Abstract
Objective
Volatile anaesthetics can inhibit the bronchociliary clearence in a dose- and time-dependend way. Moreover, they can have potential mutagenic/carcinogenic effects under chronic exposure. A genotoxicity test -micronuclei assay- was carried out in nasal epithelial cells to analyze the genotoxic effect of sevoflurane in adult patients undergoing general anesthesia.
Methods
In this study, micronucleus (MN) assay was conducted using nasal epithelial cells of 37 adult patients (age, 18–65 years) who underwent elective, minor, short surgical procedures under general anaesthesia with sevoflurane. Anaesthesia was induced and maintained using 8% sevoflurane (in 6 L min−1 of oxygen) and an inspired concentration of 2% in O2–air mixture, respectively. Nasal epithelial samples were collected at three time points: before anaesthesia induction (T1), after recovery from anaesthesia in the postanaesthesia care unit (T2) and on postoperative day 21 (T3).
Results
Sevoflurane significantly increased mean MN (‰) frequencies in nasal epithelial cells at T2 (6.97±2.33) and T3 (6.22±2.47) compared with those at T1 (3.84±1.89) (p<0.001). Similar result were observed for MN frequencies if the patients were analysed with regard to age (>40 or <40 years) or sex.
Conclusion
Short-term administration of sevoflurane anaesthesia induces MN formation in nasal epithelial cells of this patient population. Further studies are required for evaluation of the results. The prolonged administration of volatile anaesthetics in various risk groups and surgical protocols should be conducted for evaluating their safety.
Keywords: Volatile anaesthetics, sevoflurane, mask induction, genotoxicity, nasal epithelium
Introduction
Nasal cells are first-line protective cells of the respiratory system. Certain irritants, including volatile anaesthetics, are known to interfere with the first-line protective cells of the respiratory system at first. Therefore, when exfoliated mucosal cells come into contact with toxins that are present in inhaled air, they show changes that are detected using microscopy (1).
Intravenous induction and maintenance of general anaesthesia (GA) using sevoflurane is common practice in modern anaesthesia. Sevoflurane is currently the volatile anaesthetic of choice because it has a relatively lower solubility than other volatile anaesthetics and allows for rapid emergence and recovery. Besides, it is often used as an induction agent owing to its lack of airway irritation, which results in smooth induction (2, 3).
Although studies evaluating the genotoxicity of exposure to volatile anaesthetics have shown increased formation of chromosomal aberrations, micronuclei and sister chromatid exchanges (SCEs), in vitro and clinical studies evaluating the genotoxicity and mutagenicity of sevoflurane show conflicting results (2–7).
The analysis of micronucleus (MN) in exfoliated buccal and nasal cells is a sensitive method for monitoring genetic damage in human populations, especially because of its non-invasive application nature (8). The micronuclei MNi are extranuclear DNA-containing bodies that are formed because of chromosomal breakage (clastogenicity) and/or chromosome loss (9, 10). They can be microscopically evaluated. In the literature, there are 16 studies related to the use of nasal cells in MN assays, which mainly focus on the effects of formaldehyde (11).
This study determined MNi in nasal epithelial cells of patients undergoing minor ear and throat surgeries via volatile induction and maintenance. The MN assay was performed for nasal epithelial cells that were collected from patients both before anaesthesia induction (as control), at recovery, and at 3 weeks after anaesthesia induction.
Methods
With the approval of the Ethics Committee (Ankara Atatürk Training and Research Hospital-29.06.2009–2009/06/12) and written informed consent, 37 ASA I–II consecutive adult patients (18–65 years), undergoing elective, minor ear and throat surgical procedures (tympanoplasty, myringoplasty and tonsillectomy) were enrolled during 6 months’ study period. During the preoperative visit, the patients answered standardised health questionnaires related to their medical history, exposure factors and lifestyle factors such as smoking, drug consumption and diseases, in case such factors had a confounding effect.
