Abstract
Objectives
This umbrella review aimed to identify the current evidence on health education-related interventions for patients with acute coronary syndrome (ACS) or type two diabetes mellitus (T2DM); identify the educational content, delivery methods, intensity, duration and setting required. The purpose was to provide recommendations for educational interventions for high-risk patients with both ACS and T2DM.
Design
Umbrella review of systematic reviews and meta-analyses.
Setting
Inpatient and postdischarge settings.
Participants
Patients with ACS and T2DM.
Data sources
CINAHL, Cochrane Library, Joanna Briggs Institute, Journals@Ovid, EMBase, Medline, PubMed and Web of Science databases from January 2000 through May 2016.
Outcomes measures
Clinical outcomes (such as glycated haemoglobin), behavioural outcomes (such as smoking), psychosocial outcomes (such as anxiety) and medical service use.
Results
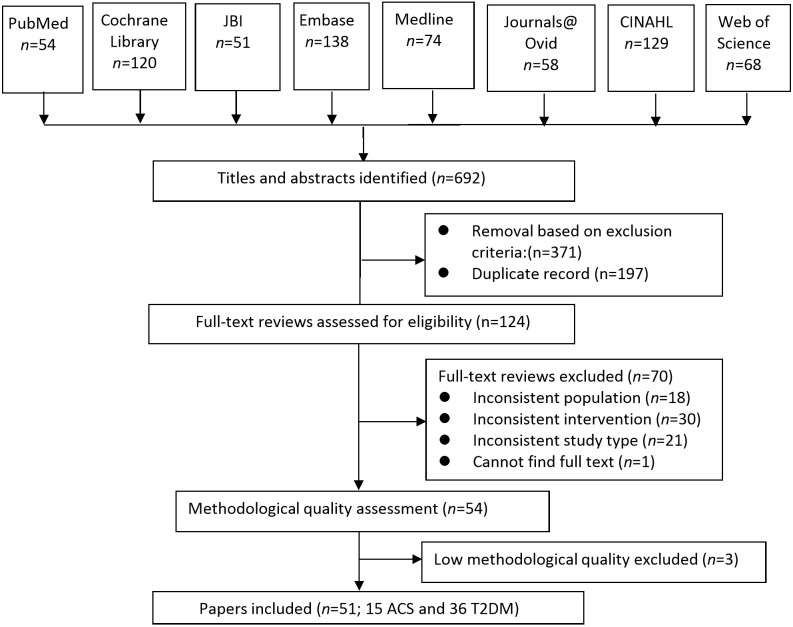
Fifty-one eligible reviews (15 for ACS and 36 for T2DM) consisting of 1324 relevant studies involving 2 88 057 patients (15 papers did not provide the total sample); 30 (58.8%) reviews were rated as high quality. Nurses only and multidisciplinary teams were the most frequent professionals to provide education, and most educational interventions were delivered postdischarge. Face-to-face sessions were the most common delivery formats, and many education sessions were also delivered by telephone or via web contact. The frequency of educational sessions was weekly or monthly, and an average of 3.7 topics was covered per education session. Psychoeducational interventions were generally effective at reducing smoking and admissions for patients with ACS. Culturally appropriate health education, self-management educational interventions, group medical visits and psychoeducational interventions were generally effective for patients with T2DM.
Conclusions
Results indicate that there is a body of current evidence about the efficacy of health education, its content and delivery methods for patients with ACS or T2DM. These results provide recommendations about the content for, and approach to, health education intervention for these high-risk patients.
Keywords: health education, acute coronary syndrome, type 2 diabetes mellitus, umbrella review
Strengths and limitations of this study.
This umbrella review is the first synthesis of systematic reviews or meta-analyses to consider health education-related interventions for patients with acute coronary syndrome (ACS) or type two diabetes mellitus (T2DM).
These results provide recommendations about the content of a health education intervention for patients with ACS and T2DM.
The diversity of the educational interventions seen in the reviews included in this umbrella review may reflect the uncertainty about the optimal strategy for providing health education to patients.
This umbrella review found no reviews focused on patients with ACS and T2DM—the intended target group; instead, all of the systematic reviews and meta-analyses focused on only one of these two diseases.
Introduction
Acute coronary syndrome (ACS) is the leading cause of death worldwide. The risk of high mortality rates relating to ACS is markedly increased after an initial cardiac ischaemic event.1 Globally, 7.2 million (13%) deaths are caused by coronary artery disease (CAD),2 and it is estimated that >7 80 000 persons will experience ACS each year in the USA.3 Moreover, about 20%–25% of patients with ACS reportedly also have diabetes mellitus (DM); predominantly type two diabetes mellitus (T2DM)).4 5 Patients with ACS and DM have an increased risk of adverse outcomes such as death, recurrent myocardial infarction (MI), readmission or heart failure during follow-up.6 Longer median delay times from symptom onset to hospital presentation, have been reported among patients with ACS and DM than patients with ACS alone.7
DM is now considered to confer a risk equivalent to that of CAD for patients for future MI and cardiovascular mortality.8 Mortality was significantly higher among patients with ACS and DM than among patients with ACS only following either ST segment elevation myocardial infarction (STEMI) (8.5% (ACS and DM) vs 5.4% (ACS)) or unstable angina/non-STEMI (NSTEMI) (2.1% (ACS and DM) vs 1.1% (ACS)).9 ACS and T2DM are often associated with high-risk factors such as low levels of physical exercise, obesity, smoking and unhealthy diet.10 Some of these and other risk factors, specifically glycaemia, high blood pressure (BP), lipidaemia and obesity, are frequently addressed by health education interventions.10
Health education interventions are comprehensive programmes that healthcare providers deliver to patients aimed at improving patients’ clinical outcomes through the increase and maintenance of health behaviours.11 Along with education about, for example, medication taking, these programmes seek to increase behaviours such as physical exercise and a healthy diet thus reducing patient morbidity or mortality.11 Most diabetes education is provided through programmes within outpatient services or physicians’ practices.12 Many recent education programmes have been designed to meet national or international education standards13–15 with diabetes education being individualised to consider patients’ existing needs and health conditions.16 Patients with T2DM have reported feelings of hopelessness and fatigue with low levels of self-efficacy, after experiencing an acute coronary episode.17
Although there are numerous systematic reviews of educational interventions relating to ACS or T2DM, an umbrella review providing direction on educational interventions for high-risk patients with both ACS and T2DM is not available, indicating a need to gather the current evidence and develop an optimal protocol for health education programmes for patients with ACS and T2DM. This umbrella review will examine the best available evidence on health education-related interventions for patients with ACS or T2DM. We will synthesise these findings to provide direction for health education-related interventions for high-risk patients with both ACS and T2DM.
An umbrella review is a new method to summarise and synthesise the evidence from multiple systematic reviews/meta-analyses into one accessible publication.18 Our aim is to systematically gather, evaluate and organise the current evidence relating the health education interventions for patients with ACS or T2DM, and proffer recommendations for the scope of educational content and delivery methods that would be suitable for patients with ACS and T2DM.
Methods
Data sources
This umbrella review performed a literature search to identify systematic reviews and meta-analyses examining health education-related interventions for patients with ACS or T2DM. The search strategies are described in online supplementary appendix 1. This umbrella review searched eight databases for articles published from January 2000 to May 2016: CINAHL, Cochrane Library, Joanna Briggs Institute, Journals@Ovid, EMBase, Medline, PubMed and Web of Science. The search was limited to English language only. The following broad MeSH terms were used: acute coronary syndrome; angina, unstable; angina pectoris; coronary artery disease; coronary artery bypass; myocardial infarction; diabetes mellitus, type two; counseling; health education; patient education as topic; meta-analysis (publication type); and meta-analysis as a topic.
bmjopen-2017-016857supp001.pdf (5.1MB, pdf)
Inclusion criteria
Participants
All participants were diagnosed with ACS or T2DM using valid, established diagnostic criteria. The diagnostic standards included those described by the American College of Cardiology or American Heart Association,3 National Heart Foundation of Australia and Cardiac Society of Australia and New Zealand,19 WHO20 or other associations.
Intervention types
For this umbrella review, health education-related interventions refer to any planned activities or programmes that include behaviour modification, counselling and teaching interventions. Results considered for this review included changes in clinical outcomes (including BP levels, body weight, diabetes complications, glycated haemoglobin (HbA1c), lipid levels, mortality rate and physical activity levels), behavioural outcomes (such as diet, knowledge, self-management skills, self-efficacy and smoking), psychosocial outcomes (such as anxiety, depression, quality of life and stress) and medical service use (such as medication use, healthcare utilisation and cost-effectiveness) for patients with ACS or T2DM. These activities or programmes included any educational interventions delivered to patients with ACS or T2DM. The interventions are delivered in any format, including face-to-face, telephone and group-based or one-on-one, and the settings include community, hospital and home. The interventions were delivered by nurses (including diabetes nurse educators), physicians, community healthcare workers, dietitians, lay people, rehabilitation therapists or multidisciplinary teams.
Study types
Only systematic reviews and meta-analyses were included in this review.
Eligibility assessment
The title and abstract of all of the retrieved articles were assessed independently by two reviewers (XL-L, YS) based on the inclusion criteria. All duplicate articles were identified within EndNote V.X721 and subsequently excluded. If the information from the titles and abstract was not clear, the full articles were retrieved. The decision to include an article was based on an appraisal of the full text of all retrieved articles. Any disagreements during this process were settled by discussion and, if necessary, consensus was sought with a third reviewer. We developed an assessment form in which specific reasons for exclusion were detailed.
Assessment of methodological quality
The methodological quality and risk of bias were assessed for each of the included publications using the Assessment of Multiple Systematic Reviews (AMSTAR),22 independently by the same two reviewers (see table 1). The AMSTAR is an 11-item tool, with each item provided a score of 1 (specific criterion is met) or 0 (specific criterion is not met, unclear or not applicable).22 23 An overall score for the review methodological quality is then calculated as the sum of the individual item scores: high quality, 8–11; medium quality, 4–7 or low quality, 0–3.23 If the required data were not available in the article, the original authors were contacted for more information. The low quality reviews (AMSTAR scale: 0–3) were excluded in this umbrella review.
Table 1.
Methodological quality assessment of included systematic reviews and meta-analyses
| Systematic review/ meta-analysis |
Item 1 | Item 2 | Item 3 | Item 4 | Item 5 | Item 6 | Item 7 | Item 8 | Item 9 | Item 10 | Item 11 | Total score | |
| Systematic reviews and meta-analysis involved patients with ACS | |||||||||||||
| 1 | Barth et al69 | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | 11 |
| 2 | Devi et al44 | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | NA | Yes | 10 |
| 3 | Ghisi et al50 | CA | Yes | Yes | Yes | No | Yes | Yes | Yes | Yes | No | No | 7 |
| 4 | Kotb et al59 | CA | Yes | Yes | Yes | No | Yes | Yes | Yes | Yes | No | Yes | 8 |
| 5 | Brown et al37 | Yes | No | Yes | CA | No | Yes | Yes | Yes | Yes | NA | Yes | 7 |
| 6 | Dickens et al45 | CA | Yes | Yes | CA | No | Yes | Yes | Yes | Yes | Yes | Yes | 8 |
| 7 | Aldcroft et al31 | CA | No | Yes | CA | NO | Yes | Yes | Yes | Yes | No | Yes | 6 |
| 8 | Brown et al70 | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | NA | Yes | 10 |
| 9 | Huttunen-Lenz et al56 | CA | No | Yes | CA | No | Yes | Yes | Yes | Yes | No | No | 5 |
| 10 | Goulding et al51 | Yes | Yes | Yes | CA | No | Yes | Yes | Yes | Yes | No | Yes | 8 |
| 11 | Auer et al34 | CA | Yes | Yes | CA | No | No | Yes | No | Yes | Yes | No | 5 |
| 12 | Barth et al36 | Yes | Yes | Yes | No | Yes | Yes | Yes | Yes | Yes | Yes | Yes | 10 |
| 13 | Fernandez et al48 | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | No | No | 8 |
| 14 | Barth et al35 | CA | Yes | Yes | CA | No | Yes | CA | Yes | Yes | Yes | Yes | 7 |
| 15 | Clark et al41 | CA | Yes | Yes | CA | No | Yes | Yes | Yes | Yes | Yes | Yes | 8 |
| Systematic reviews and meta-analysis involved patients with T2DM | |||||||||||||
| 16 | Choi et al40 | CA | Yes | Yes | No | No | Yes | Yes | Yes | Yes | Yes | Yes | 8 |
| 17 | Creamer et al42 | Yes | Yes | Yes | CA | No | Yes | Yes | Yes | Yes | No | Yes | 8 |
| 18 | Huang et al55 | CA | CA | Yes | CA | No | Yes | Yes | Yes | Yes | Yes | Yes | 7 |
| 19 | Chen et al39 | CA | CA | Yes | CA | No | Yes | Yes | Yes | Yes | Yes | Yes | 7 |
| 20 | Pillay et al71 | Yes | No | Yes | Yes | No | Yes | Yes | Yes | Yes | Yes | Yes | 9 |
| 21 | Terranova et al72 | CA | CA | Yes | No | Yes | Yes | Yes | Yes | Yes | Yes | Yes | 8 |
| 22 | Attridge et al33 | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | No | Yes | 10 |
| 23 | Odnoletkova et al66 | Yes | CA | Yes | CA | No | No | Yes | Yes | Yes | Yes | No | 6 |
| 24 | Pal et al67 | CA | Yes | Yes | Yes | No | Yes | Yes | Yes | Yes | No | Yes | 8 |
| 25 | Ricci-Cabello et al73 | Yes | CA | Yes | Yes | No | Yes | Yes | Yes | Yes | Yes | Yes | 9 |
| 26 | Saffari et al74 | CA | Yes | Yes | CA | No | Yes | Yes | Yes | Yes | Yes | Yes | 8 |
| 27 | Gucciardi et al52 | CA | Yes | Yes | No | No | Yes | Yes | Yes | Yes | No | Yes | 7 |
| 28 | Pal et al68 | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | No | Yes | 10 |
| 29 | van Vugt et al75 | CA | Yes | Yes | CA | No | Yes | Yes | Yes | NA | No | Yes | 6 |
| 30 | Amaeshi32 | CA | CA | Yes | No | No | Yes | Yes | Yes | NA | No | No | 4 |
| 31 | Nam et al62 | CA | CA | Yes | Yes | No | Yes | Yes | Yes | Yes | Yes | Yes | 8 |
| 32 | Steinsbekk et al76 | CA | Yes | Yes | CA | No | Yes | Yes | Yes | Yes | No | Yes | 7 |
| 33 | Burke et al38 | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | NA | Yes | 10 |
| 34 | Lun Gan et al57 | Yes | Yes | Yes | CA | No | Yes | Yes | Yes | Yes | No | Yes | 8 |
| 35 | Ramadas et al77 | CA | CA | Yes | No | No | Yes | Yes | Yes | NA | No | Yes | 5 |
| 36 | Hawthorne et al54 | Yes | Yes | Yes | CA | No | Yes | Yes | Yes | Yes | CA | Yes | 8 |
| 37 | Minet et al61 | Yes | Yes | Yes | No | No | Yes | Yes | Yes | Yes | Yes | Yes | 9 |
| 38 | Alam et al30 | Yes | Yes | No | CA | No | Yes | Yes | Yes | Yes | Yes | Yes | 8 |
| 39 | Duke et al46 | Yes | CA | Yes | No | Yes | Yes | Yes | Yes | Yes | No | Yes | 8 |
| 40 | Fan and Sidani47 | Yes | No | Yes | CA | No | Yes | No | No | Yes | No | Yes | 5 |
| 41 | Hawthorne et al53 | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | 11 |
| 42 | Khunti et al58 | CA | Yes | Yes | Yes | No | Yes | No | No | No | No | Yes | 5 |
| 43 | Loveman et al60 | Yes | CA | Yes | Yes | No | Yes | Yes | Yes | Yes | No | Yes | 8 |
| 44 | Wens et al78 | CA | Yes | Yes | CA | No | Yes | Yes | Yes | Yes | NA | Yes | 7 |
| 45 | Nield et al63 | Yes | Yes | Yes | CA | Yes | Yes | Yes | Yes | Yes | No | Yes | 9 |
| 46 | Zabaleta and Forbes79 | CA | CA | Yes | CA | Yes | Yes | Yes | Yes | NA | No | No | 5 |
| 47 | Deakin et al43 | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | 11 |
| 48 | Vermeire et al80 | Yes | Yes | Yes | CA | Yes | Yes | Yes | Yes | Yes | No | Yes | 9 |
| 49 | Gary et al49 | CA | Yes | No | Yes | No | Yes | Yes | No | Yes | No | Yes | 6 |
| 50 | Norris et al65 | CA | No | Yes | No | No | Yes | Yes | Yes | CA | No | No | 4 |
| 51 | Norris et al64 | CA | Yes | Yes | CA | No | Yes | Yes | Yes | NA | No | No | 5 |
Item 1: ‘Was an "a priori" design provided?’,Source:Shea et al22; Item 2: ‘Was there duplicate study selection and data extraction?’; Item 3: ‘Was a comprehensive literature search performed?’; Item 4: ‘Was the status of publication (ie, grey literature) used as an inclusion criterion?’; Item 5: ‘Was a list of studies (included and excluded) provided?’; Item 6: ‘Were the characteristics of the included studies provided?’; Item 7: ‘Was the scientific quality of the included studies assessed and documented?’; Item 8: ‘Was the scientific quality of the included studies used appropriately in formulating conclusions?’; Item 9: ‘Were the methods used to combine the findings of studies appropriate?’; Item 10: ‘Was the likelihood of publication bias assessed?’; Item 11: ‘Was the conflict of interest stated?’
