Abstract
Introduction:
There are concerns about potential overuse of colorectal cancer (CRC) screening services among average-risk individuals older than age 75 years.
Materials and Methods:
Using a 5% random noncancer sample of Medicare beneficiaries who resided in the SEER areas, we examined rates of CRC screening adherence, defined by the Medicare coverage policy, among average-risk fee-for-service beneficiaries age 76 to 95 years from 2002 to 2010. The two outcomes are the status of overall CRC screening adherence, and the status of adherence to colonoscopy (v other modalities) conditional on patient adherence.
Results:
Overall CRC screening adherence rates of Medicare beneficiaries age 76 to 95 years increased from 13.0% to 21.4% from 2002 to 2010. In 2002, 2.2% of beneficiaries were adherent to colonoscopy, and 10.7%, by other modalities; the corresponding rates were 19.5% and 1.9%, respectively, in 2010. Specifically, rates of adherence to colonoscopy were 1.1% for those age 86 to 90 years and almost nil for those age 91 to 95 years in 2002, but the rates became 13.5% and 8.2%, respectively, in 2010. Compared with white beneficiaries, black beneficiaries age 76 to 95 years had a 7-percentage-point lower adherence rate. However, overall adherence rates among blacks increased by 168.6% from 2002 to 2010, whereas rates among whites increased by 63.0%. Logistic regressions showed that blacks age 86 to 95 years were less likely than whites to be adherent (odds ratio, 0.56; 95% CI, 0.47 to 0.59) but were more likely to be adherent to colonoscopy (odds ratio, 2.34; 95% CI, 1.47 to 3.91).
Conclusion:
High proportions of average-risk Medicare fee-for-service beneficiaries screened by colonoscopy may represent opportunities for improving appropriateness and allocative efficiency of CRC screening by Medicare.
INTRODUCTION
Colorectal cancer (CRC) screening adherence rates have been widely used as a health care performance measure. Medicare-covered CRC screening modalities for average-risk beneficiaries include fecal occult blood test (FOBT) annually and flexible sigmoidoscopy (FS) or double-contrast barium enema (DCBE) every 5 years, as of January 1, 1998, and colonoscopy every 10 years as of July 1, 2001.1-3 Medicare, a nationwide program that provides healthcare insurance to those older than age 65 years or those who live with certain disabilities, has continued its CRC screening coverage policy of the four screening modalities for average-risk beneficiaries older than age 50 years since 1998, though the US Preventive Services Task Force (USPSTF) does not recommend routine CRC screening of average-risk individuals older than age 75 years.4-10
There has been no study of rates of CRC screening adherence for the elderly since Medicare coverage of CRC screening began in 1998. Determination of the CRC screening adherence may be challenging, because different screening modalities may be associated with different recommended screening intervals, and because the length of recommended screening intervals may vary by the degree of CRC risk.11-14 For example, 10-year, complete retrospective information on use of screening services is needed to accurately determine the up-to-date status of CRC screening adherence to colonoscopy for the average-risk person.15
In this study, we examined rates of CRC screening adherence, defined according to the Medicare CRC screening coverage policy of the average-risk individual, among fee-for-service (FFS) beneficiaries age 76 to 95 years, between 2002 and 2010. By using a 5% random noncancer sample of Medicare beneficiaries who resided in the Surveillance, Epidemiology, and End Results (SEER) areas, this study applied a previously published and validated, recently updated, claims-based data measurement method for (1) differentiation of the average risk from the higher risk for CRC and (2) determination of the status of CRC screening adherence.15-17 Because there have been growing concerns about the overuse of CRC screening services for the average-risk person older than age 75 years, any adherence to FOBT for those age 76 to 95 years, to FS/DCBE for those age 80 to 95 years, or to colonoscopy for those age 86 to 95 years could be considered potential overuse. As a result, we specifically focused on a subsample of average-risk beneficiaries age 86 to 95 years for whom any screening may be considered potential overuse according to USPSTF recommendations.4,11,18-20
MATERIALS AND METHODS
Data Sources
The data were from a 5% random noncancer sample from 2002 to 2010 of Medicare beneficiaries who resided in the SEER areas, which accounted for approximately a quarter of the US population. The data source was generated primarily as potential (case-control) at-risk samples that are frequently used in longitudinal comparisons, and the incident cancer samples were identified in these SEER registries.3,8,21,22 One main advantage of this data source for our study was that repeated SEER-wide representative annual cohorts of cancer-free (eg, exclusion of CRC) beneficiaries could be constructed for examination of the rates of CRC screening adherence. This sample included a summary file and claim files. The summary file included information on the Medicare eligibility status, demographics, monthly health maintenance organization (HMO) enrollment status, and residential-level socioeconomic indicators of the beneficiaries. Four claim files used for this study included Medicare FFS-covered services recorded in inpatient, physician, outpatient, and hospice settings available from 1998 to 2010. (Note that Medicare began coverage for CRC screening in 1998. As a result, this study assumed that no CRC screening services were provided to the elderly before 1998.) The key variables in the claim files relevant to this study included primary and secondary International Classification of Disease, 9th revision, clinical modification diagnostic codes and current procedural terminology, 4th edition, codes. This study was approved by the local institutional review board.
