Abstract
Introduction
Bloodstream infections with multidrug-resistant (MDR) Gram-negative bacteria (GNB) are among the most frequent complications in immunocompromised cancer patients because of their considerable morbidity and mortality. Several guidelines on antimicrobial therapy have addressed empirical treatment for such serious infections; however, the emergence of microbial resistance has become a significant problem worldwide.
Materials and methods
In this study, starting from November 2015 to October 2016, a total of 529 blood specimens were collected from febrile neutropenic cancer patients at a tertiary care cancer hospital in Egypt.
Results
On examination for positive bacterial growth, it was found that 334 specimens showed no growth, while 195 were positive. Out of the 195 positive culture specimens, 102 (102/195, 52.3%) were Gram-negative and 93 (93/195, 47.7%) were Gram-positive. Out of the 102 GNB, 70 (70/102, 68.6%) were MDR, including Escherichia coli (27/70, 38.6%), Klebsiella pneumoniae (24/70, 34.3%), Acinetobacter baumannii (9/70, 12.8%), Enterobacter cloacae (4/70, 5.7%), Pseudomonas aeruginosa (2/70, 2.8%), Klebsiella oxytoca (2/70, 2.8%), and Klebsiella ornithinolytica (2/70, 2.8%). All MDR GNB showed high resistance to ampicillin, cefepime, ceftriaxone, and cephradine (minimum inhibitory concentration at which 50% of the isolates were inhibited [MIC50] >512 μg/mL for each). However, they showed good susceptibility to colistin (MIC50 <1 μg/mL). The most common extended-spectrum β-lactamases (ESBLs) genes detected were ctx-m (39/70, 55.7%), shv (31/70, 44.3%), and tem (22/70, 31.4%). The most common aminoglycoside-resistant gene detected was aac(6′)-Ib (42/70, 60%) followed by the plasmid-mediated quinolone resistance determinants; qnrA (2/70, 2.8%), qnrB (9/70, 12.8%), and qnrS (19/70, 27.1%). ESBL determinants were significantly associated with resistance to ciprofloxacin, levofloxacin, amikacin, and carbapenems (P-value <0.005). The fractional inhibitory concentration index for ampicillin/sulbactam plus ceftriaxone, ampicillin/sulbactam plus amikacin, and amikacin plus levofloxacin showed synergism against 29 (29/70, 41.4%), 19 (19/70, 27.1%), and 11 (11/70, 15.7%) isolates of the tested MDR GNB isolates, respectively.
Conclusion
Accordingly, new empirical antibiotics should be administered including the use of colistin or meropenem alone or both against the MDR GNB in neutropenic cancer patients.
Keywords: ESBLs, plasmid-mediated quinolone resistance, PMQR, fractional inhibitory concentration, FICI
Introduction
Bloodstream infections (BSIs) are defined as positive isolate(s) of blood culture and associated with clinical findings.1 Cancer patients are among the key candidates for this type of infections due to the methods of treatment they undergo, such as invasive surgery, chemotherapy, radiotherapy, immunosuppressive agents, or administration of anticancer drugs during hospital stay. Cancer patients sustaining BSI also have higher morbidity and mortality rates. Therefore, speedy identification of isolates, clinical diagnosis, and effective treatment of BSIs decrease the risk of mortality among cancer patients with BSI.2 Infection with multidrug-resistant (MDR) pathogens including extended-spectrum β-lactamase (ESBL)-producing Enterobacteriaceae are particularly prevalent among cancer patients.3 Enterobacteriaceae cause approximately 65%–80% of documented Gram-negative infections in these patients. However, Pseudomonas aeruginosa is also associated with significant morbidity and mortality in immunocompromised hosts.4 Resistance to the β-lactams is mediated primarily through the production of a variety of β-lactamases including Ambler class C β-lactamases and ESBLs. ESBLs are derived from older, plasmid-mediated hydrolyzing enzymes, primarily the TEM and SHV types (both are ESBL enzymes). Other antibiotic resistance coding genes (i.e., to fluoroquinolones [FQs], aminoglycosides, macrolides, carbapenems, etc.) on the same plasmid can confer a MDR phenotype in a subset of these pathogens.5 Colistin resistance in Gram-negative bacteria (GNB) could be mainly attributed to excessive use of colistin in treating carbapenem-resistant bacteria.6 Clinical studies strongly suggest that combination therapy is superior to monotherapy for carbapenemase-producing Enterobacte-riaceae.7–9 To improve potential survival among patients with high risk of death, combination therapy is recommended.10 However, a combination of two or more active drugs (i.e., colistin, tigecycline, or fosfomycin) with carbapenem is associated with a better outcome.11 Several antimicrobial guidelines have addressed empirical treatment for such serious infections; however, the rapid treatment of such infections has become a significant problem worldwide. Therefore, in this study, we aimed at evaluating the genetic bases of antimicrobial resistance of MDR GNB in cancer patients against the most commonly used antimicrobial agents used for the treatment of such infections. In addition, some antibiotic combinations have been evaluated for use against the clinically relevant MDR GNB pathogens recovered in our study.
Materials and methods
Specimen collections
Starting from November 2015 to October 2016, a total of 529 blood specimens were collected from 529 cancer patients with absolute neutrophils count <500/mm3 and oral temperature >38°C over at least 1 hour from National Cancer Institute (NCI) Cairo University, Cairo, Egypt. The NCI is the largest tertiary cancer hospital in Egypt, drawing patients nationwide. The study was approved by the NCI Ethics Committee and Faculty of Pharmacy Ethical Committee Nr. 173, and written informed consent was obtained from either patients or parents of patients after explaining the study purpose. The collected blood was directly injected into Bactec® (Becton Dickinson, Franklin Lakes, NJ, USA) culture vials and incubated in the Bactec 9050® (Becton Dickinson) incubator. Positive blood culture specimens were directly streaked on blood agar, chocolate agar, and MacConkey agar (Oxoid, Cheshire, England) plates.
Identification of the recovered bacterial isolates
The recovered clinical isolates were categorized according to their Gram stain. Several biochemical tests were performed to identify different bacterial species. The biochemical tests used included triple sugar iron test, oxidase test, citrate utilization test, urease test, methyl red test, Voges–Proskauer test, and eosin methylene blue agar test; all said test media were produced by Oxoid. Identification was confirmed using Microscan® WalkAway-96 Plus auto identification system (Beckman Coulter, Miami, FL, USA).
Antimicrobial susceptibility testing
Antimicrobial susceptibility testing was carried out by both Kirby-Bauer disc diffusion method12 using commercial discs (Oxoid) on Muller Hinton agar (Oxoid) at 37°C for 18 hours and minimum inhibitory concentration (MIC), which is defined as the lowest concentration of an antimicrobial that will inhibit the visible growth of a microorganism after overnight incubation.13 MIC was carried out in triplicate and average MIC was calculated, as recommended by the Clinical and Laboratory Standards Institute (CLSI).14 Isolates resistant to three or more classes of antimicrobials were considered as MDR isolates.15 The tested agents used in Kirby-Bauer disc (μL/disc) diffusion method belonged to five different classes of antimicrobials: the aminoglycosides (amikacin 30 μg, gentamicin 10 μg, and tobramycin 10 μg), β-lactams (ampicillin 10 μg, amoxicillin/clavulanic acid 20 μg/10 μg, aztreonam 30 μg, cefotaxime 30 μg, ceftazidime 30 μg, cefoxitin 30 μg, ceftriaxone 30 μg, cefepime 30 μg, ampicillin/sulbactam 20 μg/10 μg, piperacillin/tazobactam 100 μg/10 μg, imipenem 10 μg, ertapenem 10 μg, cefazolin 30 μg, and meropenem 10 μg), FQs (ciprofloxacin 5 μg and levofloxacin 5 μg), antimetabolites (sulfonamides/trimethoprim 1.25 μg/23.75 μg), and polypeptides (colistin 10 μg). The reference strain Escherichia coli ATCC® 25922™ was used for quality control.
Combinations of antibiotics
The value of the fractional inhibitory concentration index (FICI) as a predictor of synergy has been investigated according to the protocol described by Hsieh et al,16 where FICI = FIC of antibiotic A + FIC of antibiotic B. The FIC of antibiotic A = MIC of antibiotic A in combination/MIC of antibiotic A alone. Moreover, FIC of antibiotic B = MIC of antibiotic B in combination/MIC of antibiotic B alone. The result of FICI was interpreted as follows: FICI ≤0.5, >0.5–1, >1–4.0, and >4 indicate synergism, additive, indifference, and antagonistic effects, respectively. The term “synergism” indicates that the interaction between the two antibiotics causes the total effect of the antibiotics to be greater than the sum of the individual effects of each antibiotic. An “additive” term indicates that the final effect is equal to the sum of the effects of the two antibiotics. The term “indifference” means neither the antibiotics help nor hinder one another’s activity. The term “antagonism” indicates both antibiotics’ interactions cause decrease in the effects of one or both of the drugs.17
Plasmid DNA extraction from MDR isolates
Plasmid DNA extraction was done using QIAprep® Mini-prep kit (Qiagen, Germantown, MD, USA) according to the manufacturer’s specifications. The extracted plasmids were analyzed using agarose gel electrophoresis.18
Amplification of some resistance genes by polymerase chain reaction (PCR)
Amplification of the selected antibiotic resistance genes was carried out via PCR using the appropriate primers (Table 1). The plasmid DNA of the tested MDR bacterial isolates was used as template. Primers were synthesized by Invitrogen (Paisley, UK). Detection of the amplified products was done by agarose gel electrophoresis according to the protocol described by Sambrook and Russell,18 and the expected size of DNA fragment was determined in comparison to DNA ladder (GeneRuler 100 bp or 1 kb Thermo Fisher Scientific, Waltham, MA, USA).
