Abstract
The gold standard for diagnosing syncope is to elucidate the symptom-electrocardiogram (ECG) correlation. The ECG recordings during syncope allow physicians to either confirm or exclude an arrhythmia as the mechanism of syncope. Many studies have investigated the use of internal loop recorder (ILR), while few studies have used external loop recorder (ELR) for patients with unexplained syncope. The aim of this review is to clarify the clinical usefulness of ILR and ELR in the diagnosis and management of patients with unexplained syncope. Many observational and four randomized control studies have shown that ILR for patients with unknown syncope is a useful tool for early diagnosis and improving diagnosis rate. ILR also provides important information on the mechanism of syncope and treatment strategy. However, there is no evidence of total mortality or quality of life improvements with ILR. The diagnostic yield of ELR in patients with syncope was similar to that with ILR within the same timeframe. Therefore, ELR could be considered for long-term ECG monitoring before a patient switches to using ILR. A systematic approach and selection of ECG monitoring tools reduces health care costs and improves the selection of patients for optimal treatment possibilities.
Keywords: Internal loop recorder, External loop recorder, Unknown Syncope
1. Introduction
The gold standard for diagnosing syncope is to elucidate the symptom-electrocardiograph (ECG) correlation. ECG monitoring is an established procedure in the evaluation and monitoring of patients with syncope. The ECG recordings during syncope allow physicians to confirm or exclude an arrhythmia as the mechanism of syncope. Many studies have investigated the use of internal loop recorder (ILR), while there are few studies of external loop recorder (ELR) for patients with unexplained syncope. However, there is still some uncertainty in their clinical utility and practical approach. The aim of this review is to clarify the clinical usefulness of ILR and ELR in the diagnosis and management of patients with unexplained syncope.
2. Internal loop recorders
ILRs were developed in the early 1990s. They have a battery life of approximately 3 years and are able to record an ECG signal from small leads on either end of the device. Cardiac events can be detected manually or automatically and are saved on the device for up to 40 minutes. Since September 2016, ILR has been downsized. It is expected that the chances of using ILR will increase. Although ILR is used for patients with unexplained syncope, ILR research examines the following viewpoints: 1. Early diagnosis of unexplained syncope, 2. Mortality in patients with ILR, 3. Quality of life in patients with ILR, 4. Cost effectiveness, 5. Adverse effects of ILR, 6. When should we use ILR?
2.1. Early diagnosis of unexplained syncope
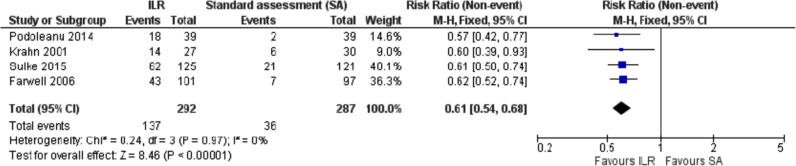
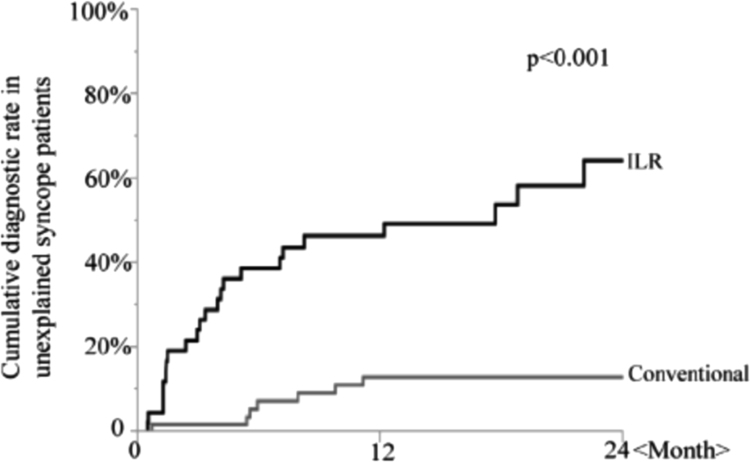
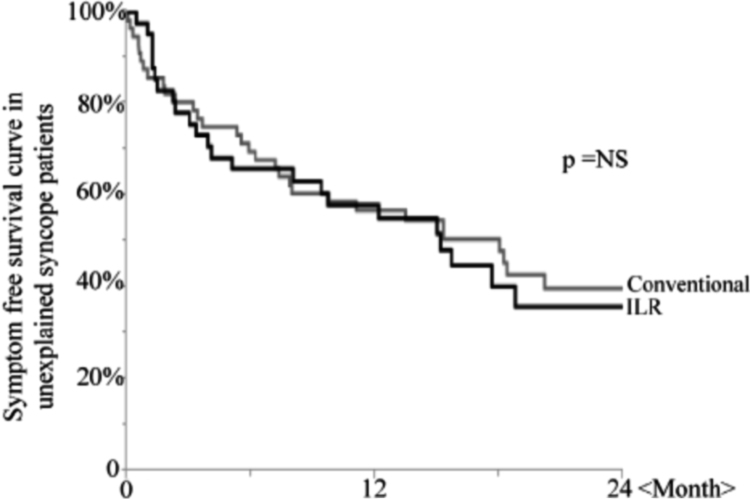
