Abstract
Introduction:
The angiotensin-converting enzyme 2 (ACE2)/angiotensin (Ang)-(1–7)/Mas axis could modulate the heart rate (HR) and blood pressure variabilities (BPV) which are important predictors of cardiovascular risk and provide information about the autonomic modulation of the cardiovascular system. Therefore we investigated the effect of Mas deficiency on autonomic modulation in wild type and Mas-knockout (KO) mice.
Methods:
Blood pressure was recorded at high sample rate (4000 Hz). Stationary sequences of 200–250 beats were randomly chosen. Frequency domain analysis of HR and BPV was performed with an autoregressive algorithm on the pulse interval sequences and on respective systolic sequences.
Results:
The KO group presented an increase of systolic arterial pressure (SAP; 127.26±11.20 vs 135.07±6.98 mmHg), BPV (3.54±1.54 vs 5.87±2.12 mmHg2), and low-frequency component of systolic BPV (0.12±0.11 vs 0.47±0.34 mmHg2).
Conclusions:
The deletion of Mas receptor is associated with an increase of SAP and with an increased BPV, indicating alterations in autonomic control. Increase of sympathetic vascular modulation in absence of Mas evidences the important role of Ang-(1–7)/Mas on cardiovascular regulation. Moreover, the absence of significant changes in HR and HRV can indicate an adaptation of autonomic cardiac balance. Our results suggest that the Ang-(1–7)/Mas axis seems more important in autonomic modulation of arterial pressure than HR.
Keywords: Renin–angiotensin system, angiotensin-(1–7), Mas receptor, autonomic modulation, blood pressure variability, heart rate variability
Introduction
The neural regulation of circulatory function is mainly accomplished through the interplay of the sympathetic and vagal outflows.1 This interaction can be explored by assessing cardiovascular rhythmicity with appropriate spectral methodologies.2 Spectral analysis of cardiovascular signal variability, and in particular of RR period (heart rate variability, HRV), is a widely used procedure to investigate autonomic cardiovascular control and/or target function impairment.1–3 The oscillatory pattern which characterizes the spectral profile of heart rate (HR) and arterial pressure short-term variability consists of two major components, at low (LF, 0.04–0.15 Hz) and high (HF, synchronous with respiratory rate) frequency, respectively, related to vasomotor and respiratory activity. With this procedure the state of sympathovagal balance modulating sinus node pacemaker activity can be quantified in a variety of physiological and pathophysiological conditions.4 Changes in sympathovagal balance can be often detected in basal conditions; however, a reduced responsiveness to an excitatory stimulus is the most common feature that characterizes numerous pathophysiological states.
Some cardiovascular control systems affect blood pressure more rapidly and others more slowly. Thus, identifying the frequency components of blood pressure variability (BPV) by power spectral analysis can potentially provide important information on individual blood pressure control mechanisms.5 In conclusion, power spectral analysis is a powerful diagnostic tool that allows identification of pathophysiological mechanisms contributing to cardiovascular diseases, such as hypertension, heart failure, and stroke, because it can separate slow from fast cardiovascular control mechanisms.
The novel axis of renin–angiotensin system (RAS), angiotensin-converting enzyme 2 (ACE2)/angiotensin (Ang)-(1–7)/Mas appears to play an important role in the cardiovascular system by influencing peripheral and central mechanisms involved in the control of vascular tonus,6,7 and cardiac function.8
The expression of Mas and Ang-(1–7)-forming enzymes in blood vessels and the development of endothelial dysfunction in Mas-KO mice illustrates the importance of the local ACE2/Ang-(1–7)/Mas axis in blood vessels.9,10 On the other hand, ACE2, Mas, and Ang-(1–7) are present in different cardiovascular-related areas of the brain including rostral ventrolateral medulla (RVLM), caudal ventrolateral medulla (CVLM), nucleus of tractus solitarius (NTS), and hypothalamus.6,11,12
In these areas, especially in the brain stem, the ACE2/Ang-(1–7)/Mas axis could modulate the HR and blood pressure variabilities which are important predictors of cardiovascular risk and provide information about the autonomic modulation of cardiovascular system.2 In this study we investigated the effect of genetic deletion of Mas, a major component of the ACE2/Ang-(1–7)/Mas axis on autonomic modulations parameters.
