Abstract
Historically, connexin hemichannels have been considered as structural precursors of gap junctions. However, accumulating evidence points to independent roles for connexin hemichannels in cellular signaling by connecting the intracellular compartment with the extracellular environment. Unlike gap junctions, connexin hemichannels seem to be mainly activated in pathological processes. The present study was set up to test the potential involvement of hemichannels composed of connexin32 and connexin43 in acute hepatotoxicity induced by acetaminophen. Prior to this, in vitro testing was performed to confirm the specificity and efficiency of TAT-Gap24 and TAT-Gap19 in blocking connexin32 and connexin43 hemichannels, respectively. Subsequently, mice were overdosed with acetaminophen followed by treatment with TAT-Gap24 or TAT-Gap19 or a combination of both after 1.5 hour. Sampling was performed 3, 6, 24 and 48 hours following acetaminophen administration. Evaluation of the effects of connexin hemichannel inhibition was based on a series of clinically relevant read-outs, measurement of inflammatory cytokines and oxidative stress. Subsequent treatment of acetaminophen-overdosed mice with TAT-Gap19 only marginally affected liver injury. In contrast, a significant reduction in serum alanine aminotransferase activity was found upon administration of TAT-Gap24 to intoxicated animals. Furthermore, co-treatment of acetaminophen-overdosed mice with both peptides revealed an additive effect as even lower serum alanine aminotransferase activity was observed. Blocking of connexin32 or connexin43 hemichannels individually was found to decrease serum quantities of pro-inflammatory cytokines, while no effects were observed on the occurrence of hepatic oxidative stress. This study shows for the first time a role for connexin hemichannels in acetaminophen-induced acute liver failure.
Keywords: connexin, hemichannel, gap junction, hepatotoxicity, acetaminophen, inflammation
1. Introduction
Drug-induced liver injury is the leading cause of acute liver failure in Western countries. A majority of the clinical cases of acute liver failure results from either accidental or intentional overdose of acetaminophen (APAP), a readily available analgesic and antipyretic drug (Ichai and Samuel, 2011; Lee, 2008). In case of an APAP overdose, a substantial amount of APAP is metabolized by cytochrome P450 2E1, yielding the reactive metabolite N-acetyl-p-benzoquinone imine (NAPQI), which depletes the glutathione (GSH) pool and that gives rise to deleterious APAP-protein adducts (Dahlin et al., 1984). As a consequence, impaired mitochondrial respiration and oxidative stress are triggered accompanied by the onset of massive hepatocyte cell death as well as the induction of an inflammatory response (Blazka et al., 1995; Cover et al., 2006; Jaeschke and McGill, 2015).
As holds for most cellular processes, cell death and inflammation are driven by the interaction between 3 communication mechanisms, namely extracellular, intracellular and intercellular signaling. The latter can be mediated by gap junctions, a group of cell-to-cell contacts composed of 2 hemichannels of adjacent cells, which in turn are built up by 6 connexin (Cx) proteins (Maes et al., 2014; Vinken et al., 2008). At present, 21 connexin proteins have been identified in humans, while in rodents 20 connexin proteins have been characterized. They all share a similar structure consisting of 4 membrane-spanning domains, 2 extracellular loops, a cytoplasmic loop, cytosolic N-terminal and C-terminal regions (Oshima, 2014). Connexins are named after their molecular weight. In liver, hepatocytes predominantly express Cx32 and to a lesser extent Cx26, while non-parenchymal cells, including Kupffer cells and stellate cells, mainly harbor Cx43 (Maes et al., 2015a). Nonetheless, hepatic connexin expression patterns undergo drastic changes upon chronic liver disease, such as in liver fibrosis and cirrhosis as well as during acute liver injury (Maes et al., 2015b; Vinken, 2012). In this respect, our and other groups previously reported a switch in RNA and protein production from Cx32 and Cx26 to Cx43 upon APAP intoxication in rodents (Maes et al., 2016a; Naiki-Ito et al., 2010). This upregulation of Cx43 is due to recruitment of Cx43-expressing inflammatory cells, but equally reflects de novo production of Cx43 by hepatocytes (Maes et al., 2016a). In fact, although being critical mediators of liver homeostasis (Maes et al., 2015a), connexins and their channels are also frequently involved in liver toxicity (Maes et al., 2015b). A number of studies have shown a role for Cx32-based gap junctions in APAP-triggered hepatotoxicity using genetically modified animals, albeit with contradicting outcomes (Igarashi et al., 2014; Maes et al., 2016b; Naiki-Ito et al., 2010; Park et al., 2013). In a recent study, our group questioned the suitability of genetically deficient rodents for investigating the involvement of Cx32 in APAP-induced hepatotoxicity (Maes et al., 2016b). A possible alternative is the use of inhibitors of Cx32-based signaling. In this regard, a non-specific inhibitor of gap junctional communication, 2-aminoethoxy-diphenyl-borate (2-APB), was reported to protect against liver failure and death in mice when co-administered with APAP (Patel et al., 2012). However, a follow-up study demonstrated that this protection was only minor or completely lost when 2-APB was administered 1.5 hour or 4-6 hours, respectively, after APAP. In addition, part of the protection could be attributed to solvent effects and inhibition of the metabolic activation of APAP as well as to inhibition of the c-jun-N-terminal kinase signaling pathway (Du et al., 2013). On the other hand, our group demonstrated that APAP-related liver injury is increased in Cx43+/- mice (Maes et al., 2016a). In line with this, inhibition of Cx43 after bile duct ligation in mice produced detrimental effects with markedly greater hepatocellular necrosis (Balasubramaniyan et al., 2013). This discrepancy between outcomes after APAP-induced toxicity of mice deficient in Cx32 or Cx43 may be due, at least in part, to opposite actions of gap junctions and connexin hemichannels. The latter not only serve as structural precursors of gap junctions, but also establish as pathway for cellular signaling on their own by connecting the cytosol of individual cells with the extracellular environment. Strikingly, while gap junctions are mainly associated with physiological functions, connexin hemichannels seem preferentially active in pathological conditions (Chandrasekhar and Bera, 2012; Decrock et al., 2009b; Maes et al., 2015b). Research in this area is largely impeded by the lack of inhibitors able to distinguish between both channel types (Bodendiek and Raman, 2010; Evans and Leybaert, 2007). An exception lies with a number of peptides, which reproduce specific amino acid modules of selected connexin proteins. In the present study, Gap24 and Gap19, both linked to a transactivator of transcription (TAT) sequence, were tested for their potential to specifically inhibit Cx32 and Cx43 hemichannels, respectively, in cultures of primary rat hepatocytes, and to reduce the clinical manifestation of hepatotoxicity in a mouse model of APAP-induced acute liver failure.
2. Materials and methods
2.1. Chemicals and reagents
TAT-Gap24 (YGRKKRRQRRRGHGDPLHLEEVKC) and TAT-Gap19 (YGRKKRRQRRRKQIEIKKFK) were synthesized by Thermo Fisher (Germany) with a purity of at least 90%. All other chemicals were commercially available products of analytical grade and were supplied by Sigma (USA) unless specified otherwise.
2.2. Rat hepatocyte isolation and cultivation
Male outbred Sprague-Dawley rats (Charles River Laboratories, France) weighing 250-275 g were kept under controlled environmental conditions with food and water ad libitum. Hepatocytes were isolated by use of a 2-step collagenase method and cell viability was assessed by trypan blue exclusion (Papeleu et al., 2006). Viable (≥ 85 %) hepatocytes were seeded on a plastic surface at a density of 0.57 x 105 cells/cm2 in William’s medium E (Thermo Fisher, USA) supplemented with 7 ng/ml glucagon, 292 mg/ml L-glutamine, antibiotics (7.33 IU/ml sodium benzyl penicillin, 50 μg/ml kanamycin monosulphate, 10 μg/ml sodium ampicillin, 50 μg/ml streptomycin sulphate) and 10 % v/v fetal bovine serum (Thermo Fisher, USA). Cell culture plates were placed in an incubator (37 °C, 5 % CO2) and after 4 hours, cell culture media were removed and replaced by serum-free medium supplemented with 25 μg/ml hydrocortisone sodium hemisuccinate and 0.5 μg/ml insulin. Hepatocyte isolation and cultivation procedures for the housing of rats as well as for the isolation and cultivation of hepatocytes were approved by the local Ethical Committee of the Vrije Universiteit Brussel, Belgium (project number 12-210-3).
