Abstract
Introduction
Minimal change disease is a common cause of nephrotic syndrome. In general, patients with minimal change disease respond to corticosteroids and have excellent long-term renal survival. However, some patients have less favorable outcome. These patients are often thought to have progressed to focal segmental glomerulosclerosis. We previously reported that a segmental loss of podocyte markers is present before the development of focal segmental glomerulosclerosis in a rat model. Here, we investigated whether loss of podocyte marker nephrin can serve as a biomarker for predicting poor outcome in patients with minimal change disease.
Methods
We obtained 47 kidney biopsy samples from patients diagnosed with minimal change disease and stained sections with periodic acid−Schiff and for nephrin. Nephrin loss was scored by 2 independent researchers who were blinded to clinical outcome. Clinical data were collected retrospectively, and nephrin loss was correlated with clinical follow-up data.
Results
Nephrin loss was present in 34% of the biopsy samples. During follow-up, patients with nephrin loss achieved remission less frequently (61%) compared to patients without (96%) (P = 0.002). Moreover, 5-year eGFR was lower in the patients with renal nephrin loss. The risk of eGFR decreasing to < 60 ml/min per 1.73m2 increased with each percentage of glomeruli with nephrin loss (hazard ratio = 1.044, 95% confidence interval = 1.02−1.07).
Conclusion
These results indicate that nephrin loss in patients with minimal change disease can help predict both remission and long-term renal outcome.
Keywords: biomarker, focal segmental glomerulosclerosis, minimal change disease, nephrin, nephrotic syndrome
Minimal change disease (MCD) is a common manifestation of nephrotic syndrome in both children and adults.1 MCD is typically diagnosed by examining a renal biopsy sample; few or no abnormalities are visible using light microscopy, but extensive foot process effacement is observed using electron microscopy.2 In general, patients with MCD respond well to corticosteroids and have excellent long-term patient and renal survival.3 However, the degree of responsiveness to corticosteroids varies widely. In addition, a substantial number of patients have poor long-term outcomes, with frequent relapses and eventual renal impairment.3, 4, 5, 6, 7 Currently, no adequate clinical parameters or biomarkers are available for predicting clinical outcome and prognosis. Thus, to provide patients a better prognosis and more targeted therapies, a marker for predicting outcome is urgently needed.
Patients with MCD who have a decline in renal function occasionally have focal segmental glomerulosclerosis (FSGS) in subsequent renal biopsy samples.5, 8 Primary FSGS is another common manifestation of nephrotic syndrome, and both primary FSGS and MCD lie within the spectrum of podocyte injury-related glomerular diseases. However, whether primary FSGS represents an advanced stage of MCD is currently a matter of debate.9, 10 In support of this notion, patients diagnosed with MCD based on their original biopsy results have shown FSGS lesions in subsequent biopsy samples.8, 10, 11, 12 A similar course of events has been reported in renal transplant cases.11 The presence of FSGS in a follow-up biopsy sample is usually associated with unfavorable outcome, and these patients often develop renal failure.8
We previously reported that the Munich Wistar Frömter rat, a model for hereditary proteinuria and glomerulosclerosis, has segmental loss of a molecule important for podocyte integrity in rats prior to the onset of FSGS.13 Interestingly, segmental loss of the podocyte marker nephrin has also been reported in patients with FSGS.14 However, whether nephrin loss also occurred in nonsclerotic glomeruli was not clarified.
Nephrin is a transmembrane protein located at the podocyte slit diaphragm. In 1998, mutations in the nephrin-encoding gene NPHS1 were identified in children with congenital nephrotic syndrome of the Finnish type.15 These mutations will lead to the complete deletion or partial truncation of the protein, and their identification revealed the key role of nephrin in maintaining the glomerular filtration barrier.15 In addition to its role in congenital nephrotic syndrome, nephrin has also been studied in various acquired nephrotic syndromes, including MCD.14, 16, 17, 18 However, the results are inconsistent; some studies reported a downregulation of nephrin expression in MCD compared to controls,16, 17 whereas other studies reported no apparent change in nephrin expression.14, 18 These results raise the question of whether these disparate findings could be due to differences in disease course.
Given that loss of nephrin expression may reflect podocyte injury prior to the onset of FSGS lesions, and because the development of FSGS in patients with MCD is associated with poor long-term outcomes, we tested the hypothesis that segmental loss of nephrin in patients with MCD could be used as an immunohistological biomarker for predicting outcome.
Methods
We retrospectively searched the archives of the Department of Pathology at the Leiden University Medical Center (LUMC) for renal biopsy samples of patients who had biopsy-confirmed MCD and were evaluated at the LUMC from 1985 through 2015. Patients were excluded if (i) the biopsy sample was obtained from a transplanted kidney, (ii) the patient had another underlying kidney disease, (iii) the biopsy sample contained < 5 glomeruli or was otherwise inadequate for evaluation, (iv) the patient had a viral infection or had taken medication known to elicit nephrotic syndrome, or (v) the patient did not have nephrotic syndrome. Our initial search yielded 194 biopsy samples of patients with MCD. Biopsy samples were then excluded for the following reasons: obtained from a transplanted kidney (22 samples), comorbidity (26 samples), insufficient tissue for analysis (48 samples), the patient did not have nephrotic syndrome (8 samples), no clinical data were available (39 samples), or the biopsy was the second from a patient already in our cohort (4 samples). Thus, a total of 47 patient biopsy samples were included in the analysis.
As a control group, we used 12 kidney samples that were obtained from Eurotransplant donors and were not suitable for transplantation for technical reasons.
