Abstract
Background
Around 63% of total health care expenditure in Bangladesh is mitigated through out of pocket payment (OOP). Heavy reliance on OOP at the time of care seeking poses great threat for financial impoverishment of the households. Households employ different strategies to cope with the associated financial hardship.
Objective
The aim of this paper is to understand the determinants of hardship financing in coping with OOP adopted for health care seeking of under five childhood illnesses in rural setting of Bangladesh.
Methods
A community based cross sectional survey was conducted during August to October, 2014 in 15 low performing sub-districts of northern and north-east regions of Bangladesh. Of the 7039 mothers of under five children surveyed, 1895 children who suffered from illness and sought care for their illness episodes were reported in this study. Descriptive statistics and ordinal regression analysis were conducted.
Results
A total number of 7,039 under five children reported to have suffered illness by their mothers. Among these children 37% suffered from priority illness. Care was sought for 88% children suffering from illnesses. Among them 26% went to a public or private sector medically trained provider. 5% of households incurred illness cost more than 10% of the household’s monthly expenditure. The need for assistance was higher among those compared to others (31% vs 13%). Different financing mechanisms adopted to meet OOP are loan with interest (6%), loan without interest (9%) and financial help from relatives (6%) Need for financial assistance varied from 19% among households in the lowest quintile to 9% in the highest wealth. Ordinal regression analysis revealed that burden of hardship financing increases by 2.17 times when care is sought from a private trained provider compared to care seeking from untrained provider (CI: 1.49, 3.17). Similarly, for families that incur a health care expenditure that is more than 10% of their total monthly expenditure (CI:1.46, 3.88), the probability of falling into more severe financial burden increases by 2.4 times. We also found severity of the hardship financing to be around half for households with monthly income of more than BDT 7500 (OR = 0.56, CI: 0.37, 0.86). The burden increased by 2.10 times for households with a deficit (CI: 1.53, 2.88) between their monthly income and expenditure. The interaction between family income and severity of illness showed to significantly affect the scale of hardship financing. Children suffering from priority illness belonging to poor households were found have two times (CI: 1.09, 3.47) higher risks of suffering from hardship financing.
Conclusion and policy implications
Findings from this study will help the policy makers to identify the target groups and thereby design effective health financing programs.
Background
Bangladesh has experienced a dramatic decline in under-five mortality in the last four decades [1] despite facing innumerable challenges and adversities. Apart from improved access to and use of health services, focus on women’s education and empowerment contributed to the reduction in child mortality [2]. Out of pocket payments are used as a means to complement government expenditure and financial protection in health care. Many households suffer financial hardship, or are even impoverished because their members pay from pocket at the time they receive health care [3]. Globally, an estimated 150 million people endure severe financial hardship and 100 million are pushed below poverty line each year as they need to use and pay for health care[3]. It is important to investigate whether households in Bangladesh suffer from financial hardship while paying for child health care services. Understanding OOP expenditure and the key factors driving the burden of borrowing & selling of asset can help policy makers recognize the intensity of the problem and adapt likely policy responses [4–5].
High OOP and low government spending characterize healthcare financing in Bangladesh. Per-capita total health spending in Bangladesh in 2012 was US$27 while households contribute almost 63% of total health care expenditure [6]. OOPs have shown an increasing trend in recent years. OOPs for child care occur frequently which are significant [7]. Sometimes these costs are sudden and unexpected [8]. More than 30 percent of people lived below the poverty line (i.e. below $PPP1.25 per person per day) in 2010 [9]. Fertility rate among the poor is higher while children from the poorer households are more prone to suffer from illness. Ensuring financial risk protection when seeking health care is key to achieving Universal Health Coverage. The Health, Population and Nutrition Sector Plan (HPNSP) 2017–2022 aims to achieve Universal Health Coverage (UHC) ensuring equity, quality and efficiency. Protecting households from financial catastrophe and impoverishment is a key to achieve UHC goal [10–11].
Heavy reliance on OOP poses financial burden on households and leads to different mechanisms to be adopted to mitigate necessary payment for healthcare for under-five child’s illness. Sometimes the coping strategies associated to OOP can be “impoverishing” if household is faced with welfare loss and pushed further to a lower wealth/income status. Coping mechanisms adopted based on the extent of financial burden and thus depends on the type of care sought, duration of illness and the level of facility utilized [7]. Private providers charge higher service fees than public providers for patients of all ages in low income countries [12–13]. Sometimes patients pay unofficial (‘under the table’) user fees at the public health facilities in many settings [14]. OOPs may differ in terms of chronic conditions of the patients and length of illness [15].
Many households in low income countries do not have access to any social health protection schemes and therefore rely on existing resources or borrow money or in worst possible scenario sell off their assets [15]. It is known that high OOP leads to high financial burden on families. However, it is critical to understand how this OOP is being mitigated and what are the triggering factors that drag households into hardship financing.
Coping mechanisms provide information on how households respond to OOPs and how these may affect their future welfare status [15]. Households adopt different strategies in the face of health expenditures [16–18]. These strategies include: use savings, sale of assets and livestock, borrow money from friends and family, take loan on interest, reduce expenditure on other basic needs including food and discontinue children study at schools. Households’ members arrange additional work to repay loan and to cover lost income [19–20]. There may be differences in the ability of households to cope with financial costs of illness. The burden of financial hardship may endanger vulnerable household livelihoods and push household members to poverty or reduced welfare [21–23].
Costs of illness that households must cover are sensitive to household income [24–27]. This association is even stronger in households of low-income countries with no social health protection mechanisms in place [28]. Households or parents with under-five children are at risk of going through financial hardship when paying for healthcare which may eventually lead to catastrophe. Although, many studies have looked at the level of households’ expenditures and cost of treating under-five children in developing country settings [29–32], there is almost no available information on factors that trigger decision on different strategies for mitigating the costs. There is very little information available on the how choice of public versus private health facilities can influence level of burden due to coping mechanisms for child health care services in developing countries. Impact of hardship financing for under-five children on household living status has received little attention in Bangladesh. This lack of knowledge is an impediment to policy formulation and implementation aimed at reducing the financial burden of child health illness. The current paper will add to this understanding by presenting empirical data to describe the factors affecting the decision to undertake different coping strategies for financing healthcare in the face of under-5 child illness. It will also shed light on what can possibly risk households to fall into deeper financial hardship as a result of the strategy adapted. It will also aide the government with useful information in designing evidence informed health financing scheme targeted to under five children.
