Abstract
Background
National Early Warning Score (NEWS) is increasingly used in UK hospitals. However, there is only limited evidence to support the use of pre-hospital early warning scores. We hypothesised that pre-hospital NEWS was associated with death or critical care escalation within the first 48 h of hospital stay.
Methods
Planned secondary analysis of a prospective cohort study at a single UK teaching hospital. Consecutive medical ward admissions over a 20-day period were included in the study. Data were collected from ambulance report forms, medical notes and electronic patient records. Pre-hospital NEWS was calculated retrospectively. The primary outcome was a composite of death or critical care unit escalation within 48 h of hospital admission. The secondary outcome was length of hospital stay.
Results
189 patients were included in the analysis. The median pre-hospital NEWS was 3 (IQR 1–5). 13 patients (6.9%) died or were escalated to the critical care unit within 48 h of hospital admission. Pre-hospital NEWS was associated with death or critical care unit escalation (OR, 1.25; 95% CI, 1.04–1.51; p = 0.02), but NEWS on admission to hospital was more strongly associated with this outcome (OR, 1.52; 95% CI, 1.18–1.97, p < 0.01). Neither was associated with hospital length of stay.
Conclusion
Pre-hospital NEWS was associated with death or critical care unit escalation within 48 h of hospital admission. NEWS could be used by ambulance crews to assist in the early triage of patients requiring hospital treatment or rapid transport. Further cohort studies or trials in large samples are required before implementation.
Keywords: Pre-hospital, Clinical research, Intensive care, Acute care emergency ambulance systems
Highlights
-
•
NEWS has a growing dominance in UK hospitals but is not widely used in ambulances.
-
•
NEWS calculated using ambulance observations is associated with in-hospital death and critical care unit admission.
-
•
NEWS could be used by ambulance crews as an objective tool to triage patients with acute illness.
-
•
A large scale trial should be carried out before widespread implementation of NEWS in ambulances.
-
•
It is unclear if NEWS could be used by a call-taker or bystander to triage a patient before the ambulance arrives.
1. Introduction
Early warning scores or rapid response systems are commonplace in UK hospitals [1]. They assign weighting to routine clinical measurements and are used to detect patients in need of clinical review or resuscitation [2]. The National Early Warning Score (NEWS), developed by the Royal College of Physicians, is designed to standardise and replace the multiple existing early warning previously used in UK hospitals (Table 1) [3]. NEWS is associated with clinical outcome, including hospital mortality and intensive care unit admission [[4], [5], [6], [7], [8]]. However, early warning scores are not widely used in the pre-hospital setting, reflecting the limited current evidence available to support their use.
Table 1.
National early warning score calculation.
| National Early Warning Score (NEWS) | |||||||
|---|---|---|---|---|---|---|---|
| 3 | 2 | 1 | 0 | 1 | 2 | 3 | |
| Temperature (°C) | <35.0 | 35.1–36.0 | 36.1–38.0 | 38.1–39.0 | >39.0 | ||
| Heart rate (beats/min) | <41 | 41–50 | 51–90 | 91–110 | 111–130 | >130 | |
| Systolic BP (mmHg) | <91 | 91–100 | 101–110 | 111–219 | >219 | ||
| Respiratory Rate (breaths/min) | <9 | 9–11 | 12–20 | 21–24 | >25 | ||
| Oxygen Saturation (%) | <92 | 92–93 | 94–95 | >96 | |||
| Supplemental oxygen | Yes | No | |||||
| CNS response (AVPU) | A | V, P, U | |||||
Only two studies have evaluated pre-hospital early warning scores. A retrospective review of patients admitted to a single emergency department by ambulance found that modified early warning score (MEWS) – a similar scoring system that pre-dates NEWS - was more sensitive than clinician judgement for identifying critical illness in the community [9]. A prospective cohort study of patients with medical and trauma presentations admitted to a single hospital by ambulance found that NEWS was associated with intensive care unit admission and mortality [10]. However, it is unclear whether these results are generalisable to other populations with different demographics and case mixes. In addition, it is unclear whether a pre-hospital early warning score could be used by hospital staff for inpatient risk stratification. Therefore the importance of ambulance early warning scores to both ambulance crews and hospital physicians remains uncertain.
