Abstract
Introduction
We investigated the association between olfactory identification and Alzheimer's disease biomarkers, including amyloid, tau, and neurodegeneration.
Methods
Thirty-four older adults, including 19 cognitively normal (CN), 10 subjective cognitive decline (SCD), and 5 mild cognitive impairment, underwent amyloid positron emission tomography, magnetic resonance imaging, and the University of Pennsylvania Smell Identification Test (UPSIT). Twenty-six also underwent tau positron emission tomography. Associations between the UPSIT and regionally sampled amyloid, tau, and temporal atrophy were evaluated. Voxel-wise regression models were also utilized. Analyses were conducted with the full sample and only CN/SCD.
Results
Lower UPSIT scores were associated with increased temporal and parietal tau burden in regional and voxel-wise analyses in the full sample and in CN and SCD only. Temporal lobe atrophy was associated with lower UPSIT score. Amyloid was not associated with the UPSIT.
Discussion
Impairment on the UPSIT may be a good marker for tau and neurodegeneration in preclinical or prodromal Alzheimer's disease.
Keywords: Olfaction, Alzheimer's disease, [18F]Flortaucipir (AV-1451), Tau, Neurodegeneration
1. Introduction
Alzheimer's disease (AD) is the most common age-related neurodegenerative disease and is characterized by gradually progressive impairment in cognitive function and dementia [1]. In addition to the dementia syndrome of AD and the more limited amnestic deficits typical of its prodromal stage, mild cognitive impairment (MCI) [2], changes in sensory function have also been reported. Olfactory identification (the ability to correctly identify a smell) is impaired in AD and MCI, as well as in patients with Parkinson's disease and other neurodegenerative conditions [3], [4], [5], [6], [7], [8], [9], [10]. Furthermore, olfactory identification measured using the University of Pennsylvania Smell Identification Test (UPSIT) is sensitive to predicting future conversion from MCI to AD and even future cognitive decline in cognitively normal (CN) older adults and Parkinson's patients [4], [11], [12], [13], [14].
The precise biological correlates of the observed changes in olfactory identification have not been specifically identified. However, previous studies have sought to determine the impact of the two major pathophysiological hallmarks of AD, amyloid β plaques and tau neurofibrillary tangles, on olfaction in animal models of AD [15], [16], [17], [18], [19], [20], [21], [22], autopsy studies [23], [24], [25], [26], [27], [28], [29], and more recently in living human beings using imaging biomarkers of amyloid pathology, measured using neuroimaging with positron emission tomography (PET) techniques [30], [31], [32]. Animal models of AD show considerable olfactory deficits that are related to the deposition of amyloid and tau in the olfactory bulb and throughout the olfactory network [15], [16], [17], [18], [19], [20], [21], [22], [33]. In human autopsy studies, amyloid and tau, as well as other pathologies such as progranulin and TDP-43 deposition, are found in the olfactory bulb and throughout the olfactory network (including temporal piriform cortex) in patients with AD and other neurodegenerative diseases, and levels of amyloid and tau deposition are associated with the level of olfactory deficits [23], [24], [25], [26], [27], [28], [29], [34]. The associations of UPSIT performance with neurodegeneration and brain function, measured using magnetic resonance imaging (MRI) or [15O]H2O PET, have also been investigated [4], [14], [31], [35], [36], [37], [38], [39], [40], [41]. In vivo imaging studies have shown weak associations between amyloid and olfactory impairments [30], [31], [32]. However, more significant relationships between olfactory impairment and atrophy are apparent in olfactory-related regions (amygdala, piriform cortex, entorhinal cortex, etc.) in MCI and AD patients, as well as amyloid-positive CN older adults [4], [14], [31], [32], [36], [38], [40]. Impaired olfactory identification on the UPSIT was also correlated with white matter degeneration in the splenium of the corpus callosum and superior longitudinal fasciculus, as measured with diffusion tensor imaging [38]. Schofield et al. (2012) also showed that poorer recovery on the UPSIT after cholinergic challenge with atropine was associated with a lower hippocampal volume in MCI and AD dementia patients [37]. Furthermore, in vivo activation of the primary olfactory cortex is reduced in patients with MCI and AD [35], [40], [41]. Despite the evidence for relationships between olfaction and amyloid, structural, and functional markers in AD, there are no in vivo assessments of the relationship between olfactory identification and tau deposition, likely due to the lack of an in vivo marker for tau until recently.
New PET tracers targeting tau neurofibrillary tangles have become available, including [18F]Flortaucipir ([18F]AV-1451) [42]. Our goal was to evaluate the association of UPSIT scores with tau deposition (indexed with [18F]Flortaucipir PET), amyloid deposition ([18F]Florbetapir or [18F]Florbetaben), and neurodegeneration (structural MRI). Our cohort included CN older adults without significant cognitive concerns, older adults with subjective cognitive decline (SCD), and patients with MCI. Previous literature examining in vivo imaging has suggested a strong association of UPSIT performance and neurodegeneration on MRI, but a weaker association with amyloid deposition. Thus, we hypothesized that impairments on the UPSIT would be associated with tau deposition and neurodegeneration (gray matter [GM] loss) in regions involved in olfactory processing (i.e., medial temporal lobe) but show less of an association with cortical amyloid deposition.
2. Methods
2.1. Participants
Thirty-four older adults (age 55+ years) were recruited from the Indiana Alzheimer Disease Center to undergo advanced PET and MRI neuroimaging and sensory testing. UPSIT administration was performed as previously described, with UPSIT total score being the primary outcome measure of olfactory identification (maximum score = 40; higher scores reflect better performance) [43]. Individuals with a history of a broken nose, severe allergies, or who were currently experiencing an upper respiratory infection, as well as those who were unable to undergo MRI or PET imaging were excluded. Five participants were diagnosed with MCI using previously established guidelines. Briefly, MCI participants had a significant complaint about their cognition from themselves and/or an informant or a clinician, as well as a significant deficit (>1.5 standard deviation below normal) in either memory or another cognitive domain [2]. Ten individuals were characterized as SCD according to the following criteria: elevated levels of subjective memory concerns on the 20-item Cognitive Change Index (CCI-20) reflected as a score of 20 or more on the first 12 items, with or without increased levels of informant-based concerns [44] and without a measurable cognitive deficit. Nineteen older adults without significant memory concerns (12-item CCI total <20) and without measurable cognitive deficit were considered CN. All procedures were approved by the Indiana University School of Medicine Institutional Review Board, and informed consent was obtained according to the Declaration of Helsinki and the Belmont Report.