Methods
Animals
Experiments were performed in male Ang-(1–7) receptor Mas-knockout (KO, n = 8) and wild type (WT, n = 6) FVB/N mice (25-30g), obtained from the transgenic animal facilities of the Laboratory of Hypertension, Federal University of Minas Gerais. The absence of expression of the Mas receptor was confirmed in all knockout animals used, based on genotypes analysis, determined from DNA extracted from the animal tail, using a polymerase chain reaction technique. The animals were housed in controlled-temperature rooms (22°C) with a 12:12-h dark-light cycle and received standard laboratory chow and water ad libitum. All animal protocols were approved by the Instituto de Cardiologia-Fundação Universitária de Cardiologia Ethics Committee under de approval number: UP: 2546/2009.
Hemodynamic measurements
Mice were anesthetized with intramuscular injection of ketamine (4.5 mg/kg) + xylazine (0.2 mg/kg) 24 h before the experimental protocol. Polyethylene catheters (PE-10, 0.28 mm ID, 0.61 mm OD, Biocorp Australia, Huntingdale, Victoria, Australia) filled with heparinized saline solution were inserted into the femoral artery for direct measurements of arterial pressure (AP). The body temperature was maintained at 37°C using a heating pad until the full recovery of animals, which were then placed in individual cages and kept in the experimental room for environmental adaptation. Conscious arterial pressure recording was performed following the protocol described previously.13
One day after the surgical procedure, a catheter was connected to a strain-gauge transducer coupled to a computer-based data acquisition system (model MP100 A-CE, Biopac Systems, CA, USA), and pulsatile arterial pressure (PAP) was continuously recorded. Mean arterial pressure (MAP) and HR were simultaneously calculated from the PAP with the software AcqKnowledge (version 3.5.3 for Windows) and continuously acquired. The files were stored and data was analyzed later.
Spectral analysis
After detecting the pulse intervals (PIs), the heart period was automatically calculated on a beat-to-beat basis as the time interval between two consecutive systolic peaks or PI. All detections were carefully checked to avoid erroneous detections or missed beats. Tachograms and systograms were created from AP signals through the beat-to-beat PI and SAP, respectively. Sequences of 200–300 beats were randomly chosen and if the randomly selected sequence included evident non stationarities the sequence was discarded and a new random selection was performed, using the stationary test reported previously.14 Frequency domain analysis of HRV and BPV was performed with an autoregressive algorithm on the PI interval sequences (tachogram) and on respective systolic sequences (systogram).2,15 The power spectral density was calculated for each time series. In this study, three spectral components were considered: very low frequency (VLF), from 0 to 0.10 Hz; low frequency (LF), from 0.10 to 1.00 Hz; and high frequency (HF), from 1.00 to 5.00 Hz. The spectral components were expressed in absolute (s2 or mmHg2) and normalized units (nu). Normalization was obtained by calculating the power of LF and HF and correlating them to the total power without the very low frequency component (frequencies that were < 0.1 Hz).4 Spontaneous baroreflex sensitivity (BRS) was calculated using the alpha-index for the LF band (0.10–1.00 Hz). The coherence between R-R interval and SAP signal variability was assessed by means of a cross-spectral analysis. Alpha index was calculated only when the magnitude of the squared coherence between R-R and SAP signals, in the LF band, exceeded 0.5 (range = 0–1). Alpha index was obtained from the square root of the ratio between RR and SAP variability within the LF band.16
Statistical analysis
Data are presented as mean ± SD (see Table 1). Results from the protocol were compared using Student t test. The software GraphPad Prism 6.0 for Windows (GraphPad Software, San Diego, CA, United States) was used for the tests. The significance level was established at p < 0.05.
Table 1.
Hemodynamic parameters and spectral analysis results.
| WT (n = 6) | KO (n = 8) | |
|---|---|---|
| SAP (mmHg) | 127.26 ± 11.20 | 135.07 ± 6.98* |
| DAP (mmHg) | 100.64 ± 14.34 | 106.88 ± 9.62 |
| MAP (mmHg) | 111.78 ± 9.49 | 118.69 ± 5.37 |
| HR (bpm) | 642.11 ± 87.80 | 601.73 ± 103.91 |
| HRV - var (ms2) | 2.92 ± 4.94 | 2.11 ± 2.02 |
| - LF peak (Hz) | 0.63 ± 0.34 | 0.68 ± 0.35 |
| - LF (ms2) | 0.56 ± 0.90 | 0.52 ± 1.07 |
| - LF (nu) | 31.54 ± 20.87 | 22.64 ± 24.92 |
| - HF peak (Hz) | 3.81 ± 0.52 | 4.06 ± 0.72 |
| - HF (ms2) | 1.12 ± 1.33 | 1.34 ± 1.11 |
| - HF (nu) | 68.46 ± 20.87 | 77.36 ± 24.92 |
| - LF/HF index | 0.64 ± 0.76 | 0.54 ± 0.93 |
| SAPV – var (mmHg2) | 3.54 ± 1.54 | 5.87 ± 2.12* |
| - LF (mmHg2) | 0.12 ± 0.11 | 0.47 ± 0.34* |
| - HF (mmHg2) | 0.25 ± 0.33 | 0.20 ± 0.13 |
| - VLF (mmHg2) | 0.02 ± 0.04 | 0.41 ± 0.68 |
| SBS – alpha LF index (ms/mmHg) | 2.25 ± 2.20 | 0.93 ± 1.09 |
Values reported as mean ± SD. Systolic arterial pressure, SAP; diastolic arterial pressure, DAP; mean arterial pressure, MAP; heart rate, HR; heart rate variability, HRV; very low frequency component, VLF; low-frequency component, LF; high-frequency component, HF; sympathovagal balance, LF/HF; systolic arterial pressure variability, SAPV; spontaneous baroreflex sensitivity SBS. *p < 0.05 compared with control group.