We hypothesise that NEWS derived from pre-hospital observations is associated with critical care unit escalation or death within 48 h of hospital admission. We further hypothesise that NEWS derived from pre-hospital observations is more strongly associated with the outcome measure than NEWS on admission to hospital.
2. Method
2.1. Study design
This was a planned secondary analysis of data from an observational cohort study of adult patients admitted to a single hospital with acute medical presentations [4,11]. The methods and results of the main study have been published previously [4,11]. All new adult medical admissions to the Acute Assessment Unit (AAU) at the Royal London Hospital between 25th March and 13th April 2013 that were brought to hospital by ambulance were included in this analysis. Patients admitted directly to the critical care unit from the emergency department were not included. The National Research Ethics Service prospectively reviewed and approved this study (12/LO/1985). The study was registered retrospectively with Research Registry (UIN: researchregistry3194). We report the results of this analysis in accordance with the SRTOBE/STROCCS reporting statements [12,13].
2.2. Data collection
The exposures of interest were NEWS calculated from physiological observations obtained by ambulance staff before hospital admission, and NEWS derived from similar observations on admission to hospital. Researchers prospectively collected physiological measurements that were recorded by nurses or healthcare assistants at the point of admission to the Acute Assessment Unit. Researchers retrospectively reviewed ambulance service patient report forms for these patients and recorded the first set of observations measured by the ambulance crew. Data were considered missing if there were no observations recorded on the ambulance patient report form or if there were no observations recorded on the bedside observation chart within 24 h of admission to hospital. Researchers recorded data on paper data collection forms and transferred this to an electronic database. The database was independently checked for accuracy. The outcome measures were determined by checking patient notes, electronic patient records and discharge summaries. We calculated NEWS retrospectively using Microsoft Excel (Microsoft Inc., Redmond WA) [4,11].
2.3. Outcome measures
The primary outcome measure was a composite of critical care unit escalation and death within 48 h of admission to hospital [4,11]. At this centre, critical care consists of level three care (renal replacement therapy, advanced respiratory support or multi-organ support) and level two care (‘step down’ from a higher level of care, single organ support, high frequency nursing care or invasive monitoring). This primary outcome definition has been used in previous studies and will identify all instances of in-hospital cardiac arrest at our institution [[4], [5], [6],11,14]. The secondary outcome measure was length of hospital stay [4,11].
2.4. Statistical analysis
Data were analysed using SPSS version 21 (IBM, Armonk, NY). Data were stratified according to the presence or absence of ambulance data. Missing data were handled by list-wise deletion. In order to test for association between NEWS and the primary outcome measure, multivariable logistic regression models were constructed and adjusted for age and gender - a strategy consistent with previous similar research [5,6]. NEWS was firstly considered as a continuous variable. Odds ratios derived from pre-hospital observations (pre-hospital NEWS) and for admission observations (admission NEWS) were calculated and compared. Secondly, NEWS was considered as a categorical variable, with the sample divided according to the recommended risk groups (NEWS 1–4, 5–6, >7) and the analysis repeated [15]. Thirdly, the correlation between pre-hospital NEWS and admission NEWS was assessed using the Pearson product-moment correlation coefficient. Finally, to test for association between NEWS and the secondary outcome measure (length of hospital stay), a linear regression model was constructed, where length of stay was considered a continuous variable. The r2 values for pre-hospital NEWS with admission NEWS were compared.
