Abstract
Objectives:
To investigate existing knowledge in the literature about end-of-life decision making by family caregivers of persons with dementia, focusing on decision aids for caregivers of persons with advanced dementia, and to identify gaps in the literature that can guide future research.
Methods:
A literature review through systematic searches in PubMed, CINAHL Plus with Full Text, and PsycINFO was conducted in February 2018; publications with full text in English and published in the past 10 years were selected in multiple steps.
Results:
The final sample included five decision aids with predominantly Caucasian participants; three of them had control groups, and three used audiovisual technology in presenting the intervention materials. No other technology was used in any intervention. Existing interventions lacked tailoring of information to caregivers’ preferences for different types and amounts of information necessary to make decisions consistent with patients’ values.
Conclusion:
Research is needed in exploring the use of technology in decision aids that could provide tailored information to facilitate caregivers’ decision making. More diverse samples are needed.
Keywords: Dementia, Alzheimer’s, family caregivers, end-of-life, decision aids
Introduction
Dementia, a collection of symptoms involving cognitive impairment severe enough to interfere with daily living, is a major public health issue worldwide. In the United States, as the number and proportion of older adults increase, the number of persons living with dementia is projected to increase from 5.4 million in 2016 to 13.8 million in 2050, with the greatest growth among those in advanced stage.1 Dementia is the sixth leading cause of death in the United States, the only one for which there is currently no treatment or cure.1
The very nature of dementia requires heavy family involvement, which can be stressful and challenging.2 Negative consequences for caregivers’ own health and well-being have been well documented.3,4 Even after placing a person with dementia in a care facility (e.g. nursing homes), the caregiver continues to be involved, supervising the care of the person with dementia at the facility and serving as a surrogate decision maker for important legal, financial, and healthcare decisions.5 The ethical and emotional responsibilities of caregivers are great, especially when decisions involve end-of-life (EOL) care. Such decisions are often high-stake, value-laden, and complex (e.g. withdrawing artificial nutrition/hydration or antibiotics, or enrolling in hospice).6–9
In response to the growing number of persons with dementia at EOL and the complexity of decision-making responsibilities of caregivers, researchers have begun to develop and test interventions that can support family caregivers’ decision making for persons with dementia. This is done primarily through the use of decision aids, which are structured tools designed to help patients and their families make specific, informed healthcare choices consistent with patients’ values.10 Decision aids typically contain pertinent educational information about a patient’s condition or disease and about the advantages and disadvantages of treatment options; assessment tools that help individuals clarify their values by asking users to rate their perceptions of the benefits and disadvantages of different treatment or options; and advice about the decision-making process.9 Formats of decision aids vary from video to print information to help decision makers consider how risk, uncertainty, and values may affect clinical and care choices.7 Developed as an adjunct to, not in lieu of, consultation and counseling from healthcare providers, decision aids have been shown to improve knowledge, engagement in shared decision making, satisfaction with decisions, and compliance with treatment plans.11 Decision aids are typically designed to be brief and simple to administer, thus addressing a major barrier to providers’ engagement with patients and their families in shared decision making—that is, time constraints.
To our knowledge, no literature review exists to systematically compare and summarize the characteristics of existing decision aids for caregivers of persons with advanced dementia. To address this gap in the literature, this literature review aims to systematically investigate existing knowledge in the literature about EOL decision making in family caregivers of persons with dementia, focusing on the types of decision aids available for family caregivers of persons with advanced dementia, and to identify gaps in the literature that can guide future research (e.g. we intend to develop and test a mobile technology–based decision aid for caregivers). Our overarching research question (RQ) was. “What were the main characteristics of existing decision aids for family caregivers of persons with advanced dementia?” Under this overarching RQ, we had two specific RQs: How might existing decision aids have involved tailoring, specifically based on patients’ values and their caregivers’ information preferences? (RQa) And what types of technology were used in existing decision aids for family caregivers of persons with advanced dementia to obtain desired information (RQb)?
Methods
Article selection
Following strategies used in earlier literature review studies,12–14 we performed three rounds of systematic selection in the PubMed database: (a) keyword search in Titles/Abstracts and MeSH terms, (b) screening of titles and abstracts, and (c) screening of full-text articles. The searches were performed on 5 February 2018.