Materials and methods
Study design and data
The data for this study were obtained from a large community based cross sectional survey conducted in 15 low performing sub districts of greater Mymensingh and northern regions of Bangladesh. This survey was carried out in 2014 as part of the baseline assessment of an integrated nutrition program of World Vision Bangladesh called “Nobokoli’. Nobokoli interventions cover areas of nutrition, water, sanitation hygiene and livelihood to address the underlying causes of undernutrition. The interventions are focused on the first 1,000 days of life from pregnancy till the child is 2 years of age. icddr,b is using a quasi-experimental study design to evaluate the impact of Nobokoli program. The survey covered villages from both intervention and comparison areas.
The survey collected a wide range of information on child health care practices such as feeding, nutritional status, morbidity, care seeking practices and it’s associated out of pocket expenditure (OOP), financing mechanisms adapted for incurring OOP and household sociodemographic indicators.
Sampling and sample size
The study followed a multistage clustered random sampling technique. At first, 15 sub districts were selected from the 20 Nobokoli intervention areas using probability proportionate to size (PPS) for optimal resource management. In the second stage, 140 clusters were randomly selected from both intervention & comparison areas by PPS where each village with a population of 1,000–1800 was defined as a cluster. Finally, 52 randomly selected mothers of under-five child were interviewed from each cluster. A total of 8,679 households were surveyed and 99.9% consented for the interview. Details of the baseline survey has been published elsewhere [33].
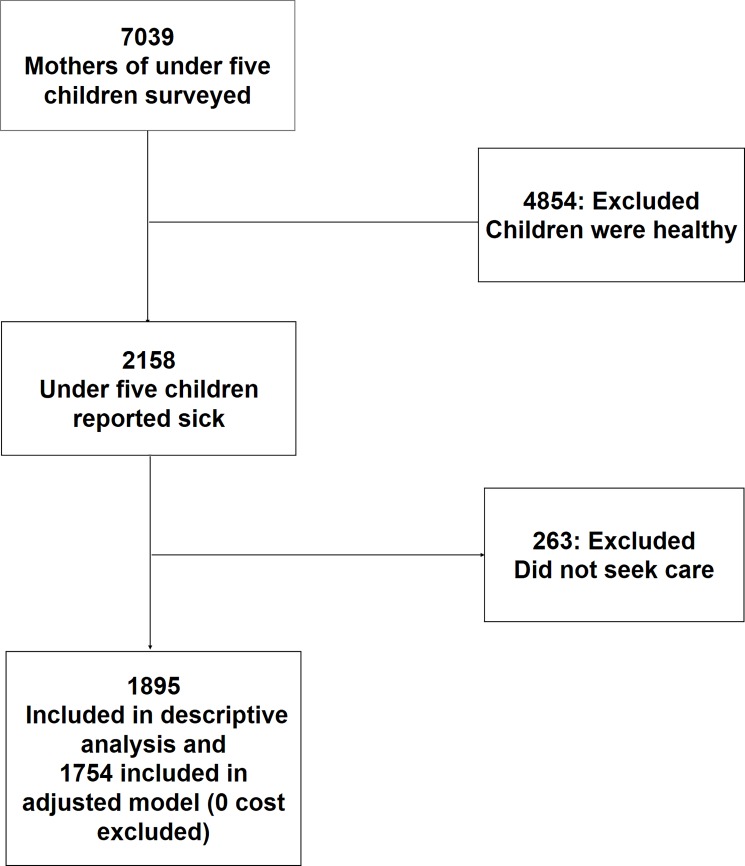
The survey covered 7039 mothers of under five children. Out of which 2158 children suffered from any sort of illnesses in the two weeks prior to survey. Our sample (n = 1895) for this paper includes the children who suffered from illnesses and sought care for their illness episodes (Fig 1)
Fig 1. Selection of sample for analysis.
Inclusion criteria: Children who suffered from illness within two weeks preceding the survey and sought care for their illness. The main objective was to explore the extent of hardship encountered in paying for healthcare expenses.
Exclusion criteria: Those who did not seek care for illness. Fig 1 details out the sample selection criteria.
Ethical consideration
The Ethics Review Board of icddr,b approved the study and the study followed the principles embodied in the Declaration of Helsinki. Informed written consent were taken from the respondents before starting the interview (PR14044).
Measurement process & quality assurance
A pretested structured validated questionnaire was administered to mothers of under-five children in national language, Bangla. The questionnaire primarily followed the Bangladesh Demographic and Health Survey 2014. This gave the opportunity to compare final outcome data with national trend. Questions on coping strategies were collected following a pre-used tool in a large community based cluster randomised trial involving more than 35,000 women (Shonjibon Trial #1026864). The tool was developed through expert consultation with health economists and administered on a large sample. Both tools have been validated in Bangla. Reference period for collected information on illness episodes of under-five children, care seeking, OOP and funding mechanisms were two weeks preceding the survey to minimize recall bias. All information collected are reported by mothers. Data collectors experienced in survey data collection was deployed for data collection after 10 days in house training and 2 days field practices. Two tiers of supervisors monitor data collection activity through regular spot checking. A separate quality assurance team conducted 5% of the re-interview to ensure data quality.
Variables
The dependent variable was an ordered variable “hardship financing” representing the burden of financing out-of-pocket payments [34–36]. Mothers were asked regarding the means the household had to undertake in the face of any out-of-pocket payments for care-seeking of under-five children over the preceding two weeks due to morbidity. They selected among regular income, savings, help from relatives/friends, loan without interest, loan with interest, sold assets/livestock’s/ personal belongings or mortgage of land or properties. These options were grouped together to create an ordinal scale based on the intensity of burden of financial hardship. Regular income and savings were grouped together considering these incur no burden for hardship financing while selling of assets/livestock’s/ personal belongings or mortgage of land or properties were grouped worst case scenario posing highest threat to household’s financial stability[35]. The scale of dependent variable ranges from 0–4 where 0 is “savings/regular income”, 1 is “took help from relative”, 2 is “took loan without interest”, 3 is “took loan with interest’ and 4 is “sold assets or mortgage lands”.
Explanatory variables include illness type, provider type, socio-economic characteristics of the household and mother’s background characteristics. Illnesses were categorized based on reported symptoms and severity of illness; priority illness (children who had pneumonia, diarrhoea with dehydration, dysentery, malaria, or measles) and non-priority illness (children who had a cough or cold, acute or chronic ear infection, diarrhoea with no dehydration, anaemia, or fever without malaria). This has been adapted from the Multi Country Evaluation (MCE) of Integrated Management of Childhood Illness (IMCI) [37]. Health care providers were classified into untrained health care providers (pharmacy, ayurveda, homeopath and traditional healer etc), public trained (trained provider working in the government health care facilities) and private trained (trained provider working in private health care facilities). Definition of trained and untrained was taken from Bangladesh Demographic and Health Survey 2014 (BDHS) [1]. Mother’s background characteristics include mother’s level of education and employment status. Information on OOP was collected in local currency (Bangladesh Taka) for up to three consecutive visits. OOP variable was constructed by aggregating the direct and indirect costs of care seeking for the patient and opportunity costs for their accompanying caregivers. Illness cost as percentage of total household expenditure was calculated as a proportion of OOP to total monthly expenditure of the household.