2.3. Measurement of extracellular adenosine triphosphate release
Connexin hemichannel activity was tested by measuring extracellular release of adenosine triphosphate (ATP) using a commercial luciferin/luciferase assay kit as previously described (Vinken et al., 2010). Briefly, 24 hours after cell seeding, cultured rat hepatocytes were exposed during 30 minutes to 20 µM TAT-Gap24, 20 µM TAT-Gap19, 50 µM carbenoxolone (CBX) or solvent control. Subsequently, cultured hepatocytes were washed with Hank’s balanced salt solution (HBSS) buffered with 25 mM Hepes (Thermo Scientific, USA), considered as the baseline condition, and divalent-free buffer in order to trigger connexin hemichannel opening. After 2.5 minutes incubation at room temperature, ATP assay mix was added and luminescence was measured spectrophotometrically. Results were expressed as percentage of ATP released in divalent-free medium after 30 minutes exposure to the solvent control.
2.4. Fluorescence recovery after photobleaching
Gap junction activity was tested by fluorescence recovery after photobleaching (FRAP) analysis as described previously (Vinken et al., 2010). Briefly, 24 hours after cell seeding, cultured hepatocytes were exposed during 24 hours to 20 µM TAT-Gap24, 20 µM TAT-Gap19, 50 µM CBX or solvent control. Thereafter, cells were loaded with 10 µM calcein-acetoxymethyl ester in HBSS-Hepes for 40 minutes at room temperature in the absence of light. The tracer solution was replaced by HBSS-Hepes and cultured cells were maintained for 30 minutes in the dark at room temperature. Fluorescence within a single cell was photobleached by 1 second spot exposure to 488 nm Argon laser light, and dye influx from neighboring cells was recorded over the next 6 minutes with a water immersion objective (Nikon Eclipse Ti, Japan). Fluorescence in the bleached cell was expressed as the percentage recovery relative to the prebleach level. At least 4 cells per culture dish were examined.
2.5. Administration of APAP and connexin hemichannel inhibitors to mice
For in vivo testing purposes, 8-week to 10-week old male C57BL/6 mice (Jackson Laboratories, USA) were used and housed in the animal facility of the Department of Pathology at the School of Veterinary Medicine and Animal Science of the University of São Paulo, Brazil. The animals were kept in a room with ventilation (16-18 air changes/hour), relative humidity (45-65 %), controlled temperature (20-24 °C) and light/dark cycle 12:12, and were given water and balanced diet (NUVILAB-CR1, Nuvital Nutrientes LTDA, Brazil) ad libitum. Mice were starved 15-16 hours prior to APAP administration. APAP was dissolved in saline (0.9 % NaCl), slightly heated and injected (30-37 °C) intraperitoneally at 300 mg/kg body weight, after which animals regained free access to food (Maes et al., 2016c). 1.5 hour after APAP injection, mice were additionally administered either 10 mg/kg TAT-Gap19, 10 mg/kg TAT-Gap24 or a combination of both dissolved in saline, or only saline through retro-orbital injection of volumes not exceeding 150 µl. The conditions for administration of both compounds were optimized during preliminary testing. No overt signs of organ toxicity were observed upon gross necropsy and histopathological examination (data not shown). Mice were euthanized at the start of the experiment and 3, 6, 24 and 48 hours after APAP injection by exsanguination during sampling under isoflurane-induced anesthesia. Blood, collected by cardiac puncture, was drawn into a heparinized syringe and centrifuged for 10 minutes at 1503xg, and serum was stored at -20 °C. Livers were excised and fragments were fixed in 10 % phosphate-buffered formalin or snap-frozen in liquid nitrogen with storage at -80 °C. This study has been approved by the Committee on Bio-ethics of the School of Veterinary Medicine and Animal Science of the University of São Paulo, Brazil (protocol number 9999100314), and all animals received humane care according to the criteria outlined in the “Guide for the Care and Use of Laboratory Animals”.
2.6. Histopathological liver examination
For microscopic evaluation, formalin-fixed liver fragments were embedded in paraffin, and 5 µm sections were cut and stained with hematoxylin and eosin for blinded evaluation of liver damage as described elsewhere (Gujral et al., 2002). The percentage of necrosis was estimated by evaluating the number of microscopic fields with necrosis compared to the cross-sectional areas over the entire section. Pictures were taken with an inverted Axio Vert A1 microscope (Carl Zeiss, Germany).
2.7. Analysis of serum alanine aminotransferase
Alanine aminotransferase (ALT) activity was measured with an automated spectrophotometric Labmax 240 analyzer (Labtest Diagnostica, Brazil) after appropriate dilution of the collected serum samples. Values were expressed in IU/L.
2.8. Analysis of hepatic protein adducts
APAP-protein adducts were measured by high-pressure liquid chromatography with electrochemical detection as described elsewhere (Muldrew et al., 2002) with some modifications (McGill et al., 2013). Briefly, low molecular weight compounds were removed via Bio-spin 6 columns (Bio-Rad, USA) and the protein fraction was subsequently digested with proteases to liberate APAP-cysteine conjugates. The protein-derived APAP-cysteine conjugates were quantified and normalized to protein concentration in the original samples.
2.9. Analysis of serum cytokines
Liver tissue was homogenized in Complete Lysis-M buffer with protease inhibitors (Roche, Germany). Homogenates were centrifuged at 14000xg for 15 minutes at 4 °C and protein concentrations in supernatants were determined according to the Bradford procedure (Bradford, 1976) using a commercial kit (Bio-Rad, USA) with bovine serum albumin as a standard. Enzyme-linked immunosorbent assay (ELISA) kits were used to measure levels of mouse interleukin (IL)-1β, IL-6, IL-10 and tumor necrosis factor (TNF)α (BD Biosciences, USA) as previously described (Maes et al., 2016a; Maes et al., 2016b).
2.10. Hepatic glutathione and glutathione disulfide analysis
GSH and glutathione disulfide (GSSG) levels in liver tissue were measured using a modified Tietze assay (Jaeschke and Mitchell, 1990). Briefly, frozen liver tissue was homogenized in 3 % sulfosalicylic acid/ethylendiaminetetra-acetic acid and centrifuged at 18000xg for 5 minutes at 4 °C to remove precipitated proteins. After further dilution with potassium phosphate buffer, samples were assayed with a cycling reaction utilizing GSH reductase and dithionitrobenzoic acid. Measurement of GSSG was performed using the same method after trapping GSH with N-ethylmaleimide and removal by solid phase extraction (Jaeschke and Mitchell, 1990). GSSG content was expressed as GSH equivalents.
2.11. Statistical analysis
All data were expressed as mean ± standard error of the mean (SEM). The number of repeats (n) for each analysis varied per experiment and/or assay are specified in the figure legends. Results were statistically processed by 1-way analysis of variance (ANOVA) followed by post hoc Bonferroni tests using GraphPad Prism6 software with probability (p) values of less than or equal to 0.05 considered as significant.
3. Results
3.1. TAT-Gap24 and TAT-Gap19 block extracellular release of ATP
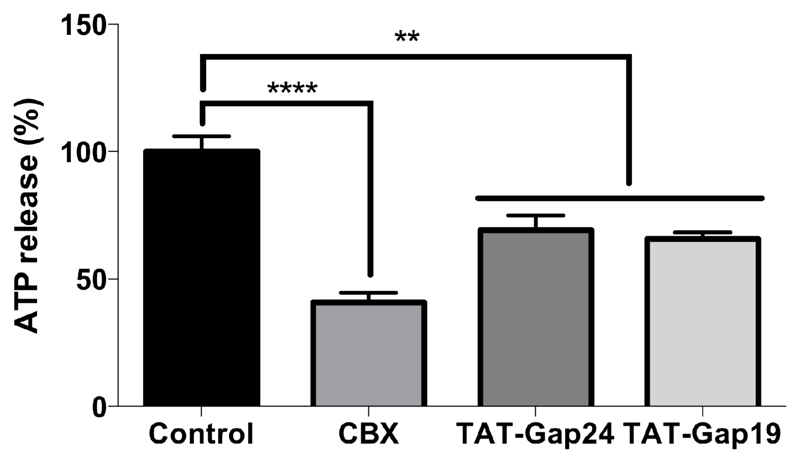
Exposure of cells to lowered extracellular divalent ion conditions is a well-known procedure to potentiate or trigger the opening of connexin hemichannels (Stout et al., 2002; Ye et al., 2003). Therefore, monitoring extracellular ATP release during the exposure of cells to divalent ion-free medium is indicative for connexin hemichannel activity. As a positive control in these experiments, CBX was used, which is a general inhibitor of connexin-based channels. CBX suppresses gap junctional and connexin hemichannel signaling at concentrations of 3 to 200 µM (Davidson et al., 1986; Goldberg et al., 1996; Wang et al., 2013a). In the present study, 30 minutes exposure of cultured primary rat hepatocytes to 50 µM CBX reduced (p < 0.0001) extracellular ATP release to 40.85 ± 17.03 %. Exposure of the cells for 30 minutes to 20 µM TAT-Gap24 or 20 µM TAT-Gap19 significantly decreased (p < 0.01) ATP release triggered by divalent ion-free medium to 69.23 ± 9.97 % or 65.79 ± 4.44 %, respectively (Fig. 1.). These results thus demonstrate that TAT-Gap24 and TAT-Gap19 efficiently inhibit connexin hemichannels in hepatocytes in the concentration range that was previously used in other cell types (De Vuyst et al., 2006; Wang et al., 2013b).