CA, cannot answer; NA, not applicable.
Data extraction
Data were independently extracted by two reviewers using a predefined data extraction form. For missing or unclear information, the primary authors were contacted for clarification.
Statistical presentation of results from reviews
All of the results were extracted for each included systematic review or meta-analysis, and the overall effect estimates are presented in a tabular form. The number of systematic reviews or meta-analyses that reported the outcome, total sample (from included publications) and information of health education interventions is also presented in tables 2 and 3.24 A final ‘summary of evidence’ was developed to present the intervention, included study synthesis, and indication of the findings from the included papers (table 4).24 This umbrella review calculated the corrected covered area (CCA) (see online supplementary appendices 2 and 3). The CCA statistic is a measure of overlap of trials (the repeated inclusion of the same trial in subsequent systematic reviews included in an umbrella systematic review). A detailed description of the calculation is provided by the authors who note slight CCA as 0%–5%, moderate CCA as 6%–10%, high CCA as 11%–15% and very high CCA is >15%.25 The lower the CCA the lower the likelihood of overlap of trials included in the umbrella review.
Table 2.
Characteristics and interventions of included systematic reviews and meta-analysis involved patients with ACS
| First author, year; journal | Primary objectives (to assess effect of interventions on….) |
Studies details | Intervention |
Outcomes
(primary outcomes were in bold) ‘−': No change ‘↑': Increase ‘↓': Decrease |
Synthesis methods | |||||
| Educational content | Provider | Number of session(s), delivery mode, time, setting | ||||||||
| Devi, 201544; The Cochrane Library | Lifestyle changes and medicines management |
Number of studies: 11 completed trials (12 publications); Types of studies: RCTs; Total sample: 1392 participants |
All internet-based interventions |
√ BEHA (-) √ CVR (-) √ DIET (-) √ EXERCISE (-) □ MED √ PSY(-) √ SMOKING (-) □ SELF |
Dietitians; exercise specialists; nurse practitioners; physiotherapist rehabilitation specialists, or did not describe. |
Number of session: weekly or monthly or unclear; Total contact hours: unclear. Duration: from 6 weeks to 1 year |
Strategies: internet-based and mobile phone-based intervention, such as email access, private-messaging function on the website, one-to-one chat facility, a synchronised group chat, an online discussion forum, or telephone consultations; or video files; Format: one-on-one chat sessions; ‘ask an expert’ group chat sessions; Theoretical approach: unclear |
Inpatient settings, postdischarge, other |
− Clinical outcomes; − Cardiovascular risk factors;
− Lifestyle changes; − Compliance with medication; − Healthcare utilisation and costs; ↓ Adverse intervention effects |
Meta-analysis used Review Manager software |
| Barth, 201569; The Cochrane Library | Smoking cessation |
Number of studies:40 RCTs; Types of studies: RCTs; Total sample: 7928 participants |
Psychosocial smoking cessation interventions | □ BEHA □ CVR □ DIET □ EXERCISE □ MED □ PSY √ SMOKING □ SELF |
Cardiologist; general practitioner physician or study nurse |
Number of session: weekly or 2–3 times per week; Total contact hours: unclear. Duration: from 8 weeks to 1 year |
Strategies: face-to-face, telephone contact, written educational materials, videotape, booklet or unclear; Format: one by one counselling; telephone call; group meetings or unclear; Theoretical approach: TTM, SCT |
Inpatient settings, postdischarge, other | ↑ Abstinence by self-report or validated | Meta- analysis used Review Manager software |
| Kotb, 201459; PLoS One | Patients’ outcomes |
Number of studies: 26 studies; Types of studies: RCTs; Total sample: 4081 participants |
Telephone-delivered postdischarge interventions | □ BEHA √ CVR □ DIET □ EXERCISE □ MED □ PSY □ SMOKING □ SELF |
Dietitians; exercise specialist; health educators; nurses and pharmacists |
Number of session: 3–6 sessions/telephone calls and was greater than six calls in five studies; or unclear; Total contact hours: 40 –180 mins or unclear; Duration: 1.5–6 months or unclear |
Strategies: telephone calls; Format: unclear, did not describe the format; Theoretical approach: unclear |
Unclear, did not describe the setting |
↓ All-cause hospitalisation;
− All-cause mortality; ↓ Depression; − Anxiety; ↑ Smoking cessation, ↓ Systolic blood pressure; − LDL-c |
Meta- analysis used Review Manager software |
| Ghisi, 201450; Patient Education and Counseling | Knowledge, health behaviour change, medication adherence, psychosocial well-being |
Number of studies: 42 articles; Types of studies: 30 were experimental: 23 RCTs and 7 quasi-experimental; and 11 observational and 1 used a mixed-methods design. Total sample: 16 079 participants |
Any educational interventions |
√ BEHA (+) √ CVR (++) √ DIET (+++) √ EXERCISE (++) √ MED (++) √ PSY(++) √ SMOKING (+) □ SELF |
Nurses (35.7%), a multidisciplinary team (31%), dietitians (14.3%) and a cardiologist (2.4%) |
Number of session: 1–24 or unclear. Total contact hours: 5–10 min to 3 hours as well as a full day of education Duration: 1–24 month; from daily education to every 6 months |
Strategies: did not describe the strategies; Format: group (88.1%) education was delivered by lectures (40.5%), group discussions (40.5%) and question and answer periods (7.1%). Individual education (88.1%), including individual counselling (50%), follow-up telephone contacts (31%) and home visits (7.1%); Theoretical approach: unclear |
Inpatient settings |
− Knowledge;
− Behaviour; − Psychosocial indicators |
Narrative synthesis |
| Brown, 201337; European Journal of Preventive Cardiology | Mortality, morbidity, HRQoL and healthcare costs |
Number of studies: 24 papers reporting on 13 RCTs; Types of studies: RCTs; Total sample: 68 556 participants |
Patient education | □ BEHA √ CVR □ DIET □ EXERCISE □ MED □ PSY □ SMOKING □ SELF |
Nurses or other healthcare professionals. |
Number of session and duration: from a total of 2 visits to a 4 -week residential stay reinforced with 11 months of nurse led follow-up Total contact hours: unclear |
Strategies: face-to-face education sessions, telephone contact and interactive use of the internet; Format: group-based sessions, individualised education and four used a mixture of both sessions; Theoretical approach: unclear |
Inpatient settings, other |
− Mortality,
− Non-fatal MI, − Revascularisations, − Hospitalisations, − HRQoL, − Withdrawals/dropouts; − Healthcare utilisation and costs |
Meta- analysis used Review Manager software |
| Dickens, 201345; Psychosomatic Medicine | Depression and depressive symptoms |
Number of studies: 62 independent studies Types of studies: RCTs; Total sample: 17 397 |
Psychological interventions |
√ BEHA (-) □ CVR □ DIET □ EXERCISE □ MED √ PSY (-) □ SMOKING √ SELF (-) |
A single health professional or by a unidisciplinary team |
Number of session: 14.4 (range, 1–156); Total contact hours: varying from 10 to 240 min Duration: unclear |
Strategies: face-to-face sessions, telephone contact or unclear; Format: group or unclear; Theoretical approach: unclear |
Unclear, did not describe |
↓ Depression;
− Adverse cardiac outcomes; − Ongoing cardiac symptoms |
Univariate analyses using comprehensive meta-analysis, multivariate meta-regression using SPSS V.15.0 |
| Aldcroft, 201120; Journal of Cardiopulmonary Rehabilitation & Prevention | Health behaviour change |
Number of studies: seven trials Types of studies: six randomised controlled trials and a quasi-experimental trial Total sample: 536 participants |
All psychoeducational or behavioural intervention | □ BEHA √ CVR (-) □ DIET □ EXERCISE □ MED √ PSY (-) □ SMOKING □ SELF |
Appropriately trained healthcare workers |
Number of session: unclear; Total contact hours: unclear; Duration: 2–12 months |
Strategies: did not describe the strategies; Format: group setting, combination of group and one-on-one education and one-on-one format only; Theoretical approach: TTM, interactionist role theory, Bandura’s self-efficacy theory, Gordon’s relapse prevention model and a cognitive behavioural approach |
Unclear, did not describe |
↓ Smoking rates; medication use;
− Supplemental oxygen use; ↑ Physical activity; ↑ Nutritional habits |
Meta-analysis and narrative presentation |
| Brown, 201170; The Cochrane Library | Mortality, morbidity, HRQoL and healthcare costs |
Number of studies: 24 papers reporting on 13 studies. Types of studies: RCTs; Total sample: 68 556 participants |
Patient education |
√ BEHA (-) √ CVR (-) □ DIET √ EXERCISE (-) √ MED □ PSY □ SMOKING □ SELF |
Nurse or did not describe |
Number of session and duration: two visits to 4 weeks residential 11 months of nurse led follow-up Total contact hours: unclear |
Strategies: face-to-face sessions, telephone contact and interactive use of the internet; Format: four studies involved group sessions, five involved individualised education and three used both session types, with one study comparing the two approaches; Theoretical approach: did not describe |
Postdischarge, other |
− Total mortality;
− Cardiovascular − mortality; − Non-cardiovascular mortality; − Total cardiovascular (CV) events; − Fatal and/or non-fatal MI; − Other fatal and/or non-fatal CV events |
Meta-analysis used Review Manager software |
| Goulding, 201051; Journal of Advanced Nursing | Change maladaptive illness |
Number of studies: 13 studies;
Types of studies: RCTs; Total sample: unclear |
Interventions to change maladaptive illness beliefs |
√ BEHA (-) □ CVR DIET □ EXERCISE □ MED √ PSY (-) □ SMOKING □ SELF |
Cardiologist, nurse, psychologist or did not describe. |
Number of session: unclear; Total contact hours: unclear; Duration: 4 days to 2 weeks or unclear |
Strategies: face-to-face sessions, telephone contact and written self-administered; Format: unclear; Theoretical approach: Common Sense Model, Leventhal’s framework |
Inpatient settings, postdischarge, other |
− Beliefs (or other illness cognition);
− QoL; − Behaviour; − Anxiety or depression; − Psychological well-being; − Modifiable risk factors; protective factors |
A descriptive data synthesis |
| Huttunen-Lenz, 201056; British Journal of Health Psychology | Smoking cessation |
Number of studies: a total of 14 studies were included Types of studies: RCTs; Total sample: 1792 participants |
Psychoeducational cardiac rehabilitation intervention | □ BEHA □ CVR □ DIET □ EXERCISE □ MED □ PSY √ SMOKING (-) □ SELF |
Cardiologist, nurse psychologist or did not describe |
Number of session: 4–20 or unclear. Total contact hours: 10–720 mins or unclear Duration: 4–29 weeks or unclear |
Strategies: face-to-face counselling, self-help materials; home visit, booklet, video and telephone contact Format: individual or unclear Theoretical approach: social learning theory; ASE model; TTM; behavioural multicomponent approach |
Inpatient settings, postdischarge, other |
↑ Prevalent smoking cessation,
↑ Continuous smoking cessation, − Mortality |
Subgroup meta-analysis was used software |
| Auer, 200834; Circulation | Multiple cardiovascular risk factors and all-cause mortality |
Number of studies: 27 articles reporting 26 studies Types of studies: 16 clinical controlled trials and 10 before-after studies Total sample: 2467 patients in CCTs and 38, 581 patients in before-after studies |
In-hospital multidimensional interventions of secondary prevention | □ BEHA □ CVR √ DIET (-) √ EXERCISE (-) √ MED √ PSY (-) √ SMOKING (-) □ SELF |
Cardiac nurses; physician, or did not describe |
Number of session: 1–5 or unclear; Total contact hours: 30–240 mins or unclear; Duration: 4 weeks–12 months |
Strategies: Written material; audiotapes; presentations; face-to-face; Format: group or unclear; Theoretical approach: unclear |
Inpatient settings |
↓ All-cause mortality;
↓ Readmission rates; − Reinfarction rates |
Stata V.9.1 |
| Barth, 200836; The Cochrane Library |
Smoking cessation |
Number of studies: 40 trials; Types of studies: RCTs; Total sample: 7682 patients |
Psychosocial intervention |
√ BEHA (+++) √ CVR (++) □ DIET □ EXERCISE □ MED √ PSY (+) √ SMOKING (+++) √ SELF(+++) |
Cardiologist, nurse, physician or study nurse |
Number of session: 1–5 or unclear; Total contact hours: 15 mins–9 hours Duration: within 4 weeks or did not report on the duration |
Strategies: face-to-face; information booklets, audiotapes or videotapes Format: group sessions or individual counselling; Theoretical approach: TTM |
Inpatient settings | ↑ Abstinence by self-report or validated | Meta-analysis used Review Manager software |
| Fernandez, 200748; International Journal of Evidence-Based Healthcare | Risk factor modification |
Number of studies: 17 trials; Types of studies: randomised, quasi-RCTs and clustered trials; Total sample: 4725 participants |
Brief structured intervention |
√ BEHA (-) □√ CVR (-) □ DIET □ EXERCISE □ MED □ PSY □ SMOKING √ SELF (-) |
Case manager; dieticians; health educator; nurses; psychologist; and research assistants |
Number of session: supportive counselling ranged from 1 to 7 calls for the duration of the study; Total contact hours: varied from 10 to 30 mins; Duration: unclear |
Strategies: written, visual, audio, telephone contact; Format: did not describe; Theoretical approach: theoretical behaviour change principles |
Unclear, did not describe |
↓ Smoking;
− Cholesterol level; − Physical activity; ↑ Dietary habits; ↓ Blood sugar levels; − BP levels; ↓ BMI; − Incidence of admission |
Cochrane statistical package Review Manager |
| Barth, 200635; Annals of Behavioural Medicine | Smoking cessation |
Number of studies: 19 trials; Types of studies: RCTs; Total sample: 2548 patients |
Psychosocial interventions |
√ BEHA (+++) √ CVR (++) □ DIET □ EXERCISE □ MED □ PSY □ SMOKING √ SELF (+++) |
Unclear, did not describe |
Number of session: unclear; Total contact hours: unclear; Duration: unclear |
Strategies: face-to-face, telephone contact or unclear; Format: unclear; Theoretical approach: unclear |
Unclear, did not describe |
↑ Abstinence;
↓ Smoking status |
Data analyses were carried out in Review Manager V.4.2 |
| Clark, 200541; Annals of Internal Medicine | Mortality, MI |
Number of studies: 63 randomised trials; Types of studies: RCTs; Total sample: 21 295 patients |
Secondary prevention programmes | □ BEHA □ CVR √ DIET (-) √ EXERCISE (-) □ MED √ PSY (-) □ SMOKING □ SELF |
Nurse, multidisciplinary team or did not describe |
Number of session: 1–12 or unclear Total contact hours: did not describe Duration: 0.75–48 months |
Strategies: face-to-face, telephone contact and home visit; Format: group and individual or unclear; Theoretical approach: unclear |
Inpatient settings, postdischarge, other |
↓ Mortality,
↓ MI, − Hospitalisation rates |
Performed analyses by using Review Manager V.4.2 and Qualitative Data Synthesis |
Smoking, smoking cessation; CVR, cardiovascular risk factors; PSY, psychosocial issues (depression, anxiety); DIET, diet; EXERCISE, exercise; MED, medication; BEHA, behavioural charge (including lifestyle modification); SELF, self-management (including problems solving); DR, diabetes risks; CHD, coronary heart disease; CAD, coronary artery disease; CHW, community health worker; HbA1c, glycated haemoglobin; BP, blood pressure; LDL, low-density lipoprotein cholesterol; SMS, short message service; BCTs, behavioural change techniques; LEA, lower extremity amputation; PRIDE, Problem Identification, Researching one’s routine, Identifying a management goal, Developing a plan to reach it, Expressing one’s reactions and Establishing rewards for making progress; ASE, attitude social influence-efficacy; CVRF, cardiovascular risk factors; PA, physical activity; EDU, patient education; GP, general practice; RCTs, randomised controlled trials; CCTS, controlled clinical trials; HRQoL, health-related quality of life; QoL, quality of life; MI, myocardial infarction; CAD, coronary artery disease; CABG, coronary artery bypass graft surgery; BMI, body mass index; SBP, systolic blood pressure; DBP, diastolic blood pressure; HDL-c, high-density lipoprotein cholesterol; TTM, transtheoretical model; SCT, social cognitive theory; HBM, health belief model; SAT, social action theory.
