Abstract
Background
The mechanisms underlying the non-antimicrobial immunomodulatory properties of macrolides are not well understood.
Objectives
To systematically review the evidence for the immunomodulatory properties of macrolides in humans and to describe the underlying mechanism and extent of their influence on the innate and adaptive immune system.
Methods
A systematic literature search was done in MEDLINE using the OVID interface from 1946 to December 2016 according to the preferred reporting items for systematic reviews and meta-analysis (PRISMA). Original articles investigating the influence of four macrolides (azithromycin, clarithromycin, erythromycin, and roxithromycin) on immunological markers in humans were included.
Results
We identified 22 randomized, controlled trials, 16 prospective cohort studies, and 8 case–control studies investigating 47 different immunological markers (186 measurements) in 1,834 participants. The most frequently reported outcomes were a decrease in the number of neutrophils, and the concentrations of neutrophil elastase, interleukin (IL)-8, IL-6, IL-1beta, tumor necrosis factor (TNF)-alpha, eosinophilic cationic protein, and matrix metalloproteinase 9. Inhibition of neutrophil function was reported more frequently than eosinophil function. A decrease in T helper (Th) 2 cells cytokines (IL-4, IL-5, IL-6) was reported more frequently than a decrease in Th1 cytokines (IL-2, INF-gamma).
Conclusion
Macrolides influence a broad range of immunological mechanisms resulting in immunomodulatory effects. To optimize the treatment of chronic inflammatory diseases by macrolides, further studies are necessary, particularly comparing different macrolides and dose effect relationships.
Keywords: azalides, azithromycin, clarithromycin, erythromycin, immunolides, roxithromycin
Background
Macrolides are mainly used as antibiotics to treat respiratory, skin and soft tissue, and urogenital infections (1, 2). They derive from Streptomyces species and are characterized by a macrocyclic lactone ring, which is either 14- [erythromycin (ERM), clarithromycin (CAM) and roxithromycin (RXM)], 15- [azithromycin (AZM)], or 16-membered (spiramycin, josamycin, midecamycin) (3). The antimicrobial activity of macrolides results from inhibition of bacterial protein synthesis through reversible binding to the peptide exit tunnel of ribosomes (4).
In addition to their antibiotic activity, macrolides have immunomodulatory properties, which were first described soon after their introduction in the 1950s (3, 5–7). The concept of using macrolides primarily for their immunomodulatory activities was introduced in the 1970s (8). The seminal study that distinguished between macrolides’ antimicrobial and their immunomodulatory effects was in adults with diffuse panbronchiolitis (DPB) in whom treatment with ERM dramatically improved survival independent of bacterial colonization (9). These results encouraged further research on the use of macrolides for the treatment of other chronic inflammatory conditions (10–14).
The mechanisms underlying the non-antimicrobial effects of macrolides are less well understood. Aside from ribosomal-mediated inhibition of pathogen virulence factor production, a number of other mechanisms have been proposed, including action on host immunity.
The objective of this review was to systematically summarize studies which investigated immunomodulatory properties of macrolides in humans and to describe the underlying mechanism and extent of their influence on the innate and adaptive immune system.
Methods
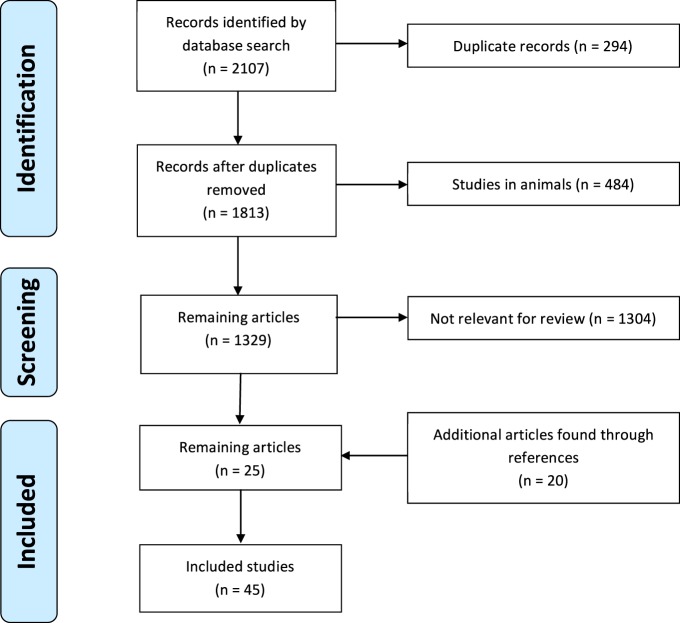
This review was done according to the preferred reporting items for systematic reviews and meta-analyses (PRISMA) (15). A literature review was done in December 2016 searching MEDLINE using the OVID interface from 1946 to 2016 using the search terms: (macrolide OR azithromycin OR clarithromycin OR erythromycin OR roxithromycin) AND (anti-inflammatory OR immunomodulatory OR immunolides) without any language limitations or limitation of study design (Figure 1). Only studies in humans, in which the participants received one of the four mentioned macrolides and which investigated immunological markers involved in inflammation were included. Studies reporting clinical endpoints only or studies in which macrolides were investigated for their antimicrobial activity were excluded. References were hand-searched for additional publications. Search results were independently screened by one reviewer, and checked by a second reviewer. Potentially eligible full-text articles were assessed according to our inclusion and exclusion criteria. The following variables were extracted from the included studies: year of study, country, study design, number of participants, age of participants, underlying disease, type, dose and duration of macrolide use, type of samples collected, and measured immune markers. Changes were classified as being significant when the p-value was ≤0.05.
Figure 1.
Selection of articles included in the review.
Review
Characteristics of Included Studies
We identified 2,107 studies, of which 45 were included in the final analysis; 22 randomized, controlled trials, 16 prospective cohort studies, and 7 case–control studies (Figure 1). Studies originated from 17 countries (Japan n = 12, United States of America n = 6, China n = 4, Australia n = 4, United Kingdom n = 4, Turkey n = 2, Serbia n = 2, Croatia n = 2, and one each from Belgium, Canada, Greece, the Netherlands, Italy, South Korea, Russia, Sweden, and Switzerland) and included a total of 1,834 participants. Six studies, including 423 participants, were done in children and adolescents (<18 years of age). Details of all studies including a risk of bias analysis are summarise in Table 1 and Table 2.
Table 1.
Macrolide-induced changes in immunological markers in 45 studies in humans categorized by disease (NS = not stated).
