to you for 66 years and all of sudden, it's gone. It was a pretty traumatic experience to go through.”
With this mindset, patients said that the main benefit of any therapy was the successful healing of the ulcer. Patients reported high tolerance for devices or treatments that were inconvenient, burdensome, or uncomfortable, as long as they successfully treated the ulcer. Treatments could take a long time, and healing was often slow, frustrating, and inconsistent. Patients also reported frequent setbacks: treatments halted and newly healed ulcers reopened. For this reason, patients were willing to try other treatments if their health care practitioner recommended them, or if those treatments showed faster healing.
“Well, it was a little bit cumbersome and heavy and hot, but I knew the downside if it didn't get healed up: I would probably face a further amputation.”
“A few years ago, we tried the air cast. It didn't work. We tried orthopedic shoes. They didn't work. We tried different types of shoes. They didn't work. We even tried a sort of cap, like a brace, that keeps the foot straight, that comes down the back of the calf and under the foot. These were all specifically made to my foot and my leg, and they didn't work. I would have problems, then the wound would open up, then I'd be back in the cast again.”
“This home care and the ulcer had been going on for 2½ years, approximately. And this was a last-ditch effort for me, so I was going to do whatever had to be done to get this over with.”
Of all the offloading devices, patients reported that total contact casting and removable cast walkers were the most commonly used and the most effective. Patients were often familiar with therapeutic shoes, but they described a wide range of these devices and stressed that therapeutic shoes were often used after total contact casting or removable cast walkers had healed the ulcer. The interview questions focused on three devices: total contact casting, removable cast walkers, and irremovable cast walkers.
We categorized comparisons between these devices as follows: the treatment process, effectiveness, comfort and mobility, and cost and access.
Total Contact Casting
Treatment Process
A health care professional is needed to apply total contact casting to a diabetic foot ulcer. Patients received total contact casting in clinic or hospital settings. Patients reported that their preparation for total contact casting was very transparent: information was readily available from a variety of sources. Patients also reported that health care staff were willing to explain the benefits, risks, and alternatives of total contact casting to their satisfaction. No patients reported surprises or being faced with unexpected consequences. Patients were aware of the standard weekly or bi-weekly appointments required to remove the old cast, examine and dress the wound inside, and reapply a new cast. These appointments typically lasted 1 to 3 hours.
Patients mostly said that the time commitment was inconvenient, but that they were willing to accept it, given the successful healing they observed with the cast. Similarly, patients were willing to travel to clinics that offered total contact casting, although they lamented the time spent travelling and wished for more convenient locations.
A few patients reported mild levels of anxiety once their foot was in the cast, because the ulcer was hidden. Having become hyper-aware of their feet and their ulcer(s), some patients imagined degradation of the wound when they couldn't see it.
“All the time I was in the cast, my mind was focused on what was happening to my wound. Was it getting worse? Would this help? What would happen when the cast came off? What options did I have left?”
Effectiveness
Patients reported high satisfaction with the healing of total contact casting. Because these patients had experience with other types of offloading devices, they could compare and contrast wound healing between devices. Patients often felt that contact casting healed ulcers more quickly than patients anticipated. Several patients reported that they had had chronic foot ulcers for several years, only to switch to total contact casting and achieve quick and effective healing. However, chronic ulcers could recur when patients' feet were unprotected. At each recurrence, patients reported seeking immediate treatment with total contact casting, avoiding other types of treatment.
“Well, like I told [the nurse], I said, ‘Just put me into a cast for the rest of my life, you know, it seems to be the only thing that works.’”
“And the healing. For the first couple of weeks, the healing on the ulcer was dramatic—absolutely unbelievable—the most we had seen in 2½ years. And she just kept it going: maybe changed the cast every week for, I'm going to guess, 6 weeks, and then every 2 weeks after that. And then finally she said to me, that's enough; we're done.”
Several patients also reported that total contact casting reduced leg edema.
“I do have a fair bit of leg edema, and the cast actually treats that quite well, too. So I've got one leg of normal size now; the other one is still fairly swollen. But the cast is actually a really effective compression device.”
Comfort and Mobility
Patients reported moderate comfort and moderate impact on mobility with total contact casting. They noted that the casting was designed to allow them an ease of mobility that closely mirrored their gait. However, this was not always completely successful, and the cast could still be inconvenient to wear. A commonly mentioned drawback was that the cast could not be removed when showering or at bedtime, unlike other types of offloading devices, such as removable cast walkers. However, patients reported a willingness to accept these inconveniences for the sake of ulcer healing.
“Walking around was a little more difficult, but not to the point where I would just say ‘Never mind, I'm not going to do this. Just skip it.’ I still tried to do it anyway.”
“Actually, I didn't find it bad at all. When I came out of the total cast I went into a mobile cast, a plastic one. And that's when [the ulcer] broke open again, because I could still have a little bit of movement in the plastic cast, where the other cast, it was good, there was no movement.”
Cost and Access
The cost of total contact casting affected patients differently depending on their income. Typical costs per cast were $50 to $100 depending on the clinic, but several clinics offered discounted unit costs for an up-front payment. The total financial burden depended on speed of healing and the total number of casts needed. For patients on a fixed income, this could become untenable, but others reported that the costs were fairly reasonable. Patients also mentioned additional out-of-pocket costs, such as parking and transportation to and from the clinic.
“But before that, I thought that the prices were really decent. You know, I didn't find it that much. So I was prepared to pay if I had to. It didn't bother me or my wife at all if we ended up paying for it, because we thought it was a reasonable price.”
“It may not be all the much money to somebody else, but on a fixed income, you know $120, $170, or whatever, even $60 a month, that's a lot of money.”
“I think it's fair, but you know, I can see people with limited income [having trouble] … But we could afford it; it wasn't an overwhelming cost by any means.”
A small number of patients reported that the cost of total contact casting was too much of a burden and had resorted to a cheaper air cast (removable cast walker), although it did not heal their ulcers.
“So because I can't afford to do that—even with insurance it's not very affordable— we're trying the air cast, and this past 2 weeks, it hasn't really been helping with the ulcer at all. If anything, it's made it worse.”
Removable Cast Walkers
Treatment Process
Patients reported no difficulty in acquiring removable cast walkers. Unlike total contact casting, removable cast walkers do not have to be applied by a health care professional. Patients reported acquiring removable cast walkers from hospitals, clinics, medical supply stores, and even from family members. One of the main reported benefits of removable cast walkers compared to total contact casting was that removable cast walkers did not require weekly appointments to check ulcer status and reapply. Patients appreciated this difference.
Although removable cast walkers were easy to obtain, a number of patients mentioned challenges in using them consistently. Some models contain air bags, which can have mechanical malfunctions. Patients also reported issues with the straps that held the walker in place.
“It was easy enough to work. There were two sides to it, and one side you'd push the little pump, and then the other side, push the little pump. I didn't know how tight I was supposed to make it. … I tried to make it feel like it did when I left the clinic. They're not the toughest of plastic bags, so one of them would constantly deflate—I forget which side.”
“It was relatively easy, when you do fill in the air bags. Trying to make sure that your foot doesn't move around too much—that was a trickier part about how much pressure to put in. And it would never stay constant. You'd always have to adjust it throughout the day.”
“And I've been trying to ask the chiropodist to explain … how should I use the air bags? The one I have right now has two. The previous one had three, and I'm not too sure what support I'm supposed to be using during the day. And it does break.”
Several patients also reported that, as a symptom of their diabetes, they had neuropathy in their extremities. This led to a loss of sensation in both the lower legs and in the fingers. This loss of sensation caused difficulties when patients applied or removed the removable cast walkers, and could cause problems if their device contained air bags that required inflating. Patients were often unsure about the degree to which the air bags should be inflated.
“…[the removable cast walker] was very difficult for somebody like me with low vision and not too much feeling in my fingers … That would have been very difficult for me to use.”
Effectiveness
Patients reported familiarity with the healing benefit of removable cast walkers. Most patients spoke about the need to remove pressure from the ulcer to promote healing. The removable cast walkers allowed patients to maintain their mobility while at the same time immobilizing the ankle and foot and removing pressure from the ulcer.
“So the foot cast is really just to make sure that the skin continues to strengthen before you add any movement … Even in a shoe or an orthotic, there is still going to be some shearing or other kinds of movement and friction on that corner of the foot.”
However, patients reported less satisfaction with ulcer healing when using a removable cast walker. Time frames to complete healing were longer, and frustration was a common sentiment expressed by the patients interviewed.
“Yeah, the past 2 weeks I've been in the air boot, and it doesn't seem like it's helped at all. I was in the cast for 3 weeks, and the ulcer was closing. Then I went to the air cast, and in 1 week the hole had reopened to three times the size it was the week before.”
Many patients who reported slower healing with removable cast walkers did not know why this was the case, but several reported that the devices did not adequately immobilize their foot, allowing for small movements that irritated the ulcer and perhaps prevented healing.
“… the air cast doesn't heal as fast. I don't know why, but it doesn't heal as fast.”
“I'll be perfectly blunt; it was a waste of time for me. The problem was (a) because of my diabetes and (b) because of my kidney transplant and the rejection drugs I was on. Healing was a definite problem for me and … the air cast did not keep my heel immobilized.”
Comfort and Mobility
Patients perceived removable cast walkers to have a moderate effect on their mobility. Removable cast walkers are designed to allow mobility while removing pressure from the ulcer, but patients reported that they could still be bulky and awkward to wear, leading to decreased activity levels and more challenges to participating in daily events. Because of the inconvenience, several patients reported having to remind themselves of the ultimate benefit of wearing such a device: a healed ulcer.
“I had to buy an offloading boot, which wasn't very easy to walk with. It altered my stance, and I ended up getting hip problems. And it was bulky, and it wasn't very easy to get around at all.”
Given the bulk of the removable cast walker, patients reported great satisfaction and appreciation for being able to remove it when they needed to. Common points at which patients removed the device were for sleeping and taking a shower.
“The air cast is walkable; you can walk with it. You can't really run with it, and people give you a lot of room at the grocery store when they see you coming down the aisle. To be able to take it off at night … it gives you so much more freedom than the other cast, but it doesn't really immobilize your foot in the same way.”
“That is one of the major, major benefits to me of that air cast was to not have to wear it to bed.”
“The air cast I wore for quite some time, and I was so thankful to be able to take it off at night and, if I had an itch in my leg to be able to put some cream on it or something or give it a little scratch or whatever. So it is, in terms of mobility and living your life, a lot better.”
Cost and Access
Patients reported a range of costs for removable cast walkers, depending on the type and model. Typical costs ranged from $100 to $260, but patients generally had to buy only one device. Most patients reported that the cost of a removable cast walker was less burdensome than that of total contact casting, although they were sympathetic to those on fixed incomes, for whom even this lower cost could be an untenable. Patients also reported that it was much simpler to have a removable cast walker covered by insurance, unlike total contact casting.
“Yeah, you had to pay for it. It was $100-ish. It's much easier … it was no trouble getting that covered by my insurance.”
However, several patients who had more chronic foot ulcers reported that they had been forced to use several removable cast walkers over time, and that the cost became more burdensome. For this reason, better healing could become a financial reason to switch to total contact casting.
“So the thing is that even at my salary, sometimes it becomes an issue because [for] the air cast not the total contact cast, because I've used it so much I've had to replace it, and … my insurance carrier will pay for an air cast once. So I've already had mine, so the next time I had to cough up the $160. Not that bad for me, but it could be an issue for others. So I can see why it would be financially easier just to go on the total contact cast, because it went so much quicker to heal than wearing an air cast.”
Irremovable Cast Walkers
We asked all patients about a range of offloading devices. While every patient was able to comment on several devices, including total contact casting and removable cast walkers, no one could provide first-hand experience with irremovable cast walkers. No patients had heard of them or seen them applied. When we described the device and its application, patients expressed skepticism and confusion about its benefits and purpose. Patients were unsure about who would be the target for such a device. In particular, several pointed to the overwhelming benefit of removable cast walkers—the ability to remove them while sleeping:
“I could see it maybe in a youngster, who would not really understand the reason, the importance, of keeping it on a lot. Maybe they do that, but … I wouldn't like to have had to wear that air cast in my bed. I would rather have had a total contact cast to sleep in than that air cast, because the boot is just so big and bulky.”
Summary
When asked to compare total contact casting and removable cast walkers, patients spoke most often about faster healing with total contact casting. The burden in terms of cost and time commitment could be higher for total contact casting, but patients said it was bearable if the ulcer healed more quickly. Several patients reported great surprise and relief at the speed of healing with total contact casting after several years of using removable cast walkers; they felt that casting improved their quality of life and allowed them to resume their regular routines. In terms of comfort and mobility, patients often rated removable cast walkers more highly than total contact casting, mainly because it was convenient to be able to remove the walker at night or in the shower. Ultimately, however, patients valued a device's effectiveness at healing the ulcer, preferring total contact casting.
