Abstract
Problem/Condition
Since the first U.S. infant conceived with assisted reproductive technology (ART) was born in 1981, both the use of ART and the number of fertility clinics providing ART services have increased steadily in the United States. ART includes fertility treatments in which eggs or embryos are handled in the laboratory (i.e., in vitro fertilization [IVF] and related procedures). Women who undergo ART procedures are more likely than women who conceive naturally to deliver multiple-birth infants. Multiple births pose substantial risks to both mothers and infants, including obstetric complications, preterm delivery, and low birthweight infants. This report provides state-specific information for the United States (including the District of Columbia and Puerto Rico) on ART procedures performed in 2014 and compares birth outcomes that occurred in 2014 (resulting from ART procedures performed in 2013 and 2014) with outcomes for all infants born in the United States in 2014.
Period Covered
2014.
Description of System
In 1996, CDC began collecting data on ART procedures performed in fertility clinics in the United States as mandated by the Fertility Clinic Success Rate and Certification Act of 1992 (FCSRCA) (Public Law 102–493). Data are collected through the National ART Surveillance System (NASS), a web-based data collection system developed by CDC. This report includes data from 52 reporting areas (the 50 states, the District of Columbia, and Puerto Rico).
Results
In 2014, a total of 169,568 ART procedures (range: 124 in Wyoming to 21,018 in California) with the intent to transfer at least one embryo were performed in 458 U.S. fertility clinics and reported to CDC. These procedures resulted in 56,028 live-birth deliveries (range: 52 in Wyoming to 7,230 in California) and 68,782 infants born (range: 64 in Wyoming to 8,793 in California). Nationally, the total number of ART procedures performed per million women of reproductive age (15–44 years), a proxy measure of the ART usage rate, was 2,647 (range: 364 in Puerto Rico to 6,726 in Massachusetts). ART use exceeded the national average in 13 reporting areas (Connecticut, Delaware, the District of Columbia, Hawaii, Illinois, Maryland, Massachusetts, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, and Virginia). Eight reporting areas (Connecticut, the District of Columbia, Hawaii, Illinois, Maryland, Massachusetts, New Jersey, and New York) had rates of ART use exceeding 1.5 times the national average.
Nationally, among ART transfer procedures in patients using fresh embryos from their own eggs, the average number of embryos transferred increased with increasing age of the woman (1.7 among women aged <35 years, 1.9 among women aged 35–37 years, and 2.3 among women aged >37 years). Among women aged <35 years, who typically are considered to be good candidates for elective single embryo transfer (eSET) procedures, the national eSET rate was 28.5% (range: 4.3% in Puerto Rico to 67.9% in Delaware).
In 2014, ART contributed to 1.6% of all infants born in the United States (range: 0.4% in Puerto Rico to 4.7% in Massachusetts) and 18.3% of all multiple-birth infants (range: 5.5% in Alaska and West Virginia to 37.3% in Hawaii), including 18.0% of all twin infants (range: 5.2% in some states to 36.2% in Hawaii) and 26.4% of all triplets and higher-order infants (range: 0% in some states to 65.2% in Hawaii). Percentages of live births that were multiple-birth deliveries were higher among infants conceived with ART (39.4%; range: 11.5% in Delaware to 55.6% in Puerto Rico) than among all infants born in the total birth population (3.5%; range: 2.2% in Puerto Rico to 4.4% in New Jersey). Approximately 38.0% of ART-conceived infants were twin infants, and 2.0% were triplets and higher-order infants. ART-conceived twins accounted for approximately 95.3% of all ART-conceived infants born in multiple deliveries.
Nationally, infants conceived with ART contributed to 5.5% of all low birthweight (<2,500 g) infants (range: 1.2% in West Virginia to 14.2% in Massachusetts). Among ART-conceived infants, 27.8% were low birthweight (range: 10.6% in Delaware to 44.4% in Puerto Rico), compared with 8.0% among all infants (range: 5.9% in Alaska to 11.3% in Mississippi).
ART-conceived infants contributed to 4.7% of all preterm (<37 weeks) infants (range: 1.2% in Puerto Rico to 13.4% in Massachusetts). Percentages of preterm births were higher among infants conceived with ART (33.2%; range: 18.9% in the District of Columbia to 45.9% in Puerto Rico) than among all infants born in the total birth population (11.3%; range: 8.5% in California to 16.0% in Mississippi).
The percentage of ART-conceived infants who were low birthweight was 8.9% (range: 3.2% in some states to 16.1% in Vermont) among singletons and 55.2% (range: 38.5% in Delaware to 77.8% in Alaska) among twins; the corresponding percentages of low birthweight infants among all infants born were 6.3% for singletons (range: 4.6% in Alaska, North Dakota, and Oregon to 9.5% in Puerto Rico) and 55.2% for twins (range: 46.1% in Alaska to 65.6% in Mississippi).
The percentage of ART-conceived infants who were preterm was 13.2% (range: 7.5% in Rhode Island to 23.4% in West Virginia) among singletons and 62.2% (range: 33.3% in some states to 81.4% in Mississippi) among twins; the corresponding percentages of preterm infants among all infants were 9.7% for singletons (range: 1.7% in the District of Columbia to 14.2% in Mississippi) and 56.6% for twins (range: 47.2% in Vermont to 66.9% in Wyoming).
Interpretation
The percentage of infants conceived with ART varied considerably by reporting area. Multiple births from ART contributed to a substantial proportion of all twins, triplets, and higher-order infants born. Low birthweight and preterm infant birth rates were disproportionately higher among ART-conceived infants than among the overall birth population. Although women aged <35 years are typically considered good candidates for eSET, on average two embryos were transferred per ART procedure with women in this group. Compared with ART-conceived singletons, ART-conceived twins were approximately five times more likely to be born preterm and approximately six times more likely to be born with low birthweight. Singleton infants conceived with ART had higher percentages of preterm birth and low birthweight than all singleton infants born in the United States. ART use per population unit was geographically variable, with 13 reporting areas showing ART use higher than the national rate. Of the four states (Illinois, Massachusetts, New Jersey, and Rhode Island) with comprehensive statewide-mandated health insurance coverage for ART procedures (i.e., coverage for at least four cycles of IVF), three (Illinois, Massachusetts, and New Jersey) had rates of ART use exceeding 1.5 times the national rate. This type of mandated insurance has been associated with greater use of ART and likely accounts for some of the difference in per capita ART use observed among states.
Public Health Action
Reducing the number of embryos transferred and increasing use of eSET when clinically appropriate could help reduce multiple births and related adverse health consequences. Because twins account for the majority of ART-conceived multiple births, improved provider practices and patient education and counseling on the maternal and infant health risks of having twins are needed. Although ART contributes to high percentages of multiple births, other factors not investigated in this report (e.g., delayed childbearing and use of non-ART fertility treatments) also contribute to multiple births and warrant further study.
Introduction
Since the birth of the first U.S. infant conceived with assisted reproductive technology (ART) in 1981, use of advanced technologies to overcome infertility has increased, as has the number of fertility clinics providing ART services and procedures in the United States (1). In 1992, Congress passed the Fertility Clinic Success Rate and Certification Act (FCSRCA) (Public Law 102–493), which requires that all U.S. fertility clinics performing ART procedures report data to CDC annually on every ART procedure performed. CDC initiated data collection in 1996 and published the first annual ART Success Rates Report in 1997 (2). Several measures of success for ART are presented in the annual report (1,3), including the percentage of ART procedures and transfers that result in pregnancies, live-birth deliveries, singleton live-birth deliveries, and multiple live-birth deliveries.
Although ART helps millions of infertile couples to achieve pregnancy, it is associated with potential health risks to both mother and infant. Because multiple embryos are transferred in the majority of ART procedures, ART often results in multiple-gestation pregnancies and multiple births (4–11). Risks to the mother from multiple births include higher rates of caesarean deliveries, maternal hemorrhage, pregnancy-related hypertension, and gestational diabetes (12,13). Risks to the infant include prematurity, low birthweight, infant death, and elevated risk for birth defects and developmental disability (4–18). Further, even singleton infants conceived with ART have a higher risk for low birthweight and prematurity than singletons not conceived with ART (19,20).
This report was compiled on the basis of ART surveillance data reported to CDC’s Division of Reproductive Health for procedures performed in 2014. Data on the use of ART are presented for residents of each U.S. state, the District of Columbia, and Puerto Rico; data also are reported for outcomes for infants born in 2014 resulting from ART procedures performed in 2013 and 2014. The report also examines the contribution of ART to select outcomes (i.e., multiple-birth infants, low birthweight infants, and preterm infants) and compares ART infant outcomes with outcomes among all infants born in the United States (including Puerto Rico) in 2014.
Methods
National ART Surveillance System
In 1996, CDC initiated data collection of ART procedures performed in the United States. ART data for 1995–2003 were obtained from the Society for Assisted Reproductive Technology (SART). Since 2004, CDC has contracted with Westat, Inc., a statistical survey research organization, to obtain data from all fertility clinics in the United States through the National ART Surveillance System (NASS), a web-based data collection system developed by CDC (https://www.cdc.gov/art/nass/index.html). Clinics can enter their data directly into NASS and verify its accuracy before sending the data to Westat. SART-member clinics can report their data to NASS through SART. Non-SART-member clinics can report their data directly through NASS. The data then are compiled by Westat and reviewed by both CDC and Westat. A small proportion of clinics (7.8%) did not report their data to CDC in 2014 and are listed as nonreporting programs in the 2014 ART Fertility Clinic Success Rates Report, as required by FCSRCA. Because nonreporting clinics tend to be smaller on average than reporting clinics, NASS is estimated to contain information on 98.0% of all ART procedures in the United States (1).
Data collected include patient demographics, medical history, and infertility diagnoses; clinical information pertaining to the ART procedure type; and information regarding resultant pregnancies and births. The data file contains one record per ART procedure (or cycle of treatment) performed. Because ART providers typically do not provide continued prenatal care after a pregnancy is established, information on live births for all procedures is collected by ART clinics either directly from the patients (73.7%) or from the patients’ obstetric providers (25.2%). Approximately 1.0% of pregnancy outcomes are missing in NASS.
ART Procedures
ART includes fertility treatments in which eggs or embryos are handled in a laboratory (e.g., in vitro fertilization [IVF], gamete intrafallopian transfer, and zygote intrafallopian transfer). Approximately 99.0% of ART procedures performed are IVF. Because an ART procedure consists of several steps over an interval of approximately 2 weeks, a procedure often is referred to as a cycle of treatment. An ART cycle usually begins with drug-induced ovarian stimulation. If eggs are produced, the cycle progresses to the egg-retrieval stage, which involves surgical removal of the eggs from the ovaries. After the eggs are retrieved, they are combined with sperm in the laboratory during the IVF procedure. If successful, the most viable embryos (i.e., those that appear morphologically most likely to develop and implant) are selected for transfer back into the uterus by clinicians. If an embryo implants in the uterus, a clinical pregnancy is diagnosed by the presence of a gestational sac detectable by ultrasound. The majority of pregnancy losses occur within the first 12 weeks. Beyond 12 weeks of gestation, the pregnancy usually progresses to a live-birth delivery, defined as the delivery of one or more live-born infants. Survival of pregnancy ranges from 95.0% at 16 weeks to 98.0% at 20 weeks (21). ART does not include treatments in which only sperm are handled (i.e., intrauterine insemination) or procedures in which a woman takes drugs to stimulate egg production without the intention of having eggs retrieved.
ART procedures are classified into four types on the basis of the source of the egg (patient or donor) and the status of the embryos (fresh or thawed). Both fresh and thawed embryos can be derived from either the patient’s eggs or the donor’s eggs. Both patient and donor embryos can be created using sperm from a partner or from a donor. ART procedures involving fresh embryos include an egg-retrieval stage. ART procedures that use thawed embryos do not include egg retrieval because the eggs were fertilized during a previous procedure and the resultant embryos were frozen until the current procedure. An ART cycle can be discontinued at any step for medical reasons or by patient choice.
Variables and Definitions
ART data and outcomes from ART procedures are presented by patient’s residence (i.e., reporting area) at the time of treatment, which might not be the same as the location where the procedure was performed. If information on patient’s residence was missing, residence was assigned as the location where the procedure was performed. ART procedures performed in the United States among non-U.S. residents are included in NASS data; however, they were excluded from certain calculations for which the exact denominators were not known. To protect confidentiality in the presentation of data in tables, cells with values of 1–4 are suppressed, as are data that can be used to derive cell values of 1–4; however, these values are included in the totals. In some cases as applicable, states are not identified when reporting ranges to protect confidentiality. Because of small numbers, ART data from U.S. territories (with the exception of Puerto Rico) are not included in this report. In addition, estimates derived from cell values <20 in the denominator have been suppressed because they are unstable, and estimates could not be calculated when the denominator was zero (e.g., preterm birth among triplets, in reporting areas with no triplet births).
This report presents data on all procedures initiated with the intent to transfer at least one embryo; however, birth outcomes are determined on the basis of procedures that involved embryo transfer. The number of ART procedures performed per 1 million women of reproductive age (15–44 years) was calculated and the resulting rate approximates the proportion of women of reproductive age who used ART in each reporting area. However, this proxy measure of ART use is only an approximation because some women who used ART might fall outside the age range of 15–44 years (approximately 10.0% in 2014) and some women might have had more than one procedure during the reporting period.
A live-birth delivery was defined as birth of one or more live-born infants. A singleton live-birth delivery was defined as a birth of only one infant who was born live. A multiple live-birth delivery was defined as a birth of two or more infants, at least one of whom was born live. Low birthweight was defined as <2,500 g and very low birthweight as <1,500 g. For comparability with births to women who did not undergo ART, for whom gestational age is determined on the basis of the date of the last menstrual period, gestational age for fresh ART procedures was calculated by subtracting the date of egg retrieval from the birth date and adding 14 days. For frozen embryo cycles and for fresh ART procedures for which the date of retrieval was not available, gestational age was calculated by subtracting the date of embryo transfer from the birth date and adding 17 days (to account for an average of 3 days in embryo culture). Preterm delivery was defined as gestational age <37 weeks and very preterm delivery as gestational age <32 weeks (22).
Elective single-embryo transfer (eSET) is a procedure in which one embryo, selected from a larger number of available embryos, is placed in the uterus, with extra embryos cryopreserved. Fresh transfer procedures in which only one embryo was transferred but no embryos were cryopreserved are considered single-embryo transfer (SET) but not considered eSET. In this report, percentages of eSET procedures and the average number of embryos transferred were calculated for patients who used fresh embryos from their own eggs, in which at least one embryo was transferred. The rate of eSET was calculated by dividing the total number of transfer procedures, in which only one embryo was transferred and one or more embryos were cryopreserved, by the sum of the total number of single-embryo transfer procedures where extra embryos were cryopreserved plus the total number of transfer procedures in which more than one embryo was transferred. Transfer procedures in which only one embryo was transferred but no embryos were cryopreserved were excluded from the calculation of eSET percentages. The average number of embryos transferred for three age groups (<35 years, 35–37 years, and >37 years) was calculated by dividing the total number of embryos transferred by the total number of embryo-transfer procedures performed in that age group.
The contribution of ART to all infants born in a particular reporting area was used as a second measure of ART use. The contribution of ART to an outcome (e.g., preterm or low birthweight infant) was calculated by dividing the total number of outcomes among ART-conceived infants by the total number of outcomes among all infants born. The percentage of infants (ART conceived and all infants) born in the reporting area was calculated by plurality (singleton, multiple, twin, and triplet and higher-order birth) by dividing the number of infants (ART conceived and all infants) in each plurality group by the total number of infants born (ART conceived and all infants). The percentage of infants with low birthweight and preterm delivery was also calculated for each plurality group (singleton, twin, and triplet and higher-order births) for both ART-conceived infants and all infants by dividing the number of low birthweight or preterm infants in each plurality group by the total number of infants in that plurality group.
Content of This Report
This report provides information on U.S. ART procedures performed in 2014 and compares infant outcomes for ART-conceived infants born in 2014 (resulting from ART procedures performed in 2013 and 2014) with outcomes for all infants born in 2014 in the United States. Specifically, this report provides data on the number and outcomes of all ART procedures performed among patients residing in 52 reporting areas (the 50 states, the District of Columbia, and Puerto Rico) in 2014. For each of these reporting areas, data are presented on the number of ART procedures and embryo transfers performed; the resulting number of pregnancies, live-birth deliveries (overall, singleton, and multiple), and live-born infants; and the number of ART procedures in relation to the number of women in the reproductive age group (15–44 years) (23).* Data are also presented on the number of embryo-transfer procedures performed, the average number of embryos transferred, and the percentage of eSET procedures performed among women who used fresh embryos from their own eggs, by age group.
For each reporting area, the proportions of singletons and multiple-birth (including twin and triplet and higher-order) infants resulting from ART are compared with the respective proportions among all infants born in that location in 2014. Infants born in the reporting area during that year include those who were conceived naturally and those resulting from ART and other infertility treatments. To accurately assess the proportion of ART births among overall U.S. births in 2014, ART births were aggregated from two reporting years: 1) infants conceived with ART procedures performed in 2013 and born in 2014 (69.0% of the live-birth deliveries reported to the ART surveillance system for 2014) and 2) infants conceived with ART procedures performed in 2014 and born in 2014 (31.0% of the live-birth deliveries reported to the ART surveillance system for 2014). Data on the total number of live-birth and multiple-birth infants in each reporting area in 2014 were obtained from U.S. natality files (24). The report presents the number and percentage of select adverse perinatal outcomes (low birthweight, very low birthweight, preterm delivery, and very preterm delivery) among ART-conceived infants and all infants and the contribution of ART to these outcomes. The percentage of adverse perinatal outcomes is reported for singleton, twin, and triplet and higher-order infants for ART-conceived infants and all infants.