Clinical Data
Clinical data were extracted from the patients’ medical records obtained from the hospitals at which the patients were treated. We collected the patients’ clinical data at the time of biopsy, at approximately 1, 4, and 16 weeks of follow-up, and for up to 5 years of follow-up. The following laboratory results were obtained at the time of biopsy and approximately 1, 4, and 16 weeks after the biopsy: estimated glomerular filtration rate (eGFR; using the Modification of Diet in Renal Disease formula for adults and the bedside Schwartz formula for children), serum albumin (in g/l), and proteinuria. In addition, we extracted information on systolic and diastolic blood pressure (in mm Hg), weight, height, sex, age, ethnicity, medication used at the time of the biopsy, and whether a steroid trial had been attempted before the biopsy.
We also collected follow-up data regarding remission, the recurrence of nephrotic syndrome (relapse), therapy/prednisone resistance, therapy dependence, and 5-year eGFR. Renal insufficiency and transplantation were measured until the patient was lost to follow-up, died, or received a transplant, or the study period ended (on 31 December 2015). The medical records were also used to identify cases in which evidence of focal segmental glomerulosclerosis (FSGS) appeared in a follow-up biopsy sample. Subanalyses of clinical outcome were performed for patients < 18 of age and for patients ≥ 18 years of age (Supplementary Tables S1 and S2).
Endpoint Definitions
Nephrotic syndrome was defined as nephrotic range proteinuria, serum albumin levels < 35 g/l, and edema. Complete remission was defined as proteinuria < 0.3 g/24 h and no proteinuria on dipstick or when clearly stated in the medical records; partial remission was defined as a reduction in proteinuria to 0.3 to 3.5 g/24 h.19
In the adult patients, hypertension was defined as systolic blood pressure (SBP) > 140 mm Hg and/or diastolic blood pressure (DBP) > 90 mm Hg, or the need for hypertension medication to maintain a normal blood pressure.20 In the pediatric patients, hypertension was defined as SBP and/or DPB values in the ≥ 95th percentile for age, sex, and height or the need for hypertension medication.21 Renal insufficiency was defined as eGFR < 60 ml/min. Steroid dependence refers to relapse while on therapy or when continuous treatment was needed to maintain remission. Steroid resistance refers to an insufficient reduction in proteinuria following a course of prednisone. A relapse was considered to have occurred when stated in the patient’s medical records after achievement of remission.
Histology
Sequential sections (4-μm thickness) were cut from paraffin-embedded samples using a Leica microtome. The sections were stained with periodic acid−Schiff (PAS) using a standard protocol.
An experienced pathologist examined the PAS-stained sections for the presence of mesangial expansion, hyalinosis, synechiae (defined as single cellular bridges),22, 23 and global sclerosis (which can also be seen in MCD and healthy control kidneys). In the sections prepared for research purposes, 2 patients had a lesion consistent with FSGS; because FSGS had not been diagnosed in the routine diagnostics, these 2 biopsy samples were included for further analysis. Data on electron microscopy were obtained from the patients’ original pathology reports.
Immunohistochemistry
For each sample, a section adjacent to the PAS-stained section was stained using a rabbit anti-nephrin antibody (ab58968; Abcam, Cambridge, UK). As a negative control, a rabbit IgG-negative control fraction (Dako, Glostrup, Denmark) was used at the same concentration as the anti-nephrin antibody. Goat anti-rabbit EnVision horseradish peroxidase−conjugated antibody (Dako) was used as the secondary antibody, and staining was visualized using diaminobenzidine as the chromogen. The sections were counterstained with hematoxylin and coverslipped with mounting medium.
To determine the presence of podocytes at the site of nephrin loss, Wilms Tumor 1 (WT1) staining (sc-192; Santa Cruz Biotechnology, Dallas, TX) was performed on adjacent sections for biopsy samples with nephrin loss.
Scoring of Staining Patterns
PAS- and nephrin-stained sections were scanned in an Ultra-Fast scanner (Phillips Healthcare, Amsterdam, the Netherlands). The sections were then scored by 2 observers who were blinded with respect to clinical outcome. Loss of nephrin expression was scored for all scorable glomeruli in each section. Loss of nephrin was defined as > 10% interruption in the circumferential nephrin staining surrounding the glomerular tuft. A single nephrin-negative capillary loop was not considered to be nephrin loss, as this was often seen in healthy controls. Supplementary Figure S1 shows examples of glomeruli with < 10% nephrin loss. Nephrin-negative cellular adhesions of visceral and/or parietal epithelial cells were also considered to indicate nephrin loss, regardless of size. Consensus between the 2 observers was reached by discussion. Finally, the number of biopsy samples with nephrin loss in at least 1 glomerulus was determined, and the percentage of glomeruli with nephrin loss was calculated. In addition, nephrin loss in glomeruli was also scored semiquantitatively (Supplementary Material). To determine whether nephrin loss was not simply a surrogate marker for segmental sclerosis, consecutive PAS-stained slides were used to examine the presence of glomerulosclerosis at the site of nephrin loss.
WT1 staining was assessed in all glomeruli with segmental or global nephrin loss. Podocytes were scored as present when WT1-positive cells were detected at the exact site of nephrin loss.
Statistical Analysis
The Statistical Package for Social Sciences (SPSS) version 23 (IBM, Armonk, NY) and Rstudio were used for statistical analysis. Continuous variables were compared between groups using the Student t test or the Mann−Whitney U test and are expressed as the mean ± SD or as the median and interquartile range (IQR). Categorical variables were compared using the χ2 test or Fisher exact test and are expressed as a percentage. The development of hypertension at 5 years was analyzed using a z test for differences between proportions and reported as a cumulative percentage. The Spearman correlation was performed with average nephrin loss score and continuous variables. Cox regression analysis was used to analyze survival. Because only 1 possible competing event was observed, we did not calculate cumulative incidence functions. A linear mixed model was used to analyze whether the difference in proteinuria between patients with and without nephrin loss was time point dependent by evaluating the interaction term between nephrin loss and time. For the linear mixed model, proteinuria data were log transformed. The area under the curve (AUC) for the percentage of glomeruli with nephrin loss was calculated using the receiver operating characteristic (ROC) curve. For renal insufficiency, the corresponding Harrell C statistic was calculated using the patients’ follow-up times, and the patients’ XBETA-predictors calculated in the Cox regression analysis.