“I really had to choose. I want my foot to be better, and that's the way it has to be. So if that's the way it is, if walking in this air cast is not going to allow my foot to heal and I have to go back to [total contact casting], well, I absolutely will do that, but you have to want to be better for sure to have that big cast on.”
“Well, the contact cast is a hassle. You can't shower, and it's an awkward walking position, because your foot's elevated on that rubber heel striker they attach to the bottom. The air cast is removable, which is more comfortable in bed, and you can shower with it. So from a comfort standpoint, the air cast is preferable.”
“Whatever works the best, whatever is going to be most successful for the care of my feet, is what I'm interested in. So that's why when she said total casting, I said, okay, I'm in. Whatever you think works the best is what I'm in for … I mean, don't get me wrong, I'm happy to be working with the boot at the moment. … And they did give me a choice whether I wanted it or not, but if the boot's not working, I'll be back into the cast without hesitation.”
Discussion
We interviewed a large number of patients about their experiences with diabetic foot ulcers and different offloading devices. Patients represented different areas of the province and reported different levels of ulcer severity. Despite these differences, however, all patients clearly reported that they and their families faced many challenges in dealing with their ulcers and their overall disease burden. All patients described the physical toll of dealing with ulcers: reductions in social life and physical activity were mentioned most often. Patients also spoke about the emotional burden of dealing with their ulcers, including the weight of constant vigilance and the dread of waiting for the next wound to occur. These emotional reflections were consistent across interviews.
Patients saw the pursuit of a variety of therapies and treatments as necessary to avoid the frightening possibility of amputation, or to prevent further amputations. The goal of all treatments was the same: to reduce the size of a foot ulcer, have it heal over, and prevent its recurrence. The wide variety of wound care options and offloading devices allowed patients to seek a balance between convenience, cost, and efficacy, but all patients were willing to deal with the inconvenience and physical burden of an offloading device, as long as it could heal their ulcers.
A particular strength of our findings was that all patients were familiar with more than one type of offloading device. Patients could speak directly to their experiences with total contact casting and removable cast walkers, and a large number had experience with other devices, such as therapeutic shoes, felt pads, and crutches. This patient expertise allowed for informed direct comparisons between different off-loading devices.
Conclusions
There is a significant daily burden of care and emotional weight associated with diabetic foot ulcers. The worrisome possibility of amputation leads patients to monitor their feet carefully and seek out effective means of treatment and healing. The wide variety of wound care treatments and offloading devices gives patients many opportunities to find an effective and convenient treatment option. Patients with diabetic foot ulcers reported a preference for total contact casting over removable cast walkers, largely because they perceived healing to be faster with total contact casting. However, cost, comfort, and convenience are concerns for patients. Patients reported no experience or familiarity with irremovable cast walkers.
CONCLUSIONS
The clinical evidence suggests that fibreglass total contact casting, removable cast walkers, and irremovable cast walkers are beneficial in the treatment of neuropathic, noninfected foot ulcers in patients with diabetes but without severe peripheral arterial disease. Compared to removable cast walkers, ulcer healing was improved with total contact casting (moderate quality evidence; risk difference 0.17 [95% confidence interval: 0.00–0.33]) and irremovable cast walkers (low quality evidence; risk difference 0.21 [95% confidence interval 0.01–0.40]). Irremovable cast walkers were as effective as total contact casting for treating diabetic foot ulcers and were associated with fewer costs.
The device costs of publicly funding total contact casting, removable cast walkers, and irremovable cast walkers in patients with diabetic foot ulcers would be $17 million to $20 million per year over the next 5 years. However, increased access to offloading devices could result in cost savings for the health system because of fewer amputations.
Patients with diabetic foot ulcers reported a preference for total contact casting over removable cast walkers, largely because they felt their wounds healed more quickly with total contact casting. However, cost, comfort, and the convenience of total contact casting were concerns for patients.
Acknowledgments
The medical editor was Jeanne McKane. Others involved in the development and production of this report were Arshia Ali, Harrison Heft, Claude Soulodre, Ana Laing, Kellee Kaulback, Vivian Ng, Anil Thota, Andrée Mitchell, Nancy Sikich, and Irfan Dhalla.
We are grateful to the following individuals for their expertise: Mariam Botros, Executive Director, Wounds Canada; Director, Diabetic Foot Canada. John M. Embil, Consultant, Infectious Diseases; Director, BSc(Med) Program, University of Manitoba; Director, Infection Prevention and Control Unit, Health Sciences Centre; Director, Infection Prevention and Control Program, Winnipeg Regional Health Authority; Professor, Department of Internal Medicine and Medical Microbiology, University of Manitoba. Devon Jahnke, Chiropodist, Diabetes Educator, Centre for Complex Diabetes Care, Diabetes Care Service, Sudbury Outpatient Centre, Health Sciences North. John D Lanthier, Assistant Professor, Northern Ontario School of Medicine, Clinical Sciences Division. Ann-Marie McLaren; Chiropodist/Wound Team, St. Michael's Hospital. Deirdre O'Sullivan-Drombolis, Physical Therapist, Wound Resource, Riverside Health Care, University of Western Ontario. Laura Teague, Ontario Woundcare Interest Group Executive, Health Policy; Adjunct Lecturer, Faculty of Nursing, University of Toronto; Adjunct Lecturer, Faculty of Rehabilitation, Western University. Ruth Thompson, Chiropodist, Ottawa Hospital Rehabilitation Centre. Kevin Woo, Assistant Professor, School of Nursing, Faculty of Health Sciences, Queen's University.
The statements, conclusions, and views expressed in this report do not necessarily represent the views of the consulted experts.
ABBREVIATIONS
- CI
Confidence interval
- GRADE
Grading of Recommendations Assessment, Development, and Evaluation
- ICER
Incremental cost-effectiveness ratio
- PRISMA
Preferred Reporting Items for Systematic Reviews and Meta-analyses
- QALY
Quality-adjusted life-year
- SD
Standard deviation
GLOSSARY
- Cost–utility analysis
A type of analysis that estimates the value for money of an intervention by weighing the cost of the intervention against the improvements in length of life and quality of life. The result is expressed as a dollar amount per “quality-adjusted life-year” or QALY.
- Diabetic neuropathy
Diabetic neuropathy is a type of nerve damage that can occur in people with diabetes. Nerves throughout the body can become injured, but diabetic neuropathy most often damages nerves in the legs and feet.
- Incremental cost-effectiveness ratio (ICER)
Determines “a unit of benefit” for an intervention by dividing the incremental cost by the effectiveness. The incremental cost is the difference between the cost of the treatment under study and an alternative treatment. The effectiveness is usually measured as additional years of life or as “quality-adjusted life years.”
- Intent-to-treat analysis
An approach to study analysis in which the results of individual participants assume they followed the treatment of their assigned study group, without regard to whether they followed instructions, changed treatment, or even finished the study. The purpose is to mimic world application, in which many people using the drug or treatment will not perfectly follow the recommended course.
- Offloading
Shifting weight from sensitive or injured parts of the feet using orthotics, specialized shoes or casts.
- Quality-adjusted life-year (QALY)
A measurement that takes into account both the number of years gained by a patient from a procedure and the quality of those extra years (ability to function, freedom from pain, etc.). The QALY is commonly used as an outcome measure in cost–utility analyses.
- Randomized controlled trial
A type of study in which subjects are assigned randomly into different groups, with one group receiving the treatment under study and the other group(s) receiving a different treatment or a placebo (no treatment) in order to determine the effectiveness of one approach compared with the other.
APPENDICES
Appendix 1: Literature Search Strategies
Clinical Evidence Search
Search date: Aug 17, 2016
Librarians: Corinne Holubowich and Melissa Walter
Databases searched: All Ovid MEDLINE, Embase, Cochrane Database of Systematic Reviews, Database of Abstracts of Reviews of Effects, CRD Health Technology Assessment Database, Cochrane Central Register of Controlled Trials, NHS Economic Evaluation Database, and CINAHL
Database: EBM Reviews - Cochrane Central Register of Controlled Trials <July 2016>, EBM Reviews - Cochrane Database of Systematic Reviews <2005 to August 10, 2016>, EBM Reviews - Database of Abstracts of Reviews of Effects <1st Quarter 2016>, EBM Reviews - Health Technology Assessment <3rd Quarter 2016>, EBM Reviews - NHS Economic Evaluation Database <1st Quarter 2016>, Embase <1980 to 2016 Week 33>, Epub Ahead of Print, In-Process & Other Non-Indexed Citations, Ovid MEDLINE(R) Daily and Ovid MEDLINE(R) <1946 to Present>
Search Strategy:
-
1
Diabetic Foot/ (18301)
-
2
Foot Ulcer/ (6031)
-
3
Diabetic Neuropathies/ (25269)
-
4
((diabet* adj4 (foot or feet or ulcer* or toe or toes or plantar* or neuropath* or neural* or wound*)) or DFU or (ulcer* adj2 (foot or feet)) or (plantar adj2 (ulcer* or neuropath*))).tw. (54615)
-
5
or/1–4 (72522)
-
6
Foot Diseases/ (18889)
-
7
Foot Dermatoses/ (55427)
-
8
Foot Injuries/ (7026)
-
9
Wound Healing/ (177675)
-
10
(skin ulcer* or ((foot or feet) adj2 (disease* or injur* or wound*)) or (wound* adj2 heal*)).tw. (124866)
-
11
or/6–10 (312475)
-
12
exp Diabetes Mellitus/ (1092969)
-
13
exp Diabetes Complications/ (837363)
-
14
(diabet* or MODY or IDDM or NIDDM).tw. (1230603)
-
15
or/12–14 (1443106)
-
16
11 and 15 (20659)
-
17
5 or 16 (80634)
-
18
Casts, Surgical/ (16787)
-
19
walkers/ (1033)
-
20
(cast or casts or casting* or total contact or TCC).tw. (99262)
-
21
(ITCC or walking boot* or aircast* or stabil d or stabild or optima diab or removable boot*).tw. (552)
-
22
(walker or walkers).ti,ab. (21428)
-
23
((offloading or off loading) adj2 (device* or technique* or intervention*)).tw. (208)
-
24
(offloading or off loading).ti. (307)
-
25
or/18–24 (131605)
-
26
17 and 25 (1224)
-
27
Meta-Analysis/ or Meta-Analysis as Topic/ or exp Technology Assessment, Biomedical/(234270)
-
28
Meta Analysis.pt. (73021)
-
29
(((systematic* or methodologic*) adj3 (review* or overview*)) or pooled analysis or published studies or published literature or hand search* or handsearch* or medline or pubmed or embase or cochrane or cinahl or data synthes* or data extraction* or HTA or HTAs or (technolog* adj (assessment* or overview* or appraisal*))).tw. (559201)
-
30
(meta analy* or metaanaly* or health technolog* assess*).mp. (365248)
-
31
Clinical Trials as Topic/ or Randomized Controlled Trials as Topic/ (402170)
-
32
(randomized controlled trial or controlled clinical trial).pt. (994669)
-
33
trial.ti. (531193)
-
34
(randomi#ed or randomly or RCT$1 or placebo* or sham).tw. (2424063)
-
35
or/27–34 (3608007)
-
36
26 and 35 (255)
-
37
36 use ppez (86)
-
38
26 use cctr,coch,dare,clhta,cleed (101)
-
39
or/37–38 (187)
-
40