Results
Overview of Fertility Clinics
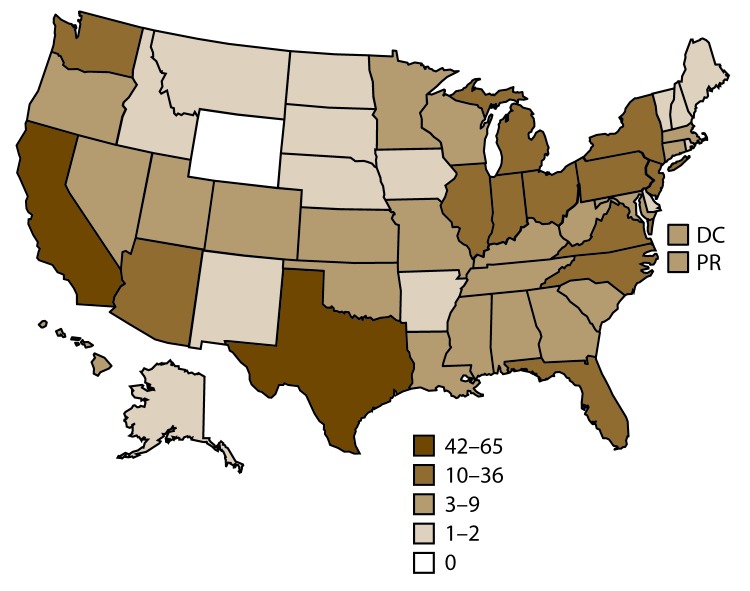
Of 498 fertility clinics in the United States that performed ART procedures in 2014, a total of 458 (92.2%) provided data to CDC, with the majority located in or near major cities in the United States. The number of fertility clinics performing ART procedures varied by reporting area. The reporting areas with the largest number of fertility clinics providing data for 2014 were California (65), Texas (42), New York (36), Florida (28), and Illinois (26) (Figure 1).
FIGURE 1.
Location and number* of assisted reproductive technology clinics — United States and Puerto Rico, 2014
Abbreviations: DC = District of Columbia; PR = Puerto Rico.
* In 2014, of the 498 clinics in the United States, 458 (92.2%) submitted data.
Number and Type of ART Procedures
The number, type, and outcome of ART procedures performed in 2014 are provided according to patient’s residence for all 52 reporting areas (Table 1). Residency data are missing for approximately 0.6% of procedures performed and 0.7% of live-birth deliveries; however, they are included in the totals. Approximately 16.6% of ART procedures were conducted in reporting areas other than the patient’s state of residence. Non-U.S. residents accounted for approximately 2.7% of ART procedures, 3.1% of ART live-birth deliveries, and 3.1% of ART infants born.
TABLE 1. Number* and outcomes of assisted reproductive technology procedures, by female patient’s reporting area of residence† at time of treatment — United States and Puerto Rico, 2014.
| Patient’s reporting area of residence | No. of ART clinics§ | No. of ART procedures performed | No. of ART embryo transfer procedures¶ | No. of ART pregnancies | No. of ART live-birth deliveries | No. of ART singleton live-birth deliveries | No. of ART multiple live-birth deliveries | No. of ART live-born infants | ART procedures per 1 million women aged 15–44 yrs** |
|---|---|---|---|---|---|---|---|---|---|
| Alabama |
6 |
1,060 |
849 |
431 |
361 |
262 |
99 |
462 |
1,102.9 |
| Alaska |
1 |
198 |
176 |
80 |
67 |
50 |
17 |
86 |
1,344.1 |
| Arizona |
11 |
2,116 |
1,808 |
972 |
794 |
605 |
189 |
993 |
1,617.7 |
| Arkansas |
1 |
457 |
388 |
187 |
165 |
118 |
47 |
212 |
795.1 |
| California†† |
65 |
21,018 |
17,429 |
8,972 |
7,230 |
5,700 |
1,530 |
8,793 |
2,607.2 |
| Colorado |
8 |
1,889 |
1,578 |
1,048 |
856 |
683 |
173 |
1,031 |
1,741.6 |
| Connecticut |
9 |
3,554 |
2,680 |
1,316 |
1,077 |
849 |
228 |
1,311 |
5,194.7 |
| Delaware |
2 |
646 |
520 |
283 |
239 |
220 |
19 |
260 |
3,580.9 |
| District of Columbia |
3 |
1,183 |
932 |
398 |
316 |
280 |
36 |
353 |
6,662.2 |
| Florida |
28 |
7,559 |
6,191 |
2,950 |
2,374 |
1,770 |
604 |
3,002 |
2,050.1 |
| Georgia†† |
8 |
3,640 |
3,065 |
1,579 |
1,293 |
1,022 |
271 |
1,574 |
1,729.6 |
| Hawaii†† |
5 |
1,119 |
847 |
486 |
407 |
291 |
116 |
527 |
4,179.9 |
| Idaho |
1 |
455 |
397 |
218 |
177 |
104 |
73 |
250 |
1,445.1 |
| Illinois |
26 |
10,671 |
8,476 |
4,096 |
3,317 |
2,542 |
775 |
4,098 |
4,109.8 |
| Indiana |
10 |
1,950 |
1,632 |
790 |
634 |
442 |
192 |
832 |
1,505.3 |
| Iowa |
2 |
1,217 |
1,007 |
634 |
512 |
394 |
118 |
630 |
2,078.1 |
| Kansas |
4 |
1,013 |
762 |
386 |
327 |
244 |
83 |
415 |
1,807.9 |
| Kentucky |
5 |
1,177 |
1,038 |
480 |
378 |
259 |
119 |
497 |
1,378.9 |
| Louisiana |
5 |
1,248 |
965 |
492 |
418 |
309 |
109 |
532 |
1,323.9 |
| Maine |
1 |
382 |
337 |
148 |
111 |
91 |
20 |
130 |
1,633.7 |
| Maryland |
7 |
5,590 |
4,519 |
2,200 |
1,720 |
1,481 |
239 |
1,965 |
4,650.9 |
| Massachusetts |
8 |
9,209 |
7,904 |
3,618 |
2,927 |
2,446 |
481 |
3,414 |
6,725.8 |
| Michigan |
12 |
3,616 |
3,006 |
1,454 |
1,164 |
851 |
313 |
1,484 |
1,915.5 |
| Minnesota |
4 |
2,012 |
1,775 |
993 |
853 |
663 |
190 |
1,045 |
1,910.1 |
| Mississippi |
3 |
593 |
482 |
229 |
194 |
134 |
60 |
254 |
986.3 |
| Missouri |
8 |
2,111 |
1,811 |
881 |
712 |
549 |
163 |
881 |
1,794.8 |
| Montana |
1 |
258 |
207 |
123 |
101 |
76 |
25 |
125 |
1,389.6 |
| Nebraska |
2 |
786 |
621 |
353 |
303 |
208 |
95 |
401 |
2,158.9 |
| Nevada |
5 |
1,246 |
957 |
544 |
449 |
341 |
108 |
560 |
2,200.4 |
| New Hampshire |
1 |
735 |
620 |
285 |
245 |
197 |
48 |
294 |
3,016.9 |
| New Jersey |
19 |
8,863 |
6,914 |
3,735 |
3,068 |
2,430 |
638 |
3,708 |
5,143.3 |
| New Mexico |
1 |
280 |
242 |
123 |
107 |
88 |
19 |
127 |
704.3 |
| New York |
36 |
20,814 |
16,212 |
6,982 |
5,447 |
4,349 |
1,098 |
6,558 |
5,144.6 |
| North Carolina |
12 |
3,693 |
2,903 |
1,542 |
1,261 |
968 |
293 |
1,556 |
1,862.4 |
| North Dakota |
1 |
311 |
252 |
128 |
99 |
76 |
23 |
123 |
2,157.8 |
| Ohio |
12 |
3,732 |
3,226 |
1,577 |
1,313 |
949 |
364 |
1,687 |
1,687.5 |
| Oklahoma |
3 |
815 |
696 |
351 |
309 |
206 |
103 |
415 |
1,068.6 |
| Oregon |
4 |
1,304 |
1,118 |
683 |
597 |
413 |
184 |
787 |
1,680.2 |
| Pennsylvania |
18 |
6,521 |
5,282 |
2,532 |
2,004 |
1,624 |
380 |
2,389 |
2,709.1 |
| Puerto Rico |
3 |
260 |
230 |
103 |
77 |
51 |
26 |
104 |
363.7 |
| Rhode Island |
1 |
701 |
599 |
266 |
210 |
165 |
45 |
256 |
3,336.3 |
| South Carolina |
5 |
1,394 |
1,175 |
589 |
483 |
361 |
122 |
608 |
1,477.5 |
| South Dakota |
1 |
266 |
217 |
95 |
78 |
62 |
16 |
96 |
1,684.7 |
| Tennessee |
9 |
1,525 |
1,264 |
660 |
568 |
416 |
152 |
724 |
1,177.0 |
| Texas |
42 |
12,750 |
10,223 |
5,406 |
4,471 |
3,341 |
1,130 |
5,636 |
2,254.8 |
| Utah |
3 |
1,492 |
1,309 |
809 |
668 |
471 |
197 |
870 |
2,333.5 |
| Vermont |
2 |
210 |
176 |
79 |
64 |
52 |
12 |
76 |
1,810.6 |
| Virginia |
13 |
5,904 |
4,781 |
2,238 |
1,795 |
1,493 |
302 |
2,103 |
3,505.7 |
| Washington |
12 |
3,261 |
2,620 |
1,414 |
1,161 |
946 |
215 |
1,381 |
2,331.8 |
| West Virginia |
3 |
298 |
259 |
128 |
107 |
82 |
25 |
134 |
885.0 |
| Wisconsin |
7 |
1,759 |
1,473 |
759 |
650 |
489 |
161 |
819 |
1,617.8 |
| Wyoming |
0 |
124 |
107 |
62 |
52 |
41 |
11 |
64 |
1,118.9 |
| Nonresident |
NA |
4,583 |
3,772 |
2,101 |
1,718 |
1,290 |
428 |
2,150 |
—§§ |
| Total | 458 | 169,568 | 138,029 | 68,988 | 56,028 | 43,544 | 12,484 | 68,782 | 2,646.5 |
Abbreviations: ART = assisted reproductive technology; NA = not applicable.
* Excludes 35,406 egg/embryo-freezing and embryo-banking procedures, 3,596 oocyte thaw procedures, and 34 procedures performed in territories not included in this report.
† In cases of missing residency data (0.6%), the patient’s residence was assigned as the location in which the ART procedure was performed.
§ The ART procedures and outcomes by patient's reporting area of residence do not necessarily reflect the procedures and outcomes of the ART clinics within the reporting area, as some patients seek treatment at a clinic in a location other than their area of residence.
¶ Embryo transfer procedures include all procedures performed in which an attempt was made to transfer at least one embryo.
** On the basis of U.S. Census Bureau estimates (23).
†† In three states, >2% of residency information was missing for procedures performed: California (2.7%), Georgia (2.1%), and Hawaii (2.1%). Overall, residency information was missing for 963 (0.6%) procedures performed and 366 (0.7%) live-birth deliveries.
§§ Non-U.S. residents excluded from rate because the appropriate denominators were not available.
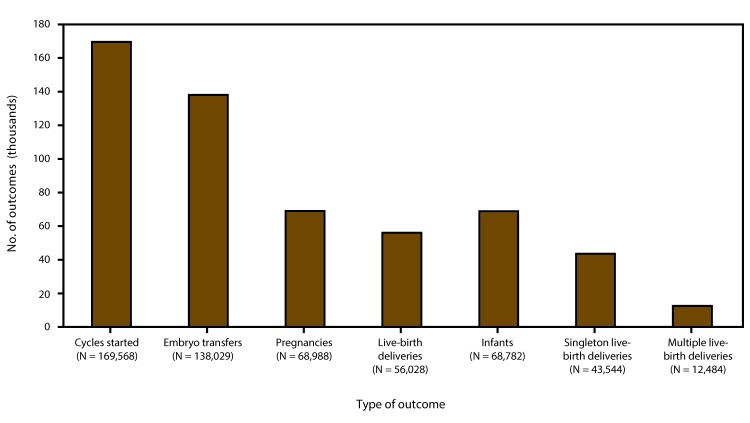
In 2014, a total of 208,604 ART procedures were reported to CDC (1). This report includes data for 169,568 ART procedures performed in the United States (including Puerto Rico) with the intent to transfer at least one embryo (Table 1). It excludes 35,406 egg/embryo-freezing and embryo-banking procedures that did not result in an embryo transfer; 3,596 oocyte-thaw procedures; and 34 procedures that were performed in the remaining territories. Of 169,568 procedures performed in the reporting areas, a total of 138,029 (81.4%) progressed to embryo transfer (Table 1). Of 138,029 ART procedures that progressed to the embryo-transfer stage, 68,988 (50.0%) resulted in a pregnancy and 56,028 (40.6%) in a live-birth delivery. The 56,028 live-birth deliveries included 43,544 singleton live-birth deliveries (77.7%) and 12,484 multiple live-birth deliveries (22.3%) and resulted in 68,782 live-born infants (Table 1) (Figure 2).
FIGURE 2.
Number of outcomes of assisted reproductive technology procedures, by type of outcome — United States and Puerto Rico, 2014
Six reporting areas with the largest number of ART procedures (California, Illinois, Massachusetts, New Jersey, New York, and Texas) accounted for 49.1% (83,325 of 169,568) of all ART procedures, 48.6% (67,158 of 138,029) of all embryo-transfer procedures, 46.8% (32,207 of 68,782) of all infants born from ART, and 45.3% (5,652 of 12,484) of all ART multiple live-birth deliveries in the United States (Table 1); however, these six reporting areas accounted for only 36.7% of all U.S. births (24).
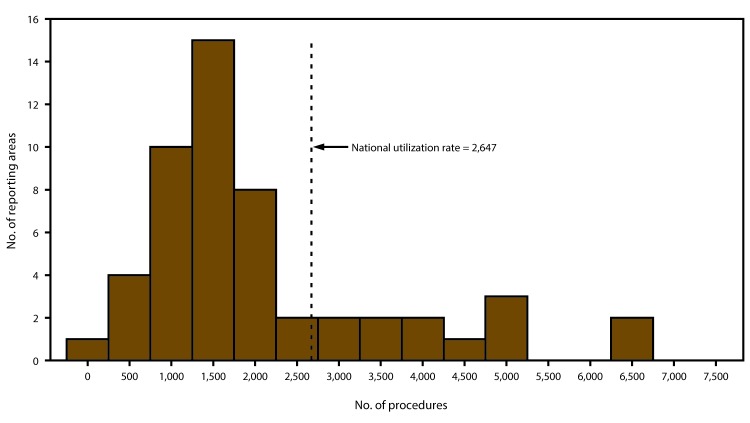
The number of ART procedures per 1 million women of reproductive age (15–44 years) varied from 364 in Puerto Rico to 6,726 in Massachusetts, with an overall national rate of 2,647. Thirteen reporting areas (Connecticut, Delaware, Hawaii, Illinois, Maryland, Massachusetts, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Virginia, and the District of Columbia) had rates higher than the national rate. Of these reporting areas, Massachusetts (6,726) and the District of Columbia (6,662) had rates exceeding twice the national rate, while Connecticut (5,195), Hawaii (4,180), Illinois (4,110), Maryland (4,651), New Jersey (5,143) and New York (5,145) had rates exceeding 1.5 times the national rate (Table 1) (Figure 3).
FIGURE 3.
Number of reporting areas by number of assisted reproductive technology procedures performed among women of reproductive age (15–44 years)* — United States and Puerto Rico, 2014
* Per 1 million women aged 15–44 years.
Embryo Transfer and Patient’s Age
The number of embryo-transfer procedures performed, the average number of embryos transferred per procedure, and the percentage of eSET procedures performed among women who used fresh embryos from their own eggs are provided by reporting area and age group (Table 2). Overall, the number of embryo-transfer procedures performed was 30,887 among women aged <35 years, 14,647 among women aged 35–37 years, and 21,504 among women aged >37 years. Nationally, the average number of embryos transferred per procedure was 1.7 among women aged <35 years (range: 1.3 in Delaware to 2.1 in Puerto Rico), 1.9 among women aged 35–37 years (range: 1.5 in Maine to 2.3 in Hawaii), and 2.3 among women aged >37 years (range: 1.9 in Nevada to 3.0 in Montana). Nationally, percentage of eSET was 28.5% among women aged <35 years (range: 4.3% in Puerto Rico to 67.9% in Delaware), 16.7% among women aged 35–37 years (range: 0% in South Dakota to 39.5% in Maine), and 4.7% among women aged >37 years (range: 0% in 9 reporting areas to 12.5% in Delaware and Idaho). Among women aged <35 years, eSET percentage exceeded 1.5 times the national rate in six reporting areas (Delaware, the District of Columbia, Maine, Massachusetts, Maryland, and New Hampshire).