Ethics Considerations
Tissue samples were collected during routine patient care. For medical research purposes, the tissues were coded and then handled anonymously in accordance with the Dutch National Ethics Guidelines (Code for Proper Secondary Use of Human Tissue).
Results
Glomerular Nephrin Expression and Renal Histology in Patients With MCD
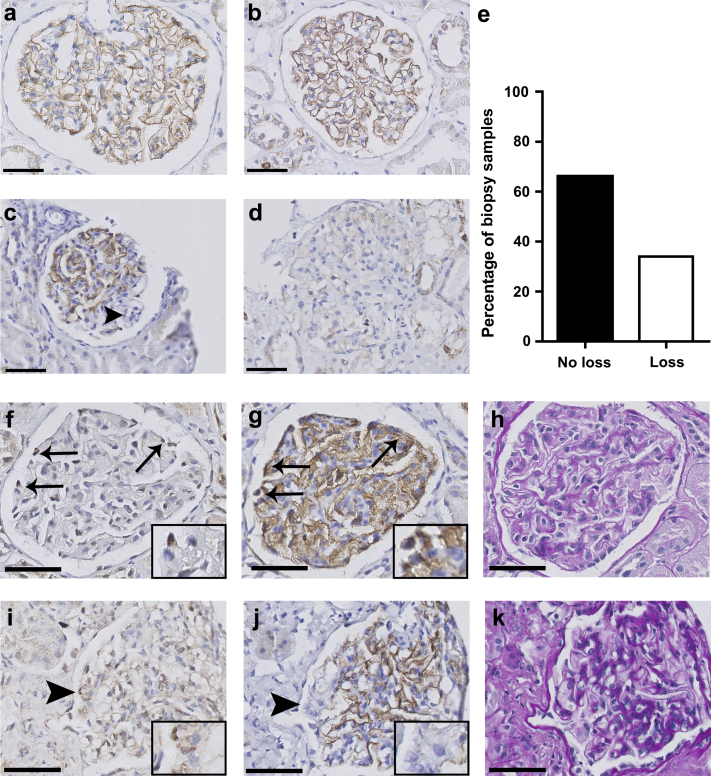
We obtained 47 renal biopsy samples from patients with MCD and 12 kidney samples from healthy controls; these were then immunostained for nephrin. As expected, control kidney sections had a linear staining pattern for nephrin; this pattern followed the glomerular basement membrane (Figure 1a and Supplementary Figure S1). A similar pattern was observed in biopsy samples obtained from patients with MCD (Figure 1b); however, we also observed glomeruli with either segmental (Figure 1c) or global (Figure 1d) nephrin loss. In total, 34% of the patient biopsy samples had nephrin loss in 1 or more glomeruli (Figure 1e). With the exception of 2 glomeruli in 2 sections, nephrin loss was not co-localized with glomerulosclerosis.
Figure 1.
Normal nephrin staining pattern and nephrin loss in patients with minimal change disease. Nephrin-stained kidney sections from a healthy control (a), a patient with minimal change disease (MCD) without nephrin loss (b), and 2 patients with MCD with nephrin loss (c,d). Panels (a) and (b) show a normal linear pattern of nephrin staining along the glomerular basement membrane. In panels (c) and (d), nephrin loss was either (c; arrowhead) segmental or (d) global. (e) Quantification of nephrin loss (defined as nephrin loss in at least 1 glomerulus) in the biopsy samples obtained from patients with MCD. (f,i) To determine whether podocytes were still present at the site of nephrin loss, sections with nephrin loss were stained for the podocyte marker Wilms Tumor 1 (WT1). Example images of WT1 (f,i), nephrin (g,j), and periodic acid−Schiff (h,k) staining in a patient without nephrin loss (f−h) and a patient with nephrin loss (i−k). Podocytes in glomeruli without nephrin loss (f−h) were WT1 positive (f, arrows) and nephrin positive (g, arrows). The presence of WT1-positive cells (i, arrowhead) at the site of nephrin loss (j, arrowhead) indicates that podocytes were still present. Bar = 50 μm.
Next, we investigated whether podocytes were still present at the site of nephrin loss. Staining sequential sections for nephrin and the podocyte marker WT1 revealed WT1-positive staining at the site of nephrin expression (Figure 1f−h) but also at the site of nephrin loss (Figure 1i−k). In total, 82% and 66% of glomeruli with global nephrin loss and segmental nephrin loss, respectively, contained WT1-positive cells at the site of nephrin loss, indicating that podocytes were still present during nephrin loss.
To determine whether kidneys with nephrin loss differed histologically from kidneys without nephrin loss, we examined the PAS-stained sections; these results are summarized in Table 1. We found that the prevalence of global sclerosis, mesangial expansion, and hyalinosis did not differ significantly between the 2 groups. Interestingly, we found synechiae in 2 biopsy samples with nephrin loss. An analysis of electron microscopy data from the original pathology report revealed that foot process effacement was similar between the patients with nephrin loss and the patients without nephrin loss.
Table 1.