Round 1: keyword search
We used the following four sets of keywords to search the Title/Abstract field in PubMed: (“dementia” OR “Alzheimer’s”) AND (“decision aid*”) AND (“caregiver*” OR “proxy” OR “proxies” OR “surrogate*”) AND (“end of life” OR “advanced dementia”). We used the following PubMed filters: (1) Text availability: Full text, (2) Publication dates: 10 years, and (3) Species: Humans. This process produced a total of seven articles. Next, we searched in MeSH terms in PubMed, using the same search terms mentioned above (except for “surrogate*,” which was not a MeSH term) and with the same three built-in filters (full text available, published in the past 10 years, and humans). A total of three results were found. Combining the results from these two searches yielded a total of 10 non-duplicate results.
In addition to PubMed, we also searched in two other databases on the same day: CINAHL Plus with Full Text and PsycINFO. We used the same four sets of keywords that we used for PubMed to search in the Abstract field of these two additional databases. We also added the following built-in filters (“Limiters”) when searching in these two additional databases: Full Text, References Available, English Language, Peer Reviewed, Research Article, Human, and Journal Article. Our searches found no additional results than we had already found in PubMed. Thus, the 10 results found during this round were used in the subsequent rounds of screening.
Round 2: screening the titles and abstracts
Author B.X. manually screened the titles and abstracts of the 10 articles to ensure they covered all four key aspects that guided our first round of searches, with the following further criteria predetermined by authors B.X., J.K., and K.R.F.:
Articles reporting original data were included; those that did not report original data were excluded.
Articles in which family caregivers of dementia patients constituted at least part of the study sample were included. For example, a study that included both healthcare providers and family caregivers was included, whereas a study that had only healthcare providers in the study sample without any family caregivers was excluded.
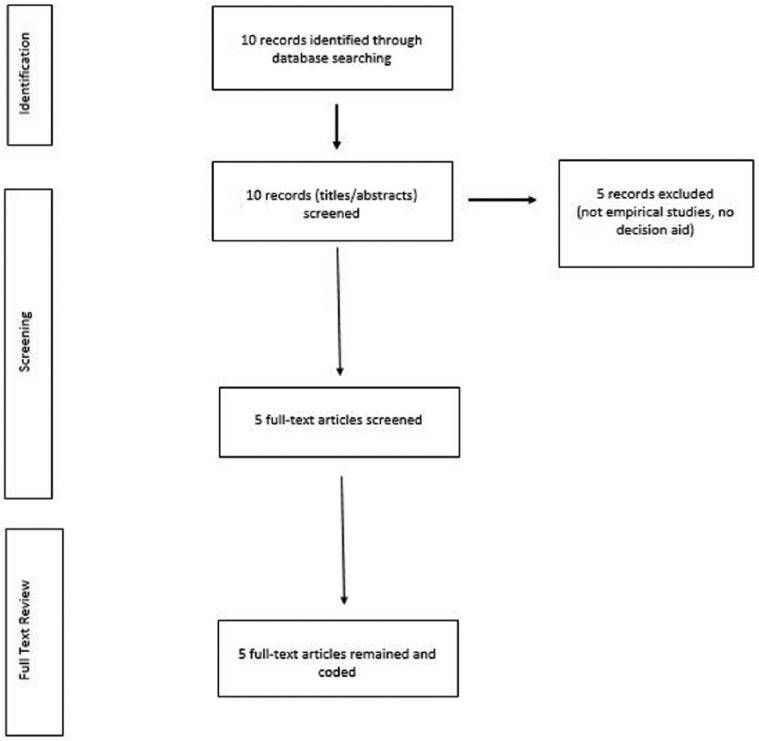
After these criteria were applied, five articles remained. The full text of the remaining five articles was examined and confirmed that they all met the criteria. This final sample comprised empirical studies published over the last 10 years that focused on decision aids for the EOL decision making of family caregivers of persons with advanced dementia. The selection process is illustrated in Figure 1.
Figure 1.
Systematic selection process.
Round 3: coding the full-text articles
We reviewed the full text of the final five articles and coded them by two independent coders (B.X. and A.S.B.) using a coding sheet predetermined by authors B.X., J.K., and K.R.F. based on prior work.12–14 Discrepancies between the two independent coders’ coding were minimal. After all five articles were coded, key information from each article was summarized.
Results
Key characteristics of the studies in our final sample are summarized in Table 1.
Table 1.