Figure 1. TAT-Gap24 and TAT-Gap19 block extracellular release of ATP.
Primary rat hepatocytes were isolated and cultivated as specified in “Materials and Methods”. 24 hours after cell seeding, cultured hepatocytes were exposed during 30 minutes to 20 µM TAT-Gap24, 20 µM TAT-Gap19, 50 µM carbenoxolone (CBX) or solvent control. Thereafter, the cells were exposed to HBSS-Hepes, considered as the baseline condition, and divalent-free buffer. After 2.5 minutes incubation at room temperature, ATP assay mix was added and luminescence was measured spectrophotometrically. ATP release in the divalent-free buffer were plotted and expressed as percentage of ATP release triggered by divalent-free medium. At least 6 wells per experiment were examined, with a total of 5 experiments (i.e. hepatocytes isolated from 5 different rats). Data are expressed as means ± SEM, with **p < 0.01 and ****p < 0.0001 compared to ATP release triggered by divalent-free medium.
3.2. TAT-Gap24 and TAT-Gap19 do not affect gap junction activity
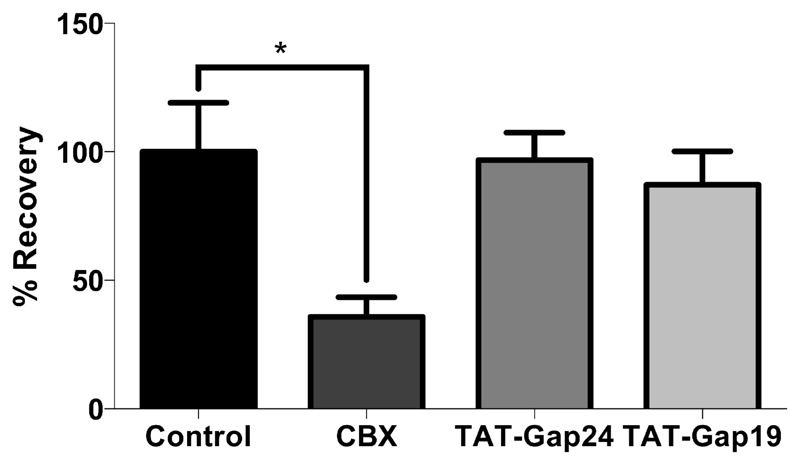
In order to confirm the specificity of TAT-Gap24 and TAT-Gap19, especially with respect to their actions on channels built up by the same proteins as their target channels, their effects on gap junctions were monitored in cultures of primary hepatocytes using FRAP analysis. Similar to the ATP release assay, CBX was used as a positive control in the FRAP experiments. 24 hours exposure of the cells to 50 µM CBX indeed decreased (p < 0.05) the fluorescence recovery signal, representative for the gap junction activity, to 35.86 ± 17.03 % compared to solvent control. Exposure of the cultured hepatocytes to 20 µM TAT-Gap24 or 20 µM TAT-Gap19 for 1 day resulted in fluorescence recovery of 96.77 ± 10.61 % and 87.14 ± 29.07 %, respectively (Fig. 2.). These results further substantiate the target specificity of TAT-Gap24 and TAT-Gap19 when applied to hepatocytes. Their specificity towards hemichannels can be partly attributed to the intracellular location of the target of TAT-Gap19 and TAT-Gap24. Indeed, other connexin peptides mimicking sequences in the extracellular loop region inhibit hemichannel activity within minutes, but also prevent the docking of 2 facing hemichannels and thus affect gap junctional communication when applied for periods of several hours (Decrock et al., 2009a; Desplantez et al., 2012; Evans and Leybaert, 2007).
Figure 2. TAT-Gap24 and TAT-Gap19 do not affect gap junction activity.
Primary rat hepatocytes were isolated and cultivated as specified in “Materials and Methods”. 24 hours after cell seeding, cultured hepatocytes were exposed during 24 hours to 20 µM TAT-Gap24, 20 µM TAT-Gap19, 50 µM carbenoxolone (CBX) or solvent control. Subsequently, cells were subjected to FRAP analysis. After loading with 10 µM calcein-acetoxymethyl ester, fluorescence within a single cell was photobleached by 1 second spot exposure to 488 nm Argon laser. The dye influx from neighboring cells was recorded over the next 6 minutes. Fluorescence in the bleached cell was expressed as the percentage recovery relative to the prebleach level. At least 5 wells per cell culture dish were examined in each experiment, with a total of 5 experiments (i.e. hepatocytes isolated from 5 different rats). Data are expressed as means ± SEM, with *p < 0.05 compared to recovery in the solvent control.
3.3. Connexin hemichannel inhibition diminishes liver damage in APAP-induced hepatotoxicity
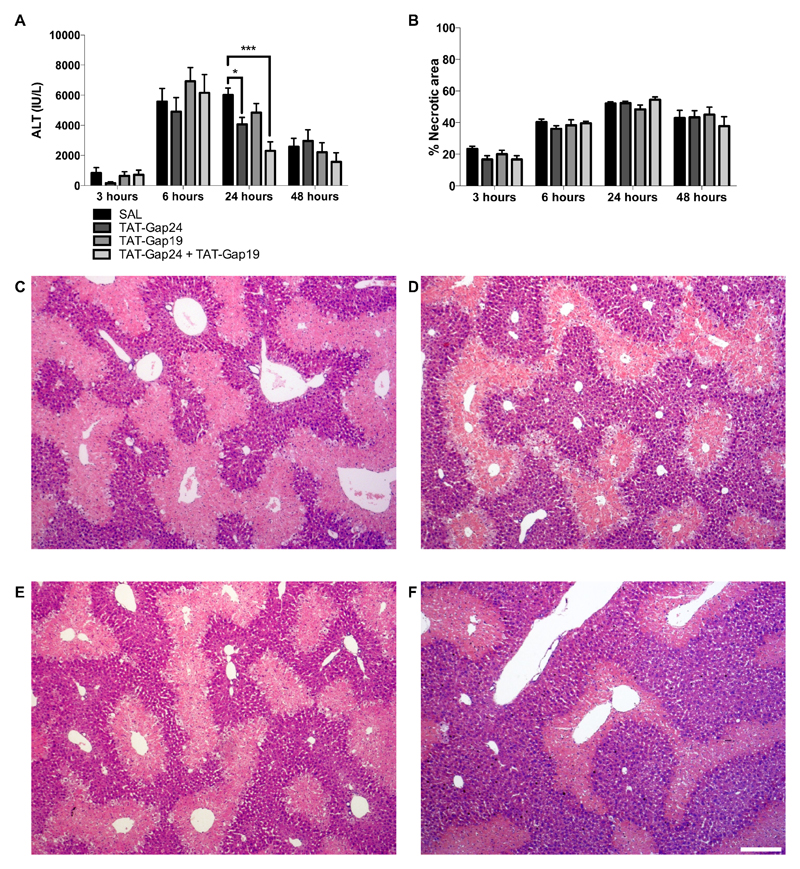
A single dose of 300 mg/kg APAP is well known to cause severe hepatocellular injury, which can be detected by massive necrosis and extensive increased serum ALT activity (Jaeschke et al., 2012b; Maes et al., 2016c). In this study, liver damage became manifested about 3 hours after APAP injection, with culminating serum ALT activity up to 24 hours (Fig. 3A.). To evaluate the effect of connexin hemichannel inhibition in vivo in this model of acute hepatotoxicity, 10 mg/kg of TAT-Gap24 and/or 10 mg/kg TAT-Gap19 were administered 1.5 hour after the APAP overdosing. These doses were extrapolated from the in vitro testing outcome and correspond to a concentration of 20 µM, thereby assuming distribution in the blood volume that is approximately 8 % of the body weight (Wang et al., 2013b). Upon treatment of APAP-overdosed mice with TAT-Gap24, TAT-Gap19 or a combination of both compounds, modest yet non-significant differences in the necrotic areas were observed after APAP administration (Fig. 3B-F.). Blockage of Cx32 hemichannels attenuated serum ALT activity after 24 hours (p < 0.05), while TAT-Gap19 only slightly decreased ALT values after 24 and 48 hours. Simultaneous treatment of APAP-overdosed mice with TAT-Gap24 and TAT-Gap19 revealed an additive effect by drastically lowering ALT serum activity (p < 0.001) after 24 hours (Fig. 3A.).