2.2. Amyloid PET
Amyloid PET scans were acquired with either [18F]Florbetapir (Amyvid, Eli Lilly and Co.) or [18F]Florbetaben (Neuraceq, Piramal Ltd.). Briefly, for the [18F]Florbetapir scans, approximately 10 mCi of [18F]Florbetapir was injected intravenously, and after a 50-minute uptake period, participants were imaged on a Siemens mCT for 20 minutes using continuous list-mode data acquisition. For the [18F]Florbetaben scans, approximately 8 mCi of [18F]Florbetaben was injected intravenously, and after a 90-minute uptake period, data were acquired for 20 minutes using continuous list-mode acquisition on a Siemens mCT. A computed tomography (CT) scan was acquired for scatter and attenuation correction. List-mode data were subsequently rebinned into four 5-minute frames. Reconstructions were conducted on the software platform (Siemens; Knoxville, TN). Ordered subset expectation maximization was applied, using parameters from the Alzheimer's Disease Neuroimaging Initiative (ADNI) protocol (http://adni.loni.usc.edu), with corrections for scatter and random coincidence events, attenuation, and radionuclide decay. Using Statistical Parametric Mapping 8 (SPM8), the four 5-minute frames were spatially aligned to each subject's magnetization-prepared rapid gradient-echo (MP-RAGE), motion corrected, normalized to Montreal Neurologic Institute (MNI) space, averaged to create a 50- to 70-minute static image for the [18F]Florbetapir or a 90- to 110-minute static image for the [18F]Florbetaben, smoothed with an 8-mm full-width half maximum gaussian kernel, and intensity normalized to the whole cerebellum to create standardized uptake value ratio (SUVR) images. The whole cerebellum region of interest (ROI) was taken from the Centiloid project (http://www.gaain.org/centiloid-project; [45]). [18F]Florbetapir scans were then processed with the Centiloid algorithm (a form of data normalization that permits grouping data from different amyloid tracers) using the formula [(175.43*SUVR)−182.26] at a voxel-wise level as previously defined by the Centiloid project (http://www.gaain.org/centiloid-project; [45]). See Supplementary Data for further information. [18F]Florbetaben was also processed with the Centiloid algorithm using the published formula [(153.4*SUVR)−155] (Supplementary Data; [45]).
Regional [18F]Florbetapir and [18F]Florbetaben data (centiloid units) were extracted from a global cortical ROI. The global cortical ROI was generated from FreeSurfer, version 5.1 (average of parcellations from 30 CN older adult individuals from ADNI-2).
2.3. [18F]Flortaucipir PET
Of the 34 individuals, 26 underwent [18F]Flortaucipir scans. Briefly, approximately 10 mCi of [18F]Flortaucipir was injected intravenously; after a 75-minute uptake, participants were imaged for 30 minutes using continuous list-mode data acquisition on a Siemens mCT and subsequently rebinned into six 5-minute frames. Scans were again reconstructed using standard scanner software (Siemens; Knoxville, TN) and as described previously, using ordered subset expectation maximization, with correction for scatter and random coincident events, attenuation, and radionuclide decay. Using SPM8, the middle four 5-minute frames (80–100 minutes) were motion corrected, normalized to MNI space, averaged to create an 80- to 100-minute static image, smoothed with an 8-mm full-width half maximum gaussian kernel, and intensity normalized to the cerebellar crus to create SUVR images.
ROIs for target regions were generated from subject-specific parcellations from FreeSurfer v5.1, and [18F]Flortaucipir SUVR for each region was extracted from the SUVR images. Specifically, bilateral mean SUVR values were extracted from the entorhinal cortex, fusiform gyri, inferior temporal gyri, parahippocampal gyri, and mean temporal lobe. In addition, bilateral mean [18F]Flortaucipir SUVR in the piriform cortex, the largest of the olfactory cortical areas, was extracted using functional ROIs defined by the main effect of olfactory stimulation in a recent functional magnetic resonance imaging (fMRI) study at P < .05 (family-wise error correction for multiple comparisons) [46].
2.4. Structural MRI
Structural accelerated 3-tesla MP-RAGE scans were collected on a Siemens Prisma scanner using the ADNI sequence (http://adni.loni.usc.edu). Scans were processed using FreeSurfer, version 5.1, to extract bilateral total hippocampal volume, total entorhinal cortex, and temporal lobe GM volumes [47], [48], [49]. The temporal lobe measurement was the sum of the following GM volumes: mean of banks of the superior temporal sulcus, inferior, middle, and superior temporal gyri, entorhinal cortex, fusiform, parahippocampus, temporal pole, and transverse temporal pole.
2.5. Statistical analyses
Continuous demographic and neuropsychological variables, as well as the UPSIT total score, were evaluated for differences between groups using a one-way analysis of covariance, covarying for age, sex, and education when appropriate, with false discovery rate (FDR) correction for multiple comparisons. Differences between groups on categorical variables were assessed using a chi-square test. Neuroimaging target variables were preadjusted to remove the effects of age, sex, and total intracranial volume as appropriate. Briefly, a linear regression model including sex and age (for UPSIT total, amyloid centiloid data, and tau SUVR) or including sex, age, and intracranial volume (for MRI variables) were calculated using CN and SCD individuals only (“CN/SCD subsample”). The resulting β-coefficients were used to calculate residuals of the target variables for all participants (“preadjusted”). Then, associations between the preadjusted (residual) UPSIT total score and the preadjusted (residual) metrics of amyloid, tau, and neurodegeneration were assessed using Pearson correlation models. Of note, all significant associations identified using the Pearson correlation model were also significant using Spearman correlation models. Given the number of associations, FDR adjustment for multiple comparisons was computed for the regional association analyses. All P-values for the association analyses (Fig. 1, Fig. 2, Fig. 3) were adjusted using FDR. The association analyses were completed for the full sample, as well as in the CN/SCD subsample. SPSS, version 24.0, was used for all statistical analyses.
Fig. 1.
