Abstract
Background
Recurrent dislocation shoulder is one of the common shoulder injuries encountered by the orthopedic surgeon in clinical practice. Bankart repair using the arthroscopic method has become one of the standard techniques in the management of recurrent dislocation shoulder. Remplissage technique can be used as adjunct to Bankart repair in certain conditions.
Method
In this case series, we have assessed the functional outcome and return to activity at midterm follow-up after arthroscopic management.
Results
51 patients with traumatic shoulder dislocation were operated using the shoulder arthroscopic technique. Rowe score improved significantly at the latest follow-up. No major complication was noticed in our case series.
Conclusion
The shoulder arthroscopy procedure requires special instrumentation and expertise. We believe that this is a less invasive and safe procedure and provides an additional tool in the management of instabilities including in cases of complex recurrent dislocation of the shoulder.
Keywords: Recurrent shoulder dislocation, Bankart lesion, Hill–Sach lesion, Remplissage
Introduction
Recurrent dislocation of the shoulder is common in the general population and is more so among athletes and military personnel due to their young age, training, and high demand of activity that is dependent on their shoulder.1 Most of the time, Bankart lesion (avulsion of the labrum from the glenoid rim) is the underlying pathology, and in some cases, ALPSA (anterior labroligamentous periosteal sleeve avulsion) lesion, Hill–Sachs lesion, capsular laxity, and SLAP lesion can also be seen. Best treatment option available for recurrent dislocation of the shoulder is repair of the underlying pathology. There are many surgical techniques that have been described for the management of this condition, which include open as well as arthroscopic repair of pathology depending upon the nature of lesions.1, 2, 3, 4, 5, 6 These techniques have used several different implants for fixation, which include staples, screws, absorbable tacks, absorbable sutures drilled transglenoid, and various types of other suture anchors.
Arthroscopic treatment of the shoulder's instability is considered to have advantages compared to the open procedure. The advantages are the following: shorter surgical time, lesser morbidity, lesser postoperative pain, lesser hospitalization time, and a reduced risk of complications. Also, few studies have reported a lesser loss of range of motion (ROM) in patients treated arthroscopically compared with those treated using an open procedure.7, 8 However, some studies have reported higher failure rate, with the arthroscopic procedure ranging from 7.5% to 23%9, 10 as compared to open surgical procedures ranging from 0% to 11%.11, 12
Shoulder arthroscopy was introduced in India and in the armed forces only in the past decade. Ours is one of the main centers in the armed forces where these kinds of surgeries have been performed for more than the past five years on a regular basis. We have evaluated the midterm results of arthroscopic management at our center in terms of the functional outcome and return to preinjury level of activity after the surgical outcome in this study.
Material and methods
All the patients operated for recurrent dislocation of the shoulder at our center between 2013 and 2015 were recruited on the basis of inclusion criteria. Records of all the patients were retrieved from the operation theater and details were obtained from the orthopedics department or hospital admission discharge summary. All the patients were evaluated at the final follow-up (Fig. 1). In this study, we have evaluated the results of arthroscopic management of recurrent dislocation of the shoulder using Bankart repair and Remplissage at midterm follow-up (minimum follow-up one year). Patients were assessed functionally using Rowe Score13 and Tegner's activity level.21
Fig. 1.

Flow chart showing details of the study.