In the educational content: ‘+’: minor focus; ‘++’:moderate focus; ‘+++’ major focus; ‘- ’=unclear what the intensity of the education was for any topic.
In the outcomes: arrow up (‘↑’) for improvement, arrow down (‘↓’) for reduction; a dash (‘−’) for no change or inconclusive evidence. Primary outcomes were in bold.
Table 3.
Characteristics and interventions of included systematic reviews and meta-analysis involved patients with T2DM
| First author, year; journal |
Primary objectives
(to assess effect of interventions on….) |
Studies details | Intervention |
Outcomes
(primary outcomes were in bold.) ‘−': No change ‘↑': Increase ‘↓': Decrease |
Synthesis methods | |||||
| Educational content | Provider | Number of session(s), delivery mode, time, setting | ||||||||
| Choi, 201640; Diabetes Research and Clinical Practice | Glycaemic effect |
Number of studies: 53 studies (5 in English, 48 in Chinese); Types of studies: RCTs; Total sample: unclear |
Diabetes education intervention | □ BEHA √ DIET (-) □ DR □ EXERCISE □ GC □ MED □ PSY □ SMOKING √ SELF (-) |
Unclear, did not describe |
Number of session: unclear; Total contact hours: unclear; Duration: 30–150 min or unclear |
Strategies: face-to-face, written materials; telephone contact and home visit; Format: unclear; Theoretical approach: unclear |
Inpatient settings, post discharge, other | ↓ HbA1cSTATA V.12 and Review Manager V.5.3 | |
| Creamer, 201642; Diabetic Medicine | Successful outcomes and to suggest directions for future research |
Number of studies: 33;
Types of studies: RCTs; Total sample: 7453 participants |
Culturally appropriate health education |
√ BEHA (-) √ DIET (-) √ DR (-) √ EXERCISE □ GC □ MED □ PSY □ SMOKING √ SELF (-) |
CHWs, clinical pharmacists dieticians, nurses, podiatrists, physiotherapists and psychologists |
Number of session: 1–10 or unclear; Total contact hours: unclear; Duration: from a single session to 24 months |
Strategies: face-to-face; phone contact; Format: group sessions (10 studies), individual sessions (13) or a combination of both; Theoretical approach: unclear |
Inpatient settings, postdischarge, other |
↓ HbA1c,
− HRQoL, − Adverse events, − BP, − BMI, − Lipid levels, − Diabetes complications, − Economic analyses, mortality and diabetes knowledge, − Empowerment, − Self-efficacy and satisfaction |
Meta-analysis using the Review Manager statistical programme |
| Huang, 201655; European Journal of Internal Medicine | Clinical markers of cardiovascular disease |
Number of studies: 17 studies; Types of studies: RCTs; Total sample: unclear |
Lifestyle interventions | □ BEHA √ DIET (-) √ CVR (-) √ EXERCISE (-) □ GC □ MED □ PSY □ SMOKING √ SELF (-) |
Nurse, pharmacist or unclear |
Number of session: unclear; Total contact hours: unclear; Duration: 6 months–8 years |
Strategies: unclear; Format: individual; group and mixed Theoretical approach: unclear |
Unclear, did not describe |
Cardiovascular risk factors such as, − BMI, ↓ HbA1c, − BP, ↓ Level of cholesterol |
Review Manager V.5.1 |
| Chen, 201539; Metabolism-Clinical and Experimental | Clinical markers |
Number of studies: 16 studies; Types of studies: RCTs; Total sample: per study ranged from 23 to 2575 |
Lifestyle intervention |
√ BEHA (-) □ DIET √ CVR (-) □ EXERCISE □ GC √ MED (-) □ PSY □ SMOKING √ SELF (-) |
Unclear, did not describe |
Number of session: monthly; Total contact hours: unclear; Duration: <6 months−8 years |
Strategies: unclear; Format: individual; group and mixed; Theoretical approach: unclear |
Unclear, did not describe |
Cardiovascular risk factors including ↓ BMI, ↓ HbA1c, ↓ SBP, DBP, − HDL-c and LDL-c |
All analyses were performed using Comprehensive Meta-Analysis statistical software |
| Terranova, 201572; Diabetes, Obesity and Metabolism |
Weight loss |
Number of studies: 10 individual studies (from 13 papers); Types of studies: RCTs; Total sample: ranging from 27 to 5145 participants |
Lifestyle-based-only intervention |
√ BEHA (-) √ DIET (-) □ DR (-) √ EXERCISE (-) □ GC □ MED □ PSY □ SMOKING √ SELF (-) |
Dietician; diabetes educator; general physician; multidisciplinary team or nutritionist; nurse |
Number of session: 1–42; Total contact hours: unclear; Duration: ranged from 16 weeks to 9 years |
Strategies and format: face-to-face individual or group-based sessions, or a combination of those. One study delivered the intervention via the telephone Theoretical approach: unclear |
Unclear, did not describe |
↓ Weight change;
− HbA1c |
Meta-analyses—Review Manager and meta-regression analysis—Stata version. |
| Pillay, 201571; Annals of Internal Medicine | HbAIc level |
Number of studies: 132; Types of studies: RCTs; Total sample: unclear |
Behavioural programme |
√ BEHA (-) √ DIET (-) □ DR √ EXERCISE (-) √ GC (-) √ MED (-) □ PSY □ SMOKING √ SELF (-) |
Trained individuals |
Number of session: unclear; Total contact hours: range, 7–40.5 hours; Duration: 4 or more weeks |
Strategies: unclear; Format: unclear; Theoretical approach: unclear |
Inpatient settings, post discharge, other |
− HbA1c;
↓ BMI |
The analysis was conducted by using a Bayesian network model |
| Pal, 201467; Diabetes Care | Health status, cardiovascular risk factors and QoL |
Number of studies: 20 papers describing 16 studies; Types of studies: RCTs; Total sample: 3578 participants |
Computer-based self-management interventions | □ BEHA □ DIET □ DR □ EXERCISE □ GC □ MED □ PSY □ SMOKING √ SELF |
Unclear, did not describe |
Number of session: 1–8; Total contact hours: 10 min– 6 hours; Duration: 8 weeks–12 months |
Strategies: online/web-based; Phone contact Format: individual; group and mixed Theoretical approach: TTM, social ecological theory, SCT and self-determination theory |
Unclear, did not describe |
− HRQoL,
↓HbA1c, − Death; ↓Cognitions, behaviours, −Social support, ↓Cardiovascular risk factors, −Complications, −Emotional outcomes, −Hypoglycaemia, −Adverse effects, −CE and economic data |
Meta-analysis using Review Manager software or narrative presentation |
| Ricci-Cabello, 201473; BMC Endocrine Disorders | Knowledge, behaviours and clinical outcomes |
Number of studies: 37 studies; Types of studies: almost two-thirds of the studies were RCTs, 27% studies were quasi-experimental design. Total sample: unclear |
DSM educational programme | □ BEHA √ DIET(+++) □ DR √ EXERCISE (+++) √ GC(+++) √ MED(++) √ PSY(++) □ SMOKING □ SELF |
Dietitian; nurse; psychologist; physician; research team or staff |
Number of session: 13.1; Total contact hours: 0.25–180 hours; Duration: 0.25–48 months |
Strategies: face-to-face; telecommunication; both Format: one on one; group and mixed Theoretical approach: unclear |
Postdischarge, other |
−Diabetes knowledge;
−Self-management; −Behaviours; −Clinical outcomes; ↓Glycated haemoglobin; −Cost-effectiveness analysis |
Meta-analyses and bivariate meta-regression were conducted with Stata V.12.0 |
| Saffari, 201474; Primary Care Diabetes | Glycaemic control. |
Number of studies: 10; Types of studies: RCTs; Total sample: 960 patients |
An educational intervention using SMS |
√ BEHA (-) □ DIET □ DR □ EXERCISE √ GC (-) √ MED (-) □ PSY □ SMOKING □ SELF |
Unclear, did not describe |
Number of session: weekly; or two messages daily or unclear; Total contact hours: unclear. Duration: 3 months–1 year |
Strategies: SMS: sending and receiving data. Receive data through text-messaging by patients only. Used a website along with SMS; Format: Unclear; Theoretical approach: Unclear. |
Inpatient settings, postdischarge, other | ↑Glycaemic control | Comprehensive Meta-analysis Software V.2.0 |
| Odnoletkova, 201466; Journal of Diabetes & Metabolism | Cost-effectiveness (CE) |
Number of studies: 17 studies; Types of studies: RCTs; Total sample: unclear |
Therapeutic education |
√ BEHA (-) □ DIET □ DR □ EXERCISE □ GC □ MED □ PSY □ SMOKING √ SELF (-) |
General physician; nutritionists or unclear |
Number of session: ~16; Total contact hours: unclear; Duration: unclear |
Strategies: face-to-face or unclear; Format: individual and group lessons; Theoretical approach: unclear |
Inhospital or unclear | −CE | Incremental cost-effectiveness ratio |
| Attridge, 201433; The Cochrane Library | HbAIc level, knowledge and clinical outcomes |
Number of studies: 33 trials; Types of studies: RCTs and quasi-RCTs; Total sample: 7453 participants |
’Culturally appropriate' health education |
√ BEHA (-) √ DIET (-) □ DR √ EXERCISE (-) √ GC (-) □ MED □ PSY √ SMOKING (-) □ SELF |
CHWs; dieticians; exercise physiologists; lay workers; nurses; podiatrists and psychologists |
Number of session: one session to 24 months; Total contact hours: unclear; Duration: the median duration of interventions was 6 months |
Strategies:
Format: group intervention method, one-to-one sessions and a mixture of the two methods. Or a purely interactive patient-centred method Theoretical approach: empowerment theories; behaviour change theories, TTM of behaviour change and SCT |
Inpatient settings, postdischarge, other |
↓HbA1c;
−HRQoL; −Adverse events; −Mortality; −Complications; −Satisfaction; ↑Empowerment; ↑Self-efficacy; −Attitude; knowledge; −BP; −BMI; ↓Lipid levels; −Health economics |
Meta-analyses used Review Manager software |
| Vugt, 201375; Journal of Medical Internet Research | Health outcomes |
Number of studies: 13 studies; Types of studies: RCTs; Total sample: 3813 patients |
BCTs are being used in online self-management interventions |
√ BEHA (-) □ DIET □ DR □ EXERCISE □ GC □ MED □ PSY □ SMOKING √ SELF (-) |
Healthcare professional |
Number of session: 6 weekly sessions or unclear; Total contact hours: unclear; Duration: unclear |
Strategies: online/web-based; Format: unclear; Theoretical approach: self-efficacy theory, social support theory, TTM, SCT, social-ecological model and cognitive behavioural therapy |
Postdischarge |
−Health behaviour change;
−Psychological well-being; −Clinical parameters |
Unclear |
| Gucciardi, 201352; Patient Education and Counseling | HbAIc level,physical activity and diet outcomes |
Number of studies: 13 studies; Types of studies: RCTs and comparative studies; Total sample: unclear |
DSME interventions. | □ BEHA √ DIET (+++); □ DR √ EXERCISE (+++); □ GC √ MED (+); √ PSY (+) □ SMOKING √ SELF (++) |
Dietitians (n=7/13); Multidisciplinary team (n=7/13); Nurse (n=5/13); Community peer worker (n=3/13) |
Number of session: low intensity: <10 education sessions (n=7); high intensity: ≥10 education sessions (n=6); Total contact hours: unclear; Duration: <6 months (n=7/13); ≥6 months (n=6/13) |
Strategies: face-to-face (n=13/13); written literature: (eg, handbook) (n=4/13); telephone (n=4/13); audiovisual (n=1/13) Format: one-on-one: (n=11/13); group (n=9/13) Theoretical approach: SAT; empowerment Behaviour change model; modification theories; pharmaceutical care model; Behaviour change theory; PATHWAYS programme; symptom- focused management model; motivational interviewing |
Inpatient settings, postdischarge |
− HbA1c levels,
− Anthropometrics, − Physical activity; − Diet outcomes |
A recently described method |
| Pal, 201368; The Cochrane Library | Health status and HRQoL |
Number of studies: 16 studies; Types of studies: RCTs; Total sample: 3578 participants |
Computer-based diabetes self-management intervention | □ BEHA √ DIET (-) □ DR √ EXERCISE (-) √ GC (-) √ MED (-) √ PSY (-) □ SMOKING □ SELF |
Nurse or other healthcare professionals |
Number of session: unclear; Total contact hours: unclear; Duration: 1 session– 18 months |
Strategies: online/web-based; phone contact Format: unclear; Theoretical approach: unclear |
Inpatient settings, postdischarge, other |
− HRQoL;
− Death from any cause; ↓HbA1c; − Cognitions; − Behaviours; −Social support; −Biological markers; − Complications |
Formal meta-analyses and narrative synthesis |
| Nam, 201262; Journal of Cardiovascular Nursing | Glycaemic control |
Number of studies: 12 RCTs; Types of studies: RCTs; Total sample: 1495 participants |
Diabetes educational interventions (no drug intervention) | □ BEHA √ DIET (-) □ DR √ EXERCISE (-) √ GC (-) √ MED (-) √ PSY (-) □ SMOKING √ SELF (-) |
Nurses (36%), dieticians (36%), diabetes educators (5%), other professionals (9%) and non-professional staff (14%) |
Number of session: 1 month or less; 1–3 months and 12 months; Total contact hours: most studies did not describe, or from 1 session to more than 30 hours; Duration: from 1 session to 12 months, frequency: 1 session to 25 weekly or biweekly education |
Strategies: teaching or counselling; home-based support and visual aids Format: group education or a combination of group education and individual counselling; or only individual counselling; Theoretical approach: unclear |
Inpatient settings, postdischarge, other | ↓HbA1c level | Meta-analysis |
| Steinsbekk, 201276; BMC Health Services Research | Clinical, lifestyle and psychosocial outcomes |
Number of studies: 21 studies (26 publications) Types of studies: RCTs; Total sample: 2833 participants |
Group-based education | Did not describe the content of the intervention | Community workers; dietician; lay health advisors nurse and nutritionist |
Number of session and total contact hours: 30 hours over 2.5 months, 52 hours over 1 year and 36 or 96 hours over 6 months Duration: 6 months to 2 years |
Strategies: face-to-face; Format: 5 to 8 participants group to 40 patients group Theoretical approach: empowerment model and the discovery learning theory, the SCT and the social ecological theory, the self-efficacy and self-management theories and operant reinforcement theory |
Inpatient settings, postdischarge, other |
↓HbA1c,
↑Lifestyle outcomes, ↑Diabetes knowledge, ↑Self-management skills, ↑Psychosocial outcomes, ↓Mortality rate, ↓BMI, ↓Blood pressure; ↓Lipid profile |
Meta-analysis using Review Manager V.5 |
| Amaeshi, 201232; Podiatry Now | Increasing good foot health practices that will ultimately reduce LEA |
Number of studies: eight studies; Types of studies: RCT or clinical controlled trial (CCT); Total sample: unclear |
Foot health education | Food care | Podiatrist, psychologist or unclear |
Number of session: unclear; Total contact hours: between 15 min and 14 hours; Duration: 3–30 months |
Strategies: face- to-face; Format: in three of the studies, educational interventions were delivered to the participants in groups, while the other five provided individualised (one-to-one) foot care education to the participants; Theoretical approach: unclear |
Unclear, did not describe |
↓ LEA;
↑Self-care |
Narrative synthesis |
| Lun Gan, 201157; JBI Library of Systematic Reviews |
Oral hypoglycaemic adherence |
Number of studies: seven studies; Types of studies: RCTs; Total sample: unclear |
Educational interventions |
√ BEHA (-) √ DIET (-) □ DR √ EXERCISE (-) √ GC (-) √ MED (-) √ PSY (-) □ SMOKING √ SELF (-) |
Nurses; pharmacists; other skilled healthcare professionals |
Number of session: 1–12 or unclear; Total contact hours: 2.5 hours or unclear; Duration: 4–12 months |
Strategies: face- to-face; Format: group and individual; Theoretical approach: unclear |
Inpatient settings, postdischarge, other |
↓ HbA1c,
− Medication adherence; ↓Blood glucose; − Tablet count; − Medication containers; − Diabetes complications; − Health service utilisation |
Narrative summary form |
| Burke, 201138; JBI Database of Systematic Reviews and Implementation Reports | HbAIc level,BP |
Number of studies: 11 RCTs and 4 quasi-experimental trials; Types of studies: RCTs and quasi-experimental trials; Total sample: 2240 patients |
Group medical visits |
√ BEHA (-) √ DIET (-) □ DR □ EXERCISE √ GC (-) √ MED (-) □ PSY □ SMOKING √ SELF (-) |