TABLE 2. Number of assisted reproductive technology embryo transfer procedures* among patients who used fresh embryos from their own eggs, by female patient’s age group and reporting area of residence† at time of treatment — United States and Puerto Rico, 2014.
| Patient’s reporting area of residence | <35 yrs |
35–37 yrs |
>37 yrs |
||||||
|---|---|---|---|---|---|---|---|---|---|
| No. of embryo transfer procedures | Average no. of embryos transferred | eSET§ (%) | No. of embryo transfer procedures | Average no. of embryos transferred | eSET§ (%) | No. of embryo transfer procedures | Average no. of embryos transferred | eSET§ (%) | |
| Alabama |
297 |
1.8 |
16.4 |
98 |
2.1 |
6.6 |
79 |
2.7 |
0.0 |
| Alaska |
47 |
1.8 |
26.8 |
27 |
1.9 |
18.2 |
15 |
—¶ |
—¶ |
| Arizona |
331 |
1.8 |
24.5 |
148 |
2.1 |
6.7 |
178 |
2.3 |
2.7 |
| Arkansas |
136 |
1.8 |
14.8 |
40 |
2.0 |
2.9 |
27 |
2.0 |
0.0 |
| California** |
2,543 |
1.7 |
29.7 |
1,650 |
1.9 |
19.0 |
2,859 |
2.6 |
3.8 |
| Colorado |
200 |
1.8 |
22.6 |
79 |
2.0 |
8.6 |
50 |
2.3 |
4.9 |
| Connecticut |
731 |
1.6 |
32.1 |
348 |
1.8 |
14.1 |
563 |
2.3 |
1.9 |
| Delaware |
89 |
1.3 |
67.9 |
23 |
1.7 |
36.8 |
34 |
2.1 |
12.5 |
| District of Columbia |
110 |
1.4 |
60.4 |
107 |
1.6 |
35.4 |
261 |
2.1 |
8.2 |
| Florida |
1,477 |
1.7 |
23.7 |
715 |
1.9 |
9.1 |
1,031 |
2.3 |
2.5 |
| Georgia** |
697 |
1.6 |
35.5 |
306 |
1.9 |
11.5 |
345 |
2.4 |
3.0 |
| Hawaii** |
114 |
1.9 |
17.4 |
87 |
2.3 |
4.9 |
179 |
2.7 |
2.6 |
| Idaho |
120 |
1.9 |
13.4 |
46 |
2.1 |
2.4 |
30 |
2.0 |
12.5 |
| Illinois |
2,091 |
1.7 |
27.2 |
945 |
1.9 |
13.1 |
1,388 |
2.3 |
2.7 |
| Indiana |
620 |
1.9 |
10.4 |
189 |
2.0 |
9.0 |
175 |
2.2 |
2.1 |
| Iowa |
310 |
1.6 |
39.6 |
80 |
1.7 |
26.5 |
77 |
2.3 |
4.3 |
| Kansas |
239 |
1.7 |
23.3 |
61 |
2.0 |
3.6 |
53 |
2.1 |
2.1 |
| Kentucky |
372 |
1.9 |
18.3 |
132 |
1.9 |
8.3 |
106 |
2.3 |
1.1 |
| Louisiana |
293 |
1.9 |
11.2 |
69 |
2.0 |
4.8 |
97 |
2.2 |
6.2 |
| Maine |
91 |
1.4 |
58.7 |
46 |
1.5 |
39.5 |
60 |
2.0 |
8.3 |
| Maryland |
1,121 |
1.4 |
51.8 |
592 |
1.6 |
35.1 |
918 |
2.1 |
8.4 |
| Massachusetts |
1,930 |
1.4 |
51.5 |
1,137 |
1.6 |
32.1 |
1,952 |
2.5 |
7.0 |
| Michigan |
861 |
1.9 |
15.0 |
308 |
2.0 |
10.5 |
370 |
2.3 |
4.1 |
| Minnesota |
571 |
1.7 |
30.2 |
175 |
1.8 |
17.3 |
194 |
2.0 |
7.8 |
| Mississippi |
120 |
1.8 |
22.4 |
43 |
2.0 |
5.3 |
52 |
2.1 |
0.0 |
| Missouri |
601 |
1.8 |
13.5 |
183 |
2.0 |
6.3 |
154 |
2.6 |
0.0 |
| Montana |
70 |
1.6 |
36.9 |
16 |
—¶ |
—¶ |
28 |
3.0 |
0.0 |
| Nebraska |
211 |
1.8 |
12.8 |
72 |
1.8 |
7.0 |
46 |
2.3 |
0.0 |
| Nevada |
191 |
1.7 |
24.4 |
73 |
1.7 |
16.9 |
92 |
1.9 |
10.0 |
| New Hampshire |
189 |
1.4 |
51.0 |
99 |
1.6 |
29.9 |
93 |
2.4 |
3.8 |
| New Jersey |
1,310 |
1.6 |
34.7 |
699 |
1.8 |
19.1 |
1,054 |
2.2 |
8.2 |
| New Mexico |
31 |
1.8 |
17.9 |
8 |
—¶ |
—¶ |
13 |
—¶ |
—¶ |
| New York |
3,075 |
1.7 |
30.0 |
1,835 |
1.9 |
15.5 |
3,883 |
2.3 |
5.2 |
| North Carolina |
621 |
1.7 |
28.1 |
280 |
1.8 |
15.9 |
310 |
2.4 |
3.3 |
| North Dakota |
89 |
1.8 |
17.2 |
22 |
1.9 |
9.5 |
25 |
2.2 |
4.5 |
| Ohio |
1,087 |
1.9 |
14.9 |
442 |
2.0 |
6.5 |
393 |
2.4 |
2.9 |
| Oklahoma |
303 |
1.9 |
6.2 |
76 |
1.9 |
3.2 |
62 |
2.4 |
0.0 |
| Oregon |
248 |
1.9 |
15.2 |
123 |
1.8 |
15.8 |
89 |
2.2 |
9.0 |
| Pennsylvania |
1,357 |
1.7 |
33.9 |
629 |
1.9 |
16.6 |
743 |
2.3 |
5.9 |
| Puerto Rico |
74 |
2.1 |
4.3 |
48 |
2.2 |
4.7 |
59 |
2.4 |
0.0 |
| Rhode Island |
162 |
1.6 |
34.5 |
96 |
1.9 |
11.4 |
138 |
2.6 |
4.1 |
| South Carolina |
265 |
1.9 |
14.7 |
120 |
2.0 |
6.4 |
154 |
2.4 |
4.5 |
| South Dakota |
68 |
1.7 |
30.2 |
21 |
1.9 |
0 |
14 |
—¶ |
—¶ |
| Tennessee |
316 |
1.8 |
22.8 |
115 |
2.0 |
6.7 |
111 |
2.4 |
2.2 |
| Texas |
2,128 |
1.8 |
21.1 |
933 |
2.0 |
8.4 |
1,139 |
2.3 |
1.6 |
| Utah |
478 |
1.8 |
18.0 |
137 |
2.0 |
7.1 |
118 |
2.2 |
3.1 |
| Vermont |
50 |
1.7 |
21.4 |
34 |
1.8 |
19.4 |
33 |
2.3 |
3.2 |
| Virginia |
1,038 |
1.5 |
40.3 |
540 |
1.7 |
31.1 |
894 |
2.1 |
7.2 |
| Washington |
540 |
1.6 |
38.0 |
235 |
1.7 |
24.8 |
297 |
2.1 |
6.4 |
| West Virginia |
92 |
1.8 |
18.5 |
30 |
1.9 |
8.3 |
27 |
2.4 |
0.0 |
| Wisconsin |
429 |
1.7 |
27.1 |
134 |
1.8 |
18.5 |
125 |
2.2 |
4.6 |
| Wyoming |
37 |
1.8 |
13.9 |
11 |
—¶ |
—¶ |
6 |
—¶ |
—¶ |
| Nonresident |
316 |
1.8 |
22.8 |
185 |
1.7 |
19.9 |
311 |
2.2 |
8.9 |
| Total | 30,887 | 1.7 | 28.5 | 14,647 | 1.9 | 16.7 | 21,504 | 2.3 | 4.7 |
Abbreviation: eSET = elective single-embryo transfer.
* Includes all procedures in which at least one embryo was transferred.
† In cases of missing residency data (0.6%), the patient's residence was assigned as the location in which the assisted reproductive technology procedure was performed.
§ A procedure in which one embryo, selected from a larger number of available embryos, is placed in the uterus. A cycle in which only one embryo is available is not defined as eSET.
¶ Estimates on the basis of N <20 in the denominator have been suppressed because such rates are considered unstable.
** In three states, >2% of residency information was missing for procedures performed: California (2.7%), Georgia (2.1%), and Hawaii (2.1%). Overall, residency information was missing for 963 (0.6%) procedures performed and 366 (0.7%) live-birth deliveries.
Singleton and Multiple-Birth Infants
Among 4,022,510 infants born in the United States and Puerto Rico in 2014 (21), a total of 65,296 (1.6%) were conceived with ART procedures performed in 2013 and 2014 (Table 3). California, Texas, and New York had the highest total number of all infants born (502,879, 399,766, and 238,773, respectively), as well as ART-conceived infants born (8,528, 5,268, and 6,492, respectively). The contribution of ART to all infants born was highest in Massachusetts (4.7%), followed by the District of Columbia (3.8%), New Jersey (3.7%), and Connecticut (3.6%). Although singletons accounted for 96.5% of all infants born in 2014 (range: 95.6% in New Jersey to 97.8% in Puerto Rico), singletons accounted for only 60.6% of all ART-conceived infants (range: 44.4% in Puerto Rico to 88.5% in Delaware).
TABLE 3. Number, proportion, and percentage of infants born with the use of assisted reproductive technology, by female patient's reporting area of residence* at time of treatment — United States and Puerto Rico, 2014†.
| Patient’s reporting area of residence | Total no. of infants born§ | No. of ART infants born | Proportion of ART infants among all infants (%) | Singleton infants among ART infants |
Singleton infants among all infants§ |
Proportion of ART singleton infants among all singleton infants (%) |
|---|---|---|---|---|---|---|
| No. (%) | No. (%) | |||||
| Alabama |
59,422 |
466 |
0.8 |
231 (49.6) |
57,307 (96.4) |
0.4 |
| Alaska |
11,392 |
56 |
0.5 |
36 (64.3) |
11,031 (96.8) |
0.3 |
| Arizona |
86,887 |
1,030 |
1.2 |
616 (59.8) |
84,240 (97.0) |
0.7 |
| Arkansas |
38,511 |
196 |
0.5 |
118 (60.2) |
37,358 (97.0) |
0.3 |
| California¶ |
502,879 |
8,528 |
1.7 |
5,389 (63.2) |
486,558 (96.8) |
1.1 |
| Colorado |
65,830 |
993 |
1.5 |
580 (58.4) |
63,748 (96.8) |
0.9 |
| Connecticut |
36,285 |
1,321 |
3.6 |
829 (62.8) |
34,715 (95.7) |
2.4 |
| Delaware |
10,972 |
226 |
2.1 |
200 (88.5) |
10,654 (97.1) |
1.9 |
| District of Columbia |
9,509 |
361 |
3.8 |
283 (78.4) |
9,153 (96.3) |
3.1 |
| Florida |
219,991 |
2,900 |
1.3 |
1,641 (56.6) |
212,467 (96.6) |
0.8 |
| Georgia¶ |
130,946 |
1,487 |
1.1 |
886 (59.6) |
126,403 (96.5) |
0.7 |
| Hawaii¶ |
18,550 |
447 |
2.4 |
230 (51.5) |
17,969 (96.9) |
1.3 |
| Idaho |
22,876 |
218 |
1.0 |
116 (53.2) |
22,186 (97.0) |
0.5 |
| Illinois |
158,556 |
4,074 |
2.6 |
2,459 (60.4) |
152,251 (96.0) |
1.6 |
| Indiana |
84,080 |
814 |
1.0 |
431 (52.9) |
81,163 (96.5) |
0.5 |
| Iowa |
39,687 |
629 |
1.6 |
399 (63.4) |
38,256 (96.4) |
1.0 |
| Kansas |
39,223 |
361 |
0.9 |
216 (59.8) |
37,964 (96.8) |
0.6 |
| Kentucky |
56,170 |
508 |
0.9 |
247 (48.6) |
54,304 (96.7) |
0.5 |
| Louisiana |
64,497 |
542 |
0.8 |
284 (52.4) |
62,124 (96.3) |
0.5 |
| Maine |
12,698 |
146 |
1.1 |
95 (65.1) |
12,224 (96.3) |
0.8 |
| Maryland |
73,921 |
1,956 |
2.6 |
1,423 (72.8) |
71,056 (96.1) |
2.0 |
| Massachusetts |
71,908 |
3,413 |
4.7 |
2,302 (67.4) |
68,839 (95.7) |
3.3 |
| Michigan |
11,4375 |
1,503 |
1.3 |
830 (55.2) |
110,146 (96.3) |
0.8 |
| Minnesota |
69,904 |
1,172 |
1.7 |
689 (58.8) |
67,312 (96.3) |
1.0 |
| Mississippi |
38,736 |
248 |
0.6 |
145 (58.5) |
37,390 (96.5) |
0.4 |
| Missouri |
75,360 |
870 |
1.2 |
492 (56.6) |
72,727 (96.5) |
0.7 |
| Montana |
12,432 |
128 |
1.0 |
65 (50.8) |
12,004 (96.6) |
0.5 |
| Nebraska |
26,794 |
351 |
1.3 |
168 (47.9) |
25,859 (96.5) |
0.6 |
| Nevada |
35,861 |
559 |
1.6 |
332 (59.4) |
34,726 (96.8) |
1.0 |
| New Hampshire |
12,302 |
295 |
2.4 |
184 (62.4) |
11,844 (96.3) |
1.6 |
| New Jersey |
103,305 |
3,786 |
3.7 |
2,384 (63.0) |
98,805 (95.6) |
2.4 |
| New Mexico |
26,052 |
129 |
0.5 |
81 (62.8) |
25,445 (97.7) |
0.3 |
| New York |
238,773 |
6,492 |
2.7 |
4,175 (64.3) |
229,570 (96.1) |
1.8 |
| North Carolina |
120,975 |
1,559 |
1.3 |
898 (57.6) |
116,626 (96.4) |
0.8 |
| North Dakota |
11,359 |
142 |
1.3 |
77 (54.2) |
10,977 (96.6) |
0.7 |
| Ohio |
139,467 |
1,672 |
1.2 |
882 (52.8) |
134,327 (96.3) |
0.7 |
| Oklahoma |
53,339 |
419 |
0.8 |
213 (50.8) |
51,681 (96.9) |
0.4 |
| Oregon |
45,556 |
672 |
1.5 |
338 (50.3) |
43,941 (96.5) |
0.8 |
| Pennsylvania |
142,268 |
2,442 |
1.7 |
1,540 (63.1) |
136,985 (96.3) |
1.1 |
| Puerto Rico |
34,434 |
133 |
0.4 |
59 (44.4) |
33,663 (97.8) |
0.2 |
| Rhode Island |
10,823 |
232 |
2.1 |
147 (63.4) |
10,453 (96.6) |
1.4 |
| South Carolina |
57,627 |
548 |
1.0 |
309 (56.4) |
55,548 (96.4) |
0.6 |
| South Dakota |
12,283 |
126 |
1.0 |
68 (54.0) |
11,882 (96.7) |
0.6 |
| Tennessee |
81,602 |
634 |
0.8 |
362 (57.1) |
78,919 (96.7) |
0.5 |
| Texas |
399,766 |
5,268 |
1.3 |
2,892 (54.9) |
386,674 (96.7) |
0.7 |
| Utah |
51,154 |
730 |
1.4 |
349 (47.8) |
49,287 (96.4) |
0.7 |
| Vermont |
6,130 |
107 |
1.7 |
56 (52.3) |
5,874 (95.8) |
1.0 |
| Virginia |
103,300 |
2,163 |
2.1 |
1,467 (67.8) |
99,469 (96.3) |
1.5 |
| Washington |
88,585 |
1,299 |
1.5 |
808 (62.2) |
85,847 (96.9) |
0.9 |
| West Virginia |
20,301 |
101 |
0.5 |
64 (63.4) |
19,623 (96.7) |
0.3 |
| Wisconsin |
67,161 |
790 |
1.2 |
464 (58.7) |
64,864 (96.6) |
0.7 |
| Wyoming |
7,696 |
54 |
0.7 |
33 (61.1) |
7,439 (96.7) |
0.4 |
| Total | 4,022,510 | 65,296 | 1.6 | 39,582 (60.6) | 3,881,877 (96.5) | 1.0 |
Abbreviation: ART = assisted reproductive technology.
* In cases of missing residency data (0.6%), the patient's residence was assigned as the location in which the ART procedure was performed.
† Includes infants conceived from ART procedures performed in 2013 and born in 2014 and infants conceived from ART procedures performed in 2014 and born in 2014. Total ART births exclude nonresidents.
§ U.S. births include nonresidents (24).
¶ In three states, >2% of residency information was missing for procedures performed: California (2.7%), Georgia (2.1%), and Hawaii (2.1%). Overall, residency information was missing for 963 (0.6%) procedures performed and 366 (0.7%) live-birth deliveries.