Inclusion criteria
-
A)
Patients diagnosed clinically with traumatic recurrent (anterior) dislocation of the shoulder and operated at our center
-
B)
Age: 20–45 years
-
C)
Both genders
-
D)
Patients who are willing to participate
Exclusion criteria
-
A)
All the patients with associated Rotator cuff tears
-
B)
Patients with associated SLAP lesions
-
C)
Large bony defects of the glenoid requiring bone grafting procedure
-
D)
Atraumatic multidirectional instabilities
-
E)
Revision surgery
-
F)
Patients operated earlier for any shoulder problem
Surgical technique
All the patients were taken up for surgery under general anesthesia and placed in the lateral position. A padded traction was applied to the arm for distracting the shoulder joint. Standard posterior portal was used as viewing portal while two standard anterior portals were made. The surgery in each case started with the inspection of shoulder joint through the posterior portal especially looking for Bankart lesion and Hill–Sach lesion along with the other lesions including ALPSA (anterior labroligamentous periosteal sleeve avulsion) lesion, SLAP lesion, rotator cuff injuries, etc. (Fig. 2). In cases where Hill–Sach lesions were present, these patients were assessed for the size and engagement of the Hill–Sach lesion on the anterior edge of the glenoid cavity with the arm in external rotation at 90° of abduction. The Bankart lesions were repaired after freshening and elevating the labrum through the anterior portals (Fig. 3). Anchors of 2.8 mm (Smith and Nephew, Mumbai, USA Ltd.™) were used to repair the labrum or labroligamentous lesion to the glenoid. In the cases where engaging Hill–Sach lesions were present, infraspinatus tenodesis (Remplissage) was also done in the humeral head defect after repairing the Bankart lesion (Fig. 4). For Remplissage procedure, an accessory posterior portal was made about 2.5 cm inferior to the conventional posterior portal; debridement and freshening of the humeral defect with a bone shaver was done, followed by placement of the double-loaded, 5-mm anchor (Smith and Nephew, Mumbai, USA Ltd.™) in the defect. The final step was tenodesis of the infraspinatus tendon to the defect (Fig. 5, Fig. 6).
Fig. 2.

Arthroscopic picture showing Bankart lesion.
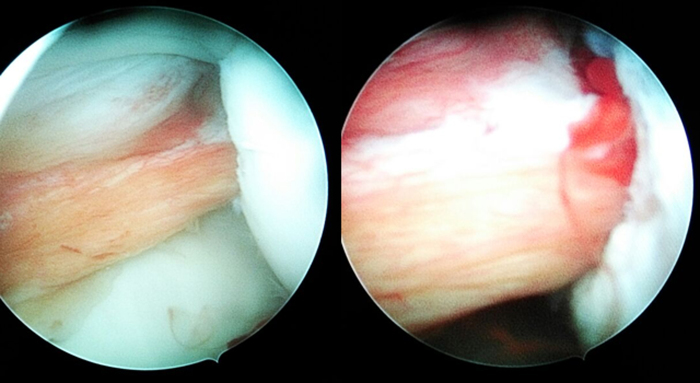
Fig. 3.
Preparation of glenoid and Repair of Bankart lesion.
Fig. 4.

Engaging Hill–Sach lesion with 5.5-mm suture anchor in place.
Fig. 5.
Remplissage procedure (Infraspinatus tenodesis).
Fig. 6.

Radiograph showing postoperative status after Bankart repair and Remplissage.
Rehabilitation
All the patients underwent a uniform exercise and rehabilitation protocol. The physiotherapy protocol consisted of keeping the shoulder in the shoulder immobilizer for four weeks. During this phase, active movements of the elbow, wrist, and fingers were allowed. Passive and passive-assisted exercises were started after four weeks as per tolerance of the patient. Gradual muscle strengthening was started after a period of two months. Return to the same level of activity was advised after six to eight months depending upon the progress of the strengthening of the shoulder.
Results
A total of 51 patients were included, with an average age of 25.82 years (range 21–45 years). There were 38 (75%) patients in the age group of 21–30 years, 11 in the age group of 31–40 years, and 2 patients were more than 40 years old. The mean follow-up of our study was 21.6 months (range 12–32 months). There were 49 males and 02 females in our study; 27 patients sustained an injury to the right shoulder and 24 patients injured their left shoulder. The dominant side was involved in 32 patients, whereas in 19 patients, the nondominant side was involved. The mode of injuries in patients at the time of the first dislocation is summarized in Table 1.
Table 1.