Household socio-economic characteristics include monthly income of the household, balance between households last month’s income and expenditure and households wealth status. Household income was collected for preceding one year while expenditure information was collected for the preceding one month. Mother’s overall opinion regarding balance between household income and expenditure was recorded as equal income and expenditure, savings and deficit. Household wealth status was determined by ownership of household durable goods, dwelling characteristics, source of drinking water, sanitation facility, possession of land and domestic animals using principle component analysis. Wealth status was stratified into five quintiles where ‘one’ represented the poorest and ‘five’ represented the richest. Mother’s education was classified as no education, primary incomplete (1–5 years of education) and primary and above (6+ years of education). Mother’s occupation was classified into unemployment, unskilled and skilled employment.
Statistical analysis
We used Stata 13.0 Special Edition software (StataCorp. 2013. Stata Statistical Software: Release 13. College Station, TX: StataCorp LP) for data analysis. Percent distribution of different sources of financial mechanisms were examined by explanatory variables The next stage of analysis explored the proportion of households who failed to meet OOP for health care and had to seek financial assistance from external sources. Going further down, we looked at details on how the costs incurred for care-seeking were paid by the families and the severity of financial hardship in terms of foregone future income of households. Finally, we developed an ordered scale for measurement of financial hardship for OOP in terms of possible loss in future income. Sale of asset that can bring people down to a lower wealth quintile have been considered to be the most severe consequence followed by loan with interest, loan without interest and loan from relatives. For the categorical explanatory variables, dummy variables were created for regression analysis. Multivariable ordered logistic regression was used to explore the determinants of hardship financing for OOP and the analysis unit was households. Only households that reported care seeking for illnesses of their under five children in the last week of survey data collection were included in the regression model. Explanatory variables found significant in the bivariate analysis were put into the multivariable model. Interaction of the explanatory variables were examined. The basic assumptions of modelling were tested and met. Covariates of risk for hardship financing were reported using odd ratios.
Results
From the survey, we gathered reports for a total number of 7,039 under five children from their mothers. Around 51% of these mothers had completed at least primary level and more than 12% completed secondary education while 90% were unemployed. The households were equally distributed across wealth quintiles. Median monthly income was Bangladesh Taka (BDT) 7525 Inter Quartile Range (IQR) (5666–11250)_with 32% households having deficit after bearing all expenses.
Among these children, 31% suffered from some illness over the two weeks preceding the survey and 37% of them were suffering from priority illness while the rest were suffering from non-priority illness. Care was sought for 88% children suffering from illnesses. Among them 26% went to a public or private sector medically trained providers (Table 1). Median out of pocket expenditure for care seeking of under five children was 150 (IQR_70–270) BDT. Only 5% households incurred illness cost more than 10% of household’s monthly expenditure.
Table 1. Background characteristics of the households having under five children in the rural areas of Bangladesh 2014.
| Background characteristics | n = 7039 | Percentage (%) | |
|---|---|---|---|
| Mother’s Education | No education (0 years) | 1,343 | 19.1 |
| Primary incomplete (1–4 years) | 1,257 | 17.9 | |
| Primary complete to secondary incomplete(5–9 years) | 3,571 | 50.7 | |
| Secondary complete or higher (10+ years) | 868 | 12.3 | |
| Mother’s Employment Status | Unemployed | 6,359 | 90.3 |
| Unskilled worker | 238 | 3.4 | |
| Skilled worker | 442 | 6.3 | |
| Monthly total household income (in taka) | Median (IQR) | 7,003 | 7525 (5666–11250) |
| Savings status of household after all expenses | Both income and expenditure equal | 3,522 | 50.0 |
| Savings | 1,238 | 17.6 | |
| Deficit | 2,279 | 32.4 | |
| Wealth Quintile | Lowest | 1,446 | 20.5 |
| Second | 1,392 | 19.8 | |
| Middle | 1,438 | 20.4 | |
| Fourth | 1,393 | 19.8 | |
| Highest | 1,370 | 19.5 | |
| Last two week morbidity among under-five children | Any illness | 2158 | 30.7 |
| Type of illnesses (n = 2158) | Nonpriority illness | 1,353 | 62.7 |
| Priority illness | 805 | 37.3 | |
| Care-seeking for illnesses among under-five children (n = 2158) | Care-seeking from any provider | 1895 | 87.8 |
| Type of provider* (n = 1895) | Untrained provider | 1,394 | 73.6 |
| Trained public provider | 235 | 12.4 | |
| Trained private provider | 265 | 13.98 | |
| Out of Pocket Expenditure | Median (IQR) | 1895 | 150(70–270) BDT |
| Illness cost as percentage share of total household’s monthly expenditure(n = 1895)** | 0–10 | 1788 | 94.6 |
| >10 | 101 | 5.4 | |
*1 provider missing
**6 cost information missing
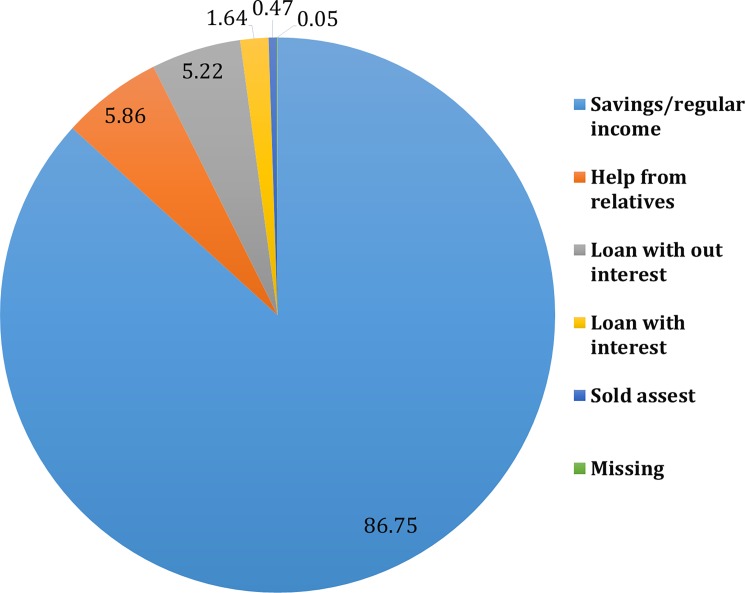
In our study area, more than 13% of the households needed external financial assistance for meeting health care expenditure for care-seeking of children under five years of age. Eighty seven percent of the families who sought care for illness were able to pay from income or savings while 6% took loan from relatives. Five percent had to seek loan without interest while 2% took loan with interest and half a percentage of households had to sell their assets (Fig 2).