exp Animals/ not (exp Animals/ and Humans/) (13633757)
-
41
39 not 40 (187)
-
42
limit 41 to english language [Limit not valid in CDSR,DARE; records were retained] (168)
-
43
diabetic foot/ (18301)
-
44
foot ulcer/ (6031)
-
45
diabetic neuropathy/ (33520)
-
46
((diabet* adj4 (foot or feet or ulcer* or toe or toes or plantar* or neuropath* or neural* or wound*)) or DFU or (ulcer* adj2 (foot or feet)) or (plantar adj2 (ulcer* or neuropath*))).tw. (54615)
-
47
or/43–46 (75899)
-
48
foot disease/ (21606)
-
49
skin disease/ (122151)
-
50
foot injury/ (7831)
-
51
wound healing/ (177675)
-
52
(skin ulcer* or ((foot or feet) adj2 (disease* or injur* or wound*)) or (wound* adj2 heal*)).tw. (124866)
-
53
or/48–52 (380916)
-
54
exp diabetes mellitus/ (1092969)
-
55
(diabet* or MODY or IDDM or NIDDM).tw. (1230603)
-
56
or/54–55 (1443106)
-
57
53 and 56 (22660)
-
58
47 or 57 (85694)
-
59
exp orthopedic cast/ (8144)
-
60
cast application/ (2063)
-
61
walker/ (1032)
-
62
walking aid/ (4024)
-
63
plaster walking cast/ (12)
-
64
(cast or casts or casting* or total contact or TCC).tw. (99262)
-
65
(ITCC or walking boot* or aircast* or stabil d or stabild or optima diab or removable boot*).tw. (552)
-
66
(walker or walkers).ti,ab. (21428)
-
67
((offloading or off loading) adj2 (device* or technique* or intervention*)).tw. (208)
-
68
(offloading or off loading).ti. (307)
-
69
or/59–68 (130904)
-
70
58 and 69 (1264)
-
71
Meta Analysis/ or “Meta Analysis (Topic)”/ or Biomedical Technology Assessment/(231708)
-
72
(((systematic* or methodologic*) adj3 (review* or overview*)) or pooled analysis or published studies or published literature or hand search* or handsearch* or medline or pubmed or embase or cochrane or cinahl or data synthes* or data extraction* or HTA or HTAs or (technolog* adj (assessment* or overview* or appraisal*))).tw. (559201)
-
73
(meta analy* or metaanaly* or health technolog* assess*).mp. (365248)
-
74
exp “controlled clinical trial (topic)”/ (109878)
-
75
randomized controlled trial/ or controlled clinical trial/ (1071158)
-
76
trial.ti. (531193)
-
77
(randomi#ed or randomly or RCT$1 or placebo* or sham).tw. (2424063)
-
78
or/71–77 (3493022)
-
79
70 and 78 (260)
-
80
(exp animal/ or nonhuman/) not exp human/ (9869733)
-
81
79 not 80 (260)
-
82
limit 81 to english language [Limit not valid in CDSR,DARE; records were retained] (245)
-
83
82 use emez (102)
-
84
42 or 83 (270)
-
85
84 use ppez (82)
-
86
84 use emez (102)
-
87
84 use cctr (48)
-
88
84 use coch (20)
-
89
84 use clhta (4)
-
90
84 use cleed (6)
-
91
84 use dare (8)
-
92
remove duplicates from 84 (174)
| # | Query | Results |
|---|---|---|
| S1 | (MH “Diabetic Foot”) | 6,111 |
| S2 | (MH “Foot Ulcer”) | 1,001 |
| S3 | (MH “Diabetic Neuropathies”) | 3,943 |
| S4 | ((diabet* N4 (foot or feet or ulcer* or toe or toes or plantar* or neuropath* or neural* or wound*)) or DFU or (ulcer* N2 (foot or feet)) or (plantar N2 (ulcer* or neuropath*))) | 12,214 |
| S5 | S1 OR S2 OR S3 OR S4 | 12,214 |
| S6 | (MH “Foot Diseases”) | 1,758 |
| S7 | (MH “Foot Injuries”) | 1,235 |
| S8 | (MH “Wound Healing”) | 15,282 |
| S9 | (skin ulcer* or ((foot or feet) N2 (disease* or injur* or wound*)) or (wound* N2 heal*)) | 24,056 |
| S10 | S6 OR S7 OR S8 OR S9 | 24,056 |
| S11 | (MH “Diabetes Mellitus+”) | 110,223 |
| S12 | (diabet* or MODY or IDDM or NIDDM) | 146,106 |
| S13 | S11 OR S12 | 146,710 |
| S14 | S10 AND S13 | 3,009 |
| S15 | S5 OR S14 | 12,777 |
| S16 | (MH “Casts”) | 1,192 |
| S17 | (MH “Cast Application”) | 204 |
| S18 | (MH “Walkers”) | 316 |
| S19 | (cast or casts or casting* or total contact or TCC) | 6,055 |
| S20 | (ITCC or walking boot* or aircast* or stabil d or stabild or optima diab or removable boot*) | 102 |
| S21 | (walker or walkers) | 2,091 |
| S22 | ((offloading or off loading) N2 (device* or technique* or intervention*)) | 56 |
| S23 | (TI offloading or off loading) | 267 |
| S24 | S16 OR S17 OR S18 OR S19 OR S20 OR S21 OR S22 OR S23 | 8,324 |
| S25 | S15 AND S24 | 418 |
| S26 | (MH “Meta Analysis”) | 24,989 |
| S27 | (PT “Meta Analysis”) or (PT “Systematic Review”) | 57,007 |
| S28 | ((systematic* or methodologic*) N3 (review* or overview*)) or pooled analysis or published studies or published literature or hand search* or handsearch* or medline or pubmed or embase or cochrane or cinahl or data synthes* or data extraction* or HTA or HTAs or (technolog* N1 (assessment* or overview* or appraisal*)) | 109,742 |
| S29 | (PT “randomized controlled trial”) | 56,679 |
| S30 | TI trial | 63,043 |
| S31 | (randomi?ed or randomly or RCT or RCTs or placebo* or sham) | 186,792 |
| S32 | S26 OR S27 OR S28 OR S29 OR S30 OR S31 | 303,016 |
| S33 | S25 AND S32 | 48 |
| S34 | (MH “Animals+”) not (MH “Animals+” and MH “Human”) | 61,724 |
| S35 | S33 NOT S34 | 48 |
| S36 | S33 NOT S34 Limiters - English Language |
48 |
Grey Literature
Performed on:
August 17, 2016
Websites searched:
HTA Database Canadian Repository, Alberta Health Technologies Decision Process reviews, Canadian Agency for Drugs and Technologies in Health (CADTH), Institut national d'excellence en santé et en services sociaux (INESSS), Institute of Health Economics (IHE), McGill University Health Centre Health Technology Assessment Unit, National Institute for Health and Care Excellence (NICE), Agency for Healthcare Research and Quality (AHRQ) Evidence-based Practice Centers, Australian Government Medical Services Advisory Committee, Blue Cross Blue Shield Center for Clinical Effectiveness, Centers for Medicare & Medicaid Services Technology Assessments, Institute for Clinical and Economic Review, Ireland Health Information and Quality Authority Health Technology Assessments, Washington State Health Care Authority Health Technology Reviews
Keywords used:
Cast, casts, casting, walker, walkers, walking boot, walking cast, offloading, off loading, diabetic foot, foot ulcer
Results: 11
Economic Evidence Search
Databases searched: All Ovid MEDLINE, Embase, Cochrane Central Register of Controlled Trials, Cochrane Database of Systematic Reviews, Database of Abstracts of Reviews of Effects (DARE), Centre for Reviews and Dissemination (CRD) Health Technology Assessment Database, National Health Service (NHS) Economic Evaluation Database and Cumulative Index to Nursing and Allied Health Literature (CINAHL)
Database: EBM Reviews - Cochrane Central Register of Controlled Trials <July 2016>, EBM Reviews - Cochrane Database of Systematic Reviews <2005 to August 17, 2016>, EBM Reviews - Database of Abstracts of Reviews of Effects <1st Quarter 2016>, EBM Reviews - Health Technology Assessment <3rd Quarter 2016>, EBM Reviews - NHS Economic Evaluation Database <1st Quarter 2016>, Embase <1980 to 2016 Week 33>, Epub Ahead of Print, In-Process & Other Non-Indexed Citations, Ovid MEDLINE(R) Daily and Ovid MEDLINE(R) <1946 to Present>
Search Strategy:
-
1
Diabetic Foot/ (18302)
-
2
Foot Ulcer/ (6031)
-
3
Diabetic Neuropathies/ (25271)
-
4
((diabet* adj4 (foot or feet or ulcer* or toe or toes or plantar* or neuropath* or neural* or wound*)) or DFU or (ulcer* adj2 (foot or feet)) or (plantar adj2 (ulcer* or neuropath*))).tw. (54599)
-
5
or/1–4 (72507)
-
6
Foot Diseases/ (18889)
-
7
Foot Dermatoses/ (55427)
-
8
Foot Injuries/ (7026)
-
9
Wound Healing/ (177695)
-
10
(skin ulcer* or ((foot or feet) adj2 (disease* or injur* or wound*)) or (wound* adj2 heal*)).tw. (124819)
-
11
or/6–10 (312440)
-
12
exp Diabetes Mellitus/ (1093007)
-
13
exp Diabetes Complications/ (837372)
-
14
(diabet* or MODY or IDDM or NIDDM).tw. (1230257)
-
15
or/12–14 (1442766)
-
16
11 and 15 (20656)
-
17
5 or 16 (80619)
-
18
Casts, Surgical/ (16787)
-
19
walkers/ (1033)
-
20
(cast or casts or casting* or total contact or TCC).tw. (99245)
-
21
(ITCC or walking boot* or aircast* or stabil d or stabild or optima diab or removable boot*).tw. (552)
-
22
(walker or walkers).ti,ab. (21423)
-
23
((offloading or off loading) adj2 (device* or technique* or intervention*)).tw. (208)
-
24
(offloading or off loading).ti. (307)
-
25
or/18–24 (131583)
-
26
17 and 25 (1223)
-
27
economics/ (252483)
-
28
economics, medical/ or economics, pharmaceutical/ or exp economics, hospital/ or economics, nursing/ or economics, dental/ (739307)
-
29
economics.fs. (384296)
-
30
(econom* or price or prices or pricing or priced or discount* or expenditure* or budget* or pharmacoeconomic* or pharmaco-economic*).tw. (699927)
-
31
exp “costs and cost analysis”/ (514073)
-
32
cost*.ti. (237954)
-
33
cost effective*.tw. (254559)
-
34
(cost* adj2 (util* or efficacy* or benefit* or minimi* or analy* or saving* or estimate* or allocation or control or sharing or instrument* or technolog*)).ab. (159339)
-
35
models, economic/ (136091)
-
36
markov chains/ or monte carlo method/ (120825)
-
37
(decision adj1 (tree* or analy* or model*)).tw. (34361)
-
38
(markov or markow or monte carlo).tw. (102870)
-
39
quality-adjusted life years/ (26928)
-
40
(QOLY or QOLYs or HRQOL or HRQOLs or QALY or QALYs or QALE or QALEs).tw. (52135)
-
41
((adjusted adj (quality or life)) or (willing* adj2 pay) or sensitivity analys*s).tw. (100499)
-
42
or/27–41 (2310792)
-
43
26 and 42 (118)
-
44
43 use ppez,cctr,coch,dare,clhta (61)
-
45
26 use cleed (6)
-
46
or/44–45 (67)
-
47
limit 46 to english language [Limit not valid in CDSR,DARE; records were retained] (67)
-
48
diabetic foot/ (18302)
-
49
foot ulcer/ (6031)
-
50
diabetic neuropathy/ (33522)
-
51
((diabet* adj4 (foot or feet or ulcer* or toe or toes or plantar* or neuropath* or neural* or wound*)) or DFU or (ulcer* adj2 (foot or feet)) or (plantar adj2 (ulcer* or neuropath*))).tw. (54599)
-
52
or/48–51 (75884)
-
53
foot disease/ (21606)
-
54
skin disease/ (122163)
-
55
foot injury/ (7831)
-
56
wound healing/ (177695)
-
57
(skin ulcer* or ((foot or feet) adj2 (disease* or injur* or wound*)) or (wound* adj2 heal*)).tw. (124819)
-
58
or/53–57 (380891)
-
59
exp diabetes mellitus/ (1093007)
-
60
(diabet* or MODY or IDDM or NIDDM).tw. (1230257)
-
61
or/59–60 (1442766)
-
62
58 and 61 (22657)
-
63
52 or 62 (85679)
-
64
exp orthopedic cast/ (8144)
-
65
cast application/ (2063)
-
66
walker/ (1032)
-
67
walking aid/ (4024)
-
68
plaster walking cast/ (12)
-
69
(cast or casts or casting* or total contact or TCC).tw. (99245)
-
70
(ITCC or walking boot* or aircast* or stabil d or stabild or optima diab or removable boot*).tw. (552)
-
71
(walker or walkers).ti,ab. (21423)
-
72
((offloading or off loading) adj2 (device* or technique* or intervention*)).tw. (208)
-
73
(offloading or off loading).ti. (307)
-
74
or/64–73 (130882)
-
75
63 and 74 (1263)
-
76
Economics/ (252483)
-
77
Health Economics/ or exp Pharmacoeconomics/ (215516)
-
78
Economic Aspect/ or exp Economic Evaluation/ (397215)
-
79
(econom* or price or prices or pricing or priced or discount* or expenditure* or budget* or pharmacoeconomic* or pharmaco-economic*).tw. (699927)
-
80
exp “Cost”/ (514073)
-
81
cost*.ti. (237954)
-
82
cost effective*.tw. (254559)
-
83
(cost* adj2 (util* or efficacy* or benefit* or minimi* or analy* or saving* or estimate* or allocation or control or sharing or instrument* or technolog*)).ab. (159339)
-
84
Monte Carlo Method/ (51291)
-
85
(decision adj1 (tree* or analy* or model*)).tw. (34361)
-
86
(markov or markow or monte carlo).tw. (102870)
-
87
Quality-Adjusted Life Years/ (26928)
-
88
(QOLY or QOLYs or HRQOL or HRQOLs or QALY or QALYs or QALE or QALEs).tw. (52135)
-
89
((adjusted adj (quality or life)) or (willing* adj2 pay) or sensitivity analys*s).tw. (100499)
-
90
or/76–89 (1898969)
-
91
75 and 90 (126)
-
92
limit 91 to english language [Limit not valid in CDSR,DARE; records were retained] (122)
-
93
92 use emez (56)
-
94
47 or 93 (123)
-
95
94 use ppez (34)
-
96
94 use emez (56)
-
97
94 use cctr (4)
-
98
94 use coch (19)
-
99
94 use clhta (1)
-
100
94 use dare (3)
-
101
94 use cleed (6)
-
102
remove duplicates from 94 (99)
| # | Query | Results |
|---|---|---|
| S1 | (MH “Diabetic Foot”) | 6,111 |
| S2 | (MH “Foot Ulcer”) | 1,001 |
| S3 | (MH “Diabetic Neuropathies”) | 3,943 |
| S4 | ((diabet* N4 (foot or feet or ulcer* or toe or toes or plantar* or neuropath* or neural* or wound*)) or DFU or (ulcer* N2 (foot or feet)) or (plantar N2 (ulcer* or neuropath*))) | 12,215 |
