Abstract
Reports regarding the changes in sperm concentration in different counties of the world are inconsistent. Furthermore, the reports that sprung up from specific epidemiological and experimental examinations did not include data of prior studies or geographical variations. The current study, following a previous report of massive fall in semen volume over the past 33 years, attempts to delineate the trend of altering sperm concentrations and factors responsible for this by reviewing article published from 1980 to July 2015 with geographic differences. The current study identified an overall 57% diminution in mean sperm concentration over the past 35 years (r = −.313, p = .0002), which, when analyzed for each geographical region, identified a significant decline in North America, Europe, Asia, and Africa. An increasing trend of sperm concentration was identified only in Australia. The association of male age with such a trend (R2 = .979) is reported. The authors also correlated male fertility with sperm concentration. Thus, this comprehensive, evidence-based literature review aims to concisely and systematically present the available data on sperm concentration from 1980 to 2015, as well as to statistically analyze the same and correlate male health with the declining pattern of sperm count in a single scientific review to serve the scientific research zone related to reproductive health. It points to the threat of male infertility in times ahead.
Keywords: semen quality, sperm concentration, sperm count
Introduction
There has been recent controversy regarding changes in sperm counts during the past 60 years worldwide (Sengupta, 2014a). It has been reported widely in last two decades that sperm count is declining (Table 1). Subsequently, Rolland, Le Moal, Wagner, Royère, and De Mouzon (2013) reported a 32% decline in sperm count from 1989 to 2005. The deterioration of semen qualities was first reported in 1974 by Nelson and Bunge. Since then, reports published regarding the changes in human semen parameters have been inconsistent. Nieschlag, Lammers, Freischem, Langer, and Wickings (1982) reported no changes, while Ng et al. (2004) revealed significantly different seminal volumes in different age groups. In 1992, Carlsen, Giwercman, Keiding, and Skakkebaek reported a worldwide decline in sperm counts in a meta-analysis of 61 studies between 1938 and 1990 evaluating the semen analyses of 14,947 presumably fertile men from 23 countries. Swan, Elkin, and Fenster (1997) published a reanalysis of the studies included by Carlsen et al. (1992). In that investigation, they reported significant declines in sperm count in the United States, Europe, and Australia, but no such decline in non-Western countries. Similar declines were also proclaimed by numerous other studies, but a clear cause was unable to be established (Auger, Kunstmann, Czyglik, & Jouannet, 1995; Swan et al., 1997). A recent article reported a decline in semen volume in aging males over the past 33 years (Sengupta, 2015). Because of reduced semen volumes, sperm concentrations were increased in older men. Moreover, significantly increased serum follicle-stimulating hormone levels sometime reflect in testicular spermatogenic function (Luetjens, Rolf, Gassner, Werny, & Nieschlag, 2002). Inhibin B as a possible marker for spermatogenesis identifies a moderate but significant decrease reflecting the aging process that possibly affects spermatogenesis (Mahmoud et al., 2003).
Table 1.
Studies on Changes of Sperm Concentrations in Different Age Groups (1980 to July 2015).
| Country | Population | Sample size (n) | Male age definition (range/mean/group, in years) | Direction of effect with increasing age | Study |
|---|---|---|---|---|---|
| Nigeria | Cohort study | 53 | 20-45 | ↓ (p < .01) | Lapido (1980) |
| United States | Cohort study | 63 | No age data | ↓ (p < .001) | Venable, McClimans, Flake, and Dimick (1980) |
| United States | Cohort study | 90 | No age data | ↓ (p < .001) | Milby and Whorton (1980) |
| Hong Kong | Andrology laboratory | 15 | 20-40 | ↓ (p < .001) | Wang and Yeung (1980) |
| United States | Andrology laboratory | 89 | 19-53 | ↓ (p < .05) | Meyer (1981) |
| Norway | Andrology laboratory | 51 | 20-45 | ↓ (p < .01) | Aabyholm (1981) |
| United States | Andrology laboratory | 132 | No age data | ↓ (p < .01) | Dougherty et al. (1981) |
| United States | Andrology laboratory | 112 | >35 | ↓ (p < .05) | Fariss et al. (1981) |
| Finland | Andrology laboratory | 13 | A. 25-53; B. 31-47 | ↓ (p < .01) | Frick, Danner, Joos, Kunit, and Luukkainen (1981) |
| United States | Andrology laboratory | 34 | No age data | ↓ (p < .005) | Wyrobek, Brodsky, et al. (1981) |
| United States | Andrology laboratory | 26 | No age data | ↓ (p < .01) | Wyrobek, Watchmaker, et al. (1981) |
| United Kingdom | Andrology laboratory | 35 | >25 | ↓ (p < .01) | Aitken, Best, Richardson, Djahanbakhch, and Lees (1982) |
| United States | Cohort study | 90 | 21-45 | ↓ (p < .05) | Hamill et al. (1982) |
| United States | Infertility clinic | 570 | A. 22-30; B. 31-40; C. 41-50; D. >50 | ↔ (NS) | Benzi, Pastoris, and Dossena (1982) |
| United States | Independent sampling | 4,435 | 21-45 | ↔ | Tjoa, Smolensky, His, Steinberger, Smith (1982) |
| Israel | Infertility clinic | 555 | A. 31 (0.2); B. 54 (4.2) | ↓ (p < .05) | Homonnai, Fainman, David, and Paz (1982) |
| Germany | Volunteers responding to advertisement | 43 | A. 29 (3.2); B. 67 (7.8) | ↑ (p < .05) | Nieschlag et al. (1982) |
| Egypt | Andrology laboratory | 45 | 19-53 | ↓ (p < .01) | Shaarawy and Mahmoud (1982) |
| France | Semen donors | 809 | A. 21-25; B. 26-30; C. 31-35; D. 36-40; E. 41-45; F. 46-50 | ↔ (NS) | Schwartz et al. (1983) |
| United States | Andrology laboratory | 22 | >40 | ↔ | Borghi and Asch (1983) |
| United Kingdom | Andrology laboratory | 38 | 20-45 | ↓ (p < .01) | Stanwell-Smith et al. (1983) |
| Sweden | Cohort study | 63 | 21-50 | ↓ (p < .01) | Osser, Gennser, Liedholm, and Ranstam (1983) |
| Libya | Infertility clinic | 1,500 | 20-45 | ↓ (p < .01) | Sheriff (1983) |
| Germany | Andrology laboratory | 25 | 25-36 | ↓ (p < .005) | Wickings, Freischem, Langer, and Nieschlag (1983) |
| Brazil | Andrology laboratory | 501 | A. 24-29; B. 30-34; C. 35-39; D. 40-44; E. >45 | ↓ (p < .05) | de Castro and Mastrorocco (1984) |
| United States | Andrology laboratory | 36 | 21-45 | ↔ | Swanson, Mayer, Jones, Lanzendorf, and McDowell (1984) |
| United Kingdom | Andrology laboratory | 47 | 23-50 | ↓ (p < .001) | Richardson, Aitken, and Loudon (1984) |
| Australia | Sperm donors | 119 | 20-40 | ↔ | Handelsman, Conway, Boylan, and Turtle (1984) |
| Israel | Andrology laboratory | 12 | 20-45 | ↓ (p < .05) | Laufer, Margalioth, Navot, Shemesh, and Schenker (1985) |
| United States | Andrology lab | 9 | No age data | ↓ (p < .05) | Lewis, Brazil, and Overstreet (1984) |
| Greece | Cohort study | 114 | 31.9 | ↓ (p < .01) | Panidis, Asseo, and Papaloucas (1984) |
| France | Andrology laboratory | 52 | No age data | ↓ (p < .05) | Spira (1984) |
| United States | Cohort study | 11 | No age data | ↓ (p < .05) | Ward et al. (1984) |
| United States | Cohort study | 71 | A. 31.6; B. 34.9 | ↓ (p < .001) | Rosenberg et al. (1985) |
| United States | Andrology laboratory | 50 | No age data | ↓ | Heussner, Ward, and Legator (1985) |
| Hong Kong | Family planning clinic | 1,239 | 19-53 | ↔ (NS) | Wang et al. (1985) |
| Thailand | Andrology laboratory | 307 | 19-50 | ↓ (p < .05) | Aribarg, Kenkeerati, Vorapaiboonsak, Leepipatpaiboon, and Farley (1986) |
| United States | Andrology laboratory | 12 | 20-45 | ↓ (p < .01) | Levin, Latimore, Wein, and Van Arsdalen (1986) |
| United States | Andrology laboratory | 42 | A. 20-25; B. 50-55 | ↓ | Rui, Thomassen, Oldereid, and Purvis (1986) |
| Nigeria | Cohort study | 100 | 20-45 | ↓ (p < .01) | Osegbe, Amaku, and Nnatu (1986) |
| Germany | Cohort study | 239 | 19-40 | ↔ (NS) | Vogt, Heller, and Borelli (1986) |
| Italy | Andrology laboratory | 18 | 20-45 | ↓ (p < .025) | Assennato et al. (1987) |
| Hong Kong | Andrology laboratory | 36 | No age data | ↓ (p < .05) | Chan and Wang (1987) |
| United States | Andrology laboratory | 190 | No age data | ↔ | Saaranen, Suonio, Kauhanen, and Saarikoski (1987) |
| United States | Andrology laboratory | 43 | No age data | ↓ (p < .05) | Ratcliffe et al. (1987) |
| Libya | Cohort study | 10 | No age data | ↓ (p < .01) | Sheriff (1987) |
| Tanzania | Andrology laboratory | 120 | 19-55 | ↓ (p < .01) | Kirei (1987) |
| United Kingdom | Andrology laboratory | 49 | No age data | ↓ (p < .05) | Barratt, Dunphy, Thomas, and Cooke (1988) |
| United States | Andrology laboratory | 28 | 19-53 | ↔ | Giblin, Poland, Moghissi, Ager, and Olson (1988) |
| Kuwait | Andrology laboratory | 20 | 20-45 | ↓ (p < .0001) | Ibrahim, Moussa, and Pedersen (1988) |
| Denmark | Andrology laboratory | 14 | A. 20-62; B. 29-42 | ↔ (NS) | Rasmussen et al. (1988) |
| Denmark | Cohort study | 68 | No age data | ↓ (p < .05) | Jelnes (1988) |
| United States | Andrology laboratory | 40 | 19-53 | ↓ (p < .01) | Welch, Schrader, Turner, and Cullen (1988) |
| Brazil | Cohort study | 12 | 20-50 | ↓ (p < .01) | Coutinho and Melo (1988) |
| United States | Cohort study | 45 | 20-45 | ↓ (p < .01) | Schrader, Turner, Breitenstein, and Simon (1988) |
| United Kingdom | Cohort study | 104 | 21-45 | ↓ (p < .01) | Badenoch, Evans, and McCloskey (1989) |
| Nigeria | Cohort study | 20 | 19-53 | ↓ (p < .001) | Sobowale and Akiwumi (1989) |
| France | Andrology laboratory | 1222 | No age data | ↓ (p < .05) | Pol, Beuscart, Leroy-Martin, Hermand, and Jablonski (1989) |
| United Kingdom | Andrology laboratory | 15 | 21-39 | ↓ (p < .01) | Shrivastav et al. (1989) |
| Denmark | Cross-sectional study | 54 | A. 33.7; B. 30.6; B. 34.5 | ↓ (p < .05) | Bonde (1990) |
| Brazil | Andrology laboratory | 1890 | No age data | ↓ (p < .05) | de Castro, Jeyendran, and Zaneveld (1990) |
| Israel | Sperm donors | 1,283 | 34.3 (0.2) | ↑ (NS) | Singer, Sagiv, Levinsky, and Allalouf (1990) |
| China | Andrology laboratory | 19 | 20-45 | ↓ (p < .01) | Zhong et al. (1990) |
| Germany | Andrology laboratory | 25 | Mean age 31.0 | ↔ | Cooper, Jockenhövel, and Nieschlag (1991) |
| United States | Andrology laboratory | 48 | 20-45 | ↓ (p < .01) | Eskenazi et al. (1991) |
| Nigeria | Andrology laboratory | 21 | 19-24 | ↓ (p < .05) | Nnatu, Giwa-Osagie, and Essien (1991) |
| Canada | Andrology laboratory | 20 | No age data | ↓ (p < .05) | Sugkraroek, Kates, Leader, and Tanphaichitr (1991) |
| France | Andrology laboratory | 20 | 24-40 | ↓ (p < .05) | Vignon et al. (1991) |
| Germany | Andrology laboratory | 42 | 20-40 | ↓ (p < .01) | Weidner, Jantos, Schiefer, Haidl, and Friedrich (1991) |
| United States | Andrology laboratory | 10 | No age data | ↓ (p < .01) | Kolon, Philips, and Buch (1992) |
| United States | Andrology laboratory | 142 | No age data | ↓ (p < .05) | Levine et al. (1992) |
| Libya | Cohort study | 1,250 | 19-53 | ↓ (p < .01) | Sheriff and Legnain (1992) |
| Germany | Andrology laboratory | 22 | 20-45 | ↓ (p < .001) | Noack-Fuller, De Beer, and Seibert (1993) |
| United Kingdom | Andrology laboratory | 28 | 23-40 | ↓ (p < .001) | Wallace, Gow, and Hu (1993) |
| Denmark | Andrology laboratory | 42 | No age data | ↓ (p < .05) | Fedder, Askjaer, and Hjort (1993) |
| Ireland | Andrology laboratory | 10 | No age data | ↓ (p < .05) | Cottell and Harrison (1995) |
| Saudi Arabia | Andrology laboratory | 50 | No age data | ↓ (p < .05) | el Shoura et al. (1995) |
| Germany | Older men planning further children | 64 | A. 32.2; B. 50.3 | ↓ (p < .01) | Haidl, Jung, and Schill (1996) |
| Spain | Assisted conception | 345 | A. ≤30; B. 31-40; C. 41-50; D. 51-64 | ↑ (NS) | Gallardo et al. (1996) |
| Germany | Infertility clinic | 78 | A. <30 (matched by year of attendance); B. <30 (matched by wives’ ages); C. >50 | ↑ (NS) | Rolf, Behre, and Nieschlag (1996) |
| Finland | Sperm donors | 5,719 | 28-40 | ↓ (p < .05) | Vierula et al. (1996) |
| Italy | Cohort study | 50 | 20-45 | ↓ (p < .001) | Figa-Talamanca et al. (1996) |
| Denmark | Andrology laboratory | 141 | No age data | ↓ (p < .001) | Jensen, Giwercman, Carlsen, Scheike, and Skakkebaek (1996) |
| United States | Cohort study | 31 | No age data | ↓ (p < .05) | Weyandt, Schrader, Turner, and Simon (1996) |
| Israel | Sperm donors | 188 | 18-53 | ↓ (p < .0001) | Benshushan, Shoshani, Paltiel, Schenker, and Lewin (1997) |
| Australia | Volunteers responding to advertisement | 689 | 21-54 | ↓ (p < .05) | Handelsman (1997) |
| Denmark | Cohort study | 1,055 | 20-30 | ↔ (NS) | Rasmussen, Erb, Westergaard, and Laursen (1997) |
| East cape province | Cohort study | 400 | >37 | ↓ (p < .001) | Robins et al. (1997) |
| United States | Assisted conception | 821 | A. ≤39; B. 40-49; C. ≥50 | ↔ (NS) | Spandorfer, Avrech, Colombero, Palermo, and Rosenwaks (1998) |
| Spain | Infertility clinic | 20,411 | 31.9 (5.4); 15-74 | ↑ (p < .004) | Andolz, Bielsa, and Vila (1999) |
| United States | Andrology laboratory | 2,065 | 33.6 (5.8); 19-67 | ↓ (p < .02) | Centola and Eberly (1999) |
| Slovenia | Infertility clinic | 2,343 | 21-45 | ↔ | Zorn, Virant-Klun, Verdenik, and Meden-Vrtovec (1999) |
| Denmark | Sperm donors | 1,273 | A. ≤35; B. >35 | ↓ (p < .0001) | Gyllenborg, Skakkebæk, Nielsen, Keiding, and Giwercman (1999) |
| Denmark and Finland | Comparative clinical study | 632 | A. 20-35 (Danish); B. 22-47 (Finnish) | ↓ (p < .0001) | Jensen et al. (2000) |
| Slovenia | Cohort study | 444 | A. ≤35; B. >35 | ↔ (NS) | Acacio, Gottfried, Israel, and Sokol (2000) |
| Australia | Sperm donors | 448 | 18-40 | ↔ (NS) | Costello, Sjoblom, Haddad, Steigrad, and Bosch (2002) |
| Germany | Infertility laboratory | 200 | A. 21-25; B. >50 | ↓ (p < .05) | Jung, Schuppe, and Schill (2002) |
| Brazil | Cohort study | 127 | 14-20 | ↓ (p < .001) | Mori, Cedenho, Koifman, and Srougi (2002) |
| United States | Fertility clinic | 1,176 | 31.2 | ↓ (p < .05) | Eskenazi et al. (2003) |
| India | Cohort study | 97 | 22-80 | ↓ (p < .005) | Marimuthu, Kapilashrami, Misro, and Singh (2003) |
| United States | Cohort study | 551 | 25-59 | ↑ | Chen et al. (2003) |
| United States | Cohort study | 201 | 20-45 | ↓ (p < .0001) | Toft, Pedersen, and Bonde (2003) |
| Brazil | Infertility patients | 889 | A. ≤45; B. >45 | ↓ | Pasqualotto, Sobreiro, Hallak, Pasqualotto, and Lucon (2005) |
| Denmark | Cohort study | 551 | ≤35 | ↑ | Carlsen, Swan, Petersen, and Skakkebæk (2005) |
| United States | Andrology laboratory | 1,174 | >45 | ↓ | Hellstrom et al. (2006) |
| India | Andrology laboratory | 368 | 25-59 | ↓ | Pal et al. (2006) |
| Japan | Cohort study | 324 | 25-40 | ↓ (p < .0001) | Iwamoto et al. (2006) |
| India | Infertility clinic | 7,770 | 20-45 | ↓ (p < .001) | Adiga, Jayaraman, Kalthur, Upadhya, and Kumar (2008) |
| Nigeria | Infertility clinic | 170 | 25-40 | ↓ (p < .001) | Ugwuja, Ugwu, and Ejikeme (2008) |
| Australia | Infertility clinic | 225 | >30 | ↓ | Stewart et al. (2009) |
| Germany | Fertility center | 320 | A. <30; B. 30-35; C. 36-39; D. >40 | ↔ (NS) | Winkle, Rosenbusch, Gagsteiger, Paiss, and Zoller (2009) |
| Tunisia | Infertility clinic | 2,940 | 20-45 | ↓ (p < .001) | Feki et al. (2009) |
| India | Andrology laboratory | 3,729 | A. 33; B. 35 (of two decades) | ↓ (p < .005) | Mukhopadhyay et al. (2010) |
| Korea | Andrology laboratory | 1,139 | A. 19-27; B. >54 | ↓ | Bahk, Jung, Jin, and Min (2010) |
| Argentina | Cohort study | 9,168 | 20-77 | ↓ (p < .05) | Molina et al. (2010) |
| Netherlands | Periconceptional prospective cohort study | 227 | 26-59 | ↓ (p < .01) | Hammiche et al. (2011) |
| Sweden | Andrology laboratory | 511 | 25-40 | ↔ (NS) | Axelsson, Rylander, Rignell-Hydbom, and Giwercman (2011) |
| Australia | Infertility clinic | 114 | 23-64 | ↓ (p < .01) | Giles et al. (2011) |
| Nigeria | Cohort study | 106 | 20-45 | ↓ (p < .01) | Akande, Isah, Sekoni, and Pam (2011) |
| Finland | Andrology laboratory | 858 | 18-19 | ↓ (p < .01) | Jorgensen et al. (2011) |
| China | Andrology laboratory | 104 | A. <35; B. 35-39; C. ≥40 | ↔ (NS) | Nie et al. (2012) |
| Denmark | Danish one-center study | 4,867 | A. 18-19; B. >54 | ↑ (p < .02) | Jorgensen et al. (2012) |
| France | Andrology laboratory | 10,932 | A. ≤35; B. >35 | ↓ (p < .05) | Geoffroy-Siraudin et al. (2012) |
| Nigeria | Infertility clinic | 316 | 20-40 | ↓ (p < .05) | Jimoh, Olawui, and Olaiya Omotoso (2012) |
| China | Infertility clinic | 201 | A. 20-40; B. 40-60; C. >60 | ↓ | Diao et al. (2013) |
| India | Infertility clinic | 100 | A. ≤30; B. >30 | ↓ | Jajoo and Kalyani (2013) |
| Brazil | Infertility clinic | 2,300 | 33-39 | ↓ (p < .001) | Borges et al. (2013) |
| Japan | Cohort study | 792 | 20-45 | ↓ (p < .01) | Iwamoto et al. (2013) |
| France | Cohort study | 26,609 | 18-70 | ↓ (p < .05) | Rolland et al. (2013) |
| China | Fertility clinic | 1,152 | 18-50 | ↓ (p < .01) | Tang et al. (2013) |
| United States | Infertility clinic | 5,081 | 16.5-72.3 | ↓ | Stone, Alex, Werlin, and Marrs (2013) |
| India | Fertility clinic | 435 | 31-44 | ↓ (p < .05) | Nirupa et al. (2014) |
| United States | Cohort study | 10,665 | No age data | ↓ (p < .05) | Belloc et al. (2014) |
| United States | Cohort study | 11,935 | Mean age 36.6 | ↓ | Eisenberg et al. (2014) |
| Spain | Cohort study | 992 | 25-40 | ↓ (p < .05) | Romero-Otero et al. (2015) |
| United States | Observational prospective cohort | 501 | Mean age 31.8 | ↓ (p < .05) | Eisenberg, Chen, Ye, and Buck Louis (2015) |
| China | Cohort study | 1,213 | No age data | ↓ | Tang et al. (2015) |
| Tunisia | Andrology laboratory | 116 | Males of mean age 32.74 | ↔ (NS) | Hadjkacem Loukil, Hadjkacem, Bahloul, and Ayadi (2015) |
Note. Data are represented as mean (SD); ↓ = decrease; ↑ = increase; ↔ = no change; NS = not significant at p < .05; no p value indicates that no statistical testing was done.