| Drug | Dose | Duration (weeks) | Patients (healthy) (n) | Age (years) (mean) | Sample | Measured immune markers | Study design | Reference | |
|---|---|---|---|---|---|---|---|---|---|
| Blepharitis | AZM | 1% topical drops | 4 | 24 (8) | 34–80 (54) | Conjunctival cells | Decrease in IL-1beta, IL-8, matrix metalloproteinase 9 (MMP-9) | CCS | Zhang et al. (16) |
| Eyelid margins | Increase in TGF-beta | ||||||||
| Periodontitis | RXM | 300 mg daily | 0.7 | 47 (16) | 28–65 (46) | Gingival cervicular fluid | Decrease in IL-1beta, TGF-beta, VEGF | RCT | Gong et al. (18) |
| Placebo | |||||||||
| Nasal polyps | CAM | 500 mg daily | 8 | 40 | 25–73 (44) | Nasal secretions | Decrease in CCL-5 in allergic and non-allergic patients | PCS | Peric et al. (19) |
| Decrease in IL-6 in allergic patients | |||||||||
| Decrease in ECP in non-allergic patients | |||||||||
| CAM | 500 mg daily | 8 | 40 | 25–73 (44) | Nasal secretions | Decrease in IL-8 in allergic and non-allergic patients | PCS | Peric et al. (20) | |
| Decrease in IL-1beta, IL-6 in allergic patients | |||||||||
| Decrease in TNF-alpha in non-allergic patients | |||||||||
| CAM | 400 mg daily | 12 | 20 | 28–84 (57) | Nasal secretions | Decrease in IL-8 | PCS | Yamada et al. (21) | |
| Rhinosinusitis | CAM | 500 mg BID | 2 | 25 | 19–70 (45) | Nasal mucosa cells | Decrease in macrophage count, eosinophil activity, neutrophil elastase, IL-6, IL-8, and TNF-alpha | PCS | MacLeod et al. (22) |
| CAM | 250 mg daily | 12 | 30 | 25–63 (46) | Nasal secretions | Decrease in IL-8, ECP | PCS | Cervin et al. (23) | |
| Decrease in MPO, alpha2-macroglobulin (not significant) | |||||||||
| CAM | 250 mg daily | 12 | 10 | 27–62 (48)* | Nasal mucosa cells | Decrease in TGF-beta, NF-kappaB (not significant) | PCS | Wallwork et al. (24) | |
| CAM | 250 mg daily | 52 | 17 | 18–67 (51) | Nasal mucosa cells | Increase in nasal nitric oxide (not significant) | PCS | Cervin et al. (59) | |
| ERM | 250 mg BID | ||||||||
| RXM | 150 mg daily | 1–46 | 12 | 16–73 (54) | Nasal secretions | Decrease in neutrophil count, IL-8 | PCS | Suzuki et al. (25) | |
| RXM | 150 mg daily | 12 | 64 | >18 | Nasal secretions | Decrease in IL-8 | RCT | Wallwork et al. (26) | |
| Placebo | Nasal mucosa cells | ||||||||
| Asthma Bronchiale |
AZM | 250 mg daily | 12 | 71 | 18–70 (43) | Sputum | No change in eosinophil count, neutrophil count | RCT | Cameron et al. (27) |
| Placebo | |||||||||
| AZM | NS | 12 | 40 | 22–52 (35) | Sputum | Decrease in IL-4, IL-5, IFN-gamma | RCT | He et al. (28) | |
| Placebo | |||||||||
| AZM | 10 mg/kg daily, 3 times a week | 8 | 16 | NS (13) | BAL | Decrease in neutrophil count | RCT | Piacentini et al. (29) | |
| Placebo | |||||||||
| CAM | 15 mg/kg BID (max 500 mg) | 0.7 | 43 | 4–17 (9) | Nasopharyngeal secretions | Decrease in TNF-alpha, IL-1, IL-10 | RCT | Fonseca-Aten et al. (30) | |
| Placebo | |||||||||
| CAM | 200 mg BID | 8 | 17 | 26–49 (38) | Sputum | Decrease in eosinophil count, ECP | RCT | Amayasu et al. (31) | |
| Placebo | Blood | Decrease in eosinophil count, ECP | |||||||
| CAM | 500 mg BID | 6 | 86 | NS (33) | BAL | Decrease in TNF-alpha, IL-5, IL-12 | RCT | Kraft et al. (32) | |
| Placebo | Airway tissue | Decrease in TNF-alpha, IL-5, IL-12 | |||||||
| CAM | 500 mg BID | 8 | 45 | 27–80 (58) | Sputum | Decrease in neutrophil count, neutrophil elastase, IL-8 | RCT | Simpson et al. (33) | |
| Placebo | Decrease in MMP-9 (not significant) | ||||||||
| CAM | 500 mg BID | 8 | 45 | 27–80 (60) | Sputum | Decrease in neutrophil count, neutrophil elastase, MMP-9, IL-8 | RCT | Wang et al. (34) | |
| Placebo | |||||||||
| RXM | 150 mg BID | 8 | 14 | 29–50 (40) | Sputum | Decrease in eosinophil count, ECP | RCT | Shoji et al. (35) | |
| Placebo | Blood | Decrease in eosinophil count, ECP | |||||||
| RXM | 150 mg daily | 12 | 20 (10) | NS (41) | PMNL | Decrease in neutrophil oxidative burst | PCS | Kamoi et al. (36) | |
| Bronchiectasis | CAM | 500 mg daily | 12 | 22 | 32–78 (58) | Blood | Decrease in Th17-cells, IL-17 | PCS | Fouka et al. (37) |
| CAM | 15 mg/kg daily | 12 | 34 | 7–18 (13) | BAL | Decrease in total cell count, neutrophil count, IL-8 | RCT | Yalcin et al. (38) | |
| Supportive treatment | Increase in macrophage count | ||||||||
| RXM | 150 mg daily | 26 | 52 | 18–65 (48) | Sputum | Decrease in neutrophil count, neutrophil elastase, IL-8, MMP-9 | RCT | Liu et al. (39) | |
| No treatment | |||||||||
| Chronic obstructive pulmonary disease | AZM Placebo |
500 mg daily | 0.4 | 24 | 35–70 (62) | Blood | Increase in neutrophil oxidative burst | RCT | Parnham et al. (40) |
| Decrease in leukocyte count, thrombocyte count, IL-8, E-selectin, CRP, lactoferrin, serum amyloid A | |||||||||
| No change in TNF-alpha, IL-6, GM-CSF | |||||||||
| Sputum | No change in neutrophil count, eosinophil count | ||||||||
| CAM | 500 mg daily | 12 | 67 | NS (65) | Sputum | Decrease in neutrophil chemotaxis (not significant) | RCT | Banerjee et al. (41) | |
| Placebo | No change in total cell count, neutrophil count, IL-8, leukotriene B 4, TNF-alpha, neutrophil elastase | ||||||||
| ERM Placebo |
125 mg TDS | 24 | 36 | ≥40 (69) | Sputum | Decrease in total cell count, neutrophil count, neutrophil elastase | RCT | He et al. (42) | |
| Diffuse panbronchiolitis | ERM | 250 mg BID | ≥24 | 14 | NS (46) | BAL | Decrease in lymphocyte count, IL-2, IFN-gamma Increase in CD4/CD8 ratio, IL-4, IL-5, IL-13 |
PCS | Park et al. (43) |
| ERM | 200 mg TDS | 24–52 | 18 (5) | 14–63 (39) | BAL | Decrease in total cell count, neutrophil count, neutrophil chemotaxis | CCS | Oda et al. (44) | |
| ERM | NS TDS | 24–52 | 19 | NS (42) | BAL | Decrease in total cell count, neutrophil count, neutrophil chemotaxis | CCS | Kadota et al. (45) | |
| ERM | 200 mg TDS | 8–68 | 22 (5) | 18–70 (45) | BAL | Decrease in neutrophil count, neutrophil chemotaxis, IL-8 | CCS | Katsuki et al. (46) | |
| No change in TNF-alpha | |||||||||
| ERM | 600 mg daily | 12 | 12 | 16–75 (47) | BAL | Decrease in neutrophil count, neutrophil elastase | CCS | Ichikawa et al. (47) | |
| Amoxicillin | |||||||||
| ERM | 600 mg daily | 4–104 | 43 (7) | (47) | BAL | Decrease in neutrophil count, IL-1beta, IL-8 | CCS | Sakito et al. (48) | |
| RXM | 150 mg daily | ||||||||
| ERM | 400 mg daily | 12 | 12 (6) | NS | Blood | Decrease in neutrophil oxidative burst | CCS | Umeki (49) | |
| Cystic fibrosis | AZM | NS | 4 | 260 | 6–18 (NS) | Blood | Decrease in neutrophil count, MPO, high-sensitivity C reactive protein, serum amyloid A, calprotection | RCT | Ratjen et al. (50) |
| AZM | 250 mg daily (≤ 40 kg) | 24 | 41 | 8–18 (NS) | Sputum | Decrease in IL-8, neutrophil elastase (not significant) (data only available from 17 patients) | RCT | Equi et al. (51) | |
| 500 mg daily (> 40 kg) | |||||||||
| CAM | 7.5 mg/kg BID | 12 | 18 | 3–15 (9) | BAL | Decrease in neutrophil count, neutrophil elastase (not significant) | RCT | Doğru et al. (52) | |
| Increase in macrophage count (not significant) | |||||||||
| CAM | 250 mg daily | 52 | 27 | 6–17 (12) | Sputum | Decrease in IL-4, IL-8, TNF-alphaDecrease in INF-gamma (not significant) | PCS | Pukhalsky et al. (53) | |
| Blood | Decrease in IL-4, IL-8, TNF-alpha | ||||||||
| Lung transplantation | AZM | NS | 12–24 | 30 | 36–61 (56) | BAL | Decrease in neutrophil count, IL-8, MMP-9 | PCS | Verleden et al. (54) |
| Diabetic nephropathy | CAM | 200 mg daily | 12 | 16 | NS (67) | Urine | Decrease CCL-2 | RCT | Tone (60) |
| Placebo | Blood | ||||||||
| Coronary atherosclerosis | CAM | 500 mg daily | 8 | 231 | NS (65) | Blood | Decrease in CRP, IL-2, IL-6, IL-8, TNF-alpha (not significant) | RCT | Berg et al. (55) |
| Placebo | |||||||||
| Healthy volunteers | AZM | 500 mg daily | 0.4 | 12 | 24–45 (29) | Blood | Increase in neutrophil oxidative burst, apoptosis of neutrophils | PCS | Culić et al. (56) |
| Increase in TNF-alpha (not significant) | |||||||||
| Decrease in IL-1beta, IL-6, IL-8, myeloperoxidase, IL-17, soluble vascular cell adhesion molecule-1 | |||||||||
| Decrease in E-selectin, lactoferrin (not significant) | |||||||||
| No change in leukocyte count, thrombocyte count, neutrophil elastase, beta2-microglobulin, INF-gamma, GM-CSF | |||||||||
| AZM | 500 mg on day 1, then 250 mg | 0.7 | 12 | 23–47 (30) | Sputum | No change in total cell count, neutrophil count, IL-6, IL-8 after ozone exposure during exercise | RCT | Criqui et al. (57) | |
| Placebo | |||||||||
| AZM | 500 mg daily | 0.4 | 19 | 18–40 (25) | BAL | No change in TNF-alpha, IL-1beta, IL-6, superoxide generation by alveolar macrophages | PCS | Aubert et al. (58) | |
| Blood | |||||||||
| AZM | 500 mg daily first day, then 250 mg daily | 0.4 | 10 | NS (30) | Gingival cervicular fluid | Decrease in IL-1beta, IL-8, TNF-alpha, VEGF | PCS | Ho et al. (17) | |
Table 2.