Summary of the studies in the final sample.
| Reference | Purpose/aims | Sample | Research design | Intervention; technology used | Key findings |
|---|---|---|---|---|---|
| Einterz et al.7 | To explore the feasibility of a decision aid intervention for caregivers and to generate preliminary evidence on the intervention’s effect on quality of communication and decision making | N = 18 pairs of persons with (moderate to severe) dementia and their caregivers | Pre-/posttest; no control | Each caregiver viewed the decision aid video and participated in a structured care plan meeting with an interdisciplinary team Technology used: video |
The intervention was feasible and relevant for the target population; it improved caregivers’ knowledge, quality of communication, and particularly quality of communication at EOL with providers |
| Hanson et al.15 | To describe the protocols of a decision aid intervention, challenges, and strategies for recruitment and retention, and approaches to ensuring research ethics | N = 256 dyads of persons with advanced dementia and their caregivers | Cluster randomized controlled trial | Caregivers reviewed information (in print or audio) about dementia, feeding options in advanced dementia. Controls received usual care Technology used: audio narration with words on a computer screen for participants with impaired vision or limited literacy |
The research team used multiple strategies to recruit and retain sites and participants; successfully enrolled 256 dyads, and 99% of them completed the 3-month study period; recognizing persons with advanced dementia as a vulnerable population is important for ensuring research ethics |
| Hanson et al.2 | To test the efficacy of a decision aid (the same one introduced in Hanson et al. 2010) in improving the quality of decision making about feeding options in advanced dementia | N = 256 dyads of persons with advanced dementia and their caregivers | Cluster randomized controlled trial | Same as reported in Hanson et al.15 | Improved knowledge among caregivers in the intervention group (16.8 vs 15.1, p < .001); after 3 months, caregivers in the intervention group had lower Decisional Conflict Scale scores than did those in the control group (1.65 vs 1.90, p < .001) and had more discussions about feeding options with a healthcare provider (46% vs 33%, p = .04). Persons with advanced dementia in the intervention group were more likely to receive a dysphagia diet (89% vs 76%, p = .04). No statistically significant difference in tube feeding between the intervention and control groups |
| Hanson et al.16 | To describe strategies used to monitor and promote the fidelity of a decision aid intervention | N = 151 dyads of persons with dementia and their caregivers | Cluster randomized controlled trial | Intervention group received (1) a 20-min video decision aid about care choices in advanced dementia, and (2) a structured nursing home care plan meeting to address goals of care. Three goals were covered: prolonging life, supporting function, and improving comfort; Control: viewed a 20-min informational video about dementia and participated in usual care plan meetings with staff Technology used: video |
Intervention fidelity strategies used in the study enabled providers to implement a decision aid intervention for caregivers of persons with advanced dementia |
| Snyder et al.17 | Aim 1: To describe caregivers’ perceptions of feeding options for their relatives with advanced dementia living in skilled nursing facilities; Aim 2: To explore how a decision aid might change caregivers’ knowledge about feeding options, expectations of tube feeding benefits, decisional conflict, and preferred feeding method | Aim 1: N = 255; Aim 2: N = 126 (only caregivers in the intervention group were studied for Aim 2) | Aim 1: semi-structured interviews with open-ended questions; Aim 2: pre-/posttest; no control | A decision aid (in audio, visual, and print formats) provided caregivers in the intervention group with information about dementia, feeding problems, pros and cons of feeding options, and surrogates’ role in decision-making Audio-visual technology |
From pre- to posttest, participants in the intervention group showed improved knowledge (15.5 vs 16.8; p < .001), decreased expectation of tube feeding benefits (2.73 vs 2.32; p = .001), and decreased decisional conflict (2.24 vs 1.91; p < .001). Their preference for assisted oral feeding did not change, but certainty about their choice improved (1.35 vs 1.05; p = .016), suggesting the efficacy of using this decision aid in improving caregiver decision making about feeding options in the care for advanced dementia patients |
EOL: end-of-life.
The studies’ samples varied widely, from 36 to 512. All interventions consisted of predominately Caucasian participants. Two of the interventions in our final sample did not have control groups;7,17 the others did.2,15,16 All interventions used audiovisual technology—intervention materials delivered in an audio/video format in addition to a conventional print format. No other technology was used in any of the interventions. The interventions focused on factors affecting typical EOL decision-making processes and outcomes (especially feeding-related), that is, knowledge about feeding options, communication skills, decisional conflicts, and decisions about treatment.