Changes in sperm count can occur after occupational and environmental exposure to toxic agents (Dutta, Joshi, Sengupta, & Bhattacharya, 2013; Sengupta & Banerjee, 2014) or from predisposing factors of the host, such as age (Kidd, Eskenazi, & Wyrobek, 2001). The innumerable evidences, mostly from clinical studies, suggest that age is associated with all the concomitant factors, resulting in diminished sperm concentration (Spandorfer et al., 1998). Men at older ages (e.g., ≥50 years) were underrepresented in many clinical studies, which restricts statistical strength and prevents unveiling of the exact form of relationship between age and sperm concentration. In addition, potential confounders that might explain changes with age, such as smoking history or duration of abstinence, were hardly ever taken into consideration (Wyrobek et al., 1983).
A detailed scrutiny of diverse studies from specific cites reveals evidence of decline in sperm concentration, but a worldwide decline has not been demonstrated. It is arduous to execute a systematic, scientific study regarding the decline in human semen quality. Thus, the objective of the current review is to build up a substantial idea regarding alterations in sperm concentration in humans by picking the huge scattered reports of the past 35 years, molding them in sequential pattern, and statistically analyzing and correlating the worldwide declining sperm count trend with male fertility.
Data Extraction and Data Analysis
Research articles on humans published in English from 1980 through July 2015 were included in the current report. The authors also included 32 of 61 reports of the study by Carlsen et al. (1992), that is, reports from 1980 to 1992. The authors selected publications about sperm concentration with predefined criteria for inclusion and exclusion, as follows. (1) The non-Carlsen studies published during 1980 to July 2015 were identified by using Medical Subject Headings (MeSH) of electronic databases, which included Medline, National Library of Medicine, Bethesda, MD, with the following key words: sperm count, sperm density, sperm concentration, semen quality, male infertility, and semen analysis. (2) Relevant literature on changes of sperm concentration and its influence on future natural and assisted conception cycles were retrieved. (3) Data on subjects with clinical problems were been excluded. (4) Studies with insufficient numbers of subjects (n < 5) were excluded. In each case, sperm concentration and its outcome were evaluated. Analytic epidemiological studies were emphasized. Therefore, the current analysis was based on 138 studies published in from 1980 to 2015 (July). In the Results section, the relative changes in the outcome with age are represented. Whenever possible, the differences between younger men (i.e., ages ≤30 years) and older men (i.e., ages ≥50 years) were summarized. The authors also analyzed the correlation of age with mean sperm concentration obtained from the published studies with proper age data. For simple statistical analyses (calculation of mean sperm concentration, median values, and Box-and-Whisker plots), Microsoft Excel 2013 was used. Correlation and regression analyses of data were done using StatSoft (2011). Correlation coefficient was considered to be significant if p was <.05 or <.001 (Fisher & Yates, 1974). Mean sperm concentrations of all 138 reports were also analyzed with linear regression weighted by number of subjects included in the individual publications.
Description of Data
During the retrieval of relevant documents, the authors found a total of 138 studies that reported temporal decline in sperm concentration in the past 35 years. The outcomes of these studies are represented in Table 1. Most of the reports are based on andrology laboratories or assisted conception populations (44.20%) and epidemiological studies (28.26%), while others used volunteers recruited from sperm banks or advertisements (6.52%) and infertility clinics (16.67%). Among the 138 published research works discussed in this article from 1980 through 2015, most were carried out in Europe, North America, and Asia, while others were carried out in South America, Australia, and Africa. Most of the studies used sample sizes less than 500 subjects (68.12%) and ≥1,000 (21.01%), while a few studies used sample sizes between 500 and 1,000 subjects (10.87%). Five reports used an extraordinarily large sample size (>10,000; Andolz et al., 1999; Belloc et al., 2014; Eisenberg et al., 2014; Geoffroy-Siraudin et al., 2012; Rolland et al., 2013). Out of 138 reports, 80.43% provided data about the age of subjects. No significant alterations in sperm concentration was identified in 15.94% of the reports, only 3.62% reports identified a significant increase, and 80.43% reports identified a significant decrease in sperm concentration from 1980 to 2015. While only the reports identifying significant decrease were taken into consideration, it was observed that out of 111 studies, 23.42% of reports identified strong significance. The current report also enlisted interval studies published during the reporting period of the current article, which proclaims alterations in sperm concentrations during 1980 to 2015 (Table 2).
Table 2.
Summary of Interval Studies Reporting Decline in Sperm Concentration Published Within the Study Period of the Current Report.
| Publication date | Author | Location | Study period | Sample size |
|---|---|---|---|---|
| 1996 | Irvine, Carwood, Richardson, MacDonald, and Aitken | Scotland | 1984-1995 | 577 |
| 1996 | De Mouzon et al. | France | 1989-1994 | 7,714 |
| 1997 | Berling and Wolner-Hanssen | Sweden | 1985-1995 | 718 |
| 1997 | Benshushan et al. | Israel | 1980-1995 | 188 |
| 1998 | Younglai et al. | Canada | 1984-1995 | 48,968 |
| 1998 | Bonde et al. | Denmark | 1986-1995 | 1,196 |
| 1999 | Zorn et al. | Slovenia | 1983-1996 | 2,343 |
| 1999 | Bilotta et al. | Italy | 1981-1995 | 1,068 |
| 1999 | Zhang et al. | China | 1983-1996 | 9,292 |
| 2002 | Costello et al. | Australia | 1983-2001 | 448 |
| 2003 | Almagor et al. | Israel | 1990-2000 | 2,638 |
| 2003 | Chen et al. | United States | 1989-2000 | 551 |
| 2003 | Marimuthu et al. | India | 1990-2000 | 97 |
| 2003 | Vicari et al. | Italy | 1982-1999 | 716 |
| 2005 | Lackner et al. | Austria | 1986-2003 | 7,780 |
| 2007 | Sripada et al. | Scotland | 1994-2005 | 4,832 |
| 2008 | Liang et al. | China | 1980-2005 | 5,834 |
| 2009 | Feki et al. | Tunisia | 1996-2007 | 2,940 |
| 2010 | Molina et al. | Argentina | 1994-2004 | 9,168 |
| 2012 | Geoffroy-Siraudin et al. | France | 1988-2007 | 10,932 |
| 2012 | Haimov-Kochman et al. | Israel | 1995-2009 | 2,182 |
| 2013 | Menidola et al. | Spain | 2001-2011 | 273 |
State of Affairs: Past 35 Years
Worldwide Variations
Mean sperm concentrations were obtained either directly from the published articles or in some cases arithmetic mean was calculated from median or geometric mean. Linear regression analysis identified a significant decrease between 1980 and 2015 from 91.65 × 106/mL to 39.34 × 106/mL (r = −.313, p = .0002). This reflected almost a 57% decline in sperm count worldwide from 1980 (Figure 1A). The current study also identifies that recruitment of a larger population for this type of study increased predominantly after 1995.
Figure 1.
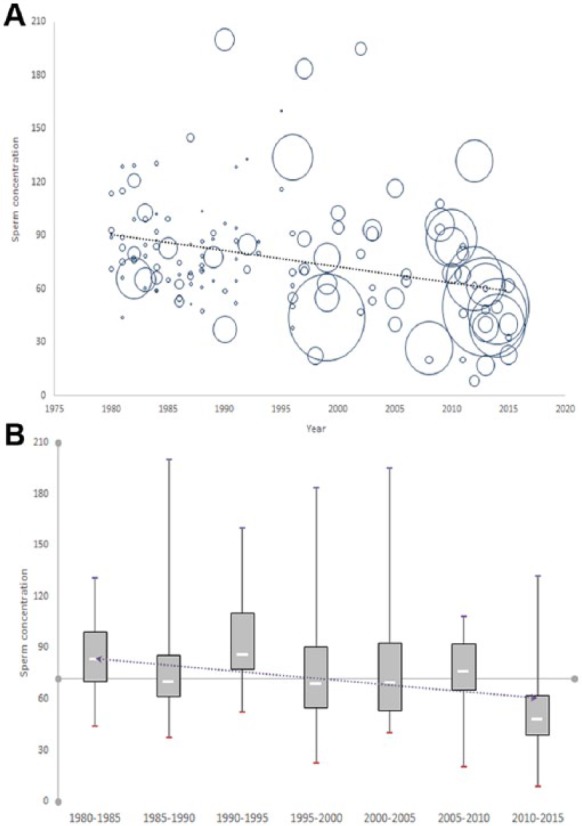
(A) Temporal decline in sperm concentration (×106/mL) (r = −.313, p = .0002, R2 = .098); bubble size corresponds to the number of men in study. (B) Changes in sperm concentrations from 1980 to 2015 shown as Box-and-Whisker plots. White bands indicate the median values for each duration. The Y-intercept shows median (71.6 × 106/mL), and the regression band (y = −3.92x + 87.72, R2 = .460) indicates significant decline from 1980 to 2015.
Median values of sperm concentrations were calculated in seven different intervals (from 1980-1985 to 2010-2015). The median value was reported to be 71.6 × 106/mL during the study period. These values are plotted in the Box-and-Whisker plot in Figure 1B, which also identifies a significant decline from 1980-1985 to 2010-2015 (y = −3.92x + 87.72, R2 = .460).
Regional Variations
Recent studies on the male reproductive system bring conflicting evidence to the forefront regarding sperm counts, with some reporting significant decline while some have reported no change. North America, Europe, Asia, and Africa are more prone to a declining trend of sperm counts over the years, whereas studies based in South America and Australia do not depict such a trend (Figures 2 and 3). An overview of the sperm counts obtained from data produced by various regions of the world is reported in Figure 1, which identifies that there was a significant decline in sperm concentrations from 1980 to 2015. However, a striking feature of much of the data is the surfacing of regional differences in semen quality. It has been suggested that these regional differences in sperm counts possibly are biologically meaningful. Most of the controversies that have aroused from past clinical studies about semen quality may be partly due to involvement of only few selected groups of men. In many studies, historical data collected for other purposes have been used without close attention to important and specific factors relevant to an analysis of secular or geographical trends.
Figure 2.
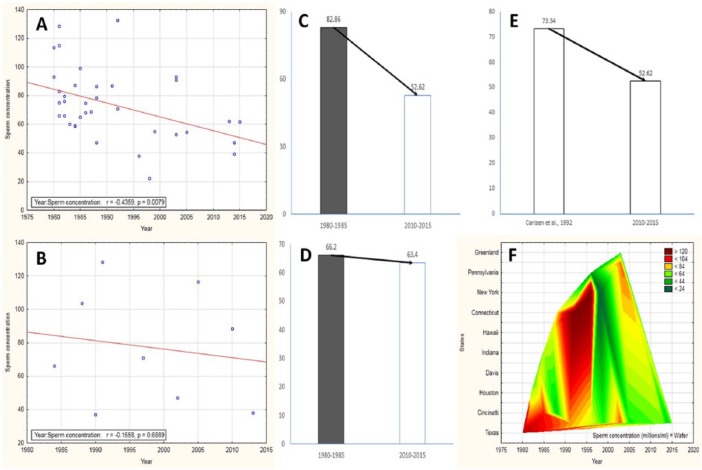
(A) Correlation plot shows significant decline in sperm concentration in North America (r = −.435, p = .007), but no such alteration in South America (B). It has decreased 36.49% in North America (C) and only 4.22% in South America (D) from 1980 to 2015. A comparative overview of Carlsen et al., 1992 and this study reveals a further 28.25% decline after that report in North America (E). Wafer plot reveals that New York and Connecticut have the highest sperm count (F).
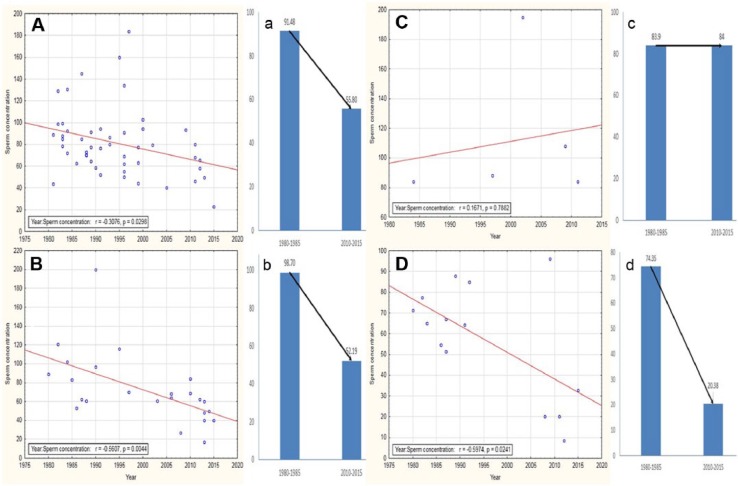
Figure 3.
(A) Correlation plots of non-American continents showed significant reduction in sperm concentrations in Europe (r = −.307, p = .02) (A), Asia (r = −.560, p = .004) (B), and Africa (r = −.597, p = .02) (D), while Australia showed an increasing trend in sperm concentration over time (r = .167, p = .788) (C). Mean sperm concentrations reflected similar trends (a-d).
North America
Numerous studies conducted in the United States have demonstrated a declining trend of mean sperm concentration in different regions over the years 1980 to 2015 (r = −.435, p = .007; Figure 2A). Data on sperm counts procured from several studies from 1938 to 1980 (following the report of Saidi et al., 1999) also depicts a significant decrease in sperm count (r = −.635, p = .004) in North American men until 1980. Thus, from these two findings it can be resolved that North American states are going on with the trend of declining sperm counts from 1938 until 2015. The authors also evaluated the mean sperm concentrations in 1980-1985 and 2010-2015, which identified a 36.49% decline in sperm concentration over the last 35 years (Figure 2C). The current study also compares the mean sperm concentrations of 2015 with the report of Carlsen et al. published in 1992. It reveals an additional 28.25% decline in mean sperm concentration after 1992 in North American men (Figure 2E).