Fig 2. Distribution of different financing mechanisms for care seeking for under five children.
Children of families who suffered from a priority illness needed more financial support (16%) from external sources compared to those having non-priority illness (12%). Mothers with secondary or higher level of education took less amount of loan compared to those without any education (1% vs 9%). Among children who were ill and for whom care was sought from trained private health care providers, nearly 6% families took loan with interest, more than 9% took loan without interest and 6% received financial help from their relatives. These rates were higher compared to those who sought care from trained public providers or untrained providers (Table 2).
Table 2. The percentage of different financing mechanisms adopted to meet OOP of care seeking for illnesses of under five children by type of illnesses, type of provider and background characteristics, in Bangladesh 2014.
| Number of under-five children who sought care | Different mechanisms for financing OOP | ||||||
|---|---|---|---|---|---|---|---|
| % Savings/ households monthly income | % took help from relatives |
% took loan without interest | % took loan with interest |
% mortgaged or sold assets/land |
|||
| Overall | 1895 | 86.8 | 5.9 | 5.2 | 1.6 | 0.5 | |
| Type of illnesses | Non-priority illness | 1157 | 88.4 | 5.2 | 4.5 | 1.3 | 0.5 |
| Priority illness | 738 | 84.2 | 6.9 | 6.4 | 2.2 | 0.4 | |
| Type of provider | Untrained provider | 1394 | 88.5 | 5.7 | 4.5 | 0.8 | 0.5 |
| Public trained provider | 235 | 85.1 | 6.8 | 5.5 | 1.7 | 0.9 | |
| Private trained provider | 265 | 78.9 | 6.0 | 8.7 | 6.0 | 0.0 | |
| Illness cost as percentage share of total household expenditure * | 0–10 | 1788 | 87.7 | 5.7 | 5.0 | 1.1 | 0.5 |
| >10 | 101 | 69.3 | 9.9 | 8.9 | 11.9 | 0.0 | |
| Mother’s Education | No education (0 years) | 339 | 82.9 | 5.3 | 9.1 | 1.8 | 0.9 |
| Primary incomplete (1–4 years) | 348 | 83.9 | 7.8 | 5.5 | 2.0 | 0.9 | |
| Primary complete to secondary incomplete (5–9 years) | 976 | 87.4 | 5.6 | 4.7 | 1.8 | 0.3 | |
| Secondary complete or higher (10+ years) | 232 | 94.0 | 4.7 | 1.3 | 0.0 | 0.0 | |
| Mother’s Employment Status | Unemployed | 1708 | 86.7 | 5.8 | 5.4 | 1.7 | 0.5 |
| Unskilled worker | 58 | 77.6 | 8.6 | 10.3 | 0.0 | 1.7 | |
| Skilled worker | 129 | 92.3 | 5.4 | 0.8 | 1.6 | 0.0 | |
| Monthly total household income (in taka)** | ≤7500 | 969 | 83.8 | 5.9 | 7.2 | 2.5 | 0.6 |
| >7500 | 918 | 89.9 | 5.8 | 3.2 | 0.8 | 0.3 | |
| Savings status after all expenses | Both income and expenditure equal | 853 | 90.5 | 4.8 | 4.0 | 0.5 | 0.2 |
| Savings | 308 | 91.2 | 5.5 | 1.6 | 1.0 | 0.3 | |
| Deficit | 734 | 80.5 | 7.2 | 8.2 | 3.3 | 0.8 | |
| Wealth Quintile | Lowest | 396 | 81.3 | 6.1 | 10.1 | 2.0 | 0.5 |
| Second | 378 | 86.0 | 6.1 | 4.0 | 2.7 | 1.3 | |
| Middle | 405 | 87.7 | 5.4 | 5.7 | 1.2 | 0.0 | |
| Fourth | 385 | 88.1 | 6.0 | 4.4 | 1.0 | 0.5 | |
| Highest | 331 | 91.5 | 5.7 | 1.2 | 1.2 | 0.0 | |
*6 missing
**8 missing
For families that incurred OOP more than 10% of total monthly household expenditure, need for financial assistance was higher compared to that the others (31% vs 13% respectively). The proportion of families who took loan with interest was as high as 12% for those who spent more than 10% of their average monthly expenditure for health care compared to those who spent less than or equal to 10% (1%). Financial burden of health care seeking was lower among mothers who completed at least primary education compared to women with less than primary or no education (11% vs 16% vs 17%). Mothers of sick children who were skilled workers faced lower risk of financial hardship compared to those who were unskilled workers or unemployed (8% vs 22% vs 13%). Households with income of less than BDT 7500 needed more external financial support compared to households with income above this threshold (16% vs 10%), major share of this difference being driven by loan without interest (7% vs 3%). Similarly, households with a monthly deficit after meeting all expenditures face the need for financial assistance (19%) for health care payments than families that end up having some savings (9%). Need for financial assistance varied from 19% among households in the lowest quintile to 9% in the highest wealth quintile. The difference has mostly been driven by the proportion of households taking loan without interest from an external source (Table 2).
Our multivariable ordered logistic regression shows that burden of hardship financing increases by 2.09 times when care is sought from a private trained provider compared to care seeking from untrained provider. Similarly, for families that incur a health care expenditure that is more than 10% of their total monthly expenditure, the probability of falling into more severe debt burden increases by 2.4 times. We also found severity of hardship financing to be around 45% lower for households with monthly income of more than BDT 7500. Mothers who had at least secondary education were less prone (one third) to be faced with hardship compared to mothers with no education. The burden increased by 2.07 times for households with a deficit between their monthly income and expenditure. The interaction between family income and severity of illness showed to significantly affect the scale of hardship financing. Children suffering from priority illness belonging to poor households was found have two times higher risks of suffering from hardship financing (Table 3).