Histologic and electron microscopy characteristics of the patients with nephrin loss and the patients without nephrin loss
| Characteristics | Loss (n = 16) | No loss (n = 31) | P valuea |
|---|---|---|---|
| Global sclerosis, n (%) | 5 (33) | 3 (10) | 0.10 |
| Hyalinosis, n (%) | 3 (20) | 4 (13) | 0.67 |
| Mesangial expansion, n (%) | 2 (13) | 0 (0) | 0.11 |
| Synechiae, n (%) | 2 (13) | 0 (0) | 0.11 |
| Foot process effacement, n (%)b | 14 (100) | 25 (100) | - |
χ2 Test.
In 8 patients, electron microscopy data were not available or were of insufficient quality.
Baseline Clinical Characteristics of the Patients With and Without Nephrin Loss
Next, we looked for differences at time of biopsy between patients with nephrin loss and patients without nephrin loss by comparing the patients’ clinical parameters; these results are summarized in Table 2. We found no significant difference between the 2 groups with respect to age, male-to-female ratio, weight, eGFR, or degree of proteinuria. Moreover, both systolic blood pressure and diastolic blood pressure did not differ between the groups, both in children and in adults, and the groups did not differ with respect to the medications used. Finally, separate analyses of nephrin loss in children and adults showed that the prevalence of nephrin loss was similar between patients < 18 years (31%) and patients >18 years (36%) of age (P = 0.77).
Table 2.
Baseline clinical characteristics of the patients with nephrin loss and the patients without nephrin loss
| Characteristics | Loss | No loss | P value |
|---|---|---|---|
| Age, yr, median (IQR) | 33 (14−58) | 25 (9−40) | 0.18a |
| Male:female, n | 10:6 | 20:11 | 0.89b |
| Weight, kg, mean (SD)c | 72 (21) | 74 (35) | 0.88 |
| BP, mm Hg, mean (SD)e | |||
| Age < 18 yr | |||
| SBP | 125 (10) | 108 (11) | 0.07d |
| DBP | 75 (14) | 64 (12) | 0.24d |
| Age ≥ 18 yr | |||
| SBP | 164 (31) | 145 (27) | 0.25d |
| DBP | 89 (12) | 83 (11) | 0.30d |
| eGFR, ml/min per 1.73/m2, median (IQR)f | 72 (50−123) | 89 (60−153) | 0.20a |
| Proteinuria, g/24 h, median (IQR)g | 8.6 (5.5−14) | 10 (7.0−13) | 0.74a |
| Medication, n (%) | 0.31b | ||
| No medication | 1 (7) | 0 | |
| Conservative treatmenth | 4 (29) | 4 (18) | |
| Prednisone | 9 (64) | 15 (68) | |
| Cyclosporine/cyclophosphamide/rituximab | 0 (0.0) | 3 (14) |
DBP, diastolic blood pressure; eGFR, estimated glomerular filtration rate; IQR, interquartile range; SBP, systolic blood pressure.
Mann−Whitney U test for nonparametric variables.
χ2 Test.
Respectively, n = 12 and n = 21.
Independent Student t test.
Respectively, n = 13 and n = 21. Of the patients, 16 were <18 years and 31 patients were ≥18 years of age, respectively.
Respectively, n = 13 and n = 18.
Respectively, n = 9 and n = 20.
Conservative treatment is defined as angiotensin-converting enzyme inhibitor or diuretic use.
To determine whether a steroid trial before biopsy could have affected nephrin loss, we determined whether patients had had a steroid trial before biopsy. We found that 69% of children and 21% of adults had had some sort of steroid trial before biopsy. The percentages of nephrin loss were similar between patients who did or did not have a steroid trial first (29% vs. 36%, respectively; P = 0.65).
Follow-up Characteristics and Response to Therapy in Patients With Nephrin Loss and Patients Without Nephrin Loss
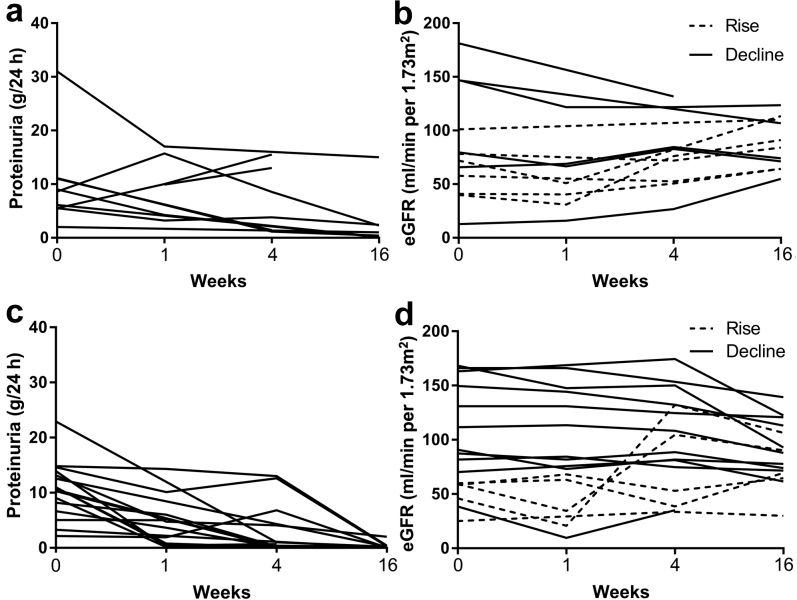
To determine the prognostic value of nephrin loss, we first compared eGFR and proteinuria between the 2 groups after a 16-week period from the start of an episode with nephrotic syndrome within which the biopsy sample was taken. At the 16-week follow-up, eGFR was similar between the groups, and linear mixed model analysis revealed that the difference in eGFR was not time point dependent. In contrast, proteinuria was higher in the patients with nephrin loss (1.0 g/24 h) compared to the patients without nephrin loss (0.15 g/24 h) (P = 0.02; Table 3). Moreover, linear mixed model analysis revealed that this difference in proteinuria was time point dependent (Pinteraction = 0.04); thus, nephrin loss is associated with higher proteinuria levels. The time course of both proteinuria and eGFR is shown for each patient in Figure 2.