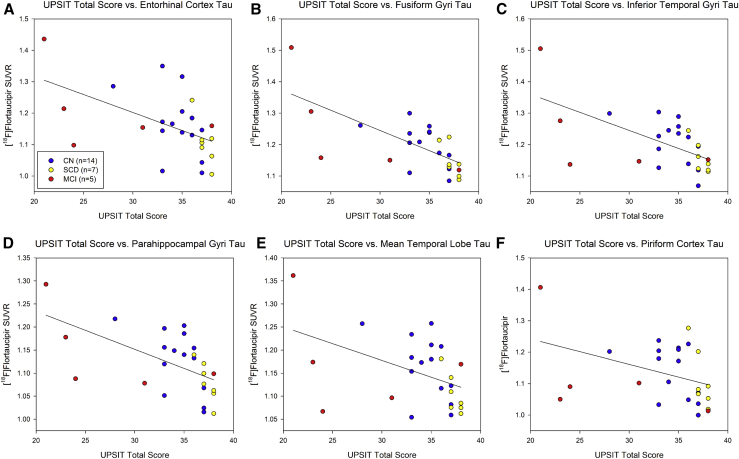
Tau in the temporal lobe is associated with UPSIT performance in the pooled sample (CN, SCD, and MCI individuals). Increased tau deposition in the (A) entorhinal cortex (r = −0.48, P < .05 FDR), (B) fusiform (r = −0.66, P < .005 FDR), (C) inferior temporal gyri (r = −0.58, P < .005 FDR), (D) parahippocampal gyri (r = −0.58, P < .005 FDR), and (E) whole temporal lobe (r = −0.45, P < .05 FDR) is associated with reduced preadjusted UPSIT total score across CN, SCD, and MCI individuals (n = 26). A trend for an association between increased tau deposition in the (F) piriform cortex and UPSIT performance (r = −0.35, P < .1 FDR) was also observed. Abbreviations: CN, cognitively normal; FDR, false discovery rate; MCI, mild cognitive impairment; SCD, subjective cognitive decline; SUVR, standardized uptake value ratio; UPSIT, University of Pennsylvania Smell Identification Test.
Fig. 2.
Tau in the temporal lobe is associated with UPSIT performance in CN individuals with and without cognitive concerns (CN/SCD subsample). Similar to the full sample, increased tau deposition in the (A) entorhinal cortex (r = −0.55, P < .05 FDR), (B) fusiform (r = −0.60, P < .01 FDR), (C) inferior temporal gyri (r = −0.63, P < .01 FDR), (D) parahippocampal gyri (r = −0.64, P < .01 FDR), and (E) whole temporal lobe (r = −0.61, P < .01 FDR) is associated with reduced preadjusted UPSIT total score in CN and SCD only (n = 21). In addition, a trend for an association between increased tau deposition in the (F) piriform cortex and UPSIT performance (r = −0.46, P < .1 FDR) was also observed. Abbreviations: CN, cognitively normal; FDR, false discovery rate; SCD, subjective cognitive decline; SUVR, standardized uptake value ratio; UPSIT, University of Pennsylvania Smell Identification Test.
Fig. 3.
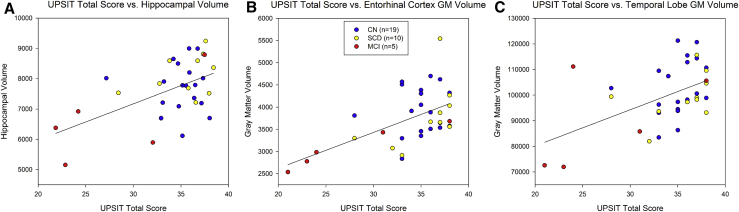
Temporal lobe atrophy is associated with UPSIT performance in the pooled sample. Atrophy in the (A) hippocampus (r = 0.53, P < .005 FDR), (B) entorhinal cortex (r = 0.45, P < .01 FDR), and (C) whole temporal lobe (r = 0.59, P < .005 FDR) is associated with reduced preadjusted UPSIT total score across CN, SCD, and MCI individuals (n = 34). No significant associations between atrophy and UPSIT performance were seen in CN and SCD only. Abbreviations: CN, cognitively normal; FDR, false discovery rate; GM, gray matter; MCI, mild cognitive impairment; SCD, subjective cognitive decline; UPSIT, University of Pennsylvania Smell Identification Test.
An exploratory analysis to investigate associations between the preadjusted UPSIT total score and tau deposition at a voxel-wise level was completed in SPM8. Specifically, the relationship between the preadjusted UPSIT total score and [18F]Flortaucipir SUVR was assessed using a linear regression model covarying for age and sex. The search area was restricted to gray matter plus white matter. The exploratory results were visualized at P < .01 (uncorrected for multiple comparisons) and minimum cluster size (k) = 100 voxels.
3. Results
3.1. Demographics
Demographics and neuropsychological performance across groups are shown in Table 1. No differences in age or education were observed; however, sex was different across the groups, with more males in the MCI group and more females in the CN/SCD subsample (P < .05). MCI participants exhibited the expected impairment in cognition, with significantly lower scores on Montreal Cognitive Assessment, Trail Making A, and story recall performance, and a significantly higher Clinical Dementia Rating scale (CDR)–sum of boxes (all P < .05). The CCI-self was significantly higher in both MCI and SCD relative to CN (P < .001), but no differences in the CCI-informant were observed. The UPSIT total score was significantly different across groups, with MCI patients showing significantly poorer performance (P < .01).
Table 1.