Figure 3. Connexin hemichannel inhibition diminishes liver cell damage in APAP-induced hepatotoxicity.
Mice (n = 5-20 per group and per time point) were injected 300 mg/kg APAP followed by administration of 10 mg/kg TAT-Gap24, 10 mg/kg TAT-Gap19, a combination of both or saline (SAL) 1.5 hour later. Sampling was performed 3, 6, 24 and 48 hours after APAP overdosing. (A) Serum levels of ALT were measured with an automated spectrophotometer and expressed as IU/L. (B) Liver sections were examined microscopically with quantification of the necrotic areas around the central veins. Data are expressed as means ± SEM, with *p < 0.05 and ***p < 0.001 compared to APAP followed by SAL administration. Microscopic pictures of the liver tissue 24 hours after APAP administration followed by (C) SAL, (D) 10 mg/kg TAT-Gap24, (E) 10 mg/kg TAT-Gap19 or (F) a combination of 10 mg/kg TAT-Gap24 and TAT-Gap19. The white scale bar represents 200 µm.
3.4. Connexin hemichannel inhibition does not affect hepatic protein adduct formation in APAP-induced hepatotoxicity
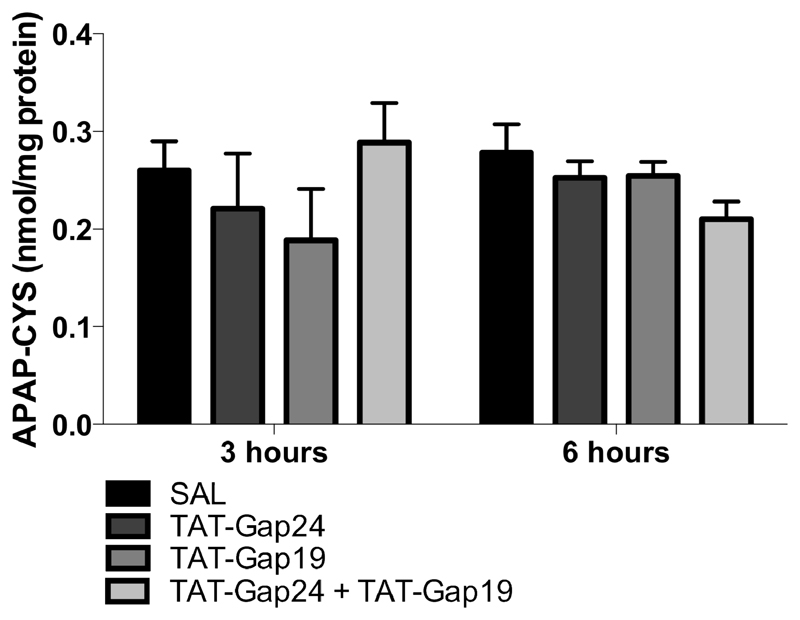
The mechanism of toxicity of APAP, and thus the mouse model as such, relies on the formation of the deleterious reactive metabolite NAPQI. In case of APAP overdosing, NAPQI reacts with protein sulfhydryl groups, which leads to the formation of noxious liver protein adducts (Mitchell et al., 1973). To confirm that the observed diminished liver damage after treatment with TAT-Gap24 and/or TAT-Gap19 occurs independently of NAPQI formation, APAP-protein adducts were measured 3 and 6 hours after APAP administration. APAP-protein adducts were detectable in all mice with no significant differences between the different experimental groups (Fig. 4.). These data show that TAT-Gap24 and TAT-Gap19 do not influence hepatic APAP adduct formation.
Figure 4. Connexin hemichannel inhibition does not affect hepatic protein adduct formation in APAP-induced hepatotoxicity.
Mice (n = 6-10 per group and per time point) were injected 300 mg/kg APAP followed by administration of 10 mg/kg TAT-Gap24, 10 mg/kg TAT-Gap19, a combination of both or saline (SAL) 1.5 hour later. Sampling was performed 3 and 6 hours after APAP overdosing. The generation of reactive metabolite results in the formation of APAP-cysteine (APAP-CYS) protein adducts, which were quantified by high-pressure liquid chromatography with electrochemical detection using total liver homogenate. Data are expressed as means ± SEM. No significant differences were found between the different experimental groups.
3.5. Connexin hemichannel inhibition differentially affects serum cytokine levels in APAP-induced hepatotoxicity
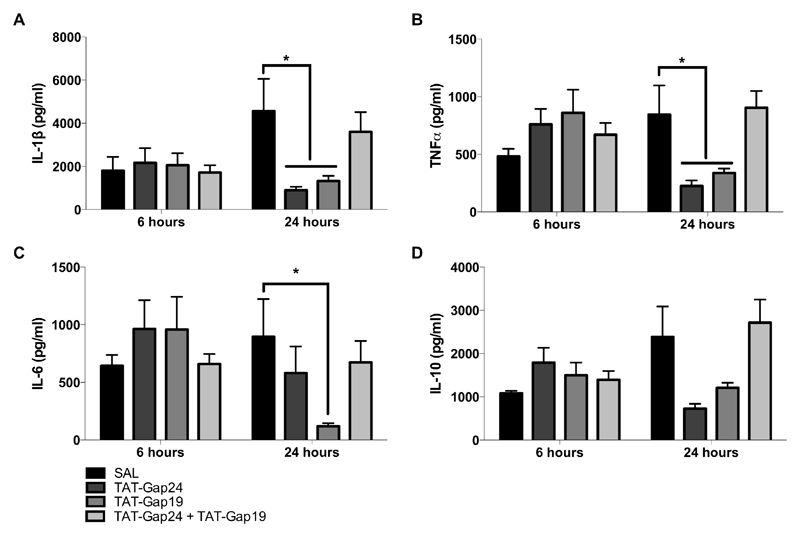
Connexin hemichannels have been identified as key mediators of inflammatory responses (Willebrords et al., 2016). Accordingly, a number of cytokines, namely IL-1β, IL-6, IL-10, and TNFα, which are considered of relevance for controlling hepatic injury-associated inflammation (Blazka et al., 1995; Cover et al., 2006), were evaluated. Serum cytokine levels of mice sacrificed after 6 and 24 hours were measured by ELISA analysis. Increased serum quantities of the pro-inflammatory cytokines IL-1β and TNFα were noticed in APAP-treated mice after 24 hours. Treatment with TAT-Gap24 and TAT-Gap19 separately decreased (p < 0.05) serum amounts of these pro-inflammatory cytokines 24 hours after APAP overdosing (p < 0.05) (Fig. 5A-B.). In addition, TAT-Gap19 reduced IL-6 serum levels (Fig. 5C.). No statistically significant differences in serum cytokines were measured when TAT-Gap24 and TAT-Gap19 were administered together to APAP-overdosed mice (Fig. 5A-D.). Effects on serum IL-10 serum levels remained absent in all experimental conditions (Fig. 5D.). These results show that closing of Cx32 or Cx43 hemichannels counteracts inflammation following APAP intoxication.
Figure 5. Connexin hemichannel inhibition differentially affects serum cytokine levels in APAP-induced hepatotoxicity.
Mice (n = 6-8 per group and per time point) were injected 300 mg/kg APAP followed by administration of 10 mg/kg TAT-Gap24, 10 mg/kg TAT-Gap19, a combination of both or saline (SAL) 1.5 hour later. Sampling was performed 6 and 24 hours after APAP overdosing. ELISA analysis of serum samples was performed to detect (A) IL-1β, (B) TNFα, (C) IL-6 and (D) IL-10. Data are expressed as means ± SEM, with *p < 0.05 compared to APAP followed by SAL administration.