Table 3.
Follow-up characteristics of the patients with nephrin loss and the patients without nephrin loss
| Characterstics | Loss | No loss | P value |
|---|---|---|---|
| Remission, n (%) | 0.002a | ||
| Complete | 8 (61) | 27 (96) | |
| Partial | 0 (0.0) | 1 (4.0) | |
| No remission | 5 (39) | 0 (0.0) | |
| Proteinuria 16-week follow-up, g/24 h, median (IQR)c | 1.0 (0.19−2.4) | 0.15 (0.0−0.21) | 0.02b |
| eGFR 16-week follow-up, ml/min per 1.73 m2, median (IQR)d | 84 (64−110) | 88 (70−114) | 0.69b |
| Relapse, n (%) | 5 (56) | 22 (76) | 0.40a |
| Steroid resistance, n (%) | 4 (29) | 1 (3.4) | 0.03a |
| Steroid dependence, n (%) | 9 (64) | 14 (48) | 0.32a |
| Transplantation, n (%) | 1 (7.1) | 0 (0.0) | 0.34a |
| 5-Year eGFR, ml/min per 1.73 m2, median (IQR)e | 54 (42−97) | 97 (78−119) | 0.08b |
| Nonhypertensive at 5 years (%)f | 31 | 62 | 0.09g |
| FSGS at follow-up, n (%) | 3 (20) | 2 (7.4) | 0.33a |
eGFR, estimated glomerular filtration rate; FSGS, focal segmental glomerulosclerosis; IQR, interquartile range.
χ2 Test.
Mann–Whitney U test.
Respectively, n = 7 and n = 15.
Respectively, n = 11 and n = 17.
Respectively, n = 5 and n = 13.
Cumulative percentage free of events at 5-year time point.
z Test for difference between 2 proportions.
Figure 2.
Proteinuria and estimated glomerular filtration rate (eGFR) during short-term follow-up. Proteinuria was measured over time in each patient with nephrin loss (a) and in each patient without nephrin loss (c). At 16 weeks, proteinuria was higher in the patients with nephrin loss (1.0 g/24 h) compared to the patients without nephrin loss (0.15 g/24 h, P = 0.02). Differences in proteinuria were associated with the time point (linear mixed model, Pinteraction = 0.04). (b,d) eGFR levels were similar between the patients with nephrin loss (b) and the patients without nephrin loss (d; P = 0.69).
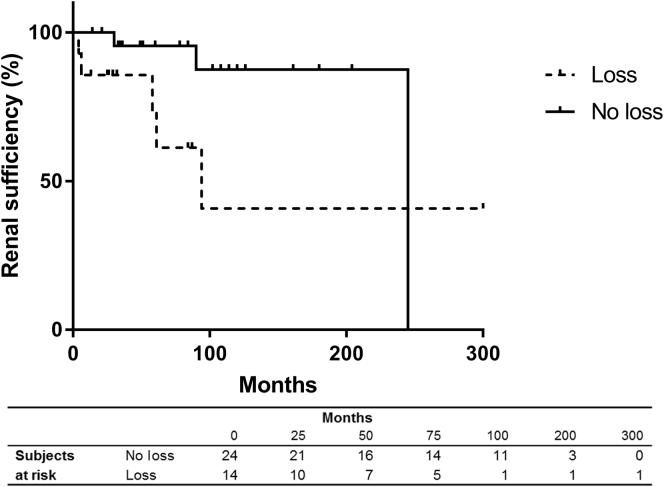
Interestingly, we also found a significant difference between the 2 groups with respect to remission rate. Specifically, 96% of patients without nephrin loss achieved remission, whereas only 61% of patients with nephrin loss achieved remission (P = 0.002) (Table 3). In addition, we found a significant difference between the 2 groups with respect to steroid resistance (P = 0.03) but not with respect to steroid dependence (P = 0.32). With respect to kidney function, the 5-year eGFR values were lower in the patients with nephrin loss (54 ml/min per 1.73 m2) compared to the patients without nephrin loss (97 ml/min per 1.73 m2); however, this difference was not statistically significant (P = 0.08). Moreover, patients with nephrin loss developed renal insufficiency (defined as eGFR < 60 ml/min per 1.73 m2) faster compared to the patients without nephrin loss (Figure 3). Cox regression analysis revealed that the chance of developing renal insufficiency increased with each percentage of glomeruli with nephrin loss (hazard ratio = 1.044; 95% confidence interval = 1.02−1.07).
Figure 3.
Renal insufficiency in minimal change disease patients with nephrin loss. Kaplan−Meier survival curve depicting renal insufficiency in patients with nephrin loss and patients without nephrin loss. Renal insufficiency developed earlier in the patients with nephrin loss compared to the patients without nephrin loss. Moreover, the likelihood of developing renal insufficiency increased with every percentage of glomeruli with nephrin loss, as shown by Cox regression analysis (hazard ratio = 1.04, 95% confidence interval 1.02−1.07).
To determine whether the degree of nephrin loss in a glomerulus might provide a better prediction of clinical outcome, we also scored nephrin loss semiquantitatively. We analyzed this in 2 different manners. First, the difference in “average nephrin loss score” was determined for several clinical outcome characteristics (Supplementary Table S3). This showed that patients who did not achieve remission and patients who were therapy resistant had a higher nephrin score, in line with the results of the dichotomous nephrin scoring. Also, average nephrin loss correlated with proteinuria at 16 weeks (rho = 0.51; P = 0.016). Second, we categorized patients based on the most affected glomerulus. Interestingly, higher scores were significantly associated with a failure to achieve remission (Supplementary Table S4) (P < 0.001).