Various scattered reports were brought under one analytical review by Saidi et al. (1999) using 29 studies based in the United States from 1938 to 1996, which analyzed semen of 9,612 fertile men. The mean sperm concentrations of selected geographic locations were determined with analysis of variance (ANOVA), and any alterations were gauged with time using linear regression analysis. From that study, it was perceptible that New York had the highest value for mean sperm concentration as compared to the other sates of the United States (as also reported by Fisch & Goluboff, 1996). It can be explained through Figure 2F, which attempts to describe the variations in sperm count among states in North America and also indicates that New York and Connecticut have the highest sperm count in the United States. Thus, sperm concentrations were reported to vary with geographical areas in the United States, the maximum being that of New York whose exact reason is yet to be identified, but factors like climate, socioeconomic status, ethnicity, and other environmental and social factors should be considered.
South America
Only a handful of studies have been conducted involving regions of South America to assess the trend of declining, increasing, or static sperm counts as well as changes of the same from place to place across the continent (Borges et al., 2013; Oliva, Spira, & Multigner, 2001; Pasqualotto et al., 2005; Tortolero et al., 1999). A study in Venezuela, carried out on the male partners of infertile couples, suggested that the proportion of men presenting azoospermia or oligospermia showed no change from 1981 and 1995 (Tortolero et al., 1999). Studies also focused on the impact of chemical exposures on various characteristics of sperm among the populations of male partners of infertile couples during the period 1995 to 1998 in the southern coastal region of Argentina (Oliva et al., 2001).
Studies retrieved during the current analysis identified that most of the reports were from Brazil and Argentina. These reports indicated no such significant alteration in sperm count in South American men (r = −.155, p = .688; Figure 2B). The mean sperm concentrations have declined from 66 × 106/mL to 63.4 × 106/mL, which is only 4.22% relative to that of 1980 (Figure 2D). A presumption about the role of environmental and occupational factors on male reproductive health can be drawn through the above-mentioned studies (Oliva et al., 2001; Tortolero et al., 1999) and the declining trend of the sperm count (though not significant at p of .05). For example, agricultural zones of South America are cursed by exposure to organochlorine pesticides and other endocrine disruptors, which might be more detrimental to fertility in the coming years.
Europe
Europe is a continent of geographic diversities. The current report included 50 studies carried out from 1980 to 2015. Most of these were conducted in the United Kingdom, France, Denmark, and Finland. The analysis revealed a significant decline in sperm concentrations over time (r = −.307, p = .02; Figure 3A), and the mean sperm concentration have declined more than 39% compared to 1980 (Figure 3A). Among the European countries, the United Kingdom and Denmark had the maximum sperm concentrations, while Spanish men were reported to have the least sperm counts. Similar cross-sectional studies were performed by Møller and Skakkebæk (1999) and Skakkebæk et al. (1998) to investigate the possible geographical differences in sperm count, involving subjects who were male partners of pregnant women from Denmark, France, Scotland, and Finland and young men from the general populations in Denmark, Norway, Finland, Estonia, and Lithuania. These studies identified a significantly better semen quality in Finland, Estonia, and Lithuania from which an East-West gradient is revealed in the European area. A major factor that has an immense impact on sperm count is seasonal changes, which is evident from the fact that sperm count differed by about 30% in summer from that in winter in all the four countries. This fact is also supported by all other previous studies, some including men of known fertility and some of known subfertility, which observed seasonal variations in sperm count being lowest during the summer and highest during autumn or winter (Gyllenborg et al., 1999; Maier, Newbold, & McLachlan, 1985; Spira, 1984; Tjoa et al., 1982). There are a few studies that could not detect any seasonal variations (e.g., Mallidis, Howard, & Baker, 1991).
Time trends in semen quality are interestingly related with almost identical patterns in the occurrence of testicular cancer, which is rising worldwide. It was reported that the incidence of this disease is five times higher among Danish men than it is among Finnish men (Adami et al., 1994; Forman & Møller, 1994), while in the previously discussed study the former had a much better sperm count. Such inverse relationship between sperm count and the risk of testicular cancer is not only apparent from the cohort studies but is also observed in individuals (Møller & Skakkebæk, 1999). This could also be supported by the study that predicts that men born in Scandinavia during the Second World War had a comparatively lower risk of developing testicular cancer in adult life than men who were born before or after the war (Adami et al., 1994; Møller & Skakkebæk, 1999). Sperm counts are thought to decline with a more recent year of birth as is suggested by a couple of studies (Irvine et al., 1996; Skakkebæk et al., 1998), for which a possible causative agent could be exogenous factors that interfere with the functions and multiplication of the fetal Sertoli cells resulting in a syndrome of reduced sperm count, hypospadias, undescended testis, and testicular cancer (Bergman, Brandt, & Brouwer, 1996; Sharpe & Skakkebæk, 1993). In this respect, it is noteworthy that the gradient in the incidence of hypospadias between Denmark and Finland is apparently parallel to the gradient of the testicular cancer in these regions (Toppari et al., 1996). Thus, it can be concluded that European cities suffer from robust variations in sperm count, which is even related to sperm production and testicular cancer. These variations might be due to differences in life styles, environmental factors, endocrine disruptions, or other factors.
Asia
Most of the Asian studies were carried out in China (Diao et al., 2013; Nie et al., 2012; ; Tang et al., 2013; Tang et al., 2015; Wang et al., 1985) and India (Jajoo & Kalyani, 2013; Marimuthu et al., 2003; Mehta, Makwana, Ranga, Srinivasan, & Virk, 2006; Mukhopadhyay et al., 2010; Pal et al., 2006), and a few in Japan (Iwamoto et al., 2013), Israel (Benshushan et al., 1997; Homonnai et al., 1982; Laufer et al., 1985; Singer et al., 1990), and Saudi Arabia (el Shoura et al., 1995).
In 1980, Wang and Yeung first reported a decline in sperm count in Chinese men. Later, numerous studies reported similar observations (Diao et al., 2013; Nie et al., 2012). In Japan, studies on altering sperm concentrations in males are scarce. Thus, very limited information could be gathered regarding male reproductive status. A severe declining trend or variations in sperm quality has been reported by few cross-sectional studies in Japan (Iwamoto et al., 2013). India has a medley of cultures, religions, life styles, and most importantly geographic and climatic diversities according to which the physical attributes of the people belonging to each region have been molded. Therefore, variations in physicality and thereby reproductive health status of men are most likely to occur among different regions of this country. Not many studies have been done to analyze such predictions (Jajoo & Kalyani, 2013; Marimuthu et al., 2003; Mukhopadhyay et al., 2010; Pal et al., 2006). However, a relevant study was conducted in laboratories at five different cities, namely, Bangalore, Kurnool, Mumbai, Jalandhar, and Jodhpur, using sperm samples from male partners of infertile couples. Samples were analyzed for sperm concentrations using standardized methods recommended by the World Health Organization (WHO). The outcome of the study suggested that prevalence of both azoospermia and oligozoospermia was highest in Kurnool, being 38.2% and 51%, respectively. The observation from the mean sperm counts in normospermic men depicts lower values for the metropolitan cities like Mumbai and Bangalore than other small cities (Mehta et al., 2006).
Current analysis reveals a similar trend of declining sperm count in males based in Asia, which is similar to the U.S. and European countries. The current report identifies a significant decline in mean sperm concentration (47.12%) from 1980 to 2015 (r = −.560, p = .004; Figure 3B-b). This may be attributable to lifestyle, food habits, and the extensive use of fertilizers in cultivation. Gui-Yuan, Meng-Chun, Jin-Lai, and Wen-Qing (1989) demonstrated that a probable cause of such declining sperm concentrations in India might be due to extensive use of Gossypol (a phenol compound isolated from the seeds, stems, and roots of the cotton plant) and other pesticides.
Africa
In 1991, the WHO had estimated that almost 20 to 35 million couples were infertile in Africa. Nigeria is suggested to have been suffering from highest infertility problems among the other African regions, with the male infertility factor accounting for 40% to 50%. The degree of infertility and its cause vary from place to place. This is evident from the study pursued in mid-western Nigeria, which reported that about 50% of the 780 couples under evaluation differed in the causes of their infertility (Okonofua, Menakaya, Onemu, Omo-Aghaja, & Bergstrom, 2005). A study associated with south-western Nigeria had reported that 42.4% of infertility resulted from the male factor (Ikechebula, Adinma, Orie, & Ikegwuonu, 2003).
In the current analysis, the authors identified that most of the studies on sperm count in Africa was carried out in Nigeria (Akande et al., 2011; Jimoh et al., 2012; Lapido, 1980; Nnatu et al., 1991; Osegbe et al., 1986; Sobowale & Akiwumi, 1989; Ugwuja et al., 2008). A time-dependent decline in sperm concentration was observed from 1980 to 2015 (r = −.597, p = .02; Figure 3D) that reflected an overall 72.58% decrease in sperm concentration (Figure 3D-d). It is thus understandable that regional variations in reproductive status prevails in Africa and the high rates of male infertility in Nigeria is thought to be due to infections, sexually transmitted diseases, and hormonal abnormalities (Akinloye, Grommok, Nieschlag, & Simoni, 2009; Emokpae, Uadia, Omale-Itodo, & Orok, 2007).
The organochlorine pesticide DDT (1,1,1-trichloro-2,2-bis (chlorodiphenyl)ethane) is one of the most persistent organic pollutants that is known to be toxic, persistent, and bioaccumulative and has been used for malaria vector in South Africa since 1945. According to a cross-sectional study in an endemic malaria area (Limpopo Province, South Africa), DDT concentrations and sperm counts were negatively correlated among African men (Jager, Aneck-Hahn, Bornman, Farias, & Spanò, 2012). Therefore, sperm counts vary in different regions of Africa based on environmental factors, chemicals, and infections that each region offers.
Australia
There are very few reports on changes in sperm count of Australian men. In 1984, the report of Handelsman et al. about the semen quality of sperm donors first predicted that there is no alteration in the sperm count of Australian men. Later, several studies reported no alteration in semen quality (Costello et al., 2002; Stewart et al., 2009). In the current analysis, the authors identified a mild increase in sperm concentration from 1980 to 2015 (r = .167, p = .788; Figure 3C) that reflected 0.11% increase in sperm concentration in Australian men (Figure 3C-c).
Links With Possible Factors
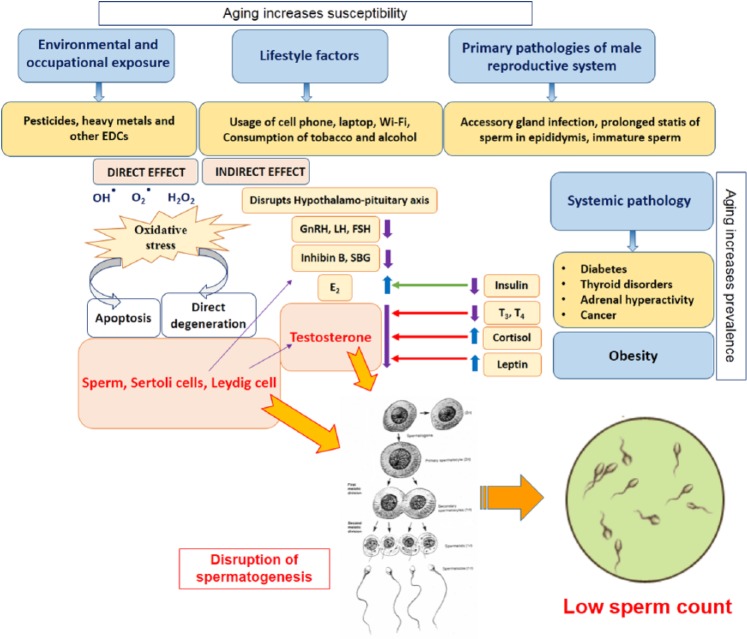
These observed trends in sperm concentration might be linked to the effects of environmental factors, including endocrine disruptors. They might also be linked to other known semen altering factors, like an increase in body mass index (BMI), stress, nutrition, or sometimes systemic pathologies, such as diabetes, cancer, or systemic infection. In previous reports, the authors mentioned various environmental, occupational, and lifestyle factors that can alter sperm count (Dutta et al., 2013; Sengupta & Banerjee, 2014; Figure 4). In addition, aging increases the risk of oxidative stress and other systemic diseases, which can also contribute to a reduction in sperm count (R2 = .979, p > .001).
Figure 4.
Possible mechanism of action of environmental toxicants, lifestyle factors, obesity, and systemic diseases in lowering sperm count in ageing male (red arrows show inhibition, blue arrows show stimulation, purple arrows indicate decrease, and blue arrows indicate increase in hormone levels).
Environmental and Lifestyle Factors: Direct Action on Spermatogenesis
Since 1961, dibromochloropropane (DBCP), a nematocide employed on various tropical crops, has been known to affect testicular functions. Torkelson (1961) reported that DBCP caused testicular atrophy in laboratory animals. Later, in 1977, Whorton, Krauss, Marshall, and Milby published an article that reported DBCP had rendered thousands of agricultural workers sterile in many countries worldwide. Since that report, many other chemical substances have been reported to have the potential to decrease sperm count in men (Bonde, 1996). These substances include pesticides such as ethylene dibromide (Ratcliffe et al., 1987) and carbaryl (Wyrobek, Watchmaker, et al., 1981), solvents such as glycol ethers (Welch et al., 1988), carbon disulfide (Lancranjan, 1972), and 2-bromopropane (Kim et al., 1996; Table 3), and heavy metals (Lancranjan, Popescu, Gavanescu, Klepsch, & Serbanescu, 1975; Sengupta, 2013; Sengupta, 2014b; Sengupta, Banerjee, Nath, Das, & Banerjee, 2015; Table 4). Along with these agents, thousands of chemicals should be included with experimental evidence that have demonstrated testicular toxicity in animals but for which data are not available for humans (Bonde, 1996; Łepecka-Klusek, Wdowiak, Pilewska-Kozak, Syty, & Jakiel, 2011; Sundaram & Witorsch, 1995). Rosenstock, Liptzin, Six, and Tomich (2013) reported a significant increase of pesticide use from 1980 to 2010 proclaiming that these chemicals play a pivotal role in declining sperm count in different age groups of males. Among thousands of chemicals that we are exposed to environmentally or occupationally, very few have been evaluated for reproductive toxicity, specifically in various age groups of men. It is known that the susceptibility to this chemical assault increases with age.
Table 3.
Studies on Pesticides and Sperm Concentration of Past Two Decades.
| Study | Compound | Subjects | Age | Compound concentration | Sperm concentration (×106 cells/mL) |
|---|---|---|---|---|---|
| Ayotte et al. (2001) | p,p′-DDE | 24 Healthy males | 16-28 | 77.9 mg/g lipid | Decreased p < .05 |
| Duty et al. (2003) | MBP | 168 Male partners of subfertile couples | 36 | 16.1 ng/mL | Decreased p < .05 |
| MEP | 175.5 ng/mL | No change | |||
| MEHP | 7.6 ng/mL | No association | |||
| Rignell-Hydbom et al. (2005) | p,p′-DDE | 195 Healthy males | 24-65 | 240 ng/g lipid (80-887) | No change |
| Charlier and Foidart (2005) | p,p′-DDE | 73 Healthy males | 25 | 1.05 µg/g lipid | No change |
| Hauser, Williams, Altshul, and Calafat (2005) | MBP | 463 Male partners of subfertile couples | 36 | 17.3 ng/mL | Decreased p < .05 |
| MEP | 180 ng/mL | No association | |||
| MEHP | 8.0 ng/mL | No association | |||
| MMP | 3.6 ng/mL | No change | |||
| p,p′-DDE | 220 ng/g lipid (72.5-7776) | No relationship | |||
| Pant et al. (2008) | DEP | 300 Healthy males | 29 | 0.64-3.11 µg/mL | Decreased p < .05 |
| DBP | 0.18-1.65 µg/mL | Decreased p < .05 | |||
| Wirth et al. (2008) | MEP | 45 Male partners of subfertile couples | 35 | 121.9 ng/mL | Decreased p < .05 |
| MBP | 26.9 ng/mL | No association | |||
| MMP | 1.1 ng/mL | No change | |||
| MEHP | 11.5 ng/mL | No association | |||
| Mendiola et al. (2010) | BPA | 375 Male partners of pregnant women | 18-53 | 1.5 µg/L | No association |
| Meeker et al. (2010) | BPA | 190 Males from infertility clinic | 36 | 1.3 ng/mL | Decreased p < .05 |
| Li et al. (2011) | BPA | 218 Healthy males | No data | 1.6-5.9 mg/L | Decreased p < .05 |
| Knez, Kranvog, Breznik, Voncina, and Vlaisavljevic (2013) | BPA | 142 Male partners of subfertile couples | 34 | 1.55 ng/mL | Decreased p < .05 |
| Jurewicz et al. (2013) | MEP | 269 Males from infertility clinic | 32 | 153.6 µg/mL | No alteration |
Note. MBP = mono-n-butyl phthalate; MEP = mono-ethyl phthalate; MMP = mono-methyl phthalate; MEHP = mono-2-ethylhexyl phthalate; BPA = biphenol-A; DBP = di-n-butyl phthalate; DEP = di-ethyl phthalate; p,p′-DDE = p,p′-Dichlorodiphenyldichloroethylene.
Table 4.