Preoperatively, the patients were asked to rinse their noses with water; then, a pre-moistened nasal smear brush was used to obtain sample cells from both the sides of the interior nostrils. The sampling was performed at three predetermined time points. The first predetermined time point was in the operating room before inducing anaesthesia (control; T1). Standard monitoring including electrocardiogram, non-invasive blood pressure and pulse oximeter (SpO2) was applied. GA was induced using 2 μg kg−1 fentanyl and sevoflurane inhalation till the loss of eyelash reflex ( 8% sevoflurane in 6 L min−1 of oxygen). Endotracheal intubation was then performed with 0.6 mg kg−1 rocuronium. For maintaining anaesthesia, MAC values of 0.5–1.5 sevoflurane in O2–air mixture were used. Mechanical ventilation was controlled to maintain end-tidal carbon dioxide at 32–35 mmHg. The inhaled anaesthetic concentration was adjusted to obtain moderate controlled hypotension (MAP, 65–75 mmHg) because even minimal bleeding in these ear and throat surgeries impairs the surgeon’s vision and increases the duration of surgery. Vital signs were measured before (baseline) and after anaesthesia induction and at every 5 min throughout the surgery using Datex Ohmeda S5. At the end of the surgical procedure, extubated patients were transferred to the postanaesthesia care unit, and as soon as the modified Aldrete recovery score was >9, the patients were regarded as being able to shift to their clinical ward; second (T2) sampling from the nasal epithelial cells was performed as soon as the patients could get into cooperation with the anaesthesiologist. At discharge from the hospital, the patients were informed about visiting the hospital for another sampling from the nose. Three weeks after the surgery (21 days after anaesthesia induction), the patients were asked to visit the hospital for a third sampling (T3). The study ended after the third sample from each participating patient was collected. Recent studies have shown that the migration of damaged cells from the basal layer to the surface takes 2–3 weeks, and the cells then divide and MN are formed (12).
Analysis of MN
Smears were air dried and fixed using 80% methanol. Slides were stained using Feulgen reaction stain and then counter-stained with Fast Green stain (13). The stained slides were viewed under oil immersion at ×100 magnification to identify and record the MN count. To minimise the bias during evaluation, all slides were coded before evaluation. All slides were examined to identify MN, and 1500 differentiated per subject were blindly scored by the same scorer. The criteria of scoring were described by Sarto et al. (14) and Tolbert et al. (15). While counting, care was taken to avoid inclusion of cells that exhibited features of degeneration and apoptosis. Counting was avoided in cell clusters and clumps. MN was determined according to a standard criteria (Figure 1) (14–15). MN frequencies were expressed as MN per thousand (‰).
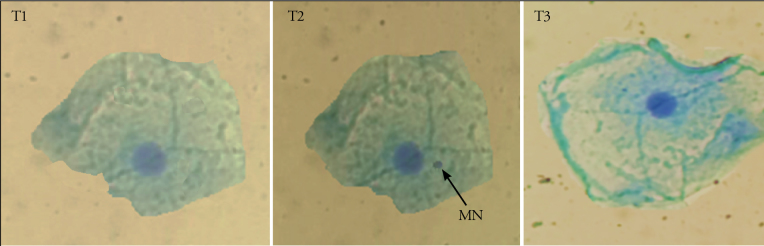
Figure 1.
The number of micronucleus, counted at T2, in the nasal epithelial cell of a patient
Sample size estimation
The primary aim of this study was to determine the difference in MN frequencies among the sampling time points. A total sample size of 33 was required to detect at least 1.0 unit difference in MN frequency between any of two sampling time points, with a power of 80% at a significance level of 5%. The 1.0 unit difference was taken from both our pilot study and former studies. The sample size was estimated using the G*Power v3.0.10 (Franz Faul, Universität Kiel, Kiel, Germany) software.
Statistical analysis
Data analysis was performed using Statistical Package for the Social Sciences for Windows v11.5 (SPSS Inc., Chicago, IL, USA). Whether the continuous variables were normally distributed or not was determined using Shapiro–Wilk test. Descriptive statistics were presented as mean±SD for continuous variables, and the number of cases and (%) were used for categorical data.