Table 3. Determinants of need for hardship financing to meet OOP for care seeking of illnesses among under-five children in Bangladesh 2014.
| Hardship financing to meet OOP | |||||
|---|---|---|---|---|---|
| Unadjusted odd ratios (95% CI) | P value | Adjusted odd ratios (95% CI) | P value | ||
| Type of illnesses | Non priority illness | Ref | Ref | ||
| Priority illness | 1.43 (1.10,1.87) | <0.05 | 0.95 (0.66, 1.37) | 0.78 | |
| Type of provider | Untrained provider | Ref | Ref | ||
| Trained public provider | 1.36 (0.92,2.01) | 0.13 | 1.99 (1.29, 3.06) | <0.05 | |
| Trained private provider | 2.18 (1.56,3.06) | <0.000 | 2.17 (1.49, 3.17) | <0.000 | |
| Illness cost as percentage share of total household expenditure (N = 1763) | 0–10 | Ref | Ref | ||
| >10 | 3.23 (2.07,5.03) | <0.000 | 2.38(1.46, 3.88) | <0.000 | |
| Mother’s Education | No education (0 years) | Ref | Ref | ||
| Primary incomplete (1–4 years) | 0.91 (0.61,1.35) | 0.63 | 1.07 (0.70, 1.64) | 0.75 | |
| Primary complete to secondary incomplete (5-9years) | 0.68 (0.49,0.96) | <0.05 | 0.84 (0.58, 1.22) | 0.36 | |
| Secondary complete or higher (10+ years) | 0.30 (0.16, 0.55) | <0.000 | 0.39 (0.20, 0.78) | <0.05 | |
| Mother’s Employment Status | Unemployed | Ref | Ref | ||
| Unskilled worker | 1.89 (1.01, 3.55) | <0.05 | 1.61 (0.82, 3.14) | 0.17 | |
| Skilled worker | 0.54 (0.28, 1.04) | 0.06 | 0.61 (0.31, 1.21) | 0.16 | |
| Monthly total household income (in taka) | ≤7500 | Ref | Ref | ||
| >7500 | 0.57 (0.43, 0.75) | <0.000 | 0.56 (0.37, 0.86) | <0.05 | |
| Savings status after all expenses | Both income and expenditure equal | Ref | Ref | ||
| Savings | 0.91 (0.58, 1.44) | 0.70 | 1.08 (0.66, 1.77) | 0.75 | |
| Deficit | 2.37 (1.77, 3.17) | <0.000 | 2.10 (1.53, 2.88) | <0.000 | |
| Wealth Quintile | Lowest | Ref | Ref | ||
| Second | 0.71 (0.48, 1.04) | <0.05 | 0.82 (0.54, 1.22) | 0.33 | |
| Middle | 0.60 (0.41, 0.89) | <0.05 | 0.76 (0.50, 1.15) | 0.20 | |
| Fourth | 0.58 (0.39, 0.86) | <0.05 | 0.90 (0.58, 1.39) | 0.62 | |
| Highest | 0.39 (0.25, 0.62) | <0.000 | 0.73 (0.42, 1.27) | 0.26 | |
| Interaction of illness type & monthly household income category | 2.19 (1.25,3.81) | <0.05 | 1.94 (1.09, 3.47) | <0.05 | |
Discussion
Our analysis found that financial help from relatives, loan with or without interest and sale of assets were the commonly adopted coping mechanisms to mitigate medical expenses. Severity of financial consequences resulting into hardship increased when care was sought from private health care providers orchildren had priority illness episodes or belonged to an economically less solvent household and when illness cost exceeded 10% of the household’s monthly expenditure. Socio-demographic factor like economic status, level of education and employment status also influenced choice of coping with health care payments. Families seeking care from private trained providers were more likely to face difficult consequences of bearing these payments.
The study is unique in its focus on the coping strategies and predictors of hardship financing mechanisms for childhood illnesses in two weeks prior to the survey at three levels (illness episode, individual and household level) in Bangladesh. Other studies that explored disease specific coping mechanisms for bearing treatment cost with specific focus on childhood pneumonia, tuberculosis, obstetric care or household level OOP, mostly focused at individual or household level determinants [34–36,38–40]. Little attention has been paid to the predictors of hardship financing mechanisms for childhood illnesses.
One limitation in our analysis is that we captured direct OOP for childhood illnesses which may under represent the actual burden as indirect cost of care seeking was not included in the analysis. Since we primarily aimed to understand the financing mechanisms of direct payments, the results would be less likely to be influenced by indirect costs. Missed opportunity of care seeking might be due to financial constraints. People due to poverty overlook or are incapable of recognizing the need for care due to economic barrier or access [41]. Yet our analysis sheds some light on possible characteristics of those who sought care and faced financial hardship to cope with high out of pocket payment for health care. Such valuable piece of information can lead to possible recommendations for improving care seeking through removal of barriers to finance treatment of childhood illnesses. Our data is also limited to detect any change in lifestyle which may have been a case for households that managed to pay from savings or regular income. Dropping out of school or food insecurity could be results of such borrowing that has not been captured in this analysis.
Financial help from relatives, loan with or without interest and selling assets were among the primary mechanisms adopted to mitigate the medical expenses. In low income countries the common trend indicates that more households in the poorest quintile sell assets or borrow money as opposed to the highest wealth quintile [15]. A study based in Indonesia explored both the direct and indirect costs of health shocks and found that through consumption smoothing, households can self-insure around two thirds of the effects of small health shocks [42]. Borrowing is a common technique of smoothing over expenditure consequences of health shocks. Borrowing money from relatives is safer and poses less risk as it is interest free while borrowing from traditional money lenders with high rates of interest can have detrimental effect on future consumption of households [36–40, 43]. When such facilities have been exhausted or not available, people tend to sell assets as a last resort. Availability of microcredit schemes may encourage the poor to borrow when needed. NGOs providing microcredit have gained a high level of trust in Bangladesh. Some of these organizations are providing micro-insurance programs for health linked to microloans and reliant on the group dynamics of microcredit [44]. However, while these programs are able to smoothen consumption in the short run, it does affect future consumption and welfare loss in the long run. In case of acute disease or failure in repayment, families can face more profound catastrophe with long term consequences.
Better preventive mechanisms focusing on child health and nutrition needs to be undertaken at scale. Studies identified stunting to be more prevalent among children in poorer households. Undernutrition poses a higher risk of disease among children leading to higher health care expenditure and therefore higher chance of households facing financial catastrophe. These children are likely to be trapped into a vicious cycle of poor health and poverty leading to lower productivity over the life course [45]. Introduction of social protection schemes such as cash transfer programs are proven to be successful in reducing under nutrition and improving welfare [46].
As a protection and curative platform, pre-payment systems for health financing such as a mandatory health insurance system could be introduced in order to protect vulnerable groups from the impoverishing effects of health care expenditure. Particular focus needs to be given on the poor, especially children when designing such scheme. A decentralised system of the government through devolved funds would reduce possible consequences to be faced by the children over their life-course. However, the constraints on the expansion of health insurance to uncovered groups, such as the informally employed or the poorest, must be considered. The potential role of private sector providers and insurers in expanding access to care can also be explored.