Many observational and four randomized control studies have investigated the use of the ILR [1]. The diagnostic yield of the ILR is higher than conventional testing, mainly due to prolonged monitoring periods [2], [3], [4]. ILR achieved a more rapid diagnosis in unexplained syncope than conventional techniques [5]. The Randomized Assessment of Syncope Trial (RAST) study randomized 60 patients to either conventional investigation with an ELR for 2–4 weeks, an electrophysiological testing, and a tilt-table test, or a prolonged monitoring for 1 year with an ILR. This study suggested that early implantation with ILR was more effective (52% diagnosed versus 20%) compared to the conventional strategy [2]. An ILR-guided diagnosis was demonstrated in 78% of 570 patients with pre-syncope or syncope during an average follow-up of 10 months in the multinational Place of Reveal in the Care Pathway and Treatment of Patients with Unexplained Recurrent Syncope Registry (PICTURE registry) [6]. In a meta-analysis, Solbiati reported on the diagnosis of ILR using four randomized control trials (Fig. 1). There was a significant difference in the number of diagnoses between patients who received ILR and those who were managed conventionally at a long-term follow-up [7]. In selected patients, the symptom-ECG correlation was as high as 88%, and the diagnostic value increased with increasing observation time [8], [9]. Studies on ILR have also provided the important details of the mechanism and treatment strategy of syncope [10], [11], [12], [13], [14]. There are fewer papers regarding ILR for patients with unexplained syncope in Japan [15], [16], [17]. Onuki demonstrated that the estimated diagnostic rates of ILR for unexplained syncope were 47% and 65% at 1 and 2 years, respectively, in a single center retrospective observational study (Fig. 2). They also presented that the symptom-free rate of patients with ILR and patients with conventional investigation was approximately the same (Fig. 3). This means that the ILR does not have any effect on occurrence of the unexplained syncope [16]. Additionally, the ILR provides information about the characteristics of the heart rhythm during syncope in patients with neutrally mediated reflex syncope, and it may help guide decisions regarding specific therapy [18], [19], [20].
Fig. 1.
Forest plot of comparison of ILR vs Standard Assessment. (Quoted from Solbiat M et al. [7]).
Fig. 2.
Cumulative diagnostic rates between the use of an ILR and conventional tests. (Quoted from Onuki et al. [16]).
Fig. 3.
Symptom-free survival curve for the use of an ILR and conventional tests. (Quoted from Onuki et al. [16]).
2.2. Mortality and ILR
There is no research on ILR that evaluates life prognosis improvement as a primary endpoint. Only two studies reported data on mortality at one year and 18 months [2], [3]. There was no evidence of a difference in the risk of mortality between patients with ILR and those who were managed conventionally at follow-up.