Diagnostic Value of Nephrin Loss
Finally, to investigate the diagnostic value of nephrin loss in biopsy samples obtained from patients with MCD, we calculated the sensitivity, specificity, and AUC values of nephrin loss in terms of remission and the Harrell C statistic for development of renal insufficiency. With respect to remission, the sensitivity and specificity of nephrin loss were 78% and 100%, respectively. The corresponding ROC curve for the percentage of glomeruli with nephrin loss showed an AUC of 0.89 (P = 0.005). With respect to renal insufficiency, the Harrell C statistic value was 0.80.
Discussion
In this study, we investigated whether nephrin loss in a renal biopsy sample can be used to predict clinical outcome in patients with MCD. We found that patients with nephrin loss were less likely to achieve remission compared to patients without nephrin loss. Strikingly, we also found that 5-year eGFR was lower in patients with nephrin loss, and we found that the risk of developing renal insufficiency increased with the percentage of glomeruli with nephrin loss. Generally speaking, patients with MCD often have a good clinical prognosis and excellent renal survival. However, some patients have an unfavorable clinical course, for example, failing to respond to therapy and/or developing renal insufficiency or failure. Therefore, it is important to find robust biomarkers to help clinicians identify patients who are more likely to have an unfavorable clinical response. Here, we report that nephrin loss can help to distinguish between these 2 patient groups with respect to remission and renal outcome. Assessing nephrin loss in a biopsy sample may help clinicians identify patients who would likely benefit from more rigorous follow-up care. Moreover, nephrin loss may indicate that a prolonged course of corticosteroids may not necessarily be recommended in patients who do not respond to therapy.
On the other hand, although nephrin loss was associated with therapy resistance, it was not associated with steroid dependence, nor was it associated with relapse. Taken together, these results indicate that detection of nephrin loss can help identify patients with a more chronic disease course, but may not help identify patients with frequent relapses and/or a fluctuating disease course.
We found that the average nephrin score, based on the degree of nephrin loss in all the glomeruli in a biopsy sample, led to the same conclusions compared to the dichotomous scoring based on the presence or absence of nephrin loss. This indicates that the simpler dichotomous scoring is sufficient to assess nephrin loss, which makes translation into clinical practice easier. Interestingly, we found that the results of the scoring based on the highest score of nephrin loss in a glomerulus was more strongly correlated with achieving remission compared to the dichotomous classification. This finding suggests that using a different cut-off value for the dichotomous classification may further improve the predictive value of nephrin loss. Future studies should examine this in further detail using a larger patient cohort.
A potential limitation of our study is that some of the patients with nephrin loss may have had FSGS all along and were missed during routine diagnostics due to sampling error. All of the patients in our study were diagnosed with MCD; however, we cannot exclude the presence of FSGS lesions due to a sampling error. Accordingly, 2 of our patients had segmental lesions that were identified only after the biopsy sample was sectioned further for research purposes; these lesions were not present in the original slides prepared for routine diagnostics. Both of these patients also had extensive segmental nephrin loss in unaffected glomeruli. Therefore, in addition to indicating poor outcome, nephrin loss may also indicate a missed diagnosis of FSGS. Nevertheless, finding nephrin loss in the same biopsy sample used for diagnostic purposes provides additional information regarding the patient’s prognosis, regardless of whether sampling error had or had not occurred. It is important to note that because nephrin loss does not affect all glomeruli in a section, sampling error of nephrin loss should still be considered when using nephrin loss as an immunohistological biomarker.
Another limitation of our study is that the biopsy samples were taken at different time points. Especially in children, biopsy samples are sometimes taken later in the disease course and not during the first episode of nephrotic syndrome, in which a steroid trial is often already attempted. However, in our study, 69% of children and 21% of adults had steroids before renal biopsy, and nephrin loss was similar between patients who did or did not have a steroid trial first. Therefore, our data do not support the notion that steroids affect nephrin loss.
In addition, our cohort contained both adults and children, and clinical response can differ between children and adults with MCD.24 We observed a similar rate of nephrin loss between the children and adults. Separate subanalyses of the children and adults revealed similar trends with respect to renal function and response to therapy, although nephrin loss appeared to have a greater effect on response to therapy among the children, as 75% of pediatric patients with nephrin loss did not achieve remission (Supplementary Table S1). Nevertheless, it is difficult to draw definite conclusions, as our study lacked sufficient power for such an analysis. Therefore, differences in the prognostic value of nephrin loss between different age categories of patients with MCD should be investigated in future studies.
In our study, we found that nephrin loss is associated with poor renal outcome. With respect to pathophysiology, it would be interesting to determine whether poor outcome was due to podocyte loss and/or the selective loss of nephrin. In our staining experiments, we found WT1-positive podocytes to be present at the site of nephrin loss. Given that MCD is considered a podocytopathy and is characterized by extensive podocyte foot process effacement, nephrin loss in MCD might be indicative of more severe podocyte damage. Although foot process effacement in MCD is generally considered to be reversible, irreversible foot process effacement is believed to underlie the development of glomerulosclerosis.25 The point at which foot process effacement becomes irreversible is currently unknown; however, in animal studies, both the dose and exposure duration to the compound causing podocyte damage have been suggested as contributing factors.26 It is believed that loss of podocytes following prolonged stress and the subsequent formation of adhesions between the glomerular filtration barrier and Bowman capsule (synechiae) play a major contributing role in the formation of sclerotic lesions.27 Consistent with this notion, we found synechiae in 2 patients with nephrin loss, which is indicative of the early development of a segmental sclerotic lesion.