Mode of injury.
| Mode of injury | Number of patients |
|---|---|
| Sports (volleyball, basketball, handball, etc.) | 20 |
| Training (BPET, PPT, etc.) | 26 |
| Fall | 02 |
| Road traffic accident | 05 |
23 patients had five or fewer episodes of dislocations, 21 patients had five to ten episodes of dislocations, and 07 patients had more than 50 episodes of dislocation. 45 patients had Bankart lesions (including bony Bankart), whereas 06 patients had ALPSA (anterior labroligamentous periosteal sleeve avulsion) lesion. 13 patients had associated small-to-moderate-sized Hill–Sach lesion, whereas 07 patients had engaging Hill–Sach lesion.
Arthroscopic Bankart repair was done in majority of the patients (44/51), whereas in 07 cases, both Bankart repair and Remplissage procedures were done. The number of anchors used in patients varied from 2 to 5 depending upon the type and size of the lesions. On an average, 2.88 anchors were used per case (Table 2).
Table 2.
Type of injuries in the affected shoulder and surgery performed.
| Type of injuries | Total patients | Surgery performed | No. of anchor used |
|---|---|---|---|
| Bankart lesions (including bony Bankart lesion) | 45 | Bankart repair | 2–3 |
| ALPSA (anterior labroligamentous periosteal sleeve avulsion) lesion | 06 | Bankart repair/capsule–labral complex repair | 2–3 |
| Small-to-moderate-sized Hill–Sach lesion | 13 | Bankart repair/capsule–labral complex repair | 2–3 |
| Engaging Hill–Sach lesion | 07 | Bankart repair and Remplissage | 3–5 |
Rowe score has improved significantly at the time of final follow-up as compared to preoperative score in our case series. Mean Rowe Score at the final follow-up was 90.16 (Range 35–100), whereas the mean preoperative score was 24.51 (Range 15–35). 45 patients had good-to-excellent results, 5 patients had fair results, and one patient had a poor result on the basis of Rowe Score. The mean preinjury Tegner's activity level was 6.25 ± 2.25, whereas the mean Tegner's activity level at the time of final follow-up was 6.1 ± 1.7. Return to the same level of Tegner's activity level was seen in nearly 85% of the patients.
There was 01 case of redislocation/failure in our series, which occurred at 14 months after the surgery, whereas one patient had traction neuropraxia, who recovered spontaneously. One patient had persistent posterior shoulder pain. One patient had significant global loss of movements (>25%) at the time of final follow-up.
Discussion
The aim of our study was to analyze the functional results of arthroscopic management of recurrent dislocation of the shoulder using Bankart repair and Remplissage at midterm follow-up. The mean age of patients in our case series was 25.82 years, with nearly 75% of patients under 30 years of age. Furthermore, in our case series, more than 95% of the patients were male, which further proves the fact that traumatic recurrent dislocation is more common in younger, physically active persons who are involved in professions having a high demand for physical activity.
Bankart lesion is the most common lesion responsible for recurrent traumatic anterior dislocation, which requires surgical intervention. In our case series, 88% of the patients had Bankart lesion, whereas the rest 06 (12%) patients had ALPSA (anterior labroligamentous periosteal sleeve avulsion) lesion. Various studies have also reported the rate of Bankart lesion between 70 and 90%.13, 17
Hill–Sach lesions were seen in 20 patients (39%); out of these 20 patients, 13 had small-to-moderate-sized lesion, whereas 07 had engaging Hill–Sach lesions. Several studies report the rate of Hill–Sach Lesion between 35 and 75% in patients with recurrent dislocation of the shoulder.16, 17, 18
The mean preoperative Rowe score13 was 24.51 (Range 15–35), which improved to 90.16 (Range 35–100) at the time of final follow-up. 88% of the patients (45) had good-to-excellent results, five had fair results, and one patient had a poor result on the basis of Rowe Score (Fig. 8). In the majority of the patients, we achieved good functional range of motion at the time of final follow-up, which is essential for professionals having high demand for physical activity because of nature of the job in which they are involved (Fig. 7). Various other studies have reported a lesser loss of movement using the arthroscopic technique as compared to open techniques.14, 15 In our series, the mean loss of external rotation as compared to opposite shoulder was minimal (mean external rotation loss 5°). The loss of external rotation was higher in the patients operated with Remplissage (mean external rotation loss 9°). However, the patients operated with Remplissage procedure were very few. This is one of the limitations of our study. A larger case series is required to compare the functional range of movements after combining Bankart repair and Remplissage procedures. The loss of movements after Remplissage procedure is still debatable, as various studies mention different kinds of results after this procedure.19, 20
Fig. 8.