Results
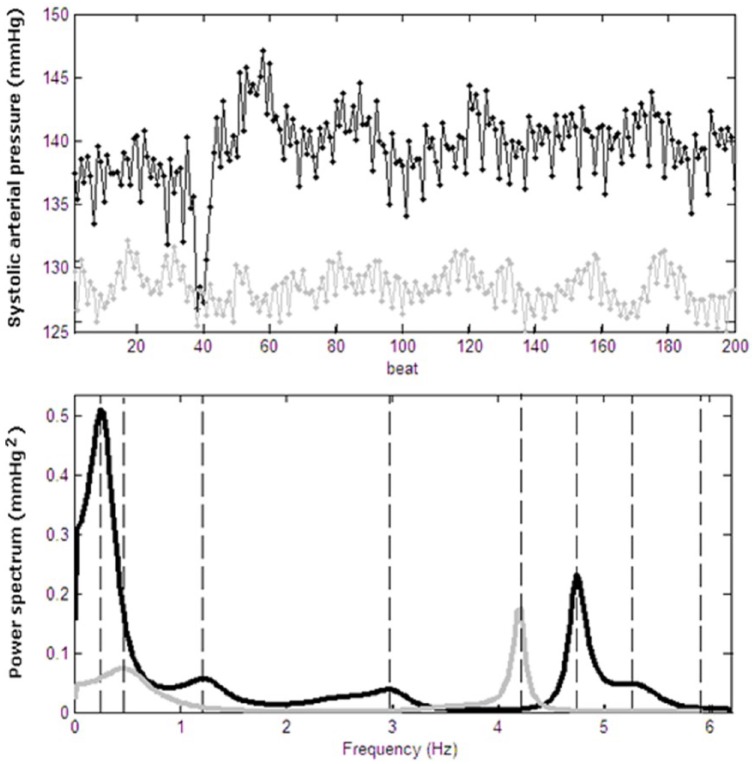
Regarding the results of this experimental protocol, the Mas deficiency group was characterized by some significant changes in power spectrum parameters in systolic BPV spectral profiles (Table 1). The Mas-KO group presented higher levels of systolic arterial pressure (SAP) and BPV when compared to control, wild type mice. In addition, the LF component of systolic BPV was higher in the Mas-KO group, indicating an increase of vascular sympathetic drive on this model. Figure 1 shows an example of spectral analysis applied to systolic series of WT group (gray lines) and KO group (black lines).
Figure 1.
The figure exemplifies the spectral analysis applied to systolic series of WT group (gray lines) and KO group (black lines). The figure is illustrative and reports an individual case.
Discussion
In this study we report for the first time an increase in SAP variability in Mas-KO mice. In addition, in keeping with previous reports,10 we observed an increase in blood pressure in Mas-KO mice. On the other hand, no significant changes in HR, in HRV, or in the sympathovagal balance were observed.
The casual interactions and relations between HRV and BPV, already recognized in the literature, can be described also by statistical characteristics related to the complexities of the time series. Such parameters demonstrate that the HRV and SAP series provide additional information and show variations on coupling information in different physiological and pathological situations.17 In this case, the mismatched variations may be related to physiological variations imposed by the model.