Table 1.
Primer sequences, Ta, and expected product sizes for the tested genes
| Gene | Primer | Primer sequence (5′ → 3′) | Expected product size (bp) | Ta (°C) | References |
|---|---|---|---|---|---|
| ctx-m | Pf Pr |
CGCTTTGCGATGTGCAG ACCGCGATATCGTTGGT |
550 | 47 | Bonnet et al20 |
| shv | Pf Pr |
GGTTATGCGTTATATTCGCC TTAGCGTTGCCAGTGCTC |
867 | 47 | Rasheed et al21 |
| tem | Pf Pr |
ATGAGTATTCAACATTTCCG CTGACAGTTACCAATGCTTA |
867 | ||
| aac(6′)-Ib aac(6′)-Ib-cr | Pf Pr |
TTGCGATGCTCTATGAGTGG CGTTTGGATCTTGGTGACCT |
358 | 46 | Hamed et al22 |
| qnrA | Pf Pr |
GCCCGCTTCTACAATCAAGT GGCAGCACTATTACTCCCAAG |
347 | 60 | |
| qnrB | Pf Pr |
TATGGCTCTGGCACTCGTT GCATCTTTCAGCATCGCAC |
193 | ||
| qnrS | Pf Pr |
TCGGCACCACAACTTTTCAC TCACACGCACGGAACTCTAT |
255 |
Notes: ctx-m, shv, and tem genes code for ESBLs; aac(6′)-Ib gene codes for aminoglycoside 6′-N-acetyltransferase type Ib; aac(6′)-Ib-cr gene codes for aminoglycoside 6′-N-acetyltransferase type Ib ciprofloxacin-resistant variant; qnrA, qnrB, and qnrS genes are PMQR determinants coding for quinolone resistance.
Abbreviations: Ta, calculated annealing temperature; ESBLs, extended-spectrum beta-lactamases; PMQR, plasmid-mediated quinolone resistance.
DNA sequencing of some selected PCR products
The PCR products were purified using GeneJET™ purification kit at Sigma Scientific Services Company (Cairo, Egypt). PCR products of some selected amplified genes of certain MDR GNB isolates were sent for sequencing at GATC (Konstanz, Germany) using ABI 3730 xl DNA sequencer (Thermo Fisher Scientific). The obtained sequence files were assembled into the final consensus sequence using Staden Package program version 3 (http://staden.sourceforge.net/).19 The final assembled sequences were analyzed, annotated, and submitted into the NCBI GenBank database.
Statistical methods
Statistical analysis was done using SPSS version 22 (IBM., Armonk, NY, USA). Qualitative data were expressed as frequency and percentage. Chi-square and Fisher’s exact tests were used for comparisons of categorical variables. All tests were two-tailed, and P-value <0.05 was considered statistically significant.
Results
Patient characteristics
In the period from November 2015 to the end of October 2016, BSIs were detected in 102 of 529 (19.3%) febrile neutropenic patients. The patients’ age ranged from 1 to 66 years, with a mean age of 16 years. There were 54 (54/102, 52.9%) males and 48 (48/102, 47%) females. Eighty-five (85/102, 83.3%) patients were diagnosed with hematological malignancies and 17 (17/102, 16.7%) with solid organ malignancies.
Antimicrobial susceptibility testing
A total of 529 blood specimens were collected of which only 195 specimens showed positive bacterial growth. Out of the 195 positive culture specimens, a total of 102 (102/195, 52.3%) were Gram-negative and 93 (93/195, 47.7%) were Gram-positive. The antibiotic susceptibility patterns of the Gram-negative isolates are shown in Table 2A and B. Out of the 102 GNB, 70 (70/102, 68.6%) isolates were resistant to three or more classes of antimicrobial agents and therefore considered MDR isolates. The MDR GNB include E. coli (27/70, 38.6%), Klebsiella pneumoniae (24/70, 34.3%), Acinetobacter baumannii (9/70, 12.8%), Enterobacter cloacae (4/70, 5.7%), P. aeruginosa (2/70, 2.8%), Klebsiella oxytoca (2/70, 2,8%), and Klebsiella ornithinolytica (2/70, 2.8%). The aforementioned MDR GNB isolates were selected for this study.
Table 2A.
Antimicrobial susceptibility patterns of Enterobacteriaceae isolates
| Antibiotic | Resistant isolates, n (%)
|
|||||
|---|---|---|---|---|---|---|
| E. coli | K. pneumoniae | K. oxytoca | E. cloacae | K. ornithinolytica | S. enterica | |
|
| ||||||
| R | R | R | R | R | R | |
| Ampicillin | 34 (100) | 32 (100) | 3 (100) | 9 (100) | 2 (100) | 0 (0) |
| Amoxicillin/clavulanic acid | 31 (91) | 28 (87) | 2 (67) | 9 (100) | 0 (0) | 0 (0) |
| Ampicillin/sulbactam | 30 (88) | 28 (87) | 2 (67) | 9 (100) | 2 (100) | 0 (0) |
| Piperacillin/tazobactam | 26 (76) | 26 (81) | 2 (67) | 3 (33) | 0 (0) | 0 (0) |
| Aztreonam | 26 (76) | 19 (59) | 2 (67) | 9 (100) | 2 (100) | 2 (100) |
| Meropenem | 16 (47) | 18 (56) | 0 (0) | 0 (0) | 0 (0) | 0 (0) |
| Imipenem | 15 (44) | 16 (50) | 0 (0) | 0 (0) | 0 (0) | 0 (0) |
| Cefoxitin | 26 (76) | 19 (59) | 0 (0) | 9 (100) | 0 (0) | 2 (100) |
| Cefepime | 32 (94) | 24 (75) | 2 (67) | 2 (22) | 0 (0) | 0 (0) |
| Ceftazidime | 32 (94) | 24 (75) | 2 (67) | 6 (67) | 0 (0) | 0 (0) |
| Cefotaxime | 32 (94) | 24 (75) | 2 (67) | 6 (67) | 2 (100) | 0 (0) |
| Ceftriaxone | 32 (94) | 24 (75) | 2 (67) | 5 (55) | 2 (100) | 0 (0) |
| Amikacin | 10 (29.5) | 14 (43) | 0 (0) | 2 (22) | 0 (0) | 2 (100) |
| Gentamicin | 19 (56) | 13 (40) | 2 (67) | 5 (55) | 2 (100) | 2 (100) |
| Tobramycin | 18 (53) | 19 (59) | 2 (67) | 2 (22) | 0 (0) | 2 (100) |
| Ciprofloxacin | 27 (79) | 21 (65) | 2 (67) | 3 (33) | 2 (100) | 0 (0) |
| Levofloxacin | 27 (79) | 18 (56) | 2 (67) | 0 (0) | 2 (100) | 0 (0) |
| Trimethoprim/sulfamethoxazole | 32 (94) | 25 (78) | 2 (67) | 9 (100) | 2 (100) | 0 (0) |
| Cefazolin | 32 (94) | 28 (87) | 2 (67) | 9 (100) | 2 (100) | 2 (100) |
| Ertapenem | 16 (47) | 19 (59) | 0 (0) | 0 (0) | 0 (0) | 0 (0) |
| Colistin | 0 (0) | 4 (12.5) | 0 (0) | 3 (33) | 0 (0) | 0 (0) |
| Total | 34 | 32 | 3 | 9 | 2 | 2 |
Abbreviations: E. coli, Escherichia coli; K. pneumoniae, Klebsiella pneumoniae; K. oxytoca, Klebsiella oxytoca; E. cloacae, Enterobacter cloacae; K. ornithinolytica, Klebsiella ornithinolytica; S. enterica, Salmonella enterica; R, resistant.
Table 2B.