Study Sample
The sample consisted of nine cohorts, one for each of the 9 years from 2002 to 2010. Because each of the nine cohorts was constructed in an identical fashion, we used the 2010 cohort to illustrate the method for the identification of a cohort.15,16 The inclusion/exclusion criteria used all three claim files for identification of average-risk individuals. A list of diagnostic codes, primarily for identification of higher-risk individuals, was based on the published research.15-17,23
The 2010 cohort included average-risk Medicare FFS beneficiaries if they were (1) age 76 to 95 years in 2010, (2) enrolled in Medicare for the age eligibility reason only, (3) enrolled in FFS plans and in Part A and B benefits in every month in 2010 and in the previous 9 years, (4) not diagnosed with any primary or secondary diagnoses in the three claim files at higher risks for CRC (eg, Crohn disease, ulcerative colitis, colorectal polyps, family history of unspecified malignant neoplasm), and (5) not in hospice settings in 2010 and the previous 4 years.15,17,23
Variables
The two outcomes are the status of overall CRC screening adherence and the status of adherence to colonoscopy (v FOBT, FS, and DCBE) conditional on beneficiary adherence in a given year. Because these two variables were measured similarly in each of the nine cohorts, we again used the 2010 cohort to illustrate the method for creating the variables.
According to the Medicare coverage policy of CRC screening of the average-risk individual, we used physician claims to determine the following adherence statuses of each beneficiary: (1) adherent to colonoscopy if there was at least one colonoscopy code from the current procedural terminology, 4th edition, in 2010 or in the previous 9 years, (2) adherent to FS/DCBE if there was at least one FS/DCBE code in 2010 or in the previous 4 years (FS and DCBE were combined as a single, modality because neither was frequently used), (3) adherent to FOBT if there was at least one FOBT code in 2010, or (4) nonadherent in 2010.13,15 Thus, the overall CRC adherence status in 2010 was coded as 1 if a beneficiary was adherent to one of the four modalities but was coded as 0 otherwise. Conditional on patient adherence, the status of adherence to colonoscopy was coded as 1 if a beneficiary was adherent to colonoscopy but was coded as 0 otherwise. (Note that, in the 2002 to 2009 cohorts, we did not search for colonoscopies before 2001, the first year when Medicare started coverage for colonoscopy of screening the average-risk individual.)
In each of the nine cohorts, demographic variables included age categorized into four groups (76 to 80, 81 to 85, 86 to 90, or 91 to 95 years), race/ethnicity categorized into three groups (non-Hispanic whites, blacks, or other), and sex. The Charlson comorbidity index, a proxy for frailty, was calculated from the primary and secondary diagnosis codes in the inpatient claims files during the given year of interest and the previous 4 years.24 The Charlson comorbidity index was categorized into three groups (0, 1, or > 1). We created a beneficiary-level Medicare state buy-in program entitlement status variable, a proxy for the socioeconomic status, which was coded as 1 if a beneficiary was eligible for a state buy-in subsidy for at least 1 month during the given year but was coded as 0 otherwise. The last variable, the rural/urban status of the residency of the beneficiary, was categorized into four groups.
Statistical Analyses
We first delineated rates of overall CRC screening adherence by year and demographic variables. With a study sample that consisted of the entire 9-year cohort, we used logistic regressions to examine the associations of demographic variables, Charlson comorbidity index, Medicare state buy-in entitlement status, urban/rural status, and year dummies with the overall CRC screening adherence status. To examine shifts in screening modality between colonoscopy and the other three modalities, we restricted the sample to those who were adherent and repeated the above model, with the dependent variable of whether adherence was achieved by colonoscopy or by the other modalities. Finally, we analyzed a subsample of beneficiaries age 86 to 95 years, because all adherences in this age range may be considered potential overusers of screening services. Because the 9-year cohort contained beneficiaries who may have been observed repeatedly, standard errors were adjusted by the clustered standard errors correction at the beneficiary level.25