Risk of bias summary of the randomized controlled trials and case–control studies included in the review (NS = not stated).
| Reference | Publication year | Selectionbias | Performancebias | Detectionbias | Attritionbias | Reportingbias |
|---|---|---|---|---|---|---|
| Randomized controlled trials | ||||||
| Periodontitis | ||||||
| Gong et al. (18) | 2013 | − | − | − | − | − |
| Rhinosinusitis | ||||||
| Wallwork et al. (26) | 2006 | − | − | − | − | − |
| Asthma bronchiale | ||||||
| Cameron et al. (27) | 2013 | NS | − | − | + | + |
| He et al. (28) | 2009 | + | NS | NS | NS | + |
| Piacentini et al. (29) | 2007 | − | − | − | + | + |
| Fonseca-Aten et al. (30) | 2006 | + | − | − | − | + |
| Amayasu et al. (31) | 2000 | + | − | − | − | − |
| Kraft et al. (32) | 2002 | + | − | − | − | + |
| Simpson et al. (33) | 2008 | − | − | − | − | + |
| Wang et al. (34) | 2012 | + | NS | NS | NS | − |
| Shoji et al. (35) | 1999 | + | − | − | − | + |
| Bronchiectasis | ||||||
| Yalcin et al. (38) | 2006 | + | NS | NS | − | + |
| Liu et al. (39) | 2014 | + | + | + | − | + |
| Chronic obstructive pulmonary disease | ||||||
| Parnham et al. (40) | 2005 | + | − | − | − | − |
| Banerjee et al. (41) | 2004 | + | − | − | − | − |
| He et al. (42) | 2010 | + | − | − | − | − |
| Cystic fibrosis | ||||||
| Ratjen et al. (50) | 2012 | − | − | − | − | − |
| Equi et al. (51) | 2002 | + | − | − | − | + |
| Doğru et al. (52) | 2009 | + | − | − | − | − |
| Diabetic nephropathy | ||||||
| Tone et al. (60) | 2011 | + | + | + | − | − |
| Coronary atherosclerosis | ||||||
| Berg et al. (55) | 2003 | + | − | − | − | − |
| Healthy volunteers | ||||||
| Criqui et al. (57) | 2000 | + | − | − | − | − |
| Case–control studies | ||||||
| Blepharitis | ||||||
| Zhang et al. (16) | 2015 | + | + | + | − | − |
| Diffuse panbronchiolitis | ||||||
| Oda et al. (44) | 1994 | + | + | + | − | − |
| Kadota et al. (45) | 1993 | + | + | + | − | − |
| Katsuki et al. (46) | 1996 | + | + | + | − | − |
| Ichikawa et al. (47) | 1992 | + | + | + | + | − |
| Sakito et al. (48) | 1996 | + | + | + | − | − |
| Umeki (49) | 1993 | − | + | + | − | − |
Immunological Markers Analyzed
A total of 47 different immunological markers were investigated. On average, four markers were investigated per study resulting in a total of 186 measurements (Table 3; Figure 2). The immunological markers were classified into groups: cell counts (n = 9 markers/41 total measurements), neutrophil function (n = 6/25), eosinophil function (n = 2/7), macrophage function (n = 1/1), cytokine concentrations (n = 16/81), inflammatory proteins (n = 6/8), cell adhesion molecules (n = 2/3), molecules involved in inflammatory signaling pathway (n = 1/1), and other markers (n = 5/5, alpha-2-macroglobulin, beta-2-microglobulin, high-sensitivity C reactive protein, calprotectin, nasal nitric oxide).
Table 3.
Macrolide-induced changes in immunological markers based on 43 studies in humans.
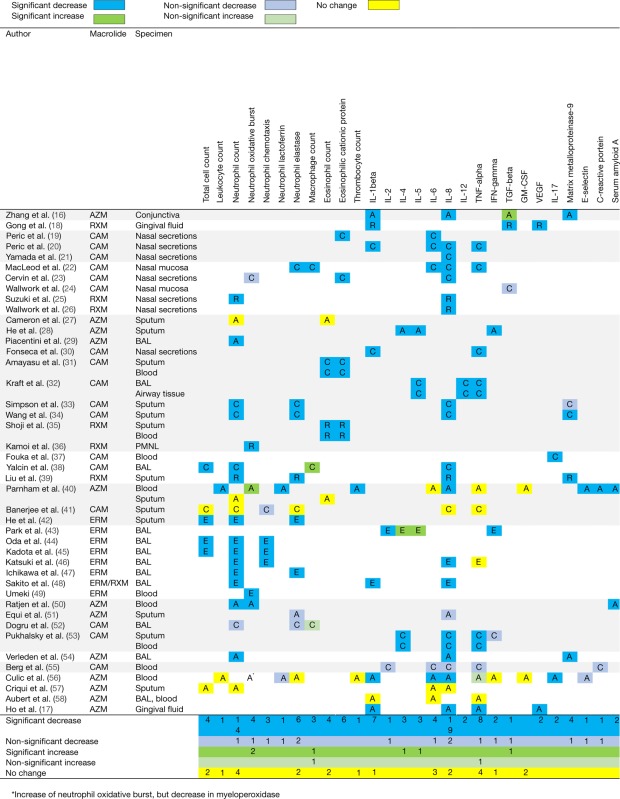 |
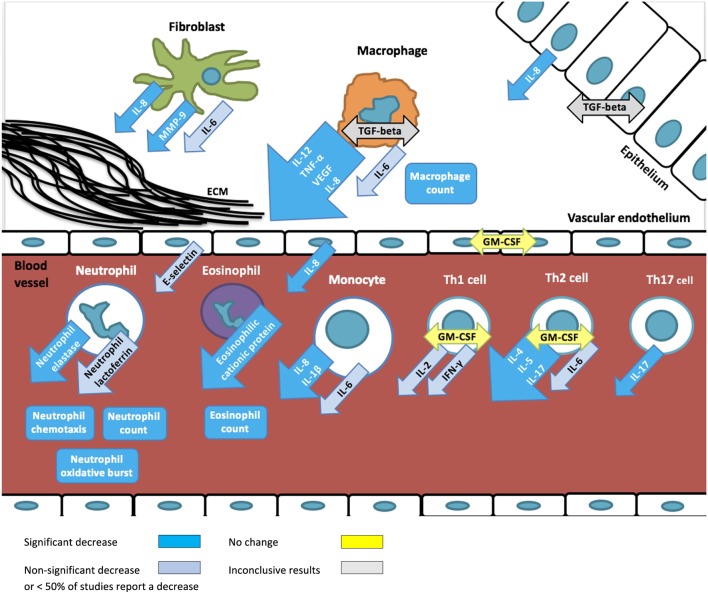
Figure 2.
Overview of immunomodulatory effects of macrolides based on studies summarized in Table 1. Arrows depict excreted proteins, boxes depict cell counts or functions.