Demographics and neuropsychological performance
| CN (n = 19) | SCD (n = 10) | MCI (n = 5) | P-value | Post hoc (P < .05 FDR) | |
|---|---|---|---|---|---|
| Age (years) | 68.5 (6.9) | 72.2 (6.4) | 75.7 (10.6) | ns | None |
| Education (years) | 17.6 (2.0) | 17.5 (2.0) | 16.0 (4.0) | ns | None |
| Sex (male, female) | 4, 15 | 4, 6 | 4, 1 | .046 | n/a |
| Race/Ethnicity (% non-Hispanic Caucasian) | 94.7% | 100.0% | 60.0% | ns | n/a |
| APOE ε4 genotype∗ (% ε4 positive) | 47.4 | 50.0 | 50.0 | ns | n/a |
| Aβ positive (no, yes)† | 13,6 | 6,4 | 3, 2 | ns | n/a |
| CDR–sum of boxes‡ | 0.2 (0.3) | 0.1 (0.2) | 1.2 (1.6) | .003 | MCI > SCD, CN |
| MoCA total score‡ | 26.8 (2.5) | 26.1 (2.3) | 22.5 (3.8) | .024 | none |
| Trail Making A (seconds)‡ | 26.6 (8.7) | 28.0 (9.6) | 41.0 (11.7) | .015 | MCI > SCD, CN |
| Trail Making B (seconds)‡ | 64.8 (23.2) | 66.3 (28.8) | 100.4 (35.9) | ns | none |
| Craft Story Immediate Recall‡,§ | 16.4 (3.5) | 16.7 (2.1) | 12.0 (2.7) | .016 | CN, SCD > MCI |
| Craft Story Delayed Recall‡,§ | 15.8 (3.5) | 17.5 (2.7) | 10.1 (4.9) | .001 | CN, SCD > MCI |
| CCI–self (12 items)‡,‖ | 16.2 (4.1) | 24.0 (4.4) | 33.5 (12.7) | <.001 | SCD, MCI > CN |
| CCI–self (20 items)‡,‖ | 25.8 (6.4) | 36.5 (5.7) | 48.2 (12.7) | <.001 | SCD, MCI > CN |
| CCI–informant (12 items)‡,¶ | 17.4 (6.6) | 15.2 (3.8) | 26.1 (2.8) | ns | none |
| CCI–informant (20 items)‡,¶ | 28.4 (11.2) | 23.7 (4.9) | 40.4 (4.2) | ns | none |
| UPSIT total score∗∗ | 34.5 (2.3) | 35.7 (3.3) | 28.7 (7.0) | .006 | CN, SCD > MCI |
Abbreviations: Aβ, amyloid β; APOE, apolipoprotein E; CCI, Cognitive Change Index; CDR, Clinical Dementia Rating scale; CN, cognitively normal; MCI, mild cognitive impairment; MoCA, Montreal Cognitive Assessment; SCD, subjective cognitive decline; UPSIT, University of Pennsylvania Smell Identification Test.
Missing one MCI participant.
Amyloid positivity: no = Centiloid < 2.51; yes = Centiloid > 2.51; cut-off determined using ADNI-GO/2 amyloid scans.
Covaried for age, sex, and education.
Missing two participants (one CN, one SCD); paraphrase scoring.
Missing five participants (two CN, three MCI).
Missing four participants (one CN, three MCI).
Covaried for age and sex.
3.2. Regional analyses
The preadjusted UPSIT total score was not associated with amyloid deposition in either the full sample or the CN/SCD subsample.
Significant associations between the preadjusted UPSIT total score and tau deposition in temporal lobe regions were observed in the full sample (Fig. 1; n = 26). Specifically, tau in the entorhinal cortex (Fig. 1A; r = −0.48, P < .05 FDR), fusiform gyri (Fig. 1B; r = −0.66, P < .005 FDR), inferior temporal gyri (Fig. 1C; r = −0.58, P < .005 FDR), parahippocampal gyri (Fig. 1D; r = −0.58, P < .005 FDR), and mean temporal lobe (Fig. 1E; r = −0.45, P < .05 FDR) was negatively associated with the preadjusted UPSIT total score. A trend for an association between the preadjusted UPSIT total score and higher tau in the piriform cortex was observed (Fig. 1F; r = −0.35, P < .1 FDR).
After restricting the analyses to cognitively intact subjects only (CN/SCD subsample; n = 21), associations across the temporal lobe remained significant (Fig. 2). As in the full sample, higher tau in the entorhinal cortex (Fig. 2A; r = −0.55, P < .05 FDR), fusiform gyri (Fig. 2B; r = −0.60, P < .01 FDR), inferior temporal gyri (Fig. 2C; r = −0.63, P < .01 FDR), parahippocampal gyri (Fig. 2D; r = −0.64, P < .01 FDR), and mean temporal lobe (Fig. 2E; r = −0.61, P < .01 FDR) was associated with a lower preadjusted UPSIT total score. In addition, higher piriform cortex tau was associated with a lower pre-adjusted UPSIT score at a trend level in this sample of CN individuals with or without complaints (Fig. 2F; r = −0.46, P < .1 FDR).
When the associations between UPSIT performance and atrophy were evaluated, significant associations were only observed in the full sample (n = 34). Specifically, lower hippocampal volume (Fig. 3A; r = 0.53, P < .005 FDR), entorhinal cortex GM volume (Fig. 3B; r = 0.45, P < .01 FDR), and temporal lobe GM volume (Fig. 3C; r = 0.59, P < .005 FDR) were associated with a lower preadjusted UPSIT total score. No significant associations were observed between any atrophy measure and the preadjusted UPSIT total score within the CN/SCD subsample.
3.3. Voxel-wise analysis
The exploratory voxel-wise analysis showed significant associations between higher tau deposition throughout the bilateral temporal and parietal lobes and poorer UPSIT performance, with stronger association in the left hemisphere. Specifically, significant negative correlations were found between the preadjusted UPSIT score and tau deposition in the left inferior occipital gyrus, left middle temporal gyrus, left precuneus, left parahippocampal gyrus, left uncus, left inferior parietal lobule, left paracentral lobule, and left medial frontal gyrus, as well as the bilateral fusiform gyri, bilateral lingual gyri, bilateral middle frontal gyrus, bilateral posterior cingulate, and bilateral cerebellum (Fig. 4A).
Fig. 4.