3.6. Connexin hemichannel inhibition does not alter the liver oxidative status in APAP-induced hepatotoxicity
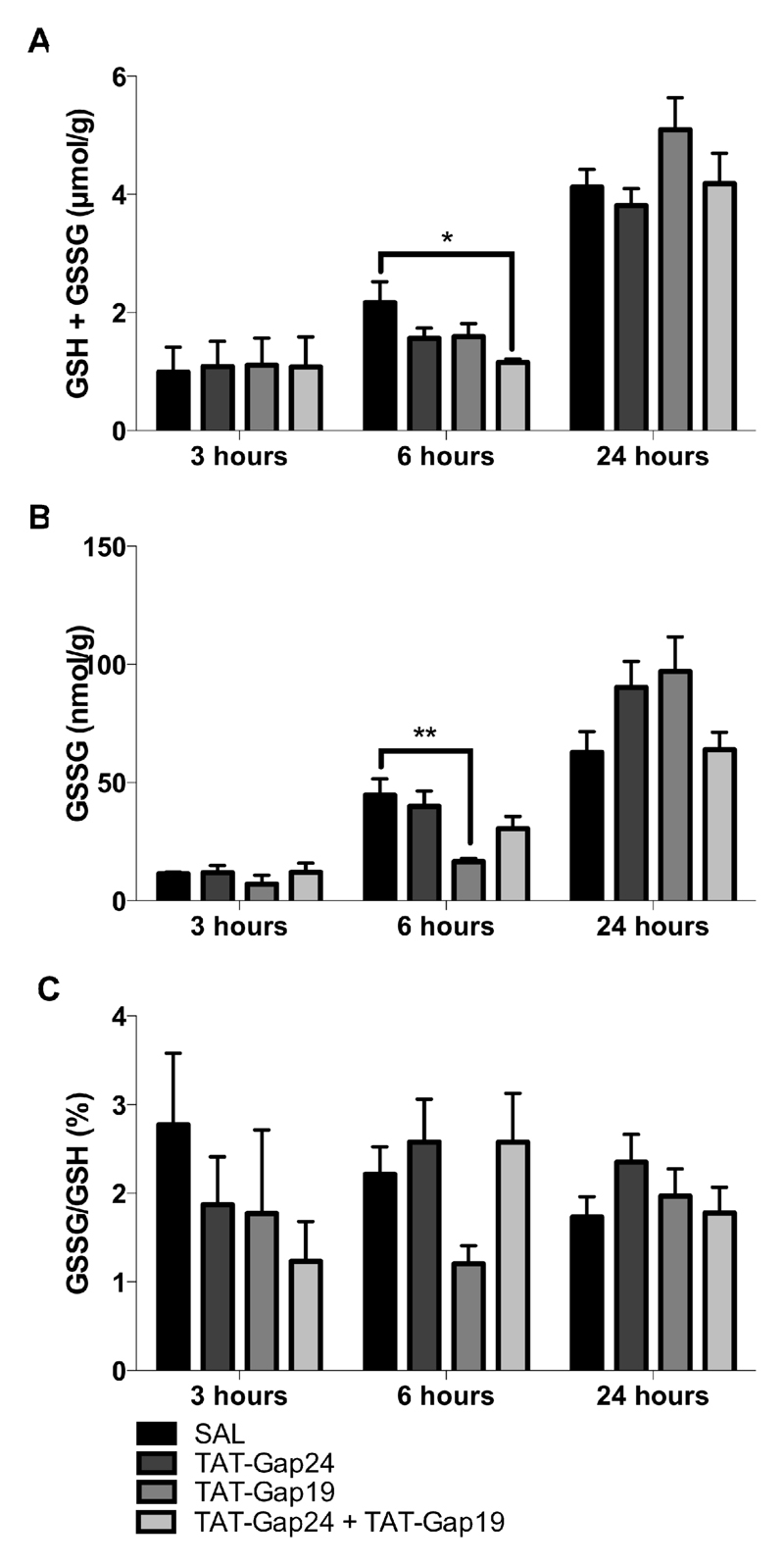
In healthy cells, more than 99 % of the total glutathione pool occurs in reduced form (GSH) and less than 1 % exists in the oxidized form (GSSG) (Jaeschke and Mitchell, 1990). However, in APAP toxicity, the GSH pool becomes depleted due to excessive NAPQI production (Jaeschke et al., 2012a). In this study, a gradual recovery of the total GSH pool became evident after 6 and 24 hours (Fig. 6A.). Although no significant differences were found in the recovery after 24 hours, the combined treatment with both mimetic peptides postponed the recovery, as significant lower (p < 0.05) total GSH levels were found 6 hours after APAP administration (Fig. 6A.). GSH acts as a critical anti-oxidant and is converted to its oxidized GSSG form upon reaction with reactive oxygen species. For all experimental groups, GSSG levels were elevated after 6 hours and peaked at the 24 hour time point (Fig. 6B.). Administration of TAT-Gap19 reduced (p < 0.01) tissue GSSG levels 6 hours after APAP overdosing. However, a tendency for higher GSSG levels was observed after 24 hours. Hence, upon normalization of GSSG values as a percentage of the total GSH amount, no differences were found 24 hours after APAP toxicity (Fig. 6C.). This indicates that connexin hemichannel closure does not affect the oxidative stress status after APAP-induced hepatotoxicity.
Figure 6. Connexin hemichannel inhibition does not alter the liver oxidative status in APAP-induced hepatotoxicity.
Mice (n = 5-13 per group and per time point) were injected 300 mg/kg APAP followed by administration of 10 mg/kg TAT-Gap24, 10 mg/kg TAT-Gap19, a combination of both or saline (SAL) 1.5 hour later. Sampling was performed 3, 6 and 24 hours after APAP overdosing. Hepatic levels of (A) GSH and (B) GSSG were measured and (D) the GSSG/GSH ratio was calculated. Data are expressed as means ± SEM, with *p < 0.05 and **p < 0.01 compared to APAP followed by SAL administration.
4. Discussion
Given their ubiquitous and well-acknowledged involvement in tissue functioning, gap junctions have been extensively explored as drug targets over the past decades. As a result, a wide variety of gap junction modulators have been successfully tested as pharmacological tools for a plethora of diseases (Bodendiek and Raman, 2010). Historically, connexin hemichannels have been considered as merely structural precursors of gap junctions. Nevertheless, a large body of evidence now points to independent roles for connexin hemichannels in cellular signaling by connecting the intracellular compartment with the extracellular environment, particularly in pathological conditions (Contreras et al., 2002; Sáez and Leybaert, 2014; Wang et al., 2013b). Research in this direction is, however, still surrounded by controversy (Spray et al., 2006), which is partly due to the lack of tools to distinguish between gap junction and hemichannel signaling. In recent years, peptides mimicking sequences in the cytoplasmic loop region of connexins, including Gap24 and Gap19, were found to act as specific connexin hemichannel inhibitors (De Vuyst et al., 2006; Wang et al., 2013b). Gap19 has been proven to bind to a sequence in the C-terminal tail of the connexin structure, thereby interfering with the intramolecular interaction between the cytoplasmic loop and C-terminal end, which is critical for connexin hemichannel opening (Bouvier et al., 2009; Hirst-Jensen et al., 2007; Iyyathurai et al., 2013; Ponsaerts et al., 2010; Wang et al., 2013b). As the targets of both peptides are located within the cell, they were linked to a HIV-1 TAT sequence in order to improve cytosolic uptake (Lindgren et al., 2000). The efficacy and specificity of Gap24 or Gap19 to suppress the opening of Cx32 and Cx43 hemichannels, respectively, has been demonstrated previously in cell lines expressing Cx32 (De Vuyst et al., 2006), astrocytes (Abudara et al., 2014) and cardiomyocytes (Wang et al., 2013b). The results of the present study show that this also holds true for hepatocytes, as evidenced by reduced extracellular release of ATP, indicative of connexin hemichannel opening, and unmodified gap junction activity. Subsequently, both peptides were applied to test the involvement of Cx32 and Cx43 hemichannels in APAP-induced hepatotoxicity in vivo, which is known to be accompanied by pronounced cell death and inflammatory responses. It should be stressed that the in vitro results obtained in rat hepatocytes are comparable to the in vivo model in mice, as there are only marginal differences between both species in Cx32 and Cx43 amino acid sequences (Beyer et al., 1987; Miller et al., 1988). In addition, rat hepatocytes were selected to set up cell cultures because connexin expression and their channel activities were previously fully characterized in this in vitro setting (Vinken et al., 2006, 2010, 2012). In contrast, mice were preferred over rats for in vivo testing purposes, since the latter are known to be poor in vivo models for APAP-induced toxicity (Maes et al., 2016c; McGill et al., 2012). Furthermore, alterations in connexin production have been studied in detail in this mouse model of APAP-induced liver injury (Maes et al., 2016a). In the present study, intoxicated mice were treated with TAT-Gap24 and/or TAT-Gap19 1.5 hour after APAP overdosing. This 1.5 hour timeframe is necessary for completion of APAP biotransformation and hence for formation of the deleterious NAPQI metabolite (McGill et al., 2013), and our results show that this process is not affected by TAT-Gap24 or TAT-Gap19. In case of TAT-Gap19, only minor changes in liver injury were recorded. In contrast, a significant reduction in serum ALT values was found upon treatment of APAP-overdosed animals with TAT-Gap24. Importantly, simultaneous treatment of mice with both mimetic peptides revealed an additive effect, as significantly lower ALT activity was found after co-treatment with TAT-Gap24 and TAT-Gap19 (Fig. 3A.). However, this was not reflected in the histopathological quantification of the necrotic areas. This could be explained by the fact that these areas are estimated per grades of 5 % and thus might overlook subtle changes between different experimental groups. Overall, these results suggest the involvement of connexin hemichannel signaling in APAP-induced acute liver failure. Connexin hemichannels hereby could facilitate the uptake of toxic substances and may contribute to the loss of essential metabolites. In this regard, ATP released through connexin hemichannels is known to decrease intracellular ATP content, as such favoring cell death through necrosis and inflammation (Decrock et al., 2009a; Kalvelyte et al., 2003; Leist et al., 1997). This corresponds with observations of the present study, since blockage of Cx32 or Cx43 hemichannels reduced serum levels of IL-1β and TNFα. Of note, co-administration of both peptides did not alter serum levels of these cytokines. The relevance of this finding remains unclear. Alternatively, cytosolic GSH may be liberated through Cx32 and Cx43 hemichannels, thus jeopardizing anti-oxidant cellular defense (Keleva et al. 2013; Rana and Dringen, 2007; Tong et al., 2015). However, the results of the current study do not seem in line with this scenario, as no differences were found in GSH amounts between the different experimental groups after 3 and 24 hours (Fig. 6A.). Interestingly, Cx32 and Cx43 have been identified in mitochondria (Boengler et al. 2013; Fowler et al. 2013) and mitochondrial Cx43-based hemichannels have been shown to contribute to cardiomyocyte cell injury and cell death (Gadicherla et al. 2017). Moreover, TAT-Gap19 administration inhibited necrotic cell death induced by hypoxia/reoxygenation (Gadicherla et al. 2017). This suggest that the beneficial effect of connexin hemichannel inhibition might not only rely on paracrine/autocrine signaling, but also on direct effects on mitochondria during the initiation of necrosis. Future studies should elucidate whether this situation also may take place in liver.
