Abstract
Background:
Too many patients, with or without significant cervical disease, unnecessarily undergo cervical epidural steroid injections (CESIs). These include interlaminar (ICESI) and transforaminal ESI (TF-CESI) injections that are not Food and Drug Administration (FDA) approved, have no documented long-term efficacy, and carry severe risks and complications.
Methods:
Here we reviewed recent reports of morbidity and mortality attributed to the various types of CESIS. Major complications included; epidural hematomas, infection (abscess/meningitis), increased neurological deficits due to intramedullary (quadriparesis/quadriplegia), and intravascular injections (e.g., vertebral artery injections leading to cord, brain stem, and cerebellar strokes). The latter injections leading to strokes were typically attributed to the particulate steroid matter (e.g., within the methylprednisolone injection solution) that embolized into the distal arterial branches.
Results:
Complications of cervical CESI/TF-CESI injections producing epidural hematoma, new neurological deficits (intramedullary injections), or intravascular injections resulting in strokes to the cord, brain stem, and cerebellum are often underreported. Interestingly, several other cases involving adverse events of CESI/TF-CESI may now be found in the medicolegal literature.
Conclusions:
Cervical epidural injecions (e.g., CESI, ICESI, and TF-CESI) which are not FDA approved, provide no long-term benefit, and are being performed for minimal to no indications. They contribute to significant morbidity and mortality, including; epidural hematomas, infection, inadvertent intramedullary cord injections or cord, brain stem, and cerebellar strokes. Furthermore, these injections are increasingly required by insurance carriers prior to granting permission for definitive surgery, thus significantly delaying in some cases necessary operative intervention, while also subjecting patients at the hands of the insurance companies, to the additional hazards of these procedures.
Keywords: Cervical, coma, death, epidural steroid injections, infection, intramedullary, intravascular, paralysis, quadriplegia
INTRODUCTION
Many patients with even minor cervical complaints without significant magnetic resonance/computed tomography (MR/CT) documentation of significant cervical pathology are increasingly being subjected to high-risk cervical epidural steroid injections (CESIs) [e.g., interlaminar (ICESI) and transforaminal (TF-CESI)]. Major complications of these injections include; epidural hematoma, infection (abscess, meningitis), new neurological deficits (e.g., monoparesis to quadriplegia) due to intramedullary injections, and strokes to the spinal cord, brain stem, and/or cerebellum attributed to intravascular injections among others. Further, these cervical injections are still not approved by the Food and Drug Administration (FDA), and have not been proven to be either safe or effective in the cervical or lumbar spine.
LACK OF FDA APPROVAL OF CERVICAL EPIDURAL INJECTIONS WITHOUT DOCUMENTATION OF SAFETY/EFFICAY
Here we reviewed the literature between 2004–2013 and 2017–2018 regarding the severe risks/complications/mortality of CESIs, interlaminar (ICESI), and TF-CESI along with selective lumbar ESI (LESI) and TF-LESI. Further, cervical and lumbar epidural injections are still not approved by FDA as their safety/efficacy have never been established. In 2007, Abbasi et al. recommended performing prospective blinded randomized controlled trials (RCTs) to document such safety/efficacy; to date, none have yet been adequately completed [Table 1].[1] Futher, the severe additionally, the severe complications of these procedures are typically under- or unreported in the spinal literature, and are more likely to be found in medicolegal suits [Table 2].
Table 1.
Summary of articles on CESIs 2004-2013
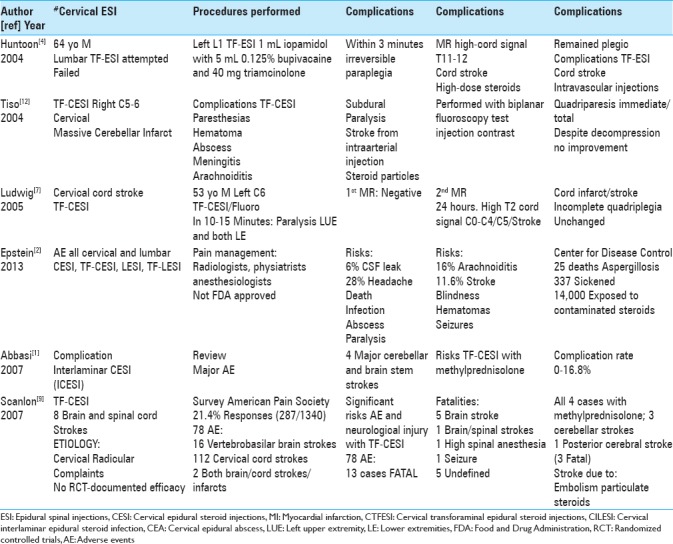
Table 2.