2.3. Quality of Life and ILR
Two studies analyzed quality of life in patients with ILR. Farwell measured quality of life using the Medical Outcomes Questionnaire (SF-12) and a visual analogue scale (VAS) at induction, 6, 12, and 18 months. They reported that there was a trend towards improved quality of life in the ILR group compared to the control group. Additionally, there were significant increases observed in VAS at 18 months, and no changes were noted in SF-12 scores. They discussed that the earlier use of appropriate therapeutic interventions using ILR significantly decreasing subsequent syncope, which may reflect improved quality of life [3]. Podopleanu performed an analysis of quality of life using the 36-Item Short Form Health Survey (SF-36) questionnaire at baseline, 6 months, and after 14 months of follow-up. There was no difference between the ILR group and the control group in terms of quality of life main composite score, suggesting general physical and psychological well-being [4].
2.4. Cost effectiveness
Two studies analyzed the cost-effectiveness of using ILR or conventional management as diagnostic tools. The RAST study suggested that early intervention with ILR was more cost-effective than the conventional strategy, which includes ELR for 2–4 weeks, electrophysiological testing, and tilt-table testing [2]. Krahn calculated the cost of investigation based on the Ontario Health Insurance Program fee schedule for technical and professional fees, and also included an estimate of materials, labor, maintenance, and overhead costs for hospital-based investigations. The mean cost of ILR as the primary monitoring strategy was greater than that of the conventional strategy, but the cost of ILR monitoring per diagnosis was less than that of the conventional strategy. Farwell reported that overall mean costs were lower in the ILR group than in the conventional management group without statistical significance [3]. Length of follow-up might influence costs, as ILR may be more costly initially, but it might be balanced by a lower need for tests and hospitalization in the long term.
2.5. Adverse effects and disadvantages of the ILR
ILRs carry the risk of pocket infections that resolve with device explanation. This complication, which can occur either in the peri-procedural phase or later during the follow-up, was reported in 1 to 5% of patients. Another disadvantage of ILR includes the presence of under-sensing or over-sensing. This is due to the difficulty of distinguishing between SVT and VT, and the ambiguous P wave [13], [21].
2.6. When should we use ILR?
Current European Society of Cardiology Guidelines recommend ILR-implantation at an early stage in patients with unexplained syncope without high-risk criteria based on efficacy, safety, and cost-utility [1], [22]. After initial evaluation (detailed history, physical examination, and orthostatic challenging ECG) for patients with unknown syncope, an arrhythmic cause is suspected, but the likelihood for recurrence is low. Therefore, early use of ILR is recommended [23]. The initial evaluations can provide the diagnosis in up to 50% of the cases [24], [25]. When the diagnosis is made, no further testing is needed and appropriate therapy can be initiated. For the remaining cases, the risk assessment and suspected etiology of the syncope determines the further diagnostic approach (Fig. 4).
Fig. 4.
The use of ECG monitoring in the work-up of syncope. (Quoted from Ruwald and Zareba [23]).
3. External loop recorder
There are a few studies using ELR for patients with unknown syncope. The diagnostic yield of ELR was higher than standard 24h-Holter monitoring [24], and it was similar to the diagnostic yield of ILR in the same timeframe [25], [26], [27]. The limitations of ELR are patient compliance, failure to operate the device correctly, and difficulties handling cutaneous patch electrodes [26]. A cost-effectiveness analysis has indicated that the improvement in diagnostic yield offsets the cost of the ELR and that they are an economically attractive alternative when compared to Holter monitoring [28]. The use of ELR could be viewed as a first-choice tool for patients with early recurrence of syncope [23].
4. Conclusion
ILR is useful as tool for early diagnosis and improving diagnosis rate for patients with unknown syncope. ILR also provides important information on syncope mechanism and treatment strategy. However, there is no evidence of improvement of total mortality and quality of life while using ILR. The diagnostic yield of ELR in patients with syncope was similar to ILR within the same timeframe. Therefore, ELR could be considered for patients for long-term ECG monitoring before ILR.
Conflict of interest
All authors declare no conflict of interest related to this study.