The mean differences in MN frequencies, between groups were compared by Student’s t-test. Whether the differences in MN frequencies among the sampling time points were statistically significant or not was evaluated by repeated measurements using ANOVA with Wilks’ lambda test. When the p value obtained from Wilks’ lambda test is statistically significant to know which sampling time point differs from which others, Bonferroni adjusted multiple comparison test was used. A p value of <0.05 was considered to be statistically significant.
Results
The mean age of the patients was 47.6±14.5 years, and 32.4% of the patients was aged <40 years; 59.5% of the patients were males. The durations of anaesthesia and surgery were 83.5±21.2 min (mean ±SD) and 72.7± 21.3 min (mean±SD), respectively. The non-smokers accounted for 70.3% of the patients (Table 1).
Table 1.
Demographic data of the study group
| Characteristics | n=37 |
|---|---|
| Age (years, %) | 47.6±14.5 |
| Sex | |
| Male | 22 (59.5%) |
| Female | 15 (40.5%) |
| Smoking | |
| Smoker | 11 (29.7%) |
| Non-smoker | 26 (70.3%) |
| Weight (kg, %) | 82.0±11.8 |
| Height (cm, %) | 167.5±8.3 |
| Malignancy in the family | 16 (43.2%) |
| Diabetes in the family | 16 (43.2%) |
| Obesity in the family | 12 (32.4%) |
| Hypertension in the family | 15 (40.5%) |
Values are mean ±SD or number (%).
There was a statistically significant formation of MN, both at T2 and T3 compared with that at T1 (p<0.001). However, there was no statistically significant difference between MN frequencies sampled at T2 and T3.
With respect to sampling time points, similar MN frequencies were observed when the patients were compared according to age (<40 or >40 years) or sex. All patients had a significant increase at T2 compared with that at T1 (Table 2).
Table 2.
The frequencies of MN with respect to sampling times
| T1 | T2 | T3 | p† | |
|---|---|---|---|---|
| All patients (n=37) | 3.84±1.89 | 6.97±2.33a | 6.22±2.47b | <0.001 |
| Age groups | ||||
| ≤40 years (n=12) | 3.17±2.04 | 6.67±1.92a | 5.50±2.65 | 0.005 |
| >40 years (n=25) | 4.16±1.77 | 7.12±2.52a | 6.56±2.36b | <0.001 |
| p‡ | 0.137 | 0.586 | 0.227 | |
| Sex | ||||
| Male (n=22) | 4.00±1.63 | 6.64±1.81a | 6.45±2.52b | <0.001 |
| Female (n=15) | 3.60±2.26 | 7.47±2.92a | 5.87±2.45b | <0.001 |
| p‡ | 0.536 | 0.339 | 0.486 | |
| Smoking | ||||
| Non-smoker (n=26) | 3.65±1.92 | 6.58±2.32a | 6.11±2.67b | <0.001 |
| Smoker (n=11) | 4.27±1.85 | 7.91±2.16a | 6.45±2.02b | <0.001 |
| p‡ | 0.371 | 0.113 | 0.709 | |
Comparison of MN frequencies among in all groups with repeated measurements of ANOVA and Wilks’ lambda test.
Comparison of MN frequencies among all groups with Student’s t-test,
T1 vs. T2 (p<0.01),
T1 vs. T3 (p<0.01).
Male smokers (n=5) showed no statistically significant difference at T2 and T3 (p>0.0125), whereas female smokers (n=6) had a statistically significant difference at all sampling time points (p=0.009), such that MN frequencies were higher at T2 than at T1 (p=0.012). In patients aged >40 years and non-smokers (n=19), there was a significant increase in MN numbers at T2 and T3 compared with those at T1 (p<0.001 and p=0.002).