Summary of articles on CESIs 2017-2018
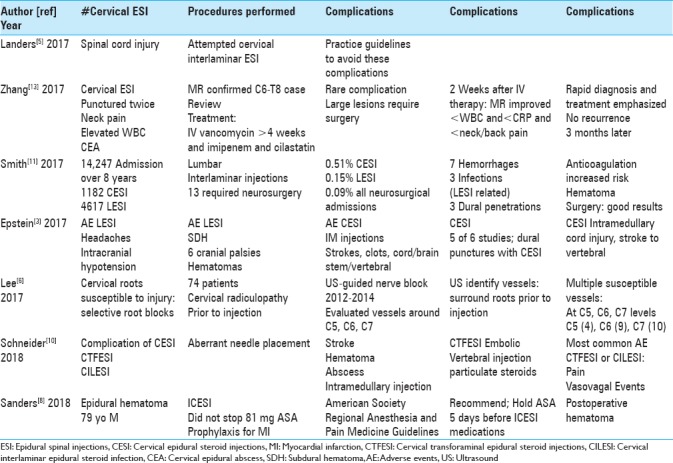
SUMMARY OF RISKS/COMPICATIONS OF CERVICAL AND LUMBAR EPIDURAL INJECTIONS 2004-2013
Multiple risk and complications of CESI (ICESI, TF-CESI) were reported between 2004 and 2013. In 2004, Tiso et al. quoted the major morbidity/mortality of TF-CESI that included; paresthesias, hematoma, epidural abscess, meningitis, arachnoiditis, subdural/subarachnoid injections, and intraarterial injections resulting in stroke [Table 1].[12] Abbasi et al. (2007)[1] documented an overall 0–16.8% frequency of complications from ICESI [Table 1]. In 2013, Epstein further summarized the morbidity/mortality of cervical injections performed by various pain management specialists (e.g. radiologists, physiatrists, or anesthesiologists [Table 1]).[2] Noteworthy, was the lack of training for all three specialists in how to perform a neurological examination, and for the latter two, how to interpret neuroradiological studies (e.g. MR/CT). Notably, cervical epidural injections were still not FDA approved, and still there are no RCT studies documenting their safety/efficacy. Further, in 2013, the Center for Disease Control (CDC) reported that contaminated steroids resulted in 25 deaths (many due to Aspergillosis), with an added 337 patients sickened, and a total of 14,000 exposed. Other life-threatening complications included spinal fluid leaks (0.4–6%), positional headaches (28%), adhesive arachnoiditis (6–16%), intravascular injections/stroke (7.9–11.6%), hydrocephalus, air embolism, urinary retention, allergic reactions, blindness, neurological deficits/paralysis, hematomas, seizures, and death.
SUMMARY OF RISKS/COMPLICATIONS OF CERVICAL AND LUMBAR EPIDURAL INJECTIONS 2017-2018
In 2017, Epstein (2017) again focused on the continued risks/complications of both cervical (CESI, ICESI, TF-CESI) and lumbar (LESI, ILESI, TF-LESI) ESI [Table 2].[3] It was noted that about 9 million epidural injections are performed per year in the US, and they are still not FDA approved. In five of the six cervical ESI studies that Epstein identified, inadvertent dural punctures (CESI) resulted in intramedullary spinal cord injuries and paralysis, or intravascular vertebral artery injections resulted in strokes (e.g., to the spinal cord/brain stem/cerebellum). Schneider et al. (2018) additionally discussed how CESI contributed not only to intramedullary and intravascular injections, leading to embolic infarcts (e.g., from particulate steroids), but also to hematomas, abscesses, vertebral artery dissections, pain, side effects of steroids, and vasovagal reactions [Table 2].[10]
RISKS OF INTRAMEDULLARY EPIDURAL SPINAL INJECTIONS
Cervical ESIs and rarely high LESIs (e.g., CESI, ICESI, TF-CESI, TF-LESI) may result in inadvertent intramedullary cervical and thoracic/conus cord injections [Tables 1 and 2].[5,7] Landers (2017) presented a patient who, immediately following an ICESI, became quadriplegic due to an intramedullary injection [Table 2].[5] The authors presented other cases of CESI resulting in intramedullary injections, and recommended that practice guidelines be revised to avoid such injuries in the future.