| S5 | S1 OR S2 OR S3 OR S4 | 12,215 |
| S6 | (MH “Foot Diseases”) | 1,758 |
| S7 | (MH “Foot Injuries”) | 1,235 |
| S8 | (MH “Wound Healing”) | 15,285 |
| S9 | (skin ulcer* or ((foot or feet) N2 (disease* or injur* or wound*)) or (wound* N2 heal*)) | 24,063 |
| S10 | S6 OR S7 OR S8 OR S9 | 24,063 |
| S11 | (MH “Diabetes Mellitus+”) | 110,259 |
| S12 | (diabet* or MODY or IDDM or NIDDM) | 146,132 |
| S13 | S11 OR S12 | 146,736 |
| S14 | S10 AND S13 | 3,009 |
| S15 | S5 OR S14 | 12,778 |
| S16 | (MH “Casts”) | 1,192 |
| S17 | (MH “Cast Application”) | 204 |
| S18 | (MH “Walkers”) | 316 |
| S19 | (cast or casts or casting* or total contact or TCC) | 6,056 |
| S20 | (ITCC or walking boot* or aircast* or stabil d or stabild or optima diab or removable boot*) | 102 |
| S21 | (walker or walkers) | 2,091 |
| S22 | ((offloading or off loading) N2 (device* or technique* or intervention*)) | 56 |
| S23 | (TI offloading or off loading) | 268 |
| S24 | S16 OR S17 OR S18 OR S19 OR S20 OR S21 OR S22 OR S23 | 8,326 |
| S25 | S15 AND S24 | 419 |
| S26 | (MH “Economics”) | 10,750 |
| S27 | (MH “Economic Aspects of Illness”) | 6,396 |
| S28 | (MH “Economic Value of Life”) | 506 |
| S29 | MH “Economics, Dental” | 103 |
| S30 | MH “Economics, Pharmaceutical” | 1,724 |
| S31 | MW “ec” | 137,776 |
| S32 | (econom* or price or prices or pricing or priced or discount* or expenditure* or budget* or pharmacoeconomic* or pharmaco-economic*) | 203,794 |
| S33 | (MH “Costs and Cost Analysis+”) | 82,005 |
| S34 | TI cost* | 37,815 |
| S35 | (cost effective*) | 24,736 |
| S36 | AB (cost* N2 (util* or efficacy* or benefit* or minimi* or analy* or saving* or estimate* or allocation or control or sharing or instrument* or technolog*)) | 15,782 |
| S37 | (decision N1 (tree* or analy* or model*)) | 4,465 |
| S38 | (markov or markow or monte carlo) | 2,473 |
| S39 | (MH “Quality-Adjusted Life Years”) | 2,434 |
| S40 | (QOLY or QOLYs or HRQOL or HRQOLs or QALY or QALYs or QALE or QALEs) | 4,809 |
| S41 | ((adjusted N1 (quality or life)) or (willing* N2 pay) or sensitivity analys?s) | 9,526 |
| S42 | S26 OR S27 OR S28 OR S29 OR S30 OR S31 OR S32 OR S33 OR S34 OR S35 OR S36 OR S37 OR S38 OR S39 OR S40 OR S41 | 269,283 |
| S43 | S25 AND S42 | 32 |
| S44 | S25 AND S42 Limiters - English Language |
32 |
Appendix 2: Clinical Evidence Quality Assessment
Table A1:
Risk of Bias Among Randomized Controlled Trials for the Comparison of Offloading Devices
| Author, Year | Random Sequence Generation | Allocation Concealment | Blindinga | Complete Accounting of Patients and Outcome Eventsb | Selective Reporting Bias | Other Limitations |
|---|---|---|---|---|---|---|
| Najafi et al, 201630 | Low risk | Low risk | Low riskc | Low risk | Low risk | Few baseline characteristics provided; no information on ulcer type; baseline ulcer area larger in the removable cast walker group than in irremovable cast walker group (unclear if clinically significant); complications reported, but not a prespecified outcome |
| Piaggesi et al, 201628 | Low risk | Low risk | Low riskd | Low risk | Low risk | — |
| Lavery et al, 201516 | Low risk | Low risk | Low riskd | Low risk | Low risk | Complications reported, but not a prespecified outcome |
| Gutekunst et al, 201133 | Low risk | Low risk | Low riskc | Low risk | Low risk | Complications reported, but not a prespecified outcome |
| Faglia et al, 201034 | Low risk | Low risk | Low riskc | Low risk | Low risk | Complications reported, but not a prespecified outcome |
| Van de Weg et al, 200835 | Low risk | Low risk | Low riskd | Low risk | Low risk | Possible difference in glycated hemoglobin |
| Caravaggi et al, 200732 | Unclear | Unclear | Low riskc | Low risk | Low risk | Table with baseline characteristics not provided; complications reported, but not a prespecified outcome |
| Piaggesi et al, 200729 | Low risk | Low risk | Low riskc | Low risk | Low risk | — |
| Katz et al, 200536 | Low risk | Unclear | Low riskc | Low risk | Low risk | — |
| Armstrong et al, 200537 | Low risk | Low risk | Low riskc | Low risk | Low risk | Possible baseline differences between the groups: “Wound size was nearly greater in the irremovable cast walker group”; complications reported, but not a prespecified outcome |
| Armstrong et al, 200138 | Low risk | Low risk | Low riskc | Low risk | Low risk | Complications reported, but not a prespecified outcome |
| Caravaggi et al, 200031 | Low risk | Low risk | Low riskc | Low risk | Low risk | — |
| Mueller et al, 198939 | Unclear | Unclear | Low riskc | Low risk | Low risk | — |
Blinding was not possible in most studies, but we did not consider this to be a risk of bias.
Some patients discontinued treatment for reasons that may have been related to at least one of the outcomes of interest, and the percentage of discontinuations may have differed between groups in some studies. However, since intention-to-treat analyses were performed, we did not consider this to be a risk of bias. The studies reported very few losses to follow-up.
No blinding of the outcome assessor. If the information in the study was not clear, we assumed that no blinding was done.
Blinding of the outcome assessor.
Appendix 3: Design and Characteristics of the Studies Identified
Table A2:
Design and Characteristics of the Randomized Controlled Trials
| Author, Year Country N (intervention/control) Funding Follow-up | Population | Methods | Intervention | Comparator | Other Treatment Procedures | Outcomes |
|---|---|---|---|---|---|---|
| Najafi et al, 201630 United States 49 (23/26) Qatar National Research Foundation 3 months or complete ulcer healing—whichever came first |
Diabetes Noninfected, nonischemic foot ulcers, plantar neuropathic foot ulcers Age >18 years Excluded: peripheral arterial disease; major foot amputation; active Charcot arthropathy |
Computer-generated randomization Sequentially numbered, opaque envelopes kept at the site Analyses: Chi-square or Fisher's exact test for proportions; Spearman correlation for the association between patient characteristics and outcomes |
Removable cast walker (DH Offloading Walker) Patients instructed to cleanse wound daily and apply a dressing Instructions to inspect the wound with dressing change and how to detect signs of worsening Instructions not to walk without the device |
Irremovable cast walker (DH Offloading Walker wrapped with a cohesive bandage) Wound care similar to intervention group, but weekly cast walker reapplication |
Standard treatment: wound debridement, moisture-retentive dressings | Ulcer size reduction Percent healed ulcers Daily physical activity Largest ulcer used for outcome assessment if >1 ulcer present |
| Piaggesi et al, 201628 Italy 65 (23/22/20) No funding support 3 months or complete ulcer healing—whichever came first |
Diabetes type 1 or 2 >5 years' duration Forefoot plantar ulcers grades >1 cm2 Lasting >6 weeks Grades 1A or 2Aa Peripheral neuropathy Excluded: peripheral arterial disease; osteomyelitis; contralateral ulcers; Charcot foot; lower limb edema; previous amputations in the affected or contralateral limb; metabolic decompensation; BMI >35 kg/m2 |
Consecutive patients Computer-generated randomization Outcome assessor was blinded to treatment group Analyses: nonparametric f-tests for continuous variables; Kaplan-Meier test for survival data; chi-square, Fisher's exact tests for proportions |
Fibreglass total contact casting (Softcast 3M and Scotchcast 3M) Padding over the ulcer |
Irremovable cast walker (Optima Diab) using dedicated straps provided by manufacturer Removable cast walker (Optima Diab) Hole cut in the intermediate layer of the insole in the location of the ulcer to reduce pressure |
Standard treatment for neuropathic ulcers Debridement Inert hydrofibre dressing Patient education on how to use devices Weekly reinforcement of the importance of adherence (wearing the removable cast walker at all times) |
Ulcer survivalb Time to healing Ulcer size reduction Percent healed ulcers Complications Patient satisfaction (VAS 0–10) |
| Lavery et al, 201516 United States 73 (23/27/23) United States National Institutes of Health 3 months or complete ulcer healing—whichever came first |
Diabetes Grades 1A or 2A forefoot plantar ulcersa Excluded: severe peripheral vascular disease; untreated osteomyelitis; Charcot arthropathy with severe residual deformity that would not permit the use of a walker boot |
Computer-generated randomization Single-blinded Analyses: ITT and per-protocol analysis; chi-square test for proportions; multivariate ANOVA for continuous outcomes; power calculation not reported |
Fibreglass total contact casting (personal communication with the author) Frequency of cast change NR |
Shear cast walker (Glidesoft) Healing sandals (Sroufe Deluxe Chevron shoe with 8 mm Plastazote insole) |
Debridement Hydrogel dressing Fine-mesh gauze for covering the wound Patients assessed every 7–10 days |
Percent healed ulcersb Patient satisfaction (VAS 0–10) Patient activity level Complications Reasons for withdrawal Largest ulcer used for outcome assessment if >1 ulcer present |
| Gutekunst et al, 201133 United States 23 (11/12) United States National Institutes of Health Follow-up NR |
Diabetes Peripheral neuropathy >1 incident plantar foot ulcer (Grade 1–2)c Excluded: wound infection; lower-extremity ischemia or cellulitis |
Com puter-generated randomization Open-label Analyses: chi-square test for proportions; f-test for continuous variables; power calculation not performed because no difference was expected between groups |
Total contact casting (plaster and fibreglass mix) Frequency of cast change NR |
Removable cast walker | Antimicrobial sock Pressure-measuring insole in offloading device for both groups | Offloading capacityb Percent healed ulcers Time to ulcer healing |
| Faglia et al, 201034 Italy 45 (23/22) Contributions from the removable cast walker manufacturer 3 months |
Neuropathic plantar forefoot ulcer Grade 1Aa Excluded: peripheral neuropathy; clinical signs of infection; osteomyelitis; impaired balance; contralateral foot ulcers |
Consecutive patients Randomization using sealed envelopes Open-label Analysis: Kaplan-Meier test/log-rank test for time to healing |
Total contact casting (Softcast 3M and Scotchcast 3M) German cotton Tubular stockinet Protective layer of rubber foam to protect bony protrusions Stick made of Scotchcast bandage in the middle of the two malleoli, extending for 20 cm to provide rigidity Rigid plantar sole built with same material as stick Aluminum stirrup for walking Device removed and dressing changed weekly |
Removable cast walker with rigid, boat-shaped, full rocker-bottom sole (Stabil D) Device removed and dressing changed weekly |
Debridement Paraffin gauze dressing | Ulcer area reductionb Percent healed ulcers Time to ulcer healing |
| Van de Weg et al, 200835 Netherlands 43 (23/20) Partially funded by a manufacturer; unclear whether it was the manufacturer of any of the devices used in the study 4 months |
Diabetes Plantar ulcers grades 1 or 2c Peripheral neuropathy Excluded: peripheral arterial disease; osteomyelitis |
Randomization using opaque sealed envelopes Ulcer measurement performed by blinded assessor (not easy to maintain) Time of ulcer healing, self-reported Analyses: ITT; type of analysis not provided for outcomes other than ulcer area reduction; power calculation based on ulcer area reduction |
Total contact casting (unclear if fibreglass) Adhesive foam over bony prominences Cast shoes with polyphasic rocker Crutch/cane to maintain balance if poor posture stability Cast changed weekly |
Custom-made temporary shoe Felt, rigid leather socket stiffened with Rhenoflex Education on the importance of adherence |
Debridement Hypertrophic edges removed Dressing (Aquacell) application Antibiotic if necessary |
Ulcer area reductionb Time to healing Percent healed ulcers Complications Reasons for withdrawal Largest ulcer used for outcome assessment if >1 ulcer present |
| Caravaggi et al, 200732 Italy 58 (29/29) Funding information NR 3 months |