Nationwide, 39.4% of ART-conceived infants were born in multiple-birth deliveries (range: 11.5% in Delaware to 55.6% in Puerto Rico), compared with only 3.5% of all infants (range: 2.2% in Puerto Rico to 4.4% in New Jersey) (Table 4). ART-conceived twins accounted for approximately 95.3% (24,514 of 25,714) of all ART-conceived infants born in multiple deliveries. ART multiple-birth infants contributed to 18.3% of all multiple-birth infants (range: 5.5% in Alaska and West Virginia to 37.3% in Hawaii). Approximately 37.5% of all ART-conceived infants were twins (range: 11.5% in Delaware to 51.1% in Puerto Rico), compared with 3.4% of all infants (range: 2.2% in New Mexico and Puerto Rico to 4.2% in Connecticut, Massachusetts, and New Jersey). ART-conceived twin infants contributed to 18.0% of all twins born in 2014 (range: 5.2% in some states to 36.2% in Hawaii). Finally, 1.8% of ART-conceived infants were triplets and higher-order multiples (range: 0% in Alaska, Delaware, and Montana to 5.6% in some states), compared with 0.1%–0.2% of all infants. ART triplet and higher-order infants contributed to 26.4% of all triplet and higher-order infants born in 2014 (range: 0% in Alaska, Delaware, and Montana to 65.2% in Hawaii).
TABLE 4. Number, percentage, and proportion of multiple-birth, twins, and triplets and higher-order infants born with use of assisted reproductive technology procedure, by female patient’s reporting area of residence* at time of treatment — United States and Puerto Rico, 2014†.
| Patient’s reporting area of residence | Multiple-birth infants among ART infants§ |
Multiple-birth infants among all infants¶ |
Proportion of ART multiple-birth infants among all multiple-birth infants (%) | Twin infants among ART infants§ |
Twin infants among all infants¶ |
Proportion of ART twin infants among all twin infants (%) | Triplets and higher-order infants among ART infants§ |
Triplets and higher-order infants among all infants¶ |
Proportion of ART triplets and higher-order infants among all triplets and higher-order infants (%) |
|---|---|---|---|---|---|---|---|---|---|
| No. (%) | No. (%) | No. (%) | No. (%) | No. (%) | No. (%) | ||||
| Alabama |
235 (50.4) |
2,115 (3.6) |
11.1 |
229 (49.1) |
2,072 (3.5) |
11.1 |
6 (1.3) |
43 (0.1) |
14.0 |
| Alaska |
20 (35.7) |
361 (3.2) |
5.5 |
20 (35.7) |
— (—)** |
—** |
0 (0.0) |
— (—)** |
0.0 |
| Arizona |
414 (40.2) |
2,647 (3.0) |
15.6 |
392 (38.1) |
2,579 (3.0) |
15.2 |
22 (2.1) |
68 (0.1) |
32.4 |
| Arkansas |
78 (39.8) |
1,153 (3.0) |
6.8 |
72 (36.7) |
1,110 (2.9) |
6.5 |
6 (3.1) |
43 (0.1) |
14.0 |
| California¶¶ |
3,139 (36.8) |
16,321 (3.2) |
19.2 |
2,976 (34.9) |
15,832 (3.1) |
18.8 |
163 (1.9) |
489 (0.1) |
33.3 |
| Colorado |
413 (41.6) |
2,082 (3.2) |
19.8 |
392 (39.5) |
2,019 (3.1) |
19.4 |
21 (2.1) |
63 (0.1) |
33.3 |
| Connecticut |
492 (37.2) |
1,570 (4.3) |
31.3 |
474 (35.9) |
1,525 (4.2) |
31.1 |
18 (1.4) |
45 (0.1) |
40.0 |
| Delaware |
26 (11.5) |
318 (2.9) |
8.2 |
26 (11.5) |
— (—)** |
—** |
0 (0.0) |
— (—)** |
0.0 |
| District of Columbia |
78 (21.6) |
356 (3.7) |
21.9 |
72 (19.9) |
344 (3.6) |
20.9 |
6 (1.7) |
12 (0.1) |
—†† |
| Florida |
1,259 (43.4) |
7,524 (3.4) |
16.7 |
1,190 (41.0) |
7,307 (3.3) |
16.3 |
69 (2.4) |
217 (0.1) |
31.8 |
| Georgia¶¶ |
601 (40.4) |
4,543 (3.5) |
13.2 |
571 (38.4) |
4,411 (3.4) |
12.9 |
30 (2.0) |
132 (0.1) |
22.7 |
| Hawaii¶¶ |
217 (48.5) |
581 (3.1) |
37.3 |
202 (45.2) |
558 (3.0) |
36.2 |
15 (3.4) |
23 (0.1) |
65.2 |
| Idaho |
102 (46.8) |
690 (3.0) |
14.8 |
— (—)** |
678 (3.0) |
—** |
— (—)** |
12 (0.1) |
—**,†† |
| Illinois |
1,615 (39.6) |
6,305 (4.0) |
25.6 |
1,552 (38.1) |
6,085 (3.8) |
25.5 |
63 (1.5) |
220 (0.1) |
28.6 |
| Indiana |
383 (47.1) |
2,917 (3.5) |
13.1 |
359 (44.1) |
2,799 (3.3) |
12.8 |
24 (2.9) |
118 (0.1) |
20.3 |
| Iowa |
230 (36.6) |
1,431 (3.6) |
16.1 |
— (—)** |
1,365 (3.4) |
—** |
— (—)** |
66 (0.2) |
—** |
| Kansas |
145 (40.2) |
1,259 (3.2) |
11.5 |
130 (36.0) |
1,213 (3.1) |
10.7 |
15 (4.2) |
46 (0.1) |
32.6 |
| Kentucky |
261 (51.4) |
1,866 (3.3) |
14.0 |
234 (46.1) |
1,794 (3.2) |
13.0 |
27 (5.3) |
72 (0.1) |
37.5 |
| Louisiana |
258 (47.6) |
2,373 (3.7) |
10.9 |
246 (45.4) |
2,295 (3.6) |
10.7 |
12 (2.2) |
78 (0.1) |
15.4 |
| Maine |
51 (34.9) |
474 (3.7) |
10.8 |
— (—)** |
453 (3.6) |
—** |
— (—)** |
21 (0.2) |
—** |
| Maryland |
533 (27.2) |
2,865 (3.9) |
18.6 |
516 (26.4) |
2,783 (3.8) |
18.5 |
17 (0.9) |
82 (0.1) |
20.7 |
| Massachusetts |
1,111 (32.6) |
3,069 (4.3) |
36.2 |
1,066 (31.2) |
2,986 (4.2) |
35.7 |
45 (1.3) |
83 (0.1) |
54.2 |
| Michigan |
673 (44.8) |
4,229 (3.7) |
15.9 |
643 (42.8) |
4,100 (3.6) |
15.7 |
30 (2.0) |
129 (0.1) |
23.3 |
| Minnesota |
483 (41.2) |
2,592 (3.7) |
18.6 |
469 (40.0) |
2,535 (3.6) |
18.5 |
14 (1.2) |
57 (0.1) |
24.6 |
| Mississippi |
103 (41.5) |
1,346 (3.5) |
7.7 |
97 (39.1) |
1,316 (3.4) |
7.4 |
6 (2.4) |
30 (0.1) |
20.0 |
| Missouri |
378 (43.4) |
2,633 (3.5) |
14.4 |
363 (41.7) |
2,567 (3.4) |
14.1 |
15 (1.7) |
66 (0.1) |
22.7 |
| Montana |
63 (49.2) |
428 (3.4) |
14.7 |
63 (49.2) |
420 (3.4) |
15.0 |
0 (0.0) |
8 (0.1) |
0.0 |
| Nebraska |
183 (52.1) |
935 (3.5) |
19.6 |
168 (47.9) |
878 (3.3) |
19.1 |
15 (4.3) |
57 (0.2) |
26.3 |
| Nevada |
227 (40.6) |
1,135 (3.2) |
20.0 |
— (—)** |
1,109 (3.1) |
—** |
— (—)** |
26 (0.1) |
—** |
| New Hampshire |
111 (37.6) |
458 (3.7) |
24.2 |
— (—)** |
452 (3.7) |
—** |
— (—)** |
6 (0.0) |
—**,†† |
| New Jersey |
1,402 (37.0) |
4,500 (4.4) |
31.2 |
1,360 (35.9) |
4,343 (4.2) |
31.3 |
42 (1.1) |
157 (0.2) |
26.8 |
| New Mexico |
48 (37.2) |
607 (2.3) |
7.9 |
42 (32.6) |
580 (2.2) |
7.2 |
6 (4.7) |
27 (0.1) |
22.2 |
| New York |
2,317 (35.7) |
9,203 (3.9) |
25.2 |
2,198 (33.9) |
8,840 (3.7) |
24.9 |
119 (1.8) |
363 (0.2) |
32.8 |
| North Carolina |
661 (42.4) |
4,349 (3.6) |
15.2 |
643 (41.2) |
4,233 (3.5) |
15.2 |
18 (1.2) |
116 (0.1) |
15.5 |
| North Dakota |
65 (45.8) |
382 (3.4) |
17.0 |
— (—)** |
360 (3.2) |
—** |
— (—)** |
22 (0.2) |
—** |
| Ohio |
790 (47.2) |
5,140 (3.7) |
15.4 |
741 (44.3) |
4,904 (3.5) |
15.1 |
49 (2.9) |
236 (0.2) |
20.8 |
| Oklahoma |
206 (49.2) |
1,658 (3.1) |
12.4 |
189 (45.1) |
1,582 (3.0) |
11.9 |
17 (4.1) |
76 (0.1) |
22.4 |
| Oregon |
334 (49.6) |
1,615 (3.5) |
20.7 |
328 (48.7) |
1,572 (3.5) |
20.9 |
6 (0.9) |
43 (0.1) |
14.0 |
| Pennsylvania |
902 (36.9) |
5,283 (3.7) |
17.1 |
875 (35.8) |
5,158 (3.6) |
17.0 |
27 (1.1) |
125 (0.1) |
21.6 |
| Puerto Rico |
74 (55.6) |
771 (2.2) |
9.6 |
68 (51.1) |
750 (2.2) |
9.1 |
6 (4.5) |
21 (0.1) |
28.6 |
| Rhode Island |
85 (36.6) |
370 (3.4) |
23.0 |
— (—)** |
358 (3.3) |
—** |
— (—)** |
12 (0.1) |
—**,†† |
| South Carolina |
239 (43.6) |
2,079 (3.6) |
11.5 |
— (—)** |
2,030 (3.5) |
—** |
— (—)** |
49 (0.1) |
—** |
| South Dakota |
58 (46.0) |
401 (3.3) |
14.5 |
52 (41.3) |
389 (3.2) |
13.4 |
6 (4.8) |
12 (0.1) |
—†† |
| Tennessee |
272 (42.9) |
2,683 (3.3) |
10.1 |
258 (40.7) |
2,596 (3.2) |
9.9 |
14 (2.2) |
87 (0.1) |
16.1 |
| Texas |
2,376 (45.1) |
13,092 (3.3) |
18.1 |
2,238 (42.5) |
12,600 (3.2) |
17.8 |
138 (2.6) |
492 (0.1) |
28.0 |
| Utah |
381 (52.2) |
1,867 (3.6) |
20.4 |
365 (50.0) |
1,797 (3.5) |
20.3 |
16 (2.2) |
70 (0.1) |
22.9 |
| Vermont |
51 (47.7) |
256 (4.2) |
19.9 |
— (—)** |
250 (4.1) |
—** |
— (—)** |
6 (0.1) |
—**,†† |
| Virginia |
696 (32.2) |
3,831 (3.7) |
18.2 |
662 (30.6) |
3,682 (3.6) |
18.0 |
34 (1.6) |
149 (0.1) |
22.8 |
| Washington |
491 (37.7) |
2,738 (3.1) |
17.9 |
470 (36.0) |
2,660 (3.0) |
17.7 |
21 (1.6) |
78 (0.1) |
26.9 |
| West Virginia |
37 (36.6) |
678 (3.3) |
5.5 |
— (—)** |
657 (3.2) |
—** |
— (—)** |
21 (0.1) |
—** |
| Wisconsin |
326 (41.3) |
2,297 (3.4) |
14.2 |
317 (40.1) |
2,236 (3.3) |
14.2 |
9 (1.1) |
61 (0.1) |
14.8 |
| Wyoming |
21 (38.9) |
257 (3.3) |
8.2 |
— (—)** |
251 (3.3) |
—** |
— (—)** |
6 (0.1) |
—**,†† |
| Total | 25,714 (39.4) | 140,633 (3.5) | 18.3 | 24,514 (37.5) | 136,086 (3.4) | 18.0 | 1,200 (1.8) | 4,547 (0.1) | 26.4 |
Abbreviation: ART = assisted reproductive technology.
* In cases of missing residency data (0.6%), the patient's residence was assigned as the location in which the ART procedure was performed.
† ART totals include infants conceived from ART procedures performed in 2013 and born in 2014 and infants conceived from ART procedures performed in 2014 and born in 2014. Total ART births exclude nonresidents.
§ Includes only the number of infants live-born in a multiple-birth delivery. For example, if three infants were born in a live-birth delivery and one of the three infants was stillborn, the total number of live-born infants would be two. However, the two infants still would be counted as triplets.
¶ U.S. births include nonresidents (24).
** To protect confidentiality, cells with values from 1–4 are suppressed, as are data that can be used to derive cell values of 1–4. These values are included in totals.
††Estimates on the basis of N <20 in the denominator have been suppressed because such rates are considered unstable.
¶¶ In three states, >2% of residency information was missing for procedures performed: California (2.7%), Georgia (2.1%), and Hawaii (2.1%). Overall, residency information was missing for 963 (0.6%) procedures performed and 366 (0.7%) live-birth deliveries.
Adverse Perinatal Outcomes
Nationally, ART-conceived infants contributed to approximately 5.5% of all low birthweight infants (range: 1.2% in West Virginia to 14.2% in Massachusetts) and 5.6% of all very low birthweight infants (range: 0.9% in some states to 14.0% in Hawaii) (Table 5). In four reporting areas (Connecticut, Hawaii, Massachusetts, and New Jersey), >10% of all low birthweight and all very low birthweight infants born were conceived with ART. In all reporting areas, the percentage of low birthweight and very low birthweight infants was higher among infants conceived with ART than among all infants. Among ART-conceived infants, 27.8% had low birthweight (range: 10.6% in Delaware to 44.4% in Puerto Rico), compared with 8.0% among all infants (range: 5.9% in Alaska to 11.3% in Mississippi). Approximately 4.9% of ART-conceived infants had very low birthweight (range: 0.9% in some states to 9.6% in Louisiana), compared with 1.4% among all infants (range: 0.9% in Alaska to 2.1% in the District of Columbia and Mississippi).
