Cutaneous calcinosis in a patient with limited scleroderma: CREST Syndrome
Calcinosis or dystrophic soft-tissue calcification occurs in damaged or devitalized tissues in the presence of normal calcium/phosphorus metabolism. It is a known manifestation in the subcutaneous tissues of patients with connective tissues diseases, especially scleroderma, systemic lupus erythematosus, or dermatomyositis, and may involve a relatively localized areas or present as widespread calcinosis (1). Little is known about its physiopathology. It occurs in tissues that are under chronic stress, such as local trauma or damage associated with underlying inflammatory processes (2).
Subcutaneous calcinosis occurs in all subsets of scleroderma but is more prominent in patients with limited scleroderma and in those with anticentromere antibody. CREST syndrome is a limited form of scleroderma, characterized by calcinosis, Raynaud's phenomenon, esophageal dysmotility, sclerodactyly, and telangiectasia (3).
A 46-year-old woman suffered from CREST syndrome for 15 years. She had sclerotic cutaneous findings on her face and fingers (sclerodactyly), prominent facial telengectasia, Raynoud’s phenomenon, and esophageal reflux. There were also multiple hardened erythematous-whitish nodules, some having a chalky appearance, around her knees (Figure 1). X-ray showed extensive calcinosis in the soft tissue of the knees (Figure 2). Pulmonary arterial pressure without pulmonary fibrosis was found to be 40 mmHg using echocardiography. Antinuclear and anti-centromere antibodies were positive. Serum calcium and phosphorus levels were within the normal ranges. She had been treated with nifedipine, low dose aspirin, and colchicine for many years. Treatment was initiated with aluminum hydroxide. Medical therapy for cutaneous calcinosis is limited and has variable benefits. Multiple treatment approaches with diltiazem, disodium etidronate, probenecid, colchicine, minocycline, low-dose warfarin, and intralesional adrenal steroids have been explored, but no standard treatment has convincingly prevented or reduced calcinosis.
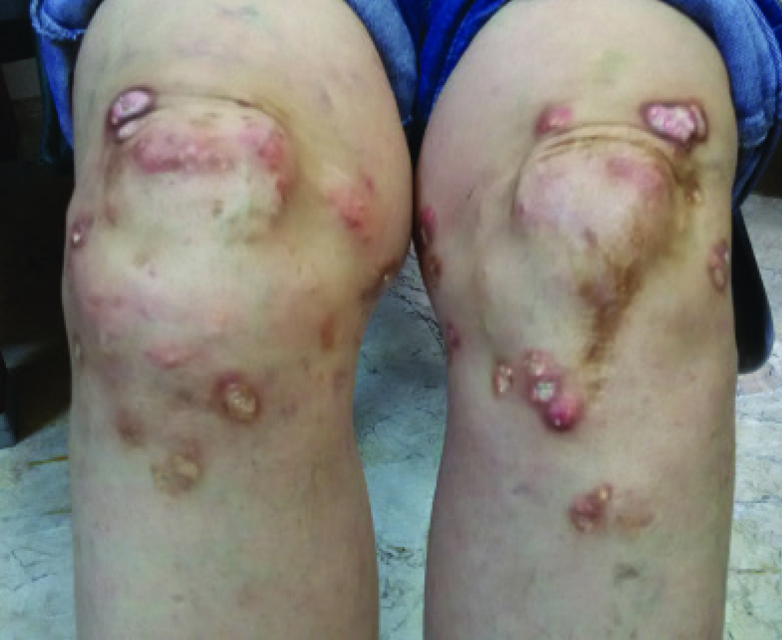
Figure 1.
Multiple erythematous and whitish papules/nodules, some of which have a chalky white material on the around knees
Figure 2. a, b.
Axial (a) and lateral (b) radiographic images of knee show wide-spread and multiple radio-opacities on the periarticular area
Footnotes
Informed Consent: Verbal informed consent was obtained from the patient who participated in this study.
Peer-review: Externally peer-reviewed.
Conflict of Interest: No conflict of interest was declared by the authors.
Financial Disclosure: The authors declared that this study has received no financial support.
References
- 1.Chander S, Gordion P. Soft tissue and subcutaneous calcification in connective tissue diseases. Cur Opin Rheumatol. 2012;24:158–64. doi: 10.1097/BOR.0b013e32834ff5cd. https://doi.org/10.1097/BOR.0b013e32834ff5cd. [DOI] [PubMed] [Google Scholar]
- 2.Boulman N, Slobodin G, Rozenbaum M, Rosner I. Calcinosis in rheumatic diseases. Semin Arthritis Rheum. 2005;34:805–12. doi: 10.1016/j.semarthrit.2005.01.016. https://doi.org/10.1016/j.semarthrit.2005.01.016. [DOI] [PubMed] [Google Scholar]
- 3.Wigley FM. Systemic sclerosis. In: Klippel JH, Dieppe PA, editors. Rheumatology. Mosby-Year Book Europe Limited; 1998. pp. 7.9.1–9.7. [Google Scholar]