Diabetes Neuropathic ulcer of the plantar surface Included ulcers correlated with Charcot neuroarthropathy deformities Excluded: superficial tissue infections; osteomyelitis; TcPO2 >30 mm Hg; peripheral arterial disease; severe visual deficit; amputation of contralateral limb |
Consecutive patients Randomization procedure not reported Analyses: Kaplan-Meier to estimate time to healing and healing rate; Fisher's exact test for proportion of ulcer healing; power calculation not reported |
Fibreglass total contact cast (Softcast 3M and Scotchcast 3M) Included rubber heel for walking for forefoot ulcers Walking stirrup for midfoot ulcers Frequency of cast changes not provided Before casting: German cotton application, especially over bony protrusions; stockinet on lower limb |
Removable cast walker (Aircast Pneumatic Walker, XP Diabetic Walker) Reminder to adhere to treatment at every visit |
Surgical debridement every 12 days Dressing: mesh of hyaluronic acid covered with polyurethane foam |
Ulcer surface area reduction Time to healing Percent healed ulcers Reasons for withdrawal |
| Piaggesi et al, 200729 Italy 40 (20/20) Contributions from the removable cast walker manufacturer 3 months or ulcer closure—whichever came first |
Diabetes (type 1 or 2) >5 years Peripheral neuropathy Forefoot plantar ulcer >3 weeks Grade 1A or 2A,a area >1 cm2 Excluded: peripheral vascular disease; infection, edema; osteomyelitis; Charcot neuroarthropathy |
All patients attending the foot clinic were screened for eligibility Computer-generated randomization Analyses: ITT analysis; Student's f-test and Kaplan-Meier for survival data; chi-square tests for proportions |
Fibreglass total contact casting (Softcast 3M and Scotchcast 3M) Layer of isolating foam over ulcer Layer of cotton wool 1–2 rubber heels for walking Changed every week |
Cast walker (Optima Diab) rendered irremovable by using a plastic nonremovable lace Layer of cotton wool 3-layer insoles Changed every week Patient education on how to use device |
Standard treatment for neuropathic ulcers Surgical debridement Paraffin gauze dressing, then covered with sterile gauze Patient education on how to use device |
Percent healed ulcersb Mean healing time Complications Patient satisfaction (VAS 0–10) Length of procedure Cost of treatment (materials) |
| Katz et al, 200536 United States 41 (20/21) Contributions from the walker manufacturer 3 months or ulcer healing—whichever came first |
Diabetes Chronic (>7 days with surrounding area of callus), noninfected, nonischemic stage IA or 2Aa ulcers Peripheral neuropathy Excluded: Charcot arthropathy |
Consecutive patients Randomization using a random number table Analyses: log-rank test for survival data; t-test for dichotomous variables; 95% power for 5% difference in primary outcome; 35% power for 25% in complication rates |
Total contact casting (unclear if fibreglass) Device replaced every week |
Irremovable cast walker (removable cast walker [Royce Medical] wrapped in fibreglass casting material) Device replaced every week |
Debridement as needed Dressing application Weekly follow-up |
Percent healed ulcersb Time to healing Complications Time to place and remove devices Cost |
| Armstrong et al, 200537 United States 50 (25/25) United States Department of Veteran Affairs 3 months or ulcer healing—whichever came first |
Diabetes Peripheral neuropathy Forefoot plantar ulcer Grade 1A ulcera Lack of severe peripheral vascular disease Lack of active infection |
Computer-generated randomization Analyses: Kaplan-Meier life table analysis (logrank test); chi-square test for dichotomous variables; power calculation provided |
Irremovable cast walker: removable walker (Active Offloading Walker; Royce Medical) wrapped entirely in a cohesive bandage | Removable cast walker (Active Offloading Walker; Royce Medical) | Surgical debridement as needed Weekly follow-up for device inspection, wound care, and debridement Patients instructed to wear their devices during ambulation |
Percent healed ulcers Time to healing Largest ulcer used for outcome assessment if >1 ulcer present |
| Armstrong et al, 200138 United States 63 (19/20/24) United States Department of Veterans Affairs 3 months or ulcer healing—whichever came first |
Neuropathic diabetic plantar foot ulcer Noninfected, Grade 1Aa At least one palpable foot pulse or TcPO2 >40 mm Hg at dorsum of forefoot Excluded: inability to walk without wheelchair assistance; wounds on the heel, rear foot, or nonplantar; severe peripheral vascular disease |
Computerized randomization schedule Analyses: ANOVA with correction for multiple comparisons for continuous variables; chi-square test for dichotomous variables; Kaplan-Meier with logrank test for survival outcomes |
Total contact casting (fibreglass and plaster) Casting change frequency NR (weekly wound inspection) |
Removable cast walker (Aircast) Half-shoe (Darco, WV) |
Wound care and debridement Surgical debridement if needed Weekly visits |
Percent healed ulcersb Time to healing Reasons for withdrawal Activity levelb Quality of life (SF-36) in separate publication40 Largest ulcer used for outcome assessment if >1 ulcer present |
| Caravaggi et al, 200031 Italy 50 (26/24) Funding information not available 30 days |
Diabetes Peripheral neuropathy Plantar ulcers Excluded: deep or superficial tissue infections; osteomyelitis; peripheral arterial disease; severe balance problems; severe visual deficit; other foot skin lesions; plantar bilateral ulcers; amputation of a limb |
Consecutive patients Centralized randomization Analyses: chi-square test for dichotomous variables; f-test for continuous variables; power calculation based on healing rate outcome |
Fibreglass total contact cast (Softcast 3M and Scotchcast 3M) Stick made of Scotchcast 3M in the middle of the two malleoli extending for 20 cm to provide rigidity Rigid plantar insole built of same material as stick Aluminum stirrup or rubber heel, depending on position of the ulcer, to allow walking Elevation of the opposite foot to ease walking, patient training Before casting: German cotton especially over bony protrusions; stockinet on lower limb |
Therapeutic shoes with rocker-bottom sole Plastazote insole with an area of offloading Unaffected foot received the same shoe without the offloading area Dressing changes every 2 days |
Surgical debridement if necessary Paraffin gauze dressing |
Ulcer healing rateb Percent healed ulcers Patient acceptance (VAS 1–100) Complications |
| Mueller et al, 198939 United States 40 (21/19) Funded by the Foundation for Physical Therapy Unclear (approximately 90 days based on ranges for ulcer healing) |
Diabetes Peripheral neuropathy Plantar ulcers Grade 1–2d No gross infection Excluded: osteomyelitis; gangrene |
Tested the hypothesis of no difference in ulcers healed or time to healing between groups No details about randomization procedure Analysis: chi-square test for dichotomous variables |
Total contact cast (plaster [inner layer] and fibreglass) Inner layer: plaster shell reinforced by plaster splints Outer layer: fibreglass for durability and to allow weight bearing sooner Walking heel attached Assistive devices (walkers, crutches) provided if needed First cast change 5–7 days after initial application; if no complications, changes every 2–3 weeks |
Traditional dressing treatment Healing sandal, extra-depth shoe with Plastazote insert Dressing change 2–3 times daily; nurse home visit for dressing change if needed Follow-up every 2–4 weeks |
— | Percent healed ulcers Time to healing Complications |
Abbreviations: ANOVA, analysis of variance; BMI, body mass index; ITT, intention-to-treat; NR, not reported; SF-36, Short-Form 36-item health survey; TcPO2, transcutaneous oxygen; VAS, visual analogue scale.
University of Texas Classification of Diabetic Wounds.42
Primary outcome.
Wagner Foot Ulcer Grading System.65
Appendix 4: Outcome Definitions and Wound Classification System
Table A3:
Definitions Used in the Studies Identified
| Author, Year | Peripheral Neuropathy | Peripheral Arterial Disease | Ulcer Healing |
|---|---|---|---|
| Najafi et al, 201630 | Not provided | Ankle-brachial index <0.5 | Not provided |
| Piaggesi et al, 201628 | Not provided | Ankle-brachial pressure index <0.90 Absence of 2 palpable pulses in affected foot |
Not provided |
| Lavery et al, 201516 | Pressure sensation evaluated at 10 points on each foot using 10 g monofilaments | Ankle-brachial pressure index <0.60 or TcPO2 <25 mm/Hg |
Healed ulcer: complete re-epithelialization with no drainage Unhealed ulcer: not meeting criteria above; treatment discontinuation, either voluntarily or because of adverse events |
| Gutekunst et al, 201133 | Sensation to light touch and pressure evaluated at 9 points on the plantar surface using Semmes-Weinstein 5.07 (10 g) and 6.10 monofilaments Sensation of vibration evaluated using a 128 Hz tuning fork Sensation of joint position evaluated at the ankle joint and first metatarsal-phalangeal joint |
Not provided | Not provided |
| Faglia et al, 201034 | Insensitivity to a 10 g Semmes-Weinstein monofilament in >6 out of 9 areas of the foot Vibration perception threshold of >25 V measured by a biothesiometer on the malleolus |
Ankle-brachial pressure index <0.9 and/or TcPO2 <50 mm Hg on the dorsum of the foot | Complete re-epithelialization of the ulcerated area |
| Van de Weg et al, 200835 | Somatosensory test using a 10 g Semmes-Weinstein monofilament | Ankle-brachial index <0.4 |
Healed ulcer: complete re-epithelialization of the ulcerated area, with no drainage or sinus formation Unhealed ulcer: not meeting criteria above; patient discontinuation |
| Caravaggi et al, 200732 | Insensitivity to a 10 g monofilament Vibration perception threshold of >25 V measured on the malleolus |
Ankle-brachial index <0.6 | Not available |
| Piaggesi et al, 200729 | Insensitivity to a 10 g monofilament Vibration perception threshold of >25 V measured on the malleolus |
Ankle-brachial index <0.9 | Complete re-epithelialization of the ulcerated area |
| Katz et al, 200536 |
Not available | Not available | Complete re-epithelialization |
| Armstrong et al, 200537 | Insensitivity measured with a vibration perception threshold meter >25 V | No palpable pulse | Complete re-epithelialization |
| Armstrong et al, 200138 | Insensitivity to a 10 g monofilament Vibration perception threshold of >25 V | No palpable foot pulse | Complete re-epithelialization |
| Caravaggi et al, 200031 | Insensitivity to a 10 g monofilament Vibration perception threshold of >25 V measured on the malleolus |
Ankle-brachial pressure index 0.6 and/or TcPO2 30 mm Hg | Not provided |
| Mueller et al, 198939 | Lowest perception of Semmes-Weinstein monofilament (4.17, 5.07, 6.10) on 7 points | Not available |
Healed ulcer: complete skin coverage and no drainage Unhealed ulcer: not meeting criteria above; patient refused to continue treatment assignment before wound healing; grossly infected, increase in size, or no improvement at 6 weeks |
Abbreviation: TcPO2, transcutaneous oxygen pressure.
Table A4:
Ulcer Classification Systems
| University of Texas Wound Grading System for Diabetic Foot Wounds42a | Wagner Foot Ulcer Grading System65 |
|---|---|
| 0A: Pre- or post-ulcerative lesion, completely epithelialized; not infected; no ischemia | 0: No open lesions in the skin; may be evidence of healed lesions |
| 1A: Superficial wound not involving tendon, capsule, or bone; not infected; no ischemia | 1: Superficial wound without penetration to deeper layers |
| 2A: Wound penetrating to tendon or capsule; not infected; no ischemia | 2: Wound involving tendon, bone, or joint capsule; no abscess or osteomyelitis |
| 3A: Wound penetrating to bone or joint; not infected; no ischemia |
3: Deep ulcer with abscess or osteomyelitis 4: Gangrene to portion of forefoo 5: Extensive gangrene of foot; amputation must be carried out |
The University of Texas Grading System for diabetic foot wounds also includes the categories B, C, and D for each grade (0–3); they were not relevant for the studies included in the clinical evidence review, so we have not described them here.