Discussion
Our results indicate that sevoflurane, induces MN formation in nasal epithelium of adults, which is ultimately not a long-lasting effect in otherwise healthy individuals.
The nasal epithelium of patients is exposed to high levels of anaesthetic gases both during mask induction and at the end of anaesthesia by exhalation of the gases. We collected samples at three time points according to the developmental stages of nasal epithelium and sevoflurane concentrations. At the first time point, the cells collected (as control) were free of the effects of sevoflurane. At the second time point, the cells were still exposed to sevoflurane. At recovery, the concentrations decreased. However, during anaesthesia maintenance, for haemodynamic stabilisation, N2O, midazolam or extra fentanyl doses were avoided. We adjusted sevoflurane concentration (MAC value, 0.5–1.5) to maintain moderate controlled hypotension. The age range of our patient population was 18–65 years, implying that sevoflurane consumption would be altered among patients owing to a wide age range. This may have resulted in a fluctuant depth of anaesthesia, causing a non-homogeneous effect of sevoflurane on MN formation. This is one of the weak points of our study.
We collected the third samples in the third week because the division and differentiation of basal cells in nasal turbinates to olfactory epithelium takes approximately 2–4 weeks (12). There are different reports regarding the analysis of MN in different epithelial cells after exposure to different chemicals. However, Nersesyan advised to select a time point between 14 and 28 days after exposure if only one time point was chosen because the exact time point for sampling remain unknown (12). Thus, 21 days after anaesthesia induction was preferred, and the MN frequency increased after exposure to sevoflurane, followed by a small decrease. However, this may be interpreted as another limitation of our study.
At third sampling time point, we observed a decreasing trend in MN frequencies. As the time point corresponded to the turnover time of epithelial cells, we evaluated this decreasing trend to be a reversible effect of sevoflurane.
Successful inhalation induction with sevoflurane for adults is well established. The most important degradation product of sevoflurane, compound A, is a vinyl-ether that directly acts as an alkylating agent in cellular targets, including DNA. In the literature, studies have reported conflicting data concerning the genotoxic and mutagenic potential of sevoflurane on operating room personnel. Factors such as sevoflurane concentration, fresh gas flow rate, ventilation rate, temperature and humidity of carbon dioxide absorbent and pre-existing status of the patient, as well as the type and duration of surgery might play an important role (16). However, there is limited data regarding the effects that occur on patients who are exposed to these agents. Braz et al. (8) showed that isoflurane did not induce strand breaks or alkali-labile sites in lymphocytes of ASA I patients who underwent tympanoplasty and septoplasty. In another study, in which sevoflurane was used, DNA strand breaks were detected on postoperative day 1 (17). Kadıoglu et al. (18) reported reversible genotoxic effects of 1%–1.5% sevoflurane in patients who underwent mastectomy. In these studies, sevoflurane was used for maintaining anaesthesia at approximately 1.5%–2% concentration after intravenous induction. The results of our study differ from those of the aforementioned studies. Another study, similar to our study in the aspect of inhalational induction, could not show increased frequencies of SCE in lymphocytes (19).
In a comparison study with halothane and isoflurane, Szyfter et al. (3) studied the potential genotoxic effects of sevoflurane on human peripheral blood lymphocytes using the comet assay. No increase in DNA migration could be demonstrated by sevoflurane, which is in contrast to previously studied anaesthetics. Furthermore, prolonged exposure of operating room personnel to sevoflurane did not show any DNA degradation (3). In another study, Karabiyik et al. (5) studied the possible genotoxic properties of two inhalation anaesthetics, namely sevoflurane and isoflurane, in peripheral blood lymphocytes of patients before, during and after anaesthesia. At 120 min of anaesthesia, the DNA damage detected in lymphocytes of patients was similar under sevoflurane and isoflurane anaesthesia. The induced DNA damage was completely repaired on postoperative day 5 (5). Akin et al. (20) investigated the genotoxic effects of another volatile agent, desflurane, on the frequency of SCE in peripheral blood lymphocytes of patients during and after anaesthesia at different time points. This was different from our study with regard to both the agent used and the method of genotoxicity assessed. However, they also showed a significant increase in the number of SCEs on postoperative days 1, 3 and 7. Similar to our study, the numbers measured postoperatively (on postoperative day 12) were not different from those measured preoperatively.