TABLE 5. Number, percentage, and proportion of infants born with use of assisted reproductive technology,* by low birthweight category and female patient’s reporting area of residence† at time of treatment — United States and Puerto Rico, 2014.
| Patient’s reporting area of residence | <2,500 g (LBW) |
<1,500 g (VLBW) |
||||
|---|---|---|---|---|---|---|
| ART infants |
All infants§ |
Proportion of ART LBW infants among all LBW infants (%) | ART infants |
All infants§ |
Proportion of ART VLBW infants among all VLBW infants (%) | |
| No. (%) | No. (%) | No. (%) | No. (%) | |||
| Alabama |
162 (35.2) |
5,989 (10.1) |
2.7 |
25 (5.4) |
1,135 (1.9) |
2.2 |
| Alaska |
16 (29.6) |
672 (5.9) |
2.4 |
— (—)¶ |
101 (0.9) |
—¶ |
| Arizona |
283 (28.3) |
6,086 (7.0) |
4.7 |
55 (5.5) |
1,004 (1.2) |
5.5 |
| Arkansas |
61 (31.1) |
3,432 (8.9) |
1.8 |
11 (5.6) |
558 (1.4) |
2.0 |
| California** |
2,091 (25.2) |
33,586 (6.7) |
6.2 |
360 (4.3) |
5,727 (1.1) |
6.3 |
| Colorado |
334 (34.2) |
5,769 (8.8) |
5.8 |
45 (4.6) |
799 (1.2) |
5.6 |
| Connecticut |
325 (24.8) |
2,763 (7.6) |
11.8 |
67 (5.1) |
499 (1.4) |
13.4 |
| Delaware |
24 (10.6) |
908 (8.3) |
2.6 |
8 (3.5) |
194 (1.8) |
4.1 |
| District of Columbia |
59 (16.4) |
934 (9.8) |
6.3 |
8 (2.2) |
198 (2.1) |
4.0 |
| Florida |
831 (29.4) |
19,065 (8.7) |
4.4 |
160 (5.7) |
3,501 (1.6) |
4.6 |
| Georgia** |
445 (30.2) |
12,385 (9.5) |
3.6 |
87 (5.9) |
2,321 (1.8) |
3.7 |
| Hawaii** |
165 (38.6) |
1,462 (7.9) |
11.3 |
34 (7.9) |
243 (1.3) |
14.0 |
| Idaho |
74 (33.9) |
1,471 (6.4) |
5.0 |
— (—)¶ |
227 (1.0) |
—¶ |
| Illinois |
1,119 (27.7) |
12,929 (8.2) |
8.7 |
186 (4.6) |
2,409 (1.5) |
7.7 |
| Indiana |
242 (29.8) |
6,715 (8.0) |
3.6 |
39 (4.8) |
1,146 (1.4) |
3.4 |
| Iowa |
156 (24.8) |
2,675 (6.7) |
5.8 |
24 (3.8) |
460 (1.2) |
5.2 |
| Kansas |
108 (30.5) |
2,759 (7.0) |
3.9 |
17 (4.8) |
493 (1.3) |
3.4 |
| Kentucky |
179 (35.9) |
4,922 (8.8) |
3.6 |
42 (8.4) |
819 (1.5) |
5.1 |
| Louisiana |
195 (36.0) |
6,786 (10.5) |
2.9 |
52 (9.6) |
1,230 (1.9) |
4.2 |
| Maine |
34 (23.6) |
960 (7.6) |
3.5 |
7 (4.9) |
157 (1.2) |
4.5 |
| Maryland |
471 (24.2) |
6,345 (8.6) |
7.4 |
78 (4.0) |
1,186 (1.6) |
6.6 |
| Massachusetts |
761 (22.6) |
5,351 (7.4) |
14.2 |
113 (3.4) |
860 (1.2) |
13.1 |
| Michigan |
458 (30.6) |
9,545 (8.3) |
4.8 |
89 (5.9) |
1,688 (1.5) |
5.3 |
| Minnesota |
308 (26.5) |
4,595 (6.6) |
6.7 |
56 (4.8) |
790 (1.1) |
7.1 |
| Mississippi |
69 (28.3) |
4,374 (11.3) |
1.6 |
13 (5.3) |
804 (2.1) |
1.6 |
| Missouri |
259 (30.9) |
6,163 (8.2) |
4.2 |
43 (5.1) |
1,022 (1.4) |
4.2 |
| Montana |
45 (35.4) |
920 (7.4) |
4.9 |
12 (9.4) |
152 (1.2) |
7.9 |
| Nebraska |
109 (31.2) |
1,775 (6.6) |
6.1 |
18 (5.2) |
312 (1.2) |
5.8 |
| Nevada |
154 (28.5) |
2,972 (8.3) |
5.2 |
20 (3.7) |
509 (1.4) |
3.9 |
| New Hampshire |
82 (28.0) |
852 (6.9) |
9.6 |
16 (5.5) |
130 (1.1) |
12.3 |
| New Jersey |
1,013 (26.9) |
8,315 (8.0) |
12.2 |
178 (4.7) |
1,519 (1.5) |
11.7 |
| New Mexico |
40 (31.3) |
2,282 (8.8) |
1.8 |
12 (9.4) |
349 (1.3) |
3.4 |
| New York |
1,676 (27.0) |
18,722 (7.8) |
9.0 |
304 (4.9) |
3,298 (1.4) |
9.2 |
| North Carolina |
425 (27.3) |
10,720 (8.9) |
4.0 |
68 (4.4) |
1,997 (1.7) |
3.4 |
| North Dakota |
43 (30.3) |
704 (6.2) |
6.1 |
13 (9.2) |
116 (1.0) |
11.2 |
| Ohio |
531 (31.9) |
11,800 (8.5) |
4.5 |
100 (6.0) |
2,185 (1.6) |
4.6 |
| Oklahoma |
143 (34.1) |
4,238 (7.9) |
3.4 |
24 (5.7) |
766 (1.4) |
3.1 |
| Oregon |
191 (28.6) |
2,842 (6.2) |
6.7 |
23 (3.4) |
455 (1.0) |
5.1 |
| Pennsylvania |
628 (25.8) |
11,713 (8.2) |
5.4 |
100 (4.1) |
2,006 (1.4) |
5.0 |
| Puerto Rico |
59 (44.4) |
3,713 (10.8) |
1.6 |
11 (8.3) |
502 (1.5) |
2.2 |
| Rhode Island |
47 (20.4) |
765 (7.1) |
6.1 |
11 (4.8) |
150 (1.4) |
7.3 |
| South Carolina |
165 (30.5) |
5,435 (9.4) |
3.0 |
32 (5.9) |
1,016 (1.8) |
3.1 |
| South Dakota |
33 (26.2) |
804 (6.5) |
4.1 |
5 (4.0) |
125 (1.0) |
4.0 |
| Tennessee |
202 (31.9) |
7,297 (8.9) |
2.8 |
39 (6.2) |
1,260 (1.5) |
3.1 |
| Texas |
1,729 (33.3) |
32,744 (8.2) |
5.3 |
353 (6.8) |
5,722 (1.4) |
6.2 |
| Utah |
261 (36.0) |
3,572 (7.0) |
7.3 |
37 (5.1) |
552 (1.1) |
6.7 |
| Vermont |
35 (33.3) |
432 (7.0) |
8.1 |
9 (8.6) |
65 (1.1) |
13.8 |
| Virginia |
497 (23.2) |
8,130 (7.9) |
6.1 |
89 (4.2) |
1,547 (1.5) |
5.8 |
| Washington |
302 (23.4) |
5,705 (6.4) |
5.3 |
31 (2.4) |
888 (1.0) |
3.5 |
| West Virginia |
23 (23.2) |
1,852 (9.1) |
1.2 |
5 (5.1) |
278 (1.4) |
1.8 |
| Wisconsin |
198 (25.3) |
4,911 (7.3) |
4.0 |
38 (4.9) |
876 (1.3) |
4.3 |
| Wyoming |
15 (27.8) |
704 (9.1) |
2.1 |
— (—)¶ |
103 (1.3) |
—¶ |
| Total | 17,875 (27.8) | 322,560 (8.0) | 5.5 | 3,174 (4.9) | 56,449 (1.4) | 5.6 |
Abbreviations: ART = assisted reproductive technology; LBW = low birthweight; VLBW = very low birthweight.
* ART totals include infants conceived from ART procedures performed in 2013 and born in 2014 and infants conceived from ART procedures performed in 2014 and born in 2014. Total ART infants exclude nonresidents and include only infants with birthweight data available.
† In cases of missing residency data (0.6%), the patient’s residence was assigned as the location in which the ART procedure was performed.
§ U.S. births include nonresidents (24).
¶ To protect confidentiality, cells with values from 1–4 are suppressed, as are data that can be used to derive cell values of 1–4. These values are included in totals.
** In three states, >2% of residency information was missing for procedures performed: California (2.7%), Georgia (2.1%), and Hawaii (2.1%). Overall, residency information was missing for 963 (0.6%) procedures performed and 366 (0.7%) live-birth deliveries.
Nationally, ART contributed to approximately 4.7% (range: 1.2% in Puerto Rico to 13.4% in Massachusetts) and 5.0% (range: 1.1% in Puerto Rico to 14.7% in Massachusetts) of all preterm and very preterm infants, respectively (Table 6). In three reporting areas (Connecticut, Massachusetts, and New Jersey), >10% of all preterm and very preterm infants were conceived with ART. As with low birthweight, the percentage of preterm and very preterm infants was higher among ART-conceived infants than among the total birth population. Among ART-conceived infants, 33.2% were born preterm (range: 18.9% in the District of Columbia to 45.9% in Puerto Rico), compared with 11.3% among all infants (range: 8.5% in California to 16.0% in Mississippi). Approximately 5.9% of ART-conceived infants were very preterm (range: 2.2% in the District of Columbia to 12.0% in North Dakota), compared with 1.9% among all infants (range: 1.3% in California, Idaho, and Utah to 2.9% in Alabama).
TABLE 6. Number, percentage, and proportion of infants born with use of assisted reproductive technology,* by preterm gestational age category and female patient’s reporting area of residence† at time of treatment — United States and Puerto Rico, 2014.
| Patient’s reporting area of residence | <37 weeks (PTB) |
<32 weeks (VPTB) |
||||
|---|---|---|---|---|---|---|
| ART infants |
All infants§ |
Proportion of ART PTB infants among all PTB infants (%) | ART infants |
All infants§ |
Proportion of ART VPTB infants among all VPTB infants (%) | |
| No. (%) | No. (%) | No. (%) | No. (%) | |||
| Alabama |
190 (41.2) |
9,051 (15.2) |
2.1 |
35 (7.6) |
1,719 (2.9) |
2.0 |
| Alaska |
20 (35.7) |
1,148 (10.1) |
1.7 |
6 (10.7) |
158 (1.4) |
3.8 |
| Arizona |
367 (35.7) |
10,100 (11.6) |
3.6 |
59 (5.7) |
1,595 (1.8) |
3.7 |
| Arkansas |
73 (37.2) |
4,857 (12.6) |
1.5 |
12 (6.1) |
743 (1.9) |
1.6 |
| California¶ |
2,490 (29.4) |
42,672 (8.5) |
5.8 |
458 (5.4) |
6,621 (1.3) |
6.9 |
| Colorado |
353 (36.0) |
6,627 (10.1) |
5.3 |
50 (5.1) |
1,022 (1.6) |
4.9 |
| Connecticut |
390 (29.7) |
3,410 (9.4) |
11.4 |
70 (5.3) |
600 (1.7) |
11.7 |
| Delaware |
43 (19.1) |
1,389 (12.7) |
3.1 |
9 (4.0) |
310 (2.8) |
2.9 |
| District of Columbia |
68 (18.9) |
1,269 (13.3) |
5.4 |
8 (2.2) |
247 (2.6) |
3.2 |
| Florida |
1,018 (35.3) |
28,724 (13.1) |
3.5 |
204 (7.1) |
5,024 (2.3) |
4.1 |
| Georgia¶ |
557 (37.8) |
16,504 (12.6) |
3.4 |
98 (6.6) |
3,003 (2.3) |
3.3 |
| Hawaii¶ |
175 (39.2) |
2,236 (12.1) |
7.8 |
40 (9.0) |
350 (1.9) |
11.4 |
| Idaho |
83 (38.1) |
2,239 (9.8) |
3.7 |
8 (3.7) |
298 (1.3) |
2.7 |
| Illinois |
1361 (33.5) |
18,760 (11.8) |
7.3 |
248 (6.1) |
3,438 (2.2) |
7.2 |
| Indiana |
305 (37.5) |
9,233 (11.0) |
3.3 |
43 (5.3) |
1,492 (1.8) |
2.9 |
| Iowa |
208 (33.1) |
4,471 (11.3) |
4.7 |
38 (6.0) |
779 (2.0) |
4.9 |
| Kansas |
136 (37.8) |
4,279 (10.9) |
3.2 |
25 (6.9) |
635 (1.6) |
3.9 |
| Kentucky |
216 (42.7) |
7,079 (12.6) |
3.1 |
46 (9.1) |
1,169 (2.1) |
3.9 |
| Louisiana |
244 (45.1) |
9,793 (15.2) |
2.5 |
57 (10.5) |
1,730 (2.7) |
3.3 |
| Maine |
45 (30.8) |
1,151 (9.1) |
3.9 |
8 (5.5) |
173 (1.4) |
4.6 |
| Maryland |
520 (26.6) |
9,051 (12.2) |
5.7 |
102 (5.2) |
1,620 (2.2) |
6.3 |
| Massachusetts |
945 (27.8) |
7,033 (9.8) |
13.4 |
163 (4.8) |
1,112 (1.5) |
14.7 |
| Michigan |
587 (39.2) |
13,547 (11.8) |
4.3 |
103 (6.9) |
2,401 (2.1) |
4.3 |
| Minnesota |
372 (31.8) |
7,000 (10.0) |
5.3 |
60 (5.1) |
1,161 (1.7) |
5.2 |
| Mississippi |
108 (43.7) |
6,193 (16.0) |
1.7 |
19 (7.7) |
1,085 (2.8) |
1.8 |
| Missouri |
305 (35.1) |
8,836 (11.7) |
3.5 |
48 (5.5) |
1,409 (1.9) |
3.4 |
| Montana |
50 (39.1) |
1,426 (11.5) |
3.5 |
13 (10.2) |
227 (1.8) |
5.7 |
| Nebraska |
153 (43.7) |
2,852 (10.6) |
5.4 |
29 (8.3) |
482 (1.8) |
6.0 |
| Nevada |
214 (38.7) |
4,678 (13.0) |
4.6 |
32 (5.8) |
730 (2.0) |
4.4 |
| New Hampshire |
87 (29.5) |
1,116 (9.1) |
7.8 |
19 (6.4) |
180 (1.5) |
10.6 |
| New Jersey |
1,208 (32.1) |
11,718 (11.3) |
10.3 |
204 (5.4) |
2,000 (1.9) |
10.2 |
| New Mexico |
45 (34.9) |
2,975 (11.4) |
1.5 |
11 (8.5) |
410 (1.6) |
2.7 |
| New York |
1,918 (29.7) |
25,398 (10.6) |
7.6 |
335 (5.2) |
4,023 (1.7) |
8.3 |
| North Carolina |
516 (33.3) |
14,550 (12.0) |
3.5 |
81 (5.2) |
2,929 (2.4) |
2.8 |
| North Dakota |
55 (38.7) |
1,126 (9.9) |
4.9 |
17 (12.0) |
182 (1.6) |
9.3 |
| Ohio |
601 (36.1) |
16,755 (12.0) |
3.6 |
102 (6.1) |
3,116 (2.2) |
3.3 |
| Oklahoma |
172 (41.1) |
6,881 (12.9) |
2.5 |
33 (7.9) |
1,098 (2.1) |
3.0 |
| Oregon |
239 (35.7) |
4,228 (9.3) |
5.7 |
37 (5.5) |
624 (1.4) |
5.9 |
| Pennsylvania |
661 (27.1) |
15,015 (10.6) |
4.4 |
121 (5.0) |
2,684 (1.9) |
4.5 |
| Puerto Rico |
61 (45.9) |
5,223 (15.2) |
1.2 |
9 (6.8) |
819 (2.4) |
—** |
| Rhode Island |
56 (24.1) |
1,107 (10.2) |
5.1 |
9 (3.9) |
193 (1.8) |
4.7 |
| South Carolina |
222 (40.7) |
7,765 (13.5) |
2.9 |
39 (7.1) |
1,432 (2.5) |
2.7 |
| South Dakota |
46 (36.5) |
1,346 (11.0) |
3.4 |
7 (5.6) |
192 (1.6) |
3.6 |
| Tennessee |
254 (40.1) |
10,221 (12.5) |
2.5 |
43 (6.8) |
1,593 (2.0) |
2.7 |
| Texas |
2,206 (42.1) |
49,527 (12.4) |
4.5 |
431 (8.2) |
7,738 (1.9) |
5.6 |
| Utah |
280 (38.8) |
5,196 (10.2) |
5.4 |
42 (5.8) |
668 (1.3) |
6.3 |
| Vermont |
40 (37.4) |
527 (8.6) |
7.6 |
7 (6.5) |
95 (1.5) |
7.4 |
| Virginia |
598 (27.8) |
11,098 (10.7) |
5.4 |
101 (4.7) |
2,017 (2.0) |
5.0 |
| Washington |
360 (27.8) |
8,505 (9.6) |
4.2 |
42 (3.2) |
1,297 (1.5) |
3.2 |
| West Virginia |
38 (37.6) |
2,683 (13.2) |
1.4 |
— (—)** |
449 (2.2) |
—** |
| Wisconsin |
273 (34.7) |
6,854 (10.2) |
4.0 |
57 (7.2) |
1,119 (1.7) |
5.1 |
| Wyoming |
14 (25.9) |
885 (11.5) |
1.6 |
— (—)** |
141 (1.8) |
—** |
| Total | 21,546 (33.2) | 456,307 (11.3) | 4.7 | 3,846 (5.9) | 76,332 (1.9) | 5.0 |
Abbreviations: ART = assisted reproductive technology; PTB = preterm birth; VPTB = very preterm birth.
* ART totals include infants conceived from ART procedures performed in 2013 and born in 2014 and infants conceived from ART procedures performed in 2014 and born in 2014. Total ART births exclude nonresidents and include only infants with gestational age data available.
† In cases of missing residency data (0.6%), the patient’s residence was assigned as the location in which the ART procedure was performed.
§ U.S. births include nonresidents (24).
¶ In three states, >2% of residency information was missing for procedures performed: California (2.7%), Georgia (2.1%), and Hawaii (2.1%). Overall, residency information was missing for 963 (0.6%) procedures performed and 366 (0.7%) live-birth deliveries.
** To protect confidentiality, cells with values from 1–4 are suppressed, as are data that can be used to derive cell values of 1–4. These values are included in totals.
The percentage of ART-conceived infants who were low birthweight was 8.9% (range: 3.2% in some states to 16.1% in Vermont) among singletons, 55.2% (range: 38.5% in Delaware to 77.8% in Alaska) among twins, and 95.3% (range: 0% in some states to 100% in several reporting areas) among triplets and higher-order infants; the corresponding percentage among all infants born was 6.3% (range: 4.6% in Alaska, North Dakota, and Oregon to 9.5% in Puerto Rico) among singletons, 55.2% (range: 46.1% in Alaska to 65.6% in Mississippi) among twins, and 94.5% (range: 88.4% in Alabama to 100% in several reporting areas) among triplets and higher-order infants (Table 7).