Overall, a decrease in immunological markers, number, or function was more frequently observed than an increase (139 measurements vs 19). No change of immunological markers reported in 11 immunological markers (28 measurements) in 7 studies. The most frequently reported macrolide-induced changes were a decrease in interleukin (IL)-8 concentration (n = 21), neutrophil count (n = 15), tumor necrosis factor-alpha (TNF-alpha) (n = 9), neutrophil elastase (n = 8), IL-1beta (n = 7), eosinophilic cationic protein (ECP, n = 6), IL-6 (n = 5), matrix metalloproteinase 9 (MMP-9) (n = 5), and oxidative burst activity (n = 5).
Immunomodulatory effects were investigated for four types of macrolides, including CAM (n = 73), AZM (n = 69), ERM (n = 27), and RXM (n = 17). AZM was more frequently associated with no influence on the immunological markers investigated (21/69) compared to any of the other macrolides (Table 4).
Table 4.
Number of measurements and changes in immunological markers for each macrolide.
| Decrease/non-significant decrease | Increase/non-significant increase | No change | Total | |
|---|---|---|---|---|
| AZM | 33/4 | 10/1 | 21 | 69 |
| CAM | 52/12 | 1/2 | 6 | 73 |
| ERM | 21/0 | 4/1 | 1 | 27 |
| RXM | 17/0 | 0/0 | 0 | 17 |
| Total | 123/16 | 15/4 | 28 | 186 |
Immunomodulatory Properties in Different Diseases
In the following, the immunomodulatory properties of macrolides are summarized and categorized by the disease in which they were investigated (Table 1).
Blepharitis
Blepharitis is a common chronic inflammation of the eye lid leading to dry, itchy, and erythematous eyes. Anterior blepharitis is often associated with bacterial infections, while posterior blepharitis is linked to dysfunction of Meibomian glands. Many studies report clinical improvement in patients with blepharitis treated with topical AZM, due to a decrease in secretions and plugging of the Meibomian glands but did not investigate the underlying immunological mechanisms. The one study which did investigate immunological markes shows that concentrations of IL-1beta, IL-8, and MMP-9 in conjunctival cells of patients with blepharitis are higher than in healthy controls (16). Concentrations of these cytokines decrease with local AZM treatment, but return to pre-treatment levels after discontinuation (16).
Periodontitis
Periodontitis is an inflammatory process of the gums with a complex pathogenesis including microorganisms as well as neutrophils, macrophages and fibroblasts. One key immunological mechanism underlying the pathogensis of periodontitis has been described as a TNF-alpha-induced increase in vascular endothelial growth factor (VEGF) leading to an aberrant angiogenesis (61). Both AZM and RXM decreased TNF-alpha and VEGF concentrations as well as other cytokines including IL-1beta, IL-8, and transforming growth factor beta (TGF-beta) in gingival crevicular fluid (17, 18). Since oral bacteria play an important role in periodontitis, however, some of the some of the benefits of macrolides may be attributable to antimicrobial rather than to immunomodulatory effects.
Chronic Rhinosinusitis and Nasal Polyposis
Chronic rhinosinusitis (CRS) with nasal polyps is characterized by a T helper (Th) 2 cells-dominated inflammation with upregulation of IL-4, IL-5, and IL-13 and an increase in eosinophil count, ECP, and immunoglobulin E. CRS without nasal polyps is characterized by Th1-dominated inflammation with upregulation of IL-2, TGF-beta, and IFN-gamma. Studies in patients with CRS treated with CAM and RXM show a significant reduction in macrophage, neutrophil, and eosinophil counts and concentrations of neutrophil elastase, ECP, CC-chemokine ligand-5 (CCL-5), IL-1beta, IL-6, IL-8, interferon (IFN)-gamma, TNF-alpha, myeloperoxidase (MPO), and alpha-macroglobulin in nasal secretions (19–23, 25, 26, 62). One of the postulated mechanisms by which macrolides inhibit the development of nasal polyps is through their anti-oxidative effects inhibiting the TGF-beta-induced production of reactive oxygen species (24). However, the immunomodulatory mechanisms differ in allergic and non-allergic nasal polyposis patients. While CAM reduces IL-6 and CCL-5 in all patients, it reduces IL-1beta and IL-6 only in patients with allergic CRS and TNF-alpha and ECP only in patients with non-allergic CRS (19, 20).
Asthma
Asthma is characterized by chronic airway inflammation, reversible airway obstruction, and airway hyper-responsiveness. In eosinophilic asthma, eosinophils, mast cells, and Th2-mediated inflammation play an important role. Concentrations of IL-4, IL-5, IL-6, IL-9, IL-10, IL-13, vascular cell adhesion molecule-1, CC chemokines, and granulocyte macrophage colony-stimulating factor (GM-CSF) are elevated. In severe asthma, in addition to eosinophils, increased neutrophils and IL-8 concentrations are found in airways. In patients with asthma, AZM, CAM, and RXM decrease eosinophil and neutrophil counts, inhibit neutrophil migration and oxidative burst activity in phagocytes, decrease concentrations of neutrophil elastase, ECP, IL-1, IL-4, IL-5, IL-8, IL-10, IL-12, MMP-9, TNF-alpha, and INF-gamma in nasopharyngeal secretions, sputum, or bronchoalveolar lavage (BAL) samples (27–30, 32–36). In addition, CAM and RXM also decrease the eosinophil counts and concentrations of ECP in blood and inhibit oxidative burst activity in phagocytes (31, 35, 36).
Bronchiectasis
Bronchiectasis is characterized by permanent enlargement of bronchi and cytokines play an important role in the pathogenesis. In BAL samples of patients with bronchiectasis, elevated concentrations of IL-1beta and IL-8, as well as Th17-cytokines (IL-17A and IL-23), are found. In this setting, CAM and RXM lead to a decrease in total cell and neutrophil counts, concentrations of neutrophil elastase, IL-8, and MMP-9 in sputum or BAL of patients with bronchiectasis (38, 39). Interestingly, in BAL samples, these drugs significantly increase macrophage counts (38). Furthermore, macrolides lead to a decrease in peripheral blood Th17 cells and IL-17 concentrations (37).
Chronic Obstructive Pulmonary Disease
Chronic obstructive pulmonary disease (COPD) is characterized by chronic inflammation of lung parenchyma and peripheral airways with an increase in alveolar macrophages, neutrophils, T cells (predominantly Th1-, and Th17- cells), and innate lymphoid cells. These cells, as well as structural cells, such as epithelial cells, endothelial cells, and fibroblasts, secrete a variety of pro-inflammatory cytokines. Although most patients with COPD have a predominantly neutrophilic inflammation, some also have elevated eosinophil counts in sputum. Oxidative stress plays a key role in COPD, and can result in activation of the pro-inflammatory transcription factor nuclear factor (NF)-kappaB. Moreover, COPD is associated with increased apoptosis and defective phagocytosis in the airways. In patients with COPD, IL-1beta, IL-4, IL-8, and TNF-alpha concentrations in blood are elevated, while IL-10 concentrations are lower compared to healthy adults. In patients with COPD, AZM leads to a decrease in white blood cell and platelet counts and concentrations of CRP, IL-8, E-selectin, and lactoferrin in blood (40). By contrast, macrolides increase neutrophil oxidative burst and neutrophil glutathione peroxidase activity in blood (40). In the sputum of COPD patients, CAM and ERM lead to a significant decrease in total cell and neutrophil count and inhibit neutrophil chemotaxis and decrease concentrations of neutrophil elastase (41, 42).
Diffuse Panbronchiolitis
Diffuse panbronchiolitis (DPB) is a chronic distal airway inflammation characterized by diffuse micronodular pulmonary lesions mostly consisting of neutrophils. Neutrophils and epithelial cells produce IL-8, which is an important chemotactic factor to attract more neutrophils. The neutrophil count in BAL samples of patients with DPB correlates to the concentrations of IL-1beta and IL-8 (48). ERM reduces IL-1beta concentrations in BAL samples of patients with DPB which leads to a subsequent reduction of IL-8 concentrations and a decrease in neutrophil count and neutrophil chemotactic activity (44–48, 63). Furthermore, ERM treatment also results in a decrease in lymphocyte count, IL-2, interferon-gamma, and to increase in CD4/CD8 ratio, IL-4, IL-5, IL-13 in BAL samples of patients with DPB (43).