RESULTS
Descriptive Analyses
The sample size of the 9-year cohort of average-risk, Medicare FFS beneficiaries age 76 to 95 years, included a total of 187,372 beneficiary-years. Table 1 lists the sample size by year, which varied from 23,119 in 2002 and 20,461 in 2006 to 19,167 in 2010. There were a total of 61,634 unique beneficiaries in the 9-year cohort.
Table 1.
Mean Descriptive Statistics of Average-Risk Medicare FFS Beneficiaries Age 76 to 95 Years From 2002 to 2010
| Variable | % of Beneficiaries by Year | P* | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| 2002 (n = 23,119) | 2003 (n = 22,353) | 2004 (n = 22,535) | 2005 (n = 21,435) | 2006 (n = 20,461) | 2007 (n = 19,841) | 2008 (n = 19,425) | 2009 (n = 19,036) | 2010 (n = 19,167) | ||
| Overall CRC screening adherence | 13.0 | 13.1 | 14.1 | 13.7 | 14.5 | 15.7 | 17.9 | 19.3 | 21.4 | < .001 |
| Colonoscopy | 2.2 | 3.9 | 5.5 | 7.3 | 9.7 | 12.4 | 15.0 | 17.1 | 19.5 | |
| FS/DCBE | 3.1 | 2.7 | 2.1 | 1.4 | 0.9 | 0.5 | 0.4 | 0.3 | 0.2 | |
| FOBT | 7.6 | 6.5 | 6.5 | 5.0 | 3.9 | 2.9 | 2.5 | 1.9 | 1.7 | |
| Age range, years | ||||||||||
| 76-80 | 49.0 | 48.5 | 47.7 | 47.0 | 46.5 | 45.8 | 45.5 | 44.9 | 44.8 | < .001 |
| 81-85 | 31.3 | 32.2 | 32.3 | 33.0 | 32.6 | 32.4 | 31.8 | 32.3 | 31.6 | |
| 86-90 | 14.7 | 14.4 | 14.7 | 14.9 | 16.0 | 16.2 | 17.0 | 17.3 | 17.8 | |
| 91-95 | 5.0 | 4.9 | 5.3 | 5.1 | 5.0 | 5.6 | 5.7 | 5.5 | 5.7 | |
| Race/ethnicity | ||||||||||
| Non-Hispanic white | 87.8 | 87.4 | 87.4 | 87.4 | 87.3 | 87.3 | 87.1 | 86.5 | 86.3 | < .001 |
| African American | 7.0 | 6.8 | 6.6 | 6.4 | 6.1 | 5.6 | 5.7 | 5.8 | 5.6 | |
| Other | 5.2 | 5.8 | 6.0 | 6.2 | 6.5 | 7.0 | 7.2 | 7.7 | 8.1 | |
| Men, % | 35.8 | 36.6 | 37.2 | 37.4 | 38.6 | 39.2 | 39.8 | 40.6 | 41.2 | < .001 |
| Charlson index | ||||||||||
| 0 | 85.3 | 85.2 | 83.9 | 85.5 | 85.8 | 86.1 | 85.9 | 86.7 | 87.3 | < .001 |
| 1 | 8.1 | 8.2 | 8.8 | 7.9 | 7.6 | 7.4 | 7.6 | 7.1 | 6.6 | |
| > 1 | 6.5 | 6.6 | 7.3 | 6.6 | 6.6 | 6.5 | 6.6 | 6.1 | 6.1 | |
| Medicare state buy-in program entitlement | 11.1 | 11.2 | 10.9 | 10.8 | 10.7 | 10.6 | 10.6 | 10.5 | 11.1 | > .05 |
| Urban/rural status | ||||||||||
| Large metro | 45.4 | 45.9 | 46.5 | 46.3 | 46.2 | 46.6 | 46.0 | 46.0 | 46.7 | < .05 |
| Metro | 32.6 | 32.1 | 32.4 | 32.2 | 32.3 | 32.1 | 32.4 | 32.3 | 32.2 | |
| Urban | 7.4 | 7.7 | 7.4 | 7.5 | 7.6 | 7.4 | 7.5 | 7.5 | 7.5 | |
| Less urban/rural | 14.5 | 14.3 | 13.7 | 14.0 | 13.9 | 13.8 | 14.2 | 14.2 | 13.6 | |
Abbreviations: CRC, colorectal cancer; DCBE, double-contrast barium enema; FFS, fee for service; FOBT, fecal occult blood test; FS, flexible sigmoidoscopy.
The Pearson χ2 test was used to test time trends.
The overall CRC screening adherence rates increased from 13.0% to 21.4% from 2002 to 2010 (Table 1). FOBT and FS/DCBE were the primary modalities in 2002. However, colonoscopy became more dominating over time. In 2002, 7.6% of individuals were adherent to FOBT; 3.2%, to FS/DCBE; and only 2.2%, to colonoscopy. In 2010, the corresponding rates became 1.7%, 0.2%, and 19.5%. Among those adherent individuals, the proportion of adherence to colonoscopy increased from 17.1% in 2002 to 91.1% in 2010.
The rates of demographic and other variables remained relatively stable during the study period (Table 1). From 2002 to 2010, the proportion of beneficiaries age 86 to 95 years increased by four percentage points. The proportion of whites ranged from 87.82% to 86.35%, and the proportions of blacks decreased slightly from 7.0% to 5.6% during the 9-year period. The proportion of men increased from 35.8% in 2002 to 41.2% in 2010. The proportion of those who had Charlson morbidity index of 0 stayed at approximately 85% throughout the 9 years. Finally, the proportion of beneficiaries who were eligible for Medicare state buy-in entitlement remained at approximately 11.0%.
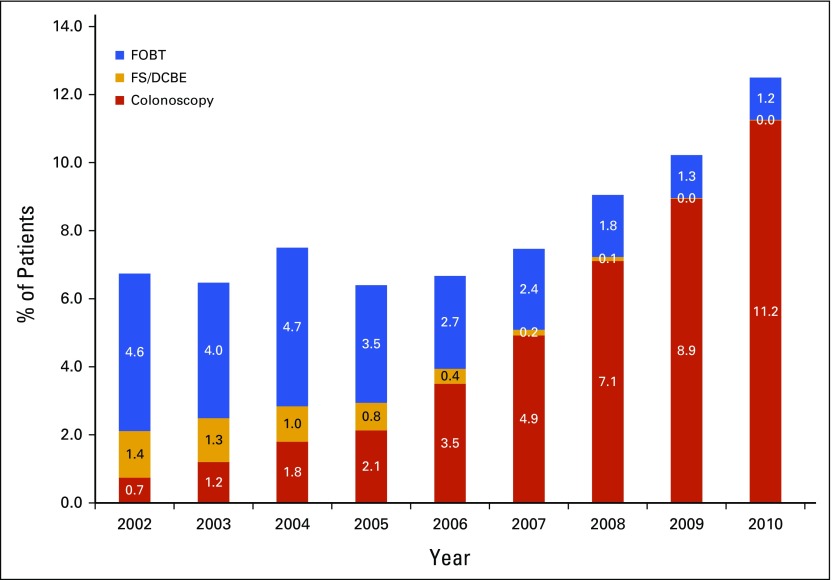
Table 2 lists the rates of overall CRC screening adherence and of adherence to colonoscopy among the subpopulations defined by demographic variables. The time trends among the four age groups were similar to the trend that averaged across all four of the age groups. Specifically, rates of adherence to colonoscopy were 1.1% for those age 86 to 90 years and almost nil for those age 91 to 95 years in 2002, but rates became 13.5% and 8.2%, respectively, in 2010. Figure 1 shows the rates of CRC screening adherence by modality among those individuals age 86 to 90 years and 91 to 95 years combined.