TABLE 7. Percentages of low birthweight infants (<2,500 g) among infants born with assisted reproductive technology* and all U.S. infants, by plurality and female patient’s reporting area of residence† at time of treatment — United States and Puerto Rico, 2014.
| Patient’s reporting area of residence | ART singleton infants (%) | All singleton infants§ (%) | ART twin infants¶ (%) | All twin infants§ (%) | ART triplets and higher-order infants¶ (%) | All triplets and higher-order infants§ (%) |
|---|---|---|---|---|---|---|
| Alabama |
9.6 |
8.1 |
59.6 |
62.2 |
—** |
88.4 |
| Alaska |
—†† |
4.6 |
77.8 |
46.1 |
—§§ |
—** |
| Arizona |
9.9 |
5.5 |
53.2 |
53.5 |
100.0 |
91.2 |
| Arkansas |
10.2 |
7.3 |
59.7 |
59.3 |
—** |
100.0 |
| California¶¶ |
8.0 |
5.1 |
52.9 |
51.4 |
94.4 |
94.1 |
| Colorado |
11.2 |
7.1 |
64.8 |
59.7 |
100.0 |
96.8 |
| Connecticut |
8.2 |
5.6 |
51.2 |
52.0 |
—** |
100.0 |
| Delaware |
7.0 |
7.0 |
38.5 |
49.8 |
—§§ |
—** |
| District of Columbia |
8.5 |
7.9 |
40.3 |
57.0 |
—** |
—** |
| Florida |
10.4 |
6.9 |
52.1 |
57.2 |
93.7 |
95.4 |
| Georgia¶¶ |
9.9 |
7.6 |
58.6 |
60.0 |
90.0 |
94.7 |
| Hawaii¶¶ |
10.9 |
6.2 |
65.6 |
59.9 |
—** |
100.0 |
| Idaho |
7.8 |
5.0 |
62.6 |
53.3 |
—**,†† |
—** |
| Illinois |
9.1 |
6.1 |
54.4 |
55.5 |
98.4 |
100.0 |
| Indiana |
6.0 |
6.2 |
54.0 |
55.2 |
91.7 |
100.0 |
| Iowa |
6.8 |
5.0 |
55.5 |
51.0 |
—**,†† |
100.0 |
| Kansas |
6.6 |
5.5 |
62.5 |
52.5 |
—** |
100.0 |
| Kentucky |
9.1 |
7.1 |
56.5 |
56.6 |
100.0 |
100.0 |
| Louisiana |
9.5 |
8.4 |
63.4 |
64.9 |
—** |
100.0 |
| Maine |
—†† |
5.6 |
58.3 |
57.3 |
—**,†† |
—†† |
| Maryland |
10.9 |
6.7 |
58.4 |
55.1 |
—** |
93.9 |
| Massachusetts |
8.5 |
5.3 |
50.6 |
54.0 |
95.2 |
94.0 |
| Michigan |
9.9 |
6.5 |
54.1 |
54.5 |
100.0 |
100.0 |
| Minnesota |
8.1 |
4.9 |
51.0 |
48.8 |
—** |
100.0 |
| Mississippi |
10.5 |
9.3 |
50.5 |
65.6 |
—** |
100.0 |
| Missouri |
8.7 |
6.3 |
58.3 |
57.8 |
—** |
100.0 |
| Montana |
10.8 |
5.8 |
61.3 |
51.7 |
—§§ |
—** |
| Nebraska |
6.0 |
5.0 |
50.6 |
50.3 |
—** |
100.0 |
| Nevada |
10.3 |
6.6 |
54.4 |
58.8 |
—**,†† |
—†† |
| New Hampshire |
10.4 |
5.2 |
55.6 |
52.3 |
—**,†† |
—** |
| New Jersey |
8.5 |
5.8 |
57.2 |
55.7 |
100.0 |
92.4 |
| New Mexico |
11.3 |
7.4 |
59.5 |
62.9 |
—** |
—†† |
| New York |
9.0 |
5.9 |
58.0 |
54.6 |
88.7 |
93.3 |
| North Carolina |
9.0 |
7.1 |
50.9 |
54.2 |
—** |
94.8 |
| North Dakota |
7.8 |
4.6 |
54.8 |
50.0 |
—**,†† |
—†† |
| Ohio |
8.9 |
6.6 |
55.0 |
56.0 |
98.0 |
95.3 |
| Oklahoma |
8.9 |
6.4 |
56.6 |
54.9 |
—** |
100.0 |
| Oregon |
8.3 |
4.6 |
48.3 |
48.7 |
—** |
100.0 |
| Pennsylvania |
8.0 |
6.5 |
54.9 |
52.4 |
100.0 |
92.8 |
| Puerto Rico |
15.3 |
9.5 |
64.7 |
65.3 |
—** |
95.2 |
| Rhode Island |
6.9 |
5.5 |
41.5 |
49.4 |
—**,†† |
—**,†† |
| South Carolina |
10.1 |
7.6 |
57.8 |
59.0 |
—** |
100.0 |
| South Dakota |
—†† |
5.0 |
44.2 |
50.1 |
—** |
—** |
| Tennessee |
9.7 |
7.2 |
59.3 |
60.1 |
—** |
100.0 |
| Texas |
10.2 |
6.5 |
59.7 |
57.5 |
93.5 |
98.0 |
| Utah |
9.2 |
5.2 |
58.5 |
51.3 |
—** |
100.0 |
| Vermont |
16.1 |
5.3 |
50.0 |
46.4 |
—**,†† |
—** |
| Virginia |
8.9 |
6.1 |
51.1 |
52.0 |
100.0 |
100.0 |
| Washington |
7.9 |
5.0 |
46.8 |
51.3 |
90.5 |
88.5 |
| West Virginia |
7.8 |
7.2 |
53.1 |
62.9 |
—**,†† |
—†† |
| Wisconsin |
5.2 |
5.7 |
53.7 |
53.0 |
—** |
100.0 |
| Wyoming |
—†† |
7.3 |
—** |
61.0 |
—**,†† |
—** |
| Total | 8.9 | 6.3 | 55.2 | 55.2 | 95.3 | 94.5 |
Abbreviation: ART = assisted reproductive technology.
* ART totals include infants conceived from ART procedures performed in 2013 and born in 2014 and infants conceived from ART procedures performed in 2014 and born in 2014. Total ART births exclude nonresidents and only include infants with birthweight data available.
† In cases of missing residency data (0.6%), the patient’s residence was assigned as the location in which the ART procedure was performed.
§ U.S. births include nonresidents (24).
¶ Includes only the number of infants live-born in a multiple-birth delivery. For example, if three infants were born in a live-birth delivery and one of the three infants was stillborn, the total number of live-born infants would be two. However, the two infants still would be counted as triplets.
** Estimates on the basis of N <20 in the denominator have been suppressed because such rates are considered unstable.
†† To protect confidentiality, cells with values from 1–4 are suppressed, as are data that can be used to derive cell values of 1–4. These values are included in totals. For all births, cell values are suppressed for cell/numerator <10 or if a total/subtotal for a range of cells with a single suppressed member.
§§ Estimates not calculated because N = 0 for the denominator.
¶¶ In three states, >2% of residency information was missing for procedures performed: California (2.7%), Georgia (2.1%), and Hawaii (2.1%). Overall, residency information was missing for 963 (0.6%) procedures performed and 366 (0.7%) live-birth deliveries.
The percentage of ART-conceived infants who were born preterm was 13.2% among singletons (range: 7.5% in Rhode Island to 23.4% in West Virginia), 62.2% among twins (range: 33.3% in some states to 81.4% in Mississippi), and 98.2% among triplets and higher-order infants (range: 50.0% in some states to 100% in several reporting areas); the corresponding percentage among all infants was 9.7% for singletons (range: 1.7% in the District of Columbia to 14.2% in Mississippi), 56.6% for twins (range: 47.2% in Vermont to 66.9% in Wyoming), and 93.8% for triplets and higher-order infants (range: 52.2% in Hawaii to 100% in several reporting areas) (Table 8).
TABLE 8. Percentages of preterm (<37 weeks) infants among infants born with the use of assisted reproductive technology* and all U.S. infants, by plurality and female patient’s reporting area of residence† at time of treatment — United States and Puerto Rico, 2014.
| Patient’s reporting area of residence | ART singleton infants (%) | All singleton infants§ (%) | ART twin infants¶ (%) | All twin infants§ (%) | ART triplets and higher-order infants¶ (%) | All triplets and higher order-infants§ (%) |
|---|---|---|---|---|---|---|
| Alabama |
14.5 |
13.5 |
66.5 |
62.4 |
—** |
100.0 |
| Alaska |
—†† |
8.6 |
80.0 |
55.9 |
—§§ |
—** |
| Arizona |
14.8 |
10.1 |
64.8 |
58.6 |
100.0 |
94.1 |
| Arkansas |
13.6 |
11.2 |
75.0 |
57.4 |
—**,†† |
76.7 |
| California¶¶ |
12.1 |
7.0 |
56.9 |
52.3 |
98.2 |
94.9 |
| Colorado |
15.6 |
8.5 |
63.0 |
57.4 |
100.0 |
88.9 |
| Connecticut |
11.9 |
7.5 |
58.1 |
50.6 |
—** |
71.1 |
| Delaware |
13.6 |
11.4 |
61.5 |
54.0 |
—§§ |
—** |
| District Of Columbia |
9.9 |
1.7 |
—†† |
52.9 |
—** |
—** |
| Florida |
14.9 |
11.5 |
59.6 |
56.6 |
100.0 |
93.1 |
| Georgia¶¶ |
14.9 |
10.9 |
70.2 |
58.0 |
100.0 |
90.9 |
| Hawaii¶¶ |
13.1 |
10.6 |
64.4 |
54.8 |
—** |
52.2 |
| Idaho |
12.9 |
8.2 |
65.7 |
60.9 |
—**,†† |
—** |
| Illinois |
13.9 |
9.8 |
62.0 |
59.4 |
100.0 |
96.8 |
| Indiana |
11.2 |
9.3 |
64.9 |
56.9 |
100.0 |
100.0 |
| Iowa |
11.0 |
9.4 |
70.9 |
59.3 |
—**,†† |
100.0 |
| Kansas |
11.6 |
9.3 |
73.8 |
58.3 |
—** |
87.0 |
| Kentucky |
11.4 |
11.0 |
68.8 |
58.7 |
100.0 |
100.0 |
| Louisiana |
17.7 |
13.2 |
74.0 |
66.7 |
—** |
93.6 |
| Maine |
12.6 |
7.3 |
62.5 |
53.4 |
—**,†† |
93.6 |
| Maryland |
13.5 |
10.4 |
60.5 |
57.7 |
—** |
100.0 |
| Massachusetts |
11.9 |
7.6 |
59.3 |
58.3 |
93.3 |
96.4 |
| Michigan |
16.7 |
10.1 |
65.6 |
57.2 |
100.0 |
89.9 |
| Minnesota |
11.6 |
8.3 |
59.3 |
52.3 |
—** |
100.0 |
| Mississippi |
16.0 |
14.2 |
81.4 |
65.5 |
—** |
66.7 |
| Missouri |
13.3 |
9.9 |
62.0 |
62.1 |
—** |
98.5 |
| Montana |
10.8 |
9.9 |
68.3 |
55.3 |
—§§ |
—** |
| Nebraska |
9.6 |
8.9 |
72.6 |
58.2 |
—** |
87.7 |
| Nevada |
15.4 |
11.5 |
73.4 |
60.3 |
—**,†† |
92.3 |
| New Hampshire |
10.9 |
7.4 |
59.3 |
52.0 |
—**,†† |
—** |
| New Jersey |
12.6 |
9.3 |
63.9 |
54.8 |
100.0 |
95.5 |
| New Mexico |
14.8 |
10.2 |
71.4 |
59.7 |
—**,†† |
100.0 |
| New York |
12.7 |
8.9 |
58.6 |
53.3 |
92.4 |
92.0 |
| North Carolina |
14.2 |
10.5 |
58.2 |
52.9 |
—** |
89.7 |
| North Dakota |
10.4 |
8.3 |
71.0 |
55.0 |
—**,†† |
68.2 |
| Ohio |
13.0 |
10.2 |
59.3 |
57.2 |
100.0 |
89.8 |
| Oklahoma |
13.1 |
11.3 |
67.2 |
61.4 |
—** |
93.4 |
| Oregon |
16.3 |
7.6 |
54.3 |
52.6 |
—** |
93.0 |
| Pennsylvania |
10.5 |
8.8 |
53.9 |
55.1 |
100.0 |
74.8 |
| Puerto Rico |
18.6 |
14.1 |
64.7 |
62.3 |
—** |
100.0 |
| Rhode Island |
7.5 |
8.7 |
—†† |
52.0 |
—**,†† |
—** |
| South Carolina |
17.3 |
11.8 |
70.3 |
57.7 |
—**,†† |
100.0 |
| South Dakota |
11.8 |
9.4 |
61.5 |
55.5 |
—** |
—** |
| Tennessee |
15.5 |
10.8 |
71.3 |
61.1 |
—** |
93.1 |
| Texas |
17.2 |
10.7 |
70.7 |
59.9 |
100.0 |
94.5 |
| Utah |
12.4 |
8.3 |
61.9 |
56.3 |
—** |
100.0 |
| Vermont |
12.5 |
6.9 |
62.5 |
47.2 |
—**,†† |
—** |
| Virginia |
11.0 |
9.1 |
61.2 |
52.6 |
100.0 |
91.3 |
| Washington |
10.5 |
8.2 |
54.3 |
52.3 |
100.0 |
80.8 |
| West Virginia |
23.4 |
11.4 |
58.8 |
64.2 |
—**,†† |
57.1 |
| Wisconsin |
11.4 |
8.6 |
67.0 |
54.6 |
—** |
96.7 |
| Wyoming |
15.2 |
9.6 |
—†† |
66.9 |
—**,†† |
—** |
| Total | 13.2 | 9.7 | 62.2 | 56.6 | 98.2 | 93.8 |
Abbreviation: ART = assisted reproductive technology.
* ART totals include infants conceived from ART procedures performed in 2013 and born in 2014 and infants conceived from ART procedures performed in 2014 and born in 2014. Total ART births exclude nonresidents and includes only infants with gestational age data available.
† In cases of missing residency data (0.6%), the patient's residence was assigned as the location in which the ART procedure was performed.
§ U.S. births include nonresidents (24).
¶ Includes only the number of infants live-born in a multiple-birth delivery. For example, if three infants were born in a live-birth delivery and one of the three infants was stillborn, the total number of live-born infants would be two. However, the two infants still would be counted as triplets.
** Estimates on the basis of N <20 in the denominator have been suppressed because such rates are considered unstable.
†† To protect confidentiality, cells with values from 1–4 are suppressed, as are data that can be used to derive cell values of 1–4. These values are included in totals.
§§ Estimates not calculated because N = 0 for the denominator.
¶¶ In three states, >2% of residency information was missing for procedures performed: California (2.7%), Georgia (2.1%), and Hawaii (2.1%). Overall, residency information was missing for 963 (0.6%) procedures performed and 366 (0.7%) live-birth deliveries.
Discussion
Overview
The use of ART has increased substantially in the United States since the beginning of ART surveillance. In 1996 (the first full year for which ART data were reported to CDC), a total of 20,597 infants were born from 64,036 ART procedures (25). Since then, the number of procedures reported to CDC and the number of infants born from ART procedures have approximately tripled. Several changes can be observed in ART use and outcomes since the preceding reporting year in 2013 (26). The rate of ART use as measured by procedures performed per 1 million women of reproductive age (15–44 years) increased from 2,521 to 2,647. Among women aged <35 years, the average number of embryos transferred decreased (from 1.8 to 1.7) and correspondingly, the percentage of eSET increased (from 21.4% to 28.5%). Overall, the percentage of ART-conceived infants born in multiple-birth deliveries decreased from 41.1% to 39.4%, the percentage of ART-conceived twin infants decreased from 39.2% to 37.5%, and the percentage of ART-conceived triplets and higher-order infants decreased from 1.9% to 1.8%. However, the contribution of ART-conceived twin infants to all twin infants and the contribution of ART-conceived preterm infants to all preterm infants remained unchanged at approximately 18.0% and 4.7%, respectively.
The contribution of ART on rates of multiple births and poor birth outcomes remained substantial in 2014, as approximately 39.0% of ART-conceived infants were born in multiple births (compared with only 3.5% of infants among the total birth population). The contribution of ART-conceived infants to all triplets and higher-order infants increased slightly from 25.2% in 2013 to 26.4% in 2014. ART-conceived twins accounted for approximately 95.3% (24,514 of 25,714) of all ART-conceived infants born in multiple-birth deliveries. On average, approximately two embryos were transferred among women aged <35 years, even though single embryo transfers have been associated with better perinatal outcomes among the majority of women in this age group (27,28). Although the rate of eSET procedures was still relatively low among women aged <35 years, from 2013 to 2014, the eSET rate increased from 21.4% to 28.5%. This is the largest annual percentage increase (33.6%) in eSET rate in the U.S ever detected through NASS. The percentage of low birthweight and preterm birth was substantially higher among ART-conceived infants (27.8% and 33.2%, respectively) than among all infants (8.0% and 11.3%, respectively). Among ART-conceived infants, twins and triplets and higher-order infants were more likely than singletons to be born preterm (more than 4.5 times and seven times, respectively). Although infants conceived with ART accounted for approximately 1.6% of total births in the United States in 2014, the proportions of twins and triplets and higher-order infants attributable to ART were 18.0% and 26.4%, respectively.