3. Results
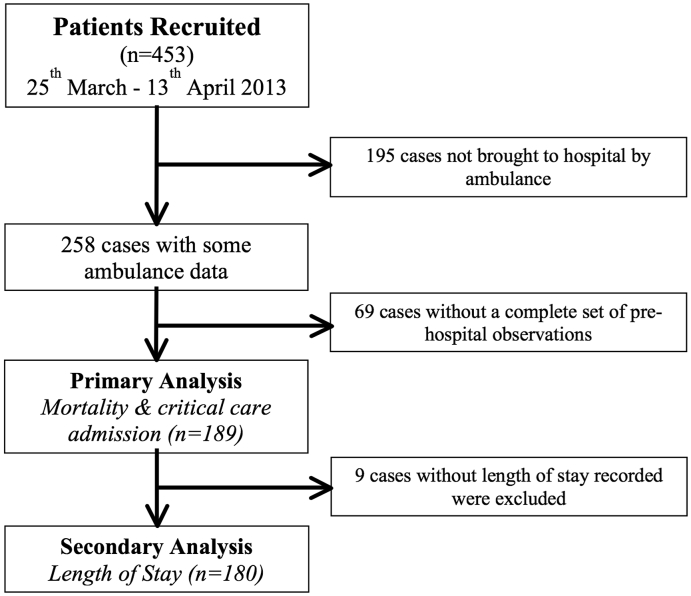
453 adult medical patients were admitted during the study period, of which 258 were brought to hospital by ambulance. After excluding cases with missing data, 189 cases were included in the primary analysis and 180 were included in the secondary analysis (Fig. 1). The mean age of the entire cohort was 61 (sd. 22) years, compared to 67 (sd. 21) years for patients admitted by ambulance. There was no difference in the gender distribution for patients admitted by ambulance, compared to entire cohort. 13 patients (6.9%) admitted by ambulance died or were escalated to the critical care unit within 48 h. The median length of stay for patients admitted by ambulance was 4 (IQR 2–8) days. Baseline characteristics are provided in Table 2.
Fig. 1.
Flow diagram of cases included in the analysis.
Table 2.
Baseline characteristics and diagnosis groups.
| Whole cohort | Admitted by ambulance | |
|---|---|---|
| Sample size (n) | 453 | 258 |
| Age in years (sd) | 60.9 (22.4) | 67.4 (20.5) |
| Female (%) | 242 (53.5) | 138 (53.5) |
| Admission NEWS (IQR) | 2 (1–3) | 2 (1–3) |
| Ambulance NEWS (IQR) | – | 3 (1–5) |
| Post-take Diagnosis Category | ||
| General Medical | 114 (25.2) | 70 (27.1) |
| Respiratory | 71 (15.7) | 47 (18.2) |
| Health Care of the Elderly | 54 (11.9) | 52 (20.1) |
| Cardiology | 54 (11.9) | 25 (9.7) |
| Gastroenterology | 35 (7.7) | 14 (5.4) |
| Neurological | 30 (6.6) | 14 (5.4) |
| Haematology | 30 (6.6) | 11 (4.3) |
| Endocrinology | 16 (3.5) | 8 (3.1) |
| Psychiatry | 13 (2.9) | 6 (2.3) |
| Oncology | 12 (2.7) | 6 (2.3) |
| Surgery | 10 (2.2) | <5 (<1.9) |
| Rheumatology | 5 (1.1) | <5 (<1.9) |
| Nephrology | <5 (<1.1) | <5 (<1.9) |
| Infection & Immunology | <5 (<1.1) | <5 (<1.9) |
| Other | <5 (<1.1) | <5 (<1.9) |
Values are presented as n (%) unless otherwise stated. Age is presented as mean (sd) and NEWS is presented as median (IQR).
Multivariable logistic regression analysis was used to test for the association between NEWS and the primary outcome measure. When considered as a continuous variable, pre-hospital NEWS and admission NEWS were both associated with the primary outcome measure (OR, 1.25; 95% CI, 1.04–1.51; p = 0.02 and OR, 1.52; 95% CI, 1.18–1.97, p < 0.01 respectively) (Table 3). When considered as a categorical variable, pre-hospital NEWS and admission NEWS were both associated with the primary outcome measure (Table 4).
Table 3.
Association of pre-hospital NEWS and admission NEWS with critical care unit escalation or death within 48 h of hospital admission.
| Odds Ratio | p-value | |
|---|---|---|
| Pre-hospital NEWS | 1.25 (1.04–1.51) | 0.02 |
| Age | 1.01 (0.97–1.05) | 0.60 |
| Gender | 3.98 (1.02–15.55) | 0.05 |
| Admission NEWS | 1.52 (1.18–1.97) | <0.01 |
| Age | 1.00 (0.96–1.04) | 0.97 |
| Gender | 5.37 (1.07–26.88) | 0.04 |
Multivariable logistic regression analysis with adjustment for age and gender. Presented as odds ratios with 95% confidence intervals.
Table 4.