Cystic Fibrosis
In patients with cystic fibrosis (CF), chronic airway inflammation results from cytokines secreted by epithelial and immune cells, which leads to neutrophil influx into airways. The release of neutrophil proteases, including neutrophil elastase, contributes to the development of bronchiectasis. Sustained inflammation is mainly due to an increase in the transcription of NF-kappaB activity, which leads to an increase in IL-8 production. These immunological mechanisms are influenced by AZM and CAM, which in CF-patients lead to a decrease in neutrophil count, concentrations of neutrophil elastase, IL-4, IL-8, TNF-alpha, and INF-gamma, and to an increase in numbers of macrophages in BAL samples or in sputum (51–53). In CF-patients macrolides also lead to a decrease in neutrophil count, concentrations of IL-4, IL-8, TNF-alpha, MPO, high-sensitivity C reactive protein, serum amyloid A, and calprotectin in blood (50, 53).
Discussion
Macrolides are important therapeutic options in the treatment of many chronic inflammatory diseases because of their immunomodulatory effects. To understand the mechanisms underlying these effects, we reviewed all human studies that analyzed the influence of macrolides on immunological markers. The non-antimicrobial effects of macrolides are extensive and range from changes in cell counts and function, up- and downregulation of cytokine production to expression of adhesion molecules.
The most frequently and consistently reported immunomodulatory effect of macrolides is a reduced neutrophilic inflammation. Reduced numbers of neutrophils and inhibition of neutrophilic function lead to lower concentrations of neutrophil elastase and IL-8, and ultimately to a decrease in tissue injury. Furthermore, macrolides also reduce IL-1beta concentrations, another key mediator of the inflammatory response that is most abundantly produced by monocytes and macrophages. Evidence from animal and in vitro studies show that the inhibition of the key pro-inflammatory cytokines IL-8 and IL-1beta results from macrolides’ ability to alter intracellular signaling, particularly through the inhibition of NF-kappaB activation and expression of activator protein-1 (64–66). Notably, this effect has been observed in the absence of an infectious agent.
On the basis of these observed in vitro immunological effects of macrolides, patients with diseases mediated by neutrophilic inflammation such as periodontitis, severe asthma, DPB, bronchiectasis, COPD, and CF should benefit from treatment with this class of antibiotics. Indeed, clinically beneficial effects have been shown in randomized controlled studies in patients with COPD and CF with improved symptom scores, respiratory function and decreased frequency of exacerbations (67–69). For DPB, bronchiectasis and asthma, however, there is an absence of randomized controlled studies showing clinical beneficial effects of macrolides (70–72).
Macrolides are more commonly and consistently reported to inhibit neutrophilic than eosinophilic function. This is consistent with clinical studies that show patients with eosinophil-driven chronic inflammatory diseases associated with increased IgE (such as CRS or atopic asthma) have significantly lower improvement rates with macrolide treatment than those with normal serum IgE (26, 62, 73). Although the effect of macrolides on eosinophils has been less commonly investigated, a few studies report decreased eosinophil counts, and concentration of ECP (a ribonuclease secreted by eosinophils responsible for local cytotoxic effect). This suggests that there may be a role for the use of macrolides in allergic chronic inflammatory diseases (43, 74, 75). The possible influence of macrolides on eosinophilic inflammation is further supported by the finding that Th2 cytokines, such as IL-4 and IL-5, are more frequently reduced than Th1 cytokines, such as IL-2 and INF-gamma (19, 20, 22, 32, 42, 43, 53, 55, 56). The stronger effect of macrolides on Th2 compared with Th1 responses is further supported by evidence from animal and in vitro studies (74, 75). However, some of the anti-inflammatory effects might also be explained through their antibiotic effect on (undiagnosed) pathogens which trigger and sustain inflammation.
It is likely that immunomodulatory effects vary between different macrolides. Although some studies included more than one macrolide, none of the human studies directly compared different macrolides. Interestingly, AZM was less frequently associated with changes in measured immunological markers compared to the other macrolides. However, most of these studies were either in healthy volunteers or AZM was administered for only a few days (56–58, 76). By contrast, clinical studies in patients with CF suggest that AZM, but not CAM, leads to an improvement in respiratory function and reduction in pulmonary exacerbations (69, 77). In vitro studies comparing the immunomodulatory effects of different macrolides suggest that CAM has less immunomodulatory activity compared to other macrolides. For example, RXM, but not CAM or ERM, was shown to decreased chemotaxis of Th1 and Th2 cells (78). Similarly, CAM had a significantly weaker effect on reducing IL-6 production by human macrophages than ERM (79). Furthermore, another study showed that AZM, but not CAM or RXM, inhibits IL-1alpha and IL-1beta production (80).
Immunomodulatory effects of macrolides have been described with the recommended dose for antimicrobial treatment. Macrolides have excellent tissue penetration compared to other classes of antibiotics resulting in tissue concentrations generally exceeding serum concentrations (except for RXM). For the immunomodulatory effects macrolides’ ability to accumulate in neutrophils and macrophages is particularly important. Concentrations in macrophages have been shown to be 400- to 800-fold higher compared to serum for CAM and AZM and 5- to 100-fold higher in tissue compared to serum for ERM, CAM and AZM (81–85). This drug accumulation in immune cells may result in immunomodulatory effects occurring at lower doses and lasting longer compared to the antimicrobial effects. The relationship between macrolide dose and immunomodulatory effect is, therefore, an interesting avenue for future research.
The main limitation of this review is the heterogeneity of study populations, underlying diseases, type of macrolide and methods used to assess the immunomodulatory effect. A further limitation is selection and reporting bias and based on study types other biases including carry-over effect in cross-over trials and recall bias in case–control studies.
In summary, there is substantial evidence that macrolides exhibit immunomodulatory effects through inhibition of neutrophilic inflammation and macrophage activation. However, there is considerable heterogeneity between studies and in the immunological markers measured. Further studies will help delineate the exact mechanisms underlying the immunomodulatory properties of macrolides and the relative activity of different macrolides. This will enable the optimal use of this class of antibiotics in the treatment of chronic inflammatory diseases.
Author Contributions
PZ and NC designed the study. PZ drafted the initial manuscript and approved the final manuscript as submitted. PZ, VZ, and NR did the risk of bias analysis. VZ, NC, and NR critically reviewed and revised the manuscript, and approved the final manuscript as submitted.
Conflict of Interest Statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Footnotes
Funding. PZ was supported by a Melbourne International Research Scholarship and a scholarship from the Ettore-Rossi-Foundation.