Table 2.
Rates of CRC Screening Adherence by Demographic Variables Among Average-Risk Medicare FFS Beneficiaries Age 76 to 95 Years From 2002 to 2010
| CRC screening type by demographic variable | % Adherence Rate by Year | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| 2002 | 2003 | 2004 | 2005 | 2006 | 2007 | 2008 | 2009 | 2010 | |
| Age 76-80 years | |||||||||
| Overall CRC screening adherence | 15.4 | 15.9 | 17.1 | 17.0 | 18.3 | 19.6 | 22.6 | 23.6 | 25.7 |
| Colonoscopy | 3.0 | 5.3 | 7.6 | 10.2 | 13.2 | 16.1 | 19.6 | 21.0 | 23.6 |
| FS/DCBE | 3.9 | 3.3 | 2.5 | 1.5 | 1.1 | 0.6 | 0.5 | 0.4 | 0.2 |
| FOBT | 8.5 | 7.3 | 6.9 | 5.2 | 4.1 | 2.8 | 2.5 | 2.2 | 1.9 |
| Age 81-85 years | |||||||||
| Overall CRC screening adherence | 12.6 | 12.4 | 13.5 | 13.1 | 13.6 | 15.4 | 16.8 | 19.1 | 20.9 |
| Colonoscopy | 1.8 | 3.2 | 4.5 | 6.3 | 8.4 | 11.7 | 13.7 | 16.8 | 19.0 |
| FS/DCBE | 3.0 | 2.5 | 2.1 | 1.4 | 0.9 | 0.6 | 0.4 | 0.3 | 0.3 |
| FOBT | 7.8 | 6.7 | 6.8 | 5.4 | 4.4 | 3.1 | 2.7 | 2.0 | 1.6 |
| Age 86-90 years | |||||||||
| Overall CRC screening adherence | 8.4 | 8.1 | 9.0 | 8.4 | 8.3 | 9.2 | 11.4 | 12.5 | 15.2 |
| Colonoscopy | 1.1 | 1.6 | 2.4 | 2.8 | 4.6 | 6.1 | 8.9 | 11.0 | 13.5 |
| FS/DCBE | 1.6 | 1.6 | 1.3 | 1.1 | 0.6 | < 1.0* | < 1.0 | < 1.0 | < 1.0 |
| FOBT | 5.7 | 4.9 | 5.4 | 4.5 | 3.2 | 2.9 | 2.4 | 1.5 | 1.6 |
| Age 91-95 years | |||||||||
| Overall CRC screening adherence | 4.4 | 4.1 | 6.0 | 3.0 | 3.9 | 5.0 | 5.6 | 6.9 | 8.7 |
| Colonoscopy | < 1.0 | < 1.0 | < 1.0 | < 1.0 | 1.6 | 3.3 | 4.5 | 6.1 | 8.2 |
| FS/DCBE | 1.2 | 1.0 | 0.8 | 0.4 | < 1.0 | < 1.0 | < 1.0 | < 1.0 | < 1.0 |
| FOBT | 3.1 | 2.6 | 4.3 | 1.7 | 2.2 | 1.6 | < 1.0 | < 1.0 | < 1.0 |
| Non-Hispanic white | |||||||||
| Overall CRC screening adherence | 13.6 | 13.7 | 14.9 | 14.3 | 15.2 | 16.4 | 18.6 | 20.2 | 22.2 |
| Colonoscopy | 2.3 | 4.0 | 5.7 | 7.7 | 10.2 | 12.9 | 15.7 | 17.9 | 20.2 |
| FS/DCBE | 3.3 | 2.8 | 2.2 | 1.4 | 0.9 | 0.5 | 0.4 | 0.3 | 0.2 |
| FOBT | 8.0 | 6.9 | 6.9 | 5.2 | 4.1 | 3.0 | 2.5 | 2.0 | 1.8 |
| Black | |||||||||
| Overall CRC screening adherence | 5.9 | 6.6 | 6.7 | 7.6 | 8.7 | 10.8 | 11.6 | 12.6 | 15.7 |
| Colonoscopy | 1.2 | 2.2 | 3.1 | 4.2 | 6.0 | 8.6 | 10.1 | 11.6 | 14.5 |
| FS/DCBE | 2.0 | 1.8 | 1.1 | 1.0 | < 1.0 | < 1.0 | < 1.0 | < 1.0 | < 1.0 |
| FOBT | 2.7 | 2.6 | 2.5 | 2.3 | 2.0 | 1.4 | 1.4 | < 1.0 | < 1.0 |
| Other race/ethnicity | |||||||||
| Overall CRC screening adherence | 11.0 | 11.4 | 11.7 | 11.0 | 10.2 | 11.3 | 13.6 | 14.5 | 16.1 |
| Colonoscopy | 2.3 | 4.0 | 5.3 | 5.8 | 6.6 | 8.8 | 10.4 | 12.4 | 14.6 |
| FS/DCBE | 2.4 | 1.9 | 1.5 | 1.0 | < 1.0 | < 1.0 | < 1.0 | < 1.0 | < 1.0 |
| FOBT | 6.3 | 5.4 | 5.0 | 4.2 | 3.5 | 2.4 | 2.9 | 1.9 | 1.4 |
| Female | |||||||||
| Overall CRC screening adherence | 12.4 | 12.4 | 13.4 | 12.8 | 13.3 | 14.2 | 16.4 | 17.7 | 20.2 |
| Colonoscopy | 1.8 | 3.2 | 4.6 | 6.5 | 8.3 | 10.7 | 13.4 | 15.5 | 18.1 |
| FS/DCBE | 2.7 | 2.4 | 1.8 | 1.1 | 0.8 | 0.4 | 0.4 | 0.3 | 0.2 |
| FOBT | 7.9 | 6.9 | 6.9 | 5.2 | 4.2 | 3.0 | 2.7 | 1.9 | 1.8 |
| Male | |||||||||
| Overall CRC screening adherence | 13.9 | 14.2 | 15.4 | 15.2 | 16.3 | 18.2 | 20.0 | 21.7 | 23.1 |
| Colonoscopy | 3.0 | 5.1 | 7.0 | 8.8 | 11.8 | 14.9 | 17.5 | 19.4 | 21.4 |
| FS/DCBE | 3.9 | 3.2 | 2.6 | 1.8 | 1.0 | 0.6 | 0.3 | 0.3 | 0.2 |
| FOBT | 6.9 | 5.9 | 5.8 | 4.6 | 3.5 | 2.7 | 2.1 | 2.0 | 1.5 |
Abbreviations: CRC, colorectal cancer; DCBE, double-contrast barium enema; FFS, fee for service; FOBT, fecal occult blood test; FS, flexible sigmoidoscopy.