Endocrinologists; DM nurse; family physician; nutritionist and rehab therapist |
Number of session: 1–4 or unclear; Total contact hours: 2–4 hours or unclear; Duration: 1 session to 2 years |
Strategies: face-to-face; Format: group and individual; Theoretical approach: unclear |
Inpatient settings, postdischarge, other |
↓HbA1c;
−Systolic and diastolic BP; −LDL measurements |
Meta-analysis |
| Ramadas, 201177; International Journal of Medical Informatics | HbAIc level |
Number of studies: 13 different studies; Types of studies: RCTs and quasi-experimental studies; Total sample: unclear |
Web-based behavioural interventions |
√ BEHA (-) √ DIET (-) □ DR □ EXERCISE √ GC (-) √ MED (-) □ PSY □ SMOKING √ SELF (-) |
Dietician; endocrinologist; physicians; researchers or research staff members and study nurse |
Number of session: unclear; Total contact hours: unclear; Duration: ranged between 12 and 52 weeks, with an average of 27.2±18.3 weeks |
Strategies: email and SMS technologies that were commonly used together with the websites to reinforce the intervention, and website, print material Format: unclear; Theoretical approach: Wagner’s Chronic Care Model; self-efficacy theory/social support theory; TTM; HBM; SCT |
Inpatient settings, postdischarge, other |
− Self-monitoring blood sugar,
− Weight loss, − Dietary behaviour, − Physical activity |
Not statistically combined and re-analysed |
| Minet, 201061; Patient Education and Counseling | Glycaemic control |
Number of studies: 47 studies; Types of studies: RCTs; Total sample: unclear |
Self-care management interventions |
√ BEHA (-) □ DIET □ DR □ EXERCISE □ GC □ MED □ PSY □ SMOKING √ SELF (-) |
Case nurse manager; group facilitator; nurse educator; multidisciplinary team; physiologist; physician; peer counsellor; researcher and pharmacist |
Number of session: 3–26; Total contact hours: unclear; Duration: 4 weeks to 4 years |
Strategies: face-to-face; home visit; phone calls; Format: group and individual; Theoretical approach: unclear |
Inpatient settings, postdischarge, other | ↓ HbA1c | Meta-analyses and meta-regression used Stata’s meta command |
| Hawthorne, 201054; Diabetic Medicine | Effects of culturally appropriate health education |
Number of studies: 10 trials; Types of studies: RCTs; Total sample: 1603 patients |
Culturally appropriate health education | □ BEHA √ DIET (-) □ DR √ EXERCISE (-) □ GC □ MED □ PSY □ SMOKING √ SELF (-) |
Exercise physiologists; dieticians; diabetes nurses; link workers and podiatrists |
Number of session: unclear; Total contact hours: unclear; Duration: 1 session to 12 months |
Strategies: face-to-face; visual aids, leaflets and teaching materials; Format: group approach, one-to-one interviews and a mixed approach; Theoretical approach: SAT, Empowerment Behaviour Change Model, SCT, Management model and the Theory of Planned Behaviour |
Inpatient settings, postdischarge, other |
−QoL;
↓HbA1c; − BP; ↑Knowledge; − BMI; ↓ Lipid levels, − Diabetic complications, − Mortality rates, hospital admissions, hypoglycaemia |
Meta -analysis using the Review Manager and narrative review |
| Fan, 200947; Canadian Journal of Diabetes | Knowledge, self-management behaviours and metabolic control |
Number of studies: 50 studies;
Types of studies: RCTs; Total sample: unclear |
DSME intervention |
√ BEHA (-) □ DIET □ DR □ EXERCISE □ GC □ MED √ PSY (-) □ SMOKING √ SELF (-) |
Unclear, did not describe |
Number of session: 10 (range 1–28); Total contact hours: 17 contact hours (range 1– 52); ≤10 (46%); 11–20 (21%); >20 (33%); Duration: 22 weeks (range 1–48); ≤8 weeks (26%); 9–24 weeks (37%); >24 weeks (37%) |
Strategies: Online/web-based (4%); video (2%); face-to-face (60%); phone contact (4%); Mixed (30%). Format: one-on-one (32%); group (40%); mixed (28%) Theoretical approach: unclear |
Inpatient settings, postdischarge, other | ↑ Diabetes knowledge,
↑ Self-management behaviours; ↓ HbA1c |
Comprehensive meta-analysis (V.2.0) |
| Duke, 200946; The Cochrane Library | Metabolic control, diabetes knowledge and psychosocial outcomes |
Number of studies: nine studies; Types of studies: RCTs; Total sample: 1359 participants |
Individual patient education |
√ BEHA (-) □ DIET □ DR √ EXERCISE (-) √ GC (-) □ MED √ PSY (-) □ SMOKING □ SELF |
Diabetes educators and dieticians |
Number of session: 1–6; Total contact hours: 20 min –7 hours; Duration: 4 weeks–1 year |
Strategies: face to face; telephone; Format: individual; Theoretical approach: unclear |
Inpatient settings |
− HbA1c;
− Diabetes complications; − Health service utilisation and healthcare costs; − Psychosocial outcomes; − Diabetes knowledge; patient self-care behaviours; − Physical measures; metabolic |
Meta-analysis |
| Alam, 200930; Patient Education and Counseling | Glycaemic control and psychological status |
Number of studies: 35 trials; Types of studies: RCTs; Total sample: 1431 patients |
Psycho-educational interventions |
√ BEHA (-) □ DIET □ DR □ EXERCISE □ GC □ MED √ PSY (-) □ SMOKING □ SELF |
Generalists; psychological specialists; or did not report the specialist |
Number of session: 1–16; Total contact hours: 20 min –28 hours; Duration: about 13.7 (±11.06) weeks |
Strategies: face to face; telephone calls; Format: group format; a single format and used a combination; Theoretical approach: TTM; motivational interviewing |
Inpatient settings, other |
↓ HbAlc;
↓ Psychological distress |
Meta-analysis |
| Khunti, 200858; Diabetic Medicine | Knowledge and biomedical outcomes |
Number of studies: nine studies; Types of studies: RCTs and RCT was followed by a before-and-after study; Total sample: 1004 patients |
Any educational intervention | □ BEHA √ DIET □ DR □ EXERCISE □ GC □ MED □ PSY □ SMOKING □ SELF |
Unclear, did not describe |
Number of session: unclear; Total contact hours: unclear; Duration: 3–12 months |
Strategies: face-to-face; Format: group and individual; Theoretical approach: unclear |
Unclear, did not describe |
− Knowledge;
− Psychological and biomedical outcome measures |
Unclear |
| Loveman, 200860; Health Technology Assessment | Clinical effectiveness. |
Number of studies: 21 published trials; Types of studies: RCTs and CCTs; Total sample: unclear |
Educational interventions |
√ BEHA (++) √ DIET (+++) □ DR √ EXERCISE (+++) √ GC (+++) □ MED □ PSY □ SMOKING √ SELF (+++) |
Community workers; diabetes research technician; diabetes nurse, dieticians; educationalist; medical students; nurses; pharmacists; physician or physician assistant |
Number of session: two to four intensive education of 1.5–2 hours followed-up with additional education at, 3 and 6 months; Total contact hours and duration: about 150 mins over 6 months or 61–52 hours over 1 year |
Strategies: face-to-face; Format: group and individual; Theoretical approach: cognitive-behavioural strategies; pedagogical principle |
Inpatient settings, postdischarge, other |
− Diabetic control outcomes; − Diabetic end points; − QoL and cognitive measures |
Narrative review |
| Wens, 200878; Diabetes Research and Clinical Practice | Improving adherence to medical treatment recommendations |
Number of studies: eight studies; Types of studies: RCTs and controlling before and after studies Total sample: 772 patients |
Interventions aimed at improving adherence to medical treatment |
√ BEHA (-) √ DIET (-) □ DR √ EXERCISE (-) √ GC (-) √ MED (-) □ PSY □ SMOKING √ SELF (-) |
Diabetes educator; nurse or did not describe |
Number of session: unclear; Total contact hours: unclear; Duration:~9 months or unclear |
Strategies: face-to-face; telephone; Format: face-to-face; group based and telemedicine; Theoretical approach: unclear |
Inpatient settings, postdischarge, other |
− Adherence;
− HbA1c; − Blood glucose |
Cochrane Review Manager software |
| Hawthorne, 200853; The Cochrane Library | HbAIc level, knowledge and clinical outcomes |
Number of studies: a total of 11 trials; Types of studies: RCTs; Total sample: 1603 patients |
Culturally appropriate (or adapted) health education |
√ BEHA (-) √ DIET (-) □ DR √ EXERCISE (-) √ GC (-) □ MED □ PSY √ SMOKING (-) □ SELF |
Dieticians, diabetes nurses, exercise physiologists; link workers; podiatrists; psychologist and and non-professional link worker |
Number of session: unclear; Total contact hours: unclear; Duration: 1 session to 12 months |
Strategies: face-to-face; booklet; Format: group intervention method; one-to-one interviews; mixture of the two methods; purely interactive patient-centred method; semi-structured didactic format and combination of the two approaches Theoretical approach: SAT; Empowerment Behaviour Change Model; Behaviour Change Theory; SCT, Management Model and the Theory of Planned Behaviour |
Inpatient settings, postdischarge, other |
↓HbA1c
↑ Knowledge scores − Other outcome measures |
Narrative presentation and meta-analysis |
| Nield, 200763; The Cochrane Library | Metablic control |
Number of studies: 36 articles (18 trials); Types of studies: RCTs; Total sample: 1467 participants |
Dietary advice | □ BEHA √ DIET □ DR □ EXERCISE □ GC □ MED □ PSY □ SMOKING □ SELF |
Exercise physiologist; dietitian; group facilitator; nutritionist; nurse educator; and physician |
Number of session: 1–12; Total contact hours: 20 min–22 hours; Duration: 11 weeks– 6 months or unclear |
Strategies: face-to-face; Format: group and individual; Theoretical approach: unclear |
Inpatient settings, postdischarge, other |
− Weight;
− Diabetic complications; − HbA1c; − QoL; − Medication use; − Cardiovascular disease risk |
Meta-analysis |
| Zabaleta, 200779; British Journal of Community Nursing | Clinical effectiveness |
Number of studies: 21 studies; Types of studies: controlled trials; Total sample: unclear |
Structured group diabetes education |
√ BEHA (-) √ DIET (-) □ DR √ EXERCISE (-) √ GC (-) □ MED √ PSY (-) □ SMOKING □ SELF |
Diabetes nurse educator; physician’s assistant and physicians |
Number of session: 4–6 or unclear; Total contact hours: 6–12 hours or unclear; Duration: 1–6 months or unclear |
Strategies: face-to-face; Format: group; Theoretical approach: unclear |
Postdischarge | −HbA1c | A tabulative synthesis |
| Deakin, 200543; The Cochrane Library | Clinical, lifestyle and psychosocial outcomes |
Number of studies: 14 publications, reporting 11 studies; Types of studies: RCTs, and CCTs; Total sample: 1532 participants. |
Group-based educational programmes | Did not describe the content of the intervention | Health professionals, lay health advisors |
Number of session: unclear; Total contact hours: from 6 to 52 hours; Duration: 3 hours per year for 2 years and 3 or 4 hours per year for 4 years |
Strategies: unclear; Format: group; Theoretical approach: the Diabetes Treatment and Teaching Programme (DTTP); empowerment model; adult learning model, public health model, HBM and TTM |
Inpatient settings, postdischarge |
↓Metabolic control; ↑Diabetes knowledge;
↑QoL; ↑Empowerment/self-efficacy |
Summarised statistically |
| Vermeire, 200580; The Cochrane Library | Improving adherence to treatment recommendations |
Number of studies: 21 articles; Types of studies: RCTs; cross-over study; controlled trial; controlled before and after studies; Total sample: 4135 patients |
Interventions that were aimed at improving the adherence to treatment recommendations | □ BEHA □ DIET □ DR □ EXERCISE √ GC (-) √ MED (-) □ PSY □ SMOKING □ SELF |
Nurse, pharmacist and other healthcare professionals |
Number of session: unclear; Total contact hours: unclear; Duration: unclear |
Strategies: face-to-face; telephone; home visit; video; mailed educational materials; Format: unclear Theoretical approach: unclear |
Inpatient settings, postdischarge |
Direct indicators, such as ↓Blood glucose level; − Indirect indicators, such as pill counts; −Health outcomes |
A descriptive review and subgroup meta-analysis |
| Gary, 200349; Diabetes Educator | Body weight and glycaemic control |
Number of studies: 63 RCTs; Types of studies: RCTs; Total sample: 2720 patients |
Educational and behavioural component interventions | □ BEHA √ DIET (-) □ DR √ EXERCISE (-) √ GC (-) √ MED (-) □ PSY □ SMOKING □ SELF |
Nurse (39%); dietitian (26%); physician (17%); other or not specified (23%); other professional (13%); psychologist (9%); exercise psychologist (9%) and health educator (4%) |
Number of session: unclear; Total contact hours: unclear. Duration: 1 month to 19.2 months |
Strategies: unclear; Format: unclear; Theoretical approach: SAT, contracting model and patient empowerment |
Inpatient settings, postdischarge |
− Glycaemic control;
− Weight |
Sufficient data were combined using meta-analysis |
| Norris, 200265; Diabetes Care | Total GHb |
Number of studies: 31 studies Types of studies: RCTs. Total sample: 4263 patients |
Self-management education |
√ BEHA (-) √ DIET (-) □ DR □ EXERCISE □ GC □ MED □ PSY □ SMOKING √ SELF (-) |
Dietitian; lay healthcare worker; nurse; physician with team; self (eg, computer-assisted instruction) and team (nurse, dietitian, etc) |
Number of session: 6 (1–36); Total contact hours: 9.2 (1–28) hours; Duration: 6 (1.0–27) months |
Strategies: online/web-based; video; face-to-face; phone contact; Format: group; individual and mixed; Theoretical approach: unclear |
Inpatient settings, post discharge, other | ↓Total GHb | Meta-analysis and meta-regression |
| Norris, 200164; Diabetes Care | Clinical outcomes, knowledge, metabolic control |
Number of studies: 72 studies (84 papers); Types of studies: RCTs; Total sample: unclear |
Self-management training interventions |
√ BEHA (-) √ DIET (-) □ DR □ EXERCISE □ GC □ MED □ PSY □ SMOKING √ SELF (-) |
CHWs; nurse; or other healthcare professionals |
Number of session: 1–16; Total contact hours: ~22 hours; Duration: ~26 months |
Strategies: online/web-based; video (2%); face-to-face; phone contact; Format: group; individual and mixed; Theoretical approach: SAT; Fishbein and Ajzen HBM |
Inpatient settings, postdischarge, other | ↑Knowledge;
↑Lifestyle behaviours; −Psychological and QoL outcomes; ↑ Glycaemic control; − Cardiovascular disease risk factors |
Outcomes are summarised in a qualitative fashion |
ASE, attitude social influence-efficacy; BCTs, behavioural change techniques; BEHA, behavioural charge (including lifestyle modification); BMI, body mass index; BP, blood pressure; CABG, coronary artery bypass graft surgery; CAD, coronary artery disease; CCTS, controlled clinical trials; CHD, coronary heart disease; CHW, community health worker; CVR, cardiovascular risk factors; CVRF, cardiovascular risk factors; DIET, diet; DR, diabetes risks; DSM, diabetes self-management; DSME, diabetes self-management education; EDU, patient education; EXERCISE, exercise; GC, glycaemic regulation; GP, general practice; HbA1c, glycated haemoglobin; HBM, health belief model; HRQoL, health-related quality of life; LDL, low-density lipoprotein cholesterol; LDL-c, low-density lipoprotein cholesterol; LEA, lower extremity amputation; MED, medication; MI, myocardial infarction; PA, physical activity; PRIDE, Problem Identification, Researching one’s routine, Identifying a management goal, Developing a plan to reach it, Expressing one’s reactions and Establishing rewards for making progress; PSY, psychosocial issues (depression, anxiety); QoL, quality of life; RCTs, randomised controlled trials; SAT, social action theory; SBP, systolic blood pressure; DBP, diastolic blood pressure; HDL-c, high-density lipoprotein cholesterol; SCT, social cognitive theory; SELF, self-management (including problems solving); SMOKING, smoking cessation; SMS, short message system; T2DM, type two diabetes mellitus; TTM, transtheoretical model.