In summary, this study substantiates the role of connexin hemichannels as “pathological pores”. This may open perspectives for the establishment of novel therapeutic strategies, in casu of acute APAP-induced liver toxicity.
Highlights.
Inhibition of connexin hemichannels by connexin mimetic peptides.
No effects of connexin mimetic peptides on gap junctions.
Cx32 hemichannel inhibition reduces ALT activity and inflammation in APAP-induced liver injury.
Cx43 hemichannel inhibition reduces inflammation in APAP-induced liver injury.
Additive effects of Cx32 and Cx43 hemichannel inhibition on APAP-induced liver injury.
Acknowledgements
The authors wish to thank Miss Tineke Vanhalewyn, Miss Dinja De Win, Miss Veronica Mollica Govoni, Mister José Alexandre Coelho Pimental and Mister Paul Claes for their dedicated technical assistance.
Funding information
This work was supported by the grants of the Agency for Innovation by Science and Technology in Flanders [IWT grant 131003], the European Research Council [ERC Starting Grant 335476], the Fund for Scientific Research-Flanders [FWO grants G009514N, G010214N], the University Hospital of the Vrije Universiteit Brussel-Belgium [“Willy Gepts Fonds” UZ-VUB], the University of São Paulo-Brazil, the Foundation for Research Support of the State of São Paulo [FAPESP SPEC grant 2013/50420-6] and the National Institutes of Health [NIH grants DK102142, P20 GM103549].
List of abbreviations
- 2-APB
2-aminoethoxy-diphenyl-borate
- ALT
alanine aminotransferase
- ANOVA
analysis of variance
- APAP
acetaminophen
- ATP
adenosine triphosphate
- CBX
carbenoxolone
- Cx
connexin
- ELISA
enzyme-linked immunosorbent assay
- FRAP
fluorescence recovery after photobleaching
- GSH
glutathione
- GSSG
glutathione disulfide
- HBSS
Hank’s balanced salt solution
- IL-1β/6/10
interleukin 1β/6/10
- n
number of repeats
- NAPQI
N-acetyl-p-benzoquinone imine
- p
probability
- SEM
standard error of the mean
- TAT
transactivator of transcription
- TNFα
tumor necrosis factor α
References
- Abudara V, Bechberger J, Freitas-Andrade M, De Bock M, Wang N, Bultynck G, Naus CC, Leybaert L, Giaume C. The connexin43 mimetic peptide Gap19 inhibits hemichannels without altering gap junctional communication in astrocytes. Front Cell Neurosci. 2014;8:306. doi: 10.3389/fncel.2014.00306. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Balasubramaniyan V, Dhar DK, Warner AE, Vivien Li WY, Amiri AF, Bright B, Mookerjee RP, Davies NA, Becker DL, Jalan R. Importance of connexin43 based gap junction in cirrhosis and acute-on-chronic liver failure. J Hepatol. 2013;58:1194–1200. doi: 10.1016/j.jhep.2013.01.023. [DOI] [PubMed] [Google Scholar]
- Beyer EC, Paul DL, Goodenough DA. Connexin43: a protein from rat heart homologous to a gap junction protein from liver. J Cell Biol. 1987;105:2621–2629. doi: 10.1083/jcb.105.6.2621. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Blazka ME, Wilmer JL, Holladay SD, Wilson RE, Luster MI. Role of proinflammatory cytokines in acetaminophen hepatotoxicity. Toxicol Appl Pharmacol. 1995;133:43–52. doi: 10.1006/taap.1995.1125. [DOI] [PubMed] [Google Scholar]
- Bodendiek SB, Raman G. Connexin modulators and their potential targets under the magnifying glass. Curr Med Chem. 2010;17:4191–4230. doi: 10.2174/092986710793348563. [DOI] [PubMed] [Google Scholar]
- Boengler K, Ungefug E, Heusch G, Leybaert L, Schulz R. Connexin 43 impacts on mitochondrial potassium uptake. Front Pharmacol. 2013;4:73. doi: 10.3389/fphar.2013.00073. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bouvier D, Spagnol G, Chenavas S, Kieken F, Vitrac H, Brownell S, Kellezi A, Forge V, Sorgen PL. Characterization of the structure and intermolecular interactions between the connexin40 and connexin43 carboxyl-terminal and cytoplasmic loop domains. J Biol Chem. 2009;284:34257–34271. doi: 10.1074/jbc.M109.039594. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bradford MM. A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem. 1976;72:248–254. doi: 10.1016/0003-2697(76)90527-3. [DOI] [PubMed] [Google Scholar]
- Chandrasekhar A, Bera AK. Hemichannels: permeants and their effect on development, physiology and death. Cell Biochem Funct. 2012;30:89–100. doi: 10.1002/cbf.2794. [DOI] [PubMed] [Google Scholar]
- Contreras JE, Sanchez HA, Eugenin EA, Speidel D, Theis M, Willecke K, Bukauskas FF, Bennett MV, Saez JC. Metabolic inhibition induces opening of unapposed connexin 43 gap junction hemichannels and reduces gap junctional communication in cortical astrocytes in culture. Proc Natl Acad Sci U S A. 2002;99:495–500. doi: 10.1073/pnas.012589799. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cover C, Liu J, Farhood A, Malle E, Waalkes MP, Bajt ML, Jaeschke H. Pathophysiological role of the acute inflammatory response during acetaminophen hepatotoxicity. Toxicol Appl Pharmacol. 2006;216:98–107. doi: 10.1016/j.taap.2006.04.010. [DOI] [PubMed] [Google Scholar]
- Dahlin DC, Miwa GT, Lu AY, Nelson SD. N-acetyl-p-benzoquinone imine: a cytochrome P-450-mediated oxidation product of acetaminophen. Proc Natl Acad Sci U S A. 1984;81:1327–1331. doi: 10.1073/pnas.81.5.1327. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Davidson JS, Baumgarten IM, Harley EH. Reversible inhibition of intercellular junctional communication by glycyrrhetinic acid. Biochem Biophys Res Commun. 1986;134:29–36. doi: 10.1016/0006-291x(86)90522-x. [DOI] [PubMed] [Google Scholar]
- De Vuyst E, Decrock E, Cabooter L, Dubyak GR, Naus CC, Evans WH, Leybaert L. Intracellular calcium changes trigger connexin 32 hemichannel opening. EMBO J. 2006;25:34–44. doi: 10.1038/sj.emboj.7600908. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Decrock E, De Vuyst E, Vinken M, Van Moorhem M, Vranckx K, Wang N, Van Laeken L, De Bock M, D'Herde K, Lai CP, Rogiers V, et al. Connexin 43 hemichannels contribute to the propagation of apoptotic cell death in a rat C6 glioma cell model. Cell Death Differ. 2009a;16:151–163. doi: 10.1038/cdd.2008.138. [DOI] [PubMed] [Google Scholar]
- Decrock E, Vinken M, De Vuyst E, Krysko DV, D'Herde K, Vanhaecke T, Vandenabeele P, Rogiers V, Leybaert L. Connexin-related signaling in cell death: to live or let die? Cell Death Differ. 2009b;16:524–536. doi: 10.1038/cdd.2008.196. [DOI] [PubMed] [Google Scholar]
- Desplantez T, Verma V, Leybaert L, Evans WH, Weingart R. Gap26, a connexin mimetic peptide, inhibits currents carried by connexin43 hemichannels and gap junction channels. Pharmacol Res. 2012;65:546–552. doi: 10.1016/j.phrs.2012.02.002. [DOI] [PubMed] [Google Scholar]