Antimicrobial susceptibility patterns of non-fermenter isolates
| Antibiotic | Resistant isolates, n (%)
|
||
|---|---|---|---|
| A. baumannii | P. aeruginosa | S. maltophilia | |
|
| |||
| R | R | R | |
| Ampicillin | 12 (100) | 6 (100) | 2 (100) |
| Amoxicillin/clavulanic acid | 10 (83.4) | 6 (100) | 2 (100) |
| Ampicillin/sulbactam | 6 (50) | 6 (100) | 2 (100) |
| Piperacillin/tazobactam | 9 (75) | 2 (33) | 0 (0) |
| Aztreonam | 8 (66.6) | 3 (50) | 2 (100) |
| Meropenem | 9 (75) | 0 (0) | 2 (100) |
| Imipenem | 10 (83.4) | 0 (0) | 2 (100) |
| Cefoxitin | 12 (100) | 6 (100) | 2 (100) |
| Cefepime | 12 (100) | 3 (50) | 2 (100) |
| Ceftazidime | 10 (83.4) | 2 (33) | 0 (0) |
| Cefotaxime | 10 (83.4) | 6 (100) | 2 (100) |
| Ceftriaxone | 8 (66.6) | 4 (67) | 2 (100) |
| Amikacin | 9 (75) | 0 (0) | 0 (0) |
| Gentamicin | 9 (75) | 2 (33) | 0 (0) |
| Tobramycin | 4 (33.4) | 0 (0) | 0 (0) |
| Ciprofloxacin | 10 (83.4) | 0 (0) | 0 (0) |
| Levofloxacin | 5 (41.6) | 2 (33) | 0 (0) |
| Trimethoprim/sulfamethoxazole | 9 (75) | 4 (67) | 0 (0) |
| Cefazolin | 12 (100) | 6 (100) | 2 (100) |
| Ertapenem | 10 (83.4) | 4 (67) | 2 (100) |
| Colistin | 2 (16.6) | 2 (33) | 0 (0) |
| Total | 12 | 6 | 2 |
Abbreviations: A. baumannii, Acinetobacter baumannii; P. aeruginosa, Pseudomonas aeruginosa; S. maltophilia, Stenotrophomonas maltophilia; R, resistant.
MIC against MDR Gram-negative isolates
All 27 MDR E. coli and 23 K. pneumoniae isolates had high MIC to ceftriaxone; therefore, they were considered as potential ESBL producers according to the CLSI guidelines.14 Table 3 shows resistance profiles for MDR Enterobacteriaceae including E. coli (27/70, 38.6%), K. pneumoniae (24/70, 34.3%), E. cloacae (4/70, 5.7%), K. oxytoca (2/70, 2.8%), and K. ornithinolytica (2/70, 2.8%). Table 4 shows resistance profiles for non-fermenter MDR GNB isolates including A. baumannii (9/70, 12.8%) and P. aeruginosa (2/70, 2.8%). The MIC50 (MIC at which 50% of the isolates were inhibited) values of MDR E. coli and K. pneumoniae are shown in Table 5. Overall, the MIC50 of ceftriaxone, cefepime, cephradine, or ampicillin was >512 μg/mL. Meropenem (4 μg/mL) and colistin (<1 μg/mL) had the lowest MIC50.
Table 3.
MIC (μg/mL) results for MDR Enterobacteriaceae isolates
| Number of isolates with MICs (μg/mL) indicated
|
||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| <1 | 1 | 2 | 4 | 8 | 16 | 32 | 64 | 128 | 256 | 512 | >512 | |
| E. coli (n=27) | ||||||||||||
| SAM | 0 | 0 | 0 | 0 | 0 | 0 | R/1 | R/6 | R/1 | R/3 | R/4 | R/12 |
| AK | 0 | 0 | 0 | S/2 | S/2 | S/3 | I/11 | 0 | 0 | 0 | R/1 | R/8 |
| CE | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/5 | R/22 |
| CRO | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/10 | R/17 |
| FEP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/4 | R/23 |
| MEM | S/3 | S/9 | 0 | R/3 | R/3 | R/3 | R/2 | R/2 | R/2 | 0 | 0 | 0 |
| AMP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 | R/25 |
| LEV | 0 | 0 | 0 | I/1 | 0 | 0 | 0 | R/2 | R/3 | R/5 | R/8 | R/8 |
| CT | S/27 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| K. pneumoniae (n=24) | ||||||||||||
| SAM | 0 | 0 | 0 | 0 | 0 | 0 | R/4 | 0 | R/3 | R/2 | R/6 | R/9 |
| AK | 0 | 0 | 0 | S/2 | S/1 | S/2 | I/3 | 0 | R/2 | 0 | R/2 | R/12 |
| CE | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/24 |
| CRO | 0 | S/2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/7 | R/15 |
| FEP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/1 | R/2 | 0 | R/21 |
| MEM | S/7 | S/4 | I/2 | R/3 | R/1 | R/2 | R/2 | 0 | R/1 | R/2 | 0 | 0 |
| AMP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 | R/22 |
| LEV | 0 | 0 | S/5 | 0 | R/2 | 0 | R/2 | R/3 | R/1 | R/2 | R/3 | R/6 |
| CT | S/21 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 | 0 | 0 | R/1 | 0 |
| E. cloacae (n=4) | ||||||||||||
| SAM | 0 | 0 | 0 | 0 | 0 | I/1 | R/3 | 0 | 0 | 0 | 0 | 0 |
| AK | 0 | 0 | 0 | 0 | 0 | S/3 | I/1 | 0 | 0 | 0 | 0 | 0 |
| CE | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/4 |
| CRO | 0 | S/3 | 0 | 0 | 0 | R/1 | 0 | 0 | 0 | 0 | 0 | 0 |
| FEP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/1 | R/3 |
| MEM | S/4 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| AMP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/4 |
| LEV | 0 | 0 | S/3 | 0 | R/1 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| CT | S/1 | 0 | 0 | 0 | 0 | R/2 | 0 | 0 | 0 | R/1 | 0 | 0 |
| K. oxytoca (n=2) | ||||||||||||
| SAM | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/1 | 0 | R/1 |
| AK | 0 | 0 | 0 | 0 | 0 | S/2 | 0 | 0 | 0 | 0 | 0 | 0 |
| CE | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 |
| CRO | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 |
| FEP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 |
| MEM | S/1 | S/1 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| AMP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 |
| LEV | 0 | 0 | 0 | 0 | 0 | R/1 | 0 | 0 | 0 | 0 | 0 | R/1 |
| CT | S/2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| K. ornithinolytica (n=2) | ||||||||||||
| SAM | 0 | 0 | 0 | 0 | 0 | 0 | R/1 | 0 | 0 | 0 | 0 | R/1 |
| AK | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/1 | 0 | 0 | 0 | R/1 |
| CE | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 |
| CRO | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/1 | R/1 |
| FEP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/1 | R/1 |
| MEM | S/1 | S/1 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| AMP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/1 | R/1 |
| LEV | 0 | 0 | 0 | I/2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| CT | S/2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
Abbreviations: MIC, minimum inhibitory concentration; MDR, multidrug resistant; E. coli, Escherichia coli; SAM, ampicillin/sulbactam; R, resistant; AK, amikacin; S, sensitive; I, intermediate; CE, cephradine; CRO, ceftriaxone; FEP, cefepime; MEM, meropenem; AMP, ampicillin; LEV, levofloxacin; CT, colistin; K. pneumoniae, Klebsiella pneumoniae; E. cloacae, Enterobacter cloacae; K. oxytoca, Klebsiella oxytoca; K. ornithinolytica, Klebsiella ornithinolytica.
Table 4.
MIC (μg/mL) results for MDR non-fermenter isolates
| Number of isolates with MICs (μg/mL) indicated
|
||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| <1 | 1 | 2 | 4 | 8 | 16 | 32 | 64 | 128 | 256 | 512 | >512 | |
| A. baumannii (n=9) | ||||||||||||
| SAM | 0 | 0 | 0 | 0 | 0 | I/2 | R/4 | 0 | 0 | R/1 | R/2 | 0 |
| AK | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 | R/3 | R/4 |
| CE | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/9 |
| CRO | 0 | 0 | 0 | 0 | S/3 | 0 | I/1 | 0 | 0 | 0 | 0 | R/5 |
| FEP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/3 | R/3 | 0 | 0 | R/3 |
| MEM | 0 | 0 | 0 | I/5 | 0 | R/3 | R/1 | 0 | 0 | 0 | 0 | 0 |
| AMP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/1 | R/8 |
| LEV | 0 | 0 | 0 | I/2 | 0 | R/2 | R/3 | R/1 | 0 | 0 | 0 | R/1 |
| CT | S/7 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 | 0 | 0 | 0 | 0 |
| P. aeruginosa (n=2) | ||||||||||||
| SAM | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/1 | R/1 | 0 | 0 |
| AK | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 |
| CE | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 |
| CRO | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 |
| FEP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 |
| MEM | 0 | S/2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| AMP | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 |
| LEV | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | R/2 |
| CT | 0 | 0 | 0 | 0 | 0 | R/1 | R/1 | 0 | 0 | 0 | 0 | 0 |
Abbreviations: MIC, minimum inhibitory concentration; MDR, multidrug resistant; A. baumannii, Acinetobacter baumannii; SAM, ampicillin/sulbactam; I, intermediate; R, resistant; AK, amikacin; CE, cephradine; CRO, ceftriaxone; S, sensitive; FEP, cefepime; MEM, meropenem; AMP, ampicillin; LEV, levofloxacin; CT, colistin; P. aeruginosa, Pseudomonas aeruginosa.