There needs to be availability of high quality services for management of childhood illnesses through the public sector to make the financing schemes successful. Studies suggest that inaccessibility to public health care facilities, poor availability of medicines and equipment, and perceptions of lower quality diagnosis and treatment drive people away from low cost public facilities. This either increases the use of expensive private sector care where families end up incurring higher out of pocket payment or increase use of untrained informal care providers [47–52]. Our findings also interestingly suggests that households are faced with worse financial conditions when choosing a private health care provider. This clearly indicates, with availability of quality and cheaper or free health care services, households are likely to move to the public sector. Improved overall perceptions of public health care service delivery would lead to less risk of potentially catastrophic health care spending and less likely use of negative coping strategies.
In Bangladesh, 63% of Total Health Expenditure (THE) is paid directly from pocket by individuals [6]. This situation is much worse in rural area where THE from public sources is even lower. Over reliance on OOP for health care is regressive and inequitable in nature. Our disaggregated analysis and other reports indicates persistent inequality in health care payments and absence of an equitable financing mechanism. The burden of managing resources to finance health care increases with declining household income. The Maternal Health Vouchers Scheme has been able to improve facility delivery significantly while reducing OOP [53–57]. However, serious concerns were raised regarding the program’s allocative efficiency and service quality. One social protection scheme “Shasthyo Suroksha Karmasuchi (SSK)”that is currently being piloted has its focus limited to people living below poverty line. The scheme is yet to be evaluated, refined and scaled up bringing those above the poverty under its umbrella and making the program sustainable. In line with this effort, scope of health insurance targeted for priority childhood illnesses are needed to be tested to prevent households from falling into financial catastrophe. Again, improvement in service quality is also essential to make these protection schemes successful. Both service quality and financial protection are two key components for achieving UHC which has been repeatedly emphasised in the National Health, Population and Nutrition Sector Plan [58]. The Health Care Financing Strategy 2012–2032 also emphasizes on ensuring financial protection for those in need and make efficient use of resources [59]. One or multiple well designed and well targeted financial protection schemes together needs to be tested and scaled up for protection against catastrophe specially among children. Our findings can feed information for better program design and implementation and ensure better resource utilization.
Conclusion
Over-reliance on direct payments at the time people need care is one key barrier to achieve universal health coverage. Evidence on OOP for care seeking of illnesses among under five children and financing mechanism to mitigate these OOP are essential for designing effective interventions to ensure universal health coverage. There are ample evidence that introduction of health insurance decreased OOP in India, Thailand, Viet men, Rwanda etc[60–61]. Aligned with global effort, the health financing strategy of Bangladesh emphasizes on ensuring an equitable payment mechanism for health care [59]. Findings from this study will help the policy makers to identify the target groups and thereby design effective health financing programs.
Supporting information
Total observation of this dataset is 7,039. The variable name started with “q” provides the morbidity information of under-five children; “r” presents the child illness cost. The variable name started with “c” and “d” refers to the information of household characteristics and respondent background respectively.
(DTA)
Acknowledgments
We would like to thank our field team and data management team for their continuous support in survey data collection, data entry and cleaning. We are grateful to the mothers of under five children for their participation in this study. Special thanks to Civil Surgeons of the respective areas for issuing the letter that facilitates our access to the field site.
Data Availability
Dataset for the paper has been uploaded as a supporting information file.
Funding Statement
The paper is an output from data collected during baseline survey for evaluation of Nobokoli project funded by the World Vision Bangladesh. The funding was received by TT and SEA from icddr,b and the protocol was approved by the Internal Review Board of icddr,b. The Grant number for this protocol is GR-01194. The funders provided information on the intervention design and provided the list of areas where intervention was going to be delivered. They are aware of the manuscript and have reviewed the manuscript as co-authors.
References
- 1.National Institute of Population Research and Training (NIPORT), Mitra and Associates, and ICF International. Bangladesh Demographic and Health Survey 2014. Dhaka, Bangladesh, and Rockville, Maryland, USA: NIPORT, Mitra and Associates, and ICF International; 2016. [Google Scholar]
- 2.Arifeen SE, Hill K, Ahsan KZ, Jamil K, Nahar Q, Streatfield PK. Maternal mortality in Bangladesh: a countdown to 2015 country case study. The Lancet. 2014; 384(9951): 1366–74. [DOI] [PubMed] [Google Scholar]
- 3.WHO. The World Health Report–Health systems financing: the path to universal coverage. Geneva: World Health Organization; 2010. Available from: http://apps.who.int/iris/bitstream/10665/44371/1/9789241564021_eng.pdf [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Russell S. Illuminating cases: understanding the economic burden of illness through case study household research. Health policy and planning. 2005; 20(5):277–89. doi: 10.1093/heapol/czi035 [DOI] [PubMed] [Google Scholar]
- 5.Xu K, Evans DB, Carrin G, Aguilar-Rivera AM, Musgrove P, Evans T. Protecting households from catastrophic health spending. Health Affairs. 2007; 26, 972–983. doi: 10.1377/hlthaff.26.4.972 [DOI] [PubMed] [Google Scholar]
- 6.MOHFW (Ministry of Health and Family Welfare). Bangladesh National Health Accounts 1997–2012. Dhaka: Health Economics Unit, Ministry of Health and Family Welfare, Government of the People’s Republic of Bangladesh; 2015. [Google Scholar]
- 7.Tahsina T, Ali NB, Hoque DME, Huda TM, Salam SS, Hasan MM, et al. Out-of-pocket expenditure for seeking health care for sick children younger than 5 years of age in Bangladesh: findings from cross-sectional surveys, 2009 and 2012. Journal of health, population, and nutrition. 2017; 36(1):33 doi: 10.1186/s41043-017-0110-4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Bonu S, Bhushan I, Rani M, Anderson I. Incidence and Correlates of ‘Catastrophic’ Maternal Health Care Expenditure in India. Health Policy and Planning. 2009; 24 (6). pp. 445–456. doi: 10.1093/heapol/czp032 [DOI] [PubMed] [Google Scholar]
- 9.World Bank Group. South Asia region. Bangladesh More and Better Jobs to Accelerate Shared Growth and End Extreme Poverty. A Systematic Country Diagnostic. 2015.