As far as we know, to date, only one study has evaluated genomic instability, cell death and proliferative index in exfoliated buccal cells of anaesthesiologists who had chronic exposure and those of non-anaesthesiologist physicians who were not exposed to anaesthetics (21). The authors concluded that exposure to modern waste anaesthetic gases did not induce systemic DNA damage, but it did result in genomic instability, cytotoxicity and proliferative changes, which were detected in exfoliated buccal cells of anaesthesiologists. We could not compare all aspects of our results to those of Souza’s study because the study populations and sevoflurane exposure times and routes were different between the two studies.
We observed that smokers who aged >40 years did not show a significant increase in MN frequencies at T3. However, the increase in the non-smoker group was significant at T2 and T3 compared with that at T1. This could be attributed to the effect of sevoflurane solely. Besides, in smokers, adaptive host defence mechanisms have been developed (22). The smoke might cause the promotion of tissue inflammation and production of high amounts of free radicals, which are remarkably reactive. The activities of oxidative enzyme systems and lipid peroxidation are all increased in these patients, leading to the mounted ability of a protective adaptive response (23).
In fact, the association between MN frequencies and the age of the patients was evaluated in only few studies. In our study, the patients aged >40 years had increased MN frequencies. This was probably owing to accumulating free radical damage in their cells over time. Overall, anaesthetic stress augmented the results.
In this study, female smokers had a higher preoperative MN frequency than female non-smokers. Interestingly, this was not the same in male smokers. Actually, this unexpected difference, observed under anaesthesia, could be attributed to the sex difference. However, the low patient numbers (11 smokers versus 26 non-smokers) are limitations of this study with respect to statistical analysis and interpretation.
Conclusion
We demonstrated for the first time with clinical data that sevoflurane induces MN formation, which is exacerbated by age. Anaesthesia and cigarette smoking promote activities of oxidative enzyme systems as expected in otherwise healthy patients.
Footnotes
Ethics Committee Approval: Ethics committee approval was received for this study from the ethics committee of Ankara Atatürk Training and Research Hospital.
Informed Consent: Written informed consent was obtained from patients who participated in this study.
Peer-review: Externally peer-reviewed.
Author Contributions: Concept – E.K., B.K.; Design – S.İ., E.K.; Supervision – B.K.; Resources – T.M., E.K.; Materials – E.C., G.U.; Data Collection and/or Processing – E.K.; Analysis and/or Interpretation – E.K., B.K.; Literature Search – E.K., B.K.; Writing Manuscript – E.K.; Critical Review – E.K., B.K., E.C.; Other – G.U.
Conflict of Interest: No conflict of interest was declared by the authors.
Financial Disclosure: The authors declared that this study has received no financial support.