Table 5.
MIC50 (μg/mL) results for MDR isolates against some selected antimicrobial agents
| MDR GNB (n) | SAM | AK | CE | CRO | FEP | MEM | AMP | LEV | CT |
|---|---|---|---|---|---|---|---|---|---|
| E. coli (27) | 512 | 32 | >512 | >512 | >512 | 4 | >512 | 512 | <1 |
| K. pneumoniae (24) | 512 | >512 | >512 | >512 | >512 | 4 | >512 | 128 | <1 |
Abbreviations: MIC50, MIC at which 50% of the isolates were inhibited; MDR GNB, multidrug-resistant Gram-negative bacteria; SAM, ampicillin/sulbactam; AK, amikacin; CE, cephradine; CRO, ceftriaxone; FEP, cefepime; MEM, meropenem; AMP, ampicillin; LEV, levofloxacin; CT, colistin; E. coli, Escherichia coli; K. pneumoniae, Klebsiella pneumoniae.
Detection of resistance genes using PCR
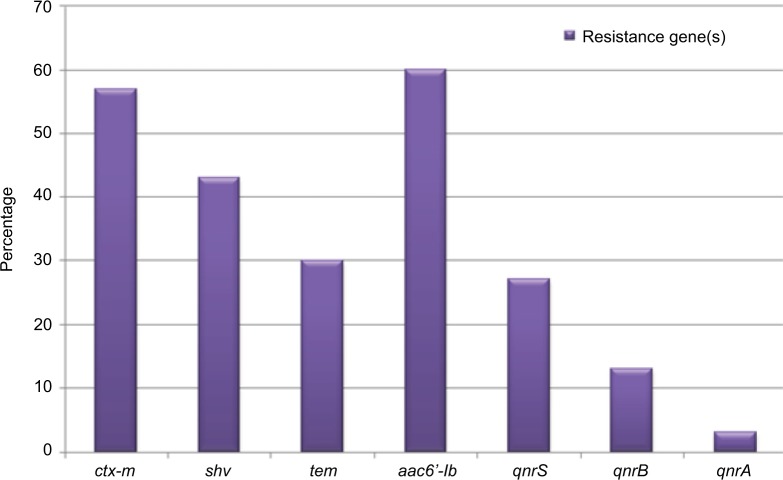
Out of the 70 MDR isolates, 13 (13/70, 18.6%), 7 (7/70, 10%), and 3 (3/70, 4.3%) isolates carried ctx-m, shv, and tem genes, respectively. While 11 isolates (11/70, 15.7%) carried the three tested genes together, 10 isolates (10/70, 14.3%) carried ctx-m and shv genes, 5 isolates (5/70, 7.1%) carried ctx-m and tem genes, and 3 isolates (3/70, 4.3%) carried shv and tem genes. Therefore, the most prevalent ESBL gene was ctx-m (39/70, 55.7%), followed by shv (31/70, 44.3%) and tem (22/70, 31.4%), as shown in Figure 1. Forty-two out of 70 MDR isolates (42/70, 60%) carried the aac(6′)-Ib/aac(6′)-Ib-cr gene. Concerning plasmid-mediated quinolone-resistance (PMQR) determinants, qnrS was more predominant (19/70, 27.1%), followed by qnrB (9/70, 12.8%) and qnrA (2/70, 2.8%), as shown in Figure 1.
Figure 1.
The prevalence of most common plasmid-mediated antimicrobial resistance genes among MDR GNB isolates.
Abbreviation: MDR GNB, multidrug-resistant Gram-negative bacteria.
Nucleotide accession codes
The PCR products of some selected plasmid-mediated resistant genes of certain MDR GNB isolates were verified by DNA sequencing. The final consensus sequences were analyzed and submitted into the NCBI GenBank database under the accession codes KX580955, KX580956, KY612437, KY612438, KY612439, KY612440, and KY612441.
Genotypes of MDR GNB isolates
A total of 22 different genotypes were obtained based on the detection of antimicrobial resistant genes on the extracted plasmids of the respective MDR GNB isolates, as shown in Table 6. The obtained genotypes have been associated with different sensitivity profiles against 21 tested antimicrobial agents. Statistical analysis showed that there were significant associations between members of FQs (such as ciprofloxacin and levofloxacin) and the detection of shv and aac(6′) genes; amikacin and the detection of shv, tem, and aac(6′) genes; members of carbapenems (such as meropenem, imipenem, and ertapenem) and the detection of shv, ctx-m, and aac(6′) genes (P-value <0.05), as shown in Table 6.
Table 6.
Percentage of different antimicrobial genotypes of MDR GNB isolates
| MDR GNB | Genotypes | No. of isolates (%a) | Significant associationsb | Pearson chi-square |
|---|---|---|---|---|
| Positive (n=58) | tem/shv/aac(6′)-Ib | 2 (3%) | Ciprofloxacin/shv | 0.022 |
| tem/shv/ctx-m/qnrS/aac(6′)-Ib | 3 (5%) | Ciprofloxacin/aac-6′ | 0.023 | |
| tem/shv/ctx-m/qnrB/aac(6′)-Ib | 2 (3%) | Levofloxacin/shv | 0.05 | |
| tem/shv/ctx-m/qnrB/qnrS/aac(6′)-Ib | 2 (3%) | Levofloxacin/aac-6′ | 0.03 | |
| tem/shv/ctx-m/qnrA/qnrS/a aac(6′)Ib | 2 (3%) | Amikacin/tem | 0.026 | |
| tem/shv/qnrS/aac(6′)-Ib | 2 (3%) | Amikacin/shv | 0.008 | |
| tem/ctx-m | 4 (7%) | Amikacin/aac-6′ | 0.031 | |
| tem/aac(6′)-Ib | 2 (3%) | Imipenem/shv | 0.037 | |
| tem/shv/ctx-m/aac(6′)-Ib | 3 (5%) | Imipenem/ctx-m | 0.022 | |
| shv/ctx-m | 3 (5%) | Meropenem/shv | 0.037 | |
| shv | 2 (3%) | Meropenem/ctx-m | 0.004 | |
| shv/aac(6′)-Ib | 2 (3%) | meropenem/aac-6′ | 0.05 | |
| shv/qnrS/aac(6′)-Ib | 3 (5%) | ertapenem/shv | 0.026 | |
| shv/ctx-m/aac(6′)-Ib | 4 (7%) | ertapenem/ctx-m | 0.004 | |
| shv/ctx-m/qnrB/qnrS/aac-6′ | 1 (1.7%) | |||
| ctx-m | 3 (5%) | |||
| ctx-m/aac(6′)-Ib | 6 (10%) | |||
| ctx-m/qnrS | 2 (3%) | |||
| ctx-m/qnrB | 2 (3%) | |||
| ctx-m/qnrB/qnrS/aac(6′)-Ib | 2 (3%) | |||
| qnrS/aac(6′)-Ib | 2 (3%) | |||
| aac(6′)-Ib | 4 (7%) | |||
| Negative (n=12) | – | 12 (17) |
Notes: Genotypes, plasmid-mediated antimicrobial resistance.
Percentages were calculated with reference to the number positive MDR GNB.
Significant association between antibiotic resistance and PCR detection of the respective gene on plasmids.
Abbreviations: MDR GNB, multidrug-resistant Gram-negative bacteria; PCR, polymerase chain reaction.
Combinations of antibiotics
All MDR GNB were tested against five different antibiotic combinations (ampicillin/sulbactam plus ceftriaxone, ampicillin/sulbactam plus amikacin, levofloxacin plus amikacin, ampicillin/sulbactam plus meropenem, and colistin plus meropenem) and the FICI was calculated for each combination. It was found that ampicillin/sulbactam plus ceftriaxone combination showed synergism against 29/70 (41.4%) isolates, while ampicillin/sulbactam plus amikacin combination showed synergism against 19/70 (27.1%) isolates. Tables 7–11 show the FICIs for five different antibiotic combinations for MDR E. coli, K. pneumoniae, A. baumannii, E. cloacae, and other MDR isolates, respectively.
Table 7.