Studies on Heavy Metals and Sperm Concentration.
| Agent | Study | Concentration of agent in seminal plasma | Sperm concentration (×106 cells/mL) | Criteria |
|---|---|---|---|---|
| Lead | Hovatta et al. (1998) | 2.5 µg/dL | 96 × 106 cells/mL | 1992 criteria |
| Telisman et al. (2000) | 36.7 µg/dL | Decreased p < .05 | 1987 criteria | |
| Hernández-Ochoa et al. (2005) | 0.2 µ/dL | 11 × 106 cells/mL | 1999 criteria | |
| Meeker et al. (2008) | 1.5 µg/dL | 42.7 × 106 cells/mL | 1999 criteria | |
| Fatima et al. (2010) | >40 µg/dL | ≥20 × 106 cells/mL | 1999 criteria | |
| Mendiola et al. (2011) | 2.93 µ/dL | ≥20 × 106 cells/mL | 1999 criteria | |
| Cadmium | Hovatta et al. (1998) | 0.15 µ/dL | 96 × 106 cells/mL | 1992 criteria |
| Akinloye, Arowojolu, Shittu, and Anetor (2006) | 65 µg/dL | 42.7 × 106 cells/mL | 1999 criteria | |
| Meeker et al. (2008) | 0.04 µ/dL | 42.7 × 106 cells/mL | 1999 criteria | |
| Benoff et al. (2009) | 0.028 µ/dL | Decreased p < .05 | 1992 criteria | |
| Mendiola et al. (2011) | 0.10 µ/dL | ≥20 × 106 cells/mL | 1999 criteria | |
| Mercury | Choy et al. (2002) | 40.6 mmol/L | ≤20 × 106 cells/mL | 1999 criteria |
| Rignell-Hydbom (2007) | 0.225 µg/dL | 48 × 106 cells/mL | 1999 criteria | |
| Mendiola et al. (2011) | 1.99 µg/dL | ≥20 × 106 cells/mL | 1999 criteria |
Besides chemical assault, researchers must also consider physical factors like ionizing radiation and heat. Spermatogenesis requires the temperature in the scrotum to be at least 3°C lower than body temperature. An increase in scrotal temperature disturbs spermatogenesis (Mieusset, Bujan, Mansat, Grandjean, & Pontonnier, 1991). Prolonged exposure to sources of radiant heat may lead to significant changes in sperm concentrations (Figa-Talamanca et al., 1992; Thonneau, Bujan, Multigner, & Mieusset, 1998). Other physical agents, such as high-frequency electromagnetic fields, may also affect testicular function (Weyandt et al., 1996; Table 5). As the use of cell phones, laptops, and Wi-Fi has increased tremendously in past three decades (Lenhart, Purcell, Smith, & Zickuhr, 2010), the possibility of radiation-induced decline in sperm count increases.
Table 5.
Reports on Cell Phone Usage and Sperm Concentration.
| Study | Sample size | Age (years, mean ± SD) | Exposure | Sperm concentration (×106/mL) |
|---|---|---|---|---|
| Fejes, Závaczki, et al. (2005) | 371 | 30.8 ± 4.4 | [Retrospective] Two groups: low transmitters (<15 min/day), high transmitters (>60 min/day) | Decreased sperm count (and motility) |
| Erogul et al. (2006) | 27 | Males of reproductive age | RF-EMR 900 MHz for 5 min | Significantly decreased (p < .05) sperm count (motility, morphology, and viability) |
| Wdowiak, Wdowiak, and Wiktor (2007) | 304 | Males of reproductive age visiting infertility clinic | [Retrospective] three groups: No cell phone use, sporadic cell phone use over last 1-2 years, regular cell phone use for more than 2 years | Decreased sperm count (motility, morphology and viability) |
| Agarwal, Deepinder, Sharma, Ranga, and Li (2008) | 361 | 31.81 ± 6.12 | [Retrospective] Four groups: no use, little use (<2 h), mid use (2-4 h), high use (>4 h) | Decreased sperm count (motility, morphology and viability) |
| Falzone et al. (2008) | NA | NA | RF-EMR 900 MHz at 2 W/kg and 5.7 W/kg SAR. Incubated for 21°C for 16 h | Significantly decreased sperm count |
| De Iuliis, Newey, King, and Aitken (2009) | 22 | 24.1 ± 1.1 | RF-EMR 1.8 GHz at 0.4 W/kg to 27.5 W/kg SAR. Incubated for 21°C for 16 h | Decreased sperm count (motility and viability) |
| Agarwal et al. (2009) | 32 | 28.2 ± 4.1 | RF-EMR 850 MHz at 1.46 W/kg. Exposed at distance of 2.5 cm for 60 min | Decreased sperm count (motility and viability), increased ROS level |
| Falzone, Huyser, Franken, and Leszczynski (2010) | 12 | Males of reproductive age (healthy non-smoking donor) | RF-EMR 900 MHz at 2 W/kg and 5.7 W/kg SAR. Incubated for 21°C for 16 h | Significantly decreased (p < .05) sperm count, increased ROS level |
| Falzone, Huyser, Becker, Leszczynski, and Franken (2011) | 12 | 31.8 ± 12.5 | RF-EMR 900 MHz for 60 min | Significantly decreased (p < .05) sperm count |
Note. RF-EMR = radiofrequency-electromagnetic radiation; SAR, specific absorption rate.
Finally, the effects of regular consumption of tobacco or alcohol, both of which are on the brink of disturbing spermatogenesis, should not be ignored (Bonde, 1996; Multigner & Spira, 1997). Stress, which is very hard to assess, has also been set forth as a factor that may have a negative impact on sperm production (Fenster et al., 1997; Negro-Vilar, 1993). In a report of the Royal College of Physicians (2012), researchers documented a massive change in consumption of tobacco from 1962 to 2007. They described an increase in tobacco consumption from 1962 to 2000 and a gentle fall from 2000 to 2012. They also recorded that this decrease is prevalent in the United Kingdom and other European countries, but in the rest of the world there are no data of decreasing active or passive consumption, specifically in developing countries, which could be related to the worldwide decrease in sperm count even in 2015. Another relevant Federal Survey (2013) reported that males in the 18 to 35 years age group are mostly addicted to tobacco consumption, followed by the age group of 35 to 60. This is of great concern in relation to declining sperm counts in aging males.
Major alterations in sperm counts have been observed in populations following changes in other diverse factors, such as catastrophes. The Kobe earthquake decreased sperm count of local men significantly (Fukuda, Fukuda, Shimazu, Yomura, & Shimizu, 1996). Clearly, a large number of environmental factors are likely to affect spermatogenesis in humans. However, most of the studies cited above were carried out in a professional environment in circumstances in which the level of chemical and physical exposure is generally high. This accounts for a nonnegligible proportion of the adult male population. In addition, given the widespread use of chemical substances in particular, it is legitimate to raise questions concerning the consequences for the general population of their accidental or deliberate release into the environment.
Effect of Endocrine Disruptors
There are numerous reports that identify the role of endocrine disrupting chemicals (EDCs) for secular changes in sperm count. These EDCs are liable to have adverse effects on individual organisms through primary effects on endocrine systems. These substances, via their estrogenic or anti-androgenic activities, are likely to hinder testicular development in the fetus and the postnatal functions of the testes (Sharpe, 1993). In 1938, estrogenic activity for a range of man-made chemicals was first documented (Dodds & Lawson, 1938). Since the 1960s, it has been known that synthetic compounds such as the chlorinated insecticides methoxychlor and DDT and polychlorinated biphenyls (PCBs) may have estrogenic activity in laboratory animals (Bitman, Cecil, Harris, & Fries, 1968; Tullner, 1961). It has been known for some time that some xenobiotics may act in a similar way to hormones (xenohormones), thereby affecting endocrine regulations. The list of chemical substances with hormonal activity in vitro or in vivo has not stopped growing in the past few decades. In addition to those already mentioned, they include insecticides (lindane), fungicides (vinchlozoline), surfactants (alkylphenols), plastics (bisphenol-A, phthalates), and industrial by-products (dioxins; reviewed in Colborn, Vomsaal, & Soto, 1993; Toppari et al., 1996). Experiments in vivo in laboratory animals have identified that the administration of methoxychlor, octylphenol, butyl phthalate, or dioxin during gestation or lactation causes a significant decrease in sperm production in the adult (Gray, 1982; Mably, Bjerke, Moore, Gendron-Fitzpatrick, & Peterson, 1992; Sharpe, Fisher, Millar, Jobling, & Sumpter, 1995). Several observations support the idea that EDCs may be involved in changes of sperm quality in humans and that these disrupting effects increase with the progression of age. Thus, the trend of declining sperm counts in aging males from 1980 to 2015 may be attributed to the persistently increased exposure of these EDCs.
Obesity Can Affect Spermatogenesis
The association between high adiposity and alterations in sperm count has not been clearly demonstrated in men. Data from large-scale epidemiological studies suggest an elevated risk for infertility among couples when the male partner is overweight or obese (Nguyen, Wilcox, Skjaerven, & Baird, 2007; Ramlau-Hansen et al., 2007; Sallmen, Sandler, Hoppin, Blair, & Baird, 2006). Several studies have reported an inverse correlation between BMI and sperm concentration or total sperm count (Jensen et al., 2004; Paasch, Grunewald, Kratzsch, & Glander, 2010), but other reports have failed to document this relationship (Aggerholm, Thulstrup, Toft, Ramlau-Hansen, & Bonde, 2008; Duits, van Wely, van der Veen, & Gianotten, 2010). The current report collected data from the past few decades regarding the association between BMI and sperm concentration and identified that overweight and obesity were associated with an increased risk of oligozoospermia or azoospermia (Table 6).
Table 6.
Body Mass Index (BMI), Obesity, and Sperm Concentration.
| Study | Country | Population | Age (years, mean ± SD) | Percentage by BMI category (kg/m2) |
Percentage by total sperm count category |
||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| <18.5 (%) | 18.5-24.9 (%) | 25-29.9 (%) | 30-39.9 (%) | >40 (%) | Azoospermia (%) | Oligozoospermia (%) | Normozoospermia (%) | ||||
| Eskenazi et al. (2003) | United States | 97 Nonsmoking male volunteers without known fertility problems | 46.4 ± 15.9 | 0 | 50.5 | 42.3 | 7.2 | 0 | 4.1 | 12.4 | 83.5 |
| Jensen et al. (2004) | Denmark | 1,558 Young military recruits | 19.5 ± 1.3 | 3.5 | 77.3 | 15.4 | 3.7 | 0.1 | 0.3 | 45.2 | 54.5 |
| Koloszar et al. (2005); Fejes, Koloszar, Szollosi, Zavaczki, and Pal (2005); Fejes et al. (2006) | Hungary | 473 Male partners from subfertile couple attending infertility center | 29.5 ± 3.6 | 6.3 | 33.6 | 32.4 | 22.0 | 5.7 | 44.0 | 30.0 | 65.6 |
| Magnusdottir, Thorsteinsson, Thorsteinsdottir, Heimisdottir, and Olafsdottir (2005) | Iceland | 72 Male partners from subfertile couple attending infertility center | 37.4 ± 5.4 | 0 | 36.1 | 44.4 | 15.3 | 4.2 | 2.8 | 27.8 | 69.4 |
| Zorn, Osredkar, Meden-Vrtovec, and Majdic (2007) | Slovenia | 189 Male partners from subfertile couple attending infertility center | 34.4 ± 5.8 | 0 | 43.9 | 41.8 | 14.3 | 0 | 22.2 | 11.7 | 61.1 |
| Aggerholm et al. (2008) | Denmark | 1,669 Male volunteers from general population | 33.9 ± 8.8 | 0.5 | 52.0 | 39.4 | 8.1 | 0 | 1.2 | 11.1 | 87.7 |
| Vujkovic et al. (2009) and Hammiche et al. (2011) | Netherland | 225 Male partners from subfertile couples during IVF or ICSI cycles | 37.5 ± 5.3 | 0.9 | 45.3 | 45.3 | 8.5 | 0 | — | 40.9 | 59.1 |
| Duits et al. (2010) | Netherland | 1,401 male partners from subfertile couple attending infertility center | 36.4 ± 6.5 | 0.4 | 47.3 | 41.9 | 9.7 | 0.7 | 6.3 | 17.5 | 76.2 |
| Martini et al. (2010) | Argentina | 793 Male partners from subfertile couples | 34.9 ± 6.2 | — | 31.0 | 49.4 | 18.5 | 1.1 | 1.9 | 52.7 | 45.4 |
| Ramlau-Hansen et al. (2010) | Denmark | 259 Sons of mothers recruited during their pregnancy in 1984-1987 | 20.1 ± 0.8 | 3.9 | 72.2 | 17.8 | 6.1 | 0 | 0.8 | 20.5 | 78.7 |
| Chavarro, Toth, Wright, Meeker, and Auser (2010) | United States | 483 Male partners from subfertile couple attending infertility center | 36.3 ± 5.4 | — | 25.5 | 48.2 | 23.8 | 2.5 | — | 10.8 | 89.2 |
| Keltz et al. (2010) and Relwani et al. (2011) | United States | 185 Male partners from sub-fertile couples during IVF or ICSI cycles | 37.5 ± 8.0 | 0.5 | 22.2 | 47.0 | 29.2 | 1.1 | — | 44.9 | 55.1 |
| Tunc, Bakos, and Tremellen (2011) | Australia | 81 Male partners from subfertile couple attending infertility center | 36.8 ± 5.2 | 0 | 25.9 | 45.7 | 28.4 | 0 | — | 28.4 | 71.6 |
| Shayeb, Harrild, Mathers, and Bhattacharya (2011) | United Kingdom | 1,966 Male partners from subfertile couple attending infertility center | 33.1 ± 6.0 | 0.9 | 40.8 | 44.9 | 12.5 | 0.9 | — | 18.2 | 81.8 |
| Lotti et al. (2011) | Italy | 222 Male partners from subfertile couple attending infertility center | 35.8 ± 7.0 | 0 | 59.0 | 32.0 | 9.0 | 0 | 20.3 | 37.8 | 41.9 |
| La Vignera, Condorelli, Vicari, and Calogero (2012) | Italy | 150 Nonsmoking male volunteers | 31.4 ± 2.3 | 0 | 33.3 | 33.3 | 26.7 | 6.7 | 2.7 | 41.3 | 56.0 |
| Eskandar et al. (2012) | Saudi Arabia | 500 Male partners from subfertile couple attending infertility center | 34.8 ± 7.7 | 11.0 | 13.4 | 24.0 | 26.4 | 25.2 | 1.4 | 29.6 | 69.6 |
| Hammiche et al. (2012) | Netherlands | 449 Male partners from subfertile couple attending infertility center | 35.4 ± 6.5 | 1.1 | 34.1 | 49.2 | 15.2 | 0.4 | 5.8 | 35.2 | 59.0 |
| Braga et al. (2012) | Brazil | 250 Male partners from subfertile couples during IVF or ICSI cycles | 38.4 ± 9.3 | 2.0 | 50.0 | 40.0 | 4.0 | 4.0 | — | 34.4 | 65.6 |
Note. IVF = in vitro fertilization; ICSI = intracytoplasmic sperm injection.
Regarding the correlation between obesity and alteration of sperm concentration, different hypotheses have been raised. First, alterations of the hypothalamo-pituitary-gonadal axis have been reported to be involved in this process. Aromatization of steroids to estrogens in peripheral tissues leads to the hypogonadotropic hyperestrogenic hypogonadism previously described in obese men (Schneider, Kirschner, Berkowitz, & Ertel, 1979), with a significant decline in total and free testosterone levels (with increased leptin) and increase in estradiol (E2), both leading to deleterious effects on spermatogenesis. Moreover, reports have identified a decrease of sex hormone-binding globulin among obese men, notably mediated by hyperinsulinemia, emphasizing the negative feedback effect of elevated total E2 levels (Stellato, Feldman, Hamdy, Horton, & McKinlay, 2000). Obesity is also associated with an increase of endorphins, leading to a both lower LH pulse amplitude and GnRH production (Bhattarai, Chaudhuri, Bhattacharya, & Sengupta, 2014; Bhattarai, Bhattacharya, Chaudhuri & Sengupta, 2014; Blank, Clark, Heymsfield, Rudman, & Blank, 1994; Dutta et al., 2013; Krajewska-Kulak & Sengupta, 2013). In an earlier report, the authors described that the role of thyroid hormones in men can also contribute to decreased sperm count (Krajewska-Kulak & Sengupta, 2013). A decreased level of circulating triiodo-thyronine (T3) may affect testicular production of testosterone, and thus affects spermatogenesis (Krajewska-Kulak & Sengupta, 2013). Some authors have also reported that obesity may directly alter spermatogenesis and Sertoli cell function (Winters et al., 2006) by the more severe diminution of inhibin B levels compared with the decrease of follicle-stimulating hormone. Another hypothesis is the increase of scrotal temperature caused by hip and abdominal fat tissue accumulation, or even scrotal fat deposition (Shafik & Olfat, 1981), would involve spermatogenesis disturbances. Preferential accumulation in fatty tissue of toxic substances and liposoluble EDCs would amplify those alterations, as indicated by serum organochlorine levels being correlated with BMI (Magnusdottir et al., 2005).
In 2007, Johnson et al. reported that obesity prevalence had increased tremendously in the second half of the 1900s, which can be correlated with the trend of declining sperm count in men. The WHO (2014) also reported the prevalence of obesity (BMI ≥30 kg/m2) had increased remarkably worldwide by 2014, and notably in the United States, where a decline in sperm count is more significant than in the rest of the world. The WHO reported worldwide obesity had more than doubled since 1980. They also reported, in 2014, that more than 1.9 billion adults 18 years and older were overweight. Of these, over 600 million were obese. In 2014, 39% of adults aged 18 years and over (38% of men) were overweight (WHO, 2014), and the prevalence of obesity increases with age. This is reassuring the data of declining sperm counts in aging males presented in this report.
Conclusion
The current study, with strong experimental evidences extracted by analyzing multitudinous studies, reports a declining trend in sperm concentration over the past 35 years with perceptions of the reasons of such deterioration in male reproductive health. These variations of sperm concentrations are observed by taking into account the different geographical regions. The outcome of this review is a systematic, concisely arranged scientific report on sperm concentration and the factors involved, from 1980 to 2015 from all over the world; statistical analysis of significant declining trend of sperm concentration over the said time period; and correlation of male health with the declining pattern of sperm count trend considering the age of an individual. With the development of more biomarkers to relate age with sperm concentrations and with upcoming studies investigating the causes of the decreasing quality of sperm parameters, greater knowledge could be developed to explore the possible remedies to overcome this expanding threat of infertility to the next generations.