References
- 1.Feron VJ, Arts JH, Kuper CF, Slootweg PJ, Woutersen RA. Health risks associated with inhaled nasal toxicants. Crit Rev Toxicol. 2001;31:313–47. doi: 10.1080/20014091111712. https://doi.org/10.1080/20014091111712. [DOI] [PubMed] [Google Scholar]
- 2.Wiesner G, Schiewe-Langgartner F, Lindner R, Gruber M. Increased formation of sister chromatid exchanges, but not of micronuclei, in anesthetists exposed to low levels of sevoflurane. Anaesthesia. 2008;63:861–4. doi: 10.1111/j.1365-2044.2008.05498.x. https://doi.org/10.1111/j.1365-2044.2008.05498.x. [DOI] [PubMed] [Google Scholar]
- 3.Szyfter K, Szulc R, Miktstacki A, Stachecki I, Rydzanicz M, Jałoszyński P. Genotoxicity of inhalation anaesthetics: DNA lesions generated by sevoflurane in vitro and in vivo. J Appl Genet. 2004;45:369–74. [PubMed] [Google Scholar]
- 4.Natarajan D, Santhiya ST. Cytogenetic damage in operation theatre personnel. Anaesthesia. 1990;45:574–7. doi: 10.1111/j.1365-2044.1990.tb14834.x. https://doi.org/10.1111/j.1365-2044.1990.tb14834.x. [DOI] [PubMed] [Google Scholar]
- 5.Karabiyik L, Şardaş S, Polat U, Kocabaş NA, Karakaya AE. Comparison of genotoxicity of sevoflurane and isoflurane in human lymphocytes studied in vivo using the comet assay. Mutat Res. 2001;492:99–107. doi: 10.1016/s1383-5718(01)00159-0. https://doi.org/10.1016/S1383-5718(01)00159-0. [DOI] [PubMed] [Google Scholar]
- 6.Kaymak C, Kadioglu E, Coskun E, Basar H, Basar M. Determination of DNA damage after exposure to inhalation anesthetics in human peripheral lymphocytes and sperm cells in vitro by comet assay. Human Exp Toxicol. 2012;31:1207–13. doi: 10.1177/0960327112446818. https://doi.org/10.1177/0960327112446818. [DOI] [PubMed] [Google Scholar]
- 7.Orosz JE, Braz LG, Ferreira AL, Amorim RB, Salvadori DM, Yeum KJ, et al. Balanced anesthesia with sevoflurane does not alter redox status in patients undergoing surgical procedures. Mutat Res Genet Toxicol Environ Mutagen. 2014;773:29–33. doi: 10.1016/j.mrgentox.2014.07.007. https://doi.org/10.1016/j.mrgentox.2014.07.007. [DOI] [PubMed] [Google Scholar]
- 8.Braz MG, Mazoti MÁ, Giacobino J, Braz LG, Golim Mde A, Ferrasi AC, et al. Genotoxicity, cytotoxicity and gene expression in patients undergoing elective surgery under isoflurane anaesthesia. Mutagenesis. 2011;26:415–20. doi: 10.1093/mutage/geq109. https://doi.org/10.1093/mutage/geq109. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Balmus G, Karp NA, Ng BL, Jackson SP, Adams DJ, McIntyre RE. A high-throughput in vivo micronucleus assay for genome instability screening in mice. Nat Protoc. 2015;10:205–15. doi: 10.1038/nprot.2015.010. https://doi.org/10.1038/nprot.2015.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.González-Arias CA, Benitez-Trinidad AB, Sordo M, Robledo-Marenco L, Medina-Díaz IM, Barrón-Vivanco BS, et al. Low doses of ochratoxin A induce micronucleus formation and delay DNA repair in human lymphocytes. Food Chem Toxicol. 2014;74:249–54. doi: 10.1016/j.fct.2014.10.006. https://doi.org/10.1016/j.fct.2014.10.006. [DOI] [PubMed] [Google Scholar]
- 11.Knasmueller S, Holland N, Wultsch G, Jandl B, Burgaz S, Misík M, et al. Use of nasal cells in micronucleus assays and other genotoxicity studies. Mutagenesis. 2011;26:231–8. doi: 10.1093/mutage/geq079. https://doi.org/10.1093/mutage/geq079. [DOI] [PubMed] [Google Scholar]