FICI calculated for five different antibiotic combinations for MDR E. coli isolates
| No. | SAM + CRO
|
SAM + AK
|
AK + LEV
|
SAM + MEM
|
CT + MEM
|
|||||
|---|---|---|---|---|---|---|---|---|---|---|
| FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | |
| 1 | 2 | Indifference | 2 | Indifference | 2.75 | Indifference | 1.5 | Indifference | 2 | Indifference |
| 2 | 1.67 | Indifference | 2.5 | Indifference | 2 | Indifference | 1.67 | Indifference | 2 | Indifference |
| 3 | 1.75 | Indifference | 1 | Additive | 2 | Indifference | 1.125 | Indifference | 1 | Additive |
| 4 | 0.5 | Synergism | 1.5 | Indifference | 1.37 | Indifference | 1 | Additive | 2 | Indifference |
| 5 | 2 | Indifference | 2 | Indifference | 1.5 | Indifference | 1.1 | Indifference | 1.1 | Indifference |
| 6 | 0.145 | Synergism | 0.145 | Synergism | 0.02 | Synergism | 1 | Additive | 2 | Indifference |
| 7 | 2 | Indifference | 0.11 | Synergism | 0.27 | Synergism | 0.53 | Additive | 1.167 | Indifference |
| 8 | 1.75 | Indifference | 2.6 | Indifference | 2 | Indifference | 1 | Additive | 2 | Indifference |
| 9 | 1 | Additive | 0.5 | Synergism | 0.2 | Synergism | 1.16 | Indifference | 2 | Indifference |
| 10 | 0.36 | Synergism | 0.5 | Synergism | 0.26 | Synergism | 1 | Additive | 1.6 | Indifference |
| 11 | 0.75 | Additive | 2 | Indifference | 2 | Indifference | 1.5 | Indifference | 2 | Indifference |
| 12 | 0.3 | Synergism | 1.5 | Indifference | 2.125 | Indifference | 1 | Additive | 2 | Indifference |
| 13 | 0.27 | Synergism | 3 | Indifference | 0.3 | Synergism | 1 | Additive | 2 | Indifference |
| 14 | 0.27 | Synergism | 1.5 | Indifference | 2.125 | Indifference | 1 | Additive | 2 | Indifference |
| 15 | 0.3 | Synergism | 1 | Additive | 1 | Additive | 1 | Additive | 2 | Indifference |
| 16 | 0.3 | Synergism | 1 | Additive | 1.25 | Indifference | 1 | Additive | 2 | Indifference |
| 17 | 1.5 | Indifference | 1.1 | Indifference | 1.1 | Indifference | 1.1 | Indifference | 1.2 | Indifference |
| 18 | 1.75 | Indifference | 2.6 | Indifference | 2 | Indifference | 1 | Additive | 2 | Indifference |
| 19 | 1 | Additive | 0.5 | Synergism | 0.2 | Synergism | 1.16 | Indifference | 2 | Indifference |
| 20 | 0.36 | Synergism | 0.5 | Synergism | 0.26 | Synergism | 1 | Additive | 1.6 | Indifference |
| 21 | 2 | Indifference | 2 | Indifference | 2.75 | Indifference | 1.5 | Indifference | 2 | Indifference |
| 22 | 1.67 | Indifference | 2.5 | Indifference | 2 | Indifference | 1.67 | Indifference | 2 | Indifference |
| 23 | 1.75 | Indifference | 1 | Additive | 2 | Indifference | 1.125 | Indifference | 1 | Additive |
| 24 | 0.3 | Synergism | 1 | Additive | 1.25 | Indifference | 1 | Additive | 2 | Indifference |
| 25 | 0.3 | Synergism | 1.5 | Indifference | 2.125 | Indifference | 1 | Additive | 2 | Indifference |
| 26 | 0.27 | Synergism | 1.5 | Indifference | 2.125 | Indifference | 1 | Additive | 2 | Indifference |
| 27 | 0.145 | Synergism | 0.145 | Synergism | 0.02 | Synergism | 1 | Additive | 2 | Indifference |
Note: Synergism ≤0.5, additive >0.5–1, indifference >1–4.0, antagonism >4.
Abbreviations: FICI, fractional inhibitory concentration index; MDR, multidrug resistant; E. coli, Escherichia coli; SAM, ampicillin/sulbactam; CRO, ceftriaxone; AK, amikacin; LEV, levofloxacin; MEM, meropenem; CT, colistin.
Table 8.
FICI calculated for five different antibiotic combinations for MDR K. pneumoniae isolates
| No. | SAM + CRO
|
SAM + AK
|
AK + LEV
|
SAM + MEM
|
CT + MEM
|
|||||
|---|---|---|---|---|---|---|---|---|---|---|
| FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | |
| 1 | 1.75 | Indifference | 2.33 | Indifference | 2.125 | Indifference | 1 | Additive | 2 | Indifference |
| 2 | 1 | Additive | 1.75 | Indifference | 0.52 | Additive | 1 | Additive | 2 | Indifference |
| 3 | 0.2 | Synergism | 2 | Indifference | 2 | Indifference | 1 | Additive | 1 | Additive |
| 4 | 0.2 | Synergism | 0.5 | Synergism | 0.5 | Synergism | 1 | Additive | 2 | Indifference |
| 5 | 0.59 | Additive | 0.3 | Synergism | 1 | Additive | 1.125 | Indifference | 1.3 | Indifference |
| 6 | 2 | Indifference | 1.5 | Indifference | 1.75 | Indifference | 1.2 | Indifference | 1 | Additive |
| 7 | 0.2 | Synergism | 0.4 | Synergism | 1 | Additive | 1 | Additive | 2 | Indifference |
| 8 | 1.5 | Indifference | 2 | Indifference | 1.2 | Indifference | 2 | Indifference | 1.7 | Indifference |
| 9 | 0.7 | Additive | 3 | Indifference | 1.5 | Indifference | 1 | Additive | 2 | Indifference |
| 10 | 0.36 | Synergism | 2 | Indifference | 2 | Indifference | 1 | Additive | 1.6 | Indifference |
| 11 | 0.26 | Synergism | 2 | Indifference | 1.16 | Indifference | 1.16 | Indifference | 2 | Indifference |
| 12 | 0.17 | Synergism | 3.5 | Indifference | 2 | Indifference | 1.16 | Indifference | 1.6 | Indifference |
| 13 | 0.6 | Additive | 1.1 | Indifference | 1 | Additive | 1 | Additive | 2 | Indifference |
| 14 | 0.8 | Additive | 2 | Indifference | 1.1 | Indifference | 0.6 | Additive | 1.25 | Indifference |
| 15 | 1 | Additive | 1 | Additive | 1.3 | Indifference | 1 | Additive | 2 | Indifference |
| 16 | 0.2 | Synergism | 2 | Indifference | 2 | Indifference | 1 | Additive | 1 | Additive |
| 17 | 0.6 | Additive | 1.1 | Indifference | 1 | Additive | 1 | Additive | 2 | Indifference |
| 18 | 0.2 | Synergism | 0.5 | Synergism | 0.5 | Synergism | 1 | Additive | 2 | Indifference |
| 19 | 0.36 | Synergism | 2 | Indifference | 2 | Indifference | 1 | Additive | 1.6 | Indifference |
| 20 | 0.26 | Synergism | 2 | Indifference | 1.16 | Indifference | 1.16 | Indifference | 2 | Indifference |
| 21 | 1 | Additive | 1 | Additive | 1.3 | Indifference | 1 | Additive | 2 | Indifference |
| 22 | 1 | Additive | 1.75 | Indifference | 0.52 | Additive | 1 | Additive | 2 | Indifference |
| 23 | 2 | Indifference | 1.5 | Indifference | 1.75 | Indifference | 1.2 | Indifference | 1 | Additive |
| 24 | 1.5 | Indifference | 2 | Indifference | 1.2 | Indifference | 2 | Indifference | 1.7 | Indifference |
Note: Synergism ≤0.5, additive >0.5–1, indifference >1–4.0, antagonism >4.
Abbreviations: FICI, fractional inhibitory concentration index; MDR, multidrug resistant; K. pneumoniae, Klebsiella pneumoniae; SAM, ampicillin/sulbactam; CRO, ceftriaxone; AK, amikacin; LEV, levofloxacin; MEM, meropenem; CT, colistin.
Table 9.
FICI calculated for five different antibiotic combinations for MDR A. baumannii isolates
| No. | SAM + CRO
|
SAM + AK
|
AK + LEV
|
SAM + MEM
|
CT + MEM
|
|||||
|---|---|---|---|---|---|---|---|---|---|---|
| FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | |
| 1 | 0.66 | Additive | 4.1 | Antagonism | 1.1 | Indifference | 1 | Additive | 1.67 | Indifference |
| 2 | 1.5 | Indifference | 0.75 | Additive | 1.1 | Additive | 2.125 | Indifference | 4 | Indifference |
| 3 | 2 | Indifference | 2.05 | Indifference | 2.02 | Indifference | 0.6 | Additive | 1.3 | Indifference |
| 4 | 0.75 | Additive | 0.59 | Additive | 1.1 | Indifference | 1.125 | Indifference | 1.3 | Indifference |
| 5 | 0.5 | Synergism | 0.45 | Synergism | 0.5 | Synergism | 1 | Additive | 1 | Additive |
| 6 | 0.87 | Additive | 0.22 | Synergism | 1 | Additive | 1.125 | Indifference | 1.1 | Indifference |
| 7 | 2 | Indifference | 2.05 | Indifference | 2.02 | Indifference | 0.6 | Additive | 1.3 | Indifference |
| 8 | 1.5 | Indifference | 0.75 | Additive | 1.1 | Additive | 2.125 | Indifference | 4 | Indifference |
| 9 | 0.87 | Additive | 0.22 | Synergism | 1 | Additive | 1.125 | Indifference | 1.1 | Indifference |
Note: Synergism ≤0.5, additive >0.5–1, indifference >1–4.0, antagonism >4.