Acknowledgments
The authors thank Dr. Sandeep Poddar, Research Manager, Lincoln University College, Malaysia, for his support in formulating this review. The authors are also thankful to him for his help in collecting information regarding data of sperm counts.
Footnotes
Declaration of Conflicting Interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The author(s) received no financial support for the research, authorship, and/or publication of this article.
References
- Aabyholm T. (1981). An andrological study of 51 fertile men. International Journal of Andrology, 4, 646-656. [DOI] [PubMed] [Google Scholar]
- Acacio B. D., Gottfried T., Israel R., Sokol R. Z. (2000). Evaluation of a large cohort of men presenting for a screening semen analysis. Fertility and Sterility, 73, 595-597. [DOI] [PubMed] [Google Scholar]
- Adami H. O., Bergström R., Möhner M., Zatoński W., Storm H., Ekbom A., . . . Rahu M. (1994). Testicular cancer in nine Northern European countries. International Journal of Cancer, 59, 33-38. [DOI] [PubMed] [Google Scholar]
- Adiga S. K., Jayaraman V., Kalthur G., Upadhya D., Kumar P. (2008). Declining semen quality among south Indian infertile men: A retrospective study. Journal of Human Reproductive Sciences, 1, 15-18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Agarwal A., Deepinder F., Sharma R. K., Ranga G., Li J. (2008). Effect of cell phone usage on semen analysis in men attending infertility clinic: An observational study. Fertility and Sterility, 89, 124-128. [DOI] [PubMed] [Google Scholar]
- Agarwal A., Desai N. R., Makker K., Varghese A., Mouradi R., Sabanegh E., Sharma R. (2009). Effects of radiofrequency electromagnetic waves (RF-EMW) from cellular phones on human ejaculated semen: An in vitro pilot study. Fertility and Sterility, 92, 1318-1325. [DOI] [PubMed] [Google Scholar]
- Aggerholm A. S., Thulstrup A. M., Toft G., Ramlau-Hansen C. H., Bonde J. P. (2008). Is overweight a risk factor for reduced semen quality and altered serum sex hormone profile? Fertility and Sterility, 90, 619-626. [DOI] [PubMed] [Google Scholar]
- Aitken R. J., Best F. S., Richardson D. W., Djahanbakhch O., Lees M. M. (1982). The correlates of fertilizing capacity in normal fertile men. Fertility and Sterility, 38, 68-76. [DOI] [PubMed] [Google Scholar]
- Akande T., Isah H. S., Sekoni V. O., Pam I. C. (2011). The semen of fertile men in Jos, Nigeria. Journal of Medical Laboratory Science, 20, 33-36. [Google Scholar]
- Akinloye O., Arowojolu A. O., Shittu O. B., Anetor J. I. (2006). Cadmium toxicity: A possible cause of male infertility in Nigeria. Reproductive Biology, 6, 17-30. [PubMed] [Google Scholar]
- Akinloye O., Grommok J., Nieschlag E., Simoni M. (2009). Androgen receptor gene CAG and GGN polymorphisms in infertile Nigerian men. Journal of Endocrinological Investigation, 32, 797-804. [DOI] [PubMed] [Google Scholar]
- Almagor M., Ivnitzki I., Yaffe H., Baras M. (2003). Changes in semen quality in Jerusalem between 1990 and 2000: A cross-sectional and longitudinal study. Archives of Andrology, 49, 139-144. [DOI] [PubMed] [Google Scholar]
- Andolz P., Bielsa M. A., Vila J. (1999). Evolution of semen quality in northeastern Spain: A study in 22,759 infertile men over a 36 year period. Human Reproduction, 14, 731-735. [DOI] [PubMed] [Google Scholar]
- Aribarg A., Kenkeerati W., Vorapaiboonsak V., Leepipatpaiboon S., Farley T. M. M. (1986). Testicular volume, semen profile and serum hormone levels in fertile Thai males. International Journal of Andrology, 9, 170-180. [DOI] [PubMed] [Google Scholar]
- Assennato G., Paci C., Baser M. E., Molinini R., Candela R. G., Altamura B. M., Giorgino R. (1987). Sperm count suppression without endocrine dysfunction in lead-exposed men. Archives of Environmental Health, 42, 124-127. [DOI] [PubMed] [Google Scholar]
- Auger J., Kunstmann J. M., Czyglik F., Jouannet P. (1995). Decline in semen quality among fertile men in Paris during the past 20 years. New England Journal of Medicine, 332, 281-285. [DOI] [PubMed] [Google Scholar]
- Axelsson J., Rylander L., Rignell-Hydbom A., Giwercman A. (2011). No secular trend over the last decade in sperm counts among Swedish men from the general population. Human Reproduction, 26, 1012-1006. [DOI] [PubMed] [Google Scholar]
- Ayotte P., Giroux S., Dewailly E., Hernández Avila M., Farias P., Danis R., Villanueva Díaz C. (2001). DDT spraying for malaria control and reproductive function in Mexican men. Epidemiology, 12, 366-367. [DOI] [PubMed] [Google Scholar]
- Badenoch D. F., Evans S. J. W., McCloskey D. J. (1989). Sperm density measurement: Should this be abandoned? British Journal of Urology, 64, 521-523. [DOI] [PubMed] [Google Scholar]
- Bahk J. Y., Jung J. H., Jin L. M., Min S. K. (2010). Cut-off value of testes volume in young adults and correlation among testes volume, body mass index, hormonal level, and seminal profiles. Urology, 75, 1318-1323. [DOI] [PubMed] [Google Scholar]
- Barratt C. L. R., Dunphy B. C., Thomas E. J., Cooke I. D. (1988). Semen characteristics of 49 fertile males. Andrologia, 20, 264-269. [DOI] [PubMed] [Google Scholar]
- Belloc S., Cohen-Bacrie M., Amar E., Izard V., Benkhalifa M., Dalléac A., de Mouzon J. (2014). High body mass index has a deleterious effect on semen parameters except morphology: Results from a large cohort study. Fertility and Sterility, 102, 1268-1273. [DOI] [PubMed] [Google Scholar]
- Benoff S., Hauser R., Marmar J. L., Hurley I. R., Napolitano B., Centola G. M. (2009). Cadmium concentrations in blood and seminal plasma: Correlations with sperm number and motility in three male populations (infertility patients, artificial insemination donors, and unselected volunteers). Molecular Medicine, 15, 248-262. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Benshushan A., Shoshani O., Paltiel O., Schenker J. G., Lewin A. (1997). Is there really a decrease in sperm parameters among healthy young men? A survey of sperm donations during 15 years. Journal of Assisted Reproduction and Genetics, 14, 347-353. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Benzi G., Pastoris O., Dossena M. (1982). Relationships between gamma-aminobutyrate and succinate cycles during and after cerebral ischemia. Journal of Neuroscience Research, 7, 193-201. [DOI] [PubMed] [Google Scholar]
- Bergman A., Brandt I., Brouwer B. (1996). European workshop on the impact of endocrine disrupters on human health and wildlife: Report of the proceedings. Brussels, Belgium: European Commission. [Google Scholar]
- Berling S., Wolner-Hanssen P. (1997). No evidence of deteriorating semen quality among men in infertile relationships during the last decade: A study of males from southern Sweden. Human Reproduction, 12, 1002-1005. [DOI] [PubMed] [Google Scholar]
- Bhattarai T., Chaudhuri P., Bhattacharya K., Sengupta P. (2014). Effect of progesterone supplementation on post-coital unilaterally ovariectomized superovulated mice in relation to implantation and pregnancy. Asian Journal of Pharmaceutical & Clinical Research, 7, 29-31. [Google Scholar]
- Bhattarai T., Bhattacharya K., Chaudhuri P., Sengupta P. (2014). Correlation of common biochemical markers for bone turnover, serum calcium and alkaline phosphatase, in post-menopausal women. Malaysian Journal of Medical Sciences, 21, 58-61. [PMC free article] [PubMed] [Google Scholar]
- Bilotta P., Guglielmo R., Steffe M. (1999). Analysis of decline in seminal fluid in the Italian population during the past 15 years. Minerva Ginecologica, 51, 223-231. [PubMed] [Google Scholar]
- Bitman J., Cecil H., Harris S., Fries G. (1968). Estrogenic activity of o,p′-DDT in the mammalian uterus and avian oviduct. Science, 162, 371-372. [DOI] [PubMed] [Google Scholar]
- Blank D. M., Clark R. V., Heymsfield S. B., Rudman D. R., Blank M. S. (1994). Endogenous opioids and hypogonadism in human obesity. Brain Research Bulletin, 34, 571-574. [DOI] [PubMed] [Google Scholar]
- Bonde J. P. (1990). Semen quality and sex hormones among mild steel and stainless steel welders: A cross sectional study. British Journal of Industrial Medicine, 47, 508-514. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bonde J. P. (1996). Environmental factors. In Comhaire F. H. (Ed.), Male infertility (pp. 267-284). London, England: Chapman & Hall Medical. [Google Scholar]
- Bonde J., Koldjensen T., Brixenlarsen S., Abell A., Scheike T., Hjollund N., . . . Olsen J. (1998). Year of birth and sperm count in 10 Danish occupational studies. Scandinavian Journal of Work, Environment and Health, 24, 407-413. [DOI] [PubMed] [Google Scholar]
- Borges E., Setti A. S., Vingris L., Figueira R. S., Braga D., Iconelli A. (2013). Decreasing sperm quality: Findings from a 1 year gap longitudinal analysis of 2300 sperm samples from Brazil. JBRA Assisted Reproduction, 17, 89-92. [Google Scholar]
- Borghi M. R., Asch R. H. (1983). Human sperm penetration in bovine cervical mucus. Clinical studies I. Journal of Andrology, 4, 316-318. [DOI] [PubMed] [Google Scholar]
- Braga D. P., Halpern G., Figueira Rde C., Setti A. S., Iaconelli A., Jr., Borges E., Jr. (2012). Food intake and social habits in male patients and its relationship to intracytoplasmic sperm injection outcomes. Fertility and Sterility, 97, 53-59. [DOI] [PubMed] [Google Scholar]
- Carlsen E., Giwercman A., Keiding N., Skakkebaek N. E. (1992). Evidence for decreasing quality of semen during past 50 years. British Medical Journal, 305, 609-613. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Carlsen E., Swan S. H., Petersen J. H., Skakkebæk N. E. (2005). Longitudinal changes in semen parameters in young Danish men from the Copenhagen area. Human Reproduction, 20, 942-949. [DOI] [PubMed] [Google Scholar]
- Centola G. M., Eberly S. (1999). Seasonal variations and age-related changes in human sperm count, motility, motion parameters, morphology, and white blood cell concentration. Fertility and Sterility, 72, 803-808. [DOI] [PubMed] [Google Scholar]
- Chan S. Y. W., Wang C. (1987). Correlation between semen adenosine triphosphate and sperm fertilizing capacity. Fertility and Sterility, 47, 717-719. [PubMed] [Google Scholar]
- Charlier C. J., Foidart J. M. (2005). Comparative study of dichlorodiphenyl dichloroethylene in blood and semen of two young male populations: Lack of relationship to infertility, but evidence of high exposure of the mothers. Reproductive Toxicology, 20, 215-220. [DOI] [PubMed] [Google Scholar]
- Chavarro J. E., Toth T. L., Wright D. L., Meeker J. D., Auser R. (2010). Body mass index in relation to semen quality, sperm DNA integrity, and serum reproductive hormone levels among men attending an infertility clinic. Fertility and Sterility, 93, 2222-2231. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chen Z., Isaacson K. B., Toth T. L., Godfrey-Bailey L., Schiff I., Hauser R. (2003). Temporal trends in human semen parameters in New England in the United States, 1989-2000. Archives of Andrology, 49, 369-374. [DOI] [PubMed] [Google Scholar]
- Choy C. M. Y., Lam C. W. K., Cheung L. T. F., Briton-Jones C. M., Cheung L. P., Haines C. J. (2002). Infertility, blood mercury concentrations and dietary seafood consumption: A case-control study. BJOG: An International Journal of Obstetrics & Gynaecology, 109, 1121-1125. [DOI] [PubMed] [Google Scholar]
- Colborn T., Vomsaal F., Soto A. (1993). Developmental effects of endocrine-disrupting chemicals in wildlife and humans. Environmental Health Perspectives, 101, 378-384. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cooper T. G., Jockenhövel F., Nieschlag E. (1991). Variations in semen parameters from fathers. Human Reproduction, 6, 859-866. [DOI] [PubMed] [Google Scholar]
- Costello M. F., Sjoblom P., Haddad Y., Steigrad S. J., Bosch E. G. (2002). No decline in semen quality among potential sperm donors in Sydney, Australia, between 1983 and 2001. Journal of Assisted Reproduction and Genetics, 19, 284-290. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cottell E., Harrison R. F. (1995). The value of subcellular elemental analysis in the assessment of human spermatozoa. Human Reproduction, 10, 3186-3189. [DOI] [PubMed] [Google Scholar]
- Coutinho E. M., Melo J. F. (1988). Clinical experience with gossypol in non-Chinese men: A follow-up. Contraception, 37, 137-151. [DOI] [PubMed] [Google Scholar]
- de Castro M., Jeyendran R. S., Zaneveld L. J. (1990). Hypo-osmotic swelling test: Analysis of prevasectomy ejaculates. Archives of Andrology, 24, 11-16. [DOI] [PubMed] [Google Scholar]
- de Castro M. P., Mastrorocco D. A. (1984). Reproductive history and semen analysis in prevasectomy fertile men with and without varicocele. Journal of Andrology, 5, 17-20. [DOI] [PubMed] [Google Scholar]
- De Iuliis G. N., Newey R. J., King B. V., Aitken R. J. (2009). Mobile phone radiation induces reactive oxygen species production and DNA damage in human spermatozoa in vitro. PLoS One, 4, e6446. [DOI] [PMC free article] [PubMed] [Google Scholar]
- De Mouzon J., Thonneau P., Spira A., Multigner L. (1996). Declining sperm count. Semen quality has declined among men born in France since 1950. BMJ, 313, 43-45. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Diao R., Fok K. L., Zhao L., Chen H., Tang H., Chen J., . . . Cai Z. (2013). Decreased expression of cystic fibrosis transmembrane conductance regulator impairs sperm quality in aged men. Reproduction, 146, 637-645. [DOI] [PubMed] [Google Scholar]
- Dodds E., Lawson W. (1938). Molecular structure in relation to oestrogenic activity. Compounds without a phenanthrene nucleus. Proceedings of the Royal Society of London. Series B, Biological Sciences, 118, 222-232. [Google Scholar]
- Dougherty R. C., Whitaker M. J., Tang S. Y., Bottcher R., Keller M., Kuehl D. W. (1981). Sperm density and toxic substances: A potential key to environmental health hazards. In McKinney J. D. (Ed.), Environmental health chemistry: The chemistry of environmental agents of potential human hazards (pp. 263-278). Ann Arbor, MI: Ann Arbor Science Publishers. [Google Scholar]
- Duits F. H., van Wely M., van der Veen F., Gianotten J. (2010). Healthy overweight male partners of subfertile couples should not worry about their semen quality. Fertility and Sterility, 94, 1356-1359. [DOI] [PubMed] [Google Scholar]
- Dutta S., Joshi K. R., Sengupta P., Bhattacharya K. (2013). Unilateral and bilateral cryptorchidism and its effect on the testicular morphology, histology, accessory sex organs and sperm count in laboratory mice. Journal of Human Reproductive Sciences, 6, 106-110. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Duty S. M., Singh N. P., Silva M. J., Barr D. B., Brock J. W., Ryan L., . . . Hauser R. (2003). The relationship between environmental exposures to phthalates and DNA damage in human sperm using the neutral comet assay. Environmental Health Perspectives, 111, 1164-1169. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Eisenberg M. L., Chen Z., Ye A., Buck Louis G. M. (2015). Relationship between physical occupational exposures and health on semen quality: Data from the Longitudinal Investigation of Fertility and the Environment (LIFE) Study. Fertility and Sterility, 103, 1271-1277. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Eisenberg M. L., Li S., Behr B., Cullen M. R., Galusha D., Lamb D. J., Lipshultz L. I. (2014). Semen quality, infertility and mortality in the USA. Human Reproduction, 29, 1567-1574. [DOI] [PMC free article] [PubMed] [Google Scholar]
- el Shoura S. M., Abdel A. M., Ali M. E., el Said M. M., Ali K. Z., Kemeir M. A., . . . Elmalik E. M. (1995). Deleterious effects of khat addiction on semen parameters and sperm ultrastructure. Human Reproduction, 10, 2295-2300. [DOI] [PubMed] [Google Scholar]
- Emokpae M. A., Uadia P. O., Omale-Itodo A., Orok T. N. (2007). Male infertility and endocrinopathies in Kano, Northern Nigeria. Annals of African Medicine, 6, 61-67. [DOI] [PubMed] [Google Scholar]
- Erogul O., Oztas E., Yildirim I., Kir T., Aydur E., Komesli G., . . . Peker A. F. (2006). Effects of electromagnetic radiation from a cellular phone on human sperm motility: An in vitro study. Archives of Medical Research, 37, 840-843. [DOI] [PubMed] [Google Scholar]