Values of < 1.0 were imputed because the numerators in these cells were too small to make reliable estimates, according to the requirement by the data provider.
FIG 1.
Rates of colorectal cancer screening adherence among average-risk Medicare fee-for-service beneficiaries age 86 to 95 years. Numbers within different bar sections represent percentages of patients who adhered to that specific test each year. FOBT, fecal occult blood test; FS/DCBE, flexible sigmoidoscopy/double-contrast barium enema.
The racial and ethnic differences in CRC screening adherence were prominent. Between blacks and whites, there was, on average, a gap of seven percentage points in overall adherence rates during the 9 years (Table 2). However, the overall adherence rates among blacks increased by 168.6%, whereas the rates among the whites increased by only 63.0%, from 2002 to 2010. By combining data of the beneficiaries who were age 86 to 95 years into a single group, we found that the proportions among blacks adherent to colonoscopy increased from 25.0% to 90.5% from 2002 to 2010, whereas the proportions among white counterparts were 10.2% and 89.6%, respectively. In sex differences, men were more likely than women to be adherent. The sex gaps that had been largely driven by differences in adherence to colonoscopy became wider over time and reached a difference of three percentage points by 2010.
Logistic Regression
Four logistic regressions used to estimate the associations of independent variables with CRC screening adherence are listed in Appendix Table A1 (online only). The first model, which used the entire sample, showed that older age was associated with lower overall adherence rates (all P < .05). Compared with whites, blacks were less likely to be adherent (odds ratio [OR], 0.61; 95% CI, 0.57 to 0.65). Men were more likely than women to be adherent (OR, 1.13; 95% CI, 1.10 to 1.16). The associations of the Charlson comorbidity index with overall adherence were mixed. Compared with a Charlson comorbidity index of 0, an index of 1 slightly increased the likelihood of overall adherence (OR, 1.06; 95% CI, 1.01 to 1.12), whereas a Charlson comorbidity index greater than 1 decreased the likelihood (OR, 0.83; 95% CI, 0.78 to 0.88). Entitlement to a Medicare state buy-in program was associated with a lower likelihood of overall adherence (OR, 0.37; 95% CI, 0.34 to 0.39). Residence in large metro areas (populations greater than 1 million) was associated with a lower likelihood of overall adherence than residence in metro or urban areas (populations between 250,000 and 1 million; both P < .05). The second model restricted the entire sample to the subsample of individuals who were adherent. As age increased, beneficiaries were less likely to be adherent to receiving a colonoscopy (P < .05). Blacks were significantly more likely than whites to be adherent to colonoscopy (OR, 1.32; 95% CI, 1.13 to 1.55); men were more likely than women to be adherent to colonoscopy (OR, 1.46; 95% CI, 1.38 to 1.55). Beneficiaries who had a Charlson comorbidity index of 1 or > 1 were more likely to be adherent to colonoscopy than those who had a an index of 0 (both P < .05). The results of the two remaining regression models, both restricted to beneficiaries age 86 to 95 years only, were similar to the first and second models, respectively.
DISCUSSION
Among average-risk Medicare FFS beneficiaries age 76 to 95 years, overall screening adherence rates increased steadily from 13.0% to 21.4% from 2002 to 2010. Among the adherent, the proportions of adherence to colonoscopy increased from 17.1% to 91.1%, and the proportions of adherence to the other three modalities continued to decline. The rapid increase in overall adherence rates was likely associated with the Medicare coverage policy of screening colonoscopy for the average-risk beneficiaries that took effect in 2001 and with the 10-year screening interval recommended for colonoscopy.
Because routine CRC screening services, particularly colonoscopy for the average-risk individual older than 75 years, were not endorsed by the USPSTF recommendations, this study additionally examined the rates among a subpopulation of the average-risk beneficiaries age 86 to 95 years, in which all CRC screening adherence, according to the Medicare CRC screening coverage policy, was the result of CRC screening services received after the age of 75 years. For this subpopulation, the overall adherence rate increased from 8.4% to 15.18% among those age 86 to 90 years and from 4.4% to 8.7% among those age 91 to 95 years during the 9-year period. These increases were largely driven by use of colonoscopy.