CERVICAL INTRAVASCULAR EPIDURAL INJECTIONS
Several articles identified intravascular CESI resulting in major morbidity/mortality [Table 1].[1,7,9,12] In 2004, Tiso et al. presented a patient with a C5-C6 disc herniation on MR; following a C5-C6 TF-CESI, he deeveloped a massive cord/brain stem/cerebellar infarct attributed to an intraarterial injection with resultant embolization of particulate steroids [Table 1].[12] This occurred even after confirming accurate needle placement with biplanar fluoroscopy, after performing several heme-negative aspirations, and utilizing trial injections of contrast. Despite emergent cerebellar decompression, the patient never recovered. In 2005, Ludwig and Burns observed a 53-year-old male who developed left upper and bilateral lower extremity quadriparesis 15 min following a left C6 TF-CESI performed under fluoroscopy [Table 1].[7] Although the first MR showed no intramedullary cord signal changes, the second MR 24 h later revealed a C0-C4/5 intramedullary cord stroke (e.g., patchy high signal intensity in the cord) attributed to an intravascular injection (e.g., embolization of particular steroids; this resulting in permanent paralysis). Abbasi et al. (2007)[1] added an additional four cases of major cerebellar/brain stem strokes [Table 1]. Scanlon et al. (2007) further questioned, after looking at the incidence of stroke following TF-CESI, whether these procedures were “more dangerous than we think” [Table 1]?[9] They again confirmed the lack of adequate RCTs to establish the safety/efficacy of TF-CESI. Additionally, the reviewed eight cases of brain/spinal cord infarction appearing in the literature, and added four cases of major cerebellum/brainstem infarction. Interestingly, when they surveyed US physician members of the American Pain Society [e.g., 21.4% response rate (287 of 1340)], they identified 78 complications of TF-CESI. These included; 16 vertebrobasilar brain infarcts, 12 cervical spinal cord infarcts, and 2 combined brain/spinal cord infarcts: 13 of these patients sustained fatal injuries [Table 1]. They observed that TF-CESIs correlated with an unacceptably high incidence of complications that included; intraarterial injections/strokes/embolism (e.g., to the basilar artery, midbrain, pons, cerebellum, thalamus, temporal, and occipital lobes), along with the occasional vertebral artery perforation, dissection, thrombosis, or vasospasm.
UTILIZING ULTRASOUND TO IDENTIFY VESSELS SURROUNDING C5-C7 CERVICAL NERVE ROOTS PRIOR TO SELECTIVE CERVICAL C5-C7 NERVE ROOT BLOCKS
Lee et al. (2017) utilized ultrasound (US) to document the size/location/number of vulnerable and susceptible perineural blood vessels prior to performing selective nerve root blocks from C5 to C7 (2012–2014) [Table 2].[6] Many vessels were at or in the projected target pathway for selective nerve root blocks; C5 level (n = 4; 5.45%), C6 (n = 9; 12.16%), and C7 (n = 10; 13.51%). This finding confirmed the increased susceptibility to arterial as well as venous intravascular injections during these procedures (e.g. stroke, hematoma, and others).
HIGH LUMBAR L1 TRANSFORAMINAL ESI INJECTION/CORD STROKE
In 2004, Huntoon and Matin (2004) identified a 64-year-old male with a history of multiple prior lumbar operations, who underwent a left L1 TF-LESI; it contained 1 mL of iopamidol (Isovue), 5 mL of 0.125% bupivacaine, and 40 mg of triamcinolone [Table 1].[4] Within 3 min, he was irreversibly paraplegic. The MRI showed a cord infarct (e.g., hyperintense intramedullary cord signal on T2-weighted images) at the T11/L2 level (e.g., conus medullaris). Despite the utilization of high-dose steroids, the patient's deficit remained fixed.
INCIDENCE OF HEMORRHAGES DUE TO VARIOUS CERVICAL/LUMBAR EPIDURAL STEROID INJECTIONS
Two studies cited the risks of peri-procedural hematomas in patients undergoing CESI and LESI [Table 2].[8,11] Smith et al. (2017), over an 8-year period, identified complications following 1182 ICESI and 4617 ILESI [Table 2].[11] Thirteen patients required emergency neurosurgery to address; 7 hemorrhages, 3 infections (all after lumbar injections), and 3 inadvertent dural punctures. Notably, six of seven patients developed epidural hematomas despite being managed with current guidelines [e.g., requiring prolonged cessation of anticoagulation (n = 3), or taking only aspirin (n = 3)]. Surgical decompression in all cases fortunately resulted in neurological improvement. In the case study from Sanders et al. (2018), a 79-year-old male continued prophylactic baby aspirin therapy (81 mg) prior to a LESI due to a recent myocardial infarction [Table 2].[8] The patient and his physicians failed to follow the antiplatelet and anticoagulation guidelines of the American Society of Regional Anesthesia and Pain Medicine that required the 81 mg of ASA be held for 5 days before such a procedure. The result was an immediate postinjection epidural hematoma and permanent paraparesis.