In the educational content: ‘+’: minor focus; ‘++’:moderate focus; ‘+++’ major focus; ‘- ’=unclear what the intensity of the education was for any topic.
In the outcomes: arrow up (‘↑’) for improvement, arrow down (‘↓’) for reduction; a dash (‘−’) for no change or inconclusive evidence.
Table 4.
Summary of evidence from quantitative research syntheses
| Intervention | Number of systematic reviews/meta-analysis, total participants | First author, year | Primary results/findings | Rating the evidence of effectiveness | |
| Patients with acute coronary syndrome | |||||
| General health education | Six/161 997 patients (Goulding et al, 201051 did not give the total sample size) | Ghisi, 201450 | Knowledge | 91% studies* | Some evidence |
| Behaviour | 77%/84%/65% studies* | ||||
| Psychosocial indicators | 43% studies* | ||||
| Brown, 201337 | Mortality | ||||
| MI | |||||
| Revascularisations | |||||
| Hospitalisations | |||||
| HRQoL | |||||
| Withdrawals/dropouts | |||||
| Healthcare utilisation and costs | |||||
| Brown, 201170 | Total mortality | ||||
| MI | |||||
| CABG | |||||
| Hospitalisations | |||||
| HRQoL | 63.6% studies* | ||||
| Healthcare costs | 40% studies* | ||||
| Withdrawal/dropout | |||||
| Goulding, 201051 | Beliefs | 30.08% studies* | |||
| Secondary outcomes | |||||
| Fernandez, 200748 | Smoking | ||||
| Cholesterol level | |||||
| Multiple risk factor modification | |||||
| Kotb, 201459 | All-cause hospitalisation | ||||
| All-cause mortality | |||||
| Smoking cessation | |||||
| Depression | |||||
| Systolic blood pressure | |||||
| Low-density lipoprotein | |||||
| Anxiety | |||||
| Psychoeducational interventions | Six/37 883 patients | Barth, 201569 | Abstinence by self-report or validated | Sufficient evidence | |
| Dickens, 201345 | Depression | ||||
| Aldcroft, 201131 | Smoking cessation | ||||
| Physical activity | |||||
| Huttunen-Lenz,201056 | Prevalent smoking cessation | ||||
| Continuous smoking cessation | |||||
| Total mortality | |||||
| Barth, 200836 | Abstinence by self-report or validated | ||||
| Smoking status | |||||
| Barth, 200635 | Abstinence | ||||
| Smoking status | |||||
| Secondary prevention educational interventions (including Internet-based secondary prevention) | Three/25 154 patients | Devi, 201544 | Mortality | Some evidence | |
| Revascularisation | |||||
| Total cholesterol | |||||
| HDL cholesterol | |||||
| Triglycerides | |||||
| HRQOL | |||||
| Auer, 200834 | All-cause mortality | ||||
| Readmission rates | |||||
| Reinfarction rates | |||||
| Smoking cessation rates | |||||
| Clark, 200541 | Mortality | ||||
| MI | |||||
| Quality of life | Most of the included studies* | ||||
| Patients with T2DM | |||||
| General health education | Five/2319 patients (Choi et al, 201640; Loveman et al, 200860; Zabaleta et al, 200779 did not give the total sample size) | Choi, 201640 | HbA1c | Some evidence | |
| Saffari, 201474 | Glycaemic control | ||||
| Duke, 200946 | HbA1c | ||||
| BP | |||||
| Knowledge, psychosocial outcomes and smoking habits | No data | ||||
| Diabetes complications or health service utilisation and cost analysis | No data | ||||
| Loveman, 200860 | Diabetic control outcomes | 46.15% studies* | |||
| Weight | 66.67% studies* | ||||
| Cholesterol or triglycerides | 40.00% studies (+) | ||||
| Zabaleta, 200779 | HbA1c | 4.8% studies* | |||
| Culturally appropriate health education | Eight/20 622 patients (Ricci-Cabello et al, 201473 and Gucciardi et al, 201352 did not give the total sample size) | Creamer, 201642 | HbA1c | Some evidence | |
| HRQoL | |||||
| AEs | No AEs | ||||
| Ricci-Cabello, 201473 | HbA1c | ||||
| Diabetes knowledge | 73.3% studies* | ||||
| Behaviours | 75% studies* | ||||
| Clinical outcomes | Fasting blood glucose, HbA1c and BP improved in 71%, 59% and 57% of the studies | ||||
| Attridge, 201433 | HbA1c | ||||
| Knowledge scores | |||||
| Clinical outcomes | |||||
| Other outcome measures | Showed neutral effects | ||||
| Gucciardi, 201352 | HbA1c levels | 3 of 10 studies* | |||
| Anthropometrics | 3 of 11 studies* | ||||
| Physical activity | One of five studies* | ||||
| Diet outcomes | Two of six studies* | ||||
| Nam, 201262 | HbA1c level | ||||
| Hawthorne, 201054 | HbA1c | ||||
| Knowledge scores | |||||
| Khunti, 200858 | Knowledge levels | Only one study reporting a significant improvement | |||
| Biomedical outcomes | Only one study reporting a significant improvement | ||||
| Hawthorne, 200853 | HbA1c | ||||
| Knowledge scores | |||||
| Other outcome measures | |||||
| Lifestyle interventions+behavioural programme | Six/10 440 patients (Huang et al, 201655; Pillay et al, 201571 and Ramadas et al, 201177 did not give the total sample size) | Huang, 201655 | HbA1c | Some evidence | |
| BMI | |||||
| LDL-c and HDL-c | |||||
| Chen, 201539 | HbA1c | ||||
| BMI | |||||
| SBP | |||||
| DBP | |||||
| HDL-c | |||||
| Terranova, 201572 | HbA1c level | ||||
| Weight | |||||
| Pillay, 201571 | HbA1c levels | ||||
| BMI | |||||
| Ramadas, 201177 | HbA1c | 46.2% studies * | |||
| Gary, 200349 | Fast blood sugar | ||||
| Glycohaemoglobin | |||||
| HbA1 | |||||
| HbA1c | |||||
| Weight | |||||
| Self-management educational interventions | Nine/19 597 patients (Minet et al, 201061; Fan et al, 200947 and Norris et al, 200164 did not give the total sample size) | Pal, 201467 | Cardiovascular risk factors | Sufficient evidence | |
| Cognitive outcomes | |||||
| Behavioural outcomes | Only one study reporting a significant improvement | ||||
| AEs | No AEs | ||||
| Vugt, 201375 | Health behaviours | 7 of 13 studies * | |||
| Clinical outcomes measures | Nine studies * | ||||
| Psychological outcomes | Nine studies * | ||||
| Pal, 201368 | HbA1c | ||||
| Depression | |||||
| Quality of life | |||||
| Weight | |||||
| Steinsbekk, 201276 | HbA1c | ||||
| Main lifestyle outcomes | |||||
| Main psychosocial outcomes | |||||
| Minet, 201061 | Glycaemic control | ||||
| Fan, 200947 | Diabetes knowledge | ||||
| Overall self-management behaviours | |||||
| Overall metabolic outcomes | |||||
| Overall weighted mean effect sizes | |||||
| Deakin, 200543 | Metabolic control (HbA1c) | ||||
| Fasting blood glucose levels | |||||
| Weight | |||||
| Diabetes knowledge | |||||
| SBP | |||||
| Diabetes medication | |||||
| Norris, 200265 | Total GHb | ||||
| Norris, 200164 | Knowledge | ||||
| Self-monitoring of blood glucose | |||||
| Self-reported dietary habits | |||||
| Glycaemic control | |||||
| Therapeutic education | One/total sample: unclear | Odnoletkova, 201466 | Cost-effectiveness | Overall high in studies on prediabetes and varied in studies on T2DM | Insufficient evidence |
| Foot health education | One/total sample: unclear | Amaeshi32 | Diabetes complications | Some evidence | |
| Incidence of LEA | |||||
| Group medical visit | One/2240 patients | Burke, 201138 | HbA1c | Some evidence | |
| BP and DBP | |||||
| SBP | |||||
| Cholesterol—LDL | |||||
| Psychoeducational intervention | One/1431 patients | Alam, 200930 | HbA1c | Some evidence | |
| Psychological status | |||||
| Interventions aimed at improving adherence to medical treatment recommendations | Three/4907 patients (Lun Gan et al, 201157 did not give the total sample size) | Lun Gan, 201157 | Oral hypoglycaemic adherence | Five of seven studies * | Some evidence |
| Wens et al., 200878 | Adherence | General conclusions could not be drawn | |||
| Vermeire, 200580 | HbA1c | ||||
| Dietary advice | One/1467 patients | Nield, 200763 | Glycaemic control (addition of exercise to dietary advice) | Insufficient evidence to determine | |
| Weight | Limited data | ||||
| Diabetic microvascular and macrovascular diseases | Limited data | ||||
*Intervention group is significantly better than control group, for example, ‘91% studies ’ means 91% studies reported a significant better compared with control group.
AEs, adverse events; BMI, body mass index; BP, blood pessure; CABG, coronary artery bypass graft surgery; HbA1c, glycated haemoglobin; HRQoL, health related quality of life; LDL-c, low-density lipoprotein cholesterol; LEA, lower extremity amputation; MI, myocardial infarction; RCTs, randomised controlled trials; SBP, systolic blood pressure, DBP, diastolic blood pressure, HDL-c, high density lipoprotein cholesterol; T2DM, type two diabetes mellitus.
Synthesising the results and rating the evidence for effectiveness
The statements of evidence were based on a rating scheme to gather and rate the evidence across the included publications.26 The statements of evidence were based on the following rating scheme: sufficient evidence, sufficient data to support decisions about the effect of the health education-related interventions.26 A rating of sufficient evidence in this review is obtained when systematic reviews or meta-analyses with a large number of included articles or participants produce a statistically significant result between the health education group and the control group.26 Some evidence, is a less conclusive finding about the effects of the health education-related interventions26 with statistically significant findings found in only a few included reviews or studies. Insufficient evidence, refers to not enough evidence to make decisions about the effects of the health education-related interventions, such as non-significant results between the health education group and the control group in the included systematic reviews or meta-analyses.26 Insufficient evidence to determine, refers to not enough pooled data to be able to determine whether of the health education-related interventions are effective or not based on the included reviews.26
Results
Characteristics of included reviews
The selection process and number of studies at each step was illustrated as presented in figure 1. The database search yielded 692 publications, with removal of 197 duplicates and 371 articles that did not meet the inclusion criteria, 124 full-text articles were retrieved after applying the methodological quality rating (AMSTAR scale), and three studies27–29 were removed due to low scores ≤3 on the AMSTAR scale. Fifty-one systematic reviews or meta-analyses30–80 conducted between 2001 and 2016 and published in English were included (figure 1; tables 1–3); 15 relating to ACS. The overlap of the trials included in the 15 reviews and meta-analyses related to ACS was slight (CCA=2.6%). For the 36 systematic reviews relating to T2DM, the overlap of trials within these 35 reviews and meta-analyses (one review47 did not report the included studies) was slight (CCA=2.1%). None of the articles included patients with both ACS and T2DM. The umbrella review involved a total of 2 77 493 patients, including 2 25 034 patients with coronary heart disease or ACS (one article did not report the total sample) and 52 459 patients with T2DM (16 papers did not report the total sample). The average sample size of included articles was 8161 (range, 536–68 556) participants, however, 63 studies related to ACS and 177 studies related to T2DM were included in more than one systematic review or meta-analysis (see online supplementary appendices 2 and 3 and CCA statistics). The sample of these studies would therefore be included more than once. Of the included systematic reviews or meta-analyses, 11 were published in The Cochrane Library. Nine of the articles described meta-analyses, 29 articles described systematic reviews and the remaining 13 articles were described as systematic reviews and meta-analyses or meta-regressions or narrative reviews.
Figure 1.
Flow chart of the systematic reviews and meta-analyses selection process.