- Eskandar M., Al-Asmari M., Babu Chaduvula S., Al-Shahrani M., Al-Sunaidi M., Almushait M., . . . Al-Fifi S. (2012). Impact of male obesity on semen quality and serum sex hormones. Advances in Urology, 2012, 407601. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Eskenazi B., Wyrobek A. J., Fenster L., Katz D. F., Sadler M., Lee J., . . . Rempel D. M. (1991). A study of the effect of perchloroethylene exposure on semen quality in dry cleaning workers. American Journal of Industrial Medicine, 20, 575-591. [DOI] [PubMed] [Google Scholar]
- Eskenazi E., Bradman A., Gladstone E., Jaramillo S., Birch K., Holland N. (2003). The association of age and semen quality in healthy men. Human Reproduction, 18, 447-454. [DOI] [PubMed] [Google Scholar]
- Falzone N., Huyser C., Fourie F., Toivo T., Leszczynski D., Franken D. (2008). In vitro effect of pulsed 900 MHz GSM radiation on mitochondrial membrane potential and motility of human spermatozoa. Bioelectromagnetics, 29, 268-276. [DOI] [PubMed] [Google Scholar]
- Falzone N., Huyser C., Becker P., Leszczynski D., Franken D. R. (2011). The effect of pulsed 900-MHz GSM mobile phone radiation on the acrosome reaction, head morphometry and zona binding of human spermatozoa. International Journal of Andrology, 34, 20-26. [DOI] [PubMed] [Google Scholar]
- Falzone N., Huyser C., Franken D. R., Leszczynski D. (2010). Mobile phone radiation does not induce pro-apoptosis effects in human spermatozoa. Radiation Research, 174, 169-176. [DOI] [PubMed] [Google Scholar]
- Fariss B. L., Fenner D. K., Plymate S. R., Brannen G. E., Jacob W. H., Thomason A. M. (1981). Seminal characteristics in the presence of a varicocele as compared with those of expectant fathers and prevasectomy men. Fertility and Sterility, 35, 325-327. [DOI] [PubMed] [Google Scholar]
- Fatima P., Debnath B. C., Hossain M. M., Rahman D., Banu J., Begum S. A., Rahman W. M. (2010). Relationship of blood and semen lead level with semen parameter. Mymensingh Medical Journal, 19, 405-414. [PubMed] [Google Scholar]
- Fedder J., Askjaer S. A., Hjort T. (1993). Nonspermatozoal cells in semen: Relationship to other semen parameters and fertility status of the couple. Archives of Andrology, 31, 95-103. [DOI] [PubMed] [Google Scholar]
- Federal Survey. (2013). Federal survey data on tobacco: Past month cigarette use among persons aged 12 or older, by age. US Department of Health and Human Services, Substance Abuse and Mental Health Services Administration, Center for Behavioural Health Statistics and Quality. [Google Scholar]
- Fejes I., Koloszar S., Szollosi J., Zavaczki Z., Pal A. (2005). Is semen quality affected by male body fat distribution? Andrologia, 37, 155-159. [DOI] [PubMed] [Google Scholar]
- Fejes I., Koloszar S., Zavaczki Z., Daru J., Szollosi J., Pal A. (2006). Effect of body weight on testosterone/estradiol ratio in oligozoospermic patients. Archives of Andrology, 52, 97-102. [DOI] [PubMed] [Google Scholar]
- Fejes I., Závaczki Z., Szöllosi J., Koloszár S., Daru J., Kovács L., Pál A. (2005). Is there a relationship between cell phone use and semen quality? Archives of Andrology, 51, 385-393. [DOI] [PubMed] [Google Scholar]
- Feki N. C., Abid N., Rebai A., Sellami A., Ayed B. B., Guermazi M., . . . Ammar L. K. (2009). Semen quality decline among men in infertile relationships: Experience over 12 years in the South of Tunisia. Journal of Andrology, 30, 541-547. [DOI] [PubMed] [Google Scholar]
- Fenster L., Katz D., Wyrobek A., Pieper C., Rempel D., Oman D., Swan S. H. (1997). Effects of psychological stress on human semen quality. Journal of Andrology, 18, 194-202. [PubMed] [Google Scholar]
- Figa-Talamanca I., Cini C., Varricchio G. C., Dondero F., Gandini L., Lenzi A., . . . Patacchioli F. R. (1996). Effects of prolonged autovehicle driving on male reproduction function: A study among taxi drivers. American Journal of Industrial Medicine, 30, 750-758. [DOI] [PubMed] [Google Scholar]
- Figa-Talamanca I., Dell’Orco V., Pupi A., Dondero F., Gandini L., Lenzi A., . . . Mancini G. (1992). Fertility and semen quality of workers exposed to high temperature in the ceramics industry. Reproductive Toxicology, 6, 517-523. [DOI] [PubMed] [Google Scholar]
- Fisch H., Goluboff E. T. (1996). Geographic variations in sperm counts: A potential cause of bias in studies of semen quality. Fertility and Sterility, 65, 1044. [DOI] [PubMed] [Google Scholar]
- Fisher R. A., Yates R. (1974). Statistical tables for biological, agricultural and medical research. London, England: Longman Group. [Google Scholar]
- Forman D., Møller H. (1994). Testicular cancer. Cancer Surveys, 19, 323-341. [PubMed] [Google Scholar]
- Frick J., Danner C., Joos H., Kunit G., Luukkainen T. (1981). Spermatogenesis in men treated with subcutaneous application of levonorgestrel and estrone rods. Journal of Andrology, 2, 331-338. [Google Scholar]
- Fukuda M., Fukuda K., Shimazu T., Yomura W., Shimizu S. (1996). Kobe earthquake and reduced sperm motility. Human Reproduction, 11, 1244-1246. [DOI] [PubMed] [Google Scholar]
- Gallardo E., Simon C., Levy M., Guanes P., Remohi J., Pellicer A. (1996). Effect of age on sperm fertility potential: Oocyte donation as a model. Fertility and Sterility, 66, 260-264. [DOI] [PubMed] [Google Scholar]
- Geoffroy-Siraudin C., Loundou A. D., Romain F., Achard V., Courbière B., Perrard M., . . . Guichaoua M. R. (2012). Decline of semen quality among 10,932 males consulting for couple infertility over a 20-year period in Marseille, France. Asian Journal of Andrology, 14, 584-590. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Giblin P. T., Poland M. L., Moghissi K. S., Ager J. W., Olson J. M. (1988). Effects of stress and characteristic adaptability on semen quality in healthy men. Fertility and Sterility, 49, 127-132. [DOI] [PubMed] [Google Scholar]
- Giles M. L., Barak S., Baker G., Perna S., Tabrizi S., Greengrass V., . . . Knight R. L. (2011). Outcomes from the first assisted reproduction program for HIV-serodiscordant couples in Australia. Medical Journal of Australia, 195, 599-601. [DOI] [PubMed] [Google Scholar]
- Gray L. (1982). Neonatal chlordecone exposure alters behavioral sex differentiation in female hamsters. Neurotoxicology, 3, 67-80. [PubMed] [Google Scholar]
- Gui-Yuan Z., Meng-Chun J., Jin-Lai C., Wen-Qing Y. (1989). The effect of long-term treatment with crude cotton seed oil on pituitary and testicular function in men. International Journal of Andrology, 12, 404-410. [DOI] [PubMed] [Google Scholar]
- Gyllenborg J., Skakkebæk N. E., Nielsen N. C., Keiding N., Giwercman A. (1999). Secular and seasonal changes in semen quality among young Danish men: A statistical analysis of semen samples from 1927 donor candidates during 1977-1995. International Journal of Andrology, 22, 28-36. [DOI] [PubMed] [Google Scholar]
- Hadjkacem Loukil L., Hadjkacem H., Bahloul A., Ayadi H. (2015). Relation between male obesity and male infertility in a Tunisian population. Andrologia, 47, 282-285. [DOI] [PubMed] [Google Scholar]
- Haidl G., Jung A., Schill W. B. (1996). Aging and sperm function. Human Reproduction, 11, 558-560. [DOI] [PubMed] [Google Scholar]
- Haimov-Kochman R., Har-Nir R., Ein-Mor E., Ben-Shoshan V., Greenfield C., Eldar I., . . . Hurwitz A. (2012). Is the quality of donated semen deteriorating? Findings from a 15 year longitudinal analysis of weekly sperm samples. Israel Medical Association Journal, 14, 372-377. [PubMed] [Google Scholar]
- Hamill P. V., Steinberger E., Levine R. J., Rodriguez-Rigau L. J., Lemeshow S., Avrunin J. S. (1982). The epidemiologic assessment of male reproductive hazard from occupational exposure to TDA and DNT. Journal of Occupational Medicine, 24, 985-993. [PubMed] [Google Scholar]
- Hammiche F., Laven J. S., Boxmeer J. C., Dohle G. R., Steegers E. A. P., Steegers-Theunissen R. P. M. (2011). Sperm quality decline among men below 60 years of age undergoing IVF or ICSI treatment. Journal of Andrology, 32, 70-76. [DOI] [PubMed] [Google Scholar]
- Hammiche F., Laven J. S., Twigt J. M., Boellaard W. P., Steegers E. A., Steegers-Theunissen R. P. (2012). Body mass index and central adiposity are associated with sperm quality in men of subfertile couples. Human Reproduction, 27, 2365-2372. [DOI] [PubMed] [Google Scholar]
- Handelsman D. J. (1997). Sperm output of healthy men in Australia: Magnitude of bias due to self-selected volunteers. Human Reproduction, 12, 2701-2705. [DOI] [PubMed] [Google Scholar]
- Handelsman D. J., Conway A. J., Boylan L. M., Turtle J. R. (1984). Testicular function in potential sperm donors: Normal ranges and the effects of smoking and varicocele. International Journal of Andrology, 7, 369-382. [DOI] [PubMed] [Google Scholar]
- Hauser R., Williams P., Altshul L., Calafat A. M. (2005). Evidence of interaction between polychlorinated biphenyls and phthalates in relation to human sperm motility. Environmental Health Perspectives, 113, 425-430. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hellstrom W. J., Overstreet J. W., Sikka S. C., Denne J., Ahuja S., Hoover A. M., . . . Whitaker J. S. (2006). Semen and sperm reference ranges for men 45 years of age and older. Journal of Andrology, 27, 421-428. [DOI] [PubMed] [Google Scholar]
- Hernández-Ochoa I., García-Vargas G., López-Carrillo L., Rubio-Andrade M., Morán-Martínez J., Cebrián M. E., Quintanilla-Vega B. (2005). Low lead environmental exposure alters semen quality and sperm chromatin condensation in northern Mexico. Reproductive Toxicology, 20, 221-228. [DOI] [PubMed] [Google Scholar]
- Heussner J. C., Ward J. B., Jr., Legator M. S. (1985). Genetic monitoring of aluminum workers exposed to coal tar pitch volatiles. Mutation Research, 155, 143-155. [DOI] [PubMed] [Google Scholar]
- Homonnai Z. T., Fainman N., David M. P., Paz G. F. (1982). Semen quality and sex hormone pattern of 29 middle aged men. Andrologia, 14, 164-170. [DOI] [PubMed] [Google Scholar]
- Hovatta O., Venalainen E. R., Kuusimaki L., Heikkila J., Hirvi T., Reima I. (1998). Aluminium, lead and cadmium concentrations in seminal plasma and spermatozoa, and semen quality in Finnish men. Human Reproduction, 13, 115-119. [DOI] [PubMed] [Google Scholar]
- Ibrahim M. E., Moussa M. A. A., Pedersen H. (1988). Sperm chromatin heterogeneity as an infertility factor. Archives of Andrology, 21, 129-133. [DOI] [PubMed] [Google Scholar]
- Ikechebula J. I., Adinma J. I., Orie E. F., Ikegwuonu S. O. (2003). High prevalence of male infertility in South Eastern Nigeria. Journal of Obstetrics and Gynaecology, 23, 657-659. [DOI] [PubMed] [Google Scholar]
- Irvine S., Carwood E., Richardson D., MacDonald E., Aitken J. (1996). Evidence of deteriorating semen quality in the United Kingdom: Birth cohort study in 577 men in Scotland over 11 years. British Medical Journal, 312, 467-471. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Iwamoto T., Nozawa S., Yoshiike M., Hoshino T., Baba K., Matsushita T., . . . Jorgensen N. (2006). Semen quality of 324 fertile Japanese men. Human Reproduction, 21, 760-765. [DOI] [PubMed] [Google Scholar]
- Iwamoto T., Nozawa S., Yoshiike M., Namiki M., Koh E., Kanaya J., . . . Jorgensen N. (2013). Semen quality of fertile Japanese men: A cross-sectional population-based study of 792 men. BMJ Open, 3, e002223. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jager C., Aneck-Hahn N. H., Bornman M. S., Farias P., Spanò M. (2012). DDT exposure levels and semen quality of young men from a malaria area in South Africa. Malaria Journal, 11, 21.22243516 [Google Scholar]
- Jajoo S., Kalyani K. R. (2013). Prevalence of abnormal semen analysis in patients of infertility at a rural setup in Central India. International Journal of Reproduction, Contraception, Obstetrics and Gynecology, 2, 161-164. [Google Scholar]
- Jelnes J. E. (1988). Semen quality in workers producing reinforced plastic. Reproductive Toxicology, 2, 209-212. [DOI] [PubMed] [Google Scholar]
- Jensen T. K., Andersson A. M., Jorgensen N., Andersen A. G., Carlsen E., Petersen J. H., Skakkabaek N. E. (2004). Body mass index in relation to semen quality and reproductive hormones among 1,558 Danish men. Fertility and Sterility, 82, 863-870. [DOI] [PubMed] [Google Scholar]
- Jensen T. K., Giwercman A., Carlsen E., Scheike T., Skakkebaek N. E. (1996). Semen quality among members of organic food associations in Zealand, Denmark. Lancet, 347, 1844. [DOI] [PubMed] [Google Scholar]
- Jensen T. K., Vierula M., Hjollund N. H. I., Saaranen M., Scheike T., Saarikoski S., . . . Skakkabaek N. E. (2000). Semen quality among Danish and Finnish men attempting to conceive. European Journal of Endocrinology, 142, 47-52. [DOI] [PubMed] [Google Scholar]
- Jimoh A. A. G., Olawui T. S., Olaiya Omotoso G. O. (2012). Semen parameters and hormone profile of men investigated for infertility at Midland Fertility Centre, Ilorin, Nigeria. Journal of Basic and Applied Sciences, 8, 16-19. [Google Scholar]
- Johnson R. J., Segal M. S., Sautin Y., Nakagawa T., Feig D. I., Kang D. H., . . . Sanchez-Lozada L. G. (2007). Potential role of sugar (fructose) in the epidemic of hypertension, obesity and metabolic syndrome, diabetes, kidney disease, and cardiovascular disease. American Journal of Clinical Nutrition, 86, 899-906. [DOI] [PubMed] [Google Scholar]
- Jorgensen N., Joensen U. N., Jensen T. K., Jensen M. B., Almstrup K., Olesen I. A., . . . Skakkebaek N. E. (2012). Human semen quality in the new millennium: A prospective cross sectional population-based study of 4867 men. BMJ Open, 2, e000990-e001003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jorgensen N., Vierula M., Jacobsen R., Pukkala E., Perheentupa A., Virtanen H. E., . . . Toppari J. (2011). Recent adverse trends in semen quality and testis cancer incidence among Finnish men. International Journal of Andrology, 34, e37-e48. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jung A., Schuppe H. C., Schill W. B. (2002). Comparison of semen quality in older and younger men attending an andrology clinic. Andrologia, 34, 116-122. [DOI] [PubMed] [Google Scholar]
- Jurewicz J., Radwan M., Sobala W., Ligocka D., Radwan P., Bochenek M., . . . Hanke W. (2013). Human urinary phthalate metabolites level and main semen parameters, sperm chromatin structure, sperm aneuploidy and reproductive hormones. Reproductive Toxicology, 42, 232-241. [DOI] [PubMed] [Google Scholar]
- Keltz J., Zapantis A., Jindal S. K., Lieman H. J., Santoro N., Polotsky A. J. (2010). Overweight men: Clinical pregnancy after ART is decreased in IVF but not in ICSI cycles. Journal of Assisted Reproduction and Genetics, 27, 539-544. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kidd S. A., Eskenazi B., Wyrobek A. J. (2001). Effects of male age on semen quality and fertility: A review of the literature. Fertility and Sterility, 75, 237-248. [DOI] [PubMed] [Google Scholar]
- Kim Y., Jung K., Hwang T., Jung G., Kim H., Park J. (1996). Haematopoietic and reproductive hazards of Korean electronic workers exposed to solvents containing 2-bromopropane. Scandinavian Journal of Work, Environment & Health, 22, 387-391. [DOI] [PubMed] [Google Scholar]
- Kirei B. R. (1987). Semen characteristics in 120 fertile Tanzanian men. East African Medical Journal, 64, 453-457. [PubMed] [Google Scholar]
- Knez J., Kranvog L. R., Breznik B. P., Voncina E., Vlaisavljevic V. (2013). Are urinary bisphenol-A levels in men related to semen quality and embryo development after medically assisted reproduction? Fertility and Sterility, 101, 215e-221e. [DOI] [PubMed] [Google Scholar]
- Kolon T. F., Philips K. A., Buch J. P. (1992) Custom cryopreservation of human semen. Fertility and Sterility, 58, 1020-1023. [DOI] [PubMed] [Google Scholar]
- Koloszar S., Fejes I., Zavaczki Z., Daru J., Szollosi J., Pal A. (2005). Effect of body weight on sperm concentration in normozoospermic males. Archives of Andrology, 51, 299-304. [DOI] [PubMed] [Google Scholar]
- Krajewska-Kulak E., Sengupta P. (2013). Thyroid function in male infertility. Frontiers in Endocrinology, 4, 1-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lackner J., Schatzl G., Waldhör T., Resch K., Kratzik C., Marberger M. (2005). Constant decline in sperm concentration in infertile males in an urban population: Experience over 18 years. Fertility and Sterility, 84, 1657-1661. [DOI] [PubMed] [Google Scholar]
- La Vignera S., Condorelli R. A., Vicari E., Calogero A. E. (2012). Negative effect of increased body weight on sperm conventional and nonconventional flow cytometric sperm parameters. Journal of Andrology, 33, 53-58. [DOI] [PubMed] [Google Scholar]