The interventions all involved delivering educational materials to family caregivers, although differences existed in how those materials were delivered. Some of the interventions featured providing participants with the same generic materials to review on their own with no other intervention elements.2,15,17 Other interventions7,16 involved participants reviewing the materials individually, followed by a structured care plan meeting with the staff, with the latter presumably enabling opportunities to provide information tailored to caregivers’ unique circumstances. Notably though, none of the interventions specifically acknowledged the need for tailoring of information to the needs of caregivers or patients in different situations.
The studies in this review involved several different instruments to measure a range of concepts, most commonly knowledge, communication skills, decisional conflict, comfort with knowledge, confidence with treatment, and satisfaction with care. Many of these instruments were developed specifically for these interventions and require further psychometric testing in different populations and contexts. The studies that focused on the efficacy of their interventions2,17 reported their interventions were effective in at least one of their outcome measures, that is, improved knowledge, quality of communication, or decreased decisional conflict. One intervention found statistically significant difference in tube feeding between the intervention and control groups.2
It should be noted that the reviewed articles provided insufficient information about the interventions, making it difficult to extract interventions’ details and make comparisons across the studies. The description of an intervention could be as simple as one sentence, for example:17 “Intervention: For intervention surrogates only, an audiovisual-print decision aid provided information on dementia, feeding problems in dementia, advantages and disadvantages of feeding tubes or assisted oral feeding options, and the role of surrogates in making these decisions” (p. 114).
Discussion
The small number of interventions in our final sample suggests that decision aids supporting EOL decision making by caregivers of persons with dementia is currently understudied and in need of extensive research. Our ability to make comparisons between studies was limited because of the differing methods employed and different types of decision aids examined. An added challenge is that insufficient information was provided in the publications with regard to various specifics about the decision aids. Future studies should report details of the interventions such as the amount of information provided (e.g., number of pages of print materials, minutes of audio/video provided, approximate time required to review the information) and the intervention’s delivery mode (e.g. group size or individual information review, presence or absence of tailored in-person guidance).
Feeding tube-related issues faced by caregivers of people with advanced dementia were the primary focus of decision aids identified in this review of empirical studies.5,7 As the condition of the person with dementia deteriorates, decisions involve more emotionally laden issues such as advance care planning or resuscitation orders.6,18 Such decisions are difficult, because they require the caregiver to exercise substituted judgment or follow best interest standards to make decisions on behalf of the person with dementia; yet, it is often difficult to know what the wishes of a person with dementia are or what the best course of treatments are, given the uncertain, protracted nature of dementia’s progression.6,18,19
A lack of focus on tailoring to caregivers’ information preferences necessary to ensure decision making consistent with patients’ values
The interventional studies in our sample generally concluded that their decision aids helped caregivers with their decision making. However, a major limitation of existing decision aids is that they typically do not take into account caregivers’ preferences for different types and amounts of information that are necessary to ensure decision making consistent with patients’ values. The decision aids in these studies were typically limited by a one-directional approach: the types and amounts of information provided were predetermined by researchers/providers, instead of tailored to the information preferences of individual caregivers. Subsequently, caregivers might not receive the right types and/or amounts of information necessary for making decisions consistent with patients’ values. This lack of focus on values and preferences may reflect an assumption in the current medical model that patients have well-formed EOL care preferences consistent with their values and that caregivers can ascertain what those preferences are, or that caregivers are fully informed of how different care decisions may, or may not, support their loved ones’ values and EOL preferences. However, such an assumption frequently fails to reflect reality. Patients and their spouses can differ significantly in EOL care preferences, with patients more likely to prefer additional treatment than their spouses.20 This is consistent with findings from earlier research showing low to modest congruence between patients and caregivers.21 When potential caregivers were asked in scenarios to predict patients’ preferences, accuracy was highest when patients’ current health status was considered and lowest in scenarios of stroke and dementia; caregivers reported that EOL discussions failed to occur for a number of reasons, but mostly because of family belief structures and personalities.22
In a study that compared hypothetical EOL decision-making vignettes between relatives and professionals acting as patient surrogates, researchers found that situational variables such as the patient’s current behavior and the views of healthcare professionals and family members had higher impacts on decisions than did the patient’s prior statements or life attitudes.8 Other researchers who have looked at EOL decision-making scenarios with healthy older adults have found other factors that influence caregivers’ decision making, such as caregivers’ own current state of health, health literacy, and communication with healthcare providers.8,22–24 Even when patients’ care preferences are known to caregivers, they might still not be implemented, due to factors such as attempting to achieve family consensus.25 Evidence from 228 community-dwelling family care dyads showed that 25% of cargivers underestimated the importance of everyday care values of persons with dementia, suggesting incongruence between patients’ and caregivers’ values.26 If and how these factors affect caregiver decision making deserves further examination and implementation in decision aids.