- 12.Nersesyan AK. The best sampling time in buccal micronucleus cytome assay. Int J Occup Med Environ Health. 2012;25:310–3. doi: 10.2478/S13382-012-0018-6. [DOI] [PubMed] [Google Scholar]
- 13.Khlifi R, Trabelsi-Ksibi F, Chakroun A, Rebai A, Hamza-Chaffai A. Cytogenetic abnormality in exfoliated cells of buccal mucosa in head and neck cancer patients in the Tunisian population: impact of different exposure sources. Biomed Res Int. 2013;2013:905252. doi: 10.1155/2013/905252. https://doi.org/10.1155/2013/905252. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Sarto F, Finotto S, Giacomelli L, Mazzotti D, Tomanin R, Levis AG. The micronucleus assay in exfoliated cells of the human buccal mucosa. Mutagenesis. 1987;2:11–7. doi: 10.1093/mutage/2.1.11. https://doi.org/10.1093/mutage/2.1.11. [DOI] [PubMed] [Google Scholar]
- 15.Tolbert PE, Shy CM, Allen JW. Micronuclei and other nuclear anomalies in buccal smears: methods development. Mutat Res. 1992;271:69–77. doi: 10.1016/0165-1161(92)90033-i. https://doi.org/10.1016/0165-1161(92)90033-I. [DOI] [PubMed] [Google Scholar]
- 16.Rozgaj R, Kasuba V, Brozović G, Jazbec A. Genotoxic effects of anaesthetics in operating theatre personnel evaluated by the comet assay and micronucleus test. Int J Hyg Environ Health. 2009;212:11–7. doi: 10.1016/j.ijheh.2007.09.001. https://doi.org/10.1016/j.ijheh.2007.09.001. [DOI] [PubMed] [Google Scholar]
- 17.Alleva R, Tomasetti M, Solenghi MD, Stagni F, Gamberini F, Bassi A, et al. Lymphocyte DNA damage precedes DNA repair or cell death after orthopaedic surgery under general anaesthesia. Mutagenesis. 2003;18:423–8. doi: 10.1093/mutage/geg013. https://doi.org/10.1093/mutage/geg013. [DOI] [PubMed] [Google Scholar]
- 18.Kadioglu E, Sardas S, Erturk S, Ozatamer O, Karakaya AE. Determination of DNA damage by alkaline halo and comet assay in patient under sevoflurane anesthesia. Toxicol Ind Health. 2009;25:205–12. doi: 10.1177/0748233709106445. https://doi.org/10.1177/0748233709106445. [DOI] [PubMed] [Google Scholar]
- 19.Krause T, Scholz J, Jansen L, Boettcher H, Koch C, Wappler F, et al. Sevoflurane anaesthesia does not induce the formation of sister chromatid exchanges in peripheral blood lymphocytes of children. Br J Anaesth. 2003;90:233–5. doi: 10.1093/bja/aeg030. https://doi.org/10.1093/bja/aeg030. [DOI] [PubMed] [Google Scholar]
- 20.Akin A, Ugur F, Ozkul Y, Esmaoglu A, Gunes I, Ergul H. Desflurane anaesthesia increases sister chromatid exchanges in human lymphocytes. Acta Anaesthesiol Scand. 2005;49:1559–61. doi: 10.1111/j.1399-6576.2005.00779.x. https://doi.org/10.1111/j.1399-6576.2005.00779.x. [DOI] [PubMed] [Google Scholar]
- 21.Souza KM, Braz LG, Nogueira FR, Souza MB, Bincoleto LF, Aun AG, et al. Occupational exposure to anesthetics leads to genomic instability, cytotoxicity and proliferative changes. Mutat Res. 2016;791–792:42–8. doi: 10.1016/j.mrfmmm.2016.09.002. [DOI] [PubMed] [Google Scholar]
- 22.Wiseman H, Halliwell B. Damage to DNA by reactive oxygen and nitrogen species: role in inflammatory disease and progression to cancer. Biochem J. 1996;313:17–29. doi: 10.1042/bj3130017. https://doi.org/10.1042/bj3130017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Fahn HJ, Wang LS, Kao SH, Chang SC, Huang MH, Wei YH. Smoking-associated mitochondrial DNA mutations and lipid peroxidation in human lung tissues. Am J Respir Cell Mol Biol. 1998;19:901–9. doi: 10.1165/ajrcmb.19.6.3130. https://doi.org/10.1165/ajrcmb.19.6.3130. [DOI] [PubMed] [Google Scholar]