References
- 1.Piscitelli SC, Danziger LH, Rodvold KA. Clarithromycin and azithromycin: new macrolide antibiotics. Clin Pharm (1992) 11(2):137–52. [PubMed] [Google Scholar]
- 2.Retsema J, Girard A, Schelkly W, Manousos M, Anderson M, Bright G, et al. Spectrum and mode of action of azithromycin (CP-62,993), a new 15-membered-ring macrolide with improved potency against gram-negative organisms. Antimicrob Agents Chemother (1987) 31(12):1939–47. 10.1128/AAC.31.12.1939 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Zuckerman JM. Macrolides and ketolides: azithromycin, clarithromycin, telithromycin. Infect Dis Clin North Am (2004) 18(3):621–49. 10.1016/j.idc.2004.04.010 [DOI] [PubMed] [Google Scholar]
- 4.Tenson T, Lovmar M, Ehrenberg M. The mechanism of action of macrolides, lincosamides and streptogramin B reveals the nascent peptide exit path in the ribosome. J Mol Biol (2003) 330(5):1005–14. 10.1016/S0022-2836(03)00662-4 [DOI] [PubMed] [Google Scholar]
- 5.Poliak MS. [Content of monomycin in bile and its effectiveness in inflammatory diseases and surgery of the biliary tract]. Antibiotiki (1963) 8:83–7. [PubMed] [Google Scholar]
- 6.Parfenova EN, Ryviakova EV. [Use of erythromycin in non-specific inflammatory diseases of the Urogenital System]. Urol Mosc (1963) 28:29–31. [PubMed] [Google Scholar]
- 7.Gluzman IS. [Erythromycin ointment therapy of inflammatory diseases of eyelid, conjunctiva and cornea. (Clinico-Experimental Studies)]. Oftalmol Zh (1964) 19:450–4. [PubMed] [Google Scholar]
- 8.Plewig G, Schopf E. Anti-inflammatory effects of antimicrobial agents: an in vivo study. J Invest Dermatol (1975) 65(6):532–6. 10.1111/1523-1747.ep12610281 [DOI] [PubMed] [Google Scholar]
- 9.Kudoh S, Azuma A, Yamamoto M, Izumi T, Ando M. Improvement of survival in patients with diffuse panbronchiolitis treated with low-dose erythromycin. Am J Respir Crit Care Med (1998) 157(6 Pt 1):1829–32. 10.1164/ajrccm.157.6.9710075 [DOI] [PubMed] [Google Scholar]
- 10.Hahn DL, Grasmick M, Hetzel S, Yale S. AZMATICS (AZithroMycin-Asthma Trial In Community Settings) Study Group. Azithromycin for bronchial asthma in adults: an effectiveness trial. J Am Board Fam Med (2012) 25(4):442–59. 10.3122/jabfm.2012.04.110309 [DOI] [PubMed] [Google Scholar]
- 11.Koutsoubari I, Papaevangelou V, Konstantinou GN, Makrinioti H, Xepapadaki P, Kafetzis D, et al. Effect of clarithromycin on acute asthma exacerbations in children: an open randomized study. Pediatr Allergy Immunol (2012) 23(4):385–90. 10.1111/j.1399-3038.2012.01280.x [DOI] [PubMed] [Google Scholar]
- 12.Clement A, Tamalet A, Leroux E, Ravilly S, Fauroux B, Jais JP. Long term effects of azithromycin in patients with cystic fibrosis: a double blind, placebo controlled trial. Thorax (2006) 61(10):895–902. 10.1136/thx.2005.057950 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Wong C, Jayaram L, Karalus N, Eaton T, Tong C, Hockey H, et al. Azithromycin for prevention of exacerbations in non-cystic fibrosis bronchiectasis (EMBRACE): a randomised, double-blind, placebo-controlled trial. Lancet (2012) 380(9842):660–7. 10.1016/S0140-6736(12)60953-2 [DOI] [PubMed] [Google Scholar]
- 14.Sadreddini S, Noshad H, Molaeefard M, Moloudi R, Ardalan MR, Ghojazadeh M. A double blind, randomized, placebo controlled study to evaluate the efficacy of erythromycin in patients with knee effusion due to osteoarthritis. Int J Rheum Dis (2009) 12(1):44–51. 10.1111/j.1756-185X.2009.01379.x [DOI] [PubMed] [Google Scholar]
- 15.Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ (2009) 339:b2700. 10.1136/bmj.b2700 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Zhang L, Su Z, Zhang Z, Lin J, Li DQ, Pflugfelder SC. Effects of azithromycin on gene expression profiles of proinflammatory and anti-inflammatory mediators in the eyelid margin and conjunctiva of patients with meibomian gland disease. JAMA Ophthalmol (2015) 133(10):1117–23. 10.1001/jamaophthalmol.2015.2326 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Ho W, Eubank T, Leblebicioglu B, Marsh C, Walters J. Azithromycin decreases crevicular fluid volume and mediator content. J Dent Res (2010) 89(8):831–5. 10.1177/0022034510368650 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Gong Y, Lu J, Ding X, Yu Y. Effect of adjunctive roxithromycin therapy on interleukin-1beta, transforming growth factor-beta1 and vascular endothelial growth factor in gingival crevicular fluid of cyclosporine A-treated patients with gingival overgrowth. J Periodontal Res (2014) 49(4):448–57. 10.1111/jre.12123 [DOI] [PubMed] [Google Scholar]
- 19.Peric A, Vojvodic D, Matkovic-Jozin S. Effect of long-term, low-dose clarithromycin on T helper 2 cytokines, eosinophilic cationic protein and the ‘regulated on activation, normal T cell expressed and secreted’ chemokine in the nasal secretions of patients with nasal polyposis. J Laryngol Otol (2012) 126(5):495–502. 10.1017/S0022215112000485 [DOI] [PubMed] [Google Scholar]
- 20.Peric A, Vojvodic D, Baletic N, Peric A, Miljanovic O. Influence of allergy on the immunomodulatory and clinical effects of long-term low-dose macrolide treatment of nasal polyposis. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub (2010) 154(4):327–33. 10.5507/bp.2010.049 [DOI] [PubMed] [Google Scholar]
- 21.Yamada T, Fujieda S, Mori S, Yamamoto H, Saito H. Macrolide treatment decreased the size of nasal polyps and IL-8 levels in nasal lavage. Am J Rhinol (2000) 14(3):143–8. 10.2500/105065800782102717 [DOI] [PubMed] [Google Scholar]
- 22.MacLeod CM, Hamid QA, Cameron L, Tremblay C, Brisco W. Anti-inflammatory activity of clarithromycin in adults with chronically inflamed sinus mucosa. Adv Ther (2001) 18(2):75–82. 10.1007/BF02852391 [DOI] [PubMed] [Google Scholar]
- 23.Cervin A, Wallwork B, Mackay-Sim A, Coman WB, Greiff L. Effects of long-term clarithromycin treatment on lavage-fluid markers of inflammation in chronic rhinosinusitis. Clin Physiol Funct Imaging (2009) 29(2):136–42. 10.1111/j.1475-097X.2008.00848.x [DOI] [PubMed] [Google Scholar]
- 24.Wallwork B, Coman W, Mackay-Sim A, Cervin A. Effect of clarithromycin on nuclear factor-kappa B and transforming growth factor-beta in chronic rhinosinusitis. Laryngoscope (2004) 114(2):286–90. 10.1097/00005537-200402000-00019 [DOI] [PubMed] [Google Scholar]
- 25.Suzuki H, Shimomura A, Ikeda K, Oshima T, Takasaka T. Effects of long-term low-dose macrolide administration on neutrophil recruitment and IL-8 in the nasal discharge of chronic sinusitis patients. Tohoku J Exp Med (1997) 182(2):115–24. 10.1620/tjem.182.115 [DOI] [PubMed] [Google Scholar]
- 26.Wallwork B, Coman W, Mackay-Sim A, Greiff L, Cervin A. A double-blind, randomized, placebo-controlled trial of macrolide in the treatment of chronic rhinosinusitis. Laryngoscope (2006) 116(2):189–93. 10.1097/01.mlg.0000191560.53555.08 [DOI] [PubMed] [Google Scholar]
- 27.Cameron EJ, Chaudhuri R, Mair F, McSharry C, Greenlaw N, Weir CJ, et al. Randomised controlled trial of azithromycin in smokers with asthma. Eur Respir J (2013) 42(5):1412–5. 10.1183/09031936.00093913 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.He J, Zhu N, Chen X. Clinical impacts of azithromycin on lung function and cytokines for athmatic patients. JMS (2009) 36(6):719–22. [Google Scholar]
- 29.Piacentini GL, Peroni DG, Bodini A, Pigozzi R, Costella S, Loiacono A, et al. Azithromycin reduces bronchial hyperresponsiveness and neutrophilic airway inflammation in asthmatic children: a preliminary report. Allergy Asthma Proc (2007) 28(2):194–8. 10.2500/aap.2007.28.2958 [DOI] [PubMed] [Google Scholar]