Electronic database searches were conducted for all systematic reviews or meta-analyses, with an average of 6 databases searched (range, 2–16). The dates searched ranged widely from inception of the database through December 2014. Most of the included reviews were randomised controlled trials (RCTs), and an average of 25.6 (range, 7–132) studies was included per systematic review or meta-analyses. Of the total, 818 unique (non-repeated) studies were included in all of the reviews or meta-analyses, 286 included patients with ACS and 532 included patients with T2DM (see online supplementary appendix 2 and 3). The included reviews assessed the risk of bias using the Cochrane risk of bias tool (22 publications), JADA quality score (7 publications), Joanna Briggs quality assessment tool (2 publications), PEDro scale (1 publication), RCT Critical Appraisal Skills Programme (1 publication) and the SIGN-50 checklist (1 publication).
Methodological quality of included systematic reviews and meta-analyses
The methodological quality of the included publications is presented in table 1. Thirty (58.8%) publications were classified as high quality (scores 8–11) and 21 (41.2%) publications were classified as medium quality (scores 4–7). Twenty-five (49%) reviews specifically provided an a priori design, while the use of such a design was unclear for 26 (51%) publications. The inclusion of other forms of literature (such as grey literature) was described in 18 (35%) reviews. Only 14 out of 51 (27%) reviews included a table of included and excluded studies. Only two (4%) reviews did not provide a characteristics table of the included papers. The scientific quality of the included papers was evaluated and documented in 47 (92%) reviews. The scientific quality of the included studies was used appropriately to formulate conclusions in 47 (92%) reviews. The methods to combine the results of the included studies were appropriate in 43 (86%) reviews. Publication bias was assessed in only 19 (37%) reviews. Finally, conflicts of interest were reported in 47 (92%) reviews.
Characteristics of health educational interventions
The description of the health educational interventions followed the Workgroup for Intervention Development and Evaluation Research reporting guidelines for behaviour change interventions.81 The characteristics of the recipients, setting, delivery methods, intensity, duration and educational content of health educational interventions for patients with ACS or T2DM are summarised in tables 2 and 3. The delivery strategies for health education included face-to-face, internet-based, phone-based, videotape, written educational materials or mixed. The format included one-on-one (individualised), group or both. Face-to-face sessions were the most common delivery formats, and many education sessions were also delivered by telephone/web contact or individualised counselling. The number of sessions, total contact hours and durations varied, and there was limited information about the intensity of health education for patients provided. The frequency of educational sessions was weekly or monthly, and an average of 3.7 topics was covered per education session. Nurses and multidisciplinary teams were the most frequent educators, and most education programmes were delivered postdischarge.
Acute coronary syndrome
The educational content for patients with ACS covered cardiovascular risk factors in eight reviews (53.33%), psychosocial issues in eight reviews (53.33%), smoking cessation in six reviews (40.00%), exercise in five reviews (33.33%), behavioural change in five reviews (33.33%), diet in four reviews (26.67%), self-management in three reviews (20.00%) and medication in one review (6.67%). Two reviews only included smoking cessation and cardiovascular risk factors. The most common educational providers were nurses and a multidisciplinary team. Six studies31 36 48 51 56 69 (6/15, 40%) described the theoretical approach that underpinned the education intervention.
Type 2 diabetes mellitus
The educational content for patients with T2DM included diet in 23 reviews (63.89%), behavioural change in 21 reviews (58.33%), self-management in 20 reviews (55.56%), exercise in 17 reviews (47.22%), glycaemic regulation in 16 reviews (44.45%), medication in 13 reviews (36.11%), psychosocial issues in 9 reviews (25.00%), smoking cessation in 2 reviews (5.56%), cardiovascular risk factors in 2 reviews (5.56%) and DM risks in 1 review (2.78%). The most common providers were dieticians, nurses and a multidisciplinary team. The number of sessions, total contact hours and durations varied. Thirteen reviews30 33 43 49 52–54 60 64 67 75–77 (13/36, 36.11%) described the theoretical approach that underpinned the education intervention.
Effect of interventions
The outcomes of the included systematic reviews and meta-analyses are summarised in table 4.
Patients with ACS
Three major types of health education-related interventions were used for patients with ACS: general health education (only included general health information), psychoeducational interventions and secondary prevention educational interventions (including strategies to promote a healthy lifestyle, manage medications and reduce cardiovascular complications) as well as internet-based interventions.
General health education
The findings are based on our synthesis of the findings from six systematic reviews.37 48 50 51 59 70 Overall, there were mixed effects of general health education on behavioural change or clinical outcomes in patients with ACS. There was some evidence of a positive effect of general health education on knowledge, behaviour, psychosocial indicators, beliefs and risk factor modification, but no effects for key clinical outcomes, such as cholesterol level, hospitalisation, mortality, MI and revascularisation. The results for health-related quality of life, healthcare utilisation and costs were mixed; several reviews reported a significant change, and other reviews reported no significant change for these outcomes. Only one review focused on telephone-based health education. There is some evidence that telephone-based health education during cardiac rehabilitation might improve all-cause hospitalisation, anxiety, depression, smoking cessation and systolic BP, but there is no evidence for improvements in all-cause mortality and reductions in low-density lipoprotein cholesterol.59
Psychoeducational interventions
Strategies for psychoeducational interventions have a specific focus on smoking cessation and depression. The findings are based on synthesis of results from six publications.31 35 36 45 56 69 There is sufficient evidence that psychoeducational programmes are effective at decreasing smoking, achieving smoking abstinence and reducing depression. One review reported no effect on smoking cessation31 or total mortality.56
Secondary prevention educational interventions
The following statements are based on our synthesis of results from three papers.34 41 44 There is some evidence that secondary prevention educational interventions reduce MI readmission rates and improve quality of life, but the intervention was ineffective in reducing revascularisation, cholesterol levels and improving smoking cessation rates. The results are mixed for mortality and re-infarction rates; two reviews34 41 found positive effects on mortality, while one review44 did not.
Patients with T2DM
Ten types of health education-related interventions were used for patients with T2DM: culturally appropriate health education (tailored to the religious beliefs, culture, literacy and linguistics of the geographical area), dietary advice, foot health education, group medical visits (a group education component taught by health professionals), general health education (only included general health information), improving the uptake and maintenance of medication regimes (eg, promoting the use of oral hypoglycaemic medications), lifestyle interventions (specific focus on dietary changes and increased physical activity, or stress management), psychoeducational interventions and self-management educational interventions (activities that promote or maintain the behaviours to manage T2DM often based on the National Standards for Diabetes Self-Management Education13) and therapeutic education (collaborative process needed to modify behaviour and more effectively manage risk factors).
Culturally appropriate health education
Findings are based on our synthesis of results from eight publications.33 42 52–54 58 62 72 Overall, there was some evidence of the effects of culturally appropriate health education on clinical outcomes for T2DM. There was sufficient evidence that culturally appropriate health education improves HbA1c reduction and knowledge scores. There is some evidence that physical activity and clinical outcomes (blood glucose, HbA1c, BP) were improved. There were no data relating to adverse events during the intervention and follow-up (such as hypoglycaemic events and mortality), and there was insufficient evidence about improvements in quality of life.
General health education
The statements are based on our synthesis of results from five papers.40 46 60 74 79 Overall, there were mixed effects of general health education programmes on clinical outcomes for T2DM, including HbA1c, cholesterol level and triglyceride level. There was some evidence of the effectiveness of general health education on the management of glycaemia, weight reduction and some diabetes management outcomes (HbA1c, diabetes complications). There were no data supporting the effectiveness of general health education on reduced health service utilisation, diabetes complications, improved knowledge, psychosocial outcomes or smoking habits.
Lifestyle interventions
The following statements are based on our synthesis of results from six reviews.39 49 55 71 72 77 Overall, there were mixed effects of the lifestyle interventions on cholesterol level, HbA1c level and body weight. There is some evidence that lifestyle interventions or behavioural programmes are effective for blood glucose and BP management, but they were ineffective for reductions in HbA1c scores.71 72
Uptake and maintenance of medication regimes
The statements are based on our synthesis of results from three publications.57 78 80 There is some evidence of the effectiveness of increased uptake and maintenance of medication regimes for taking medications for HbA1c regulation including oral hypoglycaemic agents.
Self-Management educational interventions
The statements are based on our synthesis of results from nine reviews.43 47 61 64 65 67 68 75 76 Overall, there was sufficient evidence of the effects of self-management education interventions on HbA1c level, knowledge, lifestyle outcomes and main psychosocial outcomes. However, there was insufficient evidence of the benefits of this education intervention on depression, quality of life and body weight.
Other health education-related interventions
Other health education-related interventions for patients with T2DM included therapeutic education, foot health education, group medical visits, psychoeducational interventions and dietary advice. Statements for all of these interventions are based on our synthesis of results from one review.
There is some evidence that foot health education is effective in reducing the incidence of lower extremity amputation.32 There is some evidence that group medical visits are effective for improving HbA1c and systolic BP management.38 There is also some evidence that psychoeducational programmes are effective for improving HbA1c regulation and psychological status.30
Finally, there is insufficient evidence that dietary advice improves glycaemic and weight management or reduces microvascular and macrovascular diseases.63 There is also insufficient evidence for the cost-effectiveness of therapeutic education for patients with T2DM.66
Discussion
This umbrella review identified 51 systematic reviews or meta-analyses (15 for ACS and 36 for T2DM) that assessed the outcomes of various aspects (such as the duration, contact hours, educational content, delivery mode) of the delivery of health education-related interventions relevant to high-risk patients with ACS and T2DM. Health education has become an integral part of the management for people with ACS and T2DM. The most appropriate focus of the education provided to patients with ACS and T2DM remains largely undefined in the literature. For example, it remains unknown if the focus should be primarily on cardiovascular risk factors, blood glucose monitoring or all educational components for patients with both conditions.70 76 In addition, should cardiovascular risk factors be the focus during the acute inpatient stay with other educational needs such as the smoking cessation occurring within the primary care or outpatient settings.31 69 70
It remains challenging to determine the specific strategy or format that is the most effective delivery mode for patients with ACS or T2DM. There is very limited evidence to guide clinicians on the duration, contact hours, educational content, delivery mode, total length and setting of health education programme for cardiac patients.50 For patients with DM, one study reported that more successful programme were longer than 6 months (longer duration), consisted of greater than 10 contact sessions (high intensity) and were one-on-one sessions with individualised assessment.82
Use of theoretical orientation to develop educational intervention
For patients with ACS
Use of theory when designing behavioural change interventions may also influence effectiveness.75 Health education using a cognitive behavioural strategy is most consistently effective in changing maladaptive illness beliefs,51 and studies using more than two behavioural change strategies reported significant differences between the intervention and control groups.31 In one review, a significant change in smoking cessation was not observed in subgroup analyses between studies that did or did not report using a theory in intervention planning56; however, the authors did not suggest that using a theory in programme planning should be disregarded but reported that examining actual theories or mechanisms underlying health education programmes is required.56 Owing to the considerable overlap between different theories and the detailed description of the theoretical approach in only approximately 40% of the included papers, it is difficult to determine the most effective theoretical approach, but many models can be used with success, such as the health belief model (HBM), social cognitive theory (SCT) and transtheoretical model (TTM).56 67 69 75 Three reviews31 41 44 noted that some included studies used behavioural strategies such as goal setting. These strategies were found to be beneficial for patients with coronary heart disease.
For patients with T2DM
Although the theoretical approach underpinning the health education programme was not always described, 13 of the 36 reviews (36.11%) related to T2DM reported the theoretical approach used in their included studies. The most common theories were SCT (including self-efficacy), empowerment theories (eg, empowerment behaviour change model, self-determination and autonomy motivation theory, middle-range theory of community empowerment) and TTM. There is evidence that health education interventions based on a theoretical model are likely to be effective.43 Vugt et al suggested that self-care education programmes should be based on theories and that theory-based self-care interventions are more effective than non-theory-based programmes.75 83 Theories could help to specify the key target health behaviours and behavioural change techniques required to generate the desired outcomes.75 The decision regarding the theory should be based on the aim of the programme and factor for intervention.77 Only one review reported that a theoretical approach underpinning the health education programme is not necessary for better outcomes.76 Fourteen reviews30 33 40 46 52 57 60 63 64 67 68 73 75 77 reported that goal setting was conducted in the included studies. Goal setting by patients, health professionals or mutually agreed goals were linked to improved patient outcomes.
Educational content
For patients with ACS
Most reviews reported that the educational content of the interventions was comprehensive. The most common topics, of the average 3.7 topics per education session, were behavioural change, cardiovascular risk factors management, exercise, psychosocial issues and smoking cessation. An underlying principle of health education for patients with ACS is that knowledge is necessary, but not enough to develop health behaviours and change risk factors.31 50 Age, cognitive factors, environmental factors and social and economic background are also important considerations.50 While interventions using a behavioural programme, telephone-based content or self-care are effective for smoking cessation, there was insufficient evidence to support that any type of educational programme was more efficacious than the others.69 Psychoeducation, which is defined as multimodal, educationally based, self-management interventions,31 led to enhanced physical activity levels within 6–12 months when added to cardiac rehabilitation (CR) and was more effective than an exercise programme or health education alone.31 56 Moreover, psychoeducational interventions were more effective for patients with ACS than other types of health education.31 56
For patients with T2DM
The educational content for patients with T2DM focused more on behavioural change, diet, exercise, glycaemic regulation, medication and self-management. Health education that was self-management was more effective for patients with T2DM.40 47 In addition, based on the current evidence, the educational content should be culturally sensitive, especially for patients with T2DM33 42 54; culturally appropriate diabetes health education may have a greater impact on the management of glycaemia and reduce diabetes complications.77 The educational interventions for patients with T2DM focused primarily on HbA1c, lipid levels, quality of life and body weight. HBM and SCT were the most common theories used in the included reviews.
Teaching strategies and outcomes
For patients with ACS
Most reviews reported that the education was provided using multiple teaching methods and in multiple settings. Nurses and multidisciplinary teams were the most frequent people providing education, and most education programmes were delivered postdischarge. Although face-to-face sessions were the most common delivery format, many education sessions were also delivered by telephone or through individualised counselling. Telephone-based health education appeared to be effective for reducing hospitalisations, systolic BP, smoking rates, depression and anxiety.59 The educational interventions for patients with ACS focused primarily on clinical outcomes (hospitalisation and mortality), modifiable risk factors (BP, low-density lipoprotein levels and smoking cessation) and other psychological outcomes (anxiety and depression).
For patients with T2DM
Mixed health education programmes generally included group sessions combined with educator-facilitated individual sessions, covering basic knowledge and problem-solving skills. These programmes produced greater benefits and larger effect sizes for blood glucose reduction and knowledge levels in patients with T2DM.47 In contrast, individual education programmes have been reported as more effective in achieving outcomes than group-based education. This may be because education programmes might be more efficient at addressing personal needs, with greater participant engagement.73 However, one systematic review reported that individual and group patient education demonstrated similar outcomes among patients with T2DM.46
Although face-to-face sessions were the most common delivery format, many education sessions were also delivered by telephone or individualised counselling. Face-to-face health education programmes were most effective for enhancing blood glucose regulation and knowledge levels, while mixed delivery models (face-to-face, phone contact, online or web-based or video) produced a moderate effect for knowledge levels.47 Another review reported that face-to-face health education programmes generated a greater benefit for metabolic management than those delivered using electronic communication technology.73
Nurses (including diabetes nurses educators), community workers, dieticians and multidisciplinary teams were the most frequent educators, and most of the education programmes were delivered postdischarge. Some reviews indicated that health education programmes delivered by a group of different educators, with some degree of education reinforcement at additional points of contact, may provide the best results.60 76 However, based on two studies that reported HbA1c at 12 months, it is indicated that the outcomes in studies with only a diabetes nurse as the educator also tended to do better than the outcomes in studies with a multidisciplinary team, while the biggest effect was seen when a dietician was the only educator.76 Health education programmes delivered by one person may focus more on the patient’s ability than the educational content or quality of the health education programmes.76 However, no clear conclusion can be drawn whether having one educator delivering the intervention is best due to few information.60
Delivery, timing and follow-up
For patients with ACS
Most educational sessions were delivered weekly. Few reviews provided information regarding the duration of education interventions; when the duration was reported, it varied from 4 weeks to 48 months. These findings suggest that there is a significant gap in the evidence in relation to the duration, contact hours, educational content, optimal delivery mode, total length and setting of health education programmes for cardiac patients.50 For patients with ACS, one systematic review that included 7 studies with a total of 536 participants reported that studies with education lasting at least 6 months resulted in the most significant changes in the primary outcomes (such as behavioural change, smoking cessation)31 and that at least 12 months of follow-up is needed to evaluate the impact of telephone-based education.59 Another review reported that the intensity of education programmes is important for efficacy regarding smoking cessation: interventions with a very low intensity and brief interventions do not have a significant effect,69 and programmes for smoking cessation among patients with coronary heart disease should last >1 month.69 Most of the reviews were provided for patients with ACS in inpatient settings and then within postdischarge settings, five reviews31 36 45 48 59 did not explicitly state the settings in which the health education-related interventions were provided.