Association of pre-hospital NEWS and admission NEWS (categorical variables) with critical care unit escalation or death within 48 h of hospital admission.
| Odds Ratio | p-value | |
|---|---|---|
| Pre-hospital NEWS | ||
| NEWS 0–4 (reference) | – | – |
| NEWS 5–6 | 2.95 | 0.23 |
| NEWS ≥7 | 4.45 | 0.03 |
| Age | 1.01 | 0.64 |
| Gender | 4.27 | 0.04 |
| Admission NEWS | ||
| NEWS 0–4 (reference) | – | – |
| NEWS 5–6 | 4.02 | 0.08 |
| NEWS ≥7 | 8.70 | 0.01 |
| Age | 1.01 | 0.70 |
| Gender | 3.61 | 0.07 |
Multivariable logistic regression analysis with adjustment for age and gender. Reference = reference category.
We identified a moderate correlation between pre-hospital NEWS and admission NEWS (r = 0.44, p < 0.01). Pre-hospital NEWS differed from admission NEWS in 33 cases (17.4%), of which 7 cases (21.2%) had a greater admission NEWS and 26 cases (78.8%) had a greater pre-hospital NEWS. Neither pre-hospital nor admission NEWS were associated with hospital length of stay (r2 = 5.1%, p = 0.48 and r2 = 5.2%, p = 0.92 respectively).
4. Discussion
The main finding of this analysis is that NEWS derived from pre-hospital observations is associated with critical care unit escalation or death within 48 h of hospital admission. But, NEWS derived from observations taken on admission to the medical ward were more strongly associated with critical care unit escalation or death within 48 h of hospital admission, compared to NEWS derived from pre-hospital observations. This study identified a moderate correlation between ambulance NEWS and admission NEWS – in 83% of cases NEWS at both time points was the same. Where the scores were different, ambulance NEWS was greater in the majority of cases suggesting an improvement in clinical condition between pre-hospital assessment and medical ward admission. However, the variability in measurement techniques, equipment or clinical practice must be considered when interpreting these results. Patients with a pre-hospital NEWS of 7 or more had a four-fold increase in the odds of death or critical care unit admission compared to patients with a pre-hospital NEWS of 4 or less. Pre-hospital NEWS was not associated with hospital length of stay; this is consistent with our previous findings [4].
Our results are similar to other published work in this area. A recent single-centre observational study identified association between NEWS calculated using ambulance data and both intensive care unit admission and mortality within 48 h of hospital admission [10]. Other authors found that another early warning score (MEWS), when calculated using ambulance data, was associated with in-hospital adverse outcomes [9]. Our results suggest that pre-hospital NEWS may be a useful tool in guiding patient management by ambulance crews. This supports a small but growing body of evidence advocating the use of pre-hospital early warning scores. However, their uptake by emergency medical services is reportedly slow [10]. Some authors have suggested using early warning scores to help trigger a blue-light transfer to hospital, much like the urgent clinical review triggered by an in-hospital NEWS of five or more [9]. Our results suggest that pre-hospital NEWS ≥7 would be an appropriate threshold for this. NEWS could be incorporated into the patient report forms used by emergency medical services, which would be akin to the bedside observation charts used in many hospitals. In addition, further consideration should be given to whether NEWS can be used all patient groups, since some studies suggest that population specific early warning scores should be used in hospital, for example PEWS in paediatric patients, MEOWS in obstetric patients and CREWS in patients with COPD [[16], [17], [18]]. From the point of view of the hospital physician, our results suggest that pre-hospital NEWS is not a better marker of clinical status compared to NEWS calculated on admission to hospital. Thus, whilst our results demonstrate the efficacy of pre-hospital NEWS, we are cautious in drawing conclusions regarding its effectiveness in the real clinical environment. We acknowledge that this is a single-centre study, so our results may not be generalisable to other clinical settings.
A strength of our analysis is that our sample represents a broad spectrum of medical specialities (Table 2), but unlike other research in this field, it excluded patients suffering traumatic injury [10]. Inpatient data, including admission NEWS, were collected prospectively. However, for logistical reasons we were only able to collect the ambulance data in retrospect. At the time the study was conducted NEWS was not routinely used at our institution, which necessitated retrospective calculation of NEWS. This approach avoids observer error associated with early warning score calculation, which has been previously reported with a frequency of 18–27% [4,17,19,20].