- 30.Fonseca-Aten M, Okada PJ, Bowlware KL, Chavez-Bueno S, Mejias A, Rios AM, et al. Effect of clarithromycin on cytokines and chemokines in children with an acute exacerbation of recurrent wheezing: a double-blind, randomized, placebo-controlled trial. Ann Allergy Asthma Immunol (2006) 97(4):457–63. 10.1016/S1081-1206(10)60935-0 [DOI] [PubMed] [Google Scholar]
- 31.Amayasu H, Yoshida S, Ebana S, Yamamoto Y, Nishikawa T, Shoji T, et al. Clarithromycin suppresses bronchial hyperresponsiveness associated with eosinophilic inflammation in patients with asthma. Ann Allergy Asthma Immunol (2000) 84(6):594–8. 10.1016/S1081-1206(10)62409-X [DOI] [PubMed] [Google Scholar]
- 32.Kraft M, Cassell GH, Pak J, Martin RJ. Mycoplasma pneumoniae and Chlamydia pneumoniae in asthma: effect of clarithromycin. Chest (2002) 121(6):1782–8. 10.1378/chest.121.6.1782 [DOI] [PubMed] [Google Scholar]
- 33.Simpson JL, Powell H, Boyle MJ, Scott RJ, Gibson PG. Clarithromycin targets neutrophilic airway inflammation in refractory asthma. Am J Respir Crit Care Med (2008) 177(2):148–55. 10.1164/rccm.200707-1134OC [DOI] [PubMed] [Google Scholar]
- 34.Wang Y, Zhang S, Qu Y. Effect of clarithromycin on non-eosinophilic refractory asthma. J Clin Pulm Med (2012) 17(11):1948–51. [Google Scholar]
- 35.Shoji T, Yoshida S, Sakamoto H, Hasegawa H, Nakagawa H, Amayasu H. Anti-inflammatory effect of roxithromycin in patients with aspirin-intolerant asthma. Clin Exp Allergy (1999) 29(7):950–6. 10.1046/j.1365-2222.1999.00551.x [DOI] [PubMed] [Google Scholar]
- 36.Kamoi H, Kurihara N, Fujiwara H, Hirata K, Takeda T. The macrolide antibacterial roxithromycin reduces bronchial hyperresponsiveness and superoxide anion production by polymorphonuclear leukocytes in patients with asthma. J Asthma (1995) 32(3):191–7. 10.3109/02770909509089507 [DOI] [PubMed] [Google Scholar]
- 37.Fouka E, Lamprianidou E, Arvanitidis K, Filidou E, Kolios G, Miltiades P, et al. Low-dose clarithromycin therapy modulates Th17 response in non-cystic fibrosis bronchiectasis patients. Lung (2014) 192(6):849–55. 10.1007/s00408-014-9619-0 [DOI] [PubMed] [Google Scholar]
- 38.Yalçin E, Kiper N, Ozçelik U, Doğru D, Firat P, Sahin A, et al. Effects of claritromycin on inflammatory parameters and clinical conditions in children with bronchiectasis. J Clin Pharm Ther (2006) 31(1):49–55. 10.1111/j.1365-2710.2006.00708.x [DOI] [PubMed] [Google Scholar]
- 39.Liu J, Zhong X, He Z, Wei L, Zheng X, Zhang J, et al. Effect of low-dose, long-term roxithromycin on airway inflammation and remodeling of stable noncystic fibrosis bronchiectasis. Mediators Inflamm (2014) 2014:708608. 10.1155/2014/708608 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Parnham MJ, Culić O, Eraković V, Munić V, Popović-Grle S, Barisić K, et al. Modulation of neutrophil and inflammation markers in chronic obstructive pulmonary disease by short-term azithromycin treatment. Eur J Pharmacol (2005) 517(1–2):132–43. 10.1016/j.ejphar.2005.05.023 [DOI] [PubMed] [Google Scholar]
- 41.Banerjee D, Honeybourne D, Khair OA. The effect of oral clarithromycin on bronchial airway inflammation in moderate-to-severe stable COPD: a randomized controlled trial. Treat Respir Med (2004) 3(1):59–65. 10.2165/00151829-200403010-00007 [DOI] [PubMed] [Google Scholar]
- 42.He ZY, Ou LM, Zhang JQ, Bai J, Liu GN, Li MH, et al. Effect of 6 months of erythromycin treatment on inflammatory cells in induced sputum and exacerbations in chronic obstructive pulmonary disease. Respiration (2010) 80(6):445–52. 10.1159/000321374 [DOI] [PubMed] [Google Scholar]
- 43.Park SJ, Lee YC, Rhee YK, Lee HB. The effect of long-term treatment with erythromycin on Th1 and Th2 cytokines in diffuse panbronchiolitis. Biochem Biophys Res Commun (2004) 324(1):114–7. 10.1016/j.bbrc.2004.09.018 [DOI] [PubMed] [Google Scholar]
- 44.Oda H, Kadota J, Kohno S, Hara K. Erythromycin inhibits neutrophil chemotaxis in bronchoalveoli of diffuse panbronchiolitis. Chest (1994) 106(4):1116–23. 10.1378/chest.106.4.1116 [DOI] [PubMed] [Google Scholar]
- 45.Kadota J, Sakito O, Kohno S, Sawa H, Mukae H, Oda H, et al. A mechanism of erythromycin treatment in patients with diffuse panbronchiolitis. Am Rev Respir Dis (1993) 147(1):153–9. 10.1164/ajrccm/147.1.153 [DOI] [PubMed] [Google Scholar]
- 46.Katsuki M. Neutrophil chemotactic activity in bronchoalveolar lavage fluid recovered from patients with diffuse panbronchiolitis. Kurume Med J (1996) 43(4):279–87. 10.2739/kurumemedj.43.279 [DOI] [PubMed] [Google Scholar]
- 47.Ichikawa Y, Ninomiya H, Koga H, Tanaka M, Kinoshita M, Tokunaga N, et al. Erythromycin reduces neutrophils and neutrophil-derived elastolytic-like activity in the lower respiratory tract of bronchiolitis patients. Am Rev Respir Dis (1992) 146(1):196–203. 10.1164/ajrccm/146.1.196 [DOI] [PubMed] [Google Scholar]
- 48.Sakito O, Kadota J, Kohno S, Abe K, Shirai R, Hara K. Interleukin 1 beta, tumor necrosis factor alpha, and interleukin 8 in bronchoalveolar lavage fluid of patients with diffuse panbronchiolitis: a potential mechanism of macrolide therapy. Respiration (1996) 63(1):42–8. 10.1159/000196514 [DOI] [PubMed] [Google Scholar]
- 49.Umeki S. Anti-inflammatory action of erythromycin. Its inhibitory effect on neutrophil NADPH oxidase activity. Chest (1993) 104(4):1191–3. [DOI] [PubMed] [Google Scholar]
- 50.Ratjen F, Saiman L, Mayer-Hamblett N, Lands LC, Kloster M, Thompson V, et al. Effect of azithromycin on systemic markers of inflammation in patients with cystic fibrosis uninfected with Pseudomonas aeruginosa. Chest (2012) 142(5):1259–66. 10.1378/chest.12-0628 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Equi A, Balfour-Lynn IM, Bush A, Rosenthal M. Long term azithromycin in children with cystic fibrosis: a randomised, placebo-controlled crossover trial. Lancet (2002) 360(9338):978–84. 10.1016/S0140-6736(02)11081-6 [DOI] [PubMed] [Google Scholar]
- 52.Doğru D, Dalgiç F, Kiper N, Ozçelik U, Yalçin E, Aslan AT, et al. Long-term clarithromycin in cystic fibrosis: effects on inflammatory markers in BAL and clinical status. Turk J Pediatr (2009) 51(5):416–23. [PubMed] [Google Scholar]
- 53.Pukhalsky AL, Shmarina GV, Kapranov NI, Kokarovtseva SN, Pukhalskaya D, Kashirskaja NJ. Anti-inflammatory and immunomodulating effects of clarithromycin in patients with cystic fibrosis lung disease. Mediators Inflamm (2004) 13(2):111–7. 10.1080/09629350410001688495 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Verleden SE, Vandooren J, Vos R, Willems S, Dupont LJ, Verleden GM, et al. Azithromycin decreases MMP-9 expression in the airways of lung transplant recipients. Transpl Immunol (2011) 25(2–3):159–62. 10.1016/j.trim.2011.06.006 [DOI] [PubMed] [Google Scholar]
- 55.Berg HF, Maraha B, Scheffer GJ, Peeters MF, Kluytmans JA. Effect of clarithromycin on inflammatory markers in patients with atherosclerosis. Clin Diagn Lab Immunol (2003) 10(4):525–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Culić O, Eraković V, Cepelak I, Barisić K, Brajsa K, Ferencić Z, et al. Azithromycin modulates neutrophil function and circulating inflammatory mediators in healthy human subjects. Eur J Pharmacol (2002) 450(3):277–89. 10.1016/S0014-2999(02)02042-3 [DOI] [PubMed] [Google Scholar]