Among those age 76 to 95 years, adherence rates of blacks were seven percentage points lower than those of white individuals during the study period. Across the 2002 to 2010 period though, adherence rates of blacks increased much faster than those of whites, largely driven by a notable racial/ethnic difference in adherence to use of colonoscopy. Similarly, logistic regression analyses suggested that, among those who were adherent, blacks were more likely than whites to be adherent to colonoscopy. We also observed sex gaps in adherence rates: men were consistently more likely than women to be adherent across the 9-year period. Not surprisingly, the gaps appear to be associated with much greater use of colonoscopy by men.
To our knowledge, this is the first study to report the rates of CRC screening adherence among average-risk Medicare FFS beneficiaries since Medicare started its screening colonoscopy coverage for the average-risk individual. Previous studies reported increases in CRC screening among the elderly.3,12-14,26-29 However, almost all of these studies focused on the use of CRC screening services without distinguishing the risk level for CRC. As a result, an evaluation of overuse is not possible, because the patients may have been at higher-than-average risk for CRC.
The reported gaps between blacks and whites in overall adherence rates were modestly encouraging. Although the magnitude of the disadvantages of blacks remained constant, adherence rates of blacks increased more rapidly than those of whites since 2002. Our results were similar to those reported elsewhere on the use of CRC screening services.3,26,30-33 However, there were some concerns that blacks, particularly those age 86 to 95 years, may have overused colonoscopy as the primary screening modality simply to keep the adherence rates of blacks similar to the rates of other racial/ethnic groups. The sex gaps in this study were similarly reported in veteran populations age 50 to 64 years.15
This associational study has five main limitations. First, we were concerned about potential incompatibility of the nine cohorts during the study period. The sample size became smaller over time, and higher proportions of beneficiaries age 86 to 95 years were observed in the later years. One of the main reasons for these observed shifts was the increase in Medicare HMO enrollment that kept a larger number of frailer beneficiaries in our cohorts over time. As a result, the reported rates of overall adherence and of adherence to colonoscopy in the later years may be under-reported. Second, our study may be subject to some measurement errors. The method for identifying average-risk populations and for determining types of modality, although well validated, may still be subject to this type of error. For example, although this study was intended for average-risk beneficiaries, our sample may have possibly included a small proportion of higher-risk beneficiaries (eg, diagnoses of the first-degree family members who had a history of CRC or prior polyp/adenoma history may be under-recorded in claims data). However, the recently published claims data-based measurement method used in this study had high specificity for identifying average-risk populations.15,16 Another type of measurement error is the possible unreliability of using claims data to determine adherence to FOBT.14 As a result, we might have under-reported overall adherence rates. However, studies have shown that the use of FOBT has notably decreased over time, so potential under-reporting would not significantly alter the observed rates and associations.18 In addition, our method for measuring adherence may be subject to error. For example, if CRC screening services were recommended by physicians but somehow were not delivered to patients, our method, which is based on the screening services actually rendered, may yield lower overall adherence rates. However, the information on screening recommendations is not available in claims data.
Third, this study was unable to determine inappropriateness of CRC screening services, especially colonoscopy. We used the Charlson comorbidity index as a proxy of beneficiary frailty in assessing whether higher frailty was associated with lower rates of overall adherence and of adherence to colonoscopy. The logistic regressions yielded mixed results. Thus, we were unable to infer inappropriateness of the observed high rates of overall screening adherence and of adherence to colonoscopy among beneficiaries age 86 to 95 years. Fourth, we were unable to assess whether the increased CRC screening adherence rates among the average-risk Medicare FFS beneficiaries older than age 75 years were associated with CRC outcomes (eg, early detection), because no data are currently available for such an assessment. Finally, the generalizability of this study was limited, because our results may not be applicable to other populations, such as Medicare HMO beneficiaries.
This study has made significant contributions to better understand the patterns of CRC screening adherence among average-risk Medicare FFS beneficiaries older than age 75 years. We observed that high proportions of average-risk Medicare FFS beneficiaries age 86 to 95 years were adherent to colonoscopy. This observation indicates potential overuse of colonoscopies for screening the average-risk individual older than age 75 years. This finding suggests that, to improve efficiency of CRC screening delivery, Medicare should start considering reimbursement of physicians for the time they spend discussing the benefits and risks of screening colonoscopy for the elderly.
Acknowledgment
Supported by the Hollings Cancer Center Support Grant No. P30 CA138313 and by the Veterans Affairs Health Administration Health Services Research and Development Grant No. IIR 09-066. Presented at the 51st Annual Meeting of the American Society of Clinical Oncology, Chicago, IL, May 29-June 2, 2015, and at the 2015 Kunshan Forum, Kunshan, China.
Appendix
Table A1.