- Lancranjan I. (1972). Alterations of spermatic liquid in patients chronically poisoned by carbon disulphide. Medicina del Lavoro, 63, 29-33. [PubMed] [Google Scholar]
- Lancranjan I., Popescu H., Gavanescu O., Klepsch I., Serbanescu M. (1975). Reproductive ability of workmen occupationally exposed to lead. Archives of Environmental Health, 30, 396-401. [DOI] [PubMed] [Google Scholar]
- Lapido O. A. (1980). Seminal analysis in fertile and infertile Nigerian men. Journal of the National Medical Association, 72, 785-789. [PMC free article] [PubMed] [Google Scholar]
- Laufer N., Margalioth E. J., Navot D., Shemesh A., Schenker J. G. (1985). Reduced penetration of zona-free hamster ova by cryopreserved human spermatozoa. Archives of Andrology, 14, 217-222. [DOI] [PubMed] [Google Scholar]
- Lenhart A., Purcell K., Smith A., Zickuhr K. (2010). Social media and mobile Internet use among teens and young adults. Washington, DC: Pew Research Centre. [Google Scholar]
- Łepecka-Klusek C., Wdowiak A., Pilewska-Kozak A. B., Syty K., Jakiel G. (2011). The role of age, environmental and occupational factors on semen density. Annals of Agricultural and Environmental Medicine, 18, 437-440. [PubMed] [Google Scholar]
- Levin R. M., Latimore J., Wein A. J., Van Arsdalen K. N. (1986). Correlation of sperm count with frequency of ejaculation. Fertility and Sterility, 45, 732-734. [DOI] [PubMed] [Google Scholar]
- Levine R. J., Brown M. H., Bell M., Shue F., Greenberg G. N., Bordson B. L. (1992). Air-conditioned environments do not prevent deterioration of human semen quality during the summer. Fertility and Sterility, 57, 1075-1083. [DOI] [PubMed] [Google Scholar]
- Lewis E. L., Brazil C. K., Overstreet J. W. (1984). Human sperm function in the ejaculate following vasectomy. Fertility and Sterility, 42, 895-898. [DOI] [PubMed] [Google Scholar]
- Li D. K., Zhou Z., Miao M., He Y., Wang J., Ferber J., . . . Yuan W. (2011). Urine bisphenol-A (BPA) level in relation to semen quality. Fertility and Sterility, 95, 625-630. [DOI] [PubMed] [Google Scholar]
- Liang X. W., Lu W. H., Chen Z. W., Wang X. H., Zhao H., Zhang G. Y., Gu Y. Q. (2008). Changes of semen parameters in Chinese fertile men in the past 25 years. Zhonghua Nan Ke Xue, 14, 775-778. [PubMed] [Google Scholar]
- Lotti F., Corona G., Colpi G. M., Filimberti E., Degli Innocenti S., Mancini M., . . . Maggi M. (2011). Elevated body mass index correlates with higher seminal plasma interleukin 8 levels and ultrasonographic abnormalities of the prostate in men attending an andrology clinic for infertility. Journal of Endocrinological Investigation, 34, e336-e342. [DOI] [PubMed] [Google Scholar]
- Luetjens C. M., Rolf C., Gassner P., Werny J. E., Nieschlag E. (2002). Sperm aneuploidy rates in younger and older men. Human Reproduction, 17, 1826-1832. [DOI] [PubMed] [Google Scholar]
- Mably T., Bjerke D., Moore R., Gendron-Fitzpatrick A., Peterson R. (1992). In utero and lactational exposure of male rats to 2,3,7,8-tetrachlorodibenzo-p-dioxin: 3. Effects on spermatogenesis and reproductive capability. Toxicology and Applied Pharmacology, 114, 118-126. [DOI] [PubMed] [Google Scholar]
- Magnusdottir E. V., Thorsteinsson T., Thorsteinsdottir S., Heimisdottir M., Olafsdottir K. (2005). Persistent organochlorines, sedentary occupation, obesity and human male subfertility. Human Reproduction, 20, 208-215. [DOI] [PubMed] [Google Scholar]
- Mahmoud A. M., Goemaere S., El-Garem Y., Van Pottelbergh I., Comhaire F. H., Kaufman J. M. (2003). Testicular volume in relation to hormonal indices of gonadal function in community-dwelling elderly men. Journal of Clinical Endocrinology and Metabolism, 88, 179-184. [DOI] [PubMed] [Google Scholar]
- Maier D. B., Newbold R. R., McLachlan J. A. (1985). Prenatal diethylstilbestrol exposure alters murine uterine responses to prepubertal estrogen stimulation. Endocrinology, 116, 1878-1886. [DOI] [PubMed] [Google Scholar]
- Mallidis C., Howard E. J., Baker H. W. G. (1991). Variation of semen quality in normal men. International Journal of Andrology, 14, 99-107. [DOI] [PubMed] [Google Scholar]
- Marimuthu P., Kapilashrami M. C., Misro M. M., Singh G. (2003). Evaluation of trend in semen analysis for 11 years in subjects attending a fertility clinic in India. Asian Journal of Andrology, 5, 221-225. [PubMed] [Google Scholar]
- Martini A. C., Tissera A., Estofan D., Molina R. I., Mangeaud A., de Cuneo M. F., Ruiz R. D. (2010). Overweight and seminal quality: A study of 794 patients. Fertility and Sterility, 94, 1739-1743. [DOI] [PubMed] [Google Scholar]
- Meeker J. D., Ehrlich S., Toth T. L., Wright D. L., Calafat A. M., Trisini A. T., . . . Hauser R. (2010). Semen quality and sperm DNA damage in relation to urinary bisphenol A among men from an infertility clinic. Reproductive Toxicology, 30, 532-539. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Meeker J. D., Rossano M. G., Protas B., Diamond M. P., Puscheck E., Daly D., . . . Wirth J. J. (2008). Cadmium, lead, and other metals in relation to semen quality: Human evidence for molybdenum as a male reproductive toxicant. Environmental Health Perspectives, 116, 1473-1479. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mehta R. H., Makwana S., Ranga G. M., Srinivasan R. J., Virk S. S. (2006). Prevalences of oligozoospermia and azoospermia in male partners of infertile couples from different parts of India. Asian Journal of Andrology, 8, 89-93. [DOI] [PubMed] [Google Scholar]
- Mendiola J., Jørgensen N., Andersson A. M., Calafat A. M., Ye X., Redmon J. B., . . . Swan S. H. (2010). Are environmental levels of bisphenol A associated with reproductive function infertile men? Environmental Health Perspectives, 118, 1286-1291. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mendiola J., Jørgensen N., Mínguez-Alarcón L., Sarabia-Cos L., López-Espín J. J., Vivero-Salmerón G., . . . Torres-Cantero A. M. (2013). Sperm counts may have declined in young university students in Southern Spain. Andrology, 1, 408-413. [DOI] [PubMed] [Google Scholar]
- Meyer C. (1981) Semen quality in workers exposed to carbon disulphide compared to a control group from the same plant. Journal of Occupational Medicine, 23, 435-439. [DOI] [PubMed] [Google Scholar]
- Mieusset R., Bujan L., Mansat A., Grandjean H., Pontonnier F. (1991). Heat induced inhibition of spermatogenesis in man. Advances in Experimental Medicine and Biology, 286, 233-237. [DOI] [PubMed] [Google Scholar]
- Milby T. H., Whorton D. (1980). Epidemiological assessment of occupationally related, chemically induced sperm count suppression. Journal of Occupational Medicine, 22, 77-82. [DOI] [PubMed] [Google Scholar]
- Molina R. I., Martini A. C., Tissera A., Olmedo J., Senestrari D., de Cuneo M. F., Ruiz R. D. (2010). Semen quality and aging: Analysis of 9,168 samples in Cordoba, Argentina. Archivos Espanoles de Urologia, 63, 214-222. [PubMed] [Google Scholar]
- Møller H., Skakkebæk N. E. (1999). Risk of testicular cancer in subfertile men: Case-control study. British Medical Journal, 318, 559-562. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mori M. M., Cedenho A. P., Koifman S., Srougi M. (2002). Sperm characteristics in a sample of healthy adolescents in São Paulo, Brazil. Cad Saúde Pública Rio de Janeiro, 18, 525-530. [DOI] [PubMed] [Google Scholar]
- Mukhopadhyay D., Varghese A. C., Pal M., Banerjee S. K., Bhattacharyya A. K., Sharma R. K. (2010). Semen quality and age-specific changes: A study between two decades on 3729 male partners of couples with normal sperm count and attending an andrology laboratory for infertility-related problems in an Indian city. Fertility and Sterility, 93, 2247-2254. [DOI] [PubMed] [Google Scholar]
- Multigner L., Spira A. (1997). The epidemiology of male reproduction. In Barrat C., De Jonge C., Mortimer D., Parinaud J. (Eds.), Genetics of human male fertility (pp. 43-65). Paris, France: EDK. [Google Scholar]
- Negro-Vilar A. (1993). Stress and other environmental factors affecting fertility in men and women: Overview. Environmental Health Perspectives, 101, 59-64. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nelson C. M. K., Bunge R. G. (1974). Semen analysis-evidence of changing parameters of male fertility potential. Fertility and Sterility, 25, 503-507. [DOI] [PubMed] [Google Scholar]
- Ng K. K., Donat R., Chan L., Lalak A., Pierro I. D., Handelsman D. J. (2004). Sperm output of older men. Human Reproduction, 19, 1811-1815. [DOI] [PubMed] [Google Scholar]
- Nguyen R. H., Wilcox A. J., Skjaerven R., Baird D. D. (2007). Men’s body mass index and infertility. Human Reproduction, 22, 2488-2493. [DOI] [PubMed] [Google Scholar]
- Nie Z. Y., Wu H. F., Zhang N., Guo L. N., Zhao S. Y., Zhen X. L., Lu C. T. (2012). Effects of males’ age on sperm apoptosis and DNA integrity. Zhonghua Nan Ke Xue, 18, 1004-1008. [PubMed] [Google Scholar]
- Nieschlag E., Lammers U., Freischem C., Langer K., Wickings E. (1982). Reproductive functions in young fathers and grandfathers. Journal of Clinical Endocrinology and Metabolism, 55, 676-681. [DOI] [PubMed] [Google Scholar]
- Nirupa S., Kalaiselvi V. S., Saraswathi V., Prabhu K., Sivaram E., Prashanth Krishna G. (2014). Analysis of semen parameters with age of infertile male subjects: A pilot study in an urban population, Chennai. Research Journal of Pharmaceutical, Biological and Chemical Sciences, 5, 407-410. [Google Scholar]
- Nnatu S. N., Giwa-Osagie O. F., Essien E. E. (1991). Effect of repeated semen ejaculation on sperm quality. Clinical and Experimental Obstetrics & Gynecology, 18, 39-42. [PubMed] [Google Scholar]
- Noack-Fuller G., De Beer C., Seibert H. (1993). Cadmium, lead, selenium, and zinc in semen of occupationally unexposed men. Andrologia, 25, 7-12. [DOI] [PubMed] [Google Scholar]
- Okonofua F., Menakaya U., Onemu S. O., Omo-Aghaja L. O., Bergstrom S. (2005). A case-control study of risk factors for male infertility in Nigeria. Asian Journal of Andrology, 7, 351-361. [DOI] [PubMed] [Google Scholar]
- Oliva A., Spira A., Multigner L. (2001). Contribution of environmental factors to the risk of male infertility. Human Reproduction, 16, 1768-1776. [DOI] [PubMed] [Google Scholar]
- Osegbe D. N., Amaku E. O., Nnatu S. N. (1986). Are changing semen parameters a universal phenomenon? European Urology, 12, 164-168. [DOI] [PubMed] [Google Scholar]
- Osser S., Gennser G., Liedholm P., Ranstam J. (1983). Variation of semen parameters in fertile men. Archives of Andrology, 10, 127-133. [DOI] [PubMed] [Google Scholar]
- Paasch U., Grunewald S., Kratzsch J., Glander H. J. (2010). Obesity and age affect male fertility potential. Fertility and Sterility, 94, 2898-2901. [DOI] [PubMed] [Google Scholar]
- Pal P. C., Rajalakshmi M., Manocha M., Sharma R. S., Mittal S., Rao D. N. (2006). Semen quality and sperm functional parameters in fertile Indian men. Andrologia, 38, 20-25. [DOI] [PubMed] [Google Scholar]
- Panidis D. K., Asseo P. P., Papaloucas A. C. (1984). Semen parameters in 114 fertile men. European Journal of Obstetrics, Gynecology, and Reproductive Biology, 16, 411-420. [DOI] [PubMed] [Google Scholar]
- Pant N., Manju S., Patel D. K., Shukla Y., Mathur N., Gupta Y. K., Saxena D. K. (2008). Correlation of phthalate exposures with semen quality. Toxicology and Applied Pharmacology, 231, 112-116. [DOI] [PubMed] [Google Scholar]
- Pasqualotto F. F., Sobreiro B. P., Hallak J., Pasqualotto E. B., Lucon A. M. (2005). Sperm concentration and normal sperm morphology decrease and follicle-stimulating hormone level increases with age. BJU International, 96, 1087-1091. [DOI] [PubMed] [Google Scholar]
- Pol P. S., Beuscart R., Leroy-Martin B., Hermand E., Jablonski W. (1989). Circannual rhythm of sperm parameters of fertile men. Fertility and Sterility, 51, 1030-1033. [DOI] [PubMed] [Google Scholar]
- Ramlau-Hansen C. H., Hansen M., Jensen C. R., Olsen J., Bonde J. P., Thulstrup A. M. (2010). Semen quality and reproductive hormones according to birthweight and body mass index in childhood and adult life: Two decades of follow-up. Fertility and Sterility, 94, 610-618. [DOI] [PubMed] [Google Scholar]
- Ramlau-Hansen C. H., Thulstrup A. M., Nohr E. A., Bonde J. P., Sorensen T. I., Olsen J. (2007). Subfecundity in overweight and obese couples. Human Reproduction, 22, 1634-1637. [DOI] [PubMed] [Google Scholar]
- Rasmussen K., Sabroe S., Wohlert M., Ingerslev H. J., Kappel B., Nielson J. (1988). A genotoxic study of metal workers exposed to trichlorethylene. International Archives of Occupational and Environmental Health, 60, 419-423. [DOI] [PubMed] [Google Scholar]
- Rasmussen P. E., Erb K., Westergaard L. G., Laursen S. B. (1997). No evidence for decreasing semen quality in four birth cohorts of 1,055 Danish men born between 1950 and 1970. Fertility and Sterility, 68, 1059-1064. [DOI] [PubMed] [Google Scholar]
- Ratcliffe J., Schrader S., Steenland K., Clapp D., Turner T., Hornung R. (1987). Semen quality in papaya workers with long term exposure to ethylene dibromide. British Journal of Industrial Medicine, 44, 317-332. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Relwani R., Berger D., Santoro N., Hickmon C., Nihsen M., Zapantis A., . . . Jindal S. (2011). Semen parameters are unrelated to BMI but vary with SSRI use and prior urological surgery. Reproductive Sciences, 18, 391-397. [DOI] [PubMed] [Google Scholar]
- Richardson D. W., Aitken R. J., Loudon N. B. (1984). The functional competence of human spermatozoa recovered after vasectomy. Journal of Reproduction and Fertility, 70, 575-579. [DOI] [PubMed] [Google Scholar]
- Rignell-Hydbom A., Rylander L., Giwercman A., Jönsson B. A., Lindh C., Eleuteri P., . . . Hagmar L. (2005). Exposure to PCBs and p,p¢-DDE and human sperm chromatin integrity. Environmental Health Perspectives, 113, 175-179. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Robins T. G., Bornman M. S., Ehrlich R. I., Cantrell A. C., Pienaar E., Vallabh J., Miller S. (1997). Semen quality and fertility of men employed in a South African lead acid battery plant. American Journal of Industrial Medicine, 32, 369-376. [DOI] [PubMed] [Google Scholar]
- Rolf C., Behre H., Nieschlag E. (1996). Reproductive parameters of older compared to younger men of infertile couples. International Journal of Andrology, 19, 135-142. [DOI] [PubMed] [Google Scholar]
- Rolland M., Le Moal J., Wagner V., Royère D., De Mouzon J. (2013). Decline in semen concentration and morphology in a sample of 26609 men close to general population between 1989 and 2005 in France. Human Reproduction, 28, 462-470. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Romero-Otero J., Medina-Polo J., García-Gómez B., Lora-Pablos D., Duarte-Ojeda J. M., García-González L., . . . Rodríguez-Antolín A. (2015). Semen quality assessment in fertile men in Madrid during the last 3 decades. Urology, 85, 1333-1338. [DOI] [PubMed] [Google Scholar]
- Rosenberg M. J., Wyrobek A. J., Ratcliffe J., Gordon L. A., Watchmaker G., Fox S. H., . . . Hornung R. W. (1985). Sperm as an indicator of reproductive risk among petroleum refinery workers. British Journal of Industrial Medicine, 42, 123-127. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rosenstock T. S., Liptzin D., Six J., Tomich T. P. (2013). Nitrogen fertilizer use in California: Assessing the data, trends and way forward. California Agriculture, 67, 68-79. [Google Scholar]
- Royal College of Physicians. (2012). Fifty years since smoking and health. Progress, lessons and priorities for a smoke-free UK. Regent’s Park, London: Author. [Google Scholar]
- Rui H., Thomassen Y., Oldereid N. B., Purvis K. (1986). Accessory sex gland function in normal young (20-25 years) and middle-aged (50-55 years) men. Journal of Andrology, 7, 93-99. [DOI] [PubMed] [Google Scholar]
- Saaranen M., Suonio S., Kauhanen O., Saarikoski S. (1987). Cigarette smoking and semen quality in men of reproductive age. Andrologia, 19, 670-676. [DOI] [PubMed] [Google Scholar]
- Saidi J. A., Chang D. T., Goluboff E. T., Bagiella E., Olsen G., Fisch H. (1999). Declining sperm counts in the United States? A critical review. Journal of Urology, 161, 460-462. [PubMed] [Google Scholar]
- Sallmen M., Sandler D. P., Hoppin J. A., Blair A., Baird D. D. (2006). Reduced fertility among overweight and obese men. Epidemiology, 17, 520-523. [DOI] [PubMed] [Google Scholar]