Several mechanisms of nephrin loss have been described. For example, in vitro experiments showed nephrin shedding from podocytes under diabetic conditions.28 In patients with diabetic nephropathy, nephrin can be detected in the urine, and urinary nephrin levels are correlated with renal traits.29 Menne et al. reported that nephrin loss, but not the loss of other slit-pore proteins, is mediated by protein kinase Cα in experimental diabetic nephropathy.30 Nephrin shedding has also been studied in preeclampsia. For example, Collino et al. reported that nephrin shedding is induced by endothelin-1 produced by endothelial cells after incubation with patient sera.31 Moreover, nephrin loss was also observed after in vitro stimulation of podocytes with serum obtained from patients with FSGS.32 This suggests that in MCD, nephrin loss may also be due to nephrin shedding, possibly induced by a factor derived from patient serum.
If nephrin loss in MCD is caused by shedding, nephrin should be detectable in the urine. Indeed, urinary nephrin has been studied as a biomarker for early renal complications in several diseases.29, 33, 34, 35 Importantly, measuring urinary nephrin is noninvasive and can be performed repeatedly, thereby reducing sampling error. Thus, urinary nephrin should be explored as a possible biomarker for predicting long-term outcome.
In conclusion, we report that nephrin loss in renal biopsy samples obtained from patients with MCD can be used to predict the patients’ response to therapy, the likelihood of achieving remission, and long-term renal outcome, thereby supporting the use of nephrin as a biomarker in MCD.
Disclosure
All the authors declared no competing interests.
Acknowledgments
This study was presented in part at the American Society of Nephrology Kidney Week, 15−20 November 2016, Chicago, IL (FR-PO643). We thank Prof. L.A. van Es for his excellent conceptual and clinical advice.
Footnotes
Supplementary Material. Supplementary Material contains Figure S1, Tables S1–S4, and Supplementary Material and Methods.
Supplementary material is linked to the online version of the paper at www.kireports.org.
Supplementary Material
Supplementary Material contains Figure S1, Tables S1–S4, and Supplementary Material and Methods.
References
- 1.Fogo A.B. Minimal change disease and focal segmental glomerulosclerosis. Nephrol Dial Transplant. 2001;16(suppl 6):74–76. doi: 10.1093/ndt/16.suppl_6.74. [DOI] [PubMed] [Google Scholar]
- 2.Ranganathan S. Pathology of podocytopathies causing nephrotic syndrome in children. Front Pediatr. 2016;4:32. doi: 10.3389/fped.2016.00032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Chembo C.L., Marshall M.R., Williams L.C. Long-term outcomes for primary glomerulonephritis: New Zealand Glomerulonephritis Study. Nephrology [Carlton] 2015;20:899–907. doi: 10.1111/nep.12538. [DOI] [PubMed] [Google Scholar]
- 4.Nolasco F., Cameron J.S., Heywood E.F. Adult-onset minimal change nephrotic syndrome: a long-term follow-up. Kidney Int. 1986;29:1215–1223. doi: 10.1038/ki.1986.130. [DOI] [PubMed] [Google Scholar]
- 5.Idelson B.A., Smithline N., Smith G.W. Prognosis in steroid-treated idiopathic nephrotic syndrome in adults. Analysis of major predictive factors after ten-year follow-up. Arch Intern Med. 1977;137:891–896. [PubMed] [Google Scholar]
- 6.Lee S.W., Yu M.Y., Baek S.H. Glomerular immune deposits are predictive of poor long-term outcome in patients with adult biopsy-proven minimal change disease: a cohort study in Korea. PLoS One. 2016;11:e0147387. doi: 10.1371/journal.pone.0147387. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Waldman M., Crew R.J., Valeri A. Adult minimal-change disease: clinical characteristics, treatment, and outcomes. Clin J Am Soc Nephrol. 2007;2:445–453. doi: 10.2215/CJN.03531006. [DOI] [PubMed] [Google Scholar]
- 8.Tejani A. Morphological transition in minimal change nephrotic syndrome. Nephron. 1985;39:157–159. doi: 10.1159/000183363. [DOI] [PubMed] [Google Scholar]
- 9.Maas R.J., Deegens J.K., Smeets B. Minimal change disease and idiopathic FSGS: manifestations of the same disease. Nat Rev Nephrol. 2016;12:768–776. doi: 10.1038/nrneph.2016.147. [DOI] [PubMed] [Google Scholar]
- 10.Fogo A., Hawkins E.P., Berry P.L. Glomerular hypertrophy in minimal change disease predicts subsequent progression to focal glomerular sclerosis. Kidney Int. 1990;38:115–123. doi: 10.1038/ki.1990.175. [DOI] [PubMed] [Google Scholar]
- 11.IJpelaar D.H., Farris A.B., Goemaere N. Fidelity and evolution of recurrent FSGS in renal allografts. J Am Soc Nephrol. 2008;19:2219–2224. doi: 10.1681/ASN.2007121365. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Nash M.A., Bakare M.A., D'Agati V. Late development of chronic renal failure in steroid-responsive nephrotic syndrome. J Pediatr. 1982;101:411–414. doi: 10.1016/s0022-3476(82)80072-3. [DOI] [PubMed] [Google Scholar]
- 13.Ijpelaar D.H., Schulz A., Koop K. Glomerular hypertrophy precedes albuminuria and segmental loss of podoplanin in podocytes in Munich-Wistar-Fromter rats. Am J Physiol Renal Physiol. 2008;294:F758–F767. doi: 10.1152/ajprenal.00457.2007. [DOI] [PubMed] [Google Scholar]