Underutilization of technology
Despite advances in information and communication technology, none of the decision aids in our sample involved any kind of technology beyond audio/video as a part of an intervention. Existing decision aids are typically delivered to caregivers in print (typically a hardcopy workbook), sometimes coupled with in-person discussions with trained providers in a group or individually. The printed materials’ content varied; topics included information about advanced dementia, the role of the surrogate decision maker, EOL care options and their pros and cons, common community services available, and pointers toward further information. Presented in a static print or audio/video format, such rich information can be overwhelming, and some of it may even be irrelevant to individuals with unique values, preferences, or other circumstances. Tailoring interventions to meet the needs of particular groups is critical, and such interactive information can best be delivered using more advanced technology such as a website or mobile app that would allow for interactive use beyond the scope of a particular class discussion setting. Doing so is important because caregivers are likely to think of additional questions while engaging in the everyday process of caring for persons with dementia. Unfortunately, none of the studies reviewed employed such advanced technology in their interventions.
For technology to be useful in decision aids for caregivers of persons with dementia, an important point to note is that caregivers (e.g. spouses of persons with dementia) may be of older ages themselves and/or facing other challenges (e.g. limited literacy). As such, it is critical that any technology used in a decision aid is easy to use for caregivers with limited technology experience and skills. Age-appropriate training and technical support will be necessary as well. Furthermore, integrating technology in decision aids is not to completely replace human interactions, as interactions with healthcare professionals can be instrumental to the caregiver’s decision-making process and outcomes.
The importance of advance care planning
A major topic commonly addressed in the literature was advance care planning for persons with dementia. Caregivers in various sample populations had taken on this responsibility with little or no knowledge of the values and desires of their relatives regarding EOL care and management. Decision aids have been designed to encourage caregivers to prepare advance directives and/or discuss possible treatment limitations with healthcare providers. Advance care plans are themselves a type of decision aid because they educate and prepare caregivers for the progression that they can expect as their relatives decline toward the end of life.6,7 In an ideal situation, the demands of an advance directive or any kind of advance care planning would be discussed with the family member while the person is still able to express his or her wishes about EOL care. Decisional conflict was greater with caregivers who were struggling to make sense of their relatives’ wishes, and the literature showed that decision aids did help in these situations.5–7
An important aspect of advance care planning that requires greater acceptance is the use of do not hospitalize (DNH) orders:27 barriers to these orders included a “perceived lack of physician involvement in decision-making and limited understanding of DNH orders and the resident’s prognosis” (p. 1568). Meanwhile, evidence also exists that advance directives (specifically, euthanasia directives in the Netherlands) were hardly ever actually adhered to by physicians and family members after they had been completed,18 although such a phenomenon may have limited generalizability given its specific context.
The controversies around tube feeding and use of antibiotics
Feeding is one of the most contentious areas of decision making for persons with dementia. Decision aids typically included content designed to help caregivers understand the issues surrounding feeding, percutaneous endoscopic gastronomy tube insertion, and alternative treatments. Controlled observational studies show that tube feeding does not improve survival, aspiration, or wound healing; however, this information is not routinely shared with decision makers, and families and professionals alike may have unrealistically high expectations for benefits from tube feeding.2 The decision aids in this literature review frequently involved improving caregiver knowledge about problems with tube feeding, separating the desire to support and “nourish” the person with dementia from the physical need to feed someone mechanically who has a limited life expectancy.2,5,7 However, the decision aids did not assess caregivers’ preferences for different types and amounts of information beforehand and presented little opportunity to include them in the decision-making process.