- 57.Criqui GI, Solomon C, Welch BS, Ferrando RE, Boushey HA, Balmes JR. Effects of azithromycin on ozone-induced airway neutrophilia and cytokine release. Eur Respir J (2000) 15(5):856–62. 10.1034/j.1399-3003.2000.15e08.x [DOI] [PubMed] [Google Scholar]
- 58.Aubert JD, Juillerat-Jeanneret L, Fioroni P, Dayer P, Plan PA, Leuenberger P. Function of human alveolar macrophages after a 3-day course of azithromycin in healthy volunteers. Pulm Pharmacol Ther (1998) 11(4):263–9. 10.1006/pupt.1998.0123 [DOI] [PubMed] [Google Scholar]
- 59.Cervin A, Kalm O, Sandkull P, Lindberg S. One-year low-dose erythromycin treatment of persistent chronic sinusitis after sinus surgery: clinical outcome and effects on mucociliary parameters and nasal nitric oxide. Otolaryngol Head Neck Surg (2002) 126(5):481–9. 10.1067/mhn.2002.124849 [DOI] [PubMed] [Google Scholar]
- 60.Tone A, Shikata K, Nakagawa K, Hashimoto M, Makino H. Renoprotective effects of clarithromycin via reduction of urinary MCP-1 levels in type 2 diabetic patients. Clin Exp Nephrol (2011) 15(1):79–85. 10.1007/s10157-010-0357-1 [DOI] [PubMed] [Google Scholar]
- 61.Booth V, Young S, Cruchley A, Taichman NS, Paleolog E. Vascular endothelial growth factor in human periodontal disease. J Periodontal Res (1998) 33(8):491–9. 10.1111/j.1600-0765.1998.tb02349.x [DOI] [PubMed] [Google Scholar]
- 62.Suzuki H, Ikeda K, Honma R, Gotoh S, Oshima T, Furukawa M, et al. Prognostic factors of chronic rhinosinusitis under long-term low-dose macrolide therapy. ORL J Otorhinolaryngol Relat Spec (2000) 62(3):121–7. 10.1159/000027731 [DOI] [PubMed] [Google Scholar]
- 63.Akiyoshi H, Honda J, Nakahara S, Tokisawa S, Tokunaga N, Ichikawa Y, et al. [Mechanism of efficacy of erythromycin on diffuse panbronchiolitis – effect of erythromycin on cytokine mRNA expression in human whole blood model]. Kansenshogaku Zasshi (1994) 68(2):209–16. 10.11150/kansenshogakuzasshi1970.68.209 [DOI] [PubMed] [Google Scholar]
- 64.Bosnar M, Čužić S, Bošnjak B, Nujić K, Ergović G, Marjanović N, et al. Azithromycin inhibits macrophage interleukin-1beta production through inhibition of activator protein-1 in lipopolysaccharide-induced murine pulmonary neutrophilia. Int Immunopharmacol (2011) 11(4):424–34. 10.1016/j.intimp.2010.12.010 [DOI] [PubMed] [Google Scholar]
- 65.Cheung PS, Si EC, Hosseini K. Anti-inflammatory activity of azithromycin as measured by its NF-kappaB, inhibitory activity. Ocul Immunol Inflamm (2010) 18(1):32–7. 10.3109/09273940903359725 [DOI] [PubMed] [Google Scholar]
- 66.Cigana C, Nicolis E, Pasetto M, Assael BM, Melotti P. Anti-inflammatory effects of azithromycin in cystic fibrosis airway epithelial cells. Biochem Biophys Res Commun (2006) 350(4):977–82. 10.1016/j.bbrc.2006.09.132 [DOI] [PubMed] [Google Scholar]
- 67.Yao GY, Ma YL, Zhang MQ, Gao ZC. Macrolide therapy decreases chronic obstructive pulmonary disease exacerbation: a meta-analysis. Respiration (2013) 86(3):254–60. 10.1159/000350828 [DOI] [PubMed] [Google Scholar]
- 68.Donath E, Chaudhry A, Hernandez-Aya LF, Lit L. A meta-analysis on the prophylactic use of macrolide antibiotics for the prevention of disease exacerbations in patients with Chronic Obstructive Pulmonary Disease. Respir Med (2013) 107(9):1385–92. 10.1016/j.rmed.2013.05.004 [DOI] [PubMed] [Google Scholar]
- 69.Southern KW, Barker PM, Solis-Moya A, Patel L. Macrolide antibiotics for cystic fibrosis. Cochrane Database Syst Rev (2012) 11:Cd002203. 10.1002/14651858.CD002203.pub4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Welsh EJ, Evans DJ, Fowler SJ, Spencer S. Interventions for bronchiectasis: an overview of Cochrane systematic reviews. Cochrane Database Syst Rev (2015) 7:Cd010337. 10.1002/14651858.CD010337.pub2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Kew KM, Undela K, Kotortsi I, Ferrara G. Macrolides for chronic asthma. Cochrane Database Syst Rev (2015) 9:Cd002997. 10.1002/14651858.CD002997.pub4 [DOI] [PubMed] [Google Scholar]
- 72.Yang M, Dong BR, Lu J, Lin X, Wu HM. Macrolides for diffuse panbronchiolitis. Cochrane Database Syst Rev (2013) 2:Cd007716. 10.1002/14651858.CD007716.pub3 [DOI] [PubMed] [Google Scholar]
- 73.Brusselle GG, Vanderstichele C, Jordens P, Deman R, Slabbynck H, Ringoet V, et al. Azithromycin for prevention of exacerbations in severe asthma (AZISAST): a multicentre randomised double-blind placebo-controlled trial. Thorax (2013) 68(4):322–9. 10.1136/thoraxjnl-2012-202698 [DOI] [PubMed] [Google Scholar]
- 74.Kobayashi M, Shimauchi T, Hino R, Tokura Y. Roxithromycin downmodulates Th2 chemokine production by keratinocytes and chemokine receptor expression on Th2 cells: its dual inhibitory effects on the ligands and the receptors. Cell Immunol (2004) 228(1):27–33. 10.1016/j.cellimm.2004.03.011 [DOI] [PubMed] [Google Scholar]
- 75.Ivetić Tkalčević V, Cužić S, Kramarić MD, Parnham MJ, Eraković Haber V. Topical azithromycin and clarithromycin inhibit acute and chronic skin inflammation in sensitized mice, with apparent selectivity for Th2-mediated processes in delayed-type hypersensitivity. Inflammation (2012) 35(1):192–205. 10.1007/s10753-011-9305-9 [DOI] [PubMed] [Google Scholar]
- 76.Parnham MJ, Erakovic Haber V, Giamarellos-Bourboulis EJ, Perletti G, Verleden GM, Vos R. Azithromycin: mechanisms of action and their relevance for clinical applications. Pharmacol Ther (2014) 143(2):225–45. 10.1016/j.pharmthera.2014.03.003 [DOI] [PubMed] [Google Scholar]
- 77.Robinson P, Schechter MS, Sly PD, Winfield K, Smith J, Brennan S, et al. Clarithromycin therapy for patients with cystic fibrosis: a randomized controlled trial. Pediatr Pulmonol (2012) 47(6):551–7. 10.1002/ppul.21613 [DOI] [PubMed] [Google Scholar]
- 78.Ito T, Ito N, Hashizume H, Takigawa M. Roxithromycin inhibits chemokine-induced chemotaxis of Th1 and Th2 cells but regulatory T cells. J Dermatol Sci (2009) 54(3):185–91. 10.1016/j.jdermsci.2009.01.007 [DOI] [PubMed] [Google Scholar]
- 79.Sato Y, Kaneko K, Inoue M. Macrolide antibiotics promote the LPS-induced upregulation of prostaglandin E receptor EP2 and thus attenuate macrolide suppression of IL-6 production. Prostaglandins Leukot Essent Fatty Acids (2007) 76(3):181–8. 10.1016/j.plefa.2006.12.005 [DOI] [PubMed] [Google Scholar]
- 80.Gualdoni GA, Lingscheid T, Schmetterer KG, Hennig A, Steinberger P, Zlabinger GJ. Azithromycin inhibits IL-1 secretion and non-canonical inflammasome activation. Sci Rep (2015) 5:12016. 10.1038/srep12016 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Rodvold KA. Clinical pharmacokinetics of clarithromycin. Clin Pharmacokinet (1999) 37(5):385–98. 10.2165/00003088-199937050-00003 [DOI] [PubMed] [Google Scholar]
- 82.Foulds G, Shepard RM, Johnson RB. The pharmacokinetics of azithromycin in human serum and tissues. J Antimicrob Chemother (1990) 25(Suppl A):73–82. 10.1093/jac/25.suppl_A.73 [DOI] [PubMed] [Google Scholar]
- 83.Fraschini F, Scaglione F, Pintucci G, Maccarinelli G, Dugnani S, Demartini G. The diffusion of clarithromycin and roxithromycin into nasal mucosa, tonsil and lung in humans. J Antimicrob Chemother (1991) 27(Suppl A):61–5. 10.1093/jac/27.suppl_A.61 [DOI] [PubMed] [Google Scholar]
- 84.Dette GA. [Tissue penetration of erythromycin (author’s transl)]. Infection (1979) 7(3):129–45. 10.1007/BF01641314 [DOI] [PubMed] [Google Scholar]
- 85.Schentag JJ, Ballow CH. Tissue-directed pharmacokinetics. Am J Med (1991) 91(3a):5s–11s. 10.1016/0002-9343(91)90394-D [DOI] [PubMed] [Google Scholar]