- Du K, Williams CD, McGill MR, Xie Y, Farhood A, Vinken M, Jaeschke H. The gap junction inhibitor 2-aminoethoxy-diphenyl-borate protects against acetaminophen hepatotoxicity by inhibiting cytochrome P450 enzymes and c-jun N-terminal kinase activation. Toxicol Appl Pharmacol. 2013;273:484–491. doi: 10.1016/j.taap.2013.09.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Evans WH, Leybaert L. Mimetic peptides as blockers of connexin channel-facilitated intercellular communication. Cell Commun Adhes. 2007;14:265–273. doi: 10.1080/15419060801891034. [DOI] [PubMed] [Google Scholar]
- Fowler SL, Akins M, Zhou H, Figeys D, Bennett SA. The liver connexin32 interactome is a novel plasma membrane-mitochondrial signaling nexus. J Proteome Res. 2013;12:2597–2610. doi: 10.1021/pr301166p. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gadicherla AK, Wang N, Bulic M, Agullo-Pascual E, Lissoni A, De Smet M, Delmar M, Bultynck G, Krysko DV, Camara A, Schlüter KD, et al. Mitochondrial Cx43 hemichannels contribute to mitochondrial calcium entry and cell death in the heart. Basic Res Cardiol. 2017;112:27. doi: 10.1007/s00395-017-0618-1. [DOI] [PubMed] [Google Scholar]
- Goldberg GS, Moreno AP, Bechberger JF, Hearn SS, Shivers RR, MacPhee DJ, Zhang YC, Naus CC. Evidence that disruption of connexon particle arrangements in gap junction plaques is associated with inhibition of gap junctional communication by a glycyrrhetinic acid derivative. Exp Cell Res. 1996;222:48–53. doi: 10.1006/excr.1996.0006. [DOI] [PubMed] [Google Scholar]
- Gujral JS, Knight TR, Farhood A, Bajt ML, Jaeschke H. Mode of cell death after acetaminophen overdose in mice: apoptosis or oncotic necrosis? Toxicol Sci. 2002;67:322–328. doi: 10.1093/toxsci/67.2.322. [DOI] [PubMed] [Google Scholar]
- Hirst-Jensen BJ, Sahoo P, Kieken F, Delmar M, Sorgen PL. Characterization of the pH-dependent interaction between the gap junction protein connexin43 carboxyl terminus and cytoplasmic loop domains. J Biol Chem. 2007;282:5801–5813. doi: 10.1074/jbc.M605233200. [DOI] [PubMed] [Google Scholar]
- Ichai P, Samuel D. Epidemiology of liver failure. Clin Res Hepatol Gastroenterol. 2011;35:610–617. doi: 10.1016/j.clinre.2011.03.010. [DOI] [PubMed] [Google Scholar]
- Igarashi I, Maejima T, Kai K, Arakawa S, Teranishi M, Sanbuissho A. Role of connexin 32 in acetaminophen toxicity in a knockout mice model. Exp Toxicol Pathol. 2014;66:103–110. doi: 10.1016/j.etp.2013.10.002. [DOI] [PubMed] [Google Scholar]
- Iyyathurai J, D'hondt C, Wang N, De Bock M, Himpens B, Retamal MA, Stehberg J, Leybaert L, Bultynck G. Peptides and peptide-derived molecules targeting the intracellular domains of Cx43: gap junctions versus hemichannels. Neuropharmacology. 2013;75:491–505. doi: 10.1016/j.neuropharm.2013.04.050. [DOI] [PubMed] [Google Scholar]
- Jaeschke H, McGill MR. Cytochrome P450-derived versus mitochondrial oxidant stress in acetaminophen hepatotoxicity. Toxicol Lett. 2015;235:216–217. doi: 10.1016/j.toxlet.2015.04.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jaeschke H, McGill MR, Ramachandran A. Oxidant stress, mitochondria, and cell death mechanisms in drug-induced liver injury: lessons learned from acetaminophen hepatotoxicity. Drug Metab Rev. 2012a;44:88–106. doi: 10.3109/03602532.2011.602688. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jaeschke H, Mitchell JR. Use of isolated perfused organs in hypoxia and ischemia/reperfusion oxidant stress. Methods Enzymol. 1990;186:752–759. doi: 10.1016/0076-6879(90)86175-u. [DOI] [PubMed] [Google Scholar]
- Jaeschke H, Williams CD, McGill MR. Caveats of using acetaminophen hepatotoxicity models for natural product testing. Toxicol Lett. 2012b;215:40–41. doi: 10.1016/j.toxlet.2012.09.023. [DOI] [PubMed] [Google Scholar]
- Kalvelyte A, Imbrasaite A, Bukauskiene A, Verselis VK, Bukauskas FF. Connexins and apoptotic transformation. Biochem Pharmacol. 2003;66:1661–1672. doi: 10.1016/s0006-2952(03)00540-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Keleva T, Cavar I, Vukojevic K, Babic-Saraga M, Culo F. The effect of glucagon and cyclic adenosine monophosphate on acute liver damage induced by acetaminophen. Histo Histopathol. 2013;28:245–255. doi: 10.14670/HH-28.245. [DOI] [PubMed] [Google Scholar]
- Lee WM. Etiologies of acute liver failure. Semin Liver Dis. 2008;28:142–152. doi: 10.1055/s-2008-1073114. [DOI] [PubMed] [Google Scholar]
- Leist M, Single B, Castoldi AF, Kühnle S, Nicotera P. Intracellular adenosine triphosphate (ATP) concentration: a switch in the decision between apoptosis and necrosis. J Exp Med. 1997;185:1481–1486. doi: 10.1084/jem.185.8.1481. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lindgren M, Hällbrink M, Prochiantz A, Langel U. Cell-penetrating peptides. Trends Pharmacol Sci. 2000;21:99–103. doi: 10.1016/s0165-6147(00)01447-4. [DOI] [PubMed] [Google Scholar]
- Maes M, Cogliati B, Yanguas SC, Willebrords J, Vinken M. Roles of connexins and pannexins in digestive homeostasis. Cellular and Molecular Life Sciences. 2015a;72:2809–2821. doi: 10.1007/s00018-015-1961-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Maes M, Decrock E, Cogliati B, Oliveira AG, Marques PE, Dagli MLZ, Menezes GB, Mennecier G, Leybaert L, Vanhaecke T, Rogiers V, et al. Connexin and pannexin (hemi) channels in the liver. Frontiers in Physiology. 2014;4:405. doi: 10.3389/fphys.2013.00405. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Maes M, McGill MR, da Silva TC, Abels C, Lebofsky M, de Araujo CMM, Tiburcio T, Pereira IVA, Willebrords J, Yanguas SC, Farhood A, et al. Involvement of connexin43 in acetaminophen-induced liver injury. Biochimi Biophys Acta - Mol Bas Dis. 2016a;1862:1111–1121. doi: 10.1016/j.bbadis.2016.02.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Maes M, McGill MR, da Silva TC, Lebofsky M, de Araujo CMM, Tiburcio T, Pereira IVA, Willebrords J, Yanguas SC, Farhood A, Dagli MLZ, et al. Connexin32: a mediator of acetaminophen- induced liver injury? Toxicol Mech Meth. 2016b;26:88–96. doi: 10.3109/15376516.2015.1103000. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Maes M, Vinken M, Jaeschke H. Experimental models of hepatotoxicity related to acute liver failure. Toxicol Appl Pharmacol. 2016c;290:86–97. doi: 10.1016/j.taap.2015.11.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Maes M, Yanguas SC, Willebrords J, Cogliati B, Vinken M. Connexin and pannexin signaling in gastrointestinal and liver disease. Transl Res. 2015b;166:332–343. doi: 10.1016/j.trsl.2015.05.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McGill MR, Lebofsky M, Norris HRK, Slawson MH, Bajt ML, Xie YC, Williams CD, Wilkins DG, Rollins DE, Jaeschke H. Plasma and liver acetaminophen-protein adduct levels in mice after acetaminophen treatment: Dose-response, mechanisms, and clinical implications. Toxicol Appl Pharmacol. 2013;269:240–249. doi: 10.1016/j.taap.2013.03.026. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McGill MR, Williams CD, Xie Y, Ramachandran A, Jaeschke H. Acetaminophen-induced liver injury in rats and mice: comparison of protein adducts, mitochondrial dysfunction, and oxidative stress in the mechanism of toxicity. Toxicol Appl Pharmacol. 2012;264:387–394. doi: 10.1016/j.taap.2012.08.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Miller T, Dahl G, Werner R. Structure of a gap junction gene: rat connexin-32. Biosci Rep. 1988;8:455–464. doi: 10.1007/BF01121644. [DOI] [PubMed] [Google Scholar]