Related to tube feeding is the question of treatment for infections. Treatment with antibiotics frequently brings its own set of complications, including gastrointestinal upset and other side effects. Also, transferring a person with dementia can worsen disorientation because it places the person in an unfamiliar environment. In a study that examined caregivers’ involvement in decisions about whether or not to treat minor infections in persons with dementia and how aggressively to do so, the researchers found that caregivers participated only about half of the time.5 Studies of family members’ perceptions of the EOL decision-making process and outcomes suggest important opportunities for the improvement of decision making in EOL care.28
The need for research on diverse populations
Using racially/ethnically homogeneous samples—that consisted of predominately Caucasian participants—was a major limitation in studies in this review. Decision making is culturally sensitive, and more diverse samples would enhance our knowledge in this area. In addition, ethnically and racially diverse samples may well point out a need for more flexible, customizable decision aids. For instance, prior evidence suggests that African Americans were less likely than Caucasian Americans to have advance care plans, and implementing programs in the community was effective in enhancing success because participants felt comfortable discussing sensitive topics in environments they could trust.6 A study of Hong Kong Chinese family caregivers found that reliance on collective family decisions significantly affected choices of caregivers and that filial piety and possible confrontation from relatives, combined with a lack of knowledge about life-sustaining treatments, worsened decision-making stresses.29 Compared with Caucasian elders and their caregivers, non-Caucasians and individuals with greater financial difficulty had stronger preferences for life-prolonging treatment.23
People from ethnic minority groups may prefer different EOL treatments and are, due to disparities and differences in values and beliefs, less likely to have advance directives (e.g. members of specific ethnic groups may have strong cultural taboos against open and direct discussion about death and dying30,31). The experiences of ethnic minority caregivers differ as well (e.g. higher levels of depression and stress among Hispanic caregivers than among non-Hispanic Caucasians32). Caregivers and patients in rural areas also face unique challenges: they tend to be older, in worse health, with greater financial burden and limited access to providers and support services, experiencing stigma of dementia and a lack of privacy.33–38 The coping styles of caregivers of persons with dementia in rural areas are often different from those in urban areas, suggesting unique needs.38 The significant health disparities and characteristics among caregivers who are members of racial/ethnic minority groups and/or live in rural areas call for effective interventions tailored to their unique needs and circumstances.
Limitations of this literature review
This literature review has limitations. We searched in only three databases with specific inclusion/exclusion criteria. While these criteria were necessary for our specific purposes (i.e. preparing for a larger intervention study involving using interactive technology to provide tailored decision aids for caregivers of persons with advanced dementia), using these criteria led to only five relevant articles in our final sample. One possible reason is that we used search terms common to the US context, which might not necessarily be common terms used in other national contexts. Subsequently, our study is geared more toward the US context. Also, our searches focused on decision aids, for the purpose of comparing and analyzing what has been done and what has not with existing decision aid interventions. It was beyond the scope of this current literature review to examine the literature on broader issues related to decision making.
Conclusion
This literature review has identified several issues that call for attention. Few decision aids exist for caregivers’ EOL decision making for persons with dementia. Existing studies lacked a focus on caregivers’ preferences for different types and amounts of information necessary to ensure decision making consistent with patients’ values. Advance care planning for persons with dementia is a major challenge for caregivers. Ideally, the demands of an advance directive or any kind of advance care planning would have been discussed with the person with dementia while he or she was still able to express such wishes. Yet, this is often not the case. Developers of decision aids should strive to find ways to incorporate values and preferences in decision making. None of the studies mentioned any tailoring or acknowledged the need for specific tailoring of information to the individual situations of patients or caregivers. Important variables for tailoring such as values and information preferences were typically not assessed before or during the implementation of decision aids. While recent technological developments enable great tailoring of information, existing decision aids have largely underutilized such tailoring potential. Future research should investigate whether/how we could take full advantage of recent technological developments in the design and implementation of future decision aids (that are easy to use by caregivers with limited technology literacy). Finally, existing studies involved samples predominantly of non-Hispanic Caucasians. Since EOL decision making is culturally sensitive, future research should place special emphasis on ethnically and racially diverse samples and develop tailored and interactive decision aids for underrepresented groups.
Acknowledgments
This work was part of a Pilot Research Grant from the Population Health Initiative at the University of Texas at Austin, entitled Values and Preferences in Dementia Family Caregivers’ End-of-Life Decision-Making; Principal Investigator (PI): Bo Xie; Co-PIs: Ken Fleischmann and Jung Kwak.
Footnotes
Declaration of conflicting interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was part of a Pilot Research Grant from the Population Health Initiative at the University of Texas at Austin, entitled Values and Preferences in Dementia Family Caregivers’ End-of-Life Decision-Making; Principal Investigator (PI): Bo Xie; Co-PIs: Ken Fleischmann and Jung Kwak.