Results of Logistic Regression of Associations of Demographic and Other Variables With CRC Screening Adherence
| Variable | Regression Result by Model* | |||||||
|---|---|---|---|---|---|---|---|---|
| M1 (n = 187,372) | M2 (n = 29,366) | M3 (n = 39,543) | M4 (n = 3,516) | |||||
| OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | |
| Age, years | ||||||||
| 76-80 | Ref | Ref | n/a | n/a | ||||
| 81-85 | 0.74 | 0.72 to 0.77 | 0.69 | 0.65 to 0.74 | n/a | n/a | ||
| 86-90 | 0.46 | 0.45 to 0.48 | 0.52 | 0.47 to 0.57 | Ref | Ref | ||
| 91-95 | 0.24 | 0.22 to 0.26 | 0.44 | 0.35 to 0.54 | 0.52 | 0.47 to 0.57 | 0.79 | 0.63 to 1.01 |
| Race/ethnicity | ||||||||
| Non-Hispanic white | Ref | Ref | Ref | Ref | ||||
| Black | 0.61 | 0.57 to 0.65 | 1.32 | 1.13 to 1.55 | 0.56 | 0.46 to 0.68 | 2.34 | 1.43 to 3.81 |
| Other | 0.82 | 0.78 to 0.87 | 1.01 | 0.89 to 1.15 | 0.82 | 0.69 to 0.98 | 1.36 | 0.87 to 2.11 |
| Sex | ||||||||
| Female | Ref | Ref | Ref | Ref | ||||
| Male | 1.13 | 1.10 to 1.16 | 1.46 | 1.38 to 1.55 | 1.30 | 1.21 to 1.40 | 1.15 | 0.96 to 1.37 |
| Charlson comorbidity index | ||||||||
| 0 | Ref | Ref | Ref | Ref | ||||
| 1 | 1.06 | 1.01 to 1.12 | 1.19 | 1.07 to 1.33 | 1.11 | 0.98 to 1.25 | 1.62 | 1.21 to 2.16 |
| > 1 | 0.83 | 0.78 to 0.88 | 1.15 | 1.01 to 1.31 | 0.94 | 0.82 to 1.08 | 1.51 | 1.10 to 2.07 |
| Medicare state buy-in program entitlement | 0.37 | 0.34 to 0.39 | 0.78 | 0.68 to 0.90 | 0.39 | 0.33 to 0.46 | 0.89 | 0.59 to 1.35 |
| Rural/urban status | ||||||||
| Large metro | Ref | Ref | Ref | Ref | ||||
| Metro | 1.26 | 1.22 to 1.29 | 1.20 | 1.12 to 1.28 | 1.12 | 1.03 to 1.21 | 1.21 | 1.00 to 1.46 |
| Urban | 1.10 | 1.05 to 1.16 | 1.16 | 1.04 to 1.30 | 1.02 | 0.89 to 1.17 | 1.38 | 0.99 to 1.92 |
| Less urban/rural | 0.77 | 0.74 to 0.80 | 1.24 | 1.12 to 1.36 | 0.76 | 0.67 to 0.86 | 1.66 | 1.23 to 2.24 |
NOTE. Year dummies, not reported, were all statistically significant at 5%.
Abbreviations: CRC, colorectal cancer; n/a, not applicable; OR, odds ratio; Ref, reference cell.
M1 used the study sample that consisted of the 9-year cohort, and the dependent variable was the adherence status (1 if adherent or 0 otherwise). M2 used the subsample of M1 who were adherent, and the dependent variable was the status of adherence to colonoscopy (1 if colonoscopy or 0 if the other modalities). M3 used the subsample of M1 who were age 86 to 95 years, and the dependent variable was coded similarly to the one in M1. M4 used the subsample of M2 who were age 86 to 95 years, and the dependent variable was coded similarly to the one in M2.
AUTHOR CONTRIBUTIONS
Conception and design: John Bian, Charles Bennett, Gregory Cooper, Deborah Fisher, Joseph Lipscomb, Chao-Nan Qian
Administrative support: Alessandra D'Alfonso
Financial support: John Bian
Collection and assembly of data: John Bian
Data analysis and interpretation: John Bian, Alessandra D'Alfonso, Deborah Fisher, Joseph Lipscomb
Manuscript writing: All authors
Final approval of manuscript: All authors
AUTHORS' DISCLOSURES OF POTENTIAL CONFLICTS OF INTEREST
Assessing Colorectal Cancer Screening Adherence of Medicare Fee-for-Service Beneficiaries Age 76 to 95 Years
The following represents disclosure information provided by authors of this manuscript. All relationships are considered compensated. Relationships are self-held unless noted. I = Immediate Family Member, Inst = My Institution. Relationships may not relate to the subject matter of this manuscript. For more information about ASCO's conflict of interest policy, please refer to www.asco.org/rwc or jop.ascopubs.org/site/misc/ifc.xhtml.
John Bian
No relationship to disclose
Charles Bennett
No relationship to disclose
Gregory Cooper
No relationship to disclose
Alessandra D'Alfonso
No relationship to disclose
Deborah Fisher
No relationship to disclose
Joseph Lipscomb
No relationship to disclose
Chao-Nan Qian
No relationship to disclose
References
- 1.Pignone M Rich M Teutsch SM, etal: Screening for colorectal cancer in adults at average risk: A summary of the evidence for the US Preventive Services Task Force Ann Intern Med 137:132–141,2002 [DOI] [PubMed] [Google Scholar]
- 2.Whitlock EP Lin JS Liles E, etal: Screening for colorectal cancer: a targeted, updated systematic review for the US Preventive Services Task Force Ann Intern Med 149:638–658,2008 [DOI] [PubMed] [Google Scholar]
- 3.Gross CP Andersen MS Krumholz HM, etal: Relation between Medicare screening reimbursement and stage at diagnosis for older patients with colon cancer JAMA 296:2815–2822,2006 [DOI] [PubMed] [Google Scholar]
- 4.US Preventive Services Task Force : Screening for colorectal cancer: US Preventive Services Task Force recommendation statement Ann Intern Med 149:627–637,2008 [DOI] [PubMed] [Google Scholar]
- 5.Ko CW, Dominitz JA: Complications of colonoscopy: Magnitude and management Gastrointest Endosc Clin N Am 20:659–671,2010 [DOI] [PubMed] [Google Scholar]
- 6.Fisher DA, Judd L, Sanford NS: Inappropriate colorectal cancer screening: findings and implications Am J Gastroenterol 100:2526–2530,2005 [DOI] [PubMed] [Google Scholar]
- 7.Levin TR Zhao W Conell C, etal: Complications of colonoscopy in an integrated health care delivery system Ann Intern Med 145:880–886,2006 [DOI] [PubMed] [Google Scholar]