CERVICAL EPIDURAL ABSCESS DUE TO CESI
Zhang et al. (2017) noted that CESI rarely result in cervical epidural abscess (CEA).[13] In some cases they may be effectively treated with antibiotic therapy alone, but in others, they may warrant operative debridement [Table 2].[13] Their patient had a CESI, and later developed a C6-T8 CEA on MR. The patient was effectively treated with 4 weeks of intravenous vancomycin, imipenem, and cilastatin. Following just 2 weeks of therapy, the patient's symptoms and laboratory studies improved [e.g., for the latter, the white blood cell count decreased along with the neutrophil count, and C-reactive protein (CRP)]. Three months later, the patient fully recovered, and the follow-up MR documented complete resolution of the abscess. Notably, in the US, infectious disease consultants would typically require a minimum of 6 weeks of intravenous antibiotic therapy, followed in some cases by long-term suppressive oral antibiotics.
CONCLUSION
Cervical ESI (CESI, ICESI, TF-CESI) and lumbar ESI (LESI, ILESI, TF-LESI) are not FDA-approved and have no RCT-documented long-term safety or efficacy. Further, CESI and occasionally high LESI (e.g., TF-LESI at the L1 level) risks include severe morbidity and mortality. Intramedullary or intravascular injections result in irreversible paralysis and/or strokes (e.g., cord, brain stem, and cerebellar strokes).
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Footnotes
REFERENCES
- 1.Abbasi A, Malhotra G, Malanga G, Elovic EP, Kahn S. Complications of interlaminar cervical epidural steroid injections: A review of the literature. Spine (Phila Pa 1976) 2007;32:2144–51. doi: 10.1097/BRS.0b013e318145a360. [DOI] [PubMed] [Google Scholar]
- 2.Epstein NE. The risks of epidural and transforaminal steroid injections in the Spine: Commentary and a comprehensive review of the literature. Surg Neurol Int. 2013;4(Suppl 2):S74–93. doi: 10.4103/2152-7806.109446. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Epstein NE. Neurological complications of lumbar and cervical dural punctures with a focus on epidural injections. Surg Neurol Int. 2017;8:60. doi: 10.4103/sni.sni_38_17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Huntoon MA, Martin DP. Paralysis after transforaminal epidural injection and previous spinal surgery. Reg Anesth Pain Med. 2004;29:494–5. doi: 10.1016/j.rapm.2004.05.002. [DOI] [PubMed] [Google Scholar]
- 5.Landers MH. Spinal cord injury during attempted cervical interlaminar epidural injection of steroids. Pain Med. 2017 doi: 10.1093/pm/pnx081. Epub ahead of print. [DOI] [PubMed] [Google Scholar]
- 6.Lee HH, Park D, Oh Y, Ryu JS. Ultrasonography evaluation of vulnerable vessels around cervical nerve roots during selective cervical nerve root block. Ann Rehabil Med. 2017;41:66–71. doi: 10.5535/arm.2017.41.1.66. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Ludwig MA, Burns SP. Spinal cord infarction following cervical transforaminal epidural injection: A case report. Spine (Phila Pa 1976) 2005;30:E266–8. doi: 10.1097/01.brs.0000162401.47054.00. [DOI] [PubMed] [Google Scholar]
- 8.Sanders RA, Bendel MA, Moeschler SM, Mauck WD. Epidural hematoma following interlaminar epidural injection in patient taking aspirin. Reg Anesth Pain Med. 2018 doi: 10.1097/AAP.0000000000000730. Epub ahead of print. [DOI] [PubMed] [Google Scholar]
- 9.Scanlon GC, Moeller-Bertram T, Romanowsky SM, Wallace MS. Cervical transforaminal epidural steroid injections: More dangerous than we think? Spine (Phila Pa 1976) 2007;32:1249–56. doi: 10.1097/BRS.0b013e318053ec50. [DOI] [PubMed] [Google Scholar]
- 10.Schneider BJ, Maybin S, Sturos E. Safety and Complications of Cervical Epidural Steroid Injections. Phys Med Rehabil Clin N Am. 2018;29:155–69. doi: 10.1016/j.pmr.2017.08.012. [DOI] [PubMed] [Google Scholar]
- 11.Smith GA, Pace J, Strohl M, Kaul A, Hayek S, Miller JP. Rare Neurosurgical complications of epidural injections: An 8-yr single-institution experience. Oper Neurosurg (Hagerstown) 2017;13:271–9. doi: 10.1093/ons/opw014. [DOI] [PubMed] [Google Scholar]
- 12.Tiso RL, Cutler T, Catania JA, Whalen K. Adverse central nervous system sequelae after selective transforaminal block: The role of corticosteroids. Spine J. 2004;4:468–74. doi: 10.1016/j.spinee.2003.10.007. [DOI] [PubMed] [Google Scholar]
- 13.Zhang JH, Wang ZL, Wan L. Cervical epidural analgesia complicated by epidural abscess: A case report and literature review. Medicine (Baltimore) 2017;96:e7789. doi: 10.1097/MD.0000000000007789. [DOI] [PMC free article] [PubMed] [Google Scholar]