Preop and final outcome on the basis of Rowe score.
Fig. 7.
Clinical photographs at final follow-up with good functional results.
Return to the same level of activity was assessed using Tegner's activity scale.21 In our series, 85% of the patients were able to return to preinjury activity level at the time of final follow-up.
In our case series, one patient had redislocation at 14-month follow-up. However, this patient had a fall under the influence of alcohol, which could have caused a possible significant reinjury. One patient had traction neuropraxia of axillary nerve, which resolved spontaneously, one patient had limitation of shoulder movements with significant loss of abduction and external rotation, and one patient in whom Remplissage was done had persistent posterior shoulder pain at the time of final follow-up. The failure rate (2%) in our series is consistent with newer case studies.15, 22
One of the main limitations of our case series is that we have not assessed the time taken for recovery of movements and muscle strength of the shoulder joint because of the retrospective nature of the study.
In conclusion, this study shows that arthroscopic management of traumatic recurrent dislocation of the shoulder using Bankart repair is a safe, less invasive, and successful procedure. Furthermore, in cases where engaging Hill–Sach is present, Bankart repair with Remplissage can be used as an alternative procedure to open bony procedures to provide stability to the joint in professionals having high demand for physical activity, where stability with motion is paramount.
Conflicts of interest
The authors have none to declare.
References
- 1.Bottoni C.R., Wilckens J.H., DeBerardino T.M. A prospective, randomized evaluation of arthroscopic stabilization versus nonoperative treatment in patients with acute, traumatic, first-time shoulder dislocations. Am J Sports Med. 2002;30(July (4)):576–580. doi: 10.1177/03635465020300041801. [DOI] [PubMed] [Google Scholar]
- 2.Kurokawa D., Yamamoto N., Nagamoto H. The prevalence of a large Hill–Sachs lesion that needs to be treated. J Shoulder Elbow Surg. 2013;22(September (9)):1285–1289. doi: 10.1016/j.jse.2012.12.033. [DOI] [PubMed] [Google Scholar]
- 3.Harris J.D., Gupta A.K., Mall N.A. Long-term outcomes after Bankart shoulder stabilization. Arthroscopy. 2013;29(May (5)):920–933. doi: 10.1016/j.arthro.2012.11.010. [DOI] [PubMed] [Google Scholar]
- 4.Boileau P., O'Shea K., Vargas P., Pinedo M., Old J., Zumstein M. Anatomical and functional results after arthroscopic Hill–Sachs remplissage. J Bone Joint Surg Am. 2012;94(April (7)):618–626. doi: 10.2106/JBJS.K.00101. [DOI] [PubMed] [Google Scholar]
- 5.Iwaso H., Uchiyama E., Sakakibara S., Fukui N. Modified double-row technique for arthroscopic Bankart repair: surgical technique and preliminary results. Acta Orthop Belg. 2011;77(April (2)):252–257. [PubMed] [Google Scholar]
- 6.Castagna A., Garofalo R., Melito G., Markopoulos N., De Giorgi S. The role of arthroscopy in the revision of failed Latarjet procedures. Musculoskelet Surg. 2010;94(May (1)):47–55. doi: 10.1007/s12306-010-0060-0. [DOI] [PubMed] [Google Scholar]
- 7.Arciero R.A., Taylor D.C., Snyder R.J., Uhorchak J.M. Arthroscopic bioabsorbable tack stabilization of initial anterior shoulder dislocations: a preliminary report. Arthroscopy. 1995;11(August (4)):410–417. doi: 10.1016/0749-8063(95)90192-2. [DOI] [PubMed] [Google Scholar]