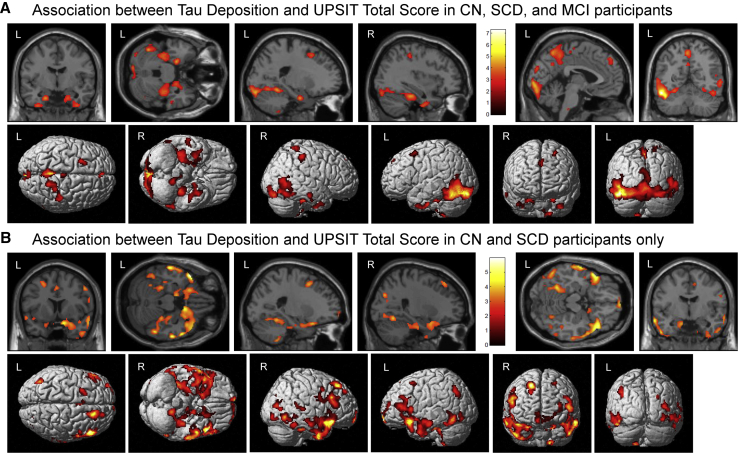
Exploratory voxel-wise associations show widespread regions where increased tau deposition is associated with reduced UPSIT performance. (A) Across all individuals (CN, SCD, MCI; n = 26), reduced preadjusted UPSIT total score was associated with increased tau in widespread medial and lateral temporal lobe regions, as well as regions of the inferior parietal and occipital lobes. (B) In CN and SCD individuals only (n = 21), reduced preadjusted UPSIT total score was associated with increased tau in the medial and lateral temporal lobes, as well as throughout the inferior, middle, and superior frontal lobes. No associations were seen in the opposite direction (i.e., increased tau associated with better UPSIT score). Voxel-wise association are shown at a voxel-wise threshold of P < .01 (uncorrected for multiple comparisons) and minimum cluster size (k) = 100 voxels. Abbreviations: CN, cognitively normal; MCI, mild cognitive impairment; SCD, subjective cognitive decline; UPSIT, University of Pennsylvania Smell Identification Test.
In the CN/SCD subsample, the exploratory voxel-wise analysis also showed widespread regions of association between tau deposition and UPSIT performance, although the areas appeared to be more anterior than the results from the full sample. Specifically, significant negative relationships existed between the preadjusted UPSIT total score and tau deposition in the bilateral inferior, middle, superior, and medial frontal gyri, bilateral precentral gyri, bilateral inferior, middle, and superior temporal gyri, bilateral uncus, bilateral anterior cingulate, bilateral thalamus, and bilateral inferior occipital, as well as the left fusiform gyrus, right cuneus, and right middle occipital gyri (Fig. 4B). No significant associations were seen in the opposite direction (i.e., higher tau associated with higher UPSIT score) for either the full sample or in the CN/SCD subsample.
4. Discussion
This study explored the relationships between olfactory identification ability and the cerebral measures of amyloid and tau deposition and GM loss. We found that tau deposition and atrophy in the temporal lobe, but not amyloid deposition, were associated with lower olfactory identification (UPSIT total score) across a population of CN individuals and older adults with SCD or MCI. We observed a similar phenomenon in the subset of individuals without measured cognitive impairment (CN/SCD subsample), with negative correlations between tau in the temporal lobe and lower UPSIT performance. There were no associations between UPSIT total score and amyloid or neurodegeneration in this subpopulation. Finally, exploratory voxel-wise analyses in both the full sample and in the CN/SCD subsample confirmed the regional findings and also suggested that parietal, occipital, and frontal lobe have correlations between higher tau and lower olfactory identification.
Although prior studies have shown that olfactory processing is related to more general evidence of cerebral integrity (e.g., GM loss), these observed relationships between tau and olfactory identification provide new evidence that poor performance on an olfactory identification test may be linked to specific ongoing pathophysiology in AD. In MCI, tau and neurodegeneration are often found in areas that are involved in olfactory processing, which may result in the observable olfactory loss, as suggested by the strong negative correlation between UPSIT performance and both tau and neurodegeneration when MCI patients were included in the analysis. However, when MCI patients were excluded, only an association with tau, but not neurodegeneration (GM loss), was seen. This suggests that early changes in UPSIT performance in at-risk CN individuals may be indicative of active tau deposition in the brain before significant atrophy. These findings support the use of the UPSIT as a biomarker of early presymptomatic disease.
Our results support previous imaging studies that found a strong significant relationship between olfactory impairment and neurodegeneration and a relatively weaker correlation with amyloid. For example, Bahar-Fuchs et al. reported a significant negative association of the UPSIT with amyloid deposition, but only across (not within) diagnostic groups, and concluded that the UPSIT impairment was due diagnostic differences rather than directly to amyloid deposition [30]. Consistent with this interpretation, we propose that tau deposition in medial temporal and other primary olfactory-related regions may be the main cause of the olfactory deficits seen in MCI, as well as in at-risk individuals such as those with SCD. Tau deposition may lead to neurodegeneration in these regions over time, in turn resulting in the observed association between olfactory deficits and atrophy in the MCI stages. Given that we observed an association between tau, but not atrophy, and UPSIT performance in the CN individuals with and without complaints, we suggest that tau is the primary driver of the early olfactory identification deficits.
Numerous studies have found amyloid and tau deposition in the olfactory bulbs of humans at autopsy and in AD animal models [15], [16], [20], [22], [23], [24], [27], [28]. PET does not offer sufficient resolution for measurement of amyloid and/or tau deposition in the olfactory bulb in humans. However, future PET studies of amyloid and tau in conjunction with olfactory mucosa sampling [50] may help to determine whether the primary olfactory system has amyloid and tau deposition that mirrors that seen in the brain.
This study has a few important limitations. The sample size is relatively small, particularly for the MCI population, necessitating larger future studies for replication and extension of the findings. In this study, we only included amyloid and tau PET imaging and structural MRI. Future studies incorporating resting-state fMRI or even task-based fMRI of olfactory response could help to further describe the early changes in olfaction in those at risk for AD. Finally, the small number of amyloid-positive individuals in our study may have limited our ability to detect amyloid-related association with olfactory performance (Table 1). However, when we limited the sample to only those who were amyloid positive or borderline amyloid positive, a very strong association between the UPSIT total score and tau deposition was observed (data not shown); in amyloid-negative participants, no association between the UPSIT total score and tau was observed (data not shown) in the full sample. These findings suggest that tau deposition in the presence of amyloid may be driving the observed associations. However, effects of other neurodegenerative conditions resulting in tau accumulation and/or neurodegeneration may result in impairment on the UPSIT, as has been previously observed in Parkinson's disease and other degenerative conditions. Future studies with larger samples of amyloid-negative and amyloid-positive individuals, along with tau PET imaging, will help to further clarify this issue.