Comparable data on ART use and embryo transfer practices from 17 European countries indicate that in 2011, ART use as defined by the number of procedures performed per 1 million women of reproductive age was 6,556; this was approximately 2.7 times higher than the rate in the United States in 2011 (29,30). Percentages of single-embryo transfers (eSET rates are not reported) varied widely in Europe, and a few countries reported a single-embryo transfer rate of over 50.0%. Overall, in these 17 reporting countries, approximately 81.0% of all IVF deliveries were singleton deliveries, compared with 72.0% in the United States (29,30).
Variations by Reporting Area
ART use (as measured by the number of ART procedures performed per 1 million women of reproductive age) varied widely by reporting area: residents of Connecticut, Delaware, Hawaii, Illinois, Maryland, Massachusetts, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Virginia, and the District of Columbia had higher ART use than the national level. Although some women who used ART might have been aged >44 years, this measure is still useful as a proxy indicator of ART use in each reporting area. Importantly, residents of California, Illinois, Massachusetts, New Jersey, New York, and Texas accounted for nearly half (47.0%) of all ART-conceived infants. The large number of ART procedures performed in these states is a result of the large size of the general population (California, Texas), higher ART use (Massachusetts, New Jersey), or both (New York, Illinois). The contribution of ART to all infants born was 4.7% in Massachusetts and 1.7% in California.
Such differences might be explained in part by variations in state health insurance coverage. A total of 15 states (Arkansas, California, Connecticut, Hawaii, Illinois, Louisiana, Maryland, Massachusetts, Montana, New Jersey, New York, Ohio, Rhode Island, Texas, and West Virginia) have passed legislation mandating insurance coverage for fertility treatments, although not all mandates require coverage for ART; mandates from four of these states (Illinois, Massachusetts, New Jersey, and Rhode Island) include comprehensive coverage for at least four cycles of IVF.† Three of the four states with comprehensive mandates (Illinois, Massachusetts, and New Jersey) had rates of ART use that were at least 50.0% higher than the national level. This type of mandated insurance has been associated with greater use of ART (31–33). Linkage of NASS data with birth certificate data in three states indicated that Massachusetts had a higher overall rate of ART use compared with Florida and Michigan, which do not have a comprehensive coverage mandate for ART (33).
Elective Single-Embryo Transfer Rates
According to the American Society of Reproductive Medicine (ASRM) and SART, eSET is recommended for favorable prognosis patients (patients who underwent their first IVF cycle and had extra embryos cryopreserved, patients with previous successful IVF procedures, or patients who are recipients of oocytes from a donor aged <35 years) (34). The guidelines issued by ASRM/SART on the number of embryos transferred have been revised several times (35–39). However, ASRM/SART guidelines on the number of embryos transferred allow for up to two embryos to be transferred even among favorable prognosis patients with patient counseling regarding risks for multifetal pregnancies (35). A high number of double-embryo transfers occur among patients who might otherwise appear to be good candidates for transferring one embryo (40). Reducing the number of embryos transferred from two to one among those patients who have a good chance of pregnancy and live birth with single-embryo transfers will lower ART-conceived twin rates (40,41).
Among women aged <35 years, the percentage of eSET procedures was higher (28.5% nationally) than among older age groups (16.7% among women aged 35–37 years and 4.7% among women aged >37 years nationally) and varied widely among reporting areas (range: 4.3% to 67.9%). The national percentage of eSET increased from 7.4% in 2009 to 28.5% in 2014 among women aged <35 years (26). From 2013 to 2014, the national percentage of eSET among women aged <35 years increased by approximately 33.0%. The percentage of eSET is still lower in the United States than in countries that impose restrictions on the number of embryos transferred and provide extensive public funding for ART services (42). The eSET rates are influenced by many factors (e.g., patient’s age, diagnostic factors, and treatment costs); ART treatment costs are high and typically paid out-of-pocket by the patient. In the United States, even where mandated, coverage for infertility treatment can vary in scope (31). In the four states with mandatory comprehensive insurance coverage for ART, the eSET percentage among women aged <35 years was higher than the national average (28.5%) in Massachusetts (51.5%), New Jersey (34.7%), and Rhode Island (34.5%) but lower in Illinois (27.2%). Because ART procedures are expensive (out-of-pocket costs to achieve a live birth estimated at $27,000 for patients with no insurance), broad insurance mandates for IVF might increase the use of eSET and decrease multiple-embryo transfer procedures (32,43,44). Wider acceptance and use of eSET procedures still face considerable barriers in the United States and might require strengthening the guidelines on embryo transfer practices along with expansion of insurance coverage for ART services (40,41,44,45).
ART Multiple-Birth Infants
Singleton live-birth deliveries have lower risks than multiple-birth deliveries for adverse birth outcomes such as prematurity, low birthweight, disability, and death (46–48). To optimize healthy birth outcomes, the transfer of fewer embryos should be encouraged, where appropriate, taking into consideration the patient’s age and prognosis (27). The percentage of ART-conceived multiple-birth infants in the United States decreased from 53.1% in 2000 to 39.4% in 2014 (49). A substantial decrease was noted in the percentage of ART-conceived triplets and higher-order infants (from 8.9% in 2000 to 1.8% in 2014), and a smaller decrease was noted in the percentage of ART-conceived twins (from 44.2% in 2000 to 37.5% in 2014).
In the past, the slow decrease in twin-infant birth rates among women who undergo ART procedures was largely attributable to gradual increases in eSET rates (40,41). From 2013 to 2014, an historically large increase of 33.0% in national eSET rate was observed. Despite this increase in eSET use, ART-conceived twin infants still accounted for approximately 40.0% of all ART-conceived infants in 2014, and on average, 1.7 embryos were transferred among favorable prognosis patients aged <35 years. In addition to embryo transfer practices, high ART-conceived twin rates also might be partially explained by a desire for more than one child among couples experiencing infertility who might believe that the benefits of a multiple-gestation pregnancy outweigh the risks (50–52). Therefore, understanding the perspective of couples undergoing infertility treatments regarding multiple-gestation pregnancies and multiple births is an important consideration. Although a major barrier to the greater use of eSET might be the high out-of-pocket cost of ART, the use and acceptance of eSET among younger patients with good prognosis can be promoted through patient education. The findings in this report indicate that ART-conceived twins and higher-order infants were more than 4.5 times and seven times more likely, respectively, to be born preterm than were ART-conceived singletons. Studies indicate that patient education focusing on maternal and perinatal morbidity and mortality, as well as the economic costs of twin gestation, has been effective in reducing the preference for twins among patients (53–55).
The economic costs of multiple births also underscore the importance of efforts to reduce ART-related multiple births. In 2013, the mean health care cost to patients and insurers was estimated to be $26,922 for ART-conceived singleton deliveries, $115,238 for ART-conceived twins, and $434,668 for ART-conceived triplets and higher-order infants (56). Transferring two embryos is associated with a slight increase in birth rate but a greater increase in the twin birth rate as compared with transferring a single embryo (27,57). However, transferring two embryos sequentially (single-embryo transfer over two sequential procedures) has similar cumulative live-birth rates and lower twin delivery rates than transferring two embryos in a single procedure and might be a cost-effective transfer approach (58–60). As a result of the data on the higher economic costs of maternal and neonatal complications that occur with multiple births, insurance companies could consider expanded coverage for ART services that also includes clinically appropriate use of eSET and other limitations placed on the number of embryos transferred (41,45,56). Evidence from other countries suggests that greater insurance coverage for ART when combined with restrictions on the number of embryos transferred per cycle can reduce multiple births (45).
ART Low Birthweight Infants and Preterm Births
The percentage of low birthweight and very low birthweight infants was higher among ART-conceived infants than among infants in the total birth population. Three states (Connecticut, Massachusetts, and New Jersey) that had large numbers of ART procedures and births also had high ART contribution (>10%) to both categories of low birthweight and preterm births. In the United States, the contribution of ART to preterm births, the majority of which are also low birthweight, is a key concern. Fertility treatments, both ART and controlled ovarian stimulations, contribute substantially to preterm births (47,61). Preterm births are a leading cause of infant mortality and morbidity; preterm infants are at increased risk for death and have more health and developmental problems than full-term infants (47,62–64). The health risks associated with preterm birth have contributed to increased health care costs. The societal economic costs associated with all preterm births in the United States was last reported in 2005 and was estimated at $26 billion annually ($51,600 per infant born preterm) (47). In 2012, the societal economic costs associated with ART-conceived preterm infants in the United States was estimated at approximately $1.3 billion (65).
In addition to the known multiple-birth risks associated with ART, even singleton infants conceived from ART procedures are at increased risk for low birthweight and preterm delivery. In 2014, of all ART-conceived singleton infants, 9.0% were low birthweight, compared with 6.3% of infants in the total birth population. The percentage of ART-conceived singletons born preterm was 13.2%, compared with 9.7% of infants in the total U.S. birth population. Therefore, adverse infant health outcomes (e.g., low birthweight and preterm delivery) among singletons also should be considered when assessing the effects of ART.
Limitations
The findings in this report are subject to at least five limitations. First, ART surveillance data were reported for each ART procedure performed rather than for each patient who used ART. Second, because patients can achieve a successful pregnancy after undergoing multiple procedures, the procedure-specific success rates reported here underestimate the true per-patient success rates. Third, prematurity and low birthweight could be associated with factors contributing to underlying infertility and not entirely to ART procedures. Fourth, approximately 8.0% of fertility clinics that performed ART in 2014 did not report their data to CDC, and these clinics might have had results differing from reporting clinics. Finally, NASS lacks data on embryo quality, which influences the use of eSET among favorable prognosis patients aged <35 years; however, having extra embryos available for cryopreservation has been shown to be a good predictor of embryo quality.
Conclusion
Since 1996, the number of ART procedures performed in the United States and the number of infants born as a result of these procedures nearly tripled. With this increasing use, ART-conceived infants represented 1.6% of infants born in the United States in 2014 and noticeably contributed to the prevalence of low birthweight and preterm deliveries, as approximately two fifths of ART-conceived infants were multiple-birth deliveries. Furthermore, among ART-conceived infants, although the percentage of triplets or higher-order infants has decreased since 2000, the percentage of twin infants has remained persistently high. Therefore, the impact of ART on poor birth outcomes remains substantial. This report documents the rates and contribution of ART to multiple-birth deliveries, low birthweight, and preterm birth by patient’s reporting area of residence. It also highlights the differences in rates of low birthweight and prematurity between ART-conceived infants and all infants in the total birth population. These findings allow state health departments to monitor the extent of ART-related adverse perinatal outcomes among singletons, twins, and triplets and higher-order infants in their reporting areas.
Comprehensive insurance coverage of ART can help increase access to fertility treatments (45). Increased use of ART in reporting areas with insurance mandates also can result in higher numbers of ART-conceived multiple-birth deliveries. The findings in this report indicate that ART use was higher than the national rate in all four states with mandated comprehensive insurance coverage. Three of these four states had use rates exceeding 1.5 times the national rate and among these three states, two had a percentage of multiple births that was lower than the national average. Further, in three of these states, among patients aged <35 years, the average number of embryos transferred was less than the national rate and the rate of eSET was higher than the national rate. Further research is needed to ascertain the influence of state health insurance mandates on ART use, embryo transfer practices, infant outcomes, and economic and out-of-pocket patient costs of multiple births (28,34,40,41). Addressing the risk for multiple-birth deliveries also requires understanding the perspectives of couples undergoing infertility treatments who might view a multiple birth, especially twins, as an acceptable or desired outcome or might lack awareness of the increased risks associated with multiple births to mothers and infants. Although the majority of clinicians acknowledge that the birth of a healthy singleton is the best outcome of ART, they might be sensitive to patient perspectives (34,35). Clinicians need to be aware of ongoing efforts to limit the number of embryos transferred to reduce the rate of multiple births, particularly twins, and encourage wider implementation of eSET, when clinically appropriate, as mechanisms of promoting singleton infant births among ART-conceived pregnancies (27,34,41).
CDC has outlined a public health oriented strategy for detection, prevention, and management of infertility, including improving ART practice and outcomes, through coordinated efforts of government and nongovernment organizations. The effort involves federal, state, and local agencies; the scientific community; health care professionals; insurance providers; employers; industry; nonprofit organizations; and organizations representing people coping with infertility (66). Of public health importance is the role of infertility treatment on adverse birth outcomes, primarily because of higher rates of multiple births. ART only partially explains the overall prevalence of these adverse outcomes in the United States. Other factors influencing multiple births include maternal age at conception and non-ART fertility treatments (47,61,67). The older age of women giving birth accounted for a substantial increase in twins during 1980–2009 (67). The risk for multiple gestations associated with non-ART fertility treatments (i.e., controlled ovarian stimulation such as superovulation-intrauterine insemination and conventional ovulation induction) is less well-documented than those from ART procedures, as clinics are only mandated to report data on ART use. Further efforts also are needed to monitor the use of non-ART fertility treatments and their role in the increasing number of multiple-birth deliveries (47,61). In 2011, approximately 19.0% of twin births in the United States were attributable to non-IVF fertility treatments (61). Multiple gestations resulting from non-ART fertility treatments also might contribute to preterm births (47,61). Additional research is needed to identify the causes and consequences of preterm births that occur because of infertility treatments and to develop and institute guidelines to reduce the number of multiple gestations (47,61). However, studies have demonstrated that singleton infants conceived with ovulation stimulation are more likely than naturally conceived infants to be small for gestational age (68). CDC is monitoring the prevalence of non-ART fertility treatment use and resultant outcomes among women who had live births in several states participating in the Pregnancy Risk Assessment Monitoring System (69). U.S. birth certificate data published annually by CDC’s National Center for Health Statistics plans to include information on the use of ART and non-ART treatments and birth outcomes from data year 2016. CDC also is working to improve state-based surveillance of ART, infertility, and other birth-related issues by linking data from NASS to data collected by states (i.e., birth certificate, infant death, hospital discharge, and birth defect registry information). This initiative, the States Monitoring Assisted Reproductive Technology (SMART) Collaborative,§ has been determined to be feasible and useful for monitoring long-term outcomes of ART (70,71). CDC will continue to provide updates of ART use in the United States as data become available.
Footnotes
Data regarding population size were compiled on the basis of July 1, 2014, estimates from the U.S. Census Bureau.
Eight states (Arkansas, Connecticut, Hawaii, Illinois, Maryland, Massachusetts, New Jersey, and Rhode Island) have insurance mandates that cover at least one ART cycle. Seven states (California, Louisiana, Montana, New York, Ohio, Texas, and West Virginia) have insurance mandates that exclude IVF coverage. Information is available at http://www.resolve.org/family-building-options/insurance_coverage/state-coverage.html.
States Monitoring Assisted Reproductive Technology (SMART) is a collaboration between CDC and state health departments in Connecticut, Florida, Massachusetts, and Michigan. Information is available at https://www.cdc.gov/art/smart/index.html.
References
- 1.CDC; American Society for Reproductive Medicine; Society for Assisted Reproductive Technology. 2014 assisted reproductive technology fertility clinic success rates report. Atlanta, GA: US Department of Health and Human Services; 2016.
- 2.CDC; American Society for Reproductive Medicine; Society for Assisted Reproductive Technology; RESOLVE. 1995 assisted reproductive technology success rates. Atlanta, GA: US Department of Health and Human Services; 1997.
- 3.CDC; American Society for Reproductive Medicine; Society for Assisted Reproductive Technology. 2013 assisted reproductive technology national summary report. Atlanta, GA: US Department of Health and Human Services; 2015.