The absence of HR variability changes in our study contrast with previous observations of Walther et al.,18 who reported an increased sympathetic modulation of the HR in Mas-KO mice. However, in their study a low sample rate (250 Hz) was used which limits the capability to detect real changes in HR or SAP variability. In addition, differences in the genetic background (BL6/N in the Walter study and FVB/N in ours) may explain the differences between studies. For example, Mas-KO in the BL6/N are not hypertensive while blood pressure is increased in FVB/N Mas-KO mice.10 In female Mas-KO a reduction in HR variability was observed; however, again the sample rate (250 Hz) rate limits any conclusion regarding this finding.18
It has been described that Ang-(1–7) increase parasympathetic activity after intracerebroventricular (ICV) infusion or microinjection in the NTS.19,20 Indeed, genetic ablation of Mas, or ICV and NTS injection of A779,21 reduced the vagal component of baroreflex.22 These observations are in contrast with our current data showing absence of the sympathovagal balance alterations in Mas-KO mice. These differences suggest that the role of Ang-(1–7)/Mas in the autonomic modulation of HR is more evident upon transient challenge (baroreflex test) than steady-state changes in vagal activity like in the present study. However, this hypothesis awaits confirmation in future studies. Another contributing factor for HR and SAP variability could be derived from the kidney. It is possible that the lack of Ang-(1–7) action in the kidney could unbalance sodium and water excretion and indirectly impact on blood pressure and hence its variability, however changes in blood volume would preferentially influence long term blood pressure regulation. An influence in the beat-to-beat variability is unlike. The increased SAP levels and variability suggested an increased sympathetic modulation in blood vessel in Mas-KO mice.23,24 This is in accordance with a recent observation showing a strong effect of Ang-(1–7) on the adrenergic system in stress-induced increase in sympathetic activity,25 or amygdala stimulation.26
Mas-KO in the FVB/N background exhibited higher blood pressures compared to the control with a possible autonomic balance shifted in favor of the sympathetic tone.27
Furthermore, the possibility that the endothelial dysfunction present in Mas-deficient mice could contribute to the increased variability and increased sympathetic modulation in SAP should be considered,10 especially in light of a similar change was absent in HR. In summary, we have presented evidence for an increased sympathetic modulation of SAP in Mas-KO mice illustrating the importance of this GCPR in cardiovascular control. The absence of changes in HR deserves further studies for clarification.
Footnotes
Declaration of conflicting interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by National Institute of Science and Technology in Nanobiopharmaceutics, National Counsel of Technological and Scientific Development (Cnpq), Programa Nacional de Pós Doutorado (PNPD-CAPES), Fundação de Amparo à Pesquisa do Estado de Minas Gerais (FAPEMIG) and by Fundação de Amparo à Pesquisa do Estado do Rio Grande do Sul (FAPERGS).
References
- 1. Malliani A, Pagani M, Lombardi, et al. Cardiovascular neural regulation explored in the frequency domain. Circulation 1991; 84: 482–492. [DOI] [PubMed] [Google Scholar]
- 2. Montano N, Porta A, Cogliati C, et al. Heart rate variability explored in the frequency domain: a tool to investigate the link between heart and behavior. Neurosci Biobehav Rev 2009; 33: 71–80. [DOI] [PubMed] [Google Scholar]
- 3. Malliani A, Montano N. Heart rate variability as a clinical tool. Ital Heart J 2002; 3: 439–445. [PubMed] [Google Scholar]
- 4. Montano N, Ruscone TG, Porta A, et al. Power spectrum analysis of heart rate variability to assess the changes in sympathovagal balance during graded orthostatic tilt. Circulation 1994; 90: 1826–1831. [DOI] [PubMed] [Google Scholar]
- 5. Stauss HM. Identification of blood pressure control mechanisms by power spectral analysis. Clin Exp Pharmacol Physiol 2007; 34: 362–368. [DOI] [PubMed] [Google Scholar]
- 6. Gironacci MM, Cerniello FM, Longo Carbajosa NA, et al. Protective axis of the renin–angiotensin system in the brain. Clin Sci 2014; 127: 295–306. [DOI] [PubMed] [Google Scholar]