In summary, we observed significant associations between tau deposition in medial and lateral temporal regions and performance deficits on a measure of olfactory identification. These associations were observed across CN, SCD, and MCI individuals, as well as within CN and SCD only. Associations between olfactory identification and temporal lobe atrophy were observed in the full sample only (CN + SCD + MCI); there were no associations observed with amyloid deposition in either the full sample or the CN/SCD subsample. These results suggest that measures of olfactory identification may be sensitive biomarkers of concurrent tau deposition. In turn, these behavioral tests, which are inexpensive and are easy and quick to administer in primary care settings, could be useful for identifying individuals at risk for the development of AD.
Research in Context.
-
1.
Systematic review: In order to investigate associations between olfactory identification and amyloid, tau, and neurodegeneration, we searched PubMed for various combinations of “olfaction,” “imaging,” “tau,” “amyloid,” and “MRI.” We then combined the returned articles to generate a summary of associations of olfaction with amyloid, tau, and Alzheimer's disease (AD) in animal models, autopsy studies, and in vivo imaging studies.
-
2.
Interpretation: Our results provide new evidence that impairment in olfactory identification in early at-risk and prodromal AD participants is related to tau deposition and neurodegeneration. These findings suggest that olfactory identification measured using the University of Pennsylvania Smell Identification Test (UPSIT) is a good biomarker for tau accumulation in individuals at risk for AD.
-
3.
Future directions: To confirm the current findings, additional analyses with larger samples would be beneficial. In addition, longitudinal follow-up studies with repeated UPSIT administration would help to determine whether the UPSIT can predict and monitor decline.
Acknowledgments
The authors thank Bradley Glazier, Kala Hall, Lili Kyurkchiyska, Madeline Cassidy, Elsa Carodenuto, Evan Finley, Yolanda Graham-Dotson, Ryan Crosbie, Steve Brown, Trina Bird, Heather Polson, Wendy Territo, Michelle Beal, Mario Dzemidzic, and William Eiler for their contributions to this work. This work was supported by the National Institute on Aging (NIA R01 AG19771, P30 AG10133, and K01 AG049050), the Alzheimer's Association, the Indiana University Health-Indiana University School of Medicine Strategic Research Initiative, and the Indiana Clinical and Translational Sciences Institute (CTSI).
Part of this research was supported in part by Lilly Endowment, Inc., through its support for the Indiana University Pervasive Technology Institute and in part by the Indiana METACyt Initiative. The Indiana METACyt Initiative at IU was also supported in part by Lilly Endowment, Inc. This material is based on work supported by the National Science Foundation under grant number CNS-0521433.
Footnotes
Supplementary data related to this article can be found at https://doi.org/10.1016/j.dadm.2017.09.001.
Supplementary data
References
- 1.McKhann G.M., Knopman D.S., Chertkow H., Hyman B.T., Jack C.R., Jr., Kawas C.H. The diagnosis of dementia due to Alzheimer's disease: recommendations from the National Institute on Aging-Alzheimer's Association workgroups on diagnostic guidelines for Alzheimer's disease. Alzheimers Dement. 2011;7:263–269. doi: 10.1016/j.jalz.2011.03.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Albert M.S., DeKosky S.T., Dickson D., Dubois B., Feldman H.H., Fox N.C. The diagnosis of mild cognitive impairment due to Alzheimer's disease: recommendations from the National Institute on Aging-Alzheimer's Association workgroups on diagnostic guidelines for Alzheimer's disease. Alzheimers Dement. 2011;7:270–279. doi: 10.1016/j.jalz.2011.03.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Alves J., Petrosyan A., Magalhaes R. Olfactory dysfunction in dementia. World J Clin Cases. 2014;2:661–667. doi: 10.12998/wjcc.v2.i11.661. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Devanand D.P., Tabert M.H., Cuasay K., Manly J.J., Schupf N., Brickman A.M. Olfactory identification deficits and MCI in a multi-ethnic elderly community sample. Neurobiol Aging. 2010;31:1593–1600. doi: 10.1016/j.neurobiolaging.2008.09.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Djordjevic J., Jones-Gotman M., De Sousa K., Chertkow H. Olfaction in patients with mild cognitive impairment and Alzheimer's disease. Neurobiol Aging. 2008;29:693–706. doi: 10.1016/j.neurobiolaging.2006.11.014. [DOI] [PubMed] [Google Scholar]
- 6.Doty R.L. Olfaction in Parkinson's disease and related disorders. Neurobiol Dis. 2012;46:527–552. doi: 10.1016/j.nbd.2011.10.026. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Mesholam R.I., Moberg P.J., Mahr R.N., Doty R.L. Olfaction in neurodegenerative disease: a meta-analysis of olfactory functioning in Alzheimer's and Parkinson's diseases. Arch Neurol. 1998;55:84–90. doi: 10.1001/archneur.55.1.84. [DOI] [PubMed] [Google Scholar]
- 8.Quarmley M., Moberg P.J., Mechanic-Hamilton D., Kabadi S., Arnold S.E., Wolk D.A. Odor Identification Screening Improves Diagnostic Classification in Incipient Alzheimer's Disease. J Alzheimers Dis. 2017;55:1497–1507. doi: 10.3233/JAD-160842. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Silveira-Moriyama L., Hughes G., Church A., Ayling H., Williams D.R., Petrie A. Hyposmia in progressive supranuclear palsy. Movement Disord. 2010;25:570–577. doi: 10.1002/mds.22688. [DOI] [PubMed] [Google Scholar]