- 8.Bacilla P., Field L., Savoie F. Arthroscopic Bankart repair in a high demand patient population. Arthroscopy. 1997;13(February (1)):51–60. doi: 10.1016/s0749-8063(97)90209-7. [DOI] [PubMed] [Google Scholar]
- 9.Gartsman G.M., Roddey T.S., Hammerman S.M. Arthroscopic treatment of anterior–inferior glenohumeral instability. J Bone Joint Surg Am. 2000;82(July (7)):991–1091. doi: 10.2106/00004623-200007000-00011. [DOI] [PubMed] [Google Scholar]
- 10.Sperber A., Hamberg P., Karlsson J., Swärd L., Wredmark T. Comparison of an arthroscopic and an open procedure for posttraumatic instability of the shoulder: a prospective, randomized multicenter study. J Shoulder Elbow Surg. 2001;10(April (2)):105–108. doi: 10.1067/mse.2001.112019. [DOI] [PubMed] [Google Scholar]
- 11.Cole B.J., L’insalata J., Irrgang J., Warner J.J. Comparison of arthroscopic and open anterior shoulder stabilization. J Bone Joint Surg Am. 2000;82(August (8)):1108. doi: 10.2106/00004623-200008000-00007. [DOI] [PubMed] [Google Scholar]
- 12.Hoffmann F., Reif G. Arthroscopic shoulder stabilization using Mitek anchors. Knee Surg Sports Traumatol Arthrosc. 1995;3:50–54. doi: 10.1007/BF01553526. [DOI] [PubMed] [Google Scholar]
- 13.Rowe C.R., Patel D. The Bankart procedure: a long-term end-result study. J Bone Joint Surg Am. 1978;60:1–16. [PubMed] [Google Scholar]
- 14.Gartsman G.M., Roddey T.S., Hammerman S.M. Arthroscopic treatment of anterior-inferior glenohumeral instability. Two to five-year follow-up. J Bone Joint Surg Am. 2000;82(July):991–1003. doi: 10.2106/00004623-200007000-00011. [DOI] [PubMed] [Google Scholar]
- 15.Erkoçak O.F., Yel M. The functional results of arthroscopic bankart repair with knotless anchors for anterior glenohumeral instability. Eur J Gen Med. 2010;7(2):179–186. [Google Scholar]
- 16.Carrazzone O.L., Tamaoki M.J., Ambra L.F., Neto N.A., Matsumoto M.H., Belloti J.C. prevalence Of lesions associated With traumatic recurrent shoulder dislocation. Rev Bras Ortop (Engl Ed) 2011;46(June (3)):281–287. doi: 10.1016/S2255-4971(15)30196-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Di Giacomo G., Itoi E., Burkhart S.S. Evolving concept of bipolar bone loss and the Hill–Sachs lesion: from “engaging/non-engaging” lesion to “on-track/off-track” lesion. Arthroscopy. 2014;30(January (1)):90–98. doi: 10.1016/j.arthro.2013.10.004. [DOI] [PubMed] [Google Scholar]
- 18.Horst K., Von Harten R., Weber C. Assessment of coincidence and defect sizes in Bankart and Hill–Sachs lesions after anterior shoulder dislocation: a radiological study. Br J Radiol. 2014;87(January (1034)):20130673. doi: 10.1259/bjr.20130673. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Koo S.S., Burkhart S.S., Ochoa E. Arthroscopic double-pulley remplissage technique for engaging Hill–Sachs lesions in anterior shoulder instability repairs. Arthroscopy. 2009;25(11):1343–1348. doi: 10.1016/j.arthro.2009.06.011. [DOI] [PubMed] [Google Scholar]
- 20.Deutsch A.A., Kroll D.G. Decreased range of motion following arthroscopic remplissage. Orthopedics. 2008;31(5):492. doi: 10.3928/01477447-20080501-07. [DOI] [PubMed] [Google Scholar]
- 21.Tegner Y., Lysholm J. Rating systems in the evaluation of knee ligament injuries. Clin Orthop. 1985;198(September):42–49. [PubMed] [Google Scholar]
- 22.Balg F., Boileau P. The instability severity index score. Bone Joint J. 2007;89(November (11)):1470–1477. doi: 10.1302/0301-620X.89B11.18962. [DOI] [PubMed] [Google Scholar]