- 4.Schieve LA, Peterson HB, Meikle SF, et al. Live-birth rates and multiple-birth risk using in vitro fertilization. JAMA 1999;282:1832–8. 10.1001/jama.282.19.1832 [DOI] [PubMed] [Google Scholar]
- 5.Schieve LA, Meikle SF, Peterson HB, Jeng G, Burnett NM, Wilcox LS. Does assisted hatching pose a risk for monozygotic twinning in pregnancies conceived through in vitro fertilization? Fertil Steril 2000;74:288–94. 10.1016/S0015-0282(00)00602-6 [DOI] [PubMed] [Google Scholar]
- 6.Reynolds MA, Schieve LA, Martin JA, Jeng G, Macaluso M. Trends in multiple births conceived using assisted reproductive technology, United States, 1997–2000. Pediatrics 2003;111:1159–62. [PubMed] [Google Scholar]
- 7.Reynolds MA, Schieve LA, Jeng G, Peterson HB, Wilcox LS. Risk of multiple birth associated with in vitro fertilization using donor eggs. Am J Epidemiol 2001;154:1043–50. 10.1093/aje/154.11.1043 [DOI] [PubMed] [Google Scholar]
- 8.Vahratian A, Schieve LA, Reynolds MA, Jeng G. Live-birth rates and multiple-birth risk of assisted reproductive technology pregnancies conceived using thawed embryos, USA 1999-2000. Hum Reprod 2003;18:1442–8. 10.1093/humrep/deg284 [DOI] [PubMed] [Google Scholar]
- 9.Wright V, Schieve LA, Vahratian A, Reynolds MA. Monozygotic twinning associated with day 5 embryo transfer in pregnancies conceived after IVF. Hum Reprod 2004;19:1831–6. 10.1093/humrep/deh338 [DOI] [PubMed] [Google Scholar]
- 10.Kissin DM, Schieve LA, Reynolds MA. Multiple-birth risk associated with IVF and extended embryo culture: USA, 2001. Hum Reprod 2005;20:2215–23. 10.1093/humrep/dei025 [DOI] [PubMed] [Google Scholar]
- 11.Reynolds MA, Schieve LA. Trends in embryo transfer practices and multiple gestation for IVF procedures in the USA, 1996–2002. Hum Reprod 2006;21:694–700. 10.1093/humrep/dei363 [DOI] [PubMed] [Google Scholar]
- 12.Murray SR, Norman JE. Multiple pregnancies following assisted reproductive technologies—a happy consequence or double trouble? Semin Fetal Neonatal Med 2014;19:222–7. 10.1016/j.siny.2014.03.001 [DOI] [PubMed] [Google Scholar]
- 13.Workshop Group TEC; The ESHRE Capri Workshop Group. Multiple gestation pregnancy. Hum Reprod 2000;15:1856–64. 10.1093/humrep/15.8.1856 [DOI] [PubMed] [Google Scholar]
- 14.MacKay AP, Berg CJ, King JC, Duran C, Chang J. Pregnancy-related mortality among women with multifetal pregnancies. Obstet Gynecol 2006;107:563–8. 10.1097/01.AOG.0000200045.91015.c6 [DOI] [PubMed] [Google Scholar]
- 15.Bukulmez O. Does assisted reproductive technology cause birth defects? Curr Opin Obstet Gynecol 2009;21:260–4. 10.1097/GCO.0b013e32832924a7 [DOI] [PubMed] [Google Scholar]
- 16.Reefhuis J, Honein MA, Schieve LA, Correa A, Hobbs CA, Rasmussen SA; National Birth Defects Prevention Study. Assisted reproductive technology and major structural birth defects in the United States. Hum Reprod 2009;24:360–6. 10.1093/humrep/den387 [DOI] [PubMed] [Google Scholar]
- 17.Fountain C, Zhang Y, Kissin DM, et al. Association between assisted reproductive technology conception and autism in California, 1997–2007. Am J Public Health 2015;105:963–71. 10.2105/AJPH.2014.302383 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Boulet SL, Kirby RS, Reefhuis J, et al. ; States Monitoring Assisted Reproductive Technology (SMART) Collaborative. Assisted Reproductive Technology and Birth Defects Among Liveborn Infants in Florida, Massachusetts, and Michigan, 2000–2010. JAMA Pediatr 2016;170:e154934. 10.1001/jamapediatrics.2015.4934 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Schieve LA, Meikle SF, Ferre C, Peterson HB, Jeng G, Wilcox LS. Low and very low birth weight in infants conceived with use of assisted reproductive technology. N Engl J Med 2002;346:731–7. 10.1056/NEJMoa010806 [DOI] [PubMed] [Google Scholar]
- 20.Schieve LA, Ferre C, Peterson HB, Macaluso M, Reynolds MA, Wright VC. Perinatal outcome among singleton infants conceived through assisted reproductive technology in the United States. Obstet Gynecol 2004;103:1144–53. 10.1097/01.AOG.0000127037.12652.76 [DOI] [PubMed] [Google Scholar]
- 21.Farr SL, Schieve LA, Jamieson DJ. Pregnancy loss among pregnancies conceived through assisted reproductive technology, United States, 1999–2002. Am J Epidemiol 2007;165:1380–8. 10.1093/aje/kwm035 [DOI] [PubMed] [Google Scholar]
- 22.Kramer MR, Hogue CR. What causes racial disparities in very preterm birth? A biosocial perspective. Epidemiol Rev 2009;31:84–98. 10.1093/ajerev/mxp003 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.US Census Bureau. Annual estimates of the resident population for selected age groups by sex for the United States, states, counties, and Puerto Rico Commonwealth and municipios: April 1, 2010 to July 1, 2014. Washington, DC: US Census Bureau, Population Division; 2014. http://factfinder.census.gov/faces/tableservices/jsf/pages/productview.xhtml?pid=PEP_2014_PEPAGESEX&prodType=table
- 24.Hamilton BE, Martin JA, Osterman MJ, Curtin SC, Matthews TJ. Births: Final Data for 2014. Natl Vital Stat Rep 2015;64:1–64. [PubMed] [Google Scholar]
- 25.CDC; American Society for Reproductive Medicine; Society for Assisted Reproductive Technology; RESOLVE. 1996 assisted reproductive technology success rates. Atlanta, GA: US Department of Health and Human Services; 1998. [Google Scholar]
- 26.Sunderam S, Kissin DM, Crawford SB, et al. Assisted reproductive technology surveillance—United States, 2013. MMWR Surveill Summ 2015;64(No. SS-11). 10.15585/mmwr.ss6411a1 [DOI] [PubMed] [Google Scholar]
- 27.Kissin DM, Kulkarni AD, Kushnir VA, Jamieson DJ; National ART Surveillance System Group. Number of embryos transferred after in vitro fertilization and good perinatal outcome. Obstet Gynecol 2014;123:239–47. 10.1097/AOG.0000000000000106 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Stillman RJ, Richter KS, Jones HW Jr. Refuting a misguided campaign against the goal of single-embryo transfer and singleton birth in assisted reproduction. Hum Reprod 2013;28:2599–607. 10.1093/humrep/det317 [DOI] [PubMed] [Google Scholar]
- 29.Kupka MS, D’Hooghe T, Ferraretti AP, et al. ; European IVF-Monitoring Consortium (EIM); European Society of Human Reproduction and Embryology (ESHRE). Assisted reproductive technology in Europe, 2011: results generated from European registers by ESHRE. Hum Reprod 2016;31:233–48. [DOI] [PubMed] [Google Scholar]
- 30.Sunderam S, Kissin DM, Crawford SB, Folger SG, Jamieson DJ, Barfield WD. Assisted reproductive technology surveillance—United States, 2011. MMWR Surveill Summ 2014;63(No. SS-10). [PubMed] [Google Scholar]
- 31.Henne MB, Bundorf MK. Insurance mandates and trends in infertility treatments. Fertil Steril 2008;89:66–73. 10.1016/j.fertnstert.2007.01.167 [DOI] [PubMed] [Google Scholar]
- 32.Hamilton BH, McManus B. The effects of insurance mandates on choices and outcomes in infertility treatment markets. Health Econ 2012;21:994–1016. 10.1002/hec.1776 [DOI] [PubMed] [Google Scholar]
- 33.Boulet SL, Crawford S, Zhang Y, et al. ; States Monitoring ART Collaborative. Embryo transfer practices and perinatal outcomes by insurance mandate status. Fertil Steril 2015;104:403–9.e1. 10.1016/j.fertnstert.2015.05.015 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Practice Committee of Society for Assisted Reproductive Technology; Practice Committee of American Society for Reproductive Medicine. Elective single-embryo transfer. Fertil Steril 2012;97:835–42. 10.1016/j.fertnstert.2011.11.050 [DOI] [PubMed] [Google Scholar]
- 35.Practice Committee of American Society for Reproductive Medicine; Practice Committee of Society for Assisted Reproductive Technology. Criteria for number of embryos to transfer: a committee opinion. Fertil Steril 2013;99:44–6. 10.1016/j.fertnstert.2012.09.038 [DOI] [PubMed] [Google Scholar]
- 36.Practice Committee of the Society for Assisted Reproductive Technology; American Society for Reproductive Medicine. Guidelines on the number of embryos transferred. Fertil Steril 2004;82(Suppl 1):1–2. 10.1016/j.fertnstert.2004.07.937 [DOI] [PubMed] [Google Scholar]
- 37.Practice Committee of the Society for Assisted Reproductive Technology; Practice Committee of the American Society for Reproductive Medicine. Guidelines on number of embryos transferred. Fertil Steril 2006;86(Suppl 1):S51–2. 10.1016/j.fertnstert.2006.07.1473 [DOI] [PubMed] [Google Scholar]
- 38.Practice Committee of Society for Assisted Reproductive Technology; Practice Committee of American Society for Reproductive Medicine. Guidelines on number of embryos transferred. Fertil Steril 2008;90(Suppl):S163–4. 10.1016/j.fertnstert.2008.08.053 [DOI] [PubMed] [Google Scholar]
- 39.Practice Committee of the American Society for Reproductive Medicine; Practice Committee of the Society for Assisted Reproductive Technology. Guidelines on number of embryos transferred. Fertil Steril 2009;92:1518–9. 10.1016/j.fertnstert.2009.08.059 [DOI] [PubMed] [Google Scholar]
- 40.Kissin DM, Kulkarni AD, Mneimneh A, et al. ; National ART Surveillance System (NASS) group. Embryo transfer practices and multiple births resulting from assisted reproductive technology: an opportunity for prevention. Fertil Steril 2015;103:954–61. 10.1016/j.fertnstert.2014.12.127 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Coddington CC, Jensen JR. Multiple pregnancy: changing expectations for patients and patterns for physicians. Fertil Steril 2015;103:898–9. 10.1016/j.fertnstert.2015.01.027 [DOI] [PubMed] [Google Scholar]
- 42.Maheshwari A, Griffiths S, Bhattacharya S. Global variations in the uptake of single embryo transfer. Hum Reprod Update 2011;17:107–20. 10.1093/humupd/dmq028 [DOI] [PubMed] [Google Scholar]
- 43.Jain T, Harlow BL, Hornstein MD. Insurance coverage and outcomes of in vitro fertilization. N Engl J Med 2002;347:661–6. 10.1056/NEJMsa013491 [DOI] [PubMed] [Google Scholar]
- 44.Nachtigall RD, MacDougall K, Davis AC, Beyene Y. Expensive but worth it: older parents’ attitudes and opinions about the costs and insurance coverage for in vitro fertilization. Fertil Steril 2012;97:82–7. 10.1016/j.fertnstert.2011.10.019 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Kissin DM, Boulet SL, Jamieson DJ; Assisted Reproductive Technology Surveillance and Research Team. Fertility Treatments in the United States: Improving Access and Outcomes. Obstet Gynecol 2016;128:387–90. 10.1097/AOG.0000000000001419 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Practice Committee of American Society for Reproductive Medicine. Multiple gestation associated with infertility therapy: an American Society for Reproductive Medicine Practice Committee opinion. Fertil Steril 2012;97:825–34. 10.1016/j.fertnstert.2011.11.048 [DOI] [PubMed] [Google Scholar]
- 47.Behrman RE, Butler AS, editors. Preterm birth: causes, consequences, and prevention. Washington, DC: National Academies Press; 2007. [PubMed] [Google Scholar]
- 48.Boulet SL, Schieve LA, Nannini A, et al. Perinatal outcomes of twin births conceived using assisted reproduction technology: a population-based study. Hum Reprod 2008;23:1941–8. 10.1093/humrep/den169 [DOI] [PubMed] [Google Scholar]
- 49.Wright VC, Schieve LA, Reynolds MA, Jeng G. Assisted reproductive technology surveillance—United States, 2000. MMWR Surveill Summ 2003;52. Erratum in: MMWR Morb Mortal Wkly Rep 2003;52:942. [PubMed] [Google Scholar]
- 50.Grobman WA, Milad MP, Stout J, Klock SC. Patient perceptions of multiple gestations: an assessment of knowledge and risk aversion. Am J Obstet Gynecol 2001;185:920–4. 10.1067/mob.2001.117305 [DOI] [PubMed] [Google Scholar]
- 51.Blennborn M, Nilsson S, Hillervik C, Hellberg D. The couple’s decision-making in IVF: one or two embryos at transfer? Hum Reprod 2005;20:1292–7. 10.1093/humrep/deh785 [DOI] [PubMed] [Google Scholar]
- 52.Pinborg A, Loft A, Schmidt L, Andersen AN. Attitudes of IVF/ICSI-twin mothers towards twins and single embryo transfer. Hum Reprod 2003;18:621–7. 10.1093/humrep/deg145 [DOI] [PubMed] [Google Scholar]
- 53.Ryan GL, Sparks AE, Sipe CS, Syrop CH, Dokras A, Van Voorhis BJ. A mandatory single blastocyst transfer policy with educational campaign in a United States IVF program reduces multiple gestation rates without sacrificing pregnancy rates. Fertil Steril 2007;88:354–60. 10.1016/j.fertnstert.2007.03.001 [DOI] [PubMed] [Google Scholar]
- 54.Hope N, Rombauts L. Can an educational DVD improve the acceptability of elective single embryo transfer? a randomized controlled study. Fertil Steril 2010;94:489–95. 10.1016/j.fertnstert.2009.03.080 [DOI] [PubMed] [Google Scholar]
- 55.Murray S, Shetty A, Rattray A, Taylor V, Bhattacharya S. A randomized comparison of alternative methods of information provision on the acceptability of elective single embryo transfer. Hum Reprod 2004;19:911–6. 10.1093/humrep/deh176 [DOI] [PubMed] [Google Scholar]
- 56.Lemos EV, Zhang D, Van Voorhis BJ, Hu XH. Healthcare expenses associated with multiple vs singleton pregnancies in the United States. Am J Obstet Gynecol 2013;209:586.e1–11. 10.1016/j.ajog.2013.10.005 [DOI] [PubMed] [Google Scholar]
- 57.Henne MB, Bundorf MK. The effects of competition on assisted reproductive technology outcomes. Fertil Steril 2010;93:1820–30. 10.1016/j.fertnstert.2008.02.159 [DOI] [PubMed] [Google Scholar]
- 58.Luke B, Brown MB, Wantman E, et al. Application of a validated prediction model for in vitro fertilization: comparison of live birth rates and multiple birth rates with 1 embryo transferred over 2 cycles vs 2 embryos in 1 cycle. Am J Obstet Gynecol 2015;212:676.e1–7. 10.1016/j.ajog.2015.02.005 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Fiddelers AAA, Severens JL, Dirksen CD, Dumoulin JC, Land JA, Evers JL. Economic evaluations of single- versus double-embryo transfer in IVF. Hum Reprod Update 2007;13:5–13. 10.1093/humupd/dml053 [DOI] [PubMed] [Google Scholar]
- 60.Crawford S, Boulet S, Mneimneh A, et al. Costs of achieving live birth from assisted reproductive technology: a comparison of sequential single and double embryo transfer approaches. Fertil Steril 2016;105:444–50. 10.1016/j.fertnstert.2015.10.032 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Kulkarni AD, Jamieson DJ, Jones HW Jr, et al. Fertility treatments and multiple births in the United States. N Engl J Med 2013;369:2218–25. 10.1056/NEJMoa1301467 [DOI] [PubMed] [Google Scholar]
- 62.Callaghan WM, MacDorman MF, Rasmussen SA, Qin C, Lackritz EM. The contribution of preterm birth to infant mortality rates in the United States. Pediatrics 2006;118:1566–73. 10.1542/peds.2006-0860 [DOI] [PubMed] [Google Scholar]
- 63.Tanner K, Sabrine N, Wren C. Cardiovascular malformations among preterm infants. Pediatrics 2005;116:e833–8. 10.1542/peds.2005-0397 [DOI] [PubMed] [Google Scholar]
- 64.Rasmussen SA, Moore CA, Paulozzi LJ, Rhodenhiser EP. Risk for birth defects among premature infants: a population-based study. J Pediatr 2001;138:668–73. 10.1067/mpd.2001.112249 [DOI] [PubMed] [Google Scholar]
- 65.Kissin DM, Jamieson DJ, Barfield WD. Monitoring health outcomes of assisted reproductive technology. N Engl J Med 2014;371:91–3. 10.1056/NEJMc1404371 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.CDC. National public health action plan for the detection, prevention, and management of infertility. Atlanta, GA: CDC; 2014. https://www.cdc.gov/reproductivehealth/Infertility/PDF/DRH_NAP_Final_508.pdf [DOI] [PubMed]
- 67.Martin JA, Hamilton BE, Osterman MJK. Three decades of twin births in the United States, 1980–2009. NCHS Data Brief 2012;80:1–8. [PubMed] [Google Scholar]
- 68.D’Angelo DV, Whitehead N, Helms K, Barfield W, Ahluwalia IB. Birth outcomes of intended pregnancies among women who used assisted reproductive technology, ovulation stimulation, or no treatment. Fertil Steril 2011;96:314–320.e2. 10.1016/j.fertnstert.2011.05.073 [DOI] [PubMed] [Google Scholar]
- 69.Barradas DT, Barfield WD, Wright V, D’Angelo D, Manning SE, Schieve LA. Assessment of assisted reproductive technology use questions: Pregnancy Risk Assessment Monitoring System Survey, 2004. Public Health Rep 2012;127:516–23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Kissin DM, Jamieson DJ, Barfield WD. Assisted reproductive technology program reporting [Letter]. JAMA 2011;306:2564–; author reply 2564–5.. 10.1001/jama.2011.1843 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Mneimneh AS, Boulet SL, Sunderam S, et al. ; States Monitoring ART (SMART) Collaborative. States Monitoring Assisted Reproductive Technology (SMART) Collaborative: data collection, linkage, dissemination, and use. J Womens Health (Larchmt) 2013;22:571–7. 10.1089/jwh.2013.4452 [DOI] [PubMed] [Google Scholar]