Abbreviations: FICI, fractional inhibitory concentration index; MDR, multidrug resistant; A. baumannii, Acinetobacter baumannii; SAM, ampicillin/sulbactam; CRO, ceftriaxone; AK, amikacin; LEV, levofloxacin; MEM, meropenem; CT, colistin.
Table 10.
FICI calculated for five different antibiotic combinations for MDR E. cloacae isolates
| No. | SAM + CRO
|
SAM + AK
|
AK + LEV
|
SAM + MEM
|
CT + MEM
|
|||||
|---|---|---|---|---|---|---|---|---|---|---|
| FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | |
| 1 | 0.75 | Additive | 0.5 | Synergism | 1.3 | Indifference | 1.16 | Indifference | 1.3 | Indifference |
| 2 | 1.16 | Indifference | 0.5 | Synergism | 1.16 | Indifference | 1.16 | Indifference | 1 | Additive |
| 3 | 1.3 | Indifference | 0.6 | Additive | 1.3 | Indifference | 1.3 | Indifference | 2 | Indifference |
| 4 | 1.16 | Indifference | 0.5 | Synergism | 1.16 | Indifference | 1.16 | Indifference | 1 | Additive |
Note: Synergism ≤0.5, additive >0.5–1, indifference >1–4.0, antagonism >4.
Abbreviations: FICI, fractional inhibitory concentration index; MDR, multidrug resistant; E. cloacae, Enterobacter cloacae; SAM, ampicillin/sulbactam; CRO, ceftriaxone; AK, amikacin; LEV, levofloxacin; MEM, meropenem; CT, colistin.
Table 11.
FICI calculated for five different antibiotic combinations for other MDR isolates
| No. | SAM + CRO
|
SAM + AK
|
AK + LEV
|
SAM + MEM
|
CT + MEM
|
|||||
|---|---|---|---|---|---|---|---|---|---|---|
| FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | FICI | Interpretation | |
| 1* | 0.29 | Synergism | 0.04 | Synergism | 0.6 | Additive | 1 | Additive | 1.1 | Indifference |
| 2* | 0.29 | Synergism | 0.04 | Synergism | 0.6 | Additive | 1 | Additive | 1.1 | Indifference |
| 3* | 0.35 | Synergism | 1.1 | Indifference | 2 | Indifference | 1 | Additive | 2 | Indifference |
| 4* | 1 | Additive | 1.1 | Indifference | 2 | Indifference | 1 | Additive | 2 | Indifference |
| 5* | 0.5 | Synergism | 0.75 | Additive | 1.1 | Additive | 1.2 | Indifference | 2 | Indifference |
| 6* | 0.5 | Synergism | 0.75 | Additive | 1.1 | Additive | 1.2 | Indifference | 2 | Indifference |
Notes: 1*, 2*, P. aeruginosa; 3*, 4*, K. oxytoca; 5*, 6*, K. ornithinolytica. Synergism ≤0.5, additive >0.5–1, indifference >1–4.0, antagonism >4.
Abbreviations: FICI, fractional inhibitory concentration index; MDR, multidrug resistant; SAM, ampicillin/sulbactam; CRO, ceftriaxone; AK, amikacin; LEV, levofloxacin; MEM, meropenem; CT, colistin; P. aeruginosa, Pseudomonas aeruginosa; K. oxytoca, Klebsiella oxytoca; K. ornithinolytica, Klebsiella ornithinolytica.
Discussion
BSI remains a major cause of life-threatening complications in patients with cancer23 and is directly associated with prolonged hospital stay, high health care costs, and increased risk of morbidity and mortality.24,25 Bacteria are the most common cause of such infections.26,27 Resistance to antibiotics is a persistent and a difficult clinical problem that is compounded by a shortage of new therapeutic compounds.28 BSIs due to GNB are common in cancer patients during aggressive therapy.4 Therefore, in this study, we evaluated both the phenotypic and genotypic bases of antimicrobial resistance of certain clinically relevant MDR GNB isolated from cancer patients against the most common antimicrobial agents used in treatment. In addition, the efficacy of some antibiotic combinations has been evaluated against such MDR GNB pathogens. In the present study, the frequency of Gram-negative isolates was slightly higher than that of Gram-positive isolates. On the contrary, another study conducted in Egypt reported that Gram-positive organisms were the predominant causative agents of BSI in cancer patients constituting about 72% compared to 24% of the Gram-negative organisms.29 The results showed that the 34 E. coli isolates were resistant to ampicillin, while the most effective antimicrobial agents were colistin, amikacin, and imipenem followed by meropenem and ertapenem. Another study by Al-Mulla et al reported that E. coli isolates were highly susceptible to imipenem, meropenem, piperacillin/tazobactam, and amikacin, and less susceptible to gentamicin (55%) and ciprofloxacin (78%).30 In the present study, K. pneumoniae isolates showed high susceptibility to colistin and were less susceptible to amikacin, imipenem, meropenem, and gentamicin. In another study conducted by Xiao et al, K. pneumoniae bloodstream isolates showed threatened resistance to the most of routine antibiotics and only meropenem, imipenem, amikacin, and piperacillin/tazobactam had relative low resistant rates.
In this study, 68.6% of isolates were resistant to three or more classes of antimicrobial agents and therefore considered MDR isolates. This finding agreed with the study conducted in Egypt by El-Mahallawy et al who reported that MDR was identified in 69% of bacteria isolated from positive blood cultures. This is due to the increasing use of chemotherapy and other immunosuppressive treatments, which result in more prevalent infections and reliance on antibiotic treatment, giving rise to a variety of resistant microbes.32
According to the 2017 guidelines on antimicrobial therapy, particularly the San Francisco Medical Center Guidelines, either cefepime or piperacillin/tazobactam is listed as an initial therapy in febrile neutropenic cancer patients.33 While according to our findings, the recovered GNB including E. coli, K. pneumoniae, and A. baumannii showed higher resistance to these two antibiotics, which are listed in most guidelines (94%, 75%, and 100% resistance to cefepime and 76%, 81.25%, and 75% resistance to piperacillin/tazobactam for the abovementioned bacteria, respectively). This finding is of great concern regarding failure of the abovementioned antibiotic regimens for use in this serious clinical condition and could be one of the major causes for increasing morbidity and mortality of cancer patients with BSI, particularly in our region. However, according to the results, the recovered clinically relevant GNB such as E. coli, K. pneumoniae, A. baumannii, and other GNB showed the lowest resistance to both carbapenems (i.e., meropenem, imipenem, ertapenem) and colistin. Therefore, the findings support use of either carbapenems or colistin as antimicrobial monotherapy for febrile neutropenic cancer patients especially for the refractory MDR GNB infections. It is advised that the aforementioned antibiotics be included in forthcoming guidelines.
Also, the study focused on the detection of the clinically relevant plasmid-mediated antimicrobial resistant genes that confer resistance to most of the antibiotics commonly used in the treatment of BSI in cancer patients such as ESBLs, aac(6′)-Ib, and most common PMQR genes (aac(6′)-Ib-cr, qnrA, qnrB, qnrS).20–22,34–37 The most prevalent ESBL genes in Gram-negative isolates in the study in decreasing order were ctx-m, shv, and tem. This finding agreed with the study conducted by Mathlouthi et al who reported that ctx-m was the most frequently detected (54%) gene.38 However, by contrast, Hamdy Mohammed el et al found that 72.7% of the isolates carried tem, 36 % harbored ctx-m, and 15% showed shv.39
Recent studies focused on the increasing occurrence of the high-level resistance to aminoglycosides. Therefore, there is a need to regularly update the prevalent aminoglycoside resistance mechanisms.40 In the present study, 42 MDR isolates carried the aac(6′)-Ib/aac(6′)-Ib-cr gene: 16 isolates (16/42, 38.1%) were E. coli, 14 isolates (14/42, 33.3%) were K. pneumoniae, 8 isolates (8/42, 19%) were A. baumannii, 2 isolates (2/42, 4.8%) were K. oxytoca, and 2 isolates (2/42, 4.8%) were E. cloacae. However, by contrast, in microorganisms tested in the study conducted by Ndegwa et al, the enzyme AAC(6′)-Ib-cr occurred at a frequency of 22% in Klebsiella spp., 19% in P. aeruginosa, 14% in E. coli, and 5% in A. baumannii.41 The level of resistance that increased by 40% over time may be attributed to the presence of this enzyme, which is not only highly transferable as it is located within integrons and transposons but has been seen to coexist with other antibiotic-inactivating enzymes such as ESBLs.