- Schneider G., Kirschner M. A., Berkowitz R., Ertel N. H. (1979). Increased estrogen production in obese men. Journal of Clinical Endocrinology and Metabolism, 48, 633-638. [DOI] [PubMed] [Google Scholar]
- Schrader S. M., Turner T. W., Breitenstein M. J., Simon S. D. (1988). Longitudinal study of semen quality of unexposed workers. I. Study overview. Reproductive Toxicology, 2, 183-190. [DOI] [PubMed] [Google Scholar]
- Schwartz D., Mayaux M.-J., Spira A., Moscato M.-L., Jouannet P., Czyglik F., David G. (1983). Semen characteristics as a function of age in 833 fertile men. Fertility and Sterility, 39, 530-535. [DOI] [PubMed] [Google Scholar]
- Sengupta P. (2013). Potential health impacts of hard water. International Journal of Preventive Medicine, 4, 866-875. [PMC free article] [PubMed] [Google Scholar]
- Sengupta P. (2014. a). Current trends of male reproductive health disorders and the changing semen quality. International Journal of Preventive Medicine, 5, 1-5. [PMC free article] [PubMed] [Google Scholar]
- Sengupta P. (2014. b). Recent trends in male reproductive health problems. Asian Journal of Pharmaceutical and Clinical Research, 7, 1-5. [Google Scholar]
- Sengupta P. (2015). Reviewing reports of semen volume and male ageing in last 33 years: From 1980 through 2013. Asian Pacific Journal of Reproduction, 4, 242-246. [Google Scholar]
- Sengupta P., Banerjee R. (2014). Environmental toxins: Alarming impacts of pesticides on male fertility. Human & Experimental Toxicology, 33, 1017-1039. [DOI] [PubMed] [Google Scholar]
- Sengupta P., Banerjee R., Nath S., Das S., Banerjee S. (2015). Metals and female reproductive toxicity. Human & Experimental Toxicology, 34, 679-697. [DOI] [PubMed] [Google Scholar]
- Shaarawy M., Mahmoud K. Z. (1982). Endocrine profile and semen characteristics in male smokers. Fertility and Sterility, 38, 255-257. [DOI] [PubMed] [Google Scholar]
- Shafik A., Olfat S. (1981). Scrotal lipomatosis. British Journal of Urology, 53, 50-54. [DOI] [PubMed] [Google Scholar]
- Sharpe R. (1993). Falling sperm counts in men—Is there an endocrine cause? Journal of Endocrinology, 137, 357-360. [DOI] [PubMed] [Google Scholar]
- Sharpe R., Fisher J., Millar M., Jobling S., Sumpter J. (1995). Gestational and lactational exposure of rats to xenoestrogens results in reduced testicular size and sperm production. Environmental Health Perspectives, 103, 1136-1143. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sharpe R. M., Skakkebæk N. E. (1993). Are oestrogens involved in falling sperm counts and disorders of the male reproductive tract? Lancet, 341, 1392-1395. [DOI] [PubMed] [Google Scholar]
- Shayeb A. G., Harrild K., Mathers E., Bhattacharya S. (2011). An exploration of the association between male body mass index and semen quality. Reproductive Biomedicine Online, 23, 717-723. [DOI] [PubMed] [Google Scholar]
- Sheriff D. S. (1983). Setting standards of male fertility. I. Semen analyses in 1500 patients-a report. Andrologia, 15, 687-692. [DOI] [PubMed] [Google Scholar]
- Sheriff D. S. (1987). Semen analyses in Hansen’s disease. Transactions of the Royal Society of Tropical Medicine and Hygiene, 81, 113-114. [DOI] [PubMed] [Google Scholar]
- Sheriff D. S., Legnain M. (1992). Evaluation of semen quality in a local Libyan population. Indian Journal of Physiology and Pharmacology, 36, 83-87. [PubMed] [Google Scholar]
- Shrivastav P., Swann J., Jeremy J. Y., Thompson C., Shaw R. W., Dandona P. (1989). Sperm function and structure and seminal plasma prostanoid concentrations in men with IDDM. Diabetes Care, 12, 742-744. [DOI] [PubMed] [Google Scholar]
- Singer R., Sagiv M., Levinsky H., Allalouf D. (1990). Andrological parameters in men with high sperm counts and possible correlation with age. Archives of Andrology, 24, 107-111. [DOI] [PubMed] [Google Scholar]
- Skakkebæk N. E., Rajpert-De Meyts E., Jørgensen N., Carlsen E., Petersen P. M., Giwercman A., . . . Muller J. (1998). Germ cell cancer and disorders of spermatogenesis: An environmental connection? APMIS, 106, 3-12. [DOI] [PubMed] [Google Scholar]
- Sobowale O. B., Akiwumi O. (1989). Testicular voltnie and seminal fluid profile in fertile and infertile males in Ilorin, Nigeria. International Journal of Gynaecology and Obstetrics, 28, 155-161. [DOI] [PubMed] [Google Scholar]
- Spandorfer S. D., Avrech O. M., Colombero L. T., Palermo G. D., Rosenwaks Z. (1998). Effect of parental age on fertilization and pregnancy characteristics in couples treated by intracytoplasmic sperm injection. Human Reproduction, 13, 334-338. [DOI] [PubMed] [Google Scholar]
- Spira A. (1984). Seasonal variations of sperm characteristics. Archives of Andrology, 12, 23-28. [PubMed] [Google Scholar]
- Sripada S., Fonseca S., Lee A., Harrild K., Giannaris D., Mathers E., Bhattacharya S. (2007). Trends in semen parameters in the northeast of Scotland. Journal of Andrology, 28, 313-319. [DOI] [PubMed] [Google Scholar]
- Stanwell-Smith R., Thompson S. G., Haines A. P., Ward R. J., Cashmore G., Stedronska J., Hendry W. F. (1983). A comparative study of zinc, copper, cadmium, and lead levels in fertile and infertile men. Fertility and Sterility, 40, 670-677. [DOI] [PubMed] [Google Scholar]
- Stellato R. K., Feldman H. A., Hamdy O., Horton E. S., McKinlay J. B. (2000). Testosterone, sex hormone-binding globulin, and the development of type 2 diabetes in middle-aged men: Prospective results from the Massachusetts male aging study. Diabetes Care, 23, 490-494. [DOI] [PubMed] [Google Scholar]
- Stewart T. M., Liu D. Y., Garrett C., Jørgensen N., Brown E. H., Baker H. W. (2009). Associations between andrological measures, hormones and semen quality in fertile Australian men: Inverse relationship between obesity and sperm output. Human Reproduction, 24, 1561-1568. [DOI] [PubMed] [Google Scholar]
- Stone B. A., Alex A., Werlin L. B., Marrs R. P. (2013). Age thresholds for changes in semen parameters in men. Fertility and Sterility, 100, 952-958. [DOI] [PubMed] [Google Scholar]
- Sugkraroek P., Kates M., Leader A., Tanphaichitr N. (1991). Levels of cholesterol and phospholipids in freshly ejaculated sperm and Percoll-gradient-pelletted sperm from fertile and unexplained infertile men. Fertility and Sterility, 55, 820-827. [PubMed] [Google Scholar]
- Sundaram K., Witorsch R. (1995). Toxic effects on the testes. In Witorsch R. (Ed.) Reproductive toxicology (pp. 99-122). London, England: Taylor & Francis. [Google Scholar]
- Swan S. H., Elkin E. P., Fenster L. (1997). Have sperm densities declined? A reanalysis of global trend data. Environmental Health Perspectives, 105, 1228-1232. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Swanson R. J., Mayer J. F., Jones K. H., Lanzendorf S. E., McDowell J. (1984). Hamster ova/human sperm penetration: Correlation with count, motility, and morphology for in vitro fertilization. Archives of Andrology, 12, 69-77. [PubMed] [Google Scholar]
- Telisman S., Cvitković P., Jurasović J., Pizent A., Gavella M., Rocić B. (2000). Semen quality and reproductive endocrine function in relation to biomarkers of lead, cadmium, zinc, and copper in men. Environmental Health Perspectives, 108, 45-53. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tang L. X., Wang Q. L., Tang Y. G., Jiang F., Wang L. L., Huang J. T. (2013). Semen quality of normal fertile men. Zhonghua Nan Ke Xue, 19, 789-793. [PubMed] [Google Scholar]
- Tang Y. G., Tang L. X., Wang Q. L., Song G., Jiang Y. J., Deng S. M., . . . Qin W. B. (2015). The reference values for semen parameters of 1213 fertile men in Guangdong Province in China. Asian Journal of Andrology, 17, 298-303. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Thonneau P., Bujan L., Multigner L., Mieusset R. (1998). Occupational heat exposure and male fertility. Human Reproduction, 13, 2122-2125. [DOI] [PubMed] [Google Scholar]
- Tjoa W. S., Smolensky M. H., His B. P., Steinberger E., Smith K. D. (1982). Circannual rhythm in human sperm count revealed by serially independent sampling. Fertility and Sterility, 38, 454-459. [DOI] [PubMed] [Google Scholar]
- Toft G., Pedersen H. S., Bonde J. P. (2004). Semen quality in Greenland. International Journal of Circumpolar Health, 63, 174-178. [DOI] [PubMed] [Google Scholar]
- Toppari J., Larsen J. C., Christiansen P., Giwercman A., Grandjean P., Guillette L. J., Jr., . . . Skakkebaek N. E. (1996). Male reproductive health and environmental xenoestrogens. Environmental Health Perspectives, 104, 741-803. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Torkelson T. (1961). Toxicological investigations of 1,2-dibromo-3-chloropropane. Toxicology and Applied Pharmacology, 3, 545. [DOI] [PubMed] [Google Scholar]
- Tortolero I., Bellabarbaarata G., Lozano R., Bellabarba C., Cruz I., Osuna J. (1999). Semen analysis in men from Merida, Venezuela over a 15-year period. Archives of Andrology, 42, 29-34. [DOI] [PubMed] [Google Scholar]
- Tullner W. (1961). Uterotrophic action of the insecticide methoxychlor. Science, 133, 647-648. [DOI] [PubMed] [Google Scholar]
- Tunc O., Bakos H. W., Tremellen K. (2011). Impact of body mass index on seminal oxidative stress. Andrologia, 43, 121-128. [DOI] [PubMed] [Google Scholar]
- Ugwuja E. I., Ugwu N. C., Ejikeme B. N. (2008). Prevalence of low sperm count and abnormal semen parameters in male partners of women consulting at infertility clinic in Abakaliki, Nigeria. African Journal of Reproductive Health, 12, 67-73. [PubMed] [Google Scholar]
- Venable J. R., McClimans C. D., Flake R. E., Dimick D. B. (1980). A fertility study of male employees engaged in the manufacture of glycerine. Journal of Occupational Medicine, 22, 87-91. [DOI] [PubMed] [Google Scholar]
- Vicari E., Conticello A., Battiato C., La Vignera S. (2003). Sperm characteristics in fertile men and healthy men of the South-East Sicily from year 1982 to 1999. Archivio Italiano di Urologia e Andrologia, 75, 28-34. [PubMed] [Google Scholar]
- Vierula M., Niemi M., Keiski A., Saaranen M., Saarikoski S., Suominen J. (1996). High and unchanged sperm counts of Finnish men. International Journal of Andrology, 19, 11-17. [DOI] [PubMed] [Google Scholar]
- Vignon F., Le Faou A., Montagnon D., Pradignac A., Cranz C., Winiszewsky P., Pinget M. (1991). Comparative study of semen in diabetic and healthy men. Diabetes & Metabolism, 17, 350-354. [PubMed] [Google Scholar]
- Vogt H. J., Heller W. D., Borelli S. (1986). Sperm quality of healthy smokers, ex-smokers, and never-smokers. Fertility and Sterility, 45, 106-110. [DOI] [PubMed] [Google Scholar]
- Vujkovic M., de Vries J. H., Dohle G. R., Bonsel G. J., Lindemans J., Macklon N. S., . . . Steegers-Theunissen R. P. (2009). Associations between dietary patterns and semen quality in men undergoing IVF/ICSI treatment. Human Reproduction, 24, 1304-1312. [DOI] [PubMed] [Google Scholar]
- Wallace E. M., Gow S. M., Wu F. C. (1993). Comparison between testosterone enanthate-induced azoospermia and oligozoospermia in a male contraceptive study. I: Plasma luteinizing hormone, follicle stimulating hormone, testosterone, estradiol, and inhibin concentrations. Journal of Clinical Endocrinology and Metabolism, 77, 290-293. [DOI] [PubMed] [Google Scholar]
- Wang C., Chan S. Y. W., Leung A., Ng R. P., Ng M., Tang L. C., . . . Kwan M. (1985). Cross-sectional study of semen parameters in a large group of normal Chinese men. International Journal of Andrology, 8, 257-274. [DOI] [PubMed] [Google Scholar]
- Wang C., Yeung K. K. (1980). Use of low-dosage oral cyproterone acetate as a male contraceptive. Contraception, 21, 245-272. [DOI] [PubMed] [Google Scholar]
- Ward J. B., Jr., Hokanson J. A., Smith E. R., Chang L. W., Pereira M. A., Whorton E. B., Jr., Legator M. S. (1984). Sperm count, morphology and fluorescent body frequency in autopsy service workers exposed to formaldehyde. Mutation Research, 130, 417-424. [DOI] [PubMed] [Google Scholar]
- Wdowiak A., Wdowiak L., Wiktor H. (2007). Evaluation of the effect of using mobile phones on male fertility. Annals of Agriculture and Environmental Medicine, 14, 169-172. [PubMed] [Google Scholar]
- Weidner W., Jantos C., Schiefer H. G., Haidl G., Friedrich H. J. (1991). Semen parameters in men with and without proven chronic prostatitis. Archives of Andrology, 26, 173-183. [DOI] [PubMed] [Google Scholar]
- Welch L. S., Schrader S. M., Turner T. W., Cullen M. R. (1988). Effects of exposure to ethylene glycol ethers on shipyard painters: II. Male reproduction. American Journal of Industrial Medicine, 14, 509-526. [DOI] [PubMed] [Google Scholar]
- Weyandt T. B., Schrader S. M., Turner T. W., Simon S. D. (1996). Semen analysis of military personnel associated with military duty assignments. Reproductive Toxicology, 10, 521-528. [DOI] [PubMed] [Google Scholar]
- Whorton D., Krauss R., Marshall S., Milby T. (1977). Infertility in male pesticide workers. Lancet, 2, 1259-1260. [DOI] [PubMed] [Google Scholar]
- Wickings E. J., Freischem C. W., Langer K., Nieschlag E. (1983). Heterologous ovum penetration test and seminal parameters in fertile and infertile men. Journal of Andrology, 4, 261-271. [DOI] [PubMed] [Google Scholar]
- Winkle T., Rosenbusch B., Gagsteiger F., Paiss T., Zoller N. (2009). The correlation between male age, sperm quality and sperm DNA fragmentation in 320 men attending a fertility center. Journal of Assisted Reproduction and Genetics, 26, 41-46. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Winters S. J., Wang C., Abdelrahaman E., Hadeed V., Dyky M. A., Brufsky A. (2006). Inhibin-B levels in healthy young adult men and prepubertal boys: Is obesity the cause for the contemporary decline in sperm count because of fewer Sertoli cells? Journal of Andrology, 27, 560-564. [DOI] [PubMed] [Google Scholar]
- Wirth J. J., Rossano M. G., Potter R., Puscheck E., Daly D. C., Paneth N., . . . Diamond M. P. (2008). A pilot study associating urinary concentrations of phthalate metabolites and semen quality. Systems Biology in Reproductive Medicine, 54, 143-154. [DOI] [PubMed] [Google Scholar]
- World Health Organization. (1991). Infertility: A tabulation of available data on prevalence of primary and secondary infertility (Programme on Material and Child Health and Family Planning, Division of Family Health). Geneva, Switzerland: Author. [Google Scholar]
- World Health Organization. (2014). Obesity and overweight. Geneva, Switzerland: Author. [Google Scholar]
- Wyrobek A. J., Brodsky J., Gordon L., Moore D. H., Watchmaker G., Cohen E. N. (1981). Sperm studies in anesthesiologists. Anesthesiology, 55, 527-532. [DOI] [PubMed] [Google Scholar]
- Wyrobek A. J., Gordon L. A., Burkhart J. G., Francis M. W., Kapp R. W., Letz G., . . . Whorton M. D. (1983). An evaluation of human sperm as indicators of chemically induced alterations of spermatogenic function. A report of the U.S. Environmental Protection Agency Gene-Tox Program. Mutation Research, 115, 73-148. [DOI] [PubMed] [Google Scholar]
- Wyrobek A. J., Watchmaker G., Gordon L., Wong K., Moore D., II, Whorton D. (1981). Sperm shape abnormalities in carbaryl-exposed employees. Environmental Health Perspectives, 40, 255-265. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Younglai E., Collins J., Foster W. (1998). Canadian semen quality: An analysis of sperm density among eleven academic fertility centers. Fertility and Sterility, 70, 76-80. [DOI] [PubMed] [Google Scholar]
- Zhang S. C., Wang H. Y., Wang J. D. (1999). Analysis of change in sperm quality of Chinese fertile men during 1981-1996. Reproduction and Contraception, 10, 33-39. [PubMed] [Google Scholar]
- Zhong C. Q., Lui Q. L., Tang Y. J., Wang Y., Shi F. J., Qian S. Z. (1990). Study on sperm function in men long after cessation of gossypol treatment. Contraception, 41, 617-622. [DOI] [PubMed] [Google Scholar]
- Zorn B., Osredkar J., Meden-Vrtovec H., Majdic G. (2007). Leptin levels in infertile male patients are correlated with inhibin B, testosterone and SHBG but not with sperm characteristics. International Journal of Andrology, 30, 439-444. [DOI] [PubMed] [Google Scholar]
- Zorn B., Virant-Klun I., Verdenik I., Meden-Vrtovec H. (1999). Semen quality changes among 2343 healthy Slovenian men included in an IVF-ET programme from 1983 to 1996. International Journal of Andrology, 22, 178-183. [DOI] [PubMed] [Google Scholar]