- 8.Warren JL Klabunde CN Mariotto AB, etal: Adverse events after outpatient colonoscopy in the Medicare population Ann Intern Med 150:849–857, W152,2009 [DOI] [PubMed] [Google Scholar]
- 9.Powell AA Saini SD Breitenstein MK, etal: Rates and correlates of potentially inappropriate colorectal cancer screening in the Veterans Health Administration J Gen Intern Med 30:732–741,2015 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Sheffield KM Han Y Kuo YF, etal: Potentially inappropriate screening colonoscopy in Medicare patients JAMA Intern Med 173:542–550,2013 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Walter LC Lindquist K Nugent S, etal: Impact of age and comorbidity on colorectal cancer screening among older veterans Ann Intern Med 150:465–473,2009 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Cooper GS, Koroukian SM: Geographic variation among Medicare beneficiaries in the use of colorectal carcinoma screening procedures Am J Gastroenterol 99:1544–1550,2004 [DOI] [PubMed] [Google Scholar]
- 13.Cooper GS, Doug Kou T: Underuse of colorectal cancer screening in a cohort of Medicare beneficiaries Cancer 112:293–299,2008 [DOI] [PubMed] [Google Scholar]
- 14.Schenck AP Peacock SC Klabunde CN, etal: Trends in colorectal cancer test use in the Medicare population, 1998-2005 Am J Prev Med 37:1–7,2009 [DOI] [PubMed] [Google Scholar]
- 15.Bian J Fisher DA Gillespie TW, etal: Using VA administrative data to measure colorectal cancer screening adherence among average-risk non-elderly veterans Health Serv Outcomes Res Methodol 10:165–177,2010 [Google Scholar]
- 16.Bian J Bennett CL Fisher DA, etal: Unintended consequences of health information technology: Evidence from Veterans Affairs colorectal cancer oncology watch intervention J Clin Oncol 30:3947–3952,2012 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Ko CW Dominitz JA Neradilek M, etal: Determination of colonoscopy indication from administrative claims data Med Care 52:e21–e29,2014 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Goodwin JS Singh A Reddy N, etal: Overuse of screening colonoscopy in the Medicare population Arch Intern Med 171:1335–1343,2011 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Schonberg MA Breslau ES Hamel MB, etal: Colon cancer screening in US adults age 65 and older according to life expectancy and age J Am Geriatr Soc 63:750–756,2015 [DOI] [PubMed] [Google Scholar]
- 20.Walter LC Davidowitz NP Heineken PA, etal: Pitfalls of converting practice guidelines into quality measures: Lessons learned from a VA performance measure JAMA 291:2466–2470,2004 [DOI] [PubMed] [Google Scholar]
- 21.Bian J, Halpern MT: Trends in outpatient breast cancer surgery among Medicare fee-for-service patients in the United States from 1993 to 2002 Chin J Cancer 30:197–203,2011 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Engels EA Pfeiffer RM Ricker W, etal: Use of surveillance, epidemiology, and end results–Medicare data to conduct case-control studies of cancer among the US elderly Am J Epidemiol 174:860–870,2011 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.El-Serag HB Petersen L Hampel H, etal: The use of screening colonoscopy for patients cared for by the Department of Veterans Affairs Arch Intern Med 166:2202–2208,2006 [DOI] [PubMed] [Google Scholar]
- 24.Charlson ME Pompei P Ales KL, etal: A new method of classifying prognostic comorbidity in longitudinal studies: Development and validation J Chronic Dis 40:373–383,1987 [DOI] [PubMed] [Google Scholar]
- 25.Huber PJ: The behavior of maximum likelihood estimates under nonstandard conditions Proceedings of the Fifth Berkeley Symposium on Mathematical Statistics and Probability 221–233,1967. Berkeley, CA: University of California Press [Google Scholar]
- 26.Shih YC, Zhao L, Elting LS: Does Medicare coverage of colonoscopy reduce racial/ethnic disparities in cancer screening among the elderly? Health Aff (Millwood) 25:1153–1162,2006 [DOI] [PubMed] [Google Scholar]
- 27.Swan J Breen N Coates RJ, etal: Progress in cancer screening practices in the United States: Results from the 2000 National Health Interview Survey Cancer 97:1528–1540,2003 [DOI] [PubMed] [Google Scholar]
- 28.Liang SY Phillips KA Nagamine M, etal: Rates and predictors of colorectal cancer screening Prev Chronic Dis 3:A117,2006 [PMC free article] [PubMed] [Google Scholar]
- 29.Phillips KA Liang SY Ladabaum U, etal: Trends in colonoscopy for colorectal cancer screening Med Care 45:160–167,2007 [DOI] [PubMed] [Google Scholar]
- 30.Semrad TJ Tancredi DJ Baldwin LM, etal: Geographic variation of racial/ethnic disparities in colorectal cancer testing among Medicare enrollees Cancer 117:1755–1763,2011 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Fenton JJ Tancredi DJ Green P, etal: Persistent racial and ethnic disparities in up-to-date colorectal cancer testing in Medicare enrollees J Am Geriatr Soc 57:412–418,2009 [DOI] [PubMed] [Google Scholar]
- 32.Ayanian JZ: Racial disparities in outcomes of colorectal cancer screening: Biology or barriers to optimal care? J Natl Cancer Inst 102:511–513,2010 [DOI] [PubMed] [Google Scholar]
- 33.Dolan NC Ferreira MR Fitzgibbon ML, etal: Colorectal cancer screening among African-American and white male veterans Am J Prev Med 28:479–482,2005 [DOI] [PubMed] [Google Scholar]