This analysis has a number of limitations. Our sample size was 258, but we were only able to include 189 cases in the primary analysis due to a higher than expected rate of missing data from the ambulance patient report forms. While our sample is a similar size to other studies of early warning scores, the missing data could represent a source of selection bias [9,10,17,21]. In order to minimise this potential source of bias, future studies should implement strategies to minimise missing data from ambulance report forms. We used a composite outcome measure of critical care admission or death within two days of hospital admission, which has been used in similar studies [5,6,14]. Our definition of critical care was based on the Intensive Care Society description, including level two and three care [22]. This reflects the organisation at our institution and may be different to other hospitals. We excluded patients who were admitted to the critical care unit directly from the emergency department, since this was a study of adult medical patients who, due to the limits of our ethics approval, were included in the study after admission to a medical ward. This could affect the event rate. However, in our sample 6.9% of patients reached the primary outcome, which is similar to other studies of this type [9,23]. Our statistical methods are appropriate to the sample size. The sample includes a small number of patients receiving palliative care. We ran a sensitivity analysis that excluded these cases and the results were very similar.
5. Conclusion
Pre-hospital NEWS is associated with death or critical care unit escalation within 48 h of hospital admission. However, admission NEWS is more strongly associated with outcome, which may represent patients who fail to improve despite treatment by the ambulance crew. Pre-hospital care may represent an important and useful extension of NEWS. However, evidence from large multi-centre studies is needed before implementing a pre-hospital version of NEWS.
Ethical approval
Research ethics approval was provided by the National Research Ethics Service (12/LO/1985).
Funding
Nil.
Author contribution
Study design: TA, NV, DI, JE.
Data collection: TA, HT, DI, NV.
Statistical analysis: NC.
Writing first draft of manuscript: TA.
Critical review and approval of manuscript: All.
Conflicts of interest
No conflicts to declare.
Guarantor
TA/NC/NV/JE.
Acknowledgements
The authors would like to thank Matt Wells for his help with the data collection.
References
- 1.Patterson C., Maclean F., Bell C. Early warning systems in the UK: variation in content and implementation strategy has implications for a NHS early warning system. Clin. Med. 2011;11(5):424–427. doi: 10.7861/clinmedicine.11-5-424. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.McGinley A., Pearse R.M. A national early warning score for acutely ill patients. Bmj. 2012;345 doi: 10.1136/bmj.e5310. [published Online First: Epub Date]|. [DOI] [PubMed] [Google Scholar]
- 3.Jones M. NEWSDIG: the national early warning score development and implementation group. Clin. Med. 2012;12(6):501–503. doi: 10.7861/clinmedicine.12-6-501. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Abbott T.E., Vaid N., Ip D. A single-centre observational cohort study of admission National Early Warning Score (NEWS) Resuscitation. 2015;92:89–93. doi: 10.1016/j.resuscitation.2015.04.020. [published Online First: Epub Date]|. [DOI] [PubMed] [Google Scholar]
- 5.Cooksley T., Kitlowski E., Haji-Michael P. Effectiveness of modified early warning score in predicting outcomes in oncology patients. QJM Mon. J. Assoc. Phys. 2012;105(11):1083–1088. doi: 10.1093/qjmed/hcs138. [published Online First: Epub Date]|. [DOI] [PubMed] [Google Scholar]
- 6.Corfield A.R., Lees F., Zealley I. Utility of a single early warning score in patients with sepsis in the emergency department. Emerg. Med. J. EMJ. 2014;31(6):482–487. doi: 10.1136/emermed-2012-202186. [published Online First: Epub Date]|. [DOI] [PubMed] [Google Scholar]
- 7.Romero-Brufau S., Huddleston J.M., Naessens J.M. Widely used track and trigger scores: are they ready for automation in practice? Resuscitation. 2014;85(4):549–552. doi: 10.1016/j.resuscitation.2013.12.017. [published Online First: Epub Date]|. [DOI] [PubMed] [Google Scholar]