For patients with T2DM
Education sessions were delivered weekly or monthly. Longer health education programmes for T2DM (>6 months) produced larger effects for all primary outcomes (such as HbA1c).47 Health education lasting >3 months resulted in the largest effect size compared with health education of a shorter duration (<3 months).33 For HbA1c, the effect size at 6 months seemed to be significantly greater than at 3 and 12 months; in other words, the effect size peaked at 6 months.62 In general, health education of a greater intensity (longer duration and more sessions) was more effective for blood glucose reduction and knowledge levels among patients with T2DM.47 74 Compared with health education programmes covering only one topic, programmes that included multiple or mixed educational topics yielded consistently greater benefits in blood glucose reduction and knowledge levels.47 In addition, health education programmes combined with specific behavioural change strategies (such as self-care strategies) seemed more effective than other programmes.47 Health education-related interventions were mainly delivered in hospital settings, primary care settings, diabetes centres or community-based settings, although six reviews32 39 55 58 67 72 did not explicitly state the delivery settings.
Recommendations about health education interventions for patients with ACS and T2DM
These results from included systematic reviews and meta-analyses help to provide recommendations about the content of a health education intervention for patients with ACS and T2DM, requiring further evaluation. Future development of educational programmes for patients with ACS and T2DM by healthcare professionals should consider the needs of people with these diseases.37 40 42 70 Based on the results and findings from this umbrella review, recommendations are made in table 5. The acute life-threatening nature of ACS requires that increased emphasis should be placed on cardiovascular risk factors in any combined education programme. Both ACS and T2DM have common lifestyle factors such as inactivity and high fat diet requiring modifications.
Table 5.
Recommendations of health education programmes for patients with ACS and T2DM
| Patients with ACS | Patients with T2DM | Both ACS and T2DM | ||
| Theoretical approach | SCT, empowerment theories. | HBM; SCT. | HBM; SCT and empowerment theories | |
| Behavioural strategies | Goal setting | Goal setting | Goal setting | |
| Educational content | Behavioural change (such as smoking cessation), cardiovascular risk factors, exercise, medication and psychosocial issues | Behavioural change, diet, exercise, glycaemic control, medication and self-management | Behavioural change (such as smoking cessation), cardiovascular risk factors, diet, exercise, glycaemic control, medication, psychosocial issues and self- management | |
| Healthcare professionals to deliver | Nurse or multidisciplinary team | Multidisciplinary team; dietitian or nurse | Nurse or multidisciplinary team | |
| Teaching approaches | Strategies | Face to face; telephone or mixed | Face-to-face, written materials; telephone or mixed | Face-to-face, written materials; telephone contact or mixed |
| Format | Individual (one by one) or mixed | Individual (one by one) or mixed | Individual (one by one) or mixed | |
| Delivery timing | Contact hours | More than 30 min per time per week | More than 30 min per time per week | More than 30 min per time per week |
| Duration | At least 6 months | About 6 months | At least 6 months | |
| Duration of follow-up | At least 12 months | At least 12 months | At least 12 months | |
| Settings | Inpatient and postdischarge settings | Hospital settings and primary care settings | Inpatient and postdischarge settings | |
ACS, acute coronary syndrome; T2DM, type two diabetes mellitus; SCT, social cognitive theory; HBM, health belief model.
Overall completeness and applicability of evidence
This overview potentially provides an estimate with the lowest level of bias for the impact of health education-related interventions for patients with ACS or T2DM and could be regarded as an all-inclusive summary of the current evidence base for health education for these patients. While this umbrella review identified evidence for each of the types of health education, there was only a small number of reviews within some categories (such as psychoeducational intervention30 and dietary advice63), and these studies were not very informative. This umbrella review also found no reviews that systematically analysed varying doses of health education; therefore, could not examine the dose-response effects. There was insufficient information about the evaluated doses (total contact hours and duration of education) to enable comparison of the benefits of differences in the magnitude of the doses across the different research. This umbrella review found no reviews focused on patients with ACS and T2DM; instead, all of the systematic reviews and meta-analyses focused on only one of these diseases.
Quality of the evidence
The methodological quality of the included systematic reviews and meta-analyses varied. All of the included reviews or meta-analyses were of moderate-to-high methodological quality, as assessed using AMSTAR. However, only 30 (58.8%) systematic reviews or meta-analyses were rated as high quality and only 3 (5.9%) systematic reviews or meta-analyses43 53 69 adequately met all 11 AMSTAR criteria. This indicates that some of the reviews included in this umbrella review may have limitations in their design, conduct and/or reporting that could have influenced the findings when considered both individually and collectively.32 65
The quality of the primary studies in the included systematic reviews or meta-analyses also varied. The main sources of bias were inadequate reporting of allocation concealment and randomisation processes, as well as lack of outcome blinding.33 42 69 70 This bias in the methodological quality led to lower quality assessments, which varied by results within each included review. Other reasons for lower methodological quality included heterogeneity in, or inconsistency of, the effect and imprecise findings. Heterogeneity between studies in this umbrella review was described in terms of the intervention, participant characteristics and length of follow-up. Heterogeneity was an important factor indicating the complexity of the health education interventions.56 The variability in the approaches, tools or scales used to measure outcomes between the included studies are likely to introduce some heterogeneity.30 The heterogeneity of the educational interventions seen in the reviews included in this umbrella review may reflect the uncertainty about the optimal strategy for providing health education to patients.37 In addition, 240 studies were included more than once in the included reviews and meta-analyses. However, the overall overlap of studies among reviews and meta-analyses-related ACS and T2DM was slight, CCA of 2.6% and 2.1%, respectively.25
This umbrella review is the first synthesis of systematic reviews or meta-analyses to take a broad perspective on health education-related interventions for patients with ACS or T2DM. Given that health education is complex, the biggest challenge for systematic reviews or meta-analyses of health education is accounting for the potential clinical heterogeneity in health education-related interventions (content and delivery approaches) and the population of patients who receive health education. To facilitate comparisons across systematic reviews of health education and the efficient future update of this umbrella review, future reviews or meta-analyses need high-quality research and to standardise their design and reporting, including the reporting of included study characteristics, assessment criteria for risk of bias, outcomes and methods to synthesise evidence synthesis.
Conclusions
For clinicians providing educational interventions to individuals with ACS and T2DM, the results from this review provide a contemporaneous perspective on current evidence on the effectiveness of health education (its content and delivery methods) for this high-risk patient group. The current evidence compiled by this umbrella review supports current international clinical guidelines, that theoretically based education interventions lasting 6 months, delivered in multiple modes (face to face, phone contact, online or web-based or video), and with individualised education delivered weekly, are more likely to generate positive outcomes. This review also supports health education-related interventions provided by health professionals, including nurses and multidisciplinary teams, delivering content including specific clinical factors for ACS and T2DM (BP, glycaemic level and medication), modifiable risk factors (unhealthy diet, inactivity and smoking) and other psychological factors (anxiety and depression). These health education interventions could be delivered postdischarge, such as rehabilitation centres, primary care centres and the community and should be at least 6 months in duration. The effectiveness of these programmes was based on HbA1c levels, knowledge, psychosocial outcomes, readmission rates and smoking status rather than clear evidence of reduced mortality, MI or short-term and long-term complications. In addition, psychoeducational interventions were more effective for patients with ACS, and health education that was culturally appropriate or taught self-management was more effective for patients with T2DM. We also found that longer durations and high-intensity health education provided in an individualised format were more helpful for patients with ACS or T2DM.
The fact that none of the included reviews included patients with both ACS and T2DM indicates a clear need for further rigorous experimental studies with patients with both diseases. Future research that includes these aspects of education are likely to determine the effectiveness of educational interventions focusing on cardiovascular and DM risk factors and complications within patients with ACS and T2DM.
Supplementary Material
Acknowledgments
We would like to thank the authors of the original articles who provided additional unpublished data.
Footnotes
Contributors: Study conception and design: XL-L, MJ, KW, C-JW, YS. Data collection: XL-L, YS. Data analysis: XL-L, YS, MJ, KW, C-JW. Manuscript drafts: XL-L, MJ, C-JW, KW, YS.
Funding: This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors. The lead author is a recipient of an Australian Catholic University Faculty of Health Sciences Tongji University Cotutelle PhD Scholarship.
Competing interests: None declared.
Provenance and peer review: Not commissioned; externally peer reviewed.
Data sharing statement: No additional data are available.
References
- 1.Scarborough P, Wickramasinghe K, Bhatnagar P, et al. Trends in coronary heart disease, 1961-2011. London: British Heart Foundation, 2011. [Google Scholar]
- 2.Finegold JA, Asaria P, Francis DP. Mortality from ischaemic heart disease by country, region, and age: statistics from World Health Organisation and United Nations. Int J Cardiol 2013;168:934–45. 10.1016/j.ijcard.2012.10.046 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Amsterdam EA, Wenger NK, Brindis RG, et al. 2014 AHA/ACC guideline for the management of patients with Non-ST-Elevation acute coronary syndromes: a report of the American College of Cardiology/American Heart Association Task Force on practice guidelines. J Am Coll Cardiol 2014;64:e139–228. 10.1016/j.jacc.2014.09.017 [DOI] [PubMed] [Google Scholar]
- 4.Kahn M, Wheatcroft S. Acute coronary syndromes in diabetes Fisher M, Heart Disease and Diabetes. Oxford: Oxford University Press, 2008. [Google Scholar]
- 5.Hasin T, Hochadel M, Gitt AK, et al. Comparison of treatment and outcome of acute coronary syndrome in patients with versus patients without diabetes mellitus. Am J Cardiol 2009;103:772–8. 10.1016/j.amjcard.2008.11.034 [DOI] [PubMed] [Google Scholar]
- 6.Franklin K, Goldberg RJ, Spencer F, et al. Implications of diabetes in patients with acute coronary syndromes. the global registry of acute coronary events. Arch Intern Med 2004;164:1457–63. 10.1001/archinte.164.13.1457 [DOI] [PubMed] [Google Scholar]
- 7.Ting HH, Chen AY, Roe MT, et al. Delay from symptom onset to hospital presentation for patients with non-ST-segment elevation myocardial infarction. Arch Intern Med 2010;170:1834–41. 10.1001/archinternmed.2010.385 [DOI] [PubMed] [Google Scholar]
- 8.Saely CH, Aczel S, Koch L, et al. Diabetes as a coronary artery disease risk equivalent: before a change of paradigm? Eur J Cardiovasc Prev Rehabil 2010;17:94–9. 10.1097/HJR.0b013e32833100f0 [DOI] [PubMed] [Google Scholar]
- 9.Donahoe SM, Stewart GC, McCabe CH, et al. Diabetes and mortality following acute coronary syndromes. JAMA 2007;298:765–75. 10.1001/jama.298.7.765 [DOI] [PubMed] [Google Scholar]
- 10.Lakerveld J, Bot SD, Chinapaw MJ, et al. Motivational interviewing and problem solving treatment to reduce type 2 diabetes and cardiovascular disease risk in real life: a randomized controlled trial. Int J Behav Nutr Phys Act 2013;10:47 10.1186/1479-5868-10-47 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Glanz K, Rimer BK, Viswanath K. Health behavior and health education: theory, research, and practice. Hoboken, NJ: John Wiley & Sons, 2008. [Google Scholar]
- 12.Powers MA, Bardsley J, Cypress M, et al. Diabetes self-management education and support in type 2 diabetes: a joint position statement of the American Diabetes Association, the American Association of Diabetes Educators, and the Academy of Nutrition and Dietetics. Diabetes Educ 2017;43:40–53. [DOI] [PubMed] [Google Scholar]
- 13.Haas L, Maryniuk M, Beck J, et al. National standards for diabetes self-management education and support. Diabetes Educ 2012;38:619–29. 10.1177/0145721712455997 [DOI] [PubMed] [Google Scholar]
- 14.Fisher EB, Boothroyd RI, Coufal MM, et al. Peer support for self-management of diabetes improved outcomes in international settings. Health Aff 2012;31:130–9. 10.1377/hlthaff.2011.0914 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Tang PC, Overhage JM, Chan AS, et al. Online disease management of diabetes: engaging and motivating patients online with enhanced resources-diabetes (EMPOWER-D), a randomized controlled trial. J Am Med Inform Assoc 2013;20:526–34. 10.1136/amiajnl-2012-001263 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.American Diabetes Association. Standards of medical care in diabetes–2014. Diabetes Care 2014;37 Suppl 1:S14–80. 10.2337/dc14-S014 [DOI] [PubMed] [Google Scholar]
- 17.Jo Wu CJ, Chang AM, McDowell J. Perspectives of patients with type 2 diabetes following a critical cardiac event - an interpretative approach. J Clin Nurs 2008;17:16–24. 10.1111/j.1365-2702.2006.01926.x [DOI] [PubMed] [Google Scholar]
- 18.Becker LA OA. Chapter 22: overviews of reviews : Higgins JPT, Green S, Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0: The Cochrane Collaboration, 2011. [Google Scholar]
- 19.Chew DP, Scott IA, Cullen L, et al. National Heart Foundation of Australia and Cardiac Society of Australia and New Zealand: Australian clinical guidelines for the management of acute coronary syndromes 2016. Heart Lung Circ 2016;25:895–951. 10.1016/j.hlc.2016.06.789 [DOI] [PubMed] [Google Scholar]
- 20.Alberti KG, Zimmet PZ. Definition, diagnosis and classification of diabetes mellitus and its complications. part 1: diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med 1998;15:539–53. 10.1002/(SICI)1096-9136(199807)15:7<539::AID-DIA668>3.0.CO;2-S [DOI] [PubMed] [Google Scholar]
- 21.ThomsonReuters. EndNote version X7. 2016. http://endnote.com/product-details/x7