The study focused on the detection of the most common PMQR genes because of their role in preparing the bacteria for high-level resistance to FQs. This is in line with other reports suggesting that the presence of PMQR genes could facilitate the accumulation of multiple chromosomal mutations in the genes coded for topoisomerase II or IV, leading to higher level of FQ resistance.42 In this study, out of the 70 MDR isolates, 19 (19/70, 27.1%), 9 (9/70, 12.8%), and 2 (2/70, 2.8%) isolates carried qnrS, qnrB, and qnrA genes, respectively. Nevertheless, in the study of El-Sokkary and Abdelmegeed (2015), the rate of presence of qnrB (49 isolates) was higher compared to that of qnrS and qnrA (14 and 24 isolates, respectively).43
In addition, there was no significant correlation between the presence of PMQR genes and resistance to FQs, which means that PMQR alone did not confer resistance to FQs. Some GNB were found to be ciprofloxacin resistant and PMQR positive, while others were ciprofloxacin resistant and PMQR negative. Therefore, the resistance to FQs was usually attributed to the copresence of other important antimicrobial resistant genes such as ESBL or aac(6′)-Ib even on the same plasmid.
Therefore, use of FQs for prophylaxis in cancer patients should be reconsidered because they can result in increasing copy number of plasmids carrying PMQR and other resistant genes such as ESBLs and, therefore, render these patients unsusceptible in the future to important classes of antimicrobial agents such as β-lactams, aminoglycosides, and FQs.
Since antibiotic combinations may play an important role in combating microbial resistance,44 various antibiotic combinations in the present study were evaluated for their efficacy on the respective clinically relevant MDR GNB. The FICIs for ampicillin/sulbactam plus ceftriaxone, ampicillin/sulbactam plus amikacin, and amikacin plus levofloxacin showed significant synergistic effects against 29 (29/70, 41.4%), 19 (19/70, 27.1%), and 11 (11/70, 15.7%) isolates of the tested MDR GNB isolates, respectively. Accordingly, new empirical antibiotics particularly colistin or meropenem, or both should be administered against the MDR GNB in the neutropenic cancer patients in our region. The results indicate high prevalence of antibiotic resistance among MDR isolates. Therefore, new guidelines should be implemented in Egypt to rationalize the use and avoid the misuse and abuse of antimicrobial agents.
Conclusion
High prevalence of microbial resistance was detected among MDR GNB against penicillins; monobactams; third- and fourth-generation cephalosporins, particularly cefepime, which is described by several antimicrobial therapy guidelines for febrile neutropenic cancer patients. On the other hand, qualitative and quantitative susceptibility testing proved that carbapenem or colistin alone showed the lowest resistance; therefore, we recommended their use as initial monotherapy in treatment of MDR GNB in our region. The presence of PMQR genes was not reflected by resistance to FQ, and it was usually copresent with other important antimicrobial resistant genes such as ESBL or aac(6′)-Ib even on the same plasmid. Accordingly, PMQR detection should be performed not for FQs resistance but for their role in conferring resistance on other important classes of antibiotics. Three antibiotic combinations including ampicillin/sulbactam plus ceftriaxone, ampicillin/sulbactam plus amikacin, and amikacin plus levofloxacin showed synergism against most of the tested MDR GNB isolates.
Acknowledgments
The authors are grateful to the Department of Microbiology and Immunology, Faculty of Pharmacy For Girls, Al-Azhar University, Egypt, for providing the laboratory facilities for this work. The authors would also like to acknowledge the Microbiology Laboratory of the National Cancer Institute, Cairo University, for providing the clinical specimens.
Footnotes
Disclosure
The authors report no conflicts of interest in this work.
References
- 1.Kuo FC, Wang SM, Shen CF, et al. Bloodstream infections in pediatric patients with acute leukemia: emphasis on gram-negative bacteria infections. J Microbiol Immunol Infect. 2017;50(4):507–513. doi: 10.1016/j.jmii.2015.08.013. [DOI] [PubMed] [Google Scholar]
- 2.Baos E, Candel FJ, Merino P, Pena I, Picazo JJ. Characterization and monitoring of linezolid-resistant clinical isolates of Staphylococcus epidermidis in an intensive care unit 4 years after an outbreak of infection by cfr-mediated linezolid-resistant Staphylococcus aureus. Diagn Microbiol Infect Dis. 2013;76(3):325–329. doi: 10.1016/j.diagmicrobio.2013.04.002. [DOI] [PubMed] [Google Scholar]
- 3.Biehl LM, Schmidt-Hieber M, Liss B, Cornely OA, Vehreschild MJ. Colonization and infection with extended spectrum beta-lactamase producing Enterobacteriaceae in high-risk patients – review of the literature from a clinical perspective. Crit Rev Microbiol. 2016;42(1):1–16. doi: 10.3109/1040841X.2013.875515. [DOI] [PubMed] [Google Scholar]
- 4.Saghir S, Faiz M, Saleem M, Younus A, Aziz H. Characterization and anti-microbial susceptibility of gram-negative bacteria isolated from bloodstream infections of cancer patients on chemotherapy in Pakistan. Indian J Med Microbiol. 2009;27(4):341–347. doi: 10.4103/0255-0857.55454. [DOI] [PubMed] [Google Scholar]
- 5.Pitout JD, Laupland KB. Extended-spectrum beta-lactamase-producing Enterobacteriaceae: an emerging public-health concern. Lancet Infect Dis. 2008;8(3):159–166. doi: 10.1016/S1473-3099(08)70041-0. [DOI] [PubMed] [Google Scholar]
- 6.Bialvaei AZ, Samadi Kafil H. Colistin, mechanisms and prevalence of resistance. Curr Med Res Opin. 2015;31(4):707–721. doi: 10.1185/03007995.2015.1018989. [DOI] [PubMed] [Google Scholar]
- 7.Hirsch EB, Tam VH. Detection and treatment options for Klebsiella pneumoniae carbapenemases (KPCs): an emerging cause of multidrug-resistant infection. J Antimicrob Chemother. 2010;65(6):1119–1125. doi: 10.1093/jac/dkq108. [DOI] [PubMed] [Google Scholar]
- 8.Zarkotou O, Pournaras S, Tselioti P, et al. Predictors of mortality in patients with bloodstream infections caused by KPC-producing Klebsiella pneumoniae and impact of appropriate antimicrobial treatment. Clin Microbiol Infect. 2011;17(12):1798–1803. doi: 10.1111/j.1469-0691.2011.03514.x. [DOI] [PubMed] [Google Scholar]
- 9.Qureshi ZA, Paterson DL, Potoski BA, et al. Treatment outcome of bacteremia due to KPC-producing Klebsiella pneumoniae: superiority of combination antimicrobial regimens. Antimicrob Agents Chemother. 2012;56(4):2108–2113. doi: 10.1128/AAC.06268-11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Gutiérrez-Gutiérrez B, Salamanca E, de Cueto M, et al. Investigators from the REIPI/ESGBIS/INCREMENT Group A predictive model of mortality in patients with bloodstream infections due to carbapenemase-producing Enterobacteriaceae. Mayo Clin Proc. 2016;91(10):1362–1371. doi: 10.1016/j.mayocp.2016.06.024. [DOI] [PubMed] [Google Scholar]
- 11.Akova M, Daikos GL, Tzouvelekis L, Carmeli Y. Interventional strategies and current clinical experience with carbapenemase-producing gram-negative bacteria. Clin Microbiol Infect. 2012;18(5):439–448. doi: 10.1111/j.1469-0691.2012.03823.x. [DOI] [PubMed] [Google Scholar]
- 12.Bauer AW, Kirby WM, Sherris JC, Truck M. Antibiotic susceptibility testing by a standardized signal disc method. Am J Clin Pathol. 1996;45(4):493–496. [PubMed] [Google Scholar]
- 13.Andrews JM. Determination of minimum inhibitory concentrations. J Antimicrob Chemother. 2002;49(6):1049. doi: 10.1093/jac/48.suppl_1.5. [DOI] [PubMed] [Google Scholar]
- 14.CLSI document M100–S24 . CLSI document M100–S24. Wayne, PA: CLSI; 2014. 2014. [Accessed May 9, 2018]. Performance Standards for Antimicrobials Susceptibility Testing; Twenty-Fourth Informational Supplement. webpage on the Internet. Available from: https://www.aacc.org/store/books/9200/performance-standards-for-antimicrobial-susceptibility-testing. [Google Scholar]
- 15.Magiorakos AP, Srinivasan A, Carey RB, et al. Multidrug-resistant, extensively drug-resistant and pandrug-resistant bacteria: an international expert proposal for interim standard definitions for acquired resistance. Clin Microbiol Infect. 2012;18(3):268–281. doi: 10.1111/j.1469-0691.2011.03570.x. [DOI] [PubMed] [Google Scholar]