- 8.Smith G.B., Prytherch D.R., Meredith P. The ability of the National Early Warning Score (NEWS) to discriminate patients at risk of early cardiac arrest, unanticipated intensive care unit admission, and death. Resuscitation. 2013;84(4):465–470. doi: 10.1016/j.resuscitation.2012.12.016. [published Online First: Epub Date]|. [DOI] [PubMed] [Google Scholar]
- 9.Fullerton J.N., Price C.L., Silvey N.E. Is the Modified Early Warning Score (MEWS) superior to clinician judgement in detecting critical illness in the pre-hospital environment? Resuscitation. 2012;83(5):557–562. doi: 10.1016/j.resuscitation.2012.01.004. [published Online First: Epub Date]|. [DOI] [PubMed] [Google Scholar]
- 10.Silcock D.J., Corfield A.R., Gowens P.A. Validation of the national early warning score in the prehospital setting. Resuscitation. 2015;89:31–35. doi: 10.1016/j.resuscitation.2014.12.029. [published Online First: Epub Date]|. [DOI] [PubMed] [Google Scholar]
- 11.Abbott T.E., Torrance H.D., Cron N. A single-centre cohort study of National Early Warning Score (NEWS) and near patient testing in acute medical admissions. Eur. J. Intern. Med. 2016;35:78–82. doi: 10.1016/j.ejim.2016.06.014. [DOI] [PubMed] [Google Scholar]
- 12.von Elm E., Altman D.G., Egger M. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet. 2007;370(9596):1453–1457. doi: 10.1016/S0140-6736(07)61602-X. [DOI] [PubMed] [Google Scholar]
- 13.Agha R.A., Borrelli M.R., Vella-Baldacchino M., Thavayogan R., Orgill D.P., for the STROCSS Group The STROCSS statement: strengthening the reporting of cohort studies in surgery. Int. J. Surg. 2017;46:198–202. doi: 10.1016/j.ijsu.2017.08.586. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Peris A., Zagli G., Maccarrone N. The use of Modified Early Warning Score may help anesthesists in postoperative level of care selection in emergency abdominal surgery. Minerva Anestesiol. 2012;78(9):1034–1038. [PubMed] [Google Scholar]
- 15.The Royal College of Physicians . 2012. National Early Warning Score (NEWS): Standardising the Assessment of Acute- Illness Severity in the NHS. Report of a working party. London. [Google Scholar]
- 16.Miranda J.O.F., Carmargo C.L., Nascimento C.L.S. Accuracy of a pediatric early warning score in the recognition of clinical deterioration. Rev. Lat. Am. Enfermagem. 2017;10 doi: 10.1590/1518-8345.1733.2912. 25:e2912. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Eccles S.R., Subbe C., Hancock D. CREWS: improving specificity whilst maintaining sensitivity of the National Early Warning Score in patients with chronic hypoxaemia. Resuscitation. 2014;85(1):109–111. doi: 10.1016/j.resuscitation.2013.08.277. [published Online First: Epub Date]|. [DOI] [PubMed] [Google Scholar]
- 18.Singh S., McGlennan A., England A. A validation study of the CEMACH recommended modified early obstetric warning system (MEOWS) Anaesthesia. 2012;67(1):12–18. doi: 10.1111/j.1365-2044.2011.06896.x. [DOI] [PubMed] [Google Scholar]
- 19.Kolic I., Crane S., McCartney S. Factors affecting response to national early warning score (NEWS) Resuscitation. 2015 doi: 10.1016/j.resuscitation.2015.02.009. [published Online First: Epub Date]|. [DOI] [PubMed] [Google Scholar]
- 20.Subbe C.P., Gao H., Harrison D.A. Reproducibility of physiological track-and-trigger warning systems for identifying at-risk patients on the ward. Intensive Care Med. 2007;33(4):619–624. doi: 10.1007/s00134-006-0516-8. [published Online First: Epub Date]|. [DOI] [PubMed] [Google Scholar]
- 21.Jo S., Lee J.B., Jin Y.H. Modified early warning score with rapid lactate level in critically ill medical patients: the ViEWS-L score. Emerg. Med. J. EMJ. 2013;30(2):123–129. doi: 10.1136/emermed-2011-200760. [published Online First: Epub Date]|. [DOI] [PubMed] [Google Scholar]
- 22.Intensive Care Society . 2009. Levels of Critical Care for Adult Patients. [Google Scholar]
- 23.Tirkkonen J., Olkkola K.T., Huhtala H. Medical emergency team activation: performance of conventional dichotomised criteria versus national early warning score. Acta Anaesthesiol. Scand. 2014;58(4):411–419. doi: 10.1111/aas.12277. [published Online First: Epub Date]|. [DOI] [PubMed] [Google Scholar]