- 22.Shea BJ, Grimshaw JM, Wells GA, et al. Development of AMSTAR: a measurement tool to assess the methodological quality of systematic reviews. BMC Med Res Methodol 2007;7:10 10.1186/1471-2288-7-10 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Sharif MO, Janjua-Sharif FN, Sharif FN, et al. Systematic reviews explained: AMSTAR-how to tell the good from the bad and the ugly. Oral Health Dent Manag 2013;12:9–16. [PubMed] [Google Scholar]
- 24.Aromataris E, Fernandez R, Godfrey CM, et al. Summarizing systematic reviews: methodological development, conduct and reporting of an umbrella review approach. Int J Evid Based Healthc 2015;13:132–40. 10.1097/XEB.0000000000000055 [DOI] [PubMed] [Google Scholar]
- 25.Pieper D, Antoine SL, Mathes T, et al. Systematic review finds overlapping reviews were not mentioned in every other overview. J Clin Epidemiol 2014;67:368–75. 10.1016/j.jclinepi.2013.11.007 [DOI] [PubMed] [Google Scholar]
- 26.Ryan RE, Weir M, Leslie B, et al. Evidence on optimal prescribing and medicines use for decision makers: scope and application of the Rx for change database. J Pharm Pract Res 2011;41:295–9. 10.1002/j.2055-2335.2011.tb00107.x [DOI] [Google Scholar]
- 27.Sapkota S, Brien JA, Greenfield JR, et al. A systematic review of interventions addressing adherence to anti-diabetic medications in patients with type 2 diabetes. PLoS One 2015;10:e0128581 10.1371/journal.pone.0128581 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Walker RJ, Smalls BL, Bonilha HS, et al. Behavioral interventions to improve glycemic control in African Americans with type 2 diabetes: a systematic review. Ethn Dis 2013;23:401–8. [PMC free article] [PubMed] [Google Scholar]
- 29.Heinrich E, Schaper NC, de Vries NK. Self-management interventions for type 2 diabetes: a systematic review. European Diabetes Nursing 2010;7:71–6. 10.1002/edn.160 [DOI] [Google Scholar]
- 30.Alam R, Sturt J, Lall R, et al. An updated meta-analysis to assess the effectiveness of psychological interventions delivered by psychological specialists and generalist clinicians on glycaemic control and on psychological status. Patient Educ Couns 2009;75:25–36. 10.1016/j.pec.2008.08.026 [DOI] [PubMed] [Google Scholar]
- 31.Aldcroft SA, Taylor NF, Blackstock FC, et al. Psychoeducational rehabilitation for health behavior change in coronary artery disease: a systematic review of controlled trials. J Cardiopulm Rehabil Prev 2011;31:273–81. 10.1097/HCR.0b013e318220a7c9 [DOI] [PubMed] [Google Scholar]
- 32.Amaeshi IJ. Exploring the impact of structured foot health education on the rate of lower extremity amputation in adults with type 2 diabetes. A systematic review. Podiatry Now 2012;15:20–7. [Google Scholar]
- 33.Attridge M, Creamer J, Ramsden M, et al. Culturally appropriate health education for people in ethnic minority groups with type 2 diabetes mellitus. Cochrane Database Syst Rev 2014;9:CD006424 10.1002/14651858.CD006424.pub3 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Auer R, Gaume J, Rodondi N, et al. Efficacy of in-hospital multidimensional interventions of secondary prevention after acute coronary syndrome: a systematic review and meta-analysis. Circulation 2008;117:3109–17. 10.1161/CIRCULATIONAHA.107.748095 [DOI] [PubMed] [Google Scholar]
- 35.Barth J, Critchley J, Bengel J. Efficacy of psychosocial interventions for smoking cessation in patients with coronary heart disease: a systematic review and meta-analysis. Ann Behav Med 2006;32:10–20. 10.1207/s15324796abm3201_2 [DOI] [PubMed] [Google Scholar]
- 36.Barth J, Critchley JA, Bengel J. Psychosocial interventions for smoking cessation in patients with coronary heart disease. Cochrane Libr 2008. [DOI] [PubMed] [Google Scholar]
- 37.Brown JP, Clark AM, Dalal H, et al. Effect of patient education in the management of coronary heart disease: a systematic review and meta-analysis of randomized controlled trials. Eur J Prev Cardiol 2013;20:701–14. 10.1177/2047487312449308 [DOI] [PubMed] [Google Scholar]
- 38.Burke RE, Ferrara SA, Fuller AM, et al. The effectiveness of group medical visits on diabetes mellitus type 2 (dm2) specific outcomes in adults: a systematic review. JBI Libr Syst Rev 2011;9:833–85. 10.11124/01938924-201109230-00001 [DOI] [PubMed] [Google Scholar]
- 39.Chen L, Pei JH, Kuang J, et al. Effect of lifestyle intervention in patients with type 2 diabetes: a meta-analysis. Metabolism 2015;64:338–47. 10.1016/j.metabol.2014.10.018 [DOI] [PubMed] [Google Scholar]
- 40.Choi TS, Davidson ZE, Walker KZ, et al. Diabetes education for Chinese adults with type 2 diabetes: a systematic review and meta-analysis of the effect on glycemic control. Diabetes Res Clin Pract 2016;116:218–29. 10.1016/j.diabres.2016.04.001 [DOI] [PubMed] [Google Scholar]
- 41.Clark AM, Hartling L, Vandermeer B, et al. Meta-analysis: secondary prevention programs for patients with coronary artery disease. Ann Intern Med 2005;143:659–72. 10.7326/0003-4819-143-9-200511010-00010 [DOI] [PubMed] [Google Scholar]
- 42.Creamer J, Attridge M, Ramsden M, et al. Culturally appropriate health education for type 2 diabetes in ethnic minority groups: an updated cochrane review of randomized controlled trials. Diabet Med 2016;33:169–83. 10.1111/dme.12865 [DOI] [PubMed] [Google Scholar]
- 43.Deakin T, McShane CE, Cade JE, et al. Group based training for self-management strategies in people with type 2 diabetes mellitus. Cochrane Database Syst Rev 2005;2:CD003417 10.1002/14651858.CD003417.pub2 [DOI] [PubMed] [Google Scholar]
- 44.Devi R, Singh SJ, Powell J, et al. Internet-based interventions for the secondary prevention of coronary heart disease. Cochrane Database Syst Rev 2015;22:CD009386 10.1002/14651858.CD009386.pub2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Dickens C, Cherrington A, Adeyemi I, et al. Characteristics of psychological interventions that improve depression in people with coronary heart disease: a systematic review and meta-regression. Psychosom Med 2013;75:211–21. 10.1097/PSY.0b013e31827ac009 [DOI] [PubMed] [Google Scholar]
- 46.Duke SA, Colagiuri S, Colagiuri R. Individual patient education for people with type 2 diabetes mellitus. Cochrane Database Syst Rev 2009;1:CD005268. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Fan L, Sidani S. Effectiveness of diabetes self-management education intervention elements: a meta-analysis. Can J Diabetes 2009;33:18–26. 10.1016/S1499-2671(09)31005-9 [DOI] [Google Scholar]
- 48.Fernandez R, Griffiths R, Everett B, et al. Effectiveness of brief structured interventions on risk factor modification for patients with coronary heart disease: a systematic review. Int J Evid Based Healthc 2007;5:370–405. 10.1111/j.1479-6988.2007.00080.x [DOI] [PubMed] [Google Scholar]
- 49.Gary TL, Genkinger JM, Guallar E, et al. Meta-analysis of randomized educational and behavioral interventions in type 2 diabetes. Diabetes Educ 2003;29:488–501. 10.1177/014572170302900313 [DOI] [PubMed] [Google Scholar]
- 50.Ghisi GL, Abdallah F, Grace SL, et al. A systematic review of patient education in cardiac patients: do they increase knowledge and promote health behavior change? Patient Educ Couns 2014;95:160–74. 10.1016/j.pec.2014.01.012 [DOI] [PubMed] [Google Scholar]
- 51.Goulding L, Furze G, Birks Y. Randomized controlled trials of interventions to change maladaptive illness beliefs in people with coronary heart disease: systematic review. J Adv Nurs 2010;66:946–61. 10.1111/j.1365-2648.2010.05306.x [DOI] [PubMed] [Google Scholar]
- 52.Gucciardi E, Chan VW, Manuel L, et al. A systematic literature review of diabetes self-management education features to improve diabetes education in women of Black African/Caribbean and Hispanic/Latin American ethnicity. Patient Educ Couns 2013;92:235–45. 10.1016/j.pec.2013.03.007 [DOI] [PubMed] [Google Scholar]
- 53.Hawthorne K, Robles Y, Cannings-John R, et al. Culturally appropriate health education for type 2 diabetes mellitus in ethnic minority groups. Cochrane Database Syst Rev 2008;3:CD006424. [DOI] [PubMed] [Google Scholar]
- 54.Hawthorne K, Robles Y, Cannings-John R, et al. Culturally appropriate health education for type 2 diabetes in ethnic minority groups: a systematic and narrative review of randomized controlled trials. Diabet Med 2010;27:613–23. 10.1111/j.1464-5491.2010.02954.x [DOI] [PubMed] [Google Scholar]
- 55.Huang XL, Pan JH, Chen D, et al. Efficacy of lifestyle interventions in patients with type 2 diabetes: a systematic review and meta-analysis. Eur J Intern Med 2016;27:37–47. 10.1016/j.ejim.2015.11.016 [DOI] [PubMed] [Google Scholar]
- 56.Huttunen-Lenz M, Song F, Poland F. Are psychoeducational smoking cessation interventions for coronary heart disease patients effective? meta-analysis of interventions. Br J Health Psychol 2010;15(Pt 4):749–77. 10.1348/135910709X480436 [DOI] [PubMed] [Google Scholar]
- 57.Lun Gan JK, Brammer JD, Creedy DK. Effectiveness of educational interventions to promote oral hypoglycaemic adherence in adults with type 2 diabetes: a systematic review. JBI Libr Syst Rev 2011;9:269–312. 10.11124/01938924-201109090-00001 [DOI] [PubMed] [Google Scholar]
- 58.Khunti K, Camosso-Stefinovic J, Carey M, et al. Educational interventions for migrant South Asians with type 2 diabetes: a systematic review. Diabet Med 2008;25:985–92. 10.1111/j.1464-5491.2008.02512.x [DOI] [PubMed] [Google Scholar]
- 59.Kotb A, Hsieh S, Wells GA. The effect of telephone support interventions on coronary artery disease (CAD) patient outcomes during cardiac rehabilitation: a systematic review and meta-analysis. PLoS One 2014;9:e96581 10.1371/journal.pone.0096581 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Loveman E, Frampton GK, Clegg AJ. The clinical effectiveness of diabetes education models for type 2 diabetes: a systematic review. Health Technol Assess 2008;12:1–116. 10.3310/hta12090 [DOI] [PubMed] [Google Scholar]
- 61.Minet L, Møller S, Vach W, et al. Mediating the effect of self-care management intervention in type 2 diabetes: a meta-analysis of 47 randomised controlled trials. Patient Educ Couns 2010;80:29–41. 10.1016/j.pec.2009.09.033 [DOI] [PubMed] [Google Scholar]
- 62.Nam S, Janson SL, Stotts NA, et al. Effect of culturally tailored diabetes education in ethnic minorities with type 2 diabetes: a meta-analysis. J Cardiovasc Nurs 2012;27:505–18. 10.1097/JCN.0b013e31822375a5 [DOI] [PubMed] [Google Scholar]
- 63.Nield L, Moore HJ, Hooper L, et al. Dietary advice for treatment of type 2 diabetes mellitus in adults. Cochrane Database Syst Rev 2007;3:CD004097 10.1002/14651858.CD004097.pub4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Norris SL, Engelgau MM, Narayan KM. Effectiveness of self-management training in type 2 diabetes: a systematic review of randomized controlled trials. Diabetes Care 2001;24:561–87. 10.2337/diacare.24.3.561 [DOI] [PubMed] [Google Scholar]
- 65.Norris SL, Lau J, Smith SJ, et al. Self-management education for adults with type 2 diabetes: a meta-analysis of the effect on glycemic control. Diabetes Care 2002;25:1159–71. 10.2337/diacare.25.7.1159 [DOI] [PubMed] [Google Scholar]
- 66.Odnoletkova I, et al. Cost-Effectiveness of therapeutic education to prevent the development and progression of type 2 diabetes: systematic review. J Diabetes Metab 2014;05:438 10.4172/2155-6156.1000438 [DOI] [Google Scholar]
- 67.Pal K, Eastwood SV, Michie S, et al. Computer-based interventions to improve self-management in adults with type 2 diabetes: a systematic review and meta-analysis. Diabetes Care 2014;37:1759–66. 10.2337/dc13-1386 [DOI] [PubMed] [Google Scholar]
- 68.Pal K, Eastwood SV, Michie S, et al. Computer-based diabetes self-management interventions for adults with type 2 diabetes mellitus. Cochrane Database Syst Rev 2013;3:CD008776 10.1002/14651858.CD008776.pub2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Barth J, Jacob T, Daha I, et al. Psychosocial interventions for smoking cessation in patients with coronary heart disease. Cochrane Database Syst Rev 2015;7:CD006886 10.1002/14651858.CD006886.pub2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Brown JP, Clark AM, Dalal H, et al. Patient education in the management of coronary heart disease. Cochrane Database Syst Rev 2011;12:CD008895. [DOI] [PubMed] [Google Scholar]
- 71.Pillay J, Armstrong MJ, Butalia S, et al. Behavioral programs for type 2 diabetes mellitus: a systematic review and network meta-analysis. Ann Intern Med 2015;163:848–60. 10.7326/M15-1400 [DOI] [PubMed] [Google Scholar]
- 72.Terranova CO, Brakenridge CL, Lawler SP, et al. Effectiveness of lifestyle-based weight loss interventions for adults with type 2 diabetes: a systematic review and meta-analysis. Diabetes Obes Metab 2015;17:371–8. 10.1111/dom.12430 [DOI] [PubMed] [Google Scholar]
- 73.Ricci-Cabello I, Ruiz-Pérez I, Rojas-García A, et al. Characteristics and effectiveness of diabetes self-management educational programs targeted to racial/ethnic minority groups: a systematic review, meta-analysis and meta-regression. BMC Endocr Disord 2014;14:60 10.1186/1472-6823-14-60 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Saffari M, Ghanizadeh G, Koenig HG. Health education via mobile text messaging for glycemic control in adults with type 2 diabetes: a systematic review and meta-analysis. Prim Care Diabetes 2014;8:275–85. 10.1016/j.pcd.2014.03.004 [DOI] [PubMed] [Google Scholar]
- 75.van Vugt M, de Wit M, Cleijne WH, et al. Use of behavioral change techniques in web-based self-management programs for type 2 diabetes patients: systematic review. J Med Internet Res 2013;15:e279 10.2196/jmir.2800 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Steinsbekk A, Rygg LØ, Lisulo M, et al. Group based diabetes self-management education compared to routine treatment for people with type 2 diabetes mellitus. a systematic review with meta-analysis. BMC Health Serv Res 2012;12:213 10.1186/1472-6963-12-213 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Ramadas A, Quek KF, Chan CK, et al. Web-based interventions for the management of type 2 diabetes mellitus: a systematic review of recent evidence. Int J Med Inform 2011;80:389–405. 10.1016/j.ijmedinf.2011.02.002 [DOI] [PubMed] [Google Scholar]
- 78.Wens J, Vermeire E, Hearnshaw H, et al. Educational interventions aiming at improving adherence to treatment recommendations in type 2 diabetes: a sub-analysis of a systematic review of randomised controlled trials. Diabetes Res Clin Pract 2008;79:377–88. 10.1016/j.diabres.2007.06.006 [DOI] [PubMed] [Google Scholar]
- 79.Zabaleta AM, Forbes A. Structured group-based education for type 2 diabetes in primary care. Br J Community Nurs 2007;12:158–62. 10.12968/bjcn.2007.12.4.23251 [DOI] [PubMed] [Google Scholar]
- 80.Vermeire E, Wens J, Van Royen P, et al. Interventions for improving adherence to treatment recommendations in people with type 2 diabetes mellitus. Cochrane Database Syst Rev 2005;2:CD003638 10.1002/14651858.CD003638.pub2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Albrecht L, Archibald M, Arseneau D, et al. Development of a checklist to assess the quality of reporting of knowledge translation interventions using the workgroup for intervention development and evaluation research (WIDER) recommendations. Implement Sci 2013;8:52 10.1186/1748-5908-8-52 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Glazier RH, Bajcar J, Kennie NR, et al. A systematic review of interventions to improve diabetes care in socially disadvantaged populations. Diabetes Care 2006;29:1675–88. 10.2337/dc05-1942 [DOI] [PubMed] [Google Scholar]
- 83.Powers MA, Bardsley J, Cypress M, et al. Diabetes self-management education and support in type 2 diabetes: a joint position statement of the American Diabetes Association, the American Association of Diabetes Educators, and the Academy of Nutrition and Dietetics. Diabetes Care 2015;38:1372–82. 10.2337/dc15-0730 [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
bmjopen-2017-016857supp001.pdf (5.1MB, pdf)