- 7. Sampaio WO, Souza dos Santos RA, Faria-Silva R, et al. Angiotensin-(1–7) through receptor Mas mediates endothelial nitric oxide synthase activation via Akt-dependent pathways. Hypertension 2007; 49: 185–192. [DOI] [PubMed] [Google Scholar]
- 8. Santos RA. Angiotensin-(1–7). Hypertension 2014; 63: 1138–1147. [DOI] [PubMed] [Google Scholar]
- 9. Santos RA, Brosnihan KB, Jacobsen DW, et al. Production of angiotensin-(1–7) by human vascular endothelium. Hypertension 1992; 19: II56–61. [DOI] [PubMed] [Google Scholar]
- 10. Xu P, Costa-Goncalves AC, Todiras M, et al. Endothelial dysfunction and elevated blood pressure in MAS gene-deleted mice. Hypertension 2008; 5: 574–580. [DOI] [PubMed] [Google Scholar]
- 11. Becker LK, Etelvino GM, Walther T, et al. Immunofluorescence localization of the receptor Mas in cardiovascular-related areas of the rat brain. Am J Physiol Heart Circ Physiol 2007; 293: H1416–1424. [DOI] [PubMed] [Google Scholar]
- 12. Xu P, Sriramula S, Lazartigues E. ACE2/ANG-(1–7)/Mas pathway in the brain: the axis of good. Am J Physiol Regul Integr Comp Physiol 2011; 300: R804–817. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. Rabelo E, De Angelis K, Bock P, et al. Baroreflex sensitivity and oxidative stress in adriamycin-induced heart failure. Hypertension 2001; 38: 576–580. [DOI] [PubMed] [Google Scholar]
- 14. Porta A, Montano N, Furlan R, et al. Automatic classification of interference patterns in driven event series: application to single sympathetic neuron discharge forced by mechanical ventilation. Biol Cybern 2004; 91: 258–73. [DOI] [PubMed] [Google Scholar]
- 15. Dias da Silva VJ, Viana Publio CC, de Melo Alves R, et al. Intravenous amiodarone modifies autonomic balance and increases baroreflex sensitivity in conscious rats. Auton Neurosci 2002; 95: 88–96. [DOI] [PubMed] [Google Scholar]
- 16. Fazan R, de Oliveira M, da Silva VJ, et al. Frequency-dependent baroreflex modulation of blood pressure and heart rate variability in conscious mice. Am J Physiol Heart Circ Physiol 2005; 289: H1968–1975. [DOI] [PubMed] [Google Scholar]
- 17. Porta A, Castiglioni P, Di Rienzo M, et al. Short-term complexity indexes of heart period and systolic arterial pressure variabilities provide complementary information. J Appl Physiol 2012; 113: 1810–1820 [DOI] [PubMed] [Google Scholar]
- 18. Walther T, Wessel N, Kang N, et al. Altered heart rate and blood pressure variability in mice lacking the Mas protooncogene. Braz J Med Biol Res 2000; 33: 1–9. [DOI] [PubMed] [Google Scholar]
- 19. Chaves GZ, Caligiorne SM, Santos RA, et al. Modulation of the baroreflex control of heart rate by angiotensin-(1–7) at the nucleus tractus solitarii of normotensive and spontaneously hypertensive rats. J Hypertens 2000; 18: 1841–1848. [DOI] [PubMed] [Google Scholar]
- 20. Nautiyal M, Shaltout HA, de Lima DC, et al. Central angiotensin-(1–7) improves vagal function independent of blood pressure in hypertensive (mRen2)27 rats. Hypertension 2012; 60: 1257–1265. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Britto RR, Santos RA, Fagundes-Moura CR, et al. Role of angiotensin-(1–7) in the modulation of the baroreflex in renovascular hypertensive rats. Hypertension 1997; 30: 549–556. [DOI] [PubMed] [Google Scholar]
- 22. Moura MM, dos Santos RA, Campagnole-Santos MJ, et al. Altered cardiovascular reflexes responses in conscious Angiotensin-(1–7) receptor Mas-knockout mice. Peptides 2010; 31: 1934–1939. [DOI] [PubMed] [Google Scholar]
- 23. Ferreira AJ, Santos RA. Cardiovascular actions of angiotensin-(1–7). Braz J Med Biol Res 2005; 38: 499–507. [DOI] [PubMed] [Google Scholar]
- 24. Stegbauer J, Oberhauser V, Vonend O, et al. Angiotensin-(1–7) modulates vascular resistance and sympathetic neurotransmission in kidneys of spontaneously hypertensive rats. Cardiovasc Res 2004; 61: 352–359. [DOI] [PubMed] [Google Scholar]
- 25. Martins Lima A, Xavier CH, Ferreira AJ, et al. Activation of angiotensin-converting enzyme 2/angiotensin-(1–7)/Mas axis attenuates the cardiac reactivity to acute emotional stress. Am J Physiol Heart Circ Physiol 2013; 305: H1057–1067. [DOI] [PubMed] [Google Scholar]
- 26. Oscar CG, Muller-Ribeiro FC, de Castro LG, et al. Angiotensin-(1–7) in the basolateral amygdala attenuates the cardiovascular response evoked by acute emotional stress. Brain Res 2015; 1594: 183–189. [DOI] [PubMed] [Google Scholar]
- 27. Alenina N, Xu P, Rentzsch B, et al. Genetically altered animal models for Mas and angiotensin-(1–7). Exp Physiol 2008; 93: 528–537. [DOI] [PubMed] [Google Scholar]