ORCID iD: Bo Xie  https://orcid.org/0000-0002-6016-6008
https://orcid.org/0000-0002-6016-6008
References
- 1. Alzheimer’s Association. 2016 Alzheimer’s disease facts and figures. Alzheimers Dement 2016; 12(4): 459–509. [DOI] [PubMed] [Google Scholar]
- 2. Hanson LC, Carey TS, Caprio AJ, et al. Improving decision-making for feeding options in advanced dementia: a randomized, controlled trial. J Am Geriatr Soc 2011; 59(11): 2009–2016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. De la Cuesta-Benjumea C. The legitimacy of rest: conditions for the relief of burden in advanced dementia care-giving. J Adv Nurs 2010; 66(5): 988–998. [DOI] [PubMed] [Google Scholar]
- 4. National Academies of Sciences, Engineering, and Medicine. Families caring for an aging America. Washington, DC: The National Academies Press, 2016. [PubMed] [Google Scholar]
- 5. Givens JL, Kiely DK, Carey K, et al. Healthcare proxies of nursing home residents with advanced dementia: decisions they confront and their satisfaction with decision-making. J Am Geriatr Soc 2009; 57(7): 1149–1155. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Bonner GJ, Wang E, Wilkie DJ, et al. Advance care treatment plan (ACT-Plan) for African American family caregivers: a pilot study. Dementia 2014; 13(1): 79–95. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Einterz SF, Gilliam R, Lin FC, et al. Development and testing of a decision aid on goals of care for advanced dementia. J Am Med Dir Assoc 2014; 15(4): 251–255. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Jox RJ, Denke E, Hamann J, et al. Surrogate decision making for patients with end-stage dementia. Int J Geriatr Psych 2012; 27(10): 1045–1052. [DOI] [PubMed] [Google Scholar]
- 9. Stirling C, Leggett S, Lloyd B, et al. Decision aids for respite service choices by carers of people with dementia: development and pilot RCT. BMC Med Inform Decis Mak 2012; 12: 21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. Stacey D, Bennett CL, Baary MJ, et al. Decision aids for people facing health treatment or screening decisions. Cochrane Database Syst Rev 2017(4): CD001431. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Shay LA, Lafata JE. Where is the evidence? A systematic review of shared decision making and patient outcomes. Med Decis Making 2015; 35(1): 114–131. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Nie L, Xie B, Yang Y, et al. Characteristics of Chinese m-Health applications for diabetes self-management. Telemed J E Health 2016; 22(7): 614–619. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. Walker LO, Gao J, Xie B. Postpartum psychosocial and behavioral health: a systematic review of self-administered scales validated for postpartum women in the United States. Womens Health Issues 2015; 25(5): 586–600. [DOI] [PubMed] [Google Scholar]
- 14. Radhakrishnan K, Xie B, Berkley A, et al. Barriers and facilitators for sustainability of tele-homecare programs: a systematic review. Health Serv Res 2015; 51(1): 48–75. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Hanson LC, Gilliam R, Lee TJ. Successful clinical trial research in nursing homes: the improving decision-making study. Clin Trials 2010; 7(6): 735–743. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16. Hanson LC, Song MK, Zimmerman S, et al. Fidelity to a behavioral intervention to improve goals of care decisions for nursing home residents with advanced dementia. Clin Trials 2016; 13(6): 599–604. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Snyder EA, Caprio AJ, Wessell K, et al. Impact of a decision aid on surrogate decision-makers’ perceptions of feeding options for patients with dementia. J Am Med Dir Assoc 2013; 14(2): 114–118. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. De Boer ME, Dröes RM, Jonker C, et al. Advance directives for euthanasia in dementia: how do they affect resident care in Dutch nursing homes? Experiences of physicians and relatives. J Am Geriatr Soc 2011; 59(6): 989–996. [DOI] [PubMed] [Google Scholar]
- 19. Mitchell SL, Tetroe J, O’Connor AM. A decision aid for long-term tube feeding in cognitively impaired older persons. J Am Geriatr Soc 2001; 49(3): 313–316. [DOI] [PubMed] [Google Scholar]