- 16.Hsieh MH, Yu CM, Yu VL, Chow JW. Synergy assessed by checkerboard. A critical analysis. Diagn Microbiol Infect Dis. 1993;16(4):343–349. doi: 10.1016/0732-8893(93)90087-n. [DOI] [PubMed] [Google Scholar]
- 17.Odds FC. Synergy, antagonism, and what the chequerboard puts between them. J Antimicrob Chemother. 2003;52(1):1. doi: 10.1093/jac/dkg301. [DOI] [PubMed] [Google Scholar]
- 18.Sambrook JJ, Russell DDW. Molecular Cloning: A Laboratory Manual. 3rd ed. New York: Cold Spring Harbor Laboratory Press; 2001. [Google Scholar]
- 19.Staden R. The Staden sequence analysis package. Mol Biotechnol. 1996;5(3):233–241. doi: 10.1007/BF02900361. [DOI] [PubMed] [Google Scholar]
- 20.Bonnet R, Dutour C, Sampaio JL, et al. Novel cefotaximase (CTX-M-16) with increased catalytic efficiency due to substitution Asp-240-->Gly. Antimicrob Agents Chemother. 2001;45(8):2269–2275. doi: 10.1128/AAC.45.8.2269-2275.2001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Rasheed JK, Jay C, Metchock B, et al. Evolution of extended-spectrum beta-lactam resistance (SHV-8) in a strain of Escherichia coli during multiple episodes of bacteremia. Antimicrob Agents Chemother. 1997;41(3):647–653. doi: 10.1128/aac.41.3.647. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Hamed SM, Aboshanab KM, El-Mahallawy HA, Helmy MM, Ashour SA, Elkhatib WF. Plasmid-mediated quinolone resistance in Gram-negative pathogens isolated from cancer patients in Egypt. Microb Drug Resist. 2018 Mar 13; doi: 10.1089/mdr.2017.0354. Epub. [DOI] [PubMed] [Google Scholar]
- 23.Montassier E, Batard E, Gastinne T, Potel G, de La Cochetière MF. Recent changes in bacteremia in patients with cancer: a systematic review of epidemiology and antibiotic resistance. Eur J Clin Microbiol Infect Dis. 2013;32(7):841–850. doi: 10.1007/s10096-013-1819-7. [DOI] [PubMed] [Google Scholar]
- 24.Howard DH, Scott RD, 2nd, Packard R, Jones D. The global impact of drug resistance. Clin Infect Dis. 2003;36(Suppl 1):S4–S10. doi: 10.1086/344656. [DOI] [PubMed] [Google Scholar]
- 25.Kuderer NM, Dale DC, Crawford J, Cosler LE, Lyman GH. Mortality, morbidity, and cost associated with febrile neutropenia in adult cancer patients. Cancer. 2006;106(10):2258–2266. doi: 10.1002/cncr.21847. [DOI] [PubMed] [Google Scholar]
- 26.Kjellander C, Björkholm M, Cherif H, Kalin M, Giske CG. Hematological: low all-cause mortality and low occurrence of antimicrobial resistance in hematological patients with bacteremia receiving no antibacterial prophylaxis: a single-center study. Eur J Haematol. 2012;88(5):422–430. doi: 10.1111/j.1600-0609.2012.01768.x. [DOI] [PubMed] [Google Scholar]
- 27.Miedema KG, Winter RH, Ammann RA, et al. Bacteria causing bacteremia in pediatric cancer patients presenting with febrile neutropenia—species distribution and susceptibility patterns. Support Care Cancer. 2013;21(9):2417–2426. doi: 10.1007/s00520-013-1797-4. [DOI] [PubMed] [Google Scholar]
- 28.Ejim L, Farha MA, Falconer SB, et al. Combinations of antibiotics and nonantibiotic drugs enhance antimicrobial efficacy. Nat Chem Biol. 2011;7(6):348–350. doi: 10.1038/nchembio.559. [DOI] [PubMed] [Google Scholar]
- 29.El-Mahallawy HA, Hassan SS, El-Wakil M, Moneer MM, Shalaby L. Update on healthcare-associated blood stream infections in febrile neutropenic pediatric oncology patients. J Cancer Ther. 2015;6(6):504–510. doi: 10.7314/apjcp.2015.16.14.5691. [DOI] [PubMed] [Google Scholar]
- 30.Al-Mulla NA, Taj-Aldeen SJ, El Shafie S, Janahi M, Al-Nasser AA, Chandra P. Bacterial bloodstream infections and antimicrobial susceptibility pattern in pediatric hematology/oncology patients after anticancer chemotherapy. Infect Drug Resist. 2014;7:289–299. doi: 10.2147/IDR.S70486. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Xiao SZ, Wang S, Wu WM, et al. The resistance phenotype and molecular epidemiology of Klebsiella pneumoniae in bloodstream infections in Shanghai, China, 2012–2015. Front Microbiol. 2017;8:250. doi: 10.3389/fmicb.2017.00250. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.El-Mahallawy H, Samir I, Abdel Fattah R, Kadry D, El-Kholy A. Source, pattern and antibiotic resistance of blood stream infections in hematopoietic stem cell transplant recipients. J Egypt Natl Canc Inst. 2014;26(2):73–77. doi: 10.1016/j.jnci.2013.12.001. [DOI] [PubMed] [Google Scholar]
- 33.Maddix D, Lampiris H, Vu M. Guide to antimicrobials, Guidelines for Empiric Antimicrobial Therapy. San Francisco, CA: VA Medical Center, University of California; 2017. [Accessed May 9, 2018]. [webpage on the Internet] Available from: http://journals.jkuat.ac.ke/index.php/jscp/search/advancedResults. [Google Scholar]
- 34.Kiratisin P, Apisarnthanarak A, Laesripa C, Saifon P. Molecular characterization and epidemiology of extended-spectrum-beta-lactamase-producing Escherichia coli and Klebsiella pneumoniae isolates causing health care-associated infection in Thailand, where the CTX-M family is endemic. Antimicrob Agents Chemother. 2008;52(8):2818–2824. doi: 10.1128/AAC.00171-08. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.N G M, C Math G. Nagshetty K, Patil SA, Gaddad SM, Shivannavar CT. Antibiotic susceptibility pattern of ESβL producing Klebsiella pneumoniae isolated from urine samples of pregnant women in Karnataka. J Clin Diagn Res. 2014;8(10):DC08–DC11. doi: 10.7860/JCDR/2014/9594.5048. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Robicsek A, Jacoby GA, Hooper DC. The worldwide emergence of plasmid-mediated quinolone resistance. Lancet Infect Dis. 2006;6(10):629–640. doi: 10.1016/S1473-3099(06)70599-0. [DOI] [PubMed] [Google Scholar]
- 37.Paterson DL, Bonomo RA. Extended-spectrum beta-lactamases: a clinical update. Clin Microbiol Rev. 2005;18(4):657–686. doi: 10.1128/CMR.18.4.657-686.2005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Mathlouthi N, Al-Bayssari C, El Salabi A, et al. Carbapenemases and extended-spectrum β-lactamases producing Enterobacteriaceae isolated from Tunisian and Libyan hospitals. J Infect Dev Ctries. 2016;10(7):718–727. doi: 10.3855/jidc.7426. [DOI] [PubMed] [Google Scholar]
- 39.Hamdy Mohammed el S, Elsadek Fakhr A, Mohammed El Sayed H, Al Johery SA, Abdel Ghani Hassanein W. Spread of TEM, VIM, SHV, and CTX-M β-lactamases in imipenem-resistant gram-negative bacilli Isolated from Egyptian hospitals. Int J Microbiol. 2016;2016:8382605. doi: 10.1155/2016/8382605. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Ho PL, Leung LM, Chow KH, Lai EL, Lo WU, Ng TK. Prevalence of aminoglycoside modifying enzyme and 16S ribosomal RNA methylase genes among aminoglycoside-resistant Escherichia coli isolates. J Microbiol Immunol Infect. 2016;49(1):123–126. doi: 10.1016/j.jmii.2014.08.012. [DOI] [PubMed] [Google Scholar]
- 41.Ndegwa DW, Budambula NLM, Kariuki S, Revathi G, Kiiru JN. Aminoglycoside modifying enzymes detected in strains of Escherichia, Klebsiella, Pseudomonas and Acinetobacter implicated in invasive infections in Nairobi, Kenya; Proceeding of 2010 JKWAT Scientific Technological and Industrialization conference; Nairobi, Kenya. 17th–19th November 2010; [Accessed May 9, 2018]. [webpage on the Internet] Available from: http://journals.jkuat.ac.ke/index.php/jscp/article/view/685. [Google Scholar]
- 42.Kim NH, Choi EH, Sung JY, et al. Prevalence of plasmid-mediated quinolone resistance genes and ciprofloxacin resistance in pediatric bloodstream isolates of Enterobacteriaceae over a 9-year period. Jpn J Infect Dis. 2013;66(2):151–154. doi: 10.7883/yoken.66.151. [DOI] [PubMed] [Google Scholar]
- 43.El-Sokkary MMA, Abdelmegeed ES. Antibacterial resistance pattern among Escherichia coli strains isolated from Mansoura hospitals in Egypt with a special reference quinolones. Afr J Microbiol Res. 2015;9(9):662–670. [Google Scholar]
- 44.Abdelkader MM, Aboshanab KM, El-Ashry MA, Aboulwafa MM. Prevalence of MDR pathogens of bacterial meningitis in Egypt and new synergistic antibiotic combinations. PLoS One. 2017;12(2):e0171349. doi: 10.1371/journal.pone.0171349. [DOI] [PMC free article] [PubMed] [Google Scholar]