- 10.Velayudhan L. Smell identification function and Alzheimer's disease: a selective review. Curr Opin Psychiatry. 2015;28:173–179. doi: 10.1097/YCO.0000000000000146. [DOI] [PubMed] [Google Scholar]
- 11.Devanand D.P., Lee S., Manly J., Andrews H., Schupf N., Doty R.L. Olfactory deficits predict cognitive decline and Alzheimer dementia in an urban community. Neurology. 2015;84:182–189. doi: 10.1212/WNL.0000000000001132. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Devanand D.P., Liu X., Tabert M.H., Pradhaban G., Cuasay K., Bell K. Combining early markers strongly predicts conversion from mild cognitive impairment to Alzheimer's disease. Biol Psychiatry. 2008;64:871–879. doi: 10.1016/j.biopsych.2008.06.020. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Fullard M.E., Tran B., Xie S.X., Toledo J.B., Scordia C., Linder C. Olfactory impairment predicts cognitive decline in early Parkinson's disease. Parkinsonism Relat Disord. 2016;25:45–51. doi: 10.1016/j.parkreldis.2016.02.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Kjelvik G., Saltvedt I., White L.R., Stenumgard P., Sletvold O., Engedal K. The brain structural and cognitive basis of odor identification deficits in mild cognitive impairment and Alzheimer's disease. BMC Neurol. 2014;14:168. doi: 10.1186/s12883-014-0168-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Cheng N., Bai L., Steuer E., Belluscio L. Olfactory functions scale with circuit restoration in a rapidly reversible Alzheimer's disease model. J Neurosci. 2013;33:12208–12217. doi: 10.1523/JNEUROSCI.0291-13.2013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Hu Y., Ding W., Zhu X., Chen R., Wang X. Olfactory Dysfunctions and Decreased Nitric Oxide Production in the Brain of Human P301L Tau Transgenic Mice. Neurochem Res. 2016;41:722–730. doi: 10.1007/s11064-015-1741-8. [DOI] [PubMed] [Google Scholar]
- 17.Macknin J.B., Higuchi M., Lee V.M., Trojanowski J.Q., Doty R.L. Olfactory dysfunction occurs in transgenic mice overexpressing human tau protein. Brain Res. 2004;1000:174–178. doi: 10.1016/j.brainres.2004.01.047. [DOI] [PubMed] [Google Scholar]
- 18.Morales-Corraliza J., Schmidt S.D., Mazzella M.J., Berger J.D., Wilson D.A., Wesson D.W. Immunization targeting a minor plaque constituent clears beta-amyloid and rescues behavioral deficits in an Alzheimer's disease mouse model. Neurobiol Aging. 2013;34:137–145. doi: 10.1016/j.neurobiolaging.2012.04.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Saiz-Sanchez D., De La Rosa-Prieto C., Ubeda-Banon I., Martinez-Marcos A. Interneurons and beta-amyloid in the olfactory bulb, anterior olfactory nucleus and olfactory tubercle in APPxPS1 transgenic mice model of Alzheimer's disease. Anatomical Rec. 2013;296:1413–1423. doi: 10.1002/ar.22750. [DOI] [PubMed] [Google Scholar]
- 20.Wesson D.W., Levy E., Nixon R.A., Wilson D.A. Olfactory dysfunction correlates with amyloid-beta burden in an Alzheimer's disease mouse model. J Neurosci. 2010;30:505–514. doi: 10.1523/JNEUROSCI.4622-09.2010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Wesson D.W., Morales-Corraliza J., Mazzella M.J., Wilson D.A., Mathews P.M. Chronic anti-murine Aβ immunization preserves odor guided behaviors in an Alzheimer's beta-amyloidosis model. Behav Brain Res. 2013;237:96–102. doi: 10.1016/j.bbr.2012.09.019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Wu N., Rao X., Gao Y., Wang J., Xu F. Amyloid-beta deposition and olfactory dysfunction in an Alzheimer's disease model. J Alzheimers Dis. 2013;37:699–712. doi: 10.3233/JAD-122443. [DOI] [PubMed] [Google Scholar]
- 23.Attems J., Jellinger K.A. Olfactory tau pathology in Alzheimer disease and mild cognitive impairment. Clin Neuropathol. 2006;25:265–271. [PubMed] [Google Scholar]
- 24.Christen-Zaech S., Kraftsik R., Pillevuit O., Kiraly M., Martins R., Khalili K. Early olfactory involvement in Alzheimer's disease. Can J Neurol Sci. 2003;30:20–25. doi: 10.1017/s0317167100002389. [DOI] [PubMed] [Google Scholar]
- 25.Doorn K.J., Goudriaan A., Blits-Huizinga C., Bol J.G., Rozemuller A.J., Hoogland P.V. Increased amoeboid microglial density in the olfactory bulb of Parkinson's and Alzheimer's patients. Brain Pathol. 2014;24:152–165. doi: 10.1111/bpa.12088. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Kortvelyessy P., Gukasjan A., Sweeney-Reed C.M., Heinze H.J., Thurner L., Bittner D.M. Progranulin and Amyloid-beta Levels: Relationship to Neuropsychology in Frontotemporal and Alzheimer's Disease. J Alzheimers Dis. 2015;46:375–380. doi: 10.3233/JAD-150069. [DOI] [PubMed] [Google Scholar]
- 27.Kovacs T., Cairns N.J., Lantos P.L. Beta-amyloid deposition and neurofibrillary tangle formation in the olfactory bulb in ageing and Alzheimer's disease. Neuropathol Appl Neurobiol. 1999;25:481–491. doi: 10.1046/j.1365-2990.1999.00208.x. [DOI] [PubMed] [Google Scholar]
- 28.Oliveira F.H., Rodrigues Neto E., Fonseca M.K., Costa A.S., Rockenbach M.A., Padilha Rdos S. Neurodegenerative changes in the brainstem and olfactory bulb in people older than 50 years old: a descriptive study. Arq Neuropsiquiatr. 2015;73:569–577. doi: 10.1590/0004-282X20150066. [DOI] [PubMed] [Google Scholar]
- 29.Wilson R.S., Arnold S.E., Schneider J.A., Tang Y., Bennett D.A. The relationship between cerebral Alzheimer's disease pathology and odour identification in old age. J Neurol Neurosurg Psychiatry. 2007;78:30–35. doi: 10.1136/jnnp.2006.099721. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Bahar-Fuchs A., Chetelat G., Villemagne V.L., Moss S., Pike K., Masters C.L. Olfactory deficits and amyloid-beta burden in Alzheimer's disease, mild cognitive impairment, and healthy aging: a PiB PET study. J Alzheimers Dis. 2010;22:1081–1087. doi: 10.3233/JAD-2010-100696. [DOI] [PubMed] [Google Scholar]