Appendix 5: Baseline Characteristics of Patients Included in the Studies Identified
Table A5:
Baseline Characteristics of Patients Included in the Randomized Controlled Trials
| Author, Year N (intervention/ control) | Demographics | Mean BMI, kg/m2 (SD) | Mean Diabetes Duration, y (SD) | Mean HbA1C, % (SD) | Ulcer | History | ||||
|---|---|---|---|---|---|---|---|---|---|---|
| Grade, n (%) | Location, n (%) | Duration, weeks (IQR) | Mean area, cm2 (SD; range) | Ulcer, n (%) | Amputation, n (%) | |||||
| Najafi et al, 201630 49 (23/26) |
Male, n (%) ICW: 21 (89) RCW: 25 (96) Mean age, y (SD) ICW: 52 (8) RCW: 55 (7) Ethnicity NA |
ICW: 31 (7) RCW: 28 (5) |
NA | ICW: 10.3 (1.7) RCW: 10.3 (2.8) |
NA | Forefoot, midfoot, and rear footb (proportions not provided) | NA | ICW: 6.5 (8.5; 0.36–39.0) RCW: 10.1 (12.0; 0.16636.8) |
NA | NA |
| Piaggesi et al, 201628 65 (23/22/20) |
Male, n (%) 39 (60) Mean age, y (SD) TCC: 61 (10) ICW: 60 (8) RCW: 62 (9) Ethnicity NA |
TCC: 30 (4) ICW 33 (4) RCW: 30 (3) |
>5 years | TCC: 8.1 (0.9) ICW: 8.0 (1.1) RCW: 8.4 (1.0) |
Grade 1A TCC: 14 (70) ICW 15 (75) RCW: 16 (80) Grade 2A TCC: 6 (30) ICW: 5 (25) RCW: 4 (20) |
All forefoot | >6 weeks | >1 cm2 | TCC: 12 (50) ICW: 10 (45) RCW: 11 (55) |
0 (exclusion criterion) |
| Lavery et al, 201516 73 (23/27/23) |
Male, n (%) TCC: 14 (61) RCW: 15 (56) Shoes: 12 (52) Mean age NA Ethnicity, n (%) White TCC: 10 (43) RCW: 8 (30) Shoes: 7 (30) Hispanic TCC: 12 (52) RCW: 17 (63) Shoes: 14 (61) African-American TCC: 1 (4) RCW: 2 (7) Shoes: 1 (4) |
NA | NA | NA | 1A and 2A included (proportions not provided) | All forefoot | NA | TCC: 2.2 (3.5) RCW: 2.3 (4.1) Shoes: 2.0 (3.5) |
TCC: 15 (65) RCW: 23 (85) Shoes: 13 (52) |
TCC: 10 (44) RCW: 4 (15) Shoes: 15 (65) |
| Gutekunst et al, 201133 23 (11/12) |
Male, n (%) TCC: 9 (82) RCW: 10 (83) Mean age, y (SD) TCC: 53 (10) RCW: 55 (13) Ethnicity NA |
TCC: 32 (5) RCW: 31 (6) |
TCC: 19 (14) RCW: 17 (13) |
TCC: 8.5 (2.3) RCW: 8.9 (1.8) |
Wagner classification Grade 1 or 2 (proportions not provided) |
Forefoot TCC: 8 (73) RCW: 11 (92) Midfoot TCC: 3 (27) RCW: 1 (8) |
NA | NA | NA | NA |
| Faglia et al, 201034 45 (23/22) |
Males, n (%) TCC: 15 (65) RCW: 15 (68) Age, y (SD) TCC: 59 (9) RCW: 62 (10) Ethnicity NA |
TCC: 32 (5) RCW: 30 (1) |
TCC: 18 (11) RCW: 17 (10) |
TCC: 9.1 (2.1) RCW: 7.5 (1.1) |
All Grade 1A | All forefoot | NA | TCC: 1.4 (1.2) RCW: 2.2 (2.2) |
TCC: 15 (65) RCW: 15 (68) |
Minor amputation TCC: 11 (48) RCW: 12 (55) |
| Van de Weg et al, 200835 43 (23/20) |
Male, n (%) TCC: 16 (68) Shoes: 18 (90) Age, y (SD) TCC: 65 (11) Shoes: 58 (11) Ethnicity NA |
NA | TCC: 12 (6) Shoes: 12 (7) |
TCC: 7.8 (0.3) Shoes: 8.7 (2.2) |
Wagner classification Grade 1 TCC: 2 (9) Shoes: 2 (10) Grade 2 TCC: 21 (91) Shoes: 18 (90) |
Forefoot TCC: 20 (87) Shoes: 18 (90) |
TCC: 4 (3, 8) Shoes: 5 (4, 8) |
TCC: 4.2 (3.1) Shoes: 3.0 (3.1) |
NA | NA |
| Caravaggi et al, 200732 58 (29/29) |
NA | NA | NA | NA | NA | NA | NA | TCC: 3.9 (3.4) RCW: 3.4 (3.0) |
NA | NA |
| Piaggesi et al, 200729 40 (20/20) |
Male NA Age, y (SD) TCC: 60 (8) ICW: 61 (6) Ethnicity NA |
NA | TCC: 15 (11) ICW: 13 (8) |
TCC: 7.9 (1.1) ICW: 7.6 (0.9) |
Grade 1A and 2A (proportions not provided) | All forefoot | >3 weeks | TCC: 3.7 (1.6) ICW: 3.9 (1.8) |
NA | NA |
| Katz et al, 200536 41 (20/21) |
Male, n (%) TCC: 14 (65) ICW: 15 (71) Age, y (range) TCC: 51 (23–65) ICW: 51 (29–65) Ethnicity, n (%) White TCC: 2 (10) ICW: 3 (14) Hispanic TCC: 12 (60) ICW: 13 (62) Black TCC: 8 (40) ICW: 6 (29) |
NA |
Mean (range) TCC: 14 (2–27) ICW: 14 (5–33) |
NA | Grades 1A and 2A (proportions not provided) |
Forefoot TCC: 15 (76) ICW: 14 (65) Midfoot TCC: 5 (24) ICW: 6 (30) Heel TCC: 0 ICW: 1 (5) |
TCC: 11 (3–38) ICW: 8 (2–37) |
Mean (median, IQR) TCC: 2.9 (1.9, 0.9–3.9) ICW: 3.1 (1.6, 0.9–3.5) |
NA | NA |
| Armstrong et al, 200537 50 (25/25) |
Males, n (%) ICW: 20 (87.0) RCW: 24 (88.9) Age, y (SD) ICW: 66.9 (10.1) RCW: 64.6 (9.8) Ethnicity NA |
ICW: 33.3 (6.8) RCW: 33.5 (6.2) |
NA | ICW: 8.5 (1.5) RCW: 8.0 (1.4) |
All Grade 1A | All forefoot | NA | ICW: 2.7 (1.3) RCW: 2.0 (1.1) |
NA | NA |
| Armstrong et al, 200138 63 (19/20/24) |
Male, n (%) TCC: 14 (74) RCW: 18 (90) Shoes: 20 (83) Age NA Ethnicity NA |
NA | TCC: 18 (9) RCW: 18 (10) Shoes: 15 (8) |
NA | All Grade 1A | Forefoot and midfoot (proportions not provided) |
Mean (SD) TCC: 17 (100.3) RCW: 22 (111.7) Shoes: 22 (137.2) |
TCC: 1.3 (0.8) RCW: 1.4 (1.4) Shoes: 1.3 (1.2) |
NA | NA |
| Caravaggi et al, 200031 50 (26/24) |
Male, n (%) TCC: 18 (69) Shoes: 24 (67) Age, y (SD) TCC: 61 (11) Shoes: 59 (10) Ethnicity NA |
TCC: 27 (2) Shoes: 27 (3) |
TCC: 17 (11) Shoes: 16 (9) |
NA | NA | NA | NA | NA | NA | NA |
| Mueller et al, 198939 40 (21/19) |
Male, n (%) TCC: 21 (62) Shoes: 14 (74) Age, y (SD) TCC: 54 (10) Shoes: 55 (12) Ethnicity NA |
NA | TCC: 17 (6) Shoes: 17 (9) |
NA |
Wagner classification Grade 1 TCC: 15 (71) Shoes: 13 (68) Grade 2 TCC: 6 (29) Shoes: 6 (32) |
Forefoot: 32 (80%) Midfoot: 5 (12.5) Heel: 3 (7.5) Proportions by study group not provided |
Mean (SD) TCC: 22 (28) Shoes: 25 (29) |
Area TCC: 1.8 (2.5) Shoes: 2.8 (3.4) Depth (mm), mean (SD) TCC: 3.6 (3.2) Shoes: 2.4 (0.9) |
NA | NA |
Abbreviations: BMI, body mass index; HbA1c, glycated hemoglobin; ICW; irremovable cast walker; IQR, interquartile range; NA, not available; RCW, removable cast walker; SD, standard deviation; Shoes, therapeutic shoes; TCC, total contact casting.
University Texas Classification, unless otherwise specified.
Based on personal communication with the authors.
Appendix 6: Results of Applicability Checklist for Studies Included in the Economic Literature Review
Table A6:
Cost-Consequence Analysis (Cost Per Patient)
| Objective: To assess the cost consequences of offloading devices for treatment of diabetic foot ulcers | |||||
|---|---|---|---|---|---|
| Author, Year | Is the study population similar to the question? | Are the interventions similar to the question? | Is the health care system in which the study was conducted sufficiently similar to the current Ontario context? | Was/were the perspective(s) clearly stated and what were they? | Are estimates of relative treatment effect from the best available source? |
| Craig et al, 201343 | Yes | Somewhat | Yes | Yes | Yes |
| Author, Year | Are all future costs and outcomes discounted? (If yes, at what rate?) | Is the value of health effects expressed in terms of quality-adjusted life-years? | Are costs and outcomes from other sectors fully and appropriately measured and valued? | Overall judgement (directly applicable/partially applicable/not applicable) |
|---|---|---|---|---|
| Craig et al, 201343 | No | No | No | Partially applicable |
Appendix 7: Budget Impact Analysis—Scenario Analysis
Tables A7 to A9 show the expected budget impact of adopting total contact casting, removable cast walkers and irremovable cast walkers over the next 5 years if the proportion of use of each device increased to 100%.
In this analysis, under different levels of access for offloading devices (50%, 75%, and 100%), we assumed that all patients with a diabetic foot ulcer would receive either total contact casting, removable cast walkers, or irremovable cast walkers. We then calculated the budget impact for each of these devices.
The budget impact of adopting total contact casting, removable cast walkers, or irremovable cast walkers for the next 5 years would range from $2.7 million to $26 million per year at 100% proportion of use.
Table A7:
Budget Impact of Adopting Offloading Devices at 50% Access and 100% Proportion of Use for Each Device in Ontario, 2016–2020
| Year | Cost | Total Contact Casting | Removable Cast Walkers | Irremovable Cast Walkers |
|---|---|---|---|---|
| 2016 | Device cost | $11,371,999 | $2,752,920 | $6,067,349 |
| Treatment cost | $32,367,332 | $57,019,365 | $33,359,364 | |
| Amputation cost | $110,393,304 | $117,633,246 | $111,103,103 | |
| Total cost | $154,132,636 | $177,405,531 | $150,529,816 | |
| 2017 | Device cost | $11,854,823 | $2,869,802 | $6,324,952 |
| Treatment cost | $33,741,561 | $59,440,251 | $34,775,712 | |
| Amputation cost | $115,080,303 | $122,627,633 | $115,820,237 | |
| Total cost | $160,676,687 | $184,937,686 | $156,920,901 | |
| 2018 | Device cost | $12,344,755 | $2,988,404 | $6,586,347 |
| Treatment cost | $35,136,020 | $61,896,777 | $36,212,910 | |
| Amputation cost | $119,836,300 | $127,695,543 | $120,606,814 | |
| Total cost | $167,317,076 | $192,580,724 | $163,406,072 | |
| 2019 | Device cost | $12,841,881 | $3,108,748 | $6,851,581 |
| Treatment cost | $36,550,955 | $64,389,372 | $37,671,211 | |
| Amputation cost | $124,662,132 | $132,837,869 | $125,463,675 | |
| Total cost | $174,054,968 | $200,335,989 | $169,986,467 | |
| 2020 | Device cost | $13,346,284 | $3,230,853 | $7,120,697 |
| Treatment cost | $37,986,602 | $66,918,456 | $39,150,860 | |
| Amputation cost | $129,558,608 | $138,055,471 | $130,391,634 | |
| Total cost | $180,891,495 | $208,204,780 | $176,663,191 |
Note: Numbers may appear inexact due to rounding.