- 10.World Health Organization. Chapter 2: How well do health systems perform? In: The World Health Report 2000—Health systems: improving performance. Geneva: WHO; 2000; p. 21–46. [Google Scholar]
- 11.Xu K, Evans DB, Kawabata K, Zeramdini R, Klavus J, Murray CJL. Household catastrophic health expenditure: a multicountry analysis. Lancet. 2003; 362: 111–7. doi: 10.1016/S0140-6736(03)13861-5 [DOI] [PubMed] [Google Scholar]
- 12.Hussein AK, Mujinja PG. Impact of user charges on government health facilities in Tanzania. East African Medical Journal. 1997; 74: 751–7. [PubMed] [Google Scholar]
- 13.Hotchkiss DR, Gordillo A. Household health expenditures in Morocco: implications for health care reform. International Journal of Health Planning and Management. 1999; 14: 201–17. doi: 10.1002/(SICI)1099-1751(199907/09)14:3<201::AID-HPM547>3.0.CO;2-H [DOI] [PubMed] [Google Scholar]
- 14.Bellii P, Godsadze G, Shahriari H. Out-of-pocket and informal payments in health sector: evidence from Georgia. Health Policy. 2004; 70: 109–23. doi: 10.1016/j.healthpol.2004.03.007 [DOI] [PubMed] [Google Scholar]
- 15.Leive A, Xu K. Coping with out-of-pocket health payments: empirical evidence from 15 African countries. Bulletin of World Health Organization. 2008; 86(11), pp 849–856. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Russell S. Ability to pay for health care: concepts and evidence. Health Policy Plan. 1996; 11:219–37. doi: 10.1093/heapol/11.3.219 [DOI] [PubMed] [Google Scholar]
- 17.McIntyre D, Thiede M, Dahlgren G, Whitehead M. What are the economic consequences for households of illness and of paying for health care in low- and middle-income country contexts? Soc Sci Med. 2006; 62:858–65. doi: 10.1016/j.socscimed.2005.07.001 [DOI] [PubMed] [Google Scholar]
- 18.Peters D, Yazbeck A, Sharmaand R, Ramana G, Pritchett L, Wagstaff A. Better health systems for India’s poor. Washington, DC: The World Bank; 2001. [Google Scholar]
- 19.Sauerborn R, Adams A, Hien M. Household strategies to cope with the economic costs of illness. Soc Sci Med. 1996; 43:291–301. doi: 10.1016/0277-9536(95)00375-4 . [DOI] [PubMed] [Google Scholar]
- 20.Kabir M, Rahman A, Salway M, Pryer J. Sickness among the urban poor: A barrier to livelihood security. J Int Dev. 2000; 12:707–22. doi: 10.1002/1099-1328(200007)12:5<707::AID-JID703>3.0.CO;2-G [Google Scholar]
- 21.Kipp W, Matukala T, Laing L, Jhangri G. Care burden and self-reported health status of informal women care givers of HIV/AIDS patients in Kinshasa, Demographic Republic of Congo, Aids Care. 2006; 18(7), 694–697. [DOI] [PubMed] [Google Scholar]
- 22.Ngalula J, Urassa M, Mwaluko G, Isingo R, Boerma JT. Health service use and hospital expenditure during terminal illness due to AIDS in rural Tanzania. Tropical Medicine and International Health. 2002; 7(10), 873–877. [DOI] [PubMed] [Google Scholar]
- 23.Piot P, Greener R, Russel S. Squarring the circle. AIDS, poverty, and human development. Plos Medicine. 2007; 4(10), 1571–1575. doi: 10.1371/journal.pmed.0040314 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Musgrove P. Family health care spending in Latin America. J Health Econ. 1983; 2(3):245–57. [DOI] [PubMed] [Google Scholar]
- 25.Parker SW, Wong R. Household income and health care expenditures in Mexico. Health Policy. 1997; 40(3):237–55. [DOI] [PubMed] [Google Scholar]
- 26.Rous JJ, Hotchkiss DR. Estimation of the determinants of household health care expenditures in Nepal with controls for endogenous illness and provider choice. Health Econ. 2003; 12(6):431–51. doi: 10.1002/hec.727 [DOI] [PubMed] [Google Scholar]
- 27.Malik AM, Syed S. 2012. Socio-economic determinants of household out-of-pocket payments on healthcare in Pakistan. Int J Equity Health 11:51 doi: 10.1186/1475-9276-11-51 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Parker SW, Wong R. Household income and health care expenditures in Mexico. Health Policy. 1997; 40(3):237–55. [DOI] [PubMed] [Google Scholar]
- 29.Galbraith A, Wong S, Kim S, Newacheck P. Out-of-pocket financial burden for low-income families with children: Socioeconomic dispartities and effects of insurance. Health services Research. 2005; 40(6), pp1722–1736. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Orem J, Mugisha F, Okui A, Musango L, Kirigia J. Health care seeking patterns and determinants of out-of-pocket expenditure for malaria for the children under-five in Uganda. Malaria Journal. 2013; 12:175 doi: 10.1186/1475-2875-12-175 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Manzi F, Armstrong Schellenberg JR, Adam T, Mshinda H, Victora C, Bryce J. Out-of-pocket payments for under-five health care in rural southern Tanzania. . 2005; 20 (suppl 1): i85–i93. [DOI] [PubMed] [Google Scholar]
- 32.Silva M, Barros A, Bertoldi A, Jacinto P, Matijasevich A, Santos I, Tejda C. Determinants of out-of-pocket health expenditure on children: an analysis of 2004 Pelotas Birth Cohort. . 2015; 14:53 doi: 10.1186/s12939-015-0180-0 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Tahsina T, Ali NB, Islam S, Hasan MM, Moinuddin M, Siddique AB, et al. Evaluation of Bangladesh Nutrition Initiative Project/Nobokoli: Findings from Baseline Survey, 2014. Division of Maternal & child Health, icddrb, Dhaka. 2015. Available from: www.icddrb.org [Google Scholar]
- 34.Alamgir NI, Naheed A, Luby SP. Coping strategies for financial burdens in families with childhood pneumonia in Bangladesh. BMC public health. 2010;10:622 doi: 10.1186/1471-2458-10-622 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Rahman MM, Gilmour S, Saito E, Sultana P, Shibuya K. Self-reported illness and household strategies for coping with health-care payments in Bangladesh. Bulletin of the World Health Organization. 2013;91(6):449–58. doi: 10.2471/BLT.12.115428 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Bhuiyan MU, Luby SP, Alamgir NI, Homaira N, Mamun AA, Khan JA, et al. Economic burden of influenza-associated hospitalizations and outpatient visits in Bangladesh during 2010. Influenza and other respiratory viruses. 2014;8(4):406–13. doi: 10.1111/irv.12254 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Arifeen SE, Hoque DE, Akter T, Rahman M, Hoque ME, Begum K, et al. Effect of the Integrated Management of Childhood Illness strategy on childhood mortality and nutrition in a rural area in Bangladesh: a cluster randomised trial. The Lancet. 2009;374(9687):393–403 [DOI] [PubMed] [Google Scholar]
- 38.Haque MA, Budi A, Azam Malik A, Suzanne Yamamoto S, Louis VR, Sauerborn R. Health coping strategies of the people vulnerable to climate change in a resource-poor rural setting in Bangladesh. BMC public health. 2013;13:565 doi: 10.1186/1471-2458-13-565 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Hoque ME, Dasgupta SK, Naznin E, Al Mamun A. Household coping strategies for delivery and related healthcare cost: findings from rural Bangladesh. Tropical medicine & international health: TM & IH. 2015;20(10):1368–75. [DOI] [PubMed] [Google Scholar]