- 20. Ayalon L, Bachner YG, Dwolatzky T, et al. Preferences for end-of-life treatment: concordance between older adults with dementia or mild cognitive impairment and their spouses. Int Psychogeriatr 2012; 24(11): 1798–1804. [DOI] [PubMed] [Google Scholar]
- 21. Shalowitz DI, Garrett-Mayer E, Wendler D. The accuracy of surrogate decision makers: a systematic review. Arch Intern Med 2006; 166(5): 493–497. [DOI] [PubMed] [Google Scholar]
- 22. Black BS, Fogarty LA, Phillips H, et al. Surrogate decision makers’ understanding of dementia patients’ prior wishes for end-of-life care. J Aging Health 2009; 21(4): 627–650. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23. Winter L, Parks SM. Elders’ preferences for life-prolonging treatment and their proxies’ substituted judgment: influence of the elders’ current health. J Aging Health 2012; 24(7): 1157–1178. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24. Volandes AE, Mitchell SL, Gillick MR, et al. Using video images to improve the accuracy of surrogate decision-making: a randomized controlled trial. J Am Med Dir Assoc 2009; 10(8): 575–580. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. Hirschman KB, Kapo JM, Karlawish JH. Why doesn’t a family member of a person with advanced dementia use a substituted judgment when making a decision for that person? Am J Geriatr Psychiatry 2006; 14(8): 659–667. [DOI] [PubMed] [Google Scholar]
- 26. Miller LM, Whitlatch CJ, Lee CS, et al. Care values in dementia: patterns of perception and incongruence among family care dyads. Gerontologist. Epub ahead of print 12 March 2018. DOI: 10.1093/geront/gny008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Formiga F, Olmedo C, López-Soto A, et al. Dying in hospital of terminal heart failure or severe dementia: the circumstances associated with death and the opinions of caregivers. Palliat Med 2007; 21(1): 35–40. [DOI] [PubMed] [Google Scholar]
- 28. Teno JM, Mitchell SL, Kuo SK, et al. Decision-making and outcomes of feeding tube insertion: a five-state study. J Am Geriatr Soc 2011; 59(5): 881–886. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29. Kwok T, Twinn S, Yan E. The attitudes of Chinese family caregivers of older people with dementia towards life sustaining treatments. J Adv Nurs 2007; 58(3): 256–262. [DOI] [PubMed] [Google Scholar]
- 30. Lines LM, Sherif NA, Wiener JM. Racial and ethnic disparities among individuals with Alzheimer’s disease in the United States: a literature review. Research report no. RR-0024-1412, December 2014. Research Triangle Park, NC: RTI Press, https://pdfs.semanticscholar.org/7ed5/b9ed14cd3e002df546134e76766d01c5c4aa.pdf [Google Scholar]
- 31. Monahan DJ. Family caregivers for seniors in rural areas. J Fam Soc Work 2013; 16(1): 116–128. [Google Scholar]
- 32. Blusi M, Asplund K, Jong M. Older family carers in rural areas: experiences from using caregiver support services based on information and communication technology (ICT). Eur J Ageing 2013; 10(3): 191–199. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33. Buckwalter K. Interventions for family caregivers of patients with Alzheimer’s disease in community-based settings: items for consideration. Int Psychogeriatr 1996; 8(suppl. 1): 121–122. [DOI] [PubMed] [Google Scholar]
- 34. Buckwalter KC, Davis LL. Elder caregiving in rural communities. In: Talley RC, Chwalisz K, Buckwalter KC. (eds) Rural caregiving in the United States: research, practice, policy. New York: Springer, 2011, pp. 33–46. [Google Scholar]
- 35. Direito A, Dale LP, Shields E, et al. Do physical activity and dietary smartphone applications incorporate evidence-based behaviour change techniques? BMC Public Health 2014; 14: 646. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36. Ehrlich K, Boström AM, Mazaheri M, et al. Family caregivers’ assessments of caring for a relative with dementia: a comparison of urban and rural areas. Int J Older People Nurs 2015; 10(1): 27–37. [DOI] [PubMed] [Google Scholar]
- 37. Morgan DG, Semchuk KM, Stewart NJ, et al. Rural families caring for a relative with dementia: barriers to use of formal services. Soc Sci Med 2002; 55(7): 1129–1142. [DOI] [PubMed] [Google Scholar]
- 38. Sun F, Kosberg JI, Kaufman AV, et al. Coping strategies and caregiving outcomes among rural dementia caregivers. J Gerontol Soc Work 2010; 53(6): 547–567. [DOI] [PubMed] [Google Scholar]