References
- 1.Moya A., Sutton R., Ammirati F. Guidelines for the diagnosis and management of syncope. Eur Heart J. 2009;30:2631–2671. doi: 10.1093/eurheartj/ehp298. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Krahn A.D., Klein G.J., Yee R. Randomized assessment of syncope trial: conventional diagnostic testing versus a prolonged monitoring strategy. Circulation. 2001;104:46–51. doi: 10.1161/01.cir.104.1.46. [DOI] [PubMed] [Google Scholar]
- 3.Farwell D.J., Freemantle N., Sulke N. The clinical impact of implantable loop recorders in patients with syncope. Eur Heart J. 2006;27:351–356. doi: 10.1093/eurheartj/ehi602. [DOI] [PubMed] [Google Scholar]
- 4.Podoleanu C., Da Costa A., Defaye P. Early use of an implantable loop recorder in syncope evaluation: a randomized study in the context of the French healthcare system (FRESH study) Arch Cardiovasc Dis. 2014;107:546–552. doi: 10.1016/j.acvd.2014.05.009. [DOI] [PubMed] [Google Scholar]
- 5.Sulke N., Sugihara C., Hong P. The benefit of a remotely monitored implantable loop recorder as a first line investigation in unexplained syncope: the EaSyAS II trial. Europace. 2016;18:912–918. doi: 10.1093/europace/euv228. [DOI] [PubMed] [Google Scholar]
- 6.Edvardsson N., Frykman V., van Mechelen R. Use of an implantable loop recorder to increase the diagnostic yield in unexplained syncope: results from the PICTURE registry. Europace. 2011;13:262–269. doi: 10.1093/europace/euq418. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Solbiat M., Costantino G., Casazza G. Implantable loop recorder versus conventional diagnostic workup for unexplained recurrent syncope. Cochrane Database Syst Rev. 2016;(issue 4) doi: 10.1002/14651858.CD011637.pub2. [Art. No.:CD011637] [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Solano A., Menozzi C., Maggi R. Incidence, diagnostic yield and safety of the implantable loop-recorder to detect the mechanism of syncope in patients with and without structural heart disease. Eur Heart J. 2004;25:1116–1119. doi: 10.1016/j.ehj.2004.05.013. [DOI] [PubMed] [Google Scholar]
- 9.Furukawa T., Maggi R., Bertolone C. Additional diagnostic value of very prolonged observation by implantable loop recorder in patients with unexplained syncope. J Cardiovasc Electrophysiol. 2012;23:67–71. doi: 10.1111/j.1540-8167.2011.02133.x. [DOI] [PubMed] [Google Scholar]
- 10.Moya A., Brignole M., Menozzi C. Mechanism of syncope in patients with isolated syncope and in patients with tilt-positive syncope. Circulation. 2001;104:1261–1267. doi: 10.1161/hc3601.095708. [DOI] [PubMed] [Google Scholar]
- 11.Menozzi C., Brignole M., Garcia-Civera R. Mechanism of syncope in patients with heart disease and negative electrophysiologic test. Circulation. 2002;105:2741–2745. doi: 10.1161/01.cir.0000018125.31973.87. [DOI] [PubMed] [Google Scholar]
- 12.Brignole M., Menozzi C., Moya A. Mechanism of syncope in patients with bundle branch block and negative electrophysiological test. Circulation. 2001;104:2045–2050. doi: 10.1161/hc4201.097837. [DOI] [PubMed] [Google Scholar]
- 13.Brignole M., Sutton R., Menozzi C. Early application of an implantable loop recorder allows effective specific therapy in patients with recurrent suspected neurally mediated syncope. Eur Heart J. 2006;27:1085–1092. doi: 10.1093/eurheartj/ehi842. [DOI] [PubMed] [Google Scholar]
- 14.Brignole M., Menozzi C., Moya A. Pacemaker therapy in patients with neutrally mediated syncope and documented asystole: third international study on syncope of uncertain etiology (ISSUE-3): a randomized trial. Circulation. 2012;125:2566–2571. doi: 10.1161/CIRCULATIONAHA.111.082313. [DOI] [PubMed] [Google Scholar]