- Mitchell JR, Jollow DJ, Potter WZ, Davis DC, Gillette JR, Brodie BB. Acetaminophen-induced hepatic necrosis. I. Role of drug metabolism. J Pharmacol Exp Ther. 1973;187:185–194. [PubMed] [Google Scholar]
- Muldrew KL, James LP, Coop L, McCullough SS, Hendrickson HP, Hinson JA, Mayeux PR. Determination of acetaminophen-protein adducts in mouse liver and serum and human serum after hepatotoxic doses of acetaminophen using high-performance liquid chromatography with electrochemical detection. Drug Metabol Dispos. 2002;30:446–451. doi: 10.1124/dmd.30.4.446. [DOI] [PubMed] [Google Scholar]
- Naiki-Ito A, Asamoto M, Naiki T, Ogawa K, Takahashi S, Sato S, Shirai T. Gap junction dysfunction reduces acetaminophen hepatotoxicity with impact on apoptotic signaling and connexin 43 protein induction in rat. Toxicol Pathol. 2010;38:280–286. doi: 10.1177/0192623309357951. [DOI] [PubMed] [Google Scholar]
- Oshima A. Structure and closure of connexin gap junction channels. FEBS Lett. 2014;588:1230–1237. doi: 10.1016/j.febslet.2014.01.042. [DOI] [PubMed] [Google Scholar]
- Papeleu P, Vanhaecke T, Henkens T, Elaut G, Vinken M, Snykers S, Rogiers V. Isolation of rat hepatocytes. Methods Mol Biol. 2006;320:229–237. doi: 10.1385/1-59259-998-2:229. [DOI] [PubMed] [Google Scholar]
- Park WJ, Park JW, Erez-Roman R, Kogot-Levin A, Bame JR, Tirosh B, Saada A, Merrill AH, Pewzner-Jung Y, Futerman AH. Protection of a ceramide synthase 2 null mouse from drug-induced liver injury: role of gap junction dysfunction and connexin 32 mislocalization. J Biol Chem. 2013;288:30904–30916. doi: 10.1074/jbc.M112.448852. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Patel SJ, Milwid JM, King KR, Bohr S, Iracheta-Velle A, Li M, Vitalo A, Parekkadan B, Jindal R, Yarmush ML. Gap junction inhibition prevents drug-induced liver toxicity and fulminant hepatic failure. Nat Biotechnol. 2012;30:179–183. doi: 10.1038/nbt.2089. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ponsaerts R, De Vuyst E, Retamal M, D'hondt C, Vermeire D, Wang N, De Smedt H, Zimmermann P, Himpens B, Vereecke J, Leybaert L, et al. Intramolecular loop/tail interactions are essential for connexin 43-hemichannel activity. FASEB J. 2010;24:4378–4395. doi: 10.1096/fj.09-153007. [DOI] [PubMed] [Google Scholar]
- Rana S, Dringen R. Gap junction hemichannel-mediated release of glutathione from cultured rat astrocytes. Neurosci Lett. 2007;415:45–48. doi: 10.1016/j.neulet.2006.12.043. [DOI] [PubMed] [Google Scholar]
- Spray DC, Ye ZC, Ransom BR. Functional connexin "hemichannels": a critical appraisal. Glia. 2006;54:758–773. doi: 10.1002/glia.20429. [DOI] [PubMed] [Google Scholar]
- Stout CE, Costantin JL, Naus CC, Charles AC. Intercellular calcium signaling in astrocytes via ATP release through connexin hemichannels. J Biol Chem. 2002;277:10482–10488. doi: 10.1074/jbc.M109902200. [DOI] [PubMed] [Google Scholar]
- Sáez JC, Leybaert L. Hunting for connexin hemichannels. FEBS Lett. 2014;588:1205–1211. doi: 10.1016/j.febslet.2014.03.004. [DOI] [PubMed] [Google Scholar]
- Tong X, Lopez W, Ramachandran J, Ayad WA, Liu Y, Lopez-Rodriguez A, Harris AL, Contreras JE. Glutathione release through connexin hemichannels: Implications for chemical modification of pores permeable to large molecules. J Gen Physiol. 2015;146:245–254. doi: 10.1085/jgp.201511375. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Vinken M. Gap junctions and non-neoplastic liver disease. J Hepatol. 2012;57:655–662. doi: 10.1016/j.jhep.2012.02.036. [DOI] [PubMed] [Google Scholar]
- Vinken M, Decrock E, De Vuyst E, De Bock M, Vandenbroucke RE, De Geest BG, Demeester J, Sanders NN, Vanhaecke T, Leybaert L, Rogiers V. Connexin32 hemichannels contribute to the apoptotic-to-necrotic transition during Fas-mediated hepatocyte cell death. Cell Mol Life Sci. 2010;67:907–918. doi: 10.1007/s00018-009-0220-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Vinken M, Decrock E, Vanhaecke T, Leybaert L, Rogiers V. Connexin43 signaling contributes to spontaneous apoptosis in cultures of primary hepatocytes. Toxicol Sci. 2012;125:175–186. doi: 10.1093/toxsci/kfr277. [DOI] [PubMed] [Google Scholar]
- Vinken M, Henkens T, De Rop E, Fraczek J, Vanhaecke T, Rogiers V. Biology and pathobiology of gap junctional channels in hepatocytes. Hepatology. 2008;47:1077–1088. doi: 10.1002/hep.22049. [DOI] [PubMed] [Google Scholar]
- Vinken M, Henkens T, Vanhaecke T, Papeleu P, Geerts A, Van Rossen E, Chipman JK, Meda P, Rogiers V. Trichostatin a enhances gap junctional intercellular communication in primary cultures of adult rat hepatocytes. Toxicol Sci. 2006;91:484–492. doi: 10.1093/toxsci/kfj152. [DOI] [PubMed] [Google Scholar]
- Wang N, De Bock M, Decrock E, Bol M, Gadicherla A, Vinken M, Rogiers V, Bukauskas FF, Bultynck G, Leybaert L. Paracrine signaling through plasma membrane hemichannels. Biochim Biophys Acta. 2013a;1828:35–50. doi: 10.1016/j.bbamem.2012.07.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wang N, De Vuyst E, Ponsaerts R, Boengler K, Palacios-Prado N, Wauman J, Lai CP, De Bock M, Decrock E, Bol M, Vinken M, et al. Selective inhibition of Cx43 hemichannels by Gap19 and its impact on myocardial ischemia/reperfusion injury. Basic Res Cardiol. 2013b;108:309. doi: 10.1007/s00395-012-0309-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Willebrords J, Crespo Yanguas S, Maes M, Decrock E, Wang N, Leybaert L, Kwak BR, Green CR, Cogliati B, Vinken M. Connexins and their channels in inflammation. Crit Rev Biochem Mol Biol. 2016:1–27. doi: 10.1080/10409238.2016.1204980. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ye ZC, Wyeth MS, Baltan-Tekkok S, Ransom BR. Functional hemichannels in astrocytes: a novel mechanism of glutamate release. J Neurosci. 2003;23:3588–3596. doi: 10.1523/JNEUROSCI.23-09-03588.2003. [DOI] [PMC free article] [PubMed] [Google Scholar]