Table A8:
Budget Impact of Adopting Offloading Devices at 75% Access and 100% Proportion of Use for Each Device in Ontario, 2016–2020
| Year | Cost | Total Contact Casting | Removable Cast Walkers | Irremovable Cast Walkers |
|---|---|---|---|---|
| 2016 | Device cost | $17,057,999 | $4,129,381 | $9,101,023 |
| Treatment cost | $48,550,999 | $85,529,047 | $50,039,046 | |
| Amputation cost | $67,861,282 | $78,721,194 | $68,925,980 | |
| Total cost | $133,470,280 | $168,379,622 | $128,066,049 | |
| 2017 | Device cost | $17,782,235 | $4,304,703 | $9,487,428 |
| Treatment cost | $50,612,342 | $89,160,377 | $52,163,568 | |
| Amputation cost | $70,742,487 | $82,063,482 | $71,852,389 | |
| Total cost | $139,137,064 | $175,528,562 | $133,503,384 | |
| 2018 | Device cost | $18,517,133 | $4,482,606 | $9,879,521 |
| Treatment cost | $52,704,030 | $92,845,165 | $54,319,365 | |
| Amputation cost | $73,666,107 | $85,454,972 | $74,821,878 | |
| Total cost | $144,887,271 | $182,782,743 | $139,020,764 | |
| 2019 | Device cost | $19,262,821 | $4,663,122 | $10,277,371 |
| Treatment cost | $54,826,432 | $96,584,059 | $56,506,817 | |
| Amputation cost | $76,632,657 | $88,896,261 | $77,834,971 | |
| Total cost | $150,721,910 | $190,143,441 | $144,619,158 | |
| 2020 | Device cost | $20,019,426 | $4,846,279 | $10,681,045 |
| Treatment cost | $56,979,903 | $100,377,685 | $58,726,290 | |
| Amputation cost | $79,642,632 | $92,387,926 | $80,892,170 | |
| Total cost | $156,641,961 | $197,611,890 | $150,299,506 |
Note: Numbers may appear inexact due to rounding
Table A9:
Budget Impact of Adopting Offloading Devices at 100% Access and 100% Proportion of Use for Each Device in Ontario, 2016–2020
| Year | Cost | Total Contact Casting | Removable Cast Walkers | Irremovable Cast Walkers |
|---|---|---|---|---|
| 2016 | Device cost | $22,743,999 | $5,505,841 | $12,134,697 |
| Treatment cost | $64,734,665 | $114,038,729 | $66,718,729 | |
| Amputation cost | $25,329,260 | $39,809,143 | $26,748,857 | |
| Total cost | $112,807,924 | $159,353,713 | $105,602,283 | |
| 2017 | Device cost | $23,709,647 | $5,739,604 | $12,649,904 |
| Treatment cost | $67,483,122 | $118,880,503 | $69,551,424 | |
| Amputation cost | $26,404,672 | $41,499,331 | $27,884,540 | |
| Total cost | $117,597,440 | $166,119,437 | $110,085,868 | |
| 2018 | Device cost | $24,689,510 | $5,976,808 | $13,172,694 |
| Treatment cost | $70,272,040 | $123,793,553 | $72,425,820 | |
| Amputation cost | $27,495,914 | $43,214,400 | $29,036,943 | |
| Total cost | $122,457,465 | $172,984,762 | $114,635,457 | |
| 2019 | Device cost | $25,683,762 | $6,217,495 | $13,703,161 |
| Treatment cost | $73,101,910 | $128,778,745 | $75,342,422 | |
| Amputation cost | $28,603,181 | $44,954,653 | $30,206,266 | |
| Total cost | $127,388,852 | $179,950,893 | $119,251,850 | |
| 2020 | Device cost | $26,692,568 | $6,461,706 | $14,241,394 |
| Treatment cost | $75,973,204 | $133,836,913 | $78,301,720 | |
| Amputation cost | $29,726,655 | $46,720,380 | $31,392,707 | |
| Total cost | $132,392,428 | $187,018,999 | $123,935,821 |
Note: Numbers may appear inexact due to rounding.
We also explored the budget impact of varying the proportion of use of irremovable cast walkers from 1.5% to 21.5% (Table A10).
Table A10:
Proportion of Use of Offloading Devices in Ontario, 2016–2020a
| Year | Total Contact Casting | Removable Cast Walkers | Irremovable Cast Walkers | Total |
|---|---|---|---|---|
| 2016 | 57.0% | 41.5% | 1.5% | 100% |
| 2017 | 57.0% | 36.0% | 7.0% | 100% |
| 2018 | 57.0% | 33.0% | 10.0% | 100% |
| 2019 | 57.0% | 29.0% | 14.0% | 100% |
| 2020 | 57.0% | 21.5% | 21.5% | 100% |
Expert opinion.
When we varied the proportion of use of irremovable cast walkers (using the figures from Table A10) and increased access to an offloading device from 50% to 75% and from 75% to 100%, we observed cost savings as a result of fewer amputations (Table A11).
Table A11:
Net Budget Impact of Adopting Offloading Devices at Varying in Proportions of Use for Irremovable Cast Walkers in Ontario, 2016–2020
| Year | Cost | Change in Accessibility | |
|---|---|---|---|
| 50% to 75% | 75% to 100% | ||
| 2016 | Device cost | $3,862,729 | $3,862,729 |
| Treatment cost | $21,297,245 | $21,297,245 | |
| Amputation cost | −$41,680,264 | −$41,680,264 | |
| Total cost | −$16,520,291 | −$16,520,291 | |
| 2017 | Device cost | $4,125,448 | $4,125,448 |
| Treatment cost | $22,693,590 | $22,693,590 | |
| Amputation cost | −$43,449,895 | −$43,449,895 | |
| Total cost | −$16,630,857 | −$16,630,857 | |
| 2018 | Device cost | $4,347,342 | $4,347,342 |
| Treatment cost | $22,018,265 | $22,018,265 | |
| Amputation cost | −$45,245,576 | −$45,245,576 | |
| Total cost | −$18,879,969 | −$18,879,969 | |
| 2019 | Device cost | $4,602,614 | $4,602,614 |
| Treatment cost | $22,332,413 | $22,332,413 | |
| Amputation cost | −$47,067,625 | −$47,067,625 | |
| Total cost | −$20,132,598 | −$20,132,598 | |
| 2020 | Device cost | $4,922,319 | $4,922,319 |
| Treatment cost | $22,217,885 | $22,217,885 | |
| Amputation cost | −$48,916,346 | −$48,916,346 | |
| Total cost | −$21,776,142 | −$21,776,142 | |
Note: Numbers may appear inexact due to rounding.
Appendix 8: Public and Patient Engagement—Interview Materials
Figure A1: Letter of Information.
Figure A2: Consent and Release Form.
Figure A3: Interview Guide.
Author contributions
This report was developed by a multidisciplinary team from Health Quality Ontario. The lead clinical epidemiologist was Vania Costa, the lead health economist was Hong Anh Tu, the public engagement senior program analysts were David Wells and Mark Weir, and the medical librarians were Corinne Holubowich and Melissa Walter.
KEY MESSAGES
What Is This Health Technology Assessment About?
About 1 in 10 people in Ontario have diabetes. Each year, about 2% to 3% of them develop a foot ulcer. Diabetic foot ulcers put people at risk for foot and lower leg amputation. Pressure offloading devices, which include fibreglass total contact casting, removable cast walkers, and irremovable cast walkers, are used to treat foot ulcers, but they are not routinely publicly funded in Ontario.
The objective of this report was to assess the clinical benefits and harms of fibreglass total contact casting, removable cast walkers, and irremovable cast walkers in people with diabetic foot ulcers. We compared these devices with each other and with therapeutic shoes. We looked at the cost-effectiveness of these devices and calculated the budget impact of publicly funding them. We also interviewed people who have used these devices to learn more about their experiences.
What Did the Health Technology Assessment Find?
Total contact casting and irremovable cast walkers showed better ulcer healing than removable cast walkers, and they were also more cost-effective. If more people used these devices, the health system would likely save money because fewer people would need amputations. Patients with diabetic foot ulcers preferred total contact casting over removable cast walkers, largely because they perceived that total contact casting led to better healing.
Contributor Information
Health Quality Ontario:
Vania Costa, Hong Anh Tu, David Wells, Mark Weir, Corinne Holubowich, and Melissa Walter
About Health Quality Ontario
Health Quality Ontario is the provincial advisor on the quality of health care. We are motivated by a single-minded purpose: Better health for all Ontarians.
Who We Are.
We are a scientifically rigorous group with diverse areas of expertise. We strive for complete objectivity, and look at things from a vantage point that allows us to see the forest and the trees. We work in partnership with health care providers and organizations across the system, and engage with patients themselves, to help initiate substantial and sustainable change to the province's complex health system.
What We Do.
We define the meaning of quality as it pertains to health care, and provide strategic advice so all the parts of the system can improve. We also analyze virtually all aspects of Ontario's health care. This includes looking at the overall health of Ontarians, how well different areas of the system are working together, and most importantly, patient experience. We then produce comprehensive, objective reports based on data, facts and the voice of patients, caregivers and those who work each day in the health system. As well, we make recommendations on how to improve care using the best evidence. Finally, we support large scale quality improvements by working with our partners to facilitate ways for health care providers to learn from each other and share innovative approaches.
Why It Matters.
We recognize that, as a system, we have much to be proud of, but also that it often falls short of being the best it can be. Plus certain vulnerable segments of the population are not receiving acceptable levels of attention. Our intent at Health Quality Ontario is to continuously improve the quality of health care in this province regardless of who you are or where you live. We are driven by the desire to make the system better, and by the inarguable fact that better has no limit.
REFERENCES
- (1).Brem H, Sheehan P, Rosenberg HJ, Schneider JS, Boulton AJ. Evidence-based protocol for diabetic foot ulcers. Plast Reconstr Surg. 2006; 117(7 Suppl):193S–209S; discussion 10S–11S. [DOI] [PubMed] [Google Scholar]
- (2).Lewis J, Lipp A. Pressure-relieving interventions for treating diabetic foot ulcers. Cochrane Database of Systematic Reviews 2013, Issue 1. Art. No.: CD002302. DOI: 10.1002/14651858.CD002302.pub2. [DOI] [PMC free article] [PubMed]
- (3).Cavanagh PR, Lipsky BA, Bradbury AW, Botek G. Treatment for diabetic foot ulcers. Lancet. 2005; 366(9498):1725–35. [DOI] [PubMed] [Google Scholar]
- (4).Wu SC, Crews RT, Armstrong DG. The pivotal role of offloading in the management of neuropathic foot ulceration. Curr Diab Rep. 2005; 5(6):423–9. [DOI] [PubMed] [Google Scholar]
- (5).Canadian Diabetes Association. Diabetes charter backgrounder - Ontario [Internet]. Canada: CDA; 2015. [cited 2015 Nov 23]. Available from: http://www.diabetes.ca/getmedia/5941b1c2-8b03-45bf-8db0-e18b969d9aa6/diabetes-charter-backgrounder-ontario-english.pdf.aspx [Google Scholar]
- (6).Ndip A, Ebah L, Mbako A. Neuropathic diabetic foot ulcers - evidence-to-practice. Int J Gen Med. 2012; 5:129–34. [DOI] [PMC free article] [PubMed] [Google Scholar]
- (7).Woo K, Carvill L, Alavi A, Queen D, Rothman A, Woodbury G, et al. An audit of leg and foot ulcer care in an Ontario Community Care Access Centre. Wound Care Canada. 2007; 5(Suppl 1):S17–S27. [Google Scholar]
- (8).Canadian Institute for Health Information. Compromised wounds in Canada [Internet]. Canada: Canadian Institute for Health Information; 2013. [cited 2015 Nov 23]. Available from: https://secure.cihi.ca/free_products/AiB_Compromised_Wounds_EN.pdf [Google Scholar]
- (9).Cross C. Risk of compromised wounds greater among patients with diabetes, CIHI study shows. CMAJ. 2013; 185(14):E664. [DOI] [PMC free article] [PubMed] [Google Scholar]
- (10).Wu SC, Armstrong DG. The role of activity, adherence, and off-loading on the healing of diabetic foot wounds. Plast Reconstr Surg. 2006; 117(7 Suppl.):248S–53S. [DOI] [PubMed] [Google Scholar]
- (11).Armstrong DG, Lavery LA, Nixon BP, Boulton AJM. It's not what you put on, but what you take off: techniques for debriding and off-loading the diabetic foot wound. Clin Infect Dis. 2004; 39(Suppl. 2):S92–S9. [DOI] [PubMed] [Google Scholar]
- (12).Braun LR, Fisk WA, Lev-Tov H, Kirsner RS, Isseroff RR. Diabetic foot ulcer: an evidence-based treatment update. Am J Clin Dermatol. 2014; 15(3):267–81. [DOI] [PubMed] [Google Scholar]
- (13).Morona JK, Buckley ES, Jones S, Reddin EA, Merlin TL. Comparison of the clinical effectiveness of different off-loading devices for the treatment of neuropathic foot ulcers in patients with diabetes: a systematic review and meta-analysis. Diabetes Metab Res Rev. 2013; 29(3):183–93. [DOI] [PubMed] [Google Scholar]