- 15.Tanno K., Onuki T. Implantable loop recorder for a patient with unexplained syncope. J Arrhythmia. 2011;27:158–159. [Google Scholar]
- 16.Onuki T., Ito H., Ochi A. Single center experience in Japanese patients with syncope. J Cardiol. 2015;66:395–402. doi: 10.1016/j.jjcc.2014.12.009. [DOI] [PubMed] [Google Scholar]
- 17.Kohno R., Abe H., Akamatsu N. Long-term follow-up of ictal asystole in temporal lobe epilepsy: is permanent pacemaker therapy needed? J Cardiovasc Electrophysiol. 2016;27:930–936. doi: 10.1111/jce.13009. [DOI] [PubMed] [Google Scholar]
- 18.Brignole M., Sutton R., Menozzi C. Lack of correlation between the responses to tilt testing and adenosine triphosphate test and the mechanism of spontaneous neurally mediated syncope. Eur Heart J. 2006;27:2232–2239. doi: 10.1093/eurheartj/ehl164. [DOI] [PubMed] [Google Scholar]
- 19.Deharo J.C., Jego C., Lanteaume A. An implantable loop recorder study of highly symptomatic vasovagal patients: the heart rhythm observed during a spontaneous syncope is identical to the recurrent syncope but not correlated with the head-up tilt test or adenosine triphosphate test. J Am Coll Cardiol. 2006;47:587–593. doi: 10.1016/j.jacc.2005.09.043. [DOI] [PubMed] [Google Scholar]
- 20.Hong P., Sulke N. Implantable diagnostic monitors in the early assessment of syncope and collapse. Prog Cardiovasc Dis. 2013;55:410–417. doi: 10.1016/j.pcad.2012.11.009. [DOI] [PubMed] [Google Scholar]
- 21.Krahn A.D., Klein G.J., Yee R. Use of an extended monitoring strategy in patients with problematic syncope. Reveal Investigation. Circulation. 1999;99:406–410. doi: 10.1161/01.cir.99.3.406. [DOI] [PubMed] [Google Scholar]
- 22.Brignole M., Vardas P., Hoffman E. Indications for the use of diagnostic implantable and external ECG loop recorders. Europace. 2009;11:671–687. doi: 10.1093/europace/eup097. [DOI] [PubMed] [Google Scholar]
- 23.Ruwald M.H., Zareba W. ECG Monitoring in Syncope. Prog Cardiovasc Dis. 2013;56:203–210. doi: 10.1016/j.pcad.2013.08.007. [DOI] [PubMed] [Google Scholar]
- 24.van Dijk N., Boer K.R., Colman N. High diagnostic yield and accuracy of history, physical examination, and ECG in patients with transient loss of consciousness in FAST: the Fainting Assessment study. J Cardiovasc Electrophysiol. 2008;19:48–55. doi: 10.1111/j.1540-8167.2007.00984.x. [DOI] [PubMed] [Google Scholar]
- 25.Brignole M., Menozzi C., Bartoletti A. A new management of syncope: prospective systematic guideline-based evaluation of patients referred urgently to general hospitals. Eur Heart J. 2006;27:76–82. doi: 10.1093/eurheartj/ehi647. [DOI] [PubMed] [Google Scholar]
- 26.Sivakumaran S., Krahn A.D., Klein G.J. A prospective randomized comparison of loop recorders versus Holter monitors in patients with syncope or presyncope. Am J Med. 2003;115:1–5. doi: 10.1016/s0002-9343(03)00233-x. [DOI] [PubMed] [Google Scholar]
- 27.Gula L.J., Krahn A.D., Massel D. External loop recorders: determinants of diagnostic yield in patients with syncope. Am Heart J. 2004;147:644–648. doi: 10.1016/j.ahj.2003.10.036. [DOI] [PubMed] [Google Scholar]
- 28.Schuchert A., Maas R., Kretzschmar C. Diagnostic yield of external electrocardiographic loop recorders in patients with recurrent syncope and negative tilt table test. Pacing Clin Electrophysiol. 2003;26:1837–1840. doi: 10.1046/j.1460-9592.2003.t01-1-00277.x. [DOI] [PubMed] [Google Scholar]