- 31.Growdon M.E., Schultz A.P., Dagley A.S., Amariglio R.E., Hedden T., Rentz D.M. Odor identification and Alzheimer disease biomarkers in clinically normal elderly. Neurology. 2015;84:2153–2160. doi: 10.1212/WNL.0000000000001614. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Vassilaki M., Christianson T.J., Mielke M.M., Geda Y.E., Kremers W.K., Machulda M.M. Neuroimaging Biomarkers and Impaired Olfaction in Cognitively Normal Individuals. Ann Neurol. 2017;81:871–882. doi: 10.1002/ana.24960. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Rey N.L., Jardanhazi-Kurutz D., Terwel D., Kummer M.P., Jourdan F., Didier A. Locus coeruleus degeneration exacerbates olfactory deficits in APP/PS1 transgenic mice. Neurobiol Aging. 2012;33:e1–e11. doi: 10.1016/j.neurobiolaging.2010.10.009. [DOI] [PubMed] [Google Scholar]
- 34.Takeda T., Iijima M., Uchihara T., Ohashi T., Seilhean D., Duyckaerts C. TDP-43 Pathology Progression Along the Olfactory Pathway as a Possible Substrate for Olfactory Impairment in Amyotrophic Lateral Sclerosis. J Neuropathol Exp Neurol. 2015;74:547–556. doi: 10.1097/NEN.0000000000000198. [DOI] [PubMed] [Google Scholar]
- 35.Kareken D.A., Doty R.L., Moberg P.J., Mosnik D., Chen S.H., Farlow M.R. Olfactory-evoked regional cerebral blood flow in Alzheimer's disease. Neuropsychology. 2001;15:18–29. doi: 10.1037//0894-4105.15.1.18. [DOI] [PubMed] [Google Scholar]
- 36.Murphy C., Jernigan T.L., Fennema-Notestine C. Left hippocampal volume loss in Alzheimer's disease is reflected in performance on odor identification: a structural MRI study. J Int Neuropsychol Soc. 2003;9:459–471. doi: 10.1017/S1355617703930116. [DOI] [PubMed] [Google Scholar]
- 37.Schofield P.W., Ebrahimi H., Jones A.L., Bateman G.A., Murray S.R. An olfactory 'stress test' may detect preclinical Alzheimer's disease. BMC Neurol. 2012;12:24. doi: 10.1186/1471-2377-12-24. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Segura B., Baggio H.C., Solana E., Palacios E.M., Vendrell P., Bargallo N. Neuroanatomical correlates of olfactory loss in normal aged subjects. Behav Brain Res. 2013;246:148–153. doi: 10.1016/j.bbr.2013.02.025. [DOI] [PubMed] [Google Scholar]
- 39.Servello A., Fioretti A., Gualdi G., Di Biasi C., Pittalis A., Sollaku S. Olfactory Dysfunction, Olfactory Bulb Volume and Alzheimer's Disease: Is There a Correlation? A Pilot Study1. J Alzheimers Dis. 2015;48:395–402. doi: 10.3233/JAD-150232. [DOI] [PubMed] [Google Scholar]
- 40.Vasavada M.M., Wang J., Eslinger P.J., Gill D.J., Sun X., Karunanayaka P. Olfactory cortex degeneration in Alzheimer's disease and mild cognitive impairment. J Alzheimers Dis. 2015;45:947–958. doi: 10.3233/JAD-141947. [DOI] [PubMed] [Google Scholar]
- 41.Wang J., Eslinger P.J., Doty R.L., Zimmerman E.K., Grunfeld R., Sun X. Olfactory deficit detected by fMRI in early Alzheimer's disease. Brain Res. 2010;1357:184–194. doi: 10.1016/j.brainres.2010.08.018. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Chien D.T., Bahri S., Szardenings A.K., Walsh J.C., Mu F., Su M.Y. Early clinical PET imaging results with the novel PHF-tau radioligand [F-18]-T807. J Alzheimers Dis. 2013;34:457–468. doi: 10.3233/JAD-122059. [DOI] [PubMed] [Google Scholar]
- 43.Doty R.L., Shaman P., Dann M. Development of the University of Pennsylvania Smell Identification Test: a standardized microencapsulated test of olfactory function. Physiol Behav. 1984;32:489–502. doi: 10.1016/0031-9384(84)90269-5. [DOI] [PubMed] [Google Scholar]
- 44.Jessen F., Amariglio R.E., van Boxtel M., Breteler M., Ceccaldi M., Chetelat G. A conceptual framework for research on subjective cognitive decline in preclinical Alzheimer's disease. Alzheimers Dement. 2014;10:844–852. doi: 10.1016/j.jalz.2014.01.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Klunk W.E., Koeppe R.A., Price J.C., Benzinger T.L., Devous M.D., Sr., Jagust W.J. The Centiloid Project: standardizing quantitative amyloid plaque estimation by PET. Alzheimers Dement. 2015;11:e1–e4. doi: 10.1016/j.jalz.2014.07.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Eiler W.J., 2nd, Dzemidzic M., Case K.R., Armstrong C.L., Mattes R.D., Cyders M.A. Ventral frontal satiation-mediated responses to food aromas in obese and normal-weight women. Am J Clin Nutr. 2014;99:1309–1318. doi: 10.3945/ajcn.113.080788. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Risacher S.L., Kim S., Nho K., Foroud T., Shen L., Petersen R.C. APOE effect on Alzheimer's disease biomarkers in older adults with significant memory concern. Alzheimers Dement. 2015;11:1417–1429. doi: 10.1016/j.jalz.2015.03.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Dale A., Fischl B., Sereno M. Cortical surface-based analysis. I: Segmentation and surface reconstruction. Neuroimage. 1999;9:179–194. doi: 10.1006/nimg.1998.0395. [DOI] [PubMed] [Google Scholar]
- 49.Fischl B., Sereno M., Dale A. Cortical surface-based analysis. II: Inflation, flattening, and a surface-based coordinate system. Neuroimage. 1999;9:195–207. doi: 10.1006/nimg.1998.0396. [DOI] [PubMed] [Google Scholar]
- 50.Ayala-Grosso C.A., Pieruzzini R., Diaz-Solano D., Wittig O., Abrante L., Vargas L. Amyloid-beta Peptide in olfactory mucosa and mesenchymal stromal cells of mild cognitive impairment and Alzheimer's disease patients. Brain Pathol. 2015;25:136–145. doi: 10.1111/bpa.12169. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.