- 40.Rahman MM, Gilmour S, Saito E, Sultana P, Shibuya K. Health-related financial catastrophe, inequality and chronic illness in Bangladesh. PloS one. 2013;8(2):e56873 doi: 10.1371/journal.pone.0056873 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.McIntyre D, Thiede M, Dahlgren G, Whitehead M. What are the economic consequences for households of illness and of paying for health care in low- and middle-income country contexts? Social science & medicine (1982). 2006;62(4):858–65. [DOI] [PubMed] [Google Scholar]
- 42.Schroders J, Wall S, Hakimi M, Dewi FST, Weinehall L, Nichter M, et al. How is Indonesia coping with its epidemic of chronic noncommunicable diseases? A systematic review with meta-analysis. PloS one. 2017;12(6):e0179186 doi: 10.1371/journal.pone.0179186 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Nguyen KT, Khuat OT, Ma S, Pham DC, Khuat GT, Ruger JP. Coping with health care expenses among poor households: evidence from a rural commune in Vietnam. Social science & medicine (1982). 2012;74(5):724–33 [DOI] [PubMed] [Google Scholar]
- 44.Werner Wendy J. "Micro-insurance in Bangladesh: Risk protection for the poor?." Journal of Health, Population and Nutrition (2009): 563–573. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Huda TM, Hayes A, El Arifeen S, Dibley MJ. Social determinants of inequalities in child undernutrition in Bangladesh: A decomposition analysis. Maternal & child nutrition. 2017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Lagarde M., Haines A., and Palmer N., The impact of conditional cash transfers on health outcomes and use of health services in low and middle income countries. Cochrane Database Syst Rev, 2009. 4(4). [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Billah SM, Saha KK, Khan ANS, Chowdhury AH, Garnett SP, Arifeen SE, et al. Quality of nutrition services in primary health care facilities: Implications for integrating nutrition into the health system in Bangladesh. PloS one. 2017;12(5):e0178121 doi: 10.1371/journal.pone.0178121 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Das S, Alcock G, Azad K, Kuddus A, Manandhar DS, Shrestha BP, et al. Institutional delivery in public and private sectors in South Asia: a comparative analysis of prospective data from four demographic surveillance sites. BMC pregnancy and childbirth. 2016;16:273 doi: 10.1186/s12884-016-1069-7 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Karim RM, Abdullah MS, Rahman AM, Alam AM. Identifying influence of perceived quality and satisfaction on the utilization status of the community clinic services; Bangladesh context. Bangladesh Medical Research Council bulletin. 2015;41(1):1–12. [PubMed] [Google Scholar]
- 50.Karim RM, Abdullah MS, Rahman AM, Alam AM. Identifying role of perceived quality and satisfaction on the utilization status of the community clinic services; Bangladesh context. BMC health services research. 2016;16:204 doi: 10.1186/s12913-016-1461-z [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Rahman AE, Iqbal A, Hoque DM, Moinuddin M, Zaman SB, Rahman QS, et al. Managing Neonatal and Early Childhood Syndromic Sepsis in Sub-District Hospitals in Resource Poor Settings: Improvement in Quality of Care through Introduction of a Package of Interventions in Rural Bangladesh. PloS one. 2017;12(1):e0170267 doi: 10.1371/journal.pone.0170267 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Wichaidit W, Alam MU, Halder AK, Unicomb L, Hamer DH, Ram PK. Availability and Quality of Emergency Obstetric and Newborn Care in Bangladesh. Am J Trop Med Hyg. 2016;95(2):298–306. doi: 10.4269/ajtmh.15-0350 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Ahmed S, Khan MM. Is demand-side financing equity enhancing? Lessons from a maternal health voucher scheme in Bangladesh. Social science & medicine (1982). 2011;72(10):1704–10. [DOI] [PubMed] [Google Scholar]
- 54.Ahmed S, Khan MM. A maternal health voucher scheme: what have we learned from the demand-side financing scheme in Bangladesh? Health Policy Plan. 2011;26(1):25–32. doi: 10.1093/heapol/czq015 [DOI] [PubMed] [Google Scholar]
- 55.Hunter BM, Murray SF. Demand-side financing for maternal and newborn health: what do we know about factors that affect implementation of cash transfers and voucher programs? BMC pregnancy and childbirth. 2017;17(1):262 doi: 10.1186/s12884-017-1445-y [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Murray SF, Hunter BM, Bisht R, Ensor T, Bick D. Demand-side financing measures to increase maternal health service utilisation and improve health outcomes: a systematic review of evidence from low- and middle-income countries. JBI library of systematic reviews. 2012;10(58):4165–567. doi: 10.11124/jbisrir-2012-408 [DOI] [PubMed] [Google Scholar]
- 57.Schmidt JO, Ensor T, Hossain A, Khan S. Vouchers as demand side financing instruments for health care: a review of the Bangladesh maternal voucher scheme. Health policy (Amsterdam, Netherlands). 2010;96(2):98–107. [DOI] [PubMed] [Google Scholar]
- 58.Program Management and Monitoring Unit (PMMU) Planning Wing, Ministry of Health and Family Welfare, Government of the People’s Republic of Bangladesh. Health, Nutrition and Population Strategic Investment Plan (HNPSIP) 2016–21, Program Implementation Plan(PIP), Dhaka: Ministry of Health and Family Welfare Bangladesh, 2016. [Google Scholar]
- 59.Health Economics Unit (HEU), Ministry of Health & Family Welfare, Government of the People’s Republic of Bangladesh. Health Care Financing Strategy 2012–2032, Dhaka: Ministry of Health and Family Welfare Bangladesh, November 2012. [Google Scholar]
- 60.Kruk ME, Goldmann E, Galea S. Borrowing and selling to pay for health care in low- and middle-income countries. Health affairs (Project Hope). 2009;28(4):1056–66. [DOI] [PubMed] [Google Scholar]
- 61.Lagomarsino G, Garabrant A, Adyas A, Muga R, Otoo N. Moving towards universal health coverage: health insurance reforms in nine developing countries in Africa and Asia. Lancet. 2012;380:933–43. doi: 10.1016/S0140-6736(12)61147-7 [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Total observation of this dataset is 7,039. The variable name started with “q” provides the morbidity information of under-five children; “r” presents the child illness cost. The variable name started with “c” and “d” refers to the information of household characteristics and respondent background respectively.
(DTA)
Data Availability Statement
Dataset for the paper has been uploaded as a supporting information file.