- 14.Kim B.K., Hong H.K., Kim J.H. Differential expression of nephrin in acquired human proteinuric diseases. Am J Kidney Dis. 2002;40:964–973. doi: 10.1053/ajkd.2002.36328. [DOI] [PubMed] [Google Scholar]
- 15.Kestila M., Lenkkeri U., Mannikko M. Positionally cloned gene for a novel glomerular protein–nephrin–is mutated in congenital nephrotic syndrome. Mol Cell. 1998;1:575–582. doi: 10.1016/s1097-2765(00)80057-x. [DOI] [PubMed] [Google Scholar]
- 16.Wernerson A., Duner F., Pettersson E. Altered ultrastructural distribution of nephrin in minimal change nephrotic syndrome. Nephrol Dial Transplant. 2003;18:70–76. doi: 10.1093/ndt/18.1.70. [DOI] [PubMed] [Google Scholar]
- 17.Furness P.N., Hall L.L., Shaw J.A. Glomerular expression of nephrin is decreased in acquired human nephrotic syndrome. Nephrol Dial Transplant. 1999;14:1234–1237. doi: 10.1093/ndt/14.5.1234. [DOI] [PubMed] [Google Scholar]
- 18.Patrakka J., Ruotsalainen V., Ketola I. Expression of nephrin in pediatric kidney diseases. J Am Soc Nephrol. 2001;12:289–296. doi: 10.1681/ASN.V122289. [DOI] [PubMed] [Google Scholar]
- 19.Kidney Disease: Improving Global Outcome (KDIGO) Glomerulonephritis Work Group: clinical practice guideline for glomerulonephritis. Kidney Int Suppl. 2012;2:139–274. [Google Scholar]
- 20.Rosendorff C., Lackland D.T., Allison M. Treatment of hypertension in patients with coronary artery disease: a scientific statement from the American Heart Association, American College of Cardiology, and American Society of Hypertension. J Am Soc Hypertens. 2015;9:453–498. doi: 10.1016/j.jash.2015.03.002. [DOI] [PubMed] [Google Scholar]
- 21.National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescents The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics. 2004;114(2 suppl 4th report):555–576. [PubMed] [Google Scholar]
- 22.Barisoni L., Gimpel C., Kain R. Digital pathology imaging as a novel platform for standardization and globalization of quantitative nephropathology. Clin Kidney J. 2017;10:176–187. doi: 10.1093/ckj/sfw129. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Jennette J.C., D'Agati V.D., Olson J.L. Wolters Kluwer Health; New York: 2014. Heptinstall's Pathology of the Kidney. [Google Scholar]
- 24.Turner N.N., Lameire N., Goldsmith D.J. Vol 1. 4 th ed. Oxford University Press; Oxford, UK: 2016. (Oxford Textbook of Clinical Nephrology). [Google Scholar]
- 25.D'Agati V.D., Kaskel F.J., Falk R.J. Focal segmental glomerulosclerosis. N Engl J Med. 2011;365:2398–2411. doi: 10.1056/NEJMra1106556. [DOI] [PubMed] [Google Scholar]
- 26.Pippin J.W., Brinkkoetter P.T., Cormack-Aboud F.C. Inducible rodent models of acquired podocyte diseases. Am J Physiol Renal Physiol. 2009;296:F213–F229. doi: 10.1152/ajprenal.90421.2008. [DOI] [PubMed] [Google Scholar]
- 27.Kriz W., Lemley K.V. Mechanical challenges to the glomerular filtration barrier: adaptations and pathway to sclerosis. Pediatr Nephrol. 2017;32:405–417. doi: 10.1007/s00467-016-3358-9. [DOI] [PubMed] [Google Scholar]
- 28.Doublier S., Salvidio G., Lupia E. Nephrin expression is reduced in human diabetic nephropathy: evidence for a distinct role for glycated albumin and angiotensin II. Diabetes. 2003;52:1023–1030. doi: 10.2337/diabetes.52.4.1023. [DOI] [PubMed] [Google Scholar]
- 29.Ng D.P., Tai B.C., Tan E. Nephrinuria associates with multiple renal traits in type 2 diabetes. Nephrol Dial Transplant. 2011;26:2508–2514. doi: 10.1093/ndt/gfq738. [DOI] [PubMed] [Google Scholar]
- 30.Menne J., Meier M., Park J.K. Nephrin loss in experimental diabetic nephropathy is prevented by deletion of protein kinase C alpha signaling in-vivo. Kidney Int. 2006;70:1456–1462. doi: 10.1038/sj.ki.5001830. [DOI] [PubMed] [Google Scholar]
- 31.Collino F., Bussolati B., Gerbaudo E. Preeclamptic sera induce nephrin shedding from podocytes through endothelin-1 release by endothelial glomerular cells. Am J Physiol Renal Physiol. 2008;294:F1185–F1194. doi: 10.1152/ajprenal.00442.2007. [DOI] [PubMed] [Google Scholar]
- 32.Doublier S., Musante L., Lupia E. Direct effect of plasma permeability factors from patients with idiopatic FSGS on nephrin and podocin expression in human podocytes. Int J Mol Med. 2005;16:49–58. [PubMed] [Google Scholar]
- 33.Jim B., Ghanta M., Qipo A. Dysregulated nephrin in diabetic nephropathy of type 2 diabetes: a cross sectional study. PLoS One. 2012;7:e36041. doi: 10.1371/journal.pone.0036041. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Jim B., Mehta S., Qipo A. A comparison of podocyturia, albuminuria and nephrinuria in predicting the development of preeclampsia: a prospective study. PLoS One. 2014;9:e101445. doi: 10.1371/journal.pone.0101445. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Wang G., Lai F.M., Tam L.S. Messenger RNA expression of podocyte-associated molecules in urinary sediment of patients with lupus nephritis. J Rheumatol. 2007;34:2358–2364. [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplementary Material contains Figure S1, Tables S1–S4, and Supplementary Material and Methods.