- (14).Armstrong DG, Isaac AL, Bevilacqua NJ, Wu SC. Offloading foot wounds in people with diabetes. Wounds. 2014; 26(1):13–20. [Google Scholar]
- (15).Miller J, Armstrong DG. Offloading the diabetic and ischemic foot: solutions for the vascular specialist. Semin Vasc Surg. 2014; 27(1):68–74. [DOI] [PubMed] [Google Scholar]
- (16).Lavery LA, Higgins KR, La Fontaine J, Zamorano RG, Constantinides GP, Kim PJ. Randomised clinical trial to compare total contact casts, healing sandals and a shear-reducing removable boot to heal diabetic foot ulcers. Int Wound J. 2015; 12(6):710–5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- (17).Greenhagen R. Complications of total contact casting. Podiatry Manage. 2012; 31(5):153–8. [Google Scholar]
- (18).Canadian Agency for Drugs and Technologies in Health. Removable off-loading devices for diabetic foot ulcers: a review of clinical and cost-effectiveness. [Internet]. Ottawa: CADTH; 2014. [cited 2015 Nov 23]. Available from: https://www.cadth.ca/sites/default/files/pdf/htis/dec-2014/RC0579-003%20Diabetic%20Foot%20Ulcers%20Final.pdf [Google Scholar]
- (19).Health Quality Ontario. Quality standards. Diabetic foot ulcers: care for patients in all settings [Internet]. Toronto (ON): Queen's Printer for Ontario. In press. [Google Scholar]
- (20).Botros M, Goettl K, Parsons L, Mendzildzic S, Morin C, Smith T, et al. Best practice recommendations for the prevention, diagnosis, and treatment of diabetic foot ulcers: update 2010. Wound Care Canada. 2010; 8(4):6–40. [Google Scholar]
- (21).McGowan J, Sampson M, Salzwedel DM, Cogo E, Foerster V, Lefebvre C. PRESS Peer Review of Electronic Search Strategies: 2015 Guideline Statement. J Clin Epidemiol. 2016; 75:40–6. [DOI] [PubMed] [Google Scholar]
- (22).O'Neill J, Tabish H, Welch V, Petticrew M, Pottie K, Clarke M, et al. Applying an equity lens to interventions: using PROGRESS ensures consideration of socially stratifying factors to illuminate inequities in health. J Clin Epidemiol. 2014; 67(1):56–64. [DOI] [PubMed] [Google Scholar]
- (23).Rao SR, Schoenfeld DA. Survival methods. Circulation. 2007; 115(1):109–13. [DOI] [PubMed] [Google Scholar]
- (24).Review Manager (RevMan) [computer program]. Version 5.3. Copenhagen, Denmark: The Nordic Cochrane Centre, The Cochrane Collaboration; 2014. [Google Scholar]
- (25).Higgins JP, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med. 2002; 21(11):1539–58. [DOI] [PubMed] [Google Scholar]
- (26).Guyatt GH, Oxman AD, Schunemann HJ, Tugwell P, Knottnerus A. GRADE guidelines: a new series of articles in the Journal of Clinical Epidemiology. J Clin Epidemiol. 2011; 64(4):380–2. [DOI] [PubMed] [Google Scholar]
- (27).Higgins JP, Altman DG, Sterne JA. Assessing risk of bias in included studies. In: Higgins JPT, Green S. (editors). Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 [Internet]. The Cochrane Collaboration, 2011. [updated 2011 Mar; cited 2017 Jan 19]. Available from www.handbook.cochrane.org. [Google Scholar]
- (28).Piaggesi A, Goretti C, Iacopi E, Clerici G, Romagnoli F, Toscanella F, et al. Comparison of removable and irremovable walking boot to total contact casting in offloading the neuropathic diabetic foot ulceration. Foot Ankle Int. 2016; 37(8):855–61. [DOI] [PubMed] [Google Scholar]
- (29).Piaggesi A, Macchiarini S, Rizzo L, Palumbo F, Tedeschi A, Nobili LA, et al. An off-the-shelf instant contact casting device for the management of diabetic foot ulcers: a randomized prospective trial versus traditional fiberglass cast. Diabetes Care. 2007; 30(3):586–90. [DOI] [PubMed] [Google Scholar]
- (30).Najafi B, Grewal GS, Bharara M, Menzies R, Talal TK, Armstrong DG. Can't stand the pressure: the association between unprotected standing, walking, and wound healing in people with diabetes. J Diabetes Sci Technol [Internet]. Forthcoming 2016. [DOI] [PMC free article] [PubMed]
- (31).Caravaggi C, Faglia E, De Giglio R, Mantero M, Quarantiello A, Sommariva E, et al. Effectiveness and safety of a nonremovable fiberglass off-bearing cast versus a therapeutic shoe in the treatment of neuropathic foot ulcers. Diabetes Care. 2000; 23(12):1746–51. [DOI] [PubMed] [Google Scholar]
- (32).Caravaggi C, Sganzaroli A, Fabbi M, Cavaiani P, Pogliaghi I, Ferraresi R, et al. Nonwindowed nonremovable fiberglass off-loading cast versus removable pneumatic cast (AircastXP Diabetic Walker) in the treatment of neuropathic noninfected plantar ulcers: a randomized prospective trial. Diabetes Care. 2007; 30(10):2577–8. [DOI] [PubMed] [Google Scholar]
- (33).Gutekunst DJ, Hastings MK, Bohnert KL, Strube MJ, Sinacore DR. Removable cast walker boots yield greater forefoot off-loading than total contact casts. Clin Biomech (Bristol, Avon). 2011; 26(6):649–54. [DOI] [PMC free article] [PubMed] [Google Scholar]
- (34).Faglia E, Caravaggi C, Clerici G, Sganzaroli A, Curci V, Vailati W, et al. Effectiveness of removable walker cast versus nonremovable fiberglass off-bearing cast in the healing of diabetic plantar foot ulcer: a randomized controlled trial. Diabetes Care. 2010; 33(7):1419–23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- (35).Van De Weg FB, Van Der Windt DAWM, Vahl AC. Wound healing: total contact cast vs. custom-made temporary footwear for patients with diabetic foot ulceration. Prosthet Orthot Int. 2008; 32(1):3–11. [DOI] [PubMed] [Google Scholar]
- (36).Katz IA, Harlan A, Miranda-Palma B, Prieto-Sanchez L, Armstrong DG, Bowker JH, et al. A randomized trial of two irremovable off-loading devices in the management of plantar neuropathic diabetic foot ulcers. Diabetes Care. 2005; 28(3):555–9. [DOI] [PubMed] [Google Scholar]
- (37).Armstrong DG, Lavery LA, Wu S, Boulton AJM. Evaluation of removable and irremovable cast walkers in the healing of diabetic foot wounds: a randomized controlled trial. Diabetes Care. 2005; 28(3):551–4. [DOI] [PubMed] [Google Scholar]
- (38).Armstrong DG, Nguyen HC, Lavery LA, van Schie CH, Boulton AJ, Harkless LB. Offloading the diabetic foot wound: a randomized clinical trial. Diabetes Care. 2001; 24(6):1019–22. [DOI] [PubMed] [Google Scholar]
- (39).Mueller MJ, Diamond JE, Sinacore DR, Delitto A, Blair IVP, Drury DA, et al. Total contact casting in treatment of diabetic plantar ulcers. Controlled clinical trial. Diabetes Care. 1989; 12(6):384–8. [DOI] [PubMed] [Google Scholar]
- (40).Armstrong DG, Lavery LA, Wrobel JS, Vileikyte L. Quality of life in healing diabetic wounds: does the end justify the means? J Foot Ankle Surg. 2008; 47(4):278–82. [DOI] [PubMed] [Google Scholar]
- (41).Moher D, Liberati A, Tetzlaff J, Altman DG, Group tP. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009; 6(7):e1000097. [DOI] [PMC free article] [PubMed] [Google Scholar]
- (42).Lavery LA, Armstrong DG, Harkless LB. Classification of diabetic foot wounds. J Foot Ankle Surg. 1996; 35(6):528–31. [DOI] [PubMed] [Google Scholar]
- (43).Craig J, Shenton R, Smith A. Economic analysis of soft-heel casting for diabetic foot ulcer: prevention and treatment. J Wound Care. 2013; 22(1):44–8. [DOI] [PubMed] [Google Scholar]
- (44).Husereau D, Drummond M, Petrou S, Carswell C, Moher D, Greenberg D, et al. Consolidated Health Economic Evaluation Reporting Standards (CHEERS)-explanation and elaboration: a report of the ISPOR Health Economic Evaluation Publication Guidelines Good Reporting Practices Task Force. Value Health. 2013; 16(2):231–50. [DOI] [PubMed] [Google Scholar]
- (45).Canadian Diabetes Association. Impact of offloading devices on the cost of diabetic foot ulcers in Ontario [Internet]. Toronto (ON): The Association; 2015. [cited 2015 November]. Available from: http://www.diabetes.ca/getmedia/5109456e-8c0b-458f-b949-a5accd41513a/impact-of-offloading-devices-ontario.pdf.aspx [Google Scholar]
- (46).Ragnarson Tennvall G, Apelqvist J. Health-related quality of life in patients with diabetes mellitus and foot ulcers. J Diabetes Complications. 2000; 14(5):235–41. [DOI] [PubMed] [Google Scholar]
- (47).Ministry of Health and Long-Term Care. Schedule of benefits: physician services under the Health Insurance Act [Internet]. Toronto (ON): MOHLTC; 2015. [cited 2016 May 25]. Available from: http://www.health.gov.on.ca/en/pro/programs/ohip/sob/physserv/sob_master11062015.pdf [Google Scholar]
- (48).Hopkins RB, Burke N, Harlock J, Jegathisawaran J, Goeree R. Economic burden of illness associated with diabetic foot ulcers in Canada. BMC Health Serv Res. 2015; 15:13. [DOI] [PMC free article] [PubMed] [Google Scholar]
- (49).Woo KY, Botros M, Kuhnke J, Evans R, Alavi A. Best practices for the management of foot ulcers in people with diabetes. Adv Skin Wound Care. 2013; 26(11):512–24; quiz 225–6. [DOI] [PubMed] [Google Scholar]
- (50).Statistics Canada [Internet]. Ottawa (ON): Government of Canada; 2016. [updated 2016 May 3; cited 2016 May 11]. Available from: http://www.statcan.gc.ca/start-debut-eng.html [Google Scholar]
- (51).Barham L. Public and patient involvement at the UK National Institute for Health and Clinical Excellence. The patient. 2011; 4(1):1–10. [DOI] [PubMed] [Google Scholar]
- (52).Messina J, Grainger DL. A pilot study to identify areas for further improvements in patient and public involvement in health technology assessments for medicines. The patient. 2012; 5(3):199–211. [DOI] [PubMed] [Google Scholar]
- (53).OHTAC Public Engagement Subcommittee. Public engagement for health technology assessment at Health Quality Ontario—final report from the Ontario Health Technology Advisory Committee Public Engagement Subcommittee [Internet]. Toronto (ON): Queen's Printer for Ontario; 2015. April [cited 2016. Available from: http://www.hqontario.ca/Portals/0/documents/evidence/special-reports/report-subcommittee-20150407-en.pdf [Google Scholar]
- (54).Tjornhoj-Thomsen T, Hansen HP. Knowledge in health technology assessment: who, what, how? Int J Technol Assess Health Care. 2011; 27(4):324–9. [DOI] [PubMed] [Google Scholar]
- (55).Rowe G, Frewer LJ. A typology of public engagement mechanisms. Sci Technol Hum Val. 2005; 30(2):251–90. [Google Scholar]
- (56).Brundisini F, Giacomini M, DeJean D, Vanstone M, Winsor S, Smith A. Chronic disease patients' experiences with accessing health care in rural and remote areas: a systematic review and qualitative meta-synthesis. Ontario health technology assessment series. 2013; 13(15):1–33. [PMC free article] [PubMed] [Google Scholar]
- (57).Kvale S. Interviews: an introduction to qualitative research interviewing. Thousand Oaks (CA): Sage; 1996. [Google Scholar]
- (58).Kuzel AJ. Sampling in qualitative inquiry. In: Miller WL, Crabtree BF, editors. Doing qualitative research. Thousand Oaks (CA): Sage Publications; 1999. p. 33–45. [Google Scholar]
- (59).Morse J. Emerging from the data: cognitive processes of analysis in qualitative research. In: Morse J, editor. Critical issues in qualitative research methods Thousand Oaks (CA): Sage Publications; 1994. p. 23–41. [Google Scholar]
- (60).Patton MQ. Qualitative research and evaluation methods. 3rd ed. Thousand Oaks (CA): Sage Publications; 2002. [Google Scholar]
- (61).Strauss AL, Corbin JM. Basics of qualitative research: techniques and procedures of developing a grounded theory. 2nd ed. Thousand Oaks (CA): Sage Publications; 1998. [Google Scholar]
- (62).Health Technology Assessment International Interest Group on Patient and Citizen Involvement in HTA. Introduction to health technology assessment (HTA) [Internet]. Edmonton (AB): Health Technology Assessment International; 2015. [cited 2016. Available from: http://www.htai.org/fileadmin/HTAi_Files/ISG/PatientInvolvement/v2_files/Resource/PCISG-Resource-Intro_to_HTA__KFacey__Jun13.pdf [Google Scholar]
- (63).Strauss AL, Corbin JM. Grounded theory research: procedures, canons, and evaluative criteria. Qual Sociol. 1990; 13(1):3–21. [Google Scholar]
- (64).Strauss AL, Corbin JM. Grounded theory methodology: an overview. In: Denzin NK, Lincoln YS, editors. Handbook of qualitative research. Thousand Oaks (CA): Sage; 1994. p. 273–85. [Google Scholar]
- (65).Wagner FW., Jr The dysvascular foot: a system for diagnosis and treatment. Foot Ankle. 1981; 2(2):64–122. [DOI] [PubMed] [Google Scholar]